Abstract
Objective:
To quantify tooth volume differences from extracted teeth when using three different three-dimensional (3D) computed tomography (CT)-based imaging modalities.
Design:
Ex vivo study.
Setting:
Laboratory and clinics of the University of Alberta.
Methods:
Cone-beam CT (CBCT) of 12 extracted teeth were scanned using 0.25- and 0.30-mm voxel size from CBCT and a 0.06-mm voxel size from micro-CT (reference standard). 3D reconstructions for each tooth from each imaging modality were made through the software ITK-SNAP®. The mean volume differences between each pair of scanning modalities were calculated and then compared and analysed through a repeated measures ANOVA.
Results:
The average overestimations of the teeth volume were 15.2% for the high-resolution CBCT and 28.1% for the low-resolution CBCT compared to micro-CT measurements. The differences in absolute volume were 81.6 mm3 and 152.8 mm3, respectively. All differences were statistically significant (P < 0.05).
Conclusions:
Orthodontists and researchers who assess root resorption through CBCT imaging should be aware that the depicted volumes may likely be overestimating tooth volume and camouflaging real root volumetric treatment changes.
Keywords
Introduction
There is a considerable amount of evidence that supports an association between orthodontic treatment and external root resorption (RR) (Roscoe et al., 2015). It is now known that the large majority of orthodontically moved teeth depict some histologically noticeable RR (Tieu et al., 2014; Walker et al., 2013; Weltman et al., 2010). Rarely, the RR amount is so significant that it can lead to important long-term viability consequences (i.e. considerable mobility and eventual loss of the affected tooth). Any clinician who provides orthodontic treatment should monitor possible RR during active treatment. Quantifying and understanding how much RR is caused by certain orthodontic devices or specific treatment approaches would also help the clinician choose an adequate appliance for each patient based on the individual baseline RR risk. Hence, understanding the accuracy and reliability of imaging tools becomes crucial.
Traditionally, RR has been quantified by measuring root length through two-dimensional (2D) radiographs. However, 2D assessment of a three-dimensional (3D) structure is destined to be incomplete and inaccurate (Forst et al., 2014; Roscoe et al., 2015; Samandara et al., 2019; Tieu et al., 2014). A more accurate RR diagnosis is expected through cone-beam computed tomography (CBCT) when compared to traditional 2D imaging. Nevertheless, CBCT imaging is not perfect. Several issues may arise when reconstructing 3D volumetric label maps of teeth or roots from CBCT images (segmentation) to assess pre- and post-treatment changes in volume. Due to these issues, the accuracy of the results may present large variability.
To be certain about RR quantification, comparing the CBCT measurements to a reference standard is necessary. Thus, the aim of the present study was to compare the tooth volume of 12 extracted teeth imaged through CBCTs with two different voxel sizes to a micro-CT scan (reference/gold standard) with significantly higher resolution. Information gathered from this study should help to improve our understanding of the accuracy of this technique.
Material and methods
The Research Ethics Committee of the University of Alberta approved this study ethics (Protocol Pro00101128). A total of 12 extracted teeth were scanned using a CBCT at voxel sizes of 0.25 mm and 0.30 mm (360°, 26.9 s and 8.9 s, respectively, 120 kV, 5 mA; CBCT ICAT, Brea, CA, USA), and a micro-CT scan at 0.06 mm (360°, 75 ms, 50 kV and 0.24 mA; Milabs U-CT, Utrecht, the Netherlands). The teeth included in the study were maxillary central incisors as well as maxillary and mandibular cuspids.
Reliability analysis was performed before the actual final measurements. For that purpose, six teeth from the sample were randomly selected using Microsoft Excel® and its randomization function. The principal investigator calculated two consecutive measurements at least one week apart of the same six teeth for the three different techniques.
Using the same technique (described below), the 12 teeth were reconstructed three times to obtain the main data of the study: one from the 0.25-mm voxel CBCT scan; one from the 0.30-mm voxel CBCT; and one from the 0.06-mm voxel micro-CT scan. The type of reconstruction performed was an automatic segmentation with manual refinements, and the software employed was ITK-SNAP® (Yushkevich et al., 2006).
