Abstract
Background
Patient safety for people experiencing dementia in acute hospitals is a global priority. Despite national strategies as well as safety and quality guidelines, how safety practices are enacted within the complexities of everyday work are poorly understood and articulated.
Methods
Using video reflexive ethnography, this 18-month study was conducted within an inpatient geriatric evaluation and management unit for people experiencing dementia and/or delirium in Australia. Patients, family members, and staff members participated by: allowing researchers to document fieldwork notes and video-record their practices and/or accounts thereof; and/or interpreting video-recordings with researchers to co-analyse and make sense of the data.
Results
Safe care for people experiencing advanced dementia involved: negotiating risk via leadership, teamwork, and transparency; practice-based learning through situated adaptation; managing personhood versus protocols by doing the ‘right’ thing; joyful and meaningful work; as well as incorporating patient and family voices to do safety together.
Conclusion
Patient safety for people experiencing dementia requires continuous responsiveness and prioritising in the context of multiple risks by a staff collective with a shared purpose. Ongoing research to better understand how the nuances of patient safety unfold in everyday complex clinical realities in diverse contexts and with key stakeholders is required.
Keywords
Introduction
Dementia was the principal and/or additional diagnosis in 93,800 hospitalisations in Australia in 2017–2018 (AIHW, 2020). Almost 40% of all patients over the age of 65 years admitted to hospital have cognitive impairment (Reynish et al., 2017). Moreover, this number is expected to increase significantly. Hospital admission among people experiencing dementia often has negative outcomes and consequences (Dewing & Dijk, 2016). Compared to people who do not experience dementia, people experiencing dementia have worse clinical outcomes, longer hospital stays, and an increased likelihood of hospital readmission (Fogg et al., 2018; Pickens et al., 2017). They are also twice as likely to experience adverse events while in hospital, such as falls, sepsis, or pressure ulcers (Reynish et al., 2017). If a person experiences dementia, they are three times more likely to sustain a fracture or experience delirium. This means that people experiencing dementia face a fivefold increase in mortality rates (Australian Commission on Safety and Quality in Health Care, 2013). A stay in hospital can be frightening for a person experiencing dementia. A recent study highlighted a significant disconnect between staff members’ view of safety and the expressed needs of people experiencing dementia when in hospital (Scerri et al., 2020).
Traditional approaches to patient safety for people experiencing dementia have relied on retrospective actions to determine the cause of clinical failures and keep future failures as low as possible (Smyth et al., 2021; Wright & Singh, 2022). This find-and-fix approach – or Safety-I – focuses on linear processes that assume the absence or reduction of error is synonymous with safety (Dekker, 2014). Although Safety-I is ‘very useful in a technical system consisting of purely technical elements’ (Ham, 2021: p. 11), it has a limited capacity to improve safety in complex systems, like health services – including those for people experiencing dementia. This spurred interest in an alternative approach – Safety-II. Proponents of Safety-II argued the need to focus on the conditions that optimise and sustain patient safety (Braithwaite et al., 2015). It is concerned with ‘an organisation’s ability to function as required under expected and unexpected conditions alike’ (Hollnagel, 2014, p. i) – it is an expression of how clinicians and teams continually adjust their performance to surrounding conditions in response to healthcare uncertainties and complexities (Hollnagel et al., 2015). While Safety-I focuses on what goes wrong, Safety-II is more concerned with what goes well.
The extent to which Safety-II is or could be adopted in different clinical contexts is poorly understood. As Lawton (2018) posited, the limited improvements to patient safety and quality might be less to do with theories and models, and more to do with how we operationalise these within complex health systems. It is unclear whether and how Safety-II will address the intractable quality and safety issues that Safety-I approaches have largely failed to address (Smith & Valenta, 2018). Specifically, there is limited clarity on how patient safety is and is not realised. This is particularly the case for the safety of the growing number of patients experiencing complex and chronic conditions, like dementia (AIHW, 2021; Ponjoan et al., 2019).
Recognising the significance of safety and quality of care for this growing group of patients, several countries in the Organisation for Economic Co-operation and Development (OECD) have national strategies to improve the care of people experiencing dementia in hospital. A better understanding of how to implement these strategies well in hospitals is imperative.
