Abstract
Sexual minority women (SMW; e.g., lesbian, bisexual) report higher rates of almost every negative physical health (e.g., asthma, arthritis, cardiovascular disease), mental health (e.g., depression, anxiety), and substance use outcome compared to heterosexual women. Adverse Childhood Experiences (ACEs) have been identified as risk factors for negative health outcomes. Despite this, no study to date has synthesized existing literature examining ACEs and health outcomes among SMW. This gap is important because SMW are significantly more likely than heterosexual women to report every type of ACE and a higher total number of ACEs. Therefore, using a scoping review methodology, we sought to expand understanding of the relationship between ACEs and health outcomes among SMW. Using the Preferred Reporting Items for Systematic reviews and Meta-Analyses extension for. Scoping Reviews protocol, we searched five databases: Web of Science, PsycInfo, CINAHL, PubMed, and Embase for studies published between January 2000 and June 2021 that examined mental health, physical health, and/or substance use risk factors and outcomes among adult cisgender SMW who report ACEs. Our search yielded 840 unique results. Studies were screened independently by two authors to determine eligibility, and 42 met full inclusion criteria. Our findings provide strong evidence that ACEs are an important risk factor for multiple negative mental health and substance use outcomes among SMW. However, findings were mixed with respect to some health risk behaviors and physical health outcomes among SMW, highlighting the need for future research to clarify these relationships.
Introduction
A rapidly growing body of literature documents substantial sexual orientation-related physical and mental health disparities. Compared to heterosexual women, sexual minority women (SMW; e.g., lesbian, bisexual, other non-heterosexual identity) are at higher risk of negative substance use and mental health issues. For example, they report higher rates of tobacco use (Caceres et al., 2019; Conron et al., 2010; Fredriksen-Goldsen et al., 2013; Matthews et al., 2014) and higher rates of almost every measure of alcohol misuse (e.g., alcohol dependence, heavy episodic drinking, intoxication) (Hughes et al., 2020). In an earlier systematic review, King and colleagues (2008) found that compared to heterosexual women, SMW had 3.42 times the risk of any substance use disorder (SUD), 3.50 times the risk of drug dependence, and 4.00 times the risk of alcohol dependence (King et al., 2008). These authors also found substantial mental health disparities. Specifically, SMW had 2.13 times the risk for past-12-month depression and 1.66 times the risk for past-12-month anxiety compared to their heterosexual counterparts (King et al., 2008). More recent reviews, such as those of Plöderl and Tremblay (2015) and Wittgens et al. (2022), have documented similarly large disparities between heterosexual and SMW’s outcomes. In addition, SMW have higher rates of many physical health conditions, such as asthma, arthritis, and cardiovascular disease (Caceres et al., 2017; Conron et al., 2010; Dilley et al., 2010; Fredriksen-Goldsen et al., 2012; Simoni et al., 2017; Veldhuis et al., 2019); body mass index of 25 or above (Caceres et al., 2019; Conron et al., 2010; Fredriksen-Goldsen et al., 2013; Simoni et al., 2017); higher hemoglobin A1C values (which increases risk of Type 2 diabetes) (Caceres et al., 2019); and poorer self-reported physical and mental health (Fredriksen-Goldsen et al., 2012, 2013; Simoni et al., 2017; Wallace et al., 2011).
Disparities in SMW’s health are often attributed to sexual minority (SM) stress, which is the predominant theory of how stressors related to identifying as a SM (e.g., discrimination, stigma, internalized homophobia) contribute to negative health outcomes among SM people (Meyer, 2003). Further, preliminary research has documented that SMW who hold multiple marginalized identities and are exposed to multiple intersecting forms of oppression (e.g., racism, sexism, homophobia, xenophobia) (Crenshaw, 1990) are at even greater risk for poor health outcomes (Aranda et al., 2015; Balsam et al., 2011; Bowleg et al., 2003; Caceres et al., 2021; Li et al., 2015; Ramirez & Paz Galupo, 2019; Veldhuis et al., 2020).
Although SM stress is the most commonly cited explanation for SMW’s heightened risk, it does not fully account for sexual orientation-related health disparities. Adverse childhood experiences (ACEs, e.g., childhood sexual abuse [CSA], childhood physical abuse [CPA], childhood poverty, incarceration of a family member, witnessing violence) have been identified as key risk factors in the development of negative health outcomes among people in the general population. For example, studies across diverse samples of adults in the general population have found that ACEs are associated with myriad negative physical health, mental health, and substance use outcomes (Iniguez & Stankowski, 2016; Mersky et al., 2013; Monnat & Chandler, 2015). In one U.S. national sample, ACEs were associated with poor self-rated health, functional limitations, diabetes, and heart attack as adults (Monnat & Chandler, 2015). In a large, regional sample of adults, there was a dose-response relationship between the number of ACEs and moderate to heavy drinking, drug use, depressed affect, and suicide attempts (Merrick et al., 2017).
However, far fewer studies have examined the relationship between ACEs and negative health outcomes among SMW. This gap is important because SMW appear to be more likely than heterosexual women to report several ACEs, including CPA, CSA, neglect, household dysfunction, and bullying (Alvy et al., 2013; Austin et al., 2008a; Friedman et al., 2011; Giano et al., 2020; McCabe et al., 2020a, 2020b; Merrick et al., 2018; Wilsnack et al., 2008; Zou & Andersen, 2015). For example, in a national sample of U.S. adults, reports of CPA were highest among lesbian (45.5%) and bisexual (47.5%) women, and women unsure of their sexual identity (51.6%), compared to 32.9% of heterosexual women (McCabe et al., 2020b). Additionally, there is some evidence that SMW experience a greater number of types of ACEs (Austin et al., 2008a, 2020b; Zou & Andersen, 2015) and more severe forms of childhood victimization than heterosexual women (Alvy et al., 2013; Wilsnack et al., 2012). Specifically, in one recent study, McCabe et al. (2020b) found that lesbian and bisexual women consistently reported significantly higher numbers of ACEs compared to heterosexual women, with lesbian and bisexual women reporting an average of 2.8 (95% CI [2.5, 3.1]) and 3.3 (95% CI [2.9, 3.6]) compared to heterosexual women, who reported an average of 2.1 (2.0–2.1) ACEs. With respect to severity of ACEs, Alvy and colleagues (2013) found that compared to heterosexual women, SMW reported more severe forms of CPA (e.g., being beaten, punched, or choked) and Wilsnack and colleagues (2012) found that they reported more severe forms of CSA (e.g., earlier age of onset, greater frequency, longer duration). While few studies to date have examined factors contributing to SMW’s increased risk of ACEs, preliminary research suggests that SMW may be more likely to engage in gender non-conforming behaviors or expression which may, in turn, place them at greater risk for ACEs (Lehavot & Simoni, 2014; Roberts et al., 2005; Rosario et al., 2022). However, there is no consensus of opinion on why SMW report higher rates of ACEs compared to heterosexual women, highlighting a need for future research in this area.
