Abstract
Objectives:
To examine physical therapists’ experience of providing telerehabilitation and their perceptions of telerehabilitation for patients with musculoskeletal conditions.
Methods:
Using a cross-sectional survey, members of the Academy of Orthopaedic Physical Therapy were invited to respond.
Results:
We received 208 completed responses to our survey invitation. Physical therapists reported using little to no telerehabilitation prior to the pandemic but increased use during the pandemic, followed by the decreased use of telerehabilitation post-pandemic. Physical therapists reported that they believed that they could deliver effective care using telerehabilitation, but that it was not as effective as in-clinic care, and that they would prefer to use telerehabilitation as a part of a hybrid care model versus using only telerehabilitation. Physical therapists suggested that certain patients were more likely than others to benefit from telerehabilitation and identified specific factors (e.g., patient preference, self-efficacy) that influenced whom they consider to be appropriate for telerehabilitation. “Patient issues with technology” was identified as the most common barrier to telerehabilitation use. Most physical therapists reported planning to use telerehabilitation in the future and agreed that telerehabilitation plays an important role in expanding access to physical therapy in the United States.
Conclusions:
Physical therapists believed that telerehabilitation continues to play an important role in the post-pandemic world. Although physical therapists reported that they considered telerehabilitation to be an effective method for delivering care, they did not consider it to be a replacement for in-clinic care, and they believed that certain patients are more likely than others to benefit from telerehabilitation.
Introduction
Prior to the COVID-19 pandemic, barriers that prevented the widespread use of telerehabilitation included state practices or acts that prohibited physical therapists from delivering care via telerehabilitation and payer policies that did not allow for reimbursement for telerehabilitation services provided by physical therapists.1,2 However, policy changes during the early stages of the pandemic facilitated the rapid expansion of telerehabilitation, 3 with reports indicating that as many as 12% of physical therapy patients accessed telerehabilitation at the peak of its use in 2020. 4 A number of studies were also conducted during that time that found telerehabilitation to be acceptable and effective among patients with a variety of health conditions, including those with musculoskeletal pain.5–9
Although telerehabilitation played a clear role in expanding access to physical therapy during the pandemic, the role of telerehabilitation in the post-pandemic world is less clear. Since their peak in the first quarter of 2020, telerehabilitation utilization rates have decreased substantially. 4 Multiple factors may have influenced this decline, such as changes in social distancing guidelines, patient demand for these services, or uncertainty surrounding reimbursement for telerehabilitation in the future. Studies conducted during the pandemic reported that physical therapists’ perceptions of telerehabilitation served as both enablers of and barriers to the adoption of telerehabilitation into practice.10,11 It stands to reason that physical therapists’ perceptions of telerehabilitation will continue to play a major role in the way that telerehabilitation is used after the pandemic. However, there has been little to no research examining physical therapists’ perceptions of telerehabilitation since the end of the public health emergency.
To address this knowledge gap, we conducted a national survey examining physical therapists’ perceptions of telerehabilitation for patients with musculoskeletal pain. Musculoskeletal conditions are among the most common conditions seen by physical therapists, and patients with these conditions represented the largest group of telerehabilitation users during the pandemic.4,12,13
Methods
SURVEY DEVELOPMENT
A survey was developed for the purposes of this study by members of the study team with expertise in physical therapy and musculoskeletal health and experience with telerehabilitation. After its development, the survey was piloted among six physical therapists with experience of providing care to patients with musculoskeletal pain and telerehabilitation. The final version of the survey incorporated feedback from the pilot regarding the survey length, content, and clarity.
The final version of the survey used in this study consisted of 29 questions, separated into five sections: (1) current and previous use of telerehabilitation, (2) perceptions of telerehabilitation, (3) future use of telerehabilitation, (4) patient subgroups appropriate for telerehabilitation, and (5) respondent characteristics. Questions included a combination of multiple choice and Likert-style response options. One question included an “other” response with a free-text option. The final version of the survey is available in the Supplementary Data.
SURVEY DISTRIBUTION
Surveys were mailed electronically to members of the Academy of Orthopaedic Physical Therapy (AOPT). This provider population was chosen as it comprises primarily physical therapists with an interest in musculoskeletal conditions, our area of interest for this study. The AOPT mailing list is commonly used to conduct studies of this nature.14–16 Surveys were distributed in March 2024. We accepted survey responses completed by the end of May 2024.
