Abstract
Introduction
Eating difficulties significantly impact the nutrition, health, and well-being of people with dementia worldwide. Training strategies, such as Spaced Retrieval and Montessori-based activities, have the potential to enhance the self-eating ability of people with dementia but have not been widely tested. This paper reports the co-design and preliminary testing of the SPREMON (Spaced Retrieval and Montessori-based activities) intervention to enhance mealtime independence and experiences for people with dementia living in nursing homes.
Methods
Informed by experience-based co-design methodology, this study used a three-phase approach to intervention development. Three initial sessions were conducted with aged care professionals to develop and refine the intervention. Four pilot sessions were conducted with people with dementia to assess the feasibility and suitability of intervention elements. A final consultation session explored the data and identified barriers and facilitators to successful implementation. While field notes were kept in early sessions, the final session was audio-recorded and transcribed for analysis. Thematic analysis was undertaken with all qualitative data, while observational data are reported using descriptive statistics.
Findings
Six aged-care professionals, 3 researchers, and 9 people with dementia participated in the intervention development. The intervention approach was positively appraised for its potential to enhance self-feeding abilities in people with dementia while saving staff time. Participants suggested improvements to the Spaced Retrieval approach by incorporating visual and verbal cues to make it less confrontational. However, challenges regarding the lack of detail and guidance for implementing Montessori-based activities made them difficult to apply without clarification. Additional barriers included staff shortages, engagement difficulties, and scheduling conflicts. Pilot activities highlighted practical considerations for intervention implementation and patient engagement.
Discussion and Implications
This study demonstrates that the SPREMON intervention holds significant potential to enhance the self-eating ability of people with dementia living in nursing homes. However, the paper also highlights potential challenges in the implementation.
Keywords
Introduction
Currently, there are approximately 55 million people worldwide living with dementia, and the annual cost of related healthcare services exceeds $1.3 trillion USD (World Health Organisation, 2023). Dementia is not a normal part of aging, and it is recognised globally as a critical public health issue (Pacifico et al., 2022). Dementia causes a range of symptoms, including memory loss, cognitive decline, and both physical and psychological deterioration, which significantly impair daily functioning (Cipriani et al., 2020). These impairments significantly affect activities of daily living, such as eating, toileting, and mobility (World Health Organisation, 2023).
Among the various challenges faced by people with dementia, eating difficulties are prevalent, particularly in nursing home environments (Yan et al., 2023). These difficulties, which include challenges in selecting food and all physical activities associated with eating, are especially common in those with more severe stages of dementia or low physical capacity (Jung et al., 2021). A recent Australian study conducted in the hospital setting reported that all participants with dementia exhibited some form of eating difficulty, with 75.5% requiring partial assistance and 24.5% needing full assistance during mealtimes (Lin et al., 2023).
The behaviours associated with eating difficulties in dementia vary. Some common behaviours include long pauses during meals, becoming easily distracted by surroundings, and experiencing issues such as food dribbling from the mouth or difficulty using utensils (Lin et al., 2023). These challenges are primarily linked to procedural memory impairment, difficulties in eating abilities, and limited attention span (O'Neill et al., 2023). Eating abilities are a cognitive and physical function, and as dementia progresses, reduced food and fluid intake can result in malnutrition, longer hospital stays, respiratory infections, and increased mortality (Espinosa-Val et al., 2020). Eating difficulties have profound implications for the health and well-being of people with dementia, leading to “nutritional frailty” (Fostinelli et al., 2020). Indeed over half (57.4%) of the people living in nursing homes are malnourished (Perry et al., 2023). Malnutrition can accelerate the decline in cognitive and physical function, further exacerbating the progression of dementia and leading to poorer outcomes, including increased risk of falls and fractures and higher mortality rates (Yan et al., 2023).
Increasing food and fluid intake by improving the dining experience can significantly enhance the quality of life and health of people with dementia. The importance of positive dining experiences is widely recognised, including by the Australian Aged Care Quality Standards, which advocate for enjoyable and safe mealtimes for people with dementia (Aged Care Quality and Safety Commission, 2024). Various countries, including the United Kingdom, the United States, and Canada, have developed guidelines to improve mealtime experiences for people living with dementia, focusing on promoting independence and managing risks, such as choking (Alzheimer Society of Cananda, 2024, Arizona Center of Aging, 2018; Murphy et al., 2019). Nursing home care staff spend considerable time assisting people with dementia during meals, which strains already limited resources and exacerbates staff burnout (Passos et al., 2024). Additionally, high turnover rates and staffing shortages in dementia care facilities exacerbate the challenges of providing adequate mealtime support (Passos et al., 2024). Therefore, implementing evidence-based interventions that enhance mealtime processes will improve time management and overall efficiency (Palese et al., 2020).
