Abstract
Background
Doctors often deal with end-of-life issues other than assisted death, such as incompetent patients and treatment withdrawal, including food and fluids.
Methods
A link to a questionnaire was sent by email three times, at one-week intervals, to the doctors registered in the Northern Section of the Portuguese Medical Association.
Results
The questionnaire was returned by 1148 (9%) physicians. This study shows that only a minority of Portuguese doctors were willing to administer drugs in lethal doses to cognitively incompetent patients at the request of a family member or other close person, and even less would do it on their initiative. Most doctors favored the withdrawal of life support measures in advanced and progressive diseases at the patient’s request. Still, much fewer doctors agreed with the suspension of supportive life measures at the request of a family member, another close person, or by their own unilateral decision. However, fewer agreed with that action concerning the rest of the food and fluids. Portuguese doctors favor the administration of drugs for suffering control, even foreseeing they could shorten life.
Conclusion
Most doctors in this study respect patients’ autonomy but disagree with measures decided by others that have an impact on patients’ survival. They also agree with the administration of drugs for suffering control, even considering the possibility of shortening life.
Keywords
Introduction
The social and economic development and the massive evolution of medicine, mainly from the middle of the 20th century, significantly prolonged human life expectancy. Modern medicine has many treatments and equipment to cure or prolong life. However, these methods are often used in patients with far advanced and irreversible diseases where it is not advisable to employ them because they may be useless or even detrimental. Withholding or withdrawing treatments often imply difficult decisions because, besides clinical considerations, they involve ethical, cultural, religious, and even legal issues.1–4
Euthanasia and physician-assisted suicide are extensively discussed in medical and non-medical literature. Nowadays, several countries and states legalized assisted death. The Portuguese Parliament approved assisted death in Portugal, but the law is not yet in force. Those issues are perhaps the most visible ones, but doctors and health care teams may have to deal with many other difficult decisions. Patients and families should also have an essential role in those decisions, directly or through advanced directives whenever possible. After all, they are the most interested persons in those processes, and their involvement may be what divides a legitimate from an illegitimate decision. However, some unilateral decisions taken by health professionals are also legitimate.
Other decisions about end-of-life issues include withholding or withdrawing artificial ventilation, hemodialysis, transfusions, or antibiotics. Even after those decisions, one question remains: should nutrition and hydration also be withheld or withdrawn?
Withholding and withdrawing some treatments are sometimes deemed euthanasia, but those actions are different. When appropriately taken, those actions respect patients’ autonomy or avoid prolonging the death process. There is an essential distinction between prolonging life and prolonging the dying process when patients are naturally close to death. When competent patients request treatment withdrawal, doctors should respect their wishes. However, how to decide when patients are incompetent? Is it acceptable that a family member decides for them, or can the doctor or the health team decide based only on their judgment?
A study in six European countries, which did not include Portugal, concluded that medical decisions frequently precede dying in all participating countries. However, patients and relatives are generally involved in decision-making in countries where the frequency of making these decisions is high. 5
Ten years ago, a study about oncologists’ attitudes on end-of-life issues, excluding assisted death, was published to find out their opinion on those questions. 6 Now the scope of this study is broader, including doctors from all specialties concerning the same issues.
Methods
The author carried out this study in collaboration with the Portuguese Medical Association. This study used a questionnaire whose development was described elsewhere. 7 A link to the questionnaire was emailed to doctors identified on the Northern Section of the Portuguese Medical Association list The questionnaire was sent three times, at one-week intervals, in February 2019. The link also explained the study and assured the anonymity of the participants. The author gave an interview to one of the main Portuguese television channels. The interview was broadcasted on news programs, including in prime time, as an additional means of encouraging doctors to reply.
The questionnaire included questions on various end-of-life issues and those concerning demographic data on assisted death and palliative care and other attitudes on end-of-life decisions. The study presented here focuses on attitudes other than assisted death.
The chi-square test was used in the statistical analysis to evaluate the existence or absence of associations between categorical variables. The variables with a significant association in univariable analysis were further analyzed using a multinomial logistic regression for the multivariable analyses. The level of significance was deemed to be 0.05. The IBM SPSS Statistics version 25.0 software was used to analyze the data. The factors included in the analyses were the demographic data in Table 1.
Demographic data.
