Abstract
Background
Population ageing in low and middle-income Asian countries is associated with increased prevalence of dementia. The proportion of people with dementia in countries such as Bangladesh and Thailand are increasing. People with dementia can have complex care and health service needs. If these needs are not adequately met, this can result in a decreased quality of life and burden on the health system. There is considerable research into the needs of people with dementia in high-income countries. However, research on the needs of people living with dementia in low and middle-income countries remains underexplored. The aim of this study was to review and summarise the literature on the health and social care needs of older people with dementia in low and middle-income Asian countries.
Methods
Five online databases (PubMed, Scopus, Web of Science, CINAHL and PsycINFO) and google scholar were searched. The databases were searched using a selection of key words. PRISMA-ScR approach was followed in reporting the process.
Key findings
We extracted eight studies related to the health and social care needs of people with dementia that met our inclusion criteria. From the available literature, needs were categorised across five categories: (i) social, cognitive, and mental health needs; (ii) physical needs; (iii) care and service needs; (iv) knowledge-related needs; and (v) spiritual care needs.
Conclusion
While eight papers were located which discussed the needs of people with dementia across a range of domains, this review demonstrates a deficit in the current evidence-base about the health and social care needs of people living with dementia in low and middle-income Asian countries. Further research is needed to identify health and care needs of people with dementia and how these needs are being met.
Background
Population ageing is a growing concern. Data shows, globally, there were 703 million older persons (60 years and above 1 ) in 2019 (UN, 2019b). It is projected that number of older persons worldwide will be more than double by 2050, reaching over 1.5 billion persons (UN, 2019a). While population ageing was initially most evident in higher income countries, more recently it is low and middle-income countries (LMICs) that are experiencing the greatest change (WHO, 2022b). By 2050, two-thirds of the world’s population, aged over 60 years, will live in low and middle-income countries (WHO, 2022b).
Ageing is a predominant risk factor for many diseases such as cancer, cardiovascular disease, and neurodegenerative conditions such as dementia (Niccoli & Partridge, 2012). Stephan et al. (2018) in their longitudinal study reported that older age is related to a higher likelihood of developing dementia. Commensurate with population ageing and population growth Nichols et al. (2022) estimates that globally the cases of people with dementia will increase to 152·8 million by 2050 from 57·4 million in 2019. Nichols et al. (2022) also reported that the number of people living with dementia will increase in all regions of the world, but East Asia along with North Africa and the Middle East will experience the largest increase. Additionally, Mukadam et al. (2019) reported that the proportion of dementia cases at LMICs in Asia such as India (41.2%) and China (39.5%) were higher than their previous worldwide estimate (35%).
Dementia has significant impacts in terms of medical and social care costs, as well as informal care costs (WHO, 2022a). There is considerable literature that reports on the needs of people with dementia from research conducted in Western and developed Asian countries (Cataldi et al., 2023). However, the findings of such research may not reflect the needs of people living in LMICs. Indeed the availability of services, varying diagnostic approaches, and stigma associated with dementia in low and middle-income Asian countries are likely to influence the needs of this population (Gauthier et al., 2022). Given the projected increases in the number of people living with dementia in Asian LMICs, understanding the needs of this population is necessary if their health and social care needs are to be adequately met. A pragmatic decision was made to focus only on literature from Asian LMICs, as this scoping review also informed a study focused on understanding the needs of people with dementia in Bangladesh.
The concept of need can be understood as that which enables a person to achieve, maintain or restore an acceptable level of social independence or quality of life (Meaney et al., 2005). Understanding the needs of older people living with dementia is necessary for ensuring their quality of life and development of responsive care services (Abdi et al., 2019). In literature from high income countries, the range of needs that have been reported for people living with dementia are diverse and include physical, social, and cognitive domains. For example, a Canadian study by Khanassov et al. (2021) identified self-reported needs of people with dementia living in the community related to memory, physical health, eyesight/hearing/communication, and the ability to undertake instrumental activities of daily living (such as looking after the home and managing money). Miranda-Castillo et al. (2013) in their UK study, reported that food, memory and activities of daily living are the most common needs. Park et al. (2021) in a South Korean study found that memory problems, financial hardship, a lack of daytime activities, and social isolation were frequently reported needs.
