Abstract
The high prevalence of sexually transmitted infections (STIs) in the Northwest Territories (NWT), Canada underscores the need for culturally relevant, community-driven sexual health initiatives for HIV and STI prevention that prioritize youth engagement and Indigenous leadership. FOXY (Fostering Open eXpression among Youth), a Northern and Indigenous NWT-based community-based organization, conducted 1-week youth Peer Leader Retreats (PLRs) focused on HIV prevention and leadership using land- and arts-based approaches. We conducted a one-group pretest/posttest with youth PLR participants aged 13 to 17 in the NWT and combined the data across PLRs conducted from 2020 to 2022. Assessments were completed at preretreat baseline, immediately postretreat, and at 6-month follow-up to measure changes in study outcomes (safer sex self-efficacy [SSSE], condom use self-efficacy [CUSE], and HIV knowledge). Of n = 133 participants at baseline, 6-month follow-up data were available for n = 122 (92%) participants. Multivariate analyses showed significant improvements in all study outcomes from baseline to 6-month follow-up. SSSE, CUSE, and HIV knowledge scores increased postretreat and continued to improve at 6 months. These findings suggest that culturally relevant, community-driven peer leadership interventions hold promise in advancing HIV prevention cascade outcomes with Northern and Indigenous youth in the NWT.
Keywords
In Canada’s Northwest Territories (NWT), sexually transmitted infection (STI) rates are seven times higher than the national average, disproportionately affecting youth aged 15–24 years. The territorial rate of new human immunodeficiency virus (HIV) diagnoses is 1.5 per 100,000 population (Public Health Agency of Canada, 2023). STI diagnoses are closely linked to increased risk of HIV transmission, driven by elevated viral concentration in the genital tract, increased blood HIV concentration, and behavioral risks (Cohen et al., 2019). These risks underline the need for multilevel prevention strategies that align with the HIV prevention cascade, a framework that identifies three steps in reducing HIV transmission in a priority population: motivation (e.g., knowledge, consequences of use), access (e.g., availability, affordability), and effective use (e.g., skills, self-efficacy, partner dynamics) of a prevention method (Hargreaves et al., 2016; Moorhouse et al., 2019). Interventions targeting motivation (e.g., HIV/STI knowledge) and effective use (e.g., confidence in condom negotiation and use) are critical for moving youth along the HIV prevention cascade, especially in under-resourced and high STI prevalence settings such as the NWT (Lys et al., 2016). Prior research shows that safer sex self-efficacy (SSSE) (defined broadly as one’s ability to navigate sexual decision-making and contraception use, and have pleasurable sex) and condom use self-efficacy (CUSE) (a multidimensional construct that includes one’s ability to successfully obtain, negotiate, and use condoms consistently and correctly) are associated with increased uptake of condom use and other preventive practices (Logie, Lys, Mackay, et al., 2019; Logie, Lys, Okumu, & Fujioka, 2019).
Indigenous peoples, who account for nearly half (49.6%) of the NWT population and 5% of Canada’s total population, experience higher STI prevalence than non-Indigenous persons in the NWT (49.9 cases per 1000 vs. 6.6). Indigenous people are also disproportionately affected by HIV, with 18.2% of new HIV infections in Canada occurring among Indigenous peoples in 2020 (Public Health Agency of Canada, 2023). These disparities are shaped by social and health inequities caused by historical and ongoing colonialism (Logie, Lys, Okumu, & Fujioka, 2019). However, a recent resurgence of Indigenous ways of knowing as central to health promotion can be seen in literature on the health and well-being of Indigenous youth (Landy & Worthington, 2021; Lys, 2018). Land-based teachings, which emphasize learning through traditional activities such as hunting, gathering, and fishing (Streit & Mason, 2017), have been shown to strengthen connections to community, culture, and self (Gittings et al., 2022). In addition, guidance from Indigenous Elders plays a crucial role in fostering empowerment and resilience among Indigenous youth. Similarly, arts-based approaches such as visual media, theater, painting, and song have been integrated into HIV prevention and sexual health education (Flicker et al., 2020; Landy & Worthington, 2021; Lys, 2018; Lys et al., 2018), promoting leadership, self-confidence, and social connectedness (Gittings et al., 2022).
