Abstract
Background:
Sleep disturbance and insomnia are common adverse events in patients with breast cancer (BC). Traditional Chinese Medicine (TCM) treatment for sleep disturbance includes acupuncture, acupressure, auricular acupressure/auricular acupuncture, and Qigong. However, the specific efficacy of these TCM treatment remains unclear.
Materials and Methods:
This systematic review and network meta-analysis (NMA) investigated the effects of various TCM treatment on improving sleep quality in BC survivors.
Methods:
Only randomized controlled trials (RCTs) reporting the results of TCM treatments were included. The main NMA included 12 RCTs involving 1011 participants. The risk of bias was assessed using the RoB 2 tool for randomized controlled trials. The certainty of evidence of the NMA was assessed in accordance with GRADE (the Grading of Recommendations, Assessment, Development, and Evaluations).
Results:
Acupressure, acupuncture, auricular acupuncture/auricular acupressure, and qigong were identified as optimal TCM treatment (P < .05) for enhancing sleep quality in BC survivors.
Conclusion:
Our results provide some evidence that TCM treatment, particularly acupressure, can be beneficial in improving sleep quality in BC survivors. However, larger-scale clinical trials with robust methodological designs are required to validate and extend our findings.
Introduction
Good sleep quality in breast cancer (BC) survivors is crucial because sleep ensures the adequate functioning of the immune system, including anticancer and anti-inflammatory activities. 1 However, sleep disturbance is a known side effect of cancer treatment, affecting physiological and psychological functions. Among patients with cancer, 25%–69% have sleeping difficulty, and 18% to 29% have insomnia.2 -4 The highest prevalence of sleep disturbance is reported in patients with breast cancer (BC, approximately 50%). 5 A study of 300 nonmetastatic BC survivors revealed that 51% of them experienced insomnia symptoms and that 19% met the diagnostic criteria for insomnia. 6 Sleep disorder plays a role in BC initiation and progression, which reduces patients’ quality of life and increases mortality.7 -9
The severity of sleep disturbances changes over time, with the most severe sleep disturbances during the chemotherapy phase of treatment. 10 The causes of sleep disturbance in patients with cancer are likely to be multifactorial, such as anticipatory anxiety, increased daytime napping impairing the circadian rhythm, and chemotherapy-induced inflammation. Adjuvant therapy may impair sleep quality through side effects, such as nocturnal hot flashes from chemotherapy or hormonal therapy,11 -14 chemotherapy-induced nausea and vomiting, 15 and pain associated with the use of aromatase inhibitors. 16 Many BC survivors take medications to manage their sleep disturbances. However, daily sedative use exerts adverse effects, such as cognitive impairment, increased risk of falls and fractures, and confusion1,17; therefore, the long-term use of hypnotics (>4 weeks) is not recommended. 18
BC survivors commonly seek complementary and alternative medicine (CAM) to manage treatment-related side effects. CAM is an umbrella term that includes alternative medical systems (such as Ayurveda, osteopathy, and TCM), mind-body interventions (such as meditation, biofeedback, and prayer), energy medicine (such as Qigong and Reiki), biological treatments (such as herbal medications and special diets), and manipulative/body-based practices (based on manipulation or body movements, including massage therapy).19,20 Traditional Chinese Medicine (TCM) is a type of CAM practiced in many parts of the world, and it is an empirical discipline with over 2000 years of accumulated knowledge and practice in East Asian countries.21,22 In recent years, TCM treatment has been employed to alleviate sleep disturbance in patients with BC; TCM treatment include qigong, acupressure, acupuncture, auricular acupressure/auricular acupuncture (AA/AT), and Chinese herbs.23 -27 However, the safety and toxicity of Chinese herbs should be considered before using them for treating sleep disturbance. 28
Qigong is a general term for traditional Chinese bioenergy exercises. It regulates individuals’ emotions, boosts their spirits, and ameliorates sleep dysfunction.29,30 Acupuncture, acupressure, and AA/AT are based on the same theories of meridians and involve stimulating acupoints to restore health and treat diseases 31 ; they regulate the balance of Yin and Yang, invigorate qi (energy), and nourish blood and body fluids. Acupuncture is a therapeutic procedure in which specific body areas or acupoints are pierced with fine needles 32 ; acupressure involves the application of light to moderate physical pressure by using the fingers, thumbs, or devices without needle insertion. 33
More randomized controlled trials (RCTs) are being conducted to assess the effects of TCM treatments on sleep disturbance in BC survivors; however, systematic reviews and meta-analyses only facilitate pairwise comparisons of qigong, acupuncture, and acupressure interventions and control conditions and cannot compare the effects of four interventions. To fill this research gap, we conducted a network meta-analysis (NMA) and systematic review to summarize the current evidence effects of qigong, acupuncture, acupressure, and AA/AT and consider their preferences with TCM remedies to provide an effective strategy for managing sleep disturbance.
