Abstract
Breastfeeding is vital to a child’s lifelong health and has significant positive benefits to mother’s health. World Health Organization recommends beginning exclusively breastfeeding within the first hour after birth and continuing during the first 6 months of infant’s life. The purpose of this review is to identify and examine breastfeeding interventions conducted across the Spanish-speaking countries. A scoping review of the literature was conducted across 14 databases for relevant publications published through April 2023 to find studies in Spanish-speaking countries that involved breastfeeding as an intervention component. A total of 46 peer-reviewed articles were included in this review, across 12 Spanish-speaking countries. Participants ranged from pregnant women, mothers, mother-infant pair, and health care professionals. Intervention at the individual level in combination with support from trained health care professionals or peer counselors seemed to have higher improvements in breastfeeding rates. The greatest improvement in exclusively breastfeeding for 6 months was seen in interventions that included prenatal and postnatal intensive lactation education, for a period of 12 months. The most effective interventions that improved rates of any breastfeeding included promotional activities, educations workshop, and training of health care staff along with changes in hospital care. Breastfeeding promotion is an economical and effective intervention to increase breastfeeding behavior and thereby improving breastfeeding adherence across Spanish-speaking countries.
While health organizations and medical experts worldwide agree on the importance of breastfeeding, there have been poor improvements in the practice of breastfeeding worldwide (Cai et al., 2012; Walters et al., 2019). According to the World Bank’s most recent statistics, in Latin America and the Caribbean, the rate at which infants less than 6 months of age that are exclusively breastfed is at 37% (Arocha-Zuluaga et al., 2022). Some countries in Latin America and the Caribbean present with alarmingly suboptimal rates, including Dominican Republic, 5%; Venezuela, 7%; and Panama, 21% (Arocha-Zuluaga et al., 2022). These rates fall very short of the World Health Organization’s (WHO’s) 2025 goal of increasing the rate of exclusively breastfeeding in the first 6 months of life to at least 50% (Walters et al., 2019; World Health Organization, 2021). Reaching these goals will require action at the individual, community, and health institutional levels.
Furthermore, it is important to understand the barriers affecting mothers from breastfeeding. These barriers can be impacted by factors at the individual, community, and health institutional levels (Snyder et al., 2021). Causes such as low self-efficacy, lack of familial support (individual level), lack of cultural acceptance of breastfeeding (community level), or lack of counseling and education from health care personnel (health institutional level) can hinder a mother from breastfeeding or exclusively breastfeeding (Atyeo et al., 2017; Colombara et al., 2015; Snyder et al., 2021). For these reasons, it is important to develop culturally congruent interventions to promote, support, and encourage mothers to breastfeed and achieve the WHO 2025 goal of extending the duration of exclusive breastfeeding for up to 6 months of age to 50%.
In Spanish-speaking sovereign countries (SSSCs), such as in Latin America and the Caribbean, more than 50% of all infants are not breastfed within the first hour of life, 37% are breastfed exclusively for the first 6 months of life, and between 31% and 55% continue to receive breastmilk for up to 2 years of age (Caribbean Public Health Agency, 2022). Not meeting the WHO/United Nations International Children’s Emergency Fund (UNICEF) breastfeeding recommendations has been linked to child malnutrition (Atyeo et al., 2017). What is needed is a communal approach in the development and implementation of interventions that promote breastfeeding practices in SSSCs.
The aim of this review is to identify breastfeeding-promotion interventions across SSSCs and help guide researchers and health care professionals in summarizing the current state of the existing literature, identify gaps in the existing literature, and identify areas where future work is needed.
Methods
Literature Search
A scoping review of the literature was conducted using 14 databases (Table 1), employing the PRISMA Extension for Scoping Reviews (Tricco et al., 2018), and the same search strategy was utilized in each of the 14 databases, using all the keywords, search terms, and phrases included in Table 1. This search was done in collaboration with a university librarian. For the purpose of this review, SSSC included Argentina, Bolivia, Costa Rica, Chile, Colombia, Cuba, Dominican Republic, Ecuador, El Salvador, Equatorial Guinea, Guatemala, Honduras, Mexico, Nicaragua, Panama, Paraguay, Peru, Spain, Uruguay, and Venezuela. In addition, reference lists of relevant studies were screened to identify publications from other studies that might be eligible for this review.
Electronic Databases Used With Relevant Search Period and Terms

Based on the PRISMA Extension for Scoping Reviews (Tricco et al., 2018), the same search strategy was employed in each of the 14 databases listed, using all the keywords, search terms, and phrases included above.
Eligibility Criteria
The inclusion criteria were set to intervention studies published up until April 30, 2023, in peer-reviewed journals. English and Spanish peer-reviewed intervention-based studies with quantitative outcomes were included. Inclusion criteria consisted of pregnant women/mothers across SSSCs receiving education, training, or other intervention that promotes breastfeeding or exclusive breastfeeding (Table 2). Only intervention-focused articles that involved the promotion of either any breastfeeding or exclusive breastfeeding for a defined period of time as either the primary intervention or as a component of a multi-behavioral intervention at all levels (individual, programmatic, community, family, or policy) were included. Studies that examined Spanish-speaking communities or migrants of Spanish origin residing in non-Spanish–speaking countries were excluded.
