Abstract
Assistive technologies hold significant potential to enhance the quality of life for persons with dementia and their caregivers by addressing key concerns related to safety, independence, and social inclusion. Although ethical issues surrounding the design and use of assistive technologies have been explored in various studies, no comprehensive overview of reviews has been conducted to synthesize the existing evidence on these issues. This study aims to categorize the ethical issues associated with assistive technologies for persons with dementia and their caregivers using established ethical principles, while also examining factors shaping the ethical debate on their design and implementation. The study was conducted across nine databases and included reviews published in the past 20 years that substantially addressed ethical considerations. Data synthesis followed the framework synthesis approach developed by Carroll et al. (2011). Out of 509 identified records, 15 reviews focusing significantly on ethical issues were included in the analysis. Findings revealed key ethical issues, including maintaining autonomy, respecting privacy, and addressing equity and accessibility. While assistive technologies demonstrate potential in enhancing safety and independence, concerns about surveillance, depersonalization, and stigmatization persist. The ethical debate is shaped by contextual, philosophical, temporal, and geographical factors, including varying stakeholder priorities, the fluctuating nature of dementia symptoms, diverse approaches to dementia care and ethics, cultural differences, and the implications of future technological advancements. This review underscores the complexity of ethical issues related to assistive technologies for dementia care and how these identified factors inform the ethical design and their use for persons with dementia and their caregivers.
Introduction
In 2019, an estimated 55 million people worldwide were living with dementia, a number expected to rise to 78 million by 2030 and 139 million by 2050 (Nichols et al., 2022). As there is currently no cure, efforts focus on improving the quality of life for individuals with dementia and their caregivers, as well as reducing associated disability (WHO, 2021). Assistive technology (AT) has emerged as a potential solution to support individuals with dementia by enhancing their functional abilities (Pappadà et al., 2021). AT in dementia care includes specialized devices tailored for dementia patients, such as monitoring systems and smart-home applications, as well as mainstream technologies like smoke alarms and voice recognition tools (Lorenz et al., 2019; Van der Roest et al., 2017). These technologies can function as standalone tools—such as medical reminders and locator devices—or as part of integrated safety systems, including automated lighting and fall detectors (Gagnon-Roy et al., 2017). AT also encompasses telephones, video-calling apps, social robots, and Internet of Things (IoT) devices that enable seamless communication between appliances (Ienca et al., 2017; Van der Roest et al., 2017). AT offers significant potential to enhance safety, independence, and overall well-being for people living with dementia.
Ethical issues in the use of AT for dementia care have been a central theme in academic literature and clinical practice, emphasizing the importance of a humanistic approach in their design and implementation (Wolff et al., 2021). Moreover, new technologies can also have ethical implications which may be overlooked, especially considering the rapid rate of such advancements in society. The ethical issues most prominently discussed in the literature and policy documents relate to respecting autonomy, obtaining consent, upholding privacy and dignity whilst maintaining safety considerations (Alzheimer Europe, 2010; Robillard et al., 2019). Additionally, AT for leisure and social inclusion, such as multimedia devices and socially assistive robotics (SAR), have been argued to enhance interaction but may also compromise dignity if perceived as infantilizing. Similarly, tracking and tagging devices have been considered to offer autonomy but have also been criticised for violating privacy and creating power imbalances (Alzheimer Europe, 2010). These ethical considerations have also been implicated for the slow uptake of such technologies in dementia care (Jotterand et al., 2019; Mahoney, 2011).
Although numerous reviews have condensed studies focusing on the ethical issues of AT use (Noviztky et al., 2015), they have never been summarised to provide a comprehensive perspective of the ethical issues associated with AT in dementia. Moreover, there is a need for further clarity on these ethical issues and what influences the ethical debate of AT use in dementia care. Consequently, this overview of reviews sought to reach the following objectives: - To describe ethical issues as obtained from the selected reviews and suggest possible recommendations on how to overcome them. - To identify the factors shaping the ethical debate of AT design and use for persons with dementia and their caregivers.
Methods
The review protocol was registered in PROSPERO (CRD42023482212), ensuring transparency and alignment with best practices (Tawfik et al., 2020). The PRIOR (Preferred Reporting Item for Overview of Reviews) statement, developed specifically for overview of reviews of healthcare interventions (Gates et al., 2022), was used to structure the general aspects of the review, including the definition of methodology, search strategy, and inclusion criteria (Appendix 1). While the PRIOR guideline provides a robust framework for healthcare interventions, it does not address the synthesis of ethical literature. To address this gap, the guiding questions proposed by Mertz et al. (2016) were adopted. These questions focused on the ethical approaches for identifying and extracting normative information units, as well as the methods used for synthesizing such information and provided a systematic and robust foundation for handling ethical dimensions in this review. This combined approach ensured methodological rigor while addressing the specific ethical focus of the study.
Eligibility criteria
The following eligibility criteria were considered: - Timeframe: Reviews published between 2004 and 2024 to capture the evolution of modern assistive technologies (ATs) in dementia care, influenced by advancements in AI, IoT, robotics, and connected devices (Novitzky et al., 2015). - Population: Individuals with minor or major neurocognitive disorders (Mild Cognitive Impairment or dementia) diagnosed using DSM-IV/DSM-5 or ICD-10/11 criteria. Family caregivers or professional caregivers (e.g., healthcare professionals) involved in dementia care. - Reviews that included studies on AT devices such as: • Monitoring technologies (e.g., fall detectors, environmental sensors). • Tracking and tagging systems (e.g., GPS, area-based alerts). • Smart home technologies (e.g., integrated daily activity systems). • Health and cognitive support devices (e.g., smart pillboxes, task reminders). • Robots and AI (e.g., social and task-assisting robots). • Communication technologies (e.g., telehealth, video calling). - Language: No language restrictions were applied. - Review Types: Included scoping, systematic, narrative, and ethical reviews, providing a systematic search strategy was used to select primary articles, and which included a substantial focus on ethical issues.
Search strategy
Searches were conducted across major databases, including AgeLine, Cochrane Database of Systematic Reviews, PsychoINFO and CINAHL Complete (all via EBSCOhost), PubMed, IEEE Xplore, ACM Digital Library (Association for Computing Machinery), Web of Science, and Scopus, between November and December 2024. To ensure transparency and replicability, the search strategy followed the structured guidance provided by the PRIOR statement (Gates et al., 2022). The search terms were carefully designed to incorporate combinations of keywords related to assistive technologies, ethics, dementia, and caregiving. The following Boolean query was used and tweaked according to the limiters of the respective databases using the following keywords: (Ethics OR ethical considerations OR ethical implications OR ethical issues OR moral OR values OR ethical analysis OR ethical evaluation OR ethical framework OR ethical guidelines OR ethical challenges OR bioethics OR professional ethics) AND (Assistive technologies OR assistive devices OR adaptive technologies OR adaptive devices OR technology ethics OR technology design OR user acceptance OR user privacy OR user autonomy) AND (Dementia OR Alzheimer Disease OR cognitive impairment OR memory loss OR MCI) AND (reviews OR systematic OR literature)
To supplement the database searches, manual reference list searches of included reviews were performed to identify additional relevant studies. The search process and inclusion criteria were pre-defined and documented in the PROSPERO-registered protocol (CRD42023482212). While the PRIOR statement was the primary framework guiding the search methodology, adaptations were made to address the specific focus on ethical literature, ensuring a systematic and transparent approach tailored to the unique requirements of this review.
