Abstract
Women experiencing intimate partner violence (IPV) in Latin America (LA)’s Spanish-speaking countries have demonstrated great need for formal services, including medical, legal, and mental health supports. However, women’s rates of formal help-seeking for IPV in the Americas remain extremely low. A systematic literature review was conducted to understand barriers to women’s help-seeking for IPV in LA’s Spanish-speaking countries. Five electronic databases were searched with search terms in English and Spanish related to IPV, help-seeking, and barriers. Articles were included in the review if they were published in peer-reviewed journals; original empirical research; published in English or Spanish; and had participants who were women exposed to IPV or service providers who worked with IPV-exposed women; and were conducted in Spanish-speaking Latin American countries. 19 manuscripts were synthesized. Inductive thematic analysis of barriers to formal help-seeking for IPV identified in the articles resulted in five key themes: intrapersonal barriers, interpersonal barriers, organization-specific barriers, systemic barriers, and cultural barriers. Findings demonstrate the need to consider culture as a driving force in why women face extensive barriers to help-seeking across the social ecology. Suggestions for interventions at each level of the social ecology to better support women exposed to IPV in LA’s Spanish-speaking countries are discussed.
Intimate partner violence (IPV) involves physical, sexual, psychological, and economic abuse, coercive control, and stalking by a current or a former intimate partner (Breiding et al., 2015). Research indicates that IPV against women is incredibly prevalent in Latin America’s (LA) Spanish-speaking countries. A recent systematic review demonstrated that rates of physical and/or sexual IPV against women in these countries were high, ranging from 14.3% in El Salvador, on the lowest end of the spectrum, to 58.5% in Bolivia, on the highest end of the spectrum (Bott et al., 2019). Negative effects of IPV exposure on women’s health and well-being are well documented in the literature, such as increased risk of substance misuse, chronic disease, and contracting sexually transmitted infections (Stubbs & Szoeke, 2021). Thus, many women could benefit from formal services to help cope with effects of IPV exposure (Kulkarni, 2019). However, epidemiological research using nationally representative data across multiple countries from LA over nearly a decade estimates that only about 14% of women exposed to IPV in LA receive such services (Palermo et al., 2014). Although several global systematic reviews have examined barriers to women’s help-seeking from formal resources, none have focused on women in the Spanish-speaking countries in LA. The current systematic review synthesized Spanish and English peer-reviewed literature from the Spanish-speaking countries in LA, aiming to understand barriers women in LA’s Spanish-speaking countries confront when seeking formal resources for IPV.
Formal help-seeking includes finding and eliciting formal assistance for IPV and its sequelae from community resources such as the legal system, shelters, crisis lines, and health professionals (Alvarez & Fedock, 2018; Kulkarni, 2019). Formal resources may support women in ways that informal supports cannot, such as providing medical or legal services. Engaging with formal resources for IPV has been demonstrated to support women’s mental health, empowerment, and safety (Wright & Johnson, 2012). Worldwide, rates of formal help-seeking for IPV-exposed women are low but variable, with only about 7% of women experiencing IPV reporting it to a formal resource, including regional variation ranging from about 2% of women in East Asia to 14% in LA (Palermo et al., 2014). These low rates indicate that, although women could benefit from utilizing formal community services, they are confronted by barriers to their help-seeking. Such barriers may include perceiving IPV as normal, language barriers, lack of resource availability, socioeconomic barriers, social stigma, and more (Lelaurain et al., 2017; Satyen et al., 2019). Understanding these barriers is therefore of critical importance for finding ways to overcome them and thus support women who have experienced IPV.
Why Focus on Women’s Help-Seeking in LA?
Variations in rates of formal help-seeking for IPV by region indicate that cultural variations may contribute to barriers to help-seeking. Indeed, extant literature indicates that understandings of what constitutes violence, healthy relationships, and gender roles are deeply rooted in culture (Alvarez & Fedock, 2018; De Coster & Heimer, 2021), and cultural values in which men are given higher status than women are a demonstrated risk factor for IPV (WHO, 2021). Given that understandings of IPV itself are culturally bound, it logically follows that the availability of resources for IPV-exposed women, as well as barriers that influence help-seeking from formal supports, may also be influenced by regional cultural factors.
In the 1990s, LA drafted and approved a regional convention to eradicate violence against women, in alignment with worldwide movements such as the 1995 U.N. World Conference on Women (Macaulay, 2005) and the work of women’s movements in LA (Sternbach et al., 1992). However, the implementation of this legislation has varied widely across countries. Joseph (2017) reviewed laws about femicide throughout LA and found that although many countries have criminalized intimate partner homicide, penalties vary greatly from country to country and laws are inconsistently implemented. Thus, although legislation is foundational in creating formal supports for IPV-exposed women, it is only part of addressing cultural views on IPV and providing services to keep women safe.
Culture includes beliefs, acts, morals, and customs that are transmitted through family, education, media, politics, and religion (Spencer-Oatley & Frankline, 2012). Alongside many differences, cultures in LA share features (e.g., in language, civil codes) due to similar colonial and post-colonial histories (Macaulay, 2005). Cultural values that may contribute to barriers to help-seeking in LA include machismo (i.e., the belief that masculinity is characterized by sexual and physical aggression), marianismo (i.e., the belief that women should be demure and live in alignment with the example of the Virgin Mary), and familismo (i.e., the belief that women should maintain familial harmony; Alvarez & Fedock, 2018; Muñoz-Martínez & Aguilar-Cacho, 2022). Cultural understandings of what it means to be a man or a woman in LA may influence power dynamics between partners, place women at risk for IPV exposure, and make it uniquely difficult for women to seek help from formal resources (O’Neal & Beckman, 2017).