This article clarifies how patient safety is enacted within a specialist hospital unit in South Australia for people experiencing advanced dementia. This is achieved by presenting findings from a study on the organisational practices that promoted quality dementia care and patient safety. This setting was selected because, unlike other hospital units in this state, this specialised unit managed and treated acute medical conditions in an environment that was sensitive to the needs of people with dementia and/or delirium. Its success was demonstrated by the relatively few behavioural issues among patients (and relatedly, reduced stress among family members), particularly during admission and discharge. For this reason, the researchers examined how safety practices were enacted in this context. The researchers included: academics; clinicians; service managers; and a consumer representative. This purposely-selected team served to bring together knowledge on dementia, palliative care, health service management, knowledge translation, VRE, nursing, and lived experience expertise.
Reflecting Safety-II, safety is here understood as when ‘many things as possible go right’ (Hollnagel et al., 2015: p. 26), rather than when ‘as few things as possible go wrong’ – in the context of dementia care, this might involve encouraging personal agency and dignity, rather than paternalistically curtailing choice. Similarly, risk is here understood as ‘the likelihood that something unwanted can happen’ (Aven, 2022: p. 3), rather than assuming that ‘Accidents are caused by failures and malfunctions’ (Hollnagel et al., 2015: p. 26) – in the context of dementia care, this might involve recognising that a person experiencing dementia can benefit from exercising personal agency (e.g., the decision to go shopping), even if they previously experienced challenges (e.g., disorientated to place).
Method
Objective
This study ascertained how safety practices are enacted within the complexities of everyday work; specifically: what approaches, strategies, behaviours, and culture are associated with delivering safe and high-quality care to people experiencing advanced dementia by a geriatric evaluation management unit team?
Methodology
Given the demonstrated value of ethnography to engage with a context, collect data, and make sense of complex phenomena (Northcott et al., 2022; Reynolds & Lewis, 2019), this study involved video-reflexive ethnography (VRE) to visibilise and examine taken-for-granted safety practices, including those deemed to be routine (Iedema et al., 2006). VRE is situated in a constructionist paradigm and involves negotiated processes between researchers and participants to capture commonplace practices via video-recordings. The researchers and participants then reflexively co-analyse the video-recordings (Iedema et al., 2019). VRE takes researchers and participants on a shared journey into areas of uncertainty. This is because video-recordings can evoke different meanings to different people at different times, in different spaces. As such, VRE is interventional in nature and, through co-constructed meanings, researcher and participant assumptions can be challenged (Collier & Wyer, 2016; Iedema et al., 2015). This is important because anything less can perpetuate the status quo, as the identification of problems, gaps, and issues and their fixes are largely based on prevailing beliefs and assumptions (Alvesson & Kärreman, 2007; Alvesson & Sandberg, 2011). Hung and colleagues (2018) also demonstrated this in their study, which aimed to improve dementia care. Given the value of VRE, the study presented in this article responds to their call for ‘Future research [to] further explore the benefits of filming staff care interactions with patients with dementia’ (p. 8). This was achieved by clarifying safety practices, in situ. To ascertain how safety practices are enacted within the complexities of everyday work, this study used VRE to consider organisational practices that promoted quality dementia care and patient safety. Rather than use VRE to ‘commit [staff] to improve dementia care’ (Hung et al., 2018: p. 8), it was used to visibilise taken-for-granted, if not routine safety practices within the research setting.
Setting
This study was conducted in an 11-bed South Australian geriatric evaluation and management (GEM) specialist unit for people experiencing dementia and/or delirium, particularly those whose communication and care was deemed difficult to manage elsewhere (i.e., home, residential aged care, other hospital units). This setting was selected because, unlike other comparable hospital units in this state, this specialised unit was designed especially for patients experiencing dementia who were also diagnosed with delirium. A comprehensive geriatric assessment informed an individualised care plan. Multidisciplinary team members trained to provide specialist care contributed to the management of common geriatric syndromes, functional impairment, and decline. The lead researcher responded to a request by the nurse unit manager to better understand how safety and quality of care is best enacted in their unit – a setting where patients’ issues are highly complex issues and have likely effects on health service staff (Costello et al., 2019).