Methods
This systematic review and NMA was conducted in accordance with the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) statement. 34 The protocol was registered with the International Prospective Register of Systematic Reviews (PROSPERO ID: CRD 42023369723).
Databases and Search Strategy
We searched the Embase, Cochrane Library, PubMed, ProQuest, Cinahl, OVID, and CNKI databases for relevant studies as well as identified ongoing unpublished trials through ClinicalTrials.gov (https://clinicaltrials.gov/). The Population, Intervention, Comparison, Outcome, and Study Type (PICOS) framework was applied to the search strategy for identifying eligible publications from inception to August 31, 2024. A search strategy for Embase is presented in Supplemental Table 1. Only RCTs were included. All search records were exported to Endnote reference managing software (V20, Thomson Reuters, Philadelphia, PA, USA).
Study Screening and Selection
First, 2 reviewers (CWC and SCW) independently screened the literature by screening the titles and abstracts and then reviewing the full text to determine which studies were eligible for inclusion. Any disagreement between the two researchers was resolved by a third reviewer (MYT). RCTs were included if they (1) included adult patients (age ≥ 18 years) with BC, regardless of the BC stage or treatment status (completed or ongoing); (2) involved qigong, acupuncture, acupressure, and AA/AT; and (3) involved one of the aforementioned TCM interventions and usual care, WLC, or other nonpharmacological interventions (eg, aerobic exercise, cognitive-behavioral therapy [CBT], and mindfulness-based stress reduction [MBSR] for insomnia) that were provided to improve sleep quality as the control arm. Concomitant use of psychotropic medications or other non-TCM treatment that could affect sleep quality were excluded from the analysis. All TCM treatment are described in Supplemental Table 2.
Quality Assessment of Included Studies
The risk of bias and the quality of the included RCTs were assessed by two independent reviewers (SCW and YFL). The Cochrane Risk of Bias 2 tool was used for quality evaluation. 35 The risk of bias in each domain was categorized as low, having some concerns, and high. Studies with some concerns in ≥3 domains were excluded from the analysis.
Data Extraction and Outcome Measures
Study characteristics and data on participants, interventions, and outcome measurements were extracted from the included studies by 2 researchers (CWC and MYT). The primary outcome was the change in patient-reported sleep quality from baseline to posttreatment. The more negative the value for changes in sleep, the more significant the reduction in sleep disturbance. The Pittsburgh Sleep Quality Index (PSQI) was used to assess sleep quality outcomes; the total PSQI scores range from 0 to 21, with a score of >5 indicating poor sleep quality. 36 All data were extracted as the mean difference (MD) and standard deviation (SD), which were used to calculate the estimated treatment effects; if a study had inadequate data for calculating these estimates, the corresponding authors were contacted for further information.
