Abstract
Objectives
Social and behavioural symptoms, prevalent across dementia syndromes, contribute to increased carer challenges and stress. However, post-diagnostic support for these symptoms remains limited. The Carers Way Ahead, initially developed for brain injury, is an online carer program addressing behavioural management of apathy, irritability, aggression, disinhibition, social difficulties, and self-care. This study aimed to explore the experiences and needs of family carers and co-design the adaptation of the Carers Way Ahead program for dementia.
Method
Ten family carers of people with dementia (4 frontotemporal dementia, 3 Alzheimer’s disease, 3 Lewy body dementia, 1 Vascular dementia) in Australia participated in focus groups and interviews. Carers completed the Carers Way Ahead modules and provided insights into their experiences and feedback on the program. Transcripts were analysed using reflexive thematic analysis.
Findings
Three themes were generated: (1) Adapting to life transitions highlighted challenges and relationship changes in the dementia journey, (2) Navigating dementia care pathways underscored complexities in accessing and navigating institutional and practical support, and (3) Finding solutions that address carers’ needs emphasised the importance of considering varying needs across disease stages and pragmatic intervention considerations.
Conclusion
Disparities in the accessibility, consistency, and quality of post-diagnostic support for carers were revealed. Substantial unmet needs exist in the current post-diagnostic experience for people with dementia and carers in Australia. This study suggests opportunities for improvement and provides valuable insight for the development and adaptation of psychosocial interventions like the Carers Way Ahead program.
Keywords
Informal care, typically provided by family members, is a cornerstone of dementia care. In Australia, 93% of informal carers provide ongoing daily support to people with dementia, with almost half devoting over 60 hours of care per week (Australian Bureau of Statistics, 2019). However, compared to carers of individuals with other disabilities, those caring for people with dementia report higher levels of unmet needs and lower service utilisation (Meaney et al., 2005; Thompson & Roger, 2014; Toseland et al., 2002). Current post-diagnostic support offered to people with dementia and their carers remains underdeveloped and may not adequately address the needs of all carers, particularly those caring for individuals with younger onset dementias and non-Alzheimer’s dementias (Morhardt, 2011). Social and behavioural symptoms common in younger onset dementias such as frontotemporal dementia have been associated with higher levels of carer strain, depression and stress compared to Alzheimer’s disease (Boutoleau-Bretonniere et al., 2008; de Vugt et al., 2006; Diehl-Schmid et al., 2013; Mioshi et al., 2009; Riedijk et al., 2006). Similarly, psychiatric features such as hallucinations and delusions in dementia with Lewy bodies are also associated with higher levels of carer distress and strain compared to Alzheimer’s disease (Aarsland et al., 2001; Ricci et al., 2009; Svendsboe et al., 2016). Given the limited efficacy of pharmacological interventions for social, behavioural and psychological symptoms in dementia (Azermai, 2015; Tible et al., 2017), a growing emphasis has been placed on the development of non-pharmacological interventions including those that focus on carer support (Ballard et al., 2017; Brodaty et al., 2018; Gitlin et al., 2012; Livingston et al., 2014; O’Neil et al., 2011).
Of relevance here, social, behavioural and psychological symptoms are not exclusive to dementia but are also prevalent in other clinical populations such as traumatic brain injury (Demakis et al., 2007; Sabaz et al., 2014; Winter et al., 2018). Given the greater emphasis on rehabilitation in traumatic brain injury, psychosocial interventions such as the Carers Way Ahead program (https://carerswayahead.psy.unsw.edu.au/) have been developed to provide support and training for families caring for individuals with brain injuries (McDonald et al., 2021). Conventional face-to-face interventions place substantial demands on clinical services and may pose accessibility challenges for those caring for family members with dementia. In contrast, the Carers Way Ahead program adopts a narrative-based, pictorial approach, and is delivered online, enhancing its accessibility. Importantly, early intervention and support for carers has the potential to improve carer wellbeing, increase carer knowledge and abilities, and delay the need for residential care for people with dementia (Gaugler et al., 2005; Kjallman Alm et al., 2014; Sorensen et al., 2002). How these types of interventions can be adapted across clinical populations is an important avenue for research. One aspect that remains unknown is whether the content and style of the Carers Way Ahead program also have the potential to yield benefits for carers of people living with dementia.
Qualitative research plays a pivotal role in understanding the ‘lived experience’ of people with dementia and carers. This approach shifts away from the traditional biomedical view, emphasising personhood as a crucial perspective in dementia research (Cotrell & Schulz, 1993; Woods, 2001). Clinical guidelines and formal inquiries such as the recent Australian Royal Commission into Aged Care Quality and Safety, advocate for comprehensive psychosocial interventions and person-centred care for people living with dementia (Commonwealth of Australia, 2021; Laver et al., 2016; NHMRC Guideline Adaptation Committee, 2016). However, the implementation of these recommendations in practice remains challenging (Chenoweth et al., 2021; Cooper et al., 2017; Wheatley et al., 2021). To address this, it is crucial to understand carers’ experiences and perspectives to inform the development of intervention programs and care models that address their needs. Of relevance here, co-design emerges as a promising method that facilitates the meaningful involvement of individuals with lived experience in both research and practice. It has gained increasing recognition as the best practice approach to research in the development of interventions (Goh et al., 2022; Leorin et al., 2019). Co-design can inform intervention design, development, and implementation (Piper et al., 2012; Steen et al., 2011). This ensures interventions are more likely to meet carer’s needs which, in turn, fosters greater utility and efficacy.
