Abstract
This study examined the use of potentially inappropriate medicines that may affect cognition (PIMcog) in people with dementia and its associated factors. Medical records of all outpatients with dementia attending a tertiary hospital in Vietnam between January 1, 2015, and December 31, 2016, were examined. Medicine use was assessed against a list of PIMcog. Variables associated with having a PIMcog were assessed using a multiple logistic regression. Of the 128 patients, 41% used a PIMcog, 39.1% used cholinesterase inhibitors (CEIs) concomitantly with anticholinergics, and 18% used antipsychotics. The number of hospital visits (adjusted odds ratio [OR]: 1.08; 95% confidence interval [CI]: 1.02-1.16) and number of treating specialists (adjusted OR: 0.61; 95% CI: 0.45-0.83) were associated with PIMcog use. This study highlights a high-level use of medicines that can further impair cognition or reduce the effectiveness of CEIs in people with dementia. Efforts to improve quality use of medicines for this population are warranted.
Keywords
Introduction
Dementia is a costly health condition that has a significant impact on individuals, their family caregivers, communities, and society. 1 By 2018, dementia will become a trillion US dollar disease and the cost continues to rise to US$2 trillion by 2030. 1 Already being the home of nearly 60% of people with dementia worldwide, compared to high-income countries, low- and middle-income countries (LMICs) are facing a much more rapid growth in numbers of people with dementia 1 often without a well-developed or well-funded health-care system, resulting in lack of diagnosis and poor-quality treatment for people with dementia. 2 Not an exception, Vietnam with a projected increase from 10% in 2015 to 28% in 2050 in the proportion of its population aged 60 years and above, 3 and an estimated dementia prevalence ranging from 4.2% to 7.9% in these elderly individuals 4,5 may have as many as 2.4 million people living with dementia by the mid-21st century.
Most people living with dementia are older, 6 thus likely to have multiple chronic conditions and taking multiple medicines 7 with the associated increased risk of adverse drug reactions due to drug interactions and altered pharmacokinetic and pharmacodynamic profiles in older persons. 8 These issues can confound dementia management where multiple medicine use and aging make individuals more sensitive to the effects of medicines on cognition. 9,10 Lack of evidence from randomized controlled trials for the use of medicines in people with dementia because of their exclusion in most clinical trials further compounds the problems of medicine use in this population. 11,12
In the absence of preventive or curative treatments of dementia, current pharmacological therapies focus on modifying symptoms of cognitive impairment (eg, using antidementia medicines such as cholinesterase inhibitors [CEIs] or memantine), managing behavioral and psychological symptoms of dementia (BPSD), and managing cardiovascular and cardiometabolic symptoms, which if not managed would make dementia worse. Other management strategies focus on maintaining cognition. For this reason, medicines with anticholinergic or sedative effects should be avoided where possible in persons with dementia due to the association between these medicines and cognitive decline. 9,13,14 Further, anticholinergic medicines have the potential to antagonize the effect of CEIs, the medicines to treat symptoms of dementia. 15 Among anticholinergic and sedative medicines, antipsychotics are often used to manage BPSD. However, they have limited efficacy 16 and can be successfully deprescribed. 17
Different factors have been reported to be associated with inappropriate medication use. 18 -21 They can be categorized into system and environmental factors (eg, residential aged care structure), 22 physician and health professional-related factors (eg, diagnostic and therapeutic knowledge and skills, prescribing culture), 23 or patient-related factors (eg, age, gender, education or socioeconomic status, comorbidity, or number of medicines prescribed). 24,25 Little is known about the quality use of medicines in people with dementia in Vietnam and its associated factors. This study was conducted to examine the prevalence of potentially inappropriate medication use for people with dementia with a focus on those that affect cognition (PIMcog) and to analyze potential variables associated with having a PIMcog to provide evidence-based information for subsequent programs supporting quality use of medicines in dementia care in Vietnam. We also examined the prevalence of concomitant use of CEIs and anticholinergics, as well as the appropriateness of selection, initiation dosing, and the length of use of antipsychotics in people with dementia in Vietnam.
Methods
Data Source and Study Design
The National Geriatric Hospital (NGH) is the leading tertiary hospital in Vietnam taking care of geriatric patients. In 2008, the hospital started its national program on “Management, care and treatment of people with dementia.” Patients referred to NGH for cognitive impairment have a thorough medical review, including medical history, assessment of mental status and mood testing, physical and neurological examination, and tests to rule out other causes of dementia-like symptoms. Patients diagnosed with dementia are included in the hospital’s dementia program and are requested to visit every month for checkup and medicine dispensing, which is subsidized under a special insurance program. A database of these patients has been established, and data since January 2015 have been computerized.