DATA ANALYSIS
Descriptive statistics were used to describe responses to all included survey questions. Responses to questions about respondents’ perceptions of telerehabilitation (questions 7–13), which included five Likert-scale response options (strongly agree, agree, neutral, disagree, strongly disagree), were collapsed into three categories (agree, neutral, disagree) to simplify comparisons between questions. Only complete survey responses were included in our analysis, defined by a respondent navigating through all questions and clicking “survey complete.”
ETHICS APPROVAL
This study was recognized as exempt by the [Removed for blinding] Institutional Review Board (IRB00402769).
Results
RESPONDENT CHARACTERISTICS
We received a total of 218 responses to our survey invitation, with 208 (95.4%) physical therapists responding to all survey questions. The sample of physical therapists who completed our survey were experienced, with over half of the respondents (n = 107; 51.7%) reporting ≥20 years of experience as physical therapists and 54 (26.1%) of the respondents reporting between 10 and 20 years of experience (Table 1). Over half of the respondents were board-certified specialists (n = 132; 64.1%), with orthopedics being the most common type of board certification (n = 126; 96.9%). Respondents practiced in diverse geographic settings, with 104 (50.7%) respondents reporting that they practiced in suburban areas, 58 (28.3%) in urban areas, and 43 (21.0%) in rural areas.
Characteristics of AOPT Member Respondents To Telehealth Utilization Questionnaire (N = 208)
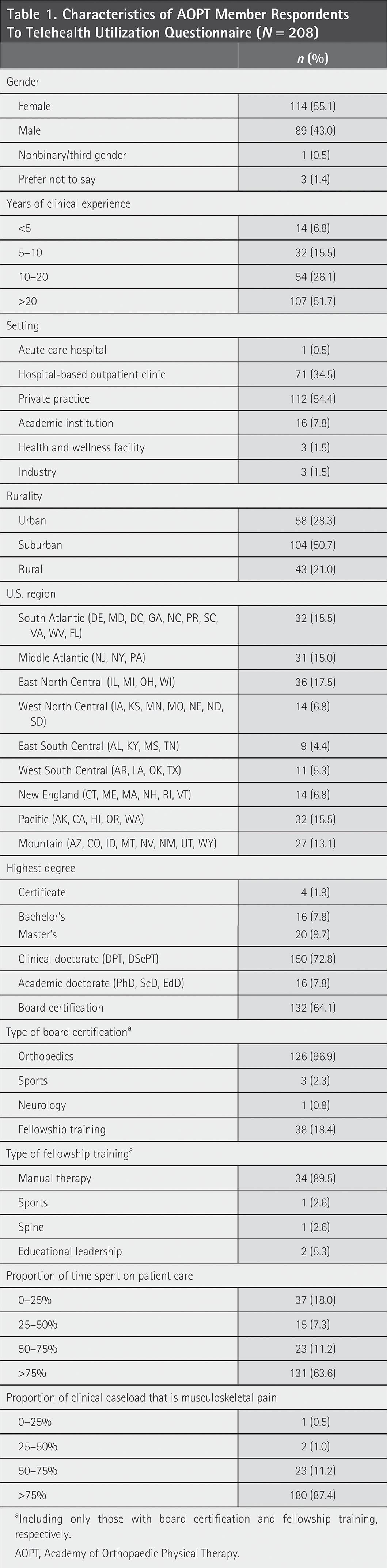
Including only those with board certification and fellowship training, respectively.
AOPT, Academy of Orthopaedic Physical Therapy.
PREVIOUS USE OF TELEREHABILITATION
Most respondents (n = 181; 87.0%) reported that they had never provided care using telerehabilitation prior to the pandemic, with the next most common response being that respondents provided care using telerehabilitation “rarely” before the pandemic, which was operationalized as less than monthly (Fig. 1). Most respondents (n = 182; 87.9%) indicated that during that timeframe, patients receiving telerehabilitation care accounted for 0% of their weekly caseload, followed by 9.2% of respondents (n = 19) reporting that telerehabilitation care accounted for 1–10% of their weekly caseload (Supplementary Fig. S1).