Despite the growing number of studies focusing on ACES among SMW, to our knowledge, there have been no reviews summarizing the current state of the literature on ACEs and health outcomes among SMW—a necessary step toward a greater understanding of SMW’s heightened risk of negative health outcomes and the development of targeted prevention and/or intervention strategies. Therefore, we conducted a scoping review guided by the following research question: “What is the current state of knowledge about the links between ACEs and mental health, physical health, and substance use among SMW?” We also aimed to identify gaps and weaknesses in the existing literature to guide future research and to support recommendations for research, policy, and practice to address sexual orientation-related health disparities among women.
Methods
Protocol and Eligibility Criteria
Following the Joanna Briggs Institute (JBI) guidelines for conducting scoping reviews (Peters et al., 2020), we developed a protocol (available upon request from the corresponding author) to screen articles for study inclusion (see Figure 1). Inclusion criteria included empirical, quantitative, or mixed methods peer-reviewed studies published in English between January 2000 and June 2021 examining mental health, physical health, and/or substance use risk factors and outcomes among adult (ages 18 or older) cisgender SMW who report ACEs. We selected 2000 as the beginning year of study inclusion given that the U.S. Institute of Medicine released its landmark report focused on lesbian health research 1 year earlier (Solarz, 1999), which resulted in substantial growth of research focused on SM women’s health. We included studies of women who identified as lesbian, bisexual, mostly heterosexual, or another non-heterosexual identity (we did not include studies that assessed only sexual attraction and/or behavior). We only included studies that used identity to measure minority sexual orientation (rather than sexual attraction or behavior) as minority-specific stress has been shown to be most strongly and consistently associated with identification as a SM, rather than attraction or behavior (Krueger et al., 2018). Studies that included both SM individuals who were younger and older than age 18 or included sexual minority men (SMM), but reported outcomes for adult SMW separately, were eligible for inclusion. Studies that focused exclusively on transgender or nonbinary individuals were excluded unless the study also assessed and reported on sexual identity. Additionally, studies were excluded if they did not assess ACEs, or if ACEs were included as a covariate, not a primary exposure variable.
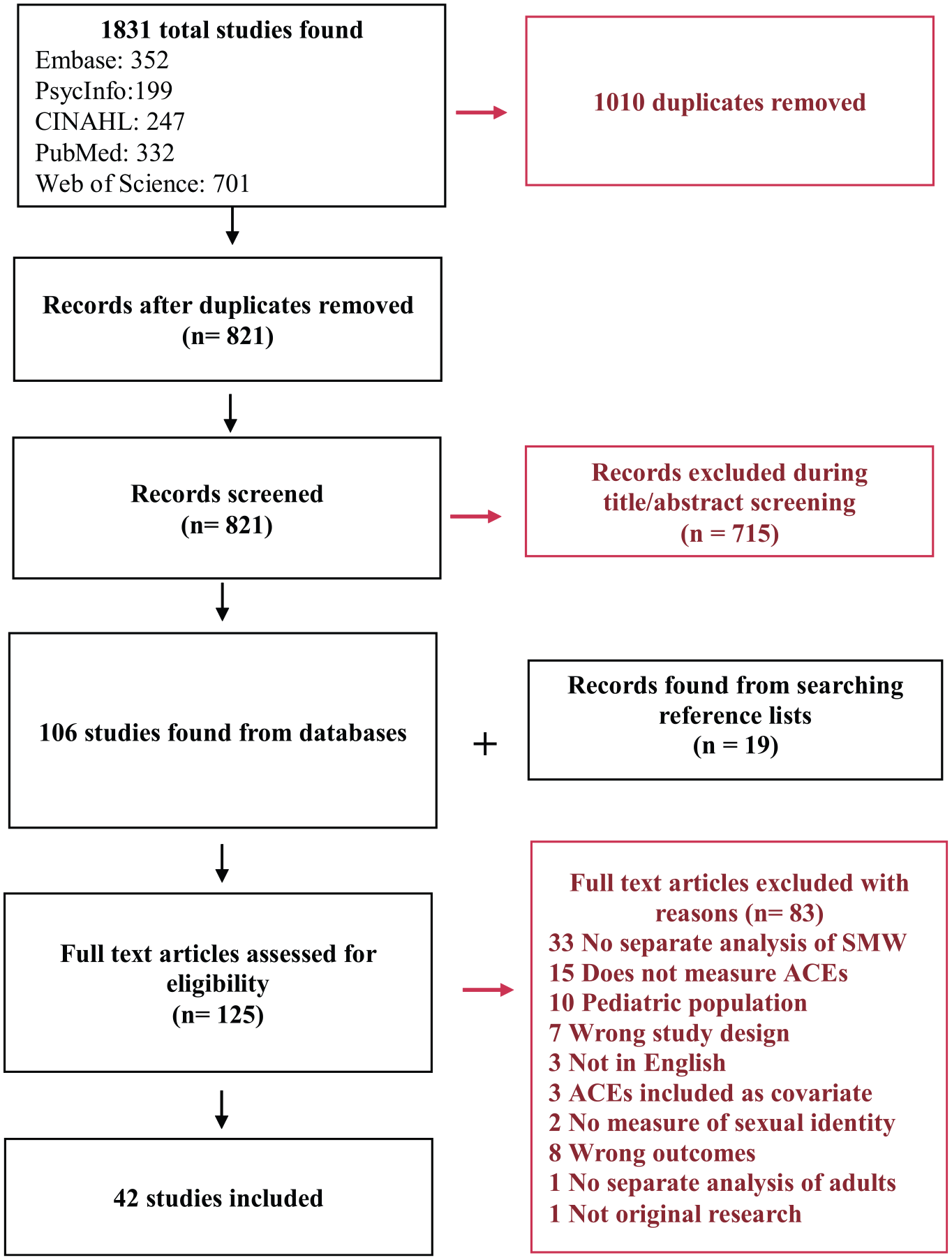
PRISMA-ScR table.
In July 2021, we searched five databases (Web of Science, PsycInfo, CINAHL, PubMed, and Embase). Table 1 shows the search terms used across databases (slight modifications were made to the organization of the search query to meet requirements of individual databases). Our search resulted in 1,831 references. Duplicate references were removed using Covidence, an online systematic review manager, resulting in 821 unique references. Next, two authors independently conducted a title/abstract screening and removed studies that did not meet eligibility criteria. At this stage, there was approximately 92% agreement between authors. We then examined the reference lists of each article meeting inclusion criteria to identify additional articles, resulting in 19 additional studies. We screened 125 studies for eligibility via full-text review. In the full-text review stage, there was 83% agreement between authors. A third researcher resolved discrepancies in inclusion/exclusion decisions during the abstract and full-text screening stage. We removed an additional 84 studies during full-text screening, leaving 42 for the final review. Reasons for exclusion during the full-text review stage included: study results aggregated across groups (e.g., sexual identity groups, age groups, or SMW and SMM) and ACEs not explicitly or separately measured (e.g., included only a lifetime trauma variable).
