Abstract
Evidencing eHealth interventions, benefits generates data as a basis for assessing whether observed changes in behavior, processes or healthcare outcomes can be attributed to the eHealth interventions. Generating such evidence requires the use of frameworks or some other type of organizing schemes to help in guiding the process and making sense of eHealth systems and the findings. The frameworks available in literature do not clearly guide on how to monitor eHealth implementation and evaluate eHealth implementation results. This study aimed to develop and validate an eHealth evaluation framework to guide the process of monitoring eHealth implementations and evaluation of eHealth results in terms of outcomes and impact on healthcare in developing countries. The Design Science Research Methodology was followed to conduct this study. Recommendations from an eHealth evaluation exploratory study in Uganda and other eHealth evaluation literature formed key inputs into the design and development of the framework. The framework consists of a generic reference model with eHealth monitoring and evaluation dimensions, performance indicators, and guidelines on how to conduct eHealth monitoring and evaluation. The eHealth evaluation framework received high acceptance (>80%) as regards its fitness for purpose during its validation.
Introduction
Across the world, healthcare systems are facing pressures to guarantee equitable access to quality and affordable healthcare. Healthcare administrators and policy makers are expected to select and implement interventions that increase the quality and efficiency of services, care and support high performance of health systems.1,2 The application of information and communication technology (ICT) in healthcare management, referred to as eHealth, 3 is becoming more popular and has proved to improve the effectiveness, access, quality and efficiency of healthcare systems.3–5 eHealth has facilitated various medicine and public health operations including patient and public health data management (electronic health records), provision of remote healthcare services (telemedicine/teleHealth), health information and services through mobile telephone technology (mHealth), health knowledge management and distant learning for health workers (eLearning), connection of medical devices (internet of things), and other areas like improved planning, organization, management of health services, and more recently the management of large public health data. The Internet has also facilitated communication between healthcare providers and their clients, sharing of information and knowledge among healthcare providers and researchers, all of which have contributed to better disease management.6,7 Many developed countries have implemented well-developed eHealth applications that have benefited their healthcare systems.
Learning from the developed world, developing countries are implementing ICT solutions as a means to improve accessibility to quality and equitable healthcare.8,9 Uganda, like most other developing countries, has employed eHealth to improve healthcare delivery and public health8,10 and this has yielded positive results, especially in disease control and prevention through disease surveillance. 11 Implemented since 2011, Uganda’s national DHIS2-based electronic Health Management Information System (eHMIS), one of the key nationally scaled up eHealth platforms, is used to capture, validate, analyze and visualize aggregate data about health events and services reported by healthcare providers, especially public healthcare facilities, across the country. Apart from the national eHMIS, other eHealth platforms are used in Uganda to support delivery of various functions including management of human resources for health, supply of essential medicines and medical supplies, laboratory information management, and integrated disease surveillance and response.
Such an increasing investment in eHealth has also increased demand for evidence to prove that there are benefits and results realized from eHealth applications. The evaluation of eHealth interventions helps to generate data that can be used as a basis for assessing whether observed changes in behavior, processes or health outcomes can be attributed to the eHealth interventions.12,13 The concept of “evaluation” is defined as a systematic and objective assessment of an intervention that aims to determine the fulfillment of objectives, efficiency, effectiveness, impact and sustainability. 14 Related to evaluation is the concept of “monitoring” which is the routine collection, review, and analysis of data intended to measure implementation progress for an eHealth initiative, and results into adjustments in intervention activities necessary to maintain or improve the quality and consistency of the eHealth deployment. World Health Organization (WHO) emphasizes that evaluation measures changes in outcome and impact that are attributed to the eHealth initiative. 13
Analysis of the existing eHealth evaluation models and frameworks.