FOXY (Fostering Open eXpression among Youth) is a Northern and Indigenous program in the NWT developed for young women, and its partner program SMASH (Strength, Masculinities, and Sexual Health), developed for young men, hold annual Peer Leader Retreats (PLRs) for Northern and Indigenous youth to promote sexual health, leadership, and mental well-being within a culturally relevant and inclusive setting. While these approaches have shown effectiveness in improving indicators of HIV/STI prevention motivation and effective use among youth (e.g., increased HIV and STI knowledge, increased condom use efficacy) (Logie et al., 2024; Lys et al., 2023; Lys et al., 2018), there remains a gap in understanding long-term impacts. To address this gap, this study aimed to evaluate the research question: what changes in HIV knowledge, safer sex efficacy, and condom use efficacy are observed following PLR participation among Northern and Indigenous youth in the NWT aged 13-17?
Materials and Methods
Study Design and Setting
We conducted a single-group pretest–posttest intervention study with NWT youth aged 13 to 17 years who participated in a land- and arts-based sexual health PLR between 2020 and 2022. Data were collected at three timepoints: preretreat baseline, immediately postretreat, and at a 6-month follow-up. This study received ethics approval from the Research Ethics Board of the University of Toronto and the Aurora Research Institute.
Participants
Between September 2020 and May 2022, FOXY/SMASH project staff recruited participants from high schools in 17 communities across the NWT (Aklavik, Whati, Fort McPherson, N’Dilo, Lutselk’e, Fort Liard, Fort Simpson, Yellowknife, Ulukhaktok, Fort Resolution, Behchoko, Inuvik, Tuktoyaktuk, Hay River, K’atl’odeeche First Nation, Fort Smith, and Norman Wells). A convenience sampling approach was used, involving recruitment through school volunteers, school outreach efforts, and peer referrals. To be eligible for the PLR, youth needed to meet the following criteria: reside in the NWT; express a willingness to engage in FOXY/SMASH workshops; be between the ages of 13 and 17 years; receive parental consent; and provide informed assent.
Intervention
Participants attended a 9-day, gender-inclusive PLR at a fly-in lodge in the NWT. PLRs provide youth with the opportunity to expand their understanding of sexual and mental health, while also promoting healthy relationships through land- and arts-based activities. These include recreational activities (e.g., swimming, hiking), traditional Northern games, Elder teachings, sharing and grief circles, traditional hand drumming, beading, digital storytelling, and body mapping (Gittings et al., 2022; Logie et al., 2024). A more detailed description of the PLR intervention is available elsewhere (Lys et al., 2016).
Measurement
HIV prevention cascade indicators of motivation (HIV knowledge) and effective use (CUSE, SSSE) were assessed as primary outcomes. CUSE (Cronbach alpha = 0.902) was measured to assess participants’ confidence in correctly and consistently using condoms, while SSSE (Cronbach alpha = 0.887) assessed their confidence in practicing safe sex across various situations.
Both the CUSE and the SSSE scales used five-item Likert-type responses, with total scores ranging from 5 to 20. Higher scores on each scale reflect greater self-efficacy in condom use and safer sex practices, respectively. HIV knowledge was measured using the 18-item HIV Knowledge Questionnaire, with total scores ranging from 0 to 18; higher scores indicate greater HIV knowledge (Cronbach alpha = 0.893). We conducted stratified analysis by gender (cisgender women and cisgender men), sexual orientation (heterosexual and sexually diverse), and ethnicity (Indigenous and non-Indigenous).
Statistical Analysis
The primary analysis comparing the retreat attendee at the three-assessment time points was conducted by a population average model using generalized estimating equations (GEE). For each outcome of interest, we used an unstructured correlation matrix to estimate the intervention effect across time while adjusting for potential confounding factors (age, gender, PLR attendance, and baseline outcome scores), with robust standard errors to account for clustering. To specify a GEE model, we used a Gaussian distribution and an identity link function for all response variables. Intervention effects are expressed as crude (β) and adjusted coefficients (aβ), along with 95% confidence intervals (CIs). Analyses were conducted using complete case analysis, with two-tailed tests of significance and a significance level of α = 0.05. Stata 14.2 (StataCorp, College Station, TX) was used for data analysis.