Both Spaced Retrieval and Montessori-based activities have shown promise in training people with dementia to enhance their self-feeding abilities (Yan et al., 2023). Spaced Retrieval involves repeated questioning to improve procedural memory related to eating, while Montessori-based activities focus on motor skills, such as scooping, cutting, squeezing and pouring (Wu et al., 2014). The combined effect of these interventions can potentially enhance the self-feeding abilities and nutritional status of people with dementia living in nursing homes (Yan et al., 2023). The SPREMON (Spaced Retrieval and Montessori-based activities) intervention was originally developed from Taiwanese research (Lin et al., 2010, 2011; Wu et al., 2014; Wu & Lin, 2013). Despite established merits, effectively implementing this intervention in a different context requires adaptation of the intervention to address environment and cultural differences. In particular, this study sought to adapt the intervention for Western-dining etiquette. To ensure appropriate adaption and translation into practice, consultation with local experts was necessary. This paper reports on the co-design process and pilot testing of the SPREMON intervention in the Australian nursing home context.
Methods
Design
This study was informed by an Experience-Based Co-design Methodology. Co-design engages stakeholders throughout the process, fostering patient-centred care, enhancing the acceptance of interventions, and improving real-world applicability and cost-effectiveness (The Australian Healthcare and Hospitals Association, 2024). The methodology is guided by core principles such as power-sharing, inclusivity, respect, reciprocity, and collaborative relationships, ensuring alignment across all research stages to address the needs of all stakeholders (The Australian Healthcare and Hospitals Association, 2024). By integrating stakeholder involvement, co-design ensures interventions align with patient and practitioner needs, facilitating the effective translation of knowledge into practice. To ensure robust and comprehensive reporting, the study adhered to the Consolidated Criteria for Reporting Qualitative Research (COREQ) checklist (Tong et al., 2007).
Development process
Intervention development was structured into three phases using two approaches: codesign workshops and pilot testing of intervention components (Figure 1). Phase 1 involved three 2-hour sessions with nursing home aged care professionals and research team members. The PhD candidate (ZMY) drafted a version of the intervention handbook, based on a literature review (Yan et al., 2023). The handbook describes participant eligibility, the intervention activities, an implementation plan and evaluation forms. This handbook was intended to provide a guide for participation selection, activity implementation and outcome evaluation. These sessions aimed to introduce, evaluate and refine the intervention and implementation handbook. SPREMON Co-design Process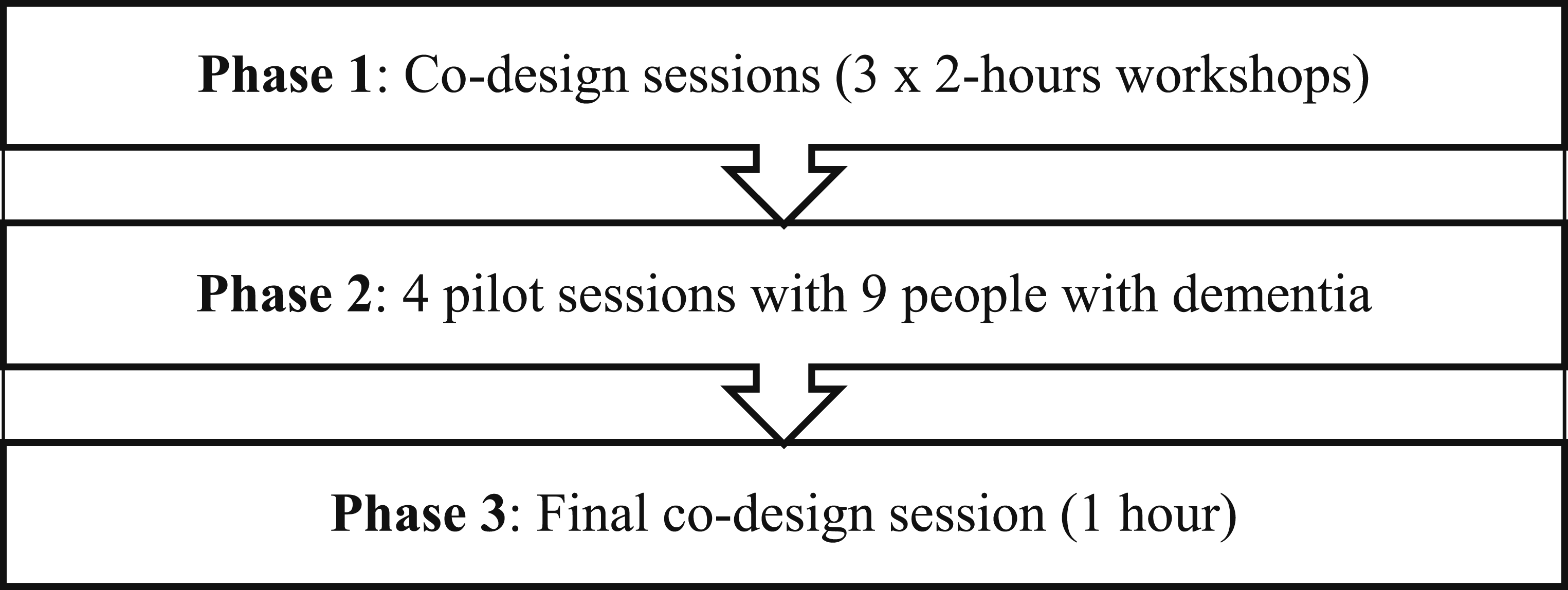
Phase 2 consisted of four pilot sessions involving nine people with dementia to assess the feasibility and suitability of aspects of the SPREMON intervention. Finally, Phase 3 involved a final co-design workshop to explore the data collected and finalise recommendations to support the intervention’s successful adoption and future application.
