Abstract
Purpose:
To demonstrate the Modified Balloon Nose Cone Technique to avoid passage of the aortic valve in endovascular branched arch repair.
Technique:
The technique is demonstrated in a 54-year-old patient after previous open repair of the ascending aorta and mechanical aortic valve replacement due to type A aortic dissection. The delivery system of a custom-made stent-graft with 3 inner branches was modified by subtotally sawing off its nose cone. Using a right transaxillary access, a sheath was introduced over a through-and-through (TAT) wire exiting the left groin and meeting the branched stent-graft in a rendezvous fashion. A balloon was used to bridge the gap between both sheaths. Passing the innominate artery, both sheaths were pushed into the ascending aorta to establish a loop configuration of the balloon until the correct landing zone was reached. The main body was deployed, and the supra-aortic target vessels were connected. After the procedure, the mechanical aortic valve showed unimpaired function.
Conclusion:
The Modified Balloon Nose Cone Technique broadens the technical armamentarium in endovascular aortic arch repair offering a feasible solution to overcome the need of aortic valve passage. Especially patients with mechanical aortic valve could benefit from this method.
Clinical Impact
To describe the feasibility and safety of the Modified Balloon Nose Cone Technique in a severely comorbid patient with residual Type A aortic dissection and history of ascending aortic repair and mechanical replacement of the aortic valve to broaden the technical armamentarium in endovascular aortic arch repair offering a feasible solution to overcome the need of aortic valve passage.
Introduction
Endovascular aortic arch repair remains challenging and often requires passage of the aortic valve to allow for landing in zone 0 close to the coronary arteries. Aortic valve damage due to manipulation with stiff and rigid introducer systems is a feared complication, especially in patients with mechanical valve replacement.1,2 Few reports describe feasibility of mechanical valve passage,3,4 which is usually associated with use of big sheaths and difficult catheterization due to challenging anatomy and often small valve diameter. Aortic valve insufficiency due to sheath placement represents additional burden to the patient. Avoiding aortic valve passage with use of an alternative method helps to overcome these problems and limits the risk of complications. 