Participants
Following research ethics committee approval from the relevant local health network (reference number: 2020/GEM01496), all individuals who received and/or delivered care at the specialised unit (people over 60 years, their family members, clinicians, and ancillary staff) were invited to participate – as such, potential participants were not sampled, as all were welcome to participate, so long as they received and/or delivered care within the unit. Following recruitment, informed consent was sourced from 50 participants, including patients (n = 3); family members (n = 5); managers (n = 2); clinicians (n = 35); and non-clinical staff members (n = 5). Although more staff members were involved, relative to patients and family members, their contributions collectively diversified the perspective represented in the findings.
Ethical considerations
In addition to following national guidelines on the ethical conduct of research (NHMRC, 2018), the researchers applied situated ethics underpinned by the VRE principle of care (Iedema et al., 2019). Specifically, ethical decisions were made in the context of particular situations, rather than adhering to prescriptive regulations alone (Clark, 2013). The researchers used process consent (Dewing, 2002). Developed for research involving people experiencing dementia, process consent requires researchers to: ‘set… the scene by prompting the researcher to check they are not taking short cuts… establish… the basis for capacity to consent and how this has been achieved… seek an initial consent for the specific research [by]… mov[ing]… from what is known about consent and assent in general terms to its translation into the specific situation… ensur[e]… initial consent is revisited and re-established on every occasion or even within the same occasion [and]… consider feedback and support… about the person’s well-being or on a particular concern’ (Dewing, 2007: pp. 15–21). A consumer representative reviewed the research protocol before submission to the ethics committee and advised on participant consent and recruitment. The field-researcher – who was also a nurse-member of the clinical team, experienced in the care of people experiencing dementia – conducted fieldwork with support from clinical academic researchers with expertise in dementia, palliative care, health service management, knowledge translation, and VRE with vulnerable groups.
Data collection and analysis
Reflecting the VRE methodology, participants were invited to contribute between June 2016 and February 2018 (inclusive), according to their preferences, to optimise inclusiveness. Participants could: consent to a video- or audio-recorded semi-structured interview about patient safety; permit the researchers to document ethnographic fieldwork notes, video-record healthcare practices, or group reflexive sessions to analyse the video-recordings; and/or co-analyse and interpret the video-recordings with the researchers to clarify safety practices. Where patient participants were unable to provide formal informed consent, their proxy provided this consent on their behalf, as per national guidelines (NHMRC, 2018).
The field-researcher and a senior researcher attended staff meetings and handovers to explain the study objective and invite participation. Additionally, the researchers placed posters about the study, including photographs of the researchers, around the unit. The researchers maintained a regular weekly presence in the unit at various times during data collection. During this period, they approached prospective participants, personally inviting their participation. Reflecting an ethnographic approach, this occurred during structured (e.g., staff meetings) and unstructured interactions (e.g., casual conversations with patients and family members), during which they introduced the study and its rationale, explained the varied ways to be involved, provided participant information sheets and consent forms, and invited participation.
The researchers: observed unit practices; documented detailed fieldnotes comprised of ‘Thick description’ (Geertz, 1973) to capture what was done, how it was done, who and what was involved, and the associated effects; and conducted semi-structured interviews with staff and family members as well as impromptu field interviews – the interview schedules were informed by positive organisational scholarship to draw attention to what goes well (Cameron et al., 2008; Collier et al., 2020; Dadich et al., 2015, 2018; Hollnagel et al., 2015). This led to the video-recording of practices and situations that clinical staff, families, and patients consented to, including: weekly case conferences; daily huddles; the care of patients within the unit; meetings between managers and clinicians; as well as field conversations between clinicians, patients, and family members, face-to-face or via telephone. The researchers facilitated six reflexive sessions where staff members viewed and interpreted video-recordings of care practices. They involved discussions of: what participants observed in the video-recordings and why; their thoughts and feelings while viewing the video-recordings and why; whether they thought the video-recordings epitomised safe and high-quality care and why; as well as the factors that influenced high-quality care and the associated reasons.
