Abstract
Keywords
Introduction
The immune system plays a critical role in cancer. While inflammation promotes tumor initiation and growth, 1 cell-mediated immunity can help identify and eliminate tumor cells in a process known as immune surveillance. 2 Tumors work to suppress the immune response, both systemically and in the tissue microenvironment. 3 Cancer treatments may also impact the immune system. Immunotherapies work to increase the anti-tumor immune response, either through stimulation of the immune response or by blocking tumor-induced suppression of the immune system. Cytotoxic chemotherapy targets rapidly dividing cells, among other mechanisms, and commonly causes leukopenia and neutropenia owing to the off-target killing of immune cells. Additionally, chemotherapy-induced leukopenia/neutropenia results in treatment delays, can lead to infectious complications, and is a major cause of treatment-related morbidity and mortality.
The current standard treatment for chemotherapy-induced neutropenia includes hematopoietic colony-stimulating factors (CSF), such as granulocyte colony-stimulating factor (G-CSF), and granulocyte macrophage colony stimulating factor (GM-CSF). These treatments are expensive, and patients frequently report significant adverse effects, such as musculoskeletal pain, fever, or development of myelodysplasia or acute myeloid leukemia.4 -7 Therefore, finding a non-pharmacological approach to decrease chemotherapy-induced neutropenia is desirable.
Prior meta-analyses on acupuncture for chemotherapy induced leukopenia or bone marrow suppression found significant improvements in white blood cell (WBC) counts,8 -11 neutrophil levels,8,9 natural killer (NK) cell counts. 8 Previous animal studies suggest that acupuncture may increase serum CSF and promote the maturation of granulocytes.12,13 One meta-analysis 11 suggested that acupuncture could increase WBC by an average of 1221 cells/mL (95% confidence interval: 636-1807 cells/mL). In preclinical models, acupuncture led to increased NK cell activity and shift T cell populations.14,15 In an effort to identify effective, safe, and cost-effective treatment approaches to maintain the integrity of the immune system during cancer treatment, the current systematic review and meta-analyses explored the effects of acupuncture on immune and inflammatory markers in cancer patients.
Methods
Literature Search
The Ovid Medline, Ovid Embase, EBSCO CINAHL, EBSCO Alt HealthWatch, Wiley Cochrane Library, Elsevier Scopus, PubMed, Wanfang Data, and China National Knowledge Infrastructure (CNKI) China Academic Journals databases were searched from inception through March 2024 for prospective randomized clinical trials (RCTs) related to acupuncture modulation of the immune system in cancer patients in Chinese/English languages. Key search topics were acupuncture, cancer, randomized controlled trial, and immunity; see Supplemental 2 for detailed search strategy.
Study Selection
See study selection PRISMA diagram in Figure 1. Seven authors (WL, KG, JM, LC, AC, BZ, and RWW) independently screened articles for inclusion. Inclusion criteria were prospective RCTs, involved needle insertion into acupuncture points, and evaluated the use of acupuncture for modulation of the immune system in cancer patients. Unpublished reports, letters to the editor, retrospective chart reviews, studies for which only interim data analyses were available, studies for which only an abstract was available, and studies that did not evaluate acupuncture for modulation of the immune system were excluded. If contact information was available from an interim analysis or abstract only, the first author was contacted via email and asked if the results had been published. Studies that did not involve needle insertion (ie, acupressure, laser acupuncture, and electrostimulation without needles) or studies that only compared 2 types of active acupuncture, without a no-acupuncture or sham-acupuncture control group, or that evaluated acupuncture in combination with herbal treatments were excluded.