Results
Participant Characteristics
A total of 133 FOXY/SMASH participants attended a PLR between 2020 and 2022 and provided baseline data. Of these, all 133 participants completed the postretreat survey and 122 (92%) completed the 6-month follow-up survey (Figure 1). Among participants, 60.9% identified as cisgender young women (n = 81), 34.6% (n = 46) as cisgender young men, and 4.5% (n = 6) as gender diverse. The mean age of participants was 14.8 years (SD = 1.5), with no significant difference by gender (p = 0.63). Over half of all participants identified as heterosexual (n = 84, 63.2%), while 36.8% (n = 49) reported a sexually diverse orientation, with no significant variation by gender (p = 0.16). Regarding ethnicity, 57.9% (n = 77) of participants were Indigenous and 42.1% (n = 56) were non-Indigenous, with a higher proportion of Indigenous participants among cisgender young men compared to cisgender young women, though this difference was not statistically significant (p = 0.067). In addition, 52.3% (n = 69) of participants were first-time PLR attendees, while 28.0% (n = 37) attended once before, 9.1% (n = 12) twice before, and 10.6% (n = 14) three or more times before, with no significant gender differences in participation frequency (p = 0.258).
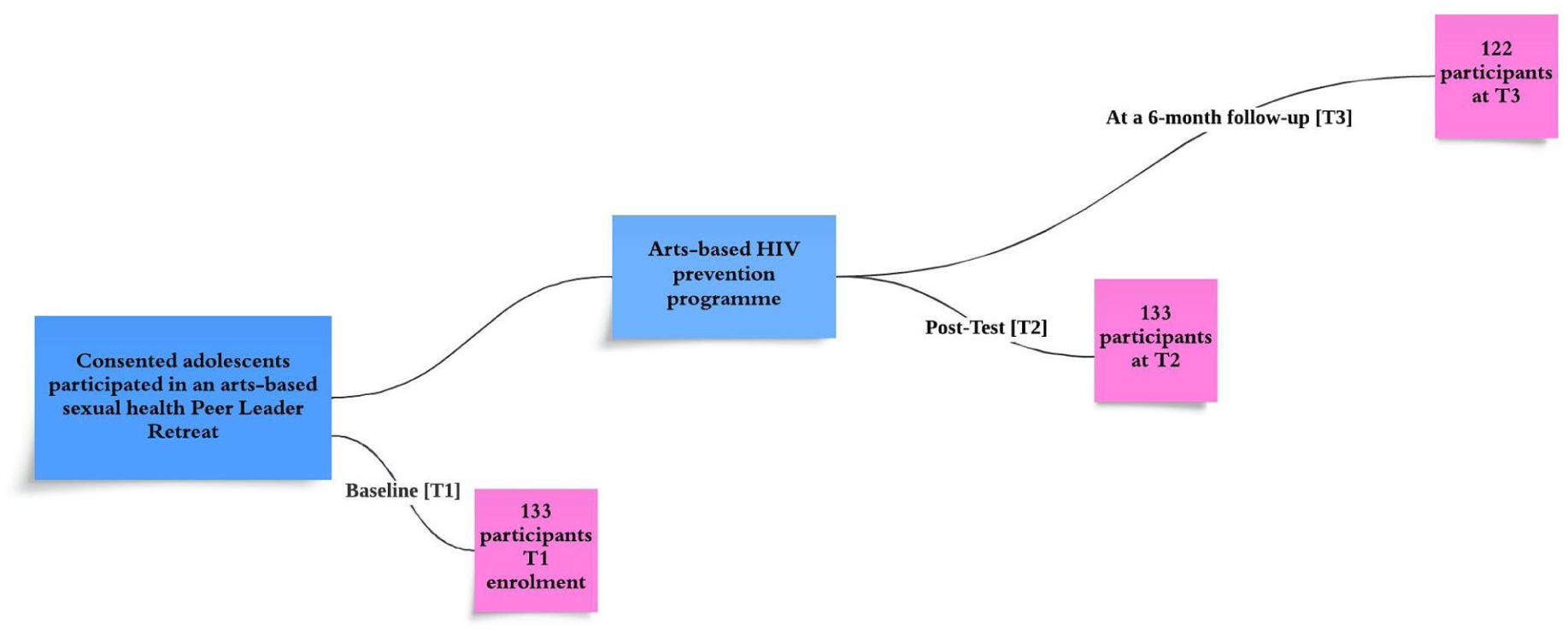
Flowchart of Participation in Land- and Arts-Based Sexual Health Peer Leader Retreats (PLRs) for HIV Prevention Among Northern and Indigenous Youth in the Northwest Territories, Canada (2020–2022)
Primary Outcome
After adjusting for age, gender, PLR attendance, and baseline outcome scores, significant improvements were observed in HIV prevention outcomes among participants after attending the PLR. We documented a notable increase in SSSE (aβ = 1.88; 95% CI: 0.99, 2.76; p < 0.001) and CUSE scores (aβ = .89; 95% CI: 0.26, 1.51; p = 0.005) postretreat. Similarly, participants at the 6-month follow-up demonstrated significant improvements in SSSE (aβ = 2.81; 95% CI: 1.73, 3.90; p < 0.001) and CUSE (aβ = 1.30; 95% CI: 0.58, 2.01; p < 0.001) (Table 1).
Effectiveness of PLRs in Improving HIV Prevention Outcomes Among Northern and Indigenous Participants in the NWT, Canada Between 2020 and 2022.
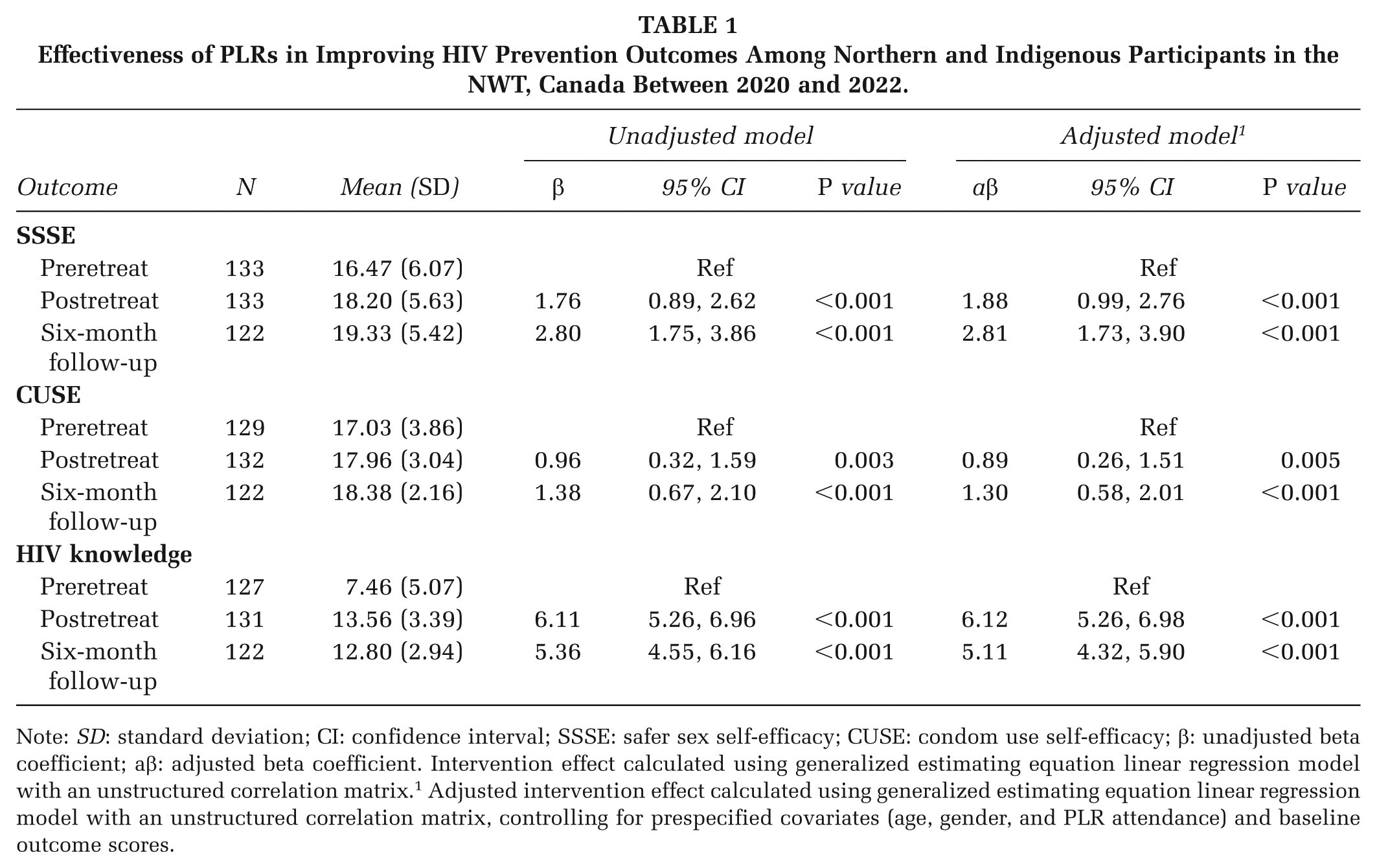
Note: SD: standard deviation; CI: confidence interval; SSSE: safer sex self-efficacy; CUSE: condom use self-efficacy; β: unadjusted beta coefficient; aβ: adjusted beta coefficient. Intervention effect calculated using generalized estimating equation linear regression model with an unstructured