Abstract
The aim of this study was to assess in practice whether assistive technologies support and facilitate the work of a family caregiver or care staff, and whether these technologies support the independence of a person with a memory disorder. A comprehensive set of supportive devices and alarm systems were experimentally tested in the care of five test subjects in an assisted living facility by eight nurses, and in the care of four test subjects in a home environment by three family caregivers and one care team. Questionnaires, diaries and logged data were used to evaluate the benefits of the devices. Simple aids and alarm systems that did not need much adjusting were considered most useful by caregivers and nurses, though multiple false alarms occurred during the test period. Technical connection problems, complex user interface, and inadequate sound quality were the primary factors reducing the utility of the tested devices. Further experimental research is needed to evaluate the utility of assistive technologies in different stages of a memory disorder.
Keywords
Introduction
The number of people with a memory disorder is expected to increase greatly in the near future (World Health Organization (WHO), 2015). Age-related memory disorders, such as Alzheimer’s disease or vascular dementia, are progressive diseases and their symptoms vary widely among individuals (Alzheimer's Society, 2015a). Current treatment may alleviate the symptoms, but did not cure the condition or stop its progress. A person who suffers from one of these memory disorders needs increasing assistance (Alzheimer's Society, 2015b). Providing this assistance can cause considerable strain to both family caregivers and nursing staff (Adelman, Tmanova, Delgado, Dion, & Lachs, 2014; Morgan, Semchuk, Stewart, & D'Arcy, 2002). Social isolation, lack of choice in being a caregiver, female sex, financial stress, and low educational attainment were found as risk factors for a family caregiver burden (Adelman et al., 2014).
In this article Assistive Technologies (AT) refer to products, equipment, and systems designed for use by people with a memory disorder and also by their caregivers, for the purpose of enhancing their daily living. Numerous assistive devices and alarm systems are available for people with dementia (Gibson et al., 2014; Gibson, Dickinson, Brittain, & Robinson, 2015; Stakes, 2008). The utility of portable one-button personal alarms (Personal Emergency Response Systems (PERS)) in real world is limited due to the reluctance of users in using their alarm system to call for help (Fleming, Brayne, & Cambridge City, 2008; Heinbüchner, Hautzinger, Becker, & Pf, 2010). This has led to the development of automated alarm systems, such as fall detectors (Jämsä, Kangas, Vikman, Nyberg, & Korpelainen, 2014; Noury, Rumeau, Bourke, & ÓLaighi, 2008) and unobtrusive integrated systems with wireless sensors (Rosetta, 2015). Devices such as simple touch screen video communication devices (Astell et al., 2010; Boman, Lundberg, Starkhammar, & Nygard, 2014), calendar clocks for time management, reminiscence aids, and games for entertainment (Gibson et al., 2014) are also available. The multiple sensors in wireless mobile devices provide possibilities to develop applications for care of people with dementia, for example global positioning system (GPS) applications to prevent wandering and getting lost (Bin Xiao, Asghar, Jamsa, & Pulii, 2013; Sposaro, Danielson, & Tyson, 2010).
The utilization of AT in the care of people with a memory disorder is considered positive (Pilotto et al., 2011; Rosenberg, Kottorp, & Nygård, 2012). Caregivers and nursing staff play an important role in adopting a device as a part of everyday life (Gibson et al., 2015). They would benefit from the easier monitoring and increased independence of a person with a memory disorder, increased safety, unobtrusive observation, and reduction of fears and worries (Olsson, Engstrom, Skovdahl, & Lampic, 2012; Pilotto et al., 2011; Rosenberg et al., 2012). The AT is considered important factor in retention of existing skills (Rosenberg et al., 2012). There are few experimental research results from benefits of using AT in elderly homecare (Martin, Kelly, Kernohan, McCreight, & Nugent, 2008; Pietrzak, Cotea, & Pullman, 2014).