Statistical Analyses
The statistical software package “netmeta” in R was used for statistical analyses. 37 The NMA was conducted using a frequentist approach, and Q statistics were applied to assess homogeneity. The node-split model and design-by-treatment interaction models were used to evaluate the inconsistency between direct and indirect evidence. The league table presented all pairwise comparisons in the NMA, including treatment estimates and confidence intervals. The ranking of treatments was presented as P-scores by using a frequentist analog of the surface under the cumulative ranking curve. Publication bias was assessed using comparison-adjusted funnel plots and Egger’s test.
Assessment of Quality of NMA Evidence
The certainty of the evidence of the NMA was assessed using the Grades of Recommendation, Assessment, Development, and Evaluation (GRADE) system. 38
Results
Study Selection and Methodological Quality of Included Studies
The database search identified 94 records, with an additional 39 studies found through manual review. After removing duplicates(n = 17), excluding irrelevant studies (n = 91), those involving the concomitant use of psychotropic medications (n = 2), TCM nursing care, not TCM treatment (n = 3) and unable to obtain sufficient data (n = 1), 19 articles remained. The full texts of these studies were retrieved for further analysis (Supplemental Figure 2). All studies reported an adequate method of randomization, and 12 studies adequately described allocation concealment.23 -25,30,39 -46 Seven studies reported the blinding of participants and care providers,25,30,39 -42,46,47 and 10 studies reported the blinding of outcome assessors.23 -25,30,40,43,45,46,48,49 Only one study reported unacceptable dropout rates (21%-50%) 42 ; most studies had small sample sizes (n = 15-45).
Overall, 12, 5, and 2 RCTs were rated as having low risk, some concerns, and high risk of bias, respectively (Supplemental Table 3).
Network Geometry and Study Characteristics