Existing Literature and Reviews
In 2017, O’Neal and Beckman noted an absence of literature on the unique barriers to Latinas’ formal help-seeking for IPV in the United States. Alvarez and Fedock (2018) also discussed the sparseness of literature about how to support Latinas exposed to IPV and called for culturally and linguistically tailored interventions. Recent research (e.g., Marrs Fuchsel & Brummett, 2021; Valdovinos et al., 2021) has begun to investigate Latinas’ experiences within the United States. However, this topic has not yet received similar attention focusing on Latinas in LA.
Existing literature reviews similarly reflect an absence of attention to barriers to formal supports for IPV that women experience in LA. Indeed, multiple “global” systematic reviews have been conducted to investigate barriers to resource access following IPV around the world (Lelaurain et al., 2017; Satyen et al., 2019). Yet, no review has included literature published in Spanish, nor have these reviews focused explicitly on women in Spanish-speaking countries. Lelaurain et al. (2017) carried out a systematic review of help-seeking from formal supports for IPV worldwide. However, although they reviewed the global literature, of the 90 articles synthesized, only three were from LA (i.e., two from Mexico and one from Brazil). Another review (Satyen et al., 2019) investigated cross-cultural differences in formal help-seeking for IPV. However, again, the authors only identified and included studies conducted in North America and the U.S. Virgin Islands. As such, barriers to help-seeking that women experience in LA have been notably absent from reviews on this topic.
The Importance of Women’s Experiences “On the Margins” of the Literature
This absence of research on barriers to formal help-seeking in LA is a gap in the literature. There is need for greater understanding of Latinas’ experiences seeking help for IPV outside of the United States. Feminist theory has long underscored the importance of understanding women’s experiences on the margins—that the literature is inadequate if it does not consider and integrate the heterogeneity in women’s experiences, including intersecting identities of women of color and/or with other marginalized identities (e.g., Crenshaw, 1995). LA women’s experiences are absent in existing reviews and are therefore likely less understood by a broader audience, representing a problem for understanding similarities and differences in women’s experiences across contexts. Certainly, IPV is a staggeringly common experience worldwide, yet epidemiological research shows that, although typologies and prevalence of IPV vary worldwide, it has common roots in gender socialization and relational power dynamics that devalue and disempower women (WHO, 2021). The current review will not integrate women’s experiences across all cultural contexts but will synthesize the experience of an underrepresented group of women in the current IPV literature. Highlighting the experiences of women exposed to IPV in Spanish-speaking countries in LA will allow for this literature to be further integrated into global conceptualizations of barriers to women’s access to formal resources.
Current Review Aims
The main question this review aimed to address is: what barriers do women in LA’s Spanish-speaking countries confront when seeking help from formal resources for IPV? Specifically, the review aimed to (a) address a gap in the literature by including work published in both Spanish and English, (b) describe the published studies’ characteristics (i.e., country, language, methodologies, and participants), and (c) synthesize studies’ findings about barriers to women’s access to formal supports for IPV.
Method
Search Protocol
The review was not preregistered; however, the proposal for the systematic review is available by request from the author for those who would like to review the original analytic plan. This review utilized the Preferred Reporting Items for Systematic Reviews and Meta-Analyses method (Page et al., 2021) to search peer-reviewed journals using PubMed, Web of Science, PsychINFO, as well as SciELO, and LILACS databases, which gather records from peer-reviewed journals in LA. Searches were performed from first record to May 16, 2022. Search terms in English included: (partner violence OR IPV OR domestic violence OR partner abuse OR spouse abuse OR dating violence) AND (help seeking OR help-seeking OR seeking help OR resources OR service utilization OR service access OR services) AND (barrier OR risk factor OR obstacles). Search terms in Spanish included: (violencia de pareja OR violencia doméstica OR maltrato conyugal OR abuso conyugal OR violencia por parte de la pareja íntima) AND (buscar ayuda OR solicitud de ayuda OR conducta de búsqueda de ayuda OR recursos OR servicios) AND (barreras OR obstáculos OR factores de riesgo OR deficiencias de apoyo). Citations were collated in RefWorks, and abstract and full-text reviews were conducted in Covidence systematic review software.
Inclusion and Exclusion Criteria
Figure 1 outlines the search and screening process. Study titles and abstracts were reviewed for relevance. Articles were included if they were: (a) peer-reviewed; (b) original empirical research; (c) published in English or Spanish; (d) participants were women exposed to IPV or service providers who worked with IPV-exposed women; (e) in Spanish-speaking LA countries (i.e., Argentina, Bolivia, Chile, Colombia, Costa Rica, Cuba, Dominican Republic, Ecuador, El Salvador, Guatemala, Honduras, Mexico, Nicaragua, Panama, Paraguay, Peru, Uruguay, and Venezuela); and (f) included barriers to accessing formal sources of support for IPV. Articles were excluded if: (a) they were not empirical, (b) participants did not identify as women, or women’s data was not disaggregated from the broader sample, (c) they were not published in English or Spanish; (d) participants were immigrants to non-Spanish-speaking countries, (e) findings were related to gender-based violence that is not IPV, (f) the focus was on resources for issues beyond help for IPV (e.g., access to health care for non-IPV-related health problems although the sample was IPV-exposed) and (g) help-seeking was for IPV perpetration.

Identification of studies via databases.
