Abstract
Background
Animal-assisted interventions and robotic animal interventions are becoming increasingly popular to support the care of people with dementia and may have the potential to improve a range of psychosocial outcomes. This review aims to identify, describe, and compare animal-assisted and robotic animal interventions delivered to people with dementia, their characteristics, effectiveness, and the proposed mechanisms underlying any potential impact.
Methods
A systematic literature search was conducted in MEDLINE, AMED, EMBASE, PsycINFO, OVID Nursing, PubMed, CINAHL and Web of Science. Random-effects meta-analyses of randomised controlled trials (RCTs) were conducted to summarise studies that evaluated common outcomes (agitation, depression, quality of life). A narrative approach was used to synthesise other findings.
Results
Fifty-one studies were included: 18 RCTs; 12 non-randomised trials, 13 cohort studies, 7 qualitative studies and one mixed-methods study. Meta-analyses were conducted for a small number of RCTs, with effectiveness of animal-assisted interventions demonstrated for agitation. Narrative findings suggested animal-assisted and robotic animal interventions may be promising in improving depression, agitation, and quality of life. Three potential mechanisms of action were identified for both animal-assisted and robotic animal interventions, namely enhancing social connections, providing engaging and meaningful activities, and the affect-generating aspect of the human-animal bond. A fourth mechanism was identified for animal-assisted interventions only: promoting physical activity. Robotic animals appear to have a place in complex human-animal relationships, but a greater understanding of robotic animal interventions is required to harness the benefits that may be derived from their use.
Conclusion
Delivering these interventions appear promising in improving psychosocial outcomes for people with dementia. As most included studies had methodological limitations, these findings are preliminary, but contribute to the body of evidence providing an understanding in terms of intervention characteristics and mechanisms of action. When developing intervention guidance, attention should be given to potential mechanisms and fundamental characteristics such as session content, delivery format and facilitator role.
Introduction
The potential benefits of using animal-assisted interventions to support the care of people with dementia have received increasing attention (Yakimicki et al., 2019). Animal-assisted interventions are based on the concept of the human-animal bond, a mutually beneficial relationship between animals and humans that can influence the health and wellbeing of both (Serpell, 2015). They are defined as interventions that “intentionally include or incorporate animals as part of a therapeutic or ameliorative process or milieu” (Kruger & Serpell, 2006). The term ‘animal-assisted intervention’ encompasses various interventions, including animal-assisted therapy, animal-assisted activities, and animal-assisted education. In animal-assisted therapy, a formally trained professional provides a goal-oriented, therapeutic intervention (Fine & Mackintosh, 2016). Animal-assisted activities also aim to provide therapeutic benefits, but they are more spontaneous in nature and lack specific treatment goals (Jegatheesan et al., 2014). Previous research indicates the potential of animal-assisted interventions for people with dementia, for example in terms of positive behavioural changes (Majic et al., 2013; Nordgren & Engström, 2014b); improved mood (Olsen, Pedersen, Bergland, Enders-Slegers, Patil, et al., 2016; Swall et al., 2015), and increased engagement and social interaction (Marx et al., 2010).
Similarly, interventions involving robotic animals (e.g., PARO the harp seal) (Abbott et al., 2019; Leng et al., 2019) to mimic animal-assisted interventions have been shown to provide emotional and physiological benefits and ameliorate agitation and depression in people with dementia (Bernabei et al., 2013; Hu et al., 2018). Robotic animals are now commonly used as substitutes for real animals within dementia care (Petersen et al., 2017). One common observation is that robotic animals are suitable for settings in which the ethological needs of live animals cannot be met (Banks et al., 2008; Filan & Llewellyn-Jones, 2006). Implementing robotic animal interventions may also reduce potential health risks such as injury and infection compared to animal-assisted interventions. However, concerns in relation to their use have been raised, for example, those related to ethics and the concept of ‘infantilisation’ (Abbott et al., 2019). Resistance to using robotic animals in care settings has been reported to be persistent (Dodds et al., 2018).
Studies on the effectiveness of animal-assisted and robotic animal interventions are characterised by varying species of animals and heterogeneous study populations including different types and severities of dementia, various intervention formats, and a range of outcomes (Batubara et al., 2022; Leng et al., 2019; Pu et al., 2019). Due to the impact of intervention characteristics on study outcomes, systematic reviews should, therefore, consider these characteristics. This is necessary to comprehensively evaluate the interventions and their potential effects. Systematic reviews investigating animal-assisted and robotic animal interventions within dementia care have often evaluated their effectiveness but lack detailed information about intervention implementation (Aarskog et al., 2019; Babka et al., 2021; Batubara et al., 2022; Bernabei et al., 2013; Klimova et al., 2019; Leng et al., 2019; Yakimicki et al., 2018). While these reviews conclude that animal-assisted and robotic animal interventions are promising for improving psychosocial outcomes for people with dementia, characteristics such as the intervention type, content and format, the facilitators’ experience and/or background, and the intervention frequency/duration are often overlooked, and should be reported to fill this gap in the literature. These reviews do highlight the need for future research to address these limitations in the existing literature. Moreover, existing systematic reviews of animal-assisted or robotic animal interventions delivered to people with dementia often do not include meta-analyses (Aarskog et al., 2019; Babka et al., 2021; Klimova et al., 2019; Yakimicki et al., 2018), are insufficiently focused on the dementia population (Abbott et al., 2019; Bernabei et al., 2013), and/or are very narrowly focused on particular animal species (Batubara et al., 2022; Klimova et al., 2019) or robotic animals only (Abbott et al., 2019). These reviews do not compare evidence across animal-assisted and robotic animal interventions, and many lack a robust discussion of the interventions and their characteristics to permit valid comparison and examination of potentially effective components.
Concerns have also been expressed over limitations of existing studies, most of which are very small and often have additional methodological restrictions (Ratschen & Sheldon, 2019), including their suitability to identify potential mechanisms of change in varied care contexts (Chur-Hansen et al., 2014; Holder et al., 2020; Stern & Chur-Hansen, 2013; Yakimicki et al., 2019). Thus, poor, and potentially harmful or unethical practice may result from relying on application of animal-assisted and robotic animal interventions in ways that are currently insufficiently evidence based (Ratschen & Sheldon, 2019). In order to improve research and practice, a better understanding of animal-assisted and robotic animal interventions is required, especially in terms of how, when, who for, and why they may lead to positive outcomes. Information about the potential mechanisms is crucial in order to explore the relationship between the intervention and its potential effects as well as to guide the implementation of these interventions into practice (Hung et al., 2019). Given the growing interest of these interventions within dementia care, this review is a timely contribution towards advancing theoretical understanding. This is important for broader implementation. Therefore, research aims were to determine: 1. What animal-assisted and robotic animal interventions have been provided to people with dementia? 2. What are the characteristics of animal-assisted and robotic animal interventions currently applied in dementia care contexts? 3. Are animal-assisted and robotic animal interventions effective for people with dementia? 4. What are the proposed mechanisms underlying any potential impact of animal-assisted interventions and robotic animal interventions for people with dementia, and in what way, if any, do these differ?
