Abstract
Exclusion, marginalization and stigma remain common experiences for people living with dementia. Dementia capable communities offer a pathway to support the wellbeing of people living with dementia by creating spaces where people living with dementia and their care partners are supported and empowered. This review of reviews examines the ideas and approaches for dementia-capable communities across disciplines and at multiple levels of action. Review articles focusing broadly on the development and implementation of dementia capable communities were analyzed for their methods, evidence base, approaches, and recommendations. The results highlighted the importance of engaging and collaborating across different parties, the need to support dementia awareness and address stigma and the key role of policy regulations and planning guidelines in facilitating dementia capable communities. They also noted the need to have a focus on the built environment and making it easier for people living with dementia to navigate the community. The importance of social and community based supports in promoting connection and wellbeing was also brought forward. Systemic critical analysis of the public policy and political conditions that would be needed for the development and maintenance of dementia capable communities was missing. Development of thriving communities where people living with dementia are supported and included will require contending with these challenges.
Introduction
“Without a major rethink, I am starting to believe that the last 20+ years of dementia advocacy has mostly been a waste of time…ripples in a pond are no longer enough” (Kate Swaffer, person living with dementia and dementia advocate) (Swaffer, 2020).
The United Nations Convention on the Rights of Persons with Disabilities enshrines the right of people living with dementia to full participation and inclusion in society (United Nations Convention on the Rights of Persons with Disabilities, 2006). Yet exclusion, marginalization and stigma remain common experiences for the over 55 million people worldwide living with dementia (Alzheimer’s Disease International, 2021; Dudgeon, 2010; Herrmann et al., 2018; Rewerska-Juśko & Rejdak, 2020; Siette et al., 2023). The majority of people living with dementia reside in the community, and there is wide consensus on the importance of maintaining independence and functionality in place. The term dementia capable communities (also referred to as dementia friendly communities) represents strategies to support people living with dementia to remain engaged and included in their communities (Alzheimer’s Disease International - Dementia Friendly Communities: Key Principles, 2016). Research and practice in the area of dementia capable communities has almost always focused on interventions at a singular level, such as training of staff in target organizations or planning accessible built environments. There is a critical need to move beyond a single level of impact and intervention to create interdependent communities that support people living with dementia at all levels from the individual level supports to broader policies (Vervaecke & Meisner, 2021).
A critical disability perspective understands disability as relational, dependent on complex layers of interactions of a person’s abilities with people, environments, things (e.g., tech, devices, animals) and social, cultural, and political structures (Dear et al., 1997; Hall & Wilton, 2017). As such, actions need to address multiple levels from individual to socio-political to overcome the complex phenomena that hinder full participation of people living with dementia (Dorey, 2005; Goodley, 2013; Goodley et al., 2019; Shakespeare et al., 2019; Vehmas & Watson, 2014). Actions at multiple scales range from the knowledge of individual community members to inclusive building design and neighbourhood planning to municipal, provincial, and federal policies mandating and supporting inclusion and accessibility (Dorey, 2005; Hobson et al., 2019; United Nations Convention on the Rights of Persons with Disabilities, 2006). The reward of multi-scalar action could be substantial to the well-being of people living with dementia. This relational understanding of disability also aligns with human rights-based approaches to dementia and supports a broader view of social citizenship.
Continued engagement through establishing dementia capable communities has many benefits: improved mental and physical health, social support and connection, and sense of worth among people living with dementia (Burton & Mitchell, 2006). Engagement of people within their communities is also important to promoting quality of life, raising awareness of people living with dementia, and reducing stigma (Biglieri & Dean, 2021; Ward et al., 2018).
Communities that fully support people living with dementia demand action across multiple scales, which includes changing the knowledge and mindset of individuals, inclusive neighbourhood planning and programming, to provincial and federal policies mandating accessibility (Dorey, 2005; Goodley, 2013; Goodley et al., 2019; Hobson et al., 2019; United Nations Convention on the Rights of Persons with Disabilities, 2006). Coordination across these scales is a major barrier to substantial change in the experience of people living with dementia (Chowdhury et al., 2011; Dorey, 2005; Hobson et al., 2019; Lin, 2017; Singh-Peterson & and Underhill, 2017). Recent scoping reviews have synthesized research related to dementia-capable communities (Hung et al., 2021; Sturge et al., 2021a). Despite similar timeframes and search strategies, it was our impression that there was little overlap in the studies included, suggesting that the fine details of focus, often defined by level of action or discipline, have influenced scope and findings. In this review of reviews, we synthesize findings for dementia-capable communities across disciplines at multiple levels of action. We also analyse gaps in current discussions of dementia capable communities and reflect on areas of action.
