Abstract
The aetiology of impacted canines is multi-factorial. Several theories have been proposed, such as lack of space, genetic predisposition, physical barriers like supernumerary teeth, odontomas and other conditions that interfere with the eruption pathway. One of the main complications that can be generated by impacted canines is the resorption of the root of the adjacent teeth. This case report examines the importance of interdisciplinary management of maxillary incisors with root resorption caused by impacted canines in a 13-year-old male patient. Careful traction of impacted canines and proper tissue management followed by space closure and retroclination of anterior incisors with orthodontic treatment. Finally, functional and aesthetic results using dental veneers for oral rehabilitation allowed the patient to obtain favourable results.
Introduction
Dental impaction is defined as the failure of a tooth to erupt in the proper position within the physiological eruption time (Bjerklin and Guitirokh, 2011; Lai et al., 2013). After the third molars, canines are the most frequently impacted teeth, with a frequency of 1%–3% (Bjerklin and Guitirokh, 2011; Kalavritinos et al., 2020; Lai et al., 2013; Oberoi and Knueppel, 2012; Ucar et al., 2017). The location of the canines in the maxilla provides important functional and aesthetic characteristics (Oberoi and Knueppel, 2012).
The impacted canine aetiology is multifactorial. Several theories have been proposed, such as lack of space, genetic predisposition especially in canines impacted in the palate (Alemam et al., 2020; Bjerklin and Guitirokh, 2011; Falahat et al., 2008; Ucar et al., 2017) and physical barriers, such as supernumerary teeth, odontomas and other conditions that interfere with the eruption pathway (Kalavritinos et al., 2020). One of the main complications that can be generated by impacted canines, is the resorption of the root of the adjacent teeth (Alemam et al., 2020; Becker et al., 2010; Cernochova et al., 2011; Falahat et al., 2008; Kalavritinos et al., 2020). The exact aetiology of root resorption is unknown; the possible causal factors are the pressure and inclination of the erupting canine, follicular activity, genetics, trauma, insufficient root development and their susceptibility to resorption enzymes (Cernochova et al., 2011). Resorption occurs more frequently in women (Alemam et al., 2020; Bjerklin and Guitirokh, 2011; Lai et al., 2013; Oberoi and Knueppel, 2012; Ucar et al., 2017).
Ericson and Kurol (1988) classify root resorption into four categories: (1) no resorption, root surfaces intact but with possible loss of cementum; (2) slight resorption, up to half the thickness of the dentine; (3) moderate resorption, more than half the thickness of the dentine, the pulpal lining is not broken and is covered by dentine; and (4) severe resorption, the pulp is exposed by resorption.
When root resorption occurs, the patient may require expensive and prolonged treatment, and even lose the associated teeth (Becker et al., 2010; Falahat et al., 2008; Kalavritinos et al., 2020). It has been considered that once the impacted canine has been treated, there is no risk of further resorption (Alemam et al., 2020; Becker et al., 2010; Bjerklin and Guitirokh, 2011; Lai et al., 2013). Factors such as the severity and the site of resorption in the root of the incisor determine the election of the therapy (Alemam et al., 2020; Bjerklin and Guitirokh, 2011). Changing the shape and colour of a canine to resemble a lateral incisor is possible by reshaping the tooth with proper polishing and restoration (Harrison and Bowden, 1992).
The aim of this case report was to describe an interdisciplinary management of a 13-year-old male patient with ectopically positioned and impacted maxillary canines that had caused severe root resorption of the maxillary right lateral and left central incisors. Treatment successfully aligned the canines and the upper and lower arches as well as giving good aesthetics and function.
History
Extra-oral and intra-oral assessment
A 13-year-old male patient presented to the private orthodontic practice to start treatment. A physical examination revealed facial symmetry with a convex profile. Intra-orally, he presented with bilateral absence of the maxillary canines, bilateral molar Class I, adequate overjet and overbite, non-coincident interdental midlines and grade II mobility of the maxillary right lateral and left central incisors (Figure 1).
