Abstract
In recent years, over 1000 reports have been published on the association between hepatic diseases and gene mutations which may result in pathogenic amino acids. Most of the studies focus on the hepatocellular carcinoma (HCC). The aim was to systematically examine the published literature on the association between the mutations of arginine, serine, and threonine and hepatic diseases, particularly HCC. The Biosciences information service database was systematically searched before July 10, 2012. Of the initially selected 471 publications, 112 articles were included in this study. Meta-analyses were conducted for 3 amino acids. Risk ratios were used to analyze the association between amino acids and liver diseases. We analyze the literature on the association between gene mutations and hepatic diseases, especially in patients with HCC. Full-text articles were analyzed by 4 independent researchers. Some amino acid mutations were found only in people with liver diseases—not in the general population. Arginine and threonine mutations occurred more frequently in patients with hepatic diseases, compared to the normal population. There is a statistically significant association between arginine mutations and the risk of HCC and serine mutations and the risk of HCC.
Introduction
For decades, the morbidity and mortality of hepatic diseases have been increasing year by year. The number of deaths was more than 35 000 cases every year in Japan 1 and approximately 2000 to 3000 cases per year in the United States. 2 Hepatocellular carcinoma (HCC) is the most common primary tumor of the liver. 3 As the fifth most common malignant tumor in males and the eighth in females and the third most common cause of cancer-related mortality in the world, HCC is a major health problem worldwide. 4 The incidence of HCC varies greatly among geographic regions and racial and ethnic groups. 5 In particular, Southern Italy has the highest rates of HCC in Europe. 6 Moreover, the incidence and mortality of HCC in low- and middle -income countries are much higher than those of high-income countries. 7 In 2008, there were approximately 748 300 new cases of primary liver cancers; 84% occurred in developing countries, and the incidence rate was the highest in East Asia. A total of 695 900 new cases were estimated to die of primary liver cancers. 8 Hepatocellular carcinoma accounts for 85% to 90% of all primary liver cancers. 9
Amino acids play an important role in organ functions. There are 3 amino acids, namely, arginine, serine, and threonine, which are more modified and thus more likely to mutate than other amino acids. This may affect the normal functions of the organs.
Methods
Study selection
Selection criteria
Studies are included if they meet the following criteria: They are published in English in online journals on or before July, 10, 2012. They are clinical trials conducted on humans (studies in which cell culture or animal experiments were carried out were excluded). Hepatic diseases in these studies are diagnosed by pathological examination. They provide sufficient information about amino acid mutations associated with liver diseases (genetic mutations or mutations of amino acids).
Studies are excluded if they had any of the following shortcomings: The study data were inaccurate. They were about virus or other antigens. They were about treatments of liver diseases.
Information sources and search
The Biosciences information service (BIOSIS) database was searched for the Medical Subject Heading (MeSH) terms “liver diseases” [MeSH Terms] AND “mutation” AND “arginine” [MeSH Terms]/“serine” [MeSH Terms]/“threonine” [MeSH Terms]. A total of 471 articles were found by searching for the title and abstract. Moreover, the reference lists of these 471 articles and of previous systematic reviews were searched for additional relevant studies.
Data extraction and preparation
In the case of sequential or multiple publications of the same or overlapping data, only the publication that reported results from the largest or most recent analysis was included. Publications with completely redundant information were excluded. If a publication included multiple source or study populations, data were extracted separately, if possible. Every eligible publication includes the following information: the first author, publishing year, diseases studied, populations of cases and controls, and populations with amino acid mutations of cases and controls.
Data pooling and statistics
All statistical analyses were performed with Review Manager, version 5.0 (The Cochrane Collaboration, Oxford, England), using 2-tailed P values and a 95% confidence interval (CI). Estimates of association with liver diseases were evaluated with risk ratios (RR), using the Mantel-Haenszel method. The choice between a random and a fixed effect model for analysis purposes was based on Q statistics. In case of substantial heterogeneity (I 2 value ≥ 50%), a random effects model was applied to pool the data; otherwise, a fixed effects model was used. Sensitivity analyses and reliability assessments were performed 1 when I2 was more than 50% (the largest group of trials that passed the test of heterogeneity) and 2 in cases of studies published in the recent 5 years. P < .05 was considered statistically significant. Publication bias was explored by looking for asymmetry in the funnel plot.
Results
Study Selection
Figure 1 shows the flowchart of study inclusion. Of 471 potentially relevant studies yielded by medical search engines, 23 studies met all predefined criteria 10 –32 ; of the 23 studies, in turn, 15 were about HCC. Table 1 summarizes the main features of the eligible studies. The sample size of the studies ranged from 1 to 434, with a total of 1948 patients.
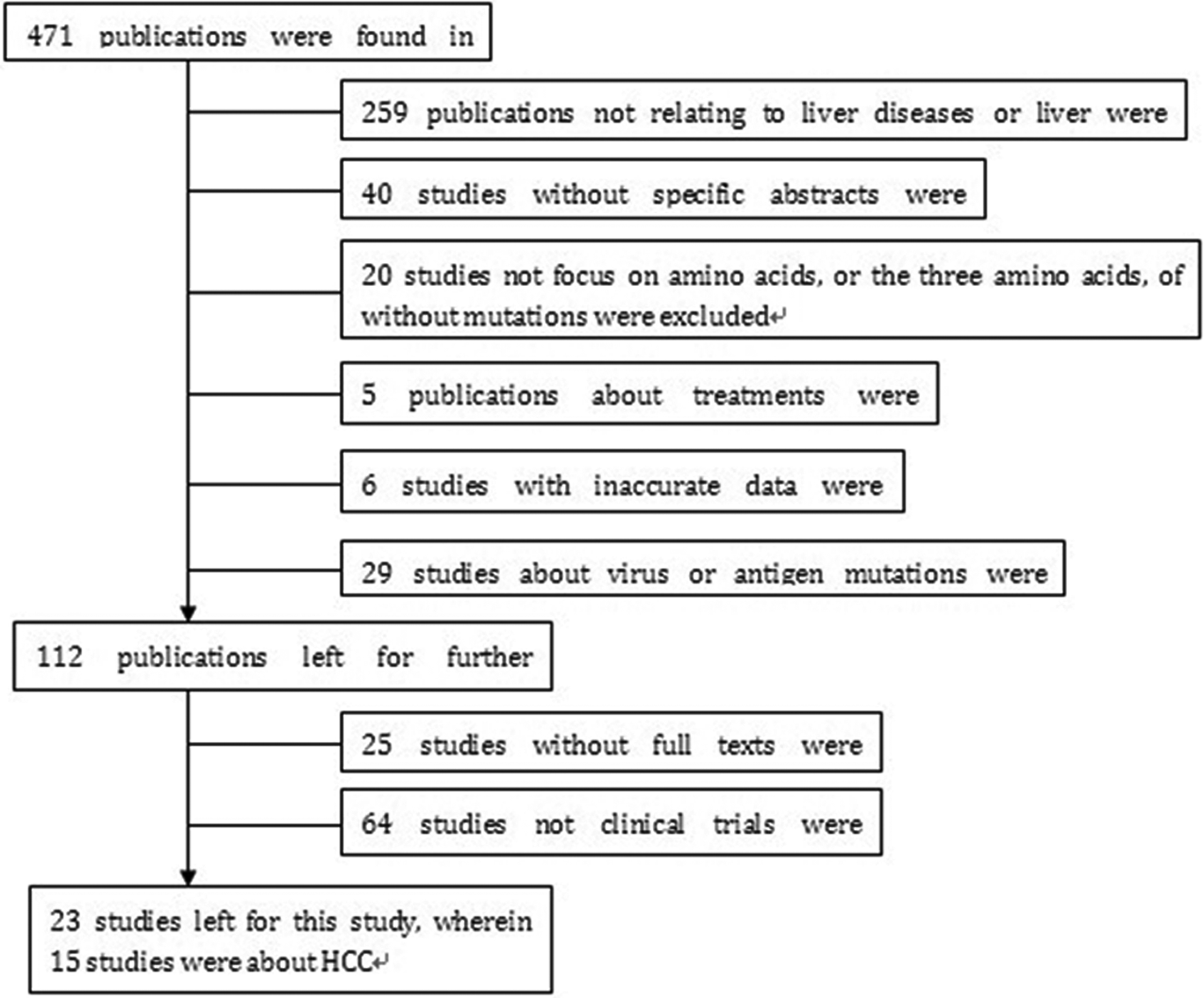
Study inclusion flowchart.
General Characteristics of Included Studies.