Methods
We report methodology in accordance with the Preferred Reporting Items for Systematic Reviews and Meta-analyses (PRISMA) guidelines (Moher et al., 2009), following a pre-registered International Prospective Register of Systematic Reviews (PROSPERO) protocol [CRD42021262813].
Search strategy
MEDLINE, AMED, EMBASE, PsycINFO, OVID Nursing, PubMed, CINAHL and Web of Science were searched up to July 2021. The search strategy published by Aarskog et al. (2019) was adapted to include additional items relating to relevant interventions (e.g., all animal-assisted and robotic animal interventions rather than only those restricted to dogs/robotic animals). Searches were limited to studies in English involving adults. The search strategy for EMBASE is presented in Supplementary Table 1 and was adapted for the other included databases. Reference lists of included papers were manually searched to identify further studies. Endnote 20 (2013) was used to record publications at all stages of the selection process (Figure 1). Titles and abstracts were screened independently by two authors to ensure consensus. If there was a disagreement, studies were included in the full-text review. Full-text screening of included articles was undertaken independently by two authors. PRISMA diagram of paper selection process.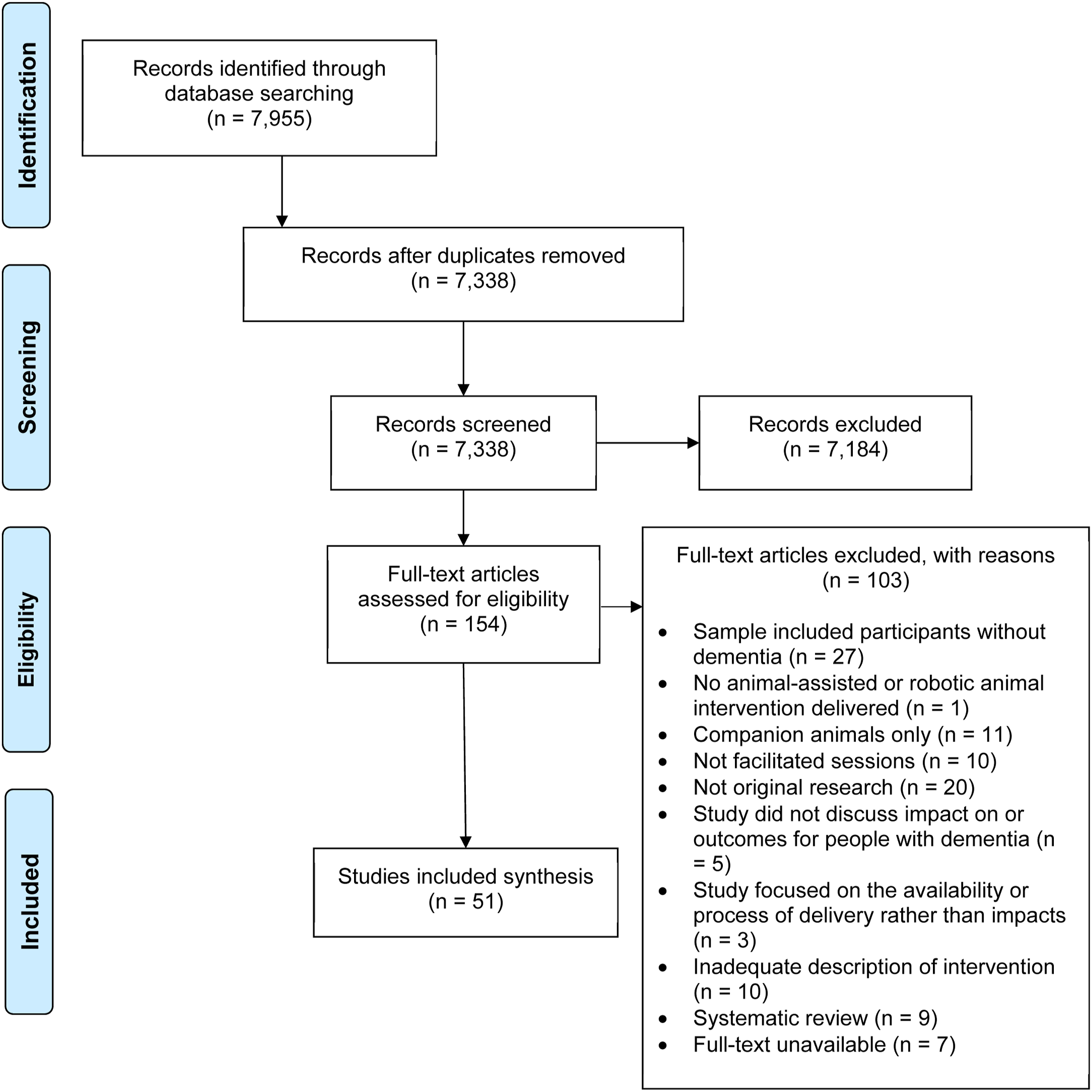
Inclusion criteria
Studies were identified for inclusion based on the population, intervention, comparator, and outcome (PICO) method for eligibility. Randomised controlled trials (RCTs) (including feasibility and pilot trials), observational cohort studies, case series, surveys or qualitative studies were considered.
Population: Studies that exclusively included people with a diagnosis of dementia, known memory problems, or known cognitive impairment deemed to be indicative of dementia in any setting.
Intervention: Studies that described or evaluated any animal-assisted or robotic animal intervention delivered specifically to people with dementia.
Comparator: A control comparator was not necessary for inclusion in this review. Studies with or without control groups were considered.
Outcomes: Studies that reported behavioural and/or emotional outcomes for people with dementia.