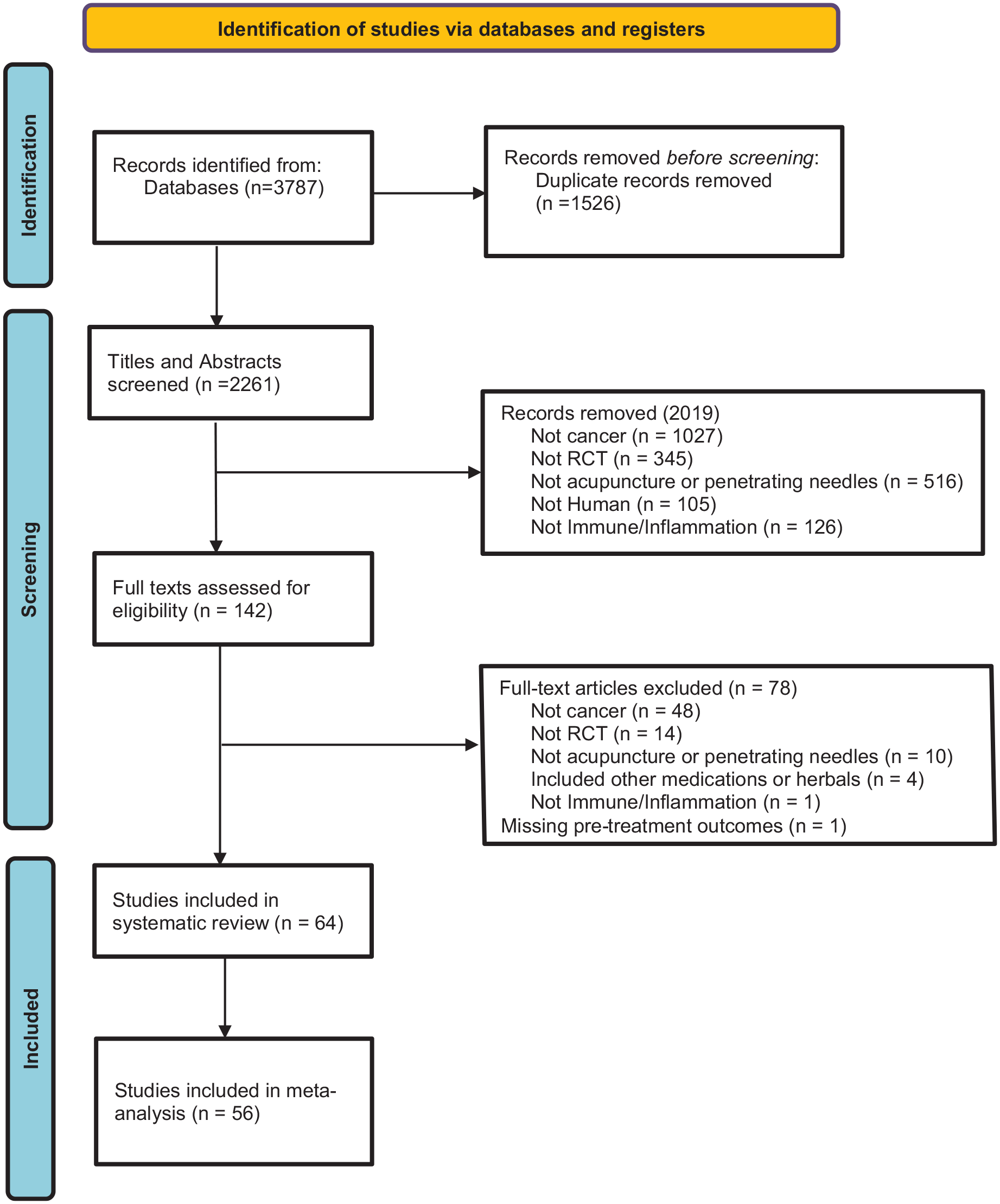
Flow chart for selection of studies.
Data Abstraction and Rating of Articles for Risk of Bias
For articles published in English, two independent reviewers (KG, JM, LC, BZ, WL, RW, and AC) abstracted data and rated articles using the Cochrane Risk of Bias (ROB) criteria (Table 1). 16 Articles written in Chinese were evaluated by two independent reviewers fluent in Mandarin (JM and WH or BZ and WL). For a study to be rated as having a low ROB, the low ROB criteria were required in all domains (sequence generation/randomization, allocation concealment, blinding, incomplete outcome data, selective outcome reporting, and other sources of bias). Secondarily, we also reported the ROB after excluding the allocation concealment and blinding domains, as the outcome measures studied are objective in nature and blood-based outcomes are less likely to be influenced by expectation and a placebo response. Discussion to consensus settled differences in ROB ratings.
Complete criteria for judgment of high, low, or unclear risk of bias may be accessed at: www.cochrane-handbook.org/ [Part 2, Chapter 8, Section 8.5, Table 8.5.d Criteria for judging risk of bias in the “Risk of bias” assessment tool]. Found here: https://handbook-5-1.cochrane.org/chapter_8/table_8_5_d_criteria_for_judging_risk_of_bias_in_the_risk_of.htm
After determining ROB, the reviewers also independently evaluated each study to determine whether the findings for the primary outcomes were positive, negative, or unclear. Although some studies reported statistical analyses for within-group changes in immune markers from baseline, between-group pre-post differences were emphasized in evaluating study outcomes.
For inclusion in the meta-analyses, studies needed to report sample size per group at baseline and follow-up time points, raw means, and standard deviations for each variable at baseline and at least 1 follow-up time point, and ideally details on any missing data. Pre-post (baseline to post-treatment), between-group differences for acupuncture treatment versus controls were compared. In most studies the control group was a non-attention standard-of-care treatment. The pre-post difference scores from the combined meta-analyses per outcome variable are presented.
Statistical Analysis
We plotted the effect measure and the 95% confidence intervals (CIs) using forest plots and assessed the studies’ heterogeneity using the I 2 statistic, which measures the percentage of total variation due to heterogeneity rather than chance. 17 I 2 values of less than 25% represent low heterogeneity, whereas I 2 values between 25% and 50% represent moderate heterogeneity. If a statistically significant percentage of the total variation was found to be due to heterogeneity, the combined effect measure from the studies in our meta-analysis was estimated using a random effects model in which each study was weighted relatively more equally (than a fixed-effect analysis). We included 2 forest plots for each analysis, with 2 including the I 2 statistic and the other including the Q statistic (Cochran’s heterogeneity statistic used to calculate I 2 ; I 2 = 100% × [(Q − df)/Q]). For the pre- and post-treatment difference outcomes, a correlation of .3 was assumed as a moderate yet realistic association between pre- and post-treatment biomarker levels, as needed. This assumption was necessary because no study except one 18 reported the standard deviations of the pre-post differences. If the correlation was greater than .3, the corresponding effect size estimates would be larger than those presented below. We also estimated potential publication bias (ie, tendency to publish either positive or negative results) using funnel plots. 19 We used the inverse variance-weighted average method when performing the meta-analysis.