The Joint Municipal Authority of Wellbeing in Raahe District (Finland) is responsible for the social care and healthcare in Raahe and two other nearby municipalities. A new pilot test site (MemoryHelp apartment) has been developed in conjunction with an assisted living facility for enabling assessment of existing devices and systems in practice, in order to improve the care of people with memory disorders and reduce institutional care. This MemoryHelp apartment is equipped with a comprehensive set of supportive devices and alarm systems. The selection process has been described elsewhere (Nauha et al., 2015).
The goal of this study was to assess (1) whether AT can support and facilitate the work of care staff, (2) whether AT can support and facilitate the work of a family caregiver, and (3) whether AT can support the independence and security of a person with memory disorder.
Materials and methods
The device listing of tested assistive technology. Devices were in experimental use in the MemoryHelp apartment and in real home environment.

Seniortek Oy, www.seniortek.com
Stella Oy, www.stella.fi
Pieni piiri Oy, www.circly.com
Dementia Online Shop, www.dementiaonlineshop.com
Sanamaailma, www.sanamaailma.net/vihrea_puhuva_valokuva-albumi
Lärum Förlaget, http://larum.fi/suomeksi/pallopeitto/
Information of the participants: the residents in the MemoryHelp apartment and subjects in home tests.
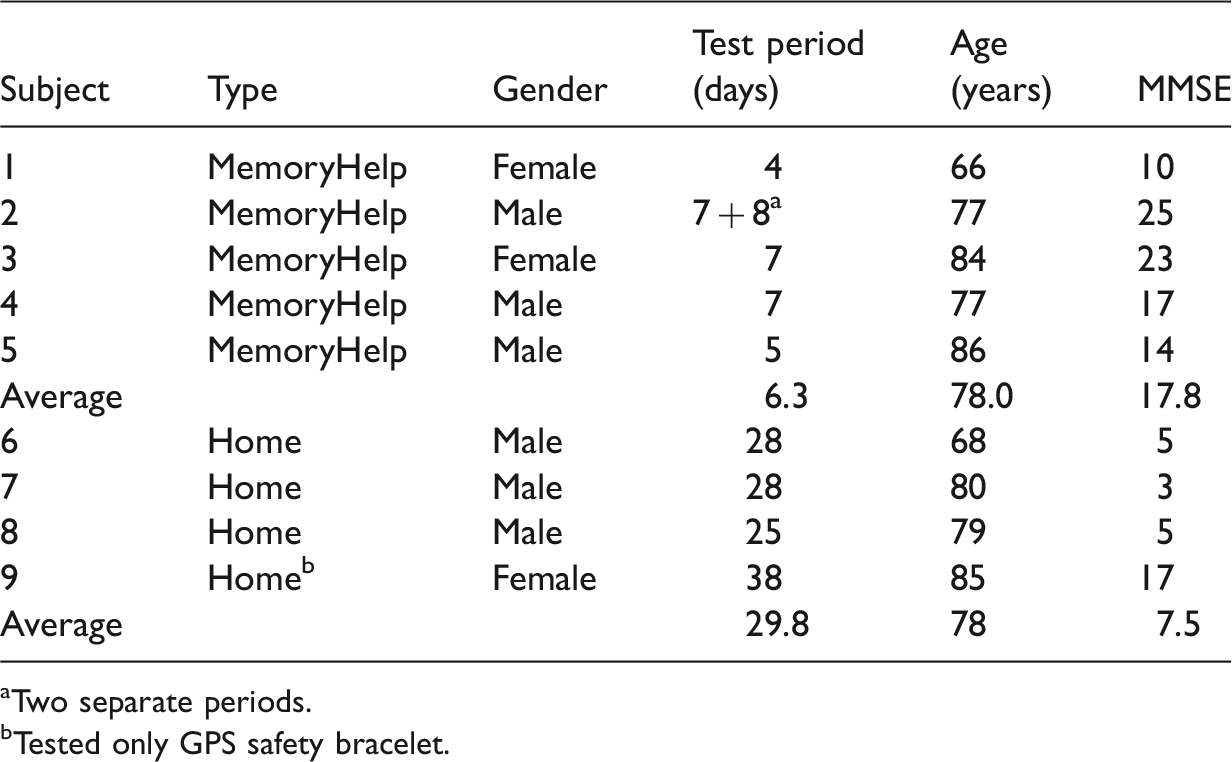
Two separate periods.