Abbreviation: HCC, hepatocellular carcinoma.
Statistical Analysis
Arginine
From 13 studies, 10 –22 912 patients and 893 controls were included in this analysis. The total number of arginine mutation events was 454 to 451 in the patient group and 3 in the control group. There was a significant difference between the 2 groups with regard to the arginine mutation (χ2 = 39.90, df = 12, P < .0001). The arginine mutation in the patient group with liver diseases was reported in all 13 studies and it was reported in only 1 study in the control group. Moreover, an association was found between the arginine mutation and liver diseases (risk ratio 14.66, 95% CI = 4.21-51.03, P < .0001; see Figure 2). Significant heterogeneity was observed (I2 = 68%, P < .0001), and the random effects model was applied.

Risk ratio and 95% arginine confidence interval (CI) analysis.
Serine
Six studies, 23 –28 536 patients and 273 controls, were included to conduct this analysis. In total, there were 221 serine mutation events in the patient group and none in the control group. Moreover, the serine mutation was found in the patient group of all 6 studies. There was no significant difference between the 2 groups (χ2 = 5.47, df = 5, P = .36). An association between the serine mutation and liver diseases was found (RR 43.28, 95% CI = 13.30-140.83, P < .00001; see Figure 3). There was no significant heterogeneity (I 2 = 9%, P = .36), and the fixed effects model was employed.

