Abstract
Keywords
Introduction
Young-onset dementia refers to people that develop symptoms of dementia prior to the age of 65 (van de Veen et al., 2021). It is estimated that currently worldwide 3.9 million individuals live with young-onset dementia. In the Netherlands, the prevalence is estimated between 14,000 to 17,000 individuals with young-onset dementia (Hendriks et al., 2021). The first symptoms of dementia in younger individuals are often subtle and may first become apparent in the workplace (Harris & Keady, 2009). Here, symptoms can lead to challenges in the ability to perform tasks, collaborate with colleagues, or lose the ability to work at all (Chaplin & Davidson, 2014; Evans, 2019; Ohman et al., 2001). This may lead to loss of employment, even before a diagnosis is made, causing a great deal of misunderstanding and frustration for the person with dementia and their loved ones (Johannessen & Möller, 2011).
Work provides people with a sense of purpose, social engagement, daily structure, and financial stability. However, these factors might be jeopardized for employees with young-onset dementia, which in turn can affect their perceived quality of life (Roach & Drummond, 2014; Robertson & Evans, 2015; Smeets et al., 2024). For people with dementia, the ability to remain active and contribute to society can be highly advantageous in terms of self-worth and identity (Harris & Keady, 2009; Phinney et al., 2007) and may also have positive impact on factors like well-being, sleep and mood (Hewitt et al., 2013; Richardson et al., 2016).
If continuing employment is possible and desired by an employee with young-onset dementia, it is vital to know their individual needs and provide them with appropriate support in the workplace with a focus on their capabilities (Ritchie et al., 2017; Silvaggi et al., 2020). In addition to support from relatives (Smeets et al., 2024), appropriate workplace support depends on the involvement of multiple stakeholders. These include employers, colleagues, human resource (HR) professionals, occupational physicians, and dementia care professionals such as case managers. Research including employers and occupational physicians also underline the importance and potential for them to be included in the support provision regarding continued employment (Bolger et al., 2021; Egdell et al., 2019; McCulloch et al., 2016).
However, only a few studies have focused on the conditions and possibilities of supporting continued employment in young-onset dementia (Omote et al., 2023; Ritchie et al., 2020). Additionally, most studies focused solely on the experiences and needs of employees with young-onset dementia (Andrew et al., 2018; Ikeuchi et al., 2020; Nygård et al., 2023; Smeets et al., 2024). These studies underline the importance of increased awareness and understanding regarding young-onset dementia, as there is often ignorance about the possibilities of continuing to work with dementia if desired. Although several studies have shown that, among others, employers should provide support for an employee with dementia (Carino et al., 2021; Kilty et al., 2022; Ritchie et al., 2017), clear guidance on how to support employees with dementia in continuing paid employment is scarce. In the Dutch context, guidelines and practical support are currently lacking to support an employee with dementia in their workplace. There is a need for such guidelines and for collaboration between different stakeholders to adequately support an employee with young-onset dementia (De Graaf et al., 2020).
Due to this scarcity of research on how to support employees with dementia in the workplace, it is crucial to delve deeper into the experiences and support needs of various stakeholders engaged in this process. These insights could lay the foundation for developing tools and guidance to facilitate continued employment for employees with dementia and those who support them in this process. This paper builds upon earlier research, which focused on the perspectives of the employee with dementia and their relatives living in the Netherlands (Smeets et al., 2024). The current study explores the perspectives and roles of various key stakeholders identified in supporting continued employment for individuals with young-onset dementia.
Methods
This qualitative study is part of the Dutch Work with DEMentia (WorkDEM) research project, aimed at the development of practical tools and guidance to support continued employment for people living with young-onset dementia. The WorkDEM consortium includes different project partners consisting of researchers, experts by experience, and stakeholders involved in the Dutch work context (e.g., employers and an occupational physician) and/or are involved in the care and/or support related to young-onset dementia (e.g., dementia care professionals, the Dutch Alzheimer’s society, FTD peer support network, and the Dutch knowledge centre for YOD).
This paper focuses on the perspectives of stakeholders, including employers, occupational physicians, and dementia healthcare professionals such as case managers, hereafter referred to as stakeholders, through semi-structured individual interviews and subsequent focus group discussions. First, the semi-structured interviews aimed to gain insight into their experiences and support needs regarding supporting an employee with dementia, either in paid employment or in volunteer work specially organized for individuals with young-onset dementia. This interview format allowed for an in-depth exploration of motivations, experiences, and attitudes on the topic (Newcomer et al., 2015). Thereafter, focus group discussions were organized to reflect on the individual interview findings and explore practical solutions for the continued employment of individuals with young-onset dementia, along with stakeholders’ support needs to facilitate this process. Focus group discussions were chosen for their ability to stimulate an interactive dialogue and collaborative idea generation. This dynamic is particularly suited to explore practical solutions and gain a thorough understanding of the interplay between various perspectives (Parker & Tritter, 2006).
