Abstract
Social constraints posed by work schedules influence sleep duration and timing. Everyday light exposure can help (or hinder) sleep outcomes. This study investigated the differences in the relationship between light exposure and sleep outcomes on days with and without social constraints using ambulatory assessment for 4–6 weeks for 15 office employees. The effects of light on sleep were investigated for both clock time and wake time (related to individual sleep times). Participants were exposed to more light during the morning and afternoon on workdays, and sleep times were later on days without social constraints. The relationship between light exposure and sleep was more pronounced, or sometimes even only present, for days without social constraints. In addition, no differences were found between clock time and wake time, which underlines the complexity of the relationship between everyday light exposure and sleep. Despite increased light exposure during workdays, the effects of light on sleep were more pronounced on days without social constraints. It may signal that office workers need a more substantial circadian stimulus (i.e. higher light exposure) for light to influence sleep outcomes on days with social constraints.
1. Introduction
Humans have synchronized their activity and rest cycles for centuries with the daily solar cycle dictated by light days and dark nights. Light still is the most important cue for their biological clock and is highly related to sleep quality and duration. 1 Modern working life deviates from this sleep/wake, activity/rest and light/dark relationship in at least three drastic ways. First, the invention of electric light has enabled humans to stay awake and work before sunrise and after sunset. Second, most daytime workers spend a much more significant proportion of their time indoors exposed to electric light, which differs in intensity and spectral composition from daylight. Third, humans now organize their activity and rest cycles according to the 24-hour clock, independent of dusk and dawn. All three of these changes can potentially affect sleep duration and quality for daytime workers. The question is how these changes in both light exposure amount and its timing affect daytime workers’ sleep.
Many people dread the sound of the alarm clock in the morning. Still, most people need an alarm to get to work (or school) on time. The so-called social constraints posed by work hours limit when and for how long daytime workers can sleep. A study looking at sleep before and after retirement found that even though weekend sleep remained the same, sleep during weekdays was significantly longer after retirement, which indicated that social constraints imposed by working hours cause daytime workers to build up sleep deprivation. 2 On the contrary, during weekends – when these social constraints are often absent – people tend to sleep later and longer, catching up on sleep loss accumulated during weekdays.3–5 Differences between weekday and weekend sleep schedules – also referred to as social jetlag – can differ substantially depending on a person’s chronotype. The most considerable differences are often found in people with a late chronotype. 3
The extent of social jetlag has been reported to be related to human performance and well-being during weekdays4,6 as well as to long-term health outcomes such as affective disorders and cardiometabolic risk.6–8 Such effects were mainly present when the misalignment between chronotype and social hours resulted in short sleep duration. 7 Short sleep duration, as well as a more considerable variability in sleep schedules, has been found related to adverse health outcomes6,9,10 and even mortality. 9 Importantly, catch-up sleep at the weekend appears to counter the adverse effects of short sleep duration during weekdays in some studies.6,9 In contrast, others have found that sleeping in during the weekend can increase sleepiness the following week. 4
It is not only sleep that differs between workdays and the weekend. Ambulatory research has indicated that daytime workers are exposed to higher light levels on working days than during the weekend due to, for example, earlier rising times and the daily commute (outdoors) to work.11–13 Everyday light exposure has been found to influence sleep and, depending on the light’s timing and spectral composition, it can advance or delay sleep.14,15 The so-called dose–response curves investigating the effects of light exposure on sleep have indicated that bright light in the morning can phase-advance sleep, whereas bright light in the late at night delays sleep.16,17 However, these studies have been conducted in laboratory settings with (very) controlled conditions. Field studies investigating the effects of everyday light exposure on sleep outcomes only partly confirm these findings11,13,18 These studies point to a more complex relationship between light and sleep in everyday life. For instance, light effects can depend on prior light exposure.19–23
This study investigated whether sleep and light exposure for office workers differed between days with and without social constraints. In addition, the effects of (the timing of) light exposure on sleep outcomes were studied. The effects of light exposure on sleep were investigated based on clock time (morning, afternoon and evening) and wake time (the first 6 hours after waking up and the last 6 hours before going to sleep, independent of clock time). It was hypothesized that (1) the light effects would depend on whether or not social constraints were present, with more pronounced effects of light exposure in the morning and evening on sleep on days without social constraints, as sleep on these days was less dictated by social schedules. In addition, it was expected that (2) on days without social constraints, wake time would be a better predictor of the effects of light on sleep than clock time. Lastly, it was hypothesized that (3a) an increase in light exposure in the morning would advance sleep, (3b) afternoon light exposure would not influence sleep and (3c) an increase in light exposure in the evening would delay sleep.