PICOS Criteria for Inclusion and Exclusion of Studies
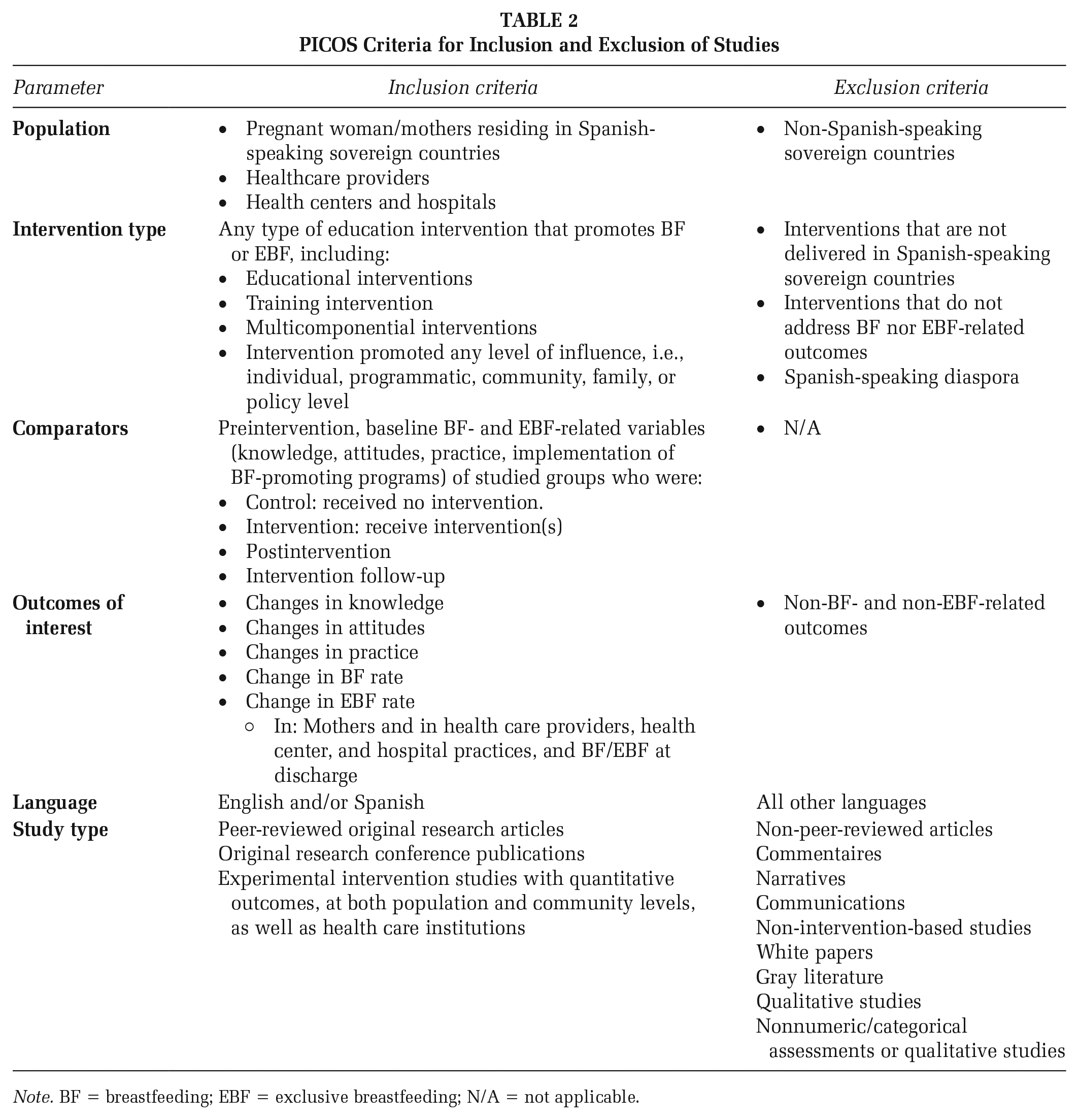
Note. BF = breastfeeding; EBF = exclusive breastfeeding; N/A = not applicable.
Study Selection and Data Extraction
BAE and SB independently conducted the literature search and selected studies for inclusion in the scoping review. Differences were discussed to reach consensus; ED resolved discrepancies if needed. Extraction and tabulation of data were done by SB and independently checked by BHA-E and NB. The search strategy was adapted according to the indexing systems of each respective database. Rayyan QCRI software (Ouzzani et al., 2016; Rayyan, 2021) was used to assist in the screening process and study selection. Titles and abstracts were screened for relevancy, and potentially relevant journal abstracts were reviewed by three of the authors (NB, ED, and BAE). Potential studies for inclusion in this review were evaluated independently by each author for relevance, merit, and inclusion/exclusion criteria (Table 2). All selected articles were then discussed with the primary author before taking the final decision for inclusion (Figure 1). Once the list of selected studied was finalized, BAE extracted and SB and NB cross-checked the following for each study: author, date, target population, country, type of study, sample size, type, details of intervention, measured parameters, main results, and main recommendations. Differences in opinion in data extracted were discussed to reach consensus and tabulated. Given that methodological quality assessment is not a prerequisite for scoping reviews, we did not appraise the included studies (Peters et al., 2020).