correlation matrix.1 Adjusted intervention effect calculated using generalized estimating equation linear regression model with an unstructured correlation matrix, controlling for prespecified covariates (age, gender, and PLR attendance) and baseline outcome scores.
The stratified analyses revealed a significant improvement in SSSE scores over time across gender, sexual orientation, and ethnicity at both time points, though young men (aβ = 0.79; 95% CI: −0.53, 2.11; p = 0. 241) and non-Indigenous participants (aβ = 0.91; 95% CI: −0.18, 1.99; p = 0.100) did not show a significant change postretreat or at the 6-month follow-up.
Similarly, significant improvements were consistent across gender, sexual orientation, and ethnicity for CUSE at both time points. However, these improvements were not significant among young men postretreat (aβ = 0.23; 95% CI: −0.80, 1.27; p = 0.659) or at the 6-month follow-up (aβ = 0.69; 95% CI: −0.51, 1.89; p = 0.260), nor among sexually diverse participants postretreat (aβ = 0.53; 95% CI: −0.30, 1.37; p = 0.543). Similarly, non-Indigenous participants showed no significant improvements postretreat (aβ = 0.50; 95% CI: −0.29, 1.30; p = 0.218) or at the 6-month follow-up (aβ = 0.76; 95% CI: −0.30, 1.82; p = 0.160) (Table 2).