Results
Of 3787 items identified, 1526 duplicates were omitted, and 2261 articles were screened. Sixty-four publications, 58 in Chinese and 6 in English, met all inclusion criteria and were evaluated for ROB according to the Cochrane criteria. Twenty-five studies examined participants with gastrointestinal cancers, 13 with unspecified cancers, 8 with lung cancer, 7 with breast cancer, 5 with gynecological cancers, and 5 with multiple cancers. Fifty-two trials used a two-group design that compared acupuncture to a heterogeneous variety of control groups. Nine studies compared 3 groups, with 5 of the studies comparing 2 different acupuncture treatments to a control group. Of the 3 four-group comparison studies, 1 study examined 2 different usual care control groups with and without acupuncture, 20 while the other 2 compared 3 different acupuncture treatments to a control group.21,22 One study used a delayed-effects group in the comparison. 23
The 64 studies examined 14 different channels (12 regular and 5 classified as “extra”) employing more than 80 unique acupuncture points. The most common channels examined were the Stomach (ST; 56 studies), Spleen (SP; 39 studies), Pericardium (PC; 26 studies), Large Intestine (LI; 17 studies), Kidney (KI; 14 studies), Dū mài/Governor Vessel (GV; 15 studies), Bladder (BL; 14 studies), Heart (HT; 11 studies), and Liver (LR; 10 studies). Among the most common acupoints used were ST36 (51 studies), ST37 (14 studies), ST39 (11 studies), SP6 (24 studies), PC6 (22 studies), and LI4 (20 studies).
Risk of Bias
Of the 64 included studies, 53 were rated unclear ROB, 11 were rated high ROB, and 0 were rated low ROB (see Tables 2 and 3 for design and treatment parameters for all included studies). Two studies used a placebo control group, and although they were rated as having a high 24 or unclear 25 ROB, both studies found acupuncture effective at supporting the immune system.24,25
Risk of Bias (ROB) for Included Studies.

Abbreviations: ROB, risk of bias; -, high ROB; 0, unclear ROB; +, low ROB; H, high ROB for one or more domains; U, unclear ROB for one or more domains; L, low ROB for all domains.
Study Design and Treatment Parameters by ROB Rating.
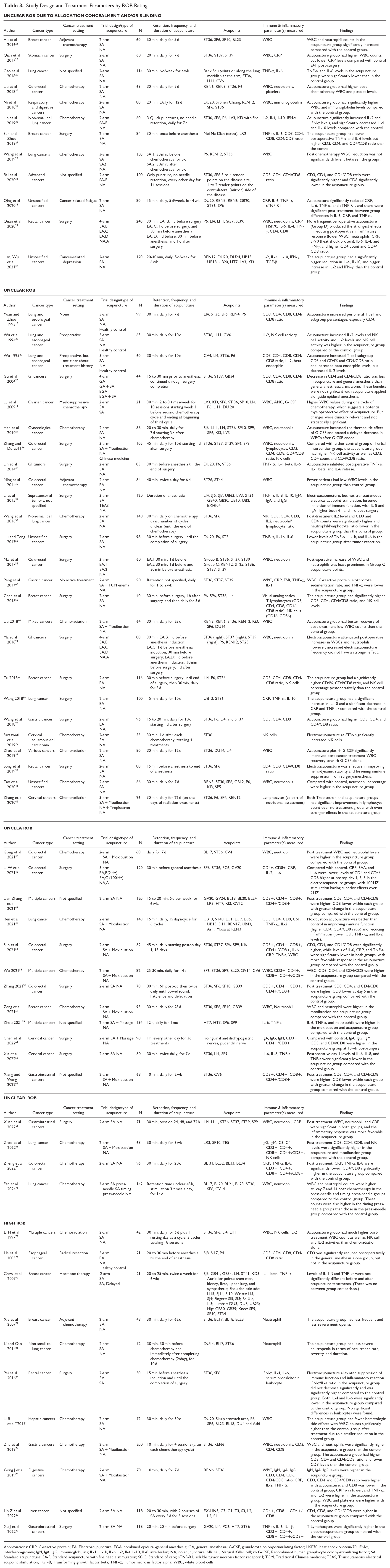
Abbreviations: CRP, C-reactive protein; EA, Electroacupuncture; EGA, combined epidural-general anesthesia; GA, general anesthesia; G-CSF, granulocyte colony-stimulating factor; HSP70, heat shock protein-70; IFN-γ, Interferon-gamma; IgM, IgA, IgG, Immunoglobulins; IL-1, IL-1b, IL-6, Il-2, Il-4, Il-10, IL-8, interleukin; NA, no acupuncture; NK cell, Natural Killer cell; rh G-CSF, Recombinant human granulocyte colony-stimulating factor; SA, Standard acupuncture; SA-F, Standard acupuncture with fire needle stimulation; SOC, Standard of care; sTNF-R1, soluble tumor necrosis factor receptor I; TCM, Traditional Chinese medicine; TEAS, Transcutaneous electrical acupoint stimulation; TGF-β, Transforming growth factor beta; TNF-α, Tumor necrosis factor alpha; WBC, white blood cells.
