Abstract
Narrow definitions of family can constrain survey items about obligations regarding who should care for older adults. Current measurement often does not account for the increased prevalence of diverse family forms and support received among older adults. We draw on six focus groups (N = 33) of family or friends caring for older adults with trouble remembering, memory issues, or dementia to explore definitions of family, caregiving, and responsibility. Although many caregivers immediately default to traditional definitions, the breadth of “family” seen as responsible and actual care networks are often broader. In many cases, caregivers considered friends and other non-kin as family because they provided care. Furthermore, both care and obligations are shaped by family dynamics and the older adult’s memory loss. Results suggest that survey measures should capture a wider range of relationship ties and dynamics to better understand family, caregiving obligations, and the tensions between them.
Despite large-scale changes in the family structures of older adults, namely rising rates of divorce or never marrying, alongside more cohabitation, step-ties, and chosen ties, 1 the measurement of families - especially in relation to caregiving and obligations - has been slow to shift. 2 For instance, many surveys of older adults and their families remain narrowly focused on “nuclear” (ie, spouse/children), biological, and legal relationships.3-7 This measurement gap for family ties leaves out other important social connections, including long-time friends and chosen kin.8-10 Similarly, the measurement of care obligations, defined as the responsibility to help an older adult in need, typically focuses solely on filial obligation, or adult children’s responsibility. 11 Yet, older adults adopt expansive definitions of family in whom they expect to help them, including extended family and even “church family”, 12 thus warranting an investigation into the disconnect with survey measures.
Investigating a diverse set of relationships is critical to understanding the various sources of support for older adults. 13 The measurements employed in investigations of these relationships neglect to capture when family members can and cannot be called upon, especially with regard to family-specific dynamics, like estrangement or ambiguity. 14 Analyses examining compositional changes in U.S. family caregivers show that a shrinking proportion of caregivers are adult children and a growing proportion are “other” types of caregivers, including other family and non-family caregivers. 15 Further, broader sets of social ties provide caregiving for members of marginalized communities—including diverse racial and ethnic communities, the LGBTQ + community, and older adults without partners or children.10,16-18 Yet, these populations are often underrepresented in large-scale caregiving studies to date.2,19,20 Thus, scholars across various fields have widely called for improved measurements of diverse family forms in relation to caregiving for older adults.21,22
Alongside measurement gaps, theoretical frameworks on caregiving have traditionally been built on the assumption of traditional family as “given” and friends or other extended relationships as “chosen”. 23 (p26) For instance, the Hierarchical Compensatory Theory, often used in the caregiving literature, relies on narrow definitions of family that prioritizes spouses and children over other types of relationships. 24 Yet, contemporary cohorts of older adults increasingly expect broad social support from both family and friends as they age regardless of their family structure, 25 and extended kin, neighbors, and friends can play vital roles in the care network.26,27 Further, hierarchical frameworks also neglect to account for issues of family dynamics including estrangement and ambiguity in relationships across the life course.28-30
In contrast, the Convoy Model of Social Relations can be used to take a more flexible and comprehensive approach to understanding relationships and care dynamics across the life course.29,31 The model captures a person’s “convoy” of relationships, including their structure, supports, and quality, as well as whether and how they can vary across the life course.29,31 Further, the model accounts for not only personal characteristics (eg, gender, race) but also social and situational characteristics like norms, roles, or culture, that influences the convoy. 31 The Convoy Model can be paired with the Informal Care Model (ICM), which has traditionally been used to understand one person’s role as a caregiver. The ICM similarly frames caregivers, in their choice to become a caregiver, as products of their individual dispositions—including attitudes, norms, and perceived barriers—within the context of larger social and family-specific norms. 32 The social norms and expectations that operate within families, also known as “kinscripts”, have been used to explain why people may behave differently from what broader social norms may prescribe, especially in relation to supports (eg, social norms may prescribe adult children to care, but within one’s family, cousins are more commonly relied upon). 33 We argue that it is important to consider how norms and obligations operate at multiple levels to shape caregiver activation, from overarching social and community norms and pressures to specific family “kinscripts” and the corresponding social assignments of individual members.
Finally, the number of older adults with dementia is expected to increase in the coming decades.
35
Family and unpaid care of older adults with dementia presents an important opportunity to understand definitions of family and obligations of care due to two main factors. First, caring for a person with dementia is more complex and requires larger care networks, including higher rates of care from others beyond a partner or children.36-38 Second, definitions of family may be either more rigid or more fluid due to the cognitive impairment of the older adult, considering that memory loss has the potential to alter family dynamics and individual family member’s thoughts and actions toward care responsibilities.39-43 Therefore, our study uses focus group methods to develop an understanding of how caregivers with traditional and non-traditional relationship ties to the older adult define “family,” caregiving obligations, and the connection between the two. We use this method with the aim of supporting the development of more comprehensive survey measures of family and caregiving obligation items and to also help inform theoretical models of caregiver activation. Among six focus groups (N = 33) of family and friend caregivers to an older adult who has trouble remembering, memory issues, or dementia (henceforth, “dementia”), we ask: 1. Who do caregivers consider to be the older adult’s family, and why? 2. Who do caregivers expect to take responsibility within the “family” for care, and why? 3. And, how does the older adult’s cognitive impairment affect definitions of family, caregiving, and obligations?