Network geometry involving 1011 participants is presented in Figure 1. The network contains 12 connected treatment nodes: auricular acupressure/auricular acupuncture (AA/AT) (n = 80), acupuncture plus acupressure (n = 15), acupuncture (n = 44), stimulating acupressure (n = 94), acupressure (n = 167), aerobic exercises (n = 33), qigong (n = 109), CBT (n = 45), sham control (n = 103), wait-list control (n = 70), MBSR (n = 28), and usual care (n = 223). The characteristics of the included RCTs are summarized in Supplemental Table 4. The trials had roughly the same population, and sleep disturbance was defined as having sleep difficulties or a higher score on PSQI, which satisfied the assumption of transitivity.
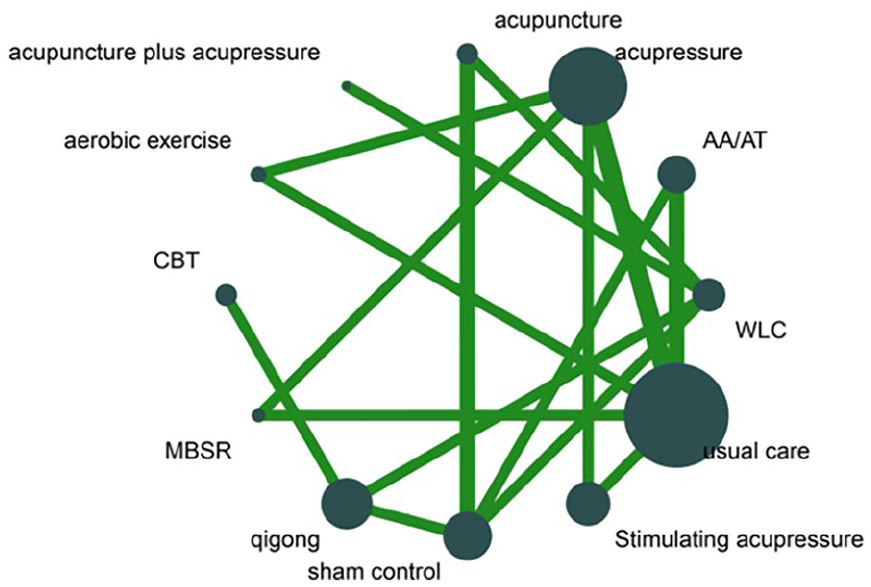
Primary network graph for all types of sleep quality outcomes. Each node indicates treatment class and represents the size of the population involved in each treatment. A solid line between nodes means a direct comparison, and line thickness corresponds to the number of comparisons
Interventions
In this NMA, the following interventions were included: acupressure, acupuncture, AA/AT, qigong, acupuncture plus acupressure, stimulating acupressure, MBSR, and aerobic exercise. The control group received sham control, usual care, and wait-list control. Three RCTs reported significantly lower PSQI scores in the acupressure therapy group than in the control group.17,43,45 Moreover, 3 other RCTs reported that 3-week AA/AT therapy significantly improved sleep quality compared with the control strategy.24,25,44 Two RCTs reported that acupuncture significantly improved sleep quality and sleep disturbance compared with sham acupuncture.39,46 Three RCTs included 2 types of qigong (Tai Chi and Baduanjin): one study indicated that qigong did not significantly decrease PSQI at postintervention, 30 but the other study noted significantly decreased PSQI scores in the Baduanjin exercise group (P < .001). 23 A study reported that Tai Chi was noninferior to CBT-I. 49 A study found the significant effects of acupuncture plus acupressure compared with the WLC. 26
NMA and Treatment Ranking
A league table and forest plot of the NMA comparing treatments and controls are presented in Table 1 and Supplemental Figure 1, respectively. MBSR (MD: −6.75, 95% CI: −12.44 to −1.06) improved sleep quality more effectively than the other TCM interventions. Among the various TCM interventions, acupressure, acupuncture, AA/AT, and qigong significantly enhanced sleep quality in BC survivors (MD: −6.38, −5.58, −5.20, and −4.43, respectively). The TCM intervention with the highest P-score was acupressure (0.784), followed by acupuncture (0.692), AA/AT (0.624), CBT (0.545), stimulating acupressure (0.514), qigong (0.414), and acupuncture plus acupressure (0.194). Among controls, CBT, usual care, and sham exerted a more favorable effect than no treatment (Table 2).
League Table for Results of the Network Meta-Analysis Within a Frequentist Framework.
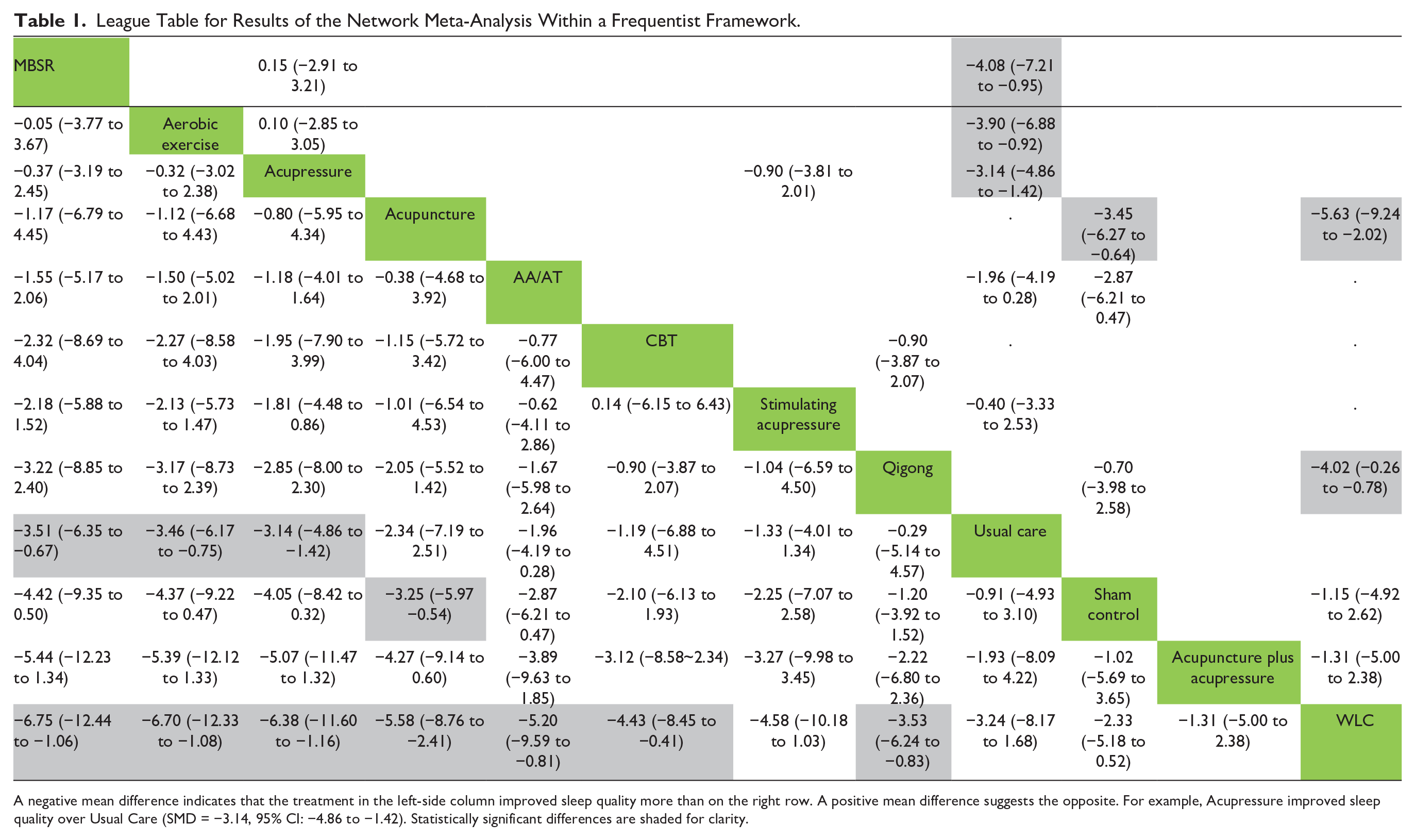
A negative mean difference indicates that the treatment in the left-side column improved sleep quality more than on the right row. A positive mean difference suggests the opposite. For example, Acupressure improved sleep quality over Usual Care (SMD = −3.14, 95% CI: −4.86 to −1.42). Statistically significant differences are shaded for clarity.
Treatment Ranking of the Primary Network.

Abbreviations: MBSR, mindfulness-based stress reduction; AA/AT, auricular acupuncture/auricular acupressure; CBT, cognitive-behavioral therapy; WLC, wait-list control.
Evaluation of Inconsistency and Publication Bias
We assessed global inconsistency by using a design-by-treatment interaction random effects model. The node-split method revealed consistency within the NMA model (Supplemental Table 5). A comparison-adjusted funnel plot and Egger’s test revealed no evidence of publication bias (P = .7054, Supplemental Figure 3).
GRADE Assessment
Supplemental Table 6 provides a summary of the ratings of direct estimates for each comparison of sleep disturbance outcomes.
By using the partially contextualized framework for evaluating the certainty of the evidence of NMA, we identified that MBSR, aerobic exercise, and acupressure had moderate certainty and large beneficial effects for improving sleep quality, and that acupuncture, AA/AT, CBT, and qigong also had moderate certainty but moderate beneficial effects for improving sleep quality. Sham control and acupuncture plus acupressure had small beneficial effects on sleep disturbance (Table 3).
Classification of Treatment Effect of the Interventions Included in the Network Meta-Analysis for Sleep Quality in BC Survivors.

Abbreviations: MBSR, mindfulness-based stress reduction; AA/AT, auricular acupuncture/auricular acupressure.
