Abstract
Alzheimer’s disease leads to progressive cognitive function loss, which may impair both intellectual capacities and psychosocial aspects. Although the current knowledge points to a multifactorial character of Alzheimer’s disease, the most issued pathological hypothesis remains the cholinergic theory. The main animal model used in cholinergic theory research is the scopolamine-induced memory loss model. Although, in some cases, a temporary symptomatic relief can be obtained through targeting the cholinergic or glutamatergic neurotransmitter systems, no current treatment is able to stop or slow cognitive impairment. Many potentially successful therapies are often blocked by the blood–brain barrier since it exhibits permeability only for several classes of active molecules. However, the plant extracts’ active molecules are extremely diverse and heterogeneous regarding the biochemical structure. In this way, many active compounds constituting the recently tested plant extracts may exhibit the same general effect on acetylcholine pathway, but on different molecular ground, which can be successfully used in Alzheimer’s disease adjuvant therapy.
Introduction
Nowadays, the increased age-related diseases prevalence (arthritis, diabetes, neurodegeneration, and pulmonary fibrosis) may be associated with increased life expectancy. 1 The etiology and pathogenesis of many age-related diseases determined by unbalanced life style habits are generally incurable but responsive to palliative treatments. In spite that, neurodegeneration remains the one which exhibits low pharmacological response considering many available treatments. 2 Moreover, neurodegeneration is irreversible, the drugs’ purpose being to ease the patient’s distress or to delay the final stages. 3 -5
One can assume that while the average life expectancy is raising due to extensive life support schemes, the occurrence of age-related disorders will increase. Unlike other organs, the effects of brain’s aging are more visible later in life. Although life support therapies are meant to prevent body degradation, brain degeneration becomes visible generally after 85 years of life, mainly in behavioral patterns—emerged as memory loss and cognitive decline. 6 In the past, due to lesser life expectancy, brain degeneration effects were less visible, the individuals conceding due to other organ failure (more frequent, according to historical and geographical particularities, lung, heart, bowels, lack of strength, etc). 7 Even though brain degeneration occurs later in life, in some cases, it could occur earlier with no chance for cure and only few opportunities for slowing the process. One of the most common disorders which cause brain degeneration is Alzheimer’s disease (AD).
In this way, this minireview aims to describe several alternatives in cognitive decline prevention or slowdown based on plant extract administration effective in cholinergic pathway impairment, the main pathological hypothesis in AD development.
Alzheimer’s Disease Memory Loss Pathways
Alzheimer’s disease can be considered responsible for more than 60% of dementia cases diagnosed after 65 years old. 8 This pathological condition progressively affects the brain through a degenerative process, significantly visible in some individuals due to physiological, neurological, psychical, biological, and molecular concerns. This process leads to progressive cognitive function loss, which may impair both intellectual capacities and psychosocial aspects, 9 all of which can determine a strong burden on the society’s shoulders due to its responsibility for the patients. Therefore, AD is extremely important to study, whereas the future predictions of its prevalence are truly concerning—its incidence could increase by 3- or 4-fold in the next 25 years. 10
