Abstract
Summary
The social care assessment is a ‘key interaction’ between a person and the local authority with ‘critical’ importance for determining a person’s needs for care and support. In order to achieve this, the guidance requires that assessments must be ‘person-centred throughout’. The concept of person-centred practice is now routinely invoked, but there remains little empirical evidence on how it gets put into practice.
Findings
This paper draws on interview data from 30 practitioners about their experiences of conducting social care assessments in England. While there was widespread support for the principles of a person-centred approach, tensions emerged for practitioners in three ways: the way in which ‘chat’ was used to build a relationship or conduct the assessment, whether to conduct the assessment via a conversation or by following the sections on the agency form and the extent to which the assessor should involve and negotiate the contributions of family members.
Applications
We argue that each of these dilemmas represents an occasion when a commitment to person-centred practice is negotiated between professionals and service users and sometimes compromised as a result. We consider the possibilities for and constraints on achieving person-centred assessments in a post-Care Act environment and discuss the implications for social work practice and research.
Introduction
The concept of being ‘person-centred’ is now well established in health and social care policy in England. Having been developed in the 1980s (O’Brien & Lyle O’Brien, 1988), it was originally established as a means of collaborative life planning in the learning disability field (Sanderson, Thompson, & Kilbane, 2006). The concept was adopted more broadly as successive New Labour governments aimed to make adult social care services more ‘personal’ by increasing the possibilities for people to have choice about and control over their use of social care services (Department of Health, 2005). In doing so, the term ‘person-centred’ was used in guidance related to assessments for care and support, support planning, direct payments and individual budgets, in what was described as the ‘personalisation agenda’ (Department of Health, 2005, 2010; HM Government, 2007). Scholars have debated whether the personalisation agenda should be supported (Duffy, 2010), or resisted (Ferguson, 2012; Lymbery, 2014) and its implementation has been the focus of studies investigating the extent to which services are prepared to deliver it (Foster, Harris, Jackson, Morgan, & Glendinning, 2006) and the extent to which ‘choice and control’ are meaningful terms for the people who are intended to exercise them (Williams & Porter, 2017). Less attention has been paid to how the concept of person-centred practice is practically applied in social care assessments, even though its status has become increasingly prominent in statutory guidance, from being identified as ‘important’ (Department of Health, 2002), to the stipulation that assessments ‘should’ be person-centred (Department of Health, 2010) and the more recent requirement in the Care Act 2014 that assessments ‘must’ be person-centred ‘throughout’ (Department of Health, 2014). With this growing imperative for person-centred practice to be at the heart of social care assessments, this article aims to analyse how social care assessors in England used the language of person-centred practice in their talk about conducting assessments and the tensions they faced in applying it in practice.
Background
Disabled adults in England are entitled to an assessment of their social care needs under section 9(1) of the Care Act 2014 ‘where it appears to a local authority that an adult may have needs for care and support’. The duties and responsibilities related to social care assessments are set out in the statutory guidance to The Care Act 2014 which requires that they are conducted by an ‘appropriately trained’ person, such as a social worker or occupational therapist, but also that they ‘must be person-centred throughout’ (Department of Health, 2014).
The Care Act replaced a patchwork of social care legislation and policy over the previous 60 years and brought together attempts to develop a more ‘personalised’ approach in which people had more ‘choice and control’ over their support. There had been piecemeal attempts to introduce choice and control into pre-Care Act legislation. For example, the Community Care Act (Direct Payments) 1996 made it possible for disabled people to purchase and organise their own support and the offer of a direct payment became mandatory for all disabled adults, or any adult over the age of 65, in the Health and Social Care Act 2001. Direct payments offered a potential means of realising a ‘person-centred’ agenda, but the uptake remained relatively low during the first decade of the millennium. At the same time, policymakers were also thinking more widely about how to create a ‘total transformation’ of services, for example moving from block purchasing to individual commissioning of services, with the goal of ‘personalising’ social services and introducing personal budgets. These strategies were portrayed as potentially offering a variety of means by which the overall goal to increase choice and control at every level could be achieved. New Labour and the subsequent coalition and Conservative governments have pursued a ‘personalisation’ agenda which set out positions committing government departments to increase choice and independence for users of adult social care services (Department of Health, 2005), and that would put ‘people first’ (HM Government, 2007). These documents regularly referred to ‘personal’ and ‘person-centred’ approaches although they did not define what these meant in practice. Nevertheless, the personalisation agenda was welcomed by many disabled people who identified an opportunity to take control over their lives (Duffy, 2010), while it was critiqued by others as motivated by the individualisation of risk and the abdication of state responsibility towards its citizens (Dodd, 2013; Ferguson, 2007), leading Needham and Glasby (2014) to describe it as an ambiguous concept. The operationalisation of personal budgets from the outset has also attracted critical attention from research, with Williams, Porter and Marriott (2013) commenting on the importance of peer-led forms of support for personal budget users, and the needs for some groups of disabled adults to have higher levels of support to use a personal budget (see also Dowse, 2009; Goodwin, 2011; Houston, 2010).
