Abstract
Introduction
Breast cancer is the most common cancer in women. 1 About 40% of women diagnosed will be postmenopausal and have tumors that are sensitive to estrogen or progesterone. 2 For these women, aromatase inhibitors are standard pharmacological treatment, which has been shown to improve disease-free survival.3,4 However, aromatase inhibitors act by blocking the production of estrogen, profoundly depleting oestrogen levels within days of administration. Consequently, this results in a severe loss of bone mass where the inhibition of estrogen causes a marked increase in bone resorption (ie, breakdown), 4 resulting in net bone loss at twice the rate of normal physiological postmenopausal bone loss.5,6 Low bone mineral density is a significant health problem as it increases the risk of fracture; the most serious complication of osteoporosis, which is associated with significantly increased morbidity, mortality, and health care expenditure. 7 The loss of bone density and increased incidence of fragility fractures associated with aromatase inhibitor use is higher when compared to other treatments such as tamoxifen. 8
The current treatment to reverse increased bone resorption is administration of oral bisphosphonates. However, these are costly pharmaceutical interventions with little benefit observed in bisphosphonate use beyond the first 5 to 10 years. 9 While generally well tolerated, they have low compliance levels (20%-57% over 1 year) due to the rigid dosing requirements 5 and are associated with negative side effects, including suppression of bone formation, gastrointestinal irritations, and its long term use is associated with secondary cancers. 10 Exercise interventions that involve an increased loading on the bone such as resistance training, jumping activity, and other weightbearing activities, have also been shown to improve bone density in pre- and postmenopausal women when performed regularly. 11 However, research to date regarding the role of exercise for bone health in breast cancer survivors reports poor intervention adherence,12-15 as well as a lack of evidence for improvements in bone mineral density.12-17 Investigation of other supportive care interventions aimed at decreasing bone resorption in breast cancer patients on aromatase inhibitors is required.
Whole-body vibration training (WBV) is a relatively new form of therapy that has been shown in certain populations to increase bone density, develop muscle function, and improve balance.18,19 This time efficient form of treatment involves having the patient stand on a platform that produces vertical accelerations at a specific frequency and amplitude in order to stimulate physiological responses in the bone and muscle tissue. Low-magnitude vibration training has previously been shown to reduce the rate of bone resorption in postmenopausal women. 20 Vibration exposure 3 times per week reduced a marker of bone resorption in postmenopausal women without cancer by 34.6% over 8 weeks. 20 By comparison, reductions of 25% in markers of bone resorption have been reported in postmenopausal women with osteoporosis/osteopenia following walking programs of 12 months duration. 21 Vibration may be more accessible to those with greater symptoms and lower mobility when compared with exercise training, given the low physical demand of standing.
In this study, we examined the effect of vibration stimulus on markers of bone turnover in postmenopausal breast cancer patients receiving aromatase inhibitor therapy. We hypothesized that the application of low-magnitude vibration stimulus for 12 weeks would decrease the bone resorption marker, N-telopeptide X/creatinine (Ntx/Cr), compared with no vibration exposure. In addition, we explored the effects of vibration stimulus on body composition and physical functioning.
Patients and Methods
Participants
Women undergoing aromatase inhibitor (AI) therapy were recruited between August 2012 and November 2014 from Perth, Australia through referral from oncologists. Participants were eligible if they were willing to continue taking any bone altering medications or supplements they were previously taking for the duration of the study, including calcium, vitamin D, or hormone replacement therapy (HRT); able to stand unassisted for sustained periods of time (ie, 20 minutes); received medical clearance from their general practitioner to participate. Exclusion criteria included taking bisphosphonates, cognitive impairment; contraindications to vibration platform training (including pacemaker and fracture within the past six months); diagnosis of bone metastases, and the diagnosis of diseases other than osteoporosis affecting bone. The study protocol was approved by the Edith Cowan University Human Research Committee and was registered with the Australian and New Zealand Clinical Trials Registry (ACTRN12611001094965). All participants gave informed written consent prior to enrolment.
