Abstract
Treatment of chronic total occlusion (CTO) in the femoropopliteal segment remains technically challenging, and some CTO lesions may require distal puncture. The anterolateral popliteal puncture technique was reported in 2017 and has many advantages, including the ability to continue the procedure in the supine position. We investigated the anatomical Merkmal of anterolateral popliteal artery puncture and verified the efficacy of the Merkmal method by contrast-enhanced lower limb computed tomography (CT) at our hospital. We assumed that the popliteal artery would run along the medial margin of the fibular head when the medial margin of the fibular head and the tibia were in the most separated oblique position. On bone 3D CT images, we set a region of interest (ROI) over the expected course of the popliteal artery according to the Merkmal method. The primary endpoint was the hit rate, defined as the ratio of the area of the popliteal artery in the ROI on 3D CT divided by the area of the popliteal artery at the same level on contrast-enhanced CT. The secondary endpoints were the diameter of the popliteal artery, its distance from the skin, and the angle of obliquity. We retrospectively validated the Merkmal method in 108 limbs of 56 patients who underwent contrast-enhanced lower limb CT at our hospital. The hit rate was 66.5% (range, 39.8%-87.0%), the mean diameter of the popliteal artery was 4.6 ± 0.7 mm, the mean distance from the skin to the popliteal artery was 48.6 ± 4.8 mm, and the mean angle of lateral obliquity was 57.3 ± 12.0°. These findings indicate the potential of the Merkmal method to facilitate anterolateral popliteal puncture.
Clinical Impact
This anatomical Merkmal method may facilitate anterolateral popliteal puncture.
Introduction