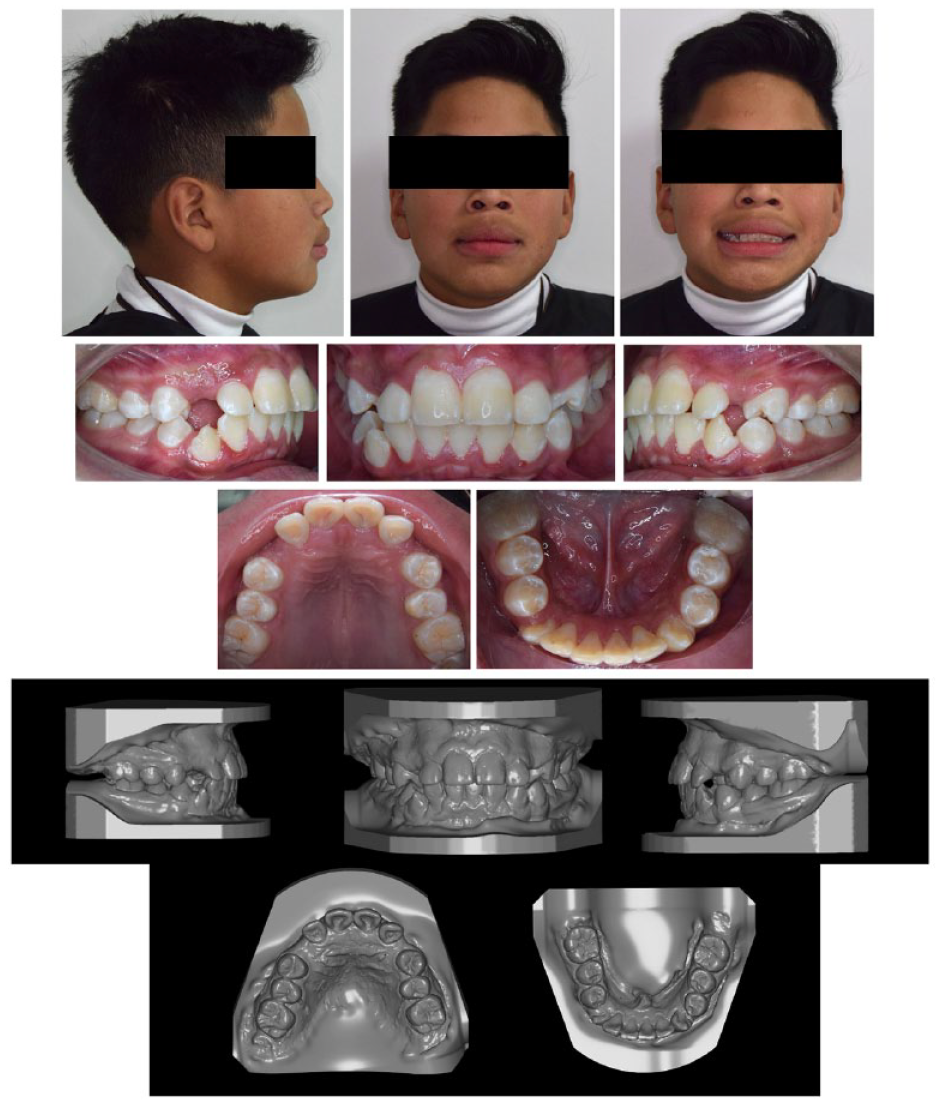
Pre-treatment facial, intra-oral photographs and casts.
Radiographic assessment
The orthopantomography (OPG) showed the impaction of the maxillary canines with ectopic position and root resorption of the four maxillary incisors. A cone-beam computed tomography (CBCT) scan was requested. Severe root resorption of the left central and right lateral incisors was observed, as well as a slight resorption of the maxillary right central and left lateral incisors (Figure 2).
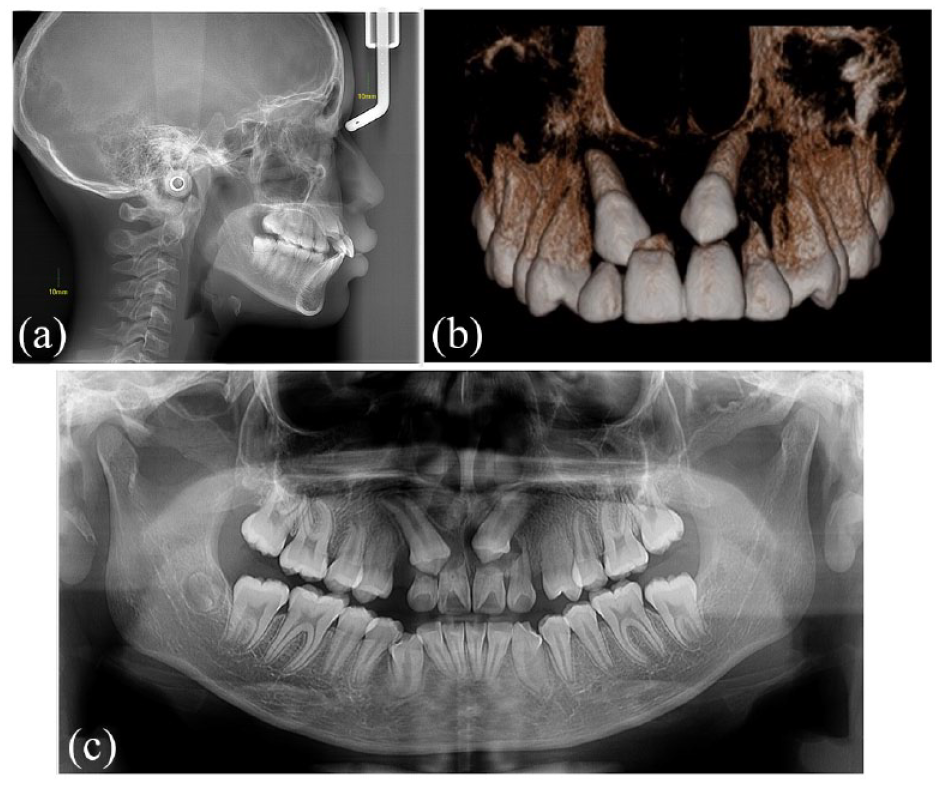
(a) Initial cephalometric, (b) pre-treatment three-dimensional image and (c) initial OPG.