The neuropsychiatric symptoms such as memory loss, confusion, hallucination, depression, and anxiety can be associated with neurodegeneration and are roughly common to all types of dementia exhibiting particular features for each and every one. The most troublesome of them remains the memory loss due to its complex mechanism of development. Several studies show that memory loss may occur after brain injuries which lead to extensive neuronal damage. 6 This injury may be caused by actual physical, vascular, or molecular incidents that trigger extensive immune responses leading to mass apoptosis or synapse distress. 2
In this way, the study by Bie et al shows that molecular unbalance such as amyloid accumulation could impair specific cellular signaling engaged in memory formation. 11 In fact, mice models revealed that memory loss mechanisms are much more complex than previously thought. Thus, molecular regulation and gene transcription both play important roles in memory formation. 12
One of the widely known theories of AD is the cholinergic theory. This theory provides significant evidence in explaining its implication in the occurrence of several important brain areas molecular signaling deprivation which can be translated in the visible pathological features such as cognitive decline. This would be the reason why the drugs that modulate acetylcholine signaling are still the main part of the symptomatic treatment of AD. 14
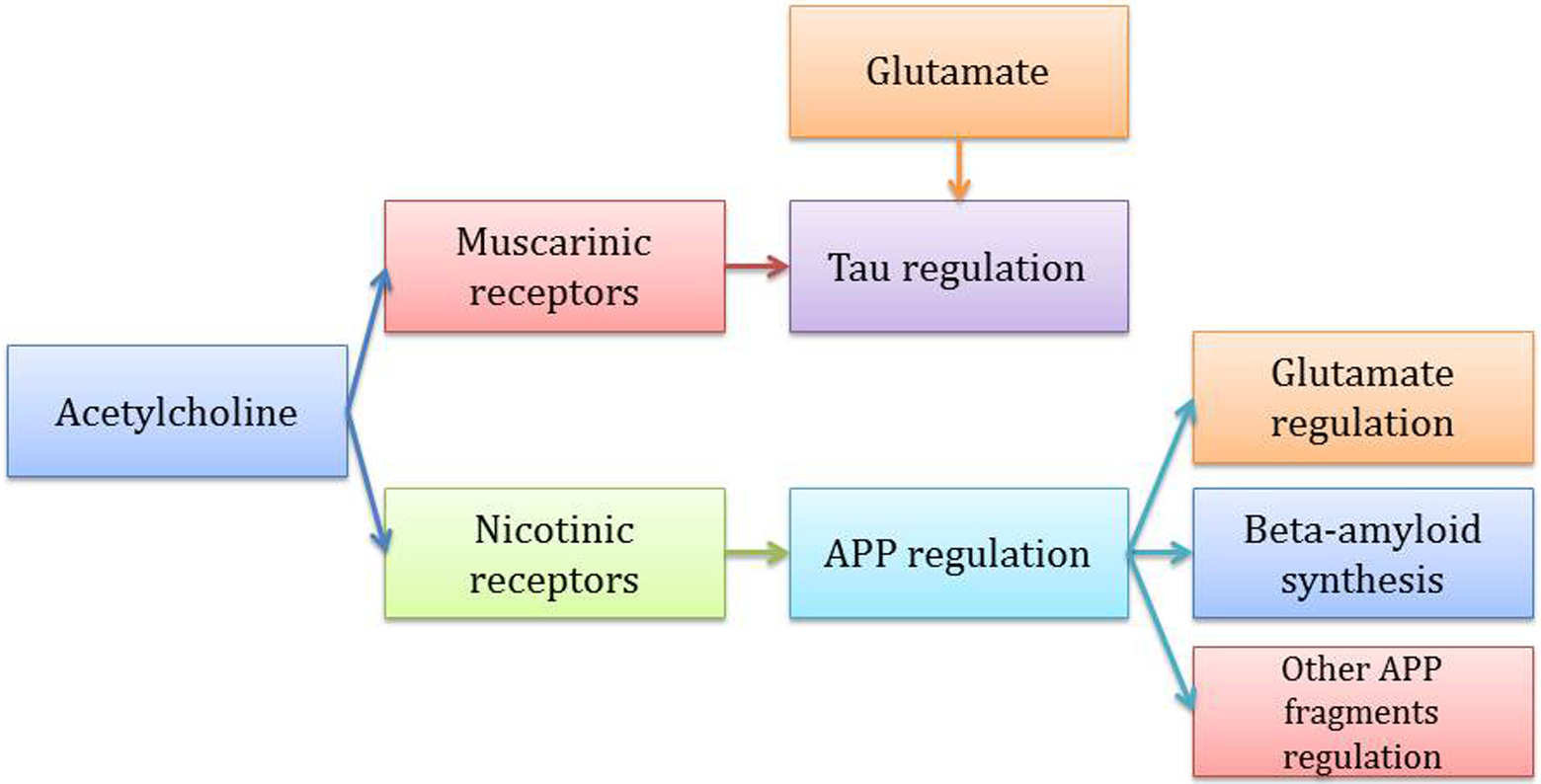
Schematic cholinergic pathway: due to choline acetyltransferase (ChAT), acetylcholine synthesis is possible in the presynaptic neuron; acetylcholine (Ach) is then released to the synaptic cleft, and it binds to muscarinic and nicotinic receptors on the postsynaptic neuron; nicotinic regulation is involved in amyloid precursor protein (APP) activation, and muscarinic regulation is coupled with tau activation which can also be coupled with glutamatergic regulation; tau protein is involved in all the major neuronal intracellular activities, and APP is cleaved into the β-amyloid and nonamyloidogenic components. Acetylcholinesterase (AchE) acts like an unbinding factor, which hydrolyzes the Ach after its purpose was accomplished. A poor ChAT activity can reduce the Ach synthesis and therefore block all the following events due to its absence. On the other hand, AchE is a remarkable drug target in the way that the small amount of Ach synthesized gets to act over and over again as receptor binders due to the hydrolyzing enzyme inhibition (AchE inhibitors therapies). 13
Several brain regions associated with cognitive functions, such as hippocampus and neocortex, are mainly affected by AD tissue pathogenesis. This would be β-amyloid accumulation in senile plaques and aberrant phosphorylation in neurofibrillary tangles which are generally associated with neuronal synapses and neuronal loss. 15 These tissue discrepancies lead to the typical AD symptomatology such as cognitive impairment with memory loss, accompanied or aggravated by aggression, depression, and wandering. 16
Besides senile plaques and neurofibrillary tangles, several studies show many biochemical features disturbed in AD. 15 In this way, substantial neocortical deficits of the enzyme responsible for acetylcholine synthesis, the choline acetyltransferase, were showed to cause memory defects. 17 The substantial role of acetylcholine in learning and memory was already demonstrated. 8 Therefore, the facts that choline uptake and acetylcholine release can be reduced and that cholinergic perikarya from the nucleus basalis of Meynert neurons can be lost represented feasible reasons so that cholinergic hypothesis of AD emerged. 18 Although, in some cases, a temporary symptomatic relief of symptoms can be obtained through targeting the cholinergic or glutamatergic neurotransmitter systems, no current treatment is able to stop or slow its progression.