Design
The study was a single blinded randomized controlled trial, with an intention-to-treat analytic strategy. The intervention consisted of a 12-week whole body vibration exposure program. Serum and urine markers of bone turnover, body composition and physical function, muscular strength, bone density, quality of life, and pain/stiffness of joints were measured at baseline and postintervention. All testing was conducted at the Edith Cowan University, Exercise Medicine Research Institute, and training was conducted either there or at Sir Charles Gairdner Hospital Department of Physiotherapy, Perth, Australia.
Randomization
Participants were randomized into a vibration-training group, or a control group following completion of baseline assessments. Randomization was performed using computer-generated, randomly permuted blocks by a researcher who was not involved in testing and training of participants. Participants were stratified by bone mineral density T-score obtained via DXA (dual-energy X-ray absorptiometry) scan (ie, ≤1 vs >1), and current physical activity participation obtained via self-report from Godin Leisure Time Exercise Questionnaire, 22 (ie, moderate and vigorous physical activity <150 vs ≥150). Participants were informed of their group allocation by means of sealed opaque envelopes given to them after completion of all baseline testing.
Vibration Exposure
Low-frequency, low-magnitude vibration was applied (30 Hz, 0.1 mm, 0.3g) using a vibration platform (Juvent Medical, Somerset, NJ, USA). This is consistent with current research that suggests that low magnitude is anabolic to bone 23 as it does not cause damage to physiology possibly associated with high-magnitude vibration. 24 Past literature has reported that low frequency vibration has greatest transmission up the axial skeleton, with this transmissibility decreasing as higher vibration frequencies are used. 25 Recently, a meta-analysis exploring the effect of whole-body vibration on bone loss in postmenopausal women showed that low-magnitude vibration (defined as <1g) was effective in reducing bone loss, whereas high-magnitude was not. 26 All participants were instructed to stand on the vibration platform with their feet shoulder width apart, knees locked, and hands by their side to receive maximum vibration exposure. The protocol was performed with participants’ shoes removed to prevent any attenuation of vibration that may result from footwear. Sessions included 20 minutes of vibration exposure 3 times a week for 12 weeks.
Control
The control group received usual care from their physician throughout the 12-week period. Those assigned to the control group were given no additional treatment or intervention but were placed on a waiting list giving them access to the vibration training facilities at the completion of the study.
Outcomes
Outcome measures were conducted at baseline (prior to randomization) and postintervention.
Primary Outcomes
Markers of bone formation (serum type 1 procollagen N-terminal propeptide [P1NP]) and resorption (N-telopeptide X/creatinine [NTx/Cr]) were assessed via blood and urine tests performed without batching by an independent NATA-accredited laboratory blinded to group allocation. Blood samples were collected between 72 and 120 hours following the last vibration exposure session to standardize previously reported acute bout effects on markers of bone metabolism. 27
Secondary Outcomes
Demographic and health history information was collected via questionnaire at baseline assessment. Baseline 25-OH vitamin D status was assessed by blood test, and analysis performed without batching by an independent NATA (National Association of Testing Authorities, Australia)–accredited laboratory blinded to group allocation.
Anthropometric Measures, Body Composition, and Bone Mineral Density
Height and weight were assessed by stadiometer (Seca GmbH & Co KG, Hamburg, Germany). Waist and hip circumference were assessed as a horizontal measure taken at the narrowest part of the torso or between the iliac crest and 12th rib, and the maximal circumference of the hip. 28 Whole body dual-energy X-ray absorptiometry scan (DXA; Hologic Discovery A, Waltham, MA, USA) was used to assess whole body and regional lean and fat mass. 29 Additionally, to characterize the study population, DXA scans were used to assess bone mineral density (BMD, g/cm2) of total hip (ie, femoral neck), spine (ie, lumbar spine L2-L4), and whole body.
