Abstract
Introduction
Lay caregivers, such as friends and family members, provide support to adult patients throughout all stages of the kidney transplant process, pretransplant through discharge.1–3 Transplant centers consider the availability of social support when deciding transplant eligibility 4 and rely on caregivers to provide emotional support and practical support, such as transportation, care navigation, and medication administration, while managing their own responsibilities (work and childcare). 5 Caregiving can be rewarding but may also impose burdens on caregivers, jeopardizing their well-being and ability to provide care.5,6 Despite the essential role that caregivers play, a paucity of programs supporting the engagement of caregivers exists.7–13
Caregiver programs in kidney transplantation have typically been mutually shared solutions for both patients and caregivers7–13 and were rarely solely for caregivers. 14 Interventions have addressed education,7–9,12,13 navigation support, 11 emotional support, 14 and resilience. 10 Sparse data exists on the most efficacious content and delivery of caregiver engagement efforts and their impact on both caregiver and patient outcomes. 2 A 2019 consensus conference, led by the American Society of Transplantation, recommended refinement of educational and other resources for caregivers as a highest priority. 2
Transplant center usual care approaches to engage caregivers include policies, processes, and culture of communication. 15 Knowledge of center-specific approaches may provide insights for intervention design and may confirm facilitators—areas that do not require intervention—which lead to more efficient use of intervention resources. This study undertook interviews of caregivers of adult kidney transplant recipients at a large kidney pancreas transplant center in the United States. The goal was to describe caregiver experience in supporting kidney patients before and early after kidney transplantation, describe barriers and facilitators of caregivers to support patients, including the usefulness of center-specific approaches and coping strategies used, as well as suggested improvements based upon caregiver experience.
Methods
Design
This qualitative descriptive 16 study involved individual interviews of caregivers recruited through kidney transplant recipients at 1 transplant center in the northeastern United States. Each participating caregiver provided written or electronic informed consent and received a $25 gift card for their participation. The COREQ guidelines were followed in the reporting of the study. The study was approved by the institutional review board (IRB ID 00002771).
Setting
The work emerged from a larger community-based participatory research (CBPR) project to conceptualize and implement kidney transplant access and outcome programs and resources with/for individuals with kidney failure. The project was pre-empted by 2 years of CBPR focused on kidney patient individual needs wherein engagement of caregivers was consistently cited as an important area to address. This program of research was proposed by a community advisory board (CAB) of 2 kidney transplant recipients, 2 dialysis patients, 2 caregivers, 1 kidney donor, and 1 dialysis social worker who work alongside researchers in anthropology, epidemiology, and transplant surgery. The purpose of this particular aspect of the project was to identify entry points for further study around the needs of caregivers of kidney transplant patients at a transplant center within a safety-net hospital in 1 northeastern US city, where citizens face disproportionate levels of social challenges. The community is characterized by high rates of chronic disease and 27.6% of the population are low income. 17
The transplant center performs approximately 140 kidney transplants annually; typical recipient demographics are age range 45-80 years, White (55%), African-American (35%), male (58%), and ≤high-school educated (60%). Caregiver demographics are not routinely ascertained. All research tools, including the semistructured interview guides, were co-created with the advisory board. Based on the CBPR approach, the research was responsive to community identified needs and sought to identify the facilitators of caregiving from within the city's only transplant program, with insights from caregivers of transplant recipients. Further, the interview transcripts were read and interpreted by a community advisory board member.
Sampling
Consecutive adult recipients who received kidney-only transplants between September 1, 2021 and December 31, 2021, were approached in the hospital or by telephone within 3 months of transplantation, after receiving a letter to opt out from receiving invitations to research studies. Recruitment was concluded when coding saturation was achieved and required extending enrollment for 1 month longer than anticipated. A researcher, who did not know the patients, asked them whether they would be willing to provide contact information for their primary or secondary caregiver. Eligible participants spoke English and were at least 18 years of age. Of 30 kidney transplant recipients, 2 declined, stating they did not have a caregiver. The remainder provided contact information for their caregiver. Twenty-eight caregivers were invited, and 23 participated (recruitment rate of 77%). One interview was incompletely recorded due to technical malfunction and was excluded, as field notes were not taken. Transplant recipients did not participate in the interviews.