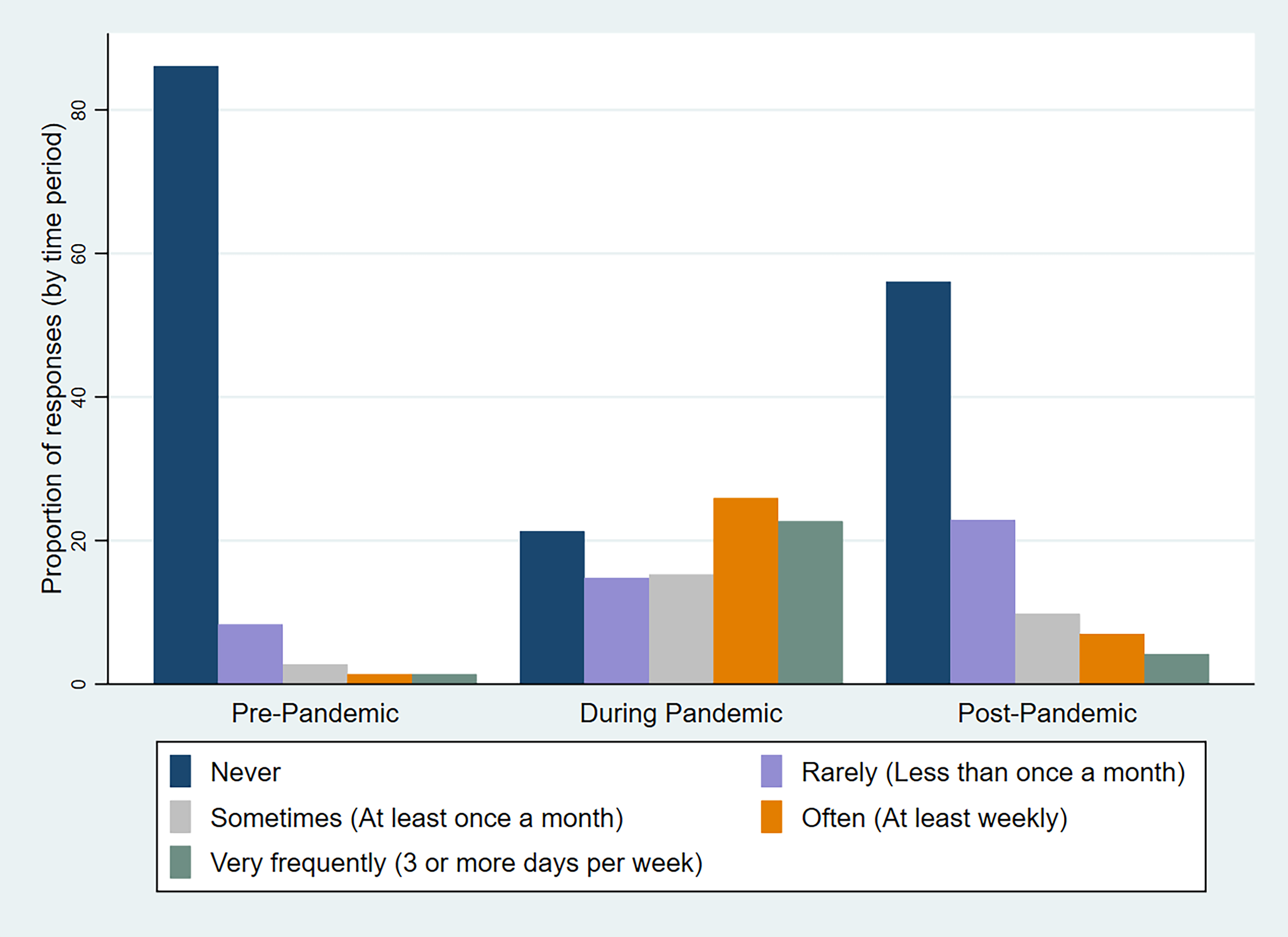
Frequency of telerehabilitation delivery before, during, and after the COVID-19 pandemic. Survey participants were asked to indicate the highest frequency during the period defined as March 2020–May 2023.
When asked how frequently they provided telerehabilitation during the pandemic, the highest proportion of respondents (n = 55; 26.4%) indicated that they provided care using telerehabilitation “often,” which was operationalized in our survey as ≥1 time per week (Fig. 1). The second most common response (n = 47; 22.6%) to this question was “very frequently,” operationalized as providing care using telerehabilitation ≥3 days per week. When asked what proportion of patients they saw via telerehabilitation during the pandemic, the highest proportion of respondents indicated that they provided care via telerehabilitation for 1–10% of their caseload (n = 73; 35.6%), followed by 0% (n = 44; 21.5%), and >50% (n = 41; 20.0%)(Supplementary Fig. S1).
