Abstract
Background:
Telenutrition offers scalable solutions for delivering nutrition care, yet postpandemic data on its adoption among registered dietitians’ (RDs) in Saudi Arabia remain limited. This study assessed telenutrition practices, perceived barriers and benefits, and readiness for adopting national telenutrition platforms among Saudi RDs to inform digital health platforms.
Methods:
A cross-sectional survey using a validated 14-item Arabic questionnaire was distributed to RDs working in Saudi Arabia (N = 309). Respondents with prior telenutrition experience (n = 221) were included in the final analysis. Descriptive and chi-square tests were used to examine associations between demographic factors and telenutrition adoption preferences.
Results:
Findings showed that 95% of RDs reported confidence in delivering telenutrition, with 74% using it weekly. Commonly delivered services included dietary consultation (71.9%) and nutritional assessments (52%), primarily conducted via phone calls (86.4%). Measurement-related barriers, such as inaccurate self-assessments (74.2%) and patients’ difficulty in following instructions (68.6%), were significantly more prevalent than technology-related challenges (42.5%, p < 0.001). Despite these limitations, 88% expressed interest in subscribing to a Saudi telenutrition platform, with 82% preferring part-time integration alongside existing roles. No statistically significant associations were found between demographic variables and adoption preferences; however, trends suggested greater interest among early to midcareer female RDs with postgraduate qualifications.
Conclusions:
Saudi RDs show strong confidence, active use, and readiness to engage with flexible, part-time telenutrition models. These findings provide foundational evidence to support the development of user-centered, nationally digital platforms tailored to the needs of RDs in Saudi Arabia.
Keywords
Introduction
The Saudi’s Vision 2030 initiatives aim to advance health care through digital innovations, recognizing telehealth as a strategic priority, where the Ministry of Health has formulated strategies to promote eHealth across the kingdom.1,2 Given the burden of chronic illnesses, telenutrition may play a major role in preventing such noncommunicable disease, allowing frequent consultations and enhancing sustained dietary behavior change for underserved areas. 3 The rapid advancement of health technologies has significantly facilitated the integration of telehealth services into health care delivery systems.4,5 Initially focused on providing remote clinical consultations, telemonitoring, mobile health applications, and digital platforms.6–8 This transformation has been seen widely during the COVID-19 pandemic, which induced health care systems worldwide to adopt virtual health care delivery methods.4,9–11 Still, telehealth requires more research to evaluate its effectiveness in managing chronic disease progression and health care accessibility. 12
The Academy of Nutrition and Dietetics defines telehealth use by clinical dietitians and nutritionists as telenutrition. It is defined as “the interactive use by an RDN of electronic information and telecommunications technologies to implement the Nutrition Care Process with patients or clients at a remote location, within the provisions of the RDN’s state license as applicable.”3,13 Evidence of its efficacy has been observed in diverse populations, with reported benefits including improved dietary adherence, weight management outcomes, and patient satisfaction.13–15 Eid et al. (2024) have demonstrated telenutrition impact in improving anthropometric measures, biochemical indicators, nutrition knowledge, quality of life, and physical activity levels, alongside low dropout rates and high patient engagement.16–25
Despite telenutrition promising potential, the adoption of telenutrition still faces several challenges. One recurring concern involves the accuracy of anthropometric measurements in remote settings. 26 Internet connectivity has been identified as a key barrier to the effective adoption of telenutrition in Saudi Arabia during the COVID-19 pandemic. 27 Other identified barriers included limited provider training, insufficient institutional support and reduced communication between dietitians and patients. 28 Thus, technological barriers remain substantial, especially in areas with limited broadband connectivity or among populations with low digital literacy.4,24 Eid et al. (2024) assessed perceptions on telenutrition among Saudi registered dietitians (RDs), highlighting that key challenges rely on the lack of anthropometric data, technical issues, and communication barriers. 29
Limited research has explored telenutrition adoption in the post-COVID era, particularly as technology has evolved to include structured platforms and artificial intelligence-supported systems that require further development.30,31 Assessing current telenutrition practices is therefore essential to guide the creation of national platforms tailored to the needs of RDs and the region's needs. Building on earlier cross-sectional studies on telenutrition adoption,11,14,15,27–29 this study is expected to update the evidence base with 2025 postpandemic data to identify provider characteristics, needs, and inform the design of responsive, applicable digital health solutions. In the present study, we aimed to develop and validate a 14-item Arabic questionnaire to explore RDs’ professional experiences, perceived challenges, perceived benefits, and willingness to adopt telenutrition in Saudi Arabia, ultimately supporting the development of effective, locally adapted digital nutrition platforms.
Methods
The current study is a cross-sectional study was conducted in four stages: (1) designing and adapting a questionnaire on telenutrition practice, including barriers, benefits, and professional readiness; (2) validating the tool through expert review and content validity assessment; (3) administering the questionnaire on RDs who has prior telenutrition practice in Saudi Arabia; and (4) exploring associations between demographic variables and RD responses.
Ethical approval and participants consent were carried in accordance with the Declaration of Helsinki and approved by the Institutional Review Board of The Research Ethics Committee at the Unit of Biomedical Ethics, Faculty of Medicine at King Abdulaziz University, Jeddah, Saudi Arabia (NCBE Registration No. HA-02-J-008 and Reference No. 3721-24), date: Monday, November 18, 2024.
QUESTIONNAIRE ADAPTATION, DEVELOPMENT, AND VALIDATION
A 14-item questionnaire was adapted from previously published studies on telenutrition adoption.15,27 The survey was designed and structured by a team of RDs’ experts into four key domains: (1) professional experiences with telenutrition, including frequency of use, confidence, types of services, and tools employed; (2) technical-related and measurement-related barriers; (3) perceived benefits and recommendations; and (4) readiness to adopt telenutrition. The 14-item questionnaire included a combination of dichotomous (yes/no), single-choice, multiple-choice, frequency-based, and Likert-type questions. Content validity was assessed prior to implementation, following a structured process previously published in health research literature, 32 to confirm the accuracy, clarity, and comprehensiveness of the questionnaire. Each item was evaluated by a panel of six experts comprised of three hospital-based RDs and three PhD-qualified academics in the Clinical Nutrition Department, Faculty of Applied medical Sciences, King Abdulaziz University, Jeddah, Kingdom of Saudi Arabia. Content validity was assessed using a 4-point scale evaluating clarity and simplicity: 1 = not clear/simple, 2 = item needs revision, 3 = minor revision needed, and 4 = very clear/simple.
Table 1 presents the results of the content validity assessment for the questionnaire evaluated by five RD experts. All five experts rated each item as either clear or simple, resulting in full agreement across all items. To assess content validity, expert ratings on a 4-point scale were recorded, where ratings of 3 or 4 were recorded as (valid), while ratings of 1 or 2 were recorded as 0 (requiring revision), following the method described by Masoud and Mosli (2023). The Item-Level Content Validity Index (I-CVI) was calculated by dividing the number of experts rating as 3 or 4 by the total number of experts. The Scale-Level Content Validity Index was computed by dividing the total number of items rated 3 or 4 by the total number of items (universal agreement methods). Consequently, the I-CVI for each of the 19 items was 1.0, indicating excellent content validity and strong expert consensus on the clarity and simplicity of the questionnaire items.