We examine current framings of dementia capable communities, leveraging a critical disability perspective to grapple with core approaches, structures and resources for dementia capable communities as identified in recent reviews. As researchers from a wide array of disciplines (planning, kinesiology, public health, gerontology, critical theories, etc.) and people with lived experiences of dementia, we conduct this examination with a conviction that establishing dementia capable communities will require an expansion of our current approaches and understandings.
Methods
Methodological Rationale
We conducted a scoping review of reviews to identify emerging guidance regarding dementia capable communities across disciplines, levels of intervention and levels of governance (e.g. local, provincial, federal governments). The methodological approach to this scoping review of reviews was informed by the framework established by Arksey and O’Malley (2005).
Inclusion Criteria and Study Selection
Reviews were included if they: (1) were published within the designated period (2012–2024); (2) were systematic or scoping reviews related to dementia capable communities; (3) were written in English. Primary research, editorials, dissertations and other publication types were excluded. Reviews focused broadly on age-friendly communities or dementia capable health care or long-term care were also excluded.
Search Strategy
Database searches were conducted in 2021 and 2024 to retrieve relevant articles. Reviews published in English between 2012 and 2021 and between 2012 and 2024 were included, respectively, where we had initially set a 10-year eligibility time and then added more recent studies in the second search. PubMed, CINHAL and SCOPUS databases were searched using the following concepts and related terms: “Dementia”, “Inclusive”, “Friendly”, “Community”, and “Review”. The terms were intentionally broad to be as inclusive as possible. The specific search strategies for each database are provided within the Supplemental Materials.
Study Selection
In the first stage of study selection, pairs of investigators (OT, RV, NA, SM, MK) independently screened the article titles and abstracts to determine relevance of studies. Disagreement was resolved through discussion and consensus, and through consultation with senior investigators (SB, LM) when needed to reach a decision (Kohl & and McCutcheon, 2015).
The second stage consisted of pairs of investigators independently reviewing the full text of each included article to determine whether it met the inclusion criteria. Upon reviewing full texts, investigators met to resolve any disagreements through discussion and consensus.
Data Extraction
Investigators extracted data using a data extraction form, which included information on study year, affiliations and areas of study of all authors, search databases and terms used and whether or not the study used any quality indicators. One investigator (NA) extracted this data to ensure consistency. All investigators reviewed the data extraction template. Any challenges in data extraction were resolved through discussion with the project team (Kohl & and McCutcheon, 2015).
Analysis
