Abstract
Participating in physical activity is beneficial for older people with dementia. Little is known however about the perceptions of people living with dementia undertaking an online-delivered exercise program. This study aimed to explore the experiences and perceptions of older people with dementia and their carers in Indonesia participating in an online-delivered exercise program, and factors that may influence acceptability to the program. An exploratory qualitative study design using semi-structured interviews was used. Data were recorded, transcribed verbatim, translated into English, and analyzed thematically. Twelve participants with dementia (mean age = 63.3 years) and 30 carers (26 family carers and 4 paid carers) (mean age = 37.9 years) were interviewed separately. Seven themes were identified: (i) Motivating factors to participate; (ii) Benefits for people with dementia; (iii) Impacts on carers; (iv) Challenges and enablers to exercising; (v) Carers’ strategies for exercise engagement; (vi) Roles, relationships and supports; and (vii) Participants’ receptiveness to online delivery of the exercise program. This study illustrated that an online-delivered exercise program was acceptable for people with dementia and their carers in Indonesia and reinforced the importance of carers’ support for the exercise program. These findings can help physiotherapists and other exercise practitioners in considering the aspects of delivery that people with dementia and their carers value in participating in online-delivered exercise programs.
Introduction
As the population continues to age, the number of people living with dementia worldwide is expected to grow markedly (United Nations, 2015). The total number of older people living with dementia worldwide currently is 55 million and over 60% live in low-and middle-income countries (LMIC) (World Health Organization, 2023). Prioritizing dementia care policy and research is extremely important, especially in LMIC that are currently experiencing rapid population aging (World Bank Publications, 2016; World Health Organization, 2021). In Indonesia, a LMIC, there are more than four million older people living with dementia which places Indonesia ninth globally for the number of people with dementia (Farina et al., 2023). The impact of this large growth in people living with dementia is likely to be substantial in Indonesia, partly because of the limited availability of health care and support services, as well as a lack of dementia care policy and effective management strategies (Mahendradhata et al., 2017). As the majority of people with dementia in Indonesia are cared for in the community by their families, the situation may be more challenging than for those in high income countries (Kadar et al., 2013) where greater care and community support options are often available.
Participating in physical activity has been shown to be beneficial for people with dementia, however older people with dementia have low physical activity levels compared with older people without dementia (Watts et al., 2016). Exercise is a structured form of physical activity that is a low cost and effective intervention that has been shown to result in significant benefits for psychological and physical health and well-being of older people with dementia (Forbes et al., 2015). Previous studies have reported that online-delivered exercise interventions are feasible as an alternative delivery method for increasing physical activity levels of older people with dementia and their carers in developed countries (Ptomey et al., 2019; Taylor et al., 2020). For the purposes of this study, “online-delivery” refers to delivering and evaluating the exercise program remotely (online) in real-time via videoconference (Weiss et al., 2020). This approach requires no travel commitment, less cost, and offers support for carer engagement to enhance participation by the person with dementia, as well as to increase reach for those living in rural areas (Ptomey et al., 2019). As such, the potential for health professionals to deliver exercise online for people with dementia, and how this may be supported by family carers in LMIC also merits attention. Factors such as acceptability of online exercise delivery, and perceived enablers and barriers to exercise participation need to be better understood from the perspectives of people with dementia and their carers, in order to better support sustained exercise participation (Weiss et al., 2020). Online-delivery methods have also been reported as a potential method to respond to the global COVID-19 pandemic to maintain health and well-being of older people living with dementia (Goodman-Casanova et al., 2020).
It has been recognized that individuals’ perceptions are important and need to be considered when implementing health program initiatives (Linsley et al., 2011), and obtaining information from people with dementia is essential to understand their needs and preferences (Clare et al., 2008). While considerable qualitative research exists investigating perceptions and experiences of people with dementia in undertaking exercise programs face-to-face (Karuncharernpanit et al., 2016; Lindelöf et al., 2017), little attention has been given to exploring perceptions in people living with dementia undertaking an online-delivered exercise program. Other factors that also warrant consideration when delivering exercise interventions include the cultural norms of a population. There may be local factors in LMIC in Asia that limit successful translation of these programs in the contexts of culture, environment, knowledge/preferences of consumers, and health care systems compared to high income countries (Chongsuvivatwong et al., 2011; Karuncharernpanit et al., 2016). Similar to many Asian countries, in the Indonesian culture, exercise is often perceived to be equated to household chores, such as cleaning and preparing meals, and ageing is often associated with rest and an avoidance of physical activity or exercise (Karuncharernpanit et al., 2016). Dementia in Asia is also often perceived as a normal part of aging and not a neurodegenerative disease (Alzheimer’s Disease International, 2014; Patel et al., 1998). It is not clear if the cultural norms of Indonesians affect their perceptions and experiences when participating in exercise. Therefore, the aims of this study were to: (1) explore the experiences and perceptions of older people with dementia and their carers in Indonesia participating in an online-delivered exercise program, and (2) determine factors that may influence their acceptance to exercises that are delivered online.
Method
Study design
This was an exploratory qualitative study design that took a descriptive approach using semi-structured interviews with low inference interpretation of phenomenon. Low inference interpretation is an approach used when aiming to reduce the researcher influence on the data interpretation, being strongly focussed on what participants state verbatim (Goins et al., 2021; Sandelowski, 2000). This study was part of a larger study with the same study participants that evaluated the feasibility of a home-based online-delivered exercise program for community-dwelling older people with dementia in Indonesia (Sari et al., 2023a). The online-delivered exercise program was conducted between January 2021 and July 2022, a period during the COVID-19 pandemic. During this time Indonesia was alternating between lockdowns where people were restricted to home and required to adhere to social distancing rules. The online-delivered home exercise program provided an alternative opportunity to exercise due to inability to engage in exercise in their community.