The aims of this study were to (1) explore the experiences and needs of family carers in the dementia post-diagnostic care landscape and (2) gather information for subsequent co-design of the adaptation of the Carers Way Ahead program for dementia. Engaging carers as active collaborators in research through participatory co-design provides valuable insights. These insights offer a deeper understanding of the existing gaps in post-diagnostic care and serve as a vital guide for the development and optimisation of psychosocial interventions in dementia. This approach ensures that these interventions are relevant and meaningful for both carers and care recipients.
Method
Participants
Ten family carers of people living with dementia participated in this study. Participants were included if they were over eighteen years of age, conversationally fluent in English and caring for an immediate family member (spouse, parent, or sibling) with a formal diagnosis of dementia. Participants were recruited through purposive sampling from the Memory Clinic at the University of Newcastle and StepUp for Dementia Research (https://www.stepupfordementiaresearch.org.au/). StepUp for Dementia Research is an online self-registration platform that enables volunteers across Australia, including carers of people living with dementia, to express their interest in taking part in research and be matched to suitable available studies (Jeon et al., 2021).
Ethical approval
Ethical approval was obtained from the University of Sydney Human Research Ethics Committee (HREC) (HREC 2022/864) and all participants provided written informed consent.
Carer’s Way Ahead
Prior to the focus group or interview, participants were given access to an existing online carers’ program ‘Carer’s Way Ahead’ which was developed as a resource for family carers of people with traumatic brain injuries (McDonald et al., 2021). The program contains seven modules. The two psychoeducational modules cover, (1) Understanding traumatic brain injury – the impact on emotions, thinking and behaviour; (2) The ABCs of behaviour – introducing the concepts of antecedents, behaviour, and consequences. Four behaviour modules cover (3) Low motivation and apathy; (4) Acting without thinking; (5) Social difficulties and (6) Irritability and aggression. One module addresses supporting carers’ emotional strain and stress: (7) Self-care. Participants were given access to all the modules and content, however, were asked to complete two specified modules, prior to the focus group or interview. Collectively, all seven modules were completed across all participants (Module 1 (1 completed); Module 2 (3 completed); Module 3 (3 completed); Module 4 (4 completed); Module 5 (4 completed); Module 6 (2 completed); Module 7 (3 completed)). Each module took approximately 15 minutes to complete.
Data collection
Carers completed a short online demographic questionnaire hosted on a secure web-based database (Research Electronic Data Capture [REDCap]) (Harris et al., 2009, 2019). This collected information about the carer including age, sex, education, employment status, geographical information and relationship to the person living with dementia. Clinical information about the person living with dementia was also collected, including dementia type (if known) and disease duration. Semi-structured interviews and focus groups were conducted either online via Zoom, by telephone, or face-to-face depending on the carers’ preferred mode. Carers were asked about their experiences as a carer more broadly, and about their experiences with the Carers Way Ahead program. On average, two carers participated in each focus group with a duration of 90 minutes, while interviews were 60 minutes. Data saturation was achieved when no new themes or insights were generated from the focus groups or interviews.
Data analysis
All interviews and focus groups were audiotaped and transcribed verbatim. Transcripts were fidelity checked and any identifying information was redacted. NVivo 14.23 (QSR International Pty Ltd.) was used to code data. Reflexive thematic analysis was used following the six phases described by Braun and Clarke (Braun & Clarke, 2006): familiarisation by reading and re-reading the transcripts; developing a list of codes in an open coding cycle; generating initial overarching themes and patterns; revision of themes and codes; developing clear definitions, categories, and refining themes; and writing up. To ensure reliability of the study findings, peer debriefing was used. To reduce researcher bias, an iterative process took place, wherein the authors met to discuss the codes alongside the supporting quotes that were representative of the themes that they were demonstrating. Discrepancies were discussed until consensus on common themes and codes was reached.
Findings
Demographics
Demographic and clinical characteristics of the study cohort.