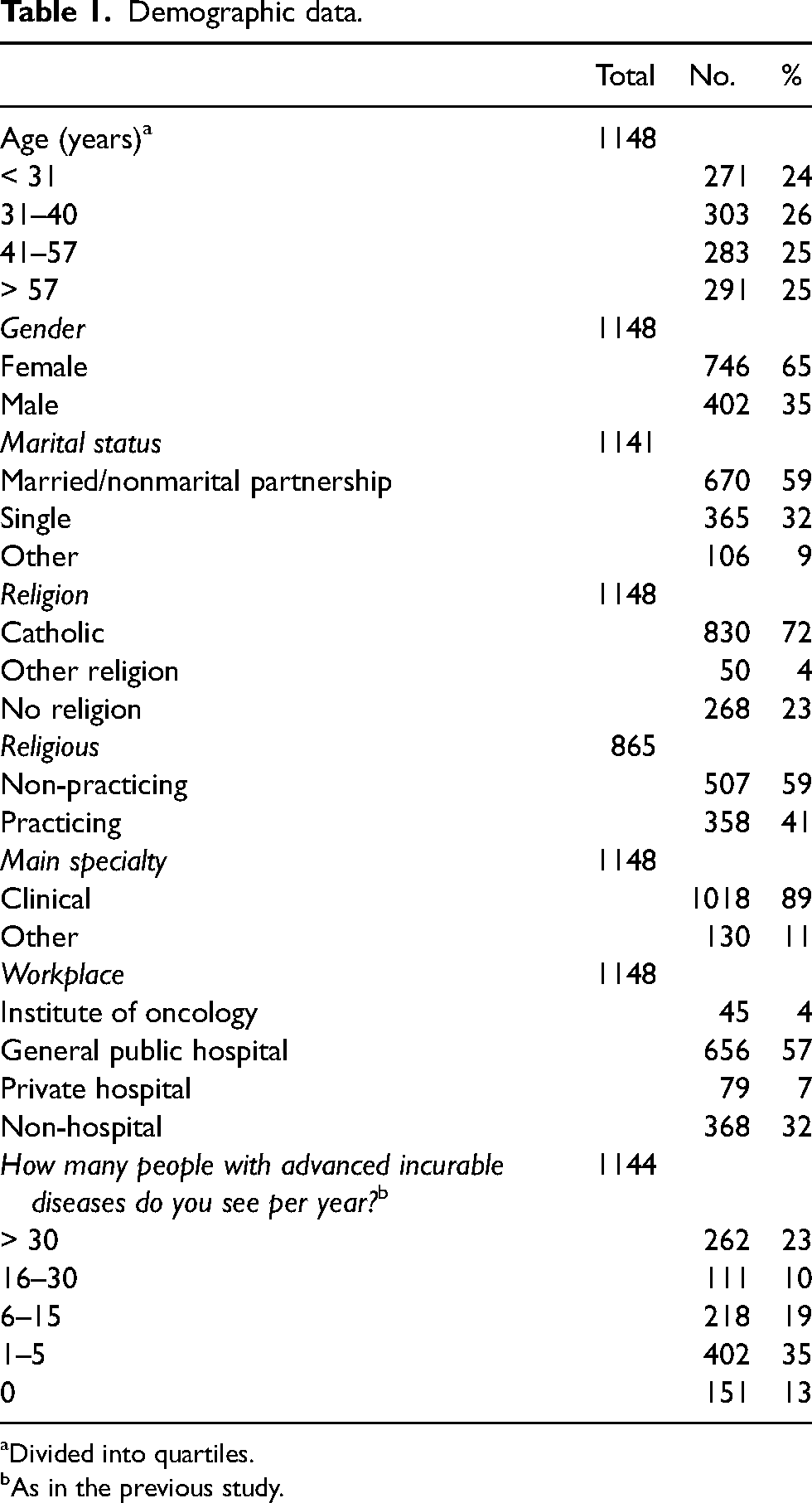
Divided into quartiles.
As in the previous study.
The Portuguese Medical Association evaluated, authorized, and collaborated with this study.
Results
Of the 13,192 questionnaires sent, 1148 (9%) were received. Table 1 displays the demographic data of the doctors. Concerning gender and age, there are significant differences (p < 0.001) between the entire population of physicians and those who replied to the questionnaires. Therefore, it is not representative of the population studied. The questionnaires were completed carefully and consistently, as most questions had a 100% rate of replies, and the highest rate for any missing answers was never higher than 0.7%.