Search Terms.

Data Extraction, Analysis, and Synthesis
Using JBI methodology (Peters et al., 2020), we charted the data using a data extraction form developed by the full team of authors. Each author conducted data charting independently; however, all studies were reviewed in duplicate to ensure internal consistency in review procedures. For each study, we charted the following: study design, sample size, participant demographics, dependent variable(s), independent variable(s), and main outcomes. Data were then summarized by major themes and gaps in the literature were identified.
Results
Description of Included Studies
Table 2 provides an overview of the included studies (e.g., sample characteristics, study design). The range of sample sizes of the included studies was 85 to 36,309, with a median of 703 and a mean of 5,273. Twenty-two studies included heterosexual comparison groups, and the remainder included only sexual minorities in their samples. Of the 42 included articles, 11 focused exclusively on mental health outcomes, 13 on alcohol and/or other substance use, 13 on physical health outcomes, two on revictimization and other experiences of violence, two focused on both mental health and alcohol use, one focused on mental and physical health, and one examined financial health (defined as having the economic resources to meet one’s basic physical needs). Thirty-seven studies used cross-sectional and four used longitudinal designs. Two of the studies employed mixed methods and the remainder used solely quantitative methods. Most (n = 39) studies were conducted in the U.S. Three studies were conducted outside of the U.S., one included participants from both the U.S. and Canada (Crump & Byers, 2017), another was based exclusively in Canada (Persson et al., 2015), and the third in Australia (Zietsch et al., 2012).
Overview of Study Design and Sample Characteristics.
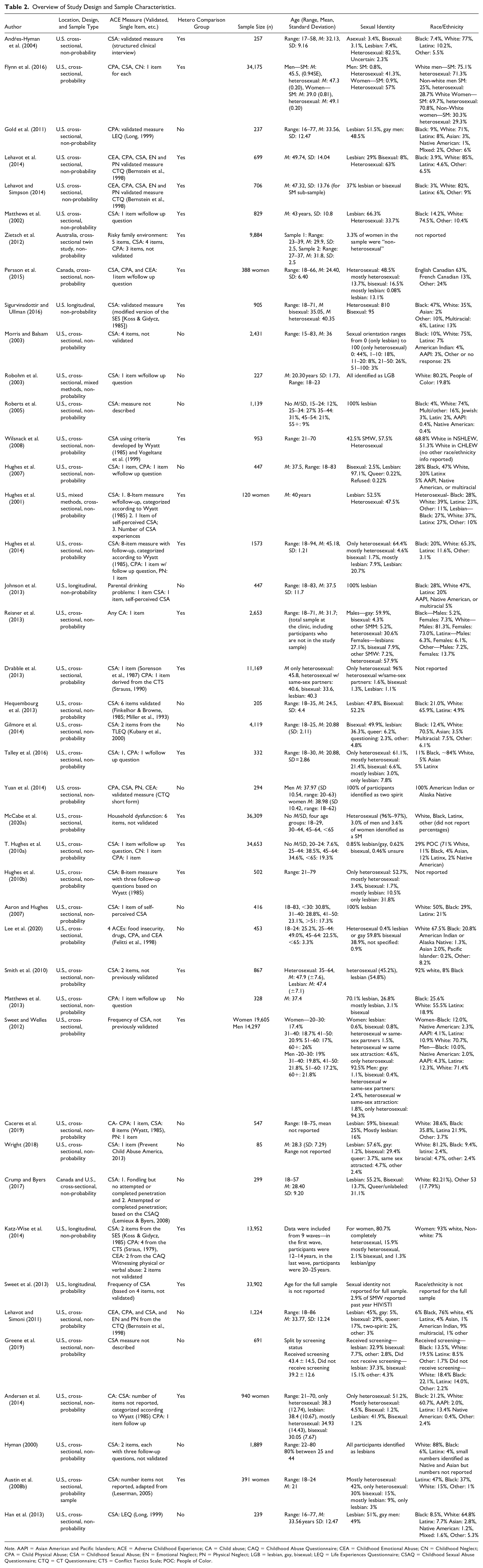
Note. AAPI = Asian American and Pacific Islanders; ACE = Adverse Childhood Experience; CA = Child abuse; CAQ = Childhood Abuse Questionnaire; CEA = Childhood Emotional Abuse; CN = Childhood Neglect; CPA = Child Physical Abuse; CSA = Childhood Sexual Abuse; EN = Emotional Neglect; PN = Physical Neglect; LGB = lesbian, gay, bisexual; LEQ = Life Experiences Questionnaire; CSAQ = Childhood Sexual Abuse Questionnaire; CTQ = CT Questionnaire; CTS = Conflict Tactics Scale; POC: People of Color.
Some studies used validated scales to measure exposure to ACEs; five used batteries of questions from Wyatt’s (1985) revised Wyatt Sex History Questionnaire (Aaron & Hughes, 2007; Hughes et al., 2001, 2007, 2010b; Wilsnack et al., 2008), four used Bernstein and colleagues (1998) full or shortened Childhood Trauma Questionnaire (Katz-Wise et al., 2014; Lehavot et al., 2014; Lehavot & Simpson, 2014; Yuan et al., 2014), one study used CSA questions from Long (1999)’s Life Experiences Questionnaire (Gold et al., 2011), another used Kubany et al.’s (2000) Traumatic Life Events Questionnaire (Gilmore et al., 2014), one used the Conflict Tactics Scale developed by Strauss (1990) (Drabble et al., 2013), and another Koss and Gidycz’s (1985) Sexual Experiences Survey (Sigurvinsdottir & Ullman, 2016). The majority of studies used a single question or a set of investigator- or clinician-developed questions regarding specific ACEs, some of which were adapted from validated scales. One study did not specify how exposure to ACEs was measured (Greene et al., 2019).