aNote. One carer was caring for both a parent and spouse with different types of dementia.
Overview of themes
Three overarching themes were identified from the data: (1) Adapting to life transitions, (2) Navigating dementia care pathways, (3) Finding solutions that address carers’ needs (Figure 1). These are described in further detail below. Overview of overarching themes and subthemes.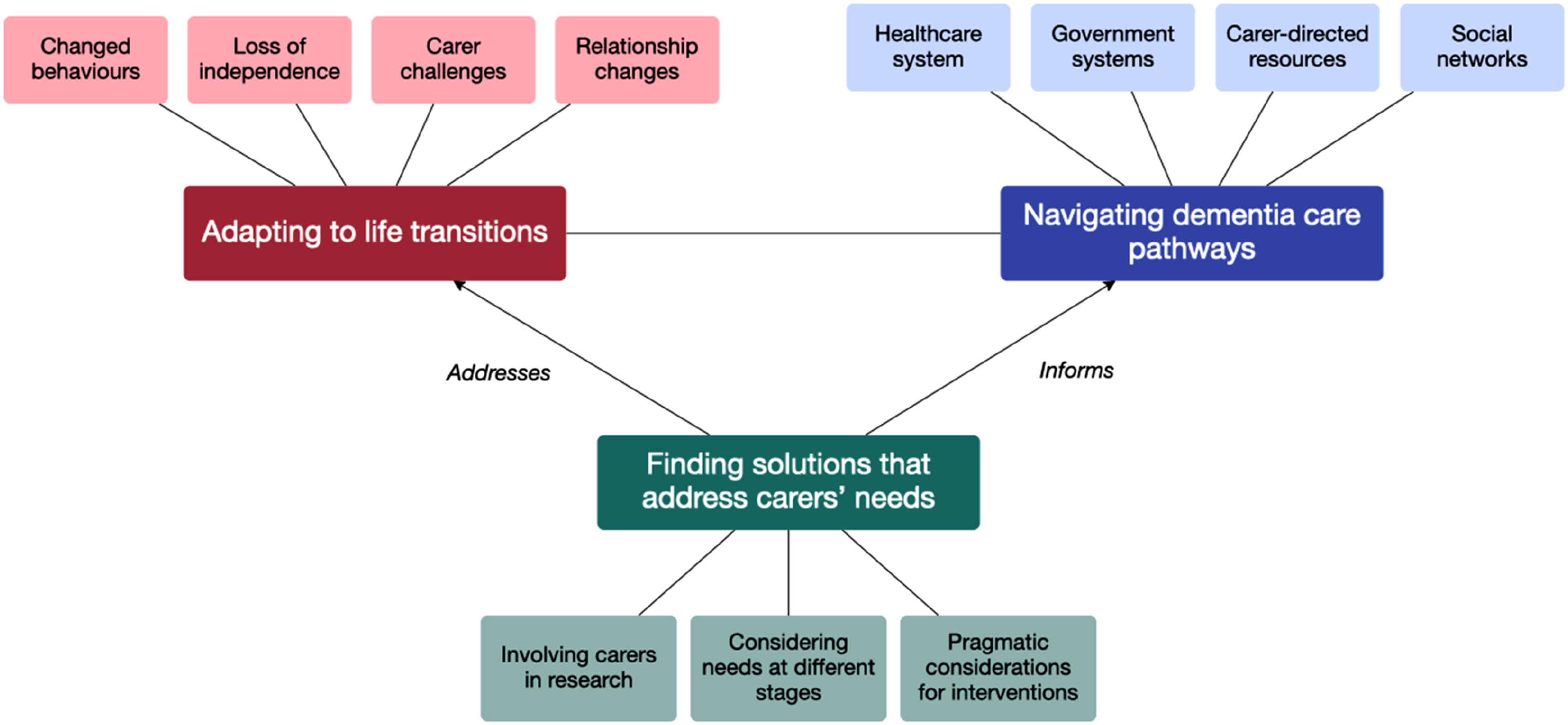
Theme 1: Adapting to life transitions
Theme 1 focused on the challenges and adjustments experienced by people with dementia and carers in the dementia journey. The subthemes identified were changed behaviours, loss of independence, carer challenges and relationship changes (Figure 1).
Changed behaviours
Carers reported a range of changed behaviours including social difficulties, antisocial behaviours, delusions and hallucinations, communication difficulties, rigidity and stereotyped behaviours, apathy, and lack of insight. These changes manifested in social dysfunction including strained relationships and withdrawal from social activities and are described in further detail below.
Social difficulties
Difficulty understanding social cues, including safety concerns such as engaging with strangers online, posed significant challenges for people with dementia, potentially placing them in risky situations. As one carer described, “She loves to connect with people. She just doesn’t know how to do it safely.” (C01). The loss of empathy in their loved one also strained relationships, with one carer noting, “It’s very rare that he’ll ask me how I am.” (C10).
Inappropriate and disinhibited social behaviours often led to social withdrawal, with carers feeling compelled to intervene or stop the person with dementia. For example, one carer shared, “Picking on people, only wanting to joke, even in very difficult situations where they are complaining about cancer and crying, he wants to come and tell a joke all the time” (C05). These behaviours also occasionally triggered conflicts within the family.
Antisocial behaviours
Engaging in social activities also elicited antisocial behaviours including risky behaviours or criminal transgressions, such as walking out of a store without paying for goods or not obeying road laws. Carers reported a lack of understanding or regret from the person with dementia regarding these behaviours, compounding the challenges they faced. As one carer explained, “He knows he does it, but he doesn’t think it’s wrong. He deliberately doesn’t pay for it, and he says, ‘Well they don’t ask me, that’s their problem.” (C10).
To mitigate these risks, one carer took proactive steps of closely supervising their loved one and “reported him as having dementia with the local police station” (C10) to ensure awareness and understanding in case of any legal issues. Many carers also contended with explosive and aggressive behaviours that were often directed towards them, which further strained their relationship. As one carer noted, “A lot of that frustration, it gets directed towards me, unfortunately.” (C01).
Psychiatric - delusions and hallucinations
Delusions often caused confusion and suspicion in people living with dementia, and sometimes escalated into arguments as well as instances of absconding from care facilities. Carers also reported auditory and visual hallucinations, with the person living with dementia “never quite sure what’s real and what’s not” (C01). The impact of these psychiatric symptoms for people with dementia was profound and led to feelings of depression, anger, embarrassment, and anguish.
The struggle to distinguish between their own mental experiences and external reality was distressing for people with dementia and further isolated them, with carers reporting it resulted in “trouble integrating into the community” (C01). Another carer described how paranoia manifested in behaviours such as whispering “She’s whispering because of her paranoia. She thinks she’s being recorded all the time.” (C04).
Speech, language, and hearing
Some carers described a loss of speech and language skills in the person living with dementia. These challenges were exacerbated in care facilities due to mask-wearing requirements (associated with COVID-19 pandemic), which hindered comprehension of speech and obscured cues such as lip reading. One carer explained the emotional impact of the disconnect when the person with dementia had “little to no comprehension, no language or conversation. He can’t communicate with anyone, it’s very, very difficult.” (C03).
Carers also expressed uncertainty regarding whether the person with dementia was able to hear or understand what was being said, especially when there is no response or acknowledgement of the communication. As one carer noted, “I’m not sure she always hears everything either.” (C06). Consequently, this resulted in the contributions of the person with dementia to conversations dwindling or revolving around “the same thing over and over again” (C10).