Data Extraction
In Table 1, extracted data included the country/countries where data collection occurred, article language, sample size and a description of participants, type of IPV participants had experienced and IPV measures used, formal supports participants sought, study design and analytic method, and identified barriers. Inductive thematic analysis (Thomas & Harden, 2008) was used to identify themes across articles.
Summary of Included Studies, Organized by Study Method (Quantitative, Mixed-Method, Qualitative) and Author Last Name.
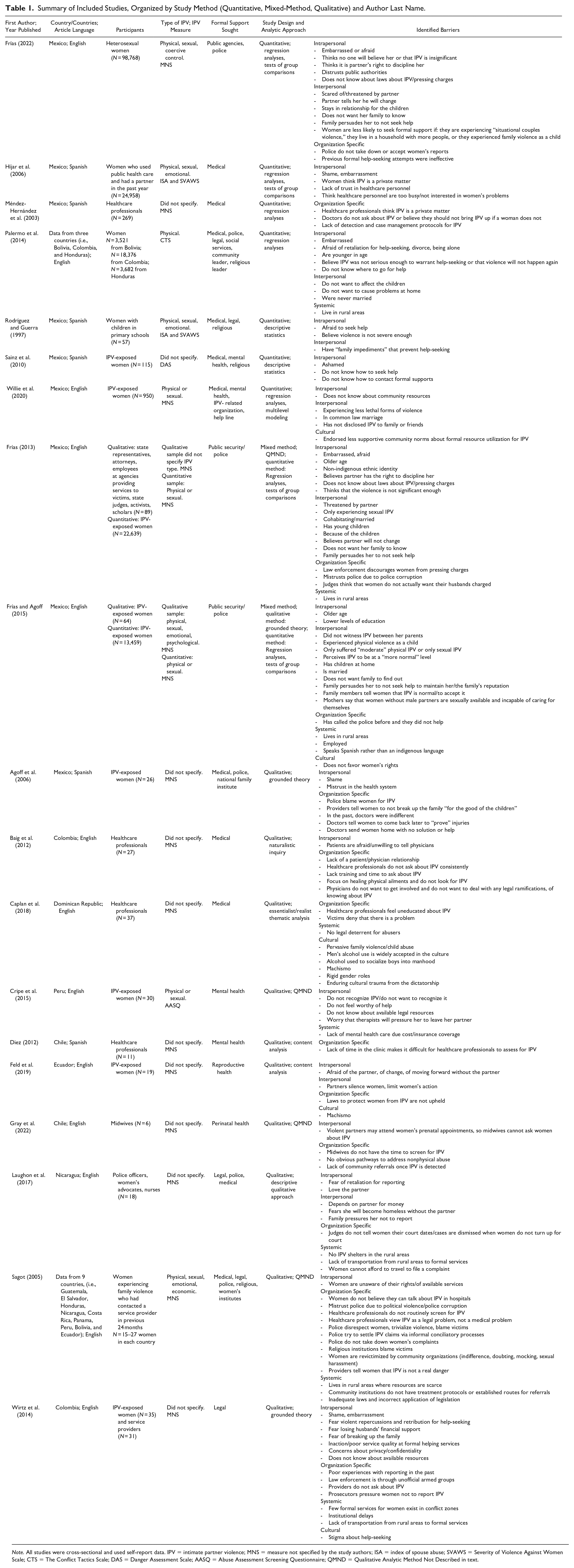
Note. All studies were cross-sectional and used self-report data. IPV = intimate partner violence; MNS = measure not specified by the study authors; ISA = index of spouse abuse; SVAWS = Severity of Violence Against Women Scale; CTS = The Conflict Tactics Scale; DAS = Danger Assessment Scale; AASQ = Abuse Assessment Screening Questionnaire; QMND = Qualitative Analytic Method Not Described in text.
Results
Data were extracted from 19 articles. Data about the studies (i.e., country, language, methodologies, and participants) are presented first below. Then, the barriers discussed within the articles are presented in accordance with themes identified in the thematic analysis. These included Intrapersonal, Interpersonal, Organization-Specific, and Systemic and Cultural barriers.
Included Countries, Languages, Methodologies, and Participants
Of the 19 included articles, 2 were from Chile, 2 from Colombia, 1 from the Dominican Republic, 1 from Ecuador, 9 from Mexico, 1 from Nicaragua, and 1 from Peru. Two articles included data from multiple countries; findings were extracted only for the included countries (see Table 1). Most (i.e., 13) were written in English and used qualitative data (i.e., 10); articles’ countries of origin, publication language, data collection, and analysis methods are summarized in Table 1. All studies were cross-sectional and used self-report data.
Participants in seven studies were service providers for IPV-exposed women; most interviewed healthcare providers (see Table 1). Thirteen studies’ participants were women, and of those, nine used a sample of only women who had experienced IPV.
Barriers to Help-Seeking
Articles identified an array of barriers to help-seeking from formal sources of support for IPV (see Table 1). When appropriate, quotes were pulled from qualitative studies to elucidate this review’s findings. Quotes in Spanish were forward translated by the author, a fluent Spanish speaker, into English.
Intrapersonal barriers
Study findings demonstrated that some barriers to help-seeking emanate from within women, including emotional barriers, women’s lack of knowledge about resources, cognitions about resources, cognitions about IPV, and individual factors.