Study selection
Searches across the selected databases were compiled into the Rayyan Intelligent Systematic Review tool, for initial screening and management. Before proceeding with the screening, duplicate records were identified and removed within the Rayyan platform. The first screening was conducted independently by six authors working in pairs, with each pair classifying the reviews as “included,” “maybe,” or “excluded” based on predefined eligibility criteria. For reviews classified as “maybe” or where discrepancies arose between pairs, a second screening was performed by two independent reviewers. Disagreements during this second stage were resolved by involving a third reviewer. This three-stage process was designed to uphold methodological rigor while balancing efficiency and fostering consensus. In alignment with the PRIOR statement (Gates et al., 2022), the study selection was transparently documented using the PRIOR flow diagram (in relation to preferred reporting items for overviews of reviews), ensuring clarity and replicability.
Quality assessment
Two reviewers independently assessed the methodological quality of the selected reviews using a checklist adapted from the RESERVE guidelines (Kahrass et al., 2023). Since existing tools like the PRIOR statement (Gates et al., 2022) focus on healthcare interventions and overlook the unique challenges of ethical reviews, the authors developed a customized checklist (Appendix 2). Based on RESERVE’s 22 items, the checklist was refined into concise, targeted questions with response options: “Yes,” “No,” or “Partially Yes.” This approach enhanced the transparency and comprehensiveness of ethical reviews. Discrepancies between reviewers were resolved through discussion or third-party consultation, ensuring consistency and reliability. The adapted framework provides a more tailored solution for evaluating ethical reviews while maintaining methodological rigour.
Data extraction and synthesis
Ethical principles with description used to categorise ethical issues.
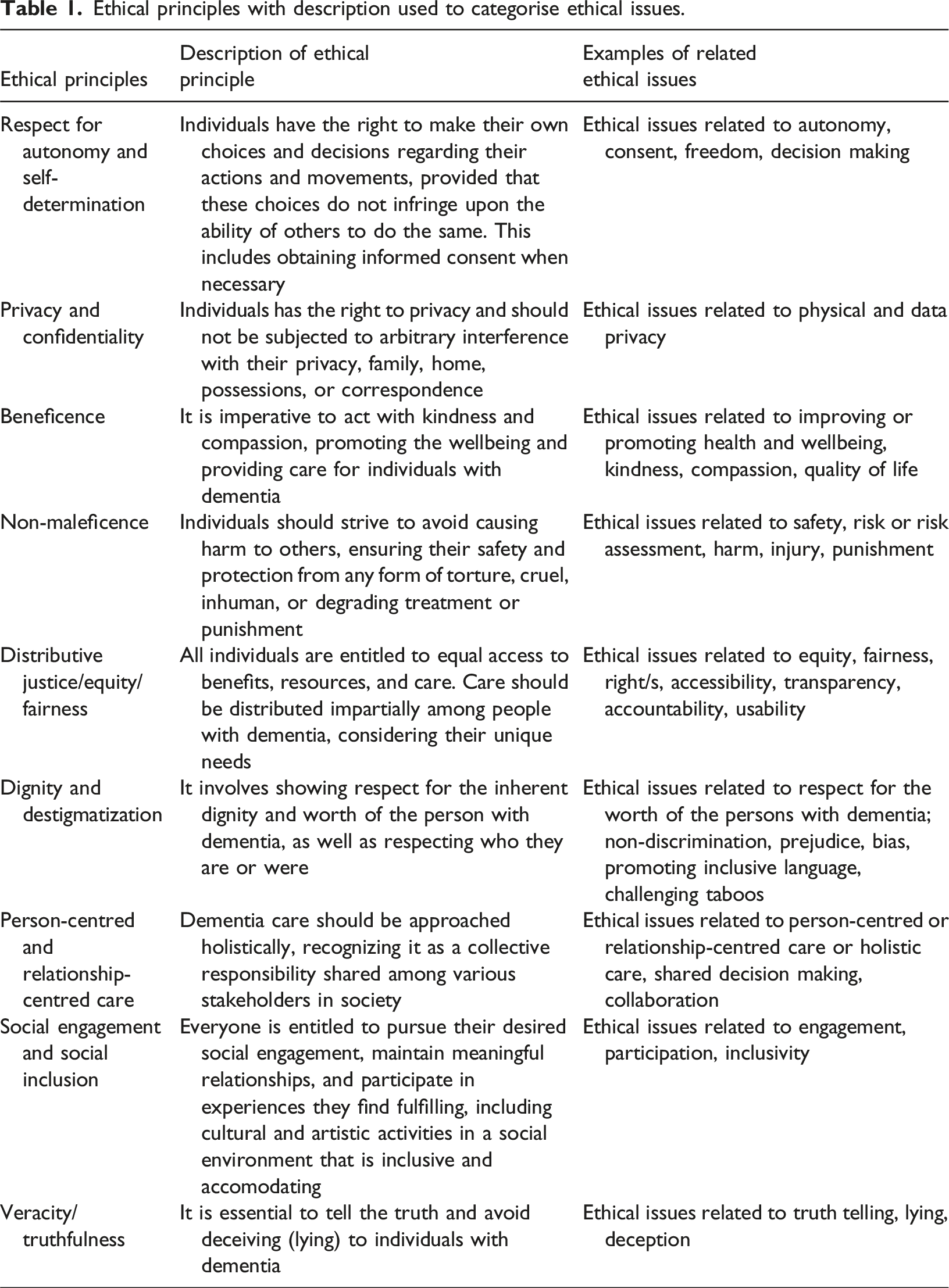
To address emerging themes focusing on factors shaping the ethical debate, the authors employed thematic analysis using an inductive and interpretive approach. Two reviewers cross-verified the categorization and coding of data to ensure accuracy and reliability. Discrepancies were discussed, and alternative categorizations were considered critically. The framework synthesis allowed for both deductive categorization of ethical issues and the inductive identification of emerging themes that did not fit within the predefined framework.
Quality appraisal
Quality appraisal of the selected reviews [Y: Yes; N: No; PY: Partially Yes].