Subsequently, several studies led to cholinergic hypothesis update. In this way, since the multifactorial hypothesis was formulated, 19 new explanations about AD etiology arose. An interesting and complex theory was described by Craig et al. 20 Based on the multifactorial hypothesis, they demonstrated that AD is actually the result of the interaction between risk factors and cholinergic impairment.
Therefore, it could be explained why the most efficient treatment is the acetylcholine therapy based on acetylcholinesterase inhibitors (such as donepezil, tacrine, rivastigmine, and galantamine). 21 However, it seems that this therapy cannot be considered a universal working tool. The study by Connelly et al 21 have reported that patients with AD having high levels of medial temporal lobe atrophy are less likely to respond to donepezil. In spite that, donepezil may be more efficient in ∊4 apolipoprotein E variant carriers among the patients with AD. 22,23
Notwithstanding the AD research extent, a fully feasible treatment had not been found. 24 There are many studies that addressed several biologically active compounds which can lead to novel therapy discovery. In fact, partially functional therapy consists in an acetylcholinesterase inhibited or extracted from Galanthusnivalis (family Amaryllidaceae) plant—galantamine. 25
While the usage of plant extracts in neurological therapies has been intensely studied and reviewed, 26 -34 yet no study discusses the prevention potential which many plant extracts have. In this way, we describe the plants which can be used in memory loss reversal research on the most common memory loss animal model and propose further strategies to prevent acetylcholinergic system impairments.
Plant Extracts Used in Scopolamine-Induced Animal Models Studies
The link between cholinergic system and AD had been made long ago based on the finding that the loss of cholinergic activity is commonly observed in the brains of patients with AD. 35,36 More than that, the later experimental studies on humans and nonhuman primates associated AD memory loss with cholinergic neurons loss due to the role of acetylcholine in learning and memory. 36 Actually that was the first study which used scopolamine in order to model memory loss (Figure 2) in rodents. In this way, it has been shown that by blocking central cholinergic activity with scopolamine, young participants would demonstrate reversible memory deficits similar to those seen in aged individuals. Moreover, physostigmine could reverse those due to cholinergic agonist activity, 37,38 which led to acetylcholinesterase inhibitor usage in AD therapy. More than that, it seems that high cholinergic agent doses can also interact with the acetylcholine receptors. In this way, the study by Katzung et al 39 showed that excessive physostigmine administration led to muscarinic and nicotinic receptors stimulation. Also, acetylcholinesterase inhibition potential was noted. 39 Therefore, muscarinic and nicotinic stimulation treatment approaches were formulated based on physostigmine administration.
