Abstract
In this study we investigate day-care centres as a form of community-based support designed to facilitate ageing in place for individuals with dementia, with the goal of delaying or preventing their transition to institutional care. Day-care centres provide structured activities designed to alleviate loneliness and isolation, affirm personal identity, and offer respite for family caregivers. In Sweden – the context of this research – some 16,000 older adults with dementia attend day-care centres. Our aim is to explore how individuals with dementia experience day-care centres, and to examine the types of identities that are made possible and enacted within this setting. The empirical material consists of 14 qualitative interviews conducted across six day-care centres located in two Swedish cities. The participants were 8 women and 6 men, aged between 60 and 90. Thematic analysis was used to analyse the data. The findings showed that participants viewed the day-care centres as accepting, non-demanding environments, in contrast to the more problematic identities they encountered in ordinary life. While participants acknowledged dementia as a shared condition and expressed their appreciation that they were part of a community where others also experienced memory difficulties, there was little effort to cultivate a collective identity centred on dementia. Participants seldom shared personal information with one another and generally deferred to staff to decide about group activities. Although their limited self-disclosure might suggest a lack of opportunity for deeper engagement, an alternative interpretation is that the group setting enabled participants to maintain an identity as competent social actors – individuals capable of navigating and adapting to the social expectations of the group. We thus highlight the nuanced ways in which day-care centres can support personhood and social participation among people living with dementia.
Introduction
Supporting older adults to remain in their own homes and stay connected with their communities has become a central focus of ageing policies globally. The concept of ageing in place is recognised as a key priority in international policy (Auriemma et al., 2024; Gibson et al., 2024; OECD, 2023), including people living with dementia. In Sweden, the context of this study, most people with dementia live in ordinary housing, rather than institutional settings (Odzakovic et al., 2019). We therefore examine day-care centres, which are one of the services designed to support ageing in place for people with dementia, delaying or preventing the transition to institutional care (Ellen et al., 2017; Lee et al., 2019).
We specifically focus on the interplay of day-care services and identity. Identity is central in the context of dementia, as the condition often leads to memory problems that challenge both personal continuity and social connectedness. The dominant biomedical discourse often frames dementia in terms of cognitive decline, dependency, and loss (Kitwood, 1997), and this framing can contribute to the erosion of personal identity and reinforce societal stigma. The concept of stigma describes how individuals with attributes deemed undesirable by society are reduced to problem identities, leading to exclusion and discrimination. People living with dementia frequently experience such stigma, which can silence their voices and limit their agency (Nguyen & Li, 2020). Identity, meanwhile, is crucial to organisations that are striving for empowerment and the formation of social movements for collective action. By uniting around shared experiences and goals, individuals with dementia may resist marginalisation and assert control over their social identities (Bartlett & O’Connor, 2010).
People with dementia are often excluded from research for ethical reasons, but there are strong ethical arguments for including their voices (Alzheimer Europe, 2019). There is thus a need for further studies of the views and experience of day-care service users, relating their descriptions to the complex question of identity. Exploring how identities are enabled by day-care services is also relevant because of the person-centred approach of most care practices (Rose & Dening, 2023). Further, greater knowledge of the identities offered by day-care services can be used to design improved interventions for people with dementia. Our aim with this study is thus to explore how people with dementia experience day-care centres and what identities that are made possible and enacted within this setting.
Identity, Dementia, and Day-Care Centres
Social identity theory (Tajfel & Turner, 1979) offers a useful lens through which to examine the evolving sense of self in people living with dementia. According to this theory, identity is not solely an internal construct, but is shaped by group membership and social interactions within and between groups. As dementia progresses, individuals may experience a loss of valued roles and group affiliations, and by corollary a diminished sense of social identity and belonging (Haslam et al., 2008). However, identity is not simply lost; it can be reconstructed and maintained through everyday social practices. Örulv (2008) highlights how people with dementia actively negotiate identity in their interactions, using narrative and repetition to sustain a coherent sense of self in group settings. These micro-level dynamics underscore the importance of social environments in supporting identity continuity. The ‘social cure’ approach, rooted in social identity theory, emphasises the protective role of social group identification for well-being (Jetten et al., 2012). Importantly, the term
Day-care services for people with dementia are organised in various ways, usually with the aim of promoting independence, quality of life, and health (Abramson, 2009; Ellen et al., 2017; Strandenæs et al., 2018), as well as providing respite care for family caregivers (Symonds-Brown et al., 2021). In Sweden, the national guidelines for health and social care in dementia state that local social services should offer tailored day-care services to individuals with mild to moderate dementia, as well as to younger individuals with dementia. The service is granted as a form of assistance under the Social Services Act, and day-care service users often also receive other types of support, such as home care. Service users pay a fee that is heavily subsidised and calculated together with other eldercare services – users of Swedish eldercare pay fees based on the extent of the services and their own income, though the fees are capped at approximately 240 euros a month in 2025. Approximately 85% of Swedish local authorities have day-care centres for people with dementia, and around 16,000 persons participate in the programmes at any one time. Many local authorities operate multiple day-care centres and provide services for both younger and older individuals (Svenskt Demenscentrum, 2024).