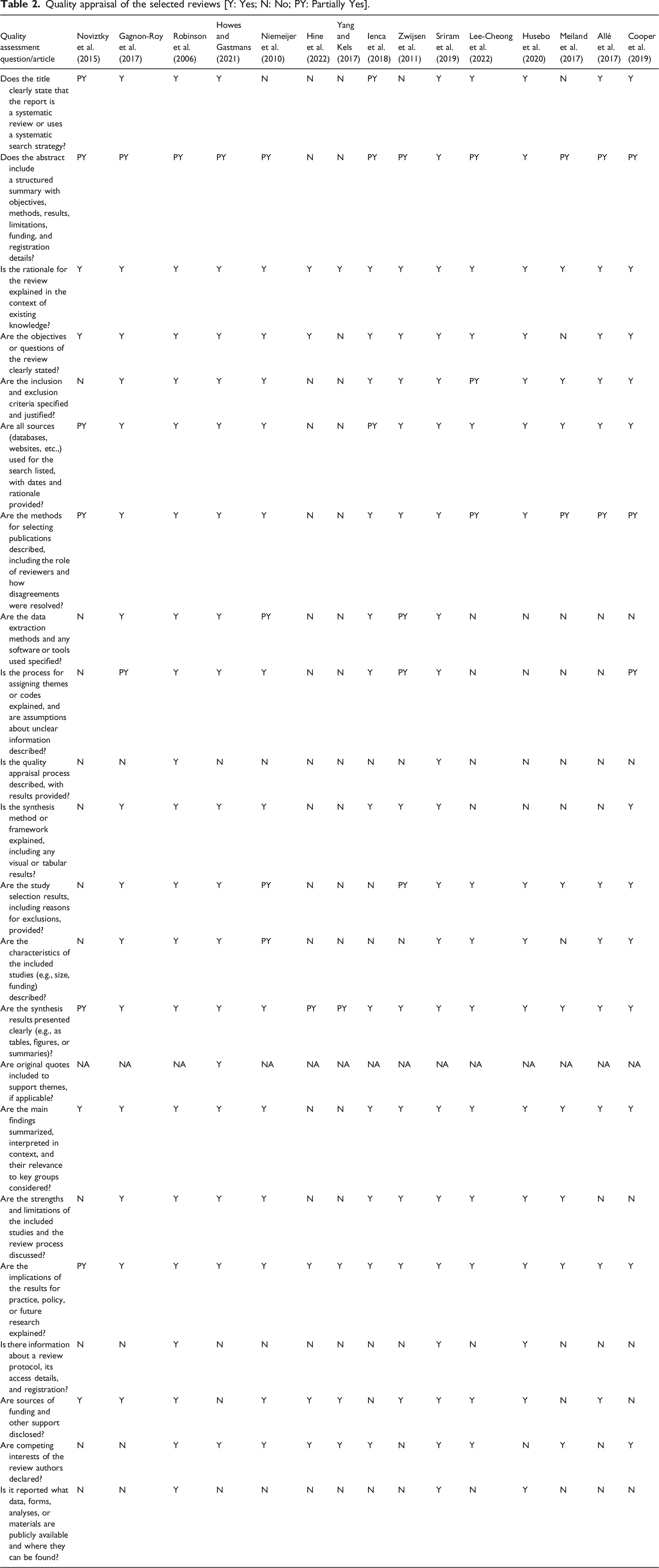
Findings
Search trail
Five hundred and nine records from database searches were initially identified. After removing 123 duplicate records, 386 unique records were screened for relevance. Of these, 353 records were excluded based on the eligibility criteria during the first screening after six authors read the abstracts of these reviews. The full text of 33 potentially relevant reviews were retrieved for further screening. Eight reviews were included although there was still debate on the remaining 25 articles. A second screening was performed independently by two authors (AS, AG) and a third author (CBX) decided on the articles when there was no agreement. Ultimately, 15 reviews met the eligibility criteria and were included in this overview of reviews. Figure 1 shows the PRISMA flowchart. The PRISMA flowchart.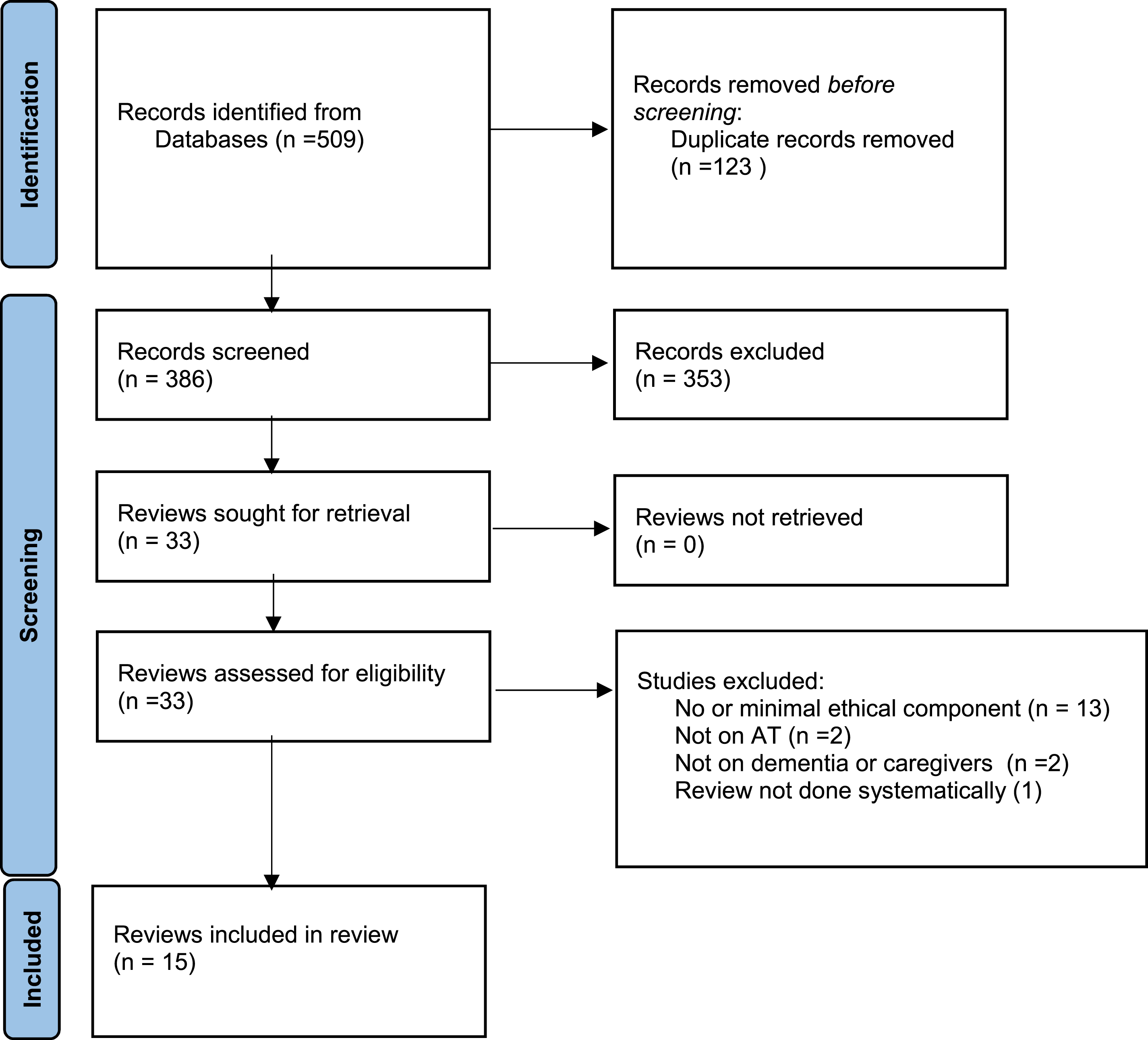
Characteristics of the selected reviews
Characteristics of the selected reviews.