Exclusion criteria
Studies were excluded if: (1) the sample included any participants without a diagnosis of dementia, known memory problems or known cognitive impairment deemed to be indicative of dementia; (2) they described or evaluated the benefits of companion animals (pets) only; (3) interventions were self-initiated rather than led by any professional or volunteer; (4) they did not discuss the impact on or outcomes for people with dementia; (5) they did not provide an adequate and clear description of the intervention or (6) they were systematic reviews, theses, dissertations or not original research.
Data extraction
Using a pre-defined table, relevant data were extracted from all studies by one author. Comparable information included research methodology, type and content of the intervention, animal species, mode of delivery, frequency and duration, and outcomes of the intervention. As potential mechanisms of effects are seldom evaluated in animal-assisted intervention literature, one author extracted content relating to the potential mechanisms of the interventions as identified by the study authors (for example, in the discussion sections).
Quality assessment
Version 2018 of the mixed methods appraisal tool (MMAT) (Hong et al., 2018) was used to assess each study. The MMAT was developed for complex systematic reviews, permitting quality appraisal for a range of methodological studies. The tool’s validity and reliability have been established (Hong et al., 2019; Pace et al., 2012). One author independently rated the studies. A second author independently reviewed a random sub-sample of ratings spread across the study categories to ensure consensus. Any disagreements were resolved through discussion. The full sample was then rechecked by the first author, based on this discussion, to identify any potential inconsistencies in papers not subject to double review. Quality assessment was used as a tool for critique of the research evidence and not as an exclusion criterion.
Data synthesis
For RCTs, meta-analyses were conducted to summarise studies that evaluated similar outcomes using RevMan version 5.4 (Higgins & Green, 2011). Where outcomes were measured using different instruments, the standardised mean differences (SMD) were calculated to compare these studies. Heterogeneity between study outcomes was assessed using the I 2 statistic, suitable for smaller meta-analyses (Higgins et al., 2003). Due to the likelihood of significant heterogeneity, a random-effects model was used. Publication bias was not statistically assessed as the number of studies pooled for each meta-analysis was less than ten (Deeks et al., 2011).
A narrative synthesis was conducted to synthesise findings relating to any reported mechanisms underlying an observed impact of animal-assisted and robotic animal interventions for people with dementia. Narrative synthesis is a valuable method for synthesising qualitative data (Campbell et al., 2019), and can be used to examine how contextual or temporal variables influence outcomes (Popay et al., 2006). The author explored the similarities and differences and organised these data into themes. An inductive approach was employed, whereby theme development was driven by the potential mechanisms described in the included studies. An initial programme theory was created to link intervention characteristics to potential mechanisms that may lead to positive outcomes. A second author reviewed the construction of themes and the initial programme theory to reach consensus.
Results
Description of studies
Individual study characteristics.
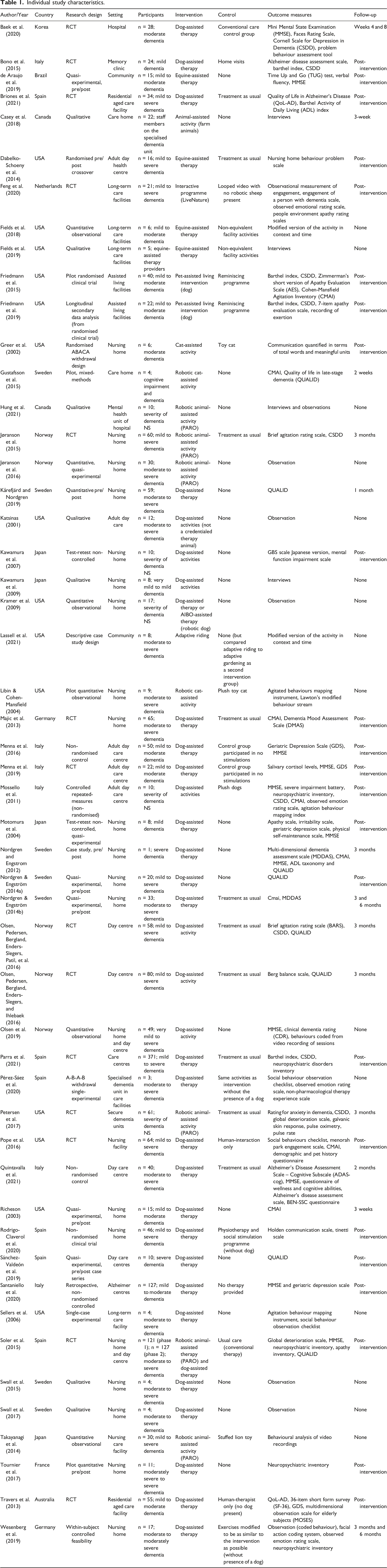
The majority of studies were conducted in Europe (n = 28) or the United States (n = 17) (Table 1). Most studies were conducted in care facilities (e.g., nursing homes, care homes) (n = 31), followed by day centres (n = 11), assisted living facilities (n = 2), hospitals (n = 2), the community (e.g., therapeutic riding centres) (n = 2), and memory clinics (n = 1). Two studies delivered their intervention in nursing homes and day care centres (Table 1).
Quality assessment
There was large variation in ratings, ranging from low to high methodological quality (20%–100% of quality criteria met; see Supplementary Table 2). The qualitative studies were generally rated as higher quality (80%–100%) compared to RCTs, quantitative non-randomised designs and quantitative descriptive designs (20%–100%).
Intervention characteristics
Interventions varied by type (e.g., therapy or activity), content, role of facilitator, delivery mode, frequency and duration, and animal species involved (Supplementary Table 3).
Intervention content
All interventions involved activities such as talking to or playing with the animal, petting the animal, or exercising with the animal (Supplementary Table 3). Both animal-assisted and robotic animal interventions frequently allowed participants to freely engage with the animal in any way they wished to do so, encouraging the participant’s autonomy (Greer et al., 2002; Gustafsson et al., 2015; Jøranson et al., 2015; Pope et al., 2016). Thirteen animal-assisted interventions introduced individually tailored protocols for each participant, based on their needs and preferences.
Role of facilitator
For animal-assisted interventions, the majority of interventions were delivered by professionally trained animal handlers (n = 32), whereas the majority of robotic animal interventions were delivered by care facility staff members (n = 5).
Delivery mode
Delivery mode varied between animal-assisted and robotic animal interventions, as the majority of animal-assisted interventions were delivered on a group basis (n = 31), whereas the majority of robotic animal interventions were delivered on an individual basis (n = 5).