The results and discussion sections of each article were analysed using thematic analysis (Braun & Clarke, 2006; Richards & Hemphill, 2018). A critical disability lens was leveraged when conducting thematic analysis to draw attention to the multiple levels of action, from individual to socio-political, that would contribute to dementia capable communities. Selected articles were independently reviewed by at least two reviewers to select relevant extracts and assign initial codes to selected extracts via an inductive process. Once all articles had gone through an initial coding process, reviewers discussed each of the codes applied to extracts and arrived at a set of consensus codes. Following this, reviewers grouped the consensus codes into themes and sub-themes, which were then iterated and consolidated into the final set of themes and sub-themes in collaboration with the research team. Themes and sub-themes were then defined and refined to ensure that data was adequately and accurately captured.
Results
Our initial search in 2021 yielded 110 review articles of which 42 were duplicates. Following title and abstract screening, 54 articles were excluded that did not meet the inclusion criteria. A further 7 articles were excluded after full text screening, leaving 7 reviews included in the analysis. The second search conducted in 2024 resulted in 177 articles being extracted, of which 19 duplicates were removed leaving 158 review articles. A title and abstract search resulted in the exclusion of 151 articles. The full text of the remaining seven articles was reviewed, resulting in the exclusion of a further 5 articles, and the remaining two articles were included for a total of nine articles. Figure 1 shows the Prisma flow diagram. PRISMA flow diagram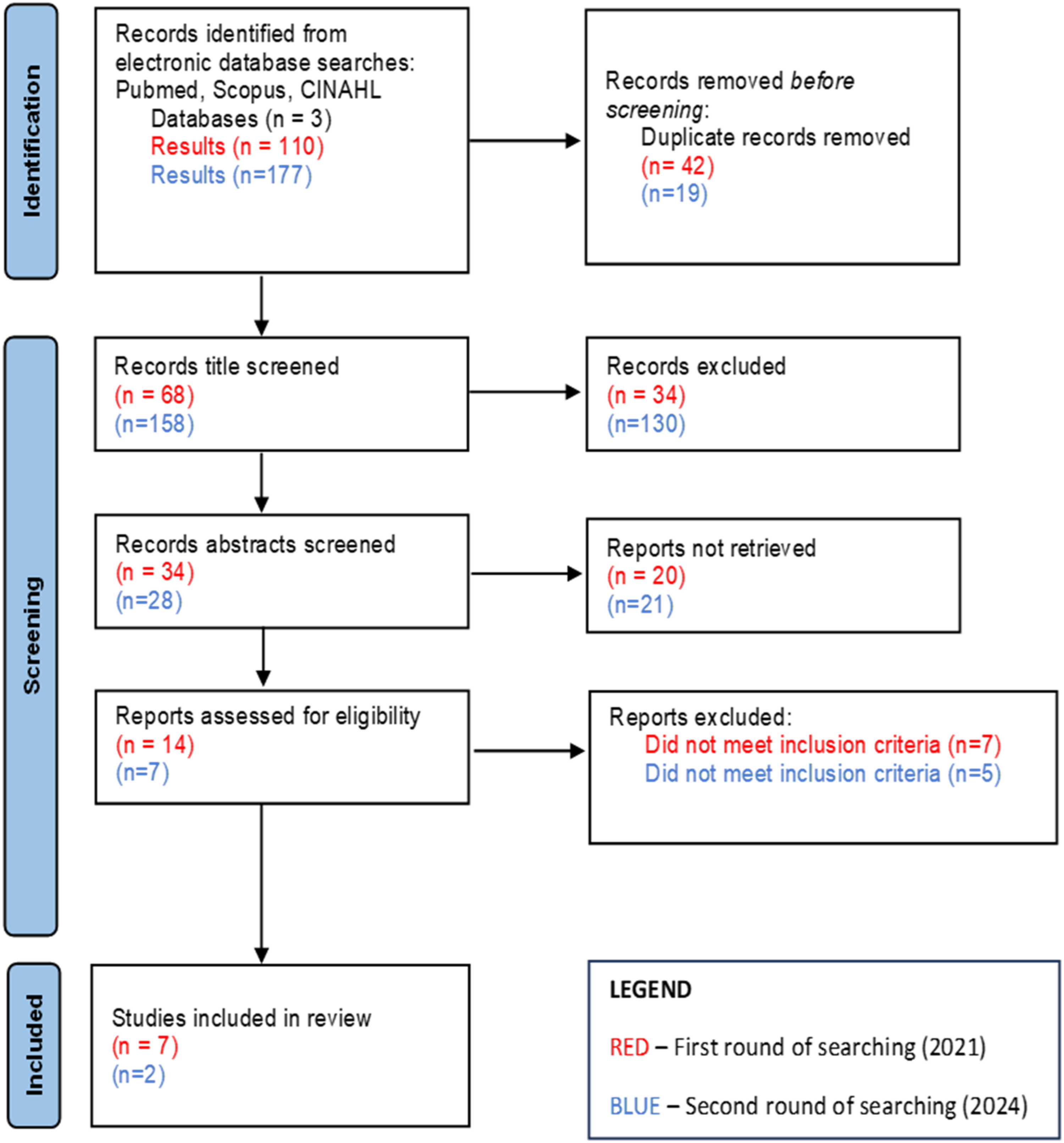
Characteristics of Included Review Articles
Characteristics of Included Reviews

Authors of the reviews came from a variety of academic disciplines, with the most common ones being gerontology, nursing and public health and with disciplines such as urban and community planning being the least common. Two of the reviews also included dementia advocates and community engagement advisors among the authors. The authors were largely affiliated with universities in high income countries in the global North, with one PhD student listed as an author from India. Most reviews did not meaningfully describe or engage with the racial, ethnic, cultural or migrant status of the study population included in individual papers. One of the reviews included explicit mention of the racial composition of the population of their component papers in their summary table (Craig et al., 2024). The other 8 reviews made some mention of diversity or some component of diversity (race, age, etc.) in their results or discussion section.
Across the 9 articles, 173 original articles were included in the reviews (Supplemental Materials: Table 2). None of the original articles were included in all the review papers and only five original articles were included in at least 4 of the review papers – Smith et al. (2016) n = 5; Mitchell & Burton (2010) n = 4; Mitchell, Burton and Raman (2004) n = 4; Wiersma & Denton (2016) n = 4 and Heward et al. (2017) n = 4). Nine original articles were included in 3 out of the nine reviews. Most original research articles (n = 159) were included in 2 or fewer reviews.
Qualitative Results
The thematic analysis identified themes reflecting actions and processes needed to create dementia capable communities, as well as gaps in how the literature addresses dementia capable communities.