Participants and Recruitment Procedure
Three target groups were identified in this study through stakeholder mapping (Shirey, 2012) since they are involved in the work context or in supporting an individual with young-onset dementia in the Netherlands: (1) Work environment: employers, HR-professionals, colleagues, and volunteer supervisors or facilitators (2) Occupational physicians and vocational experts, (3) Dementia healthcare professionals: dementia case managers, specialized nurses, and healthcare psychologists.
Purposive sampling was used to recruit a variety of relevant stakeholders to gather comprehensive insights (Palinkas et al., 2013). Participants for the interviews and focus group discussions were mainly recruited through project partners. Recruitment methods involved multiple posts across social media platforms, as well as personalized outreach through direct connections of project partners. Participants who already participated in the individual interviews were also invited to participate in the focus group discussions.
Based on the study aim and the stakeholder groups included, a sample size of three to five participants per group was deemed appropriate for the interviews. This size allows for in-depth qualitative analysis while maintaining manageable and rich data collection (Malterud et al., 2016). The aim of the focus group discussions was to organize two groups with a mix of identified stakeholders, each consisting of approximately three to six participants (Raats, 2019). This number was considered sufficient to achieve data saturation and to enable in-depth exploration and elaboration of specific topics (Litosseliti, 2003).The inclusion criteria for both interviews and focus group discussions comprised (1) Being at least 18 years old and (2) Having first-hand experience with supporting an employee with dementia (e.g., as an employer or dementia case manager of an employee with dementia et. cetera).
Interested individuals were encouraged to contact the researcher (BS) for further details. Eligible participants received an information letter and signed an informed consent form before taking part in the online interview and/or focus group discussion. Anonymity was maintained by anonymizing the entire process and eliminating all personally identifiable information.
Data Collection and Procedures
Individual interviews were conducted in July and August 2022 using a topic guide informed by existing literature and the expertise of project partners and researchers (BS, MdV, CB, and KP). The topic guide allowed flexibility for follow-up questions and further elaboration during the interviews (Galletta & Cross, 2013). The topic list covered the following: experiences with (1) the early symptom phase, (2) working with dementia, and (3) post-diagnosis workplace support. The topic list was tailored for each stakeholder group to reflect their distinct roles and support responsibilities in relation to an employee with dementia. This resulted in three topic lists (Appendix 1). Interviews were recorded and mainly conducted online via Zoom due to COVID-19 restrictions and participants’ geographical dispersion across the Netherlands. Participants received Zoom instructions beforehand. The interviews lasted 45-90 minutes. Afterwards, participants were invited to review interview summaries for verification. No revisions were needed. This member check procedure enhanced interview data quality (Thomas, 2016).
The focus group discussions were conducted in May 2023 via Zoom and expanded upon the findings of the individual interviews. The topic list for the focus group discussion (Appendix 2) was based on the outcomes of the semi-structured interviews and was reviewed by several researchers and healthcare psychologists with different backgrounds (BS, MdV, CB, and NJ). Each focus group aimed to include a mix of the three target groups to encourage discussion between professions, however not all groups were represented in every focus group discussion. Each focus group discussion was recorded and lasted between 90 and 120 minutes. Before the focus group discussions, participants received a factsheet summarizing the findings of the individual interviews (Appendix 3) and were asked to complete three questions: (1) What are the three most important points from the summary for you? (Related to your own target group), (2) Do you feel anything is missing from this factsheet summary, (3) Do you have any interesting experiences from practice when it comes to working with young-onset dementia? This pre-discussion preparation sensitized participants to the topic (Visser et al., 2005). Each discussion was moderated by an experienced moderator (LB), while another researcher (BS) took field notes, made observations and monitored the focus group process and dynamics. Afterwards, participants were invited to review the focus group discussion summary for verification. No changes were made.
To ensure the trustworthiness of the data, method and data source triangulation were applied by using both interviews and focus group discussions. Diverse data sources were utilized, including audio and video recordings, field notes, and contextual mapping supported by a factsheet and a booklet with sensitizing and prioritizing questions (Creswell, 2013). Investigator triangulation was applied by involving at least two researchers in the coding process and engaging researchers with diverse backgrounds to reflect on the overall research process, data collection, and results during team meetings (Carter et al., 2014). Additionally, adherence to the Consolidated Criteria for Reporting Qualitative Research (COREQ) ensured rigorous qualitative methods and transparent reporting (Tong et al., 2007).
Data Analysis
Recordings of the individual interviews and focus group discussions were transcribed verbatim. The interview data were analysed using inductive thematic analysis (Braun & Clarke, 2006), allowing concepts to emerge directly from the data rather than being imposed beforehand. This approach follows the principles of the grounded theory (White & Cooper, 2022). Three researchers (BS, KP, and NJ) with different backgrounds independently coded the data using Atlas.TI (Elo & Kyngäs, 2008). The researchers then compared their transcripts and codes, discussing any discrepancies to reach consensus on the main concepts. These concepts were verified in team meetings with two other researchers with a background in qualitative research and experience with clinical practice in the support of people with young-onset dementia (MdV and CB).