When asked how frequently respondents provided care using telerehabilitation after the pandemic, the most common response (n = 117; 56.8%) was “never,” followed by “rarely” (n = 47; 22.8%) (Fig. 1). Most respondents indicated that the proportion of their patients who used telerehabilitation on a weekly basis was 0% (n = 139; 66.8%), followed by 1–10% (n = 49; 23.6%) (Supplementary Fig. S1).
PERCEPTIONS OF TELEREHABILITATION
Participant responses to questions about their overall perceptions of telerehabilitation are summarized in Fig. 2. The highest proportion of respondents (n = 101; 48.6%) indicated that they believed that they could deliver effective care using telerehabilitation, but the majority of respondents (n = 129; 62.0%) indicated that they did not consider telerehabilitation to be as effective as in-clinic physical therapy. Most physical therapists (n = 96; 46.4%) agreed that some patients may respond better to telerehabilitation than to in-clinic care.
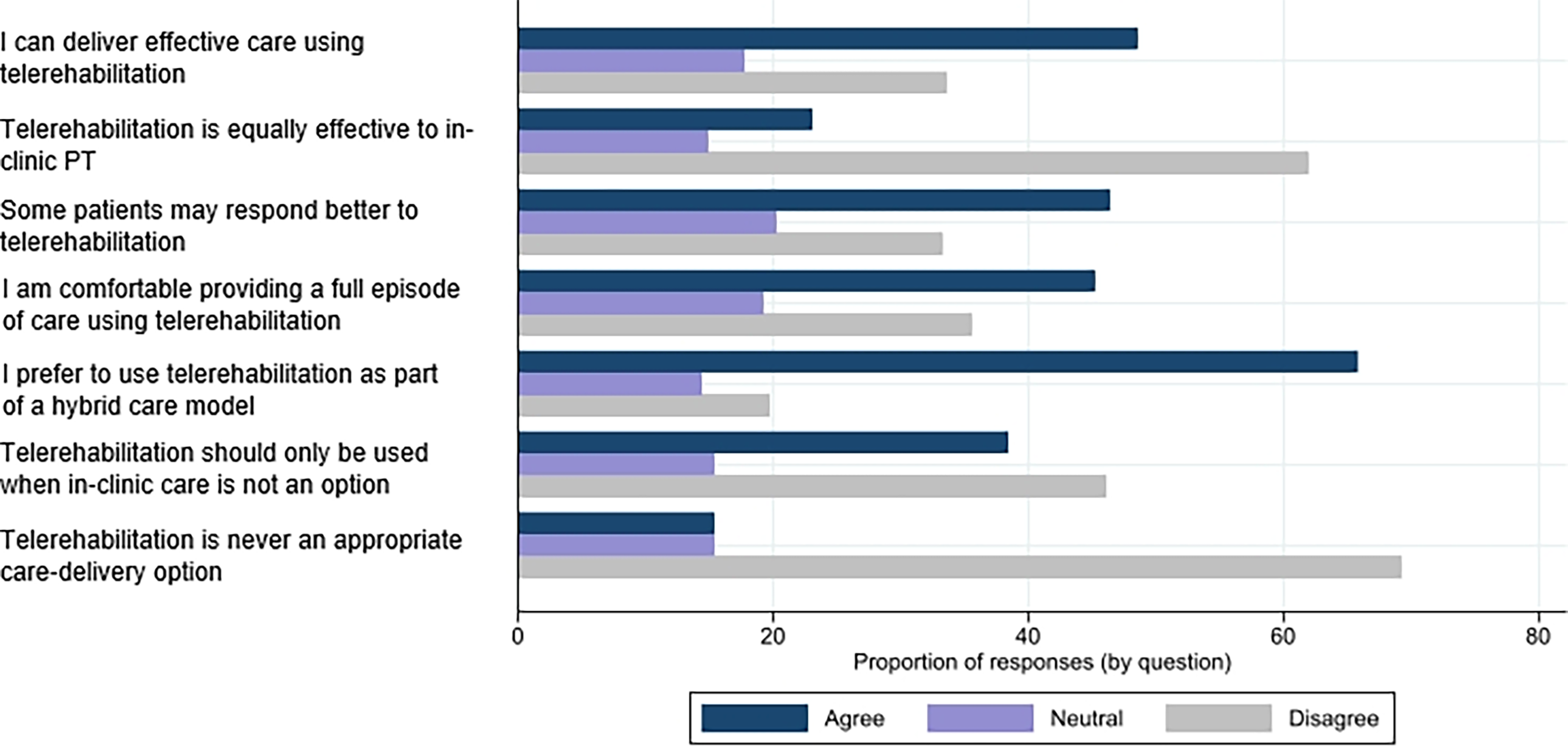
Physical therapists’ perceptions of telerehabilitation effectiveness and appropriateness.