Sampling and recruitment
All participants in the home-based online feasibility exercise program were eligible for inclusion in this qualitative study. Inclusion criteria for older participants with dementia in the online-delivered exercise program were: (a) community-dwelling (living in Indonesia); (b) aged ≥60 years; (c) medical diagnosis of dementia (any type); (d) mild to moderate severity of dementia (score of 7–23 on the Telephone Mini Mental State Examination (MMSE)) (Newkirk et al., 2004); (e) ability to understand/follow instructions for exercises in the Indonesian language; (f) independent mobility (with/without a gait aid, but independent of human assistance); (g) no other major neurological history/medical conditions preventing exercise participation; (h) having a carer to supervise exercises; and (i) having a computer/tablet and internet connection. People with dementia with unstable medical conditions, or speech/hearing impairments that impeded participation in the online delivered exercise program were excluded.
For the online-delivered exercise study, carers included people who provided care to an older person with dementia (including family members and/or a paid carer). A paid carer in Indonesia is a person who is paid to help the family carer to look after the older person or the person with dementia, although they usually do not have a qualification or formal training in caring for older people or people with dementia (Schröder-Butterfill & Fithry, 2014). Inclusion criteria for carers were: (a) aged ≥18 years; (b) availability to participate in online exercise sessions; (c) able to supervise the person with dementia to exercise in-between online sessions; (d) familiarity with the participant’s medical conditions; and (e) ability to communicate with the person with dementia and the researcher in the Indonesian language. Carers were excluded if they had conditions preventing them from participating in the program (e.g., physical and/or other mental illness).
In the online-delivered exercise program, participants undertook an individualized home-based exercise program for 12 weeks, comprised of four online exercise sessions delivered via videoconferencing by the researcher who is a physiotherapist. Participants engaged by using either a computer, laptop, or tablet computer. Dyads were instructed to continue the home exercises five days/week, 20–30 minutes/day in-between the scheduled online visits in alignment with recommendations set out by Lam et al. (2018). This exercise program was modified from the Otago Exercise Programme, an exercise program for prevention of falls (https://www.livestronger.org.nz/assets/Uploads/acc1162-otago-exercise-manual.pdf) to ensure safety of the dyads. Modifications included exercising with a stable chair/bench on either side to use for steadying if required and standing with a wider distance between feet as required to ensure the participant’s safety. Exercise participation was encouraged and monitored for safety by the carer, who also received training by the researcher, adapting the approach and resources used by Suttanon et al. (2013) in the first online exercise visit. After the 12-week intervention, dyads were encouraged to continue the exercises for an additional six weeks without physiotherapist online visit/supervision.
People with dementia and their carers were recruited through the Alzheimer’s Indonesia Association newsletter, mailouts to the Alzheimer’s Indonesia members including people with dementia and their carers, local newspaper advertisements, local dementia and carer support groups, hospitals, community services for older people and social media. Interested people were asked to contact the researcher for further information.
Data collection and interviews
Individual semi-structured interviews were conducted between May 2021-April 2022, within seven days of completion of the 12-week exercise program or within seven days of withdrawal from the program (where applicable). Interviews were conducted using online platforms (e.g., zoom, WhatsApp video call), audio-recorded and transcribed verbatim. Interview transcripts were then translated into English by a professional translator and checked by YMS who is fluent in English and Bahasa. Interviews were conducted in Bahasa (Indonesian language) by the researcher (YMS). YMS is a native Indonesian, and was also the physiotherapist who administered the exercise program. During data collection, YMS acknowledged their positionality as an Indonesian trained physiotherapist, with clinical experience working with older people, including people living with dementia. Throughout the project, including analyses, the project team, comprising interdisciplinary professionals (physiotherapy, exercise science and occupational therapy), reflected on their diverse backgrounds and clinical and research experience with people living with dementia. Additionaly, one team member has personal experience with a parent living with dementia, offering insights into the associated important role and impact of carers in supporting individuals living with dementia.
An interview schedule was used, which was trialled to ensure questioning flow and clarity with older adults with dementia and their carers prior to being used in the study. Copies of interview schedules are available from authors on request. Participants with dementia and their carers were interviewed separately where possible. Questions for people with dementia or their carers explored their perceptions and experiences of (a) participating in the exercise program (e.g., program intensity and perceived changes to physical function and behavior); (b) online interactions with the physiotherapist, suitability and performance of technology for participating in online-delivered exercise sessions, exercise program support and program safety; (c) barriers and facilitators to participating in the online-delivered exercise program, and suggestions/preferences for future online-delivered exercise programs; and, (d) attitudes towards exercise in general. Both family and paid carers were asked additional questions about impacts on them from supervising/monitoring the exercise program. Paid carers were asked additional questions about their role, and impact of their participation in the exercise program on their usual role or duties. Participants with dementia and their carers who withdrew from the program were asked additional questions about reasons for withdrawal and preferences for future programs.
Ethics approval
Monash University Human Research Ethics Committee (Project ID: 22163) and Health Research Ethics Committee – Indonesia (No: 2856/B.1/KEPK-FKUMS/III/2020) granted ethics approval. All participants with dementia and carers were given a participant information sheet, provided with an opportunity to ask questions and then asked to sign a consent form prior to commencing study participation. All participants with dementia were assessed for their capacity to give consent using the Participant Cognitive Capacity Checklist (Hegde & Ellajosyula, 2016). Family carers were asked to provide written consent on behalf of the participants with dementia to participate, if the person with dementia was unable to provide informed consent. Ten participants with dementia (83.3%) were able to provide consent on their own.