Arguments about the personalisation agenda have also focused on support planning and direct payments but these tasks are based on the understanding that a person’s needs have already been established as a result of the assessment. The assessment meeting itself has received less research attention and has been less contentious as a site of debate, even though it has acquired greater force in statutory guidance. For example, in 2002, guidance stated that it was ‘important’ for assessments to be ‘rounded and person-centred’ (Department of Health, 2002), but this became stronger in 2010 with the expectation that assessments ‘should’ be person-centred, and further again in the Care Act that assessments ‘must’ be person-centred ‘throughout’ (Department of Health, 2014).
Person-centredness has therefore become a central concept in the duties of those involved in social care assessments, but the meaning of it in relation to assessments is not clearly defined. Glyn et al. (2008) argued that being person-centred is treated as self-evidently ‘a good thing’ even though it is used in different contexts and for different purposes. With the statutory requirement that assessments must be person-centred, it is important to be clear what is meant by being person-centred in that specific context.
Person-centred practice
The term ‘person-centred’ originated from the writings of the humanist psychotherapist Carl Rogers (1961) who developed person-centred counselling on the premise that, given the right environmental conditions, people have a natural tendency to grow and develop towards a state of self-actualisation (Murphy, Duggan, & Joseph, 2013). The term was applied to a model of life planning with adults with learning disabilities as they moved from long stay institutions to community-based settings (O’Brien & Lyle O’Brien, 1988). Resting on the premise that the provision of support was already established, person-centred planning focused on organising support so that the right ‘environmental conditions’ were created for individuals to identify and achieve their own goals and became an increasingly widespread model of support planning in the field during the 1990s (Dowling, Manthorpe, & Cowley, 2007; Mansell & Beadle-Brown, 2004; Sanderson et al., 2006).
There is no agreed definition of being ‘person-centred’ and Dowling et al. (2007) described it as ‘an umbrella term’ for a range of approaches founded on a common philosophy of ‘choice, independence and inclusion’ (p. 5). Mansell and Beadle-Brown (2004) identified three distinct features of person-centred planning as the focus on the person’s own expressed aspirations and capacities; the mobilisation of a person’s family and social network; and providing services to support the achievement of goals rather than limiting goals to fit available services (pp. 1–2). Essentially, these key features conceptualised person-centred practice in contrast with the systems of assessment that it challenged, those which were solely deficit and ‘needs’ based; bureaucratic and authoritarian; and service-led. Thus ‘person-centred’ signified a breaking away from existing practices felt to be oppressive and exclusionary. Taylor and Taylor (2013) also noted the absence of an agreed definition in the literature, but drew on Kilbane and Thompson’s (2004) work that differentiated it from ‘traditional’ service plans in three ways: by emphasising the power and control of the person in making the plan, in moving towards more informal modes of support and in making services responsive to a person’s requirements. The focus on the ‘plan’ and ‘support’ reiterate the emphasis placed on the support planning process and in the next section, we consider how person-centredness has been discussed in relation to assessments.