Cognitively incompetent patients
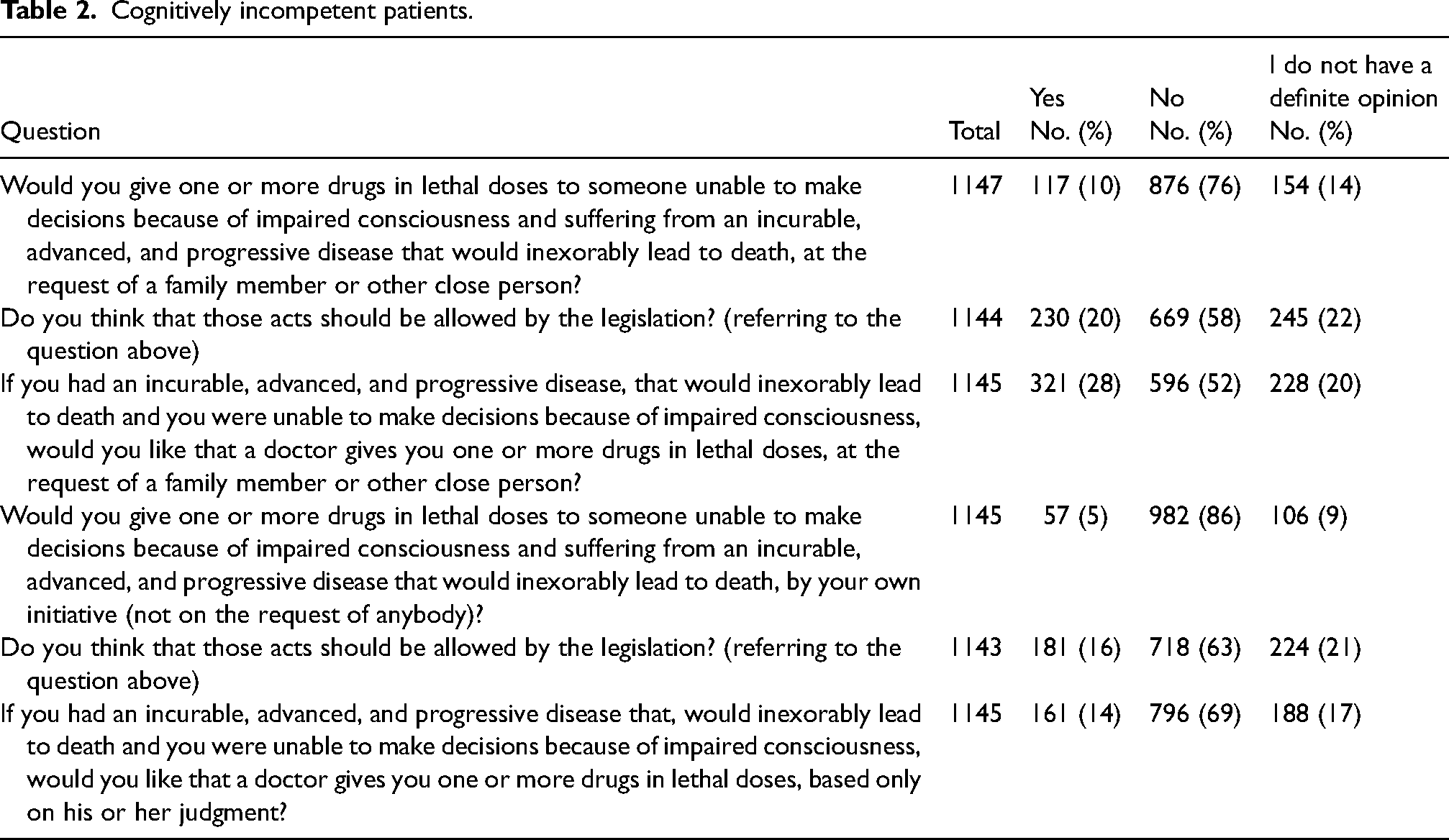
To the question, “Would you give one or more drugs in lethal doses to someone unable to make decisions because of impaired consciousness and suffering from an incurable, advanced and progressive disease that would inexorably lead to death, at the request of a family member or other close person?,” 117 (10%) answered, “yes” (Table 2). In the univariable analysis, gender, religion, religious practice, specialty, and the number of patients seen last year, were associated with the doctors’ opinion. In contrast, age, marital status, and workplace were not. In the multivariable analysis, catholic doctors, religious practicing, and clinical specialties were less often in favor of those practices (Table 3). Fourteen (1%) doctors said they received such requests frequently, and 146 (13%) received them rarely; 10(1%) said they had already performed such an act.
Cognitively incompetent patients.
Cognitively incompetent patients – multivariable analyses.