The co-design workshops (Phase 1 and 3) were structured using the “rose, thorn and bud” framework (Pineo et al., 2022). This framework has been widely used in co-design to enhance the quality of healthcare service design and delivery (Vargas et al., 2022) and is designed to gather feedback on strengths, weaknesses, and opportunities for improvement (Cui, 2022). The “rose” symbolises the project’s successes and highlights, the “thorn” identifies flaws or imperfections, and the “bud” represents areas with potential for growth and actionable improvements (Cui, 2022). To explore the rose elements, questions focussed on ‘What aspects of the SPREMON intervention are done well?’ In contrast, thorn questions focused on: ‘What aspects of the SPREMON intervention are not done well? What barriers exist to the intervention’s successful adoption? Finally, questions to explore the bud sought to understand; What areas of the SPREMON intervention could be improved? What facilitators could enhance its implementation?’
Setting, sampling and participant recruitment
This study was undertaken within a single aged care organisation with multiple sites across a regional area in New South Wales, Australia. A senior staff member emailed study information and calendar invitations to ten potential participants. Eligible participants were those in leadership roles, including nursing home managers (baccalaureate prepared or equivalent registered nurses), lifestyle team leaders, and allied health team leaders (e.g. physiotherapists). These participants were selected for their expertise in the aged care sector and knowledge of issues relevant to the project, such as feeding challenges and practice change. Focussing on this group was seen as crucial given the role that leadership plays in implementing evidence-based practice, particularly when launching a new research project. Participants could respond to the invitation via email, and written consent was gained prior to data collection.
Convenience sampling was used to recruit people with dementia for the pilot sessions from one participating site. A lifestyle team leader employed within the facility facilitated the recruitment. Residents were eligible to participate if they had a diagnosis of dementia, safe swallowing abilities as confirmed by a registered nurse and could sit in a chair or wheelchair for 45 minutes. Verbal consent was obtained from participants with dementia as their family members had agreed to their participation in research on nursing home admission.
Data collection
Phase 1 workshops were held face-to-face in a meeting room at a participating site. Two researchers (ZMY and VT) led all workshops, while another team member (PD) attended to record meeting notes and manage audio recordings. Two research assistants supported the co-design workshops by setting up the room and distributing participation information sheets, consent forms and a hard copy of the intervention handbook and the interview guide. Participants were sent the implementation handbook electronically