Collaborative Processes for Dementia Capable Communities
A. Engaging and Collaborating With Interested and Affected Parties
The pivotal role of engaging and collaborating with a range of partners emerged as a strong theme within the selected reviews. Dementia capable communities began as community development efforts to assemble people living with dementia and collaborators to better support people living with dementia in the community (Hebert & Scales, 2019). Five out of the nine reviews highlighted the importance of engaging local residents in the development of dementia capable initiatives and in decision making related to dementia capable communities (Craig et al., 2024; Gan et al., 2022; Hebert & Scales, 2019; Hung et al., 2021; Shannon et al., 2019). The reviews emphasized that establishing dementia capable communities requires the inclusion of a wide array of collaborators, including people living with dementia, care partners, local businesses, advocacy organizations and other residents at every stage of the project (Craig et al., 2024; Hebert & Scales, 2019; Hung et al., 2021; Shannon et al., 2019). Engagement of people with lived experience (i.e., people living with dementia and care partners) was broadly considered imperative to planning of dementia capable communities and was specifically highlighted as important for guiding land-use diversity and nature area provision in one review (Gan et al., 2022). The reviews recognized that knowledge shared by people with lived experience was an important component of the dementia capable community development process and supporting the engagement and autonomy of people living with dementia should be a key aim of such initiatives (Hebert & Scales, 2019; Hung et al., 2021).
Engagement of local residents living with dementia in the development of new policy and planning decisions was identified among the principles for planning of built environments derived by Gan and colleagues (2021) in their review (Gan et al., 2022). Reviews also noted that dementia capable communities thrive in rural settings where there is a strong sense of community, which in turn may make it easier to engage collaborators (Craig et al., 2024). Conversely, the inclusion of a variety of groups brings several challenges, such as attracting commitment from organizations and ensuring adequate representation from the local community. For example, some reviews noted that business support for dementia capable initiatives is often driven by reputational concerns and shaped by commitment from organizational leadership (Craig et al., 2024).
Recruitment of people with lived experience of dementia was also recognized as challenging (Hebert & Scales, 2019; Hung et al., 2021). The reviews mentioned several factors contributing to this challenge, such as the stigma of dementia, barriers to communication, multiple gatekeepers and low diagnosis rates (Hebert & Scales, 2019; Hung et al., 2021). An additional challenge is the lack of representation of people living with dementia from diverse and racialized populations, whose experiences of dementia, access to resources and ideas of dementia capable communities may vary (Hebert & Scales, 2019; Hung et al., 2021).
B. Dementia-Related Training and Awareness Could Contribute to Dementia Capable Communities
A majority of the reviews pointed to dementia related education, training and awareness as a key contributing factor to develop dementia capable communities. Dementia awareness and education can counter stigma and improve communication and other supportive skills (Hebert & Scales, 2019; Hung et al., 2021). As a result, awareness and education initiatives could play a key role in garnering the commitment and collaboration of diverse groups for the successful implementation of dementia capable communities (Craig et al., 2024). Some reviews highlighted that education in community settings may improve the quality of interactions that people living with dementia experience in their communities, resulting in a more supportive environment (Sturge et al., 2021b). Reviews also drew attention to the importance of dementia awareness and training for different groups, such as businesses (Craig et al., 2024) and transportation services (Lanthier-Labonté et al., 2024). Some reviews also identified faith communities as another welcoming site for providing dementia related education, which may help address people of diverse ethno-cultural groups (Hebert & Scales, 2019).
Enabling Policies and Infrastructure for Dementia Capable Communities
A. Policy Regulations and Planning Guidelines are Needed to Facilitate Dementia Capable Communities
A continuum of commitments is needed to create and sustain dementia capable communities, including supportive policies, regulations and guidelines, staffing, funding and other infrastructure. Some reviews highlighted that action plans can facilitate the process and focus of dementia capable communities and promote sustainability by identifying resources and funding (Shannon et al., 2019). These plans can also mandate the inclusion of people living with dementia and clarify strategies to monitor progress (Shannon et al., 2019). Action plans can help local steering groups to establish dementia capable policies and priorities in their own community (Sturge et al., 2021b). Policy regulations and planning guidelines that support the design of dementia capable communities can encourage built environment professionals (like urban planners, policymakers, urban designers and architects) to build and design in a manner that is dementia capable (Shannon et al., 2019; Sturge et al., 2021b).
B.Impact of Individual-and Community-Level Socioeconomic Status
Socioeconomic conditions of individuals and neighbourhoods may significantly impact the experiences and outcomes of people living with dementia and care partners. However, research investigating the impact of socioeconomic conditions on dementia capable communities was sparse. Gan and colleagues (2021) suggested that neighbourhoods with higher socioeconomic status typically have better outcomes for people living with dementia (Gan et al., 2022). Social capital is associated with richer neighbourhoods 1 . Neighbourhood characteristics such as feelings of safety, trust in neighbours, availability and use of local amenities and parks, and better reputation outside of the community were also linked to higher rates of walking in the community (Keady et al., 2012).
The personal costs of dementia care and management are also under examined within the reviews. Many of the costs of caring for a person living with dementia are placed on care partners and family and can be a significant challenge (Keady et al., 2012). Moreover, these costs grow when the person with dementia is no longer able to independently access their local neighbourhood and services (Keady et al., 2012). Developing and sustaining effective dementia capable communities may help mitigate personal costs by facilitating a longer period of independence in the community (Keady et al., 2012).