Content Validity Index for Clarity and Simplicity
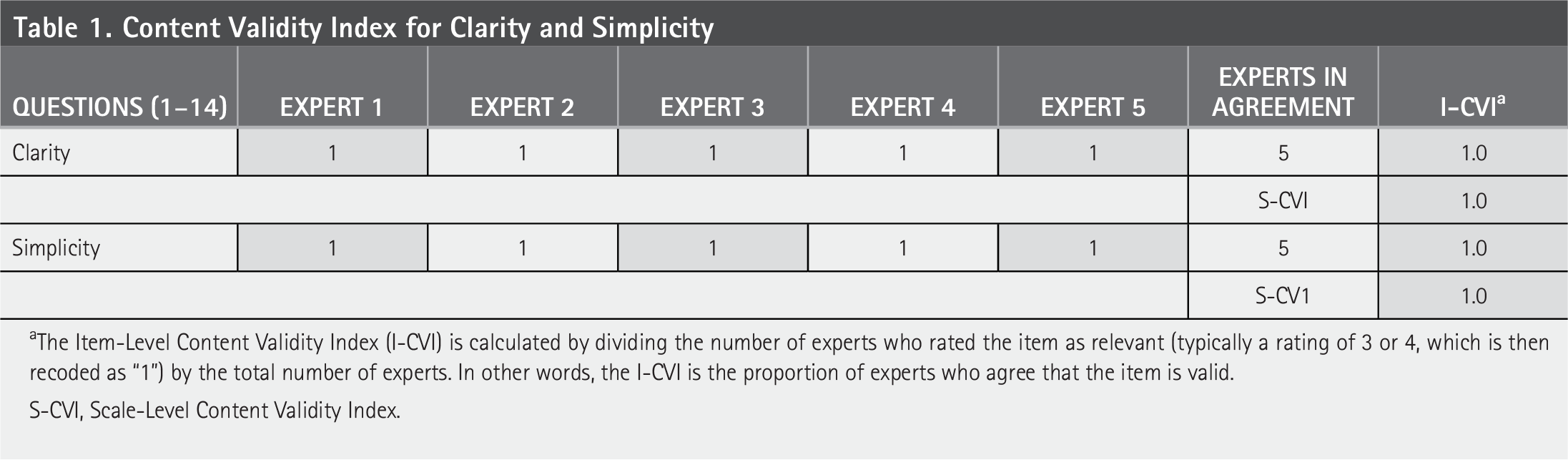

The Item-Level Content Validity Index (I-CVI) is calculated by dividing the number of experts who rated the item as relevant (typically a rating of 3 or 4, which is then recoded as “1”) by the total number of experts. In other words, the I-CVI is the proportion of experts who agree that the item is valid.
S-CVI, Scale-Level Content Validity Index.
APPLYING THE VALIDATED 14-ITEM ARABIC QUESTIONNAIRE TO ASSESS RDS’ EXPERIENCES, CHALLENGES, AND ADOPTION READINESS FOR TELENUTRITION IN SAUDI ARABIA
A validated 14-item Arabic questionnaire was distributed through professional groups and social media platforms between December 2024 and April 2025. Participation was entirely voluntary, and electronic informed consent was obtained from all respondents prior to initiating the survey. A total of 1,000 questionnaires were distributed electronically to Saudi RDs, and 309 responses were received, which was considered sufficient for preliminary validation and feasibility assessment.27,32 After the exclusion of 88 responses, comprising 4 incomplete questionnaires and 84 from participants without prior experience in telenutrition, a total of 221 responses were included in the final analysis (Fig. 1).
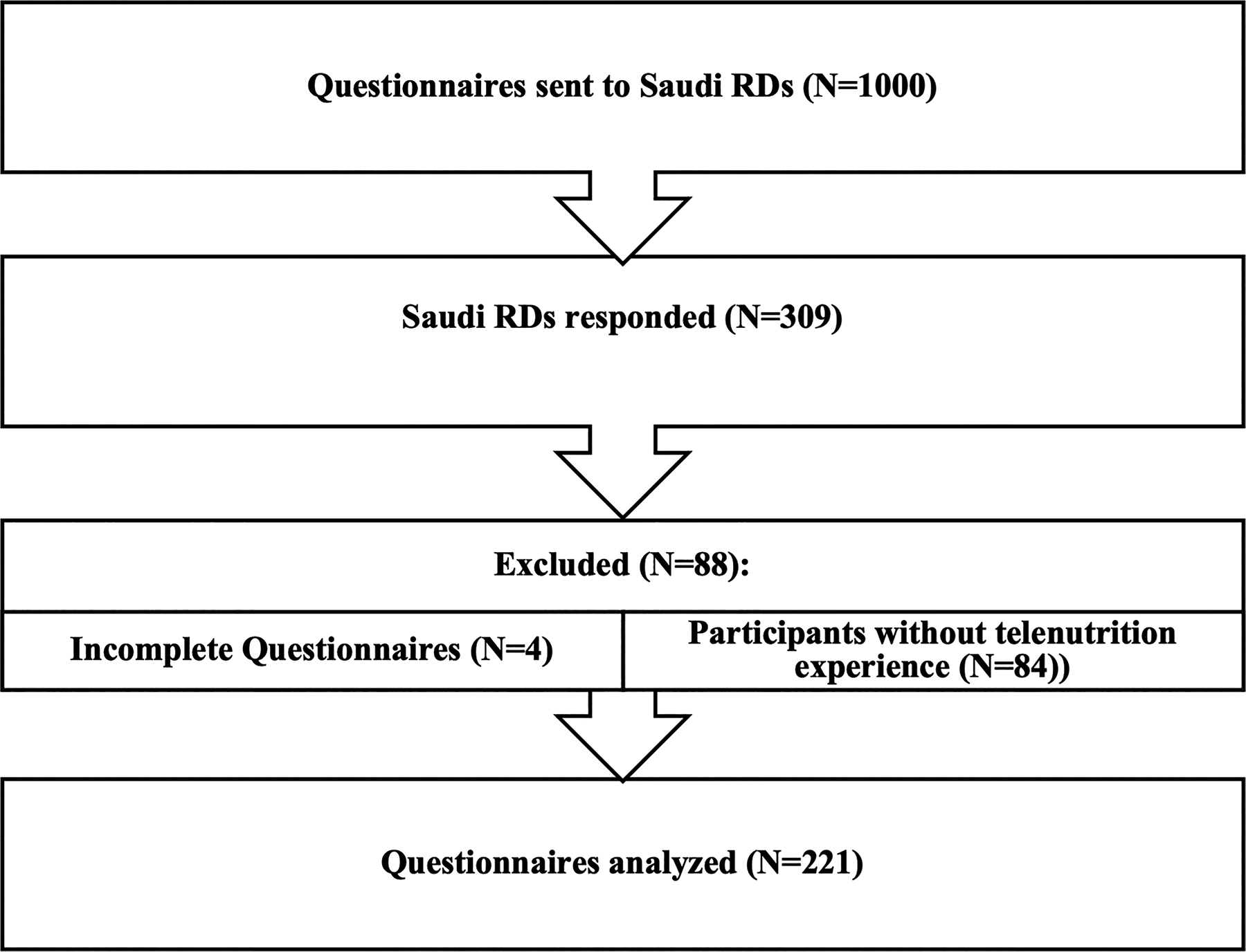
Flowchart of the study.
STATISTICAL ANALYSIS
Statistical analysis was performed using IBM SPSS version 26. Frequencies (n) and percentages (%) were used for descriptive data. Chi-square test was conducted, and statistical significance was determined using a two-tailed criterion of p < 0.05. Cramér’s V was calculated as a measure of effect size for all categorical associations. Interpretation thresholds for effect size followed standard conventions: negligible |(<0.1), small (0.1–0.3), medium (0.3–0.5), and large (>0.5).
Results
CHARACTERISTICS OF PARTICIPANTS WHO RESPONDED TO THE QUESTIONNAIRE
Table 2 demonstrates characteristics of 309 participants, who completed the 14-item Arabic questionnaire, showing slightly more than half were females (54%), and the most reported age group was 40–50 years (44%), followed by 18–28 years (37%). Most respondents (95%) identified their current designation as RD Specialist, with fewer reporting roles as Senior RDs Specialist (5%) or Dietitian Technician (<1%). Most participants held bachelor’s degree (86%), while a smaller proportion reported graduate-level education, including 14% with a master’s degree and less than 1% with a doctoral degree. Years of professional experience were distributed across the sample, with the highest proportion reporting 2–4 years of experience (28%), followed by 5–7 years (25%). Thus, 72% of respondents, which is a total of 221 RDs, reported prior experience with telenutrition.