Emotional barriers
One study in Nicaragua (Laughon et al., 2017) found that women’s love for their partner was a barrier to help-seeking. Seven studies (five in Mexico: Agoff et al., 2006; Frías, 2013, 2022; Hijar, 2006; Sainz et al., 2010; one in Colombia: Wirtz et al., 2014; and one in Bolivia: Palermo et al., 2014) indicated that women feel shame or embarrassment that prevents help-seeking. For example, a woman in Colombia said, “he [husband] would force himself on me and I was terribly sick . . . I felt too embarrassed to go to the doctor to tell them. I cried by myself, but I couldn’t tell anybody what was going on” (Wirtz et al., 2014, p. 9).
In addition, eight studies (three in Mexico: Frías, 2013, 2022; Rodriguez & Guerra, 1997; two in Colombia: Baig et al., 2012; Wirtz et al., 2014; one in Nicaragua: Laughon et al., 2017; one in Bolivia: Palermo et al., 2014; and one in Ecuador: Feld et al., 2019) found that women’s fear is a barrier. Women’s fears were attributed to varying causes. Some women were afraid of retaliation from the partners for help-seeking; one provider in Nicaragua, said, [Abusers say] “If you denounce me [i.e., report to the police], I won’t give you anything. If you denounce me, you’re going to be on the street because you are illiterate, nobody will pay attention to you.” So because of that fear, many of the women go back to the house again. (Laughon et al., 2017, p. 854)
Some women were afraid of divorce or being alone (Palermo et al., 2014). A study from Colombia found that women were afraid to lose partners’ financial support and to break up their families (Wirtz et al., 2014). A woman in Ecuador described intersecting nature of intrapersonal fear and shame with interpersonal barriers, saying, Sometimes you don’t split up because you are afraid, you don’t split up because what neighbors may say, that was my case. I would tell my mother, once again I have to start over, how embarrassing, what will people say . . . I mean, you either decide to denounce, to speak up or you keep quiet. But if you keep quiet, it becomes your problem, because nobody on the outside knows what goes on inside the home. But we keep quiet for different reasons, fear, shame, because you don’t want the family to know, because there are always people that criticize you. (Feld et al., 2019, p. 278)
Lack of knowledge about resources
Not knowing about community resources for IPV was found in five studies (two in Mexico: Sainz et al., 2010; Willie et al., 2020; one in Bolivia: Palermo et al., 2014; one in Colombia: Palermo et al., 2014; and one in nine countries: Sagot, 2005). A study in Mexico stated, “The reasons for not seeking help . . . were not knowing what to do . . . and not being able to arrange an appointment” (Sainz et al., 2010, p. 247). Four studies (two in Mexico: Frías, 2013, 2022; one in Peru: Cripe et al., 2015; and one with participants in nine countries:Sagot, 2005) found that women lack knowledge about legal processes, including not knowing they could press charges for IPV, not knowing the laws about women’s rights, and not knowing about available legal resources.
Cognitions about resources
In three studies from Mexico (Agoff et al., 2006; Frías, 2022; Híjar et al., 2006), women not trusting resources was a barrier to help-seeking. Other barriers, such as perceiving resources to be ineffective, that service quality is poor, or that service providers are not interested in IPV, were found in three studies (one from Peru: Cripe et al., 2015; one from Mexico: Híjar et al., 2006; and one from Colombia: Wirtz et al., 2014).
Cognitions about IPV
Women normalizing or minimizing IPV as a barrier to help-seeking was found in five studies (three in Mexico: Frías, 2013, 2022; Rodriguez & Guerra, 1997; one in Bolivia: Palermo et al., 2014; and one in Peru, Cripe et al., 2015). Women may not recognize IPV, may believe that IPV was not severe enough to warrant help-seeking, or may think that men have the right to discipline women. Cripe and colleagues’ (2015, p. 6) participants “underscored the importance of helping women recognize that abuse is a problem, is not acceptable, and it has adverse effects on women and her children.” Other cognitions about IPV that constituted barriers were thinking that no one would believe her (Mexico; Frias, 2022), that IPV is a private matter (Mexico; Híjar et al., 2006), that IPV would not happen again (Bolivia; Palermo et al., 2014), and that women do not feel worthy of help (Peru; Cripe et al., 2015).
Individual factors
Women’s age was found as a barrier to help-seeking in three studies. Findings were mixed. Two studies in Mexico (Frías, 2013; Frías & Agoff, 2015) found that older women were less likely to seek help from formal resources, whereas a study in Bolivia, Colombia, and Honduras (Palermo et al., 2014) found that younger women were less likely to seek help. With regard to other individual factors, two studies from Mexico (Frías, 2013; Frías & Agoff, 2015) found that nonindigenous women and women with lower levels of education were less likely to seek help.
Interpersonal barriers
The included studies found barriers to help-seeking that come from women’s interpersonal relationships with their partners, family, and children.
Partner
Partner-related barriers to help-seeking were discussed in eight studies (four in Mexico: Frías, 2013, 2022; Frías & Agoff, 2015; Willie et al., 2020; one in Chile: Gray et al., 2022; one in Nicaragua: Laughon et al., 2017; one in Ecuador: Feld et al., 2019; and one in Bolivia, Colombia, and Honduras: Palermo et al., 2014). Partner-related barriers included women’s marital status, although findings were mixed. Three studies from Mexico (Frías, 2013; Frías & Agoff, 2015; Willie et al., 2020) found that women who were married to a violent partner were less likely to seek help from formal resources than unmarried women, while another study with participants in Bolivia, Colombia, and Honduras (Palermo et al., 2014) found that never-married women were less likely to engage in help-seeking than married women.
