Abstract
Capacity building and training help empower the community and population health organizations to partner with local health departments and collaboratively design multisectoral interventions that account for the complexity of public health and health promotion challenges in the era of COVID-19 and beyond. Ideally, training programs should be informed by an understanding of the needs and priorities of the professionals for whom they are intended. This brief report focuses on the results of a pilot online survey conducted as part of a larger pilot study by the New York State Association of County Health Officials and the Region 2 Public Health Training Center among population and community health professionals (n = 27) from four counties in New York State during the COVID-19 pandemic. Survey participants included a diverse group of staff members from various large and small nonprofit organizations, federally qualified health centers, academic institutions, hospitals, and insurers. Survey findings provide preliminary insights into the extent to which these organizations have been involved in the COVID-19 response in partnership with LHDs, barriers they faced in responding to the needs of the populations they serve and adjusting their work routines/operations to COVID-19 guidelines, and their top emerging organizational and training needs. Lessons learned from conducting an online survey during a public health emergency and implications for future training interventions for population and community health professionals are also discussed within the context of promoting multisectoral collaboration with local health departments, solving complex public health problems, and advancing health equity.
Keywords
Local health departments (LHDs) have been playing a critical role in the response to the COVID-19 pandemic through such activities as setting up and staffing testing sites, conducting contact tracing, and administering vaccines. In this work, they have frequently relied on collaborations with nongovernmental population and community health organizations to address community needs and reach groups experiencing marginalization or specific vulnerabilities (Hathaway et al., 2021; Michener et al., 2020).
Solving complex public health problems while advancing health, racial, and social equity increasingly involves such multisectoral collaborations, but population and community health organizations face numerous barriers to partnering effectively with LHDs—especially in the context of a public health emergency (PHE). Years of underfunding and state and federal spending restrictions have threatened the nation’s public health infrastructure and limited opportunities for growth among population and community health organizations (Ye et al., 2015).
In 2019, the New York State Association of County Health Officials (NYSACHO) and the Region 2 Public Health Training Center (Region 2 PHTC) launched a pilot audience analysis in four New York State (NYS) counties to develop strategies to engage population and community health professionals in training opportunities, inform future training programs, and ultimately build the capacity of community health organizations and strengthen their collaboration with LHDs. This brief report focuses on the COVID-19-related results of the study, and lessons learned from conducting an online survey during a pandemic.
Method
This pilot study was originally approved by Columbia University Irving Medical Center’s institutional review board (Protocol number AAAS3706) on April 11, 2019; the IRB approved the last modification on August 14, 2020.
Study Design
Researchers conducted an online pilot survey with nongovernmental population and community health professionals in four NYS counties. The survey, administered on Qualtrics, remained open from June to September 2020.
Research Instrument
Key informant interviews conducted with local health officials before the pandemic informed the development of the survey questionnaire (Schiavo et al., 2019). Beyond professional demographic information, the 35-question survey covered the priorities, opportunities, and challenges of participants’ organizations and participants’ general training needs, preferred communication methods for engagement in training opportunities, and priorities during the COVID-19 pandemic. Five questions—four multiple-choice, one open-ended—were COVID-19-related. These were added during the pandemic (IRB modification approved April 2, 2020) and informed by routine assessments by the Region 2 PHTC and NYSACHO.
Participant Recruitment
Participants were recruited from four counties, each one in a different NYS region: Suffolk (Metropolitan), Rensselaer (Capital), Chautauqua (Western), and Cortland (Central). The team used cluster sampling technique to select the four participating NYS counties. Participants included individuals from nonprofit organizations, federally qualified health centers (FQHCs), academic institutions, and hospitals.
Based on the total number of employees working at the above organizations in the four counties (n = 257,547, as determined by a review of county-level data, open-source data dashboards, institutional directories, reports from the Office of the Comptroller, and Census data), researchers calculated a sample size of 270–384 participants to achieve statistically significant findings in a large-scale survey project. This pilot survey recruited 10% of that sample size (27 participants).
Participants were recruited via a broad dissemination campaign including social media, newsletters, email, and other online and offline resources (e.g., list-servs, phone calls). Participants were asked to reply affirmatively to an informed consent question after reading about the study and before proceeding with the survey. Participation was voluntary, with participants free to skip any question.