Previous studies about day-care services have mostly used quantitative methods or focus on the perspectives of family caregivers (Strandenæs et al., 2018), and have drawn particular attention to the physical environment and how staff attitudes affect service users (Myren et al., 2017; Parker, 2005). Further, the literature finds that day-care service users exhibit fewer behavioural problems or symptom severity compared to those who only receive care at home (Lee et al., 2019). Greater well-being and perceived social support, along with lower levels of depression and agitation, have been reported among those who use day-care services compared to those who do not (Zank & Schacke, 2002). However, behavioural issues such as depression have also been described as a common reason for ceasing to attend day-care services (Måvall & Malmberg, 2007). Some studies have qualitatively explored service users’ own experiences, highlighting positive experiences such as gaining structure in their daily lives or being part of a context that offers social connections and meaningful activities (Brataas et al., 2010; O’Shea et al., 2019; Rokstad et al., 2017; Strandenæs et al., 2018). Staff interactions have been singled out as being highly valued (Rokstad et al., 2017), but there are also studies where participants described a lack of influence in organised activities or felt they were treated in a non-affirming manner (O’Shea et al., 2019).
Method
Data was collected from six day-care centres for people with dementia in two Swedish cities. The day-care centres were selected to capture variation in target populations and municipal size. Four centres were located in a larger city (over 300,000 inhabitants) and two in a small city (approximately 35,000 inhabitants). The websites of each city described their day-care centers as an opportunity to meet others and to give structure and meaning to the day. Two of the centres were aimed at younger people with dementia and four targeted older individuals.
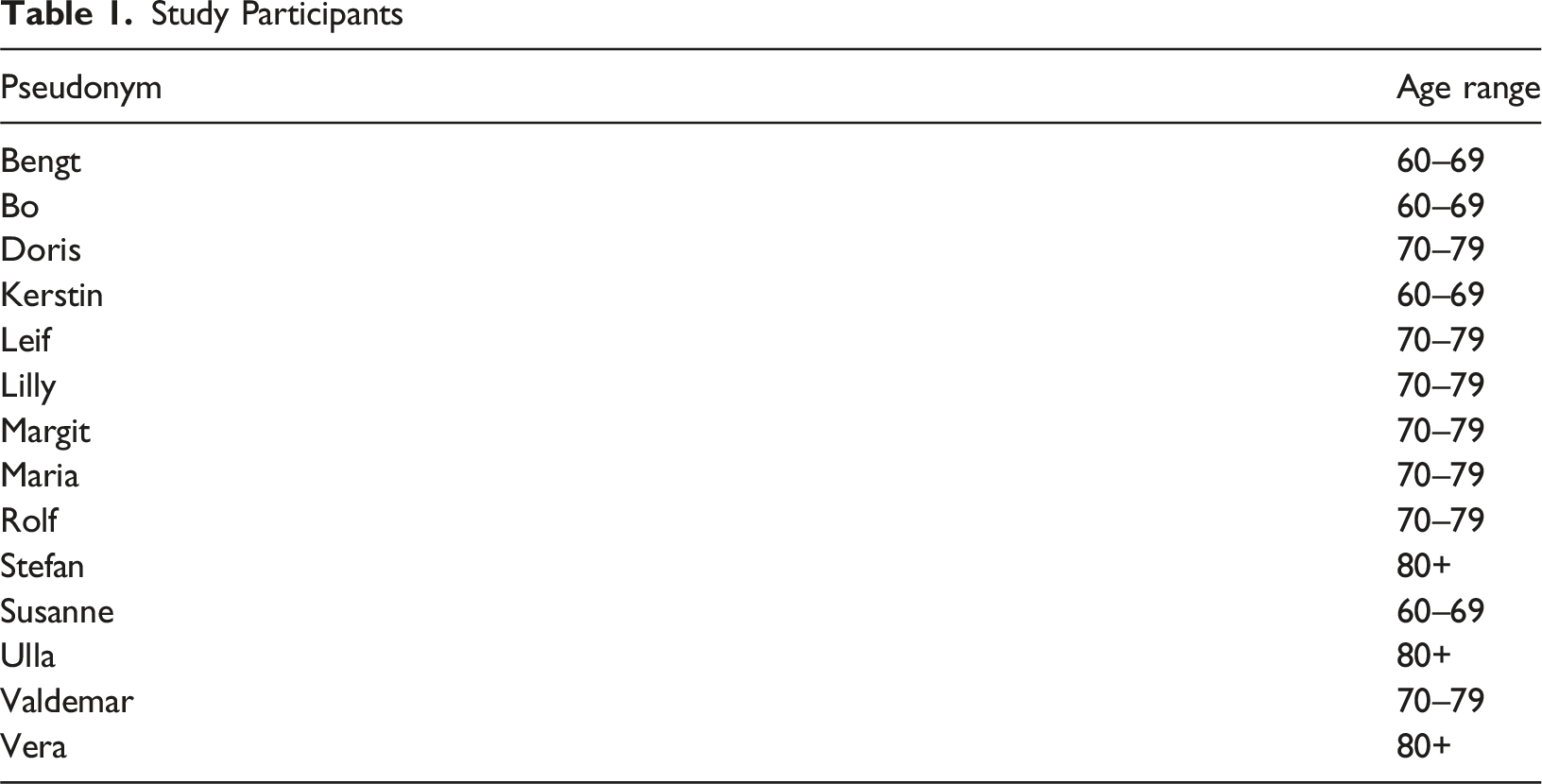
Fourteen day-care centre users were recruited for the present study – eight women and six men, aged between 60 and 90 years old (mean age = 74). The majority were born in Sweden, and only one had moved to Sweden as an adult. All respondents lived in ordinary housing, either alone or with a partner. Respondents were chosen in collaboration with the day-care staff to reduce the risk of including individuals who might be harmed by participating. The inclusion criteria included a sufficient language ability to take part in a conversation and a basic understanding of the purpose of participation.