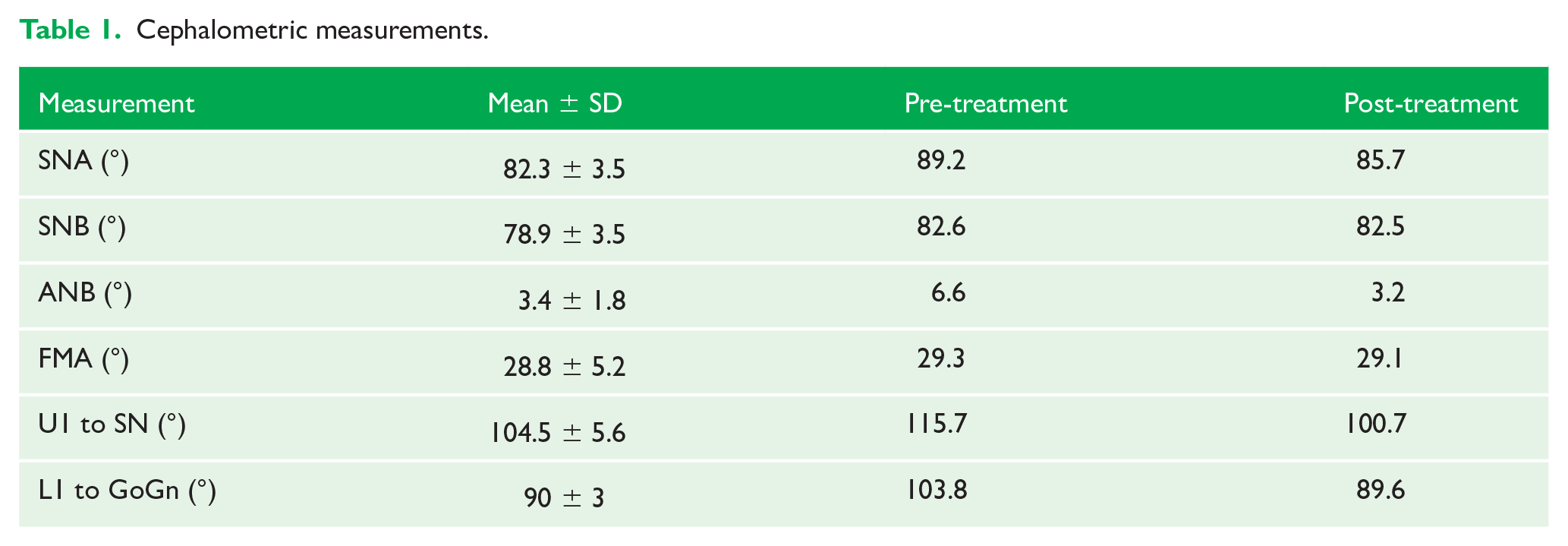
In the cephalometric analysis, a protrusive position of the maxilla was determined (point A), probably due to the eminence of the crown that surrounded the impacted canines, the mandible was in an adequate position and a proclination of the upper and lower incisors was observed (SNA = 89.2°, SNB = 82.5°, U1 to SN = 115.7°, L1 to GoGn = 103.8°) (Figure 2 and Table 1).
Cephalometric measurements.
Aims of treatment
The treatment objectives were as follows: (1) to coordinate the arches; (2) to align the maxillary canines; (3) to achieve an adequate facial profile; (4) to generate adequate occlusion; and (5) to restore dental aesthetics to the patient.
Treatment progress
Treatment began with extractions of the maxillary right lateral and left central incisors, and the mandibular first premolars. MBT appliances (0.022 × 0.028-in slot; 3M, USA) were used on the premolars, maxillary molars and in the complete mandibular arch. On the maxillary incisors, edgewise (0°) brackets were used in order to control the torque as necessary. The wire sequence used was as follows: 0.014-inch nickel titanium (NiTi); 0.016-inch NiTi; 0.016 × 0.022-inch NiTi; 0.019 × 0.025-inch NiTi; and 0.019 × 0.025-inch stainless-steel (SS) wires, in the upper and lower arches.
Four months after the extractions, no clinical signs of eruption of the canines were observed. The surgical exposure of the maxillary canines was performed under local anaesthesia using an apical repositioning flap of the two impacted canines with the aim of preserving the keratinised gingiva. Buttons were placed on the vestibular surface for traction through a metal ligature (0.012-inch SS) fixed directly to the maxillary arch (0.014-inch NiTi) with activations every 3 weeks.
Once the crowns of the maxillary canines were exposed, edgewise (0°) brackets were placed, and the alignment and levelling phases continued. The space closure phase was performed with 0.019 × 0.025-inch SS wires and active lace back ligatures.
Before bracket removal, a lateral cephalogram radiograph was taken to determine the torque of the anterior teeth. It demonstrated an acceptable position of the canines, so it was not necessary to make additional bends to improve root torque (Figure 3).