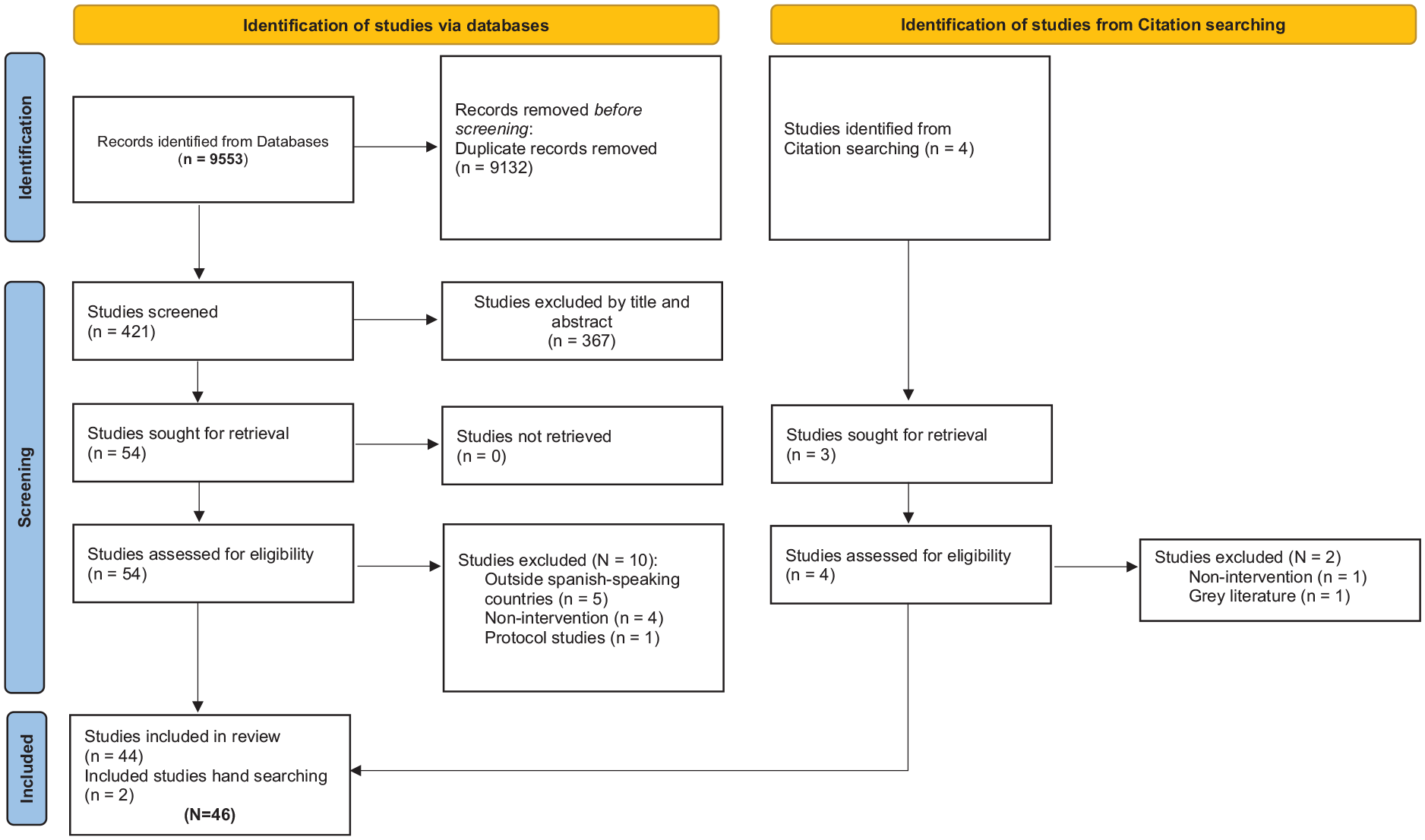
Flow Diagram
Results
In total, 46 peer-reviewed articles were included in this review, across 12 SSSCs: 16 from Spain (Artieta-Pinedo et al., 2013; Balaguer Martínez et al., 2018; Cebrián et al., 2006; Estalella et al., 2020; Franco-Antonio et al., 2020; Gámez Requena et al., 2004; Gonzalez-Darias et al., 2020; Guijarro et al., 2014; Hernández Perez et al., 2018; Lasarte Velillas et al., 2007; Martínez Galiano & Delgado Rodríguez, 2013; Martínez-Galiano & Delgado-Rodríguez, 2014; Roda et al., 2002; Santamaría-Martín et al., 2022; Seguranyes et al., 2014; Soriano-Vidal et al., 2018), 10 from Mexico (Bolaños-Villar et al., 2023; Bueno-Gutiérrez et al., 2021; Iñarritu-Pérez et al., 2022; Langer et al., 1998; Monterrosa et al., 2013; Morrow et al., 1999; Ortiz-Félix et al., 2021; Perez-Escamilla et al., 1993; Rodriguez-Garcia et al., 1990; Sanchez-Espino et al., 2019), seven from Chile (Alvarado et al., 1996; Burkhalter & Marin, 1991; Lucchini Raies et al., 2013; A. Pérez & Valdés, 1991; Pugin et al., 1996; Valdés et al., 1993, 1995), three from Peru (Chumpitaz Durand et al., 2021; Leyva et al., 2015; Velásquez Rondón & Huaman Hernández, 2020), two from Colombia (Arias Ramírez et al., 2021; Ulloa Sabogal et al., 2023), one from Honduras (Cohen et al., 1999), two from Cuba (Morales et al., 2021; Tamayo Velázquez et al., 2022), one from Dominican Republic (Navarro et al., 2013), one from Ecuador (Maslowsky et al., 2016), one from Nicaragua (K. Perez et al., 2018), one from Venezuela (Rojas et al., 2019), and one from Guatemala (Prieto et al., 2017; Table 3). Study designs included 14 randomized control trials (Balaguer Martínez et al., 2018; Bueno-Gutiérrez et al., 2021; Cohen et al., 1999; Franco-Antonio et al., 2022; Gonzalez-Darias et al., 2020; Hernández Perez et al., 2018; Langer et al., 1998; Lucchini Raies et al., 2013; Morrow et al., 1999; Perez-Escamilla et al., 1993; Rodriguez-Garcia et al., 1990; Santamaría-Martín et al., 2022; Seguranyes et al., 2014; Ulloa Sabogal et al., 2023), 14 quasi-experimental studies (Arias Ramírez et al., 2021; Burkhalter & Marin, 1991; Estalella et al., 2020; Iñarritu-Pérez et al., 2022; Lasarte Velillas et al., 2007; Monterrosa et al., 2013; Morales et al., 2021; Navarro et al., 2013; Ortiz-Félix et al., 2021; Perez-Escamilla et al., 1993; Pugin et al., 1996; Tamayo Velázquez et al., 2022; Valdes et al., 1995; Velásquez Rondón & Huaman Hernández, 2020), 12 prospective (Alvarado et al., 1996; Artieta-Pinedo et al., 2013; Bolaños-Villar et al., 2023; Cohen et al., 1999; Guijarro et al., 2014; Martínez Galiano & Delgado Rodríguez, 2013; Martínez-Galiano & Delgado-Rodríguez, 