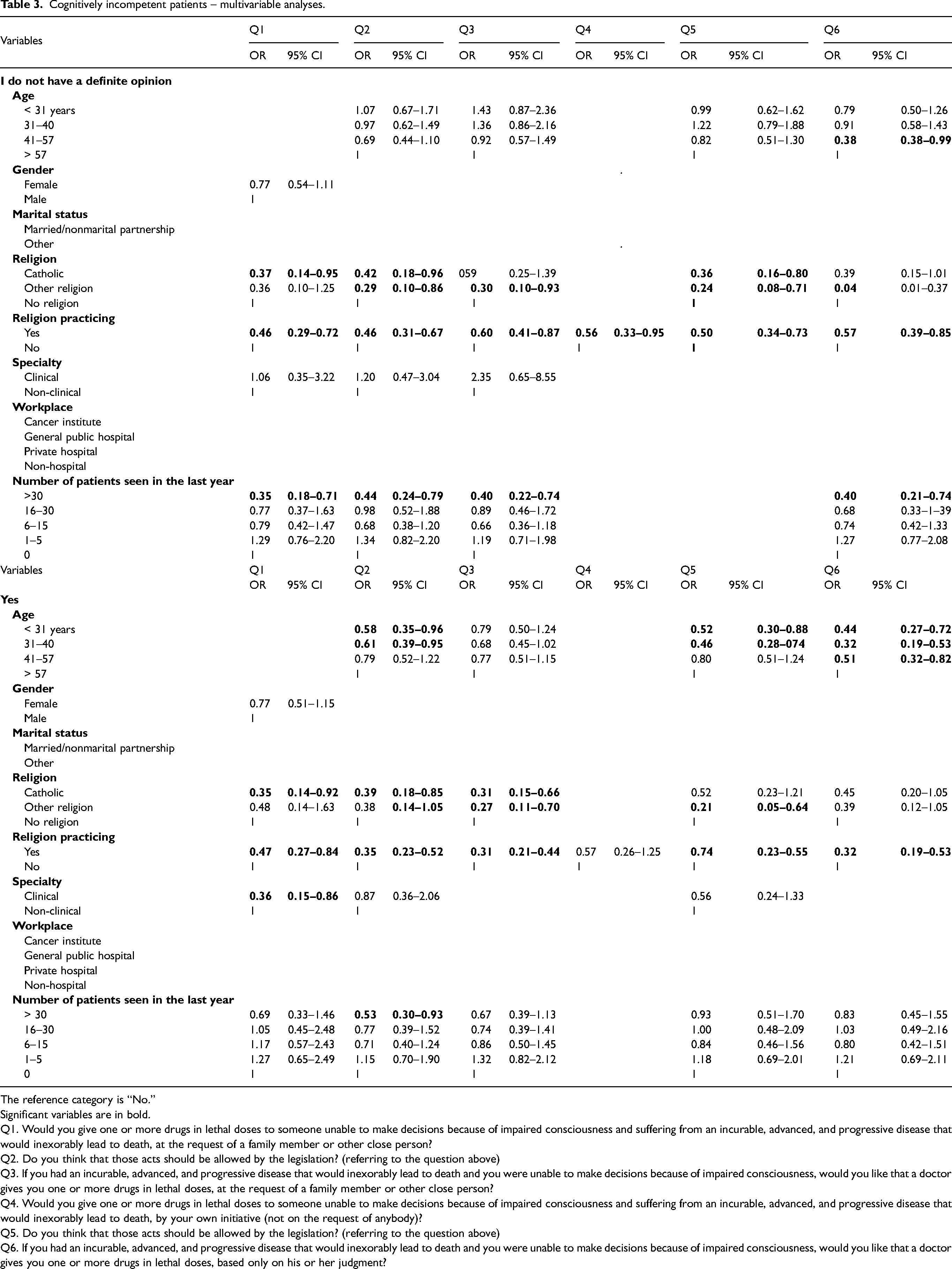
The reference category is “No.”
Significant variables are in bold.
Q1. Would you give one or more drugs in lethal doses to someone unable to make decisions because of impaired consciousness and suffering from an incurable, advanced, and progressive disease that would inexorably lead to death, at the request of a family member or other close person?
Q2. Do you think that those acts should be allowed by the legislation? (referring to the question above)
Q3. If you had an incurable, advanced, and progressive disease that would inexorably lead to death and you were unable to make decisions because of impaired consciousness, would you like that a doctor gives you one or more drugs in lethal doses, at the request of a family member or other close person?
Q4. Would you give one or more drugs in lethal doses to someone unable to make decisions because of impaired consciousness and suffering from an incurable, advanced, and progressive disease that would inexorably lead to death, by your own initiative (not on the request of anybody)?
Q5. Do you think that those acts should be allowed by the legislation? (referring to the question above)
Q6. If you had an incurable, advanced, and progressive disease that would inexorably lead to death and you were unable to make decisions because of impaired consciousness, would you like that a doctor gives you one or more drugs in lethal doses, based only on his or her judgment?
Referring to the above question, 230 (20%) patients thought the legislation should allow those acts (Table 2). In the univariable analysis, age, religion, religious practice, specialty, and the number of patients seen, were associated with that opinion, whereas gender, marital status, and workplace were not. In the univariable analysis, age, religion, religious practice, specialty, and the number of patients seen, were associated with that opinion, whereas gender, marital status, and workplace were not. In a multivariable analysis, younger doctors, religion, religious practicing, and the higher number of patients with advanced diseases seen were less likely to agree with the legalization of those practices (Table 3).