Characteristics of Respondents (N = 309)
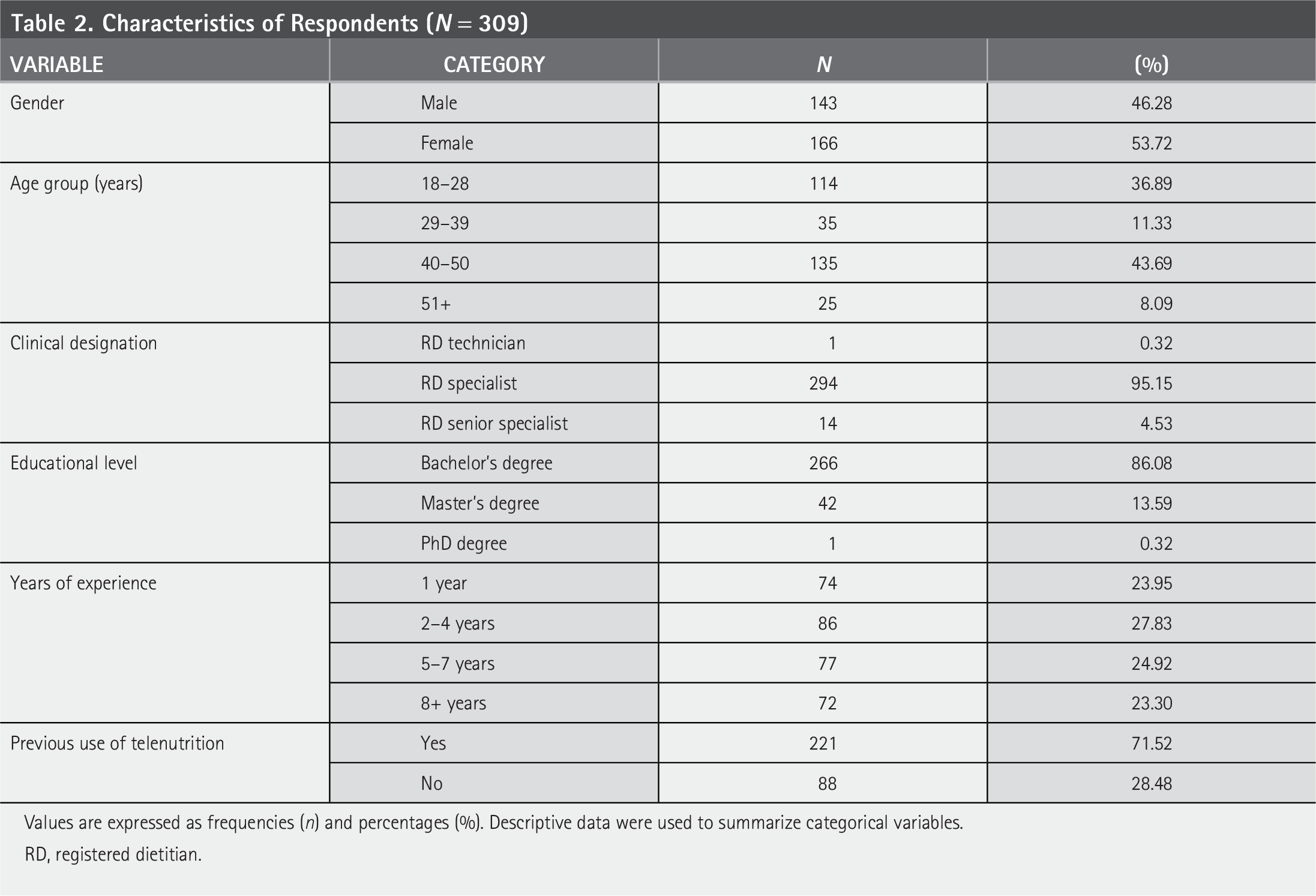
Values are expressed as frequencies (n) and percentages (%). Descriptive data were used to summarize categorical variables.
RD, registered dietitian.
PARTICIPANTS’ PROFESSIONAL EXPERIENCES WITH TELENUTRITION
Table 3 shows that 95% of respondents were confident in delivering telenutrition services, and 73.8% of respondents reported using telenutrition on a weekly basis. The most provided services via telenutrition were dietary consultation (71.9%) and nutritional assessments (52.0%). Less frequently reported services that included meal planning (8.1%), telemonitoring (0.5%), and follow-up with discharged patients through virtual clinics (0.5%). Regarding anthropometric data collection, weight (90.0%), height (84%), and body mass index (BMI; 82.8%) were the frequently assessed metrics. In contracts, waist circumference was infrequently used (5.0%). Regarding patients’ instructions, the most common method was via phone calls (86.4%), followed by email or applications (20.8%), live video guidance during consultations (12.7%), and video demonstrations (6.3%).
Professional Experiences in Providing Telenutrition Services (N = 221)
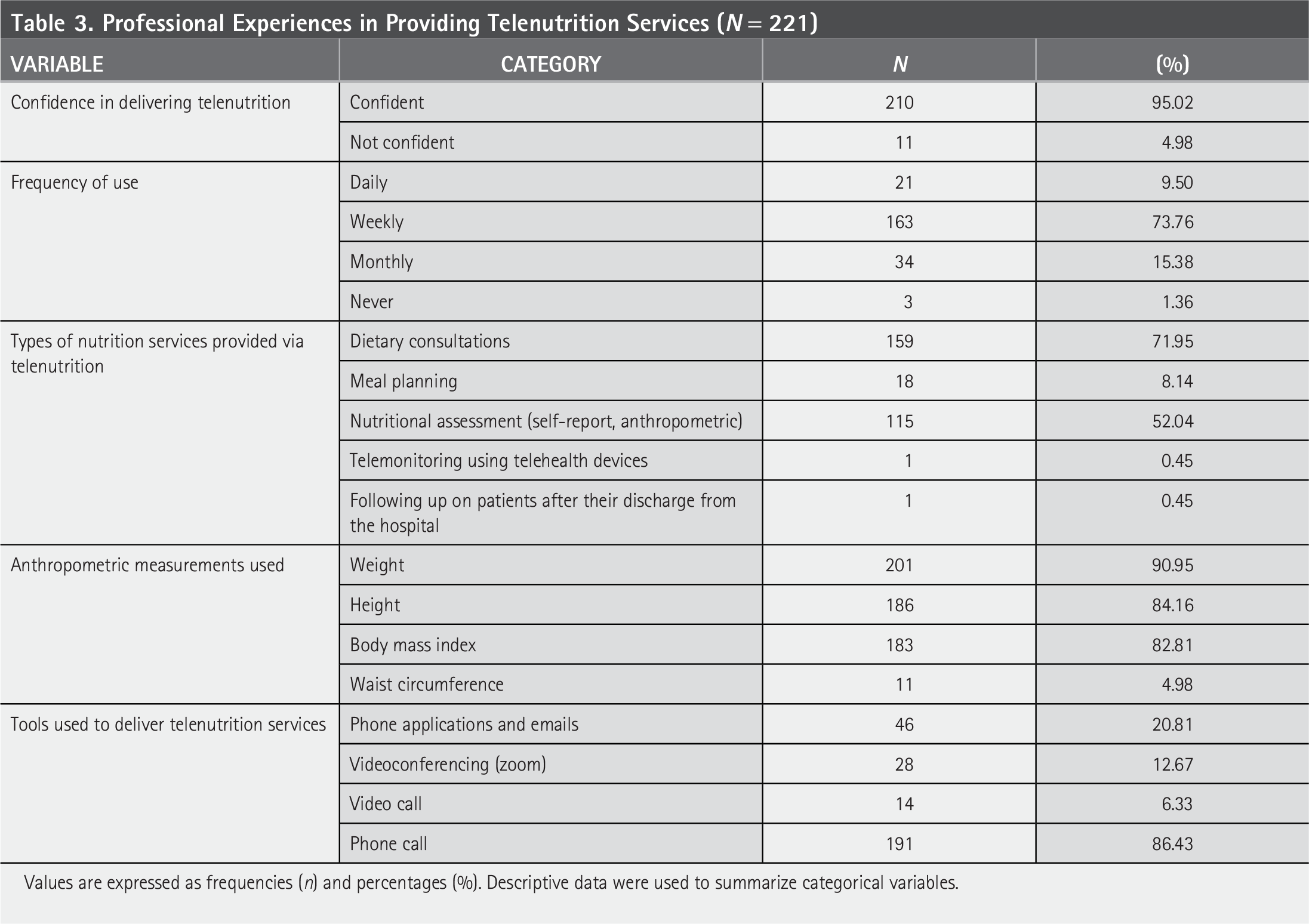
Values are expressed as frequencies (n) and percentages (%). Descriptive data were used to summarize categorical variables.