With regard to the way that telerehabilitation is used as a part of a full plan of care, 94 (45.2%) respondents indicated that they would feel comfortable providing a full episode of care entirely through telerehabilitation. At the same time, 137 (65.9%) respondents indicated that they would prefer to provide telerehabilitation as a part of a hybrid care model, if this was an option.
Most respondents (n = 96; 46.2%) disagreed with the statement that telerehabilitation should be used only when in-clinic care is not an option. Most (n = 144; 69.2%) also disagreed with the statement that telerehabilitation is never an appropriate way to deliver care.
FUTURE USE OF TELEREHABILITATION
When asked about the future use of telerehabilitation, the highest proportion of respondents (n = 46; 22.3%) indicated that they “agree” with a statement suggesting they plan to provide telerehabilitation in the future (Table 2). The most common response (n = 84; 40.4%) was to “agree” with a statement suggesting that telerehabilitation plays an important role in expanding access to physical therapy.
Future Use of Telerehabilitation and Potential Barriers to Use
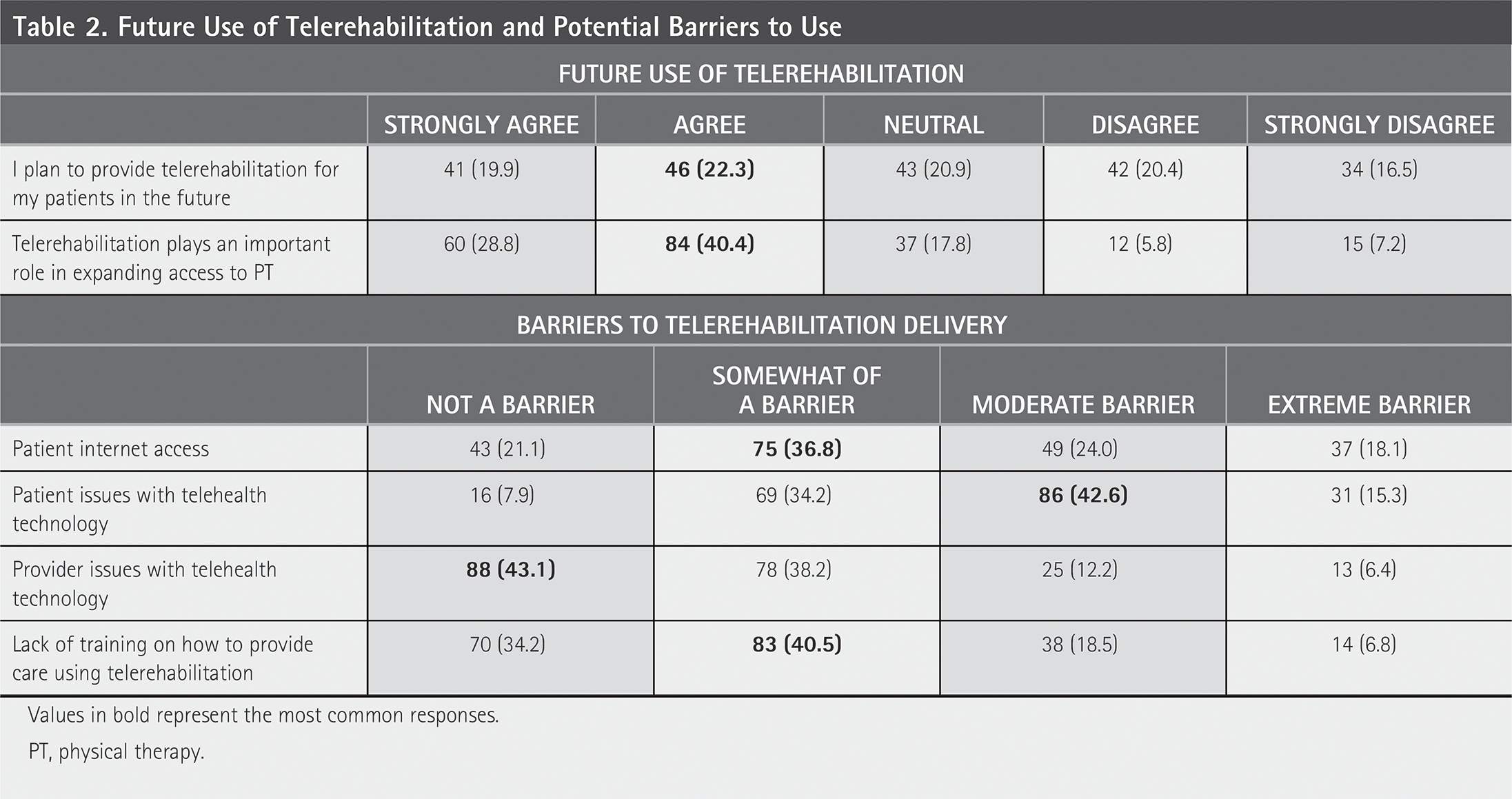

Values in bold represent the most common responses.