Four studies in Mexico (Frías, 2013, 2022; Frías & Agoff, 2015; Willie et al., 2020) found that type and severity of IPV were barriers to help-seeking, such that women who experienced only sexual IPV or less severe (i.e., less likely to be lethal) IPV were less likely to seek help. Partner coercive control was reported as a barrier to help-seeking in four studies (one in Ecuador: Feld et al., 2019; one in Chile: Gray et al., 2022; and two in Mexico: Frías, 2013, 2022) such that partners limit women’s ability to leave the house or attend healthcare appointments alone. A midwife in Chile said, “there are other partners that come with the patient to the intake. So there they are, the two together, so how am I [if I were the patient] going to say ‘Yes, I am the victim of him’” (Gray et al., 2022, p. 9).
Partners’ economic abuse was a barrier to women’s formal help-seeking in one study in Nicaragua (Laughon et al., 2017), which reported that women depend on partners for money and may become homeless without the partner’s financial support. Women’s cognitions about the partner were reported as barriers in three studies (two in Mexico: Frías, 2013, 2022; one in Bolivia: Palermo et al., 2014), such as women believing help-seeking is not worth it because the partner will not change, and women not seeking help to avoid causing problems at home.
Family
Barriers to help-seeking from women’s families were found in six studies (five in Mexico: Frías, 2013, 2022; Frías & Agoff, 2015; Rodriguez & Guerra, 1997; Willie et al., 2020; and one in Nicaragua: Laughon et al., 2017). In two studies in Mexico (Frías, 2013; Frías & Agoff, 2015), barriers were reported related to women’s childhood environments; women who experienced childhood physical abuse and who did not witness interparental IPV were less likely to seek help from formal supports. Another barrier, from four studies in Mexico (Frías, 2013, 2022; Frías & Agoff, 2015; Willie et al., 2020), was women not wanting their families to find out about help-seeking. Finally, five studies (four in Mexico: Frías, 2013, 2022; Frías & Agoff, 2015; Rodriguez & Guerra, 1997; and one in Nicaragua: Laughon et al., 2017) found that women’s families pressured them not to engage in help-seeking. A woman in Mexico said, I think that from the beginning of the marriage, he started lowering my self-esteem . . . and, unfortunately, you believe it because who can you tell? You go and tell your mother-in-law, and your mother-in-law tells you “Don’t tell anyone.” (Frías & Agoff, 2015, p. 287)
The same five studies reported that family members tell women to accept IPV, that IPV is normal, that divorced women are incapable of caring for themselves, and to not seek help from formal supports to maintain the family’s reputation. Another woman in Mexico said, My mom says, “I have lived with your father all my life and you have to live with that man all your life.” Those are restrictions that your own family places on you. My mom says, “Better the devil you know than the devil you don’t.” (Frías & Agoff, 2015, p. 286)
Children
Child-related barriers were found in four studies (three in Mexico: Frías, 2013, 2022; Frías & Agoff, 2015; and one in Bolivia: Palermo et al., 2014). This was not elaborated in any of the studies, and instead, it was just reported that women did not engage in formal help-seeking “for the children.”
Organization-Specific barriers
Healthcare, legal, and police-related organization-specific barriers to women’s help-seeking were discussed across contexts.
Healthcare related
Barriers to women’s help-seeking in medical settings occurred in six articles (two in Chile: Diez, 2012; Gray et al., 2022; one in Colombia: Baig et al., 2012; one in the Dominican Republic: Caplan et al., 2018; one in Mexico: Mendez-Hernandez et al., 2003; and one study with participants in nine countries: Sagot, 2005). Healthcare professionals not asking women about IPV directly or routinely was identified in Colombia (Baig et al., 2012) and in Mexico (Mendez-Hernandez et al., 2003) and by a study in nine countries (Sagot, 2005). When women disclose IPV to healthcare professionals, they may receive unhelpful, confusing, or blatantly demeaning responses that undermine trust in the medical system’s capacity to help. For example, a woman in Mexico said, Well, the doctor . . . he only checks us, right? Because I have had to be checked and I have told them that my husband hit me, and they ignore me, and they do not give him the proper channeling . . . there is no answer from the doctor. (Agoff et al., 2006, p. 313)
Similarly, studies in Colombia (Baig et al., 2012), Chile (Diez, 2012), and the Dominican Republic (Caplan et al., 2018) reported that healthcare professionals lack training about how to ask about IPV and feel they do not have time to ask patients who present with injuries about IPV. They may be uncomfortable talking about IPV or may not want to deal with legal ramifications of knowing about IPV, as was found in Colombia (Baig et al., 2012), Mexico (Mendez-Hernandez et al. 2003), and the study in nine countries (Sagot, 2005). Baig et al.’s (2012) study with healthcare professionals in Colombia reported, “they did not want to ‘invade the patient’s private life’, ‘they did not want to get involved’, or ‘feared further legal involvement or having to testify in legal proceedings’” (p. 256). This aligns with findings from the Dominican Republic (Caplan et al., 2018) and a study in nine countries (Sagot, 2005) that women do not disclose IPV to healthcare professionals because women believe providers are not interested in hearing about IPV or because of the lack of a patient/physician relationship.
Findings in one study in Chile (Gray et al., 2022) and another in Mexico (Mendez-Hernandez et al., 2003) indicated that healthcare professionals may want to support women exposed to IPV but do not know what to do or where to send women once women disclose having experienced IPV. In Chile, midwives described frustration about a lack of pathways to address nonphysical IPV, and a lack of community referrals once IPV is detected. One midwife said, “I believe that what is lacking [is the knowledge] of the places where we can turn to” (Gray et al., 2022, p. 11). In Mexico (Mendez-Hernandez et al., 2003), medical professionals discussed a lack of detection and case management protocols for IPV in hospitals.