Physical Functioning
Physical functioning was assessed by a series of tests. Cardiovascular fitness was assessed by the 400-m walk test. 30 Functional ability was assessed via repeated chair rise and stair climb. 31 To assess ambulatory ability, electronic timing gates were used to assess usual, fast-paced and backward 6-m walk. 32 Functional tests were performed in triplicate with standardized rest-times given between trials. 31 Static balance was assessed in six different positions (feet apart in parallel stance, feet together in parallel stance, half tandem stance, tandem stance, one-legged stance, one-legged stance eyes closed), without the use of assistive device for a maximum of 15 seconds in each position. Total static balance is calculated by summing the time recorded for each of the six stances. 33 Maximal strength was by a 1-repetition maximum test for lower body (leg press) and upper body (chest press). 34
Patient-Reported Outcomes
Patient-rated outcomes were assessed using well-validated self-report questionnaire. The Western Ontario and McMaster Universities Arthritis Index (WOMAC) was applied to assess joint pain and stiffness and difficulty with daily activities. 35 Fatigue was assessed by the Functional Assessment of Cancer Therapy–Fatigue subscale. 36 Exercise behavior was assessed by a validated modified version of the Godin Leisure Time Exercise Questionnaire.22,37
Sample Size Calculations
Sample size estimates were driven by hypothesized differences between the vibration and control subjects in NTx over the study. Changes were derived from a previous study using vibration training in postmenopausal women. 20 A priori, 2-tailed power calculations at an alpha of .05 and beta of .20 gave an actual power of 0.82 for a total sample size of 40 using G-Power software (University of Trier, Germany).
Statistical Analysis
Data were analyzed using the SPSS statistical software package (version 22.0, IBM Corp, Armonk, NY, USA). Data distributions were inspected for normality. Normally distributed data were described using mean ± SD and non-normally distributed data using median and interquartile range (IQR). Non-normally distributed continuous variables were log-transformed prior to use with parametric statistics if possible, otherwise nonparametric statistics were used. Analyses included standard descriptive statistics, unpaired t tests, chi-square, and Mann-Whitney U tests. Analysis of covariance (ANCOVA) models were constructed to compare groups, using the change scores as the dependent variable, with adjustment for baseline score and time on aromatase inhibitors. Although this difference between groups for time on AI therapy at baseline was not statistically significant (P = .06), we felt the difference between groups was clinically meaningful and therefore included it as a covariate in the analysis. Association between variables was determined by Pearson correlation. An intention-to-treat analysis was performed with missing outcome scores imputed from participants’ baseline scores (last observation carried forward). An alpha level of .05 was set as the criterion for statistical significance. Clinical relevance was assessed relative to the meaningfulness of bone and musculoskeletal outcomes compared with existing literature.
Results
Thirty-one participants were enrolled into the study. Recruitment ended at the completion of the funding period. Participant flow is presented in Figure 1. On average, participants attended 91.5% (range 78%-100%) of WBV training sessions.

Flow of subject progress through each stage of the trial.
Participant Characteristics
Baseline participant characteristics are presented in Table 1. The cohort had a mean age of 61.6 ± 8.3 years. The participants were on average overweight (body mass index = 28.8 ± 4.7 kg/m2), and the majority were nonsmokers. Baseline characteristics of the participants did not differ between groups, except for duration of AI therapy with participants in the vibration group having been on treatment for longer than the control (median 19 months, IQR 26.5 vs median 3 months IQR 13.5; P = .06). Approximately half (53.3%) of the participants were taking anastrozole, with the remainder taking letrozole. Osteoporosis was present in only 4 participants, with no group differences (P = .35). Baseline levels of 25-OH vitamin D, P1NP, and NTx/Cr were not different between groups (P > .53).