2014; Maslowsky et al., 2016; K. Perez et al., 2018; A. Pérez & Valdés, 1991; Soriano-Vidal et al., 2018; Valdés et al., 1993), and three retrospective studies (Cebrián et al., 2006; Chumpitaz Durand et al., 2021; Gámez Requena et al., 2004), one cross-sectional study using educational sessions (Rojas et al., 2019), one educational intervention (Sanchez-Espino et al., 2019), and one quantitative pre-experimental with pre-post evaluation study (Leyva et al., 2015). Sample size ranged from 35 to 1,400 pregnant women/mothers. Two studies were a multi-part Breastfeeding Promotion Program, which included training of health care personnel, education, and activities in the prenatal and outpatient clinics, as well an open lactation clinic (Rojas et al., 2019; Valdes et al., 1995). Fathers or extended families were not involved in any of the included studies. Most of the studies reported exclusive breastfeeding (N = 24), any form of breastfeeding was reported in 11 studies, and 11 studies reported knowledge and attitude toward breastfeeding. Two studies involved helping mothers achieve re-lactation (Atalah et al., 2004; Cohen et al., 1999).
Summary of Literature Search (N = 46)
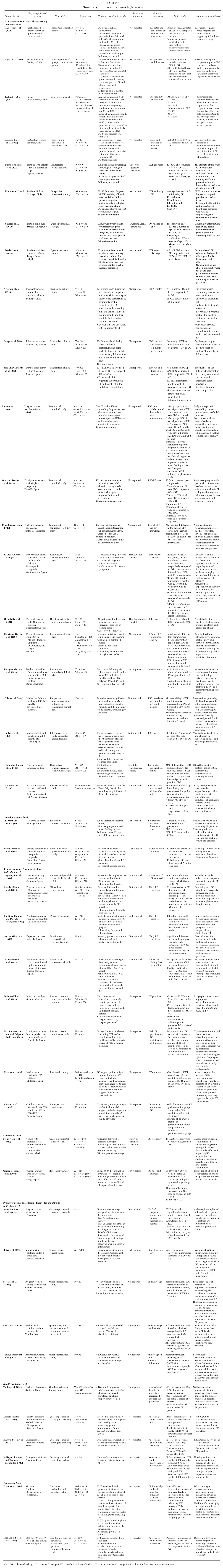
Note. BF = breastfeeding; CG = control group; EBF = exclusive breastfeeding; IG = interventional group; KAP = knowledge, attitude, and practice.
Most of the studies reported positive changes in knowledge, attitudes, and/or practices of breastfeeding. There were various forms of interventions used ranging from participants receiving a single brief motivational session (Gámez Requena et al., 2004) to intensive lactation education plus support from trained personnel through weekly and monthly home visits for 1 year (Estalella et al., 2020). Many of the interventions included patients receiving educational sessions, eight included home visits from trained personnel (Alvarado et al., 1996; Burkhalter & Marin, 1991; Cohen et al., 1999; Langer et al., 1998; Lucchini Raies et al., 2013; Morrow et al., 1999; Navarro et al., 2013; Roda et al., 2002), and one receiving support from a doula (Langer et al., 1998). Four studies reported on peer support (Burkhalter & Marin, 1991; Gonzalez-Darias et al., 2020; Morrow et al., 1999; Prieto et al., 2017), and six studies utilized video, radio, phone, virtual, or telehealth interventions (Guijarro et al., 2014; Hernández Perez et al., 2018; Maslowsky et al., 2016; Monterrosa et al., 2013; Prieto et al., 2017; Seguranyes et al., 2014). Three studies noted no significant difference between control and intervention groups (Artieta-Pinedo et al., 2013; Balaguer Martínez et al., 2018; Ulloa Sabogal et al., 2023).