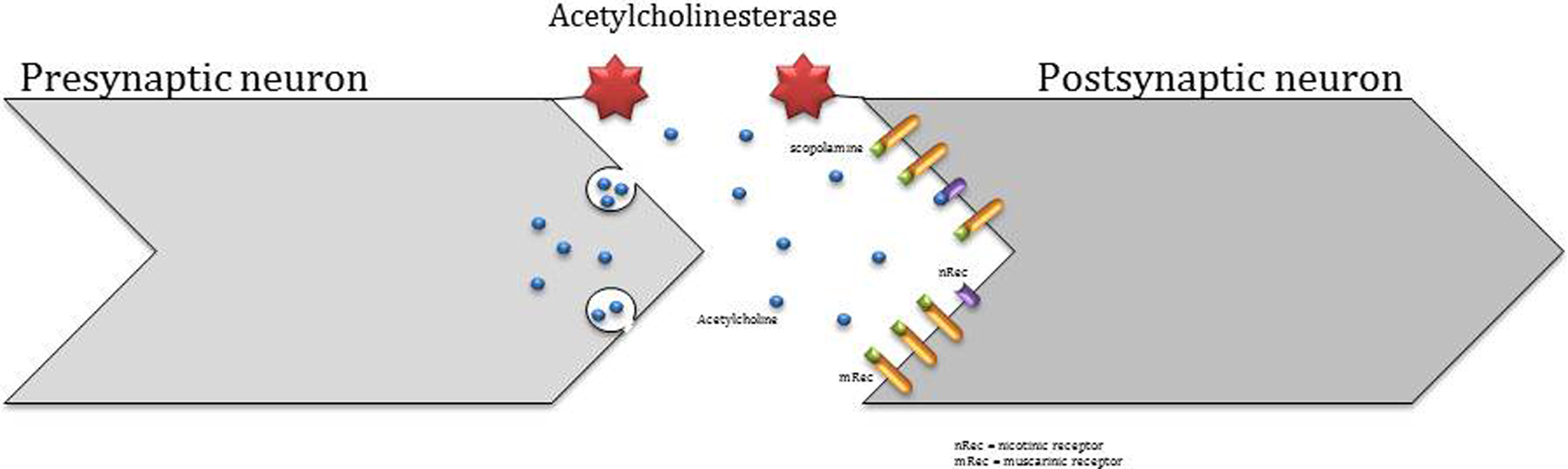
Scopolamine molecular action in synaptic cleft.
Although the cholinergic theory stated that AD is determined by acetylcholine synthesis enzyme (choline acetyltransferase) defects, many of the studies were conducted on either acetylcholine hydrolysis enzyme (acetylcholinesterase) or nicotinic or muscarinic acetylcholine receptors. Furthermore, it seems that the acetyltransferase enzyme was never successfully controlled by artificial modulation. Therefore, the study by Fu et al 40,41 proposed exogenous choline acetyltransferase administration as a slowdown approach. In this way, the group showed that an intravenously injected transferase-based fusion protein could improve memory and cognition in a β-amyloid administration mice model of AD.
However, since the enzymatic components can’t be easily retrieved from exogenous sources and considering the high selective blood–brain barrier, the plant bioactive components must target receptor modulation. This is the reason why many pharmacological studies on memory deficits successfully use scopolamine-induced amnesia as a research model.
The muscarinic receptor binding is not the only activity which acetylcholine exhibits. It also negatively regulates tau protein phosphorylation. 14 In this way, alongside the muscarinic receptors blockage, tau protein activation via phosphorylation is inhibited, leading to signal transduction impairments along the neuronal axons. Therefore, any signal transduced through the axons including survival signaling may be partly or totally disrupted causing neuronal loss. As the cholinergic systems is a key element in several areas of the brain (which are actually impaired in AD), 42 scopolamine action on acetylcholine pathway can easily mimic cognitive impairment which also occurs in AD.
Scopolamine-induced memory loss was extensively used in research studies. Some of them follow the implications of cholinergic system in cognition and in AD pathology. 43 -45 Other studies address the receptor response modulation via nicotinic or muscarinic regulation, 46 -50 but most of them search for the pharmacological potential of some plant extracts which can be used as a substitute or novel treatment in AD therapy.
The lack of full efficiency showed by acetylcholine inhibitors was considered by several studies, the proof that AD origins are not based on cholinergic hypothesis and, therefore, they focused on other abnormalities which occur in AD, molecular changes such as in tau protein production, amyloid deposition, and mutations in amyloid precursor protein processing genes. 5 1 However, others have continued to study neurotransmitter roles in Alzheimer’s development hopping to explain whether the abnormalities are causes or effects of AD pathology. 51,52
Scopolamine, or hyoscine, isolated by Albert Ladenburg, in 1880, may be considered one of the most influent hallucinogenic alkaloid found in plants. It is a secondary metabolite rather abundant in Datura and Hyoscyamus genres. Scopolamine is one of the earliest isolated alkaloids used in purified extracts since antiquity, as an anesthetic, 53 and later on, antiasthmatic and antihistaminic. Due to its amnestic and hallucinogenic properties, 54 multiple studies show that scopolamine can in fact be an efficient antidepressant and anxiolytic agent. 55
Disregarding all its wide properties, the most valued feature of scopolamine in neuropsychiatric research is the amnestic potential. It has been shown that scopolamine can block cholinergic system by binding to muscarinic receptors (as reviewed by Terry). 56 The amnestic effects of scopolamine were studied on many animal model paradigms (Table 1), and it was demonstrated in several of them. As a result, the scopolamine-treated animal models are now generally regarded as a main memory loss animal models.