Information Collection
Individual interviews were conducted one-to-one between October 28, 2021 and March 15, 2022 in private meeting rooms in the participating transplant center or over video conference using Zoom at the caregiver's discretion to facilitate participation. Interviews were led by a White female social science researcher who holds a PhD in communication and also had 18 months of experience as a transplant research coordinator, with none in the realm of caregiving. Interviews were structured around 3 areas of experience: (a) navigating phases of the kidney transplant process (initial evaluation, outpatient testing, waiting for the transplant, and surgical recovery); (b) modalities of education and support offered at the transplant center (provider communication, caregiver agreement, supplemental information, and support resources); and (c) coping strategies. While discussing areas of experience, participants were asked about barriers, facilitators, and recommendations, where appropriate. The interview guide is provided (

Participant interview guide.
Data Analysis
Qualitative description was conducted to present the accounts of caregiver experiences and the meanings and emotions participants gave to those accounts as well as describe what was found in everyday language as entry points for further study. 16 The research team members, including the lead author, an anthropologist, a medical student, and a transplant surgeon, independently read the transcripts and discussed their thoughts together and with a lay caregiver from the transplant center's community advisory board, who also independently read the transcripts. The lead author generated initial codes by open coding each participant statement inductively in Microsoft Word according to their stated meaning. The preliminary coding scheme was reviewed and discussed by the research team for accuracy and consistency. Disputes over code definitions and applications were resolved through discussions and then applied to the remaining manuscript. Coding saturation was achieved when no further coding modifications were needed. NVivo software (version 10) was used to organize the data using content analysis, the research team generated domain and subdomain areas. The incidence of some subdomains was counted for each participant; however, emphasis was placed on range and exploration, rather than the recurrence or quantification of responses. Participants were not involved in the analysis process or in confirming the accuracy of the transcripts and findings to avoid further burden of research. The lay caregiver on the research team helped to confirm the domains and subdomains and their implications.
