Abstract
Breastfeeding is a key nutritional behavior for infants during their first years of life. While prenatal breastfeeding intentions do not differ significantly between non-Hispanic Black and White mothers, the ability to meet those intentions decreases over time, and to a greater extent among Black mothers. This is partially due to environments inadequately supportive of individuals’ breastfeeding needs (i.e., not breastfeeding-friendly). The Community Readiness Assessment is a powerful tool to assess a community’s readiness to take action on pressing health issues. While it is frequently used to understand readiness to prevent negative health outcomes, this study explores how it can be used to understand readiness to promote breastfeeding friendliness and subsequently identify appropriate intervention strategies. Between November 2020 and June 2021, we conducted interviews with 23 key respondents in New Haven, Connecticut, representing five community sectors. Respondents scored five dimensions of readiness on a 9-point scale (1 = no awareness, 9 = community ownership). The overall community readiness score was 4.2, denoting the “preplanning” stage of readiness. The highest-scoring readiness dimension was “community knowledge about the issue” (mean score: 4.5), and the lowest-scoring dimension was “resources related to the issue” (mean score: 3.3). Small business owners reported the highest readiness score by sector (mean score: 5.0), while large employers reported the lowest (mean score: 3.1). Scores stratified by both sector and dimension revealed specific areas within the community where readiness-level-appropriate interventions could be implemented. This study highlights the benefit of assessing community readiness prior to intervention to identify tailored, equitable, and effective intervention strategies.
Keywords
Breastfeeding is largely considered the optimal form of nutrition during a child’s first years of life (Division of Nutrition, Physical Activity, and Obesity, 2022). In addition to facilitating infant growth and development, breastfeeding can reduce infants’ risk of asthma, type 1 diabetes, ear infections, gastrointestinal infections, and sudden infant death syndrome (Division of Nutrition, Physical Activity, and Obesity, 2022). Breastfeeding parents also experience benefits, such as lower risks of hypertension, type 2 diabetes, and breast and ovarian cancer (Division of Nutrition, Physical Activity, and Obesity, 2022). These short- and long-term benefits highlight the value and relevance of this health behavior in the current landscape of maternal and child health.
While prenatal intentions to breastfeed do not significantly differ between non-Hispanic Black mothers and non-Hispanic White mothers, the ability to meet those exclusive breastfeeding intentions does significantly differ at both 1 and 3 months after childbirth (Hamner et al., 2020). This suggests that many women, and especially non-Hispanic Black women, face barriers to meeting their breastfeeding intentions over time. In Connecticut, non-Hispanic Black women have lower rates of any breastfeeding at both 4 and 8 weeks after delivery when compared with non-Hispanic White women (at 4 weeks: 75.4% vs. 85.1%; at 8 weeks: 63.2% vs. 78.9%, respectively; Connecticut Department of Public Health, 2021). This points to systemic inequities in breastfeeding support, with breastfeeding laws, policies, feeding norms, and institutional lactation support all influencing individuals’ breastfeeding abilities (Tran et al., 2023). Considering that 32% of New Haven, Connecticut’s population identifies as Black or African American, actions must be taken citywide to address these inequities (United States Census Bureau, 2020). However, we first must understand if, where, and how the community is ready to intervene (Center for Community Health and Development, 2024).
In partnership with the New Haven Breastfeeding Task Force, a coalition of New Haven residents, community-based activists, clinicians, and public health practitioners, we heard from community leaders about the extent to which New Haven was ready to act on improving the city’s breastfeeding friendliness, an environmental characteristic describing how supportive the community is of individuals’ breastfeeding needs. This study documents the design, implementation, and evaluation of such efforts through a Community Readiness Assessment (CRA). Community assessments like the CRA are an important aspect of public health practice; identifying at which stage various sectors of a community are in their readiness to take action on a pressing health issue like breastfeeding can inform the equitable and effective selection and application of public health intervention strategies (Ravaghi et al., 2023).
About the CRA
Based on the social action process for community development (Bohlen et al., 1964; Hoffer, 1958) and the Transtheoretical Model of Behavior Change (Grimley et al., 1994; Prochaska & DiClemente, 1983), the CRA measures a community’s preparedness to act on certain health issues (Plested et al., 2006; Tri-Ethnic Center for Prevention Research, 2014). This evaluation tool is used commonly in public health settings globally to bolster how a community views and takes ownership of a health issue, to help communities identify sustainable and culturally responsive intervention strategies, and to elevate local resources and expertise rather than external perspectives (Center for Community Health and Development, 2024; Plested et al., 2006). Many CRA studies have assessed a community’s readiness to decrease the prevalence of outcomes that negatively impact health, such as unhealthy substance use (Peña-Purcell et al., 2021), HIV/AIDS (Larcombe et al., 2019), and obesity (Islam et al., 2019); fewer have focused on promoting health environmental characteristics like breastfeeding friendliness (Zerfu et al., 2021).