The focus groups were analysed using deductive thematic analyses. Where the codes from the previous interviews were used to validate and expand the findings. This combined approach, inductive analysis for interviews, followed by deductive analysis for focus groups, ensured that new concepts could be identified while previous findings were validated. The transcripts were independently analysed by the same two researchers (BS and KP). Subsequently, all concepts were extensively deliberated upon in team meetings with the involvement of other researchers (MdV, CB, and SH) to establish agreement on the ultimate concepts derived from both interview and focus group data. This method minimized researcher bias (Norris, 1997), and helped confirm that data saturation had been reached.
Triangulation not only strengthened the trustworthiness of the methods but also informed the data analysis. Using multiple data sources allowed validation and refinement of themes derived from the interviews and the identification of additional insights from the focus groups. Although the main themes largely overlapped, the focus groups helped to prioritize them, leading to a sharper and more focused set of final themes. They also helped to distinguish between what participants themselves needed and when they spoke on behalf of employees with dementia, expressing assumptions about their needs. This distinction clarified the perspectives of different stakeholder groups and helped to separate direct experiences from proxy views. Investigator triangulation further enhanced the credibility of the findings by providing multiple perspectives on emerging themes and their interpretation. Overall, triangulation refined and deepened the analysis, resulting in a more nuanced and reliable interpretation of the data (Ajemba & Arene, 2022).
Results
Participant Characteristics
Participant Characteristics in Interviews (n = 18) and Focus Groups (n = 13)
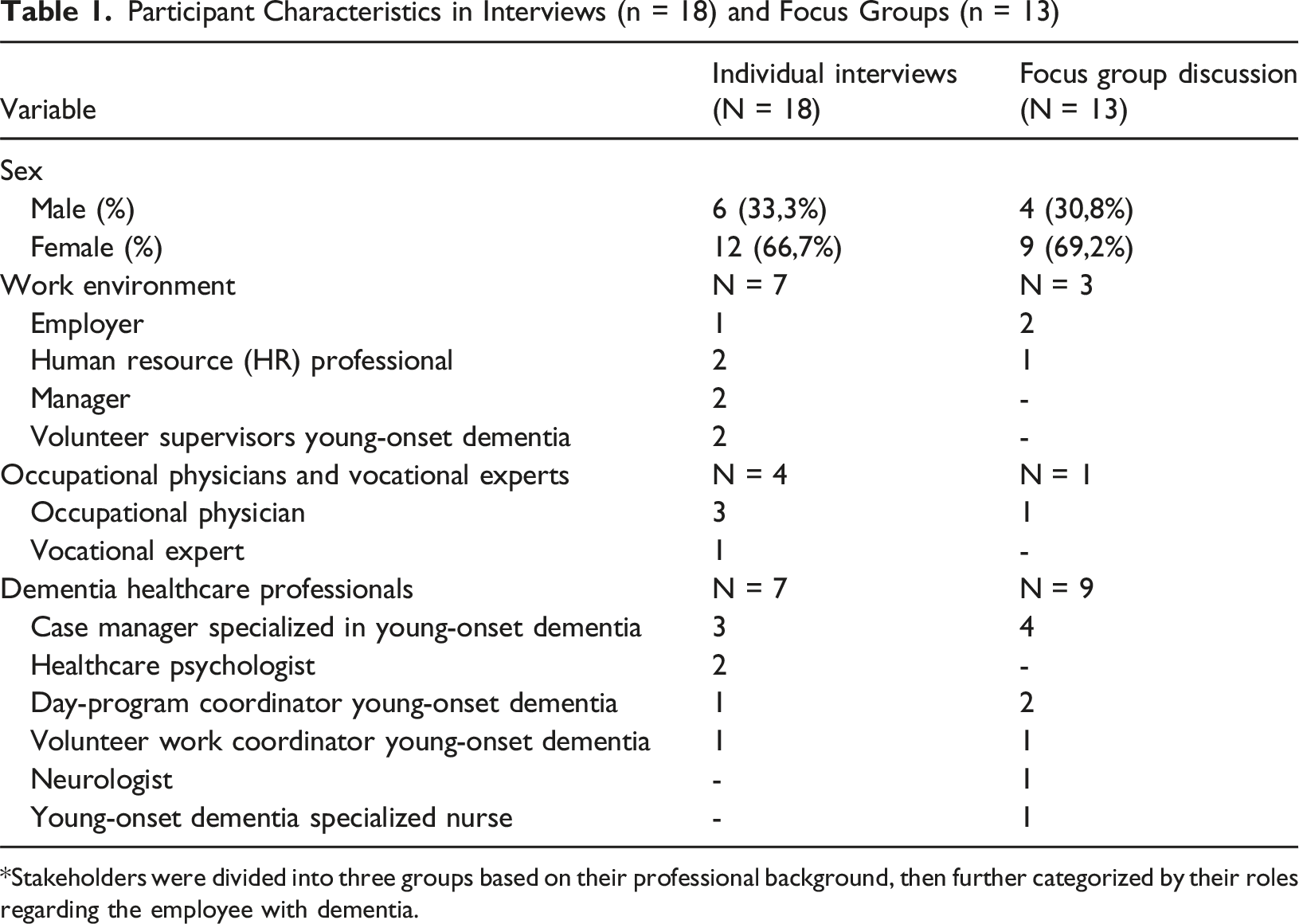
*Stakeholders were divided into three groups based on their professional background, then further categorized by their roles regarding the employee with dementia.