Outcome: Exclusive Breastfeeding
Across all studies, exclusive breastfeeding rates either increased or were maintained. For example, a breastfeeding program that included community health promoters during prenatal and postnatal home visits for 6 months in Chile reported that exclusive breastfeeding at 6 months was significantly higher in the intervention group than in the control group (42%; 0%, p ≤ .01; Alvarado et al., 1996). However, two interventions showed no significant difference in intervention group compared to control group, which included home visits from lay community volunteers (Navarro et al., 2013) and home visits from a doula (Langer et al., 1998). A nursing educational intervention in a hospital in Colombia showed no significant difference in the rates of exclusive breastfeeding at 6 months between groups; however, significant improvements in knowledge of breastfeeding were reported (Ulloa Sabogal et al., 2023).
Nine randomized control trials in this review had significantly higher rates of exclusively breastfeeding in the intervention group than in the control group (Balaguer Martínez et al., 2018; Bueno-Gutiérrez et al., 2021; Cohen et al., 1999; Franco-Antonio et al., 2022; Langer et al., 1998; Lucchini Raies et al., 2013; Rodriguez-Garcia et al., 1990; Santamaría-Martín et al., 2022; Seguranyes et al., 2014). A telephone-delivered educational session in Ecuador, given by trained breastfeeding nurses, and access to on-call nurse for 30 days reported significantly higher rates of exclusively breastfeeding in the intervention group than in the control group at 3 months; 87% compared to 67% (Maslowsky et al., 2016). A prenatal breastfeeding skills group in Chile, which included training of the health care team and implementation of breastfeeding education and hands-on skills activities to initiate and maintain breastfeeding, reported 67% of mothers in the intervention group were exclusively breastfeeding at 6 months compared to 32% of the control group (A. Pérez & Valdés, 1991). A multicomponent prenatal and postnatal educational program in Chile, using lectures, monthly support groups, peer support, and home visits, reported 74% of intervention group exclusively breastfeeding compared to 30% in the control group, at 6 months (Burkhalter & Marin, 1991). In a hospital in Mexico, mothers who planned to breastfeed delivered in a maternity ward where either the newborn remained separated in a nursery room or the newborn roomed in with mother. Mothers who roomed in with newborns either received individual breastfeeding guidance during the hospital stay or received the hospital’s usual support. This intervention reported that mothers who roomed with newborns and received breastfeeding guidance showed a significant higher rate of exclusively breastfeeding throughout the first 4 months compared to the infants who went to the nursery (p < .05; Perez-Escamilla et al., 1993). Mothers with late pre-term infants in Spain received a postnatal booklet with evidence-based easy-to-understand breastfeeding education along with a feeding chart diary, and results showed 68% of infants in the intervention group were exclusively breastfeeding compared to 51% in the control group at discharge (Estalella et al., 2020).
The breastfeeding promotion programs in Chile, a health system–based intervention including training of health care team in breastfeeding along with prenatal educational activities and open outpatient lactation clinic for mothers, produced a positive impact on exclusively breastfeeding at 6 months in the intervention group compared to the control group (Pugin et al., 1996; Valdés et al., 1993).
Outcome: Any Type of Breastfeeding
In a quasi-experimental media intervention in Mexico, nurses delivered breastfeed promotion through scripted messages via radio, for 21 days; the intervention group reported a 3.7-times higher frequency of breastfeeding than the control group which did not receive any messages (Monterrosa et al., 2013). In Spain, a community intervention organized activities to promote breastfeeding such as workshops aimed at health care professionals, hosted public events, and implemented changes in hospital health care services, and reported results showed that 85% of women in the intervention group started breastfeeding compared to 28% of women in the control group (Gámez Requena et al., 2004). In a prospective study, in Mexico, mothers were provided with printed infographic materials, at different perinatal periods, promoting breastfeeding, and results showed that 92% of mothers in the intervention group who received three or more printed infographics planned to breastfeed compared to 78% of the control group (Bolaños-Villar et al., 2023). A two-step educational intervention carried out in a public hospital in Mexico provided breastfeeding training for the labor and delivery staff of the hospital and educated participants on early breastfeeding; results showed early breastfeeding were achieved in 77% of the cases (Sanchez-Espino et al., 2019). One intervention in Spain relating to an educational intervention involving virtual consultations from a midwife reported no significant difference of breastfeeding prevalence between intervention and control groups: 64.5% and 65.4% (Seguranyes et al., 2014); however, in another study, an educational intervention conducted by a midwife achieved early breastfeeding (81%) compared with educational intervention given by other health care professionals (68%; Martínez-Galiano & Delgado-Rodríguez, 2014). An educational intervention for primiparous women showed no significant difference with initiation of breastfeeding between control and intervention groups; however, a positive relationship was reported between attending educational classes and continuation of breastfeeding for the first month only (Artieta-Pinedo et al., 2013).