The interviews were conducted between September and October 2024 at the six day-care centres during ordinary opening hours. At the time of the interviews, the respondents were attending one of the six day-care centres and participating in its activities at least one day a week. The information letter provided to participants stated that staff could offer support if the interview caused discomfort. One participant requested such support before the interview began. In this case, staff assisted on a few occasions by helping the participant put into words details they were trying to describe.
Since people with dementia may have varying levels of awareness and different attitudes towards their own diagnoses (Scott, 2021), the interviewers aimed to reflect the language the respondents used themselves to describe their difficulties. However, all respondents demonstrated some awareness of their diagnosis. Slightly more than half explicitly stated, on their own initiative, that they had a cognitive illness. Others referred to their difficulties more indirectly, mentioning memory problems.
For ethical reasons, out of respect for participants, awareness of diagnosis was considered important, as the individuals in this study are presented as persons living with dementia. During the interviews and in the coding process, however, the focus was not on diagnostic insight but rather on the kinds of identities that were made possible and enacted within the settings.
The interviews were based on a semi-structured interview guide, inspired by previous similar studies (for example, O’Shea et al., 2019; Strandenæs et al., 2018). The questions primarily focused on the respondents’ experiences of day care, but also addressed lifestyle and self-image. The interviews lasted between 33 and 71 minutes. All interviews were audio recorded and transcribed verbatim using the software program Whisper.
Ethical Considerations
The study was approved by the Swedish Ethical Review Authority (Ref. 2022-00825-01 & Ref. 2024-03835-02). To obtain informed consent, staff at the day-care centres distributed information letters about the study to interested individuals during the recruitment period. Close relatives of potential participants also received the information letter to ensure transparency; however, only the person with dementia provided written consent. To preserve the respondents’ anonymity, we have not included their exact age or other information that might be used to identify them.
To minimise the risk of distressing respondents during the interviews, the interviewers adjusted the follow-up questions and approached respondents’ stories with sensitivity, acceptance and respect. During interviews, the interviewers continually assessed whether consent remained in place. Day-care centre staff and an external licensed social worker were available should a respondent require additional support.