We use team debriefs, analytical memos, and the Rigorous and Accelerated Data Reduction (RADaR) technique to code transcripts in an iterative process,44,45 following grounded theory whereby themes emerged from the participants directly.
Methods
Research Design and Data Collection
This study serves as a starting point for a larger research agenda on understanding the measurement of family and caregiving obligations among diverse family forms of older adults. We conducted six focus groups (N = 33), as this method is well-suited for efficiently eliciting collective themes, challenges, and experiences through interactive discussions, allowing for information sharing and reflection. 46 In addition, focus groups present a clear way to include the population of interest in developing new measures. We used purposive sampling whereby recruitment efforts aimed for diversity in caregivers’ relationships with the older adult and in their demographic characteristics (eg, age, race/ethnicity, and LGBTQ + identity).
The Principal Investigator listed the study on the University of Michigan's UMHealthResearch.org Research Participant Registry, allowing the public to express interest in participating. The research team also distributed flyers in the community (eg, libraries, community organizations). The tagline on both flyers and the registry asked, “Do you help someone who is age 65 or older and has trouble remembering?” The materials further defined “help” as “assisting” the older adult, excluding paid work. We focused on “help/assistance” (vs “care”) because not all caregivers self-identify with that label, even though many would be considered caregivers by research standards. 47 Furthermore, we did not stipulate that the older adult needed a dementia diagnosis due to systemic disparities in receiving a formal diagnosis. 48 Individuals who indicated interest were directed to complete an online preliminary questionnaire designed to screen for study eligibility (eg, providing an example of the older adult’s difficulty with memory). Those who met the preliminary criteria were then contacted by phone for a second-stage screening, during which the research team confirmed eligibility, collected self-reported demographic information, and scheduled their focus group participation.
Focus Group Instructions and Questions

“Family” Roster and Grid
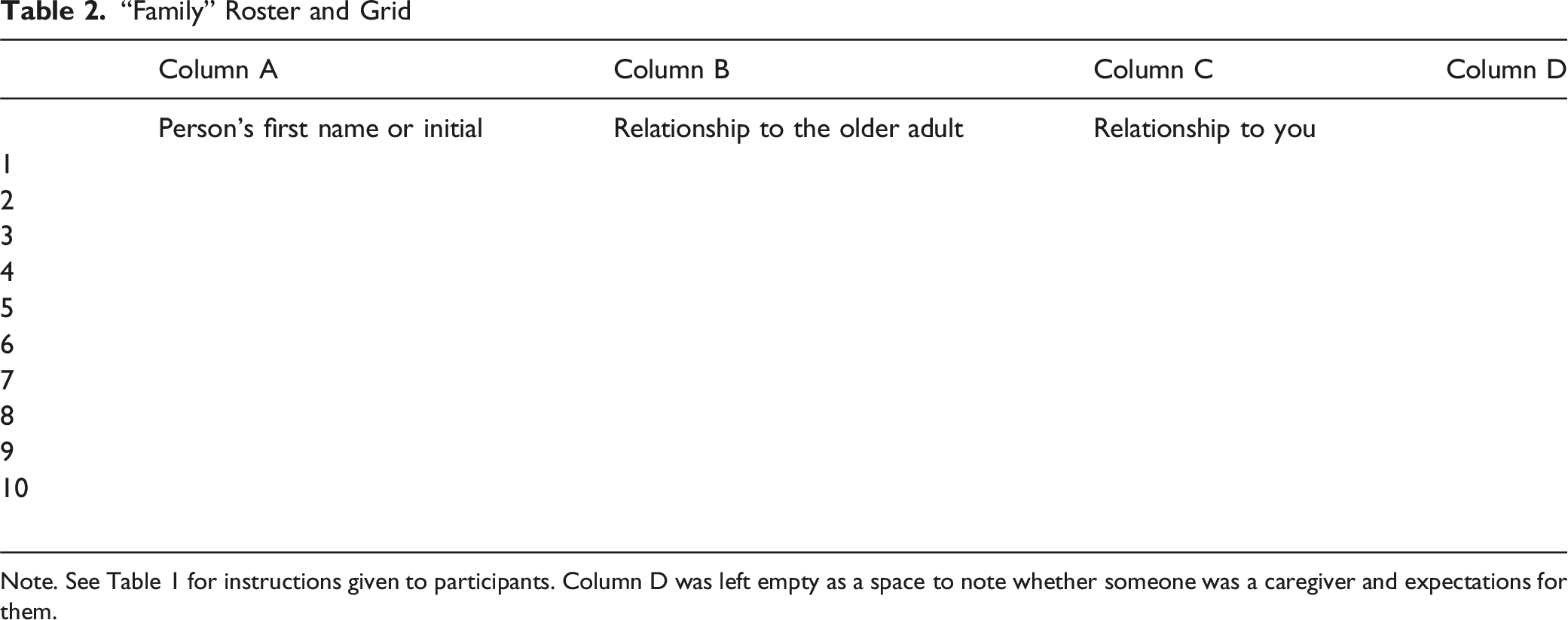
Note. See Table 1 for instructions given to participants. Column D was left empty as a space to note whether someone was a caregiver and expectations for them.