Analyses of medicine use in all outpatients with dementia attending NGH were conducted for the period January 1, 2015, to December 31, 2016. Medical records and prescriptions of all patients diagnosed with dementia during the study period were examined. The medical record contains information on patients’ demographics, diagnosis of dementia, cognitive function test (eg, Mini-Mental State Examination score), other comorbidities, and prescribing information (medicine name, strength, dosage, quantity, and route of administration). Health service characteristics were recorded, including the specialty of prescribers.
Medicines Included in Analyses
Data were collected using a data collection form developed in a macro-enabled excel spreadsheet. Medicines were coded according to the World Health Organization’s Anatomical Therapeutic Chemical classification system. 26 Antidementia medicines included in the analysis were donepezil (N06DA02), rivastigmine (N06DA03), and galantamine (N06DA04). Memantine (N06DX01) was not available in the Vietnam market. A master list of all medicines used in people with dementia at the hospital during the study period was established. The medicines on this list were first assessed against a PIMcog list 24 —Vietnamese modification, which contained individual medicines available in Vietnam considered potentially inappropriate for use in older people with cognitive impairment (Appendix A) and developed based on Beers 2012 criteria 27 and STOPP 2014 criteria 28 but limited to those medicines that are related to cognitive impairment. 24 Second, concomitant use of CEIs with anticholinergic medicines was assessed using a list of medicines available in Vietnam with clinically relevant anticholinergic and sedative properties (Appendix B) following a previously published approach 29,30 and based on a consensus combination of different anticholinergic scales. 31 Concomitant use was defined where coprescribing of ECIs with anticholinergic agents was recorded at the same hospital visit. Medicines accounting for the difference between the PIMcog list and the list of medicines with anticholinergic or sedative effects are presented in Appendix C.
A list of antipsychotics used by study participants was also compiled. Incident use of antipsychotics was defined as prescribing antipsychotics after no prescription of antipsychotics was recorded at any of the previous 3 monthly hospital visits. Continuous use of antipsychotics was defined as prescribing antipsychotics at consecutive monthly hospital visits. Information on type, initial and maximum doses, as well as duration of antipsychotics continuously prescribed were collected and assessed against the Australia’s dementia care guidelines 16 and Australian Medicines Handbook. 32 These references were used in the absence of Vietnam’s dementia care guidelines. In Australia, risperidone is the only antipsychotic medicine subsidized for treatment of BPSD resistant to nonpharmacological measures in Alzheimer’s-type moderate-to-severe dementia (for up to 12 weeks), with an initial dose of 0.25 mg twice daily, increasing by 0.25 mg daily every 2 or more days if necessary to a maximum dose of 2 mg per day. 32
Statistical Analyses
Descriptive statistics were used to describe the demographics and medicine use in the population with dementia, including the proportion of patients who used at least 1 medicine on the PIMcog list, who used CEIs with anticholinergic medicines concomitantly, or who used at least 1 antipsychotic medicine during the study period. The median number of unique medicines used by individual patients across hospital visits was calculated, and the median of median value across patients was reported. Multiple logistic regressions were conducted to assess the association of different variables and having a PIMcog, including age, gender, type of dementia, severity of dementia, number of comorbidities, number of medicines used other than PIMcog, number of hospital visits, and number of treating specialists. Missing data were imputed using the fully conditional method in a multiple imputation approach. 33 All analyses were performed using the SAS 9.4 statistical package (SAS Institute, Cary, North Carolina).
Results
Participant Characteristics
Data were retrieved from 128 patients who participated in the national program on “Management, care, and treatment of people with dementia” at some time during the study period (Table 1). The mean age (standard deviation) of the participants at the first hospital visit for dementia treatment during the study period was 71.9 years (11.0). Sixty four (50%) patients had at least 1 comorbidity and 32 (25%) had 2 or more comorbidities. The most common comorbidities include hypertension (n = 30, 23.4%), hyperlipidemia (n = 24, 18.8%), and diabetes (n = 12, 9.4%).
Participants’ Demographic Characteristics.