2. Method
In an ambulatory field study, the personal light exposure and sleep quality of 15 participants were monitored for 4–6 weeks during workdays and weekends. A more extensive description of the methodology can be found in Aries et al. 24
2.1 Participants
The 15 participants (7 females, aged between 29 and 63 years, M = 43.33 ± 10.42) included in the study were office workers of two companies working in separate buildings in Sweden (both ~57°N, 14°E). Exclusion criteria were being pregnant, using sleep medication, being professionally diagnosed with a sleep disorder, working less than 4 days per week and having children younger than 1 year.
2.2 Materials
Light exposure was measured with a wearable light detector (LYS Technologies LTD™) at a 15-second interval. The light sensor measures illuminance (in lux) as well as Red (R), Green (G) and Blue (B) 16-bit values. All 15 light detectors (one per person) were checked and calibrated before the study, for indoor and outdoor light conditions, against two Hagner EC1 illuminance meters (calibrated by B. Hagner AB in February 2019 with limited use after; calibration accuracy ±3%). Light exposure was investigated in terms of illuminance level. The focus was comparing days with and without social constraints and the differences between clock time and wake time. Unfortunately, sensitivity curves for the B (‘blue’) and G (‘green’) values overlapped too much for a reliable separation. Therefore, the RGB/spectral composition of the light exposure could not be studied. Sleep variables were measured with a SleepScore Max (SleepScore Labs™) sleep analyser (based on sonar and radiofrequency).
2.3 Procedure
The data collection occurred in the office and at home on workdays and days off. Participants were followed for at least 4 weeks during late winter and early spring (between 27th February and 6th April). Before the experiment, the experiment’s general setup and procedure were explained for both companies separately. The participants wore the light sensor from when they woke up until they went to bed and manually switched on the sleep device before going to sleep. All participants gave their written consent for participation and data collection. The study protocol was approved by the Swedish Ethical Review Authority (no. 2019-05453).
2.4 Data analysis
Given the nested nature of the data, Hierarchical Linear Models were used to test the relationships between light exposure and sleep outcomes, with responses nested within individuals. Five separate models were run for the morning (06.00–11.59 hours), afternoon (12.00–17.59 hours), evening (18.00–23.59 hours), the first 6 waking hours and the last 6 waking hours. The night was not considered relevant for this paper, as the focus is on daytime light exposure. In 6% of the cases, participants woke up before 6.00. Adding these cases to the data did not alter the outcomes. Three sleep variables were included as outcome variables: sleep efficiency (ratio of wake time after sleep onset and total sleep time), sleep onset and sleep offset. Full-factorial models were run with light exposure (median illuminance level; the median is taken on a group level) and social constraints (yes or no) as predictors. The median illuminance level is commonly used to indicate light exposure and is less vulnerable to outliers or skewness. 25 Median level based on group level was chosen since the analyses were also performed on a group level. As light exposure during the daytime was related to sleep outcomes during the consecutive night (and morning) in the analysis, the light exposure on Friday and Saturday was used to predict sleep outcomes on the consecutive days without social constraints (Saturday and Sunday) as participants did not have to be at work at a particular time the following morning. A previous analysis 24 indicated that sleep and light exposure differed between workdays in the office and workdays at home. Therefore, the type of day (workday at home vs. in the office) was added to all models as a control variable.