Behavioral Studies on Scopolamine-Treated Animal Models.
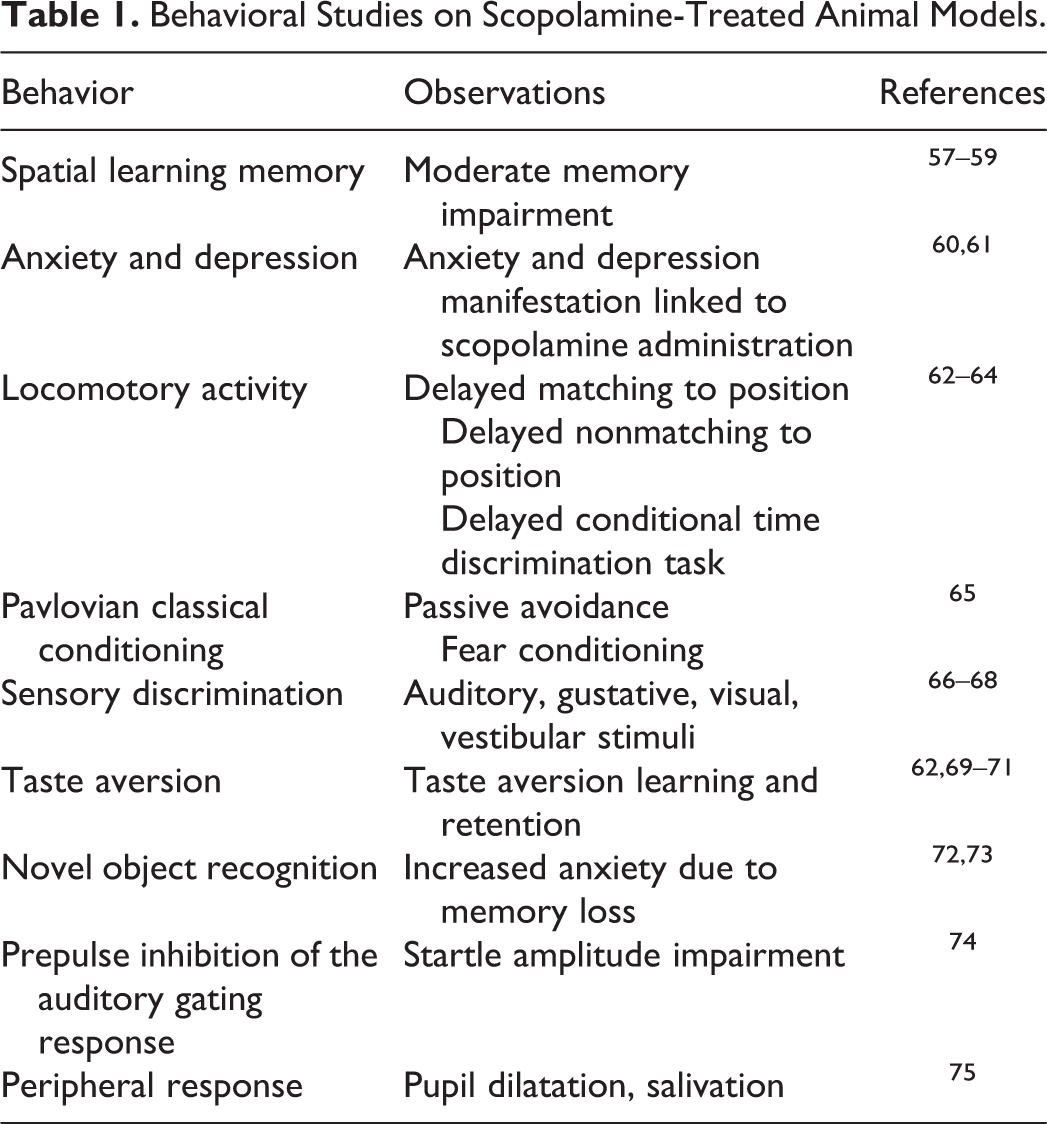
Keeping in mind the effects of scopolamine on memory and cholinergic pathways, 76 several plant extracts were tested for cholinergic modulatory potential in scopolamine-induced cognitive dysfunction (as referenced in Table 1).
Although few studies relied on scopolamine as an amnestic agent in nonhuman primates, 77,78 the majority of studies has been conducted in rodents (particularly rats and mice) due to extensive knowledge on their behavior and numerous available precise evaluation behavioral testing methods. In this way, many plant extracts have been tested on scopolamine-treated models leading to important cognitive impairment therapy candidates (Table 2).
Some Plant Extracts Used in Scopolamine-Induced Memory Deficits Reversal Studies.