Tested only GPS safety bracelet.
The research protocol is introduced in Figure 1. The following background information of test subjects was gathered at baseline: Mini Mental State Examination (MMSE) score (Folstein, Folstein, & McHugh, 1975), age, and gender. The MMSE is a widely used screening and evaluation tool for the stage of dementia, with cutoff points of 24/30 for mild, 20/30 for moderate, and 12/30 for severe dementia (Tests for Alzheimer's disease and dementia, 2016). In the home test, family caregivers filled the Carers of Older People in Europe questionnaire (Cope index; Juntunen & Salminen, 2012) in order to get information about the impact of AT on experience of caregiver’s burden. The COPE index has been developed and validated as European collaboration for the evaluation of the coping and support needed by caregivers caring for an elderly family member with dementia (Balducci et al., 2008). The latest version is based on 15 questions with three subscales: positive and negative impacts of caregiving, and the quality of support from family, friends, neighbors, or social care. The index has also been translated into Finnish and shown to correlate with the quality of life of family caregivers in Finland (Juntunen & Salminen, 2012). The COPE index was also already in use in Raahe district.
The research protocol, the used methods, and reached information.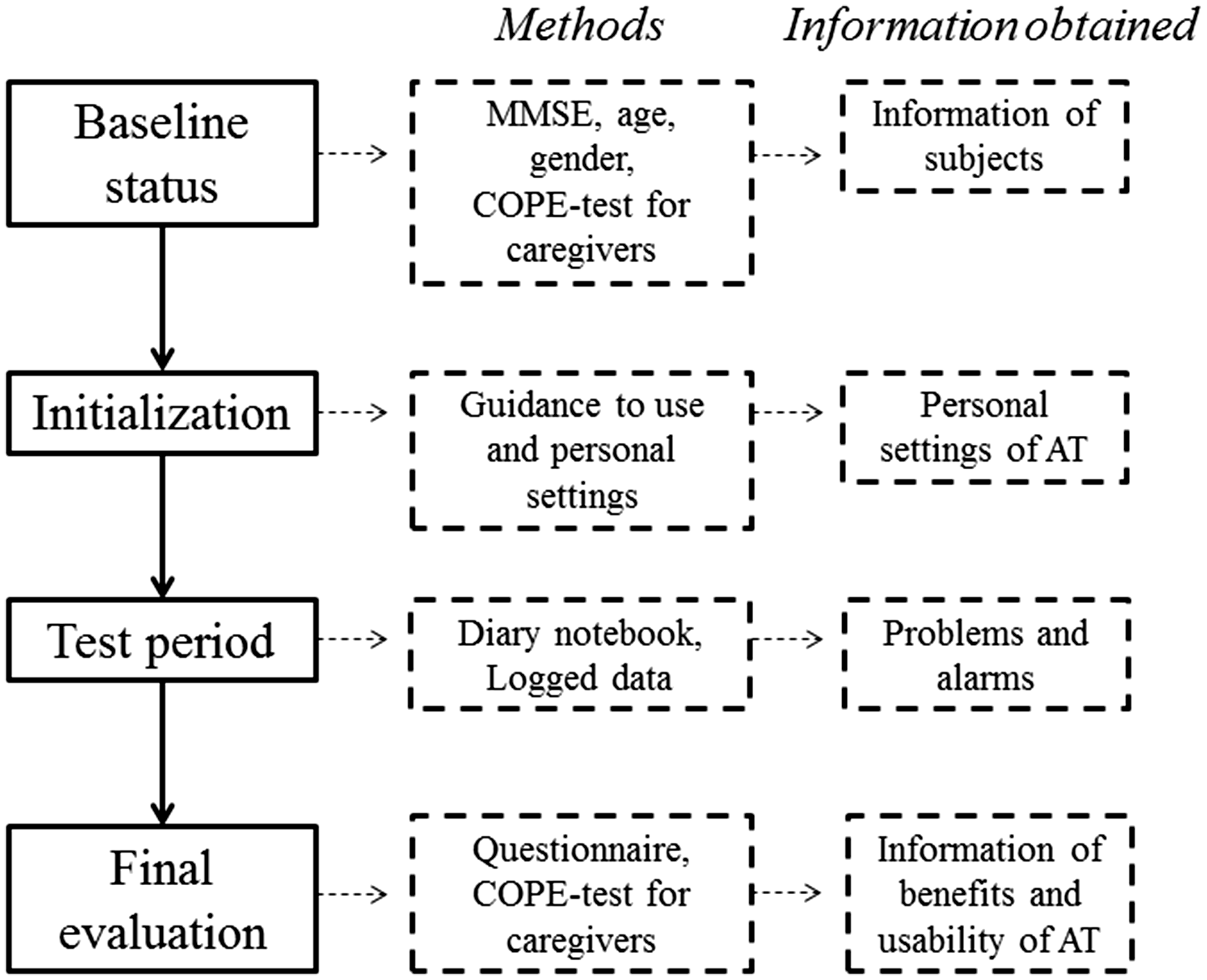
Personal settings for the various devices during the test period.