Only hours for which at least 40% of the data was above a threshold of 10 lx were included. All values were log-transformed as the illuminance values ranged between very low and very high peak values (e.g. between 10 and 29,825 lx). Light levels below 10 lx were considered not reliable based on initial data analysis (and adding these values did not alter the outcomes). Within the study period, the clock was adjusted to Daylight Saving Time (DST) on 29th March. According to an earlier study using actigraphy measures after a DST transition, 26 sleep can shorten by 40 minutes to 1 hour and sleep efficiency can decrease by approximately 10%. Especially sleep on the first Monday after the change is affected; after, effects decrease rapidly across days 1–3. Therefore, data from 3 days after DST were deleted from the analyses. However, an internal chrono-disruption manifested in sleep rhythms after the initial 3 days is highly differentiated by individual factors. 26
3. Results
A total of 124 days without social constraints (Friday and Saturday) and 279 days with social constraints (Monday to Thursday) were included in the dataset. Additional descriptions of measurements and data points can be found in Aries et al. 24
3.1 Sleep outcomes
Table 1 shows an overview of sleep outcomes for days with and without social constraints. On days without social constraints, participants went to bed on average 41 minutes later than on days with social constraints and got out of bed 96 minutes later. No significant difference in sleep efficiency was found between days with and without social constraints. See Figure 1 for an overview of wake versus clock time during the weekend and weekdays. The light grey bars represent the range of the hours included as the first 6 hours after waking up on days with and without social constraints, whereas the black bars represent the range of the times of the last 6 hours of being awake on these days. This figure illustrates a relatively large variability in sleep onset and offset during weekdays.
Overview of the EMMs with SEs for sleep outcomes for days with and without social constraints. The text in bold indicates a significant difference between a day with and without social constraints
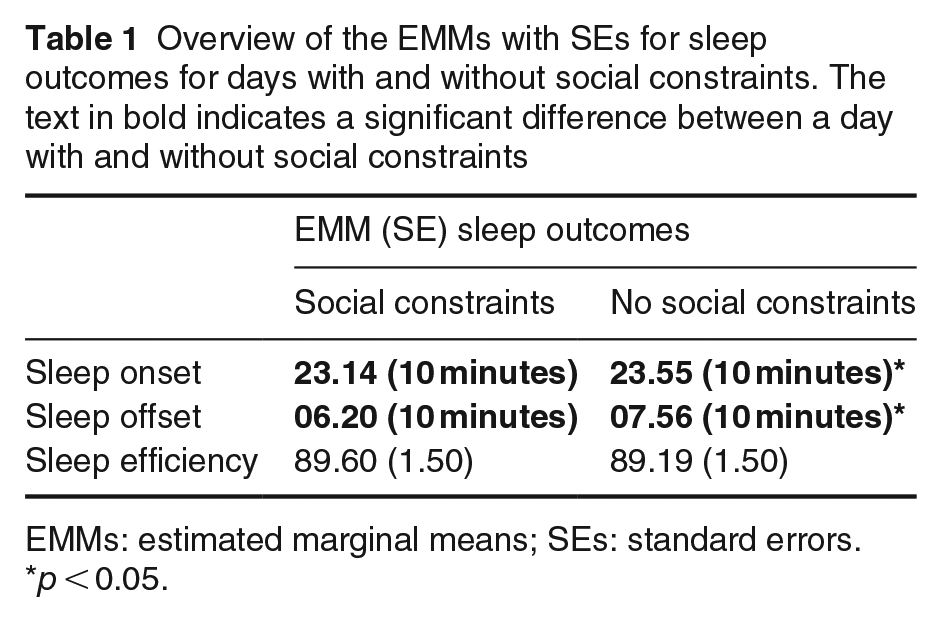

EMMs: estimated marginal means; SEs: standard errors.
p < 0.05.