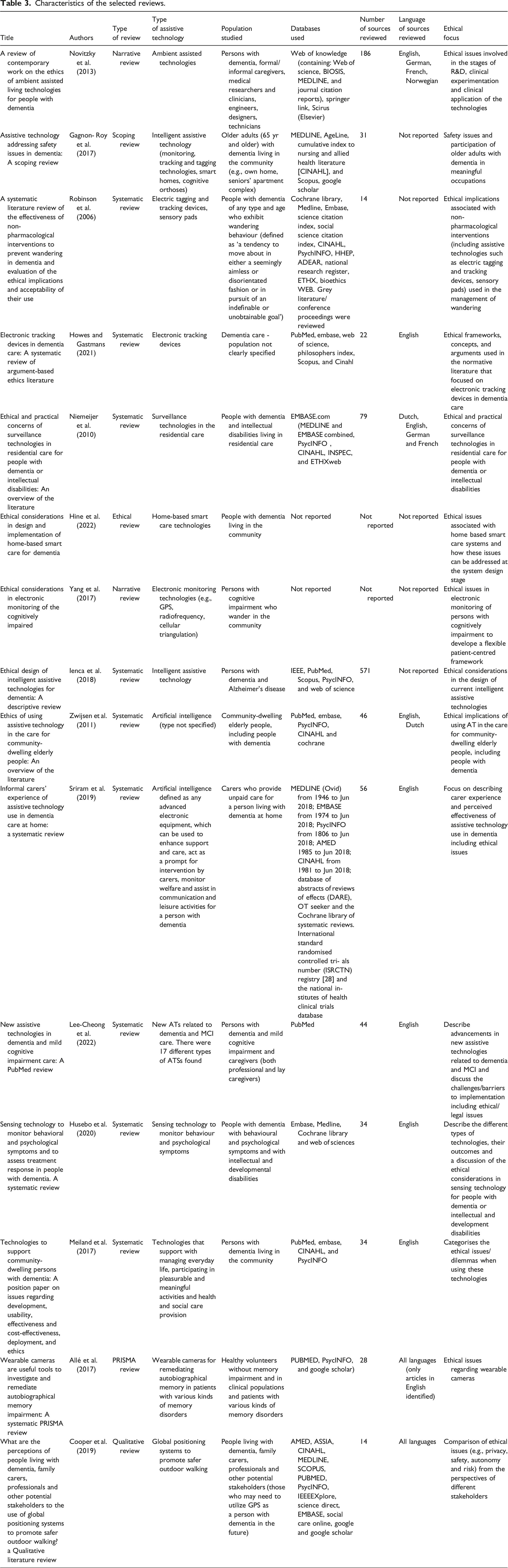
Ethical issues based on predefined ethical principles
Ethical issues categorised according to ethical principles and possible recommendations to overcome them.

Respect for autonomy and self-determination
Respect for autonomy means recognizing and upholding individuals’ right to make one’s own choices and decisions and obtaining informed consent when necessary. Respect for autonomy and self-determination has been highlighted by almost all selected reviews, particularly the challenges of balancing autonomy with safety. There seems to be some debate about whether AT increases or decreases autonomy, for example whilst tracking devices may facilitate the person’s ability to independently leave the house, this may be restricted by the family caregiver if geo-fencing is applied. A significant challenge was to obtain informed consent in view of the challenges that persons with dementia may have to understand the potential consequences of both using or not using electronic tagging and other electronic monitoring devices (Gagnon-Roy et al., 2017). This is more challenging in view of the fluctuating cognitive abilities of persons with dementia (Yang et al., 2017). Consequently, a rolling consent has been proposed (Novitzky et al., 2015) that continuously assesses the choices made by the person with dementia. Alternatively, Husebo et al. (2020) identified studies that proposed advance directives, earlier wishes and discussion of AT use at an early stage of the dementia progression. Other possible solutions found in these reviews were personalizing AT, involving stakeholders and including the person with dementia during the design phase (Hine et al., 2022; Ienca et al., 2018).
Privacy and confidentiality
Privacy refers to the right not to be subjected to arbitrary interference and exert control over one’s lives, whilst confidentiality refers to the obligation to safeguard one’s personal information entrusted to others. Reviews on assistive technology (AT) use identify two key privacy concerns: physical privacy and data privacy (Howes & Gastmans, 2021). The terms ‘intrusiveness’, ‘pervasiveness’, and ‘obtrusiveness’ are commonly used to describe how ambient assistive living (AAL) devices impact physical privacy (Husebo et al., 2020; Ienca et al., 2017). However, Zwijsen et al. (2011) argued that these terms, mainly used by AT designers, can obscure ethical concepts of privacy and confidentiality. The extent to which monitoring devices infringe on privacy is debated, especially compared to alternatives such as continuous caregiver observation or physical restraints, which may be more intrusive (Husebo et al., 2020; Robinson et al., 2006).
Regarding data privacy, ethical concerns focus on data ownership, access, and security, raising questions about how personal and medical information is managed (Novitzky et al., 2015). Suggested strategies include encryption, restricted data access, and ensuring data collection aligns with intended purposes (Hine et al., 2022). Additionally, privacy considerations extend to caregivers and other residents who may not have consented to data collection, such as through wearable cameras. Ethical guidelines recommend notifying third parties and granting them the right to stop or delete data capture (Allé et al., 2017).