Despite recent advances in the treatment of chronic total occlusion (CTO) in the femoropopliteal segment, including progressive wiring methods 1 and intravascular ultrasound-guided outcomes in the femoropopliteal segment CTO, 2 its treatment remains technically challenging. Some CTO lesions do not respond to progressive wiring and may require distal puncture. Various techniques have been reported for distal puncture, including distal superficial femoral artery (SFA) puncture from the anterior side, 3 popliteal artery puncture from the posterior side, 4 and foot lifted popliteal artery puncture. 5 The anterolateral popliteal puncture technique reported by Tan et al 6 has many advantages, including less risk of bleeding and the ability to continue the procedure in the supine position. Peripheral arterial disease (PAD) is an atherosclerotic disease that is associated with chronic kidney disease (CKD). In patients with CKD, distal puncture must have a high success rate and should be performed without repeated injections of contrast medium. To improve the accuracy of puncture, and thus the success rate of anterolateral popliteal artery puncture, it is useful to know the anatomical Merkmal of the popliteal artery. The aim of this study was to evaluate the anatomical Merkmal for anterolateral popliteal artery puncture and to retrospectively verify the efficacy of the anatomical Merkmal method, using contrast-enhanced lower limb computed tomography (CT).
Methods
We retrospectively validated the images of 56 patients who underwent contrast-enhanced lower limb CT at our hospital between January 2020 and July 2023. Imaging was obtained with a syngo.via CT system (Siemens, Bayern, Germany). The vessel diameter and the distance from the skin of the popliteal artery assumed to be punctured were evaluated. As anterolateral popliteal artery puncture is performed at the P3 level, 7 we measured vessel diameter and depth at the level of the fibular head on contrast-enhanced CT (Figure 1). No actual puncture was performed.