An unmet need is defined as a situation in which an individual has a need for which an intervention exists, but the individual does not, or cannot, access the intervention (Herr et al., 2014). Research in Western countries such as Ireland (Meaney et al., 2005) and the United States (Cohen-Mansfield et al., 2015) have identified high levels of unmet needs in behavioural and mental health domains, social interaction, loneliness and meaningful activities. Unmet needs in physical, psychological, or social domains can contribute to behavioural and psychological symptoms of dementia and lead to decreased quality of life (Miranda-Castillo et al., 2010). In addition to unmet needs for social interaction, Mazurek et al. (2019), in research conducted in Poland, also found that people living with dementia frequently had unmet needs associated with carrying out activities of daily living and psychological distress. Gorska et al (2013) found that people with dementia in the UK had unmet needs related to early diagnosis, post-diagnostic support, and interventions to support social engagement. However, for less developed Asian countries, Zhang et al. (2021) also reported that unmet needs of the person with dementia often centre on social needs (company and intimate relationships) and assistance with looking after their home, self-care, and caring others (usually grandchildren). Lim et al. (2012) suggested that issues with service utilisation, could be due to lack awareness of available services.
A recent report commissioned by Alzheimer’s Disease International (Gauthier et al., 2022) that addressed global issues with post diagnostic support for people with dementia, highlighted the importance of care being tailored to the needs of individuals within their cultural, social and health care contexts. It is an imperative to understand the needs of people living with dementia in low and middle-income Asian countries if post diagnostic and longer-term care is to adequately meet the needs of people with dementia and their family members. Hence, this paper addresses the following scoping review question: What are the health and social care needs of older people living with dementia in low and middle-income Asian countries?
Methods
This review followed the methodological framework of Arksey and O'Malley (2005) for scoping reviews. Reporting of the evidence was based on “Preferred Reporting Items for Systematic reviews and Meta-Analyses extension for Scoping Reviews (PRISMA-ScR) checklist (Peters et al., 2021).
Data sources and search strategy
Five electronic databases (PubMed, Scopus, Web of Science, CINAHL and PsycINFO) were searched. In addition, hand-searching of reference lists of included studies was carried out. The searches were conducted between August 2019 to April 2020. Key terms used for searches were older, aged, dementia, Alzheimer disease, lower middle-income countries, health, and social care needs. Search terms were categorised into four concepts: i) aged, older; ii) geographic focus; iii) dementia; iv) needs. MeSH (Medical Subject Headings) terms, Extenders and SmartText were also applied during searches. Details of the search strategy and key terms are made available in Supplementary Materials.
Eligibility criteria
The scoping review applied the following inclusion and exclusion criteria.

Screening
Search results were managed using EndNote and Microsoft Excel. After removing duplicate records, initial screening of all titles and abstracts was carried out by the first author (JM), and reviewed by a second member of the research team. Documents were excluded based on criteria detailed in Table 1. Any disagreement between the reviewers was resolved by discussion amongst all four reviewers until consensus was reached. Full text review of the remaining papers (182) was carried out by the first author (JM) and reviewed by the fourth author (Sharon). Studies were excluded because they did not meet one or more inclusion criteria, or at least one of the exclusion criteria applied. Several of the excluded studies were not in the Asian context or did not focus precisely on review topic or belonged to a high-income bracket. Further manual searching of the reference lists was carried out for the selected eight publications and no additional papers were found. The same inclusion and exclusion criteria were applied while undertaking a manual search of the reference lists. Data was extracted from studies selected for this review using a data-extraction chart designed by the first author (JM) and reviewed by the research team.
Data extraction
The following information was extracted from included papers: author and year, study objectives, setting or context of the study, study population, sample size, time of study, design of the study, and key findings. When papers reported on multiple objectives, only information related to the needs of older people with dementia was extracted. In papers where data on the needs of a person with dementia was reported from a dyad (person with dementia-family caregiver), only data that could be identified as coming from the person with dementia was extracted. If data could not be traced back to the person with dementia, then the paper was excluded. Needs related categories were identified while extracting the data. To ensure clarity and quality, these categories were reviewed by the author’s team. New categories were created where findings did not fit with existing categories. For example, the need of spiritual carewas identified in one paper, and was clearly linked to the impact of dementia. Ithad significance in relation to cultural background of the participants and thus warranted a discrete category. All data are reported in tabular and narrative format. Based on the advice from Munn et al. (2018, p. 3) “scoping reviews do not aim to produce a critically appraised and synthesised result/answer to a particular question” but rather aim to map the evidence of an emerging field. In such an endeavour there is no requirement to assess the quality of the publications. Thus, there was no critical appraisal undertaken of the quality of literature.