Roles and Perspectives of Key Stakeholders in Continued Employment
Based on the interviews and focus group discussions, results can be structured in three distinct phases of the continued employment process: I) experiences with early symptoms at work, II) experiences with continuing employment, and III) experiences with phasing out work. In addition to these experiences, key facilitators, barriers, and support needs were identified across the different phases and stakeholders involved. These are demonstrated in Table 2
Phase I: Stakeholder’s Experiences with Early Symptoms at Work
According to the participants, the first symptoms of dementia are often noticed in the workplace. Employers and managers observed that employees often exhibit growing difficulties in performing their work tasks and noticeable changes in behaviour. However, they stated that they did not initially notice these symptoms or failed to associate them with dementia and attributed this to a lack of awareness and knowledge about young-onset dementia. Consequently, this sometimes hindered the timely involvement of an occupational physician. Participants stressed the importance of open communication and transparency about an employee’s declining performance to ensure timely workplace support. “It was clear in her work, such as patient care and administrative tasks, where she struggled to communicate clearly, or not at all, or express things inaccurately. It was also noticeable in her behaviour, as well as in how she dressed and took care of herself. The behavioural changes, in particular, became more and more apparent.”– Manager-02, interview “And this wasn’t something that came to my mind—dementia, young-onset dementia, or anything like – it wasn’t necessarily on my list. I thought; there must be something else going on…” – Manager-01, interview
Participants also indicated that it is important to respond with understanding to the changing situation and decline in work performance. This might foster an open and trusting environment to eventually assess the underlying issue affecting the employee’s work performance. “Ultimately, it's about understanding each other, not just having empathy, but also trying to understand what causes it.” – HR-professional-02, interview
Occupational physicians stated that identifying the underlying aetiology can be challenging for them in these cases. Symptoms can resemble conditions such as stress, burnout, or depression. Participants emphasized that a lack of knowledge and experience with young-onset dementia may hinder specialist referrals. This, in turn, can increase the risk of misdiagnosis or delayed diagnosis. “I had a significant learning moment, realizing that if symptoms don't improve at that age, I should consider dementia in my differential diagnosis. It's a real trap, isn't it? Initially, I attributed it to stress and possibly burnout or mild depression.” – Occupational physician-03, interview “And I notice in my field that very few vocational experts are familiar with different forms of young-onset dementia and do not know how to manage them.”– Vocational expert-01, interview
Additionally, occupational physicians stressed the importance of collateral history in this phase. Consulting different involved stakeholders, for example relatives and colleagues, about the employee’s changing performance helps to obtain a thorough understanding of the situation. Additionally, participants highlighted the importance of managers involving occupational therapists early to provide timely support and accommodations. Participants emphasized that the occupational physician is often involved too late or not at all, this delayed or no involvement can negatively affect the employee. “Yes, and perhaps what made things more complicated was that one of her two sons worked here as well. He kept talking about [the suspicion of] dementia, constantly bringing it up, which only fuelled the situation. I would have liked to invite him to a meeting with his mother to discuss it openly. But each time, I had to rely on the lady herself, as no one accompanied her, despite my requests.” – Occupational physician-01, interview
Healthcare professionals, particularly dementia case managers, emphasized the importance of a timely diagnosis. However, they are typically involved after the diagnosis has been confirmed, even though they believed their early involvement could be highly beneficial. According to the participants, they possess specialized knowledge that is often lacking among employers and occupational physicians. This knowledge enables them to provide valuable support earlier in the process. “Therefore, I believe the importance of involvement should be a priority. Perhaps mutual involvement is beneficial, as you are also familiar with the home situation. You hear a lot from a different perspective than that of the GP and the employer.”– Dementia case manager-07, focus group discussion
Phase II: Stakeholder’s Experiences with Continuing Employment
Employers and managers highlighted that openness about the diagnosis in the workplace is considered essential for continuing employment, otherwise the possibilities for providing support are limited. Furthermore, participants mentioned that openness helps foster better understanding within the work environment, clearing up misconceptions about young-onset dementia and its effects on work performance. “Everyone knows the image [having dementia at an older age] of course, but not what it means for work.” – Manager-01, interview “It is [disclosing the diagnosis] often very important to be able to do something. The diagnosis needs to be shared. Because otherwise, of course, you can't do much or provide much support.” – Employer-01, interview
