Abstract
Posterior cortical atrophy (PCA) is a neurodegenerative condition primarily characterized by visuospatial deficits. Research on visual, spatial orientation, and functional impairments in PCA patients is limited. This report explores the impact of occupational therapy on 5 PCA cases with severe visuospatial and functional difficulties over 2 years. Patients, diagnosed through neuropsychological assessments and brain imaging, underwent occupational therapy focusing on cognitive remediation and rehabilitation strategies. Interventions included attention to contextual characteristics and errorless learning to promote independence in self-care. Two patients showed notable improvement on the Loewenstein Occupational Therapy Cognitive Assessment, while 4 demonstrated slight functional gains in activities such as grooming, bathing, dressing, and stair navigation. These findings suggest that cognitive stimulation and training can slow the decline in visuospatial skills and improve daily function. Future studies should incorporate a control group receiving standard occupational therapy and evaluate the long-term impact of these interventions on patients with PCA.
Keywords
Introduction
Posterior cortical atrophy (PCA) is an atypical form of dementia characterized by a core set of neuropsychological features primarily associated with the progressive impairment of various visual functions, including visual processing, spatial reasoning, and visuomotor organization, 1 as well as a decline in praxic skills. 2 A retrospective literature review in 2021, examining 65 patients diagnosed with PCA through neuroimaging between 1995 and 2020, revealed that their primary visual complaint was the inability to locate specific items in the environment. 3 Additionally, symptoms of cortical visual dysfunction can hinder patients’ ability to independently perform activities of daily living and participate in social activities. 4 Recent research indicates that patients diagnosed with PCA are more likely to experience moderate to very severe impairment in both basic and instrumental activities of daily living compared to those with Alzheimer’s disease. 3 Therefore, the implementation of effective rehabilitation programs, including cognitive stimulation, training, and rehabilitation to address the visual and functional problems of PCA patients, becomes paramount.
As most cases of PCA occur in individuals of working age, a person-centered care plan delivered by occupational therapy (OT) is necessary for managing their special visuospatial challenges rather than standardized dementia care. Cognitive stimulation for enhancing visual processing problems include training in visual exploration and ocular motor skills, thereby reducing errors in daily life. 5 By employing multi-sensory techniques, including auditory, kinesthetic, and tactile stimuli alongside visual tasks, patients can enhance not only their visuospatial skills but also address visual field deficits.6,7 Alongside visuospatial and visual perceptual impairments, a very high proportion of PCA patients exhibit constructional apraxia, a type of visuomotor organization dysfunction. 8 Recent literature revealed that cognitive training, such as arranging patterns of sticks and blocks has been found to effectively improve constructional apraxia in PCA patients, with sustained effects through short-term and long-term follow-up evaluations.9,10 Moreover, there is moderate to strong evidence supporting OT interventions utilizing cognitive rehabilitation to address visual and visual-perceptual impairments.11-14 Delivering an effective visual scanning strategy can help patients localize objects with stability and improve ocular-motor and searching skills, which assist in locating and identifying objects in a living context.15,16
The recent clinical practice guidelines for OT in older people should focus on developing their capacity to perform activities of daily living (ADL) and meeting their occupational challenges. Thus, occupational therapists should work with PCA patients and their families to reinforce residual visual abilities, decrease errors in daily life, and promote participation in meaningful activities.17-19 Considering that attention and orientation deficits significantly affect the independence of ADLs for PCA patients, strategies such as enhancing attention to contextual characteristics and employing errorless learning with a stepwise model were implemented. In this model, patients received clear verbal instructions followed by demonstrations to help reinforce the correct actions in their long-term memory. 20 However, currently, there are not many reports on the effect of a combining cognitive stimulation, training and rehabilitation strategies on improving visual-related problems and functional performance in PCA patients. To bridge the gap, the purpose of this report was to explore the effects of a hybrid approach of OT programs on improving or reducing progression in impairment of visual processing, visual motor skills and functioning in daily life for PCA patients through 5 case reports with multiple-case design.
Cases Report
Participants Information
Five patients with clinically defined PCA were referred by neurologist Dr Ming-Chyi Pai between May 2019 and May 2023.