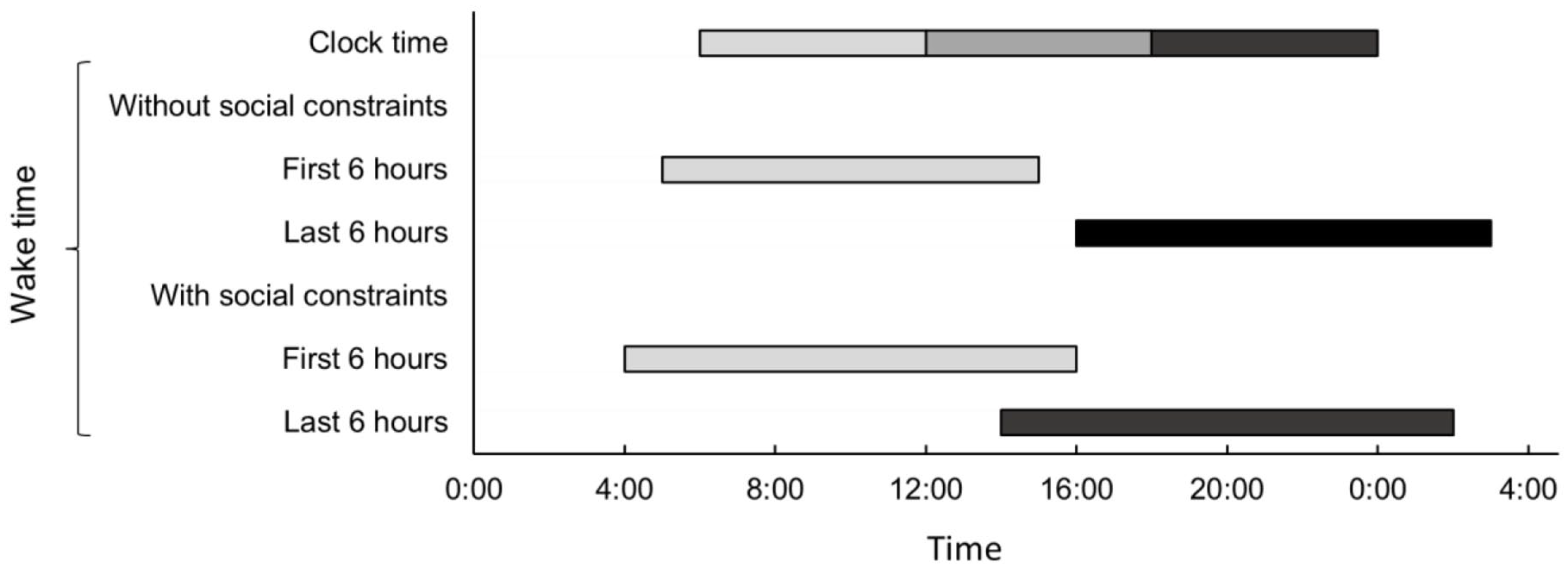
Clock time versus wake time. The light grey bars represent the range of the hours included as the first 6 hours after waking up on days with and without social constraints, whereas the black bars represent the range of the times of the last 6 hours of being awake on these days
3.2 Personal light exposure
Light exposure differed between workdays and the weekend; see Table 2. Note that this table displays the difference in light exposure between a workday and a day at the weekend. The analyses were performed on a Friday and Saturday, as these are the days with no social constraints the following morning. Afternoon light exposure was positively skewed; hence, the results for the afternoon need to be interpreted with caution.