Results
The search of five databases produced 1495 records/publications and 113 records were returned from google scholar for a total of 1608. The records comprised peer-reviewed publications, editorials, commentary papers, policy papers and protocols. After removing duplicates, 1400 records remained. Initial screening of titles and abstracts excluded 1218 publications as these did not meet inclusion criteria. Full-text screening of the remaining 182 publications yielded eight primary research papers which were eligible for inclusion in the review (Figure 1). Study populations included older people with dementia and health professionals. Five studies were conducted in urban settings, one in a rural setting, and two in both rural and urban contexts. Geographic locations of the studies were China, India, Pakistan, and Malaysia. Quantitative research methodologies (3 survey and 1 cohort study) (Bao et al., 2019; Liu et al., 2009; Nikmat et al., 2015; Prince et al., 2011) accounted for half of the studies included in this review. Four studies (Asghar et al., 2018; Lian et al., 2017; Willis et al., 2020; Wu et al., 2016) were qualitative in approach. PRISMA-ScR reporting flow chart.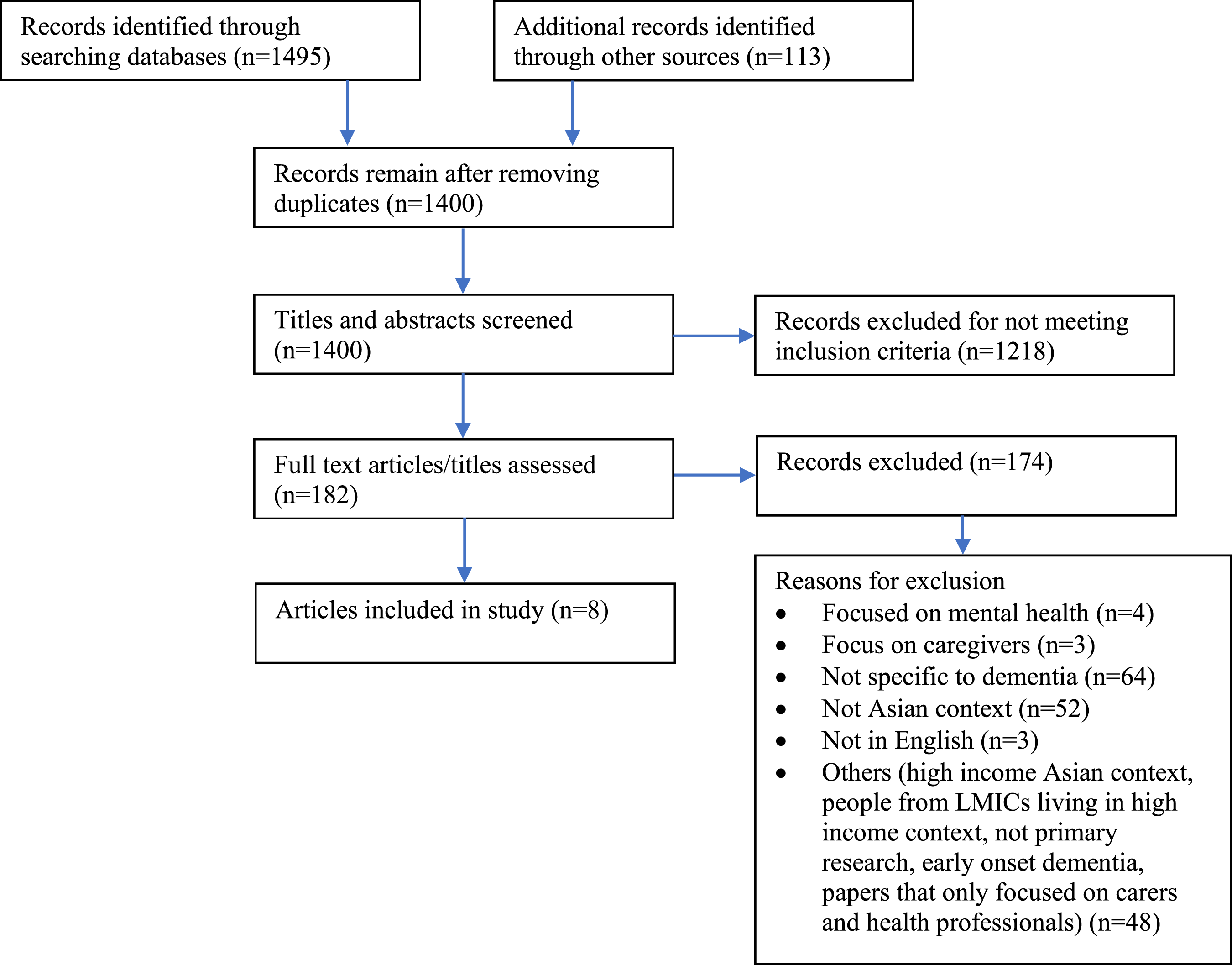
Key findings
A range of key needs of older people with dementia were reported (Table 2). Here we report these under five categories: (i) social, cognitive, and mental health needs; (ii) physical needs; (iii) care and service needs; (iv) knowledge-related needs; and (v) spiritual care needs. Some studies reported multiple needs and as such are reported across more than one category. (i) Social, cognitive, and mental health needs Characteristics of selected studies.
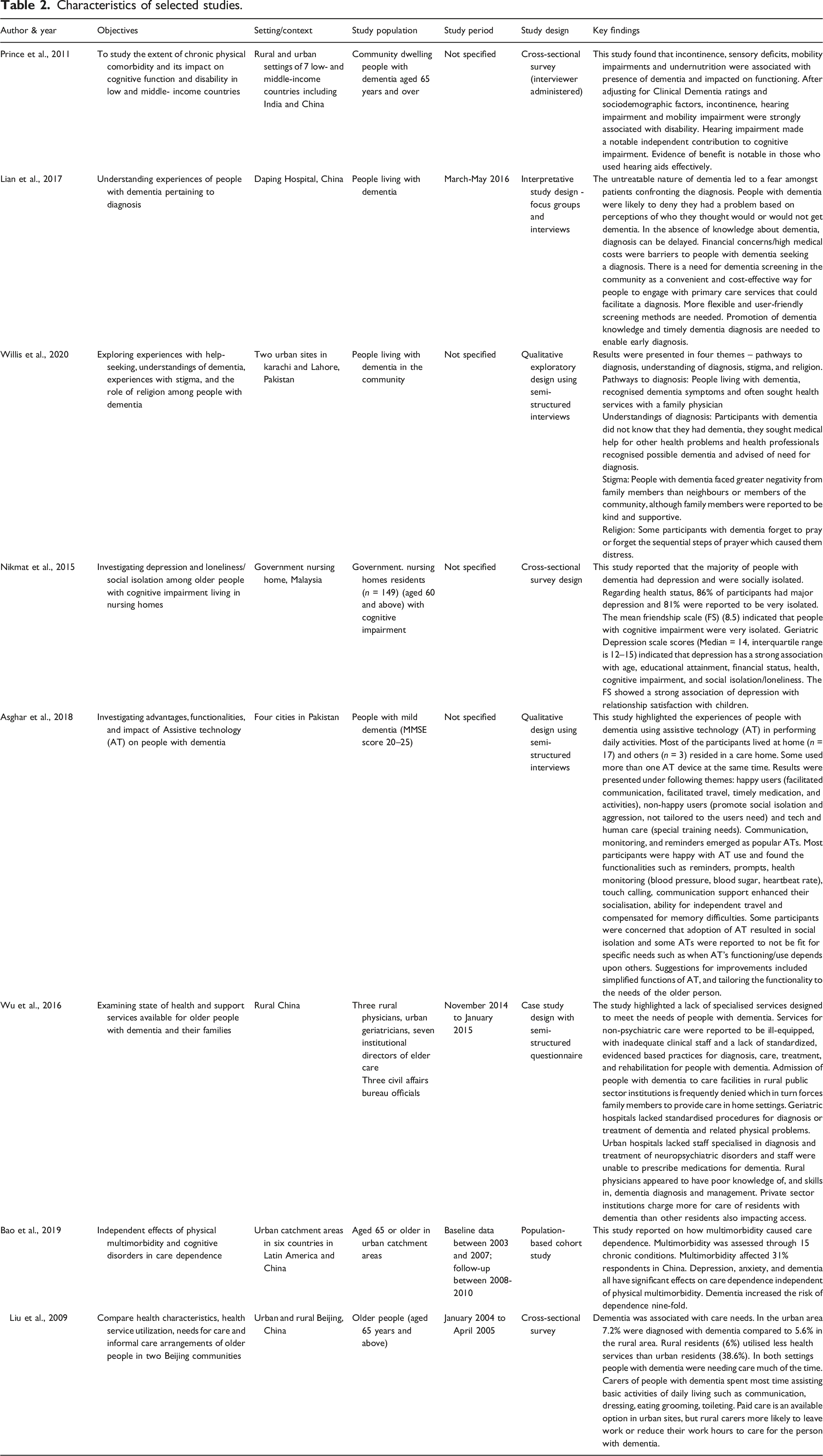