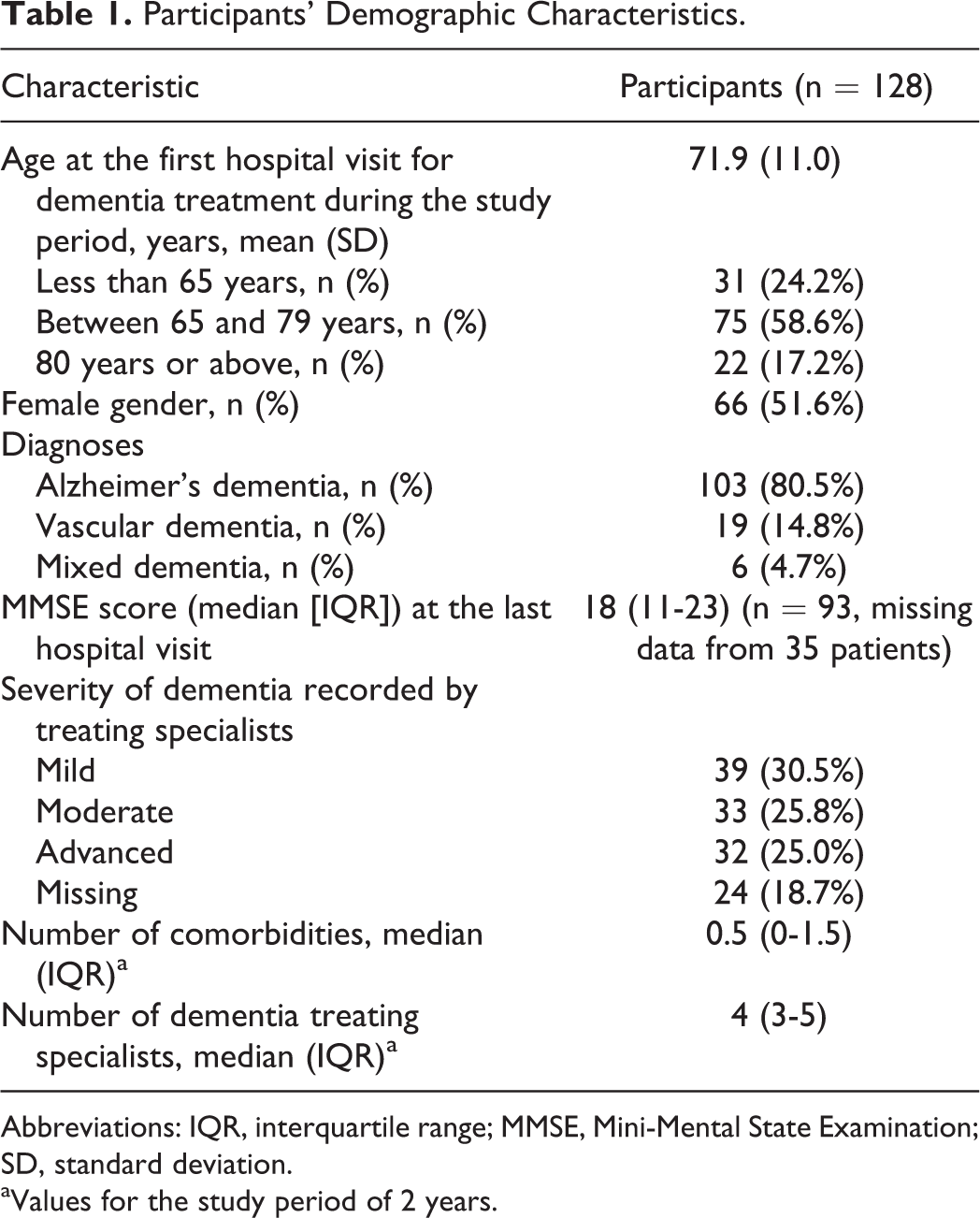
Abbreviations: IQR, interquartile range; MMSE, Mini-Mental State Examination; SD, standard deviation.
aValues for the study period of 2 years.