Data analysis
Interview data were analyzed using reflexive thematic analysis in accordance with Braun and Clarke’s (2006) six-phase process to identify themes and patterns in the data. An inductive approach was used to generate themes from the “bottom up” and based on the meanings in the data (Braun & Clarke, 2021). Two researchers (YMS and AFL) independently undertook initial coding using NVivo software (version 20) after familiarizing themselves with the data, by reading interview transcripts multiple times. Initial codes were generated by highlighting systematically relevant words, phrases and sentences across each interview to then be collated for each relevant code. Codes with the same meaning were grouped into categories and collapsed to form themes (Braun & Clarke, 2022). Both researchers met several times to reflect on codes and the development and refinement of themes. The coding schedules and initial themes were also discussed with a third researcher (KH) to compare and collate analyses, leading to refinement of final themes. Quotes from the participants verbatim statement have been edited for grammar and readability.
A thematic map was developed to organize and establish the relationship among themes (Novak & Alberto, 2007). Analyses then included further discussion and review of the data and identified themes by the research team (YMS, AFL, KH, EB) and by maintaining detailed records of coding and theme development decisions (Shenton, 2004). All authors provided feedback before the confirmation of the final thematic map to generate the report.
Findings
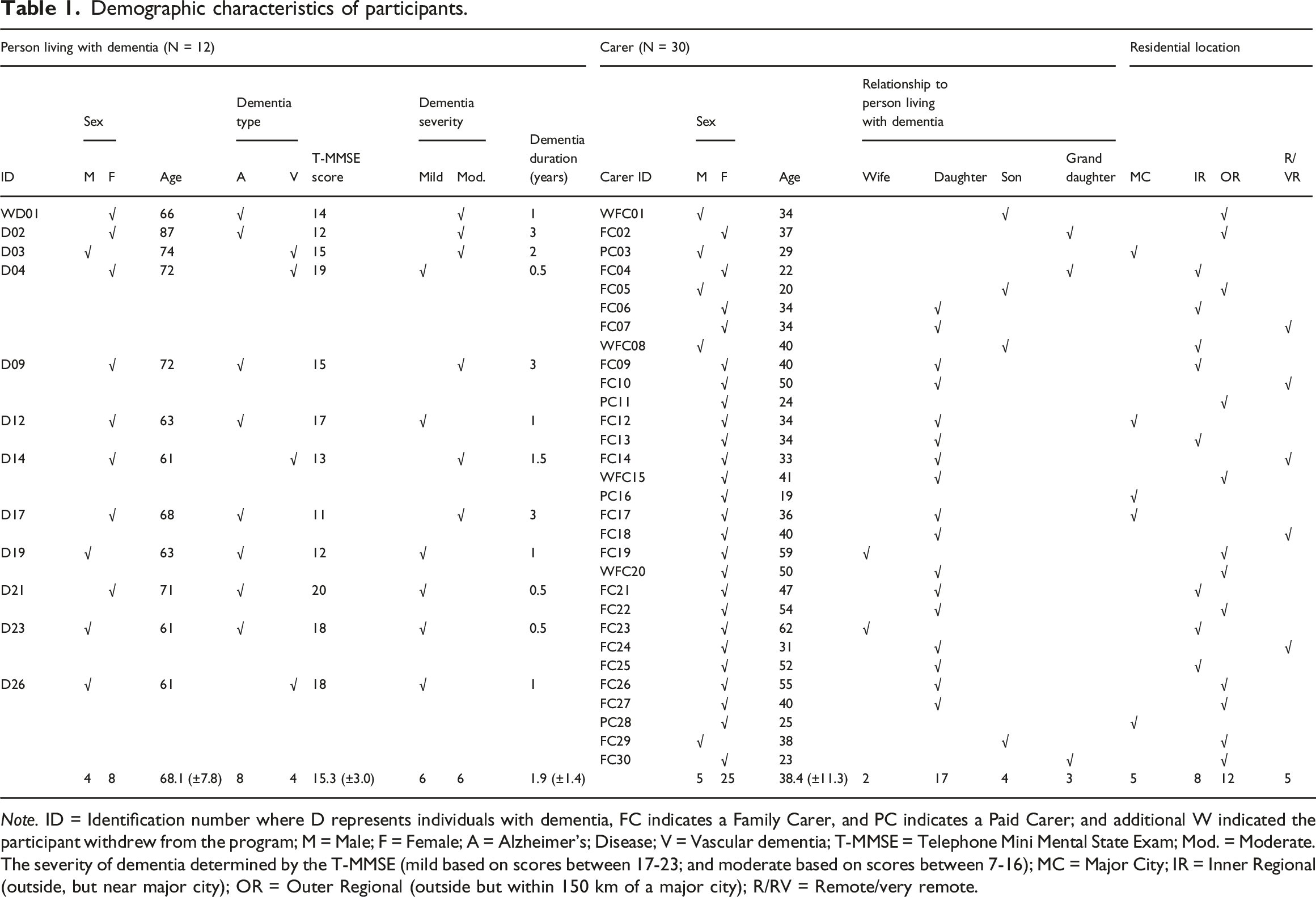
The flow diagram of participant recruitment, withdrawals, and exclusions is shown in Figure 1. In our feasibility study from which participants for interviews were recruited (Sari et al., 2023a), 30 people with dementia and their 30 family carers, and 10 paid carers were involved. Of these, only 12 of the 30 people with dementia were deemed able to participate in the interview process, while 26 family carers, and 4 paid carers involved in part or all of the 12-week online-delivered exercise program were interviewed. Five interviewees, one person with dementia and four family carers, did not complete the exercise program and withdrew at weeks 5, 7, 8, and 10 of the exercise program. All participants with dementia and their carers were interviewed separately. Most participants with dementia were female (66.7%) with an average age of 63.3 years (range 61–87 years). Carers were predominantly family members (86.7%) and female (83.3%) with an average age of 37.9 years (range 19–62 years). Interview duration for