Findings
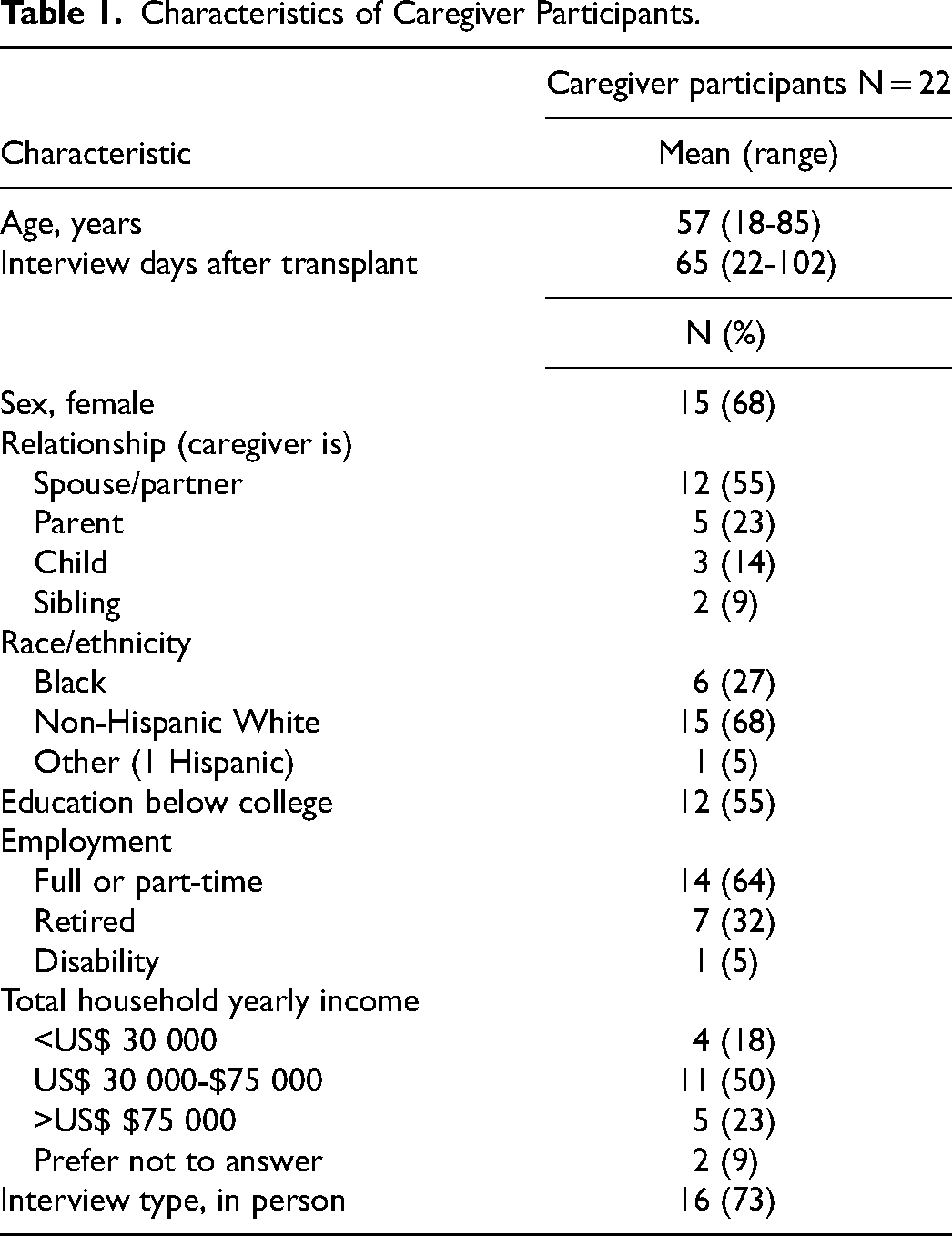
Overall, 23 caregivers of adult kidney-only transplant recipients participated in individual interviews. Interview sessions occurred at a mean of 65 days after kidney transplantation, were conducted predominantly in person, and lasted between 19 and 51 min (in person [N = 16]: mean 30, range 19-40 min; Zoom [N = 6]: mean 36, range 28-51 min). Participant characteristics are shown in
Characteristics of Caregiver Participants.

Domains and subdomains that emerged through inductive analysis of caregiver interviews are presented below and in
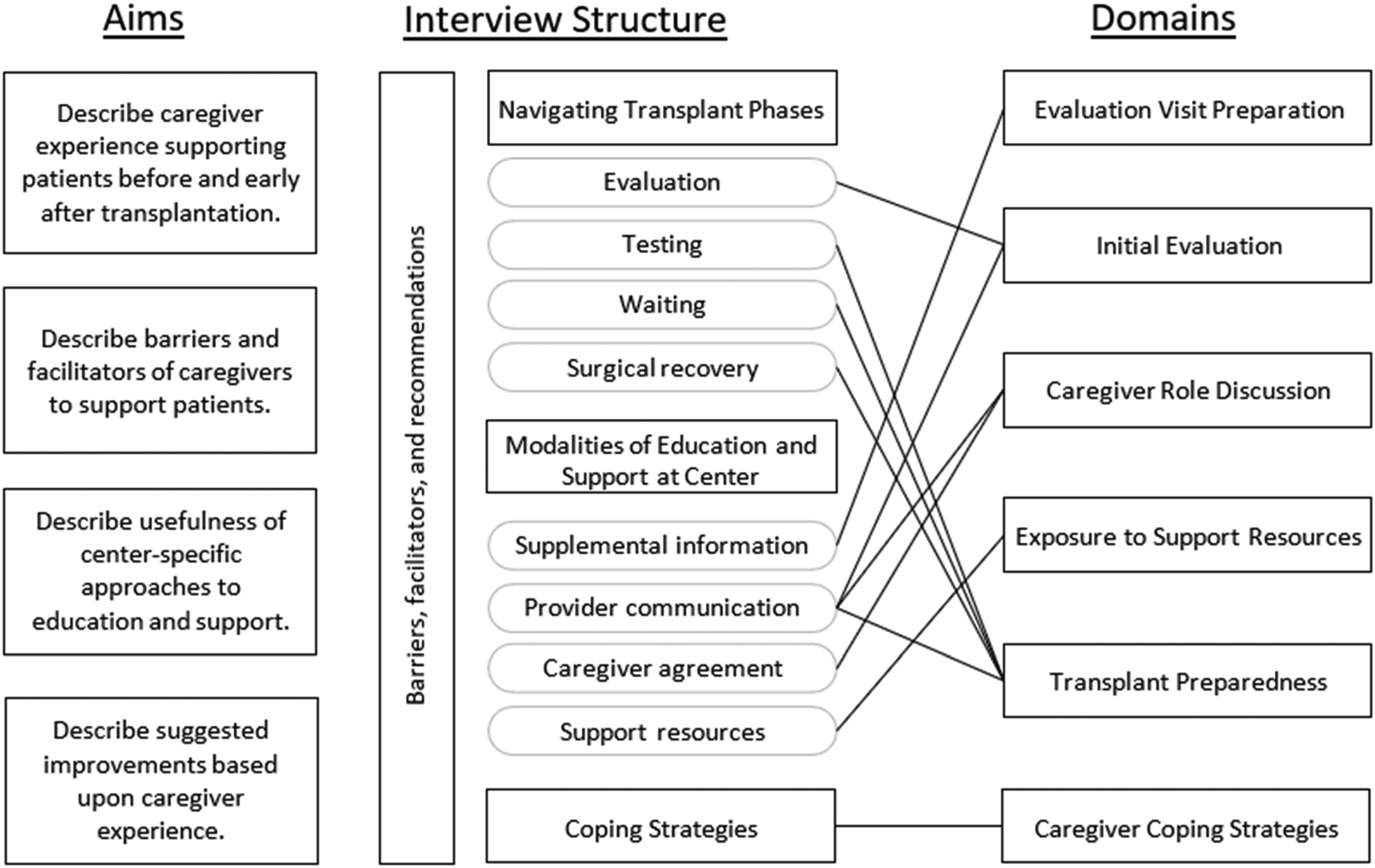
Structure of the study.
Caregiver Interview Domains, Subdomains, and Representative Quotes. a

Each quote was adapted with corrections of verbal and nominal agreement, including removal of interruptions (you know, okay, like), language voices (um, uh, yeah, then), and word repetitions (no, no). Inside parentheses (caregiver self-reported relationship to patient, age in years, gender).
Evaluation Visit Preparation
Caregivers were prompted to comment on the transplant center education booklet that had been mailed to the patient prior to the evaluation visit. Caregiver responses fell into subdomains of booklet not aware (n = 3) and aware (n = 19). A couple of respondents did not remember receiving the booklet or forgot about it. Most remembered the booklet and found it useful. They described it to be informative and thorough. One recounted bringing the booklet to the subsequent initial evaluation. Others found the booklet useful to reinforce information and to review after time had passed: “It's nice to have it all in writing to go back and refer to it in case you forgot something or you wanna double check something.” Some used the booklet alongside other resources, such as websites and videos. Some mentioned the center's video education that they had received as research participants, finding the videos helpful to reinforce print education and to educate family members.
Suggestions for improvement to the visit preparation materials included to add content about caregiver role and unexpected transplant outcomes, and to make sure material is available online, preferably in video format, but to not rely only on video/digital material: “What the social worker was planning to say could be put online. So, in cases like this, where there's kind of information overload, there's something to refer to.”