Rigidity and stereotyped behaviours
Carers reported that individuals with dementia became highly inflexible with their thinking, with one carer noting, “he is extremely resistive to almost anything that anyone wants him to do” (C03). This rigidity extended to daily routines, such as strict mealtimes, and some carers observed the development of obsessive interests such as golf or puzzle games. One carer described how their loved one “will sit there doing find-a-words for 7 hours.” (C05).
While these fixations could be challenging, they were also seen as a positive outlet by carers, providing a means of mental stimulation and physical exercise. As one carer described, “His obsession is golf. He used to play golf but now he’s now literally obsessed. I don’t mind him playing golf because it’s exercise and he’s got to think about those clubs to use.” (C08).
Apathy
Some carers described apathy in their loved one, which resulted in disengagement from activities and a decline in participation in daily life and routine tasks. One carer shared, “I said to him, ‘Should we go for a walk? We have to go and walk the dog, and then he goes, ‘I don’t feel like it. I think I’m becoming lazy.” (C05). Others observed prolonged periods of inactivity, such as one carer noting “She sits there for hours with eyes closed” (C05), while another stated “his motivation is a problem” (C09).
Insight
Carers reported varying levels of insight among people with dementia. One carer noted that awareness of their condition led to feelings of shame, saying “I would say there’s some shame or there is an awareness of her condition for sure.” (C06). On the other end of the spectrum, others appeared to be in denial, with one carer describing their loved one as saying, “What condition? I’ve just got a little memory issue.” (C10). This lack of insight was challenging for the carer, as they reported they would be “more depressed afterwards because [they] would see how every other carers’ loved ones were not in denial” (C10).
Loss of independence
Carers expressed concern regarding the gradual loss of independence experienced by people with dementia as the condition progressed. Carers often reported finding themselves constrained by the “need to be able to make arrangements for the person living with dementia to be safe” (C02). Perceived loss of independence of their loved one stemmed from the inability to work, drive or “catch a bus on [their] own” (C05) or from challenges posed by cognitive and functional impairment. This led to increased social isolation and withdrawal of both the carer and person living with dementia. Some carers noted that the progression of dementia necessitated constant supervision due to the individual’s diminished understanding, issues with time perception, and difficulty performing day-to-day functions. This reliance on carers extended to responsibilities such as organising and managing appointments and making everyday decisions, with carers taking on a central role in guiding and safeguarding the person with dementia through daily activities. One carer noted, “It’s very difficult to find something for her that she can occupy herself with, where I don’t have to be there.” (C07).
Carer challenges
Carers often struggled to balance their own needs with the increasing needs of the person with dementia, leading to exhaustion and frustration. Some carers also shouldered additional responsibilities such as caring for adult children or taking on extra employment to provide financial support, on top of managing their ongoing caregiving responsibilities. Carers openly shared the emotional strain they experienced, encompassing a range of sentiments including grief, guilt, sadness and hopelessness. One carer shared, “It’s hard though, because it’s a big job and there’s periods of time where you’re exhausted and the day-to-day of it gets very tiring.” (C01). Amidst this emotional strain, some carers sought moments of solace through brief cathartic episodes such as a “little five-minute cry” (C01), while others spoke of the frustration of feeling overlooked, with one carer sharing, “very rarely I get asked how I am because it’s all about them.” (C05).
Relationship changes
Carers often found themselves assuming unfamiliar roles in their relationships, with some noting a shift from a spousal dynamic to more of a parent-child relationship. As one carer described, “I’ve become his mother in a way. I’m not his wife anymore, I’m like his mum.” (C10).
Carers also reported frustrations and strains in their relationships, grappling with feelings of guilt stemming from their reluctance to visit or engage with their loved ones at times. With disease progression, carers also wrestled with feelings of grief over the loss of the person they once knew. One carer expressed, “most of the time, she’s not really my mum as I knew her anymore.” (C01), while another described the gradual loss as “the long goodbye” (C03), where the familiar person seemed to gradually fade away despite their physical presence.
Theme 2: Navigating dementia care pathways
Theme 2 focused on the complexities and challenges people living with dementia and carers faced in navigating institutional, structural, and social support pathways in dementia. The subthemes identified were the role of the healthcare system, government systems, carer-directed resources, and social networks in facilitating or hindering caregiving.
Healthcare system
The process of obtaining a dementia diagnosis could often be protracted and challenging, involving multiple tests over many years. Some carers reported a lengthy journey involving contact with multiple clinicians and early misdiagnoses, where doctors were reluctant to label individuals at a younger age or failed to recognise early symptoms in those with a high level of premorbid functioning. Following diagnosis, many carers expressed a dissatisfaction with their relationship with medical professionals, citing a perceived lack of direction and “no support or information” (C02). One carer shared, “She gave us the report and said ‘Here’s the report. Yes, he’s got dementia and I’ll see you in six months.’ So that was that. That was our introduction.” (C02). Carers reported feeling left to cope, adjust, and seek answers and assistance on their own, beyond a check-in once or twice a year which was primarily “just to keep an eye on the medication” (C03). Many carers felt unsupported, with one describing the early stage as “like sink or swim” (C03). Carers expressed having to take initiative themselves, seeking information and referrals for relevant services and additional care from allied health professionals. As one carer noted, “the GPs have been really good at referring to different areas, but generally I’ve initiated it.” (C09).