Analysis
The research team analyzed quantitative data using Qualtrics survey data analysis tools for descriptive statistics and in some cases cross-tabulation. Two researchers analyzed qualitative data, using thematic analysis to identify and analyze means and common themes.
Results
Profile of Participants and their Organizations
Twenty-seven participants completed the pilot survey. They primarily identified themselves as working in public health (24%) or health care (48%), with some employed in nursing, social work, social services, or academia. The largest share of participants (41%) worked for FQHCs, while one in four worked at self-identified “small” nonprofits.
Of the 22 participants who answered a question about their organization’s involvement with the COVID-19 pandemic response, 18 (82%) replied affirmatively. Of these individuals, 12 (67%) said their organizations were involved in partnership with an LHD. See Table 1 for characteristics of survey respondents and their organizations.
Profile of Survey Respondents and their Organizations
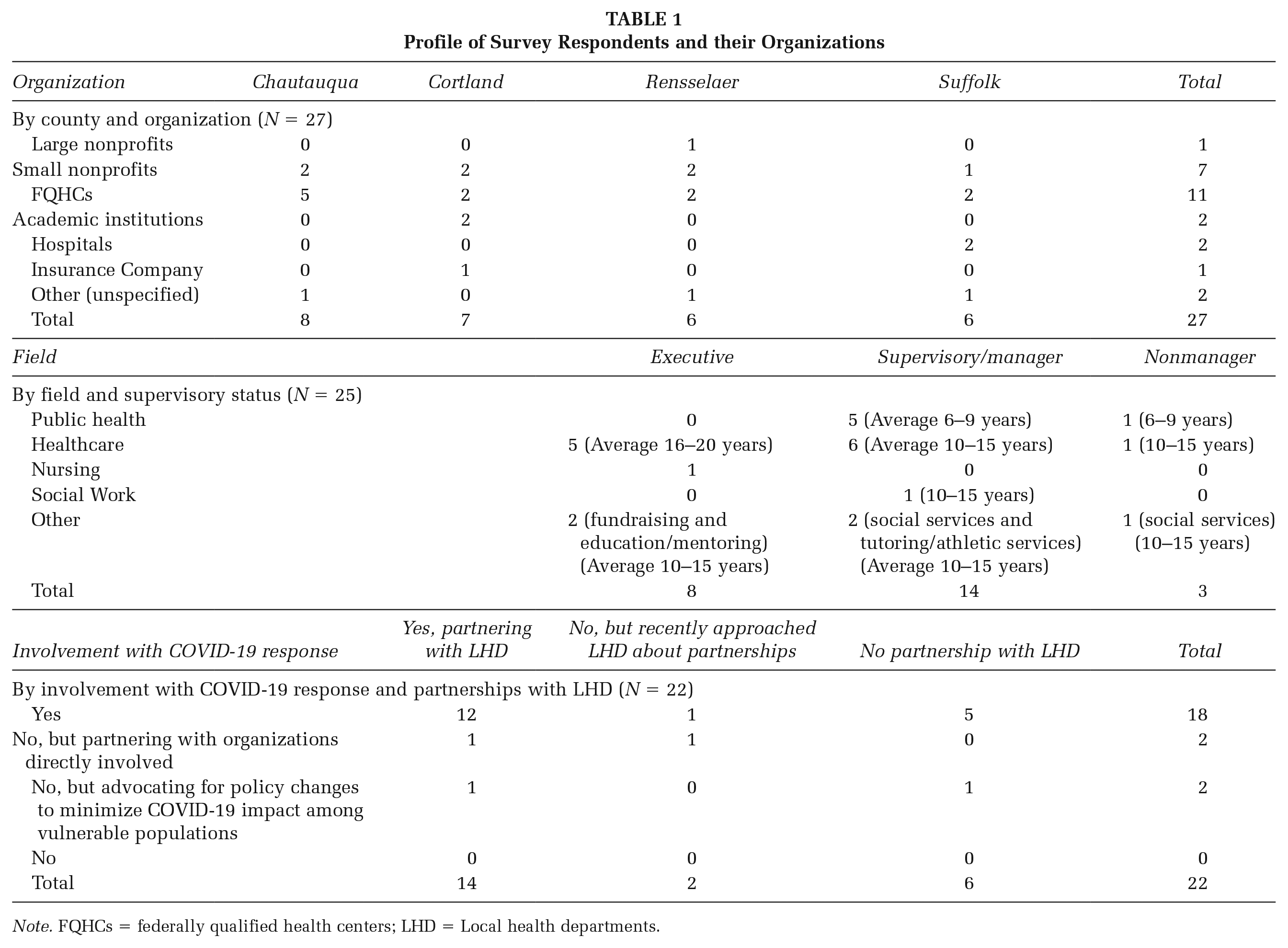
Note. FQHCs = federally qualified health centers; LHD = Local health departments.