In our study, we assess community readiness to become more breastfeeding-friendly by stratifying the community into sectors to ensure diverse representation; identifying dimensions of readiness, or key factors that influence how ready a community is to take action (Table 1); and scoring the dimensions of readiness on a 9-point scale that ranges from 1 = “no awareness” about the issue to 9 = “community ownership” of the issue (Table 2) (Center for Community Health and Development, 2024; Plested et al., 2006; Tri-Ethnic Center for Prevention Research, 2014). Collectively, these actions, recorded alongside qualitative comments from key respondents, provide an in-depth understanding of New Haven’s readiness to promote breastfeeding.
Dimensions of Community Readiness to Promote Breastfeeding

Note. Adapted from Plested et al. (2006), the Tri-Ethnic Center for Prevention Research (2014), and the Center for Community Health and Development (2024) with permission from the author.
The Community Readiness Scale to Promote Breastfeeding, with Suggestions for Taking Action Based on Stage of Community Readiness
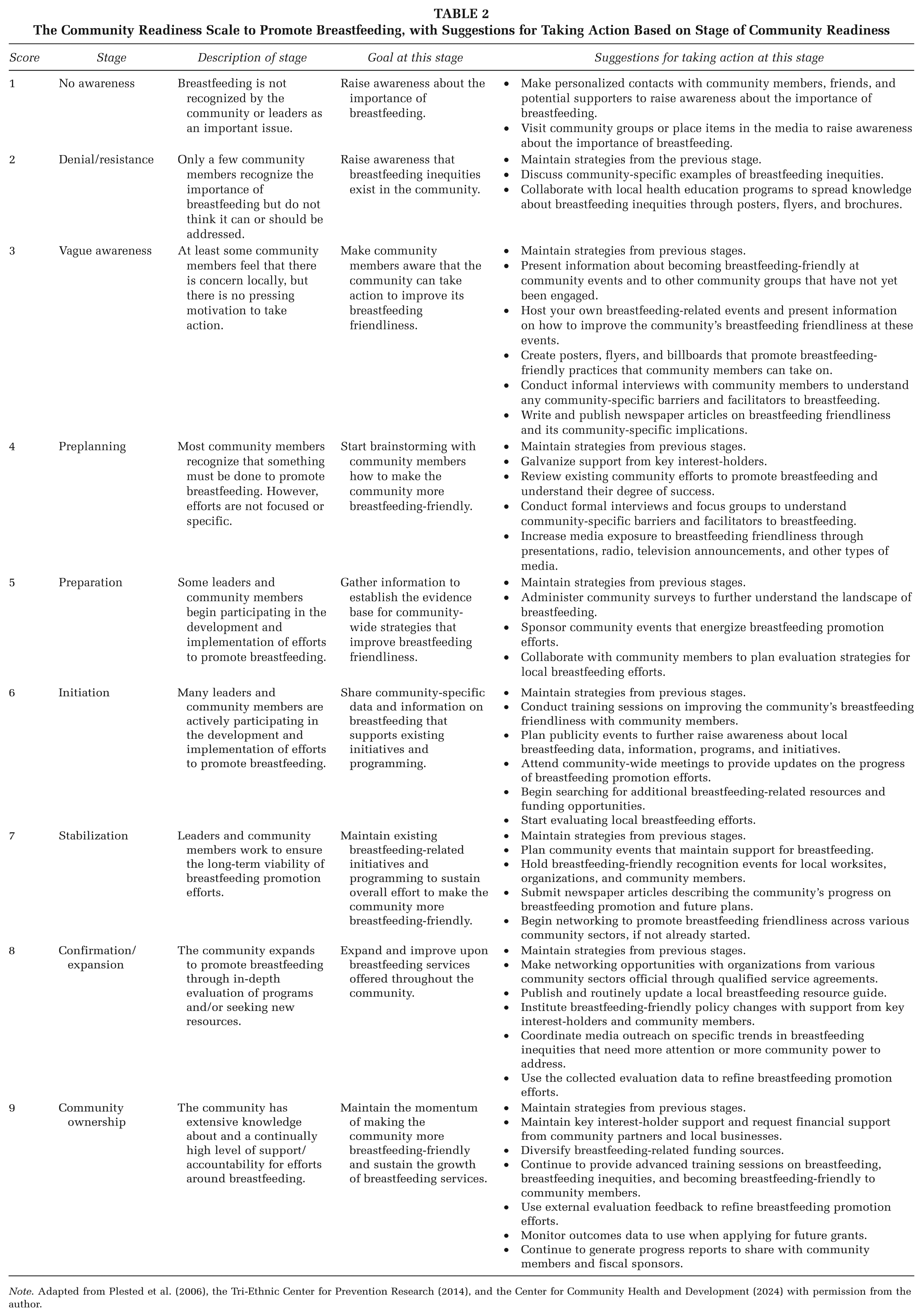
Note. Adapted from Plested et al. (2006), the Tri-Ethnic Center for Prevention Research (2014), and the Center for Community Health and Development (2024) with permission from the author.