Assessments
Assessments should represent a different (and prior) activity to support planning and there might therefore be different implications in what it means to be person-centred. One example of an attempt to put people in the centre of their assessments was the provision for disabled people to conduct their own self-assessments, but has been argued to have failed because of the requirement for local authorities to apply eligibility criteria (Slasberg & Beresford, 2017). From the beginning of the personal budgets agenda, however, Glendinning et al. (2006) argued for people to identify their own ‘outcomes’ in their lives as a means of assessments becoming more ‘person-centred’ and this focus on outcomes has been incorporated into the Care Act. The relationship between focusing on outcomes and taking a person-centred approach was considered in a literature review by Miller (2010) who contrasted an outcomes-focused with a needs-led assessment style. In her conclusions, Miller argued that an outcome-focused assessment was more likely to treat the person as a citizen with rights, more likely to focus on strengths and capacities, and more likely to draw on the person’s family and social network, features associated with those elements of a person-centred approach identified by Mansell and Beadle-Brown (2004). One of the tensions that lies at the heart of person-centred assessments is the eventual decision made by the local authority as to whether the person’s needs are ‘eligible’ for funded support from a limited budget. Slasberg and Beresford (2017) have argued that the need to determine eligibility renders the potential for assessments to be truly person-centred vulnerable to the same problems that have beset policies in the past. Ultimately, they argue, the potential for the person to have control over their assessment is mitigated by the power of the local authority. This places practitioners in an invidious position of being required to conduct an assessment where the person ostensibly has choice and control over some aspects, but which is dependent ultimately on the agreement of the local authority. Murphy et al. (2013) took a similar position and argued that because statutory tasks have a specific purpose, practitioners inevitably design their interaction to pursue the completion of the task in an ‘instrumental’ way, in contrast with the ‘principled non-directive’ stance outlined in Rogerian psychotherapy. As a result, the authors concluded that the person-centred approach was logically incompatible with statutory social work.
Studies investigating the practice of social care assessments also reflect this tension. For example, Richards (2000) conducted an ethnographic study of social care assessments and found that practitioners steered the conversation towards agency priorities and away from individuals’ needs. In a later study, Foster et al. (2006), concluded that the tension made the concept of personalised assessments ‘problematic’. Practitioners have been found to use their professional discretion to resolve this tension in interview studies conducted by Chevannes (2002) and Ellis (2007, 2014), drawing on Lipsky’s (1980) concept of the street level bureaucrat. Although Ellis (2007) argued that the ‘dynamics of discretion’ could lead to ‘conservative’ practice, she has argued that the Care Act could support a more person-centred approach and recommended that more empirical studies investigate this further (Ellis, 2014). The current article aims to contribute to this research agenda by considering interview data from 30 practitioners working in adult social care in England about the assessments they conducted.
Methods and analysis
This article reports on the findings from a study conducted in the south west of England shortly after the Care Act was implemented in 2015. The aim of the study was to investigate the practices of social care assessments in three different ways: from the perspectives of people who have been assessed, of practitioners who have conducted assessments and through the collection of audio recordings of actual assessments. Throughout the study, we sought to achieve a co-produced approach in which people with lived experience of being assessed were involved in each stage of the research process. Since Oliver’s (1992) call for a new emancipatory model of research, there have been many attempts to create forms of ‘participatory’ research design, where disabled people are not just the subjects of research, but are also the researchers (Barton, 2005). Various groups of disabled people have carried out their own research, and the term ‘co-production’ has been used in connection with participatory models. Although we do not claim our study was emancipatory, it did follow a co-produced design with the academic team comprising of both disabled and non-disabled members, and worked in partnership with an organisation of disabled people that was involved in initiating and advising on the research. A ‘co-research group’ of participants with lived experience was also convened and met on a monthly basis to develop the analysis presented in this article.
The study involved collecting data about assessments in three phases, an overview of which is provided here. The first phase involved speaking with 30 disabled people, who responded to study information disseminated through the disabled people’s organisation and researcher networks, about the experience of being assessed. In the second phase, we interviewed 30 assessors in adult social care teams from local authorities different to the areas in phase one. In the third phase, six of the practitioners from phase two made audio recordings of seven assessments with the consent of the people they assessed.