Basic information
a) Case A, Mr. Chang, a 77-year-old retired professor, began experiencing difficulties with motor planning in instrumental activities of daily living approximately 7 years ago. Over the past year, he has faced significant challenges related to visuospatial functions, such as reading difficulties and poor integration of visual and motor skills, which are evident when he buttons his clothes. His handwriting has also become structurally impaired. These issues have led to a decline in his autonomy in daily life, raising concerns for his wife. Therefore, it is hoped that occupational therapy can improve his independence and autonomy in daily activities. b) Case B, Mr. Chen, a 59-year-old former market vegetable vendor, was referred to OT due to cognitive impairment, poor upper extremity coordination, and constructional apraxia. Approximately 2 years ago, he began experiencing significant visuospatial and functional difficulties, such as being unable to accurately locate and retrieve items purchased by customers. During his initial OT visit, he was also unable to write his full name or read a sentence, further highlighting his visuospatial and functional challenges. c) Case C, Ms. Lin, a 62-year-old retired office worker, visited the clinic accompanied by her niece, who described several concerns. Ms. Lin complained of blurry vision and an inability to read. She has also become incapable of managing household chores. Due to getting lost on her way home twice, she has hardly ventured out alone in the past 2 years. Ms. Lin expressed frustration with her vision problems, stating that she cannot find the things she needs and cannot correctly press the elevator’s floor buttons. Both Ms. Lin and her family strongly hope to improve her impaired visual skills and overall functioning. d) Case D, Mrs. Lin, a 63-year-old woman, has experienced slowly progressive memory and cognitive impairment for over 2 years. She exhibited significant visuospatial and functional difficulties, including trouble differentiating the colors of stairs, dressing apraxia, and mis-reaching for items during daily activities and while preparing hot meals. She was referred for a cognition-perception examination and OT services to promote her independence in both basic and instrumental activities of daily living. e) Case E, Mr. Chen, a 75-year-old retired professor, visited occupational therapy accompanied by his wife due to his inability to independently perform daily activities. He has experienced slowly progressive cognitive impairment for 2-3 years, though no active treatment had been pursued. His wife became particularly concerned when she noticed his struggles with finding and using the door handle, reluctance to go out alone, and difficulty recognizing his surroundings. These visuospatial and functional challenges prompted them to seek OT to improve his quality of life.
Clinical impairment information;
The Characteristics of Clinical Impairment of the PCA Patients.

Intervention
The Detailed Treatment Programs for Managing Visual-Related Problems and Improving ADL Performance for Patients With PCA.

Timeline
Outcomes were assessed at the baseline visit (T0) and after 16 weeks of treatment (T1).
Clinical Finding of the Participants Before and After Intervention
The relevant clinical findings of the participants were described based on their cognitive-perceptual and ADL profiles.
Cognitive-perceptual profile of the participants (Figure 1): The Loewenstein Occupational Therapy Cognitive Assessment (LOTCA), known for its good assessment validity and reliability,
21
was used for basic cognition and perceptual assessment of patients with posterior cortical atrophy symptoms. It includes domains of orientation, visual perception, spatial perception, motor praxis, visuomotor organization, and thinking operations. It provides detailed cognitive profile with sufficient sensitivity to differentiate levels of dementia.
22
The possible score range is from 26 to 115. Item scores below 16 for orientation, 16 for visual perception, 12 for spatial perceptions, 12 for motor praxis, 28 for visuomotor organization, and 31 for thinking operation have been classified as impaired cognitive function. According to Figure 1, we found heterogeneity in the participants’ cognitive abilities across various domains. Based on the baseline LOTCA evaluation, deficits in motor and constructional apraxia, poor spatial perception and thinking operation were found of all the recruited PCA patients. The Moreover, most of the participants showed deficits in visuospatial disorganization in subtests of geometric copy and clock drawing (Figure 2). LOTCA sub-scores and total score for 5 cases at 2 different time points. (T0: Time point of baseline evaluation; T1: Time point at which persistence through 16 weeks of treatment was observed). Moderate to severe constructional apraxia is present on the tests of copying geometric figures and drawing a clock. Examples from 2 of the patients, upper showed the performance of Case A and lower showed the performance of Case B.