Purpose and Aims
The purpose of this study is to understand New Haven, Connecticut’s readiness to become more breastfeeding-friendly and inform the types of and areas for intervention. Furthermore, this study aims to contribute to the growing bodies of literature on breastfeeding, maternal health equity, community health practice, and public health promotion. This study’s focus on community readiness highlights the importance of community-derived decision-making for public health action planning. Without a clear understanding of how prepared a community is to address breastfeeding inequities, resulting programs, practices, or policies may be misled or ineffective (Plested et al., 2006; Tri-Ethnic Center for Prevention Research, 2014). Furthermore, a mismatch between readiness and intervention can lead to a lack of intervention uptake and impact (Livet et al., 2022). Contributing to the fields of community health practice and public health promotion, this study applies the CRA to breastfeeding friendliness, a promotive health environmental characteristic that, to our knowledge following a thorough literature review, has only been assessed using a CRA once before (Zerfu et al., 2021). Understanding a community’s perceptions of breastfeeding is integral to identifying effective intervention strategies.
Method
Adapting the CRA
In adapting the CRA questionnaire to assess breastfeeding friendliness, we prepared the introductory script and dimension-specific anchored rating scales based on the CRA Brief Assessment Guidelines (Plested et al., 2006; Tri-Ethnic Center for Prevention and Research, 2014) (Supplementary Tables 1–5). In this Brief Assessment, each of the five scales, representing the five dimensions of readiness, lists nine numbered statements, which gradually increase from describing no awareness or support for breastfeeding initiatives to full community ownership and support. The benefits of this abbreviated approach include conducting a less time-intensive assessment, reducing the burden on respondents who, at the time, were engaged in addressing the COVID-19 crisis, and standardizing how respondents ranked community readiness. The New Haven Breastfeeding Task Force Community Advisory Board (CAB), comprising residents with lived breastfeeding experience, provided feedback on the script, scales, and types of respondents who would best reflect the perspectives of New Haven community members. The study was approved by the Yale Institutional Review Board.
Recruiting Key Respondents
Respondents were recruited through purposive sampling based on their leadership and involvement within one of five sectors: health care/lactation support, city administration, small business owners (having less than 100 employees), large employers (having 100 or more employees), and community leaders (individuals whose positions grant them influence over a large number of residents and whose work is not encapsulated by other sectors—for example, pastors and community management team leaders). The insights of key respondents from different sectors should ideally collectively represent most community members’ perceptions of a community’s readiness to take action on an issue (Center for Community Health and Development, 2024; Plested et al., 2006; Tri-Ethnic Center for Prevention Research, 2014). Thus, the primary criteria for key respondents were familiarity with the New Haven community and being well-integrated within their respective sectors. To avoid bias, we did not limit respondents to those with knowledge of local breastfeeding initiatives. We developed a list of 44 potential respondents and contacted them via phone or email to inquire about their interest in participating, resulting in 23 individuals who agreed to participate. Following consent, trained interviewers conducted 30- to 60-minute interviews with respondents via phone or a virtual meeting platform. Seventeen interviews were conducted individually, and two were conducted in groups of three. Respondent characteristics are included in Table 3.