CHALLENGES INFLUENCING EFFECTIVENESS OF TELENUTRITION
Table 4 shows reported barriers to telenutrition delivery via a checklist. The most frequently reported measurement-related barriers included, patients’ difficulty in conducting accurate assessments (n = 164, 74.21%), following instructions (n = 152, 68.78%), maintaining consistent measurement techniques across visits (n = 117, 52.94%), lack of validated measuring equipment at home (n = 111, 50.23%), inadequate follow-up procedures (n = 137, 61.99%), and lack of patient engagement (n = 148, 66.97%). Regarding technology-related barriers, poor internet connectivity (n = 94, 42.53%), restricted access to digital tools (n = 53, 23.98%). Table 5 reveals the frequency of measurement and technical barriers occurrence using a Likert-scale format (always, often, rarely), which showed a statistically significant difference (McNemar–Bowker test, p = 0.004, and chi-square test, p < 0.001), where higher frequency of measurement barriers was found.
Reported Barriers in Delivering Telenutrition (N = 221)
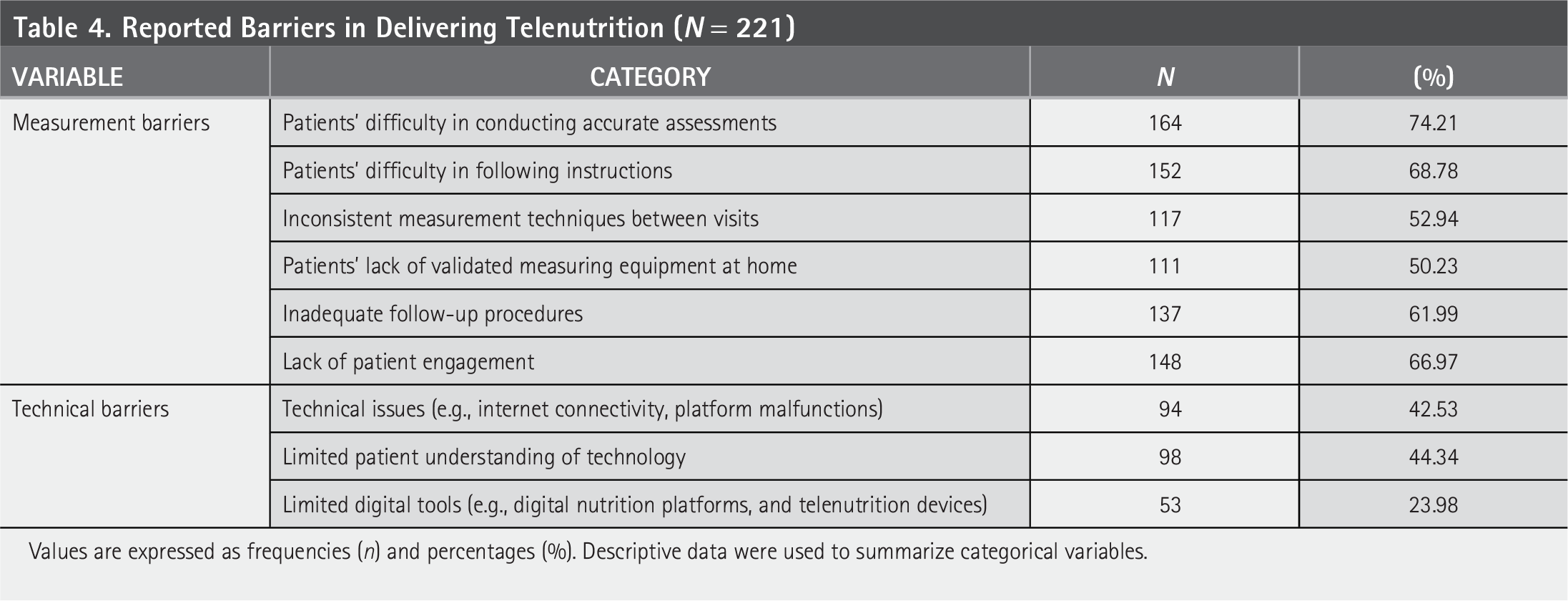
Values are expressed as frequencies (n) and percentages (%). Descriptive data were used to summarize categorical variables.
Comparison of Reported Technical and Measurement Barriers in Telenutrition Delivery (N = 221)
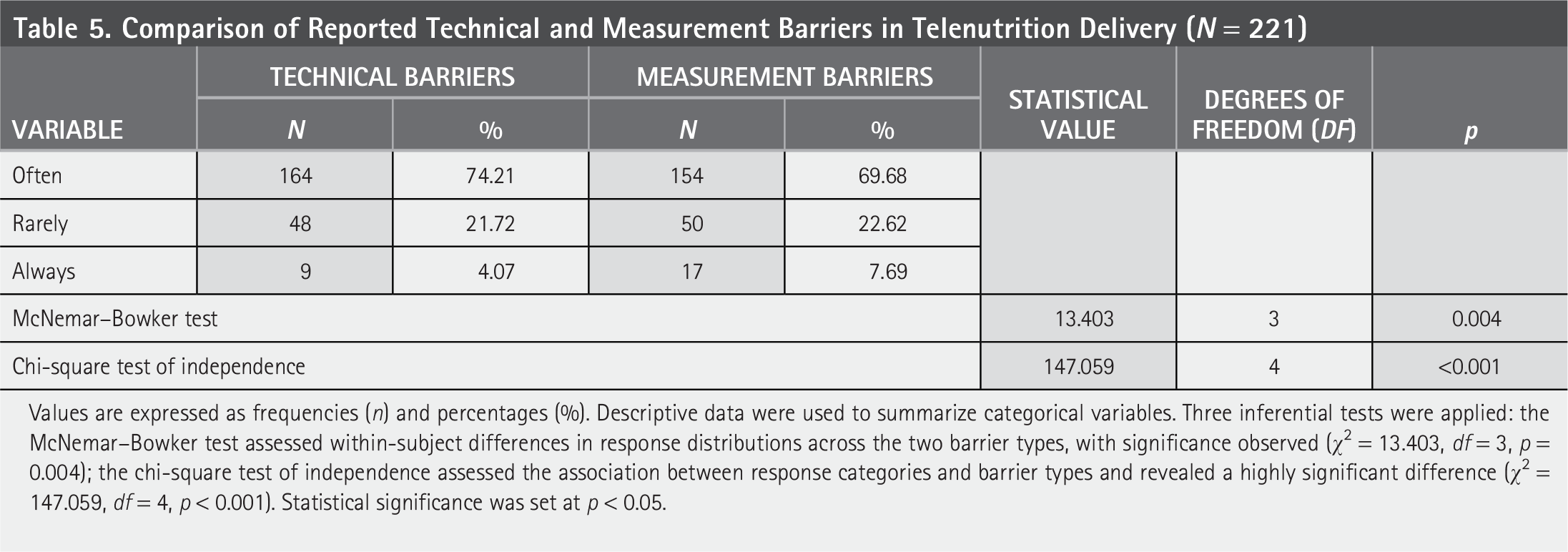
Values are expressed as frequencies (n) and percentages (%). Descriptive data were used to summarize categorical variables. Three inferential tests were applied: the McNemar–Bowker test assessed within-subject differences in response distributions across the two barrier types, with significance observed (χ² = 13.403, df = 3, p = 0.004); the chi-square test of independence assessed the association between response categories and barrier types and revealed a highly significant difference (χ² = 147.059, df = 4, p < 0.001). Statistical significance was set at p < 0.05.
PERCEIVED BENEFITS, SUPPORT NEEDS, AND STRATEGIC RECOMMENDATIONS FOR TELENUTRITION ADOPTION AMONG RDS IN SAUDI ARABIA
Table 6 demonstrates that the most frequently benefited was increased accessibility to nutrition care services (n = 157, 71.04%), followed by flexibility in scheduling (n = 129, 58.37%). Greater comfort in a familiar environment was perceived as a benefit by 41.18% of respondents, and convenience was reported by 31.22% followed by 29.41% improved patient monitoring and 28.96% increased accessibility for patients. Fewer respondents identified cost-effectiveness and improved patient compliance as benefits. Respondents highlighted key needs for successful telenutrition adoption, including user-friendly digital platforms (29.4%), provider training on technology (29.0%), and patient education materials (7.7%). The most frequently proposed strategies were the development of standardized national guidelines (71.0%) and specialized training for dietitians on digital tools (58.4%). Other suggestions included improving internet infrastructure (41.2%), integrating advanced tools for remote assessment (31.2%), providing telehealth equipment for patient use (29.0%), enhancing interprofessional collaboration (29.4%), offering government incentives (11.8%), and utilizing patient engagement tools such as mobile apps and reminders (7.7%).