General Use of Medicines and Antidementia Medications
Half of the participants were prescribed between 2 and 4 medicines per hospital visit (Table 2) and 18 (14.1%) patients had a median of 5 or more medicines prescribed per visit. Throughout the study period, the most commonly used medicines included CEIs and ginkgo biloba. In total, 122 (95.3%) patients used medicines considered to improve cognitive function at some time during the study period, of whom 115 (89.8%) patients used CEIs and 77 (60.2%) used ginkgo biloba products. Among 115 patients who were prescribed CEIs, 94 (81.7%) patients had these medicines prescribed continuously for more than 6 months and 31 (27.0%) patients were at a severe stage of dementia. Cholinesterase inhibitors being prescribed to patients were galantamine (n = 109, 85.2%), rivastigmine (n = 23, 18.0%), and donepezil (n = 11, 8.6%).
Medicine Use.

Abbreviations: CEIs, cholinesterase inhibitors; IQR, interquartile range; PIMcog, potentially inappropriate medicine for people with cognitive impairment.
aThe median number of unique medicines prescribed for individual patients across hospital visits was first calculated and the median of median values across patients was reported.
Other medicines commonly prescribed were vitamins, for example, vitamin E (n = 86, 67.2%), vitamin B1 (n = 63, 49.2%), vitamin B6 (n = 47, 36.7%), and vitamin B12 (n = 45, 35.2%). The use of diazepam (n = 42, 32.8%) and piracetam (n = 31, 24.2%) was also frequently observed.
Use of PIMcogs
Fifty three (41.4%) patients were prescribed at least 1 PIMcog at some time during the study period. Three patients were prescribed 2 or more PIMcog concomitantly at the same visit on at least 1 occasion in the 2-year period (Table 2). Similar figures were observed when assessing the PIMcog use in study participants aged 65 years or above only (data not shown).
The most commonly used classes of PIMcog were sedatives (eg, benzodiazepines: n = 42 and nonbenzodiazepine hypnotic: n = 1) and anticholinergics (eg, tricyclic antidepressants: n = 10; antiparkinson agents: n = 5; and antipsychotics: n = 2). The most commonly used individual PIMcogs were diazepam (n = 42), amitriptyline (n = 10), and trihexyphenidyl (n = 5).
Our initial multiple logistic regression model consisted of the following variables: age, gender, type of dementia, severity of dementia recorded by treating doctors, number of comorbidities, median number of medicines other than PIMcog used per hospital visit, number of hospital visits, and number of treating specialists. The backward elimination using a significance level of 0.2 to retain variables in the model resulted in a final model, which contained the following variables: gender, age, number of hospital visits, and number of treating specialists. The final logistic regression model indicated that a higher number of hospital visits during the study period (adjusted odds ratio [OR]: 1.08; 95% confidence interval [CI]: 1.02-1.16) was positively associated with PIMcog use. By contrast, higher number of treating specialists (adjusted OR: 0.61; 95% CI: 0.45-0.83) was negatively associated with PIMcog use. No statistically significant associations between older age (adjusted OR: 1.02; 95% CI: 0.99-1.06) or female gender (adjusted OR: 1.55; 95% CI: 0.72-3.30) and PIMcog use were found.
Concomitant Use of CEIs With Anticholinergics
Seventy-eight (60.9%) patients were prescribed at least 1 medicine with sedative or anticholinergic effects at some time during the study period. Excluding those using medicines with sedative effect only, 66 (51.6%) patients were prescribed at least 1 anticholinergic medicine at some time during the study period. Fifty patients concurrently used an anticholinergic agent with CEIs, accounting for 39.1% of all 128 patients or 43.5% of 115 patients who were using CEIs.
Antipsychotics Use
Twenty-three (18.0%) patients were prescribed at least 1 antipsychotic medicine at some time during the study period. Sixteen (12.5%) patients were concomitantly prescribed antipsychotic medicines with CEIs. Antipsychotic medicines most commonly used were sulpiride (n = 9), followed by risperidone (n = 8), quetiapine (n = 8), clozapine (n = 1), and olanzapine (n = 1). Ten patients initiated antipsychotics during the study period and 13 patients were prescribed antipsychotics within their first 3 hospital visits. Six patients used antipsychotics continuously for more than 3 months.
Among 8 patients who used risperidone, 3 patients initiated risperidone during the study period, all of whom had their initial dose of more than 0.5 mg/d; one with an initial dose of 2.0 mg/d and 2 with 1.0 mg/d.
Discussion
Our results show that potentially inappropriate medicine (PIM) use is common in patients with dementia attending a tertiary hospital in Vietnam. Forty-one percent of patients used at least 1 medicine considered potentially inappropriate for use in older people with cognitive impairment, while 39.1% used CEIs together with an anticholinergic agent. Eighteen percent of patients were prescribed antipsychotics, of whom a quarter used the medicines continuously for more than 3 months. Of those who initiated risperidone, the initial dose of risperidone was not optimal in treatment of BPSD.