PT, physical therapy.
Respondents indicated that “patient issues with technology” was a barrier to providing telerehabilitation, with 86 (42.6%) respondents indicating this to be a “moderate barrier” (Table 2). Respondents indicated that internet access, provider issues with technology, and lack of provider training were less likely to be barriers, with respondents indicating that these were only “somewhat of a barrier” or “not a barrier.”
INDIVIDUAL PATIENT FACTORS INFLUENCING THEIR APPROPRIATENESS FOR TELEREHABILITATION
For the statement that telerehabilitation is best suited for specific groups of patients with musculoskeletal pain, the most common response (n = 85; 40.9%) was “agree.” According to survey responses, providers believed that patients who prefer video visits (n = 165; 80.1%), have access to the internet (n = 98; 47.8%), have high self-efficacy (n = 123; 60.3%), and are comfortable using technology (n = 145; 70.7%) are more appropriate for telerehabilitation (Table 3). Respondents believed that patients who are available for in-clinic appointments (n = 127; 62.0%), have acute conditions (n = 112; 54.9%), have high psychosocial risk (n = 77; 38.1%), have low self-efficacy (n = 122; 59.8%), or have a postoperative status (n = 144; 70.2%) may be less appropriate for telerehabilitation. Respondents indicated that other individual factors included in our survey had no impact on patients’ appropriateness for telerehabilitation.
Individual Factors Influencing Patient Appropriateness for Telerehabilitation
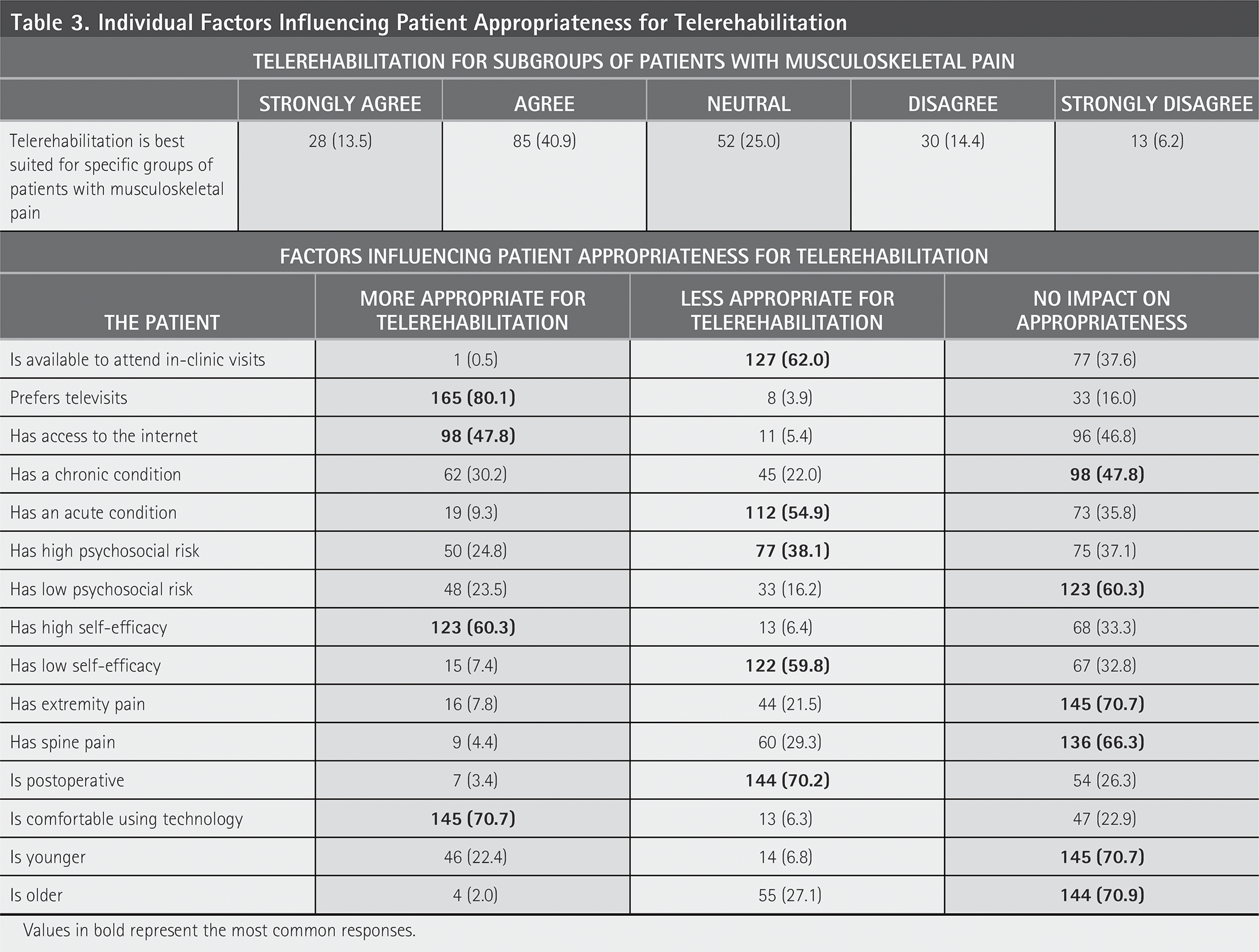

Values in bold represent the most common responses.
We also provided a free-text option for respondents to indicate other factors they believed might influence patients’ appropriateness for telerehabilitation. Common factors listed by respondents included social determinants of health, safety (e.g., fall risk), medical complexity, access to technology, caregiver support, and likelihood that patients would benefit from hands-on interventions.