The first step of the segmentation consisted of reconstructing 3D volumetric label maps of the tooth, which is done automatically by the software. The second step was the manual refinements of the contours of the initial automatic reconstruction layer by layer. The final result of the segmentation of one of the teeth can be observed in Figure 1. The third step was to collect the main dependant variable, volume, to compare the two CBCT reconstructions to the gold standard, the micro-CT scan reconstruction for each tooth.

Three-dimensional volumetric representation of one of the teeth.
Statistical analysis
For a repeated measures design, we estimated the minimum sample size of 12 for a large effect size (the ratio of mean difference to standard deviation). For sample size estimation, we set the effect size at 1.20, power at 0.80 and type I error rate at 0.05 (see Table C.2, page 720 in Portney and Watkins (2000)).
A significance level of α=0.05 was chosen for all the computations, and SPSS® version 21 (IBM Corp., Armonk, NY, USA) was employed. Regarding the reliability analysis, interclass correlation coefficient (ICC) values <0.5, at 0.5–0.75, at 0.75–0.9 and >0.90 indicated poor, moderate, good and excellent reliability, respectively (Koo and Li, 2016). The ICC model used was two-way mixed effects, absolute agreement, single rater/measurement (Koo and Li, 2016). Regarding the main objective of this study, the mean volume difference between each pair of scanning modalities was analysed through a repeated measures ANOVA. Normality check for ANOVA was not performed for two reasons: (1) sample size is small (n = 12); and (2) repeated measures ANOVA is robust to departure from normality.
Results