A range of theoretical frameworks guided the studies (see Table 3). Researchers used Minority Stress Theory as a guiding framework in 15 of the studies (Caceres et al., 2019; Drabble et al., 2013; Flynn et al., 2016; Hequembourg et al., 2013; T. L. Hughes et al., 2001; T. L. Hughes et al., 2014; T. Hughes et al., 2010a; T. L. Hughes et al., 2010b; Katz-Wise et al., 2014; Lehavot & Simpson, 2014; McCabe et al., 2020a; Persson et al., 2015; Sigurvinsdottir & Ullman, 2016; Wilsnack et al., 2008; Wright, 2018), and four studies used Self-Medication Hypothesis (Gilmore et al., 2014; Johnson et al., 2013; Lehavot et al., 2014; Talley et al., 2016). The following theories or frameworks were each used in one study: Emotional Processing Theory (Gold et al., 2011), the Traumagenic Dynamics Model (Crump & Byers, 2017), traumatic sexualization (Robohm et al., 2003), which is part of the Traumagenic Dynamics model, the Social Norms Approach to Drinking (Gilmore et al., 2014), Intersectionality Theory (Greene et al., 2019), common cause explanations (Zietsch et al., 2012), protective measures theory (Smith et al., 2010), life course (Reisner et al., 2013), and socialization and human capital formulations of financial earnings (Hyman, 2000). However, 15 of the included studies did not explicitly mention a theoretical framework (Aaron & Hughes, 2007; Andersen et al., 2014; Andrés-Hyman et al., 2004; Austin et al., 2008b; Han et al., 2013; Hughes et al., 2007; Lehavot & Simoni, 2011; Matthews et al., 2002, 2013; Morris & Balsam, 2003; Roberts et al., 2005; Sweet & Welles, 2012; Sweet et al., 2013; Yuan et al., 2014).
Theoretical Frameworks, Prevalence of Abuse, and Study Outcomes.
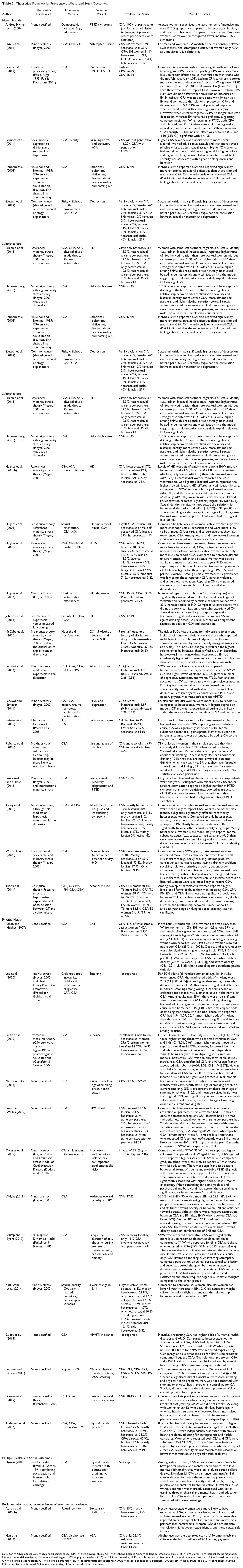
Note. CA = Child abuse; CSA = childhood sexual abuse; CPA = child physical abuse; CN = childhood neglect; CEA = childhood emotional abuse; TS = two-spirit; IH = internalized homophobia; EA = experiential avoidance; EN = emotional neglect ; PN = physical neglect; CTQ = CT Questionnaire; SUDs = substance use disorders; AUD = alcohol use disorder; HD = hazardous drinking; CV = childhood victimization; CT = childhood trauma; PTSD = posttraumatic stress disorder; ACE = adverse childhood experiences (ACEs); BMI = Body Mass Index; CI = confidence interval; LGB = lesbian, gay, bisexual; SM = sexual minority; SMW = sexual minority women.
In the following five sections, study findings are synthesized and categorized by themes.
Mental Health
Eleven studies examined the relationship between ACEs and negative mental health outcomes, including suicidal thoughts and/or behavior (e.g., attempts/ideation) (Flynn et al., 2016; Matthews et al., 2002), symptoms of posttraumatic stress disorder (PTSD) (Andrés-Hyman et al., 2004; Caceres et al., 2019; Gold et al., 2011; Lehavot & Simpson, 2014; Sigurvinsdottir & Ullman, 2016), depression (Hughes et al., 2014; Persson et al., 2015; Zietsch et al., 2012), emotional/behavioral difficulties (Robohm et al., 2003), psychological distress (Hughes et al., 2007; Morris & Balsam, 2003), and experiential avoidance (i.e., the desire to avoid emotions, cognitions, or body sensations related to painful events) (Gold et al., 2011). Overall, the results of these studies indicate that ACEs are significantly associated with depression, psychological distress, PTSD symptoms, and suicidal ideation and attempts among SMW.
Suicidal Thoughts and Behaviors
Matthews et al. (2002) and Flynn et al. (2016) examined the relationship between CPA and CSA and suicidal thoughts and behaviors (e.g., ideation and attempts). In their study of 829 lesbian and heterosexual women, Matthews et al. (2002) found that CSA was significantly associated with suicidal ideation among all participants; however, CSA was only significantly associated with suicide attempts among lesbian women. Similarly, CPA was associated with suicidal ideation among all participants, but CPA was only associated with suicide attempts among lesbian women. In Flynn et al. (2016)’s study of 34,175 SM and heterosexual men and women, CSA mediated the relationship between lesbian, gay, bisexual (LGB) identity and attempted suicide for men and women; CPA mediated the relationship between sexual identity and suicide for SMW only.
Posttraumatic Stress Disorder
Four studies examined the relationship between CSA and symptoms of PTSD. In a study of 257 SMW and heterosexual women CSA survivors, Andrés Hyman et al. (2004) found that asexual women reported the lowest number of intrusive and total PTSD symptoms among all groups (i.e., asexual, heterosexual, lesbian, and bisexual). Further, compared with African American/Black, White, and other racial/ethnic minority women, Latina women reported the fewest intrusive PTSD symptoms. In a longitudinal study of the relationship between race, sexual identity, and PTSD symptoms, Sigurvinsdottir and Ullman (2016) found that Black bisexual women and non-Black bisexual women reported the highest levels of PTSD symptoms compared to all heterosexual women. Lehavot et al. (2014) found in their sample of 706 SM and heterosexual veterans that lesbian and bisexual women were more likely than heterosexual women to report childhood victimization (i.e., CPA, CSA, childhood emotional abuse, emotional neglect, and physical neglect). In logistic regression models, childhood trauma and trauma experienced during military service added the most variance to models examining PTSD and depression. Finally, in a study of lifetime trauma, cardiometabolic risk, and psychosocial risk factors, Caceres et al. (2019) found significant associations between all forms of trauma (CPA, CSA, childhood parental neglect, physical abuse, sexual abuse, and intimate partner violence) and probable PTSD diagnosis. Study participants who reported trauma (i.e., childhood and/or adult) also reported lower perceived social support.