The placebo-controlled study with the high ROB rating 24 had unclear allocation concealment and conclusions that did not match the outcomes shown in tables. The authors compared 25 patients who received electroacupuncture to ST36 and SP6 beginning 15 minutes before rectal cancer surgery and continuing until the surgery’s completion to 25 patients who received sham acupuncture during the same period. Their findings revealed that interleukin (IL)-4 and IL-6 levels slightly increased, while interferon (IFN)-γ/IL-4 ratio went down in the control group. 24 IL-4 and IL-6 levels went down in the acupuncture group compared to the control group, and the IFN-γ/IL-4 ratio increased post-surgery in the real acupuncture group but went down significantly in the control group, with between-group differences (P < .05). 24 The other placebo-controlled study, a pilot, randomized, two-arm study by Lu et al 25 conducted at Dana Farber Cancer Institute, had an unclear ROB rating because of the small sample size (N = 21 patients with gynecological cancers randomized), but was otherwise rated as having a low ROB. The incidence of grade 2-4 leukopenia with chemotherapy was less in the acupuncture arm than in the sham arm (30% versus 90%; p = 0.02). 25 The median leukocyte nadir, neutrophil nadir, and recovery absolute neutrophil count (ANC) were all higher in the acupuncture arm, but not statistically significant after adjusting for baseline differences. 25 Unfortunately, neither study met the criteria to be included in the meta-analyses.
Review of the Highest-Quality Studies
When the allocation concealment and blinding ROB criteria were removed, 12 studies were rated low ROB. Three of these studies were conducted in the perioperative setting, 6 while patients were undergoing chemotherapy or radiotherapy, and 3 during an unspecified timeframe.
Acupuncture in the perioperative setting
Qian et al 28 treated stomach cancer patients post-surgery with 20 minutes of daily acupuncture for 7 days (n = 30) or standard care (n = 30). There were significant increases in WBC counts among all participants, but more so in the control group than the acupuncture group immediately postop. 28 However, the acupuncture group’s WBC count was higher than the control group 24 hours postop. 28 This study was given a weight of 0% in the meta-analysis because the large variance associated with the effect size estimates from the study when examining WBC counts. C-reactive protein (CRP) was significantly lower in the acupuncture group than the control group at the end of surgery and 24 hours postop. 28 Sun and Zhou 27 compared 1 electroacupuncture (EA) session (n = 42) before anesthesia for breast cancer surgery to a patient-controlled anesthesia dosing control group (n = 42). After surgery, tumor necrosis factor (TNF)-α and IL-6 increased significantly in the control group, with no changes in the EA group, resulting in significant between-group differences. 27 CD3, CD4, and CD4/CD8 ratio levels were significantly higher in the EA group than in the control group, and the EA group remained closer to pre-surgery levels. 27 Quan et al 22 examined the effects of EA provided 1, 2, or 3 times (n = 60 in each group) versus usual care (n = 60) in the perioperative period among rectal cancer patients. Each EA session was 30 minutes long and provided: (1) 1 day before surgery; (2) 1 day before surgery and 30 minutes before anesthesia; and (3) 1 day before surgery, 30 minutes before anesthesia, and 1 day after surgery. 22 The 3-dose acupuncture group had the greatest difference from the control group, resulting in lower levels of CRP, IL-4, IL-6, neutrophils, and WBC counts, and significantly higher IFN-γ/IL-4 ratio, CD4, and CD4/CD8 ratio. 22