to review before the first session. During the first two sessions, the researchers introduced the SPREMON intervention (Figure 2) and demonstrated some of the included activities. Participants were encouraged to share feedback and raise any issues regarding the implementation of the intervention. The third session focused on gathering participants’ insights after four weeks to reflect and review the intervention materials. SPREMON Intervention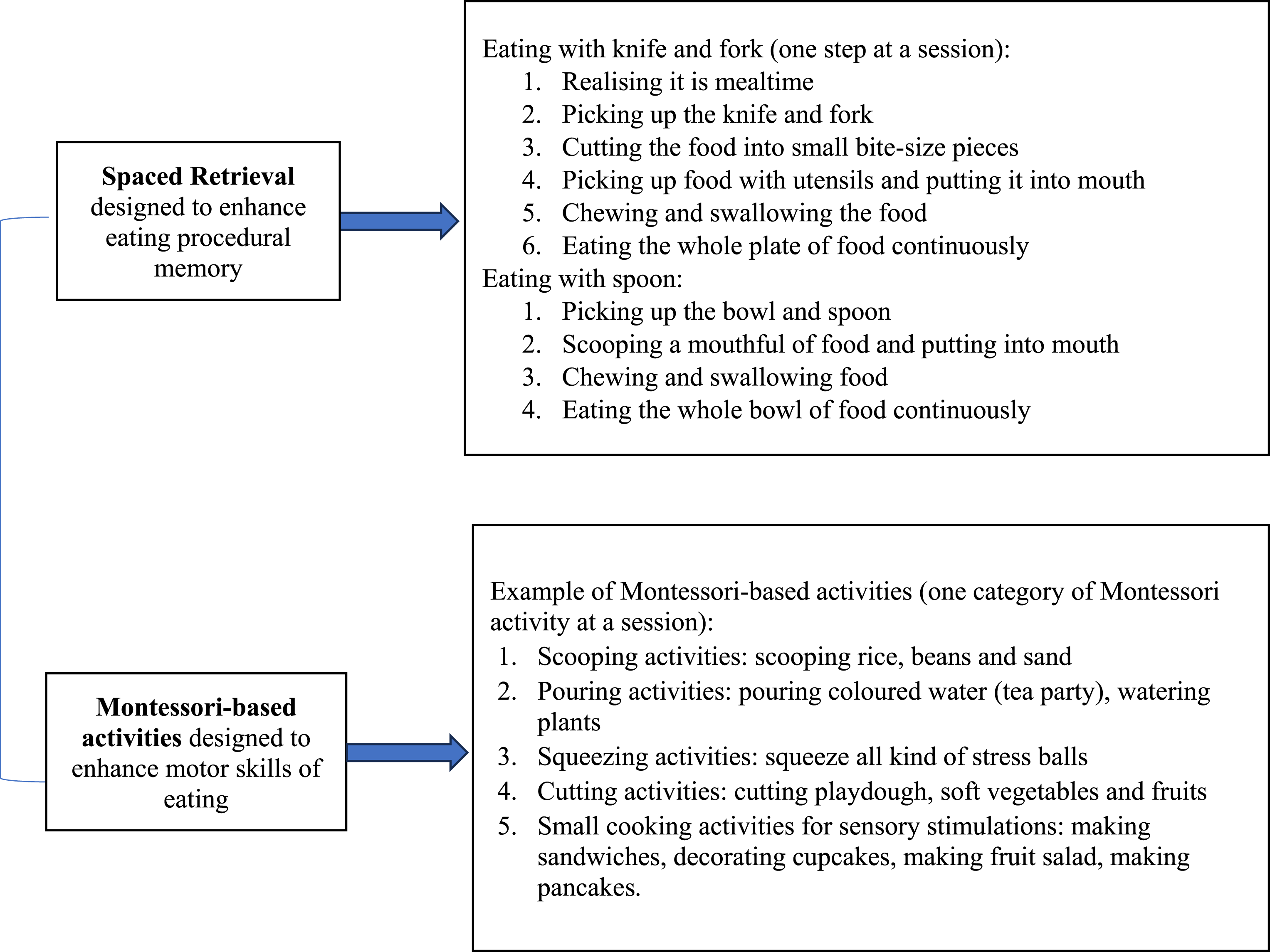
The pilot sessions (Phase 2) involved nine participants living with dementia at a single site. Participants were divided into two groups based on the severity of their dementia, as measured by Mini-Mental State Examination (Cockrell & Folstein, 2002). Each group participated in two sessions and every session consisted of one Spaced Retrieval activity and one Montessori-based activity. As they were going to be conducting the intervention in the larger trial, the PhD candidate (ZMY) conducted these sessions, lasting 45–60 minutes each. These sessions replaced the regular daily activities scheduled in the facility to avoid disruption to routines. An assistant in nursing from the facility helped set up the activities and escorted participants to the activity room. These sessions focused on three key areas: (1) participants’ adherence to intervention procedures, (2) participants’ responses to the activities, and (3) participants’ level of engagement with the activities. A data collection tool was developed for the PhD candidate (ZMY) to capture these data during each session. Field notes also provided qualitative observations of the sessions.
In the final co-design workshop (Phase 3), those individuals who participated in Phase 1 were given an overview of all data collected and invited to review the updated implementation handbook. Participants provided final comments and recommendations regarding the SPREMON intervention and handbook, including aspects such as staff-to-participant ratios, the use of group activities, and adaptations for individuals with special needs. The final workshop was audio recorded and transcribed verbatim for analysis, while in the other sessions, field notes were taken to capture the researcher’s observations.
Data analysis
Transcripts were imported into NVivo for data analysis. Qualitative data (Phase 1 and 3) were analysed using deductive thematic analysis (Braun & Clarke, 2013). Through a realist and contextualist lens, data was grouped according to three predefined themes as guided by the “rose, bud and thorn” framework (Cui, 2022). Data analysis initially involved transcribing the audio recordings and the researchers’ familiarising themselves with the data. ZMY and PD then generated codes together and grouped them into predefined themes. All researchers then reviewed the codes and themes until a consensus was reached before the findings were reported (Braun & Clarke, 2013). Observational data from the pilot sessions were summarised using descriptive statistics and summary tables of observational data.