To the question, “If you had an incurable, advanced, and progressive disease, that would inexorably lead to death, and you were unable to make decisions because of impaired consciousness, would you like that a doctor gives you one or more drugs in lethal doses, at the request of a family member or other close person?,” 321 (28%) answered, “yes” (Table 2). In the univariable analysis, age, religion, religious practice, specialty, and the number of patients favored that opinion, whereas gender, marital status, and workplace did not. In the multivariable analysis, only religion and religious practices were more likely to be against that practice.
The question “Would you give one or more drugs in lethal doses to someone unable to make decisions because of impaired consciousness and suffering from an incurable, advanced, and progressive disease that would inexorably lead to death, by your initiative (not on the request of anybody)?,” had a positive answer from 57 (5%) doctors (Table 2), and 15 (1%) said they had already done it; 181 (16%) thought that those acts should be allowed by the law. In the univariable analysis, religion and religious practice were associated with that opinion. Only religious practice was less likely to be associated with supporting that practice in the multivariable analysis.
To the question, “If you had an incurable, advanced, and progressive disease, that would inexorably lead to death, and you were unable to make decisions because of impaired consciousness, would you like that a doctor gives you one or more drugs in lethal doses, based only on his or her judgment?,” 161 (14%) answered, “yes” (Table 2). In the univariable analysis, age, religion, religious practice, and the number of patients seen, were associated with that opinion. Only age and religious practice were associated with that opinion in the multivariable analysis, less likely to support it.
Treatment withdrawal
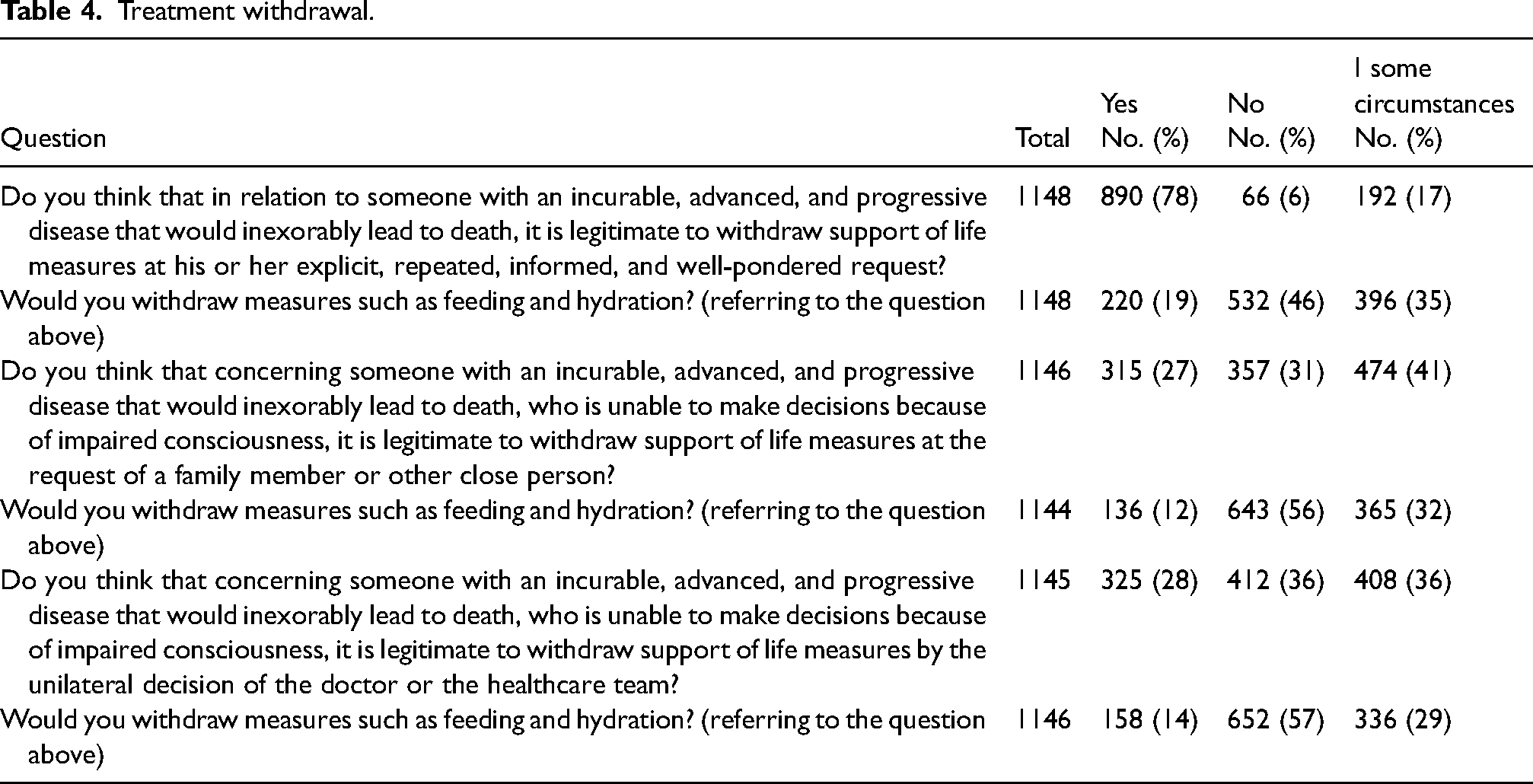
To the question “Do you think that concerning someone with an incurable, advanced, and progressive disease that would inexorably lead to death, it is legitimate to withdraw support of life measures at his or her explicit, repeated, informed, and well-pondered request?” 890 (78%) doctors replied, “yes” (Table 4). In univariable analysis, age, gender, marital status, religion, religious practice, workplace, and the number of patients with advanced diseases seen in the last year were significantly associated with that opinion. In the multivariable analysis, the younger doctors and those who see more patients are more likely to answer yes. In contrast, religious non-Catholic doctors and religious practicing were more likely to answer differently (Table 5).