Legal
Barriers within the legal system were found in five studies (one in Nicaragua: Laughon et al., 2017; one in Mexico: Frías, 2013; one in Colombia: Wirtz et al., 2014; one in Ecuador: Feld et al., 2019; and one in nine countries: Sagot, 2005). Barriers related to prosecutors’ attitudes and actions were found in three of these studies, including judges believing that women do not actually want their husbands charged for IPV. A judge in Mexico said, The main objective of the administrative and criminal process is to teach the man a lesson . . . if a woman turns for help to law-enforcement agencies and they subsequently call her husband to initiate the conciliation process to tell him to stop being violent, the woman will probably report that she received quality service. (Frías, 2013, p. 18)
A study in Colombia (Wirtz et al., 2014) found that prosecutors pressure women not to report their partners because prosecutors are afraid of retribution. It was also reported that judges in Nicaragua sometimes do not tell women their court dates, leading to women’s cases being dismissed when women do not appear in court. A service provider in Nicaragua said, The trials aren’t doing justice. Many times, the cases are lost and are not brought forward because, because simply, well, they don’t call you . . . the subpoenas don’t arrive, or the victims don’t even know that they set a trial. (Laughon et al., 2017, p. 855)
An absence of laws or inadequate application of existing laws for protecting women from IPV was found in two studies (one in Ecuador: Feld et al., 2019; one in nine countries: Sagot, 2005), including excessive bureaucracy and little protection once women try to seek legal help.
Police related
Problems with police were reported in five studies (Mexico: Agoff et al., 2006; Frías, 2013, 2022; Frías & Agoff, 2015; and one in nine countries: Sagot, 2005), such as that police dismiss women’s claims by not accepting women’s reports, trying to settle IPV claims via informal processes, discouraging women from pressing charges, telling women to go home and settle family matters by having sex with their husbands, turning women away to keep official crime statistics low, and not responding when women call the police for help with IPV. A woman in Mexico said, He didn’t weigh the consequences, and he lashed me against a piece of furniture we had, and it cut open my head . . . I didn’t call the patrol car again because the patrol car had come many times and they didn’t pay any attention to me. (Frías & Agoff, 2015, p. 284)
Mistrust in police was a barrier to women’s formal help-seeking in three studies (two in Mexico: Agoff et al., 2006; Frías, 2013; and one in nine countries: Sagot, 2005) due to police blaming women for IPV or histories of police corruption. Frías (2013) found that police in Mexico accept bribes from IPV perpetrators to not prosecute reports; this undermines women’s confidence in public authorities. A worker at Mexico’s State Commission of Human Rights said, Their husband has economic resources, he paid the officer to not follow up on the violence case, or to get favorable reports. Almost 50% of the complaints about MPs in cases of domestic violence are about officers’ inappropriate conduct because of accepting money from the husband. (Frías, 2013, p. 17)
General service providers
Three studies indicated harmful reactions by service providers (one in Colombia: Wirtz et al., 2014; one in Mexico: Agoff et al., 2006; and one in nine countries: Sagot, 2005). These studies did not specify which types of providers reacted to women harmfully, so findings could not be sorted into other organization-specific barriers. Women’s formal help-seeking was reportedly thwarted by providers not asking about IPV and institutional delays (Colombia; Wirtz et al., 2014); women being revictimized by indifference, doubting her story, mocking, and sexual harassment at community organizations (study in nine countries; Sagot, 2005); and providers telling women not to break up their families for the children’s sake (Mexico; Agoff et al., 2006).
Systemic barriers
Systemic barriers to women’s help-seeking included a lack of IPV-related resources in women’s communities.
Lack of resources for IPV-exposed women
A scarcity of IPV-related resources was found in seven studies (two in Mexico: Frías, 2013; Frías, & Agoff, 2015; one in Nicaragua: Laughon et al., 2017; one in Colombia: Wirtz et al., 2014; one in Peru: Cripe et al., 2015; one in Bolivia, Colombia, and Honduras: Palermo et al., 2014; and one in nine countries: Sagot, 2005). Of these, four studies discussed resource scarcity in rural areas (Frías, 2013; Frías & Agoff, 2015; Palermo et al., 2014; Sagot, 2005), and two studies reported a lack of affordable transportation to formal services in urban areas (Laughon et al., 2017; Wirtz et al., 2014). Other barriers included a lack of IPV shelters (Nicaragua; Laughon et al., 2017), no legal deterrent for IPV perpetrators (Dominican Republic; Caplan et al., 2018), and few formal services for women in zones affected by armed political conflict in Colombia (Wirtz et al., 2014). In Peru (Cripe et al., 2015), a barrier was the lack of mental healthcare due to cost and lack of coverage by Peru’s national insurance.
Cultural barriers
Participants described cultural barriers, including gender-related barriers and community stigma about women’s help-seeking for IPV.