Study Participants
Data Analysis
The data was analysed using a reflexive thematic analysis, following the six-phase approach outlined by Braun and Clarke (2006). This process involved familiarisation with the data; generating initial codes; searching for themes; reviewing themes; defining and naming themes; and producing the final version. In the first stage of the analysis, two of the authors (LN and EF) familiarised themselves with the material to gain a sense of each interview as a whole. In the second stage, all interviews were coded with the software program NVivo by taking an inductive approach, whereby all material that seemed connected to the day-care centre experience was included. At this stage of the coding process, all the authors had ongoing discussions about the codes to explore the nuances in the data. In the third stage of the analysis, the preliminary themes were selected, focusing on their meaning and the codes’ interpretative contribution rather than their frequency. The process was not linear, and the final two stages took place partly in parallel with the writing of the final text.
Results
We identified four themes related to identity formation: (
Respite from Troubled Identities in Everyday Life
In contrast to their appreciative comments about their day-care centres, respondents talked about stigmatised identities in their home lives. The problems of daily life stemmed from living with dementia in interaction with the surrounding environment. One concern was people’s lack of understanding about the condition, which Kerstin described using the example of her partner – she wanted to talk to him about her situation but ‘he doesn’t want to listen’. Bo described his experience of not feeling understood in everyday situations outside the day-care centre: No, but many people don’t understand what, how the illness, the condition appears. Because when people see you out on the street, or, or when my siblings see me, they say, ‘well, you look, you look fine. You look healthy. You’re not sick, are you?’ They have a hard time understanding that I’m limited in many things I can’t manage. And that, that doesn’t show on the surface, but it… it’s there. (Bo)
There was also anxiety about not being able to adhere to social conventions and norms. Lilly explained that she and her husband used to have an active social life, but she had chosen to withdraw for fear of seeming strange or not being able to contribute to the conversation. What these experiences had in common was the difficulty of interacting with an uncomprehending environment, which in Lilly’s case resulted in self-stigmatising thoughts and a reduction in social contact (cf. Gajardo et al., 2021).
The question of why respondents attended a day-care centre also pointed to problematic identities in everyday life. Several described themselves as lonely, both from their own perspective and in their interactions with others. ‘It was my daughter who thought I was sitting at home alone too much’, said Margit. In Lilly’s case, it was her husband and daughter who thought that ‘I was too passive at home.’
While Margit was aware that her daughter experienced their frequent contact as burdensome, a more complex problematic identity in relation to close relatives was found in Leif’s description of his participation. Leif was the respondent who was least satisfied with the day-care centre and did not attend because it met his needs: It was probably a relief for my wife so that she could go into town without me having to be with her all the time. […] So we’ve set aside two days a week here. So it’s quite okay. (Leif)
Leif signalled a perception of himself as a burden to his wife, but at the same time emphasised his own involvement in the decision to attend a day-care centre, which relieved his wife. This allowed him to adopt an identity as a considerate, responsible partner. In addition to participating in the day-care centre, Leif was also a member of a Parkinson’s association, which gave him the opportunity to compare the two settings. Leif emphasized that he enjoyed being part of the Parkinson’s association, which was more structured, but that the day-care centre was ‘quite okay’ and offered him perspective on his own situation: I have nothing against coming here, absolutely not. It works well. I’m well taken care of by the staff, so it feels safe. I think it’s good that it [the day-care centre] exists. It would be sad if it disappeared. It gives me… by taking part like this, I can see that there are others who are much worse off than I am.
Attending a day-care centre – and considering it a self-chosen act – can thus be understood as enabling identities that reflect thoughtfulness and have a positive effect not only on everyday life, but also on the respondents’ relationships with concerned or overextended relatives. Doris noted that both she and her husband thought it was ‘really nice’ that she had started attending the day-care centre.
Recognition Without Focusing on Dementia as an Identity
All respondents expressed their awareness that they had a dementia-related condition, but it varied in prominence in their narratives about day-care centres. Kerstin, for example, openly stated “I have Alzheimer’s” while Rolf explained that he had “memory issues”. Bo referred to situations where other participants lost the thread of a conversation, but he was understanding of others’ memory and communication difficulties because he himself was ‘in that situation sometimes’.