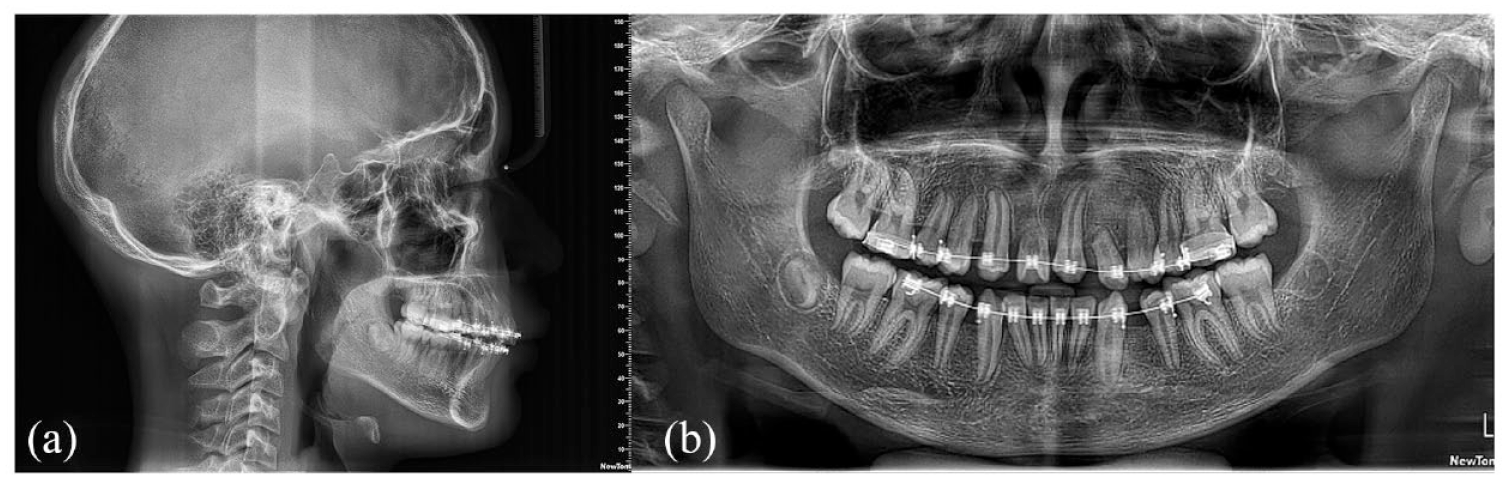
(a) Mid-treatment cephalometric and (b) mid-treatment OPG.
Twenty months later, the fixed appliances were removed, and a removable upper and fixed lower retainer were placed (Figure 4). The cephalometric analysis showed a more retruded position of point A, an adequate maxillomandibular relationship and an acceptable inclination of the upper and lower incisors (SNA = 85.7°, SNB = 82.8°, ANB = 3.3°, U1 to SN = 100.7°, L1 to GoGn = 89.6°) (Figures 5 and 6, Table 1).
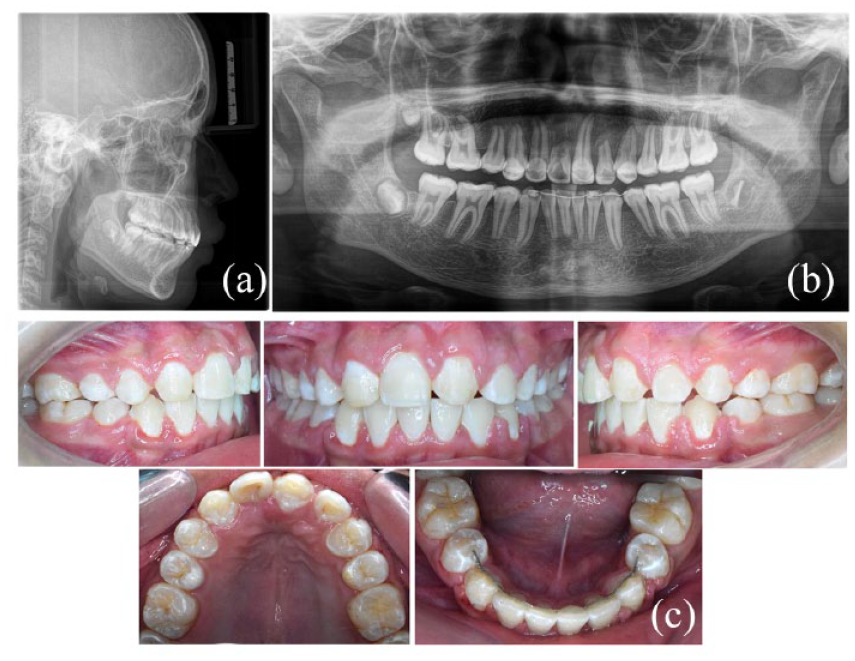
(a, b) Post-treatment radiographs and (c) post-treatment intra-oral photographs.