Frequency and duration
There was a large variation in the frequency and duration of the interventions (Supplementary Table 3), with session length ranging from 3 minutes (Kramer et al., 2009) to a full day programme (Katsinas, 2000), and frequency ranging from one daily session for 4 days (Motomura et al., 2004) to one weekly session for 12 months (Sanchez-Valdeon et al., 2019).
Session lengths were longer for animal-assisted interventions compared to robotic animal interventions. The most frequent session length for animal-assisted interventions was 60 min (n = 15), compared to 30 min for robotic animal interventions (n = 3). The session duration never exceeded 30 min for robotic animal interventions. Additionally, animal-assisted interventions were delivered more frequently than robotic animal interventions, as animal-assisted interventions were more likely to be delivered weekly and robotic animal interventions were more likely to be delivered biweekly.
Animal characteristics
For animal-assisted interventions, dogs were the most commonly involved species (n = 34), followed by horses (n = 5). Two studies involved cats (Greer et al., 2002) and farm animals (Casey et al., 2018). For dog-assisted interventions, the majority of studies selected breeds characterised by certain traits (e.g., calm demeanour and controllability). The most common breed was a retriever (Labrador, golden, flat-coated) (n = 20), with other studies involving a range of dog breeds (Supplementary Table 3). Dogs were frequently selected who were certified in accordance with a national standard and/or had prior experience in animal-assisted interventions in care homes.
For robotic animal interventions, PARO the harp seal was the most commonly used animal (n = 6), followed by robotic cats (n = 2) and robotic dogs (n = 1). One study combined the use of a robotic sheep with an augmented reality display presenting video content of sheep to stimulate an experience of typical farm scenery (Feng et al., 2020).
Intervention outcomes
Studies included a wide range of outcomes measures (see Table 1), commonly evaluating agitation (n = 17); depression (n = 15), and quality of life (n = 12).
Agitation
Seventeen studies reported agitation as an outcome. In seven studies (6 = animal-assisted interventions; 1 = robotic animal intervention), a significant reduction in agitation was reported (Baek et al., 2020; Jøranson et al., 2015; Majic et al., 2013; Parra et al., 2021; Richeson, 2003; Sellers, 2006; Soler et al., 2015). Six studies (4 = animal-assisted interventions; 2 = robotic animal interventions) reported agitation decreased over time but was not found to be significant (Libin & Cohen-Mansfield (2004); Friedmann et al., 2015; Gustafsson et al., 2015; Mossello et al., 2011; Nordgren & Engström, 2014b; Tournier et al., 2017). In four studies, no benefits of taking part in animal-assisted interventions (n = 4) were found for agitation. Of the seven studies showing significant improvements (5 = RCTs; 2 = quantitative descriptive), six were rated as high quality and one was rated as moderate quality, providing confidence for the validity of their findings.
Depression
Fifteen studies reported depression as an outcome. In 9 studies (7 = animal-assisted interventions; 2 = robotic animal interventions), a significant improvement in depression scores were reported (Friedmann et al., 2015; Jøranson et al., 2015; Majic et al., 2013; Menna et al., 2016; Menna et al., 2019; Olsen, Pedersen, Bergland, Enders-Slegers, Patil, et al., 2016; Parra et al., 2021; Petersen et al., 2017; Travers et al., 2013). Three animal-assisted intervention studies reported improvement in depression scores as an outcome of the intervention but was not found to be significant (Friedmann et al., 2019; Mossello et al., 2011; Santaniello et al., 2020). Conversely, three animal-assisted intervention studies found no benefits of taking part in the intervention on depression scores (Baek et al., 2020; Bono et al., 2015; Motomura et al., 2004). Of the eight studies showing significant improvements (7 = RCTs; 1 = non-randomised), six were rated as moderate to high quality (meeting 60–80% of the quality criteria), and two were rated as low quality.
Quality of life
Twelve studies reported quality of life as an outcome. In six animal-assisted intervention studies, a significant improvement in quality of life was reported (Fields et al., 2018; Kårefjärd & Nordgen, 2019; Nordgren & Engström, 2014a; Olsen, Pedersen, Bergland, Enders-Slegers, Patil, et al., 2016; Sanchez-Valdeon et al., 2019; Travers et al., 2013). Three studies (2 = animal-assisted interventions; 1 = robotic animal intervention) reported positive trends in quality of life, although these were not statistically significant (Briones et al., 2021; Gustafsson et al., 2015; Lassell et al., 2021). However, in two animal-assisted intervention studies, no benefits of taking part were found (Nordgren & Engstrom, 2012; Olsen, Pedersen, Bergland, Enders-Slegers, & Ihlebæk, 2016). One study comparing a live dog with a robotic animal also reported a significant decrease in quality of life in the robotic animal group (Soler et al., 2015). Of the seven studies showing significant improvements (2 = RCTs; 3 = quantitative descriptive), four were rated as moderate to high quality (meeting 60–100% of the quality criteria), and one was rated as low quality.