Gender related
Cultural perceptions of gender were described as a barrier in three studies (one in Ecuador: Feld et al., 2019; one in Mexico: Frías & Agoff, 2015; and one in the Dominican Republic: Caplan et al., 2018). In Mexico, women who did not favorably view women’s rights were less likely to engage in formal help-seeking for IPV (Frías et al., 2015). Women in Ecuador (Feld et al., 2019) identified machismo as a barrier to help-seeking. Doctors in the Dominican Republic discussed rigid gender roles, machismo, and the transmission of cultural trauma from the dictatorship as barriers to help-seeking for IPV; a physician said, It’s basically a cultural problem. If we look at our history, from our freedom in 1844 until today . . . during these 180 years, we have had 100 years of dictatorship, which is a force that affects [our mentality] . . . that’s the disaster we have today in our society . . . our men think they are superior to women. (Caplan et al., 2018, p. 887)
Stigma about help-seeking
Two studies (one in Mexico: Willie et al., 2020; and one in Colombia: Wirtz et al., 2014) identified barriers related to cultural perceptions of women’s help-seeking. In Mexico, women who endorsed less supportive community norms about women’s formal resource utilization were less likely to engage in help-seeking, and in Colombia, stigma associated with help-seeking was reported as a barrier.
Discussion
This systematic review aimed to synthesize peer-reviewed English and Spanish literature about barriers to women’s help-seeking from formal resources for IPV in LA’s Spanish-speaking countries. Across 19 empirical studies, the review identified intrapersonal, interpersonal, organization-specific, systemic, and cultural barriers to women’s help-seeking across contexts (Table 2).
Critical Findings.

Note. IPV = intimate partner violence; LA = Latin America.
The 19 articles in this review reflect women’s experiences across sixteen countries. The review included literature published in both English (13 studies) and Spanish (6 studies) as well as qualitative (10 studies), mixed-method (2 studies), and quantitative (7 studies) methodologies. Quantitative and qualitative studies both included perspectives of service providers and IPV-exposed women and covered the full range of themes for barriers to formal help-seeking. The breadth of represented countries, research methods, and inclusion of both service providers and IPV-exposed women represents a strength of this review, bringing attention to the experiences of women that have been neglected in other literature reviews on this topic. Implications of study findings for practice, policy, and research are delineated in Table 3.
Implications for Practice, Policy, and Research.

Note. IPV = intimate partner violence; LA = Latin America.
Contending With Cultural Barriers to Formal Help-Seeking for IPV
Multiple studies indicated that cultural influences such as gender roles and stigma about women’s help-seeking constituted barriers to women’s formal help-seeking for IPV. Across the world, cultural values that ascribe higher status to men than women are a risk factor for IPV (WHO, 2021), and high rates of stigma about IPV among individuals in LA have been demonstrated in the literature (Nelson et al., 2023; Tsapalas et al., 2021). Beyond constituting its own layer of barriers to women’s help-seeking, culture also clearly permeated every other level of the barriers delineated in this review such that, across contexts, resources for women exposed to IPV either do not exist or are inadequate to address women’s needs. This lack of support reflects broad-ranging devaluation of women’s rights and safety, which helps explain why the women participating in studies throughout this review experienced such extensive barriers to formal help-seeking.
However, there is hope for addressing IPV at the cultural level. Approaching IPV prevention and facilitating women’s help-seeking at the cultural level in LA’s Spanish-speaking countries was demonstrated in Nicaragua. In 20 years, past-year physical IPV decreased by 70% nationwide (Ellsberg et al., 2022); this reduction was significantly associated with women’s knowledge of their rights, exposure to media campaigns about how IPV is unacceptable, as well as higher levels of women’s education, property ownership, and membership in labor unions. The proportion of Nicaraguan women who sought formal help for IPV increased by over 30% (Ellsberg et al., 2022). Ellsberg et al. (2022) attribute these changes to Nicaraguan feminist organizations’ efforts to create more formal services for women exposed to IPV and media campaigns to increase women’s access to justice and raise cultural awareness about women’s rights. The Nicaraguan example holds great promise for considering how to address barriers to women’s formal help-seeking for IPV at the cultural level.
Contending With Barriers at the Organizational and Systemic Levels
Although this review separated organization-specific and systemic barriers, recommendations for contending with these barriers are similar so they have been collapsed for the purpose of discussion. Systemic barriers to formal help-seeking for IPV included a lack of IPV-related resources in women’s communities (particularly in rural areas). Regarding organization-specific barriers, women face invalidation, harassment, discouragement, and disinterest from police, and healthcare, and legal service providers. Providers described a lack of clear protocols for addressing IPV. These findings reveal that much remains to be done to reduce barriers to women’s help-seeking for IPV at the organizational and systemic levels.
Reducing these barriers may be most effective through interdisciplinary collaborations, such as providing trainings about how to screen women for IPV exposure as a routine part of service provision. This seems particularly important in the medical field, with studies in this review demonstrating that healthcare providers do not know how to ask about IPV and only inquire about IPV exposure sporadically. It would be greatly beneficial, therefore, if service providers, and specifically medical providers, ask women about IPV exposure routinely and directly. Furthermore, creating protocols for referring women to other services when IPV is detected is also important given that providers in this review reported frustration about not knowing what to do once IPV was detected. Given the dearth of services available in rural areas across multiple studies, particular attention should be paid to creating formal services outside of urban centers.
Trainings should be implemented about how to respond to IPV-exposed women, since the current review found that service providers across organizations and countries may invalidate, shame, revictimize, and harass women who disclose IPV. Women in multiple contexts described prior negative reactions by service providers as leading to discouragement about seeking help in the future. Teaching service providers about how to validate women’s experiences, educate them about their rights, and follow through on women’s claims in alignment with formal legal guidelines may help to build women’s trust in formal services. For example, Ammar et al. (2005) published recommendations for training police in the United States to better serve Latinas exposed to IPV, including improving police sensitivity to IPV dynamics and culturally sensitive responses. However, the literature is greatly lacking about how to improve services providers’ responses to women seeking help for IPV in LA’s Spanish-speaking countries. Clinical trials research in LA that implements trainings for providers to improve their sensitivity to the needs of women exposed to IPV represents a key future direction.