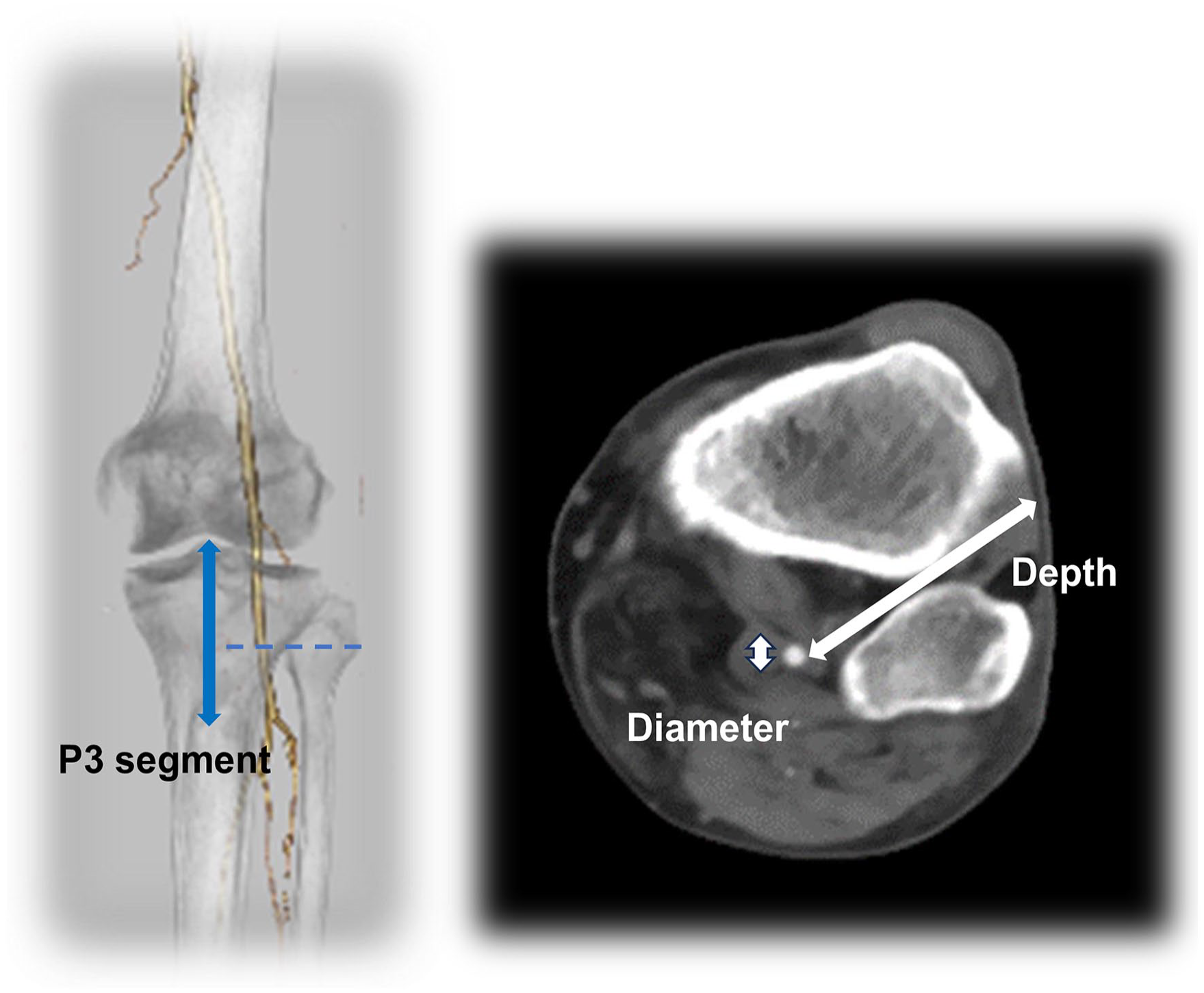
Diagrams showing measurements for secondary endpoints. The diameter of the popliteal artery and depth from the skin to the vessel at the level of the fibular head (blue dotted line) are shown.
Anatomical Merkmal Method
We assumed that the popliteal artery would run along the medial margin of the fibular head when the medial margin of the fibular head and the tibia were rotated to the greatest separation in the ipsilateral oblique position. We regarded this anatomical Merkmal as the site of puncture for the anterolateral popliteal puncture technique (Figure 2). After this position was achieved using a 3D CT image with bone windows, a 5.0 × 10 mm region of interest (ROI) (800 pixels) was set on the medial margin of the fibular head (Figure 3A), as the expected location of the popliteal artery.
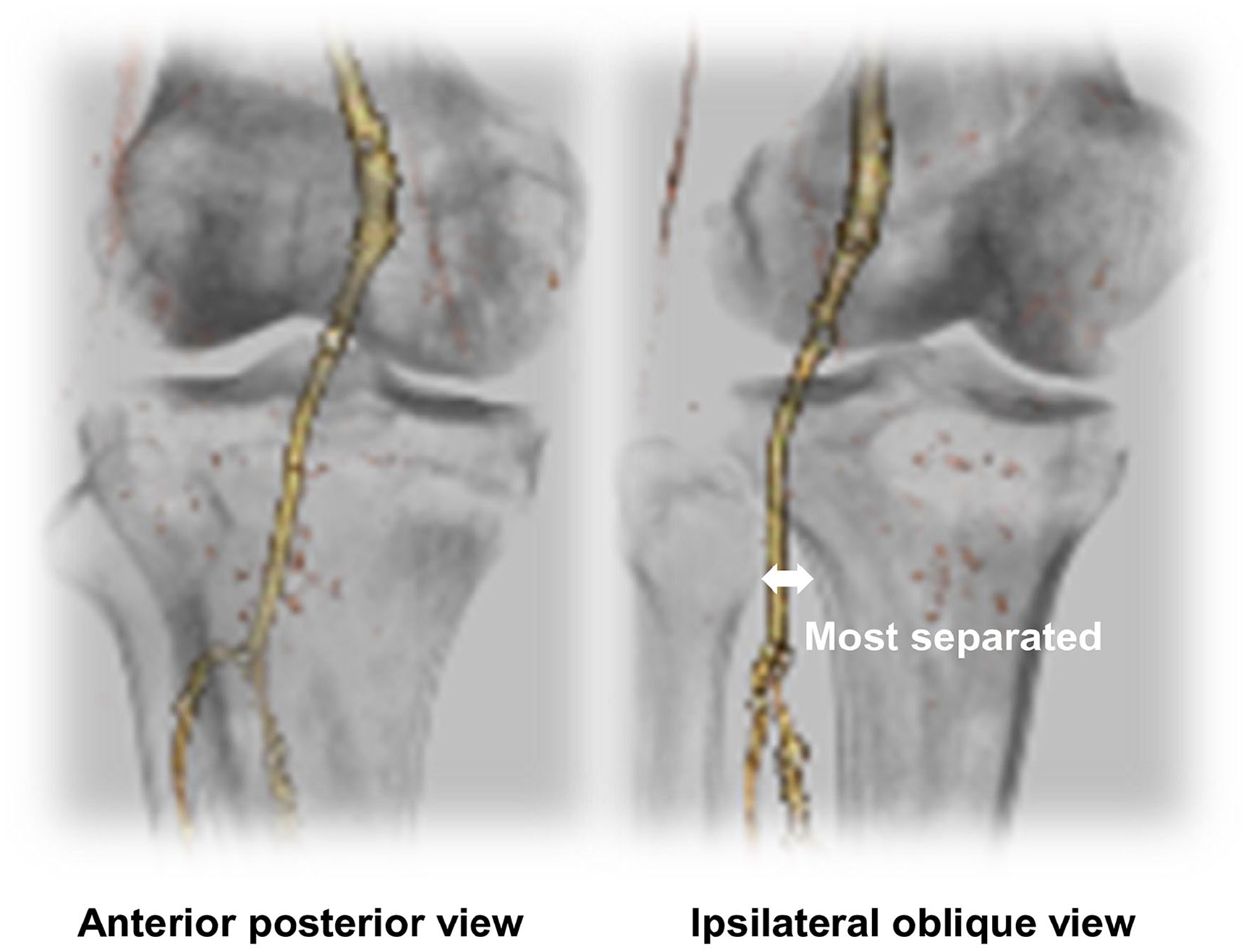
Positioning of the limb in the anatomical Merkmal method. In the ipsilateral oblique position where the medial margin of the fibular head and the tibia are most separated, the popliteal artery runs along the medial margin of the fibula.
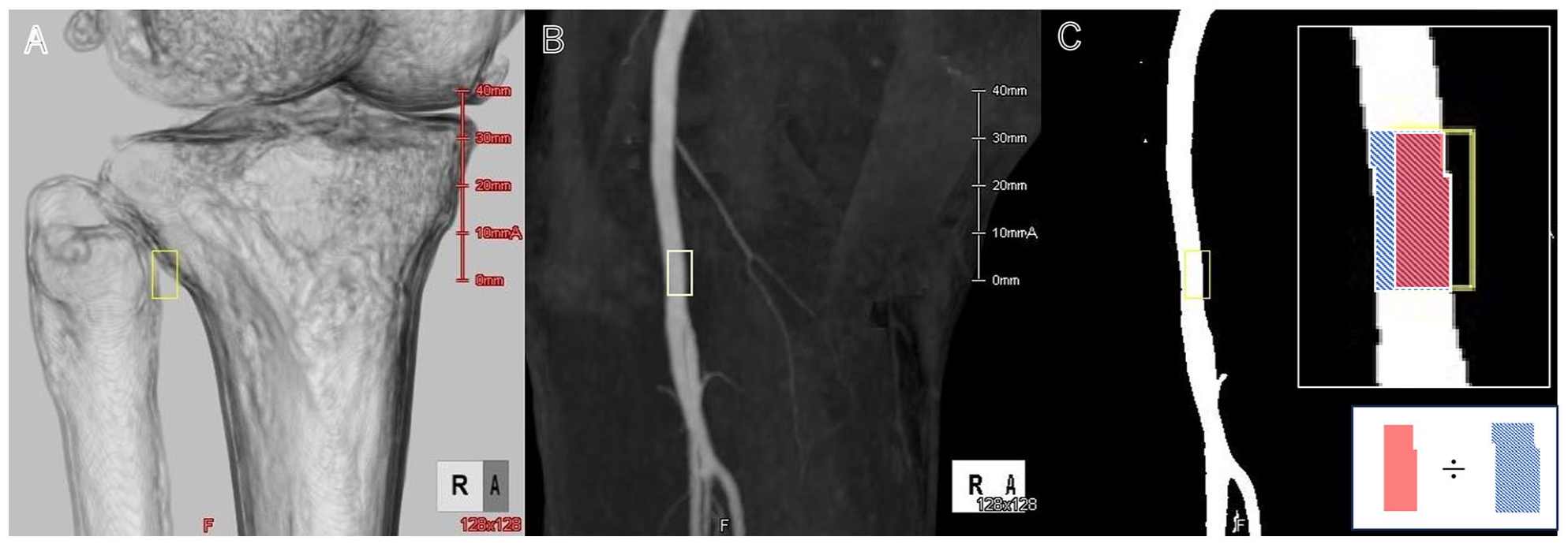
Calculation of hit rate. (A) 3D CT image displayed with bone windows is rotated to ipsilateral obliquity, and an ROI (5.0 × 10 mm) is placed on the medial margin of the fibular head. (B) The ROI placed in (A) is superimposed on a 3D CT angiogram. (C) The hit rate is calculated as the ratio of the number of pixels in the ROI placed on the rotated CT image to the number of pixels in the actual contrast-enhanced popliteal artery at the same level.