persons with dementia ranged between 19–39 minutes and 24–42 minutes for carers. Most participants lived in outer regional areas (outside but within 150 km of a major city) (n = 12, 40%) or remote and very remote areas (n = 5, 16.7%). Details on participant demographics are shown in Table 1. Flow diagram of recruitment and exclusions. Demographic characteristics of participants. Note. ID = Identification number where D represents individuals with dementia, FC indicates a Family Carer, and PC indicates a Paid Carer; and additional W indicated the participant withdrew from the program; M = Male; F = Female; A = Alzheimer’s; Disease; V = Vascular dementia; T-MMSE = Telephone Mini Mental State Exam; Mod. = Moderate. The severity of dementia determined by the T-MMSE (mild based on scores between 17-23; and moderate based on scores between 7-16); MC = Major City; IR = Inner Regional (outside, but near major city); OR = Outer Regional (outside but within 150 km of a major city); R/RV = Remote/very remote.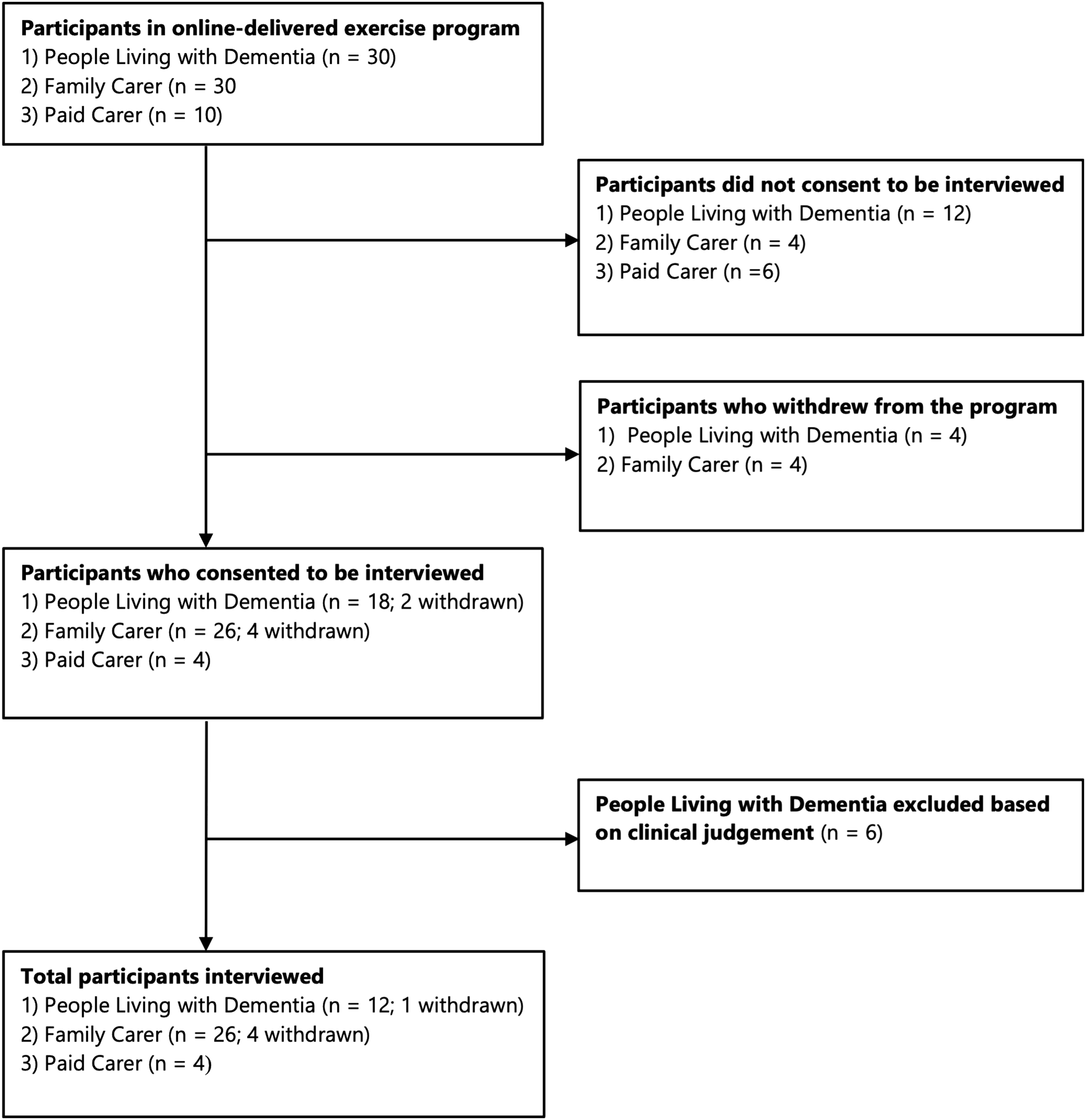
Seven themes were identified: (i) Motivating factors to participate; (ii) Benefits for people with dementia; (iii) Impacts on carers; (iv) Challenges and enablers to exercising; (v) Carer’s strategies for exercise engagement; (vi) Roles, relationships and supports; and (vii) Participants’ receptiveness to online delivery of the exercise program. Figure 2 illustrates the concept map of themes and sub-themes from the interview data and illustrative quotes for themes and subthemes are presented in the text below, with additional quotes provided in Table 2. Thematic map. Themes, subthemes and additional illustrative quotes from participant interviews.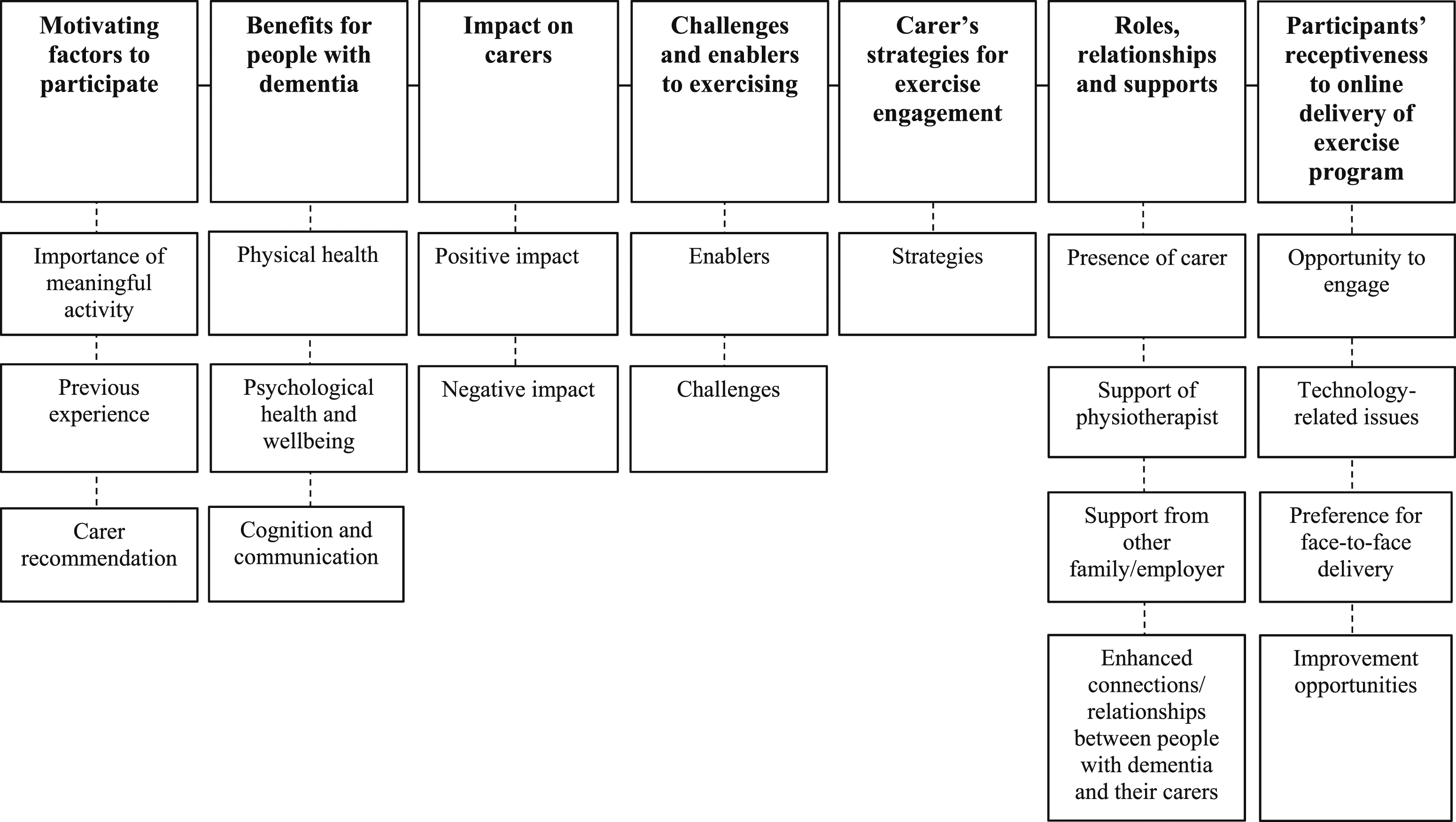

Theme 1: Motivating factors to participate
Participants, both people with dementia and their carers, identified similar factors motivating them to participate in the exercise program, with people with dementia also reporting additional motivators.
Importance of meaningful activity
Participants with dementia and their carers highlighted their belief that exercise was important and had benefits to people with dementia as their common motivation to participate in/supervise the exercise program. People with dementia also noted they were looking for activities that could be completed at home but were not able to find activities they could engage in, and therefore the exercise provided such an opportunity. “I thought that this program should be good for my health, and I want to join some activities, so I have some activities at home” (D19). A few family carers also mentioned they had been