COVID-19 Emerging Needs and Priorities: A Preliminary Look into Barriers
Participants identified up to five barriers that were making it difficult to respond to the pandemic and the needs of the communities they serve. Limited funding accounted for 22.5% (9/40) of responses. Other frequently identified barriers included misinformation/lack of information consistency (12.5%, 5/40), weak communication systems (10%, 4/40), and current organizational systems (10%, 4/40). The relevance of such barriers varied across organizational type and county. Limited funding was, for example, identified as a top barrier among small nonprofits, FQHCs, and academic institutions, while existing community barriers to implementing recommended measures was a barrier primarily among respondents from large nonprofits.
In identifying barriers to their organizations’ adjustment of work routines/operations to COVID-19 guidelines, survey participants from all four counties again highlighted misinformation/lack of information consistency (23%, 7/31 responses) as one of the five most notable barriers; misinformation may have disproportionately affected FQHCs, employees of which contributed five responses. Other notable barriers were limited organizational preparedness for remote activities, limited staff, lack of clarity about roles and responsibilities (12.9%, 4/31 each), as well as changes in the political climate (9.7%, 3/31). All participants who identified limited organization preparedness for remote activities as a barrier were working for small or large nonprofit organizations. See Figure 1 for a breakdown of the number of responses by each barrier to meeting community needs and adjusting work operations during the pandemic.