Government systems
Caregivers consistently voiced their dissatisfaction with formal dementia care systems and services, emphasising the complexity of navigating the “labyrinth” (C06) of aged care and dementia support options. One carer with a background in disability support and prior familiarity with government systems found the aged care system considerably more complex. Carers’ experiences were riddled with bureaucratic obstacles, describing the system as “crazy complicated” (C07), replete with extensive forms, applications, and assessments. Many carers reported frustrations with various entities including Centrelink (now Services Australia) and My Aged Care, feeling lost due to a lack of clarity about available services and how to access them. Carers greatly appreciated when they had a primary point of contact with a “dementia support person” (C06), who could “walk [them] through that journey” (C06) and provide them with information and guidance on accessing various services, care suppliers, home care packages and other aspects of caregiving. Some carers found it difficult to obtain additional support services due to financial constraints on their allocated funds. Carers also encountered difficulties finding appropriate support, often discovering it was unsuitable or inadequate for their loved ones’ needs. Here, carers highlighted the lack of appropriate services tailored for people living with younger-onset dementia or those in earlier stages of dementia, with understanding of dementia often falling short. Carers shared experiences of being informed that long-term care facilities were ill-prepared and “not cut out to look after people with dementia” (C04) due to their complex needs. Further, carers highlighted the scarcity of appropriate care options, particularly in regional areas. One carer mentioned, “the provision of aged care dementia facilities in regional areas is not good. It’s very, very hard to get respite care. It’s very, very hard to get a bed. They’re full. We just don’t have the number of places and that’s confronting and difficult to live with.” (C09). These collective criticisms substantially outweighed any positive feedback, pointing to systemic issues, convoluted processes, and the pressing need for more accessible and suitable services.
Carer directed resources
Carers relied on non-profit organisations, local support groups, and online resources for dementia support, however, access was typically self-directed. Carers highlighted the lack of promotion of vital resources, such as Dementia Australia by healthcare professionals, with one caring noting it was “not promoted very well” (C02). This created concerns for those unaware or unable to access available resources and services. For instance, one carer explained “We did nothing to begin with because we didn’t know that you could.” (C09). Several gaps were identified, including the absence of services and activities catering to different conditions and needs as they predominantly catered to an older age group at a “fairly advanced stage with their dementia” (C07). Carers reported this could be quite confronting, disturbing, and upsetting for people with younger-onset dementia or during the earlier stage of the disease. Peer support from other carers was highly regarded and carers found comfort in discussing their concerns with people “going through a similar journey” (C03). They also emphasised the usefulness and practicality of information and skills training programs such as courses with Dementia Australia and the University of Tasmania Understanding Dementia course, providing them with a baseline of understanding as well as tips and strategies they could use to “deal with these different things” (C09). As one carer put it, “There’s lots of information out there. It’s just you have to find it.” (C10).
Social networks
Carers shared a range of experiences regarding social support. Some felt supported by family, friends, and the community, while others described strained relationships, conflicts over caregiving responsibilities, and increasing distance from loved ones. Carers frequently cited external factors such as bereavement, geographical distance, or restrictions due to the COVID-19 pandemic as reasons for the diminished social support they received. A lack of “in-depth understanding” (C02) about dementia among family and friends further contributed to reduced social support. One carer explained, “they just don’t realise that there is so much more involved with dementia and the different types of dementias” (C03). As a result, carers reported increasing social isolation and becoming “shut off from the world and enclosed within your own environment” (C03). As one carer shared, “Once something happens in your life like this, a lot of people just sort of move away from you. They don’t want to deal with it.” (C05).
Theme 3: Finding solutions that address carers’ needs
Theme 3 focused on finding solutions that address carers’ needs. The subthemes identified were involving carers in research, considering needs at different stages and pragmatic considerations for interventions.
Involving carers in research
Carers expressed an active engagement in advocacy and willingness to participate in research programs. Carers expressed beliefs that contributing to research offered “a sense of hope” (C04) and contribution to future advancements. Many carers found fulfilment in “being consulted” (C09) and the opportunity to “add value” (C04), with research serving as a “chance just to vocalise” (C10) and seek support while connecting with others who understood their journey. Research also served as “an opportunity to bounce off people and to vent and to share that sense of I’m not alone in this.” (C04).
Considering needs at different stages
Carers noted that the type of support needed varied at different stages across the disease course. Carers reported lacking in support at the early stage and wanted to receive more information about dementia and practical advice on accessing formal support services with “a really clear instructional pathway for new people to dementia” (C01). As one carer explained, “the early stages of getting that diagnosis, there’s some real gaps for people just not having an understanding.” (C02). Carers also expressed that they “probably weren’t quite given the warnings on the psychotic behaviours early on” (C09) and saw value in “knowing what to expect” (C08) and “being aware of what the behaviours are as [they] go forward” (C08). However, some carers noted it may be overwhelming to engage with interventions like the Carers Way Ahead program in the initial post-diagnostic period as they “would be too taken by the enormity of that diagnosis” (C05). When reflecting on the Carers Way Ahead material, carers reported some strategies “wouldn’t be appropriate because he wouldn’t remember that” (C10) at the more severe stages of the disease due to cognitive decline.
Pragmatic considerations for interventions
Carers appreciated the online format as a convenient and accessible resource, allowing them to engage “when it suits me” (C08), despite caregiving demands. Short modules were preferred as many carers faced time constraints due to their caregiving obligations. As one carer explained, “If it had been longer, it would have been more difficult because she would have stopped doing whatever she was doing and she would have been wondering what I was doing.” (C07).