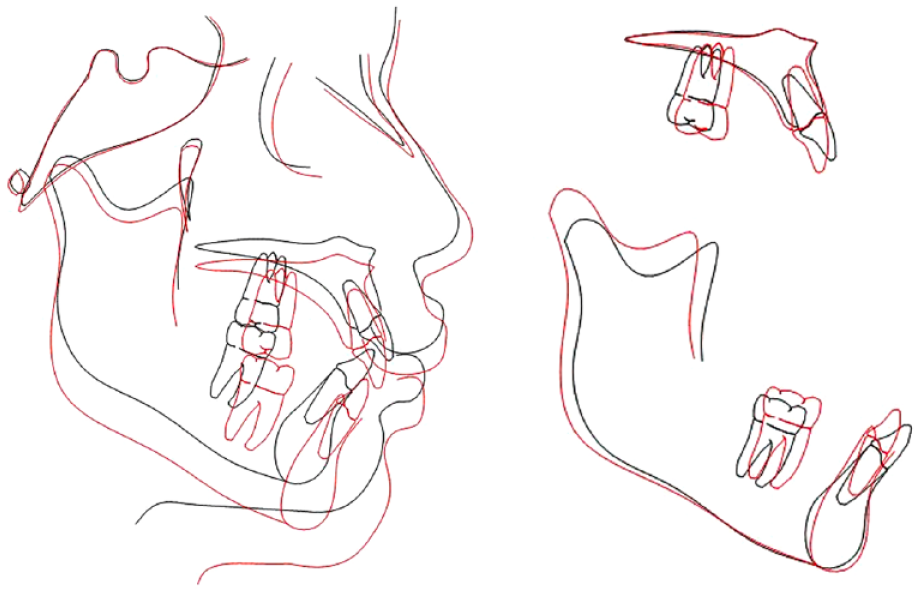
Lateral cephalometric superimposition. Black, pre-treatment; red, post-treatment.
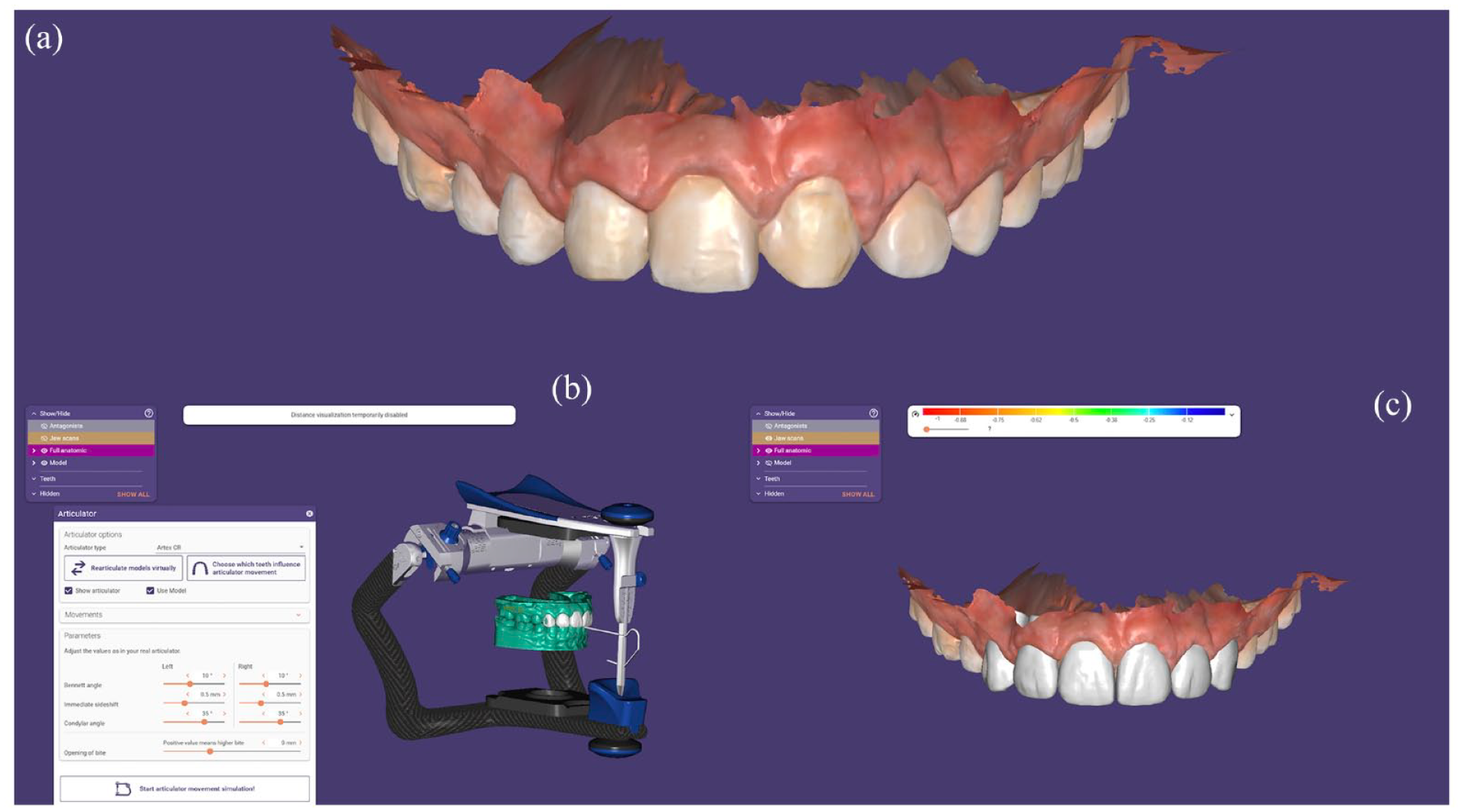
(a) Initial scan, (b) digital wax-up in a digital articulator to determine function, and (c) digital wax-up.