Ethics considerations
This research was approved by the Human Research Ethics Committee of University of Wollongong prior to commencement (Approval Number: 2023/268). Participants were informed that they were free to cease their involvement in the study at any time, although none chose to do so.
Findings
Co-design sessions (Phase 1 and 3)
Six aged care experts from three sites attended the co-design sessions. Five of these experts were female (83%), with a mean age of 37 years (SD 10 years). The experts had an average of 11 years (SD 6 years) experience working in aged care and 12 years (SD 6 years) experience working with people with dementia. Four participants (67%) were Australian-born, and two (33%) were born overseas. Four participants held Bachelor’s Degrees (66%), one (17%) had a Diploma, and one (17%) had a Master’s degree. Additionally, the research team had three female nurse participants, including the Doctoral candidate (ZMY) and two nurse experts in aged care and implementation science (VT and PD).
Theme 1. positive aspects of the intervention
The SPREMON intervention received positive feedback for integrating Spaced Retrieval and Montessori-based activities. Participants particularly valued the intervention’s detailed, task-based approach, which supports people with dementia in performing essential mealtime tasks. As P1 noted, “It kind of describes the types of actions that need to be facilitated or supported through an activity… pouring, cutting, squeezing, scooping, and then a sensory activity”.
Participants also highlighted the dual impact of enhancing feeding as it “helps staff to save their time, and the residents can gain their independence back” (P2). Other participants emphasised the potential impact of the intervention’s success on staff workloads; “If we can learn techniques and a structure that helps some of our residents with dementia to self-feed for longer, that would be really beneficial” (P1). “If they’re able to self-feed for longer, staff won’t need to spend as much time assisting with spoon-feeding” (P6).
Research projects like SPREMON promoted the development of new skills, the adoption of evidence-based practices, and enhanced care standards. Moreover, participants demonstrated a commitment to improving the quality of life for residents, positively influencing staff morale and the public perception of the organisation. This involvement underscored the organisation’s role as a leader in driving progressive and person-centred approaches in aged care. As P5 highlighted “we take the learnings from the study and then someone else may or so it might still expand that study, but it’s still great to be a part of as an organisation to be contributing to research.”
Theme 2. Challenges and barriers associated with intervention
Participants identified several potential challenges with the intervention, particularly with the Montessori-based activities. They indicated that the implementation handbook lacked sufficient detail and concrete examples to guide some activities. For example, although the handbook provided the Montessori-based activities the lack of details included in these activities could hinder practical application for those unfamiliar with the intervention. P1 noted, “one of the missing pieces is actually identification of the actual intervention activity, which probably requires a bit more work”. Without clearer guidance, staff might struggle to implement the activities as intended. P5 asked, “What are they scooping?” while P6 added, “What are the actual activities we can do for practising the scooping ability?” This lack of clarity and specific examples was seen as a significant barrier to successful implementation.
Another challenge identified was the difficulty of securing staff commitment and the impact of the intervention. P2 explained, “My concern would be the regularity and the impact on the rest of the care team, and whether some may decide to do it”. This highlights the challenge of ensuring that the intervention is integrated as a regular part of the care routine, rather than an optional activity. The importance of routine was emphasised by P4 who stated, “I just know that from previous things that we’ve brought in.. you’ve got to have them. On that day, that time. And it’s good because then they get into the flow of, OK, today is Monday, 2:00pm, Bingo. And then you kind of change it. Then you’re in trouble”.
The importance of staff motivation was also emphasised as a critical factor for success. One participant noted that interventions are more likely to succeed when staff recognise the positive impact, especially if it resonates with their own work experience. As P1 explained, “We’ve had success when staff see that it makes a difference… particularly if it appeals to the difference it makes to them”. P2 also indicated that “I don’t think they feel that sometimes that their job is super important. So maybe if we could even like get, I know they’ve got more outspoken stuff. Some reason giving them that importance”. She suggested that promoting the project by encouraging how “we really need you [staff] to help” and emphasising the importance of the staff’s role in the intervention would get “more of their buy-in”. Several participants provided key insights into ways in which to promote staff engagement. “Just to let them know that the project is happening, and this is the basis behind it and this is the benefit what we hope to look for in the future.... So they all feel involved rather than we tend to do a lot of things that don't make it down to ground level….. And they don't feel like they're involved” (P3). “I think if they get a good understanding of what's happening and why it's happening, once they will all be on board” (P4).
Another challenge raised was group dynamics, with concerns about interference between participants during group activities: “If you’re doing it in a group, what’s to stop one resident from listening and using another resident’s answer?” (P2). P3 pointed out the potential issue of residents copying each other’s answers during Spaced Retrieval activity: “I’m picturing a few residents in my head. Whether or not, I just told you the answer to that, that one was like, you know”. These insights highlighted the need for careful management of the group setting to ensure the effectiveness of the intervention for each resident.