looking for a program for the person with dementia that they care for to participate in: “This is an activity I wish I could join from a long time ago and finally had a chance, especially in this COVID-19 pandemic and living in a small city where Physiotherapy is not common” (FC14). Additionally, the impact of the COVID-19 pandemic, particularly social isolation, was identified as a motivating factor to participate in the exercise program. Participants highlighted the need for alternative activities to keep them active while being restricted to staying at home.
Previous experience
Participating in previous exercise programs or exercise-related activities by people with dementia were factors for their motivation to participate in the exercise program: “I used to do jogging and join some exercises in a community centre for older people, and I would like to keep being active” (D21).
Carer’s recommendation
A number of participants with dementia mentioned their reason for participating in the exercise program was due to their family carer feeling it would benefit them or asking them to participate. “Actually, my wife was the one who informed and asked me to join this program and I thought this should be good to try” (D19).
Theme 2: Benefits for people with dementia
Participants with dementia and their carers identified some effects from the exercise program on physical and psychological health and wellbeing, and cognition for the person with dementia.
Physical health
Both people with dementia and carers identified benefits of the exercises on the physical health of the person with dementia, including feeling healthier, having better mobility and balance, reduced joint pain, improved flexibility, and increased functional independence. One person with dementia reported: “I feel a lot better and stronger now because I use my muscles a lot when exercising” (D03), while a carer stated: “I can see that she has been looking fresher and more energetic” (FC05).
Psychological health and wellbeing
Positive psychological changes of the person with dementia were identified by all participants. People with dementia reported feeling happier and excited, along with improved mood, appetite, and sleep. “I think my mood became better. I feel that I have been more passionate in doing that and other activities” (D12). Many of the family and paid carers also highlighted positive changes in care recipients’ behavior and psychological health including becoming less upset and having a brighter mood: “She has better behavior, less grumpy, looked energetic and happy now, it was together with her improved physical health, I think” (FC07).