Two weeks later, a gingivoplasty was performed with the aim of levelling the zeniths and improving the gingival thickness before the anterior aesthetic restoration. An intra-oral scan (Medit i500; Medit Corp, South Korea) of the maxillary and mandibular arches was performed with an interocclusal record in maximum intercuspation (MI) and digital models were obtained in standard triangulation language (STL) files. Subsequently, these STL files were imported into design software (Exocad; Exocad GmbH, Germany) to perform a diagnostic wax-up of the six maxillary anterior teeth with the models mounted in a virtual articulator. A condensation silicone guide was made for the manufacture of the mock-up in order to establish functional parameters, position, shape, colour of the restorative material, lip profile, phonetics, position of the incisal edge and gingival orientation (Figure 7).
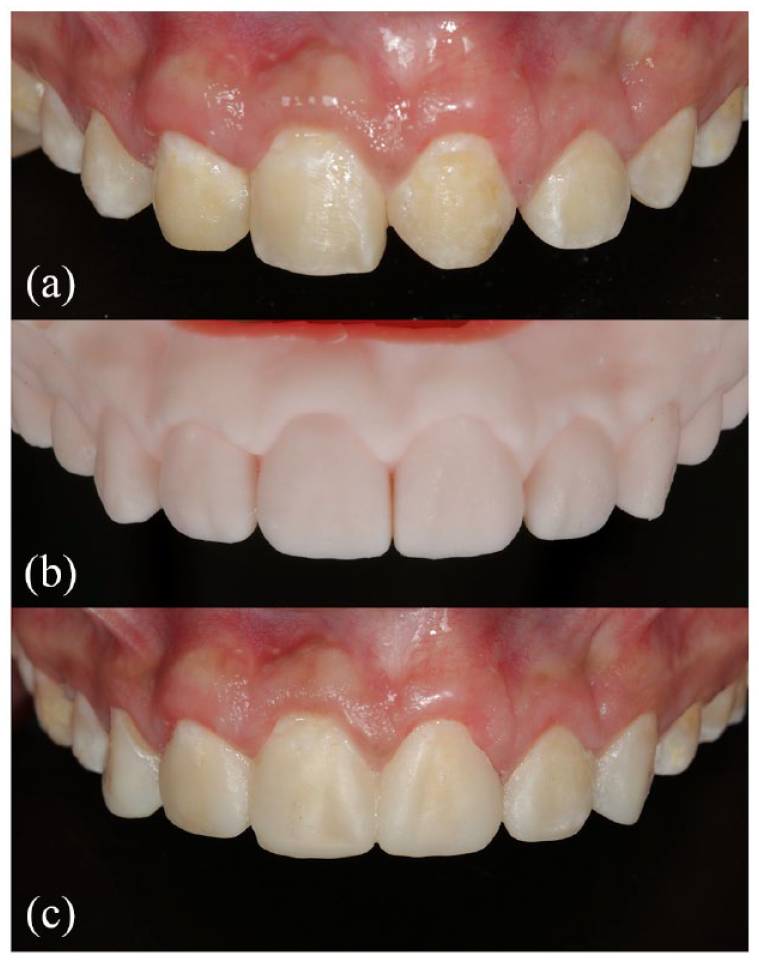
(a) Postorthodontic photograph, (b) three-dimensional waxed impression, and (c) mock-up.
Once the mock-up was approved, transparent polyvinyl siloxane (PVS) was injected into the individual tray. The PVS was then drilled at the level of the central incisors to provide access to the flowable resin. Guilda nanohybrid resin (Tetric N-Flow; Ivoclar Vivadent) in shade A1 was injected and light-cured for 20s. A layer of glycerine was placed on the resin and light cured for 20s in order to remove the oxygen inhibited layer. Excess material was carefully removed and finished strips for the interproximal area.
Treatment results
Proper coordination of the maxillary and mandibular dental arches was obtained, as well as dental alignment, a pleasing facial profile, periodontal health, and stable aesthetics and function. An adequate overjet and overbite were obtained, maintaining bilateral molar Class I and having replaced the maxillary canines with the maxillary first premolars. Adequate facial proportions were obtained at the end of treatment and the upper and lower lips were slightly retracted. The facial photographs showed a harmonic and pleasant smile. Radiographically, root parallelism was acceptable and adequate occlusion was achieved. The prognosis for the right central incisor remained uncertain (Figure 8).