Participants indicated that after the diagnosis is disclosed in the workplace, an assessment phase starts to determine which tasks and roles are still feasible for the employee. This involves extensive consultations with the employee and various stakeholders, along with necessary workplace adjustments. For this purpose, employers and managers emphasized the need for sufficient knowledge about young-onset dementia and its potential impact on future work performance. In addition, participants mentioned that organizations need to carefully assess whether employees can transition to alternative roles, while also considering the financial impact on the organization. Nevertheless, employers also indicated that organizations prioritizing social responsibility over economic interests are often willing to support employees and keep them within the organization for as long as possible. However, achieving this typically requires significant effort and extensive exploration for employers. “Once the condition was clearly understood, there was more empathy in the workplace. We started collaborating on how to make the situation workable for everyone, and things have improved. We’ve made numerous adjustments and have been deeply involved. A lot of time, energy, and resources, including interventions, have been invested to retain him and provide a dignified workplace where he can make a meaningful contribution.”– HR-professional-01, interview “Why does it work? Because we all understand the situation. I believe awareness and understanding have been key. We’re not a harsh company; it's more like a family, and [employee with dementia] is a part of that too.”– Employer-01, interview
Employers and managers highlighted the need for regular communication and evaluation regarding the employee’s role and necessary workplace adjustments. They emphasized that all parties involved, including the employee, should be actively engaged in this process. Additionally, close collaboration with other stakeholders, e.g. a dementia case manager, is considered essential by the participants in supporting an employee with dementia due to their expertise. Employers also expressed a need for practical tools and guidelines, a clear roadmap, to better support employees throughout this process, as they felt such resources were currently lacking. Employers and managers also highlighted that not all organizations might have the capacity or resources to retain an employee, as it often requires tailored solutions for only one individual. Nevertheless, employers were supportive of the idea of continued employment for employees with dementia within their organizations. They recognized the value of helping employees maintain dignity and a sense of purpose through continued employment. “Well, by at least thinking along with us about what steps we could potentially take. And then, not looking at the interests of [organization], but looking and thinking along in the interests of [employee with dementia]. So that you take both the employer and the employee into consideration in your thought processes and then take the right steps from there.” – Manager-01, interview “First, there is a need for guidelines and directives for employers. It's somewhat of an unfamiliar situation for employers, so they want to know: What can you do? What should you do? What are the options?”– Manager-02, focus group discussion “We agreed that we wouldn’t overlook [employee with dementia], but instead, we would gradually and progressively reduce his workload. We’ve always involved and supported him in areas where needed. The understanding that was there from the start has remained, including from his colleagues.”– Employer-01, interview
Occupational physicians highlighted the importance of disclosing the diagnosis to facilitate continued employment, if desired by the employee, such as making necessary workplace adjustments. However, they reported that due to medical confidentiality and GDPR compliance, they cannot force an employee to share their diagnosis. In turn, this can complicate for instance the involvement of close colleagues in providing support and fostering understanding in the workplace for employees with dementia. “It can be very practical to be open [about the diagnosis] because then everybody knows exactly what's going on and it can foster understanding. However, legally speaking, as an employer, you're not allowed to demand that someone discloses their diagnosis, even though in practice, this often happens. So, to officially advise [as an occupational physician] to do so would contradict the current legislation. Therefore, it's a sensitive issue; there are distinct formal and informal aspects to consider.” – Occupational physician-04, focus group discussion
Occupational physicians also emphasized the importance of considering the type of work the employee does when evaluating the possibility of continued employment. Safety, both for the employee and for co-workers or customers/clients/patients, was mentioned as a critical aspect that they must remain vigilant about. “ I've had people with dementia who were very eager to keep working, but their employers didn't tolerate it due to the associated risks.” – Occupational physician-04, focus group discussion
Healthcare professionals indicated that there is often still a stigma surrounding young-onset dementia, despite opportunities for individuals to continue employment. They also reported a current lack of early or adequate involvement in their clients’ work environments. These professionals emphasized their potential role in fostering collaboration, providing information, and offering support within the workplace for employees. They identified themselves as a vital link between the home and work setting, using their expertise to assess the feasibility of continued employment or to help plan a gradual transition. They perceived that they have a good understanding of the balance between the employee’s wishes and their abilities. “If people indicate that they would like that [continue their employment], then I think you should explore together with the employer and, of course, the colleagues of that person, what the possibilities are.” – Dementia case manager-02, interview “It doesn’t have to be an either-or situation where we are only involved in the home environment; we could also play a role at work. Whether it's mediating with an occupational physician, family, general practitioner, or employer.” – Healthcare psychologist-01, interview