Cognition and communication
A number of family and paid carers mentioned noticing improved cognition of their care recipient, particularly memory and communication. They also noted better ability for the person with dementia who they care for being better able to understand and respond to instruction. “Her memory and speech are now more eloquent, understandable, even though sometimes it doesn’t make 100% sense. She used to lose that ability, she cannot communicate well. Now we can tell her what to do slowly and she understands” (FC07), while another carer stated “He’s getting better in receiving and following instruction, he also responded well on the simple commands like, “let’s take a shower” “stand up” “let’s eat” and he responded like “what will we eat?” His ability to respond is getting better” (PC03).
Theme 3: Impacts on carers
Some carers reflected on the effects on themselves as a result of supporting someone with dementia to participate in the exercise program.
Positive impacts
Both family carers and paid carers reported being more patient and compassionate in caring for someone with dementia. They also highlighted becoming more understanding with the person with dementia, their condition and needs. Some family carers further identified being less worried to look after their care recipient, making them feel less stressed: “Now I feel more confident and less worried in looking after my Mom because she improved well, I also become less stressed out playing this role as a carer” (FC18).
Negative impacts
While some family and paid carer’s stress reduced, others expressed distress, increased stress and exhaustion having to assist the person with dementia in the exercise program. Paid carers did however also acknowledge that despite the stress on them, it was worth it to see the benefit of participating for the person with dementia. “I guess I got more exhausted. Usually she doesn’t want to move by herself and asks me to hold her when she tried to stand up, or when she doesn’t want to move, she’d just lean her full weight on me and that could make me tired. But seeing all the good impacts on her makes me happy too” (PC28).
Theme 4: Challenges and enablers to exercising
Challenges
People with dementia and their carers identified some barriers in undertaking the exercise program. Various factors for not wanting to exercise were expressed by people with dementia, including body pain, difficulty with some movements, or forgetting movements. Both family and paid carers highlighted the behavior of the person with dementia, including their mood, as challenging sometimes resulting in refusal to exercise. Some paid carers also expressed frustration, with one highlighting: “the challenge I found was sometimes she forgot the movements and I have to remind her again and again” (PC11). Carers, particularly family members, also acknowledged their own time and availability impacted their ability to support the person with dementia in participating in the exercise program. “The thing might be my availability as it was sometimes hard to find a time to help my Mom because of my other commitments” (FC12). People with dementia also reported challenges associated with doing the exercises, including: “There are some movements that are a bit challenging for me like turning around” (D09), and “Sometimes I just did not want to do that, was not in the mood to do that, or when I was tired” (D02)
Enablers
Most of the family and paid carers acknowledged the challenges in doing the exercise could be minimized, or avoided, depending on how receptive or compliant the person with dementia was. “I found no challenge at all; I think because my mother was willing and happy to do it. It will be a different story if she was reluctant to do it” (FC07). Some family carers also mentioned that additional support from a paid carer to motivate the person with dementia in the exercise program was beneficial. “The thing that really helpful was I have a paid carer who also helped me in supporting my mom to do the exercise” (FC10). People with dementia also expressed receptiveness to exercise that was linked to the reassurance and prompting provided by their carer. One person with dementia stated: “I usually forget about the movement and sometimes I forget that I need to do it (the exercise) that day, but my daughter always helps and reminds me, so all was good because of her” (D12).
Theme 5: Carer’s strategies for exercise engagement
Family and paid carers highlighted developing strategies that assisted them to support people with dementia including instructing the exercise, initiating/giving example of the exercises, correcting movements, or reminding and inviting the individual to do the exercises. Some carers also noted some strategies for maintaining adherence of the program, including sharing the carer role with another person “because I have no spare time for something else, I switch with my sister in helping my Mom doing the exercises. So, we just share responsibility to maximize our support to my Mom and maintaining her participation” (FC05). Persuading the person with dementia to do the exercises and being more patient in supporting the person with dementia was also noted by some family and paid carers as strategies for maintaining adherence to the exercise program “It needed extra effort from us as the carers to invite him (participant with dementia), [we] (i.e., carers) should be more patient, (we need to) stabilize our mood also, otherwise we can be stressed out and will not be able to continue the program” (FC25).
Theme 6: Roles, relationships and supports
Presence of carer
All participants with dementia reported feeling supported and safe while undertaking the exercise program due to the presence, assistance and availability of their family and/or paid carer while they were exercising. One person with dementia noted “Yes, I feel safe as my wife [was] always there with me, helping me. You [physiotherapist] also told my wife how to do the exercise correctly and safely” (D19).
Support of physiotherapist
In addition to the reassuring presence of their carer, participants with dementia acknowledged the support from the physiotherapist who delivered the exercise online. “I also feel supported from you. You always visited (online), reminded, and taught me about the exercise” (D21). Physiotherapist support was highlighted across a number of formats, including the exercise session with the physiotherapist, ability to consult directly and specifically with the physiotherapist, and also the prompts and instructions about the exercises provided by the physiotherapist. Both family and paid carers also reported feeling reassured they were supporting their care recipient correctly and safely due to the physiotherapist’s advice in undertaking the exercise as it was conducted, as well as additional guidance provided via the exercise booklet, diary and video availability.
Support from other family/employer
Some family carers mentioned they received support from other family members, and some paid carers mentioned they received support (e.g., technology support) from their employer (i.e., the family carer of the participant with dementia) in supervising the exercises. “All of my siblings support us in doing this exercise program and we are always sharing her (participant with dementia) progress in this exercise program and changes to her health condition” (C06).
Enhanced connections/relationships
Several people with dementia expressed the joy they got from the exercise program as it meant they spent more time together with their carers. “I do that together with my daughter who always helps me with the exercise. So happy that I spent more time with my daughter” (D09). Many family and paid carers also acknowledged better connections between them and the person with dementia they care for, either during the program or as a result of the program. “I got additional experience between me and the person I look after and it makes our relationship even better” (PC03). As a result of a better relationship between them, family carers felt the person with dementia seemed happier and more responsive to them when they had time together, in addition to improved relationships between all family members as a result of participating in the exercise program.