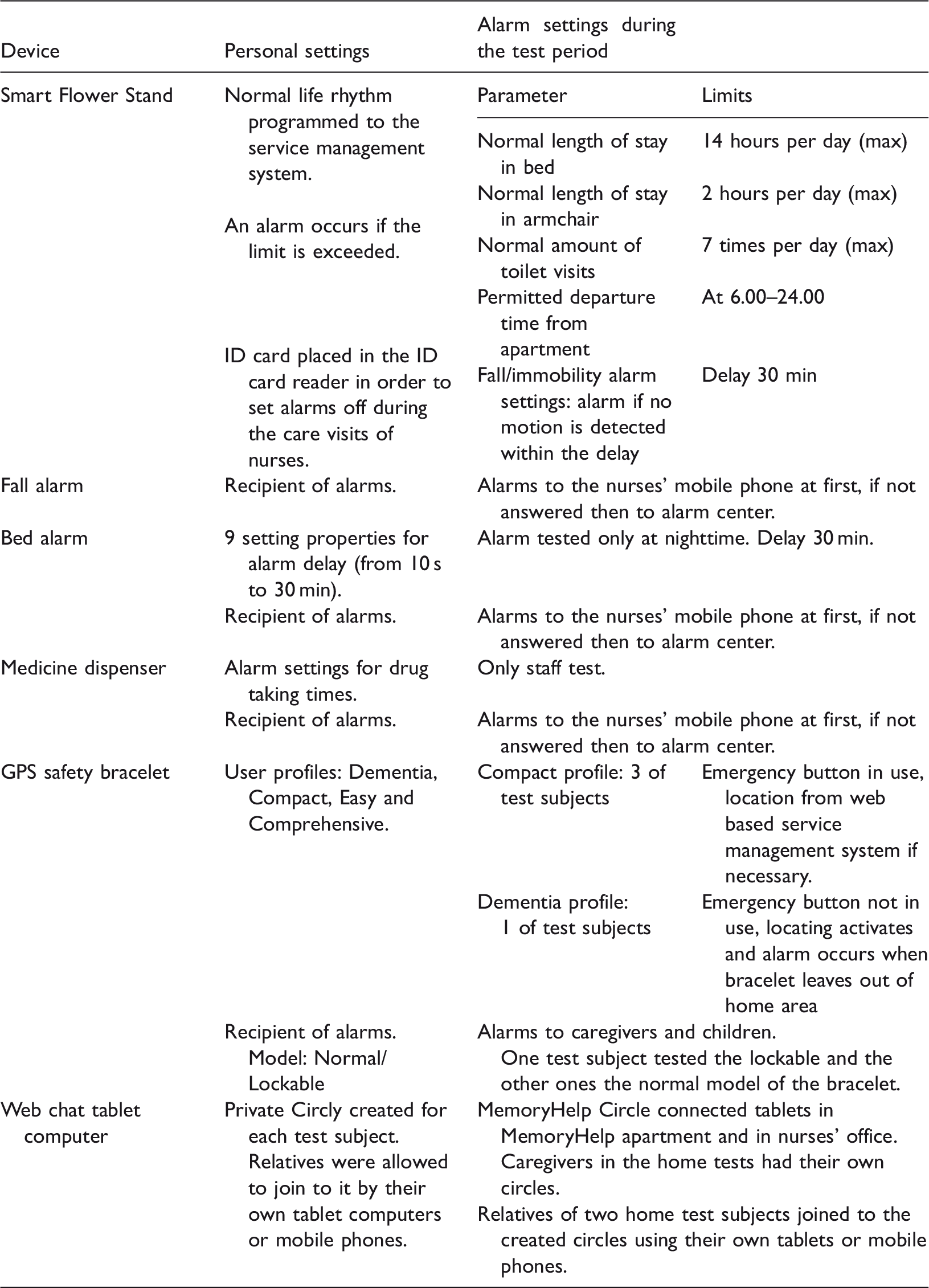
During the test period they were asked to keep track of alarms and any technical problems in a diary notebook as follows: Date and time, device in question, and the reason of alarm/technical problem. Prepared forms for this structured information were given to the caregiver participants for use at home. The nurses used an unstructured notebook to write down the requested information, which was kept in the nurses’ office in the assisted living facility. The gathered data were transferred to Excel spreadsheet for review and analysis. In addition, logged data were gathered from the Smart Flower Stand-service and GPS safety bracelet. Smart Flower Stand-service automatically gathered information of average bed time, average length of stay in armchair, average length of stay in the living room, and the number of toilet visits. This data was retrieved at the end of the testing period. The logged data from GPS safety bracelet included timestamps of events (departure from home, alarm button press, signal loss) and was received in table form from the technical service. Fall alarm and bed alarm logs were only available for alarms that went to the alarm center, not those responded to locally by nurses. The logged data were compared and, if necessary, supplemented with diary notes. The research person who faced some technical difficulties gave guidance and contacted customer support if necessary.