The primary endpoint was the hit rate of the Merkmal method, which was calculated as follows. The area of the ROI that was placed over the assumed location of the popliteal artery on the rotated CT image was converted to pixels and then divided by the number of pixels in the area of the popliteal artery on the 3D CT angiogram image at the same level (Figure 3C) was the hit rate. The secondary endpoints were the vascular diameter of the popliteal artery, its distance from the skin, and the angle of obliquity.
Ziostation2 (Ziosoft) was used to determine obliquity in the 3D CT image, and the ImageJ image processing software was used to convert the ROI area to pixels.
This study was approved by the ethics committee of this institution. The details of the study are published on the institution’s Web site, including a guarantee that research subjects and others had the opportunity to refuse to participate in the study. This study was registered with the University Hospital Medical Information Network Clinical Trial Registry (UMIN 000052461).
Statistical Analysis
All data were statistically analyzed using EZR (Saitama Medical Center, Jichi Medical University, Saitama, Japan), which is a graphical user interface for R (The R Foundation for Statistical Computing, Vienna, Austria) 8 . Categorical variables are presented as the n (%). Continuous variables are presented as the mean ± standard deviation if normally distributed according to a test of normality (Kolmogorov-Smirnov test) or as the median (interquartile range) if not normally distributed. Primary and secondary endpoints are presented as the mean ± standard deviation if normally distributed and as the median (interquartile range) if not normally distributed.
Results
Table 1 shows the backgrounds of patients who underwent contrast-enhanced lower limb CT. Many patients with PAD were complicated by atherosclerotic disease. Four limbs were excluded from the analysis because of popliteal artery occlusion in both lower limbs (in 1 patient) and popliteal artery occlusion in 1 limb (in 2 patients). Therefore, 108 limbs were analyzed in total. As secondary endpoints, the mean diameter of the popliteal artery at the level of the fibular head, assuming puncture, was 4.6 ± 0.7 mm, the mean depth from the skin to the popliteal artery was 48.6 ± 4.8 mm, and the mean angle of lateral obliquity set on the 3D-CT images was 57.3 ± 12.0° (Figure 4). As the primary endpoint, the hit rate for the popliteal artery with the Merkmal method was 66.5% (39.8%-87.0%) (Figure 5). Images of the 4 highest and lowest hit rates using the Merkmal method are shown in Figure 6A-D and Figure 6E-H, respectively.
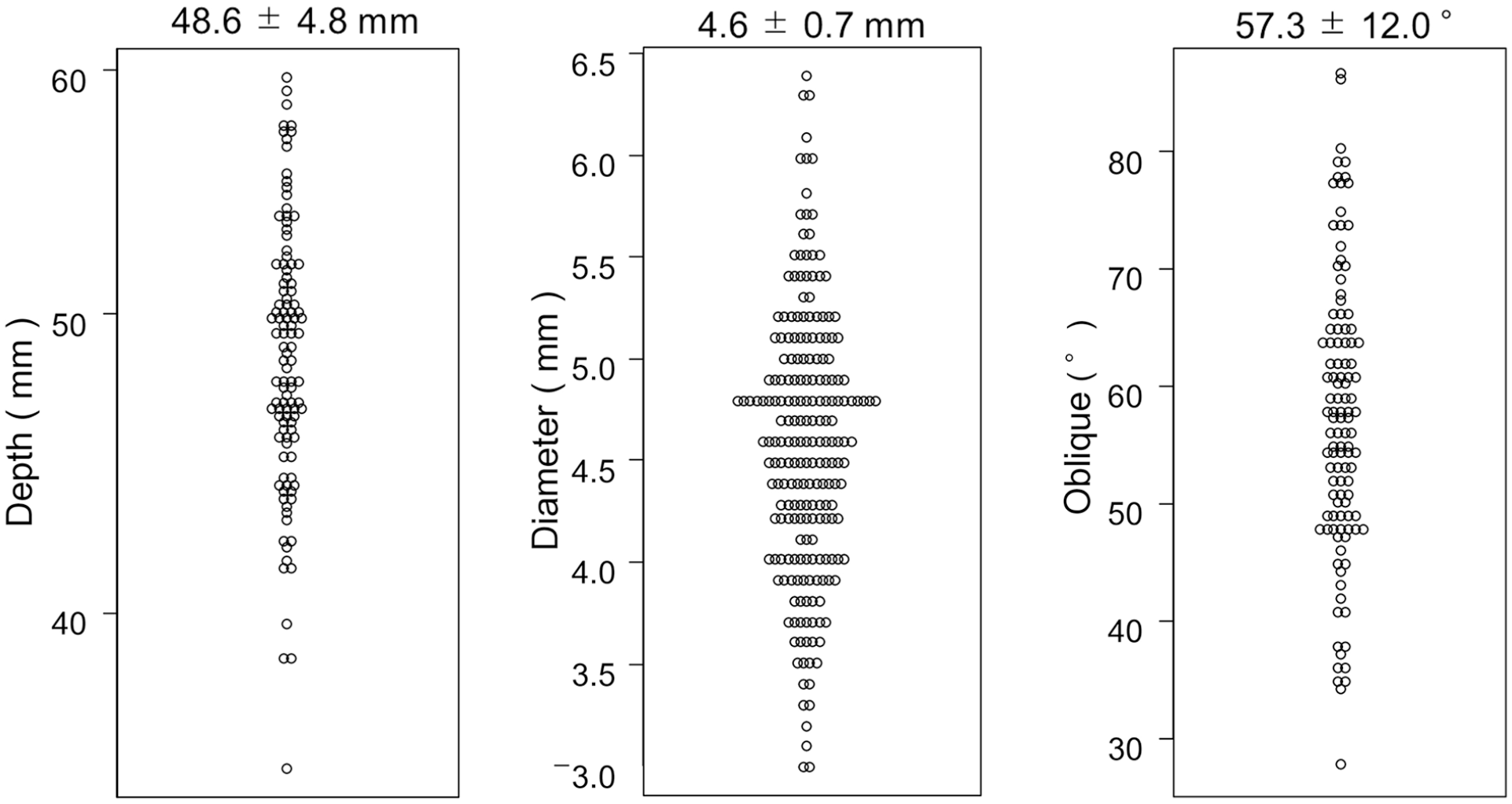
Secondary endpoints. Dot plots show the results of the vascular diameter of the popliteal artery, the distance of the artery from the skin, and the angle of obliquity.
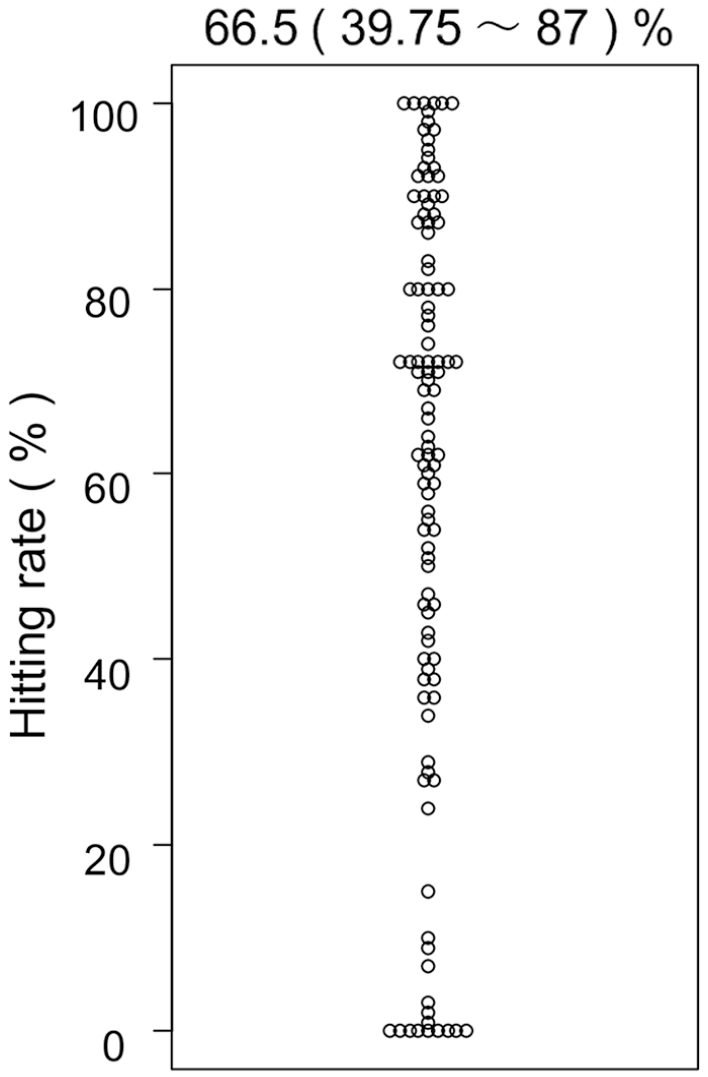
Primary endpoint. The dot plot shows the hit rate for each limb evaluated.