This article reports on the second phase of data collection conducted through interviews with 30 practitioners and managers employed in statutory adult social care teams. Six local authorities in the south west of England were approached about the study, four of which agreed to take part. In order to minimise the possibility of disabled participants in the co-research group recognising practitioners, the local authorities were different from those in which the disabled people’s organisation operated. The local authorities had similar geographical features, each covering large rural areas with small urban centres and pockets of deprivation. After information about the study was disseminated to adult social care teams, members of the research team were invited to attend team meetings in four local authorities to introduce the study (numbers attending these meetings were not collected). For practitioners who agreed to be interviewed, semi-structured interviews were conducted at a location of their choice. Data collection began in May 2015, but was delayed in two local authorities due to structural reorganisations following the implementation of the Care Act, and interviews were completed in January 2016. The topic guide for the interviews with practitioners was developed by the university team and covered topics about the practitioner, their accounts of how they conducted assessments and their views as to what constitutes effective practice.
The interviews lasted approximately an hour and followed a semi-structured format that allowed flexibility to explore areas in more detail if they appeared particularly relevant to the practitioner (Brinkmann & Kvale, 2015). The interviews were transcribed verbatim before being transferred to NVivo 10 to assist with analysis. Analysis of the transcripts was informed by the principles of grounded theory (Charmaz, 2014) that followed a process of open and then subsequent, more focused coding of the transcripts before developing categories. Four members of the research team were involved in drafting the analysis with three members conducting and checking each other’s coding for agreement. Three meetings were held to discuss and resolve instances where there was disagreement on coding and categorisation. In addition, the team held monthly meetings with the co-research group of participants to review sections of interview transcripts and discuss the emerging analysis. This iterative process of ‘collaborative sense-making’ is argued by Nicholls (2009) to be an important reflexive element of participatory research and one that has been promoted by Nind (2011) in research with children and adults with learning disabilities.
The study received funding from the School for Social Care Research and received ethical approval from the Social Care Research Ethics Committee. The remainder of this article will report on the interviews with practitioners and presents extracts related to the theme of person-centred practice and the tensions that emerged in achieving it.
Findings
The findings presented here focus on a single theme in the data: that of a tension in the practitioners’ talk between pursuing a person-centred assessment and settling for a more instrumental approach that achieves the statutory task. This tension is reflected in how practitioners understand the concept of being person-centred and is also evident in three examples of practice that practitioners oriented to in their talk: using ‘chat’ in the assessment, using the form, and involving family members. The characteristics of the 30 practitioners are presented in Tables 1 and 2.
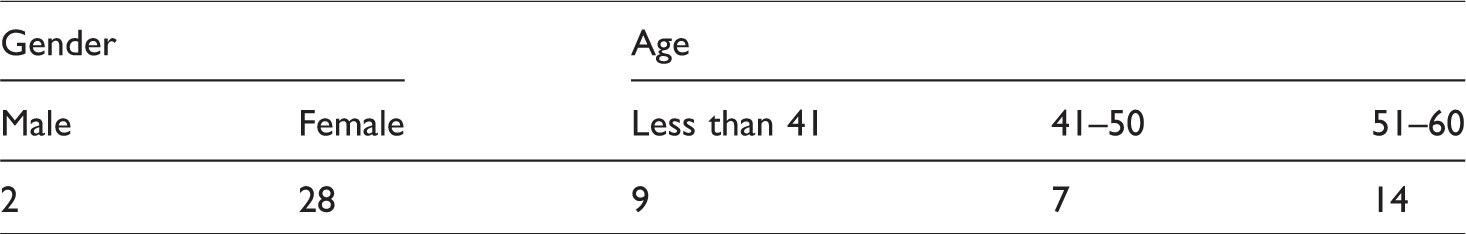
Characteristics of practitioners.
Characteristics of practitioner roles.