Non-maleficence
Since the Hippocratic Oath, the ethical principle of non-maleficence or ‘not doing harm’, has exemplified the fundamental principles of modern medicine (Askitopoulou, 2018). Assistive technologies like ambient assistive living and electronic tracking devices have been proposed as to reduce harm, injuries and relieve anxieties. However, numerous authors of these reviews have argued that the ‘medicalisation of the home environment’ (Novitzky et al., 2015) could result in over-dependence or a false sense of security (Robinson et al., 2006); which in turn could lead to an increase in at-risk behaviours (Gagnon-Roy et al., 2017). However, Howes & Gastmans (2017) argued that measuring risk is hard and subjective, thereby requiring a compromise between stakeholders like persons with dementia, caregivers and healthcare professionals of weighing all risks with the benefits. Moreover, there could also be direct harm caused by device malfunctions or false alarms. This could be avoided through rigorous safety testing at the design stage (Novitzky et al., 2015). Finally, some reviews highlighted the fact that the studies they have reviewed, seem to prioritise the benefit of tracking devices and ambient assisted living technologies in reducing physical harm over the ‘social harm’ that they could potentially cause, due to depersonalization and objectification (Howes & Gastmans, 2017; Novitzky et al., 2015).
Beneficence
According to Childress (2013), the principle of beneficence refers to the moral obligation of the other’s best interests and benefits. However, there is still debate whether AT primarily benefits individuals with dementia or their caregivers (Hofmann, 2013 in Novitzky et al., 2015). Whilst it may be argued that what benefits persons with dementia will eventually benefit family caregivers and vice versa (Howes & Gastmans, 2017), it very much depends on whether they have the same vested interests, what constitutes a positive outcome (benefit) and how it is measured. For example, Brims and Oliver (2017) found that whilst AT improves safety in persons with dementia living at home, it does not reduce care home admission. Furthermore, the benefits of home-based assistive technologies and telecare technologies are still inconclusive in improving the persons with dementia’s quality of life (Lauriks et al., 2020) and/or reducing caregiver burden (Davies et al., 2020). With regards to new AT in dementia and MCI such as ‘smart phones’ and ‘smart home systems’, and ‘artificial intelligence’ (AI), Lee-Cheong et al. (2022) argued that when efficacy studies have been done to test the benefits of these technologies, these consisted of studies with small sample size, few data points and poor heterogeneity of the participants. Consequently, larger-scale trials are needed to test the efficacy of these AT devices (Allé et al., 2017).
Distributive justice, equity and fairness
Within the context of dementia care, this set of principles affirms that all individuals are entitled to equal access to benefits, resources, and care and that the latter should be distributed impartially among people with dementia whilst considering their unique needs. Whilst there has been interest in these principles, especially in accessing dementia care services and resources (Kerpershoek et al., 2020), these are less frequently discussed in the selected reviews when compared to other principles. However, the reviews highlight concerns about the digital divide exacerbating inequalities, particularly for economically disadvantaged populations, rural or remote communities with limited internet access, and individuals unfamiliar with technology (Novitzky et al., 2015). Despite the state’s obligation under the United Nations Convention on the Rights of Persons with Disabilities to provide affordable technologies, significant barriers to equitable access remain (Howes and Gastmans, 2017). Many home-based assistive technologies are not classified as medical devices in numerous countries, requiring out-of-pocket purchases by persons with dementia and their caregivers. Additionally, the design phase of smart care devices often lacks data representation from diverse populations, necessitating cultural retesting to ensure applicability across different settings (Hine et al., 2022).
Proposed solutions to enhance access and align with distributive justice include making AT devices affordable through low-cost and open-source hardware and software, enabling reproduction without copyright restrictions (Ilenca et al., 2018). Alternatively, personalizing devices by allowing users to purchase specific hardware or download tailored software can help reduce costs. These approaches aim to ensure AT systems are accessible, culturally adaptable, and equitable for all populations.
Dignity and de-stigmatization
In dementia care, the concept of dignity has been operationalised as ‘the promotion of worthiness and the accordance of respect that allows the presence and expression of a person’s sense of self, regardless of physical, mental, or cognitive health.’ (Zhang et al., 2024, p. 1220). Most reviews refer to ethical issues associated with maintaining dignity and avoiding stigmatisation when using electronic tagging. Although electronic tagging devices may reduce potentially compromising situations in some circumstances (e.g., being lost or half dressed), they may increase the stigma because of the negative connotations, since such devices as associated with criminal justice, animals, frailty and dependency (Robinson et al., 2006; Zwijsen et al., 2011). Moreover, if such devices become more commonly used in dementia care, they can be seen as a way of ‘labelling’ persons with dementia, further perpetrating the associated stigma (Cooper et al., 2021; Howes & Gastmans, 2021). This could also occur if sensitive information, such as a dementia diagnosis, is disclosed due to a data breach involving ambient assisted living technologies (Novitzky et al., 2015). To overcome this stigma associated with electronic tagging devices, there has been discussion in the literature of reframing the language used when referring to such devices, from the term ‘tracking’ to ‘locator’. However, a change in terminologies needs to be accompanied by developing AT designs that reduce their visibility, size and weight and make them aesthetically pleasing (Novitzky et al., 2015; Zwijsen et al., 2011).
Person-centred and relationship-centred care
Although person-centred dementia care, such as the VIPS framework (Brooker, 2003), has been conceptualised for some time now, the ethical challenges of maintaining person-centred and relationship-centered dementia care when using AT have not been comprehensively discussed in the selected reviews, possibly because to date, ethical debates on AT use in dementia, have be informed by Principlism, rather than Care Ethics approaches (Howes & Gastmans, 2021). AT can significantly influence care relationships and care giving roles. For example, automated diagnosis through AT may influence the clinician-patient relationship by eroding the patient’s trust and their perception of clinician responsibility, accountability and perceived competencies. Moreover, in care homes AT, such as monitoring devices, may lead to a reduction in staffing levels to save staffing costs, leading to further depersonalisation and reduction in the quality of care (Niemeier et al., 2010; Robinson et al., 2006). In the community, AT may create virtual long-distance care relations instead of a personal and compassionate care relationship between persons with dementia and family members leading to further social isolation (Zwijsen et al., 2011). Hine et al. (2022) points out that home-based smart devices should be designed to support not replace human judgement. Similarly, surveillance technologies in residential care should support but not replace human contact or care (Zwijsen et al., 2011). Moreover, social robots in the person with dementia’s own home, could replace the only human companionship, such as those supported by current community care services (Novitzky et al., 2015). A user-centred design of AT and models that encourages shared decision-making during their use along the disease trajectory, could ensure that these devices are truly person and relationship-centred (Yang et al., 2017).
Social inclusion
Pinkert et al. (2019), argued that the principle of social inclusion in the context of dementia is hard to define and conceptualise. This could be a reason why there is still debate about whether AT in dementia enhances or reduces social inclusion (Novitzky et al., 2015). For example, whilst devices like video calls can facilitate connections with others including healthcare professionals (Zwijsen et al., 2011), they do not necessarily address feelings of loneliness or improve social relationships (Novitzky et al., 2015). As discussed above, the benefits of AT should not replace the need for human contact and companionship.