Two studies (Asghar et al., 2018; Nikmat et al., 2015) reported on social, cognitive, and mental health needs of people with dementia. Nikmat et al. (2015) investigated social and mental health needs among older people with cognitive impairment living at government nursing homes in Malaysia. The authors (Nikmat et al., 2015) reported that people with cognitive impairment were socially isolated and had high rates of depression, as assessed by a self-reporting Geriatric Depression Scale. Depression was strongly associated with loneliness/social isolation (Nikmat et al., 2015). However, relationship satisfaction with children was reported to help reduce depression (Nikmat et al., 2015).
In Pakistan, Asghar et al. (2018) studied the experiences of people living with dementia using assistive technology (AT) in performing daily activities and the needs that these technologies met. The results highlighted key social and communication needs of the participants which could be met by ATs. ATs included smart watches and smart walkers with Global Positioning Systems (GPS) which facilitated communication with friends and independent travel (Asghar et al., 2018). ATs were reported by participants to address needs such as loneliness through increased interaction and socialisation. ATs also supported participant’s cognitive needs by providing reminders to take medication on time (Asghar et al., 2018). (ii) Physical needs
Two studies (Asghar et al., 2018; Prince et al., 2011) reported physical needs of people living with dementia. Prince et al. (2011) in their cross-sectional survey reported that continence, hearing, and mobility support were the most common physical needs across low-and middle-income countries and these physical needs were significantly associated with dementia severity. They also reported that hearing impairment made the most notable contribution to cognitive impairment. Asghar et al. (2018) in their study reported that ATs such as a smart walker with GPS, minimised functional difficulties in daily activities for people living with dementia and thus helped to meet their physical mobility needs. They also reported that other physical health needs of people with dementia such as blood pressure, weight and glucose monitoring could be met by ATs at home reducing the need for transport to health facilities for ongoing health monitoring. (iii) Care and service needs