Data Analysis
The research team conducted data analysis using a series of iterative analytical techniques framed by grounded theory, whereby themes emerged from the participant responses. 49 First, after each focus group, team members and the trained facilitator conducted a debrief session, recording initial observations, emerging themes, and codes. Second, after all focus groups were conducted and transcribed, three team members (the Principal Investigator and two research assistants) holistically reviewed the transcripts, debrief sessions materials, and notes taken during the focus groups to independently write four integrative memos. Each memo focused on one analytic area aligned with the study question sections fielded to participants: definitions of family, caregiving responsibilities and obligations, the influence of cognitive impairment, and cross-cutting themes. These memos each contained preliminary analysis of the given section, representative quotes from the transcripts, and suggested codes, which were used to further define and systematically organize emerging themes and codes during the third step. 50
RADaR Analysis Table Example
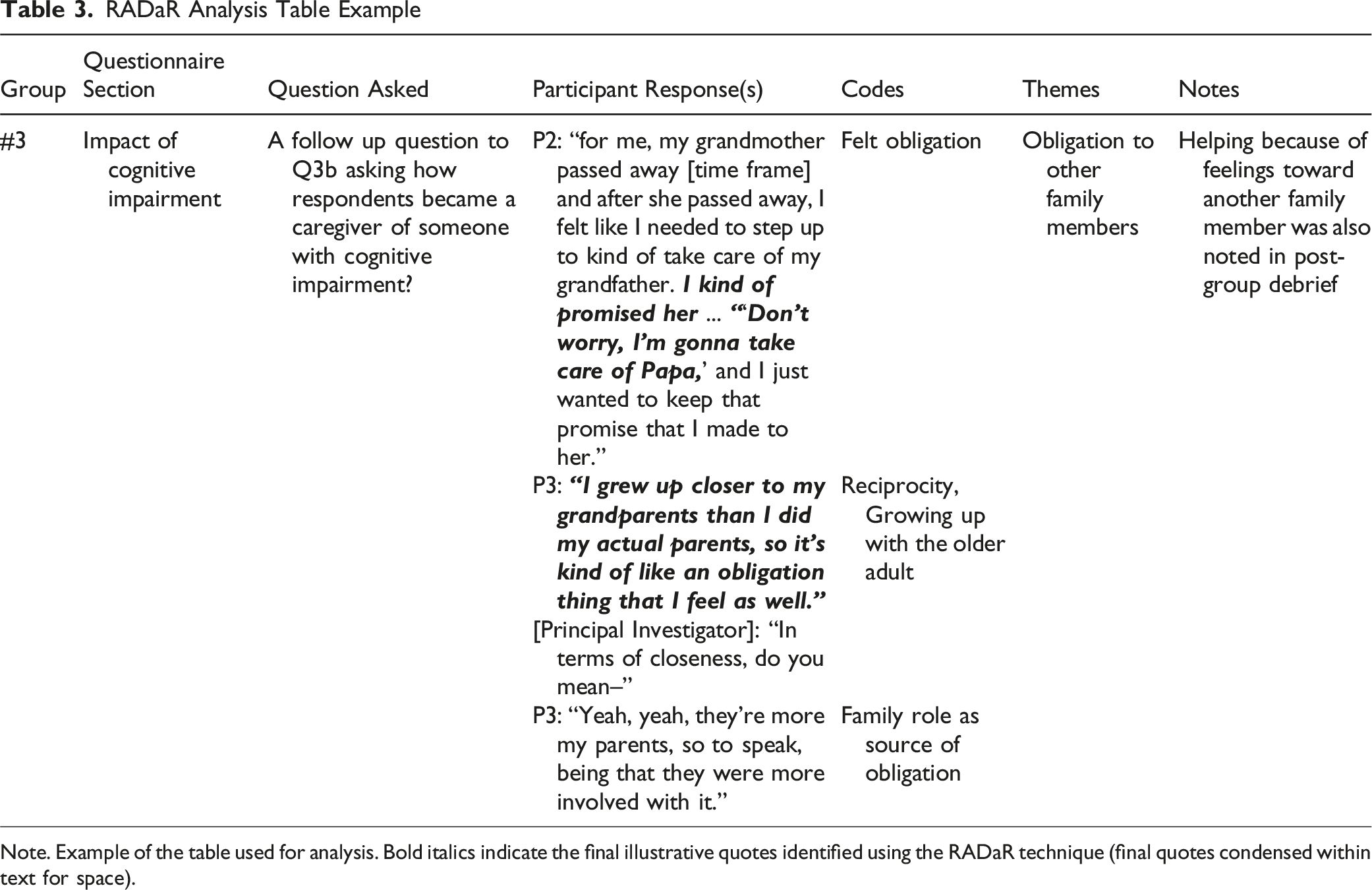

Note. Example of the table used for analysis. Bold italics indicate the final illustrative quotes identified using the RADaR technique (final quotes condensed within text for space).