Effects on outcomes
When pooling RCTs with similar outcomes (all of which were dog-assisted interventions), an overall effect was found in favour of the intervention groups for agitation (standard mean difference (SMD) = 0.74; 95% confidence interval (CI) = 0.25–1.23; Figure 2a). However, no effect on animal-assisted interventions were found for depression (SMD = 0.51; 95% CI = −0.14 – 1.16; Figure 2b), or quality of life (SMD = −0.03; 95% CI = −0.34 – 0.28; Figure 2c). (a) Comparison of agitation at longest follow-up in randomised controlled trials (RCTs). (b) Comparison of depression at longest follow-up in RCTs. (c) Comparison of quality of life at longest follow-up in RCTs.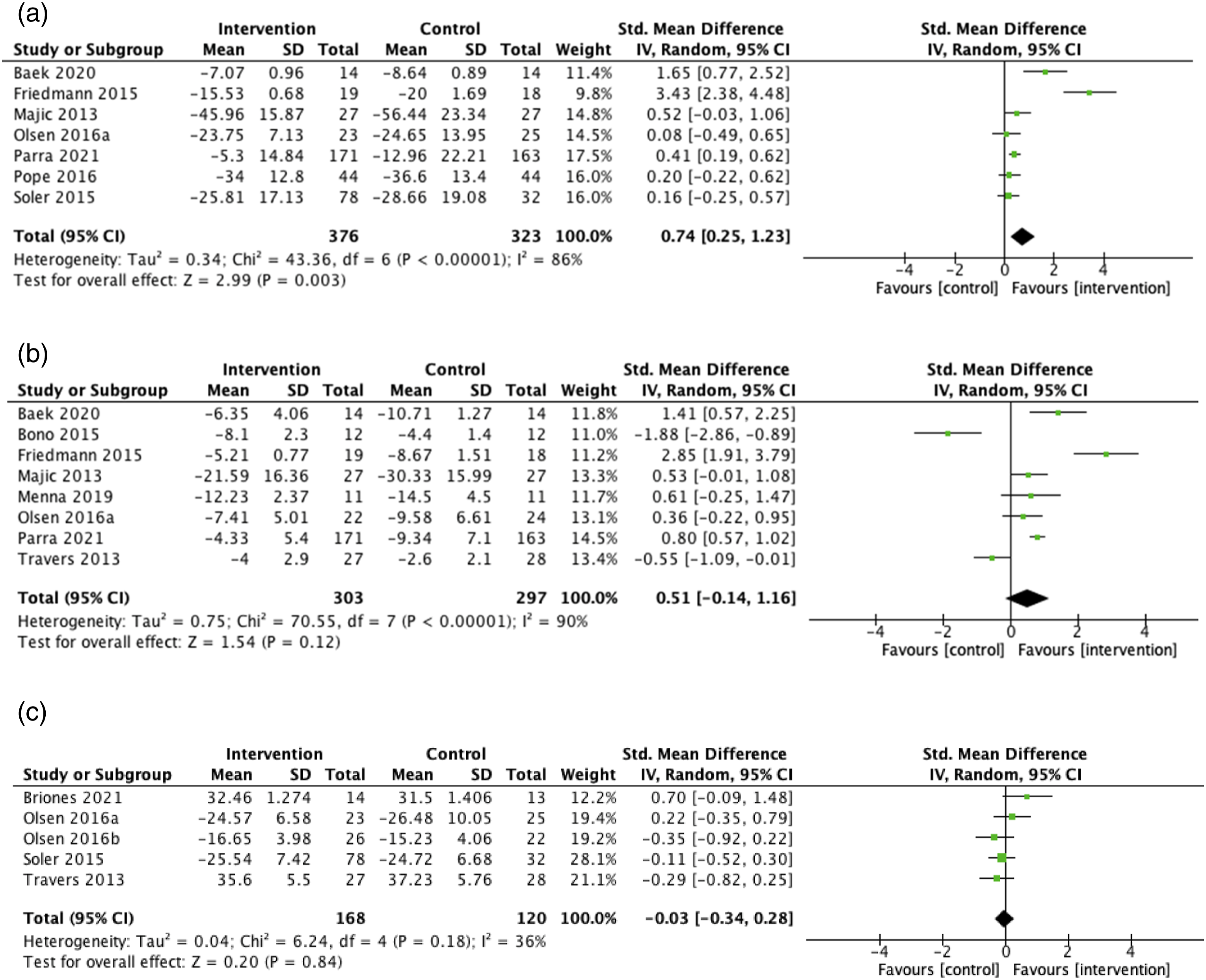
Potential mechanisms leading to impact of interventions
Potential mechanisms of intervention impact were suggested by authors of 37 studies (animal-assisted interventions = 29; robotic animal interventions = 8), (Supplementary Table 4). For both animal-assisted and robotic animal interventions, these included: (1) enhancing social connections; (2) providing engaging and meaningful activities, and (3) the affect-generating aspect of the human-animal bond. A fourth mechanism was identified for animal-assisted interventions only: (4) promoting physical activity. A brief narrative is provided for each mechanism below, and Supplementary Table 4 reports content presented from studies that contribute to our understanding of each mechanism.
Enhancing social connections
Robotic and live animals were described to act as a social facilitator and became the focal point for interaction in the respective intervention settings (Jøranson et al., 2015; Perez-Saez et al., 2020; Richeson, 2003). Engagement led to increased socialisation with peers and facilitators, and the animal provided a common topic that connected the participants and provided a positive focus for discussion and interaction (Fields et al., 2019; Greer et al., 2002; Lassell et al., 2021; Perez-Saez et al., 2020; Richeson, 2003). The animal (robotic or live) may be perceived as a connection within their social network, which may provide an enhanced sense of belonging and reduce loneliness (Baek et al., 2020; Rodrigo-Claverol et al., 2020).
Interacting with animals also appeared to provide an opportunity to establish physical contact, an experience that may enhance wellbeing and provide tactile stimulation (Fields et al., 2019; Perez-Saez et al., 2020; Swall et al., 2015, 2017; Travers et al., 2013; Wesenberg et al., 2019). The comforting nature of physical contact with the live animal was indicated as a potential mechanism for explaining enhanced emotional wellbeing (Fields et al., 2019; Lassell et al., 2021; Olsen, Pedersen, Bergland, Enders-Slegers, & Ihlebaek, 2016). Although this finding was predominantly reported for animal-assisted interventions, one robotic animal intervention study indicated that physical contact (e.g., holding the robotic animal) may reduce loneliness experienced by some residents (Gustafsson et al., 2015).
Two studies reported that animal-assisted and robotic animal interventions are better than plush toys for generating social interaction (Greer et al., 2002; Takayanagi et al., 2014). When comparing live cats to a plush cat, participants interacted with the live cats more than they did the plush cats (Greer et al., 2002). Takayanagi et al. (2014) compared a PARO seal with a stuffed lion and reported PARO initiated conversation, whereas there was a greater need for staff to initiate communication with participants when they were presented with the plush lion. Kramer et al. (2009) compared the impact of a live and robotic dog, and both dogs were found to increase socially interactive behaviour. Although these studies are rated as low quality, these findings suggest that both robotic and live animals have the ability to create a social environment compared to plush animals.
Providing engaging and meaningful activities
Many studies reported that animal-assisted and robotic animal interventions may provide engaging and meaningful activities to people with dementia (Dabelko-Schoeny et al., 2014; Fields et al., 2019; Gustafsson et al., 2015; Jøranson et al., 2016; Olsen et al., 2019; Perez-Saez et al., 2020; Rodrigo-Claverol et al., 2020; Swall et al., 2017; Travers et al., 2013). Studies frequently introduced individually tailored protocols or content for participants (animal-assisted interventions = 13; robotic animal intervention = 1) to ensure the content was meaningful for each person. By providing meaningful activity, participants may feel a responsibility of caring and a sense of usefulness (Swall et al., 2017). Studies of animal-assisted interventions also highlighted the importance of the whole experience including its meaningfulness, the physical environment and social stimulation components (Dabelko-Schoeny et al., 2014; Fields et al., 2019), rather than all impacts being related to the animal interaction alone. The authors noted that this may be more challenging to provide within a formal care facility (Dabelko-Schoeny et al., 2014).