Acupuncture during chemotherapy or radiotherapy
Qing et al 33 studied the effects of acupuncture on the immune system during radiotherapy and chemotherapy, comparing a sample that received acupuncture (n = 44) once daily, 5 days a week, over 4 weeks to a usual care group (n = 36). Significant decreases in TNF-α, IL-6, and soluble TNF receptor 1 levels were found after the acupuncture intervention, and there were significant post-intervention group differences in IL-6, CRP, and TNF-α. 33 Hu et al 26 examined the effects of daily acupuncture sessions for 5 days during chemotherapy to treat breast cancer (n = 30) compared to usual care (n = 30) and found significantly higher post-treatment WBC and neutrophil counts in the acupuncture group than the control group. 26 Ni et al 34 compared acupuncture daily for 12 days (n = 40) to standard Western medical care (n = 40) in respiratory and digestive cancer patients getting chemotherapy. They reported significant increases in WBC counts in the acupuncture group, significant differences in immunoglobulin M (IgM) scores between the 2 groups, with increases in the acupuncture group and decreases in the control group, and significant increases in IgG in the acupuncture group and decreases in the control group. 34 Liu et al 32 compared acupuncture provided daily for 5 days (n = 32) to usual care (n = 31) in patients receiving chemotherapy for colorectal cancer. Both groups had lower WBC and neutrophil counts post chemotherapy, but WBC counts were higher in the acupuncture group, and no between-group differences in neutrophil counts were found. 32 Lin et al 35 examined the effect of acupuncture (n = 30) provided concurrently with chemotherapy, once daily for 7 consecutive days, compared to usual cancer care (n = 30) in patients with advanced non-small cell lung cancer. The study revealed that IFN-γ and IL-2 levels significantly increased, while IL-4 and IL-10 levels significantly decreased in the acupuncture group relative to the control group. 35 Wang et al 29 examined WBC counts after 3 separate chemotherapy sessions. Acupuncture was provided 30 minutes before chemotherapy (N = 50) or 30 minutes after chemotherapy (N = 50), or the patients were in a usual care control group (N = 50). 29 No statistically significant pairwise differences were found in WBC counts across the 3 groups. 29
Acupuncture treatment setting unspecified
Gao et al 30 examined the effect of acupuncture delivered for 30 minutes, 6 days a week, for 4 weeks compared to a group that did not receive acupuncture among patients with lung cancer. Findings revealed significantly lower post-treatment TNF-α and IL-6 levels in the acupuncture group than the control group. 30 Bai et al 31 provided acupuncture every other day for 2 weeks (N = 50) compared to usual care (N = 50) in patients with unspecified cancers. They found significantly higher CD3, CD4, and CD4/CD8 ratio, as well as significantly lower CD8 levels in the acupuncture group relative to the control group. 31 Lian et al 36 examined patients with unspecified cancers who were provided acupuncture 5 days a week for 6 weeks (N = 60) or usual care (N = 60). Findings revealed increases in IL-2 and IFN-γ levels in both groups, but they were significantly higher in the acupuncture group than the controls. Similarly, both groups had a decrease in IL-4 and IL-10 levels, which was significantly lower in the acupuncture group than controls. 36
Meta-analysis