Four studies (Bao et al., 2019; Lian et al., 2017; Liu et al., 2009; Wu et al., 2016), were based in China. These studies focused on care and service needs associated with service utilisation, dependence on care, and staffing and resourcing of services.
Bao et al. (2019) in a recent cohort analysis in rural China showed that older adults with physical multimorbidity had a higher risk of care dependence and thus service utilisation. Care dependence was defined as the requirement for additional support from family carers (Bao et al., 2019). Multimorbidity was reported as impairments in areas such as vision, joints, or conditions such as hypertension, diabetes, heart failure (Bao et al., 2019). The researchers (Bao et al., 2019) argued that multimorbidity can cause depression or anxiety among older people with cognitive impairment which can in turn increase their level of dependence and need for care from others and increase their service needs.
Wu et al. (2016) carried out qualitative research in rural China and identified unmet service needs of older people with dementia. The research pointed to a lack of specialized non-psychiatric medical services designed for people with dementia. They further highlighted that existing long-term care facilities were ill-equipped to meet the needs of individuals living with dementia. Appropriate prescription of medication in rural China was also highlighted as a service need by Wu et al. (2016). Urban township hospitals lacked adequately qualified staff to prescribe medications for dementia and rural physicians with short-term basic health care training were reported to have poor knowledge in diagnosing dementia and its management (Wu et al., 2016). People with dementia were often denied admission to residential care facilities (Wu et al., 2016). These unmet service needs resulted in families having to provide care for people with dementia in home settings.