Data analysis occurred at four levels. First, the field researcher and two senior researchers analysed all types of data, informed by Braun and Clarke’s (2020) phases. This involved: ‘data familiarisation and writing familiarisation notes’ (p. 331), which involved the purposive transcription of video-recordings (Halcomb & Davidson, 2006) and (re)reading the ethnographic fieldwork notes; ‘systematic data coding’, whereby features of the data relevant to the objective were identified; ‘generating initial themes from coded and collated data’; ‘developing and reviewing themes’; and ‘refining, defining and naming themes’. Second, visual data were edited into short clips, based on the thematic analysis, which staff participants analysed and critiqued during the reflexive sessions, following consent from those appearing in the footage. These sessions were also video-recorded. Third, reflexive sessions underwent a further analysis using Braun and Clarke’s phases. Specifically, the researchers listened to and/or watched the short clips again in relation to the reflexive session video-recordings and themes were further refined. Finally, all researchers reviewed and discussed these refined themes. Digital data were maintained on a secure, online platform, while paper-based were maintained in a secure cabinet. Although the different forms of data were complementary, the video-recordings were particularly helpful, because – unlike fieldnotes – the participants found them engaging and conducive to analysis during the reflexive sessions.
Results
Approximately 65 hours of fieldwork were recorded – these included field observations (12.5 hr); video-recordings of practice (41 hr); participant interviews (9 hr); and reflexive sessions, where staff members viewed and interpreted video-recordings of care practices (2.5 hr). The findings highlighted several themes that underpinned patient safety for people experiencing dementia. These included: negotiating risk via leadership, teamwork, and transparency; practice-based learning through situated adaptation; managing personhood versus protocols by doing the ‘right’ thing; joyful and meaningful work; as well as incorporating patient and family voices to do safety together. Each theme is addressed in turn.
Negotiating risk: Leadership, teamwork, and transparency
Data substantiating the results.
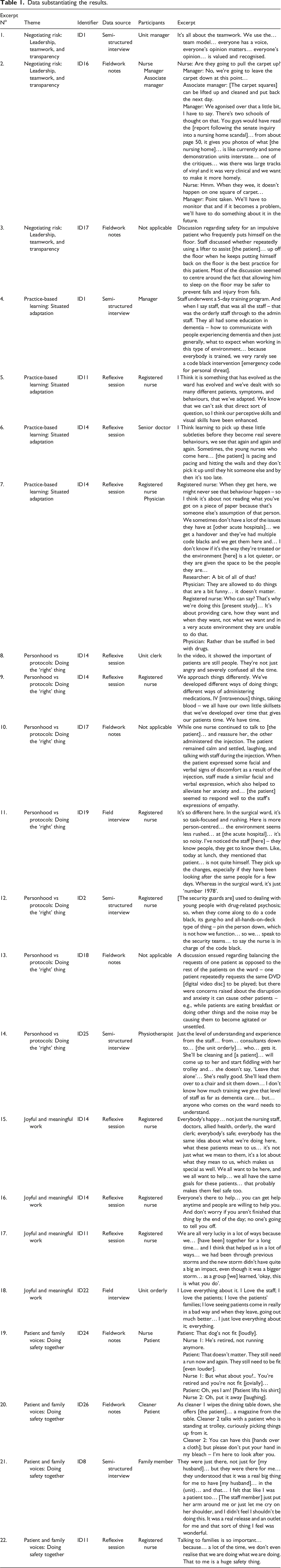
Consider the following example involving a senior manager, an associate unit manager, and a unit registered nurse. During a team meeting about flooring, they deliberated on why the unit was carpeted, the associated implications for patient safety and care, and how these will be managed. In addition to justifying the decision to retain the carpet with reference to report (Prendergast, 2015), the manager noted that issues would continue to be monitored (see Table 1, excerpt 2).
This highlights the strong nature of teamwork in this setting as well as recognising and valuing the important role staff play in patient safely. Similarly, staff members openly discussed their daily practices, notably those that affected patient care and safety, the rationale for these practices, and how they negotiated risk. That is, issues of safety and risk often involved team decisions, rather than individual decisions by one professional. This afforded regular opportunity to demonstrate openness to each other and the people they supported (see Table 1, excerpt 3).
Collectively, these findings demonstrate how leadership, teamwork, and transparency informed the negotiation of risk. Specifically, the team openly discussed decisions – a practice that the leadership style reinforced.