Theme 7: Participants’ receptiveness to online delivery of exercise program
Opportunity to engage
Almost all participants, both people with dementia and their carers, mentioned having a positive experience using the videoconferencing platform to deliver the exercise program. Most people with dementia said the exercise program was good and suited their needs. “I think this is already good enough and suits me” (D04). Both family and paid carers also acknowledged similar recognition of the program: “This is a really good program for sure, with positive experience as well” (FC07). Most participants reported that the online delivery enabled opportunity to exercise conveniently at home, particularly due to Covid implications. “We can do (exercise) at home without traveling outside, we also can save our time and (this is) also safe for my Mom in this Covid situation” (FC17).
Technology-related issues
Most participants experienced little or no issues using technology to access the exercise program. However, a few family carers and people with dementia experienced problems with the online exercise approach, including internet connection issues, visual issues, and audio issues: “I think just a little problem on the signal sometimes” (FC25); and “I think I had several times that I cannot hear you (physiotherapist) clearly” (D03). However, all mentioned any issues were minor and did not impact their overall participation. “That was just a very small problem, and it did not bother me” (D03). Individuals with dementia highlighted they could only attend the online exercise sessions because the family carers assisted them with technological requirements. “I do not think I have any problem with that because my daughter always helped me. But without my daughter, it might be a lot of problem” (D09). Paid carers similarly mentioned the support of their employer (family carers) to assist them with the technology. A small number of people with dementia initially reported feeling unusual when exercising through the technology modality, but this resolved as they became more used to the online-delivered exercise program.
Preference for face-to-face delivery
Despite the benefits of the online delivery method used, especially in the COVID-19 situation, many people with dementia and their carers mentioned their preference for face-to-face delivery of the exercise program. “I think it helps me a lot in this kind of situation but if I can choose, I prefer face-to-face” (D23). Persons with dementia noted various reasons for preferring face-to-face, including “[With face-to-face method] I can communicate with the experts, can go outside and socialise with other people. Sometimes there are some limitations if we just meet online and not seeing each other” (D03). Several participants with dementia, and both family and paid carers highlighted having a hybrid delivery including both face-to-face visits with online could be helpful in the future. “Maybe it will be good in the future if there is no longer a pandemic, the program could be made available combining online with face to face” (FC05).
Improvement opportunities
A few participants with dementia suggested having music while exercising: “Probably movements with music will help to improve the participation. I like some songs but it was really hard to find it now” (D02). Family carers also suggested a video recording of each exercise for subsequent review, particularly when the physiotherapist was not available, as well as ongoing, frequent supervision from the physiotherapist subsequent to completion of the formal exercise program to aid adherence.
Discussion
In this study, experiences, perceptions and factors that influenced the acceptance of an online-delivered exercise program were explored with people living with dementia and their carers in Indonesia. While there is growing evidence exploring participants with dementia’s experience in participating in exercise programs (Karuncharernpanit et al., 2016; Lindelöf et al., 2017), limited evidence was found in Indonesia and other developing countries in Asia (Sari et al., 2023b).
Participants acknowledged benefits of the online-delivered exercise program on physical and psychological health of the people with dementia. The benefits reported in this qualitative study align with objective outcomes from this study (Sari et al., 2023a), including improved physical activity levels, improvement in some aspects of function and disability, exercise enjoyment and quality of life. Other studies on online-delivered exercise programs have also reported benefits, including increasing levels of moderate physical activity in both people with dementia and their carers (Ptomey et al., 2019) and improved falls efficacy for the person with dementia (Taylor et al., 2020). Even though this online exercise program was conducted during the height of the COVID-19 global pandemic, this approach is likely to be a suitable longer-term option beyond any remaining impacts of the pandemic. It may be useful for some older people who will have ongoing reluctance to resume interactions for physical activity participation that involve being away from home or older people who are living in rural areas in Indonesia.
While some carers mentioned the positive impact of supervising the exercise including being more patient and compassionate in caring for someone with dementia, negative impacts were also reported, including distress and exhaustion. Other studies have also found people with dementia often have more care needs (Wang et al., 2022), and that families or carers of people with dementia often experienced more distress, were more vulnerable to suffering from anxiety and depression, and potentially suffer more physical health problems than families or carers of people without dementia (Liu et al., 2017; Pinquart & Sörensen, 2003).
People with dementia stated they felt supported by both their family and paid carers presence and identified that the exercise program also enhance their relationship between each other. Family have been described as the “most important support system for older people in Indonesia” (Kadar et al., 2013). Some factors including the filial piety notion in most countries in Asia, including Indonesia, mean the family and relatives of older people are often more willing to care for older people at home and the care is organized by the joint family system (Wang et al., 2022). A study in China found that 80% of people with dementia are looked after by their families at home (Xiao et al., 2014). In our main feasibility study (Sari et al., 2023a) from which the interviewees were recruited, a third of the people with dementia also had a paid carer supporting their care at home, including supporting their participation in the exercise program. Research in China shows that having a paid carer or adding the number of helpers looking after the person with dementia reduces the impact experienced by a sole family carer (Wang et al., 2022). Overall, interview responses of carers were generally similar whether they were a paid carer or unpaid family carer. Additional supports to family carers of people with dementia such as employing a paid carer may assist with family carers’ high level of anxiety and depression, and provide additional resources to enable participation by the person with dementia in additional activities, such as exercise programs. However, having sufficient resources to fund a paid carer position is a challenge for a high proportion of families in Indonesia because of the low socioeconomic status of much of the population (Abia Asha & Juliannisa, 2023). There is a need for further research investigating the use, roles and outcomes associated with paid carers for people with dementia in Indonesia.