Initial Evaluation
When asked about their experience with the initial evaluation appointment, caregiver responses centered around what happened in the appointment and the information received—both helpful and overwhelming. Caregivers reported that the evaluation involved meeting many medical providers, receiving “a lot of” information, and having tests done. Overwhelm was primarily attributed to the length of the evaluation and extent of information given: “It was a lot to take in all at once.” Challenges with information uptake were observed by caregivers of patients who were older and non-English speaking. Comments reflecting helpfulness of the evaluation involved providers who were “nice,” gave good explanations about the process, were reassuring about the outcome, and took time to answer questions.
Caregivers recommended not lengthening the evaluation day and to repeat information throughout the journey: “I’ll say repeated information, not just having that one day.”
Caregiver Role Discussion
Participants were prompted to comment on their discussion with the transplant social worker during the initial evaluation about the caregiver role and the caregiver agreement (a 1-page document that describes general caregiving activities and is signed by caregivers to indicate willingness to be a caregiver to the recipient). Caregiver responses were grouped in the subdomains of neutral and positive. Some respondents seemed neutral or somewhat matter-of-fact on the topic, either stating that it was already part of their role or identity to care for the patient or that it was something that the patient had done for them in the past or would do if needed. Most respondents stated that the discussion helped to confirm their understanding about what their caregiver role would be. Caregivers generally thought positively about the caregiver agreement, stating that it helped them prepare: “I thought it made sure that you understood, that there's a lot that can go on here that they might need help with.” One participant said it formalized the role and encouraged people to really think about what they were “getting into.” Caregivers recounted their involvement in later conversations to recruit other caregivers, especially when the primary caregiver was intending to donate a kidney. Comments implied a need for more details on caregiver responsibilities.