Liu et al. (2009) in a cross-sectional survey in two areas of China reported that diagnosis of dementia is higher in urban areas than rural settings. The authors (Liu et al., 2009) reported dementia was associated with higher health service utilisation (access and use of formal healthcare services) due to higher care needs. They further highlighted that carers (informal and formal) of older people with dementia provide help in areas of need associated with basic activities of daily living such as dressing, eating, grooming and toileting.
Lian et al. (2017) carried out an interpretative study to understand experiences of people with dementia and their caregivers regarding a diagnosis of dementia. The authors, (Lian et al., 2017), reported a lack of staff and resources for dementia screening in local facilities. This study highlighted the need for more easily accessible, cost efficient and flexible cognitive screening and dementia services in the community. (iv) Knowledge-related needs
Two studies (Lian et al., 2017; Willis et al., 2020) considered knowledge-related needs of people with dementia. Willis et al. (2020) reported in their qualitative study that people with dementia in Pakistan had variable understandings of the disease and held predominantly lay perceptions about its causes. Given these understandings, the authors (Willis et al., 2020) identified that the person with dementia needed family caregivers who also understood about the disease and its common symptoms. In the absence of this, the person with dementia could be subject to negativity from family related to their symptoms. Likewise, Lian et al. (2017) in their interpretive study reported on information needs about dementia for those diagnosed with the condition. (v) Spiritual care needs
Willis et al. (2020) identified spiritual care needs as an important issue for people with dementia and their carers in Pakistan. In this qualitive study it was reported that people with dementia may forget steps in their obligatory daily prayer that would then require them to start the ritual again or seek assistance from family members. This study highlighted that the impacts of memory impairment on religious practices was upsetting not only for the person with dementia, but was a challenge for the carers.
Discussion
This review explored the needs of older people living with dementia in low and middle-income Asian countries. With the predicted increases in the number of people with dementia in these countries an understanding of their needs is paramount to designing responsive health and social care services, especially given that dementia care services and supports are still developing in these regions (Herat-Gunaratne et al., 2019). The needs of people living with dementia have significant impacts on the uptake of health care services and costs associated with social care and informal care (WHO, 2022a). The cost of dementia (for informal care, social care and direct medical care) worldwide was estimated to US$1313 billion in 2019, of which 74% was reported from high-income countries despite the majority (61%) of people with dementia living in low and middle income countries (Wimo et al., 2023).
While the health and social care needs of people living with dementia in developed countries has received considerable attention (Gorska et al., 2013; Hopper et al., 2017; Prince et al., 2014), significantly less is reported about the needs of people with dementia in low and middle-income countries (WHO, 2023). Our findings indicate that there is limited literature on needs of people living with dementia in some low and middle-income countries in Asia. Eight studies (Asghar et al., 2018; Bao et al., 2019; Lian et al., 2017; Liu et al., 2009; Nikmat et al., 2015; Prince et al., 2011; Willis et al., 2020; Wu et al., 2016) reported data from only four Asian countries - China, Pakistan, India, and Malaysia. The methodologies (qualitive and qualitative) were diverse reflecting the varied nature of the research questions. Interestingly, no literature was located that met our inclusion criteria for Bangladesh, which is the country of focus for a larger study that this scoping review was intended to inform, or Vietnam. One reason identified for the lack of research from Bangladesh is the shortage of resources to invest in research (Roy et al., 2020). While in Vietnam, research has focused on caregiver needs (Nguyen et al., 2021) and implementation of interventions previously tested in Western countries to improve caregiver outcomes, arguably there has been limited focus on the actual needs of people with dementia in that context.