Questions of functional utility and usability issues of the tested AT.

Home use only.
Results
Summary of the results. Number of nurses and caregivers given as a portion of those who responded that they had used the device in their work.
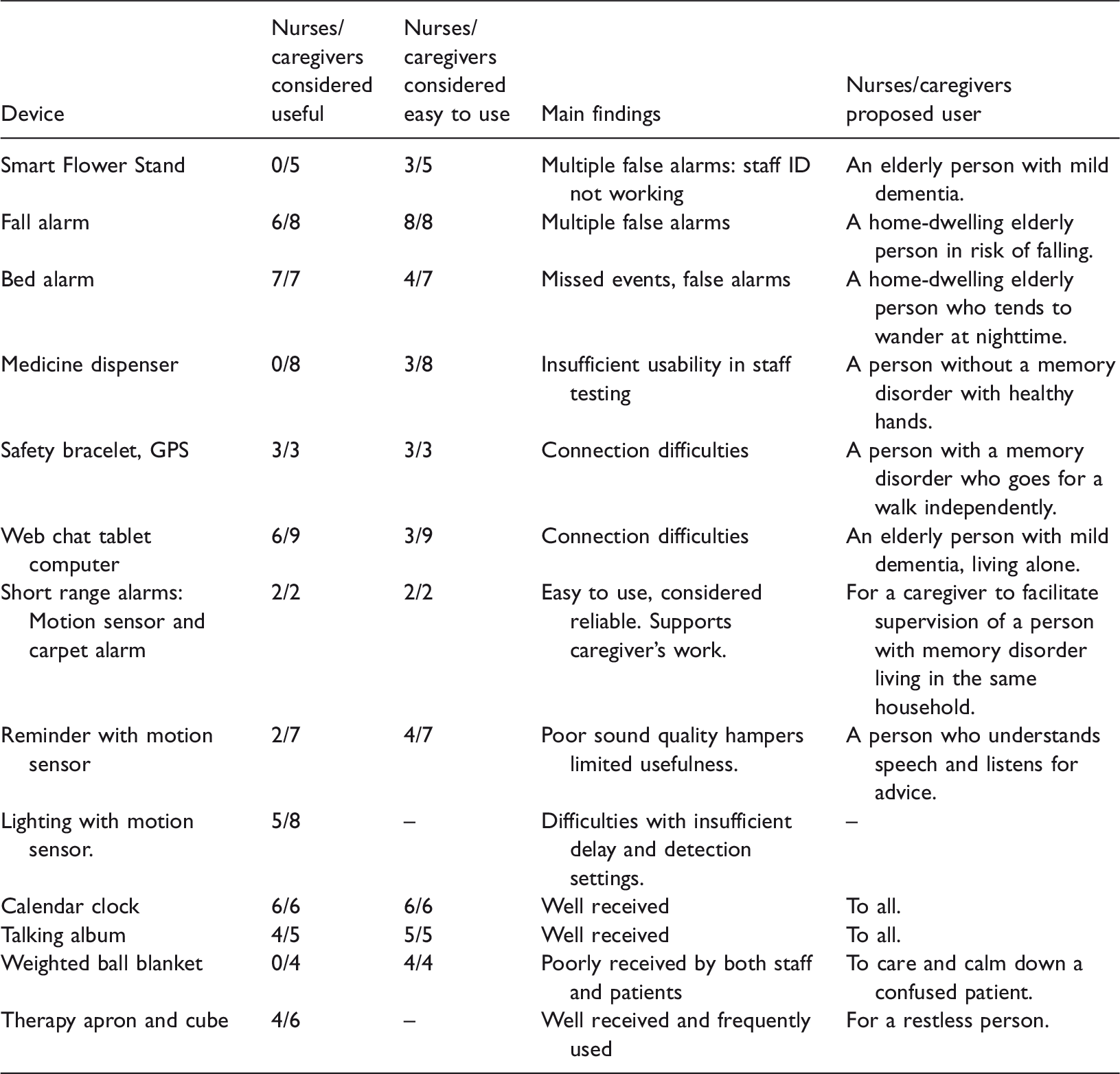
Smart Flower Stand
The flower stand was not considered useful. The nurses reported receiving dozens of false alarms during the first test week. The ID card reader for staff had technical problems, and alarms could not be disabled for staff visits. The problem could not be solved during the study. Starting from week two, the fall/immobility alarm was not in use. Logged data from the system corresponded to realistic and known events. For example, the average number of toilet visits per day was 20, which also includes cleaners’ and nurses’ visits in the toilet. Similarly, the average bedtime per day (4.2 hours) corresponded to the apartment being unoccupied on some days during the test period. The average length of stay in armchair was 3.5 hours per day, and in the living room 8.4 hours per day.
Devices connected to the safety phone service
The fall and bed alarms connected to the safety phone service were considered useful by most participants. There were some problems in activating the bed alarm throughout the testing period. Attempts to turn on the device caused false alarms. No actual fall events occurred, but the fall alarm caused 10 false alarms during dressing or other normal daily activities. The medicine dispenser was tested by the nurses and deemed too difficult to learn and use, as it required hand strength and dexterity. Based on this evaluation it was not installed in the MemoryHelp apartment.
GPS safety bracelet
All respondents considered the GPS safety bracelet useful, and that it improved the safety of the test subjects. According to the feedback, two test subjects were able to continue their independent walks thanks to the GPS bracelet. Connection difficulties disturbed the use of the GPS safety bracelet, which can be seen from the logged data and from diary notes. Also the batteries had to be charged daily. Two of the four test subjects did not wear the bracelet willingly and took it off sometimes. The lockable model was considered usable because the device could not be taken off and misplaced.
Web chat tablet
Most of the nurses considered that the Circly web chat tablet was useful in the care of test subjects. The tablet computer was used by two family caregivers of the home-dwelling subjects, to communicate with their children. One caregiver also used it for communication with caregiving coordinator and participating in interest-based groups. Connection difficulties disturbed the test use of video phones. The problem of using the mobile phone application of Circly was that the application consumed a lot of power and phone’s battery run out of power quickly.