Reported Perceived Benefits, Support Needs, and Strategic Recommendations for Telenutrition Adoption (N = 221)
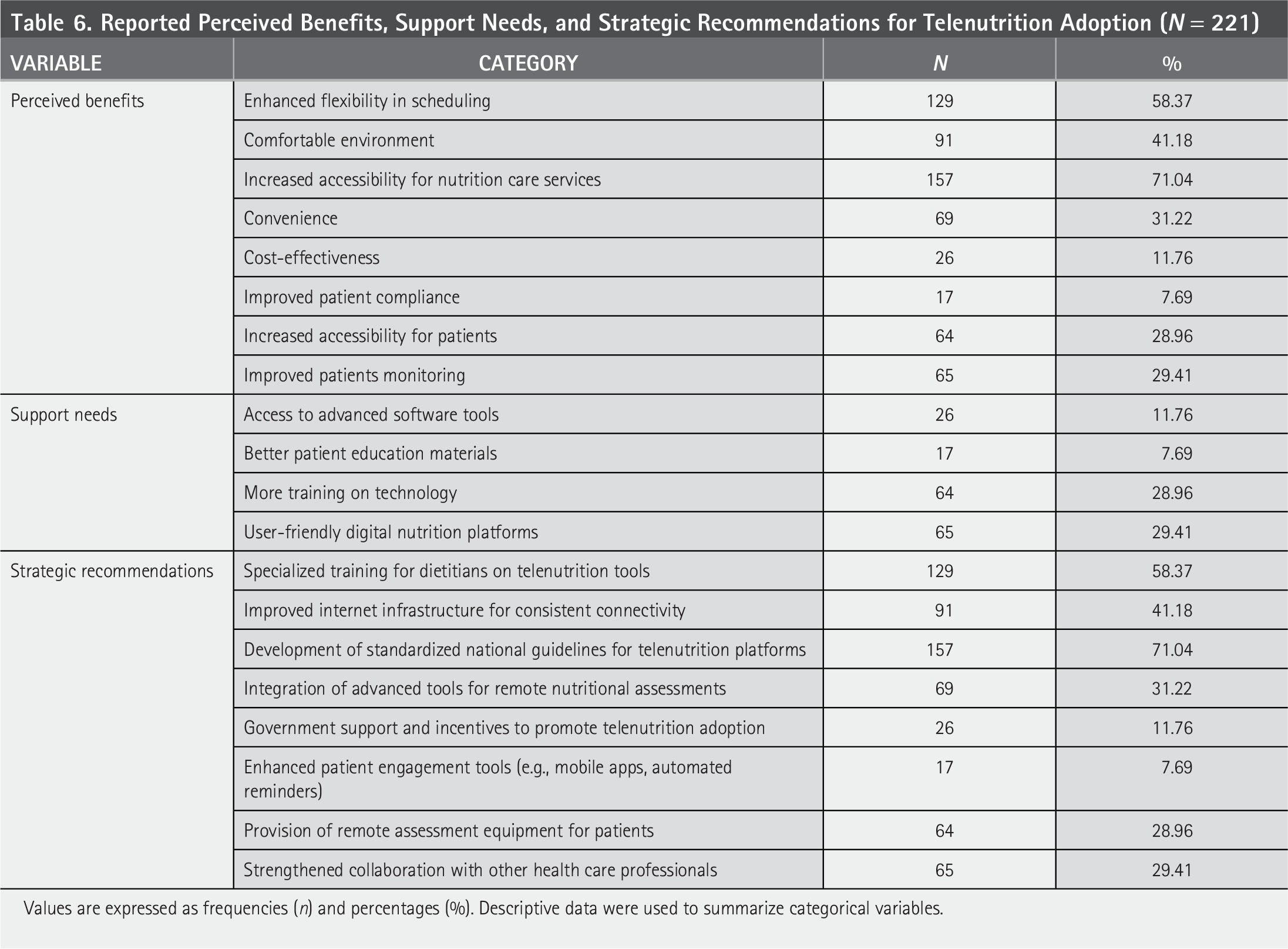
Values are expressed as frequencies (n) and percentages (%). Descriptive data were used to summarize categorical variables.
DIETITIANS’ READINESS IN ADOPTING TELENUTRITION VIA DIGITAL PLATFORMS
Fig. 2 demonstrates that most respondents (n = 194.92, 88.2%) were interested in subscribing to a Saudi-based telenutrition platform for delivering telenutrition services. Additionally, most respondents (n = 181.54, 82.14%) expressed a preference for integrating telenutrition as a part-time practice alongside their existing full-time roles, a smaller proportion (n = 22.10, 10.7%) indicated that they were not interested in adopting telenutrition in their consultations, while only (n = 7.14, 7.1%) expressed willingness to transition fully to telenutrition by leaving their current full-time positions, as shown in Fig. 3.
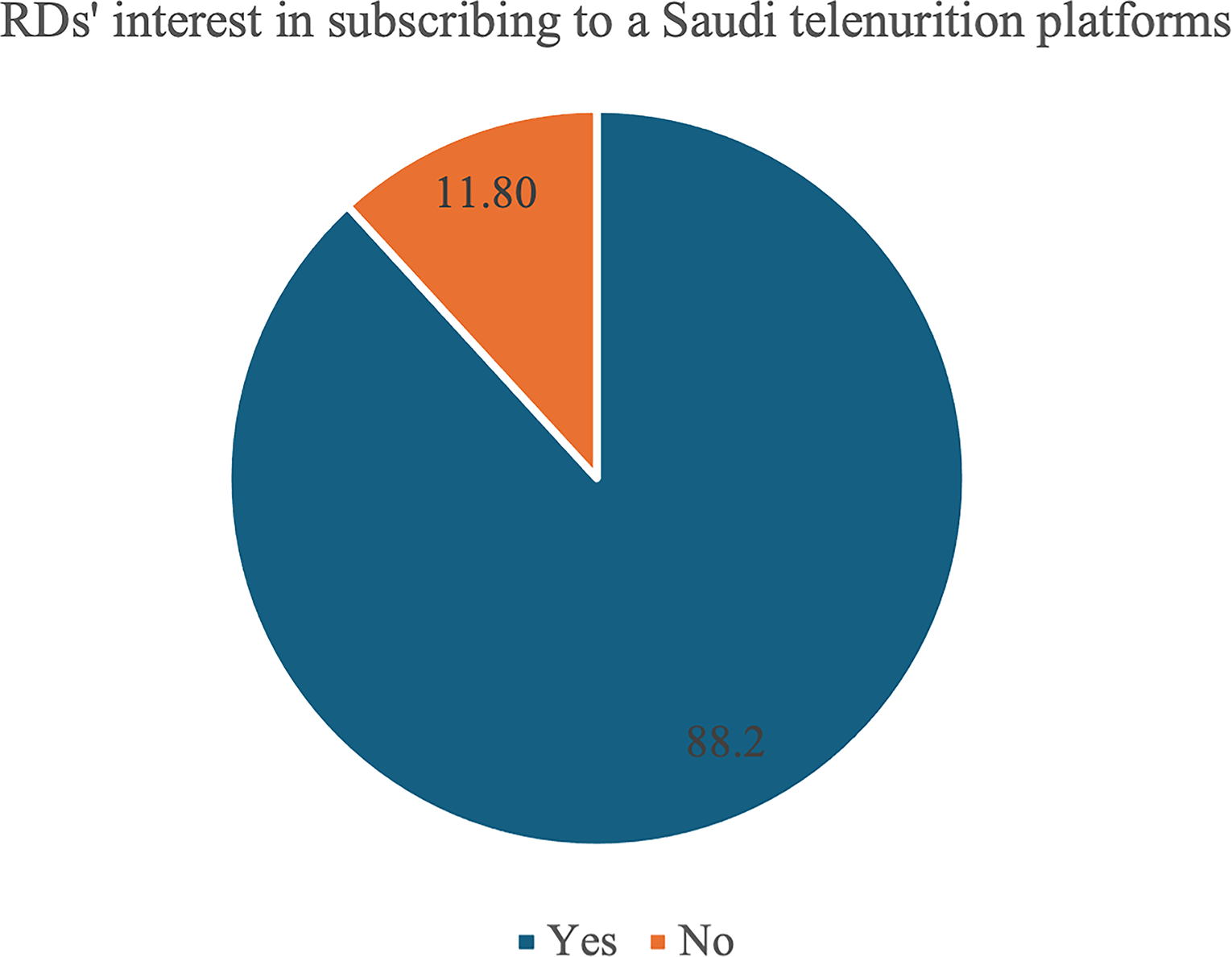
RDs’ interest in subscribing to a Saudi telenutrition platform (N = 221). RD, registered dietitian.