Theme 3. Areas for improvement
Participants identified several areas for improvement in the intervention design, focusing on making the intervention more engaging and practical. One key suggestion was to modify the approach to Spaced Retrieval by replacing repetitive questions with more appealing and less confrontational methods. “For some people with dementia, asking the same question repeatedly could feel patronising and confrontational” (P1). Instead, it was suggested to have “pictures that indicate dining or eating, so participants recognise it’s mealtime” (P1) to provide a more appropriate prompt.
Participants also emphasised the importance of ensuring a screening process was used to identify individuals most suited for the intervention. P1 remarked that “a screening process would ensure that participants won’t feel patronised, and the intervention suits their needs”. P5 suggested that “a trial would give us insights to refine eligibility and assess the impact of the group activity”.
Several key facilitators that could enhance the successful implementation of the intervention were also identified. Organisational leadership, sufficient human resources, and access to training materials and space were all seen as critical elements for ensuring the successful implementation of the intervention. “Organisational leadership support is critical to the success of this project” (P1) as they can secure the necessary resources and foster a culture that prioritises the intervention. Beyond organisational leadership ensuring staff buy-in was also important. “I know that we’ve got team leaders in each area of the home, but they already have so much to do I think if we put this to the care staff to help drive it, I think” (P2).
Pilot sessions (Phase 2)
Pilot session findings.
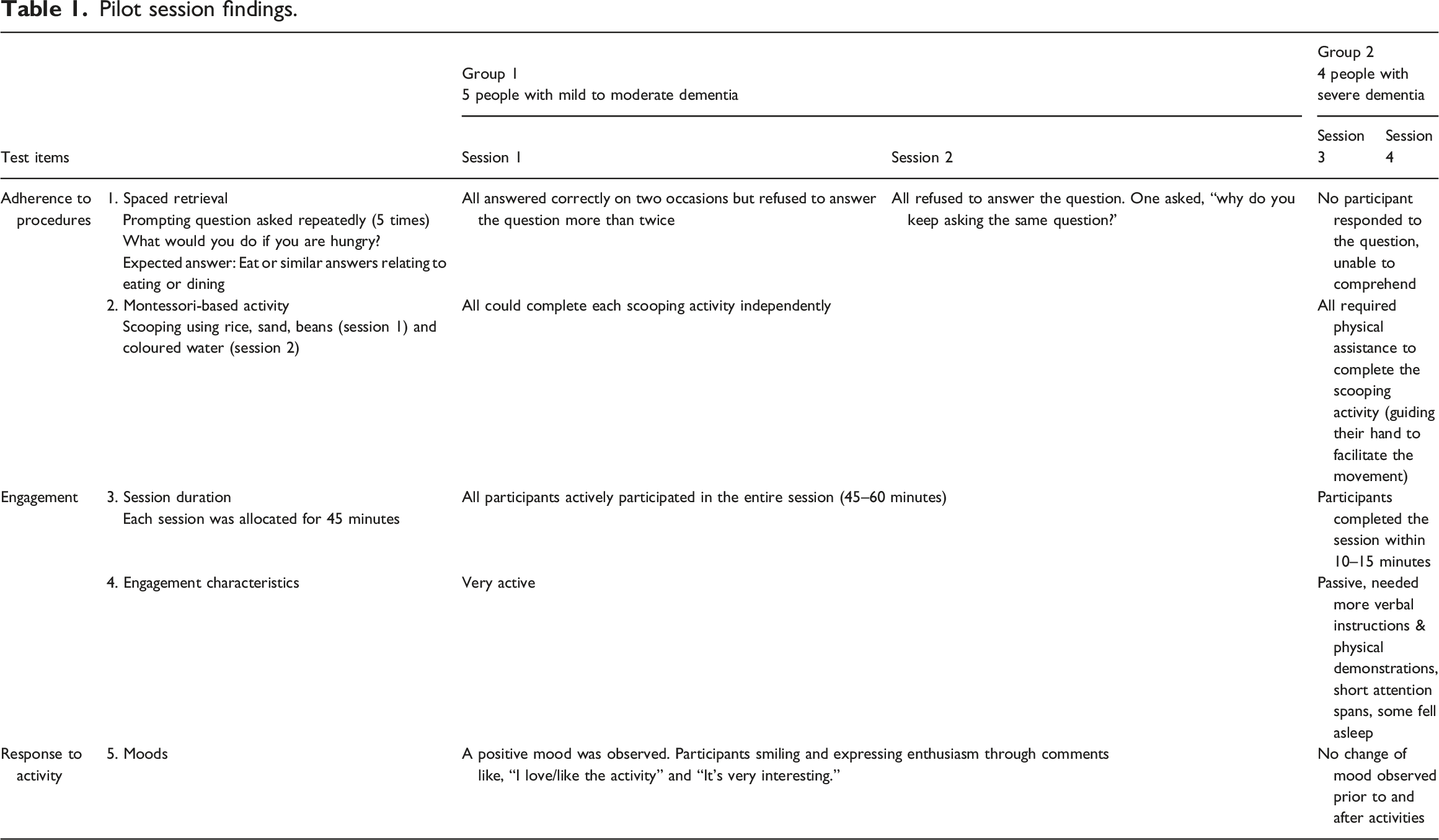

In contrast, participants in the severe dementia group were observed to struggle to understand and follow instructions. Some were affected by physical symptoms (e.g. lethargy, drowsiness) or exhibited behavioural issues (e.g. wandering) that impacted their ability to engage. During the pilot sessions group interference was identified as a challenge during the Spaced Retrieval exercises. Some participants who knew the answers would respond on behalf of others. To address this, the pilot session initially directed questions to specific participants, confirmed their responses, and instructed them to avoid assisting others. This approach appeared effective in reducing group interference.