Stratified Analysis of the Effectiveness of PLRs in Improving HIV Prevention Outcomes Among Northern and Indigenous Participants in the NWT, Canada Between 2020 and 2022
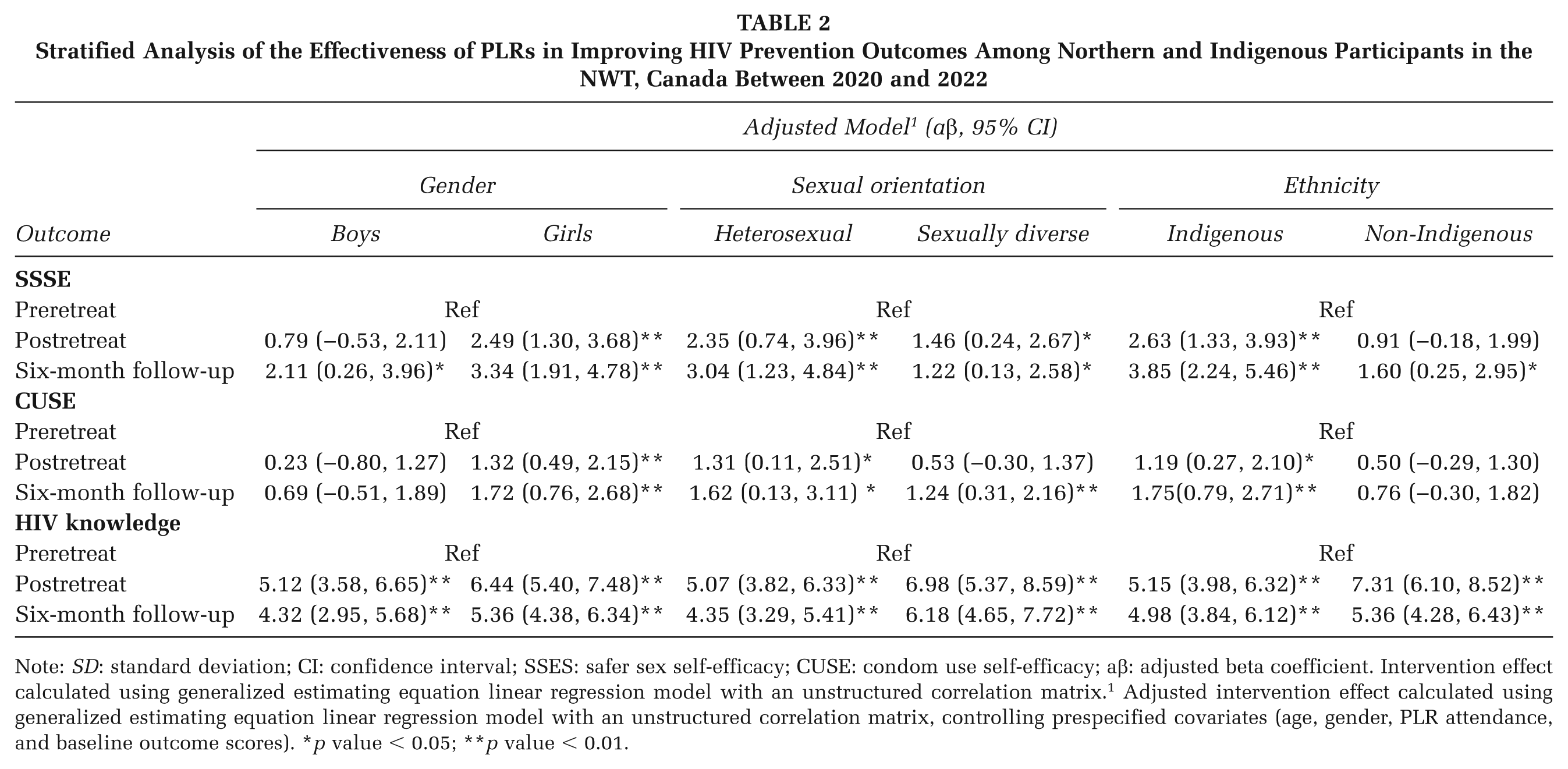
Note: SD: standard deviation; CI: confidence interval; SSES: safer sex self-efficacy; CUSE: condom use self-efficacy; aβ: adjusted beta coefficient. Intervention effect calculated using generalized estimating equation linear regression model with an unstructured correlation matrix.1 Adjusted intervention effect calculated using generalized estimating equation linear regression model with an unstructured correlation matrix, controlling prespecified covariates (age, gender, PLR attendance, and baseline outcome scores). *p value < 0.05; **p value < 0.01.