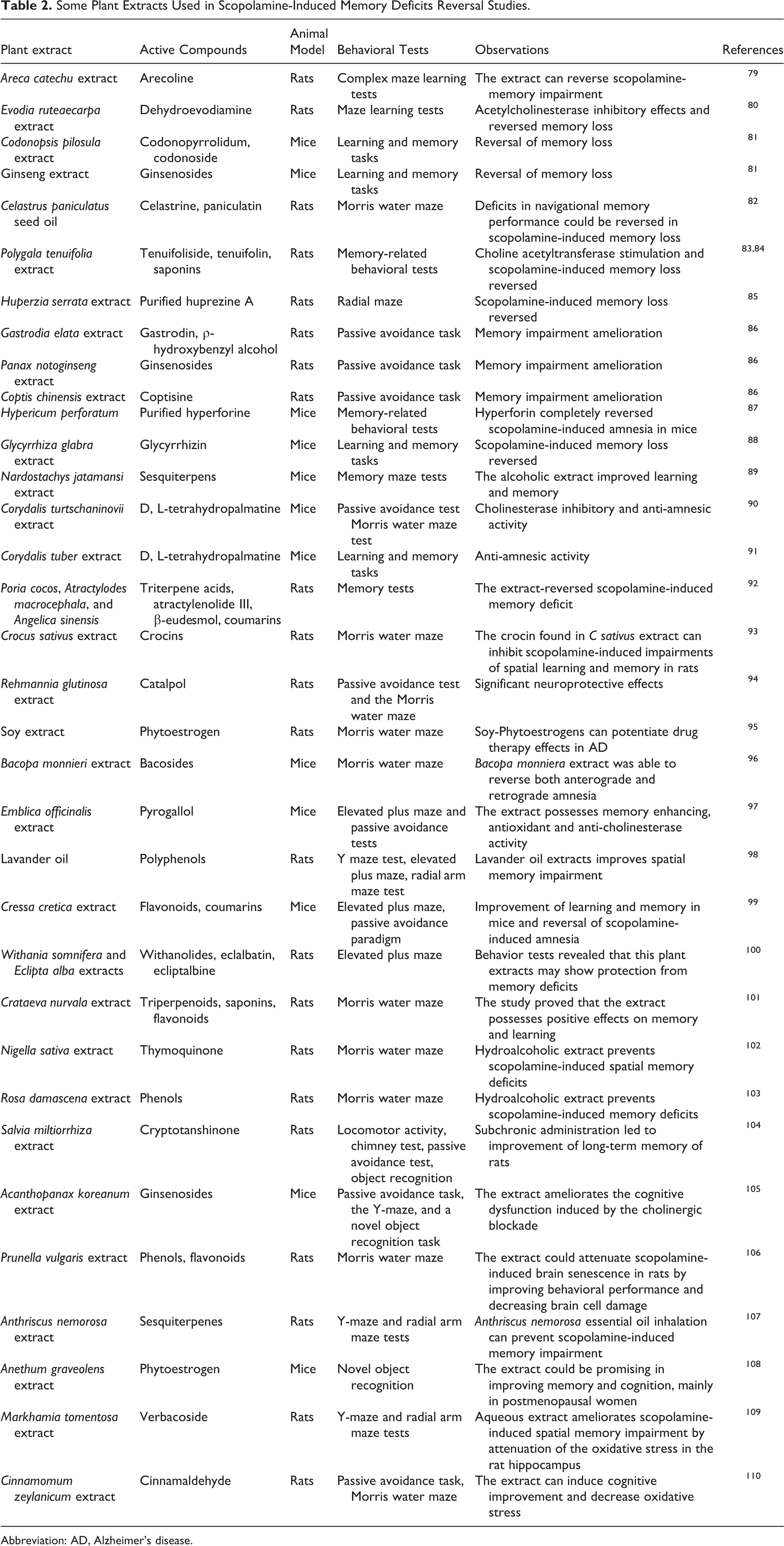
Abbreviation: AD, Alzheimer’s disease.
Some Molecular Aspects of Plant Extract Components Relevant to Scopolamine-Induced Dementia
Mainly due to its inhibiting action, scopolamine can be successfully used in pharmacological studies. As previously described, it can efficiently inhibit acetylcholine system through muscarinic receptors blockage. In this way, other acetylcholine pathway components’ receptor activity modulators may be observed.