A Holistic Perspective to the Built Environment
A. Ease of Access to Outdoor Environments and Spaces within the Community and Impact on Wellbeing
The majority of reviews discussed the importance of access to outdoor environments and community spaces for people living with dementia. Being able to safely and comfortably access outdoor environments was noted as valuable for enhancing physical, social and mental health for people living with dementia (Hebert & Scales, 2019; Keady et al., 2012; Li et al., 2021; Sturge et al., 2021b). The reviews noted evidence that walking, which is impacted by ease of navigating the outdoor environment and engaging in physical and social activities, may help to maintain cognitive functioning in people living with dementia (Keady et al., 2012; Li et al., 2021). It was also noted that the placement of familiar landmarks improves the perceptions of the community as safe and inclusive (Gan et al., 2022; Hebert & Scales, 2019; Hung et al., 2021).
Many built environment factors may influence how persons living with dementia experience their community, which include but are not limited to the design of sidewalks, availability of signage and rest spaces, type and presence of traffic calming measures as well as time of day (with more risk perceived in the evening) (Gan et al., 2022). Gan and colleagues (2021) synthesized their findings into a series of planning and design principles for neighbourhood built environments that would be supportive for people living with dementia (Gan et al., 2022). Hebert and Scales (2019) note that principles of design, which include both indoor and outdoor environments, are a significant part of current research on dementia capable communities (Hebert & Scales, 2019). In this context, environmental design connotes any adaptation to enhance the physical, social or functional ability of people living with dementia, such as signage with photos, noise reduction and transit that is safe and easy to use (Hebert & Scales, 2019).
B. Making it Easier to Navigate the Community
Most reviews reflected on the factors that facilitate community navigation and wayfinding for people living with dementia. Reviews highlighted that many factors can impede a person living with dementia’s ability and level of comfortability during the wayfinding process, including traffic noises, unexpected obstacles, and going out at night. Wayfinding and the ability to overcome challenges can get worse with the progression of dementia (Gan et al., 2022; Hung et al., 2021). Helpful characteristics of the environment include familiarity, distinctive landmarks, variation of building appearances, clear and uncluttered signage, sufficient lighting, and clear and smooth paths (Gan et al., 2022; Keady et al., 2012). Sensory cues, such as noise, smell, and visual stimuli, can also influence the wayfinding experience (Keady et al., 2012).
Some reviews discussed accessibility of transportation as another important consideration for navigating the community (Lanthier-Labonté et al., 2024; Li et al., 2021). As people living with dementia often stop driving relatively soon after diagnosis, accessible transportation options are important to maintaining mobility, connection to the community, and sense of belonging (Craig et al., 2024; Hebert & Scales, 2019; Keady et al., 2012; Li et al., 2021). 2 However, people living with dementia may have more difficulty adjusting to changes in bus routes or schedules so consistency is important in transportation planning (Keady et al., 2012).
Social and Community-Based Supports and the Impact of Stigma
A. Supportive Programs and Networks Can Enhance Inclusion
Community events, programs, and social hubs like coffee shops can support the development of meaningful relationships and foster a sense of inclusion for people living with dementia. Social connection also creates opportunities for support, which can promote wellbeing (Hebert & Scales, 2019).
Reviews pointed out that community-based programs and services are essential for people living with dementia to be able to age in place (Hebert & Scales, 2019). They highlighted that programs may improve functional abilities and autonomy, especially when the services provided are person-centered— that is, designed to be appropriate and relevant to the needs of the individual (Hebert & Scales, 2019; Hung et al., 2021). One of the reviews positioned the person-centred approach as best practice in dementia care (Hebert & Scales, 2019). One of the reviews also highlighted that persons living with dementia and their families have identified several services that may support aging in place, which should be key components of dementia capable communities such as meal services, personal care assistance, and connection to and navigation of other resources (Hebert & Scales, 2019).
Supports are also needed for care partners, who often provide substantial care (Hebert & Scales, 2019; Hung et al., 2021). Reviews also mention that challenges of care can have negative implications to care partners mental, physical, and social wellbeing especially when supports and respite are not available (Hung et al., 2021; Shannon et al., 2019). Additional barriers to accessing resources include difficulty getting to programs and services, low socioeconomic status, and ethno-racial identity, where people of minority ethno-racial identity may be less likely to be referred to programs by health care providers (Hung et al., 2021).
Some of the included reviews mentioned that rural areas may have fewer formal programs and services for people with dementia (Hebert & Scales, 2019; Shannon et al., 2019). As a result, people living with dementia often rely more heavily on friends and family for support in rural communities, increasing the importance of a strong social support network (Hebert & Scales, 2019; Shannon et al., 2019).