5 We demonstrate the Modified Balloon Nose Cone Technique for branched arch repair in a multimorbid patient with a history of replacement of the ascending aorta and mechanical aortic valve repair due to type A aortic dissection and progression of the false lumen aneurysm.
Technique
The Modified Balloon Nose Cone Technique is demonstrated in a 54-year-old male patient with progressive, asymptomatic 54 mm thoracoabdominal false lumen aneurysm involving the aortic arch after previous open repair of the ascending aorta (in 1999) and mechanical aortic valve replacement (in 2002) due to type A aortic dissection (Figure 1). The patient was scheduled for elective treatment. He had a history of arterial hypertension and atrial fibrillation; his medication included antihypertensive treatment and warfarin.
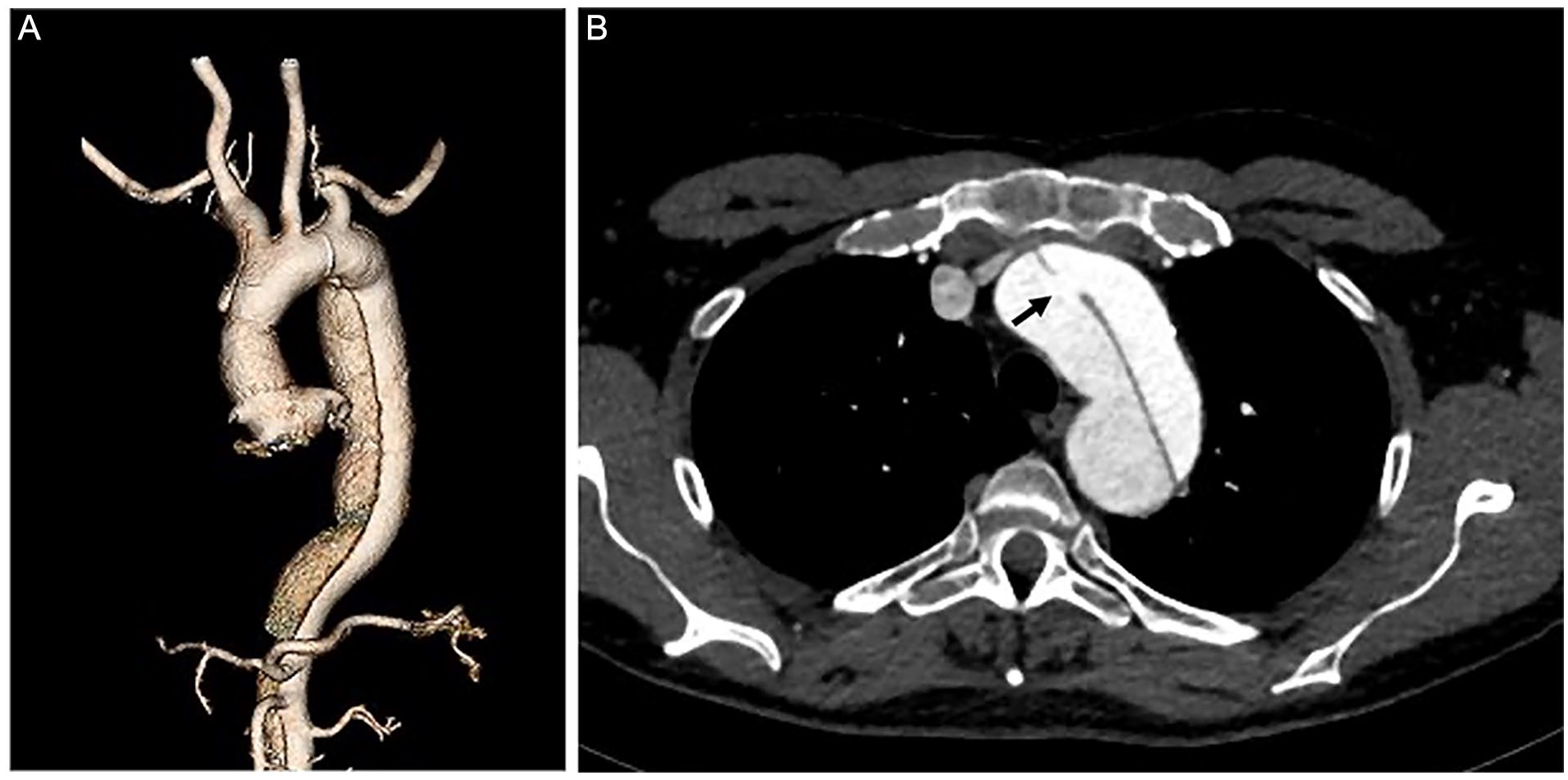
3D-volume-rendering (A) and axial computed tomography angiography (B) showing the residual type A aortic dissection with progressive false lumen aneurysm and large proximal entry tear at the level of the innominate artery (black arrow).
Considering the patient’s medical and surgical history as well as the anatomy, endovascular management was decided after discussion in an interdisciplinary board. To stage the procedure, endovascular distal extension with a branched thoracoabdominal stent-graft was planned as a second step.
Procedure and Technical Modification
Decision was made for a custom-made device with 3 inner branches, 2 antegrade branches for the innominate artery and the left common carotid artery, and a retrograde branch for the left subclavian artery (Cook Medical, Bloomington, Indiana) (Figure 2A). The main body was loaded into a precurved introducer system of 24F. The patient was in supine position under general anesthesia. Systemic heparinization at 100 IU/kg with a target activated clotting time between 250 and 350 seconds was obtained.