Treatment withdrawal.

Treatment withdrawal – multivariable analyses.
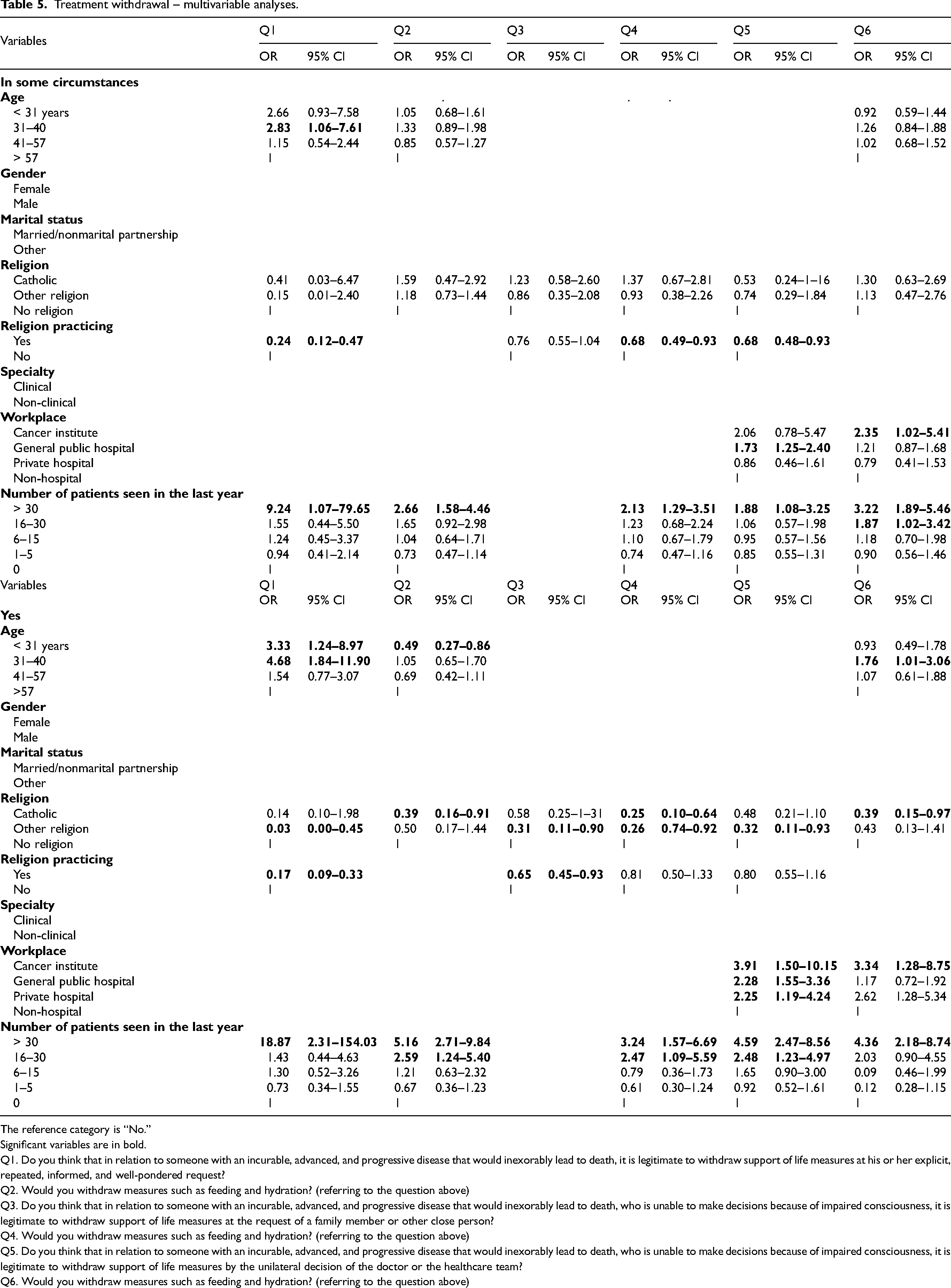
The reference category is “No.”