Practice-based learning: Situated adaptation
Significant attention was given to preparing staff members to work on the unit. Education was expansive, focusing on the delivery of psychosocial and non-pharmacological interventions, the facilitation of personalised activities, as well as social interaction and exercise. Furthermore, non-clinical staff members were included in this education. This recognised and valued their important role in patient safety, promoting shared understandings and shared expectations (see Table 1, excerpt 4).
Along with the more formal education for all staff members, the reflexive sessions helped them to see how their safety skills had evolved and had become more attuned overtime. This reinforces the interventional nature of VRE – facilitated by the researchers, the sessions visibilised what was often taken-for-granted (see Table 1, excerpt 5).
Staff members recognised the importance of this situated learning for patient safety. This kind of learning enabled them to detect subtle changes in a person’s behaviour, which might indicate an unmet need. Such early detection of behavioural changes served to prevent the behaviour from escalating in such a way as to make the environment unsafe for other patients and staff members (see Table 1, excerpt 6).
Reflexive sessions became part of the unit ‘norm’ of situated learning. The sessions enabled staff members within this unit to connect high-level concepts of safe and quality care to their daily experiences, rationalise their practice, and identify improvement opportunities. It also provided a formal framework to recognise excellent practice, provide support and encouragement, as well as give meaning to work (see Table 1, excerpt 7).
These findings reinforce the need to prepare all staff for the care practices that optimise patient safety and risk management for and with people experiencing advanced dementia. While formal education was important, so too was situated learning.
Personhood versus protocols: Doing the ‘right’ thing
Recognising patients as people with life stories was a strong feature of the unit’s culture and made explicit in reflexive sessions (see Table 1, excerpt 8).
Over time, clinicians within the unit learnt specific strategies to adapt and respond to the individual needs of people experiencing advanced dementia (see Table 1, excerpt 9).
These varied management practices focused on the specific needs of people experiencing advanced dementia. These skills helped to ensure clinical flexibility to accommodate the changing needs and preferences of patients and their family members (see Table 1, excerpt 10).
Such flexibility deviated from established practices within other hospital units. While other units typically focused on ‘doing things right’, as per protocols and conventions, this specialised unit prized ‘doing the right things’ (Drucker, 2006: p. 83), guided by patients and family members. These practices permeated the ways staff members within the unit conducted themselves, particularly senior staff who served as role models (see Table 1, excerpt 11).
‘Doing the right things’ meant the culture and practices of the unit needed to reach beyond the walls of the unit to include external staff members. For example, the hospital security team received training on how to respond to a person experiencing dementia. Rather than be ‘led’ by security guards, unit nurses co-ordinated responses to a code black emergency (see Table 1, excerpt 12).
In addition to reinforcing the importance of leadership and teamwork, this finding highlights the importance of flexibility, requiring the staff members to continuously distinguish, negotiate, and respect different priorities and interests. They had to be perceptive of their environment, recognise others’ needs and preferences, appreciate the myriad ways people affected each other – be they patients, family members, or staff members – and resourcefully find ways to balance different agendas (see Table 1, excerpt 13).
The staff members demonstrated flexibility in a concerted way. Collectively, they evaluated and balanced risks, respectfully and unobtrusively. Irrespective of their position or role, they approached their work with a similar ethos. This helped to ensure that patients and family members did not feel scrutinised or micro-managed, but rather, could exercise personal agency and be ‘free to roam’ (patient’s wife), safely (see Table 1, excerpt 14).
These findings suggest that safe care for people experiencing dementia was not dictated by protocols and conventions. Instead, it required a genuine focus on patients and their family members, and efforts to accommodate their changing needs and preferences.
Joyful and meaningful work
Staff members found joy and meaning through a shared focus on person-centred care. Regardless of their position, together, they were motivated to optimise care, safety, and wellbeing – not just for older people experiencing advanced dementia, but also for each other. This joy and meaning in work contributed to a feeling of safety (see Table 1, excerpt 15).
With regular opportunities for reflection through team meetings and informal conversations, staff members reported being comfortable to share their vulnerabilities and seek guidance, without fear of criticism or derision. Regardless of seniority, they were actively encouraged to ask for help. This fostered connectedness and collective learning, which the staff members valued. For example, there was a shared understanding that: their work was not exclusively task-orientated; support was always available; and they would not be disrespected, blamed, or punished for incomplete work (see Table 1, excerpt 16).