Discussion
This study is one of the first to examine physical therapists’ perceptions of telerehabilitation since the end of the COVID-19 pandemic. The results of this study indicated that physical therapists felt that they can deliver effective care for patients with musculoskeletal pain through telerehabilitation. However, most did not believe that the care provided through telerehabilitation is as effective as the care provided in clinics. Our results also suggest that physical therapists considered the method by which patients receive care (i.e., in-person or using telerehabilitation) to be a multifactorial decision that includes the consideration of patient preference and individual patient characteristics.
The results of this study are consistent with those of previous studies that have reported an increase in the use of telerehabilitation during the early phases of the pandemic and a decline in telerehabilitation utilization during the later stages of the pandemic, based on data from insurance claims and a physical therapy outcomes database.4,17 Our results build on these previous studies by examining telerehabilitation use after the end of the public health emergency, providing insights into its use following the pandemic. It is not surprising that our respondents reported that they provide care through telerehabilitation less often since the pandemic ended. However, the survey results suggest that telerehabilitation utilization rates have not returned to the pre-pandemic rates. When surveyed on the pre-pandemic use of telerehabilitation, 87.0% of physical therapists reported that they “never” provided telerehabilitation. When surveyed on the post-pandemic telerehabilitation use, 56.8% of the therapists reported that they “never” provided telerehabilitation. This suggests that approximately 30% more of the physical therapists surveyed are providing telerehabilitation after the pandemic than before the pandemic.