Overview of EMMs with SEs for illuminance levels (log-transformed) for workdays and weekends for the five different HLMs. The text in bold indicates a significant difference between a workday and a weekend day
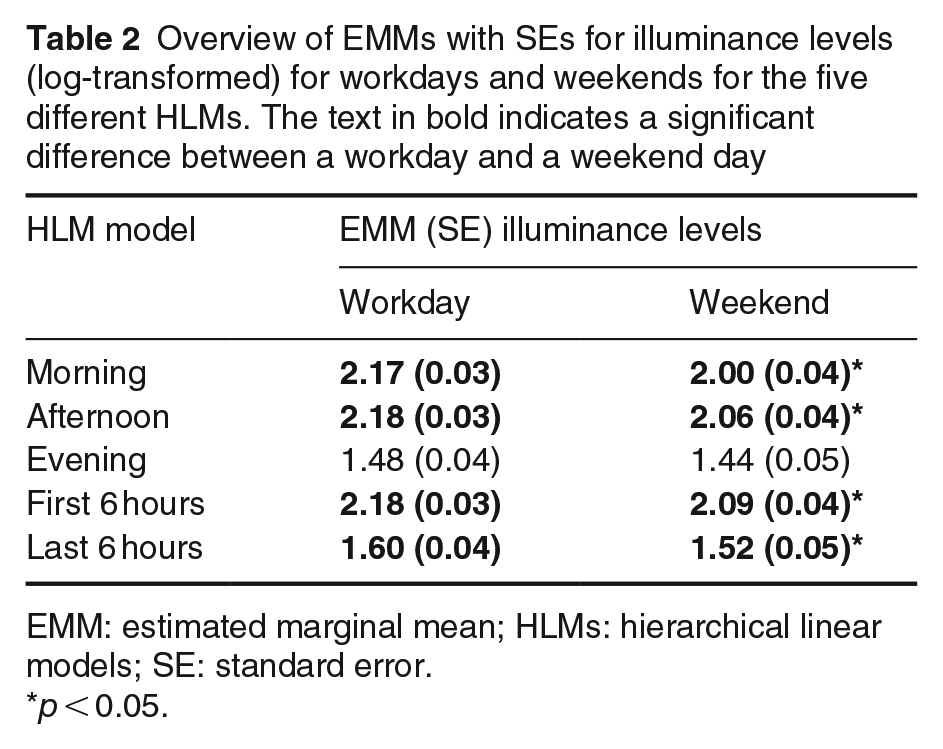
EMM: estimated marginal mean; HLMs: hierarchical linear models; SE: standard error.
p < 0.05.
3.3 Relationship light exposure and sleep outcomes
Table 3 shows the outcomes of the five models for median illuminance level. The main effects of social constraints were included in the models but omitted in the table due to redundancy. As seen in Table 1, there were significant differences in sleep onset and offset between days with and without social constraints.
The unstandardized estimates (Est.) with SEs, 95% CIs (lower and upper CI), and ICCs of three sleep outcomes (efficiency, onset and offset) for light exposure measured by the median illuminance level (log), for clock time and wake time
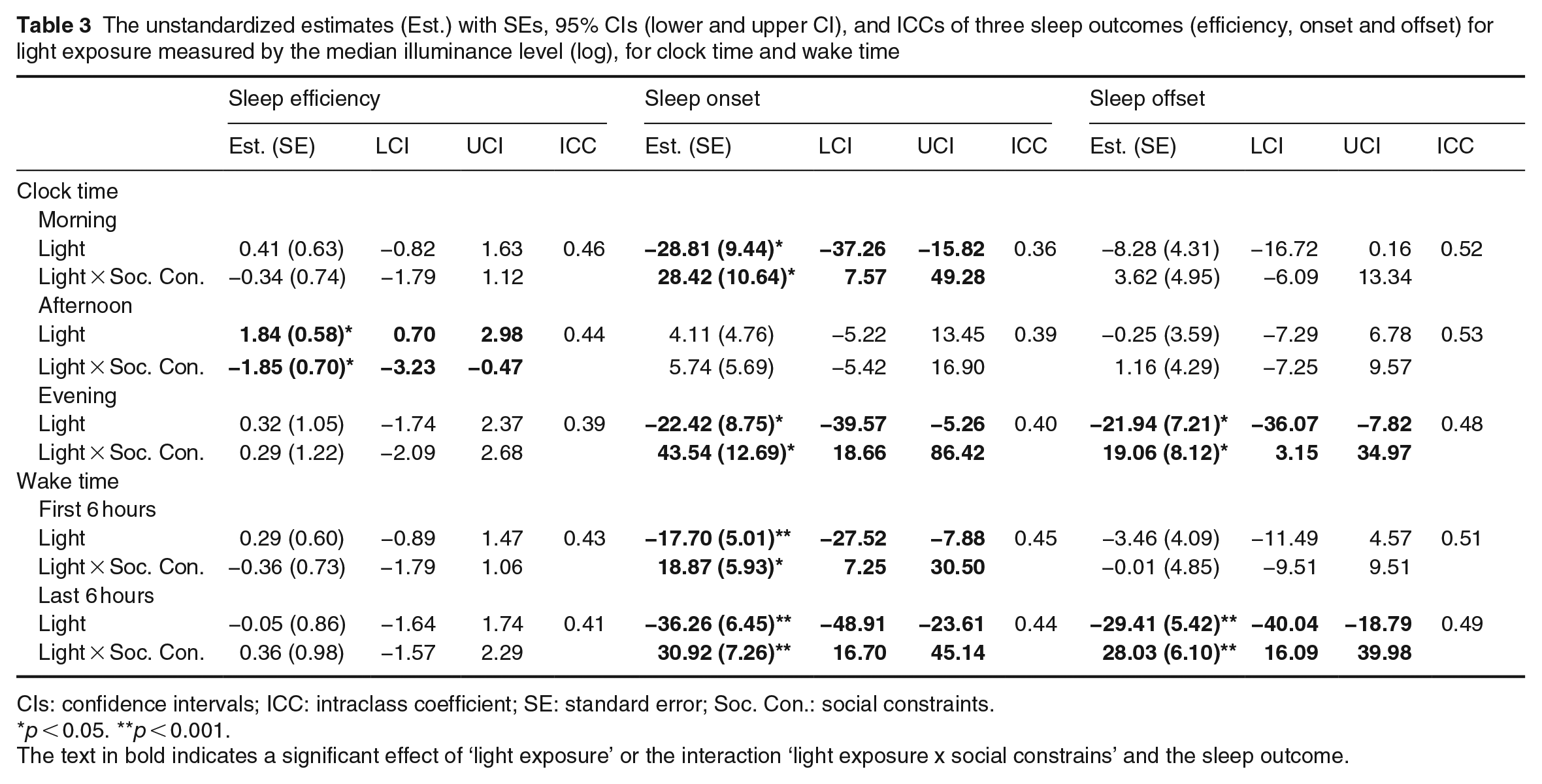
CIs: confidence intervals; ICC: intraclass coefficient; SE: standard error; Soc. Con.: social constraints.
p < 0.05. **p < 0.001.
The text in bold indicates a significant effect of ‘light exposure’ or the interaction ‘light exposure x social constrains’ and the sleep outcome.
Sleep efficiency was only affected by afternoon median illuminance levels, with higher light exposure related to better sleep efficiency. The interaction of social constraints with light was significant, with more light in the afternoon related to better sleep efficiency for days without social constraints only.
More light in the morning, evening, first 6 hours after waking up and last 6 hours before going to bed was related to earlier sleep onset. In addition, social constraints significantly interacted with light exposure during all four measurement periods. A higher median illuminance level in the morning was related to earlier sleep onset for days with no social constraints. In contrast, light levels appeared to have relatively little effect on sleep onset on days with social constraints. Regarding sleep onset, sleep onset was earlier on days with social constraints than on days without social constraints for the lowest median illuminance levels. For the highest median illuminance levels, sleep onset was later on days with social constraints than without social constraints. Similar patterns were found for evening light exposure and the first and last 6 hours of light exposure.
Sleep offset was significantly related to median illuminance levels in the evening as well as to the last 6 hours before going to sleep, with earlier sleep offset related to higher median illuminance levels. The interaction of social constraints and light exposure was significant for both periods (Clock Time and Wake Time). Again, sleep offset mostly appeared affected by light exposure on days without social constraints, with a more pronounced relationship between median light exposure and sleep offset on days without social constraints compared to days with social constraints.
4. Discussion
This ambulatory study investigated the relationship between the amount and timing of light and sleep on days with and without social constraints. Outcomes were compared for days with no assumed social constraints (Friday and Saturday) versus days with social constraints (Sunday through Thursday).