These findings are not unique to Vietnam. Studies in developed countries have shown that anticholinergic and sedative medicines have been frequently prescribed in people with dementia or concurrently used with CEIs although the extent might vary. 24,29,34 -36 The PIMcog use was reported among 21.4% of patients with dementia attending memory clinics in Australia, with anticholinergics and sedatives being the most common classes of PIMcog. 24 In our study, these 2 classes were also the most frequent among PIMcog with benzodiazepines (eg, diazepam), which have both sedative and anticholinergic properties, topping the list. The prevalence of PIMcog in our study (41%), however, almost doubles the number in the Australian study. 24 One possible explanation for this difference is the different designs of the studies. In our study, we looked at all prescriptions at repeated hospital visits of individual patients during the study period of 2 years, whereas the Australian study only looked at medication exposure of individual patients at one time point of recruitment. 24 Another possibility is the difference in the quality of health service delivery between a high-income country and an LMIC with LMICs having been reported to have a more severe problem of inappropriate medication use. 37
In the United States, 37% of CEI users received anticholinergics, 34 which is similar to the finding in our study (39.1%). A study on the use of antipsychotics among people with dementia in Australian residential aged care facilities showed that 44% of patients with dementia received antipsychotics concomitantly with antidementia medicines at some time during the study period; of the subset who initiated antipsychotics, 53% used antipsychotics continuously for more than 6 months and 43% had suboptimal initial doses of risperidone. 38 The institutional setting of residential aged care facilities might explain the higher prevalence of antipsychotic use in the Australian study compared to that in our study of community-dwelling outpatients (18.0%). 39,40 A prevalence of antipsychotic use of 12.8% and 25.3% (18.1% overall) was reported for people with dementia in noninstitutional and institutional settings, respectively, in Sweden, 40 and up to 25% of people with dementia in the United Kingdom were estimated to be on antipsychotics at any time. 41
Our results show antidementia medicines used to boost cognitive function in people with dementia in Vietnam included CEIs and ginkgo biloba. More than 95% of patients were prescribed at least 1 antidementia medicine, of which 89.8% were prescribed a CEI and 60.2% were prescribed ginkgo biloba products. Cholinesterase inhibitors and ginkgo biloba have a modest efficacy if any in dementia and cognitive impairment 42,43 and conflicting evidence or no long-term efficacy (more than 6 months). 44,45 Cholinesterase inhibitors have been associated with a number of adverse reactions (eg, bradycardia and syncope). 44 Ginkgo biloba has a better safety profile 43,46 but cerebral bleeding and prolonged bleeding have been reported to be associated with ginkgo biloba use, and this may be intensified with use of antidepressants, 47 a common medicine class used by people with dementia. 40 The antidementia medicines therefore should be considered for deprescribing when patient’s dementia has progressed to a severe stage. 44 Among patients who were prescribed CEIs in this study, 81.7% had these medicines prescribed continuously for more than 6 months, and 27.0% were at a severe stage of dementia. Periodical review taking into account both perceived benefits and adverse effects to consider stopping antidementia medicines is recommended. 16
In our study, more than 2 of 5 patients with dementia used a PIMcog. We found that PIMcog use was positively associated with a higher number of hospital visits. A potential explanation is that patients in the NGH’s national program were requested to visit the hospital every month for checkup and medicine dispensing, higher number of hospital visits therefore means longer participation in the program and more exposure to neurologists. This might have led to more health complaints being communicated, hence higher variety of medicines prescribed during the study period (ie, higher total number of unique medicines in 2 years, data not shown), although the number of medicines prescribed per visit was actually decreased. Previous studies have shown that taking a higher total number of medicines was associated with PIMcog use. 24,48,49 In contrast, the number of medicines other than PIMcog prescribed at each hospital visit was found not associated with PIMcog use in this study.