Ethics Approval
The study was reviewed and approved for implementation by the University of Michigan Institutinoal Review Board (IRB).
Data Availability
The supporting data are not publicly available to ensure participant confidentiality and to comply with Institutional Review Board (IRB) and research ethics guidelines. The study was not preregistered.
Results
Focus Group Participant Self-Identified Demographics
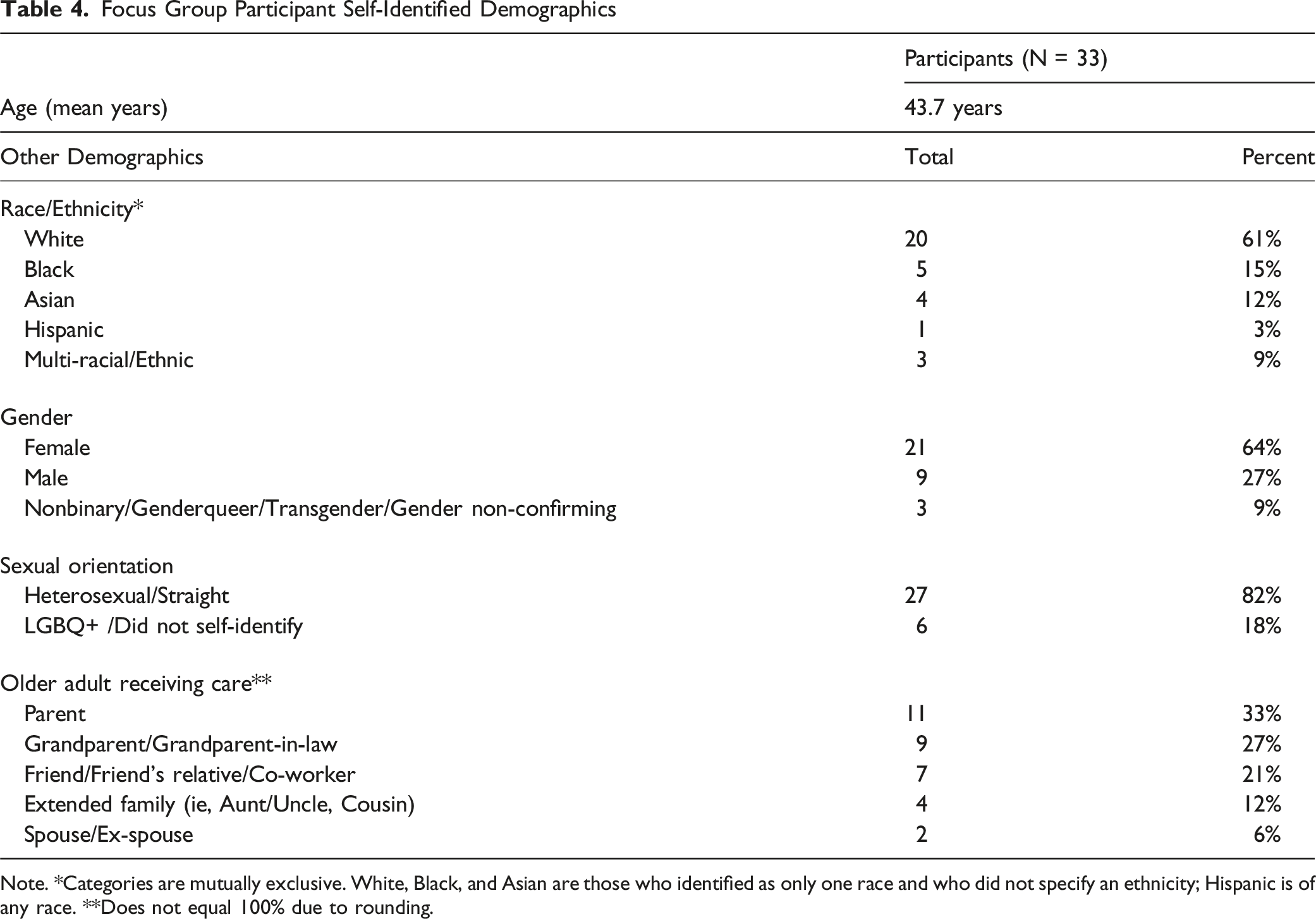
Note. *Categories are mutually exclusive. White, Black, and Asian are those who identified as only one race and who did not specify an ethnicity; Hispanic is of any race. **Does not equal 100% due to rounding.