Conducting these pilot sessions highlighted the importance of the staff-to-participant ratio in supporting engagement during activities. Ratios of 1:2 or 1:3, depending on participants’ cognitive and physical abilities, were found most effective. Ensuring adequate staffing levels before implementing the intervention was observed to help address staffing challenges and provide the necessary support for individuals' to participate. Following the co-design process, all findings were integrated into the implementation handbook to guide future implementation of the SPREMON intervention.
Discussion
The co-design process used in this study ensured that the SPREMON intervention was adapted to local nuances and needs. A key strength of the intervention is its focus on enhancing mealtime independence and the nutritional status of people with dementia living in nursing homes in a practical and engaging way. The integration of Spaced Retrieval and Montessori-based activities focuses on enhancing procedural memory and motor skills required to maintain feeding independence (Wu et al., 2014; Wu & Lin, 2013). Promoting mealtime independence can reduce the risk of malnutrition, malnutrition-related compilations and responsive behaviours (Liu et al., 2023; Perry et al., 2023). The co-design processes used in this study are crucial as they address uncertainties around intervention design and implementation, thereby informing larger-scale implementation trials (Pearson et al., 2020).
The SPREMON intervention handbook provides a comprehensive guide to successfully implementing the intervention. It contains three key sections: (1) Participant Selection, outlining the eligibility criteria for selecting participants; (2) Implementation Plan, detailing the activities, timeline, group setting and frequency of the intervention; and (3) Evaluation Forms, offering tools for assessing the intervention outcomes. The handbook breaks down each phase of participant selection, implementation, and evaluation into manageable, actionable steps, ensuring a clear and structured approach. It serves as a step-by-step resource to guide users through the entire intervention process. While the initial draft of this handbook was developed based on the international literature around the use of Spaced Retrieval and Montessori-based training to support feeding difficulties in those living with dementia (Yan et al., 2023), the engagement of local stakeholders ensured that the intervention was suited to Australian context and met local needs.
This study highlighted the dual benefit of the intervention. With its potential to enhance the self-eating ability of people with dementia, the intervention can enhance nutrition and well-being and reduce staff time burden related to feeding. Beyond the nutritional benefits (Lin et al., 2010, 2011; Wu et al., 2014; Wu & Lin, 2013), maintaining self-eating abilities fosters personal control and enhances a sense of worth, ultimately supporting dignity and promoting person-centred care (Tabari et al., 2016). Enhancing the self-feeding abilities of people with dementia can save staff time, reduce carer burden, and improve the quality of care in resource-constrained settings (Zanini et al., 2021). This is particularly important in the current residential care context, where staff time is stretched due to limited resources, high care needs and workforce shortages (Kaldy et al., 2022; Mueller, 2022). Understanding end-users perceptions of the benefits of the intervention to their practice and health outcomes is important in promoting future intervention uptake (Marshall et al., 2020).
This study identified several key challenges in engaging nursing home staff in research. One major issue was time constraints, particularly during busy morning shifts, which aligns with previous research indicating that nursing home staff often face difficulties participating in research due to demanding schedules (Law & Ashworth, 2022; Stephens & Knight, 2022). Additionally, the study found that a lack of awareness about research and limited staff initiative can impede engagement. Given the rotating shifts and nature of the residential aged care environment, staff will potentially miss important project information. This observation is consistent with findings from previous literature, which emphasises that improving access to project information enhances staff engagement (Law & Ashworth, 2022; Stephens & Knight, 2022). Furthermore, this study highlighted that staff knowledge and confidence are crucial in their willingness to participate in research. To this end, appropriate training will facilitate greater involvement of staff in future research activities (Law & Ashworth, 2022). Identifying and addressing these factors can increase staff engagement and willingness to participate in research activities.