The results of the present study suggest that physical therapists view telerehabilitation as a useful tool for patients with musculoskeletal pain but are skeptical about its use as a replacement for in-clinic care. Multiple factors may contribute to this viewpoint. For example, physical therapists may perceive a lack of hands-on interventions (e.g., manual therapy, modalities) as a limitation to telerehabilitation, which is supported by the comments provided by physical therapists indicating that patients who can benefit from hands-on care are less appropriate for telerehabilitation. It is also possible that a lack of experience or confidence in providing telerehabilitation contributes to this perspective. Telerehabilitation has not historically been included in physical therapy curricula, and most physical therapists had no experience of providing telerehabilitation before the pandemic. Moreover, there is little to no evidence available in this area, and best-practice recommendations for telerehabilitation are only now beginning to be published. 18 Given the lack of telerehabilitation training, experience, evidence, and guidance, it is possible that physical therapists prefer providing care in-person because they are more familiar and comfortable with this approach.
Taken together, the survey results suggest that patient preference plays an important role in determining how physical therapy care is provided. For example, the majority of physical therapists agreed that some patients may respond better to care provided through telerehabilitation, and they disagreed with the statement indicating that telerehabilitation should be used only when in-clinic care is not an option. Approximately 80% of physical therapists indicated that telerehabilitation is more appropriate when patients have a preference for telerehabilitation. This is an important finding, as it suggests that there may not be a single answer to the question of whether telerehabilitation is an effective treatment for patients with musculoskeletal pain. Rather, the effectiveness of telerehabilitation as a care-delivery mechanism may be dependent on individual patient factors, such as patient preference. Researchers conducting studies examining the effectiveness of telerehabilitation might consider including subgroup analyses that examine the effects of telerehabilitation among patients with preferences for or against telerehabilitation.
The strengths of this study are the use of a nationally distributed survey and access to a geographically diverse provider sample. The study also has important limitations to consider. As is common in studies using survey data, the results of our study may be influenced by recall bias, especially for questions that required survey respondents to recall information from prior to the pandemic. We also used a convenience sample of physical therapists belonging to the AOPT, which included a high percentage of board-certified physical therapists with ≥10 years of experience. It is possible that this sample is not representative of the entire population of physical therapists caring for patients with musculoskeletal pain, which may limit the generalizability of our results. Our results may have also been influenced by response bias, as physical therapists with stronger opinions on telerehabilitation may have been more likely to respond to our survey invitation.
Conclusions
The surveyed physical therapists reported providing care using telerehabilitation less frequently after the pandemic than during the pandemic, but at higher frequencies than prior to the pandemic. Physical therapists also reported that telerehabilitation can be an effective approach for treating patients with musculoskeletal pain, especially those who are unable to or prefer not to receive care in clinic. However, the surveyed physical therapists do not view telerehabilitation as a replacement for in-clinic care. More research is needed to examine the effectiveness of care provided using telerehabilitation compared with in-clinic care to inform decisions made by physical therapists surrounding care delivery options.
Authors’ Contributions
K.H.M. and R.L.S. conceptualized the study, acquired funding, conducted the investigation, administered the project, provided resources and software, supervised the study, provided visualization, and wrote the original draft. K.H.M. performed data curation and formal analysis. K.H.M., K.I.M., J.M.F, N.T., A.S., M.F., M.W., E.O., J.A., and R.L.S. developed the methodology and performed critical review and editing of the article.
Footnotes
Acknowledgments
Study participants were not involved in the design, conduct, interpretation, or translation of the current research. A preprint version of this article is available on MedRxiv at ![]() . For editorial assistance, we thank Denise Di Salvo, MS, in the Editorial Services group of The Johns Hopkins Department of Orthopedic Surgery.
. For editorial assistance, we thank Denise Di Salvo, MS, in the Editorial Services group of The Johns Hopkins Department of Orthopedic Surgery.
Funding Information
This article is the result of funding in whole or in part by National Institutes of Health (NIH; UH3AR083838). It is subject to the NIH Public Access Policy. Through acceptance of this federal funding, NIH has been given a right to make this article publicly available on PubMed Central upon the official date of publication, as defined by NIH.
Ethics Approval
This study was recognized as exempt by the Johns Hopkins Medicine Institutional Review Boards (IRB00402769).
Data Sharing
The datasets generated and/or analyzed in the current study include sociodemographic information and physical therapists’ perceptions of telerehabilitation. The data are not publicly available because of their confidentiality but are available for noncommercial use from the corresponding author on reasonable request.
Disclosure Statement
The authors affirm that they have no financial affiliation (including research funding) or involvement with any commercial organization that has a direct financial interest in any matter included in this article, except as disclosed and cited in the article. Any other conflict of interest (i.e., personal associations or involvement as a director, an officer, or an expert witness) is disclosed and cited in the article.
Supplemental Material
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