Traditional and Non-traditional “Family”
We first asked respondents to chart and define the older adult’s family in their own terms. Many defaulted to the “family tree” at first but expanded their networks to include people who were “like family,” or those classified as chosen kin throughout the discussion. Respondents consistently used family language to describe and explain these relationships. For instance, a friend caregiver described, “I’ve known my friend for [decades], and we just, over those years, we became closer...to the point that we’re close enough to just feel like sisters” (FG5P1, caring for a friend). In addition to friends, chosen kin also included former legal ties who remained connected after their legal relationship ended (eg, divorce), extending their linked lives beyond legal bounds. An adult child caregiver describes, “[M]y parents are divorced, but my father’s brother and sister-in-law are still…close, kind of like family [to my mother]” (FG1P1, caring for mother). Both traditional and non-traditional ties described that their lives had been linked to the older adult receiving care. Accordingly, childhood experiences, and being “raised” by the older adult, were salient factors in caregivers’ perceptions of who counts as family. For instance, a grandchild caregiver noted, “My grandfather has two stepchildren, but he pretty much raised them and they're close with him…Even though they’re technically not blood, they’re still family” (FG3P2, caring for grandfather). These definitions of family established a foundation for how caregivers conceptualize the provision of care and, later, how obligations to provide care are assigned to individuals in the older adults’ convoy.
“Families are Messy, aren’t They?”
Family dynamics, including those between the caregiver, the older adult they care for, and other network members, greatly influenced who was activated as a caregiver for the older adult. Two members of the first focus group and their respective families—a wife nested within a stepfamily and an ex-husband—contrasted one another in whether other family members, especially adult children, provided care for the older adult. When asked to complete the family roster and identify who helps, the ex-husband caregiver remarked that “there’s nobody” and that his ex-wife's adult children “don’t want to spend time with [their mother], and they use me as an excuse for the reason why” (FG1P4, caring for ex-wife). Within the same group, a wife caregiver within a stepfamily provided the opposite account: “My [biological] kids are fairly helpful, but I think…they’re doing it for me” (FG1P2, caring for husband). Another respondent followed up immediately by stating, “To relieve your stress levels” (FG1P6, caring for father) to which the wife caregiver agreed “to relieve my load” (FG1P2, caring for husband). The caregiver and the older adults’ relationships within the larger family and social network were key to understanding who can be called upon and why.
However, perceptions of family and care were impacted not only by family dynamics, but also by their interaction within the context of cognitive impairment. Participant narratives showed how memory issues could exacerbate family relations. For instance, the aforementioned wife caregiver proceeded to describe how obligations for her husband’s biological children (her stepchildren) were not clear-cut, due to strain caused by a complicated family history. She explained how their strained relationship with their father was further complicated by his cognitive impairment because he “doesn’t remember the trauma that he created” (FG1P2, caring for husband). In contrast, the older adult’s cognitive impairment could lead to positive interactions or feelings due to forgetting certain family dynamics. For instance, a caregiver, who serves as the main and sometimes only caregiver for her cousin, observed, “She doesn’t remember [her son’s absence], so, yeah, there’s positives [to not remembering]” (FG1P3, caring for cousin).
“Doing It Anyways” Often Without Plans
Small families (eg, being an only child) or having no family at all (eg, due to death or estrangement) meant that some respondents had limited support in their caregiving responsibility. Family availability was sometimes seen as akin to financial resources, reflected by an adult child caregiver’s response to questions about obligation: “[I]t really all [comes] down to privilege and who has the ability to receive care, who has the money to receive care, who has the family, who has the resources, all of the above” (FG6P4, caring for father). One grandchild caregiver listed other family on the older adult’s family roster but clarified that her mother was truly the only other current caregiver: “[M]y family structure is very simple. There’s nobody else, so [it’s] just my mom right now” (FG4P2, caring for grandmother).
Furthermore, we heard from a majority of caregivers that the older adult did not often make care plans, and instead, caregivers came into their position reactively rather than through planning. For instance, a friend caregiver provided a blunt picture of the impact of having no family available and the precarity of the care situation if he had not decided to step into the role: “[My friend’s wife] would not have survived six months without getting me involved in her life after her husband [my friend] died. She would have died in a fire or on the floor” (FG5P5, caring for a friend’s wife). A lack of other options sometimes forced caregiving responsibilities, eliciting internalized or felt obligation to the older adult based on traditional roles. For example, a friend caregiver (FG6P2, caring for a friend’s father) described the relationship between the older adult she helps and his biological son: “His son…[is] not the best choice, to be honest. But [the father] doesn’t have...a lot of options. So, [his son] is doing it anyways, even though it’s triggering for him to care for his dad because he didn’t get cared for [by his father], and that makes things complicated.”