After completing the OT program, the mean change in LOTCA total scores from T0 to T1 for the 5 cases ranged from zero to 8 points, with an average improvement of 2.6 points. Case C and Case D, showed considerable improvement in LOTCA total scores. Case C specifically showed remarkable improvement in the scores of the visual perception and visuomotor organization subtests, while Case D performed better in orientation and spatial perception. Case A and Case B showed substantial improvement in spatial perception even though they did not show significant improvement on total score of LOTCA. Case E also showed no improvement in the total LOTCA score. While there was some improvement in visuomotor organization skills, there was a decline in orientation.
ADL profile of the participants (Figure 3): The Functional Independence Measure (FIM) motor subscale was utilized to assess patients’ functional abilities. Each of the 13 items on the motor domain of the FIM is scored from 1 to 7, indicating a range from total dependence to complete independence. The FIM has clinical utility in measuring the disability of patients with dementia.
23
At the baseline evaluation, most of the PCA participants’ self-care activities ranged from complete independence to requiring supervision. Only Case E needed moderate assistance with bowel and bladder control. ADL profile of the participants using FIM motor subscale. (T0: Time point of baseline evaluation; T1: Time point at which persistence through 16 weeks of treatment was observed).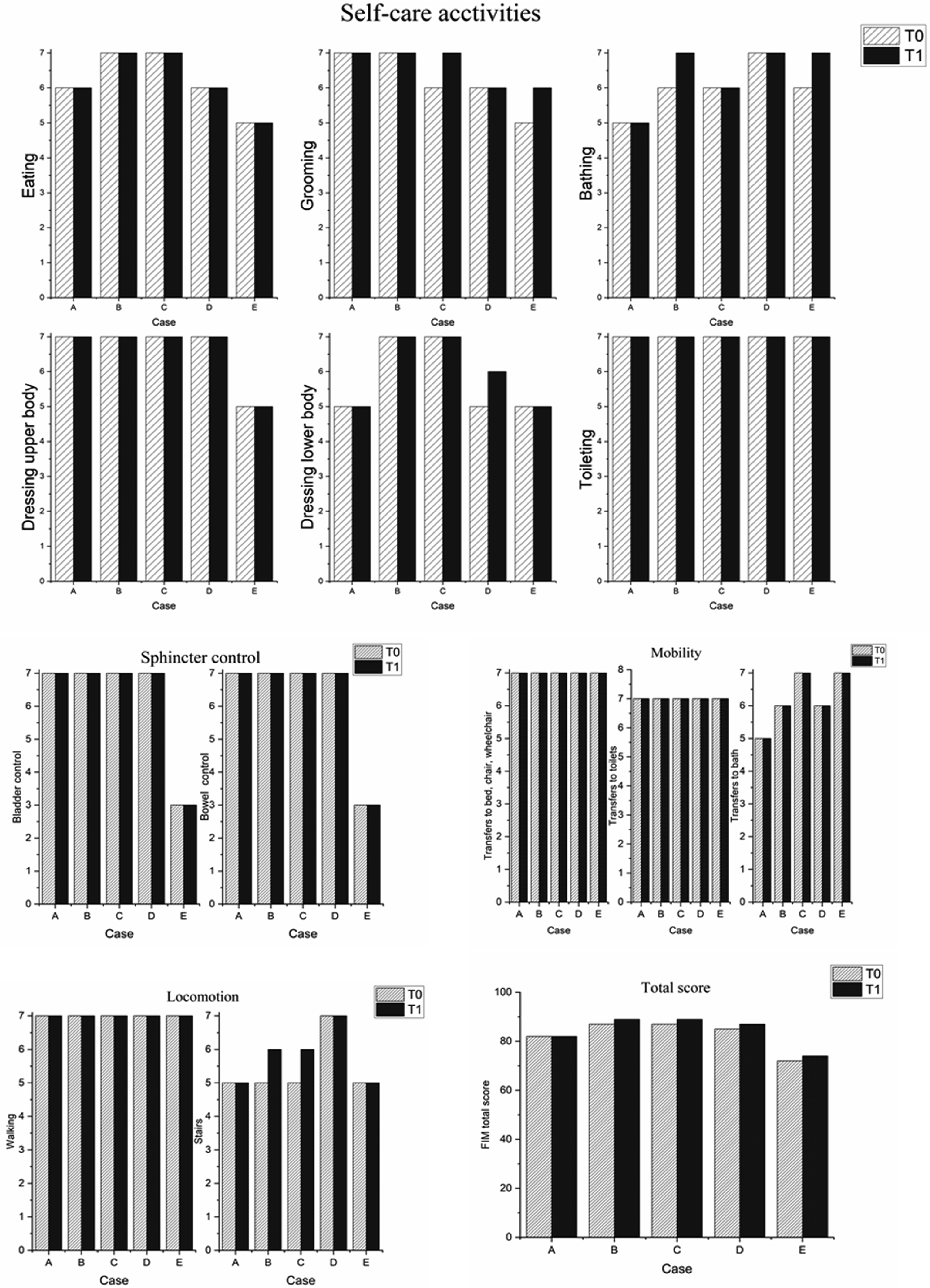
After treatment, 4 out of 5 patients achieved slight improvements in their functional abilities, such as grooming, bathing, dressing the lower extremities, and going up and down stairs. Only Case A maintained the same functional status. He was able to perform activities such as bowel and bladder control, transfers, locomotion, and communication, as well as self-care activities, ranging from complete independence to requiring supervision.