Affect-generating aspect of the human-animal bond
Another mechanism considered was the affect-generating aspect of the human-animal bond. Interacting with live animals appeared to provide the opportunity to experience a bond with an animal without the presence of judgement, which may have influenced positive outcomes (Fields et al., 2019; Kawamura et al., 2009; Perez-Saez et al., 2020). The authors suggested that it was the human-animal bond based on affection that implicitly drove participant engagement and interaction (Perez-Saez et al., 2020). This potential mechanism was not just identified for live animals only. One study reported that PARO the harp seal was able to generate affection, emotional attachment and invite a sense of relationship in the dementia study population (Hung et al., 2021). The authors stated that emotional bonding with PARO was beneficial to participants wellbeing, aligning with the positive affect generating aspect of the human-animal bond found in live animal relationships.
Promoting physical activity
Many animal-assisted interventions promoted participants’ physical activity, which can have subsequent health benefits for the individual. For equine-assisted and dog-assisted interventions, activities were offered to promote physical activity that would enhance motor skills (e.g., riding the horse, walking, or grooming the horse or dog) (Supplementary Table 3). As a result, studies reported improvements in balance and functional capacity (De Araujo et al., 2019; Olsen, Pedersen, Bergland, Enders-Slegers, & Ihlebæk, 2016), increased physical activity over time (Friedmann et al., 2015), and enhanced motivation to engage in physical activity (Dabelko-Schoeny et al., 2014; Fields et al., 2018).
Overall, multiple characteristics and underpinning mechanisms may offer potential explanations for the outcomes of both animal-assisted and robotic animal interventions. Despite the varying intervention designs and methods, a number of common features and mechanisms were identifiable across the successful animal-assisted and robotic animal interventions. These individual characteristics and mechanisms are not mutually exclusive, and it is likely that multiple characteristics and mechanisms best explain how these interventions result in their observed effects. Figure 3 is an initial programme theory of how animal-assisted and robotic animal interventions may ‘work’ within dementia care (Skivington et al., 2021). Initial programme theory of how animal-assisted and robotic animal interventions may ‘work’ within dementia care.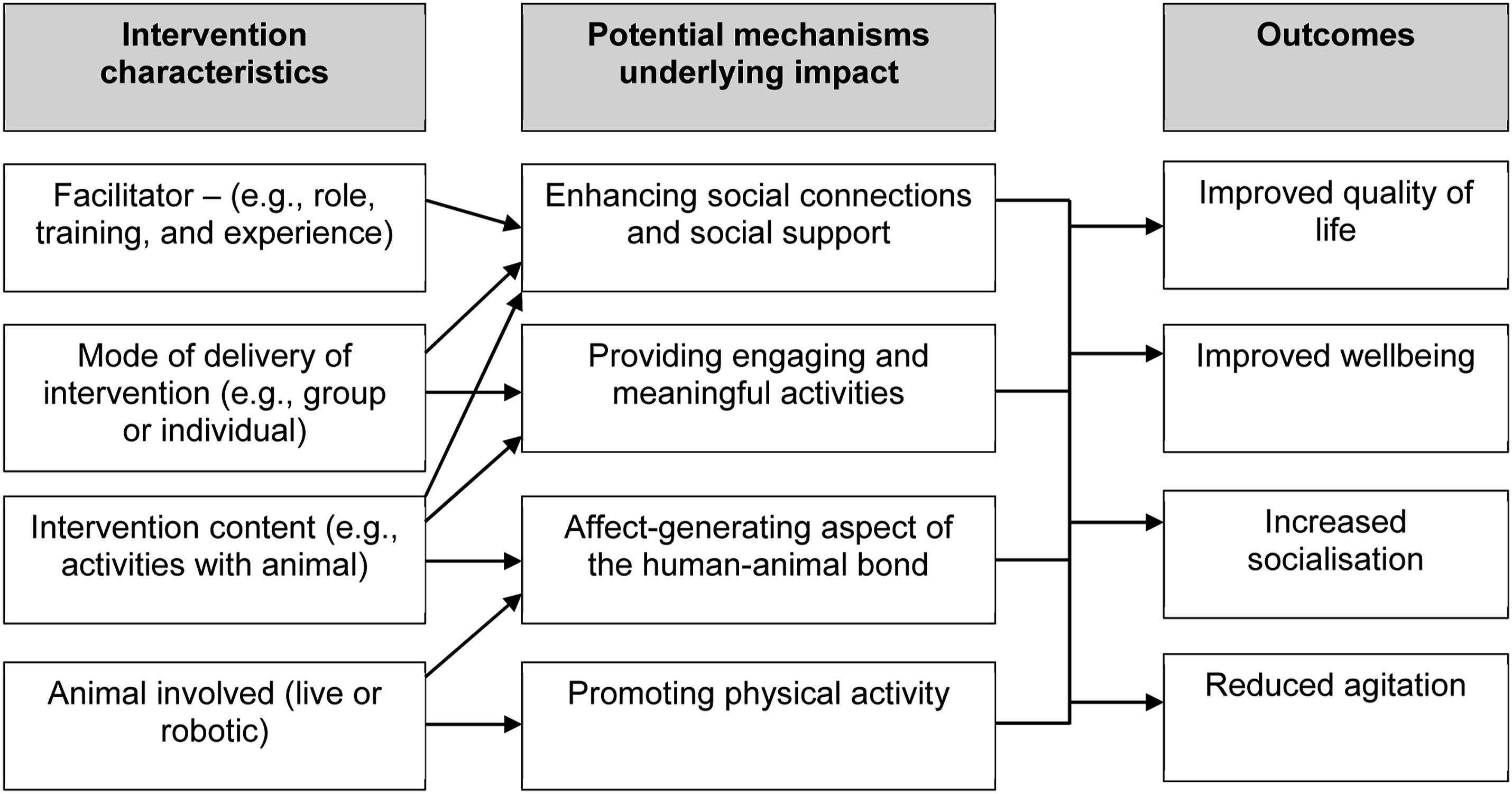
Discussion
To the best of our knowledge, this is the first review to examine the characteristics of robotic animal and animal-assisted interventions (including all species) delivered to people with dementia, their effectiveness, and the potential mechanisms of intervention impact. Our narrative findings suggest that animal-assisted and robotic animal interventions appear to be promising in enhancing behavioural and psychological outcomes for people with dementia. However, the meta-analyses were restricted to a small number of RCTs implementing dog-assisted interventions, which were unlikely to be sufficiently powered to detect effects. We were unable to conduct a meta-analysis on the effectiveness of robotic animal interventions and animal-assisted interventions involving other species due to the dearth of research in these areas. Therefore, our overall findings are preliminary, but do contribute important pointers in terms of interventions characteristics and potential mechanisms. This is an important contribution as this has not been investigated in detail, and failure to advance the evidence base is likely to result in poor, potentially unethical practice (Ratschen & Sheldon, 2019).