Phase III: Stakeholder’s Experiences/Insights with Phasing out Work
All participants emphasized the importance of providing adequate guidance during the gradual transition from work to phasing out work. In their opinion, ensuring a dignified farewell is critical as it provides closure for the employee. Participants indicated that honest and open communication is essential in determining the appropriate time to begin the phasing-out process. Additionally, safety and/or personal considerations might play a central role in deciding the timing of a gradual transition or to stop work entirely at this stage. “I see the profound impact it has at home and what it does to a person. There was one woman where the process was particularly difficult. At first, it was thought to be burnout, but it later turned out to be dementia. By then, a lot had already happened [at work], and she never really got a proper farewell.”– Dementia case manager-07, focus group discussion “I believe they handled the phasing out of his work quite gracefully. They gradually assigned him simpler tasks, even though these no longer matched his skill level. Now, however, he has reached a point where he could ease off even more. He himself has noticed that it’s just not working anymore.” – Dementia case manager-01, interview “As a case manager, I see my role in closely monitoring this [situation at work] and assessing how it progresses. Eventually, I had to acknowledge that it was becoming too much for him. What we observed was that when he stopped working, he seemed to improve and function better in his home environment.” – Dementia case manager-03, interview
In addition, occupational physicians highlighted the importance of applying for the appropriate benefits for an employee. This is often experienced as a challenging process by occupational physicians, due to the complexity of the different rules and eligibility requirements. Occupational physicians also identified several challenges with the government agency (UWV), which is responsible for employee benefits. These included gaps in the agency’s knowledge and understanding of young-onset dementia, as well as difficulties in collaboration. They are often unaware of the possibilities available and the arrangements that may apply to an employee with a dementia diagnosis in terms of employment and benefits.
Furthermore, healthcare professionals expressed that there is currently a gap between working life and other support services, such as day care for individuals with dementia. They explained that this gap exists because day care facilities are often considered the next step. However, these facilities may be too early for some individuals with young-onset dementia, as not everyone has reached that stage of the disease. They suggested that this gap could be addressed by considering alternatives, like volunteer work, in a timely manner. This approach could also warrant a smoother transition towards the end of working life for the employee. Healthcare professionals believed that such approach would allow employees to adapt to the changes and the post-work phase at their own pace. Additionally, volunteer work can be a valuable option after work. Healthcare professionals stated that it can boost self-esteem and help individuals feel connected and valued in society, especially for employees who have recently stopped working. “I believe it’s important to approach this as a process. At some point, you know that saying goodbye [to working life] is inevitable. However, during the interim period, it’s crucial to understand the person’s situation and gradually guide them toward the next step, whether that’s day care, volunteer work, or something similar. Starting this process early is key to preventing them from falling into a void. Ideally, we want to avoid that altogether.” – Occupational physician-04, focus group discussion “Having a structured routine during the week and fulfilling commitments provides not only a sense of purpose and daily engagement but also a feeling of belonging to a group. It alleviates isolation and fosters the sense that one can contribute to others. Volunteers often experience a profound sense of satisfaction and joy from seeing the positive impact they have on others, such as providing a pleasant afternoon for someone, which brings both work and life satisfaction.” – Volunteer coordinator-01, interview
Summary of Facilitators, Barriers, and Support Needs
Perceived Facilitators, Barriers and Support Needs of the Different Stakeholders Regarding Dementia and Continued Employment

Discussion
In the present study, we investigated the experiences and support needs of key stakeholders regarding continued employment of persons with young-onset dementia in the Dutch context. Our study demonstrates that stakeholders have varied roles and experiences, but they all play a crucial role in supporting employees in this area. Various facilitators, barriers, and support needs were identified across and within the three stakeholder groups regarding continued employment in young-onset dementia. Facilitators included adequate knowledge of and experience with dementia, a proactive organizational attitude regarding continued employment and dementia, effective communication, regular performance evaluations, and timely involvement of relevant professionals, such as occupational physicians and dementia case managers, particularly during the work and post-work transition phase. Barriers predominantly arose from stigma, lack of knowledge and awareness of dementia, limited resources, legal constraints (e.g., GDPR), and insufficient communication with other stakeholders, notably governmental agencies responsible for benefits for employees. Support needs emphasized timely involvement of different stakeholders, improved collaboration between stakeholders, guidelines for workplace support, practical support tools, improved communication between stakeholders, and increased awareness and knowledge of dementia in general and in the workplace.