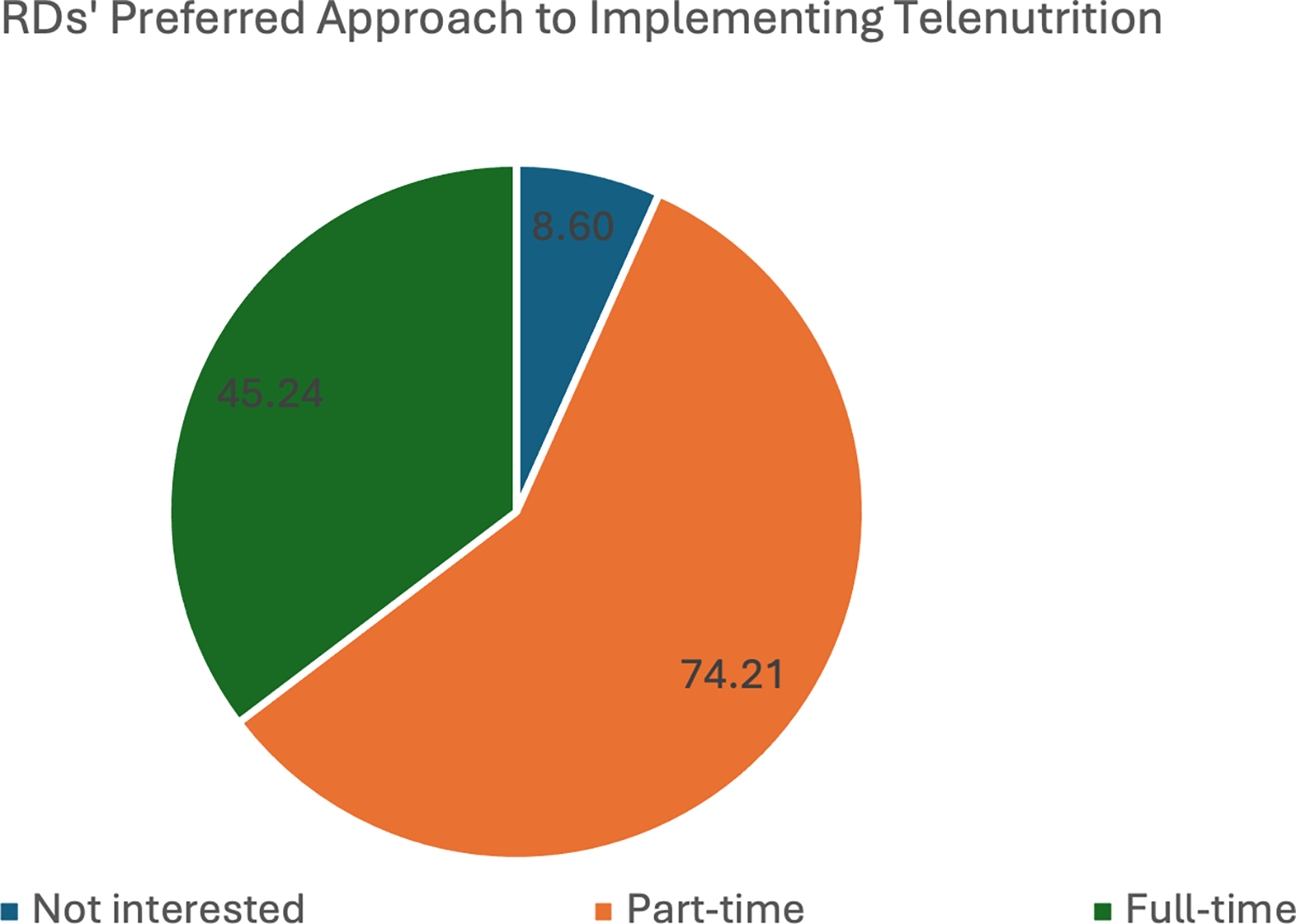
RDs’ preferred approach to implementing telenutrition (N = 221).
DEMOGRAPHIC CHARACTERISTICS’ ASSOCIATIONS WITH RDS’ INTEREST IN SUBSCRIBING TO TELENUTRITION PLATFORMS IN SAUDI ARABIA
In Table 7, chi-square analysis indicated that none of the demographic variables including gender, age group, clinical designation, education level, or years of experience were significantly associated with expressed interest in Saudi telenutrition platform (all p values >0.05), where effect sizes across all comparisons were minimal. However, interest levels were consistently high across all groups, with 84.1% of females and 89.9% of males expressing interest. The highest interest was observed among RDs aged 29–39 (90.7%), senior dietitians (90.0%), those with postgraduate degrees (92.6%), and those with more than 8 years of experience (90.9%).
Demographic Associations with Interest in Subscribing to a Saudi Telenutrition Platforms (N = 221)
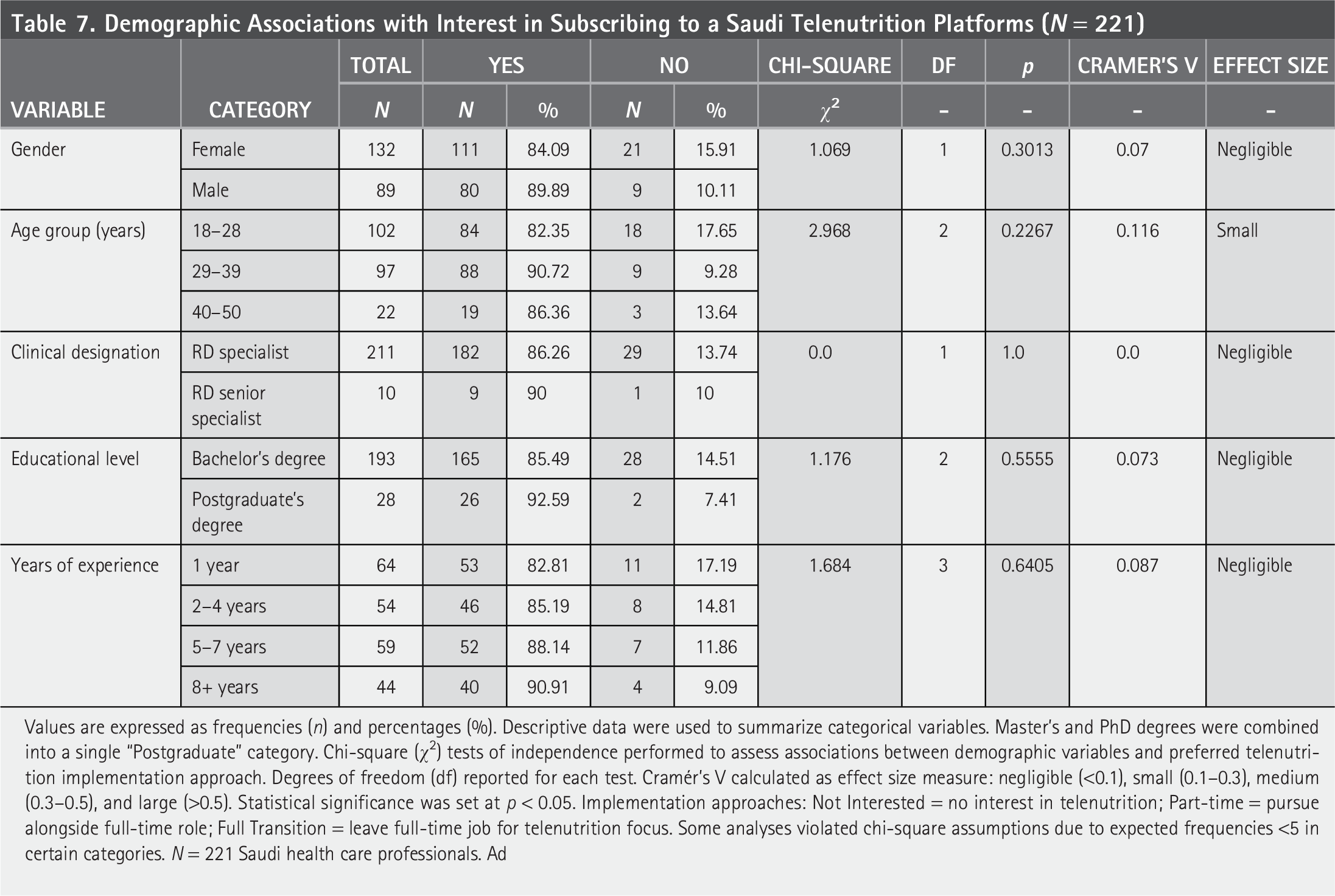
Values are expressed as frequencies (n) and percentages (%). Descriptive data were used to summarize categorical variables. Master’s and PhD degrees were combined into a single “Postgraduate” category. Chi-square (χ²) tests of independence performed to assess associations between demographic variables and preferred telenutrition implementation approach. Degrees of freedom (df) reported for each test. Cramér’s V calculated as effect size measure: negligible (<0.1), small (0.1–0.3), medium (0.3–0.5), and large (>0.5). Statistical significance was set at p < 0.05. Implementation approaches: Not Interested = no interest in telenutrition; Part-time = pursue alongside full-time role; Full Transition = leave full-time job for telenutrition focus. Some analyses violated chi-square assumptions due to expected frequencies <5 in certain categories. N = 221 Saudi health care professionals.