Although the evidence base is improving, there is largely an absence of rigorous methodology to demonstrate the benefits, and findings are mixed (Stern & Chur-Hansen, 2013; Yakimicki et al., 2019). The studies in this review frequently included small sample sizes that could undermine the internal and external validity of the study (Faber & Fonseca, 2014), and there was a lack of RCTs to ascertain the effectiveness of animal-assisted and robotic animal interventions, with insufficient reporting of content for both intervention and control groups. In practice, complex interventions are often implemented in a diverse manner by various stakeholders in different settings, all of which can affect the outcomes (Pawson et al., 2004). This variability raises challenges in terms of developing an optimal animal-assisted intervention and/or robotic animal intervention manual that could be adopted by providers for implementation in further practice.
There has been a growing recognition in the field that standard RCT designs may not be suitable for complex intervention evaluation (Skivington et al., 2021), as this approach does not allow a detailed understanding of how different intervention elements affect outcomes of importance to participants or staff delivering them. There is currently work underway to examine more appropriate trial designs, which aim to increase the efficiency with which complex intervention research generates knowledge that contributes to health improvement (Skivington et al., 2021). Nonetheless, it is vital rigorous RCTs should be conducted to support the use of animal-assisted and robotic animal interventions for people with dementia to provide the scope to develop interventions more rigorously based on hypothesised mechanisms.
Characteristics of animal-assisted and robotic animal interventions
Interventions in this review varied substantially in terms of mode of delivery, frequency, and duration. Compared to individual interactions, group-based interventions with live animals appeared to offer participants the opportunity to interact and engage with the animal, the facilitator, and their peers at the same time. Findings suggested that the benefits of animal-assisted interventions may be due to the combined effects of social stimulation and enriching, meaningful activity (Dabelko-Schoeny et al., 2014; Fields et al., 2019). Although robotic animals offered similar benefits for promoting socialisation, individual interactions were more common. This mode of delivery allowed the participants to interact and engage with the robotic animal in a very personalised way (Gustafsson et al., 2015). Furthermore, individual interventions can minimise the interactions with others in the setting, indicating that the benefits are due to the intervention rather than any confounding variables. Of the robotic animal studies that reported dementia severity, the majority included participants with severe dementia. Conversely, the majority of animal-assisted intervention studies included people with milder dementia. It may be that group sessions are feasible for individuals with milder dementia, whereas individualised sessions may be necessary for those with more advanced dementia. However, one animal-assisted intervention study reported that improvements in social behaviour were found to be unrelated to severity of dementia (Quintavalla et al., 2021).
Our review identified a lack of evidence investigating the optimal frequency and duration of both interventions for participants with dementia. Evidence did report that weekly one-hour sessions were beneficial for both the participants and facilitators (Tournier et al., 2017; Travers et al., 2013), aligning with previous research that reported intensive animal-assisted interventions may lead to an exhaustion of intervention effects in older adults (Virués-Ortega et al., 2012). It is also crucial to consider animal welfare during animal-assisted interventions, as long sessions may lead to overburdening the animal if the same animal is involved in several and/or long sessions (Marinelli et al., 2009). Thus, when developing guidance for animal-assisted or robotic animal intervention delivery in terms of frequency, duration and mode of delivery, it may be beneficial to consider the individual abilities and impairments that can be supported, the outcomes hoped to be achieved, and to decide on session characteristics based on the needs and preferences of the intended participants (Kachouie et al., 2014). Based on the findings from this review, a one-hour session may potentially be the minimum recommended ‘dose’ for this population, but it is important to develop such guidance with animal behaviourists and other specialists in the field to ensure both the needs of the client and the animal(s) are met.
Intervention content may be more important to consider than intervention length. Both animal-assisted and robotic animal interventions frequently provided engaging and meaningful activities that maximised engagement (Feng et al., 2020; Fields et al., 2018; Jøranson et al., 2015). Engagement in activities beyond routine care is an important indicator of quality of life in care facilities (Olsen et al., 2019), and is important for improving mood and a sense of independence (Travers et al., 2013). In order to maximise engagement, many studies adopted a person-centred approach in their intervention design. For example, the content was frequently tailored to individual needs and abilities and offered a positive social environment to highlight individual strengths. Therefore, this review has identified that both animal-assisted and robotic animal interventions may address unmet needs of participants by offering meaningful activity, stimulation, pleasurable social interaction, and comfort through physical contact (Travers et al., 2013). The current findings contribute to the overall discussion about the positive impact of person-centred activities on people with dementia. Interventions should provide participants with the opportunities to engage in tailored, high-interest and enjoyable activities with animals, whether these are live or robotic.
Additionally, the role of the facilitator differed between animal-assisted and robotic animal interventions. Interventions with live animals were more likely to be delivered by a professionally trained animal handler, whereas interventions with robotic animals were frequently delivered by care staff. This is a commonly cited characteristic in robotic animal intervention research (Koh et al., 2021), and robotic animal interventions are often deemed a valid and potential alternative to animal-assisted interventions due to the lack of requirement for specialist trained facilitators (Peluso et al., 2018). However, research has highlighted that care staff themselves recognise they require more training to effectively implement interventions involving robotic animals (Abbott et al., 2019), and training should include more than an explanation of technical issues (Melkas et al., 2020). In order to enhance the positive outcomes achieved from robotic animal interventions, it is important that care staff receive appropriate training and support (Abbott et al., 2019).