Devices connected to short range audio alarm (motion sensor and carpet alarm)
Both caregivers considered the motion sensor useful. Both had selected to place it by the door to monitor exits. Feedback on the carpet alarm varied. One caregiver was woken up by the carpet alarm by the bed although the person with a memory disorder did not need help during bathroom visits. The other caregiver was able to sleep better at nights, because she knew she would be woken up if the person with a memory disorder left the bed.
Reminder with motion sensor
The reminder was considered easy to use and over half of the respondents considered it useful. The primary limiting factor, mentioned by seven respondents, was the poor sound quality.
Lighting with motion sensor
Five of eight nurses considered the lighting with motion sensor useful in the care of test subjects. The delay in the toilet was occasionally too short, and test subjects were unable to activate the light again from the toilet seat. This caused unnecessary risk. Continuous dim lighting was suggested as an alternative or necessary supplement.
Calendar clock, talking album, therapy apron and cube, and weighted ball blanket
The calendar clock was considered useful in the care of the test subjects. The benefits of analog display and night-time visibility were specifically mentioned. The talking album, the therapy apron and cube provided activity and tinkering for restless test subjects. The weighted ball blanket was not found useful in the care of test subjects by any of the nurses; rather it had caused anxiety and was considered an additional risk factor if it fell.
The COPE scores of caregivers as defined at baseline status and in the final evaluation. Higher scores indicate greater negative impact or positive value, or improved quality of support.
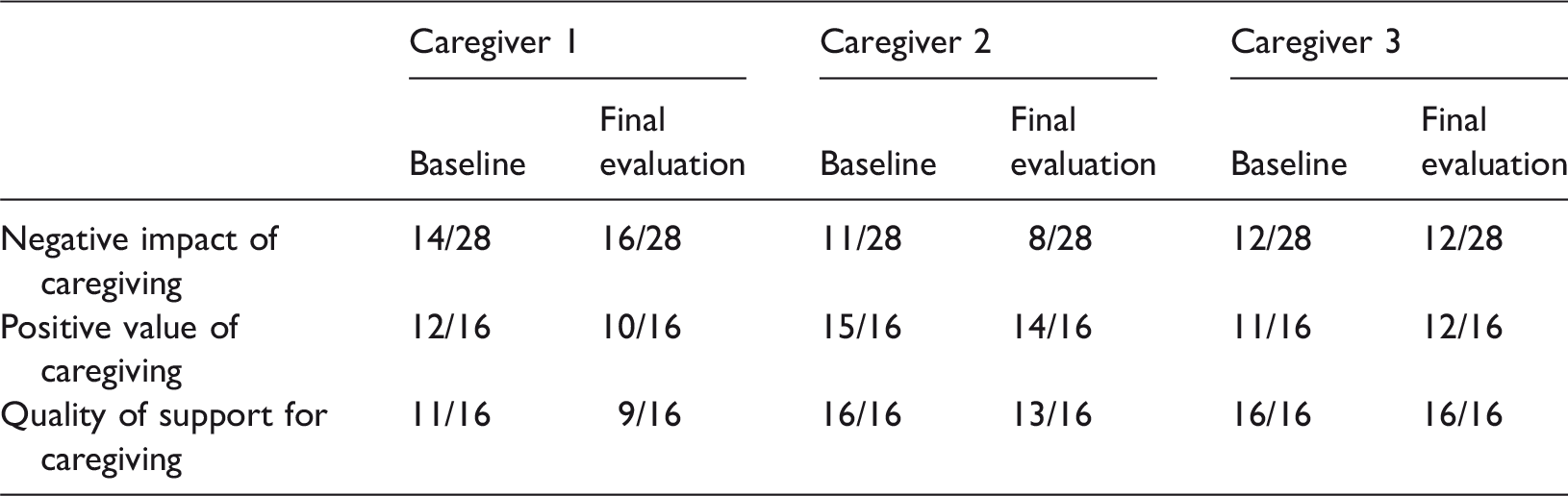
Discussion
During this study, the nursing staff and family caregivers considered many different aids and alarm systems useful in the care of a person with a memory disorder, in spite of several technical difficulties. Multiple false alarms occurred during the test period. The technological solutions deemed most useful were typically simple. Devices and systems rated with poor usability, such as complex user interface and inadequate sound quality, were also considered less useful.