Outcome: Knowledge and Attitudes
The level of knowledge a mother has regarding the importance of breastfeeding is one of the major factors that influence breastfeeding duration and abandonment (Ávila-Ortiz et al., 2020; Vázquez-Osorio et al., 2022). Results from studies identified in this review showed that educational interventions significantly improved mothers’ level of knowledge about the importance of exclusively breastfeeding for 6 months. For example, one study reported improved results after the intervention based on multiple intelligence, 57% of the mothers developed more knowledge than 42% of mothers who received traditional education (Chumpitaz Durand et al., 2021). Similar results were reported in another study (Rojas et al., 2019), where 29% of mothers with deficient level of knowledge improved to 60% with good level of knowledge among 1,132 pregnant women and mothers who attended educational breastfeeding workshops. Another study (Leyva et al., 2015) reported that after applying an educational program to a group of 55 mothers of children younger than 6 months from a health center in Trujillo, Peru, they managed to change the level of knowledge with respect to breastfeeding, from the average level of 96% to 100% at high level. In Cuba, weekly workshops for pregnant women during their third trimester resulted in a 100% perceived benefit for breastfeeding for 6 months compared to 62% before intervention (Morales et al., 2021). With regards to the effectiveness of mothers understanding the benefits of breastfeeding infants up to 2 years of age, percentages ranged from 18% before intervention to 51% after intervention in a study in Colombia (Arias Ramírez et al., 2021). A cross-sectional investigational study of mothers in Venezuela reported that topics with the greatest impact included milk conservation, breastfeeding practices, and measures to increase milk production and that mothers’ knowledge level increased from 29% to 61% (Rojas et al., 2019).
Three quasi-experimental (pre-posttest) studies on health care professionals receiving multicomponent intensive training and educational workshops, including about breastfeeding, showed that the percentage of correct answers increased from 80% pretest to 88% posttest (p = .0028; Lasarte Velillas et al., 2007), and knowledge level increased from 30% to 95% in female medical students and 26% to 84% in medical students, along with an increase in positive attitude toward breastfeeding after intervention; 91% in female medical students and 82% male medical students (Iñarritu-Pérez et al., 2022). A study in Guatemala reported that the most effective intervention in terms of improved levels of knowledge was through one-way communication, utilizing breastfeeding promotional texts (Prieto et al., 2017). A two-phase program conducted in the Dominican Republic with adolescent mothers aimed to discuss their postpartum experience, and an interventional program was created based on the topics that the adolescents felt were the most important to them. Participants indicated that the highest priority of desired knowledge included maternal lactation and infant feeding (Navarro et al., 2013). These results show that programs designed to improve knowledge and attitudes about breastfeeding are feasible and should be offered as part of a routine primary care component.
Discussion
The objective of this scoping review was to examine the existing available literature on interventions that promote breastfeeding among pregnant women/mothers residing in SSSCs. These interventions showed a positive impact in promoting breastfeeding knowledge, attitude, and practices of breastfeeding, exclusive breastfeeding, early initiation, and duration of breastfeeding, including knowledge and confidence of health care professionals. Similar results were found in a systematic review (Sinha et al., 2015) which reported that educational interventions and counseling have the greatest impact on promoting maternal breastfeeding, including exclusive breastfeeding for 6 months of infants’ age. These findings show that there is an urgent need to increase and invest in continued support for breastfeeding in SSSCs, through implementation of education and training to individuals, community, and health care system.
Successful interventions included in this review were provided by trained health care professionals, peer counselors, or lay community volunteers, as well as from doulas and midwives. A key success to these interventions was that mothers were drawn to the emphatic, reassuring, and motivating support from the trained health care professionals and peer counselors. The relationship between mothers and her health care team is important in building and maintaining a bond of trust that would serve as a greater motivating factor for breastfeeding. Breastfeeding counseling should be provided as a continuum of care, by appropriately trained health care professionals and community-based lay and peer breastfeeding counselors who are associated with positive attitudes and more confidence when providing breastfeeding recommendations and support to mothers.
This review showed that the increase in practice of exclusively breastfeeding up to 6 months resulted from education and counseling interventions. The studies in this review showed significantly higher rates of exclusive breastfeeding are observed when educational group discussions are used as the principal strategy, and the majority occurred in the postnatal period. It has been noted that a focus on the early postnatal period should be of high priority as it is the most critical time to reinforce desired breastfeeding behaviors. Successful programs provided education and information about breastfeeding to pregnant women and mothers during the prenatal and postnatal periods and included training of health care team and lactation support groups for mothers who were nursing. Such programs should provide timely and repeated breastfeeding interventions, including education of health care staff, and it provided the necessary support to help mothers successfully achieve breastfeeding. Future studies could include longer duration of intervention to determine if countries are reaching the WHO global target of 50% prevalence of exclusive breastfeeding by 2025.