Discussion
The case reports demonstrate that a hybrid model of occupational therapy has shown promising potential in managing the visuospatial and functional problems of the PCA patients. The hybrid model of occupational therapy was adopted to address the patients’ visuospatial issues. Additionally, increasing their attention to contextual characteristics and implementing errorless learning training improved functional outcomes. Based on the cognitive and functional profiles of the 5 cases, the hybrid treatment model indeed slowed the deterioration of their visuo-perceptual and visuomotor skill problems and maintained their self-care abilities. Notably, among the patients included in this report, 3 belong to the type of early-onset dementia and are under 65 years old.
Cognitive rehabilitation programs and psychoeducational programs are indeed among the most commonly used training strategies for PCA patients. 24 However, recent scientific research analyzing the effects of an environment decluttering strategy on the functional performance of PCA patients found that it did not impact the time taken to locate objects. 16 Impairments in visuospatial processing in PCA patients can trigger brain reorganization, leading to an increase in behavioral deficits. 25 Consequently, eliciting plasticity has emerged as a new perspective to enhancing treatment outcomes. Cognitive remedial approaches, have demonstrated efficacy in activating the brain and improving visuospatial and visuomotor skills. 26 Recent studies indicate that integrating spatial auditory cues with voluntary visual training enhances brain activation during multisensory integration, alters functional activation across multiple brain regions and leads to measurable performance improvements in PCA patients. 27 Furthermore, studies show that orientation cues assist navigation and spatial orientation in PCA patients. 28 Utilizing multimodal cues, such as audiovisual or tactile-visual processing, promotes faster and stronger gamma-band synchronization in the occipital cortex 29 and enhances both visuospatial perception 30 and processing. 31 These findings align with our case report, highlighting the potential benefits of multisensory approaches for PCA rehabilitation. Additionally, adopting a neurofunctional approach involved real-world skills training, 32 such as practicing tasks like copying, drawing, or constructing simple figures, to enhance constructional apraxia. Two patients, Case C and Case D, had reduced performance in most household chores over the past 2 years due to visual perception issues and fear of making mistakes in daily living, resulting in widespread nonuse of brain activity. By adopting the cognitive stimulation and training for brain activities described in this report, significant improvements in cognitive-perception abilities were observed. 33 Moreover, other several factors may explain the overall improvement in LOTCA scores for Cases C and D, including: (1) Baseline clinical factor: Case C exhibited less severe impairment, as indicated by a CDR score of 0.5 and a CDR-SB score of 2.5, which may have contributed to a more favorable response to the training; (2) Age factor: Both patients were significantly younger than the other participants, which may have positively influenced their cognitive plasticity and overall improvement; and (3) Training factor: Cases C and D demonstrated greater independence in daily living and did not become easily fatigued or distracted during cognitive stimulation and training sessions. Each treatment session lasted approximately 50 minutes and focused on visual-related issues, incorporating 1 to 2 treatment items each for cognitive stimulation, training, and rehabilitation. This approach was more intensive compared to the interventions received by Cases A, D, and E for managing visual-related problems.