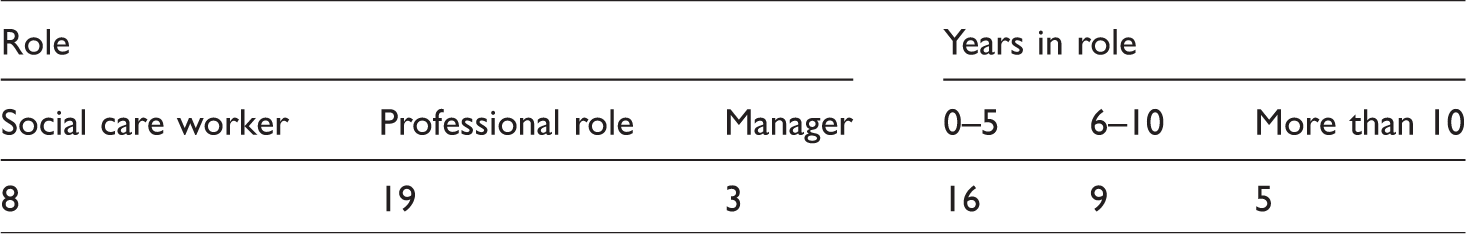
Twenty-eight practitioners, including all three managers, were female. Twenty-two had professional qualifications (21 social workers, and one occupational therapist). Eight participants were in roles that did not require a professional qualification (we have described this as social care worker), supporting the assertion that the assessment task is becoming de-professionalised (see Lymbery, 2014). It was also of note that more than half the practitioners had been in their role for less than five years, perhaps reflecting the turbulence in the social care workforce in recent times.
In the following paragraphs, we introduce tensions in practitioners’ talk of ‘being person-centred’, before considering in more detail the occasions where practitioners faced tensions in practice.
Tensions in being person-centred
Practitioners were not asked directly about person-centred practice in the interview, but the importance of the concept appeared frequently in responses. For example, when asked what made a good assessment this practitioner responded: ‘An assessment that looks like you’ve talked to people, that you’ve really understood that person. Spending time on that support plan so it really is person-centred’ (Practitioner 30, manager, local authority 4). This manager’s response was typical in our data where an equivalence was drawn between person-centredness and a successful assessment. Practitioners viewed the introduction of the Care Act 2014 as supporting these principles with one practitioner describing the possibilities it afforded for recognising the expertise of the individual: ‘I’m quite positive about the Care Act. It’s so much person-centred and outcome-based, and very much from the service user’s point of view, you know, assuming that they’re the expert in their condition’ (Practitioner 12, social worker, local authority 3). Being person-centred was something that was valued by practitioners and this practitioner was pleased that the Care Act would facilitate this model of practice. By treating the service user as the expert in their life, this practitioner is also aligning with the Rogerian principles of self-determination that were discussed earlier. Despite the broad agreement that being person-centred was self-evidently ‘a good thing’ (Glyn et al., 2008), when we asked practitioners how they approached assessments, elements of the institutional process became evident. One practitioner described the contrast between using the assessment to focus on the person, while determining whether the person would be eligible for funded support. An assessment is like a way to get to know somebody, and it is, it's a really good way of getting information. But I suppose really the outcome of it is to work out whether they're eligible for social care services. (Practitioner 14, social worker, local authority 1)
Using ‘chat’ in the assessment
The first tension was in how practitioners used ‘chat’ in the assessment, both to build a relationship, and to conduct the institutional task of the assessment. An example of the former is shown in this extract: ‘So I did quite a few visits for the assessment, so just going and chatting to him, talking about his daily routine’ (Practitioner 26, social worker, local authority 4). Spending time to get to know a person is supported by researchers of person-centred practice (Beresford et al., 2011) and was used by this practitioner as a means of getting to understand the person’s life. In other interviews, ‘chat’ was used by practitioners in ways that were more instrumentally related to the assessment task. For example, the following practitioner explained the part that ‘chatting’ played in the assessment process. ‘And just to build that rapport and get the most out of them you can, and then try and get the service in. So by chatting to them and getting that picture’ (Practitioner 27, social care worker, local authority 4). The chatting in this extract represents a more instrumental approach than simply getting to know a person and was used with the distinct purpose of getting information that could justify the provision of a service. A third practitioner spoke of how she would chat with the person in the kitchen, using it as an opportunity to gather information that would be relevant to the assessment: And it doesn’t hurt to say yes if they ask if you want a cup of tea, you know? I think, Why not? They’re offering a cup of tea. Also, it helps you make an assessment, are they able to use the kitchen safely? (Practitioner 6, social care worker, local authority 2)
Using the form