Demographics and Health Status. a
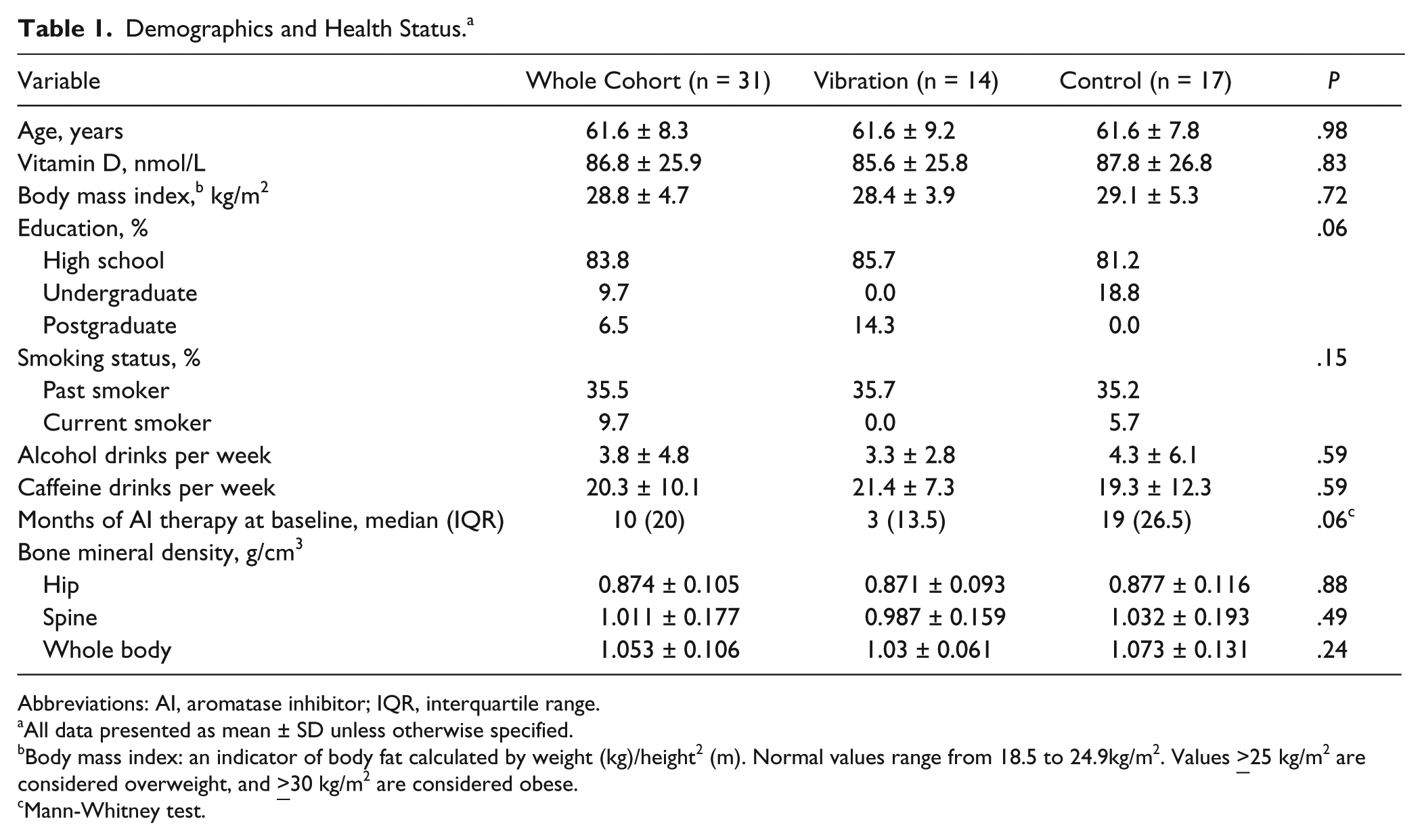
Abbreviations: AI, aromatase inhibitor; IQR, interquartile range.
All data presented as mean ± SD unless otherwise specified.
Body mass index: an indicator of body fat calculated by weight (kg)/height
2
(m). Normal values range from 18.5 to 24.9kg/m2. Values
Mann-Whitney test.
Markers of Bone Resorption and Formation
Results are presented in Table 2. Following 12 weeks of vibration training, NTx/Cr levels did not change differentially between groups (adjusted group difference −0.5, P = .929). Change in NTx/Cr was significantly negatively associated with duration of aromatase inhibitors (r = −0.46, P = .009), as well as baseline vitamin D (r = −0.41, P = .026). The change in NTx/Cr was not associated with changes in body composition (Ps > .657) or changes in physical function (Ps > .147), with the exception of chair rise, which was significantly negatively correlated (r = −0.38, P = .039).
Changes in Markers of Bone Resorption and Formation Following the Intervention.

Abbreviations: BCE, bone collagen equivalent; Cr, creatinine; NTx, N-telopeptide X; P1NP, type 1 procollagen N-terminal propeptide.
Adjusted for baseline value and time on aromatase inhibitors at baseline.
P1NP levels did not change differentially between groups over the 12-week intervention (adjusted group difference +5.3, P = .286). Changes in P1NP were not associated with aromatase inhibitor duration (r = 0.80, P = .670), or baseline vitamin D levels (r = 0.089, P = .645). Changes in P1NP were not associated with changes in body composition (Ps > .135) or physical function (Ps > .089), with the exception of chair rise, which was significantly negatively correlated (r = −0.36, P = .049).