Discussion
TCM is one of the oldest healing systems; it is based on the principle that all natural phenomena are categorized into Yin and Yang, and all things constantly change toward a balance or harmony of Yin and Yang. This concept is applied to understand, prevent, and cure diseases. In TCM theory, sleep disturbance is usually expressed in terms of Yin deficiency and Yang excess; thus, Yang-qi is not hidden at night, causing the individual to remain in a state of excitement and making it difficult for the individual to fall asleep. 50 In addition, a deficiency of essence, qi, and spirit—the three energies of the human body—can cause sleep disturbance. 51 Qigong, acupressure, acupuncture, and AA/AT all aim to restore the balance or harmony of Yin and Yang, thus improving sleep quality.
Qigong has a long history in China; practicing qigong can enhance qi circulation through body movements, breath control, and meditation. Meng et al 27 concluded that qigong had no significant improvement in sleep quality but can decrease cytokines. It is known that reducing these cytokines levels can improve sleep quality. 52 However, our NMA indicated that qigong interventions had statistically significant benefits for sleep quality. Apart from the many factors involved in sleep disturbance, this discrepancy may be due to the following reasons. First, most of the included studies in our NMA had a low risk of bias. Second, the intervention duration was 2 to 3 months in the included studies. A study reported that the benefits of sleep became nonsignificant after 3 months. 53 Third, the participants and care providers could not be blinded to the qigong intervention, which may influence the result. Together, these findings imply that more studies should be conducted to identify changes in qigong practice in serum cytokine levels and sleep quality and to assess whether the intensity and duration of qigong practice can affect serum cytokine levels and sleep quality.
Acupressure, acupuncture, and AA/AT also stimulate the qi, which can reestablish the Yin-Yang balance. Consistent with the TCM theory, our findings support that acupressure, acupuncture, and AA/AT can significantly improve sleep quality in BC survivors. Acupressure and acupuncture are based on the same TCM theory. Acupuncture has been reported to be safe and efficacious for managing insomnia in BC survivors.26,32 An NMA including patients with arthralgia reported that acupuncture was more effective in reducing pain than exercise, medications, or other interventions. 54 In summary, acupuncture not only balances Yin and Yang but can also reduce pain and discomfort, thereby decreasing the difficulty of falling asleep and reducing the frequency of waking up in the middle of the night.
Acupressure had the highest ranking among the TCM treatments; it has fewer side effects than acupuncture and is also less expensive. A previous NMA reported that acupressure might be more promising than acupuncture for improving sleep in patients with cancer. 31 In our NMA, both acupressure and acupuncture improved sleep quality. However, the effect size of acupressure for reducing sleep disturbance was larger than that of acupuncture, but its 95% CI was also wider; therefore, further research is warranted to compare the effectiveness of acupuncture and acupressure. Despite the heterogeneity of acupoint selection in acupuncture and acupressure, the certainty of the evidence presented was moderate.
The mechanism of AA/AT for insomnia treatment may involve the regulation of melatonin to normalize sleep cycles. 55 From the Zang-Fu perspective of TCM, which refers to the internal organ system in traditional Chinese medicine and emphasizes the physiological and pathological relationships of the organs, sleep disturbance is mainly due to dysfunction of the heart. Therefore, the heart-related acupoints of Shenmen (TF4) and Heart (CO15) are primarily selected. These acupoints were also used in the studies included in our NMA,47,56 suggesting that AA/AT is a practical therapeutic approach for improving sleep quality. Moreover, during study selection, one study incorporated different modalities (acupuncture plus auricular acupressure), leading to difficulty in interpreting the effect of acupuncture alone or auricular acupressure alone. However, more studies are required to examine the combined effect of acupuncture plus auricular acupressure for evaluating the combination effect of different intervention combinations because these interventions are not mutually exclusive.
Limitations
This study has several limitations. First, the included RCTs had small sample sizes. Second, blinding was not always possible in the intervention or control group. Third, in subjective appraisals, self-report bias cannot be neglected. Finally, the long-term treatment effects of various TCM interventions could not be reported, and thus, the lasting effects of optimal TCM interventions on sleep quality remain unclear. Future studies should investigate the long-term effects of TCM interventions on sleep quality.