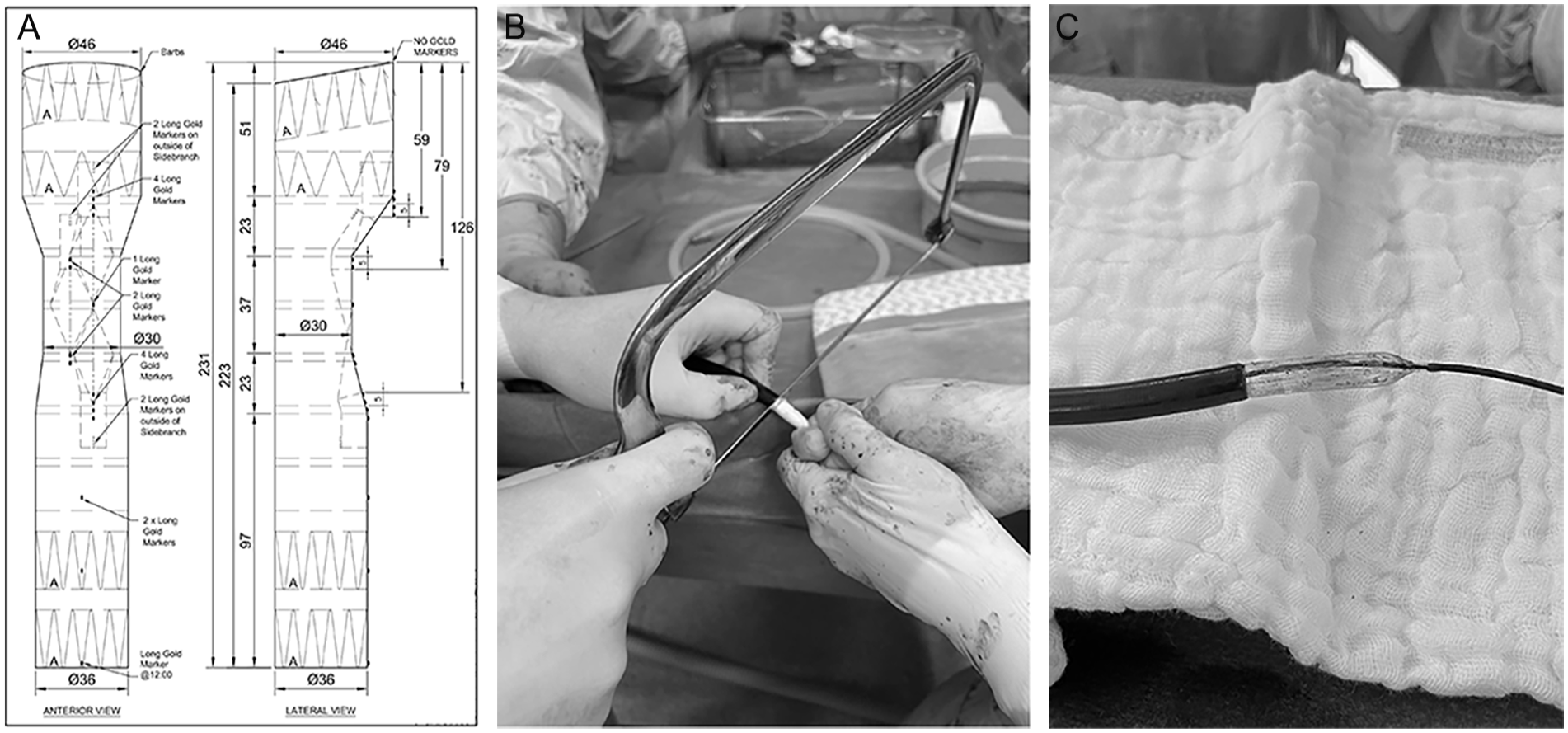
(A) Draft with anterior and lateral view of the custom-made inner branch device for the aortic arch with 2 antegrade branches for the innominate and left common carotid artery and a retrograde branch for the left subclavian artery. The device relied on the Zenith Platform (Cook Medical). Photograph of the (B) sawing-maneuver and (C) balloon, inserted into the 24-F sheath to function as a dilator tip after sawing the nose cone. The balloon is advanced transaxillary through an 8-F/90-cm sheath.
Access pathways were established through the left common femoral artery for the arch branch device, the right axillary artery and left common carotid artery for the supra-aortic bridging stent-grafts, using a cut-down approach for each site. Owing to severe kinking and dissection of the thoracoabdominal aorta, decision was made to use a right axillary-left femoral TAT-wire to advance the graft.
To avoid crossing of the mechanical valve, back-table modification by subtotally sawing the nose cone was performed (Figure 2B). The remaining part of the nose cone was intentionally preserved to secure the inner cannula after deployment. A 9/40-mm balloon catheter (Cordis Medical GmbH) was introduced through an 8-F/90-cm sheath (Cook Medical) from the right axillary artery over the TAT-wire exiting the left groin and meeting the branched stent-graft in a rendezvous fashion. The balloon was inflated, partially entering the 24-F sheath mirroring the nose cone (Figure 2C). Afterwards, the gap between the 2 sheaths was closed, and the whole connected system (8F sheath, balloon, 24F sheath) was secured by 2 clamps on the wire at the end of each sheath. The introduction of the system to the femoral artery was performed by pulling of the 8-F sheath from transaxillary. (While) Entering the femoral artery, the balloon was deflated first and inflated again to mimic the characteristics of a dilator, enlarging the access hole to the required diameter of the 24-F sheath (Figure 3A). The hole system was advanced to the level of the innominate artery (Figure 3B); from this point, the system was pushed from the femoral site to allow formation of a balloon loop and then pushed from both sites to be advanced to the indicated landing zone (Figure 3C).