B. Stigma is a Barrier to Participation
A majority of reviews identified that stigma of dementia is a major challenge for people living with dementia and dementia capable communities. Several reviews identified community support networks and social relationships as a central part of dementia capable communities, which people living with dementia and care partners rely on (Hebert & Scales, 2019; Hung et al., 2021; Li et al., 2021). Independent of whether the entire community is dementia capable, interacting with welcoming and helpful people is supportive to people living with dementia (Lanthier-Labonté et al., 2024). However, reviews identified that community members can have poor understanding and limited experience of dementia (Hebert & Scales, 2019; Hung et al., 2021). These community members may be wary of interacting with people living with dementia due to concerns about disruptive behaviours and have greater concerns about the funding required to accommodate people living with dementia (Hebert & Scales, 2019).
Dementia capable initiatives could help to reduce stigma through awareness of and increased interaction with people living with dementia (Hebert & Scales, 2019; Hung et al., 2021). This could include intergenerational relationships and initiatives to have conversations about dementia and break down stereotypes (Hebert & Scales, 2019; Hung et al., 2021). Exposure could also be accomplished through other forms of education and awareness including educational campaigns, social media presence, and memory cafes 3 (Hung et al., 2021).
Usability of Technology for People Living With Dementia
The ubiquitous presence of everyday technologies, such as kettles, alarms, self-service checkouts, ATMs, and smartphones has the potential to promote, or restrict, the inclusion of people living with dementia in their communities.
The reviews highlighted several barriers, facilitators, and outcomes related to different kinds of technology. In some instances, technology such as cell phones can support the day-to-day living of people living with dementia and can lead to higher levels of engagement in public spaces (Gan et al., 2022; Keady et al., 2012). However, reviews also pointed out that people living with dementia often have to learn and remember new practices to use such technology, which can present challenges—for example, self-checkout machines in stores or trying to book appointments using digitized answering systems or booking transit tickets online (Gan et al., 2022; Keady et al., 2012; Lanthier-Labonté et al., 2024). Hung and colleagues (2021) suggested that to enable inclusive design and address the challenges associated with new technologies, strategies such as the use of low technology spaces and programs should be used (Hung et al., 2021).
Discussion
Siloing Persists
We analysed 9 review papers, which together included 173 original articles. Despite using similar search terms and being within similar time frames, none of the original articles was included in all reviews. While some discrepancy is not surprising due to different dates of study and differences in search strategy, the degree of independence is notable. This is reflected in our results, where many themes or sub-themes are primarily informed by a couple review articles with a focus on the area rather than a synthesis across all areas. The divergence in papers and findings reveals that dementia capable community research is still siloed, emphasizing the need to think across disciplines and levels of intervention (individual, neighbourhood, municipality, etc.). The lack of collaboration across levels and disciplines is surprising given that the strongest area of agreement across reviews is that the success of dementia capable communities hinges on the inclusion of a spectrum of collaborators such as local residents, businesses, social and policy actors, advocacy organizations, funding sources, people living with dementia and their care partners (Craig et al., 2024; Gan et al., 2022; Hebert & Scales, 2019; Hung et al., 2021; Shannon et al., 2019; Sturge et al., 2021b). Reviews highlighted that bringing together this wide array of collaborators and sustaining long-term partnerships can be challenging and requires recognition of the varying interests, incentives, resources and challenges of each party. No reviews were found that addressed these foundational issues beyond a surface level mention.
Lack of Research from Global Majority Nations and on Diverse Populations
Six out of the nine scoping reviews reference less than 30 articles, and the vast majority of articles included focused on the high-income countries. These findings highlight that dementia research continues to struggle with the inclusion of globally racialized and marginalized communities (Babulal et al., 2019). In high income countries, racialized and ethnic minority communities continue to experience inequities in dementia care, prognosis and treatment (Brijnath et al., 2022). Our findings echo this concern, with most review papers either not stating the racial and migrant status of their participants or, when they do, being skewed toward white populations. Further, research participants included in individual studies are often not representative of ethno-racially, culturally, linguistically and economically diverse populations. These gaps are highlighted by some of the included studies (Hebert & Scales, 2019; Hung et al., 2021; Keady et al., 2012). There is a need to expand studies not only to those with different intersectional identities (e.g. race, ethnicity, language, immigration status, religion, gender identity, sexual orientation, ability, age, socio-economic status etc.) but also to different countries to truly understand promising practices for context-based design.
The challenges in the recruitment of racialized and marginalized populations are likely a reflection of the systemic barriers these populations face. These systemic barriers also contribute to siloing of the discipline, due to the exclusion of certain voices and perspectives. Building partnership and trust with communities is important to reaching populations that have historically been excluded from dementia research (Brijnath et al., 2022). Yet the strategies for inclusion mentioned in some of the reviews do not address the issue of systemic injustices and barriers to access that continue to have a detrimental impact on the health of these populations.