Conclusion
The differences between Traditional Chinese Medicine (TCM) treatment methods mainly lie in their holistic view of health and balance, as well as the formulation of personalized treatment plans based on individual characteristics. Qigong, acupressure, acupuncture, and auricular acupressure/auricular acupuncture (AA/AT) provided some degree of improvement for the sleep quality of breast cancer survivors with sleep disturbance. Among these TCM interventions, the highest impact was noted with acupressure therapy given twice daily for 6 to 8 weeks. The findings of this study can provide considerations for breast cancer patients who are considering using Traditional Chinese Medicine (TCM) for the treatment of insomnia. Additionally, most of the included studies had a small sample size and could not apply blinding. Future larger-scale studies with robust methodological designs are warranted to validate our findings while overcoming the limitations of the existing studies.
Supplemental Material
sj-docx-1-ict-10.1177_15347354241308857 – Supplemental material for Chinese Medicines Treatment for Sleep Disturbance in Breast Cancer Survivors: A Network Meta-Analysis
Supplemental material, sj-docx-1-ict-10.1177_15347354241308857 for Chinese Medicines Treatment for Sleep Disturbance in Breast Cancer Survivors: A Network Meta-Analysis by Chia-Wen Chuang, Ming-Yen Tsai, Shih-Chung Wu and Wen-Chun Liao in Integrative Cancer Therapies
Supplemental Material
sj-tiff-2-ict-10.1177_15347354241308857 – Supplemental material for Chinese Medicines Treatment for Sleep Disturbance in Breast Cancer Survivors: A Network Meta-Analysis
Supplemental material, sj-tiff-2-ict-10.1177_15347354241308857 for Chinese Medicines Treatment for Sleep Disturbance in Breast Cancer Survivors: A Network Meta-Analysis by Chia-Wen Chuang, Ming-Yen Tsai, Shih-Chung Wu and Wen-Chun Liao in Integrative Cancer Therapies
Supplemental Material
sj-tiff-3-ict-10.1177_15347354241308857 – Supplemental material for Chinese Medicines Treatment for Sleep Disturbance in Breast Cancer Survivors: A Network Meta-Analysis
Supplemental material, sj-tiff-3-ict-10.1177_15347354241308857 for Chinese Medicines Treatment for Sleep Disturbance in Breast Cancer Survivors: A Network Meta-Analysis by Chia-Wen Chuang, Ming-Yen Tsai, Shih-Chung Wu and Wen-Chun Liao in Integrative Cancer Therapies
Supplemental Material
sj-tiff-4-ict-10.1177_15347354241308857 – Supplemental material for Chinese Medicines Treatment for Sleep Disturbance in Breast Cancer Survivors: A Network Meta-Analysis
Supplemental material, sj-tiff-4-ict-10.1177_15347354241308857 for Chinese Medicines Treatment for Sleep Disturbance in Breast Cancer Survivors: A Network Meta-Analysis by Chia-Wen Chuang, Ming-Yen Tsai, Shih-Chung Wu and Wen-Chun Liao in Integrative Cancer Therapies
Footnotes
Acknowledgements
This manuscript was edited by Wallace Academic Editing.
Author Contributions
CWC, MYT, and SCW were responsible for the study design and coordination. CWC and MYT extracted the data. SCW evaluated the risk of bias. CWC, MYT, and WCL drafted the manuscript. CWC and WCL analyzed the trial outcomes. CWC and MYT contributed equally to this work. All authors have contributed to, read, and approved the final manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Consent to Participate
This study is a Network Meta-Analysis and does not involve human participants, hence consent to participate is not applicable.
Consent for Publication
This study does not involve human participants or identifiable personal data, hence consent for publication is not applicable.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.