A gap found in the scoping review was lack of familial intervention, that is, involving fathers or family members, and so on, as many mothers report needing more support from significant family members throughout childbirth and postpartum period. In other breastfeeding education and intervention studies, familial support was found to significantly and positively predict changes in knowledge and attitudes related to breastfeeding and to increase the practices of breastfeeding including incidence and duration (Ekström et al., 2003; Hanafi et al., 2014; Haneuse et al., 2000; Ratnasari et al., 2017; Swanson & Power, 2005), suggesting that interventions that include components of education for family members in support of breastfeeding may increase their intended effect. A lack of support from partners and family serves as an obstacle to mothers achieving their breastfeeding goals and in turn leads to reduced rates of breastfeeding. There is a strong need for public health messages not solely targeted toward mothers but also with a focus on their significant others and families which would be vital when developing breastfeeding campaigns. Indeed, a focus group found that among Mexican-American mothers in the United States, a lack of partner and family support was found to be a barrier to breastfeeding, even when knowledge about the benefits of breastfeeding was high (Gill et al., 2004). Understanding such barriers to breastfeeding can suggest areas for curricular and intervention improvement in support of increased incidence and duration of breastfeeding. More research that examines the crucial role that significant others and family play in promoting and supporting breastfeeding is warranted.
Along with family support, cultural beliefs and practices are also very important components in promoting breastfeeding. It has been found in other studies cultural tailoring or incorporation of different cultural, traditional, and/or familial values can positively impact the efficacy of breastfeeding interventions (Cidro et al., 2015; Cook et al., 2021; MacVicar et al., 2015; Rhodes et al., 2021; Segura-Pérez et al., 2021). Interventions that utilized cultural tailoring or peer support for Hispanic women were found to increase exclusive breast feeding and the duration of breastfeeding (Linares et al., 2019; Lutenbacher et al., 2018). In general, it has been found that cultural tailoring of health promotion interventions tends to increase the efficacy of the initiative (Chandler et al., 2022; Ehrlich et al., 2016; McCurley et al., 2017). Because the rates of breastfeeding are low across Spanish-speaking countries, it is imperative to understand how to design the most impactful interventions to increase breastfeeding incidence and duration.
Another observation found in this review was that the majority of the studies took place in either Spain or Mexico. No study was identified during the literature search that was conducted in Argentina, Bolivia, Costa Rica, El Salvador, Panama, Paraguay, Uruguay, and the Spanish-speaking central African country of Equatorial Guinea. Consequently, more studies including those conducted in these countries are needed to add to the literature on the effectiveness of breastfeeding interventions in these identified SSSCs. Understanding cultural practices from different countries across SSSCs can offer a wider explanation to the variation in successful promotions that can increase breastfeeding practices, knowledge, and attitudes across different countries.
To help meet the WHO recommendations of continued breastfeeding along with introducing appropriate complementary foods for up to 2 years of age or longer, breastfeeding interventions should be given at both antenatal period and postnatally for up to 2 years. No study in this scoping review analyzed the effects of breastfeeding up to 2 years of age or beyond. Further research is needed regarding promotional interventions within Spanish-speaking countries in maintaining breastfeeding practices for more than 24 months. A systematic review and meta-analysis found that of the articles included and assessed as “continued breastfeeding” (12–23 months in duration), the interventions evaluated showed a significant improvement of 61%, with higher effects in higher-income and urban settings than in low-moderate-income and rural settings (Sinha et al., 2015). However, studies that include either intervention duration of or follow-up at 2 years are incredibly limited and thus offer additional opportunities for research.
Scaling up breastfeeding policies and programs effectively has been identified as a global health priority for its role in achieving the Sustainable Development Goals. There was a lack of policy-related interventions in this scoping review. Poor regulation of marketing campaigns for artificial foods and the lack of funding for programs that promote, protect, and support breastfeeding are barriers in SSSCs that national policies could address.
Mobile health strategies could also serve as a potential vehicle to promote breastfeeding and improve levels of knowledge through direct communication delivering breastfeeding messages. Text messaging programs could be informative and improve exclusive breastfeeding rates and duration in communities with low prevalence of breastfeeding practices. Mobile health applications are becoming increasingly popular in SSSCs (Farach et al., 2015), which can benefit communities by making breastfeeding promotion more accessible and affordable. Further research is needed to test how best they can be used to promote breastfeeding.
Implications
Interventions in this review demonstrate a positive relation between breastfeeding interventions and knowledge, attitude, and practices. These findings were consistent with previous systematic reviews conducted with nurses, midwives, and physicians, which reported increased knowledge and breastfeeding skills and improved attitudes toward breastfeeding following their participation in educational programs (Sandhi et al., 2023). The implications of these findings are summarized in Table 4 and expanded below.