Exposure to Support Resources
Caregivers were prompted to comment on flyers they received from the social worker during the transplant evaluation and in monthly email blasts among those who opted in. The flyers promoted 3 support options available to patients and friends/family: a certified art therapist, the transplant center's Facebook support group, and a patient-run support group (in-person before March 2020 and on Zoom after). Responses related to support resources fell into the subdomains of used (n = 7) or not used (n = 15) by caregiver and/or patient. Respondents generally remembered getting the information both from the social worker and via email. The only service used was the center's Facebook support group. For those who did use the social media resource, both caregivers and patients found it helpful to see others going through the same experience: “Believe it or not, you learn from people's experiences.” They indicated that they mostly read the material but did not post or actively engage in the online community. Reasons for not joining the social media resource were unfamiliarity with technology, aversion to social media, or had not pursued yet. Suggested improvements related to providing more reminders about the Facebook resource.
Transplant Preparedness
Participants were asked about their feeling of preparation for the transplant process. Responses were categorized as Yes and No and predominantly focused on the post-transplant course. Those who answered no also stated that there were “complications” and “You can’t really prepare.” Participants who answered that they were prepared generally stated that they knew what they were getting into and that it had all been explained. Some stated that the transplant process happened faster than expected. Also, family was around to help. One participant said that the information that was shared with caregivers “all made sense afterwards.” Participants who answered that they were not prepared cited the post-transplant monitoring and medications and the amount of time they spent caring for their loved one. One person stated that they were not prepared for the mood swings their loved one experienced. Among those who were not prepared, participants discussed the unexpected complications that emerged. These included being readmitted to the hospital, rejection or fear of rejection, and communication with the providers/physicians. Finally, among those who did not feel prepared, 3 people stated that you cannot prepare, it “happens in the moment.”
Caregivers suggested improved communication with patients and caregivers about patients’ health status and treatments: “You did have some kind of brochure because I read through… I felt like I needed more.”
Caregiver Coping Strategies
When discussing their coping strategies, caregivers expressed that it was an emotional roller coaster and very hard/taxing. Other common words/phrases used were “scary,” “nerve-racking,” “stressful,” “overwhelming,” “rocky,” “upset,” “too much,” and “not a piece of cake at all.” Strategies for coping fell into 3 categories: attitudes, actions and supportive people.
There were a number of attitudes that caregivers adopted or adhered to. These included attitudes of altruism, resilience, patience/optimism, gratitude, flexibility, relativism, the feeling of going down the road together, and reciprocity–perceiving that the patient would have done the same for them or had done the same for them in the past: “He was my caregiver for all that time. And then we reversed it.”
Actions taken to cope included having support from friends and/or family, taking time for oneself, and spending time with the patient: “I go shopping. I do a lot of things by myself and he's home. He's okay. If there's an issue, he calls my phone, but he's doing so well.”
Caregivers often relied on supportive people to help them or the patient during the transplant journey. Some caregivers spoke about support in general, citing family members or friends who were there and helped out. Sometimes this meant taking turns with appointments or staying home with the patient while the other went out for work or errands. Participants sometimes specified types of support—informational or physical support. Informational support came from friends or family who had gone through similar processes, people working in the health profession, or someone else who could help remember the details of appointments. Physical support included transportation, shopping, cooking, and wound care. Participants also brought up support groups, saying they were very helpful and allowed them to relate to others experiencing the same things. A few respondents mentioned they or the patient should have engaged in a support group. One participant expressed the need to talk with and hear from other caregivers, particularly those caring for older adults. A couple of respondents mentioned that they did not have any people who could relate to their situation, sometimes despite efforts to find support. One participant said that they did not need or want other support.
Suggested improvements related to creating pathways to connect patients and caregivers with others going through the same experience.