DEMOGRAPHIC CHARACTERISTICS’ ASSOCIATIONS WITH RDS’ PREFERRED APPROACH TO IMPLEMENTING TELENUTRITION IN SAUDI ARABIA
In Table 8, chi-square analysis revealed that none of the demographic variables, including gender, age group, clinical designation, education level, or years of professional experience, were significantly associated with preferred telenutrition approach (all p values >0.05), where effect sizes across all comparisons were minimal. Overall data revealed that female RDs showed a higher preference for part-time telenutrition (78.8%) compared with males (67.4%), while full-time preference was most common among males (23.6%) and RDs aged 40–50 (31.8%).
Demographic Associations with RDs’ Preferred Approach to Implementing Telenutrition (N = 221)
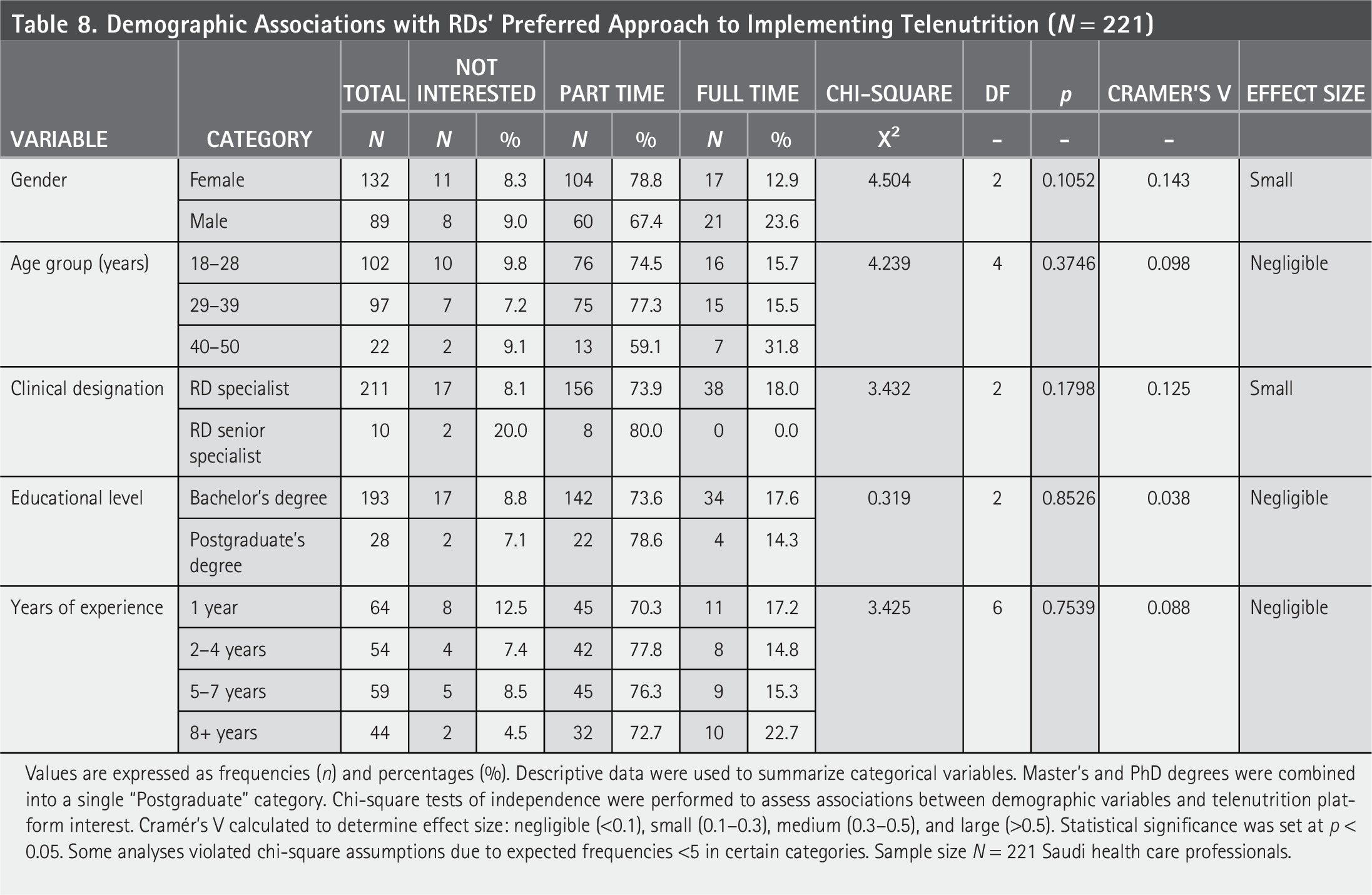
Values are expressed as frequencies (n) and percentages (%). Descriptive data were used to summarize categorical variables. Master’s and PhD degrees were combined into a single “Postgraduate” category. Chi-square tests of independence were performed to assess associations between demographic variables and telenutrition platform interest. Cramér’s V calculated to determine effect size: negligible (<0.1), small (0.1–0.3), medium (0.3–0.5), and large (>0.5). Statistical significance was set at p < 0.05. Some analyses violated chi-square assumptions due to expected frequencies <5 in certain categories. Sample size N = 221 Saudi health care professionals.