Fifty-six (83%) of the studies were included in the meta-analysis. The study outcome variables explored were as follows: WBC,21,22,26,28,29,32,34,37,41,43,44,46,50,53,57,58,60,62,64,66,76,78,81 CD3,18,23,27,31,40,46,47,49,53 -55,61,62,65,67,68,75,76,78 CD4,18,22, 23,27,31, 37,38,40,45-47,49,53-55,62,67- 70,75,76, 78,80 CD8,18,22,23,27,31,36,38,40,45,49,54, 55,57,62,65,67,68,70,75,76,78,80 CD4/8 ratio,18,22,23,27,31,38,40,45- 47,49,53,55,61,62,65,67,70,76,78,80 Neutrophils,21,22,41,43,46,57,58,62,64,66,71 NK cells,38,46,54,67,68,72,73 IgG,34,52,78 IgM,34,52,61,68,78 IL-1,48,56,60 IL-2,36,38,45,49,54,73,78 IL-4,22,24,36 IL-6,22,24,30,33,45,48,56,59,63 IL-10,23,36,52 TNF-α,23,30,33,48,49,52,56,60,78 IFN-γ,22,24,36 and CRP.22,28,33,45,60,66,69,70,78 Details of the meta-analysis, sample size, and heterogeneity can be found in Table 4 (see Supplemental Tables S1–17 for the meta-analysis forest plots of individual studies and outcomes).
Meta-Analysis Results. a
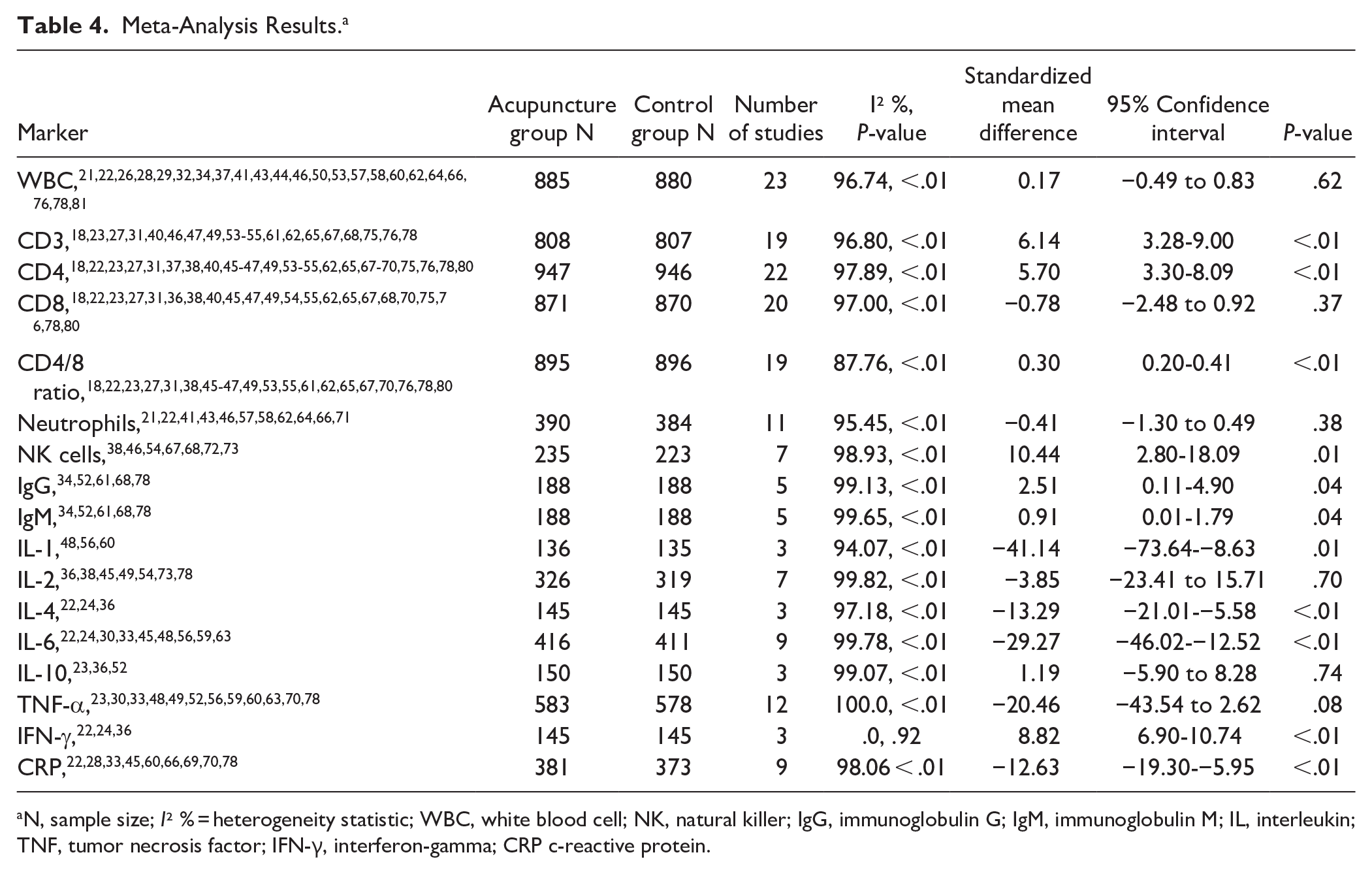
N, sample size; I² % = heterogeneity statistic; WBC, white blood cell; NK, natural killer; IgG, immunoglobulin G; IgM, immunoglobulin M; IL, interleukin; TNF, tumor necrosis factor; IFN-γ, interferon-gamma; CRP c-reactive protein.
Acupuncture was associated with significant increases in CD3 (19 studies), CD4 (23 studies), and the CD4/CD8 ratio (20 studies), with sample sizes of over 1000 participants for each outcome. However, for each outcome there was high heterogeneity in the results. Similarly, acupuncture led to increases in NK cell numbers, but there was a high level of heterogeneity in the results between the 7 studies included in the meta-analysis. Five acupuncture studies included in the meta-analysis led to increases in both IgG and IgM, but there was a high level of heterogeneity in the results. Acupuncture was also found to lower IL-1 (3 studies), IL-4 (3 studies), IL-6 (10 studies), and CRP (9 studies), but there was high heterogeneity in results for each marker included in the meta-analysis. One meta-analysis found acupuncture was associated with increases in IFN-γ, and no concerns with heterogeneity.
Acupuncture was not significantly associated with increases in WBCs, neutrophils, CD8-positive cells, or IL-2. Acupuncture was not associated with decreases in TNF-α or IL-10. In all the studies with negative outcomes, there was a high level of heterogeneity in the results.
Discussion
This systematic review and meta-analysis were conducted to examine the use of acupuncture for immune and inflammatory modulation in cancer patients. Sixty-four publications examining the effect of acupuncture on immune function and inflammation met the inclusion criteria for this review, with 56 studies included in the meta-analysis. More than 80 acupuncture points associated with 14 different channels were used, with the most common point being ST36. All reviewed studies were scored as having unclear or high ROB. The meta-analysis showed that acupuncture resulted in improvements in multiple outcomes, but there was a high level of heterogeneity among all the studies except those showing that acupuncture was associated with increases in IFN-γ.
All studies contained some bias, which raises questions about the veracity of the findings. In general, ROB was worse for the oldest studies, with more recent studies having more domains with low ROB ratings, which is similar to a prior meta-analysis. 11 The study by Lu et al 25 was blinded and had a low ROB for all of the rating criteria except “other sources of bias” due to a small sample size, which caused an unclear ROB rating. Similarly, the study by Lin et al 35 met all the criteria for a low ROB except the acupuncture group participants were not blinded to group assignment. Twelve studies appeared well designed, with low ROB, but had a risk of bias owing to the lack of allocation concealment and blinding.22,26 -36 The majority of the studies had design or reporting biases resulting in unclear or high ROB ratings.