Both visual scanning exercise and cognitive rehabilitation approaches help patients develop strategies to compensate for impairments and optimize their remaining cognitive-perceptual abilities. As PCA patients often demonstrate oculomotor abnormalities, 34 such as impaired smooth pursuit and shorter object-fixation time, visual scanning techniques involving a series of short, regularly-spaced eye movements can enhance the ability to locate and identify objects. 35 Additionally, symptoms of simultanagnosia prevent patients from perceiving the overall picture of their entire visual field 36 ; using a strategy of considering the whole before focusing on details can help them navigate their visual environment effectively. 37 Other compensatory strategies described in this report included using anchors to guide visual search and maintaining a clutter-free environment. These strategies help direct eye movements toward the impaired visual field, enhancing residual vision 38 and reducing errors in daily life. Based on the obtained LOTCA scores, 4 patients showed improvement in spatial perception, while another patient maintained his spatial perception despite PCA being a progressive neurodegenerative disease.
Errorless learning, which involves breaking daily tasks into smaller steps and providing prompts, has been reported to support patients with dementia 39 or apraxia 40 in achieving success in daily living. Particularly, impaired scene perception noted in most PCA patients 41 severely affects their daily life performance. Therefore, exercises focused on identifying and describing key features in an environment help PCA patients attend to contextual characteristics, promoting independence in daily living. In this report, combining exercises to enhance patients’ environment awareness with errorless learning has demonstrated effectiveness in optimizing performance in daily activities and reducing functional decline. This finding is supported by previous evidence. 4 During the training process, there was graduated practice of increasingly complex tasks, a focus on enhancing attention to contextual characteristics, and errorless learning. Among the 5 patients we recruited, 4 showed improvement in self-care abilities, including tasks such as grooming, bathing, and climbing stairs. One patient maintained their self-care abilities. These results demonstrate the effectiveness of our interventions in daily living activities.
In summary, our interpretation of the improvement in skills over time, despite neurodegenerative decline, is multifaceted. First, cognitive remediation through cognitive stimulation and training likely overrides the learned non-use phenomenon associated with visuospatial issues. This intensive practice may lead to temporary performance enhancements, particularly in tasks specifically targeted during the intervention. Second, we propose that these improvements might contribute to a slowing of the overall trajectory of functional decline. By maintaining higher levels of engagement and cognitive stimulation, the intervention could help preserve neural pathways and delay the progression of deficits. While the intervention may offer immediate competence gains through overlearning, we believe its long-term impact includes a deceleration of the decline in functional abilities. However, given the high heterogeneity of symptoms among PCA patients, the degree of improvement with the intervention varied significantly across individuals. This highlights the necessity for additional research to evaluate the treatment’s overall effectiveness. While this case report provides valuable insights, it is important to acknowledge its limitations. One limitation is that the visual perception assessment using the LOTCA may not effectively detect visual problems in PCA patients. Despite reports of visual issues from both patients and their caregivers in daily life, 2 patients still received perfect scores. Secondly, we lacked longitudinal LOTCA data for PCA patients who receive standard OT, which constrained our ability to make comparisons. Additionally, the lack of blinding for participants and researchers indicates insufficient evidence for the effectiveness of the hybrid model of OT. To address this limitation, future research should address these limitations by incorporating blinding procedures and including a control group to strengthen the robustness and credibility of the findings. Additionally, we will conduct extended follow-up assessments to evaluate the long-term effects and confirm the effectiveness of this intervention.
Conclusions
This case report emphasizes the critical importance of a hybrid model of occupational therapy for managing cortical visual problems and enhancing life autonomy in patients with PCA. As our understanding of the rare evidence regarding visuo-perceptual issues in PCA patients grows, continued research on developing and testing clinically feasible interventions will be essential for improving care.
Footnotes
Author Contributions
HYH, LCK and MCP were the main contributors in the determination of unmet clinical needs, the study design, and data collection. HYH and HCY carried out the development of the occupational therapy programs for the posterior cortical atrophy. HYH, TSK, and HCY participated in the examinations of the participants. HYH, and LCK participated in the data interpretation, and analysis. HYH, LCK and MCP helped to draft the manuscript. All authors read and approved the content and format of the final manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Data Availability Statement
The research group is continuing to perform additional analyses using the current experimental data set from this study. However, portions of the data set may be made available upon reasonable request, pending approval from the Institutional Review Board and the corresponding author.