Understanding Interpersonal Relationships’ Role in Formal Help-Seeking for IPV
Interpersonal barriers arose from women’s relationships with their partners, family members, and children. Partner-related barriers included experiencing perceived less severe IPV, experiencing coercive control, and economic abuse. Worldwide, interventions have been developed that aim to reduce men’s IPV perpetration, but a recent meta-analysis found that little evidence exists for any effective intervention to reduce perpetration by adult men (Stephens-Lewis et al., 2021). Instead, gender-transformative violence prevention interventions show great promise for early intervention, such as the Program H intervention from Brazil and Mexico (Promundo et al., 2013), which foster adolescent boys’ critical analysis of and skills to challenge gender norms, and encourage equitable treatment of their female peers.
Studies reported that children are a barrier to women’s help-seeking, although the studies did not explain why children function as a barrier. One study in Mexico (published after the current review’s literature search) found child-related barriers such as worries that children would be subjected to poverty if women separated from their partners, and partners threatening to take women’s children if women sought help for IPV (Carney et al., 2022). Providers’ role in reducing child-related barriers may thus include educating women about laws related to child support, custody, and child protection. These findings underscore the importance of service integration across sectors to combat interpersonal barriers to formal help-seeking for IPV.
Since family is a primary setting for the transmission of cultural values regarding gender roles and power structures (e.g., Musitu, 2006), the current study’s findings indicate that more research is needed to understand family’s complex role in women’s help-seeking for IPV. Family hindered women’s help-seeking from formal IPV supports by normalizing IPV, persuading women to not seek help to maintain the family’s reputation, and pressuring women to stay in violent relationships. However, families’ roles in women’s navigation of IPV is complex. Two studies in this review (Cripe et al., 2015; Willie et al., 2020) also found that women’s families facilitated women’s help-seeking for IPV. Thus, while family represents a key source of informal social support for many women, family can also simultaneously reinforce harmful expectations about gendered power dynamics that prevent women from seeking help for IPV.
Contending With Barriers at the Intrapersonal Level
Many evidence-based interventions developed in high-income countries for women exposed to IPV utilize cognitive-behavioral approaches (see Trabold et al., 2020, for review) to intervene with intrapersonal processes that may represent barriers to help-seeking, such as shame, minimizing the impact of IPV, or lack of trust in others. However, few evidence-based interventions have been developed specifically for IPV-exposed women in LA. Interventions developed within LA (Cripe et al., 2010; Gupta et al., 2017) represent promising first steps in addressing this gap. The development and implementation of additional culturally relevant interventions for women exposed to IPV in LA is a much-needed area of future research.
Alvarez and Fedock (2018) called for intervention research tailored to support Latinas. The current review’s findings indicate that future interventions to be implemented in LA should be mindful that women may not understand what constitutes IPV and may believe IPV is normal. Women may distrust service providers or be unaware of existing community resources. Interventions should educate women about what IPV is while being mindful that it may take time for women to trust providers. Community resources for women exposed to IPV should engage in multiple strategies to reach women who do not know about IPV-related services. Finally, given that women may experience shame about IPV, future interventions should integrate content about the role of cultural and interpersonal messaging that contribute to women’s shame. This may provide women space to explore what larger cultural messaging they want to ascribe to.
Limitations
The current review sought to provide a regional overview of patterns across contexts, but it is critical to underscore that the wide variation of and nuance in women’s experiences within contexts is beyond the scope of this review. LA is vast, with immense variability within countries regarding resource availability, language, and culture. Elucidating within-country differences in women’s experiences is better left to individual studies within a particular context.
Other limitations include the exclusion of the non-Spanish-speaking countries in LA (i.e., Belize, Brazil, French Guiana, Guyana, Suriname). Literature from these countries, as well as any literature published in indigenous languages in Spanish-speaking countries, was excluded from the current review. Additionally, many titles and abstracts that were reviewed during the literature search did not state the country where data were collected; the current review may have overlooked articles that met inclusion criteria for this reason. It is recommended that future manuscripts explicitly describe the location where data were collected. No intercoder reliability was conducted for study inclusion. Additionally, no risk of bias assessment was conducted on the included studies.
All included studies used cross-sectional data collection, representing a limitation to this review’s findings. Longitudinal studies of help-seeking for IPV from formal resources represent a key future direction that could identify which barriers endure over time and mechanisms that may facilitate women’s help-seeking. Additionally, four studies did not specify which method they used to analyze qualitative data, creating a lack of clarity in understanding their methods. Finally, 9 of the 19 included articles (i.e., 47%) were from Mexico. Some findings may therefore be biased toward Mexican women’s experiences with formal help-seeking for IPV, while no literature was found from Argentina, Costa Rica, Cuba, Paraguay, Uruguay, or Venezuela. This absence highlights an important direction for future research and represents a gap in the representativeness of the current review. Finally, IPV can happen to people of any gender; the current review focused on women’s experiences in LA, but this work could be meaningfully expanded to include IPV-exposed individuals with other gender identities.
Footnotes
Declaration of Conflicting Interests
The author declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was supported by a graduate student fellowship from the Eck Institute for Global Health at the University of Notre Dame.