Implications for Practice, Policy, and Research
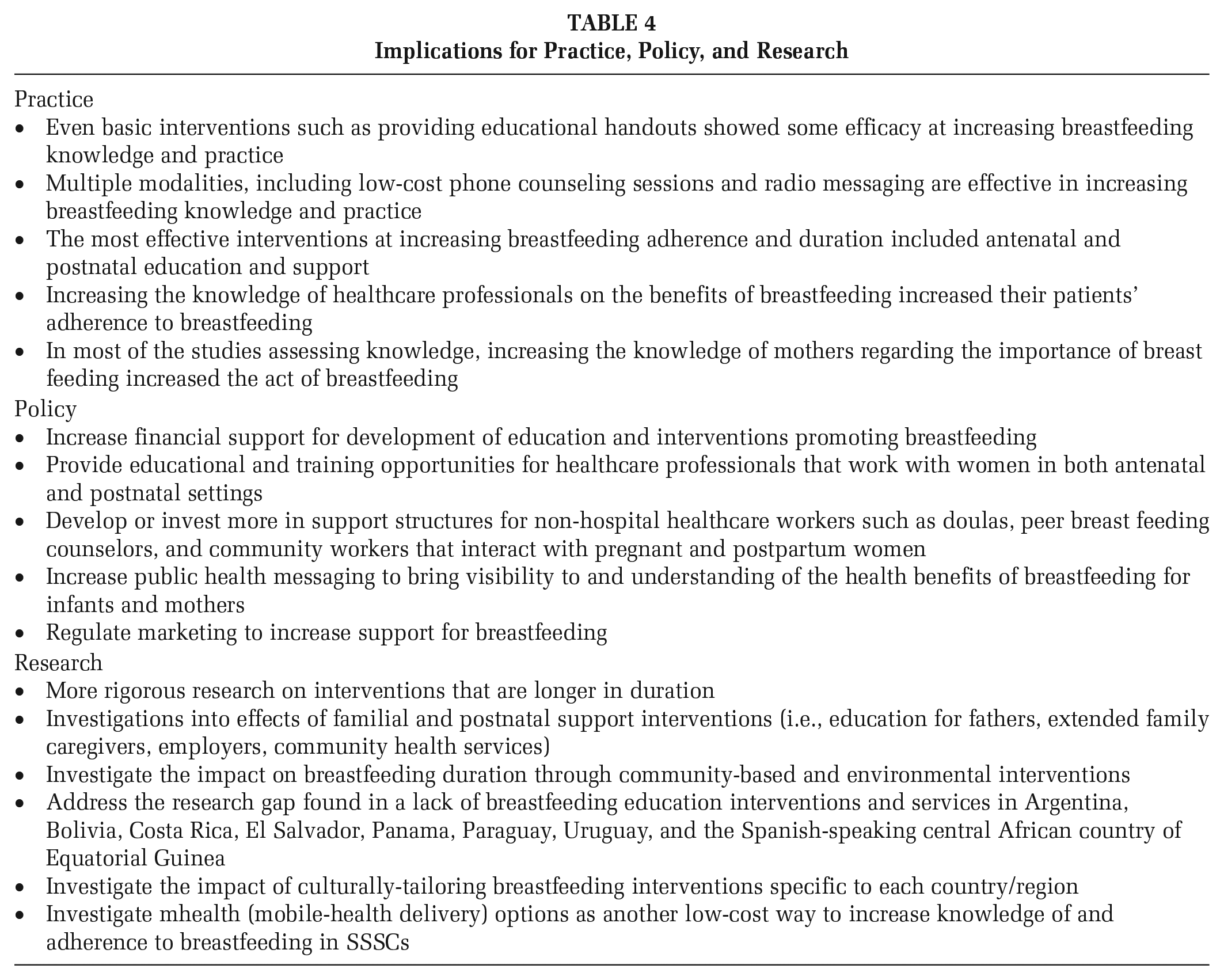
Initiatives that include giving mothers the support they need to breastfeed, programs that educate and provide support to mothers, as well as education and training in breastfeeding for all health professionals that provide health care for mothers and children are highly effective. Yet the most effective intervention to improve and maximize breastfeeding practices includes promotional activities, educations workshop, and training of health care staff along with changes of policies in health care settings. The influence of maternal education is critical at increasing breastfeeding practices and durations in SSSCs.
Conclusions
Breastfeeding is a highly cost-effective, disease-preventive intervention with a global health priority. This review suggests that breastfeeding education should be offered as part of a routine primary care component. This current review has found that even low-cost approaches to increasing knowledge of the benefits of breastfeeding among health care providers, in mothers prepartum and postpartum, and in a variety of settings have the ability to increase both knowledge of and adherence to breastfeeding. In addition, a supportive environment that includes health care professionals in both the hospital and community environments, as well as peer and community support, can impact the incidence of breastfeeding. Ensuring that messaging and education is culturally tailored has the potential to increase efficacy of breastfeeding education interventions and initiatives. Future research is needed on the impact of promoting an environment in which breastfeeding is encouraged and supported through larger public health policy initiatives and is important in creating universal support for breastfeeding mothers. This could include targeted marketing campaigns, education for extended family (such as fathers and other caregivers) and community members (such as the important role employers can play in supporting working mothers that have to pump and store breastmilk through options such as breast pumping rooms and dedicated breast milk storage), and state-sponsored education on the public health importance of breastfeeding in the media. Appropriate global policies and programs, providing breastfeeding education and counseling, as well as training health care professional should be implemented to create a positive environment for successful breastfeeding in SSSCs.
Limitations
There are some limitations to this scoping review that are worth noting. Although the authors searched several biomedical databases using various search terms, relevant intervention studies may have been missed. This review did not differentiate how many references were ascertained from each of the searched databases. Also, scoping reviews do not necessarily employ certain methodologically solid methods such as quality assessment and bias risk appraisals, as in the case of systematic reviews.