The resultant ICC values were 0.99 (95% confidence interval [CI] = 0.95–0.99), 0.99 (95% CI = 0.96–0.99) and 0.91 (95% CI = 0.57–0.98) for the micro-CT, the 0.25 mm CBCT and the 0.30 mm CBCT, respectively. Therefore, this method displays an excellent reliability for the three types of scans.
In Table 1, the estimated volume (in mm3) of the 12 teeth is presented. From left to right, the three initial columns show the volume on the segmentations made from the micro-CT 0.06-mm, CBCT 0.25-mm and CBCT 0.30-mm scans. The next columns show the comparisons between the three techniques. These comparisons are presented in two forms. The first one is the difference between the larger value over the lower value and the second one is the percentage increase from the smaller value. Consistently, the lower the definition, the higher the portrayed volume. This happened for every tooth and for every series of three different scans. In other words, the increase was always in the same direction, from CBCT 0.30 to CBCT 0.25 to micro-CT, which ease the computations. The average of all the values is shown in the last row.
Volume (in mm3) of each tooth scanned by micro-CT, CBCT at 0.25-mm and 0.30-mm voxel sizes and their comparisons in volume difference and percentage increase.
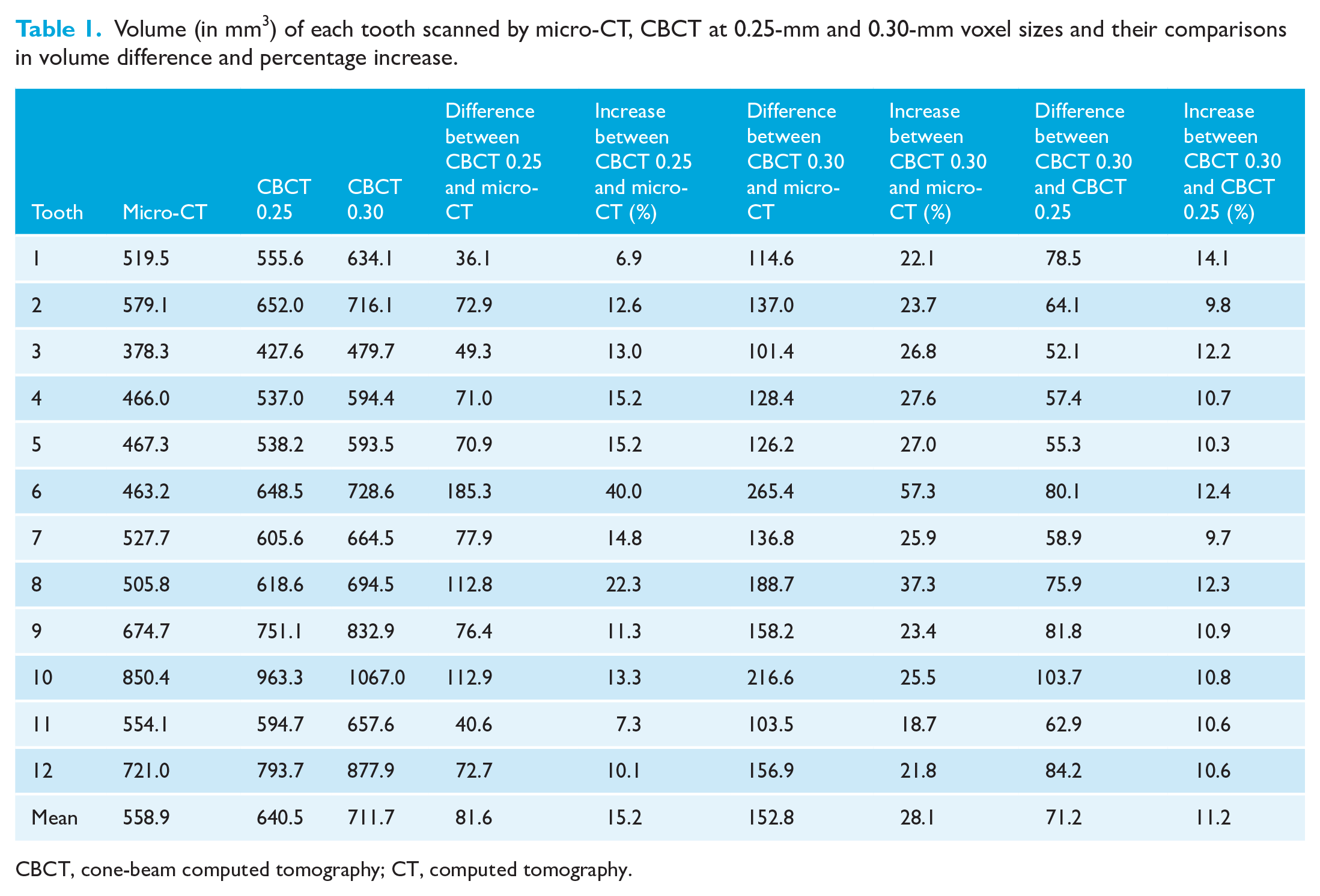
CBCT, cone-beam computed tomography; CT, computed tomography.
Mean differences, standard errors (SE) and 95% CIs for all pairwise comparisons are reported in Table 2. The average increases of the volume were 15.2% for the high-resolution CBCT and 28.1% for the low-resolution CBCT when each of them was compared to the gold standard, the micro-CT reconstructions. Between CBCTs, the average percentage increase when the high-resolution CBCT reconstructions were compared to the low-resolution CBCT reconstructions was 11.2%.
Mean differences, SE and 95% CIs for all pairwise comparisons.