Risk ratio and 95% serine confidence interval (CI) analysis.
Threonine
Four studies, 29 –32 500 patients and 482 controls, were included in this analysis. Threonine mutations were discovered in all 4 studies—59 in patients and 13 in controls. A significant difference between the 2 groups was observed (χ2 = 83.52, df = 3, P < .00001). The association between threonine mutation and liver diseases was not significant (RR = 6.29, 95% CI = 0.05-763.05, P = .45; see Figure 4). Significant heterogeneity was observed (I 2 = 96%, P < .00001), and the random effects model was applied.

Risk ratio and 95% threonine confidence interval (CI) analysis.
Sensitivity analysis and publication bias
Sensitivity analysis obtained homothetic results. The sensitivity analysis of arginine was shown (Figure 5). An extensive search strategy was chosen to minimize the potential of publications. Funnel plots adopted for analysis of arginine indicated that there is a possibility of missed small-scale experiment to obtain the opposite or small result, while the other analyses did not detect obvious publication bias.

Arginine sensitivity analyses. A, All studies. B, Largest group of studies that passed the heterogeneity test. C, Studies published in recent 5 years.
Discussion
Number of People With Amino Acid Mutations
The arginine mutation analysis showed that 451 (49.45%) of 921 patients and 3 (0.34%) of 893 controls had the arginine mutation. The incidence rate ranged from 8.06% 22 to 100% 10,11,20,21 in the patient groups. The incidence rate of the control groups was 0% in most studies except for the study by Kirk (5.66%). 14 Analysis showed that 221 (41.23%) of 536 patients had the serine mutation. There were no serine mutations in the control groups. The incidence rate ranged from 14.29% 25 to 66.13% 24 in the patient groups. There was a significant difference with regard to the incidence rate between the patient and the control groups.
The threonine mutation analysis revealed that 59 (11.80%) of 500 patients had the threonine mutation. In the control groups, 13 (2.70%) of 482 patients had the same mutation. The incidence rate ranged from 7.83% 29 to 53.85% 30 in the patient groups and from 0% 29,30 to 100% 32 in the control groups, surprisingly indicating that no significant differences existed in the threonine mutation between the 2 groups.
Heterogeneity
The heterogeneity of the 3 meta-analyses differed from each other. Two analyses showed a large heterogeneity: 70% (arginine mutation) and 96% (threonine mutation). The third analysis displayed a mild heterogeneity of 9% (serine mutation). The reason for the differences in heterogeneity may be that arginine and threonine mutations appeared only in the patient groups, but in the control groups, all the controls were without serine mutation.
Association Between Amino Acid Mutations and Liver Diseases
Our final analysis revealed that more amino acid mutations occurred in the patient groups than in the control groups, and the heterogeneity indicators reflected our finding. This suggests an association between amino acid mutations and liver diseases. Most of the liver diseases in the studies analyzed by the meta-analysis were HCC. Therefore, we draw a further and more specific conclusion that the amino acid mutations may relate to HCC or the effective factors causing it. Amino acid mutations may cause 1 amino acid to change to another. This, in turn, may lead to the production of a different protein that is unnecessary or even harmful to normal liver functions or to a production stop of a protein that is essential for normal liver functions. Amino acid mutations may also cause a production stop of certain peptide chains and lead to the conversion of a codon that is responsible for a normal amino acid to a stop codon and subsequent errors in the translation process. All these potential consequences of amino acid mutations may raise the risk of liver diseases.
The Effects of Mutations in a Variety of Liver Diseases
Alcohol consumption is generally accepted to aggravate the hepatitis C virus (HCV)-related chronic liver diseases and increase the risk of HCC. Takahashi et al 33 analyzed the quasi-species of the hypervariable region 1 of the HCV genome and found the mutation events seemed to occur randomly when amino acid sequences of this region were compared between drinkers and nondrinkers in their target population. Lee et al 34 studied 301 blood specimens of patients with chronic hepatitis B and summarized the correlations between the mutation status of the reverse transcriptase (RT) domain and biochemical parameters such as hepatitis B virus DNA and hepatitis B e antigen positive rate. The presence of RT gene mutations could provide guidance for clinical chronic hepatitis B. In HCV, Kaul et al 35 identified a correlation between HCV polyprotein processing and cyclophilin A (CypA) dependence of HCV replication. The replication of subgenomic HCV replicons of different genotypes is reduced up to 1000-fold with CypA depletion using the CypA knockdown cell lines, while the CypB depletion had no effect.
Limitations of the Study
The final conclusions of some analyses, for example, those of the threonine mutation, may be inaccurate, since there is little quantity of related literature. Another limitation of this study is the lack of data concerning control groups. Few studies had information on both the patient and the control groups. We must take measures to make the population of the patient groups comparable to that of the control groups to avoid inaccurate conclusions.
Footnotes
Abbreviations
Authors’ Note
The authors contributed equally to this work. This is an independent study. None of the authors received any support for this study nor do any of the authors have any financial relationships whatsoever with any organizations that might have an interest in this study.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