Veracity and truthfulness
Truth telling in dementia care has been debated for many years, and there is still no consensus in which circumstances is therapeutic lying acceptable (Casey et al., 2020). However, genuineness and keeping the best interests of individuals with dementia as the motivation behind lying, is considered as an effective intervention and is more likely to result in a positive outcome (Murray et al., 2025). In the context of AT use, there seems to be few ethical issues debating this principle in the selected reviews (Yang et al., 2017). In some cases, caregivers may use persuasive techniques or even covertly conceal devices, such as hiding GPS trackers in personal belongings, to ensure the technology is used. These practices can undermine trust and diminish the person’s right to autonomy. Moreover, substituting human emotions or relationships with AT, for example when using social robots, raise questions about whether these technologies subtly involve a form of deception (Novitzky et al., 2015).
Factors shaping the ethical debate of AT design and use for persons with dementia
Based on the inductive approach utilised, the following six emerging themes were identified that shape the ethical debate of AT design and use - different priorities of various stakeholders, different approaches/models in dementia care, different interpretations of the ethical principles, technological advances in AT and innovative applications, variability of the dementia symptoms and cultural and regional variability (Figure 2). Each of these themes will be discussed in turn. Conceptual framework incorporating the deductive and inductive themes obtained from the selected studies.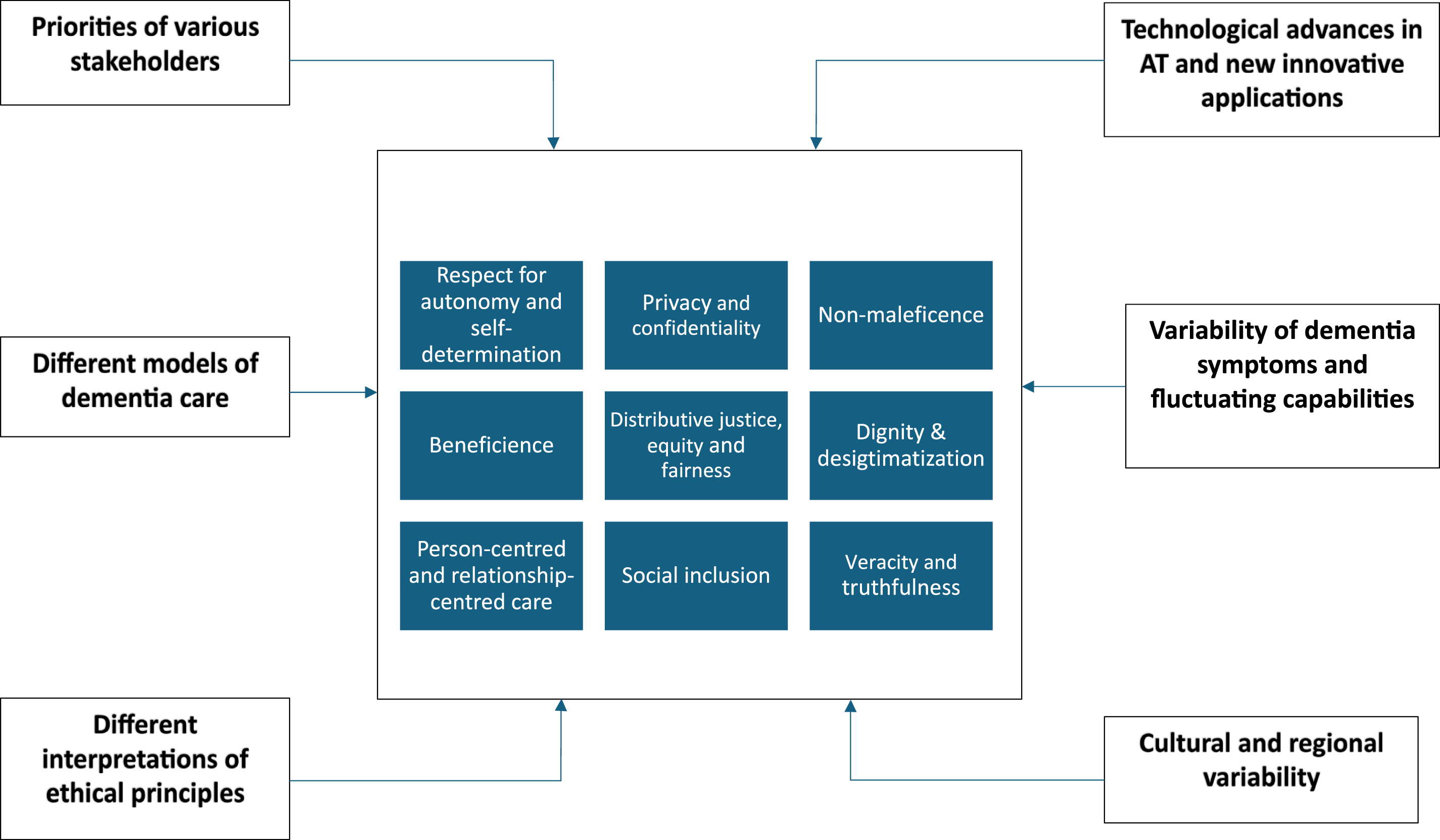
Different priorities of various stakeholders
Reviews highlighted challenges in balancing the perspectives of stakeholders, including persons with dementia, family caregivers, and professional caregivers (Robinson et al., 2006, 2007). Persons with dementia value involvement in decision-making and prefer early discussions about assistive technology (AT) adoption while cognitive abilities allow for informed consent (Ienca et al., 2018). They generally accept monitoring by family members but resist privacy intrusions by institutions or the state (Zwijsen et al., 2011). Many perceive AT as a trade-off, tolerating privacy concerns to maintain independence and avoid institutionalization. However, most reviews focused on older adults or those with mild cognitive impairment, with limited exploration of the perspectives of persons with advanced dementia on specific technologies, such as GPS for safe outdoor walking (Cooper et al., 2019). Professional caregivers often prioritize safety over autonomy and privacy (Sriram et al., 2019), justifying decisions based on the need to protect persons with dementia. Neimeijer et al. (2010) and Topo (2009) noted that the ethical debate has been dominated by caregivers’ perspectives, prioritizing safety and caregiver well being over other ethical concerns. More recent evidence (e.g., Cooper et al., 2019) indicates that the voices of persons with dementia remain underrepresented in AT design and ethical discussions, emphasizing the need for greater inclusion.