Findings from the studies included in the meta-analyses suggest that acupuncture may play a role in improving immune outcomes and reducing inflammation during different phases of cancer treatment. Meta-analyses revealed improvements in immune function among the acupuncture treatment groups, with increases in CD3 cells, CD4 cells, and the CD4/CD8 cell ratio, as well as NK cell counts, IgG, and IgM. Acupuncture did not affect WBCs, neutrophils, CD8-positive cells, and IL-2 immune markers. IL-1, IL-4, IL-6, and CRP inflammatory markers all decreased in the acupuncture groups, while no significant reductions were found for TNF-α or IL-10. All immune and inflammatory markers, except for IFN-γ, were found to have significant heterogeneity concerns across studies, as expressed by the I 2 statistic from the meta-analyses.
Several factors may have contributed to the high heterogeneity of the meta-analyses’ outcomes. There were many differences in the acupuncture designs, including the number of acupuncture sessions, the duration of each individual acupuncture session, the acupuncture techniques used, and the number of points and channels/acupoints used. Other design differences included the type of cancers treated and the timing of the acupuncture treatment (eg, before, during, or after surgery, chemotherapy, or radiotherapy). Despite these differences in the design of the acupuncture interventions and patient populations, the improvements in immune and inflammatory markers seen among individuals undergoing cancer treatment suggest that more studies are needed to increase design homogeneity to determine best practices of acupuncture treatments to improve immune and inflammatory markers.
Our study is the first systematic review/meta-analysis to examine the effects of acupuncture on multiple immune and inflammatory markers among people receiving cancer treatment. However, previous studies do provide support for our findings. In one review of acupuncture and moxibustion that focused on leukopenia, 83 all unblinded acupuncture trials were rated as having a high ROB, as we did here. One meta-analysis of acupuncture’s effect on patients with chronic obstructive pulmonary disease found significant improvements in immune function through an increase in the CD4/CD8 ratio, as did our study, but differed in finding a significant reduction in CD8-positive T cells. 84 Like the current study, another meta-analysis of acupuncture’s effect on cytokines in rodent animal models by Lee and Kim 85 found significant reductions in IL-1 and IL-6, but unlike the current study, they found a significant reduction in TNF-α, as well as increases in IL-10. 85 Our findings differed from prior meta-analyses on acupuncture for chemotherapy induced leukopenia and bone marrow suppression where they found that acupuncture improved WBC counts and neutrophils,8,9,11 while another found no significant differences in neutrophil counts. 10 However, one of the meta-analyses of acupuncture’s effect on leukopenia reported the poor methodological quality of studies included in their analyses. 11 Oh and Kim 86 conducted a literature review of acupuncture at ST36 (the most common acupoint used in the current study) and reported clinical benefits in reducing inflammation.
As with any systematic review, our study had several important limitations. An attempt was made to include databases with the most relevant literature. Other databases and/or search strategies may have produced a different list of RCTs to be screened, and important studies may have been overlooked due to publication bias. Although previous animal and human studies12,13,83 have shown that the use of moxibustion had a positive effect on immune modulation, cancer centers in the US do not use this technique because of smoke exposure and the associated strong smell. In addition, 61 studies were conducted in China, with only 2 studies conducted in the US and one study conducted in Indonesia. The feasibility of conducting these types of studies outside of China is also at issue. The studies conducted in China included only inpatient populations, and patients were treated daily. Long peri-treatment hospitalizations for cancer patients without complications are standard in China, but not in the US. It is unclear if a less intensive therapy would yield similar outcomes. One study conducted in the US 25 screened 587 patients to enroll 21 patients. Over 50% of these patients were excluded based on the treating physician’s decision and 20.7% were not enrolled because of competing protocols. This is a significantly lower rate of enrollment than for other trials of acupuncture reported by Dana Farber as well as other institutions, possibly reflecting skepticism of the utility of acupuncture for this indication. Many of the studies included were underpowered because of small sample sizes. Furthermore, as optimal treatment and dosing parameters are unknown, heterogeneity in study design, outcome measures, and treatment parameters makes comparisons across studies difficult. There was also a high I 2 heterogeneity statistics for the results for all meta-analyses except IFN-γ. Moreover, no studies used the same interventions, which limited each meta-analysis calculation, and suggests that these findings cannot determine which treatments are best for which immune and inflammatory markers. The study also could not explore subgroup analyses to determine specific factors that could optimize the benefits of acupuncture on immune outcomes. The meta-analyses assumed an arbitrary within-subject correlation of .3 for calculating SDs of the pre-post difference outcomes, as needed, which may have skewed outcomes to certain extent, either downward or upward. Despite this limitation, we believe the moderate correlation assumption is realistic and likely not far off from the truth. Finally, calculations for 6 biomarker meta-analyses employed only 3 studies and should be interpreted with caution.
Although the exact mechanisms of acupuncture are not yet fully understood, leading researchers suggest that acupoints and meridians may function as part of the autonomic nervous system, 87 helping to explain the broad physiological effects observed. However, to explore acupuncture’s role more effectively as it related to immune regulation, well-designed, adequately powered studies with low risk of bias are necessary to provide meaningful clinical guidance. In our review, most of the 64 studies included were rated as having unclear ROB, with 11 rated as high risk. These challenges in study design and reporting are well-known in acupuncture research, 88 and our finding was no exception. One key issue is the appropriate selection of controls. Given that the mechanisms of acupuncture are still being explored, we advocate for a research design that mirrors real-world practice as closely as possible, using best standard practices as the control. 89 This is particularly important because syndrome differentiation is a crucial factor in selecting acupuncture points in real practice, yet sham control points do not account for this, which may make them suboptimal controls. Yet many will see this approach as a challenge to control and still advocate for the sham-controlled design. Immune outcomes being a more objective outcome allays some of the concerns typically associated with the placebo response. Future research should also be designed in a manner to explore demographic or medical factors that can predict better or worse immune response to acupuncture treatment.