Tensions also appeared in practitioners’ accounts of achieving person-centred practice related to the extent to which they used the form. One social worker described how she conducted the assessment meeting in deliberate contrast to following a form: ‘Just try and talk about their backgrounds and their lives, and try and make it not like a form that you follow’ (Practitioner 14, social worker, local authority 1). This social worker drew a contrast between two approaches to conducting the meeting, either following a form or talking about a person’s life. The contrast between the two approaches suggests that for this practitioner, the two are not compatible and her ability to pursue a flexible approach is constrained by a form which she would need to ‘follow’. Another social worker who worked in sensory impairment team described the process by which he achieved this in practice: [I] often start with a very sort of open question, like, ‘Can you tell me about the impact of your vision on you?’ And then some people might then just blurge out about sort of everything. And then what I normally do is I normally scribble down the odd notes; they might talk about the emotional impact, they might talk about the fact that they can no longer get to the shops, they might talk about whatever. So I normally just scribble down the odd word, and then sort of use what they then said to form the agenda, almost, so: You’ve told me a bit about not being able to get to the shops. Can you tell me more about that? (Practitioner 1, social worker, local authority 1)
The influence of the institutional framework was more explicit in accounts of other practitioners, who were more inclined to follow the questions on the form, as described by this social worker: I go question by question. And I explain to them that it is a fairly lengthy document. Apologies, but if we just go question by question, then hopefully it will be done and dusted. But I do, I am absolutely question by question. (Practitioner 20, social worker, local authority 3)
In one of the participating authorities, a project was in process where managers had given explicit support to practitioners to visit people without considering the form, but simply to get to know a person and understand what was happening in their lives. Although this was daunting for some practitioners, one manager explained that it was about ‘giving people permission’ (practitioner 30) to step outside the constraints of the form in the belief that when they saw it going well, they would ‘never take [the form] out again’ (practitioner 30). One of the social workers involved in this pilot described a successful piece of work that started with her learning about a man’s career and his life without any reference to the form. In her view, this constituted ‘proper social work’ (practitioner 28) before going on to explain: What made that social work was that I interacted with him on a very human level, I didn’t objectify him, I didn’t make it about services and about funding, even though I had to do that in order to oil it along. But he felt valued by me, and recognised, and trusted, me. (Practitioner 28, social worker, local authority 4)
Involving family members
There is a statutory requirement to involve carers in the assessment process under section 9(5)(b) of the Care Act, but knowing when and how to best achieve this while maintaining the focus on the assessed person represented a third tension for practitioners. In most cases, family members were viewed as a supportive influence in the assessment process: ‘Sometimes it’s definitely best for them to have their carer or other family members around them, and they can be incredibly supportive, and can help them to open up and say how things are’ (Practitioner 1, social worker, local authority 1). Activating the social networks of a person, including their family and informal support, is a key element of person-centred practice (Mansell & Beadle-Brown, 2004). In our interviews, practitioners, such as the social worker above, described family members as helpful in explaining ‘how things are’, enabling people to ‘open up’ and ensuring their needs were met. There were also times when practitioners maintained their awareness of family member reactions to verify (or dispute) what the person was saying about their circumstances. In the following extract, the practitioner noted her use of peripheral vision to ‘clock’ reactions of family members during assessments. So when I’m asking questions to the service-user, the client, I’m still clocking the occasional – well, I ask the question, and then if their spouse is sitting there, [the person will] go, ‘Oh, no, no, I can do that fine’, and then you look at the spouse, and they’re kind of doing a look. They don’t say anything, but quite often they do a look, and you think, OK, well that’s not maybe quite right. (Practitioner 13, occupational therapist, local authority 3) So [I] called her step-son, who has power of attorney, and I said, do you mind if she has extra carers put in, just to kind of monitor, just to have a bit of help, and he refused to pay for it. (Practitioner 17, social worker, local authority 3)
The practitioners in our study showed commitment to the principles of a person-centred approach in their assessments, but were tasked with determining eligibility as well as focusing on the person, producing tensions in their accounts of practice. The emphasis on the instrumental task of the assessment led some practitioners to rely on the form in the meeting with the intention that it would ensure a complete and accurate assessment, even though they acknowledged that this was not ideal. Family members’ contributions were valued, but added another factor that practitioners had to resolve. These tensions are not new, but in a new legislative environment, where a person-centred approach has become a statutory duty, it is important to revisit and reanalyse how these tensions place constraints on the capacity to achieve this in practice.