Discussion
The current study explored the current practices, reported challenges, perceived benefits, and readiness of RDs in Saudi Arabia to adopt telenutrition. It represents one of the few postpandemic national assessments aimed at guiding the development of locally adapted digital nutrition platforms. In comparison with our previous work, 29 this study included a broader and more diverse demographic profile, reflecting a shift in research focused from perceptions alone to actual practices. The most represented age group in the study was 40–50 years (43.7%), reflecting a maturing profession with midcareer RDs increasingly engaged in digital health. Interestingly, prior research has shown that middle-aged adults (40–69 years), despite reporting lower confidence in using these technologies. 33
This paradox highlights the importance of designing digital platforms that are supportive for users with moderate digital self-efficiency. Most respondents are holding a bachelor’s degree (86.1%) and working as RD specialists (95.2%), indicating consistent academic and professional roles across the sample. However, the even distribution of years of professional experience from early career to seniors suggests the interest in telenutrition is not limited to a specific career stage. Indeed, no previous study has investigated RDs characteristics in adopting telenutrition. The literature confirms that both junior and senior practitioners show enthusiasm for telehealth, 34 with younger providers more likely to adopt it. 35 Untimely, findings from this demographic profile offer strategic insights for platform developers to scale digital nutrition sustainably and equitably. Our findings indicated that RDs had notably high confidence in telenutrition delivery (85%), which aligns with a previous study by Singh et al. (2021), where 97% of RDs expressed some level of satisfaction with telehealth services. 36
Although studies on RDs’ confidence are limited, research on other specialties provides insights. For example, spine surgeons reported confidence in telemedicine for communication but expressed concerns about its limitations for physical examination. 37 Similarly, in China, most health care professionals held positive perceptions of telemedicine, with over 95% reporting satisfaction and a willingness to continue using it. 38 This reported confidence is more likely due to positive feedback and increased usage, which together build familiarity and reinforce satisfaction. Confidence was also likely driven by the accelerated adoption of telehealth services from 6% to 37% prepandemic to 63–78% during pandemic.12,14,15,28
The present study’s findings revealed that most respondents were using telenutrition on a weekly basis, which included primarily for dietary consultations and nutritional assessments by phone. Alolayan et al. (2024) found that Saudi physicians most commonly used familiar platforms such as WhatsApp, Zoom, and the Sehha app for telemedicine, reflecting a preference for simple technologies consistent with RDs reliance on phone-based telenutrition. 39 Gnagnarella et al. (2022) noted a shift among Italian RDs toward audiovisual platforms such as Google Meet, suggesting regional disparities in digital readiness. The continued dominance of phone calls as the primary communication method illustrates reliance on simple, accessible technologies, yet it may include barriers that may influence the effectiveness of telenutrition delivery. 15
Regarding anthropometric data collection, weight, height, and BMI were the most assessed metrics, while waist circumference was rarely used during telenutrition services. Indeed, concerns were raised about the accuracy of anthropometric measurements taken remotely, due to the limited availability of telehealth devices and standardized home equipment in Saudi Arabia. 40 Still lower dropout and failure rates compared with traditional consultation. 41
Recent studies in Saudi Arabia reveal both potentials and challenges of telehealth implementation. While telenutrition is perceived as useful and convenient. 9 Cultural factors, including language barriers and privacy concerns regarding video consultations, also impact effectiveness. 42 Despite overall satisfaction, technical issues and preferences for in-person care persist. 43 The lack of telemedicine knowledge among health care remains a major barrier. To enhance telehealth services, recommendations include improving internet accessibility and offering better training for health care providers. 44 Our study divided barriers into two categories: measurement-related and technical-related, for the first time in the literature.
Interestingly, measurement challenges, including patients’ difficulty in performing accurate self-assessments and in following instructions, were reported significantly more frequently than technical issues. These findings are consistent with Bookari et al. (2023), who reported that 26.9% of Arab dietitians struggled to obtain accurate measurements during remote consultations. 11 Indeed, measurement challenges facing patients’ difficulty in accurate self-assessments and adherence to instructions have been prevalent. 45 Previous research in Saudi Arabia confirmed mostly issues to be related to internet connectivity 39 and patients’ disengagement. 27 Athletic trainers have also reported both advances and barriers to telemedicine, with technology playing a crucial role in implementation. 46
Additional concerns include privacy, data confidentiality, reimbursement, and inability to perform physical examination. 47 This likely reflects Saudi Arabia’s strong internet infrastructure, shifting primary challenge to the lack of telehealth tools and patients’ limited ability to perform accurate self-measurements. While these barriers exist, much of the existing literature, focused on patient-centered benefits and health outcomes of telehealth interventions.13,41,48–50 Eid et al.’s research group in 2024 demonstrated the effectiveness of telenutrition in weight loss, along with improvements in quality of life, adherence, engagement, and low dropout rates.16–23 In the current study, operational and practice-related perceptions were collected from RDs practicing telenutrition. Findings showed that increased accessibility and flexible scheduling were identified as the top benefits, while fewer respondents mentioned convenience, patient comfort, or cost-effectiveness.
Beyond nutrition, demand for telehealth is rising across Saudi health care, seen in telenursing, especially with video calls and virtual appointments. 51 Alolayan et al. (2024) reported strong physician agreement that telemedicine reduces outpatient visits, supports chronic care, and is effective depending on specialty. 39 Still, few studies have specifically explored the benefits of telenutrition, particularly within the context of Saudi Arabia.29,52 Despite Saudi Arabia’s digital health shift under vision 2030. 53 Telenutrition remains relatively novel in clinical practice, highlighting the need for systematic reviews and evidence-based guidelines to inform the development of standardized protocols. 3
This study is the first to assess Saudi RDs’ interest and approaches toward national telenutrition platform. Findings showed that 88.2% expressed interest, with 74.21% preferring part-time implementation alongside their current job, reflecting strong motivation and flexible approach to digital care. Though no significant demographic associations were found, trends indicated that female RDs, senior specialists, and those with postgraduate degrees were more likely to prefer part-time practice. Telemedicine enables part-time practice and part-time work is increasingly favored by health professionals seeking work–life balance 54 and retired specialists to utilize their services to reach retired specialists to expand access to specialized care in underserved areas. 55 Among health practitioners, part-time practice is common among dietitians 56 and physicians, 57 where part-time work supports work–life balance, reduces burnout, 58 and is commonly favored by female professionals, 59 for its flexibility in managing family responsibilities.60,61 Part-time clinical practice enables academics to maintain clinical skills and competency. 62
Additionally, digital platforms may enhance RD employability, especially in rural or remote settings where many need to work despite initial preferences. 63 These trends suggest a strong potential for integrating telenutrition into clinical workflows if designed to meet the needs of diverse providers, for example, accommodating flexible part-time models across remote locations in Saudi Arabia. Despite the adaptation and validation of a newly national assessment tool, several limitations should be noted. The cross-sectional design limits causal interpretation, and self-reported data may introduce bias to the findings, as RDs could have overestimated their confidence or underreported challenges.
The study did not assess clinical outcomes of patients’ perspectives, and findings may not generalize to other health care professionals or other regions with differing digital health infrastructures. On the contrary, a key strength of this study lies in its national scope, postpandemic timing, and inclusion of a diverse sample of RDs across various age groups, gender, experience levels, clinical designation, and education backgrounds. It also introduces an updated categorization of barriers into measurement- and technical-related challenges, providing a clearer framework for future interventions. It also provides, for the first time, data that can inform digital nutrition platform developers on effective implementation strategies.
Conclusions
The current study is the first of its kind to explore postpandemic comprehensive investigation of Saudi RDs’ current practices, perceived barriers, benefits, preferences, and readiness for adopting telenutrition. Findings revealed a high level of confidence in telenutrition delivery, with measurement-related barriers reported as more persistent than technical issues. Interestingly, trends suggested that younger, early to midcareer female RDs with advanced education were more motivated toward part-time telenutrition engagement. These findings can inform the development and piloting of a national telenutrition platform tailored to the needs of Saudi health professionals. Future approaches should include a systematic review to synthesize global and gulf region evidence to standardize telenutrition adoption and implementation. Followed by long-term adoption interventions to assess outcome metrics such as patient satisfaction, clinical effectiveness, cost-effectiveness, and retention rates. Thus, integrating validated digital tools for remote anthropometric measurements is crucial to enhance clinical metrics accuracy.
Authors’ Contributions
N.M.S.E.: Conceptualization, formal analysis, investigation, methodology, project administration, supervision, writing—original draft, and writing—review and editing. E.A.A.: Conceptualization, investigation, methodology, project administration, supervision, writing—original draft, and writing—review and editing. G.E.A.: Conceptualization, data curation, formal analysis, investigation, and writing—original draft. All authors have read and agreed to the published version of the article.
Footnotes
Acknowledgments
The authors, therefore, acknowledge KAU Endowment (WAQF) and the Deanship of Scientific Research for technical and financial support.
Funding Information
The project was funded by WAQF at King Abdulaziz University, Jeddah, Saudi Arabia.
Informed Consent Statement
Informed consent was obtained from all subjects involved in the study.
Data Availability Statement
The data presented in this study are available upon reasonable request from the corresponding author (
Disclosure Statement
The authors declare no conflicts of interest.