In general, light exposure in the morning and afternoon was lower during weekend days (Saturday and Sunday) than on a weekday (Monday to Friday). It has also been found in earlier studies,11,18 even though an opposite pattern has also been reported. 27 No differences were found in evening light exposure. Due to the placement of the light sensor on indoor clothing, outdoor exposure to daylight (with potentially brighter values) may be missing, which could have affected the outcomes. The lack of data during part of the day is a general issue with wearable light sensors. 28 Within the study period, DST was applied; hence, data of 3 days were deleted. The spring effect could be long lasting until the autumn transition (or at least for 4 weeks in actigraphy data 29 ), affecting predominantly subgroups such as students and extreme evening types. However, a problem in earlier studies is the lack of reporting on the rapid adjustment process in sleep across days after DST change. Therefore, generally stating that 1 week or 5 days is needed for readjustments is somehow misleading. 30 This study included office workers subjected to regular work hours and work and family responsibilities. These settings have a substantial impact on sleep timing. Therefore, the risk of DST interference should be considered weak, even though some rhythms, like sleep-affecting cortisol, have been found resistant to the arbitrary changes in clock time with DST. 31
At the same time, results indicated that people went to bed later and got out of bed later with no social constraints, which agrees with the results from earlier studies.5,32–34 It signals that, even though some participants still had obligations during the weekend, people had fewer social constraints these days. As this study was undertaken during the uprise of the COVID-19 pandemic, social schedules during the weekend may have been more free than usual due to cancelled weekend activities. At the same time, participants may also have had fewer leisure activities during workdays.
Results indicated that higher light levels in the morning and evening were related to earlier sleep onset, whereas higher light levels in the evening also resulted in an earlier sleep offset. Sleep efficiency was only affected by afternoon light exposure, with higher afternoon levels related to higher sleep efficiency. The effects of morning light were in line with expectations, but the effect of evening light exposure was counter to what could be expected based on laboratory studies.14,15 These counterintuitive outcomes may be due to differences between highly controlled laboratory studies and everyday light exposure (i.e. affected by light history or differences in light levels19–21,24). The translation between laboratory and field results certainly deserves more attention. In addition, the present outcomes highlight the importance of afternoon light exposure for sleep outcomes, whereas earlier studies did not report the effects of mid-day light exposure.18,35
Having established that light exposure and sleep outcomes differ between days with and without social constraints, the aim was to determine whether these differences translated into how exposure to light and the timing of this exposure on days with and without social constraints affected sleep (quality). The effects of light on sleep were more pronounced – or even only present – on days without social constraints, even though higher light exposure was found on days with social constraints. Assuming that office employees spent most of their time on less constrained days at home, this study highlights the importance of healthy home lighting, which has not received ample attention compared to office lighting.36,37 The outcomes signal that on working days, the potential beneficial effects of everyday light exposure on sleep are diminished by the demands of social schedules. Conversely, it may signal that on days with social constraints, office workers need a more substantial circadian stimulus (i.e. higher light exposure) for light to influence sleep outcomes.
No differences were found between light timing based on the clock (morning and evening) compared to waking hours (first and last 6 hours of light exposure). This finding is especially striking given that there was a substantial difference between the timing of the measurement frames. It signals that the relation between the timing of light exposure (and potentially the light’s composition) in everyday life of office workers may be more complex than previously assumed based on highly controlled laboratory studies. Daily life may be orchestrated by social schedules and more complex lighting profiles throughout the day. Providing office workers with office lighting (including daylight integration) that supports circadian function is quintessential to help maintain a healthy sleep pattern while phasing social demands imposed by work schedules.
Footnotes
Acknowledgements
The authors would like to thank the participants and office managers in the field study offices for their input, feedback and efforts in facilitating this project. The free-of-charge provision of the SleepScore Max sleep analysers, including a research application by SleepScore Labs™, is particularly appreciated.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship and/or publication of this article: This work was supported by the Bertil & Britt Svenssons Stiftelse för Belysningsteknik [2018-11-26] and the Department of Construction Engineering and Lighting Science’s Internal Strategic Funds [2019-01-30].