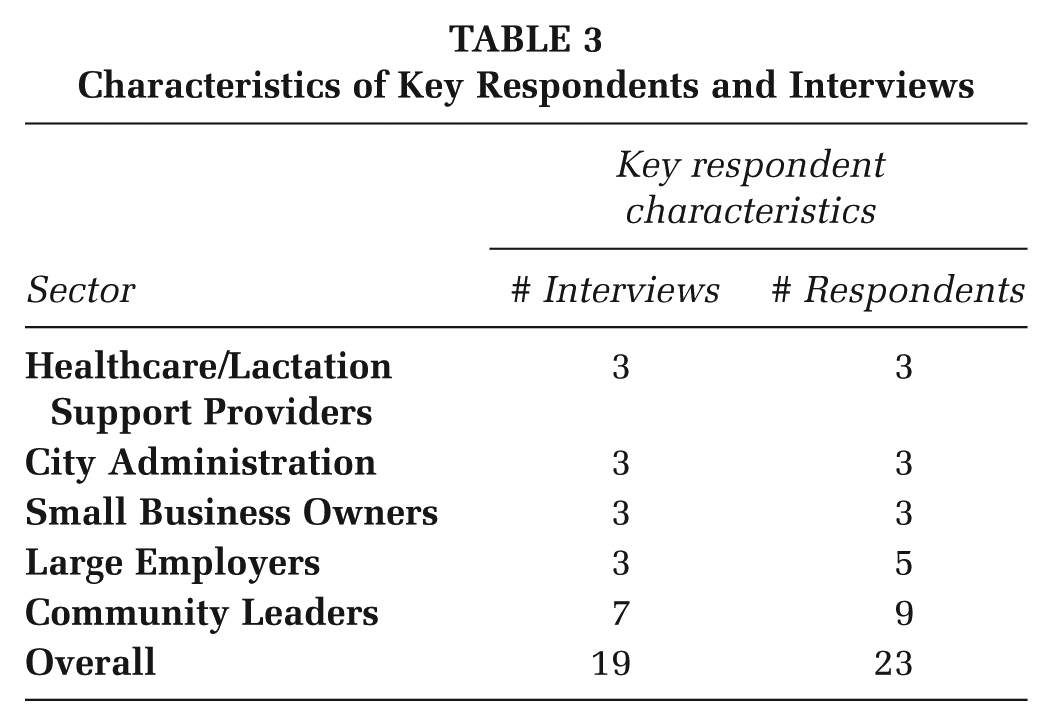
Characteristics of Key Respondents and Interviews
Conducting the Interviews
Two research team members were trained to conduct CRA interviews, which consisted of reviewing with respondents each dimension of readiness along with its associated readiness scale (Supplementary Tables 1–5), starting with the lowest score on the scale and gradually moving toward the highest score. Respondents then noted the highest score at which they reported complete (not partial) agreement with the affiliated statement. This was recorded as their final score. Interviewers recorded the scores in Qualtrics and allowed respondents to expand on why certain scores were selected through qualitative comments. A separate, password-protected document was used to note any comments. Of the 23 individuals who participated in the interviews and provided quantitative CRA scores, 15 (65.2%) expanded on their scores by providing additional qualitative comments.
As individuals, respondents may have their own opinions on the breastfeeding friendliness of New Haven. However, within the CRA, they are asked to share their perceptions of how the community views New Haven’s readiness to become breastfeeding-friendly based on their interactions with, observations about, and/or conversations with community members, effectively asking them to distinguish their personal thoughts from those of the community (Center for Community Health and Development, 2024; Plested et al., 2006; Tri-Ethnic Center for Prevention Research, 2014). By asking respondents to think at a level of perspective beyond their own, the CRA attempts to feasibly gauge community perceptions, with the benefit that, if chosen carefully, respondents can adequately provide insight into the state of a community. Upon conclusion of the interviews, a list of local breastfeeding resources was sent to all participants.
Data Analysis
The overall community readiness score, as well as the mean readiness scores for each community sector, each dimension of readiness, and each dimension of readiness within each community sector, were calculated using R (R Core Team, 2023). Respondents’ qualitative comments, which were provided during the interview and expanded on why they chose specific scores, were coded via content analysis, whereby the two interviewers utilized inductive coding to separately identify overarching themes and met together to adjudicate, combine, and refine the themes until three main themes that adequately captured both interviewers’ interpretations emerged. A finding was considered to be a theme if at least 20% of respondents who provided their qualitative comments mentioned the finding during their feedback. The research team then met again with the CAB and the New Haven Breastfeeding Task Force to present findings and determine next steps.
Results
From November 2020 to June 2021, 19 interviews were conducted with 23 respondents (Table 3). Seventeen interviews were conducted individually, and two were conducted in groups of three, where respondents, who all represented the same sector, agreed on one community readiness score for each dimension. According to CRA methodology, where four to five interviews are sufficient for accurate community representation (Plested et al., 2006; Tri-Ethnic Center for Prevention Research, 2014), having 23 respondents from various sectors ensured adequate alignment for accurately scoring community readiness.
As shown in Table 4, the mean overall community readiness score was 4.2, indicating that New Haven is in the “preplanning” stage of improving breastfeeding friendliness (see Table 2 for “preplanning” definition). To understand the specific ways in which New Haven was ready to improve its breastfeeding friendliness, we stratified community readiness scores by dimension of readiness, sector, and dimension of readiness within each sector. The results of this analysis are shown in Table 4.