Work, in the context of this study, represents more than just employment. It provides social connections, a sense of purpose, and structure. For individuals with young-onset dementia, the transition away from work can be especially challenging, affecting not only financial stability but also identity, autonomy, and social participation. Given that young-onset dementia involves significant loss across multiple areas of life, understanding the broader value of work, as part of someone’s social health, is crucial in supporting continued employment for people with dementia. This aligns with the growing focus on social health in dementia care and research (de Vugt & Dröes, 2017). Huber et al. (2011) operationalized social health through three dimensions: (1) Fulfilling one’s potential and obligations, (2) ability to manage life with some degree of independence, and (3) Participating in social activities. This conceptualization of social health is particularly relevant in the context of employment while living with dementia, where fulfilling one’s potential, maintaining autonomy, and engaging in meaningful social roles are closely connected. However, this potential requires more than the willingness or capacity of an individual. It depends on the presence of a supportive (work)environment, shaped by informed and engaged stakeholders. The involvement of these stakeholders, including employers, HR-professionals, occupational physicians, colleagues, and dementia healthcare professionals is paramount in this regard. Employers and HR-professionals can implement inclusive policies and practices, foster understanding among colleagues, and adjust job roles as necessary. Occupational physicians can assess work capacity, provide guidance, collaborate on accommodations, symptom management, and refer to support services. Dementia case managers and other healthcare professionals can provide ongoing education, counselling, and support, which benefit both the individual with dementia and their work environment. Thus, involvement and effective collaboration among these stakeholders can enable employees to maintain their identity and contribute meaningfully at both workplace (micro) and societal (macro) levels. Our findings highlight that such coordinated support helps preserve autonomy and might reduce the social and emotional impact of a (delayed) diagnosis. Prior research confirms that lack of understanding of for instance employers and co-workers, and a lack of flexibility regarding continued employment negatively affect autonomy (Thomson et al., 2018), while individualized, supportive approaches promote continued employment (Ohman et al., 2001; Robertson et al., 2013; Silvaggi et al., 2020). Continued employment further enhances social connection, purpose, and meaningful engagement (Thomson et al., 2018). Studies also show that employees with dementia can stay engaged when employers adopt a positive, supportive approach (Bak et al., 2023; Thomson et al., 2018). Our findings also suggest that, with appropriate support and collaboration, individuals with young-onset dementia can remain involved in their work environment. Staying engaged at work may help them maintain aspects of their social health.
While the active involvement of stakeholders is critical in supporting individuals with dementia to maintain meaningful employment and positively influence their social health, several barriers and facilitators to this process remain. Most of our findings are consistent with prior research that highlight several barriers in continued employment for people with dementia, including a general lack of knowledge about dementia, inadequate workplace adaptations, and the negative impact of misdiagnosis or delayed diagnosis on employment (Evans, 2019; Kilty et al., 2022; Thomson et al., 2018; Williams et al., 2017). Additionally, studies have shown barriers to supporting an employee with dementia, such as the absence of clear guidance on how to manage dementia symptoms in the workplace, stigma, and the failure to recognize employees’ remaining abilities, all of which were similarly identified in our study (Chaplin & Davidson, 2014; Cox & Pardasani, 2013; Gove et al., 2015; Ritchie et al., 2017). Our study also shows that legal constraints often make it difficult to facilitate continued employment. Navigating these constraints requires openness from the employee about their situation, as well as clear communication from both the employer and the occupational physician about the options that are available for the employee and the organisation within the legal frameworks. Additionally, our findings indicate that collaboration with certain governmental agencies is of great importance, as they play a significant role in the employee’s financial situation. Next to identified barriers, a key facilitator identified in both our study and the work of Omote et al. (2023) is the necessity to foster an environment in which employees feel comfortable disclosing their diagnosis. This openness can help overcome legal and regulatory barriers, facilitating support from employers, colleagues, and occupational physicians. Our study further emphasizes that clear communication is essential in supporting employees with dementia. Timely involvement of relevant professionals, particularly during the transition from working to not working, significantly contributes to this support. A more nuanced understanding of all these factors, as perceived by the stakeholders involved, is necessary to optimize support.
To further inform and optimize this support, it is also important to understand the specific needs of all stakeholders involved. Consistent with previous literature, our study highlights the importance of strategies to promptly recognize the early signs of young-onset dementia. It also underscores the need for clear workplace policies that support continued employment for individuals living with dementia (Egdell et al., 2019; Kilty et al., 2022; Omote et al., 2020; Sakata & Okumura, 2017; Thomson et al., 2018). Addressing stakeholder needs requires clear guidelines, practical support tools, and strong collaboration networks (Edahiro et al., 2023; Omote et al., 2020). Additionally, our study also reveals the need for an expanded role for occupational physicians and dementia case managers, along with comprehensive knowledge of dementia across all stakeholder groups. As shown in our study and supported by Andrew et al. (2018), occupational physicians contribute by facilitating diagnosis and ensuring appropriate workplace adjustments. This gives them a crucial role in the support of an employee with dementia. Our study further highlights the vital role of dementia case managers, whose expertise about dementia in younger individuals enables them to advocate for employees and guide appropriate workplace adaptations. Overall, although stakeholders may have different perspectives and responsibilities, their shared need for effective communication and coordinated efforts remains critical for employment opportunities regarding individuals with young-onset dementia.