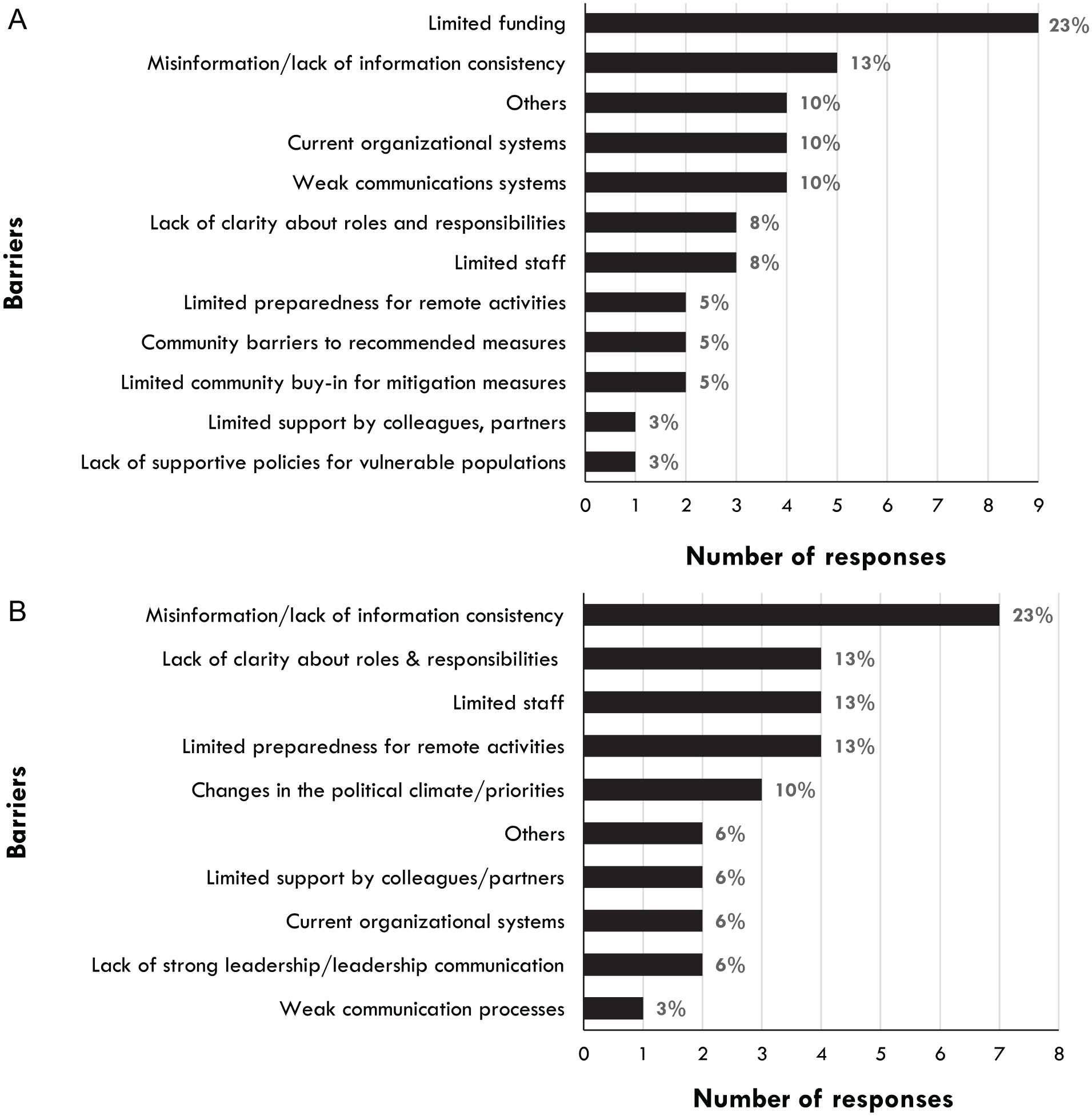
Number of Responses by Each Barrier: (A) Number of Responses by Each Barrier to Responding to the COVID-19 Pandemic and Tending to Community Needs and (B) Number of Responses by Each Type of Barrier to Adjusting Work Routines/Operations to COVID-19 Guidelines
A Preliminary Look into Top Organizational and Training Needs during the Pandemic
Table 2 summarizes top organizational and training needs that have emerged during the COVID-19 pandemic for different types of organizations, as indicated by survey participants in reply to open-ended questions. These training needs resonate with key domains for core skillsets by The Public Health Foundation, Council on Linkages between Academia and Public Health Practice (2014), and key strategic skills areas by the de Beaumont Foundation (2017) as rated by survey respondents (Schiavo et al., 2020).
Top Emerging Organizational and Training Needs
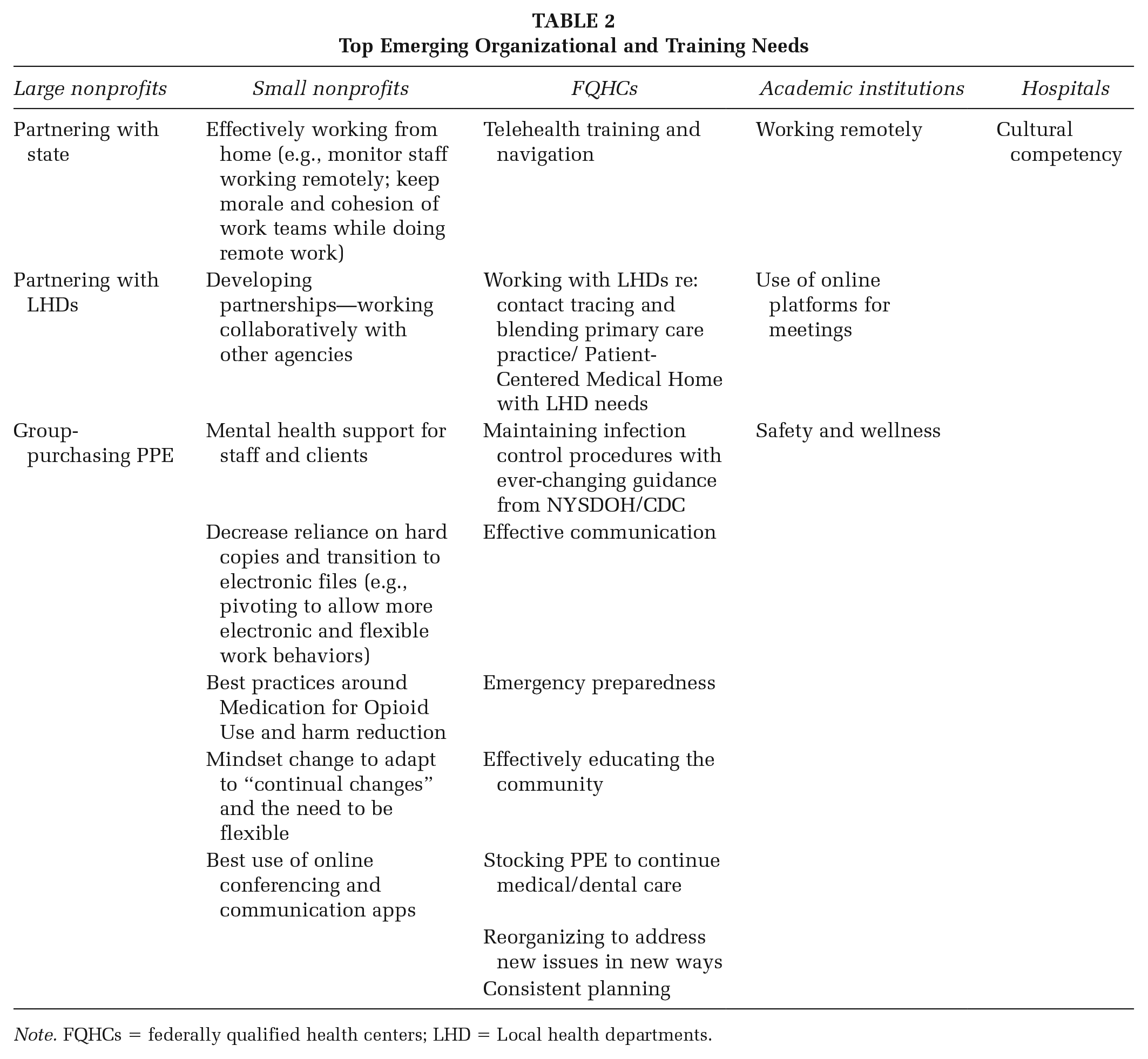
Note. FQHCs = federally qualified health centers; LHD = Local health departments.
Large and small nonprofits and FQHCs all identified the development of skills to partner with state and local stakeholders as a top need (Schiavo et al., 2020). Other needs described by participants were either topic- or organization-specific, such as training on best practices around medication used for opioid use and harm reduction, strengthening organizational systems for remote work, and providing services via telehealth.
Discussion
Priorities and Needs of Population and Community Health Organizations During the Pandemic
Findings from this pilot study provide the first look at the priorities and needs of these professionals in one small U.S. region during the COVID-19 pandemic.