Community Readiness Scores
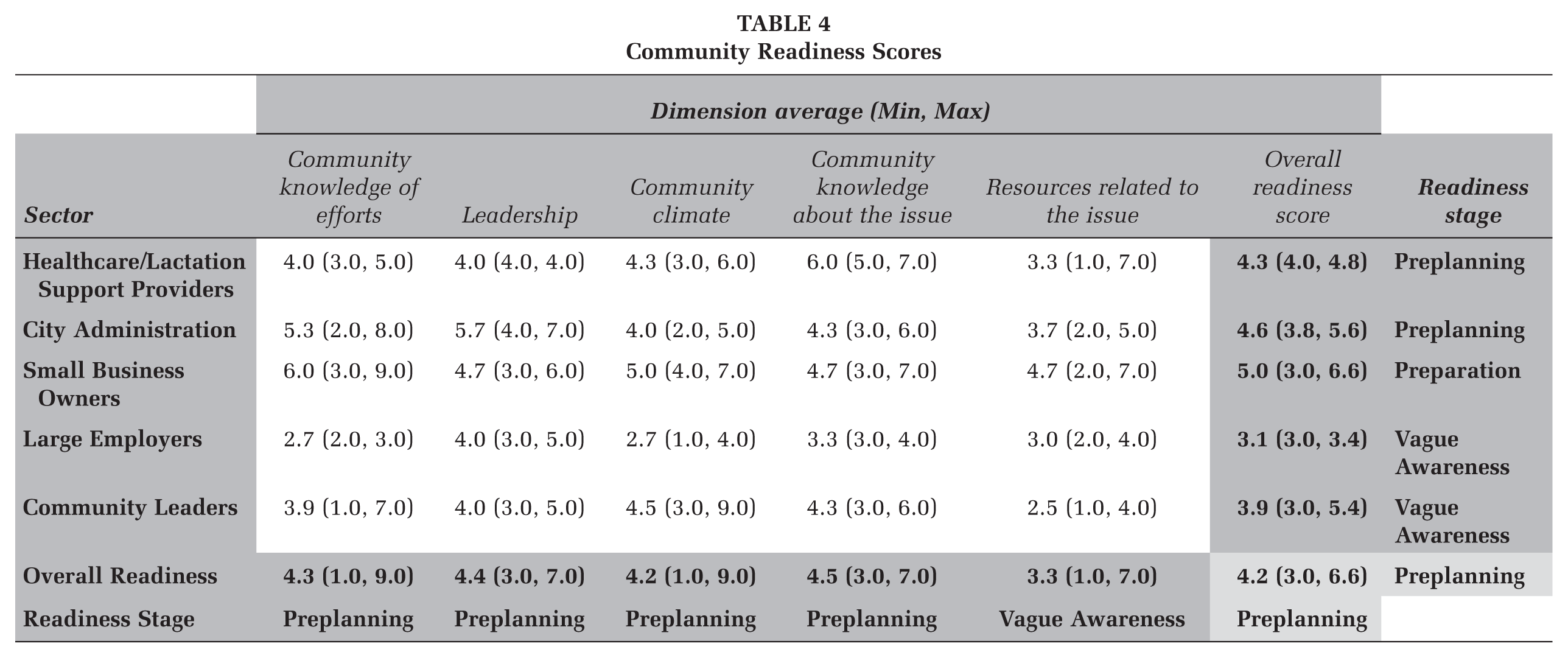
The overall highest-scoring dimension of readiness was community knowledge about the issue, with a readiness score of 4.5. The overall lowest-scoring dimension of readiness was resources related to the issue, with a readiness score of 3.3. When examining scores at the sector level, the overall highest-scoring community sector was small business owners, who had a mean score of 5.0. The overall lowest-scoring community sector was large employers, who had a mean score of 3.1.
Data analyzed by both sector and dimension revealed that within the highest-scoring community sector (small business owners), readiness to support breastfeeding was highest for the community knowledge of efforts dimension (mean score: 6.0) and lowest for the leadership, community knowledge about the issue, and resources related to the issue dimensions, all with mean scores of 4.7. On the other hand, within the lowest-scoring community sector (large employers), readiness to support breastfeeding was highest for the leadership dimension (mean score: 4.0) and lowest for the community knowledge of efforts and community climate dimensions, both with mean scores of 2.7. Individual score ranges varied, representing the spectrum of respondent scores, with mean scores indicative of mean readiness for change.
We excluded one interview from the overall community readiness score calculation because one respondent, a community leader, noted that they could not score any readiness dimension except community knowledge of efforts since they had not previously had any discussions about breastfeeding support with community members. Therefore, while the community knowledge of efforts score factors in scores from all 19 interviews, the average score of all other dimensions, including the overall community readiness score, is based on only 18 interviews.
Emerging Themes From Respondents’ Qualitative Comments
Of the 23 respondents interviewed as part of the CRA, 15 (65.2%) provided qualitative comments to support their readiness scores. Based on respondents’ feedback, three themes emerged, exemplary quotes for which are included in Table 5.
Themes Derived from Respondents’ Qualitative Comments and Exemplary Quotes

The first theme, mentioned by three (20.0%) of the respondents who provided qualitative comments, was the need to make more breastfeeding-friendly public and worksite-specific spaces. One respondent noted the importance of policy to create and maintain breastfeeding spaces; two respondents mentioned the value of normalizing breastfeeding in public to make all spaces more accessible to breastfeeding individuals.