Secondary Outcomes
All results of secondary outcomes are reported in Tables 3 and 4. No measures of physical functioning changed differentially between groups (Ps > .140). Changes in maximal strength and functional ability are illustrated in Figures 2 and 3. Body composition measures of lean and fat mass remained unchanged after 12 weeks (Ps > .548). There was no difference between groups for changes in joint pain, stiffness and difficulty with daily activities as measured by the WOMAC scale (P > 0.051). The intervention had no significant effect on fatigue (P = .079).
Changes in Physical Functioning and Patient-Rated Outcomes Following the Intervention.

Abbreviations: 1RM, one repetition maximum; IQR, interquartile range; WOMAC, Western Ontario and McMaster Universities Arthritis Index (higher scores indicate worse symptoms).
Adjusted for baseline value and time on aromatase inhibitor at baseline.
Mann-Whitney test.
n = 28 due to inability to complete upper body strength measures.
Fatigue was assessed by the Functional Assessment of Cancer Therapy–Fatigue subscale (higher scores indicate greater fatigue).
Changes in Body Composition and Bone Mineral Density Outcomes Following the Intervention.
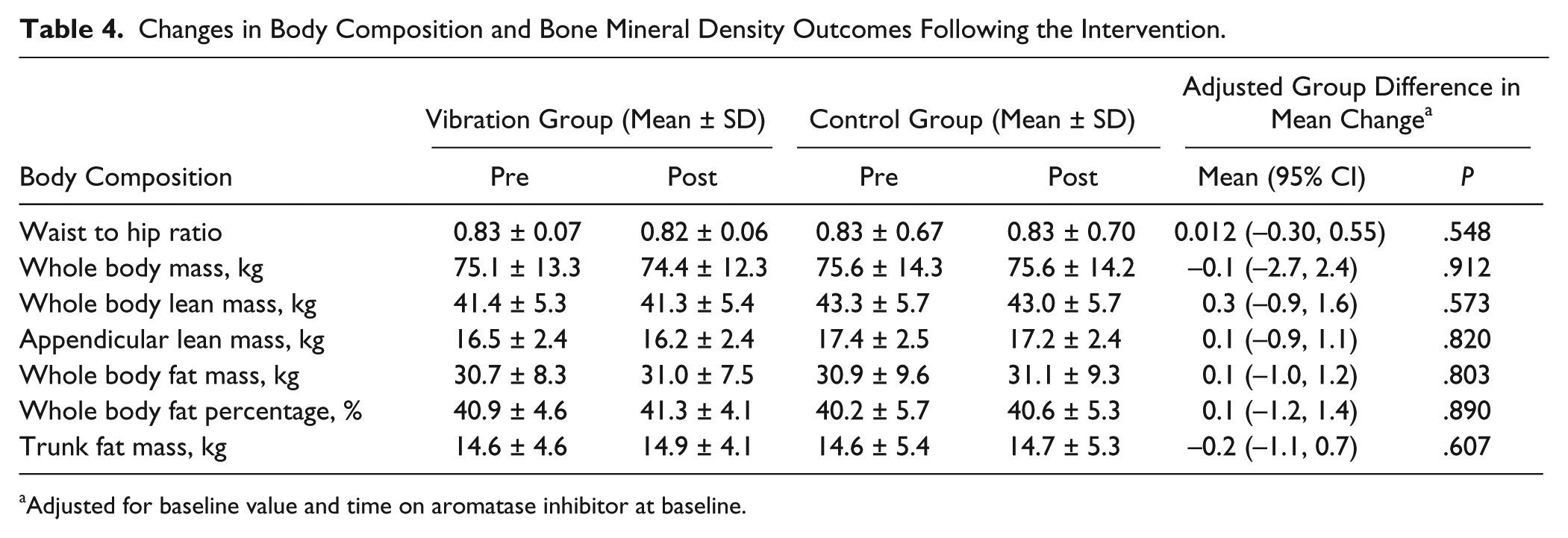
Adjusted for baseline value and time on aromatase inhibitor at baseline.