Lastly, dogs were the most commonly involved live animal (n = 34) and PARO the harp seal was the most commonly used robotic animal (n = 6). PARO is the most common therapeutic robotic animal used in studies with people with dementia (Bemelmans et al., 2012), and the prevalent involvement of dogs may be attributable to dogs’ well-established emotional connections with humans and their receptiveness to training (Bert et al., 2016; Jain et al., 2020). This review suggests that dog-assisted interventions and PARO the harp seal are promising interventions to improve wellbeing for people with dementia. However, rigorous RCTs are required to further our understanding of the impact of interventions involving other species, breeds, and robotic animals. The current review indicates the benefits that animal-assisted interventions involving other species and robotic animal interventions may have.
Are robotic animals an appropriate substitute for live animals?
From the limited insight we have in relation to robotic animal interventions within dementia care, they appear to be promising for people with dementia, in some studies offering similar benefits for increasing socially interactive behaviour as a live animal. However, this was not found for plush toy animals, suggesting the interaction with and feedback from the animal plays an important role in influencing positive outcomes. The study which found a decline in quality of life in the robotic animal intervention compared to the animal-assisted intervention may have a number of possible explanations. Firstly, the robotic animal’s novelty effect may decline over time, although this may not be an effect exclusive to robotic animal interventions (Kawamura et al., 2007; Tournier et al., 2017). Alternatively, participants may be unwilling to engage with stimulus that is too unfamiliar to be easily accepted, a commonly cited barrier in robotic animal intervention implementation (Banks et al., 2008). This may be more pertinent to studies implementing PARO the seal, where the reduction in quality of life was found, compared to more familiar robotic animals such as dogs and cats (Moyle et al., 2018).
Additionally, live animals have the ability to read human body language, show genuine affection and initiate intuitive and spontaneous interactions (Filan & Llewellyn-Jones, 2006), all of which contribute to the affect-generating aspect of the human-animal bond. Although content presented in relation to potential mechanisms indicated that PARO was able to generate emotional attachment and invite a sense of relationship (Hung et al., 2021), this was unidirectional as PARO is clearly unable to create a reciprocal bond. Despite this, the shape and behaviours of robotic animals are designed to mimic a live animal, and therefore, are able to display the repertoire of behaviours and emotions that are central to the affect-generating aspect of the human-animal bond (Melson et al., 2009). It appears that robotic animals are able to evoke an association with the powerful companionship benefits of living animals and are thus viewed as a social companion. This aligns with our current findings as robotic animals often acted as a social facilitator for participants with dementia.
When considering robotic animal interventions as replacements for animal-assisted interventions, a common observation is that robotic animals may resolve concerns around infection, injury, animal care and cleanliness (Feng et al., 2020; Kramer et al., 2009; Petersen et al., 2017). Therefore, robotic animal interventions may offer an opportunity to specific populations to stimulate social interaction without the difficulties associated with live animal visits. However, it is important to consider that robotic animals come with their own hygiene issues. For example, some robotic animals may be challenging to clean effectively, such as those covered with synthetic fur (Libin & Cohen-Mansfield, 2004). Conversely, other robotic animals do not have a soft covering (Kramer et al., 2009). This may facilitate infection control, but could affect engagement as the robot looks and feels much less like a live animal (Melson et al., 2009). Regardless of the type of robotic animal, it is important to have a strict infection policy in place as effectively cleaning the robotic animal is an essential part of the implementation process (Hung et al., 2021). Despite the increasing use of both animal-assisted and robotic animal interventions, the development and/or application of infection control policies was not reported by all studies; information which is required to appropriately implement and evaluate the interventions. Previous literature has indicated that infection control protocols for animal-assisted interventions are variable and potentially inadequate (Bert et al., 2016; Lefebvre et al., 2006). Future interventions should ensure adequate reporting of their applied policies, particularly in light of the current Covid-19 pandemic.
Overall, as robotic animals develop and become increasingly social-autonomous, reactive, and personified, it is possible that people may anthropomorphise robotic animals and treat them like live animals (Melson et al., 2009). However, a greater understanding of robotic animal interventions is required to facilitate understanding of human-robot interactions and identifying an optimal robotic animal intervention model. In situations where animal visits are not feasible, robotic animals appear to be promising in terms of enhancing behavioural and psychosocial outcomes for people with dementia and appear to have a place within the complex relationships that humans have with animals.
Limitations
The meta-analyses only included a small number of RCTs, all of which were very small in size and therefore unlikely to be sufficiently powered to detect effects. Additionally, the meta-analyses were restricted to dog-assisted interventions only, so findings do not extend to interventions involving other species or robotic animals. Therefore, it remains difficult to ascertain any definitive conclusions in relation to whether animal-assisted and robotic animal interventions are effective for people with dementia. However, many reviews investigating the effectiveness of animal-assisted and robotic animal interventions within dementia care have not conducted meta-analyses, despite being appropriate when two or more studies can be meaningfully pooled (Ryan, 2016). The current meta-analyses contribute to our understanding, as they indicate animal-assisted interventions are promising for reducing agitation in people with dementia and highlights that highly controlled and adequality powered studies are required to provide more robust evidence on the effects of animal-assisted and robotic animal interventions within dementia care. A further limitation of this review is that it can only reflect evidence from which it is derived. A number of studies did not include specific detail about certain components of the intervention (e.g., the context/setting). Lastly, included papers were only published in English, excluding non-English language studies that might have contributed to further understanding.
Conclusion
Animal-assisted and robotic animal interventions appear to be promising in enhancing behavioural and psychological outcomes for people with dementia, but the evidence base in this area needs to be further developed. When designing and evaluating interventions, special attention should be given to potential mechanisms of effect and fundamental characteristics that can influence outcomes such as the session content, delivery format and role of facilitator. Facilitators must ensure that interventions are targeted to the experiences, needs and level of cognitive impairment of participants, while considering the welfare of the animal. Robotic animals may be an appropriate substitute for live animals, as they offer meaningful and engaging activities with the opportunity for increased social interaction. However, a greater understanding of robotic animal interventions is required to harness the benefits that can be derived from their use.
Supplemental Material
Supplemental Material - Animal-assisted and robotic animal-assisted interventions within dementia care: A systematic review
Supplemental Material for Animal-assisted and robotic animal-assisted interventions within dementia care: A systematic review
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Tees, Esk and Wear Valleys NHS Foundation Trust Research Capability Funding Award. Emily Shoesmith and Elena Ratschen are supported by the NIHR Yorkshire and Humber Applied Research Collaboration: https://arc-yh.nihr.ac.uk.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