The second theme, mentioned by four (26.7%) of the respondents who provided comments, was health care settings’ influence on individuals’ decisions to breast- or formula-feed. One interviewee noted that when their wife was struggling to breastfeed in the hospital after delivery, a hospital nurse told them that it would be easier to formula feed than breastfeed, neglecting to provide the family with breastfeeding resources. In contrast, two other respondents shared how breastfeeding was particularly successful in hospital settings because of the WIC peer navigators located there, the baby-friendly hospital designation, the provision of pumps, and lactation counselor support.
The final theme, mentioned by five (33.3%) of the respondents who provided comments, was the importance of broadening how and to whom breastfeeding is promoted. Two respondents indicated that their expectation was that only those actively breastfeeding would know about breastfeeding promotion efforts, signaling that those without lived experience may need to be made aware of such efforts. Another respondent stated that some may not view breastfeeding as a priority to address, given that there are many pressing societal issues. Focusing on how breastfeeding might be promoted despite competing priorities, one respondent mentioned how many people are taught that formula feeding is just as beneficial as breastfeeding and that, unless taught otherwise, people will continue to believe this. Thus, to rectify misinformation and broaden the scope of how and to whom breastfeeding is promoted, one respondent suggested creating a unifying message, where breastfeeding is presented as a sustainability issue, detailing the amount of energy consumed in formula production and how exclusive breastfeeding can improve lives.
Discussion
The CRA was applied to assess a community’s readiness to become more breastfeeding-friendly and guide intervention implementation. The study found the community overall at the “preplanning” stage of readiness, primed for various interventions. However, results revealed sector- and dimension-specific variation in the community’s readiness to become more breastfeeding-friendly. For example, compared with small business owners in the “preparation” stage and city administration and health care/lactation support providers in the “preplanning” stage, community leaders and large employers scored as having “vague awareness” in their breastfeeding-friendly community readiness (Table 4). Small business owners may have scored the highest in overall community readiness because, as research shows, small businesses tend to be integrated into their local environments and thus able to build more intimate relationships with customers (Gilboa et al., 2019). These owners may have felt that the community members they interacted with understood the importance of breastfeeding. Similarly, research supports that city administration officials are typically knowledgeable about health disparities in their communities (Godinez Puig et al., 2021). As these officials often interact with community members in their daily responsibilities, their knowledge of health disparities may reflect a greater knowledge of city-level health issues, such as breastfeeding, of which they believe their constituents are aware, influencing their CRA scores. In addition, research shows that healthcare and lactation support providers are key members of breastfeeding support teams with burgeoning breastfeeding knowledge (Weshahy et al., 2019). Based on the actively breastfeeding community members with which these providers likely interact in their occupation, they may have scored the overall readiness of the community to support breastfeeding as relatively high. Nevertheless, community leaders may have scored New Haven’s readiness as lower because they may not have recognized breastfeeding as a topic that is frequently discussed among the community members with which they interact, as was the case with the community leader who did not complete the interview because no discussion of breastfeeding support had ever arisen for them. Finally, large employers may not have the necessary depth of interactions with individual employees and community members to know if and where breastfeeding knowledge and resources are housed (Tansel & Gazîoğlu, 2014), influencing their scores.
Analyzing the results by the highest- and lowest-scored dimensions of readiness also reveals key information about the city and where intervention should be focused. Community knowledge about the issue was the highest-scored sector, indicating that community members are generally knowledgeable about breastfeeding, including its benefits, challenges, and community-specific initiation rates. However, with this score only representing the “preplanning” stage of readiness, more must be done to foster a breastfeeding-friendly community. On the other hand, resources related to the issue was the lowest-scored dimension of readiness, in the “vague awareness” stage, indicating that the most work needs to be done around spreading awareness of existing breastfeeding resources in New Haven. Together, the highest- and lowest-scored dimensions of readiness suggest that while community members generally understand breastfeeding benefits, the lack of community knowledge about resources to support breastfeeding goals, such as breastfeeding support groups and public lactation spaces, may hinder breastfeeding initiation and continuation, perpetuating breastfeeding inequities. As research suggests, the presence of community resources plays a major role in breastfeeding outcomes (LoCasale-Crouch et al., 2024).
The low score of the resources related to the issue dimension is consistent with Zerfu et al.’s (2021) prior breastfeeding CRA conducted in Kenya, highlighting that knowledge of breastfeeding resources is generally a challenge for communities and indicating that more can be done in the field of public health promotion to ensure widespread awareness of culturally relevant breastfeeding resources. On the other hand, this study’s highest-scored dimension, community knowledge about the issue, was inconsistent with Zerfu et al.’s (2021) highest-scored dimension, leadership, highlighting the community-specific nature of CRA findings.
Analyzing findings by both sector and dimension highlights the strengths and areas of improvement in New Haven’s readiness to address breastfeeding. For example, within the highest-scoring sector, small business owners, taking action to increase readiness within the lowest-scoring dimensions (leadership, community knowledge about the issue, and resources related to the issue) will eventually allow the overall readiness score for that sector to rise (Plested et al., 2006). The same strategy is appropriate for the lowest-scoring sector overall, large employers. By taking action to increase readiness within the community knowledge of efforts and community climate dimensions, the readiness of the entire sector will increase. These are key areas for intervention, as employer support for breastfeeding plays a critical structural role in breastfeeding continuation after returning to work (Chang et al., 2021).