This shared purpose developed over time. Working with the same colleagues, patients, and family members afforded opportunity to establish rapport and ride the highs and lows of working or being cared for in this specialised unit. This fostered shared understandings, gratitude, and collective resilience (see Table 1, excerpt 17).
Participants spoke of a shared sense of togetherness, choosing to be part of the unit, as well as a strong affection for the unit and everyone therein. This might be partly because of the joy and satisfaction they experienced. This suggests a commitment to the unit, to each other, and to the patients and family members they supported (see Table 1, excerpt 18).
These findings highlight the reciprocal nature of safe care. Staff members who experienced joy, found meaning in their work, and felt safe were better able to ensure the safety of people experiencing dementia and their family members.
Patient and family voices: Doing safety together
In this specialised unit, where most patients had significant cognitive impairment, the staff members were committed to closely engaging with patients and their family members. For instance, they proactively got to know the patients. They made a concerted effort to know about their lives, what they deemed important, their (dis)likes, family members’ names, and so on. This familiarity was developed respectively and unobtrusively in conversation with patients and their family members (see Table 1, excerpt 19).
Both clinicians and non-clinicians demonstrated such skilled, yet light-hearted interaction. This indicates a shared ethos. They demonstrated a shared approach when interacting with patients, family members, and each other (see Table 1, excerpt 20).
The staff members recognised family members as critical to patient safety. In addition to being an important source of patient information, family members were deemed to be equal partners in patient care. This required the family members to understand and have confidence in the staff members’ person-centred approach. It also required staff members to recognise and appreciate the difficulties that family members were likely to have experienced while caring for a loved one experiencing advanced dementia (see Table 1, excerpt 21).
Recognised for their skills and expertise, family members were regarded as active contributors to the team. They offered experiential wisdom and helpful strategies to improve patient safety. Staff members, including managers, encouraged them to provide feedback directly and/or via a proxy, if preferred. These feedback mechanisms fostered open communication between staff members, patients, and family members. They were also deemed to be pivotal to continuous improvement in patient safety within the unit (see Table 1, excerpt 22).
These findings speak to the role of patient and family engagement in patient safety for people experiencing dementia. A strong rapport with patients and family members ensured their experiences and perspectives informed safe care practices – what was done, how it was done, when it was done, and who was involved.
Discussion
Despite the progress reported in academic research (Moon et al., 2022), patient safety is less than ideal, particularly for people experiencing dementia in hospital (Smyth et al., 2021; Wright & Singh, 2022). Patient safety continues to be hindered by myriad factors (Emanuel et al., 2005; Gandhi et al., 2018).
The findings demonstrate that, despite the challenges that test health systems, like limited budgets and new public management (Willis et al., 2017), safe and high-quality care can be achieved for older people experiencing advanced dementia and complex care needs. The staff members who participated in this study, representing different disciplines and levels of seniority, recognised the specialised unit in which they worked as a place of potential risk – risk that was omnipresent, as per Safety-II (Hollnagel et al., 2015). Although a patient safety agenda can impel paternalistic approaches that inhibit the rights and autonomy of people experiencing dementia (Ó Néill, 2019), these staff members enacted a respectful approach, adroitly balancing patient autonomy and agency with risk management.
This collective capacity was fostered in two main ways. First, safe and high-quality care required leadership that ‘mobilis[ed]… the attention, resources and practices of others towards particular goals, values or outcomes’ (National Advisory Group, 2013 on the Safety of Patients in England, 2013, p. 15). The manager’s invitation to the researchers to observe practices within the unit, and the staff members’ openness to the study signified a tone of transparency (Dewar et al., 2019; Gehlert et al., 2014). Furthermore, the manager proactively communicated to others: key decisions that affected them; the rationale for these decisions; and opportunities for further action, if required. Additionally, the manager regularly asserted the importance of privileging the safety needs of everyone within the unit – patients, family members, clinicians, and non-clinicians. The manager and associate manager made themselves available to colleagues, patients, and family members – they had an active clinical presence and would intervene in situations they deemed unsafe or that contravened the unit ethos. This ethos focused on privileging the person experiencing dementia’s own routines and corresponding care needs rather than those of the institution. This contrasts with what Featherstone and colleagues (2019) described as ‘cycles of resistance’, driven by the efficiencies and routinised care seen in general units of contemporary institutions, resulting in poor experiences for people experiencing dementia as well as staff burnout.
