Abstract

Dear Editor,
We would like to share the findings of our study on the quality of assessment of postural hypotension in a UK District General Hospital (DGH). Hospital admissions related to postural hypotension is common, particularly in the elderly population, and can have a significant negative impact on their quality of life. 1 Our findings are of great interest to physicians who care for general internal medical patients.
The National Institute for Health and Care Excellence guidelines advise assessing for postural hypotension in patients who are symptomatic or those who present with a fall. 2 A drop in systolic blood pressure (BP) ⩾20 mm Hg and/or diastolic BP ⩾10 mm Hg within 3 min of standing from a sitting/lying position can be diagnostic. 3 An accompanying increase in heart rate (HR) of <15 beats per minute may suggest a neurogenic cause, and an increase in HR of >15 beats per minute may suggest a non-neurogenic cause, that is, cardiogenic. 4 However, postural BP measurements are generally poorly done in the inpatient setting. Often, only one set of BP measurement is recorded without HR reading.
To examine whether postural BP assessments were requested and performed appropriately with HR recorded at 0 and 3 min, we reviewed the records of all patients admitted to Medical Assessment Unit at King’s Mill Hospital between 1st and 31st March 2023 with a plan for a postural BP check or one of these symptoms: collapse, fall, syncope, loss of consciousness or unresponsive episode. Demographics, relevant comorbidities and reasons for admissions of all patients can be found in Table 1.
Patient demographics and reasons for admissions.
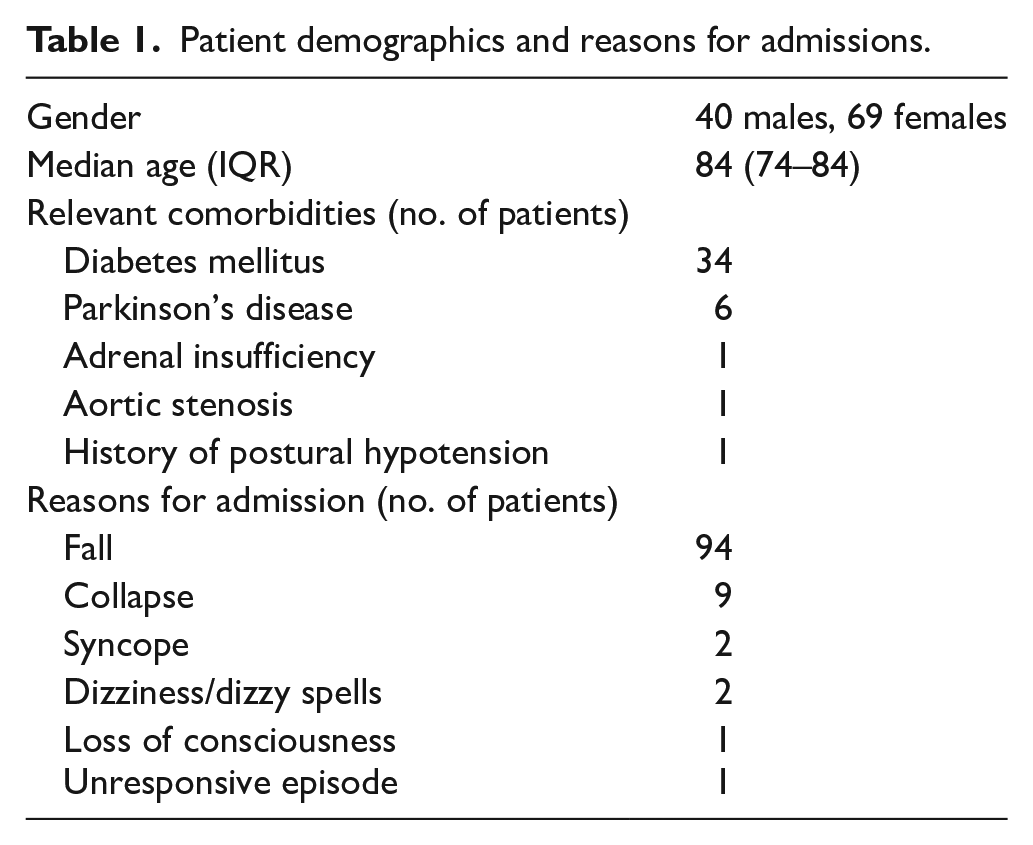
Despite their presenting complaints, only 65 patients (60%) had postural BP assessment documented as part of their initial medical plans. 53 (82%) of these patients had their postural BP measured, and 14 (26%) of whom had it measured correctly at a three-minute interval. The majority of assessments were completed in >3 min. None had a concurrent HR assessment performed.
Although understaffing could be a contributing factor, it is important that the standing BP is measured at the correct time frame as premature readings can lead to false negative results. Whilst falls are often multifactorial and not all causes can be easily addressed, postural hypotension is a condition that is treatable. An assessment of the HR allows clinicians to have a better understanding of the aetiology of a patient’s postural drop and delineate whether an underlying cardiogenic or neurogenic cause exists. Management and treatment plans can then be tailored to the patient based on the pathophysiological cause of the postural hypotension.
Education among physicians and nursing teams and mandatory entry of concurrent HR when uploading postural BP electronically should improve postural BP assessment. Physicians, especially those who work in acute medicine, would want to reflect on their local practice in light of our findings. A multicentre study involving regional tertiary centres and DGHs in the future will provide a better overview of the quality in assessing this commonly encountered medical complaint.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