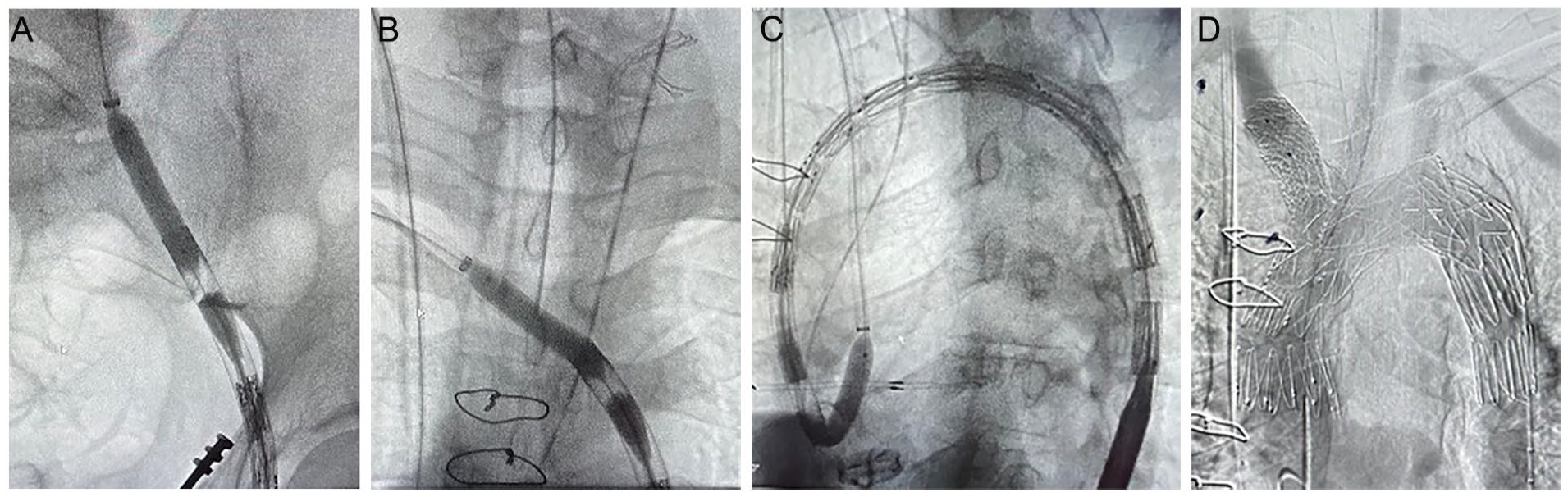
Fluoroscopy demonstrating the 8-F sheath (white arrow) and the 9/40-mm balloon partially inserted into the 24-F sheath (black arrow) of the main body at the iliac level after introduction into the vascular system (A) and after advancement to the level of the innominate artery (B). From that point, the system is looped and pushed into the ascending aorta to position the main body at the correct proximal landing zone (C). (D) Completion angiography confirmed aneurysm exclusion, with target vessel patency and without endoleak.
The final positioning of the graft was done under angiographic control. The balloon was now deflated and covered by the 8-F sheath to avoid entanglement of the balloon and the barbs of the main body. The main body was deployed in a regular fashion using rapid pacing for cardiac output reduction. After correct deployment of the branched arch graft, the TAT-wire and the balloon were removed over the 8-F sheath, and the sheath was retracted into the innominate artery. The supra-aortic target vessels were connected, innominate artery via right axillary approach: 18/73 mm Thoracic Extension (Cook Medical) and Begraft Aortic 24/37 mm (Bentley InnoMed, Hechingen, Germany), left common carotid artery via cut down: Begraft plus 10/57 mm and Begraft Aortic 14/38 mm (Bentley InnoMed), and retrograde branch for the left subclavian artery transfemorally: Begraft plus 10/57 mm (Bentley InnoMed). After completion and adequate selective angiogram, the left common carotid artery and right axillary artery were closed immediately with Prolene 6-0 sutures. Final angiogram confirmed good apposition of the graft and adequate perfusion of the supra-aortic vessels without endoleak (Figure 3D). A distal thoracoabdominal extension was planned in a next stage to reduce the risk of spinal cord ischemia. The mechanical aortic valve showed unimpaired function as any manipulation was avoided using the described technique. The remaining sheath and wires were retrieved under fluoroscopy, and the left common femoral artery was closed using Prolene 5-0 sutures. The patient was extubated and transferred for 48 hours to the intensive care unit. He remained hemodynamically and neurologically stable. The patient was discharged on the 9th post-operative day on anticoagulation with warfarin and antiaggregation with clopidogrel.