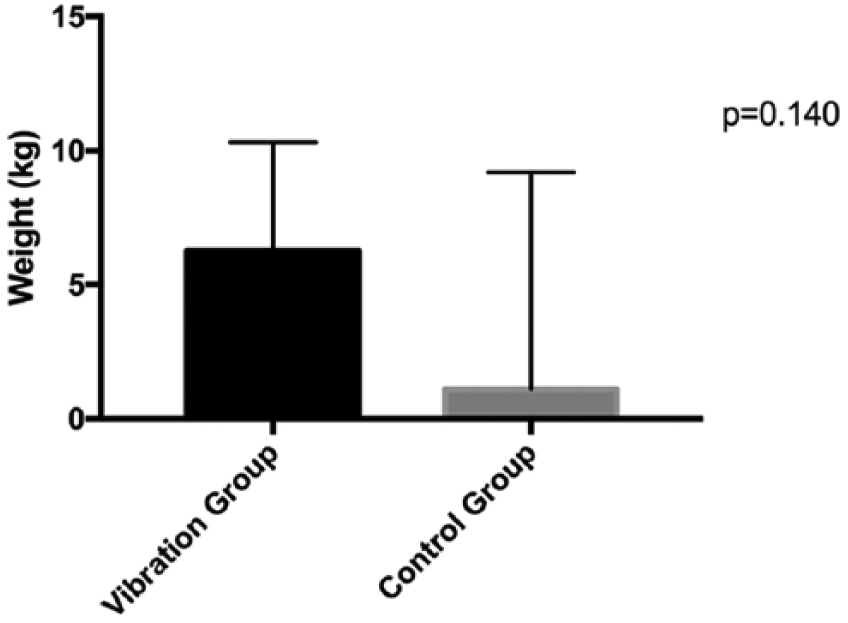
Median change in lower body strength (leg press) at 12 weeks.

Mean change in stair climb time at 12 weeks.
Adverse Events
Three adverse events occurred during the trial. One participant reported syncope during a training session. Another experienced increased swelling in her arm after exercise testing. A third experienced extreme distress on being allocated to the control group. All participants were able to continue with the intervention and the intervention was otherwise well tolerated.
Discussion
Aromatase inhibitor use secondary to breast cancer results in significant bone loss that puts women at risk for morbidity. This study examined the effect of short-term, low amplitude and low g-force vibration stimulus on markers of bone turnover in postmenopausal breast cancer patients receiving aromatase inhibitor therapy. Following 12 weeks of vibration training, there were no differences between intervention and control groups for markers of bone turnover, physical functioning, body composition, arthralgia symptoms, or fatigue.
Vibration training was well-tolerated by participants. Twenty minutes of vibration exposure 3 times a week for 12 weeks was not effective in changing markers of bone resorption or bone formation in the current study. Previous studies have shown beneficial effects on bone metabolism after vibration training in postmenopausal women, 20 and after combined aerobic and resistance training in female cancer survivors. 38 However changes observed in bone metabolism may not consistently translate into clinically or statistically significant improvements in bone density or strength. A recent meta-analysis suggests that vibration training in postmenopausal women has little effect on bone outcomes, as measured by DXA, at 6-month follow-up. 39 Comparison with other studies, however, is problematic because of large variations in study durations and dose of vibration. 40
A range of pharmaceutical interventions are available to improve bone mass. Bisphosphonates such as alendronate increase bone mineral density by approximately 5% to 15%, with better results observed in the lumbar spine and more modest results at the femoral neck.41,42 Different forms of exercise have been shown to be effective in improving bone density. Combined impact protocols, impact exercise training combined with resistance training, is the most effective option for maintaining or preserving bone mineral density in postmenopausal women. 43 A meta-analysis of the effect of exercise on bone mineral density on postmenopausal women showed a small effect at both the lumbar spine and femoral neck of a magnitude that is similar to vitamin D and calcium supplementation, but smaller than observed with bisphosphonates.42,44 Recent research suggests that 12 months of aerobic and resistance training does not improve bone mineral density in postmenopausal breast cancer patients taking aromatase inhibitors 16 or in those who have completed treatment. 13 The authors suggest that the amount of exercise required to sufficiently provide osteogenic stimulus for healthy postmenopausal women could be inadequate for those on aromatase inhibitor therapy. 16 The same could be true for the level of WBV stimulus tested in this study.