Respondents’ qualitative comments also revealed emerging themes related to breastfeeding friendliness, such as (1) the need for more public and workplace-specific spaces for breastfeeding, (2) the influence of health care settings on decisions to breast- or formula-feed, and (3) the importance of broadening how and to whom breastfeeding is promoted, themes that are consistent with prior research (Tran et al., 2023; Marshall & Cook, 2023; Subramani et al., 2024). Many respondents provided critiques of the current state of breastfeeding in their community, even when they were only asked to score community readiness, highlighting specific and high-interest areas where the community can become more breastfeeding-friendly.
Using CRA Results to Inform Intervention Strategies
Given the varying stages of community readiness, the CRA model recommends specific goals, strategies, and activities for intervention (Table 2) (Center for Community Health and Development, 2024; Plested et al., 2006). Of note, when utilizing the CRA methodology, it is important to avoid rounding up to the nearest readiness level, and instead to identify intervention strategies within the current level of readiness, even if the mean readiness score is only a few decimal points away from the next readiness stage. This is to account for the fact that, according to respondents’ collective responses, the community is not yet positioned to fully achieve all aspects of the next readiness stage. For example, if a mean readiness score is 3.9, it is important to identify intervention strategies under the “vague awareness” (score = 3) stage rather than the “preplanning” (score = 4) stage, as the city has not yet met all criteria to fully achieve the “preplanning” (score = 4) stage of readiness, and thus, any higher-stage intervention strategies may be premature in most adequately increasing the city’s readiness.
Thus, at the “vague awareness” stage among community leaders and large employers, the CRA suggests raising awareness of the need to take action to improve breastfeeding friendliness. To this end, recommended next steps include presenting at local events, posting flyers, and publishing newspaper editorials about local breastfeeding efforts (Center for Community Health and Development, 2024). At the “preplanning” stage among city administration and health care/lactation support providers, the CRA suggests brainstorming how to improve breastfeeding friendliness. Accordingly, recommended next steps include speaking with key interest-holders about the issue, conducting focus groups to identify community-specific barriers and facilitators to breastfeeding (as this research team has done (Tran et al., 2023)), and increasing media exposure on breastfeeding through radio-based public service announcements (Center for Community Health and Development, 2024). Moreover, at the “preparation” stage among small business owners, the CRA suggests gathering information to establish an evidence base for strategies to improve breastfeeding friendliness. Therefore, recommended next steps include conducting community surveys in partnership with small businesses, sponsoring community events that energize breastfeeding promotion efforts, and collaborating with small businesses to plan evaluation strategies for breastfeeding efforts (Center for Community Health and Development, 2024). These and other actionable steps require consistent communication and collaboration with community partners in each of the identified sectors.
Study Strengths and Limitations
This study has several strengths, including adhering to community-engaged research principles in study design, implementation, and evaluation. Moreover, findings from this study can and are being used to inform applicable public health interventions. This study also provides key insight into the state of a community in promoting breastfeeding friendliness, which has been studied infrequently in CRA-based literature. Furthermore, by interviewing more respondents than typically required by a CRA, this study is aligned with recommendations for accurately scoring the community (Plested et al., 2006; Tri-Ethnic Center for Prevention and Research, 2014).
Nevertheless, this study also has some limitations. We did not collect data on respondents’ gender or racial/ethnic identity, which could have influenced individual biases and affected how different individuals scored New Haven’s readiness. Follow-up assessments will include these demographics. An additional limitation pertains to how respondents were asked to score community readiness. Applying the CRA Brief Assessment Guidelines may have led to some loss of the richness of qualitative data that could have been collected through full-length interviews. Nevertheless, we took rigorous notes during the brief interviews and used content analysis to thematically analyze the qualitative data, which was beneficial in a time- and resource-limited environment. Finally, in conducting the CRA, respondents were asked to think of community perceptions of breastfeeding friendliness rather than their own. In doing so, personal bias is possible. Although interviewers routinely reminded participants to distinguish between their individual perceptions and those of their community, future studies should explore how to further minimize personal bias when conducting CRA Brief Assessments.