The fact that the majority of survey participants who described their organizations as being involved in pandemic response reported their organizations as doing so in partnership with a LHD confirms the key premise of this study: Consideration should be given to increasing capacity-building efforts to enhance multisectoral partnerships, as these are at the core of advancing health equity (Schiavo et al., 2018) and addressing the COVID-19 pandemic (Chen et al., 2020). Study participants identified the development of skills to partner with other state and local stakeholders as a top training need for their organizations in the context of the pandemic.
Participants reported limited funding as a key barrier to responding to the PHE and the needs of the community groups they serve. Unfortunately, even that limited funding often “dries up when there is no epidemic to worry about” (Chen et al., 2020), leaving LHDs and their partners without the resources and skills they will need for future epidemic surveillance, control, and recovery efforts.
Notably, survey participants also identified the political climate as a barrier to adjusting their work routines/operations to COVID-19 guidelines. “Politics, economics, and public policy are important determinants of population health,” according to McCartney et al. (2019), as they influence all kinds of investment in organizational capacity, and health and social systems. Sustaining such systems may require increased outreach and advocacy to engage governmental and nongovernmental grantmakers in consistently prioritizing infectious disease outbreak preparedness (National Academy of Medicine, Secretariat, Commission on a Global Health Risk Framework for the Future, 2016).