Second, all staff members – regardless of role or seniority – were educated on how to enact the unit ethos. Clinicians and non-clinicians engaged in formal and informal training on how to care for people experiencing advanced dementia. The former included structured training programs, while the latter included vicarious adaptive learning through role modelling and situated learning experiences.
Irrespective of role or seniority, staff members spoke of their work with joy, pride, gratitude, and love. Gandhi and colleagues (2018) linked joyless and meaningless work with burnout – physical and psychological symptoms activated by an incongruity of staff expectations and the observed reality of their job (Moss et al., 2016). Collaboration and support can prevent burnout; as such, they have implications for patient and staff safety (Hofmeyer & Marck, 2008; Schulman, 2004). The staff members’ joy and pride in their work was underpinned by relationships – they forged relationships with patients, family members, and each other. This trust and solidarity can foster the confidence and risk-taking that teams require to be adaptive when working within complex health systems. Conversely, limited trust can compromise patient safety. The findings in this article align with those of Baxter et al. (2019) who found staff members on positively deviant wards felt strongly about ‘knowing one another’, helping them to support one another to deliver safe patient care. Reflecting Baxter and colleagues’ study, the participants in this study shared a purpose and mutual respect. This respect was extended to non-clinicians, like the receptionist and unit orderly.
Although the findings are presented as discrete themes for readability, they were interrelated. That is, transparency – as demonstrated by staff members who shared information and their opinions – occurred in the context of the joy and pride they experienced about their work. Equally, the staff members expressed joy in their work partly because they were supported by a shared team purpose and ethos. The richest source of improvement ideas is those delivering and receiving care. It is they who live the complexities of the system, understand what works and does not work, and recognise opportunities for improvement (Iedema, 2011). Staff members were encouraged to contribute their ideas about how to deliver care to ultimately optimise patient safety. Moreover, the unit’s ethos of care aligned with their values of compassionate, safe, and high-quality care for people experiencing dementia and their families and they felt educationally equipped to deliver care that reflected this ethos.
Despite the value of the findings in this article, four methodological limitations warrant mention. First, the observations were conducted at one point in time, thereby limiting the lifespan of the findings. Second, there is no claim that the sample is representative of all specialised units for people experiencing advanced dementia, within or beyond Australia, particularly given the recruitment strategies and the voluntary nature of participation. Third, the nature of the setting meant that carers often had to come to terms with no longer being able to care for their family member at home. They often noted the ‘burden’ of making multiple decisions for a person experiencing dementia. Thus, many felt unable to consent as proxy decision-maker to something as intimate as recording and/or filming care. The researchers’ and carers’ caution meant that those who participated might have had a lesser sense of burden and guilt than those who choose not to participate (Spector, 2004).
Notwithstanding the aforesaid limitations, this study serves to advance current understandings of how to foster patient safety for people experiencing dementia in hospital. The findings presented in this article have implications for those who manage or deliver care to people experiencing dementia and their family members, as well as scholars. For those who manage or deliver care, the findings suggest that safe care for people experiencing advanced dementia requires: a leadership style that promotes an environment in which staff members are permitted to ‘break free’ from the routinised, task-focused culture, typical of general hospital units; a recognition that risks are an inherent unit characteristic to be continually negotiated and the potential for harm, constantly mitigated; as well as an environment in which situated education and consumer voices are valued, resulting in joyful and meaningful work – here, safety was never fixed – rather, staff members continually negotiated risks, adapting and readapting to situations. For scholars, this article offers fertile ground for research that serves to build on the findings. Beyond the customary call for more research, future scholarship is required to offer in-depth, phenomenological explorations of how patient safety unfolds during everyday clinical practices within diverse settings – furthermore, to harness their expertise, such scholarship should be conducted with patients, family members, managers, clinicians, and non-clinical staff members.
Footnotes
Acknowledgement
The authors thank the patients, family members, and staff who generously contributed to this study.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was funded by the Nurses Memorial Foundation of South Australia Limited, which had no role in data collection, interpretation, or the reporting of the results.
Associate Professor
Ms
Dr
Associate Professor
Ms
Mr
Mr
Dr