When reflecting on the Carers Way Ahead, carers commented that the material was “very easy to understand…avoided too much technical or medical speak” (C01), and offered “strategies and the practical elements of what you could do” (C06). The practical behaviour modification strategies resonated with carers, many of whom commented they were “really useful” (C09) and “really helpful” (C06) and they had already successfully implemented them. Relevant real-life scenarios resonated with carers as “very real” (C10) and “things that would and could happen” (C02). Some carers suggested adding live video for engagement, while others recommended supplementing the online modules with “downloadable resources” (C02) or printed materials for notetaking and later reference.
Discussion
These findings shed light on the intricacies of the experiences and needs of family carers and post-diagnostic support pathways in dementia. Three overarching themes were identified in the focus groups and interviews with carers. Here, these key themes and clinical implications that were generated from this study are considered.
The first theme explored the challenges in adapting to life transitions in the dementia journey. Carers often found themselves dealing with the loss of independence and challenges of managing changed behaviours in dementia including social difficulties, antisocial behaviours, delusions and hallucinations, rigidity and stereotyped behaviours, speech, language and hearing difficulties, apathy, and loss of insight. These contributed to diminished social engagement and reciprocity, and increased relationship strain. Notably, the range of changed behaviours identified by carers here informed the adaptation of the Carers Way Ahead program, guiding the development of targeted new modules designed to better address the specific needs of people with dementia. Carers also reported increased feelings of grief, loss, stress, and challenges associated with caregiving and difficulty adapting to changes in their existing spousal or parental relationships. These findings highlight the need to consider the carers, often referred to as the hidden patients (Brodaty & Donkin, 2009) through not only providing practical support through respite, but also coping strategies and tools to help carers maintain their own psychological and emotional wellbeing. Further, education and carer training in behaviour management strategies and communication skills can empower carers in their role, foster positive interactions and mitigate carer challenges (Eggenberger et al., 2013; Mittelman et al., 1996; Pinquart & Sorensen, 2006; Roth et al., 2005).
The second theme revealed the challenges people with dementia and carers faced in navigating dementia care pathways. Many carers felt that current service provision predominantly focused on the point of diagnosis, with limited guidance provided regarding post-diagnostic care pathways beyond medication titration. The role of the healthcare professionals, as the first point of contact in the dementia journey, is pivotal in initiating access to post-diagnostic support for people with dementia and their carers. The concerns raised by carers in this study echo previous studies and underscore the need for better integration (Lo et al., 2022), for instance by appointing a single point of contact for care and support throughout the disease course (Burley et al., 2023; Sutcliffe et al., 2015). Providing carers with access to a specialist dementia care coordinator, or clinical nurse specialist, who can deliver personalised guidance can bridge the gap between carers, government systems and other support services. Integrating these specialists into primary healthcare settings can facilitate smoother transitions for carers and ultimately streamline post-diagnostic care to ensure carers and people with dementia are provided with appropriate support options.
Notably, almost all carers were openly critical of the lack of clarity, suitability, and undue complexity of accessing formal dementia care systems and services. In Australia, a shift towards the consumer directed care model aims to empower consumers; however, its success hinges on carers’ awareness and availability of relevant government and community services (Gill et al., 2017; Ottmann & Mohebbi, 2014). The absence of a coordinated system for providing care and support services was further compounded by the disproportionate geographical concentration of these services. Specifically, carers reported that long term care facilities, respite and day care services were notably lacking in coverage in regional settings, leading to variability in cost and quality. Furthermore, a shortage of age-appropriate and dementia-specific services exacerbated the difficulties faced by carers. Carers also described a notable lack of capacity among care staff and facilities in dealing with the complex needs of individuals with dementia, emphasising the urgent need for greater training and education of care staff.
Carers accessed a multitude of dementia resources through a combination of non-profit organisations, local support groups and online means. The predominantly self-directed nature of this pursuit highlighted the need for improved signposting to these resources. While a wealth of relevant and useful information and resources are available online and through various channels, the primary challenge lies in the overwhelming nature of synthesising this information and absence of early and consistent information provision which can lead to carers’ underutilisation of available services (Brodaty et al., 2005; Wolfs et al., 2010). Addressing these barriers to access can significantly impact the overall effectiveness of these dementia support resources. In this way, incorporating references to other relevant resources within programs such as the Carers Way Ahead can be a beneficial approach to enhance utilisation and accessibility for carers.
Furthermore, carers shared a wide range of experiences regarding informal care in the form of social support from family, friends, and the community. These experiences were diverse and included both positive and negative facets. Some carers reported receiving inclusive support from those close to them and the wider community. Conversely, others described strained familial relationships and conflicts arising in their social networks. External factors including bereavement, geographical distance or constraints imposed by the COVID-19 pandemic played a substantial role in the perceived reduction of social support available to carers. Aligning with previous findings by Davies et al. (Davies et al., 2019), this study also identified a lack of in-depth understanding about dementia among family and friends which created an additional barrier to receiving effective social support. This lack of adequate social support led to increased social isolation and exacerbated the emotional impact of caregiving. To address these issues, education and awareness programs and dementia-friendly community initiatives are needed to foster a more supportive social environment for people living with dementia and their carers. Further, carers should be encouraged to engage in support groups, providing them with a source of social support and platform to connect with others navigating similar challenges.
The third theme identified carers’ needs in finding solutions. This included the importance of engaging carers in research, considering carers’ needs across different disease stages and pragmatic considerations for intervention design. Here, this study found that carers expressed a strong inclination towards advocacy and participation in research. Their active engagement not only contributed to the development of relevant solutions and support services but also provided them with a sense of purpose, hope and a supportive community. These findings underscore the importance of involving carers in research, particularly in the co-design of interventions as a key stepping stone towards the successful delivery and implementation of appropriate support services that meet their needs.