Respondents viewed other day-care users as understanding the difficulties they were living with, which fostered both tolerance and a sense of community. Bengt noted: ‘We’re in the same boat. We who are… not the staff, but we who attend here.’ Bo also pointed out that the condition was something they shared: ‘Yes, we have the illnesses in common, we have different symptoms and diagnoses, and it’s quite nice to feel that you’re not alone.’
In some cases, respondents spoke of their irritation with those who downplayed symptoms, which Margit described as an attempt to stand out: So I ask [another service user] who seems so confident, ‘Do you remember what we had for lunch?’ ‘No’, she says too. So she doesn’t remember either. Even though she acts all cocky. So I’m not the only one who forgets, and that’s something to be glad about.
The expression ‘that’s something to be glad about’ points, in a somewhat unusual way, to a sense of similarity among service users based on their memory difficulties, which, in this context, was contrasted with one person’s attempt to appear less affected by the condition.
From the participants’ descriptions of the day-care centres, we concluded they were not organised around a shared identity of the kind found in social movements. Neither service users nor staff initiated discussions about dementia or group reflections about living with the condition or relationships with others. Valdemar described it as an ‘unspoken understanding’ about why people were at the day-care centre, and it was not a matter which they dwelled on, which Susann expressed gratitude for: ‘Everyone has an illness, so it’s also a bit… but not too much, thank goodness.’ Two respondents differed about the general reluctance to focus on the diagnosis, and said it could be valuable to discuss what dementia means together with others in the groups they visited.
A Supportive Environment Allowing Participants to Step Back
Social settings and organised gatherings make it possible for individuals to create collective identities based on their relationships and shared communities (Tajfel & Turner, 1979). In the case of the day-care centres, such an identity was signalled through membership of ‘the Club’, a term used by both staff and service users. Several respondents linked their enjoyment of the Club to activities such as talking, socialising, and eating together. Some mentioned that they looked forward to going to the day-care centre and seeing the others, and that the specific group they belonged to was important to them.
Several respondents felt that the social climate at the day-care centre contributed to the feeling of being ‘warmly welcomed’, as Vera put it, and ‘you can be who you are, on that day’. When asked why she enjoyed the day-care centre, Lilly replied: Lilly: Well, it’s that you meet others and do things together and so on. Interviewer: And what does that do to a person? Lilly: Well, you’re part of something.
That ‘something’ had specific characteristics: the staff planned and organised activities, while participants were able to take a step back. Several respondents said they were able to relax at the day-care centre because there were fewer demands than in everyday life, which often included heavy expectations about routines and performance. Rolf spoke about the practical issues with his interest in motors, and how he could ‘disconnect from all that completely’ at the day-care centre. As he summed it up, it was where ‘I don’t feel any pressure to perform or anything’.
Maria was another who commented on the low-pressure nature of the day-care centre setting: ‘We’re in there to listen to what they [the staff] have to say and what activity we’ll be doing today. And it’s very relaxing.’ This may also explain the prevailing view among respondents that it was the staff’s role to plan and lead activities. The staff were also expected to pick the topics for the group to discuss, as mentioned by Maria when asked about influencing the choice of activity: No, I haven’t thought that I’m missing anything or that I should suggest that we do this or that. No, honestly not. Since we are several people, it might not suit everyone, and someone might even say ‘no, I don’t want to do that’, so it’s just as well that the staff decide what we can do, whether we want to or not. (Maria)
Maria felt that the staff could determine what was appropriate, noting that ‘I’m one of those who just sit around together with the others.’ Doris said something similar, reasoning that staff ‘know more than we do’.
The respondents’ sense of stepping back was also evident in their descriptions of a typical day at the centre. Susanne summarised its as ‘Now we’re going to rest for a while. Now we’re going to eat. Now we’re going to… go for a walk. And yes. That’s kind of how it is.’ Some mentioned interests they could pursue at the day-care centre, such as painting or watching football, but said they had not requested these activities. Even though they said they appreciated having some influence, saying they could decline activities or make suggestions, none expressed a desire to have greater control over the everyday running of the centre. Instead, they deferred to staff.
The staff were consistently described in positive terms: they praised, affirmed, and cheered people up in ways that were appreciated, but also provided emotional support, both related to dementia and to other concerns in life. Some respondents highlighted the staff’s knowledge of dementia, or noted that they could offer answers and support at difficult moments. The staff also helped participants stay informed about various issues. Ulla explained that staff could answer all kinds of questions: ‘It could be something I’ve read, seen in a book, or watched on TV or something. And then I get an explanation of what I didn’t understand.’