During the co-design process, the importance of clearly articulating the nature and scope of the intervention was identified. Without detailed, step-by-step explanations, staff may become confused and uncertain about implementing the intervention consistently. The important role of detailed instructions in intervention design has been reported in the literature, as these details guide and inform successful intervention implementation (Donadey et al., 2024; Kinney et al., 2024). Without a comprehensive protocol to guide the intervention, consistency of intervention delivery between sites can be problematic (Friese et al., 2017). Variability in the consistency of intervention implementation across sites can lead to biased estimates of intervention effectiveness, impacting the generalizability and study conclusions (White & Barnett, 2019).
Participants identified several factors that could enhance the successful implementation of the SPREMON intervention. Foremost among these was the necessity of support from organisational leadership and allocating sufficient resources. Strong leadership has been widely recognized as a critical enabler of change in healthcare settings, with evidence linking effective leadership to the successful adoption of new programs (Farahnak et al., 2020). Additionally, participants suggested introducing staff incentives, such as gift vouchers or badges, to foster engagement with the project. This recommendation aligns with motivational theories, which highlight the importance of recognition and rewards in driving staff participation and commitment (Shepherd et al., 2022). These strategies underscore the need for a supportive organisational environment to promote the intervention’s success.
Implications for future research and practice
The findings from this study offer valuable experiences for both future research and the practical implementation of eating ability training projects in aged care. First, a comprehensive guiding handbook or protocol is needed to guide the intervention step-by-step in multiple sites to ensure consistency. Second, the implementation barriers and challenges identified during the co-design process, suggest that further refinement and testing are needed before the intervention can be widely adopted. Conducting pilot sessions, as suggested by participants, provided essential feedback to optimise the intervention from a patient perspective. However, in this pilot, the PhD candidate (ZMY) who was a nurse delivered the intervention. This may have led to differences compared to sessions conducted by nursing home activity staff members. Future research should explore how usual care providers could facilitate the sessions and examine the impact on fidelity and outcomes.
Moreover, addressing the barriers identified in this study will require strategic planning and resource allocation, particularly in overcoming staff shortages and ensuring staff engagement. The facilitators identified in the study, including leadership support and staff incentives, offer a pathway toward successful implementation of the SPREMON project, but they also highlight the importance of a supportive organisational culture in fostering innovation in dementia care.
The SPREMON mealtime intervention holds significant promise for improving the mealtime independence, mealtime experience and nutritional status of people with dementia living in nursing homes. However, its success will depend on continuous refinement, flexibility in activity design, and strong support from both staff and organisational leadership. Future research should focus on addressing the identified challenges and further exploring how such interventions can be scaled up to benefit a larger population of people with dementia in aged care.
Limitations
The study’s strengths include the involvement of aged care experts joining with researchers in the co-design process, ensuring practical relevance, and considering the implementation factors. Additionally, this will be the first study combining Space Retrieval and Montessori-based activities amongst people with dementia using Western style dining etiquette. The focus on real-world application through pilot sessions and a holistic evaluation of both strengths and challenges enhance the robustness of the study. However, the modest sample size and the single organisation used in the co-design process potentially limits the generalisability of the findings. While the co-design process engaged a range of expert participants within the setting, assistants in nursing and carers were not included due to resource constraints. Future research should involve these groups in the evaluation. Additionally, the PhD candidate (ZMY) conducted the pilot sessions instead of training staff, aiming to reduce the burden on the organisation. However, this may have introduced bias and overlooked challenges in usual staff delivery. Future studies should assess the intervention’s implementation by care staff for a more realistic evaluation.
Conclusion
The SPREMON mealtime intervention presents a promising approach to enhancing mealtime independence, mealtime experience and nutritional status for people with dementia in nursing homes by integrating Spaced Retrieval and Montessori-based activities. Developed through a co-design process involving aged care experts, the intervention is grounded in practical experience and tailored to real-world care settings. Additionally, four pilot sessions have refined the design, offer valuable insights for future practices, and incorporate the learning into the implementation handbook as a step-by-step guide for future applications. The study highlights the potential benefits, such as improving self-feeding skills and reducing staff burden, challenges related to activity clarity, staff shortages, group dynamics, and logistical barriers must be addressed.
This study also underscores the intervention’s broader significance in bridging research and practice. By demonstrating the feasibility of translating evidence-based approaches into real-world care, it provides a foundation for larger-scale studies to refine and evaluate its long-term impact. With careful planning, resource allocation, and ongoing refinement, the SPREMON intervention has the potential to improve the mealtime independence, mealtime experience and nutritional status for people living with dementia, while contributing to the advancement of dementia care research and improve the overall quality of life for this cohort.
Footnotes
Acknowledgements
We would like to thank all the nursing home staff especially Shiva Gopalan, as well as the people living with dementia and their families, for their support and participation in this research .
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study is supported by The first author (ZMY) awarded tuition fee from the University of Wollongong and living stipend from China Scholarships Council for four years.