Further, carers also highlighted the progressive nature of dementia which necessitated services to adapt to the evolving needs of individuals across the disease course. Notably carers’ readiness levels for engaging with information about behavioural changes varied. Timing and the screening of needs and symptoms, considering the stage and severity of dementia, were recognised as critical factors in ensuring that interventions effectively targeted the right audience with tailored support.
Lastly, in terms of the Carers Way Ahead program, carers found the online format to be a convenient and readily accessible resource. The preference for online delivery overcomes barriers such as geographical distance, scheduling conflicts and mobility issues that might hinder participation in in-person programs. This reflects a growing trend in healthcare to harness digital platforms for delivering information and support (Hopwood et al., 2018; Sin et al., 2018). Time constraints stemming from caregiving responsibilities made shorter, more focused modules of information more feasible. Further, carers appreciated user-friendly materials devoid of excessive technical jargon, with an emphasis on practical guidance and behaviour modification strategies that directly addressed the challenges they encounter. The incorporation of real-life scenarios in the materials also helped carers contextualise the information and apply it to their own situations. While carers provided feedback regarding the Carers Way Ahead program and materials, these pragmatic considerations remain relevant for the design and implementation of non-pharmacological interventions more broadly.
These findings highlight the need for accessible, practical and flexible interventions to support carers in managing behavioural and emotional challenges associated with dementia. Many existing programs, such as i-HARP (Jeon, Simpson, et al., 2025), i-CHARP (Jeon, Hobbs, et al., 2025), COPE (Clemson et al., 2018), SPICE (D’Cunha et al., 2025) and SHARE for Dementia (Stockwell-Smith et al., 2024), require ongoing professional involvement, multiple home visits, or intensive time commitments, which can make participation difficult for some carers. In contrast, the Carers Way Ahead program offers a more scalable and practical digital solution. For example, in contrast to the iSupport manual (World Health Organisation, 2019), which is comprehensive but spans 275 pages, the Carers Way Ahead provides succinct, self-paced content in an accessible video format. This design reduces the time burden on carers while allowing for flexible engagement that accommodates the needs of diverse caregiving circumstances such as those who may not need more comprehensive or intensive interventions at their stage of caregiving.
An additional consideration with respect to existing interventions is their restricted availability due to time-limited program offerings, region-specific eligibility criteria, or high resource demands. For example, i-HARP (Jeon, Simpson, et al., 2025), i-CHARP (Jeon, Hobbs, et al., 2025) and COPE (Clemson et al., 2018) require multiple professional-led home visits, while others are confined to specific geographic locations (e.g., SPICE in the Australian Capital Territory, and iREADI in the South Eastern Sydney Local Health District). These constraints underscore the need for a widely accessible, scalable intervention that does not rely on professional facilitation, or location-based eligibility. The Carers Way Ahead program addresses these gaps by offering a flexible, low-resource model that can be accessed by carers regardless of their location, making it a sustainable and practical alternative in the landscape of post-diagnostic dementia support.
Overall, these findings reveal disparities in the accessibility, consistency and quality of support encountered by carers, and offer important insights that inform the development of non-pharmacological interventions. Recommendations for enhancing post-diagnostic support in dementia from the findings described above, across healthcare and government sectors and for carer interventions more broadly, are presented in Figure 2. Recommendations for improvements to post-diagnostic support in dementia.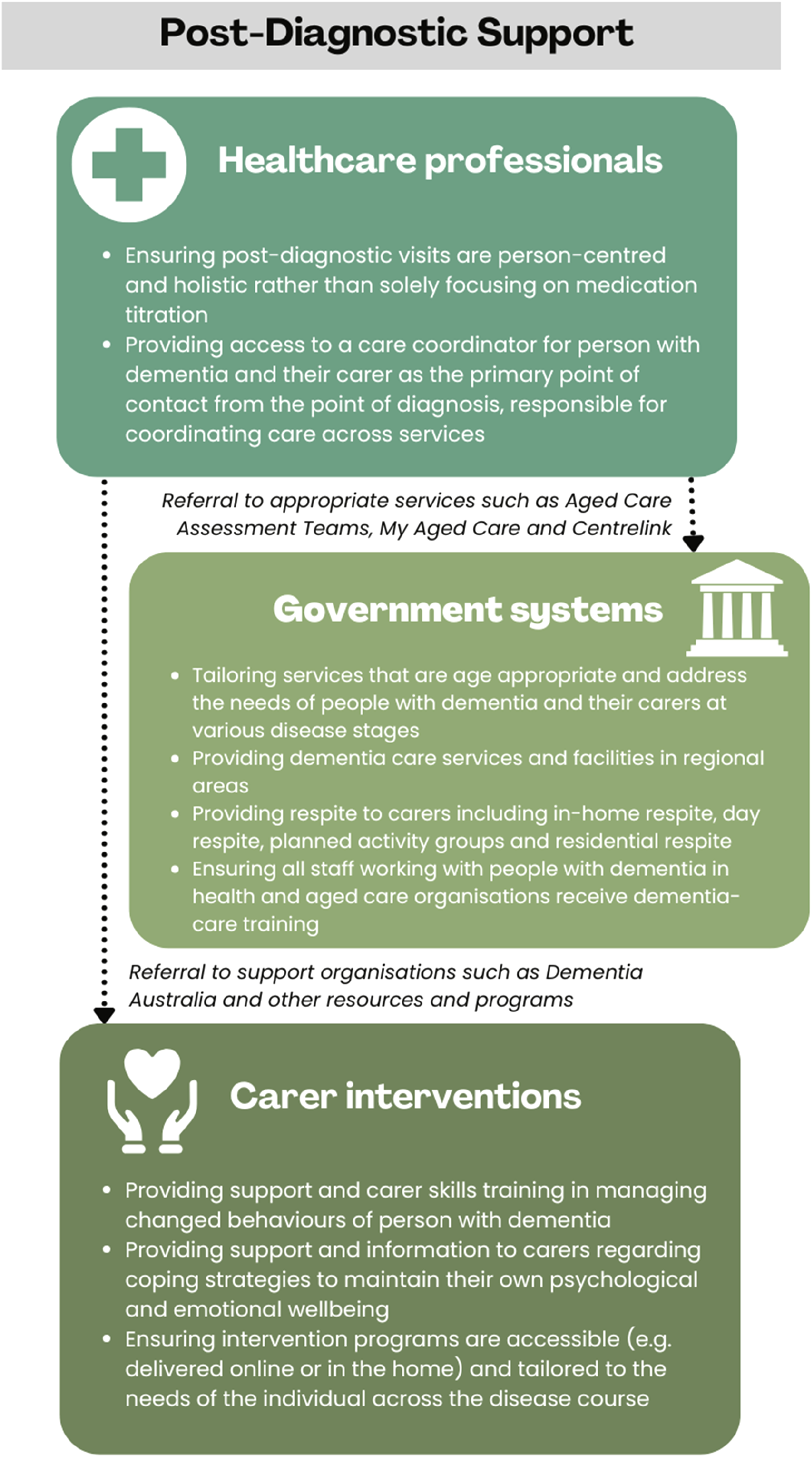
Limitations