This review identified needs of people with dementia across categories of social, cognitive, and mental health; physical health; care and services; knowledge; and spiritual needs. Our findings in several of these categories echo those in the international literature from developed nations about the needs of people with dementia. In particular, the findings of this review about needs of people with dementia related to social isolation, daytime activities, psychological distress, and dementia knowledge have also been reported by Miranda-Castillo et al. (2013) in their United Kingdom study and other European studies (Mazurek et al., 2019; Michelet et al., 2021). In an Australian study Bauer et al. (2019) reported that people with dementia had a need for increased education, and care that was unmet. Likewise, Khanassov et al. (2021) in the Canadian context found physical health, eyesight/hearing/communication, medications, looking after the home, money/budgeting as key areas required to address the needs of people with dementia, which is also congruent with our findings. Moreover, a scoping review by Soong et al. (2020) that investigated health service information needs amongst people living with dementia in high-income countries reported dementia knowledge need which resonates with our findings about the knowledge-related needs of people living with dementia (Lian et al., 2017; Willis et al., 2020).
Across the studies reviewed, the care and service need of people with dementia were at times clearly highlighted, while in some studies these were implied. For example, Bao et al. (2019) clearly highlighted care needs of people with dementia when they reported how physical multimorbidity (hence physical needs) resulted in higher risk of care dependence. However, the relationship between high care needs, service needs and care outcomes were less clear. Future research which looks explicitly at care and service needs of people with dementia in low and middle-income Asian countries and how these interact to impact quality of life is needed. Additionally, Wu et al (2016) highlighted unmet service needs in terms of people with dementia being denied admission to formal services, which in effect means that they needed to rely on family carers. However, other research (Andrews et al., 2017; Bressan et al., 2020) has highlighted that family members have a range of unmet information/knowledge-related needs about dementia. It is feasible that in addition to service needs, people with dementia cared for at home will also have a range of care needs which family members may not be equipped to manage.
Just one paper (Willis et al., 2020), included in this review, reported on the spiritual needs for the person with dementia. Other research, that did not meet our inclusion criteria, explored how religious beliefs of Vietnamese (Hinton et al., 2008) and Bangladeshi caregivers (Hossain & Mughal, 2021) can serve as a source of support and a way of understanding and accepting the condition particularly from the perspective of the caregivers. However, culturally and religiously sensitive resources are needed to support both caregivers and people living with dementia (Hossain & Mughal, 2021). We chose to exclude papers where needs of people with dementia were reported by family caregivers, and this is a potential limitation of this scoping review. As such, we suggest that future reviews should include the voice of family caregivers, especially given the cultural importance of family-based care in low and middle-income countries in Asia (Yamashita et al., 2013).
Finally, the results of this scoping review should raise concerns about the lack of research in which people with dementia can give voice to their needs. Recent literature has prioritised the voice of people with dementia in co-designing interventions and services (Lord et al., 2022; Wang et al., 2019). Without research that is focused on hearing the perspectives of people with dementia in LMICs, the development of person-centred services that are responsive to consumer needs is unlikely.
Conclusion
This scoping review provides evidence that there is a lack of literature about needs of people living with dementia in Asian LMICs. There are opportunities for future research to explore the spiritual needs of people living with dementia in this context. Given the highly integrated nature of religion and spirituality, a greater focus on this area could enhance our understandings, and inform creation of future resources that may be needed to support people living with dementia. Additionally, research that prioritises the experiences of people with dementia in Asian LMICs more broadly is needed. The development of person-centred, culturally appropriate care frameworks and systems for people living with dementia in these countries, will be reliant on increased research investment and outputs.
Supplemental Material
Supplemental Material - Needs of older people living with dementia in low and middle-income Asian countries: A scoping review
Supplemental Material for Needs of older people living with dementia in low and middle-income Asian countries: A scoping review by JM Abdullah, Helen Courtney-Pratt and Kathleen Doherty, Sharon Andrews in Dementia
Footnotes
Author’s contribution
Conceptualisation: JM Abdullah, Sharon Andrews, Helen Courtney-Pratt, Kathleen Doherty, Data gathering and curation: JM Abdullah, Data review: Sharon Andrews, Helen Courtney-Pratt, Kathleen Doherty, Data extraction: JM Abdullah, Review of extracted data: Sharon Andrews, Analysis and primary draft: JM Abdullah, Review of primary draft: Sharon Andrews, Review and editing: JM Abdullah, Sharon Andrews, Kathleen Doherty
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was carried out under generous support from University of Tasmania through Research Training Programme (RTP) scholarship.
Ethical statement
Ethical approval is not required for this scoping review because the methodology of the study only consists of data from articles already in public domains.
Supplemental Material
Supplemental material for this article is available online.
Note
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