Discussion
We demonstrate the feasibility and safety of the Modified Balloon Nose Cone Technique avoiding aortic valve crossing in a severely-comorbid patient with residual type A aortic dissection and history of ascending aortic replacement and mechanical replacement of the aortic valve. 2 Endovascular techniques involving the ascending aorta and aortic arch are more and more established as a treatment strategy in selected group of patients, especially those ones in need for re-do procedures or unfit for open repair. 6 Many stent-grafts intended to land in zone zero require passage of the aortic valve for placement of a stiff wire inside the left ventricle. Ahead of deployment, big sheaths of the stent-graft delivery system often need to be advanced through the aortic valve, causing acute aortic insufficiency. Even special configuration of the delivering system with shortened nose cone lengths cannot avoid this problem in landing zones close to the aortic root. In addition, reflecting vulnerable structures, manipulation in this area can lead to feared complications such as valve injury or ventricular perforation. This might apply even more for patients with mechanical aortic valve. Despite some reports showing the feasibility of crossing the mechanical valve,1,3 avoiding valve passage in general appears to be less aggressive and more likely to prevent the potential complications. In addition, in severely-kinked aorta and aortic dissection, stable positioning of the stiff wire in the left ventricle and even loss of the wire can occur during advancement of the stent-graft system. The reported technique reflects an alternative pathway to overcome these problems.
Another aspect that could be avoided is delay of the procedure due to difficult valve catheterization, especially in patients after valve replacement with small diameter of the valve. This could be associated with additional need of radiation, procedural lengths, use of materials, and contrast medium.
During back-table modification, the first step is to retract the sheath until the nose cone is subtotally uncovered. To prevent potential trauma during deployment of the stent-graft, the inner cannula should be secured by preserving the end portion of the nose cone during sawing. A Liston cutter might be needed to cut the inner cannula, which should be protected by a 0.035 stiff wire to avoid squeezing of the central lumen. The 8-F sheath and, afterwards, the 40-mm balloon catheter are inserted over the 400-cm TAT-wire from right axillary approach and should be chosen in adequate lengths to allow for externalization at the common femoral artery level. This is needed to prepare the transfemoral introduction of the stent-graft system, which is loaded onto the wire from below to meet the balloon. Afterwards, the remaining nose cone part is retracted into the sheath to accommodate about a quarter of the lengths of the balloon. The diameter of the balloon should be chosen according to the outer diameter of the delivery system; in our patient, we used a 9/40-mm balloon for 24-F (9.1-mm outer diameter).
Possible limitations of the method are calcified supra-aortic vessels due to higher risk of cerebral embolization and unsuitable anatomy. In addition, pushing the system in the ascending aorta with a balloon in front may be associated with a potential risk of damage and injury to the aortic wall; this is less likely in patients after surgical ascending repair. Nevertheless, the Modified Balloon Nose Cone Technique offers a feasible solution to avoid crossing of the aortic valve in endovascular arch repair.
Conclusion
The Modified Balloon Nose Cone Technique broadens the technical armamentarium in endovascular aortic arch repair, offering a feasible solution to overcome the need of aortic valve passage. Especially patients with mechanical aortic valve could benefit from this method.
Footnotes
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: P.K. is a consultant and proctor for and has intellectual property with Cook Medical as well receives speaking fees and research, travel, and educational grants from Cook Medical and Bentley InnoMed. F.R. receives speaking, travel, and educational fees from Cook Medical. All authors declare no support from any organization for the submitted work; no financial relationships with any organizations that might have an interest in the submitted work; and no other relationships or activities that could appear to have influenced the submitted work.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