Caregiving is Doing Family
Despite varying interpretations on what classifies someone as a caregiver, aligned with the caregiving literature at-large, 47 participants overwhelmingly thought of caregiving as a way to “do” family. This concept—that individuals can reinforce or redefine family bonds and relationships through the provision of care—was especially relevant for people in the older adult’s network who were considered chosen family or “like family”. Chosen family included friends, neighbors, members of the church, and in some cases, formal, paid caregivers who had developed a deep connection with the older adult over a long duration. One nephew caregiver classified his uncle’s former student as a “family friend” who is “super helpful in helping to care for [his] uncle,” elaborating, “I definitely think of [my uncle’s former student] as part of the family. He’s closer to my uncle than a lot of [my uncle’s] own siblings” (FG3P6, caring for uncle). A grandchild caregiver similarly described a neighbor across the street as a “huge help,” expressing that the neighbor has become “like family with everything that she’s helped with” (FG4P1, caring for both grandparents).
Defaulting to Social Schemas of Obligation
Even though respondents discussed how the progression of cognitive impairment may change the form of caregiving provided, cognitive impairment did not necessarily alter perceptions of who is obligated to provide that care. One caregiver explained, “[I]t requires…more care overall…but I don’t think it changes who should be providing the care” (FG3P5, caring for grandmother). Overwhelmingly, respondents initially evoked traditional social schemas of duty and obligation to explain their expectations for immediate family members, especially for adult children of the older adult. A cousin who provided most of the care to her couin echoed this sentiment when discussing the older adult’s son: “I don’t think it’s my job. I think it’s his job” (FG1P3, caring for cousin). The group responded strongly to her story with agreement and discussion of how the son would need to pay someone to replace her if she was not there to provide care. After lengthy discussions about the extent of older adults’ networks, the “family as default” social norm was surprisingly resilient, often due to family norms that prioritize keeping problems private. For instance, a daughter caregiver noted: “The culture of my family is…we don’t let other people know we need help….[M]y parents would be mortified if I asked a neighbor to come in and help, mortified” (FG2P1, caring for mother).
Obligation to Other Family Members
Within-family dynamics and family history influenced who respondents felt should provide care, and obligation did not always align with what the older adult might expect. Across different family units, reciprocity (ie, giving back to those who gave to you), internally motivated many respondents to assume responsibility and care for the older adult. One grandson describes, “I grew up closer to my grandparents than I did my actual parents, so it’s kind of like an obligation thing that I feel [to care for them]” (FG3P3, caring for both grandparents). Some caregivers were motivated by their desire to give back to another family member—not necessarily the older adult with cognitive impairment. For instance, a grandchild expressed how she felt obligated to care for her grandfather because of the promise she made to her late grandmother, explaining, “I kind of promised her… ‘Don't worry, I’m gonna take care of Papa.’ and I just wanted to keep that promise” (FG3P2, caring for grandfather). However, expectations of reciprocity were not always met. One grandchild caregiver detailed unmet reciprocity in the current care of her grandfather, complicated by family dynamics. Her mother cared for her stepmother, but after the stepmother’s death, rather than help care for their stepfather, the grandfather’s stepchildren were only “...in his life in a tertiary way,” providing little help. The grandchild caregiver goes on to describe how she feels for her mother, saying: “I’m like, ‘You can’t reciprocate that [care]? You can’t show that kind of love back [to my grandfather] that my mom put into her stepmom?’” (FG3P1, caring for grandfather).
Kinscripts Interact with Larger Social Norms
Although respondents sometimes referenced an ideal hierarchy or flow chart for obligation, frequently mentioning adult children first, most groups ultimately resolved, “I don’t know that there is [a hierarchy], because there can be exceptions to everything” (FG5P5, caring for a friend’s wife). The interplay between defaulting to traditional social norms and the realities of family dynamics became apparent across the focus groups and during each of the conversations as they progressed. Family “kinscripts,” or within-family obligations and social norms, sometimes assumed that one family member had greater care responsibility due to their perceived ability and availability to provide care, not necessarily because of their relationship tie. For instance, obligation was intricately linked with implied gender expectations for capacity-based caregiver roles which, in the sample, were overwhelmingly assigned to women. One respondent mentions how she has always been seen as the “responsible” one in her family: “I think when you get that label, you probably [tend to] be a rescuer too.” (FG2P4, caring for father and uncle) to which the group replied in agreement.
Similar to the effect of limited families on who cares, limited families also affected assessment of obligation. For instance, a niece caregiver explained that her own family structure affected how other relatives perceived her responsibility: “I have no husband. I have no children. So other people, if you say you can’t do something, they’re like ‘I don’t know why not? You don’t have any kids!’” (FG2P3, caring for aunt). Additionally, the older adult’s family structure was salient for perceived obligations where difficult dynamics were also present, with one daughter caregiver explaining her felt responsibility: “I’m an only child. [T]here really is just nobody else to do it, especially since my mom makes everybody else angry.” Earlier, she had explained that her mother was estranged from her family and other social connections (FG2P7, caring for mother).