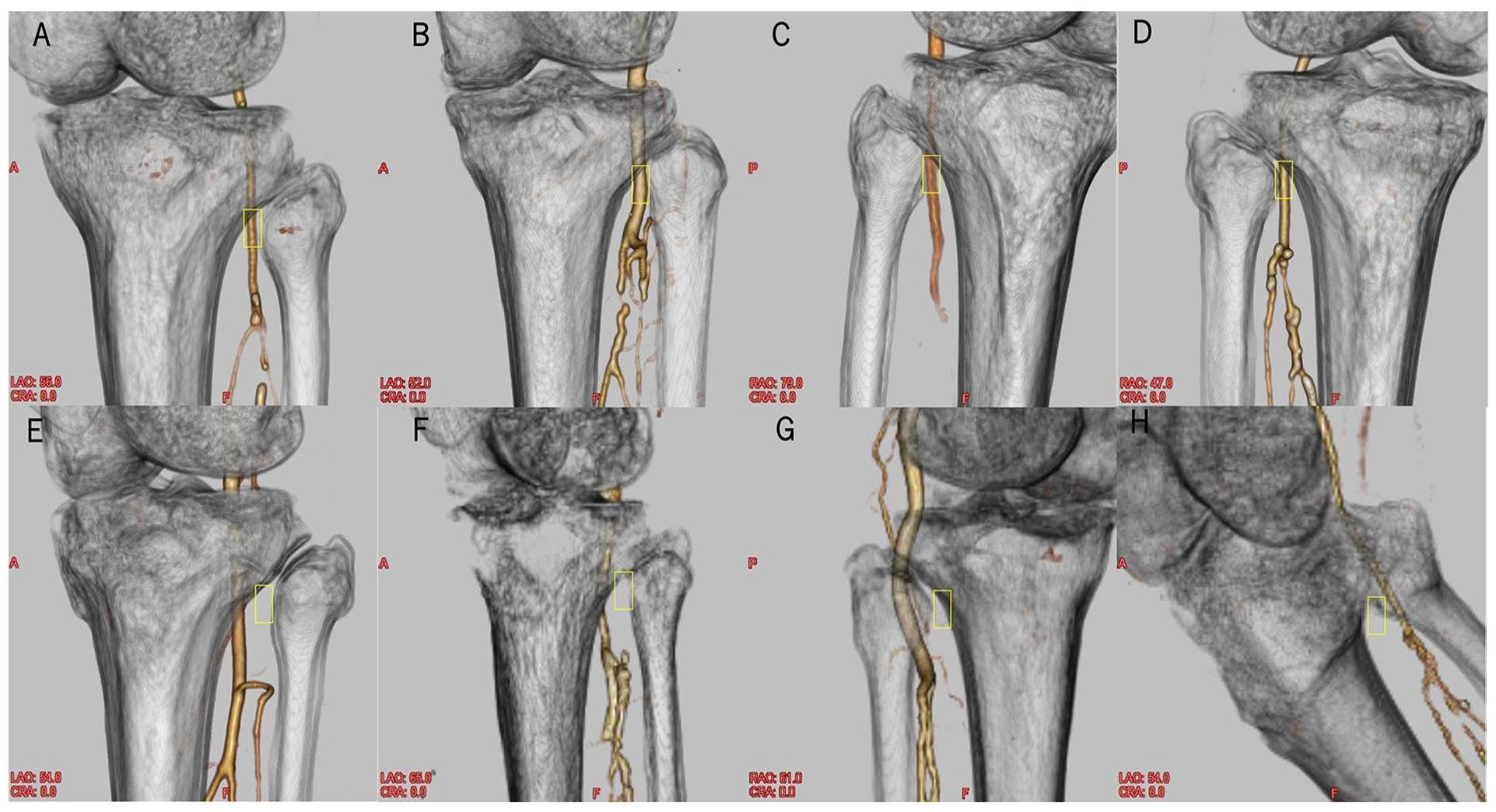
Four most hit and 4 most missed cases. Contrast-enhanced lower limb CT images of the 4 highest (A-D) and the 4 lowest (E-H) hit rates. (E) is of a male patient in his 60s with independent ADL. The ROI was positioned initially at the left anterior oblique (LAO) 54° using the Merkmal method. Contrast-enhanced CT revealed that the popliteal artery ran along the medial border of the fibula at LAO 66° (ie, error of 12° compared with the expected angle). (F) is of a bedridden with a history of stroke and atrophy of the lower limb muscles. The ROI was positioned initially at LAO 65°, but the popliteal artery actually ran along the medial border of the fibula at LAO 80° (error of 15°). (G) is of a late 80s with low ADL. The popliteal artery is snaking (error of 20°). (H) The patient had severe knee contractures and was unable to extend the lower limb during CT imaging, and it was difficult to perform the Merkmal method simply by changing the oblique position.
Patient Characteristics.