Lack of Examination of Stigma, Ageism/Ableism, Governmentality and Human Rights
All reviews highlighted stigma as a key barrier, which was framed as happening at particular scales, typically between individuals or within community networks and social connections. Stigma was also used as rationale for the need for dementia related training (Hebert & Scales, 2019). However, stigma was rarely framed as influencing all scales and being a result of structural forces. Dominant structural ideologies regarding disability and mental capacity like ableism and ageism have led to the stigmatization of dementia, and the use of discriminatory practices that do not plan for or support the inclusion and participation of people living with dementia (Bogart & Dunn, 2019; Rabheru & Gillis, 2021). Ableism and ageism result in socio-spatial boundary setting between ‘normal’ people and those perceived as not in control of themselves (i.e., people living with dementia) (Dear et al., 1997).
The structural impact of ableism and ageism is evident in everyday practices – from city planners who do not consider the diverse abilities of people living with dementia when planning spaces and interactions, service providers who do not understand and accommodate the needs of people living with dementia, and individual community members who ignore or dismiss their neighbours living with dementia. Challenging stigma only on an individual level may lead to dementia-capable communities that use ‘friendliness’ as a rationale, assume vulnerability and incapacity and take a fundamentally patronizing approach. But critical perspectives call on us to see people living with dementia as full citizens and contributors of the places they live in, with the same human rights afforded to others (Biglieri, 2021; Lin, 2017).
The process of developing dementia-capable communities was mentioned in each of the reviews, but often at a surface level, or describing the types of methods used to engage people living with dementia in these community conversations. While citizenship can be enacted through public spaces and communities (also called social citizenship), citizenship should also be enacted through having one’s voice heard in the development of government policies and practices (Biglieri, 2021; Sonnicksen, 2016). Using public spaces to facilitate discussions between the systems (e.g., government, organizations, institutions, etc.) and community (including culture, society, people) is a powerful means to produce change (Habermas, 1981). Within the processes of creating dementia capable communities, this means shifting power from decision-making being a top-down approach (e.g., from government to the people), to an approach that actively engages people living with dementia, care partners, and community members in decision-making processes.
The importance of working with people living with dementia during every stage of the policy, planning and development processes was a dominant theme in our results and a key facilitator of dementia capable communities. The benefits of such a process would be multiple. First people living with dementia would explicitly share their needs and preferences to directly inform policies, planning, programs, business, and other services. Second, people involved in the planning process may learn and be influenced directly by the people living with dementia, which may break down stereotypes and stigma (Biglieri et al., 2021). This would likely have long-standing benefits, given that the built environment is actively shaped by perspectives of the planners, designers, policy-makers and politicians that plan them (Hamraie, 2013). Within the context of creating dementia capable communities, there is a need to overcome stigma as a fundamental step towards inclusive practices, planning and policy.
Despite the human-rights based underpinnings of the idea of dementia capable communities, reviews lacked a clear engagement with human rights principles and how they might be leveraged to impact policy change. Clear instruments such as the United Nations Convention on the Rights of Persons with Disabilities, which lay out the rights and protections for people living with dementia, are not critically engaged with in the reviews. Five out of nine reviews mentioned the ideas of human rights or a rights-based approach (Craig et al., 2024; Hebert & Scales, 2019; Keady et al., 2012; Li et al., 2021; Shannon et al., 2019) and, of these, only one explicitly mentioned the Convention (Shannon et al., 2019). Neither was there much analysis of other theoretical perspectives, such as a critical disability, which understands disability as relational, dependent on complex layers of interactions of a person’s abilities with people, environments, things (e.g., tech, devices, animals) and social, cultural, and political structures (Dear et al., 1997; Hall & Wilton, 2017). The absence of significant engagement with the tools and theoretical perspectives that could provide foundations to address the challenges faces by people living with dementia remains a major gap in the field of dementia research and dementia capable communities.
Concrete Engagement with Funding Particularities and Incentives is a Gap
The role of funding and incentives was mentioned in several reviews (Craig et al., 2024; Gan et al., 2022; Hebert & Scales, 2019; Keady et al., 2012; Lanthier-Labonté et al., 2024; Shannon et al., 2019). However, additional research is needed on best practices for funding models for dementia capable communities. Moreover, practical consideration of the material resources required to create and maintain dementia capable communities is lacking. This includes concrete understandings of the human resources and financial resources required. There is also a need for a concrete understanding of incentives that would allow for the development of dementia capable communities (Biglieri, 2018). The broader trends of austerity and fiscal restraint have a significant impact on the financial resources for care infrastructures in general (Dowling, 2022) and are rarely analysed when discussing dementia capable communities (Dowling, 2022; Lerven et al., nd; Linovski, 2024; Stokes et al., 2022). There is also a lack of consideration of how the normalization of austerity may shape the realm of possibility for policymakers and policy directions. Mentions of the pivotal role of care partners and the need to support them also did not consider the material factors, including a lack of care providers, diminishing services and increasing waitlists, that are shaped by policy decisions and funding that give rise to the caregiver experience. This lack of engagement with fiscal realities poses a risk to the outcomes and sustainability of dementia capable communities.