Unclear Obligations for Extended Family and “Like Family” Members
Respondents were not as strong in their responses regarding obligations for extended family, friends, and neighbors compared to those for immediate family members. Respondents often struggled to define obligations for extended and non-family social ties, as they, again, relied heavily on traditional social schemas that see nuclear family, especially adult children, as automatically responsible. For instance, one daughter questioned the obligation of non-immediate family: “How we can determine if somebody ‘should’ be…? I have my nephew, my niece, my sister-in-law, but [should they be expected to help] just because they are related to my mom?” She ultimately concluded, “I’m not sure if they should [be obligated],” yet clarified that they likely would help if asked (FG1P5, caring for mother). A lack of clear-cut obligations and boundaries between should vs would care were often compounded by the complexities of caring for a person with cognitive impairment in particular. One caregiver noted that obligations may be more fluid when the older adult has cognitive impairment because it is difficult “for people to wrap their head around [how to help]” (FG3P6, caring for uncle). The tension between non-traditional ties helping and what is expected of them is best illustrated by the example provided by a niece. She talked about how the neighbor “watches after” her aunt but clarified that family members are “the only people that are really obligated…unless there’s a best friend or some[one who is] like family, and so they help out” (FG2P3, caring for aunt).
Discussion
There is a growing population of older adults with dementia who have complex care needs and who receive many hours of help from large, diverse care networks.2,38 Yet, measurement of family ties and caregiving obligations for various members of these networks is lagging, despite the fact that contemporary families and support systems for older adults are diverse in their size, shape, and form (Seltzer, 2019). Therefore, this study explores how traditional and non-traditional family and friend caregivers of older adults with memory issues, trouble remembering, or dementia think about family, caregiving, and obligations. Six focus groups (N = 33) were conducted to evaluate who is providing care, who should be responsible for care, and how cognitive impairment influences caregiving dynamics and activation, with the goal of informing survey research. The findings provide insights into how traditional and non-traditional caregivers think about family and family dynamics in relation to who is obligated and activated to provide care.
Overwhelmingly, participants immediately defaulted to traditional social schemas about family, caregiving, and obligation. However, when given the space to discuss these issues further, many clarified that it depends on many factors including their definitions of family, caregiving, and responsibility. For instance, respondents first referenced popular schemas, like “the family tree,” but ultimately expanded out to other members within the older adult’s social network who could be considered family. Both traditional and non-traditional ties who were described as “like family” or those who became family through caregiving were important sources of support for the older adult. Caregiving became a way that non-traditional and more remote ties, such as the neighbors and former students described by participants, “do family” or “do kinship” in relation to the older adult, extending research on how care can reinforce or redefine family bonds.51-53 Obligations for caregiving were similarly traditional by default, but discussions among the focus groups showed that feelings of obligations are often much more complex than a sole reliance on filial obligation.
These findings can inform theories often used to understand caregiver activation. Although using the Convoy and ICM frameworks together advances our understanding of the complexity of caregiver activation within the context of the older adult’s network of social relationships, our results illustrate a few limitations of these models. For instance, the ICM conceptualizes the family and social network ties as concentric circles around the older adult, with the family subset into the larger social network, reifying a hierarchical structure. 34 Similarly, the Convoy Model uses “hierarchical mapping” with concentric circles to measure a person’s number of relationships and their strength, but in contrast to ICM, placement within the convoy is dictated by closeness to the person and is flexible over the life course. 31 However, traditional definitions of family maybe be too narrow for the reality of many care networks and the ways in which people’s lives are linked—and unlinked—across the life course. Instead of viewing family as a subset of the larger social network and being first in line before more extended ties, results suggest that an older adults’ family and social network may be two overlapping circles, where some non-traditional ties, like friends, may be located in the inner circle and, conversely, some family may not be included in the inner circle. Some people reside completely outside the circles, and these positions are not fixed like in the Convoy Model. Further, while immediate family may feel compelled and obligated to care, others may not perceive them as a good option for meeting some of the older adult's care needs as illustrated by stories shared in these focus groups.
Additionally, the findings here emphasize the intimate and intertwined definitions of family and caregiving obligations, while questioning the emphasis on planned behavior in existing caregiving frameworks like the ICM. That is, we found that most caregivers were often responding to immediate concerns instead of making plans to become caregivers, especially in relation to the changes of the older adult’s behavior due to memory loss. A friend caregiver, who provided care for his late friend’s wife due to a lack of other options, serves as the starkest example; this respondent did not feel as if he really had a choice in the matter and was driven by his values and commitment to his friend. Many of the theoretical models implicitly suggest a choice in providing care for older adults, but our results show otherwise. The idea of planned behavior or choice is also reflected in the limited amount of survey items that investigate these nuances, as many items to date rely on a single yes/no question about choice.