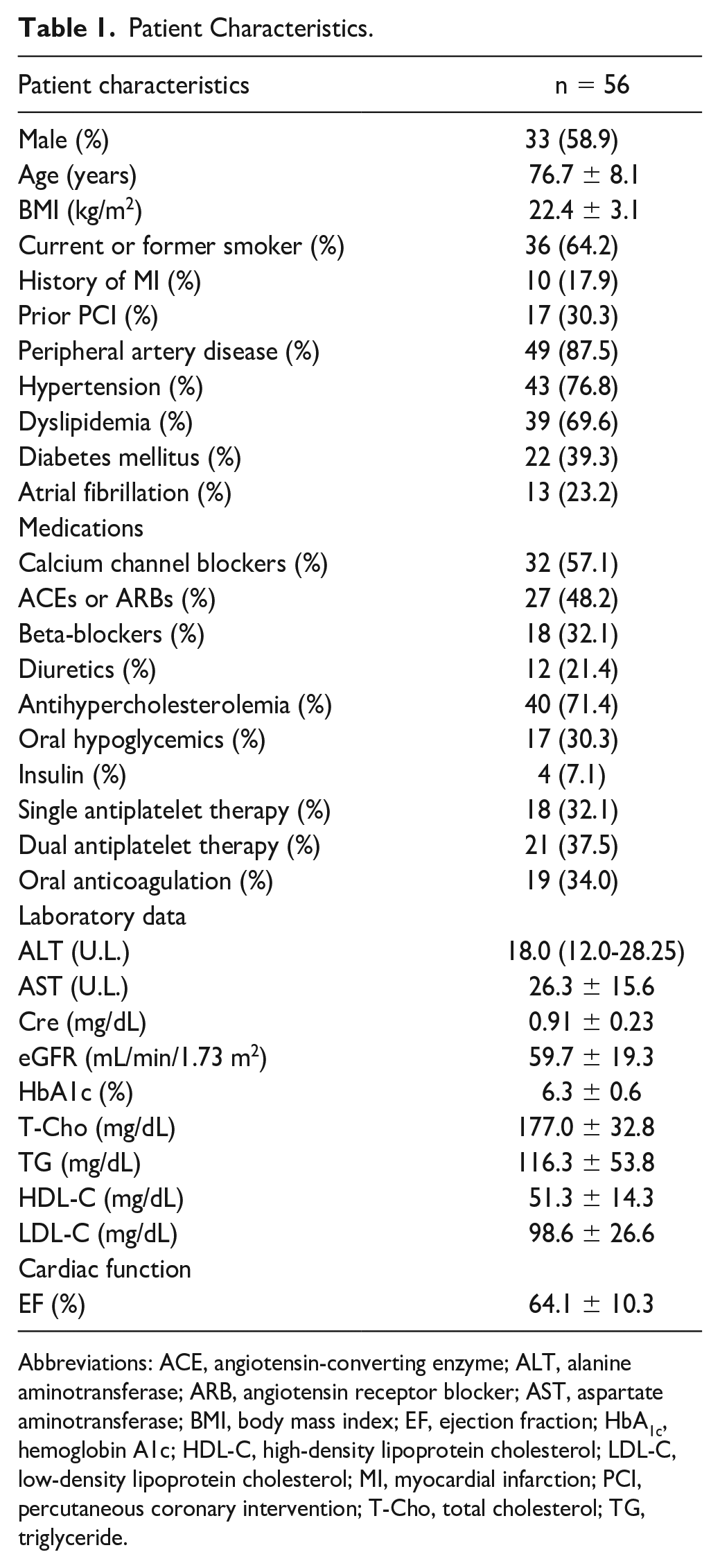
Abbreviations: ACE, angiotensin-converting enzyme; ALT, alanine aminotransferase; ARB, angiotensin receptor blocker; AST, aspartate aminotransferase; BMI, body mass index; EF, ejection fraction; HbA1c, hemoglobin A1c; HDL-C, high-density lipoprotein cholesterol; LDL-C, low-density lipoprotein cholesterol; MI, myocardial infarction; PCI, percutaneous coronary intervention; T-Cho, total cholesterol; TG, triglyceride.
Discussion
When the passage of a wire into the true lumen is unsuccessful in the antegrade approach for the treatment of CTO of the SFA, the retrograde approach is considered, for which various techniques have been proposed. In posterior popliteal artery puncture, 4 puncture is easy but requires the patient to be in the prone position, which is inconvenient. Proposed improvements include methods such as popliteal artery puncture while in the supine position with the leg in a squatting position 9 and popliteal artery puncture with the foot raised. 10 Schmidt et al 3 reported a retrograde approach technique by SFA puncture distal to the adductor canal in the supine position. However, this method can lead to the formation of pseudoaneurysms, and the distal SFA is difficult to compress because of its depth. Furthermore, in the event of bleeding, reserve space can be large because of the lack of structures such as ligaments to stop bleeding in the surrounding area, which can lead to the expansion of hematoma. The retrograde approach from the posterior tibial artery is also relatively shallow and can be punctured under ultrasound guidance. Furthermore, hemostasis is easy. However, training is required because the vessels are thin and superficial, which makes it easy for them to escape during puncture and may be difficult to puncture. In addition, the vessel may be too stenosis or obstructed to be used for the approach. Reentry devices such as the Outback catheter (Cordis, California, USA) have been developed for use in the antegrade approach, 11 but they can be difficult to manipulate if the iliac artery flexes strongly, and repeated contrast injection is required during reentry. Pioneer Plus (Philips, Amsterdam, the Netherlands) can reduce the use of contrast but can be as difficult to operate as Outback if the iliac artery is highly flexed. Tan et al 6 reported the efficacy and safety of the anterolateral popliteal puncture technique, which can be performed in the supine position and has fewer bleeding complications. The popliteal artery is more open than the posterior tibial and dorsal foot arteries in many cases and is easier to puncture due to its larger diameter. Because of these advantages, we often use this approach at our hospital. There are no data on complications or risks of the anatomical Merkmal method as no actual puncture was performed in this study.