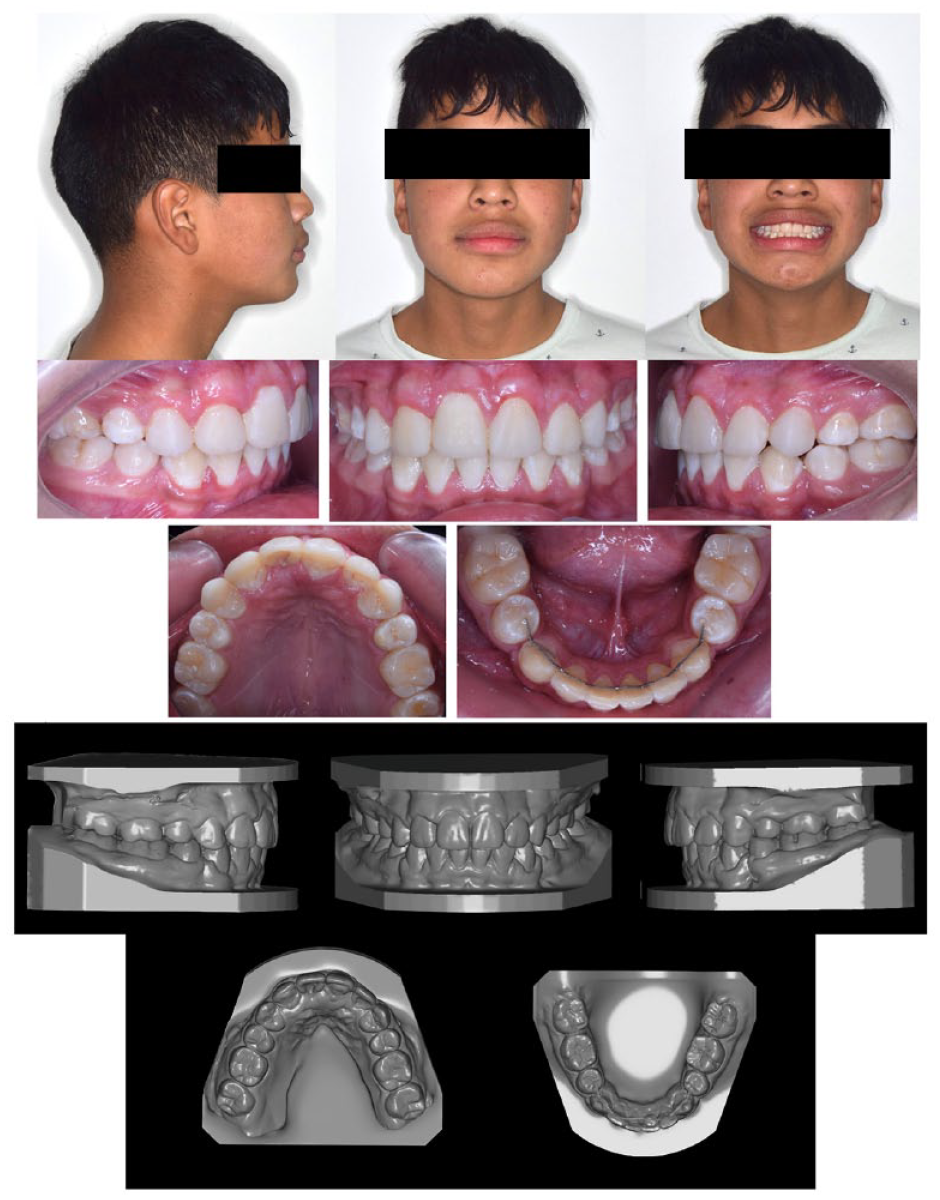
Post-treatment facial and intra-oral photographs and casts.
Discussion
Root resorption of maxillary incisors associated with impacted teeth, is a challenge. The choice of treatment will depend on the degree of involvement, periodontal health and position of the included teeth. In this case report, we describe the treatment of impacted maxillary canines that caused root resorption of the four maxillary incisors.
Root resorption caused by impacted canines has been described as a rapid and progressive process that almost always stops when the impacted canine has been removed from the affected root area (Becker et al., 2010; Bjerklin and Guitirokh, 2011; Falahat et al., 2008; Lai et al., 2013). There is not enough evidence about this type of long-term root resorption to determine if these lesions progress, are limited or repaired (Becker et al., 2010). It has been shown that on occasions where the pulp has been affected, the incisors have not shown clinical symptoms and have shown good healing (Bjerklin and Guitirokh, 2011). During treatment planning, it is important to assess the status of the roots of affected teeth to determine whether they are to be extracted or preserved (Becker and Guitirokh, 2010; Bjerklin and Guitirokh, 2011; Falahat et al., 2008; Lai et al., 2013). In this case, it was decided to extract the maxillary left central incisor and right lateral due to the degree of root resorption and mobility with which they presented.
When it is decided to extract the incisors, the ideal orthodontic treatment remains controversial. The discussion is centred between opening the space for the prosthetic replacement of missing teeth or closing the spaces with orthodontics, followed by an anatomical recontouring of the canines (Silveira et al., 2016; Zachrisson, 2008). Factors such as age, type of sagittal malocclusion, presence or absence of dental crowding and type of facial profile are determining factors when choosing the appropriate treatment plan (Silveira et al., 2016; Zachrisson, 2008). Other factors include size, shape and gingival margin of the maxillary canines (Zachrisson, 2008).
When choosing to replace canines through orthodontic space closure, the challenge is to achieve acceptable aesthetic factors due to differences in size, shape and shade between the maxillary canine and lateral incisors (Harrison and Bowden, 1992). However, among the advantages of this choice is avoiding long-term use of the prosthetic replacement with a denture, bridge or implant (Brough et al., 2010; Silveira et al., 2016).
The aesthetic result with space closure is more natural and the orthodontist can perform a correct ameloplasty on the canine and adequately control the torque of the lingual root (Silveira et al., 2016). Various mechanics can be used to mask the differences between canines and lateral incisors, such as inverting the bracket of the canine to increase torque, which could reduce the canine eminence (Brough et al., 2010), another alternative is to place the bracket of the canine towards the gingiva to extrude the canine and lower its gingival zenith and remodel the shape of the canine (Tuverson, 1970). In this case report, edgewise 0° brackets were used in the maxillary canines in order not to use an established prescription for the upper incisors, due to the difference in the buccopalatal width of the roots. 0° brackets were used to make compensation bends in the arch during descent and positioning of the canines, which was not necessary in this case.