Different approaches/models in dementia care
Cooper et al. (2019) highlighted how a shift toward rights-based and disability models in dementia care has influenced the ethical debate surrounding assistive technologies (AT). Traditional approaches, rooted in medicalized and risk-management models, focused on reducing caregiver burden by managing behaviours. Early studies on GPS devices, for example, prioritized the perspectives of caregivers and professionals, often undermining autonomy and reinforcing dependency narratives (Cooper et al., 2019). In contrast, newer psycho-social and citizenship models emphasize the rights and agency of individuals with dementia. These frameworks advocate viewing persons with dementia as active participants in their care, capable of making decisions and using technology to maintain independence (Howes & Gastmans, 2021). They stress the importance of involving persons with dementia in AT design and evaluation, promoting mobility, social inclusion, and self-determination. For instance, ethical issues surrounding electronic tagging are being shaped by viewing dementia as a subset of aging or disability (Howes & Gastmans, 2021). Despite progress, tensions persist between risk management and empowerment. Many applications such as electronic tagging devices continue to be imposed by caregivers, perpetuating paternalistic dynamics that undermine autonomy. A genuine rights-based approach requires a cultural and systemic shift, framing AT as a tool for empowerment rather than control (Cooper et al., 2019).
Different interpretations of the ethical principles
New ethical approaches are also contributing to the debate on the use of AT in dementia care, for example by shifting from the traditional ethical principle of autonomy to more inclusive perspectives. Traditional liberal autonomy, rooted in independence and self-determination, often fails to capture the realities of people with dementia (PWDs), whose autonomy is deeply shaped by relationships, vulnerability, and dependency (Howes & Gastmans, 2021). Consequently, newer frameworks like relational autonomy and identity autonomy have emerged, offering richer conceptions that align more closely with the lived experiences of PWDs (Agich, 2003; Nordgren, 2018). Relational autonomy recognizes that autonomy is not exercised in isolation but within the context of relationships and social support networks (Klein, 2022). It emphasizes the importance of meaningful interactions and the role of caregivers and their loved ones in enabling them to express their preferences and make decisions. This approach shifts the ethical debate from solely safeguarding independence to fostering environments where relationships can support autonomy despite cognitive decline. Similarly, identity autonomy focuses on maintaining a person’s sense of self, even amidst dependencies and vulnerabilities. It moves beyond independence as a marker of autonomy, proposing that decisions reflect a person’s values, identity, and sense of self, even when they rely on others for care. These ethical approaches highlight the importance of recognizing and respecting their evolving preferences and needs (Nordgren, 2018).
Technological advances in AT and new innovative applications
Advancements in assistive technology (AT) such as artificial intelligence (AI), ambient-assisted living (AAL) systems, and the Internet of Things (IoT) are reshaping the ethical landscape in dementia care, presenting both opportunities and challenges. AI-driven systems enable real-time analysis of behavior and cognition, offering novel insights into care. However, reliance on algorithms raises concerns about accountability, biases in data interpretation, and the potential dehumanization of care. AI’s limitations in understanding human emotions necessitate human oversight, prompting ethical questions about balancing technology with human input (Lee-Cheong et al., 2022). As technology becomes more affordable, AT may achieve wider adoption (Lee-Cheong et al., 2022). However, collective implementation of AAL systems in nursing homes risks fostering surveillance cultures and undermining individuality, with debates over the feasibility of an opt-out policy persisting (Novitzky et al., 2015). Moreover, large-scale use of these technologies may exacerbate socio-economic disparities, further marginalizing vulnerable populations. Ethical considerations need to be proactive, addressing potential challenges during the design stage of AT products rather than after deployment (Ienca et al., 2018). Similarly, Howes and Gastmans (2018) emphasize that many ethical issues related to electronic tagging devices should be resolved during AT development.
Variability of the dementia symptoms and fluctuating capabilities
Dementia is characterized by progressive cognitive decline, yet individuals often experience fluctuating decision-making capacity, particularly in the earlier stages of the condition. A central challenge is the temporal nature of cognitive abilities. While individuals with mild or early-stage dementia can often consent to AT use, those in moderate or severe stages may lack the capacity to make such decisions consistently (Hine et al., 2022; Zwujsen et al., 2011). This also highlights the importance of timing the introduction of such devices (Sriram et al., 2019). Moreover, many devices are designed for individuals with early-stage dementia, leaving those in advanced stages without suitable support. Future technologies must accommodate increasing needs and diminishing cognitive abilities, ensuring that AT evolves alongside the individual (Lee-Cheong et al., 2022).
Cultural and regional variability
Cultural and regional factors can shape the ethical debate in various ways for example by shaping attitudes, priorities, and legal frameworks. Differences in cultural norms and healthcare systems can lead to varied perspectives on autonomy, privacy, and the integration of technology in caregiving. For example, Niemeijer et al. (2010) refers to literature which showed that in the U.S., there is a general cultural readiness to embrace technological solutions to complex issues, sometimes at the expense of deeper ethical issues such as privacy. Contrary, in the U.K. and parts of Europe, the adoption of AT is accompanied by more ethical scrutiny.
Legal frameworks also vary across regions, impacting how AT is implemented and debated. For example, the European General Data Protection Regulation (GDPR) includes provisions to protect individuals with dementia from being coerced into providing consent, but interpretations differ by country. In Norway, a family member or legal advocate can consent on behalf of a person with dementia, while Germany limits participation in research to those likely to benefit directly from the outcomes (Husebo et al., 2019). Moreover, cultural differences in technology adoption and familiarity can create barriers, particularly for older adults with dementia who are unaccustomed to devices like smartphones and tablets. Moreover, cultural sensitivity should be introduced at the design stage to ensure that these technologies are culturally relevant for different populations (Lee-Cheong et al., 2022).
Discussion
This overview of reviews sought to comprehensively describe ethical issues associated with AT for persons with dementia according to predefined principles and identify the factors shaping the ethical debate on AT design and use. The findings from these reviews indicate that of all the ethical principles, respecting autonomy and self-determination seems to be the most debated ethical issues due to challenges in obtaining informed consent from individuals with fluctuating cognitive capacities. Hegde et al. (2016) argued that even persons with severe dementia may retain partial capacity. Consequently, when evaluating the use of AT, clinicians need to balance respect for autonomy with acting in the patient’s best interest.
Privacy issues have also been identified as an ethical concern, as AT devices such as surveillance and tagging devices, often collect sensitive data, raising debate about ownership, access, and confidentiality, particularly when involving other stakeholders like caregivers or co-residents. Recommendations to address these issues include encryption, limiting data access, and non-intrusive designs. For example, Fang et al. (2021) used passive infrared (PIR) sensors rather than cameras or wearable devices that discreetly monitors movement patterns and detects anomalies without requiring constant surveillance, preserving the dignity and independence of older persons living at home. Moreover, they encrypted and stored the data in a blockchain system to maintain data privacy.