Implications for Practice
To equitably serve a community and identify the most appropriate and effective intervention strategies, it is important to first understand where the community stands on a health concern; a mismatch between readiness and intervention can lead to a lack of intervention uptake and impact (Livet et al., 2022). Thus, health promotion practitioners should employ assessments like the CRA as a first step in public health practice to garner community input and to identify appropriate intervention strategies prior to implementation. Specifically related to breastfeeding promotion in community-based settings, this study adds to the evidence base for future assessments of communities’ readiness to support breastfeeding. While CRA results are community-specific, Table 2 (Center for Community Health and Development, 2024; Plested et al., 2006; Tri-Ethnic Center for Prevention Research, 2014) provides actionable steps that any health promotion practitioner can put into practice to improve breastfeeding friendliness based on their city’s level of community readiness. For example, should a city score in the “denial/resistance” stage of community readiness, health promotion practitioners can discuss community-specific examples of breastfeeding inequities and collaborate with local health education programs to spread knowledge about breastfeeding inequities through posters, flyers, and brochures. By contrast, should a city score in the “confirmation/expansion” stage of community readiness, practitioners should publish and routinely update local breastfeeding resource guides, coordinate media outreach on specific trends in breastfeeding inequities that need more attention or community power to address, and/or use collected evaluation data to refine their breastfeeding promotion efforts. Appropriate actions should be based on the corresponding level of community readiness.
This study also highlights the importance of stratifying CRA data by community sector and dimension of readiness to best understand where and how to intervene. Should large employers have the lowest overall readiness score, for example, there is great value in understanding which dimension of readiness health promotion practitioners should prioritize when working to improve the score. For instance, prioritizing the resources related to the issue dimension of readiness for large employers may require a different approach than the community climate dimension of readiness. By addressing the former dimension, practitioners may focus on ensuring that the community has sufficient resources to support breastfeeding parents, especially in the workplace, or they may desire to increase large employers’ knowledge of existing community resources. By addressing the latter dimension, practitioners may focus on understanding barriers to prioritizing breastfeeding support within the city and implement communications campaigns in partnership with large employers centered around the importance of supporting working parents’ breastfeeding goals. Adding this level of specificity to practitioners’ understanding of where and how to intervene can improve the applicability, uptake, and impact of these interventions within different sectors of the community.
Implications for Research
The CRA is also a useful tool to employ both before and after a public health intervention to understand how a community’s readiness to address a health issue has changed. Thus, health promotion researchers should view the CRA as a key evaluation tool that can be used at various points throughout public health interventions to seek community input in planning and to assess program effectiveness, identifying specific areas of success and opportunities for growth. After the initial CRA is conducted, for example, local organizations can collaborate to address readiness gaps based on the most appropriate action steps (Table 2). A follow-up CRA post-intervention can then reveal how community readiness has changed over time and what actions still need to be taken to ensure optimal health promotion, in line with CRA guidelines. During this follow-up CRA, the same key respondents, or respondents in similar roles as those who responded in the first CRA, can be contacted for interviews, which will ensure that similar perspectives are provided pre- and post-intervention.
Without assessment tools like the CRA, public health interventions may lack critical community voice. By reporting CRA results and qualitative feedback back to the community of focus and working with the community to design, implement, and evaluate public health initiatives, the CRA can inform strategies that bolster community strengths, leverage assets, and improve upon areas of growth.
Conclusion
Breastfeeding is a key nutritional behavior for infants, yet community environments must become more breastfeeding-friendly—that is, adequately supportive of individuals’ breastfeeding needs. The CRA is a key tool for understanding a community’s readiness to promote such environments, and stratifying results by sector and dimension of readiness helps us understand which, where, and how interventions should occur. CRA scores in New Haven demonstrated that the city as a whole is in the “preplanning” stage of readiness to support breastfeeding, which is an ideal stage to take action and initiate stage-specific interventions. Sector- and dimension-stratified results offer additional opportunities to take action. Utilizing the CRA ensures that community voice is incorporated when planning interventions and informs the types of interventions needed to most effectively promote health.
Supplemental Material
sj-docx-1-hpp-10.1177_15248399251362887 – Supplemental material for Listening to Community to Improve Breastfeeding Friendliness: Findings From a Community Readiness Assessment on Breastfeeding
Supplemental material, sj-docx-1-hpp-10.1177_15248399251362887 for Listening to Community to Improve Breastfeeding Friendliness: Findings From a Community Readiness Assessment on Breastfeeding by Tomeka Frieson, Amelia Reese Masterson, Victoria Tran, Frankie Douglass and Kathleen O’Connor Duffany in Health Promotion Practice
Footnotes
Authors’ Note:
We would like to acknowledge the significant and invaluable contributions of Francesca Maviglia for her role in reframing the Community Readiness Assessment questions to address breastfeeding friendliness; New Haven Breastfeeding Task Force members—and especially the Community Advisory Board, composed at the time of Danielle Freeman, Shamica Frasier, Debbie Vitalis, Tycharmel Denny, Irene Cullagh, Oni Muhammad, Aubrey Roscoe, and Sadie Witherspoon—for their input at every stage of the study process; and the key respondents who lent their time and energy to share their perspectives for this study. Funding information: Centers for Disease Control and Prevention, Grant/Award Number: 6NU58DP006579.
ORCID iDs
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.