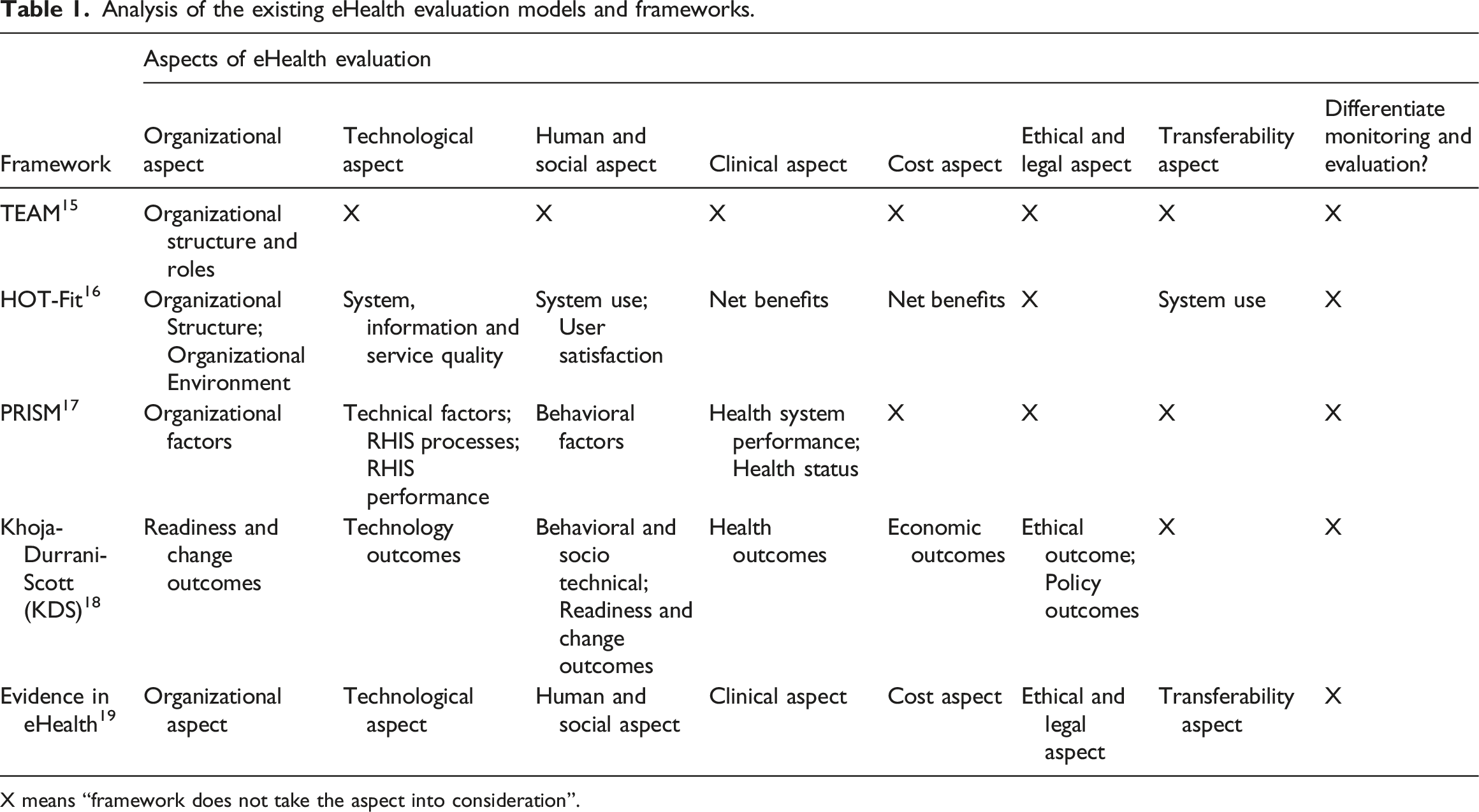
X means “framework does not take the aspect into consideration”.
Accordingly, this study aimed to develop and validate an eHealth evaluation framework to guide monitoring of eHealth implementations and evaluation of their results in terms of outcomes and impact on healthcare in developing countries, using Uganda as a case study.
Methodology
Study setting
The study was conducted in a period between 2019 and 2020 within the context of Uganda as a developing country. The study was well documented based on literature on eHealth evaluation practices and challenges. The study was conducted in close consultation with Uganda Ministry of Health (Division of Health Information), which is the custodian of digital health and health information management in Uganda.
Study design
The Design Science Research Methodology (DSRM)23,24 was followed to conduct this study. DSRM was used because of its ability to study the connection between research and professional practices by designing, implementing and evaluating artifacts that address a specific need, and embodies the creative, artistic, and goal-oriented spirit within which purposeful artifacts are created. 25 Particularly, the six DSRM activities were carried out as detailed below;
Respondent’s level of eHealth experience and organizations’ role.

Validation criteria for the eHealth evaluation framework.