Critical Analysis of Public Policy and Political Conditions is Missing
Though several reviews mentioned the need to engage with policymakers and levels of governance such as municipalities (Craig et al., 2024; Gan et al., 2022; Hebert & Scales, 2019; Keady et al., 2012; Lanthier-Labonté et al., 2024; Shannon et al., 2019; Sturge et al., 2021b), there was a noticeable lack of consideration of how to engage with levels of government responsible for planning decisions and how this research might be effectively translated into concrete actions and policymaking. For instance, reviews discussing transportation for people living with dementia do not concretely lay out how to engage policy-makers and levels of government who are involved in transportation planning (Hebert & Scales, 2019; Lanthier-Labonté et al., 2024). While some reviews mentioned factors that create a safe and easily navigable environment (e.g., walkability, sufficient lighting, signage), policy changes that are needed to embed these factors in community design and planning were not mentioned (Gan et al., 2022; Hung et al., 2021; Keady et al., 2012). There is a need to be concrete in how engagement with and between public policy and political structures contributes to the creation of communities that are safe and easy to navigate for people living with dementia.
Evidence points to the role of political and policy decisions in diminishing the capacity to provide appropriate services for people living with dementia via actions such as inadequate funding, shifting priorities and focusing on individual rather than systemic approaches, and even fueling further inequities (Ward et al., 2018). The lack of unifying perspectives in the reviews we analysed may be addressed by centering political decision making and public policy as key pillars that shape the experiences of people living with dementia.
Limitations
Our study was limited in its scope to only include literature broadly focused on dementia capable communities. It excludes care environments, such as long-term care. The included reviews posited varying understandings of the concept of dementia capable communities (such as dementia friendly, dementia inclusive, etc.), neighbourhoods, community and environment. Our analysis grouped these terms for analytical simplicity, however this may have obscured the finer differences between these concepts.
Conclusion
Our analysis identified core approaches, structures and resources for dementia capable communities as identified in recent reviews, as well as gaps in our understanding. We leveraged the lens of critical disability theory and a human rights framework to examine these aspects and consider the structures and supports needed for sustainable dementia capable communities. Firstly, best practices for planning, programming, and design must be combined with engagement of the people living with dementia. The attitudes, practices and behaviors of people must also shift from seeing people living with dementia as individuals to feel sympathetic towards, to seeing them as valued members of society. However, lack of inclusion of racialized and marginalized populations in research studies and at participatory tables is a major gap that must be addressed. These is also a critical need to think across academic disciplines, levels of intervention, and levels of governance to clearly identify, connect, and address barriers to dementia capable communities and identify where systemic changes need to occur. Purposeful, interdisciplinary funding is necessary to address these gaps in knowledge and action. Without this shift to a systemic, structural approach, dementia care and the development of dementia capable communities will remain relegated to “ripples in a pond” (Swaffer, 2020).
Supplemental Material
Supplemental Material - Developing and Sustaining Dementia Capable Communities: An Analysis of the Current evidence
Supplemental Material for Developing and Sustaining Dementia Capable Communities: An Analysis of the Current evidence by Samantha Biglieri, Neha Ahmed, Sarah Main, Olivia Leslie Tupling, Roslyn Vijayakumar, Jennifer Boger, Christine Daum, Sherry Dupuis, Melissa Koch, Lili Liu, Kimberley Lopez, Jim Mann, Michelle Martin, Carrie McAiney, Huda Jamal Nasir, Nada Nasir, Bethany Pearce, Rachel Weldrick, Kathleen Vanderlinden, Laura Middleton in Dementia.
Supplemental Material
Supplemental Material - Developing and Sustaining Dementia Capable Communities: An Analysis of the Current evidence
Supplemental Material for Developing and Sustaining Dementia Capable Communities: An Analysis of the Current evidence by Samantha Biglieri, Neha Ahmed, Sarah Main, Olivia Leslie Tupling, Roslyn Vijayakumar, Jennifer Boger, Christine Daum, Sherry Dupuis, Melissa Koch, Lili Liu, Kimberley Lopez, Jim Mann, Michelle Martin, Carrie McAiney, Huda Jamal Nasir, Nada Nasir, Bethany Pearce, Rachel Weldrick, Kathleen Vanderlinden, Laura Middleton in Dementia.
Footnotes
ORCID iDs
Ethical Considerations
This article does not contain any studies with human or animal participants.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The study was funded through the Government of Canada’s New Frontiers in Research Fund (grant# NFRFE-2020-00612), through the three federal research funding agencies (CIHR, NSERC and SSHRC).
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
Notes
Author Biographies
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