Significant variables are in bold.
Q1. Do you think that in relation to someone with an incurable, advanced, and progressive disease that would inexorably lead to death, it is legitimate to withdraw support of life measures at his or her explicit, repeated, informed, and well-pondered request?
Q2. Would you withdraw measures such as feeding and hydration? (referring to the question above)
Q3. Do you think that in relation to someone with an incurable, advanced, and progressive disease that would inexorably lead to death, who is unable to make decisions because of impaired consciousness, it is legitimate to withdraw support of life measures at the request of a family member or other close person?
Q4. Would you withdraw measures such as feeding and hydration? (referring to the question above)
Q5. Do you think that in relation to someone with an incurable, advanced, and progressive disease that would inexorably lead to death, who is unable to make decisions because of impaired consciousness, it is legitimate to withdraw support of life measures by the unilateral decision of the doctor or the healthcare team?
Q6. Would you withdraw measures such as feeding and hydration? (referring to the question above)
Concerning the question, “Would you withdraw measures such as feeding and hydration? (referring to the question above),” only 220 (19%) replied, “yes” (Table 4). Age, religion, religious practice, workplace, and the number of patients with advanced diseases seen were associated with that opinion in the univariable analysis. Doctors seeing more patients favored feeding and hydration withdrawal in the multivariable analysis; on the contrary, younger and catholic doctors did not.
To the question, “Do you think that concerning someone with an incurable, advanced, and progressive disease that would inexorably lead to death, who is unable to make decisions because of impaired consciousness, it is legitimate to withdraw support of life measures at the request of a family member or other close person?,” 315 (27%) doctors responded, “yes” (Table 4). In the univariable analysis, religion, religious practice, and specialty were statistically associated with that answer. In the multivariable analysis, only non-Catholic religion and religious practices were more likely to disapprove of that opinion (Table 5). To the question, “Would you withdraw measures such as feeding and hydration? (referring to the question above),” only 136 (12%) answered “yes.” In the multivariable analysis, doctors who see more patients were more likely to favor that position, and religious doctors were more likely to disapprove.
To the question, “Do you think that concerning someone with an incurable, advanced, and progressive disease that would inexorably lead to death, who is unable to make decisions because of impaired consciousness, it is legitimate to withdraw support of life measures by the unilateral decision of the doctor or the healthcare team?,” 325 (28%) patients responded “yes.” In univariable analysis, age, marital status, religion, religious practicing, specialty, workplace, and the number of patients seen were statistically associated with that answer. In the multivariable analysis, doctors working in hospitals were more likely to favor that practice, and doctors who see more patients; on the other hand, doctors with non-Catholic religions were more likely to be against that opinion. To the question “Would you withdraw measures such as feeding and hydration? (referring to the question above),” only 158 (14%) replied “yes.” In a multivariable analysis, doctors in the age range of 31 and 40 years, doctors working in cancer institutes, and doctors who see more patients were likelier to favor that practice. In contrast, Catholic doctors were more likely to disapprove of that practice (Table 5).
Suffering control
To the question of administering drugs (e.g. morphine) for suffering control, even foreseeing they could shorten life, 969 (84%) answered: whenever it is necessary. Furthermore, to the doctor’s hypothesis being in that suffering situation, 1103 (96%) would like someone to administer such a drug to relieve their suffering even if it could shorten their lives.
Discussion
Cognitively incompetent patients
The practice, called nonvoluntary euthanasia, meaning killing patients incapable of giving consent, was first reported in Nederland’s. 8 The term euthanasia applied to those acts is misleading. Euthanasia is usually defined as a response to a voluntary request from a patient. 9 Therefore, voluntary euthanasia is an incongruent term as it implies that euthanasia can be nonvoluntary or involuntary. This study shows that only a minority of Portuguese doctors were willing to participate in the hastened death of cognitively incompetent patients at the request of a family member or other close person. Even fewer doctors would do it on their initiative.
More doctors, but even so, a minority, answered that if they were the patient, they want their death hastened at the request of a family member or other close person. A fewer number would want doctors to take that decision on their initiative. The same gave similar answers when asked about euthanasia in another study. 10 Our study published in 2010 also showed similar results. 6 Those data mean that some doctors want for themselves what they are not prepared to do for their patients. They feel perhaps that those decisions involve a responsibility they cannot take. A small percentage of doctors, although a little higher, think that the legislation should allow those acts.