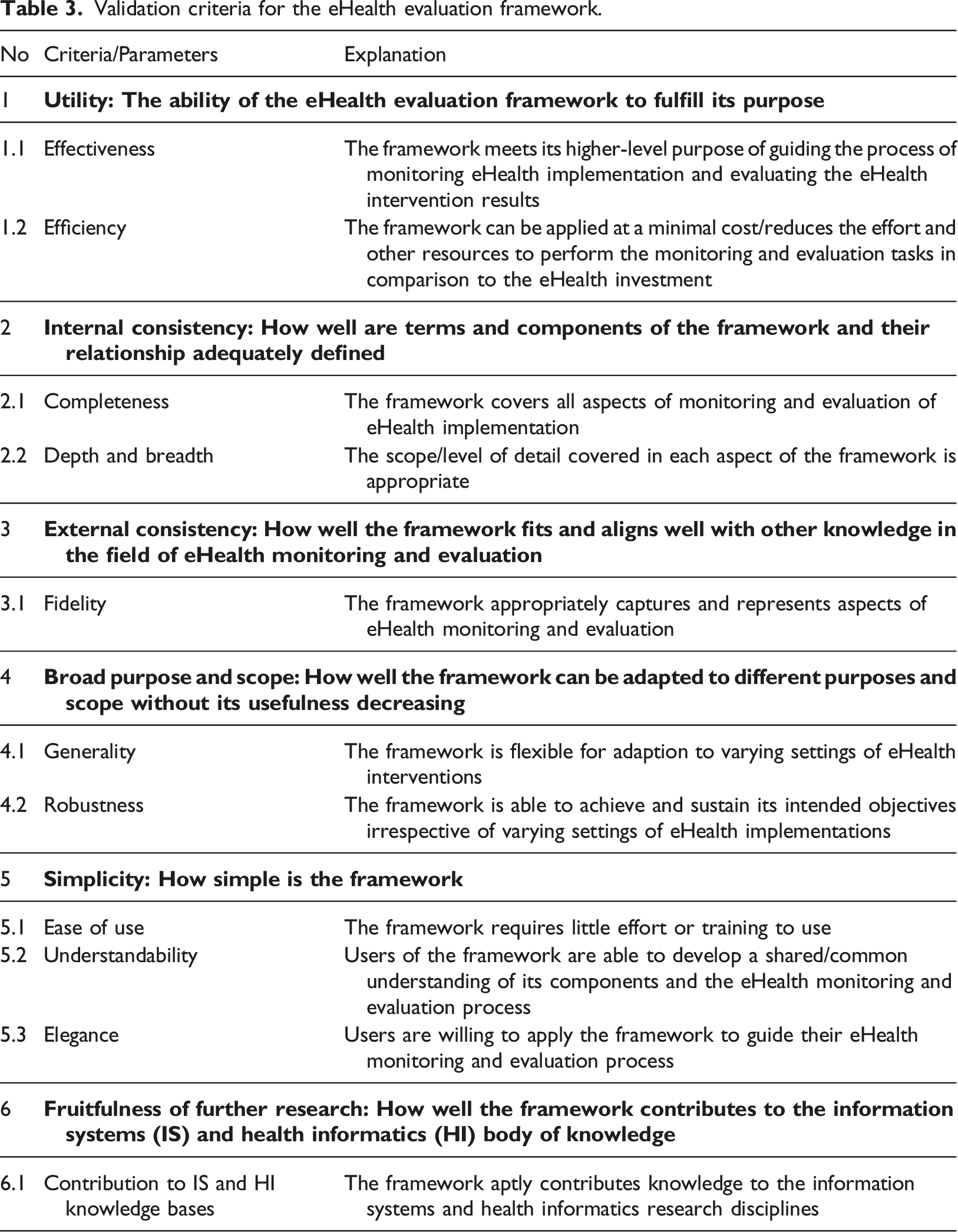

Ethical consideration
Researchers obtained written authorization from Uganda Ministry of Health to conduct the study within Uganda’s eHealth implementation settings. For participants engaged in the demonstration and validation of the framework, the researchers verbally informed participants that participation to give feedback about the framework was voluntary, and submission of feedback would mean consent to participate.