With survey participants pointing to misinformation/lack of information consistency as a barrier to both responding to the needs of community groups during the pandemic and adjusting work routines/operations to COVID-19 guidelines, this study also highlights the need for strong communication systems during a PHE. Risk communication has emerged as an important skill set for the public health workforce and their population and community health partners during the pandemic (Schiavo, 2020; Schiavo et al., 2014), and training interventions may help local leaders and organizations address misinformation and mitigate the “trust crisis” among populations that have historical reasons for their distrust of health and social systems (World Health Organization, 2020).
With the ability to work remotely now a priority for many population and community health professionals, it is also critical that organizations build their capacity to support employees collaborating from home.
Challenges of and Strategies for Conducting an Online Survey During a PHE
Administering an online survey during a PHE presented unique challenges and resulted in important lessons learned. After adding a series of COVID-19-related questions to the original instrument, we found that study recruitment took longer than expected, based on similar experiences, and a number of respondents who began the survey did not meet the eligibility criteria listed on online advertisements. In moving forward, researchers should consider using short prescreening, web-based forms for survey eligibility questions, to minimize the time spent on such questions. Our team also found that recruitment efforts were more successful via interpersonal channels (e.g., individual and group emails, phone calls) than through social media and web-based outreach. The participation of a membership or community-based organization with strong interpersonal ties—such as NYSACHO—can be key to efficient study recruitment, especially during a time of crisis.
Our survey’s timing also affected response rates to different questions. Unsurprisingly, COVID-19-specific questions elicited the highest response rate, followed by questions on priority health and social issues at organizational levels, and training needs. Open-ended questions, which were more time-intensive, and questions on training logistics and communication preferences, which may have proved challenging to answer due to the evolving nature of the pandemic and related guidelines, yielded a low response rate.
Overall, our experience indicates that it may be important to conduct pilot studies to anticipate potential issues during a PHE and assess optimal duration and procedures for future studies.
Limitations of This Study
Given the pilot nature of this study and limited sample size, results are not generalizable to the counties of focus, New York State, or the United States.
Another limitation of this study is its novelty: As far as we know, no other work has been published in the peer-reviewed literature on emerging needs and priorities of nongovernmental population and community health professionals from any regional or local perspective during the pandemic. We were, therefore, unable to contextualize our findings with results from similar assessments.
Implications for Future Training Interventions and Practice
Results and lessons learned from this online survey can be used to inform future training programs for nongovernmental population and community health professionals working in partnership with LHDs to address community needs during PHEs, overcome barriers to collaboration, and improve the administration of online assessments in emergency situations.
The call for capacity building, coordinated efforts, a strong focus on regional public health systems, and multisectoral collaborations issued 10 years after the 2002-2003 Severe Acute Respiratory Syndrome outbreak (Koplan et al., 2013) “still stands true” (Chen et al., 2020), because, in the words of one survey participant, “no one agency can be the answer for everyone.” We should meet this call by equipping LHDs and their community partners with the skills and resources for building back better, advocating for new policies, establishing stronger collaborations, and addressing the pandemic’s disproportionate health and economic burden on communities experiencing marginalization or disadvantage. If not now, when?
Supplemental Material
sj-docx-1-hpp-10.1177_15248399211065412 – Supplemental material for Barriers to Meeting Community Needs in New York State during COVID-19: Results From a Pilot Survey of Nongovernmental Population and Community Health Professionals
Supplemental material, sj-docx-1-hpp-10.1177_15248399211065412 for Barriers to Meeting Community Needs in New York State during COVID-19: Results From a Pilot Survey of Nongovernmental Population and Community Health Professionals by Renata Schiavo, Mayela Arana, Nicole Levy, Yesenia Grijalva, Sarah Ravenhall, Margaret DiManno and Marita Murrman in Health Promotion Practice
Footnotes
Authors’ Note:
The authors thank Samantha Cinnick, formerly the Center’s Coordinator at the Region 2 PHTC, for her contribution to the preliminary design and initial stages of this project. This project is supported by the Health Resources and Services Administration (HRSA) of the U.S. Department of Health and Human Services (HHS) under grant number UB6HP31686, Regional Public Health Training Center Program for $767,470.00 (2022). This information or content and conclusions are those of the author and should not be construed as the official position or policy of, nor should any endorsements be inferred by HRSA, HHS, or the U.S. Government.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