With interdisciplinary management in these cases, where the adequate closure of spaces is achieved with orthodontics and aesthetic dental techniques, results are obtained that can be almost indistinguishable from natural dentition (Zachrisson, 2008).
In the present case, the decision to close the space was based on a series of factors, such as the skeletal pattern I, with maxillary and mandibular incisal proclination; therefore, opening spaces to place implants could worsen their profile. After the extraction of the maxillary incisors, we considered it appropriate to wait 4 months for a passive eruption of the canines, since there was no physical barrier to contemplate a longer time. Not observing any clinical signs of eruption, it was decided to perform surgical exposure of the maxillary canines and their subsequent traction. During space closure, the gingival tissue and interdental papillae would change simultaneously with the displaced natural teeth. An integral part of the treatment plan was a restorative camouflage consisting of injected resin veneers from the upper right first premolar to the left first premolar.
Regarding the canine relationship, a protected canine occlusion may not be considered completely stable since over the years it tends to be replaced by a group function due to the inevitable and common wear of the maxillary canines (Brough et al., 2010; Silveira et al., 2016). Furthermore, the aetiology of temporomandibular disorders is multifactorial, with aesthetic and functional occlusions playing a secondary role (Silveira et al., 2016).
Studies have concluded that patients with space closure and replacement of canines by premolars did not impair the function of the temporomandibular joint and favoured periodontal health compared to prosthetic replacement (Brough et al., 2010; Zachrisson, 2008). The roots of the first premolars are usually thinner and smaller than the canines, so there would be periodontal concern. However, this damage has not been demonstrated and some studies are in favour of the space closure option (Al-Anezi, 2011; Brough et al., 2010; Qadri et al., 2016; Silveira et al., 2016; Zachrisson, 2008).
When replacing with implants, certain long-term aesthetic drawbacks have arisen, such as gingival recession, darkening of the overlying gum, incomplete filling of the interdental space by the papilla, infraocclusion of the implant and, in terms of functionality, even bone loss around the implants has been reported, varying between individuals (Mota and Pinho, 2016; Silveira et al., 2016).
The factors that lead to the retention of bacterial plaque, such as pontics, hooks in removable prostheses, excessive contours and poor adaptations to teeth that adjoin conventional fixed prostheses, have been identified as the main characteristics responsible for periodontal problems (Nordquist and McNeill, 1975; Robertsson and Mohlin, 2000; Silveira et al., 2016).
Andrade et al. (2013) found no scientific evidence to support any treatment option for maxillary lateral incisor agenesis because they did not identify any randomised clinical trials. Pithon et al. (2021) compared cases of orthodontic space closure versus cases with no treatment to determine the social impact and quality of life. The results were in favour of the cases treated with orthodontics, improving quality of life and self-esteem in the patients.
Digital technologies applied in dentistry have made it possible to have a variety of tools to handle different clinical scenarios. The CAD phase allows simulating the result without altering the teeth intra-orally. Each step in this process is reversible and modifiable, making it versatile and recoverable (Coachman et al., 2020; Hirata, 2021).
Placing direct resin restorations can be a tedious, time-consuming process, requiring meticulous care and attention. They are not made from a pre-established dental shape, making this procedure operator-dependent and unpredictable (Coachman et al., 2020). When anterior restorations are required, indirect restorations are the clinician’s choice. However, their manufacture is generally carried out by a dental technician, which means an increase in treatment times and costs.
The injected resin technique is an indirect/direct process that predictably translates an analogue or digital diagnostic wax-up to high-load fluid resin restorations (Sillas, 2018). This non-invasive technique allows aesthetic and functional problems to be resolved before performing any ceramic treatment and can be used for months, or even years, by patients (Terry, 2012). The use of this technique, in combination with prosthodontic and orthodontic options, offers a different approach to restoring teeth in young patients at a lower cost than an indirect restoration (Hirata, 2021; Sillas, 2018). The clinical applications of this type of technique are numerous: repair of fractured teeth and restorations; fabrication of provisionals; paediatric cases; occlusal wear in posterior restorations; and establishing the length of the incisal edge before ceramic restorations (Sillas, 2018; Terry and Powders, 2019). However, the main disadvantages are their reduced physical properties and higher shrinkage, due to polymerisation compared to conventional resins (Coachman et al., 2020).
Considering the age and economic situation of the patient, it was decided to make the aesthetic restorations using the injected resin technique provisionally. The patient was very satisfied with the results. An upper Essix type removable retainer was provided and a lower fixed retainer was placed from premolar to premolar and periodic monitoring of retention was performed.
Conclusion
The adequate diagnosis and planning of interdisciplinary treatment, for the management of maxillary incisors with root resorption generated by impacted canines, allowed the closure of spaces, retraction of the anterior segment and improvement of the profile with the orthodontic treatment. Careful traction of the impacted canines, gingival recontouring and finally restorative reshaping of the affected teeth, led us to obtain good aesthetic and functional results.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