Results
Design and development of an eHealth evaluation framework
An eHealth evaluation framework was designed and developed. It constitutes of three components-i) a reference model that demonstrates key aspects of eHealth monitoring and evaluation; ii) performance indicators for measuring eHealth performance and how these can be operationalized; and iii) a set of guidelines on how to conduct monitoring and evaluation of eHealth interventions.
i). eHealth evaluation reference model derivation and description
Findings of the exploratory field study
22
on indicators supposed to be assessed during the eHealth evaluation were corroborated with the suggestions from other eHealth evaluation frameworks in literature13,16–19 to derive substantial and fundamental all-encompassing eHealth evaluation domains and sub-domains that are supposed to be assessed (see detailed derivation
29
). The resultant indicator domains and sub-domains were further aligned with the results chain provided in the results-based management strategy (see Figure 1)
30
and the evaluation questions provided in the categorization of the eHealth indicators (see Figure 2)
13
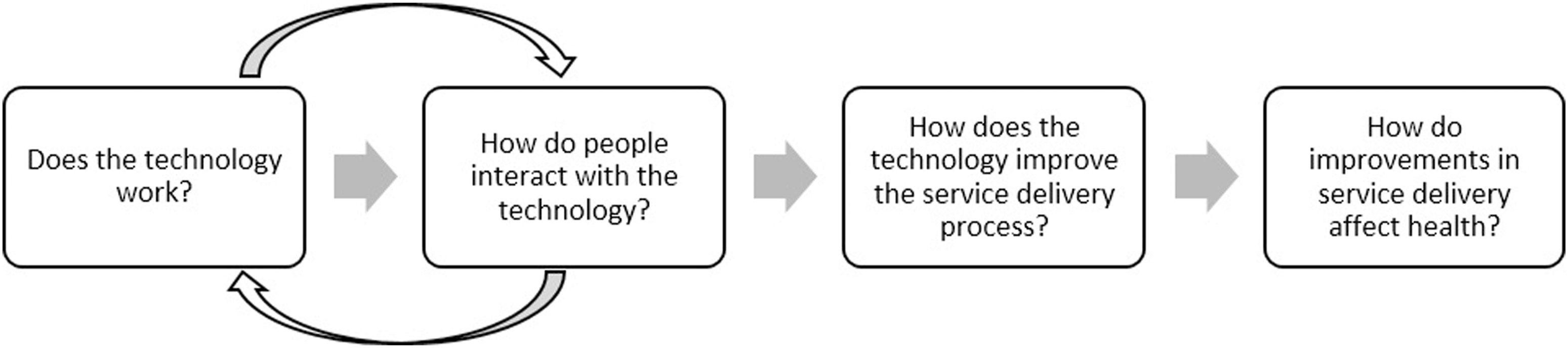
in order to further distinguish between the aspects of “monitoring” and “evaluation” of eHealth implementation results in the developed eHealth evaluation reference model (see Figure 3). The Results-based management strategy provides that all actors, contributing directly or indirectly to achieving a set of results, should ensure that their processes, products and services contribute to the achievement of the desired results in terms of outputs, outcomes and higher-level goals or impact. It is a results chain of inputs-activities-outputs-outcomes-impact on the basis that actions taken at one level will lead to a result at the next level; and in this sense, the results chain stipulates the sequence of actions taken to achieve a particular result. The categorization of eHealth indicators provides guidance on the key monitoring and evaluation questions that can help to assess various areas through which eHealth interventions can achieve results, and the questions include a) Does the technology work; b) How do people interact with the technology; c) How does the technology improve the service delivery process; and d) How do improvements in service delivery affect health? Results chain from the results-based management strategy.
30
Categorization of eHealth indicators.