Therefore, scopolamine-induced impairments can be used in several plant extract studies which are thought to be consisting of small biologically active molecules that can interfere in the acetylcholine system by many mechanisms. For example, the well-known phospholipid lecithin from the Brazil nuts (Bertholletia excelsa) can participate in the acetylcholine pathway as an efficient precursor for acetylcholine synthesis. 111
In this way, some intriguing questions may be asked. As long as scopolamine blocks the muscarinic receptors on the acetylcholine signaling pathway, what would the features of the tested extracts be in order to theorize a closely and reliable effect on memory and learning developed by the acetylcholine system? More than that, what features should the tested extracts show in order to closely resemble their effects on animal testing as well as on human testing? And last but not the least, what types of molecules the extracts should carry in order to be valuable to scopolamine-induced models as well as human dementia therapy?
As previously shown in Table 2, it seems that the tested plant extract components are extremely heterogeneous regarding biochemical structure and properties. In this way, it has been shown that volatile oils, alcoholic extracts, and aqueous extracts may be considerably active in scopolamine-reversal therapies. Only several classes of molecules can pass the blood–brain barrier which almost fully blocks many potentially successful therapies. However, the plant extracts’ active molecules are extremely diverse and heterogeneous regarding the biochemical structure.
It is well known that if the blood–brain barrier is reached, powerful inflammatory or immune responses can be triggered in order to block any active compounds that should attain the neurological level. 112,113 Still in our best of knowledge, little is known about how the plant extracts reach the central nervous system, if they pass the blood–brain barrier or they bypass it though other pathways. In this way, as it can be seen in Table 2, volatile oils and lipid extracts as carriers assuring the lipophilic or liposoluble molecules transport through the cell membranes. 114 Therefore, any other active compound that was previously missed by extraction process could now be tested as an essential oil administration. In this way, the possibility that the active compounds would not pass through the blood–brain barrier could be minimalized.
At the same time, the many studies performed until now could suggest that there are many types of molecules that could be extremely useful in acetylcholine system impairments reversal and scopolamine-induced memory loss reversal. It is one of our goals to find why the different molecules could actually act as inhibitors or stimulators on acetylcholine signaling pathway, as long as only few modulatory systems are known to be efficient in this case. In this way, it seems that the modulatory system is not fully known and it could be possible that several key points are yet undiscovered, but as long as the acetylcholine hypothesis was studied for more than 30 years, postulated, demonstrated, then rejected, reconsidered, and reformulated, 18 there is no evidence that stand for this argument, although new information could arise every day.
Although the plant extracts which can reverse scopolamine-induced memory loss consist in a great variety and heterogeneity of active molecules, acetylcholine signaling impairments could be summarized based on the molecular modulatory targets. Therefore, the latest pharmacological studies show several groups of active compounds which are efficient in scopolamine-induced impairments reversal.
A naturally occurring furanocoumarin imperatorin, which can be found in several plants (Angelica archangelica and Angelica duharica), shows acetylcholinesterase inhibitory activity. 115 In this way, acetylcholine breakdown following receptor activation may be inhibited. Moreover, using the passive avoidance paradigm, this inhibitory potential can be associated with scopolamine-induced memory impairment reversal. 116 Although it was admitted that no clear mechanism of action was found, imperatorin may be a good candidate for further clinical tests due to its memory enhancement and antioxidant properties.
In this way, 3 other important active compounds which can be found in Nigella sativa (thymoquinone, dithymoquinone, and nigellin) were showed to possess high antioxidant potential. 117 Thymoquinone in particular was demonstrated to inhibit nitric oxide production and to decrease inducible nitric oxide synthase expression. Also, the study by Hosseini et al 102 shows that N sativa extract could interact with cholinergic system since extract administration to scopolamine-treated rats results in memory and cognition enhancement and amnesia reversal. While cholinergic pathway modulatory properties were not explained, the considerable reported antioxidant effect was made responsible for the memory impairment reversal potential. Furthermore, Acanthopanax koreanum extract 105 and Anthriscus nemorosa essential oil 107 ameliorate the cognitive dysfunction induced by the cholinergic blockade, in a similar manner.
Another study pointing to a correlation between cholinergic pathway impairment via scopolamine administration and oxidative stress shows the beneficial effect of Rosa damascena extract against brain tissue damage in scopolamine-treated rats. 103 Moreover, it seems that R damascena was confirmed to interact with neurogenesis and synaptogenesis. 118 While R damascena extract significantly influence oxidative stress in hippocampus and cerebral cortex, it was indicated that hippocampal total thiol concentrations were not affected. 103 In this way, it seems that R damascena extract improves memory by decreasing free radical synthesis but with no effect on antioxidant defense.