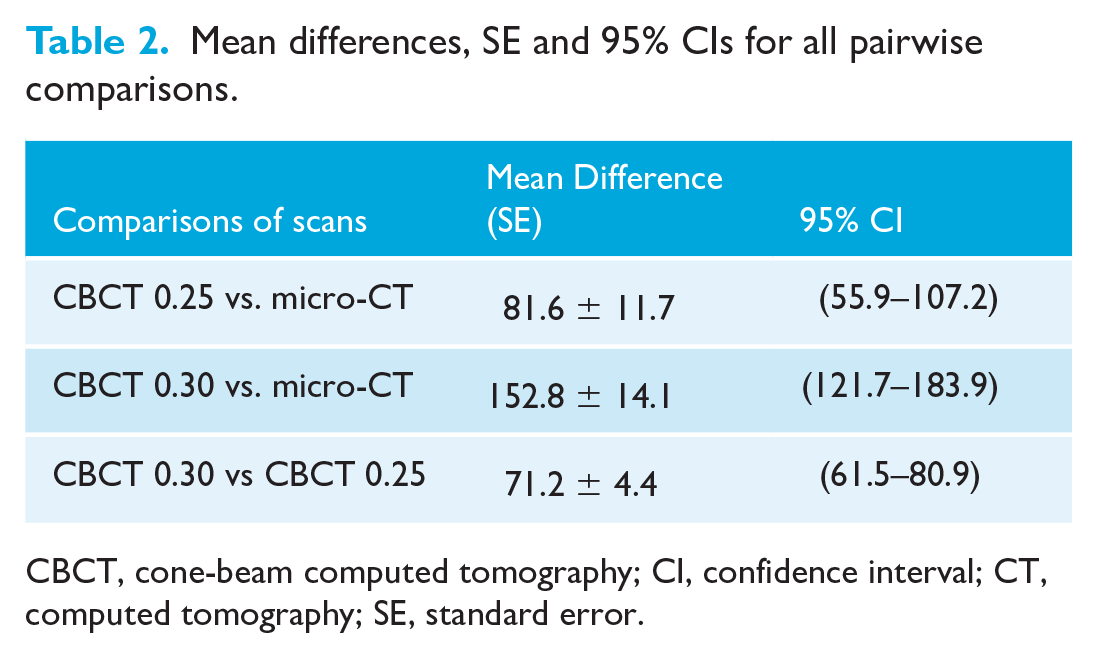
CBCT, cone-beam computed tomography; CI, confidence interval; CT, computed tomography; SE, standard error.
Regarding the absolute difference in volume, the average increase was 81.6 mm3 when the high-resolution CBCT was compared to the gold standard. Regarding the low-resolution CBCT, the yielded difference was 152.8 mm3. Between CBCTs, the increase was 71.2 mm3.
All comparisons were statistically significantly different, yielding a P value < 0.0001.
Discussion
Different CBCT resolution parameters are used in different scenarios. Therefore, it is important to understand the limitations of the imaging parameters when diagnosing and assessing RR. Different ways of measuring RR have been previously described in the literature, from volume and surface reduction to shape change analysis (Ahlbrecht et al., 2017; Puttaravuttiporn et al., 2018). The percentage of volume change is the most intuitive for clinicians and, therefore, the most helpful to put the results into perspective.
Several factors affecting the images obtained by the employed CBCT scanning may explain the consistent overestimation of the volume. Among them, one can identify the voxel size, the partial volume effect, the scattered x-rays, the field of view (FOV) and the subjectivity in the segmentation process.
In CBCT imaging, the scanned body is reconstructed as a 3D matrix of voxels. For each voxel, a grey value is assigned depending on the attenuation of the material inside. Voxel size is one of the factors that determine special resolution in CBCT-acquired images. However, it may also cause noise. Noise and spatial resolution are managed as a trade-off: the factors that increase one decrease the other. In the case of voxel size specifically, its increase causes a reduced noise but decreases in image sharpness and vice-versa (Pauwels et al., 2015).
The definition of the images generated by CBCT with the voxel sizes used in our study, 0.25 and 0.30 mm, may neither be accurate nor precise enough to detect specific amounts of volume change. Thus, this can lead to wrong diagnostic conclusions when used clinically. The problem with smaller voxels, which would provide a higher resolution (Lund et al., 2012), and more accurate results, is that longer scanning times and greater patient exposure to ionising radiation are required.
Whereas very-high- and high-resolution CBCTs are reserved for research purposes and generally are not used in private clinical settings, lower-resolution CBCTs are more commonly employed in private clinical orthodontic settings (Lund et al., 2012). In this study, the CBCT imaging employed was a full FOV (16 × 13 cm) with 0.25-mm and 0.30-mm voxel sizes. These settings are intended to emulate the conditions in private practice. They are also adequate to obtain a full FOV CBCT, a useful diagnostic and treatment planning adjunctive tool for orthodontists.