With regards to the principle of beneficence and non-maleficence, there is still lack of robust evidence regarding AT’s effectiveness and benefits in improving outcomes such as safety, independence, and well-being of persons with dementia and their caregivers at their own home (Lauriks et al., 2020). Moreover, the reviews selected pose questions on whether electronic tagging devices benefit primarily individuals with dementia or caregivers (Howes & Gastmans, 2017). Non-maleficence concerns as identified in these reviews, highlight the risks of AT, including malfunctions, alarm fatigue, social isolation, and depersonalization. Justice and equity issues focus on accessibility and affordability, particularly in rural or low-income areas. Whilst not discussed extensively in these reviews, maintaining dignity is also debated, as AT, especially electronic tagging devices, can reinforce stereotypes of dependency and frailty. Also, while the notion of dignity and stigmatisation are logically distinct, these two principles are generally discussed together. This review identified contextual, philosophical, temporal and geographical factors that shape the ethical debate in AT use, including different stakeholders’ priorities, fluctuating dementia symptoms, different approaches to dementia care and ethics, cultural differences, and future technological advancements. Figure 2 summarises these findings in a conceptual framework that incorporates the ethical principles with inductive themes obtained from the selected studies.
Whilst the use of AT technologies, for example remote monitoring/consultations and social robots, have been fast-tracked during the Covid-19 pandemic (Barbosa, 2024), there are considerable challenges to the development and utilisation of these innovations (Meiland et al., 2017; Moyle, 2019). One of the reasons for the lack of uptake of such innovations could be attributed to the ethical issues such the fear persons with dementia may have of losing one’s autonomy or privacy or unequal and unjust availability of these innovations. However, most of the current literature on AT use in dementia care does not seem to give much importance to these ethical issues. In fact, when compared to the significant number of reviews retrieved related to AT in dementia, only 15 reviews have been identified that substantially discuss these issues and most of them do not so exclusively, with most of these reviews discussing them in combination with other outcome measures such as user acceptance or effectiveness. Moreover, there seems to be a dearth of literature on the ethical issues related to the use of AT in persons with dementia residing in nursing homes with only one review identified.
The findings of this review indicated that while non-maleficence is somewhat more prevalent or explicitly articulated in the selected reviews, the principle of beneficence is implicitly embedded within many of the other ethical principles. AT in dementia, can be used to create opportunities for positive experiences, personal growth, and improving quality of life rather than solely being considered as a measure to reduce harm. Moreover, this review has highlighted a move towards a more positive and human rights approach to dementia care. Similarly, an Alzheimer Europe (2010) report, recommended that when taking ethical decisions in the use of AT it is important to reframe dementia as a disability. This can be done by integrating their views and developing user-centred devices, during the design and the implementation phase, that can more holistically address the needs of individuals with dementia and acknowledge their ethical concerns (McCabe & Innes, 2013). Moreover, there needs to be a clear understanding of the lived experience of using these technologies in real life situations, besides those obtained during technical and clinical research (Hine et al., 2022). Howes and Gastmans (2021) acknowledged that there is still limited understanding of whether and how ethical issues in the use of electronic tracking devices change from AT design to their implementation. Moreover, the ethical implications associated with the simultaneous use of multiple AT devices, as it is envisaged in the future, has not been properly studied.
Future research on the ethical issues surrounding assistive technologies (AT) in dementia care should focus on numerous critical areas to address existing gaps. Studies should explore the evolving ethical considerations across the entire lifecycle of AT, by understanding how ethical concerns change as technologies transition from theoretical and clinical trials to real-world use, particularly in diverse cultural, geographical, and care settings. Research should also examine the simultaneous use of multiple AT devices, such as electronic tracking devices and surveillance cameras, as their combined ethical implications, such as increased surveillance or reduced autonomy, remain underexplored. AT research should adopt participatory and rights-based approaches, involving individuals with dementia and their caregivers in co-design processes. Finally, greater emphasis should be placed on exploring the intersectionality of ethical principles—balancing autonomy, privacy, and safety while ensuring equity and accessibility across socio-economic and geographical boundaries.
Strengths and limitations of the review
This study used systematic, narrative and scoping reviews with a significant ethical component, to provide an overview of the ethical issues in dementia when using AT. A systematic approach was used to select the reviews using nine databases. The selection of the reviews based on the criteria that they had to have an extensive ethical component, could have been subjective. However, at least three authors were engaged during the second screening process, during which they independently read the full-texts and arrived at a decision through consensus. This ensured rigour. The utilisation of a framework synthesis for data extraction enabled the application of a deductive/inductive approach that provided a comprehensive description of the ethical issues whilst ensuring further critical discussion of the factors that shape the ethical debate. However, a more detailed discussion of ethical issues related to specific AT and devices, was not possible due to the nature of the review. Whilst attempts have been made to ensure that the framework used to categorise ethical issues was inclusive (Table 1), the selection of the ethical principles was based solely on ethical literature, with the risk of missing important ethical issues. Nevertheless, the selected ethical principles in this review were closely related to six ethical principles as obtained through empirical research of a qualitative study that explored the ethical issues associated with the adoption of robots in long-term care settings (Hung et al., 2022), indicating that these ethical issues truly reflected practical concerns.
Conclusion
This review synthesizes the ethical issues associated with assistive technologies (AT) for persons with dementia and their caregivers. Central concerns include autonomy, privacy, non-maleficence, beneficence, and justice, which intersect and shape the ethical implications of AT use. The ethical debate surrounding ATs is influenced by the varying priorities of stakeholders, differences in the interpretation of ethical principles, and cultural factors. These elements contribute to the complexity of ethical considerations in the design and implementation of AT in dementia care. This overview of review highlighted how future research on assistive technologies (AT) in dementia care should explore ethical considerations throughout the AT lifecycle, from design to real-world use, across diverse settings. It also emphasises the need to balance ethical principles while ensuring accessibility and inclusivity. The ethical principles described in this review should ultimately guide the future development and implementation of AT in dementia care.
Supplemental Material
Supplemental Material - Ethical issues associated with assistive technologies for persons living with dementia and their caregivers – An overview of reviews
Supplemental Material for Ethical issues associated with assistive technologies for persons living with dementia and their caregivers – An overview of reviews by Anthony Scerri, Frederik Schou Juul, Rosa Silva, Rodrigo Serrat, Adrienne Grech, Gabija Jarašiūnaitė Fedosejeva, Montserrat Celdrán, Elzbieta Trypka, Christian Borg Xuereb, Nilufer Korkmaz-Yaylagul, Melina Evripidou, Isabel Machado Alexandre and Sigurd Lauridsen in Dementia
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This article is based upon the work from COST Action (Ethics in Dementia (EDEM) [CA21137] supported by COST (European Cooperation in Science and Technology).
ORCID iDs
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