While this study provides valuable insights into the experiences of dementia carers, it is important to acknowledge its limitations. Firstly, participants in this study may not represent a random sample of family carers as they volunteered to take part in the research, potentially introducing selection bias. Consequently, carers with fewer resources or greater needs may have been inadvertently excluded due to potential time constraints that hindered their participation. Secondly, the average age of the sample was relatively young (63 years), and thus, may be more comfortable and familiar using digital platforms like the Carers Way Ahead. Older carers may require additional assistance with technology, however, the Carers Way Ahead program is designed to be accessible with minimal technological demands, requiring only a basic web browser. Additionally, the COVID-19 pandemic has accelerated the adoption of digital tools in dementia care, leading to greater acceptance and familiarity with technology among both carers and older adults more broadly (Barbosa et al., 2023; Chirico et al., 2022; Ruggiero et al., 2023). As future generations of carers become increasingly proficient with digital platforms, the relevance and practicality of technology-based interventions will continue to grow, playing a critical role in improving access to dementia care.
Thirdly, carers in this study predominantly consisted of English-speaking individuals from a Caucasian background, and it is unclear whether the findings can be generalised to carers from culturally and linguistically diverse backgrounds. The Carers Way Ahead program, however, was designed with characters from culturally diverse backgrounds to enhance representation and relatability. Despite this, future research should actively seek to include a broader range of cultural perspectives to ensure interventions are inclusive and responsive to the unique needs of all carers. Cultural differences in the context of dementia care, coupled with a scarcity of culturally and linguistically appropriate services may further compound challenges faced by carers and exacerbate health inequities (Giebel et al., 2015; Gillespie et al., 2015; Mukadam et al., 2019; Samson et al., 2016; Watson et al., 2023). Lastly, this study was conducted within an Australian health and social care context, and its applicability and relevance in care systems of other countries remains unclear. While similar challenges have been observed in other counties such as the United Kingdom and Brazil (Durgante et al., 2020), further research is needed to explore how these findings translate to diverse cultural contexts, various organisations, and care systems around the world.
Conclusion
In summary, this study highlights the vital need for healthcare professionals, stakeholders, and researchers to consider the perspectives of people with lived experience of dementia. By understanding their experiences, we can ensure the most appropriate and effective support is implemented. This aligns with the growing momentum to prioritise person-centred approaches to care (McKeown et al., 2010; Woods, 2001).
While acknowledging that the current post-diagnostic experience for people with dementia and carers fell short of optimal, this study points towards several opportunities for improvement. Findings from this study will inform the development and adaptation of psychosocial interventions for dementia carers, such as the Carers Way Ahead program. Notably, our findings closely align with the recently published Australian National Dementia Action Plan (Australian Government Department of Health and Aged Care, 2024), which emphasises the need for accessible education and training for care partners, as well as leveraging technology to deliver flexible dementia support. The Carers Way Ahead program addresses these priorities by providing a digital, scalable intervention that offers practical, non-pharmacological strategies to help carers manage behavioural and emotional challenges associated with dementia. Through a collaborative and holistic understanding of the needs and experiences of carers, these endeavours can contribute to improved quality of life and overall outcomes for people living with dementia and their families.
Supplemental Material
Supplemental Material - Post-diagnostic care pathways in dementia: Experiences and needs of family carers and considerations for interventions
Supplemental Material for Post-diagnostic care pathways in dementia: Experiences and needs of family carers and considerations for interventions by Grace Wei, Skye McDonald, Michelle Kelly, Kirrie J Ballard and Fiona Kumfor in Dementia
Footnotes
Acknowledgements
The authors are grateful to all the participants for their time and contribution to this study. We thank Jye Marchant for his assistance with the transcriptions of the interviews and focus groups.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: G.W is supported by an Australian Government Research Training Program (RTP) Scholarship. F.K is supported by an NHMRC Career Development Fellowship (GNT1158762).
Ethical statement
Data Availability Statement
The data that support the findings of this study are not publicly available due to privacy reasons but are available from the corresponding author upon reasonable request.
Supplemental Material
Supplemental material for this article is available online.
Author Biographies
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