Several respondents gave examples of activities such as quizzes and reading aloud from the newspaper, which helped them stay up to date on current affairs: So you’re a bit informed [laughs], about what’s happening. Because you’re still the same as before. You read newspapers, but you don’t really have the energy to keep up with it, so… it’s the TV [at home], and then we talk about the news here.
Doris’s description of being ‘still the same as before’ was her motivation to stay informed, and the day-care centre contributed to a sense of preserved abilities, competence, and continuity in her self-image. We found that a clear picture emerged of service users stepping back from the planning and execution of day-care centre activities, a role that respondents described as appropriate given the staff’s expertise and the need to accommodate their diverse preferences.
Shared Presence Without Close Personal Ties
Participants described socialising with others as important, but there was a marked absence of community based on shared characteristics or interests. Despite the fact that several respondents had attended the same day-care centre for years, none mentioned having ever met up with other service users outside opening hours. Loneliness was one of the main reasons for going to day care. Ulla said of the days she didn’t attend: ‘So last week, when I wasn’t here on Tuesday, those were really tough weeks. […] It was just too much loneliness.’ That degree of loneliness might be expected to encourage people to build on relationships made at the day-care centre, but this did not seem to be viewed as an option by the respondents. Stefan noted: ‘We who gather here, we don’t then go and have coffee somewhere.’
The day-care centres did not contribute to the development of dyadic friendships, and identities rooted in a connection with another individual participant were absent from the material. Instead, a temporary sense of group belonging was formed while at the centre. When asked whether she had anything in common with the other service users, Margit replied: ‘No, I don’t think we do. But we do sit and talk about world affairs and things like that, but we don’t have anything in common.’ Respondents described a shared presence, but also reflected on how close they wanted to be with other service users: They know I’m married, but not… if you say, I mean, you don’t go as deep as with a female friend, for example. Not those kinds of things, but more… When we talk about the kids, we talk about this one or that one. That kind of stuff. So, just general, really. (Doris)
Doris contrasted the kind of depth found in a friendship with a female confidante to the relationships between people at the day-care centre, relationships she was nonetheless content with. Several respondents reflected on the absence of personal relationships, and in some cases, there was dissatisfaction at the lack of deeper personal knowledge about one another. Leif, who was generally more dissatisfied with the day-care centre than the other respondents were, remarked, ‘It felt a bit tough at the beginning, not being able to connect with anyone.’ Valdemar expressed a different attitude and enjoyed contributing his knowledge and skills, at times taking on a central role. During the interview he described a situation where he shared some personal texts he had written with other service users: They, well, they’re a bit less educated, but they might have worked in an office or whatever, but they clearly understood. They said it hit home, and that made me really happy, actually. (Valdemar)
Valdemar’s effort to step forward as an individual also involved risk, something hinted at in his own characterisation of other service users. Among the respondents, there was some irritation directed at people perceived as overly talkative or as trying to stand out by talking about status markers like education or past careers. Lilly explained that in the beginning she had tried to talk more and ‘make a name for myself’ among the others. She said she would have liked to know more about the others personally but felt there were social rules that made this difficult: ‘Sometimes I’d like to know a bit more about each person and why they’re here, but it also feels a bit like you’re being nosy… in the wrong way.’ Other respondents had similar considerations about other people and the norms of the setting, talking of trying to ‘read the room’, avoiding ‘long speeches’, or ‘disturbing others.’
Discussion
In this study, we explore how people with dementia experience day-care centres and what identities are made possible and realised by those who use the service. The term ‘social cure’ is informed by social identity theory, and refers to the strong connection between participation in group communities and people’s health and well-being (Jetten et al., 2012). Efforts that help create and maintain social relationships, identification, and inclusion in groups can therefore counteract poor physical and mental health. Previous studies have highlighted the supportive role of staff at day-care centres in affirming and encouraging service users individually and in relation to the group (O’Shea et al., 2019; Rokstad et al., 2017). The social aspects of day care have also been described as important by service users (Strandenæs et al., 2018; Telenius et al., 2020) and the provision of adapted social settings has been associated with breaking the social isolation of dementia (Brataas et al., 2010).