Discussion
Studies exploring kidney transplant caregiver experiences, including caregiving burden, depression, and quality of life, suggest that effective informational and support interventions are needed to facilitate caregiver engagement.18,19 There is a paucity of caregiver intervention studies in kidney transplantation. Most have a single focus, such as increasing knowledge or resilience, and there is minimal evidence of program impact from qualitative and single-group studies. Kidney transplant programs routinely use different methods to facilitate caregiver strengths, capacity to use center-specific supports, and coping. This article describes a qualitative study including lay caregivers of kidney transplant recipients at an east coast urban transplant center who described their experiences and perspectives of the transplant process, from evaluation through discharge.
Although caregivers used and appreciated information intended for the patient, they requested some information directed to them, both within passive materials (including online modalities) and communication with providers. Previous kidney transplant interventions have provided mutually shared content delivered through video,7,8,13 collaborative care model activities, 12 and patient ambassadors. 9 Most of these interventions increased caregivers’ knowledge; it is unclear whether any of the content was tailored to caregivers. Content helpful to caregivers suggested previously includes detailing caregiver role and responsibilities,2,20 self-care, 2 legal and financial considerations, 2 and how to acquire information related to resources. 19
In this study, caregivers described not feeling prepared for transplant complications. Nonpreparedness was attributed to insufficient information in passive materials and suboptimal communication with healthcare providers, particularly when complications occurred. Suboptimal flow of treatment information to caregivers engenders feelings of insecurity.20–22 Studies have highlighted the importance of healthcare workers with high communication and empathy skills 5 and optimizing patient/caregiver self-advocacy skills and communication styles. 2
Caregiver coping methods in our study included attitudes, taking time to do things they like to do, and receiving help from their social network to share caregiving duties and for informational and emotional support. The extent that these coping methods were described supports potential high utility of interventions aimed at maximizing benefit-finding, 23 promoting caregiver quality of life, 2 and mobilizing additional social supports. 2
Some caregiver participants described the value of the transplant center's Facebook support group and recommended promoting connection pathways to peer support that is separate for caregivers and patients. Support interventions for kidney transplant caregivers have generally involved both patients and caregivers together, except for a private Facebook group intervention solely for transplant caregivers. 14 Evidence suggests that these interventions have been satisfying to caregivers 10 and improved anxiety10,11 and support cognition,11,14 among other psychosocial outcomes.10,11
Limitations
The sample comprised caregivers of patients recruited from 1 transplant center, which could limit the generalizability of the results. This analysis was dominated by female spouses of older male patients. The spousal relationship may be protective of caregiver burden. 24 The number of non-White participants was small (although representative of the population), and all were English speaking. Although a more diverse sample may have provided a broader range of experience, few participants were needed to uncover core elements. Patients identified caregivers for study participation. Caregivers not identified for participation might have contributed different insights. However, the recruitment rate of 77% suggests high caregiver participation and interest in the topic. Findings could have been influenced by the unique health care experience encountered during the COVID-19 pandemic. The study relied on self-reported perception, which is a risk to receive socially desired answers. However, caregivers were purposefully interviewed after the transplant was received to reduce efforts by respondents to minimize fears or worries so as not to jeopardize patient transplant candidacy status, such as was found by other researchers. 25
Conclusion
Caregivers of kidney transplant recipients described a broad range of experiences, navigating the pre- and early post-transplant process. Efforts to engage caregivers in supporting patients through all phases of kidney transplant are needed. Future research should investigate the potential importance of content and delivery formats (print, video, in-person) that meet caregivers’ needs and should elicit suggestions for improving caregiver engagement through a range of interventions that extend beyond information, such as psychological/emotional needs, and health system and service needs. 22 Such efforts may include delivering information starting prior to evaluation, using different delivery modalities, featuring caregiver content prominently, providing caregiver-specific peer support, promoting social network support mobilization, and enhancing communication with both patients and caregivers. Effects of caregiver engagement—those events, behaviors, or conditions that follow engagement—remain unclear.
Footnotes
Acknowledgment
We thank medical writer Beth Dolph, PhD, for her assistance with manuscript preparation.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Dr Kayler and Dr Cadzow were supported by National Institute of Diabetes and Digestive and Kidney Diseases of the National Institutes of Health under award number R01DK129845-01. The funding organization played no role in the collection of data, analysis, interpretation, or the right to approve or disapprove publication of the finished manuscript.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