This study had several strengths. This is the first to quantify acupuncture’s effects on multiple immune and inflammatory markers among people receiving cancer treatment. Biomarkers are less prone to the influence of allocation concealment and participant blinding than a self-report measure like pain or nausea, and 12 studies were well designed in this regard. The majority (65%) of the meta-analyses for a specific immune or inflammatory outcome used 6 or more studies.
It is important to put the use of acupuncture for immune modulation into its full clinical context. Acupuncture is a safe and cost-effective treatment for many indications. In the case of leukopenia/neutropenia, it would be important to examine the cost-benefit ratio in terms of number of patients needed to treat to prevent febrile neutropenia, the clinically relevant endpoint. The field of cellular immunity has rapidly evolved over the past 10 years. It would be particularly interesting to examine the impact of acupuncture on regulatory T-cell populations and tumor-infiltrating lymphocytes, or to examine the effects of combining acupuncture with the new immune checkpoint inhibitor immunotherapies to “prime” the immune system, as is being done with combined vaccine and checkpoint-inhibitor protocols.
Conclusion
Acupuncture appears to result in significant and meaningful improvements in immune function and reduced inflammatory biomarkers without unwanted side effects. However, the findings from this systematic review and meta-analyses suggests that better-designed, well-powered studies with low ROB designs are needed. More rigorous trials using sham acupuncture groups and/or research design that mirror real-world practice in larger populations are required to validate these findings. Multi-armed research studies comparing interventions focused on specific immune/inflammatory markers could increase acceptance among oncologists that acupuncture may help modulate immune and inflammatory outcomes. Even so, 12 studies would have met low ROB criteria except for allocation concealment and blinding, which is less of an issue for an objective outcome like immune and inflammatory markers relative to subjective outcomes like pain. Acupuncture could be part of an integrative cancer treatment approach for supporting surgery, chemotherapy, and radiotherapy. As a safe and cost-effective treatment, acupuncture could be used to help reduce immune suppression and inflammation in cancer patients.
Supplemental Material
sj-docx-1-ict-10.1177_15347354241302072 – Supplemental material for Systematic Review and Meta-analysis of Acupuncture for Modulation of Immune and Inflammatory Markers in Cancer Patients
Supplemental material, sj-docx-1-ict-10.1177_15347354241302072 for Systematic Review and Meta-analysis of Acupuncture for Modulation of Immune and Inflammatory Markers in Cancer Patients by Wenli Liu, Baisong Zhong, Richard W. Wagner, M. Kay Garcia, Jennifer L. McQuade, Wen Huang, Yisheng Li, Graciela M. Nogueras Gonzalez, Michael R. Spano, Alessandro Cohen, Yimin Geng and Lorenzo Cohen in Integrative Cancer Therapies
Supplemental Material
sj-docx-2-ict-10.1177_15347354241302072 – Supplemental material for Systematic Review and Meta-analysis of Acupuncture for Modulation of Immune and Inflammatory Markers in Cancer Patients
Supplemental material, sj-docx-2-ict-10.1177_15347354241302072 for Systematic Review and Meta-analysis of Acupuncture for Modulation of Immune and Inflammatory Markers in Cancer Patients by Wenli Liu, Baisong Zhong, Richard W. Wagner, M. Kay Garcia, Jennifer L. McQuade, Wen Huang, Yisheng Li, Graciela M. Nogueras Gonzalez, Michael R. Spano, Alessandro Cohen, Yimin Geng and Lorenzo Cohen in Integrative Cancer Therapies
Footnotes
Author Contributions
Conception and design: JM, MKG, WH, YL, MS, LC Collection and assembly of data: WL, BZ, AC, JM, MKG, RWW, YG, LC. Data analysis and interpretation: WL, BZ, JM, MKG, YL, GMNG, AC, YG, LC. Funding acquisition: JM, MKG, LC Writing – original draft: WL, JM, MKG, RWW, LC Writing – review & editing: All authors. Final approval of manuscript: All authors. Accountable for all aspects of the work: All authors.
Data Availability Statement
All data generated or analyzed during this study are included in this published article (and its supplementary information files).
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Support was provided in part by the United States National Cancer Institute (NCI) grants CA148707 and CA160880, and The University of Texas MD Anderson Cancer Center. Partial support for Lorenzo Cohen was also provided by the Richard E. Haynes Distinguished Professorship in Clinical Cancer Prevention. We would especially like to thank Greg Pratt, The University of Texas MD Anderson Cancer Center, for library support and assistance in database searches and strategy, and Dawn Chalaire from the office of Scientific Publications for her editorial support and assistance.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.