Given the stigma of dementia, it is possible that day-care service users will distance themselves from the diagnosis by describing themselves as less affected than others, as noted by O’Shea and colleagues (2019). Conversely, it is also possible for a dementia diagnosis to be central, bringing people together in a collective identity – similar to what occurs in organisations where people unite around a shared diagnosis or experience of disability, forming the foundations for a social movement (Bartlett & O’Connor, 2010). However, this was not the case in the present study; the shared diagnosis of dementia was neither hidden nor defining to social life at the day-care centres. One possible explanation for this lack of focus might be the nature of dementia: several respondents spoke of their awareness of a future with far more serious problems than they currently faced. Lilly mentioned that other ‘sicker’ people might serve as a reminder of her own future, and one respondent had a negative experience with a group where dementia had progressed to a point that made communication difficult.
We found that respondents, regardless of age, valued the context provided by day-care centres, contrasting with the loneliness they experienced at home and the demands placed on them outside the centre. Day-care centres were experienced as a form of respite from troubled identities in everyday life: a space where participants could be recognized without a focus on dementia; an environment that allowed them to take a step back while feeling supported and accepted; and a setting that offered a sense of shared presence without close personal ties.
Their descriptions of their motives for participating can be used to interpret the identity work at the day-care centre, and what emerged was a picture of problems with loneliness, relatives’ concerns, personal worry about being a burden to family members, and difficulties in interacting with an uncomprehending environment. Participation at the day-care centre was associated with words such as community, laughter, and joy. However, participants did not discuss their attendance in terms of preventing or delaying institutional care. Rather, participation was connected to the here and now, to everyday life with staff and other participants.
Based on a theoretical framework in which identities are developed in interaction with others, a picture emerges of how acceptance at a day-care centre enables flexible identity formation, where dementia is neither denied nor placed at the centre. Both the setting and the group offer opportunities to form identities that can move between the healthy and ill aspects of the person. Mutual acceptance as described by respondents is not a given. O’Shea and colleagues (2019) have highlighted how participants can distance themselves from and stigmatise others with dementia in day-care centres. Possibly, the homogeneity within the group influences how likely day-care users are to position themselves against their peers. Previous studies have shown that users may prefer age-segregated programmes (Beattie et al., 2004; Telenius et al., 2020), and that frustration at being unable to communicate with other participants can become problematic (O’Shea et al., 2019). In this study too, there were comments about such difficulties, related to past participation in a group for people with communication challenges. It is possible that the ambition to create relatively homogeneous groups in terms of age and cognitive ability – which is standard practice in Sweden – contributes to the rarity of such descriptions in our data.
Although the respondents rarely talked with each other about their diagnosis, several described how they related to and accepted others’ difficulties because they resembled the challenges they themselves lived with. Dementia is associated with both stigma and social difficulties (Nguyen & Li, 2020), and one question we asked before the data collection was whether the activities had the character of support-groups, or whether they built a collective identity aimed at changing perceptions of dementia. This was not the case. Respondents described shared experiences based on their diagnoses, but they were limited to memory and communication issues. The type of in-group cohesion built around opposition to out-groups was also absent (Sedikides & Brewer, 2001; Tajfel & Turner, 1979). However, day-care centres seem to offer something else, which could be related to Brewer’s description (1991) of social identities as arising from different needs. Implicitly, such positive social interactions can be seen as a counterpoint to the stigmatisation of people with dementia – a stigma that partly consists of the perception that they are incompetent and repellent.
Questions of participation and involvement in services for people with dementia have been explored using approaches that emphasise citizenship and human rights (Kelly & Innes, 2011; Nedlund & Bartlett, 2017). Approaches aimed at encouraging various roles among service users have been discussed in relation to day-care centres (Myren et al., 2017), and in a review article, Ingard et al. (2023) introduced an adapted version of Shier’s model (2001) of participation, where the highest level involves opportunities for power-sharing and shared responsibility within services.
Beyond the issue of democracy, power-sharing and responsibility can be seen as contributing to empowerment and to identities of being competent and capable. The question is particularly interesting since participants in our study expressed their appreciation for the unequal distribution of responsibility between service users and staff – a distribution they defended by referring to their admiration of the staff and the way the service was run. One possible interpretation is that this position enabled them to see themselves as socially competent collaborators in a group where it is necessary to be considerate of others, and that the active relinquishment of responsibility reduced the demands they found difficult to meet in other contexts. This interpretation is supported by the participants’ positive descriptions of the service as an accepting, low-pressure environment, as well as their many references to the need to take others into consideration.