The essential factors consistently associated with doctors’ opinions were religion and religious practice. It is not surprising that religious doctors were more likely to be against those practices, as several studies showed that they oppose euthanasia and assisted suicide more often than non-religious doctors.10–18 Nevertheless, not all studies reach that conclusion.15,19,20 Younger doctors were also more against the legalization of giving lethal doses to cognitively incompetent patients. This position is curious because the same younger doctors favored more assisted death practices in another study. 10 They were even against those practices if they were the patient.
Doctors who followed more patients with advanced diseases were more frequently against the legalization of those acts. Authors of other studies also observed that physicians who more frequently deal with patients with far advanced diseases were more likely to oppose assisted death than others,12,14,21 but not in all. 22 Emmanuel explains this fact as the different perspectives of those doctors who are more distant from terminally ill patients and see the problem of assisted death in the abstract as a philosophical question. Nevertheless, doctors who deal directly with the situations may see them as more authentic and personal. 14
Treatment withdrawal
Only 6% of doctors answered “no” to withdrawing support of life measures in advanced and progressive diseases at the patient’s request. Seventy-eight percent answered “yes,” and 17% answered, “in some circumstances.” However, much fewer doctors agreed to suspend supportive life measures at the request of others or by their unilateral decision. These data suggest that most Portuguese physicians are prepared to respect patients’ autonomy but do not recognize the right of others to decide on patients’ behalf.
As in many other countries, 23 the Portuguese law grants patients without cognitive impairment the right to refuse therapies, even those that sustain life. Under Portuguese law, family members are not legal representatives of mentally incompetent patients. Therefore, the wishes of family members are not determinant for decision-making in those situations. The role that families may have in those situations, according to the law, is different among countries. For example, in the United Kingdom, the law is like the Portuguese one. 24 On the contrary, in the United States, patients’ relatives may be legally appointed decision-making surrogates. 23
Concerning suspending feeding and hydration, the percentage of “No” varied from 46 to 57%, and the percentage of “In some circumstances” was roughly one-third. Therefore, most physicians would not suspend feeding and hydration, but about one-third admitted it could be justified in some circumstances. Probably most consider feeding and hydration basic care and not a treatment even if delivered through medical devices. When patients at the end of life are able and willing to eat and drink, it is straightforward that food and fluids should be provided; without a doubt, this is basic care. However, if patients cannot do so, the provision of nutrition by artificial means is controversial; if this is basic care or medical treatment is debatable. A study in six European countries, which did not include Portugal, showed that decisions to forgo feeding and hydration varied among countries and that withholding was more frequent than withdrawal. 25
The results of this study go in a similar direction compared to the previous Portuguese study. 6 In this study, younger doctors tend to favor treatment withdrawal at the patients’ request, but most did not favor withdrawal of feeding and hydration. Doctors who see more patients mostly favor treatment withdrawal and even feeding and hydration. On the contrary are religious doctors who do not favor withdrawing treatment, feeding, and hydration, even at the patients’ request The comparison with other studies is problematic because physicians’ characteristics are usually not as detailed as in this study.
Suffering control
Portuguese doctors seem to accept the administration of drugs for suffering control, even foreseeing they could shorten life. If the doctors themselves were suffering from advanced disease, even more of them would want to receive a drug such as morphine, even foreseeing that it could shorten their life. This attitude is often justified by the doctrine of double effect. However, Sykes and Thorns conclude that this doctrine is not essential for the justification of using these drugs because there is no evidence that the use of opioids and sedatives is associated with hastening death and may act as a deterrent to the provision of good symptom control. 26
Limitations of this study
The main weakness of this study is the relatively small percentage of questionnaires sent back and the lack of representativeness of the sample of physicians. This fact may cast doubts on the generalizability of the data. Much effort was made to call the attention of doctors to this study, and obviously, they cannot be compelled to reply. Nevertheless, the absolute number of doctors who replied is not low, and this is, so far, the best approximation to the opinions of Portuguese doctors on end-of-life issues, as there are no other data on this topic in Portugal.
Conclusion
Most doctors in this study disagree with administering drugs to incompetent patients with incurable, advanced, and progressive diseases. Nevertheless, they would respect the patient’s wishes to withdraw life-supporting measures, although not so much when the request came from another person. Most disagree with the withdrawal of feeding and hydration. Physicians, nonetheless, accept administering drugs for suffering control, even foreseeing it could hasten death.
Footnotes
Acknowledgements
The author would like to thank the Portuguese Medical Association (Ordem dos Médicos), mainly the Northern Section, for assisting in this study.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