Multivariate analysis indicated a substantial improvement in HIV knowledge scores across assessment time points, with a six-fold increase postretreat compared to baseline (aβ = 6.12; 95% CI: 5.26, 6.98; p < 0.001) and more than a five-fold increase at the 6-month follow-up (aβ = 5.11; 95% CI: 4.32, 5.90; p < 0.001) (Table 1). The improvement in HIV knowledge scores remained consistent across genders, sexual orientations, and ethnicities (Table 2).
Discussion
This longitudinal study explored the potential of land- and arts-based sexual health PLRs to enhance HIV prevention outcomes among Northern and Indigenous youth in the NWT. Our findings reveal postretreat improvements in SSSE, CUSE, and HIV knowledge. These findings align with and build upon previous nonlongitudinal research that has highlighted the promise of land-based and arts-based approaches in improving sexual health outcomes among Northern and Indigenous youth (Logie et al., 2024; Lys et al., 2023; Lys et al., 2018). The HIV prevention cascade includes dimensions of motivation, access, and effective use (Lys et al., 2023, 2016), and HIV knowledge reflects the motivation domain while safer sex and condom use efficacy reflect the effective use domains. Our findings therefore have implications for other Northern, Indigenous, and remote communities in youth-centered approaches for advancing the HIV prevention cascade.
A distinctive feature of this study is the collection and analysis of data 6 months following the intervention, which provides critical insights into the sustainability of the observed outcomes. At 6-months postretreat, SSSE, CUSE, and HIV knowledge scores remained higher than at baseline. Findings indicate that PLRs may equip Northern and Indigenous youth with practical, actionable knowledge to support their sexual health over time. The continued gains suggest that PLRs not only yield immediate benefits but also empower participants to internalize and apply knowledge and practices in their daily lives, such as negotiating condom use and understanding HIV prevention strategies.
While our findings indicate that land- and arts-based PLRs are generally effective in enhancing HIV prevention outcomes, not all youth participants appeared to benefit equally from the intervention. Specifically, young men and non-Indigenous participants did not report significant improvements in SSSE or CUSE, suggesting that our intervention did not fully address the needs or experiences of these subgroups. This underscores the importance of intersectionality in intervention design, where differences in gender norms, cultural expectations, and lived experiences shape how youth engage with and benefit from programming (Heard et al., 2020). Future iterations of the PLRs should incorporate targeted strategies to address these gaps, such as gender-specific content or activities tailored to the unique experiences across the diversity of youth lived experiences.
Strengths and Limitations
This study contributes to the growing body of evidence supporting land- and arts-based approaches in sexual health education and promotion, with its longitudinal design providing new insights into the durability of intervention effects. Study limitations included the absence of a control group, which limits our ability to conclusively attribute observed improvements in HIV prevention among participants to the intervention alone, as other variables may have influenced the results. In addition, the small sample size increases the margin of error and limits the generalizability of the findings. Finally, all data are self-reported, which may introduce biases related to memory recall and social desirability. Despite these limitations, the longitudinal nature of this research underscores the sustained positive effects of the intervention on HIV prevention outcomes. However, continued engagement with youth through follow-up or refresher trainings may further reinforce these gains and help address emerging challenges over time.
Implications for Practice
This study highlights the effectiveness of culturally grounded, youth-led interventions in enhancing HIV prevention outcomes among Northern and Indigenous youth. The sustained improvements in SSSE, CUSE, and HIV knowledge at the 6-month follow-up suggest that land- and arts-based approaches, such as those used in FOXY’s PLRs, can advance the HIV prevention cascade domains of motivation and effective use with NWT youth.
These findings support the integration of community-driven, culturally responsive programming into public health strategies aimed at addressing the disproportionate impact of STIs and HIV in the NWT. Practitioners working in similar contexts should prioritize Indigenous leadership, youth engagement, and culturally relevant content when designing sexual health initiatives. In addition, the high retention rate over 6 months underscores the feasibility of longitudinal youth-focused programming in remote and Northern regions.
Footnotes
Authors’ Note:
Research received funding support from the Canadian Institutes of Health Research (CIHR; Project Grant 425987: (Indigenous People’s Health), Canada Research Chairs (Logie, Tier 2), Public Health Agency of Canada, Arctic Inspiration Prize.