Depression
In an Australian study examining mental health in twin pairs (N = 9884 individuals), in both male and female twins, pairs of one heterosexual and one SM twin had higher rates of depression than did pairs of heterosexual twins. CSA partially explained the correlation between sexual identity and depression (Zietsch et al., 2012). There were no differences based on sex. In a study conducted with a community-based sample of SMW, Caceres et al. (2019) found that childhood and lifetime trauma were significantly associated with higher odds of depression (OR: 1.41; CI [1.12, 1.77]). Persson et al. (2015) examined the relationship between sexual identity and depression and anxiety in a sample of 388 heterosexual and SM women. The relationships of sexual identity with depression and anxiety were mediated by sexual orientation disclosure and risky sexual behavior: lower levels of disclosure and higher levels of risky sexual behavior were positively associated with higher levels of depression and anxiety. Childhood abuse did not mediate this relationship. The authors hypothesized that the lack of association may have been due to collapsing three childhood abuse variables (CSA, CPA, and psychological abuse), potentially masking differences between the forms of abuse assessed. Johnson et al. (2013) found a direct relationship between CSA and depression in a sample of 443 SMW. Additionally, using data from a pooled sample in a study of SMW in Chicago and women from a national general population study (that included both heterosexual and SM women), Hughes and colleagues (2014) found that compared to participants who did not report victimization, those who reported childhood victimization (i.e., CSA, CPA, parental neglect) were significantly more likely to report depression.
Other Psychological Outcomes
Using data from a national U.S. sample of 2,431 SMW, Morris and Balsam (2003) found that history of CSA was associated with current psychological distress (measured using a scale developed by Derogatis & Spencer, 1982). In a study of 227 lesbian and bisexual women, Robohm et al. (2003) found that SMW who reported CSA reported significantly more emotional/behavioral difficulties than those who did not report CSA. Gold et al. (2011) compared lesbian women and gay men, and found that lesbian women were more likely to endorse CPA; those reporting CPA were more likely to report lifetime sexual victimization. Lesbian CPA survivors also reported more symptoms of depression and PTSD (e.g., experiential avoidance or the desire to avoid emotions, cognitions, or body sensations related to painful events) than those who did not report CPA. Among lesbian women, CPA was not associated with internalized homophobia, nor did internalized homophobia mediate the relationship between CPA and depression or PTSD symptoms. However, experiential avoidance mediated the relationships between CPA and depression and CPA and PTSD. Finally, Hughes et al. (2007) found that CPA had a direct relationship with psychological distress (defined as combination of two negative mood states: depression and anxiety).
Substance Use
Fifteen studies examined the relationship between ACEs and substance use-related problems (Drabble et al., 2013; Gilmore et al., 2014; Hughes et al., 2007, 2010a, 2010b; Lehavot et al., 2014; McCabe et al., 2020a; Reisner et al., 2013; Roberts et al., 2005; Wilsnack et al., 2008; Yuan et al., 2014). Of these, 11 focused exclusively on alcohol-related outcomes and four examined both alcohol and other drug use outcomes. Five of the fifteen studies used data from the Chicago Health and Life Experiences of Women (CHLEW) study, a longitudinal study of more than 800 SMW (447 from Wave 1 and a supplemental sample of 368 SMW added in Wave 3). Together, results of these studies provide compelling evidence that ACES are associated with substance use outcomes among SMW.
In a small pilot study, Hughes et al. (2001) found that compared to heterosexual women (n = 57), lesbian women (n = 63) reported more forms of CSA (range = 0–8; e.g., sexual kissing, fondling, intercourse), were more likely to meet criteria for CSA based on Wyatt’s (1985) definition, and to define their experiences as CSA. Among both lesbian and heterosexual women, CSA was associated with lifetime alcohol abuse. Using data from an internet-based survey of 699 U.S. veterans, Lehavot et al. (2014) examined mediators of sexual orientation-related disparities in alcohol misuse among heterosexual and SM women veterans. Lesbian and bisexual women were more likely than their heterosexual counterparts to report childhood victimization (emotional, physical, and sexual abuse; emotional and physical neglect) and more severe forms of victimization. They were also more likely to report alcohol misuse, greater number of depressive symptoms, and worse symptoms of PTSD. Path analysis revealed that childhood victimization was associated with depressive symptoms, PTSD symptoms, and alcohol misuse. Minority sexual identity was also indirectly associated with alcohol misuse via childhood trauma and depression, civilian physical victimization and PSTD, and military physical victimization, depression, and PSTD. Similarly, in a national sample of 4,119 SMW, Gilmore et al. (2014) found that more severe forms of CSA (i.e., involving penetration) were indirectly associated with greater number of drinks consumed per week and higher perceived peer norms for drinking (i.e., estimation of the number of drinks that lesbian/bisexual women consume daily).
In a study of 1,139 lesbian women from the Boston Lesbian Health Project, Roberts et al. (2005) found that 12% self-identified as alcoholic. Among these participants, 67% reported CSA, compared with 47% of those who did not report alcoholism. No results of statistical analyses were reported in this study. In a later study using a community sample of SM and heterosexual men and women, Reisner et al. (2013) found that lesbian and bisexual women reported greater substance misuse than heterosexual women, and that sexual orientation-related disparities in substance misuse were mediated by childhood abuse.
Using data from a college sample of 332 women, Talley et al. (2016) found that compared with all other sexual identity subgroups (i.e., exclusively gay/lesbian, mostly lesbian, mostly heterosexual, and exclusively heterosexual), bisexual women were most likely to report CSA. Mostly heterosexual women were more likely to report lifetime substance abuse (e.g., tobacco, marijuana) and meet criteria for alcohol use disorder than exclusively heterosexual women. No information about associations among CSA, sexual identity, and alcohol use disorder was reported—reducing the ability to make inferences about sexual orientation-related disparities in substance use in this study sample.
Using data from the National Alcohol Survey, Drabble et al. (2013) examined sexual identity differences in the relationship between CPA and CPA and adult physical and sexual victimization with hazardous drinking among women (N = 11,169). SMW had higher odds of hazardous drinking than exclusively heterosexual women. Regardless of sexual identity, women who reported histories of having a same-sex partner were more likely to report lifetime victimization than heterosexual women without such histories. Even when controlling for victimization, significant sexual orientation-related disparities in hazardous drinking remained, suggesting that victimization only partially explains elevated hazardous drinking among SMW.