Discussion
This article contributes to a growing debate about the ways in which statutory social work sets obstacles for a person-centred approach to social work (Murphy et al., 2013; Slasberg & Beresford, 2017). When practitioners spoke to us about their assessment practices, person-centred practice was self-evidently ‘a good thing’ (Glyn et al., 2008), aligned with a conceptualisation of it that emphasised the control of the individual over the plan, made the plan responsive to the person’s needs, and involved the person’s family and informal support networks (Kilbane & Thompson, 2004; Mansell & Beadle-Brown, 2004). Person-centred practice appeared most achievable when the practitioner spent time getting to know the person; when they did this without reference to the assessment form; and when they involved family members in the person’s plan, but in an ancillary way. In contrast, when person-centred practice was likely to be compromised, this was characterised in practitioners’ accounts when they used ‘chat’ in an instrumental way for assessment purposes; when they used the assessment form to conduct the meeting; and when they involved family members as more authoritative sources of information than the person.
These tensions might be understood as reflecting variations in practice that should be addressed by training and supervision, but as Slasberg and Beresford (2017) have argued, there are deeper tensions in pursuing an outcomes-based, person-centred approach within a statutory context based on determinations of eligibility. Equitable decisions require accurate assessments, but our data suggest that this may become manifest in face-to-face encounters when practitioners go through the form ‘question by question’ (as practitioner 20 put it), or treat family members as more authoritative about a person’s needs. It is through this dynamic that obstacles are introduced to the possibility of achieving a person-centred approach ‘throughout’ the assessment that is required by current statutory guidance.
The tensions described in this article introduce a dilemma as to whether it is possible to pursue person-centred practice in the statutory environment that is currently configured. We are not arguing for a retreat from the commitment to person-centred practice in the Care Act. The concept has done much to advance the possibilities of people in need of support and reflects a rights-based approach to citizenship that generations of disabled activists have struggled to achieve. Instead, we argue for the exploration of possibilities to extend person-centred practice further in adult social care with implications for practitioners and policymakers.
The implications for practitioners extend the direction already taken in the guidance for the Care Act. The practitioner should have knowledge and expertise that might be used by people needing support, but our results suggest that these should be used in a process which is led by the person, rather than as the basis for organising the assessment meeting. For example, one possibility could be an exploration of the person (or their chosen representative) setting the agenda for, and chairing, the assessment meeting.
An implication for policymakers would be to revise existing guidance for practitioners to reflect a more nuanced understanding of the person-centred approach in practice, including the tensions we have described and the possibilities to address them, even within a statutory framework. As the Care Act is embedded in local authorities, further research should evaluate the design and use of different forms and focus on the extent to which it is achieving its aims of enabling person-centred practice. This will not be possible without a better understanding of how assessments get conducted in practice. As researchers such as Richards (2000) have long argued, further research that collects data from face-to-face encounters is necessary in order to understand the ways that legislation and policy support or inhibit the facilitation of person-centred practice in adult social care.
Limitations
The sample of practitioners in this study was self-selecting and from one region of England so their views may not reflect those of the wider social care workforce. Based on ethical considerations, we took the decision not to interview people who had been assessed by practitioners, and this limits the extent to which the data should be considered to reflect actual practice. The study also relates to the statutory environment in England which may have different implications for statutory environments in other countries.
Conclusion
Person-centred practice is a statutory requirement of practitioners conducting assessments in adult social care in England, but the extent to which this is possible within existing frameworks is not yet established. In this article, we have described three ways in which practitioners encountered tensions in combining a person-centred approach with completing a statutory assessment. We conclude that these tensions reflect the constraints inherent in the assessment task, and which need to be resolved to enable practitioners to fulfil their duty to be ‘person-centred throughout’.
Footnotes
Ethics
Ethical approval was granted by the Social Care Research Ethics Committee (reference SCREC 14/IEC08/1022).
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was funded by the NIHR School for Social Care Research reference C088/CM/UBDA-P60. The views expressed are those of the authors and not necessarily those of the NHS, the NIHR or the Department of Health and Social Care.