This current study highlights some challenges in participating in this online-delivered exercise program by people with dementia, including physical, functional and other limitations associated with comorbidities, forgetting movements, or not wanting to exercise. Barriers to exercise in people with dementia have been identified previously, including people with dementia’s perspectives about exercise, memory impairment, limited support, lack of knowledge how to exercise and fear of injury (Freeman et al., 2022; Watts et al., 2016). Carers highlighted the behavior of the person with dementia, including their mood, as challenging sometimes resulting in refusal to exercise. Cheng (2017) suggested that the most common challenges experienced by carers of people living with dementia relate to Behavioral and Psychological Symptoms associated with Dementia, as they can substantially contribute to distress for the carer. A study by Royse et al. (2023) identified that positive social influences and the desire to spend time with family members can mitigate the challenges of older people in engaging in exercise. The factors in motivating older people to exercise can inform future programs in designing the online-delivered exercise program for people with dementia.
This study also identified enablers to participating in the exercise program, including carer availability and support in exercise adherence and motivation of the program. Previous studies indicated that support from carers is an essential part of successful program participation for people with cognitive impairment and dementia (Suttanon et al., 2013; Taylor et al., 2004). An ethnography study also identified that caring for older parents or family members is a cultural duty for all family members in Indonesian society, which is also in line with religious values (Schröder-Butterfill & Fithry, 2014). Being a caregiver of their loved one in Indonesia might be interpreted as gratitude and as a natural consequence of kinship ties and moral values (Putri et al., 2022).
People with dementia and their carers were receptive to online delivery of the exercise program in this study. They perceived they had an opportunity to engage despite living in rural areas and during the COVID-19 pandemic. COVID-19 has left many older people, including those with dementia, restricted to home, with few resources and limited opportunities to participate in physical activity or exercise in the community (Goethals et al., 2020; Prevention, 2019), and online-delivered exercise programs have been recognized as providing an opportunity for exercise to be initiated and continued within the home, despite the barriers imposed by the pandemic (Goodman-Casanova et al., 2020). Participants with dementia and their carers also felt supported in this exercise program and valued the additional guidance provided via the exercise booklet, diary and video availability. The acceptability of the exercise programme is consistent with findings from other studies in developed countries. Taylor et al. (2020) reported that an individualized tailored exercised program delivered through tablet computers was acceptable and scored well on enjoyment for older people with dementia in Australia.
An interesting finding in our study was that while the majority of participants with dementia and their carers perceived that exercise delivered by the online-delivery method was acceptable and met their needs, they preferred to have a face-to-face delivery or have face-to-face visits as part of the program, especially if the COVID-19 pandemic was controlled, so they could meet the physiotherapist and communicate directly. This preference also aligned with a study by Lindelöf et al. (2017) for people with dementia who resided in nursing homes. They identified meeting exercise supervisors individually or meeting other people in the group exercise program was beneficial because they experienced feelings of being understood, seen and respected. Having a face-to-face meeting with physiotherapists and other peers in group exercise may improve their motivation and self-efficacy in participating in the exercise program and is worth considering incorporating into future hybrid online exercise programs. In addition, participants with dementia in this study reported not being able to participate in this program without the carer’s assistance in digital skills. Carers in this study generally managed the technology well, with some guidance from the physiotherapist through the online communications and initial orientation session. However, lower levels of digital literacy and skills, and reduced access to computers and stable internet may impact this online exercise approach being widely implemented across Indonesia and other LMIC. A study in India by Rasekaba et al. (2022) demonstrated the low rate of digital and health literacy, and low use of the internet to contact health professionals. They also found that low digital usage was potentially due to limited exposure and confidence in using digital devices and physical aspects of ageing, like poor vision.
Strengths and limitations
There were several strengths to this study. This is the first study in Indonesia to explore experiences of older people with dementia and their carers participating in an online-delivered exercise program, and carers who participated in this study were reflective of the common care arrangement seen in Indonesia, being a mix of family carers and paid live-in carers. In addition, the interviews were conducted by the primary researcher who is a native Indonesian who has an understanding of the cultural sensitivities in Indonesia. A limitation of this study was that participants were limited to those who could afford the relevant technology and internet access, and had sufficient digital skills to navigate the internet, which may limit generalisability of study findings in Indonesia. The authors also acknowledge reliability of the findings may be limited given the interviewer was the same person as the physiotherapist involved in delivering the intervention. While participants in the interviews may have responded differently with an independent interviewer, it is noted that the responses obtained were not solely favourable, with some carers highlighting the added workload, and preference for the program to be face-to-face, indicating participants were able to respond in an open manner with the interviewer about their experience. To offset any potential bias to some degree, the interviewer focussed on being as objective as possible with questions and prompts during interviews, and an independent coder reviewed all English transcripts in depth.
Conclusion
This study provided important insight on the experiences of older people with dementia and their carers and illustrated that an online-delivered exercise program was acceptable for people with dementia and their carers in Indonesia and reinforced the importance of carers support in the exercise program. The findings can help physiotherapists, exercise physiologists, and other health professionals in delivering online exercise programs to older people with dementia and their carers. It highlighted some challenges and enablers in undertaking exercise by people with dementia and their carers via this method. Future studies may consider using a hybrid format i.e., combining online with some face-to-face sessions in delivering exercise programs and examining the benefits of this mode of exercise delivery.
Footnotes
Acknowledgements
We would like to thank all participants involved in this study and Alzheimer’s Indonesia for their support in the recruitment process of this study.
Declaration of conflicting interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Dr Yulisna Mutia Sari was funded by an Australia Awards Scholarship for her PhD study and Associate Professor Elissa Burton was supported by a National Health and Medical Research Council Investigator Grant.
Ethical statement
Data availability statement
The data underlying this article cannot be shared publicly due to the privacy of individuals that participated in the study. The deidentified interview data can be made available on reasonable request to the corresponding author.