Implications for Practice and Future Research
The findings of this study emphasize the need for a more collaborative approach to supporting continued employment for people with dementia, highlighting the crucial role of key stakeholders. There is currently little guidance on how to support continued employment for people with dementia, especially within country-specific legal and financial systems. To address this, practical tools, clear guidelines, and tailored workplace policies are needed. Key measures should include flexible work arrangements, phased transition plans, and active support from, among others, employers and occupational physicians. Equipping all stakeholders with the knowledge and resources to handle legal, financial, and organizational challenges is essential to enable continued employment for individuals with dementia.
Future research should focus on several areas. Studies could examine which workplace adaptations are most effective in supporting employees with dementia. Long-term studies can explore the impact of continued employment on e.g., well-being and autonomy. Comparative research across countries can offer insights into how legal and financial systems influence employment with young-onset dementia and which key stakeholders should be involved in the particular context of that country.
To improve continued employment in the context of young-onset dementia, recognizing that there is an increasing need for guidance and practical support for key stakeholders involved in the work context is crucial. Focus of the WorkDEM project is to meet the needs of these stakeholders and develop a practical support toolkit regarding work and young-onset dementia. This toolkit could be adapted for use in various international contexts.
Strengths and Limitations
This research has some strengths and limitations. First, we included a range of stakeholders, such as occupational physicians, employers, and healthcare professionals, who have diverse experiences with employees living with dementia. This approach allowed us to gain a more comprehensive understanding of the current situation and the opportunities for continued employment for people with dementia in the Netherlands. This diverse input provided valuable insights throughout the entire work process. However, a potential limitation is selection bias (Smith & Noble, 2014), as professionals who are more positive about supporting continued employment in young-onset dementia may have been more willing to participate. Additionally, only a small number of individuals from each stakeholder category was involved in the study, which may limit the diversity of perspectives. Consequently, the findings may not be representative of the stakeholder group as a whole.
Second, in our focus group discussions, bringing together stakeholders from various fields led to rich, in-depth discussions. Additionally, the use of method triangulation, integrating interviews, focus group discussions, and context mapping, has enhanced the depth and credibility of the research. This approach allowed for cross-validation of findings, and helped uncover nuanced insights that might have been overlooked using a single method (Korstjens & Moser, 2017).
Lastly, investigator triangulation was ensured by involving two researchers in the coding process and incorporating diverse perspectives during the analysis. This approach enhanced the reliability and validity of the findings by reducing individual bias, allowing for a more balanced interpretation of the data, and strengthening the overall reliability of the research (Carter et al., 2014). However, it must be considered that the study findings are based on the Dutch context, which may limit transferability due to differences in labour laws, healthcare systems, and cultural attitudes towards young-onset dementia. Variations in rules and regulations regarding employers, social security, and stigma across countries could affect how workplace support is implemented, making the findings somewhat less universally applicable (Korstjens & Moser, 2017; Mwita, 2022).
Conclusion
This research highlights that continued employment for individuals with young-onset dementia can play a crucial role in maintaining social health by providing a sense of purpose, preserving autonomy, and fostering meaningful social connections. To support this, timely involvement from and collaboration between various key stakeholders is crucial. Key facilitators identified in this study include increased knowledge and awareness of dementia and its implications, proactive organizational attitudes, and effective communication and collaboration. Barriers, such as stigma, lack of knowledge, and insufficient resources, need to be addressed to create a supportive work environment. While there is growing attention on continued employment for individuals with dementia, more research is needed. Furthermore, the development of practical tools and guidelines for stakeholders are essential to navigate the complexities of this issue. This study underscores the importance of a tailored approach that aligns with the individual’s abilities and needs, ensuring that employment remains both desirable and achievable for both employee and employer. For individuals with dementia, this requires a multi-stakeholder approach, timely recognition, workplace adaptations, and ongoing support.
Supplemental Material
Supplemental Material - Supporting Continued Employment for Individuals With Young-Onset Dementia: Insights From a Qualitative Study Into Key Stakeholders’ Roles and Perspectives
Supplemental Material for Supporting Continued Employment for Individuals With Young-Onset Dementia: Insights From a Qualitative Study Into Key Stakeholders’ Roles and Perspectives by Bo Smeets, Kirsten Peetoom, Niels Janssen, Lizzy Boots, Christian Bakker, Marjolein de Vugt, Stevie Hendriks in Dementia
Footnotes
Acknowledgements
We want to thank all project partners for their valuable contributions, as well as all participants who took part in the interviews and focus group discussions.
Ethical Approval
Ethical approval for both the individual interviews and focus group discussions was granted by the Medical Ethics Review Committee (METC) of Maastricht UMC+ (azM/UM) (METC 2021-3052 and METC 2022-3267). Informed consent forms were signed by all participants in this study prior to participation.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Dutch national organisation for Health research and Development (ZonMw) under Grant: 10320052010007.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The data supporting the findings of this study are available on request from the corresponding author. The data are not publicly available due to privacy or ethical restrictions.
Supplemental Material
Supplemental material for this article is available online.
Author Biographies
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