Social interaction has been highlighted both as a way to strengthen the experience of continuity in one’s identity (Fuchs, 2020; Örulv, 2010), and as something shaped by the social environment and norms of the group with which one identifies (Higgins & May, 2001). The respondents’ interactions with other service users could therefore be understood as an opportunity to ‘do’ identity (Örulv, 2008), where the norms associated with the context provide the framework for how this is done. This ‘doing’ of identity also allows participants to be, and experience themselves as, social agents with social needs and competences within the particular context of a day-care centre.
It is thus possible that the supportive approach of the staff, as described by our respondents, made it possible to focus on socialising and relating to group dynamics, thereby promoting socially grounded identities. Paradoxically, even the concern about breaking group rules can be understood as part of the process – duly supported – of constructing an identity as a socially competent member of a group-based activity. Neither the concern nor the irritation with others was linked to symptoms of dementia. Instead, respondents tended to comment on general social norms: talking too much and dominating the group; intruding into others’ private lives; or trying to appear ‘better’ than others in terms of status and achievements. Group belonging thus appeared as a hindrance for those who wished to present themselves with admirable or remarkable traits.
The issue of influence, participation, and power-sharing is important, and the possibility of different interpretations based on service users’ perspectives calls for further in-depth studies using an ethnographic approach that includes service users’ observations.
The absence of friendships and personal relationships also stands out as difficult to interpret. One possible explanation may be people’s ability and interest in creating social bonds through the kind of individual differentiation processes described by Sedikides and Brewer (2001). The respondents’ descriptions of community focused on the group under the leadership of staff. Establishing friendships and then transferring them to other contexts outside the day-care setting would require maintaining the interaction even when the supportive elements were no longer present. This question, too, should be the subject of further study. Could day-care centre become arenas for communities that extend into other contexts, or are they appreciated precisely because they offer a distinct safe space, far from the problems of ordinary life outside?
Limitations
Our results in this study are based on the perceptions of the respondents; staff, family members, and others with insight into the question were not included. All respondents were interviewed individually, except for one who wished to have a staff member present. This may have affected their ability to express criticism, but likely also contributed to a greater sense of security during the conversation. The staff member provided linguistic support and help in recalling past events. This arrangement raises the question of whether the results would have been different if all the interviews had been conducted with support present. In order to avoid interviewing individuals who lacked the capacity to give informed consent, the staff selected which participants would be asked to take part, and this too may have influenced our findings, as it is possible that participants with plainly negative views were not included.
Conclusion
Our aim with this study was to explore how people with dementia experienced day-care centres, and what identities that are made possible and enacted within this setting. The day-care centre emerges as a place where acceptance, both from staff and service users, enables identities that move between states of health and illness. Acceptance also appears to counteract stigmatisation and support flexible identity formation, in contrast to troubled identities of outside contexts. We would argue that it is the interaction and sense of group belonging, rather than the dementia diagnosis or individual relationships, that unite care service users. The day-care centre can thus be understood as a place where the social ‘doing’ of identity is made possible, rather than a site of clearly defined relational or collective identities.
Supplemental Material
Supplemental Material - Dementia as Neither Hidden nor Defining: Identity, Group Belonging, and Wellbeing in Day-Care Centres
Supplemental Material for Dementia as Neither Hidden nor Defining: Identity, Group Belonging, and Wellbeing in Day-Care Centres by Linnea Nyström, Ellen Foucard, Tove Harnett, Håkan Jönson in Dementia.
Footnotes
Acknowledgements
The authors wish to thank the participants of the study for generously sharing their thoughts and experiences. The authors also wish to acknowledge the valuable contributions of Eva Hoff, who served as the co-supervisor for the Master’s thesis on which this article is based.
Ethical Considerations
The study was approved by the Swedish Ethical Review Authority (Ref. 2022-00825-01 & Ref. 2024-03835-02).
Consent to Participate
All participants provided informed consent.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The study was funded by the Swedish Research Council for Health, working Life and Welfare (FORTE Ref. 2021-01815)
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
Due to ethical concerns and sensitive information on health, supporting data cannot be made openly available. Further information about the data and conditions for access is available at the Lund University Data Archive:
Supplemental Material
Supplemental material for this article is available online.
Author Biographies
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