Anatomical Merkmal methods of vascular puncture are well-known for central venous catheter placement (internal jugular vein and femoral vein) and axillary venipuncture for pacemaker implantation. Currently, most vascular punctures are performed under ultrasound guidance for safety reasons. In the case of anterolateral popliteal puncture, however, ultrasound-guided puncture is difficult because the target vessel is deep and the ultrasound beam may be obstructed by bone. Therefore, the anatomical Merkmal technique can enable the procedure to be performed quickly and accurately.
Design decisions regarding how best to evaluate the efficacy of the Merkmal method presented challenges. It was difficult to conduct a single-center study with a prospective 2-group comparison (ie, a group using Merkmal vs a group not using Merkmal) because of the small number of patients who undergo endovascular treatment at our hospital. We set a primary endpoint to enable quantitative assessment of the efficacy of the method, rather than conduct a subjective evaluation.
As we did not conduct a 2-arm comparative study, it is not possible to determine statistical effectiveness against the results for the primary endpoint (66.5% [39.8%-87.0%]). Therefore, opinion may be divided regarding the utility of the present anatomical Merkmal method. The size of the ROI was determined based on the vessel diameter of the popliteal artery at the secondary endpoint.
The popliteal artery hit rate using the Merkmal method was 66.5% (39.8%-87.0%), which is lower than we had expected in our initial observation of the bone 3D CT images. In addition, the hit rate was not normally distributed, possibly due to the population that had a hit rate of 0%. Images of the 4 lowest rates are shown in Figure 6E-H.
Figure 6E shows a man in his 60s with independent activities of daily living (ADL), while Figure 6F and g show an elderly patient in his late 80s with low ADL and atrophied lower limb muscles. Figure 6H was difficult to perform with the Merkmal method due to the severe contracture of the knee joint.
Atrophy of the lower limb muscles and deformity of the knee joint due to age and reduced ADL may have contributed to the reduced accuracy of the Merkmal method. Other patients with a hit rate of 0% (not shown in Figure 6) had a smaller oblique error than those shown in Figure 6E-H. We considered that the error could possibly be corrected by rotating the lower limb during the actual contrast injection and puncture.
Difficulties are occasionally experienced with anatomical Merkmal puncture during femoral and axillary vein puncture; similarly, failure of the anterolateral popliteal artery puncture technique by the anatomical Merkmal method used in this study is unavoidable in a certain number of patients.
The ultimate goal of the Merkmal method is to enable vessel puncture without the requirement for contrast injection; however, the anterolateral popliteal puncture technique is better performed with a combination of contrast injection and the present Merkmal method.
The angle of obliquity, a secondary endpoint, was large in some cases. In addition, the range of motion of the C-arm of the angiographic unit is limited but can be compensated for by internal rotation of the lower limb during the actual procedure.
When performing anterolateral popliteal puncture from the anterior aspect, the puncture must be made behind the tibia. From the anterior aspect, the popliteal artery runs deep and it is difficult to advance a long puncture needle deep into the back of the tibia. The anatomical Merkmal technique described in this study is performed in an oblique position with the tibia and fibula separated, so the needle rarely strikes the bone during puncture. This is an effective method when performing the procedure with single-plane angiography. Patients with PAD may have CKD insufficiency, which may necessitate performing the procedure with a minimum amount of contrast medium or by carbon dioxide angiography. If the course of the popliteal artery can be predicted in advance, the success rate of popliteal artery puncture will increase, thus contributing to minimizing the amount of contrast medium required for the procedure. In addition, our Merkmal method is considered useful because although carbon dioxide contrast results in poor images, the accuracy of the puncture is improved if the distance between the assumed location of the popliteal artery with the Merkmal method and the actual location confirmed with contrast medium is small.
Limitations
This study was a retrospective, single-arm analysis of a small number of patients. As it was not a 2-arm comparative study, its efficacy cannot be evaluated in terms of statistical significance.
Conclusion
The described anatomical Merkmal method may facilitate anterolateral popliteal puncture.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