Prunella vulgaris extract was also demonstrated efficient in scopolamine-induced amnesia reversal seen in behavioral performance improvement following brain cell damage decrease. 106 Molecular analysis in brain tissues of treated-rats revealed that the notable acetylcholinesterase activity reduction may be correlated with plant extract administration. Also, P vulgaris extract shows efficient antioxidant effects outlined from lipid peroxidation decrease and antioxidant enzymes activities improvement following plant extract administration in scopolamine-treated rats. The same mechanism was suggested for Markhamia tomentosa extract while exposing scopolamine-treated rats to plant aqueous formulations. 109 In this way, it seems that a major mechanism in scopolamine-induced memory impairment reversal exhibited by the tested plant extract may be linked with oxidative stress decrease in several key brain areas such as hippocampus or brain cortex followed by working memory improvement.
Also, scopolamine-induced memory impairment model was used in procholinergic properties research. Kulkarni et al 119 studied Prunus amygdalus nuts antiamnestetic effects. In this way, it has been shown that acetylcholinesterase activity is significantly inhibited by almond nut extract administration in scopolamine-treated rats. More than that, they emphasize that no previous study had shown antiamnestetic properties in P amygdalus extract, but it is possible that alongside the lipid metabolism normalization potential, the omega-3 fatty acids could exhibit neurological effects.
Similarly, subchronic administration of Salvia miltiorrhiza extract leads to long-term memory improvement in rats and also exhibits significant acetylcholinesterase inhibitory effect mainly in hippocampal and frontal cortex region leading to the observation that S miltiorrhiza may possess an important neuroprotective effect. 104 The study by Ozaroski et al 104 also suggested that the main S miltiorrhiza active compounds of mechanism of action may be the inhibition of acetylcholine esterase and butyrylcholinesterase messenger RNA transcription in frontal cortex area, but not in the hippocampal area.
In addition, a recent study 120 demonstrated that the known alkaloid caffeine could act as an effective acetylcholinesterase inhibitor. In this way, it has been proved that caffeine administered to scopolamine-treated rats triggers a noncompetitive inhibition between the caffeine molecule and the enzyme. More than that, it seems that caffeine could only inhibit acetylcholinesterase, having no effect on the other enzyme involved in acetylcholine pathway, the butyrylcholinesterase.
Also, an interesting study shows that the cholinergic pathway can even be controlled through acetylcholinesterase synthesis modulation. 121 In this way, the study by Aravind et al 122 suggested that one of the Sphaerantus indicus extract components can efficiently lower the acetylcholinesterase levels in scopolamine-treated mice. Therefore, it have been concluded that this may be a useful way of modulating the cholinergic deficits in AD. The actual mechanism in which S indicus extract decreases acetylcholinesterase levels may be linked to chemical energy synthesis blockage needed in gene expression. Therefore, a key point in acetylcholinesterase depleting mechanisms may be linked to those components which can inhibit energy formation or consumption at the central cholinergic system level. On the other hand, it is well known that the antioxidant system is actually one of the mechanisms which control chemical energy during reactive particles exchange. In this way, a negative modulation of the acetylcholinesterase synthesis may be attained by antioxidant agent’s administration. 123
Interestingly enough, it seems that a synergistic modulation between acetylcholinesterase inhibition, N-methyl-
In addition, another study performed by the group of Abbasi et al 124 reported that vitexin (a flavonoid derivate found in Tartary buckwheat sprouts, wheat leaves, Mimosa pudica, and Passiflora subspecies) can actually interact with several receptors involved in gamma-aminobutyric acid release, therefore modulating postacetylcholine release activities. More than that, they demonstrated that Urtica circularis extract can correct memory impairment in mice and therefore could be useful in AD therapy, although they admit that the scopolamine treatment may not be the most reliable AD model. Therefore, it seems that the many active compounds constituting the recently tested plant extracts may exhibit the same general effect but on different molecular ground. This fact could be a novel starting point in finding new molecules that can be useful in acetylcholine system impairment reversal.
Conclusions
Alzheimer’s disease is the most important and most aggressive neurodegenerative disease that needs all the attention that can get. In this way, many efforts have been made in order to find causes and treatments. Many animal models that mimic several important AD symptoms and mechanisms have been developed, but none could ever reproduce the entire pathology pattern observed in human. The scopolamine-induced memory loss mouse or rat model can be the most reliable model in cholinergic theory study. Therefore, many pharmacological studies rely on scopolamine-induced memory loss models in order to observe the different plant extract effects on cholinergic system. Many of the studied plant extracts show important acetylcholinesterase modulation potential and scopolamine-induced memory loss reversal, in spite that few of the active components have been clearly demonstrated their mechanism of action.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflict of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The authors are supported by Romanian Government Research grant PN II PN-II-RU-TE-2014-4-1886.