The benefits of activating the life of a person with a memory disorder and easing the worry of caregivers found in this study are similar to previous research results, which have been largely based on demonstrations and interviews or focus groups rather than experimental settings (Olsson et al., 2012; Pilotto et al., 2011; Rosenberg et al., 2012; Stakes, 2008). Our findings show that AT is able to support and facilitate the work of a family caregiver and nurse in practice.
The GPS safety bracelet eased the worry of family caregivers and allowed the test subjects to continue independent walks, supporting the independency of the person with a memory disorder. At its best, AT supports the independency of person with a memory disorder and the work of a caregiver/nurse at the same time.
Life situation affects the utility of AT. Short range alarms are beneficial for a family caregiver because they facilitate the supervision of a person with a memory disorder. They were also considered beneficial by caregivers, though the needs varied between subjects. A person living alone benefits from alarms which send information remotely, such as devices connected to a safety phone service.
The weighted ball blanket, the medicine dispenser, and the Smart Flower Stand were not considered useful in the care of older persons with memory disorder. Encountered problems included complex user interface, inadequate sound quality, connection difficulties, and lack of customer service. Smart Flower Stand includes lots of possibilities to observe the rhythm of life, but its ability to detect fall/immobility could not be tested in the study. In addition, the personal setting of the system had to be programmed to suit each test subject who lived in the MemoryHelp apartment. These aspects have to be noticed in the interpretation of the results. Test period in a real home environment would be recommended for further research. Usability problems or unsuitable user interface have been previously shown to be a problem for the uptake of AT (Pietrzak et al., 2014).
Previous studies showed that there are few experimental research results from benefits of using AT in elderly homecare (Martin et al., 2008; Pietrzak et al., 2014). In this study, the COPE test was used to evaluate the impact of AT on caregivers’ experience of burden in a small group. Changes during the test period were minor. Because of the small sample size, these findings can be further confounded by other coinciding events or disease progression, or the research itself might have caused extra work for the caregiver.
The results are based on the test use of AT in the care of only nine test subjects. The test period of each test subject living in the MemoryHelp apartment was typically one week. However, the nurses used the AT for three months in total, and the home tests had a duration of one month each. This time can be considered long enough to adopt the devices into everyday use, and obtain valid feedback of usefulness.
Problems were experienced particularly with the devices that used wireless networks and browser-based service management systems. Not all of these problems could be addressed during the study, which might have impact on the results. On the other hand, such problems are part of testing in a real-world environment. The importance of well-functioning customer service in utilizing AT was noticed.
Colored images of the devices were used in the questionnaire to assess the utility of AT. However, it is possible that a caregiver or nurse may have erred in identifying the devices. Due to the simultaneous testing of multiple new systems the users might misunderstand the operating principles of the devices.
The typical proposed user who would benefit from the tested devices was a home living elderly with mild dementia. The life situation and the severity of dementia are significant factors affecting the utility of AT. Further research is needed to evaluate the utility of AT in different stages of a memory disorder and different life situations. Ideally the tested system should be easily modifiable as the disorder progresses, to include additional products and services. The evaluation requires a sufficiently long test period in order to obtain reliable research results, and to adopt the devices in everyday use. Longer test periods would also give information of long-term durability of AT in practice. In-depth interviews of all user groups, including the persons with dementia themselves, would also yield more information.
As a conclusion, ATs are able to support and facilitate the work of care staff and family caregivers if the devices have sufficient utility and usability, such as easy commissioning, maintenance, and personalization to the user’s specific usability needs. The ability of AT to support the independence of a person with a memory disorder could not be evaluated due to the type of devices that were selected in this study based on other criteria (Nauha et al., 2015).
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Academy of Finland and Japan Science and Technology Agency: ASTS (Assistive Technologies for Seniors, Teleassistance for seniors with Dementia – A Novel Concept for Safety). Academy of Finland 270816; European Union and Ministry of Internal Affairs and Communication, Japan, Research and Innovation action: iKaaS; EU 643262; Finnish Cultural Foundation; Infotech Oulu.