Using data from a U.S.-based sample, the National Epidemiologic Survey of Alcohol and Related Conditions (NESARC), Hughes et al. (2010a) examined victimization (i.e., CSA and adult sexual assault (ASA) and SUD in a sample of 34,653 heterosexual and SM women and men. Compared to heterosexual women, bisexual women were more likely to report CSA, CPA, intimate partner violence, and non-partner violence, whereas lesbian women were only more likely to report CSA. Compared to heterosexual women and those unsure about their sexual identity, both lesbian and bisexual women were twice as likely to meet criteria for any past-year SUD and to report any form of victimization (childhood or adulthood). Among lesbian women, the prevalence of SUDs was higher among those who reported CPA, childhood neglect, and intimate partner violence. Among bisexual women, SUD prevalence was higher among those who reported CSA, partner violence, and assault with a weapon. Reporting childhood neglect strengthened the association between lesbian identity and alcohol dependence. In a later study using NESARC data, McCabe et al. (2020a) examined associations among childhood household dysfunction (e.g., an adult in the home was a problem drinker or alcoholic), sexual identity, alcohol, tobacco, and other SUDs in adulthood. Results indicated a curvilinear relationship between the number of indicators of household dysfunction and each SUD, suggesting that there were no differences in the probability of developing a SUD between participants (both male and female) who reported one type of household dysfunction and those who reported multiple types. Further, even when accounting for household dysfunction, SMW had a higher risk of alcohol use disorders, tobacco use disorders, and other SUDs than heterosexual women. Finally, Yuan and colleagues (2014) found no significant associations between CSA and substance-related outcomes (i.e., alcohol dependence, hazardous and harmful alcohol use, binge drinking) among SMW in a study of Two-Spirit identified individuals (a term used by North American indigenous people who identify as having both feminine and masculine spirit).
Of the five studies using CHLEW data, three included a heterosexual comparison group from the National Study of Health and Life Experiences of Women (NSHLEW). Wilsnack et al. (2008) found that SMW were more likely than heterosexual women to report CSA, and that bisexual women were most likely to report CSA. In another study using a pooled sample of CHLEW and NSHLEW participants, Hughes et al. (2010b) found that hazardous drinking differed by SMW’s history of victimization (e.g., none, CSA only, ASA only, revictimization). Compared to SMW without a history of sexual victimization and those who reported one form of victimization (CSA or ASA), women with a history of adult revictimization reported significantly higher levels of hazardous drinking (a summed score of responses to several indicators of hazardous drinking, e.g., heavy drinking, problem drinking consequences). Bisexual women who reported CSA alone had the highest estimated adjusted mean level of hazardous drinking. Finally, Hughes et al. (2014) found that the number of victimization types (i.e., CSA, CPA, parental neglect, ASA, adult physical assault, and intimate partner violence) was significantly associated with hazardous drinking. Specifically, each additional type of victimization reported by participants in the study sample corresponded with 20% increased odds of reporting hazardous drinking.
In CHLEW studies using data focused exclusively on SMW, Hughes and colleagues found significant associations between CSA and alcohol abuse. Specifically, Hughes et al. (2007) found that among lesbian women (N = 447), CSA had a direct relationship with alcohol abuse (a summed score of four problem drinking indicators). Using data from CHLEW Waves 1 and 2, Johnson et al. (2013) examined self-medication and impaired-functioning models of the associations among minority stress, hazardous drinking, and mental health within a developmental framework. The researchers found a significant association between CSA and depression at Wave 1, but no significant association between depression at Wave 1 and hazardous drinking at Wave 2. Additionally, there were no significant associations between CSA and any age of onset measures (age at first time consuming alcohol, sexual orientation, sexual intercourse).
Physical Health
Fourteen studies examined associations between ACEs and physical health risk factors or outcomes, including chronic physical health problems (Andersen et al., 2014; Lehavot & Simoni, 2011; Matthews et al., 2013), smoking (Lee et al., 2020; Lehavot & Simoni, 2011; Matthews et al., 2013), BMI (Aaron & Hughes, 2007; Caceres et al., 2019; Katz-Wise et al., 2014; Smith et al., 2010; Wright, 2018), and sexual health (Austin et al., 2008a; Crump & Byers, 2017; Greene et al., 2019; Sweet et al., 2013; Sweet & Welles, 2012). Overall, the findings of these studies suggest that ACES are associated with a range of physical health outcomes among SMW, including cardiometabolic risk factors, smoking, and poorer perceived health.
Overall Physical Health
In Wave 1 of CHLEW, CPA was indirectly associated with poorer self-perceived health status among SMW (Matthews et al., 2013). In analyses using data from Wave 1 (2000–2001) of CHLEW and from heterosexual women in Wave 5 (2001) of the nationally representative NSHLEW sample, women who reported both CPA and CSA had significantly higher scores on a summed index of physical health problems (i.e., cardiovascular conditions, metabolic conditions, and immune diseases), whereas reporting one trauma type (i.e., either CPA or CSA) was not (Andersen et al., 2014). There was no significant interaction between sexual identity and CPA or CSA, suggesting that women who reported multiple forms of childhood abuse had poorer physical health, regardless of sexual identity. Lehavot and Simoni (2011) found that childhood abuse (assessed using a latent variable that included emotional, physical, and sexual abuse and emotional and physical neglect) was directly associated with physical health problems (a latent variable using BMI and a summed score of arthritis, diabetes, respiratory conditions, hypertension, high cholesterol) (Lehavot & Simoni, 2011).
Body Mass Index
In Wave 1 of CHLEW, Aaron and Hughes (2007) found that SMW who reported CSA had almost two times higher odds of having a BMI between 30.0 to 39.9 kg/m2 and 2.3 times higher odds of having a BMI ≥ 40.0 kg/m2 than women who did not report CSA. However, in analyses of Wave 3 CHLEW data that included a supplemental sample of younger (ages 18–24), bisexual and Black and Latinx SMW, Caceres et al. (2019) reported mixed findings. Compared with SMW who did not report childhood trauma (i.e., CPA, CSA, childhood neglect), those who did had 1.58 times higher odds of diabetes and 1.44 times higher odds of past-3-month overeating, but there were not significant differences in BMI over 30 or hypertension. Further, Caceres and colleagues (2019) found no significant differences by SM identity subgroup.
In another study using a small convenience sample (N = 85) of SMW from the South, researchers investigated participants’ attitudes toward the concept of “obesity” and found there were no significant associations between CSA and attitudes toward “obesity” (Wright, 2018). Further, there was an unexpected negative association between CSA and BMI (i.e., SMW who reported CSA had lower BMI). In a large (N = 13,952) and diverse (i.e., by race/ethnicity and sexual identity) national cohort in the Growing Up Today Study (GUTS; a longitudinal study consisting of children of participants in the Nurses Health Survey II, from age 12 to 25), bisexual women had a higher BMI at age 17 and greater 1-year increases in BMI than heterosexual women; child abuse partially explained this relationship (i.e., CPA, CSA, childhood emotional abuse, witnessed abuse as a child) (Katz-Wise et al., 2014). Lesbian women, however, did not significantly differ from heterosexual women. Finally, in a primarily White convenience sample in Pittsburgh (N = 867), lesbian sexual identity and history of intrafamilial CSA were associated with BMI over 30 (compared to heterosexual identity and no history of intrafamilial CSA, respectively) (Smith et al., 2010). There was no association between extrafamilial CSA and BMI over 30 in the adjusted model.