With our results in mind, we propose two main advancements to the measurement of caregiving and obligation. First, narrow measures of “family” in surveys miss a variety of different aspects of family structures and dynamics that impact both obligation and caregiving. Although our sample included both traditional and non-traditional caregivers, more work should be done to capture the understanding of family, caregiving, and obligation among chosen kin and “like family” members, as well as social ties who may no longer be formal family (eg, ex-wife or ex-husband). Measurement of family also has implications for policy; to date, most organizations and policies rely on traditional definitions that emphasize and assume personal or family responsibility for care, with their scope of family narrowly tailored to particular types of network members (eg, family of origin, people with children).52,54-56
Second, little is known about obligations and expectations for non-traditional ties and “like family” members potentially due to the narrow definitions of family across the caregiving literature. Current survey measures of obligation continue to follow a hierarchical structure without consideration of a more flexible and fluid conceptualization of family across the life course. By capturing more information about obligations for individuals beyond adult children only, we may be able to better understand the connection between expectations and actual care for non-traditional caregivers better than we are able to currently. That is, we need more work to understand under what circumstances do obligations change within the context of the older adults’ social and family network, including due to memory loss. This line of work could also help better understand how “doing caregiving” may be “doing family” for both traditional and non-traditional ties.
Our study has limitations. Despite efforts to post information throughout the community and recruit a diverse sample, our sample is limited. Future research could sample larger groups to compare and analyze more group differences. In addition, the use of help or assistance (and not care) in our materials may not have allowed us to capture all caregivers. However, research consistently shows that not all caregivers define themselves as such, so we felt that a broad definition would best ensure inclusive recruitment and alignment with national surveys that use the language of help (eg, see the National Study of Caregiving, NSOC). Future research could further tease apart the difference between help and care from the family perspective and continue to examine the boundary of family in relation to caregiving obligations. Finally, our study’s sample focused on caregivers for older adults with trouble remembering, memory issues, or dementia, potentially limiting the generalizability of our findings to other types of caregivers of older adults.
In the context of caring for an older adult with cognitive impairment, the boundaries of family and caregiving obligations are complex and ever-evolving. Our findings confirm that many caregivers for an older adult with dementia continue to see caregiving as the immediate family’s responsibility, even within complex families and when friends or neighbors are helping. However, tensions emerge as limited family availability—due to the number or quality of ties—affects the resulting care provisions. Further, the reality for many caregivers is that obligations often depend on other characteristics within the older adult’s network, including the family and networks’ dynamics and expectations. Understanding processes and obligations around caregiving is urgent as more family members and other unpaid caregivers are expected to provide care for the growing number of older adults with dementia within the context of changing families.
Footnotes
Acknowledgments
Thank you to the focus group participants and to group facilitator Margaret Hudson at the Survey Research Organization (SRO). Thank you to Judith A. Seltzer for your review and feedback on the paper. Thank you as well to Vicki A. Freedman, Bob S. Schoeni, Esther M. Friedman, and Jana Deatrick. We appreciate generous methodology advice from Donna Walter, Emina Dopp, and the Participant Engagement Team (PET) at the Institute for Social Research. Thank you to the following colleagues for guidance and feedback along the way: Jessica Halliday Hardie, Kristine Ajrouch, Melanie Baird, Rin Reczek, HwaJung Choi, Sheria Robinson-Lane, Amanda Leggett, and Sana Shaikh. Thank you to the Undergraduate Research Opportunity Program (UROP) for connecting students to research opportunities and to family and friends who provided feedback. This line of work was inspired by witnessing my brother, Mike, care for our grandmother, Dorothy, over a decade ago, and wanting research to better reflect families and care experiences of all forms (SP).
Ethical Considerations
The study was reviewed and approved for implementation by the University of Michigan Institutional Review Board (IRB).
Consent to Participate
All participants received both written and verbal consent to participate in the study.
Consent to Publication
All participants informed consent included a statement about publications.
Author Contributions
S.E.P. contributed conceptualization, funding acquisition, and project administration. S.E.P. and O.M. contributed to methodology. S.E.P., S.M.P, and O.M. contributed data curation and investigation. S.E.P., K.C. and S.M.P contributed formal analysis. S.E.P., K.C., S.M.P, and O.M. contributed writing original draft and writing and editing.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the National Institute on Aging (NIA) of the National Institutes of Health (NIH) (K99AG073473, R00AG073473, & P30AG012846 to SP; T32AG000221 to KC). The authors also gratefully acknowledge use of the services and facilities of the Population Studies Center at the University of Michigan, funded by NICHD Center Grant (P2CHD041028). The content is solely the responsibility of the authors and does not necessarily represent the official views of the NIH or the authors’ employers.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The supporting data are not publicly available to ensure participant confidentiality and to comply with Institutional Review Board (IRB) and research ethics guidelines. The study was not preregistered.