13
An eHealth evaluation reference model to evaluate eHealth interventions.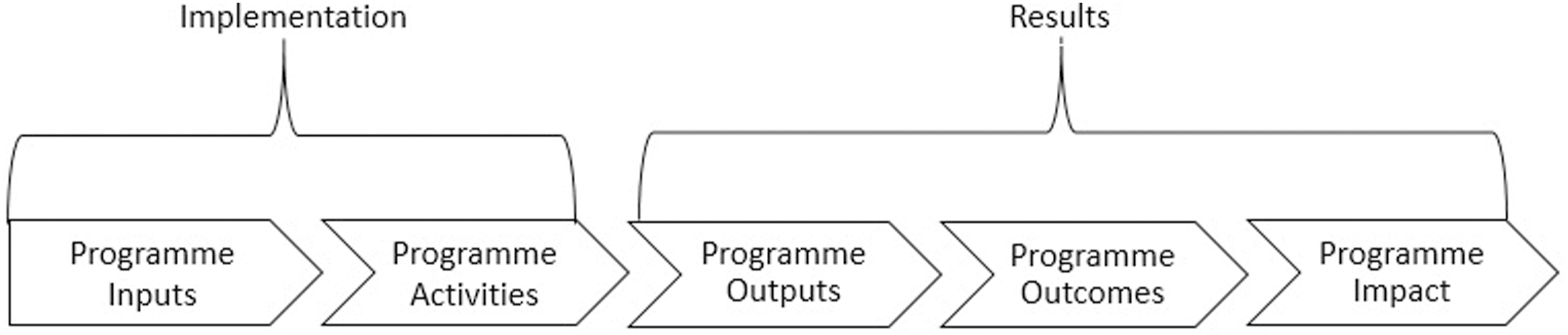
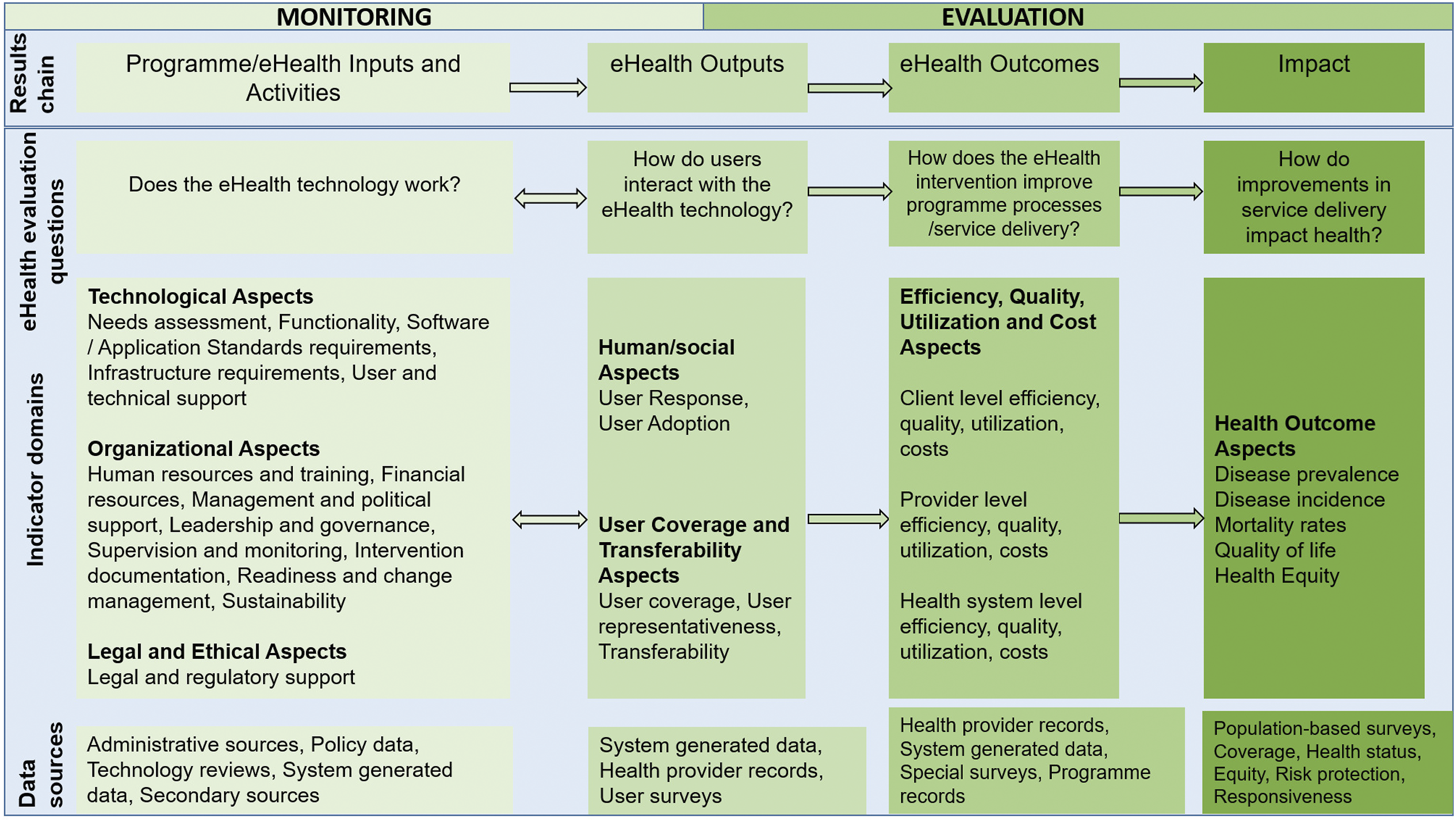
The eHealth evaluation reference model provides a basis for evaluating the performance of eHealth implementations along the results chain, starting with the programme inputs and activities until the impact. The model indicates the key eHealth evaluation questions that should be answered; the key domains of performance indicators, and the data sources where the data needed to measure the indicators can be collected from at each stage of the results chain. The monitoring of programme inputs and activities answers whether the eHealth technology works; and it relates to the assessment of the feasibility of the eHealth implementation and the inputs for developing the initiative. Monitoring of eHealth outputs assesses how the users interact with the initiative; and it relates to the service output measures intended to capture and assess the immediate results of the eHealth initiative as well as the usability measures to help quantify how the users interact with it. Evaluation of eHealth outcomes helps to ascertain how the eHealth improves programme processes and service delivery; and it captures the effect of the eHealth implementation on programme service utilization outputs or the extent to which the clients use the programme service, and intermediate population-level outcomes. The “evaluation of impact” focuses on establishing how improvements in service delivery impact health by capturing long-term outcomes, and impact on health that are attributed to the health intervention being supported by the eHealth initiative. Also, to note is a feedback loop in monitoring of the programme inputs and activities, and eHealth outputs. From a technical perspective, eHealth inputs affect the respective outputs and users’ experience, while the user experience/feedback informs the eHealth development process. Feedback from end-user adoption and satisfaction rates loops around to further inform the eHealth development process and determines the quality of the technological inputs. This, in turn, affects the performance of the revised version of the eHealth system among end-users, making the technology development process iterative.
ii). eHealth evaluation framework indicators and operationalization tools derivation
An indicator is defined as “a quantitative or qualitative factor or variable that provides a simple and reliable means to measure achievement, to reflect the changes connected to an intervention or to help assess the performance of a development actor”. 31 In order to demonstrate how the eHealth interventions’ performance can be measured at each stage of the results chain in the reference model, suggestions and best practices provided in various eHealth evaluation literature13,16–20,22,30,32 were synthesized and used to develop a set of example indicators and their respective operationalization tools (see detailed list 33 ). To note is that, this set of example indicators and operationalization tools are general and non-exhaustive; henceforth requiring that priority indicators and their operationalization tools for use to monitor and evaluate a specific eHealth intervention should be selected based on the relevance of the intervention and modified to reflect the specific objectives of the intervention.