Smoking
In Wave 1 of CHLEW, age of smoking onset and current smoking mediated the indirect relationship between CPA and poorer perceived health status among SMW survivors of CPA (Matthews et al., 2013). Lehavot et al. (2014) found that childhood abuse (assessed using a latent variable that included emotional, physical, and sexual abuse and emotional and physical neglect) had a direct association with smoking behaviors (i.e., a latent variable created from three questions: having smoked at least 100 cigarettes in their life, current smoking status, and past-12-month quit attempt). However, smoking did not mediate the relationship between childhood abuse and chronic physical health problems (i.e., high BMI, arthritis, diabetes, respiratory conditions, hypertension, high cholesterol) (Lehavot & Simoni, 2011). Conversely, in a nationally representative, dual-frame, random-digit-dialing survey, none of the ACEs examined (i.e., food insecurity, substance abuse in the home, physical abuse, emotional abuse) were associated with smoking among a subgroup of 129 lesbian women (Lee et al., 2020).
Sexual Health
There was mixed evidence for an association between ACEs and sexual health-related outcomes in several studies. Findings from Wave 3 of CHLEW using Classification and Regression Tree analysis indicated that CPA (but not CSA) was one of six most strongly associated predictor variables (e.g., demographic, healthcare, age at drinking onset, adult victimization, CSA, CPA) of past-year Pap screening (Greene et al., 2019). In an online convenience sample of 299 primarily white SMW of diverse sexual identities in the U.S. and Canada, participants who reported experiencing penetrative CSA had significantly lower sexual desire and satisfaction and significantly more frequent negative automatic thoughts about sexual activity than SMW with no history of sexual abuse, SMW who experienced adult sexual abuse only, and SMW who experienced CSA involving fondling only (Crump & Byers, 2017). In Wave 2 of the NESARC, SMW who reported experiencing CSA “almost never” were 7.1 times more likely, and those who reported CSA “sometimes/frequently” were 3.8 times more likely to have an STI or HIV diagnosis in the past 12 months compared to SMW who reported never experiencing CSA (Sweet & Welles, 2012). While the authors did not provide an explanation for this counter-intuitive outcome, this finding may be related to small subgroup sample sizes (55 reported almost never and 67 reported sometimes/frequent CSA). Additionally, it is unknown if the differences between those two groups were statistically significant. In another study using Wave 2 NESARC data, Sweet and colleagues (2013) found that SMW with no history of CSA, SMW who reported rare experiences of CSA, and those who reported sometimes/frequently experiencing CSA had 1.9, 8.3, and 6.3 times higher odds of past-year HIV or STI diagnosis, respectively, than heterosexual women with no history of CSA. They also found that among SMW who reported CSA, the relationship between CSA and HIV/STI risk was mediated by mental health disorders. However, neither drug use disorder nor alcohol use disorder mediated the relationship between CSA and HIV/STI risk. In a cross-sectional community-based sample of 391 mostly Black and Latina women, Austin and colleagues (2008b) found that “mostly heterosexual” women were more likely than exclusively heterosexual women to have experienced CSA. In addition, mostly heterosexual women in the sample were more likely than exclusively heterosexual women to report having had an STI, earlier age at first intercourse, and a higher number of sexual partners. CSA was not found to mediate the relationship between sexual identity and sexual risk factors in this sample.
Multiple Health and Social Outcomes
Only one study examined multiple health or social outcomes simultaneously. Using data from the National Lesbian Health Care Survey, a large cross-sectional sample (N = 1889) of lesbian-identified women, Hyman (2000) found that multiple forms of CSA significantly predicted greater numbers of both physical and mental health problems reported by participants. In addition, women who reported extrafamilial CSA or intrafamilial CSA without coercion were less likely to have completed college than women who did not report these forms of CSA. Finally, controlling for several demographic variables, women who reported intrafamilial CSA without coercion and women who reported extrafamilial CSA by an unknown person had significantly lower incomes. Findings from this study suggest that SMW reporting CSA may experience a range of co-occurring sequelae, including negative financial outcomes (Hyman, 2000).
Revictimization and Other Experiences of Interpersonal Violence
Two studies examined the association between CSA and sexual revictimization (i.e., ASA) in adulthood. Hequembourg et al. (2013) recruited a community-based sample of 205 lesbian and bisexual women to investigate associations between CSA and revictimization cross-sectionally, and found that more severe CSA was associated with more severe adult victimization. Han et al. (2013) similarly examined associations between ASA and alcohol use in a convenience sample of 239 gay men and lesbian women. Among lesbian women, 13.9% reported revictimization in adulthood (defined as having experienced both CSA and ASA compared to 28.2% of gay men). Using structural equation modeling, alcohol use was identified as the strongest predictor of ASA among lesbian women, and CSA was identified as the strongest predictor of ASA among gay men. In another study, Lehavot and Simoni (2011) found that 45% of SMW reporting any form of childhood abuse also reported ASA, compared to 20% of those reporting no childhood abuse. Childhood abuse was directly associated with ASA, smoking, and chronic physical health problems. Finally, in a sample of 299 SMW, Crump & Byers (2017) found that SMW who reported penetrative CSA, and SMW who reported CSA limited to fondling, were significantly more likely to report sexual revictimization (77% and 56% respectively) in adolescence or adulthood than those who reported no CSA (32% reported ASA).
Discussion
Although somewhat mixed, findings from this review provide support for the contention that ACEs are associated with a wide range of negative mental and physical health and substance use outcomes among SMW (see Table 4 for a summary of key findings). Of the 11 studies examining relationships between ACEs and mental health outcomes, all but one (Persson et al., 2015) found significant associations. Compared to SMW without histories of ACEs, those with such a history were more likely to report psychological distress, emotional and behavioral difficulties, depression, and PTSD (Andrés-Hyman et al., 2004; Matthews et al., 2002; Morris & Balsam, 2003; Robohm et al., 2003). These findings are consistent with those from studies examining mental health outcomes of women in the general population (McCauley et al., 2015). However, additional research is needed to better understand if sexual identity mediates the relationship between ACEs and mental health disparities.
Key Findings.

Note. ACEs = adverse childhood experiences; SMW = sexual minority women.
Similarly, of the 15 studies examining the relationship between ACEs and negative substance use outcomes, all but one (Yuan et al., 2014) found significant associations, highlighting the importance of examining ACEs as a risk factor for hazardous drinking and SUDs among SMW. Findings are largely consistent with extant literature among presumably heterosexual women. For example, in their scoping review of studies of adults in the general population, Leza et al. (2021) found a consistent, positive relationship between ACEs and substance use. However, using a large dataset from the National Alcohol Survey, Drabble et al. (2013) found that among all women with victimization histories, SMW reported higher levels of drinking than heterosexual women (Drabble et al., 2013), suggesting the need to examine additional factors that may influence SMW’s increased risk of alcohol abuse.