Another plausible explanation for this consistent increase of volumetric measurements in images generated by CBCT is the partial-volume effect. This effect is present at sharp edges with high contrast to neighbouring structures. A voxel can show only one density value. If that voxel entirely lies within a structure, it will reflect the density of that structure. However, suppose that voxel lies at the junction of two different structures of different density levels, i.e. enamel and air. In that case, the voxel will reflect an average value between the densities of both structures. This increase in the surface is challenging to eliminate in the segmentation process, leading to an artificial increase in the resultant volume (Baumgaertel et al., 2009; Ye et al., 2012). It seems that CBCTs with a high spatial resolution are less affected by the partial volume effect because their voxel sizes are smaller. Moreover, the images become less sharp as the voxel size increases and specific features, such as tooth fissures, are less visible on images obtained with a CBCT of 0.30-mm voxel size or larger (Maret et al., 2012).
Another possible source of an artificial increase in volume could be scattered x-rays. The photons diffracted from their original path after interaction with matter can cause scatter, affecting the density values of the tissues, leading to larger tooth volumes (Schulze et al., 2011; Ye et al., 2012).
FOV is another factor that helps to understand the volume overestimation. The smaller the FOV, the less noise from scatter radiation is generated (Lund et al., 2012). A small FOV is preferred to measure RR more accurately because of its lower scatter radiation, which produces less noise and a higher signal-to-noise ratio. Nevertheless, it is doubtful that small FOV CBCT, with its increased radiation, will be routinely used in a clinical setting to increase the level of certainty regarding RR. This is also the case because a small FOV CBCT does not include all the dentition. Hence, more than one small FOV CBCT would be required. The large FOV CBCT is the one typically used in orthodontic offices (Lund et al., 2012). This modality has relatively lower contrast and a lower signal-to-noise ratio, which generates challenging situations for the segmentation process (Liu et al., 2010). Even if its quality is not ideal for all types of measurements, including RR, it seems that CBCT voxel sizes are usually in the range of 0.30–0.40 mm (Ahlbrecht et al., 2017). This has logical reasons such as the need for a comprehensive orthodontic diagnostic (lateral cephalogram and panoramic radiography) through a full FOV at the lowest possible ionizing radiation levels.
On top of all that, there is also a certain degree of subjectivity inherent to the manual parts of the segmentation process that can consistently bias the results towards an increase or a decrease in volume (Liu et al., 2010), which can be verified when two researchers segment the same tooth (Maret et al., 2012).
Finally, some limitations are noted. The use of extracted teeth imaged ex vivo eliminates some additional factors that affect the measurement accuracy in real-life conditions. Attenuation effects provided by surrounding structures (periodontal ligament, alveolar bone, soft tissues) are inexistent in this sample. The impact of those factors was not assessed in this study design.
Conclusion
This project intended to quantify the differences in tooth volume (ex vivo) using three different 3D imaging modalities. A consistent artificial increase in volume ranged between 15.2% (81.6 mm3) and 28.1% (152.8 mm3) when CBCT segmentation was compared to the reference standard. The volume obtained from the reconstructions increased with the voxel size. It seems that the sources of this constant overestimation could be the voxel size, the partial-volume effect, the scatter x-rays, the FOV size and/or the subjectivity of the segmentation process. Even if no scale of RR severity has reached a consensus, the CBCT imaging, as used in this study, will probably not be able to detect minor, moderate, and even large amounts of RR. Orthodontists and researchers who assess RR through a day-to-day CBCT imagining technique should be aware of the limitations of this technique and understand that the volumes depicted may be overestimating and camouflaging real root changes that may occur through treatment.
Footnotes
Acknowledgements
We thank Kevin Chen and Antonio Rossi for valuable discussion on segmentation using ITK-SNAP software. We also thank Maria Alexiou for her help with micro-CT scanning.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: GH would like to thank the National Sciences and Engineering Research Council of Canada (NSERC DG 2016-05167). GH and CFM thank the McIntyre Memorial fund from the School of Dentistry at the University of Alberta.