The mechanism by which vibration stimulus affects bone is not fully understood. It has been hypothesized that the anabolic effect of vibration on bone may be a result of stress exerted on bone through repeated loading and unloading, resulting in increased fluid flow. 45 Greater activation of muscle through enhanced sensitivity of mechanoreceptors, and increased osteogenesis in osteoblasts have also been observed, suggesting that vibration is anabolic at a cellular level.46,47 Human studies have reported potential benefits in bone,23,24,48-55 muscle function,52,54,56,57 balance and prevention of falls, 58 reduction of muscle spasticity in those with cerebral palsy, 59 and postural control in those with Parkinson’s disease. 60 However, the optimal time course, dose, and frequency of vibration to elicit optimal changes in bone are currently not established, with a wide variety of vibration exposure protocols leading to variation in changes in bone outcomes. Inconsistency in study nomenclature, design, and measurement of bone outcomes, reporting of adverse effects and noncompliance, highlight the lack of uniformity and small pool of information available on the effects of vibration on bone. 61 While improvements in BMD have been demonstrated in postmenopausal women following 6 months of WBV training, 54 the lack of effect observed in the current study may be partially explained by the short study duration, the dose of exposure, or the lack of intermittent vibration exposure. 62 However, the challenge of overcoming bone loss during AI therapy is great. While treatment with bisphosphonates has shown to be effective in improving BMD, in the adjuvant setting among women undergoing AI therapy such treatment does not prevent fractures. 63
No improvements in physical function or body composition were observed in the current study. Previous research indicates that WBV can improve muscular strength as well as physical functioning in older women, 64 as well as those with fibromyalgia. 65 Even low doses of vibration have previously improved physical function, with increases in lower limb muscle strength in older adults of 14% observed after 13 weeks. 66
Given the lack of change in physical function or muscle strength, the lack of change in body composition is unsurprising. Whole body vibration has previously been shown to improve body composition in other clinical populations, such as people with rheumatoid arthritis 67 and obese women. 68 However these interventions used a much higher dose of vibration of approximately 5g to 6g compared to our 0.3g—a dose chosen for its osteogenic effects. 23 It has been suggested that for muscular adaptation, higher frequencies and amplitudes are optimal. 69
Arthralgia is a commonly reported side effect of AI therapy with the incidence reported in clinical trials from 16.8% to 35.9%. 70 While aerobic and resistance exercise have been shown to improve symptoms of AI-induced arthralgia, 71 we did not observe such an effect with WBV. Similarly, while numerous studies have demonstrated an improvement in cancer–related fatigue with exercise, 72 no such effect was observed with WBV. As WBV has only a modest effect on energy expenditure and heart rate,73,74 the muscle contractions and perturbation of the cardiovascular system in short 20-minute bouts may not be sufficient to elicit such adaptations.
This study has limitations that should be considered in interpreting the results. We did not reach our target sample size, as such we were underpowered to detect a significant difference between groups, although this was unlikely to have affected the primary outcomes given no trend was observed. Further research is required in order to determine if higher doses of vibration, intermittent vibration combined with exercise on the platform, or longer duration of training (eg, 24 weeks) can elicit beneficial effects on bone during AI therapy. Recent evidence from meta-analyses suggest that side-alternating vibration platforms produce superior outcomes in postmenopausal women39,75—future research should focus on this mode of vibration delivery. Further research into the potential benefits of other forms of prescribed exercise on bone health during AI therapy should be considered.
To our knowledge this is the first application of WBV therapy in breast cancer patients undergoing AI therapy. Well-validated outcomes measured assessed markers of bone turnover, body composition, as well as a comprehensive assessment of physical functioning. We also report an excellent adherence rate to WBV training.
Conclusion
Short-term, low-amplitude and low g-force vibration stimulus does not appear to be effective for altering markers of bone turnover secondary to aromatase inhibitors in breast cancer patients. There also appears to be no benefit in physical functioning, body composition, arthralgia symptoms, or fatigue.
Footnotes
Authors’ Note
The funding source played no role in the design, collection, analysis, or interpretation of the data.
Nigel spry is also affiliated to Genesis Cancer Care, Joondalup, Western Australia, Australia.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was funded by The Cancer Council of Western Australia.