The evidence linking ACEs and health risk behaviors and attitudes is somewhat mixed. Although ACEs were associated with overeating (Caceres et al., 2019) and smoking behaviors (Matthews et al., 2013; Lehavot & Simoni, 2011) among SMW, Lee et al. (2010) failed to find evidence of an association between ACEs and smoking among SMW, and Wright (2018) did not find an association between ACEs and attitudes toward “obesity.” Further, Austin et al. (2008b) found that ACEs did not explain the association between minority sexual orientation and sexual risk factors. Also unexpected was Green et al.’s (2019) finding that CPA predicted past-year cervical cancer screening among SMW, and CSA did not predict cervical cancer screening in either direction.
Evidence of an association between ACEs and physical health outcomes was also mixed. We found evidence that ACEs were associated with diabetes (Caceres et al., 2019), higher BMI (Katz Wise et al., 2014), higher odds of BMI over 25 (Aaron & Hughes, 2007), poor sexual health (e.g., STI and HIV diagnosis) (Crump & Beyers, 2017; Sweet & Welles, 2012; Sweet et al., 2013), general physical health problems (Lehavot & Simoni, 2011), and worse perceived health status (Matthews et al., 2013) among SMW. However, Andersen et al. (2014) failed to find evidence of an association between CSA or CPA and physical health problems, and Caceres et al. (2019) found no significant associations between childhood trauma and BMI over 30 or hypertension. Studies by Sweet and Wells (2012) and Sweet et al. (2013) failed to find a dose-response relationship between frequency of CSA and likelihood of a STI or HIV diagnosis; although “no CSA” was associated with the lowest odds of STI or HIV diagnosis, “rarely or almost never” experiencing CSA was associated with higher odds than “sometimes/frequent CSA.” Also counterintuitively, in a study with a small snowball sample of 85 SMW, CSA was associated with lower BMI among SMW (Wright, 2018).
Findings related to sexual identity differences were also somewhat mixed. For example, Andersen et al. (2014) found no significant differences in chronic physical health problems when comparing heterosexual and SMW with histories of ACEs, but Katz-Wise et al. (2014) found that bisexual women with histories of ACEs reported higher BMI at age 17 than their heterosexual counterparts. Similarly, Smith et al. (2010) found that lesbian women reporting intrafamilial or extrafamilial CSA had higher odds of BMI over 30 than heterosexual women reporting either form of CSA. Further, Sweet et al. (2013) found that women with histories of CSA had higher past-year HIV or STI diagnosis than women without history of CSA; this was more pronounced among SMW than heterosexual women.
Limitations of the Studies Included in the Scoping Review
Unfortunately, there are significant shortcomings in the existing research that limit our understanding of ACEs and health outcomes among SMW—and that likely account for some of the mixed findings. There is a lack of research on ACEs and health among SMW using large probability samples, as well as of studies that examine differences across race/ethnicity or sexual identity subgroups. Few studies include older adults or investigate associations across the lifespan. Further, studies included in this review used widely variable definitions and measurement tools to assess ACEs, making it difficult to compare outcomes across studies. Of the 42 papers included, 36 assessed CSA, 17 assessed CPA, seven assessed childhood emotional abuse, seven assessed neglect, two assessed adult substance use, one assessed household dysfunction and one study assessed risky family environment, food insecurity, and a broadly defined variable of childhood maltreatment, respectively. Given that no studies examined all of the more common 10 types of ACEs (Felitti et al., 1998), and most studies focused only on CSA and/or CPA, it is essential that future research include more comprehensive measures of ACEs to better understand the scope of ACEs reported by SMW and how they are associated with mental health, substance use, and physical health risk factors and outcomes.
Additionally, while most studies (n = 27) framed their research questions and findings using existing theories, no studies drew on theories that explicitly reference the relationship between trauma exposure and the development of traumatic stress symptoms and related conditions over the life course. This is particularly important as growing evidence suggests that early adversity (e.g., ACEs) may sensitize individuals to developing later mental health problems (e.g., depression, anxiety) by reducing tolerance to subsequent stressors (Hammen et al., 2000; Harkness et al., 2006).
Moreover, of the 42 studies, only four studies used longitudinal data, limiting our ability to hypothesize about the direction of effects (i.e., are SMW who report ACEs more likely to report mental health problems as well or are individuals with mental health problems more likely to report or to perceive experiences as traumatic). The rarity of those studies highlights the importance of future research using prospective designs and/or longitudinal data to better understand the direction of these associations. Finally, all but three studies were conducted within the U.S., highlighting the need to study the experiences of SMW outside of the U.S. where societal attitudes and/or treatment of ACEs may differ.
Study Limitations
Our review also has several limitations. First, only articles published in English between January 2000 and June 2021 were included, potentially leading to the exclusion of relevant articles published in other languages or after this time period. Additionally, relevant articles may have been excluded if they did not use the same terminology as listed in our keyword search strategy. Finally, this review followed scoping review guidelines (Tricco et al., 2018) and therefore did not include evaluations of study quality. Systematic reviews that examine the quality of studies are also needed.
Conclusion
There is strong evidence that ACEs are a risk factor for multiple negative mental health and substance use outcomes among SMW. However, additional research is needed to better understand the associations between ACEs and both health risk behaviors and physical health outcomes among SMW. First, future research should seek to replicate studies with counterintuitive findings, such as whether CPA is associated with preventive health behaviors and the lack of a dose-response relationship between CSA and STI/HIV diagnoses. Second, although there is limited research on the prevalence and consequences of revictimization among SMW who have experienced ACEs, the few extant studies suggest that revictimization in adulthood is prevalent, and that having experienced childhood abuse is associated with ASA. Given the dearth of literature examining revictimization, future research is essential to confirm these findings.
Implications of Findings for Future Research, Policy, and Practice
More research is necessary to understand the higher rates of ACEs among SMW and to further illuminate the mechanisms and pathways that lead to negative health outcomes (see Table 5 for a summary of implications of findings). This will contribute to the development of tailored, culturally appropriate interventions for SMW who have histories of ACEs. In addition, future research on ACEs among SMW should examine the impact of structural level minority stressors (e.g., discrimination) on the relationship between ACEs and health. Overall, the findings from this review emphasize the importance of screening for ACEs in the context of child, adolescent, and adult health care. Clinicians should be trained to screen SMW for ACEs and to offer those who report ACEs appropriate mental health care referrals and resources.
Implications.

Note. ACEs = adverse childhood experiences, SMW = sexual minority women.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Dr. Bochicchio’s work is supported by National Institutes of Health/National Institute on Alcohol Abuse and Alcoholism (F32AA029957, P.I.: Bochicchio). Drs. Hughes’ work is supported by National Institutes of Health/National Institute on Alcohol Abuse and Alcoholism (R01AA027252, P.I.: Hughes)