Adjusted for other variables in our multiple logistic regression, age (adjusted OR: 1.02; 95% CI: 0.99-1.06) and female gender (adjusted OR: 1.55; 95% CI: 0.72-3.30) were not significantly associated with PIMcog use. This finding is consistent with prior research in which the authors found a similar adjusted OR of 1.02 (95% CI: 0.91-1.14) and 1.24 (95% CI: 0.79-1.93), respectively. 24 Lack of coordinated care and poor communication between treating physicians have been the reason for the association between the number of physicians involved in a patient’s medical management and the risk of inappropriate prescriptions or drug-related hospital admissions in developed countries. 50,51 Interestingly, a higher number of treating specialists, who were all neurologists, were found negatively associated with PIMcog use in this study. A possible explanation is that seeing different providers creates a check and balance system that helps to reduce the discretion of individual physicians in prescribing. However, further exploration is warranted to understand the rationale behind the prescribing practices of medical specialists for people with dementia in Vietnam.
In this study, we also looked at the use of all PIMs with sedative and anticholinergic properties. Anticholinergics have been known to be associated with cognitive decline 9,13,14 and might reduce the efficacy of CEIs due to an antagonistic mechanism. 9,15 Apart from worsening cognitive impairment, 52 sedatives also increase the risk of falls. 53 People with dementia have impaired cognition and are vulnerable to falling, 54 thus should not be prescribed sedatives and anticholinergics where possible. Nearly 61% of our participants were prescribed sedatives and anticholinergics during the study period and almost 40% used CEIs and anticholinergics concomitantly.
Eighteen percent of our patients used antipsychotics for the management of BPSD. Sulpiride was the most commonly used antipsychotic, which may not be ideal because sulpiride has been found to be associated with an increased risk of extrapyramidal symptoms at a similar level to haloperidol. 55 Risperidone might be a better option as it is considered the best evidenced treatment of BPSD. 56 -58 Nevertheless, due to modest efficacy and poor tolerability 57,59 as well as association with stroke, 60 hip fracture and pneumonia, 61 a poorer quality of life, 62 and increased mortality 63 of antipsychotics, these medicines should only be used as a last resort to manage severe BPSD with low initial dose and regular review every 1 to 3 months for deprescribing. 16
Our study had some limitations. First, we only examined the use of medicines in patients with dementia attending 1 tertiary teaching hospital in Vietnam, and these patients were in a national program on “Management, care and treatment of people with dementia.” The pattern of medicine use in people with dementia in our study therefore only reflects the prescribing practice within the teaching hospital. There is a special insurance cap that limits the total cost of medicines per prescription for patients in this program and this is likely to affect the prescribing practice. In addition, our sample is quite small and of one ethnicity only. While these shortcomings limit the generalization of our findings to dementia treatment in Vietnam and to other samples, particularly those in high-income countries, our study has identified the scope for improvement in prescribing practice for people with dementia at a tertiary teaching hospital level.
Secondly, PIMcog list was developed based on Beers and STOPP criteria which are for patients aged 65 years or over and 24.2% of our patients aged less than 65 years. However, while reporting the prevalence of PIMcog use for all study participants, this prevalence was similar to the PIMcog use prevalence assessed in the subgroup of patients aged 65 years or over only. We also examined the use of medicines against a list of medicines with anticholinergic and sedative effects, which should be avoided in people with dementia because of their potential adverse effects including but not limited to cognitive impairment. Several scales have been developed for screening anticholinergic medications but considerable variation exists across those scales. 31 Using a uniform list of anticholinergic medicines developed based on consensus on the clinical relevance of alleged anticholinergic properties among different scales in addition to sedative medicines for screening PIMs with anticholinergic and sedative effect can be considered as strength of our study.
In conclusion, PIMcog use, anticholinergics and sedatives use, and concurrent use of CEIs with anticholinergics were prevalent in patients in the Vietnam national dementia care program. The use of antipsychotic medicines seemed suboptimal from the selection of antipsychotic products to the initiation dosing to the treatment duration. Further research exploring the rationale behind the current prescribing practice and interventions such as pharmacist medicine review, clinical audits, and targeted deprescribing is needed to improve quality use of medicines and health outcomes of people with dementia in Vietnam.
Footnotes
Appendix A
Appendix B
Appendix C
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the China-Australia Centre for Health Sciences Research seed funding grant (T.A.N, S.Q, E.E.R, L.K.E, M.G, and H.W). T.A.N and L.K.E are the recipients of an Australian NHMRC-ARC Dementia Research Development Fellowship (T.A.N Grant identification number APP1103860; L.K.E Grant identification number APP1101788). E.E.R is supported by an NHMRC Senior Principal Research Fellowship (Grant identification number APP1110139). The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