iii). Guidelines for conducting evaluation of eHealth interventions derivation
The last component of the eHealth evaluation model provides a set of guidelines that are intended to guide/facilitate the users through a step-by-step process of planning and executing activities for monitoring and evaluation of eHealth interventions. Informed by findings of the exploratory study by Ashaba and Nabukenya,
22
and the guidance from World Health Organization, International Telecommunication and Uganda eHealth Strategy,13,20,32 this paper provides a set of key strategies and course of actions that should be followed with adaptation to the eHealth context, while planning for and conducting monitoring and evaluation of eHealth interventions in Uganda and other low- and middle-income countries with similar or related eHealth settings; 1. Establish dedicated resources and effort to ensure an effective process, and such considerations should be provided from the inception of the initiative. eHealth implementers should plan and budget for monitoring and evaluation of the interventions during planning and costing of their eHealth programmes, to ensure that appropriate resources are dedicated;
32
2. Identify all key stakeholders of the eHealth initiative, involve them and consider their interests in the eHealth intervention while designing the monitoring and evaluation plans, and ensure their consensus on the public health need or goal that the eHealth addresses or supports;
13
3. Make use of/refer to the eHealth reference model (Figure 3), indicator domains and sub-domains (see details
29
) as well as the examples indicators (see details
33
) as guides to think through the necessary monitoring and evaluation aspects of the eHealth intervention. The reference model provides a graphical representation to aid the clarification of monitoring and evaluation scopes and identification of expected causal links between inputs and activities, outputs, outcomes and impacts for eHealth implementations, while the indicator domains and indicators provide a non-exhaustive list of some examples of indicators that can be measured under each stage of the results chain; 4. Define the appropriate eHealth initiative implementation phases and timeframes
20
to specify and harmonize the stages of the eHealth maturity, timing for delivery of the defined results and frequency of measuring the results. It should be noted that defining the eHealth initiative implementation phases helps to refine and focus on the appropriate results and indicators to be monitored or evaluated at each stage of maturity of the eHealth intervention. Stakeholders should agree on the stage of maturity of the eHealth intervention and determine the appropriate monitoring or evaluation activities to avoid embarking on premature.
13
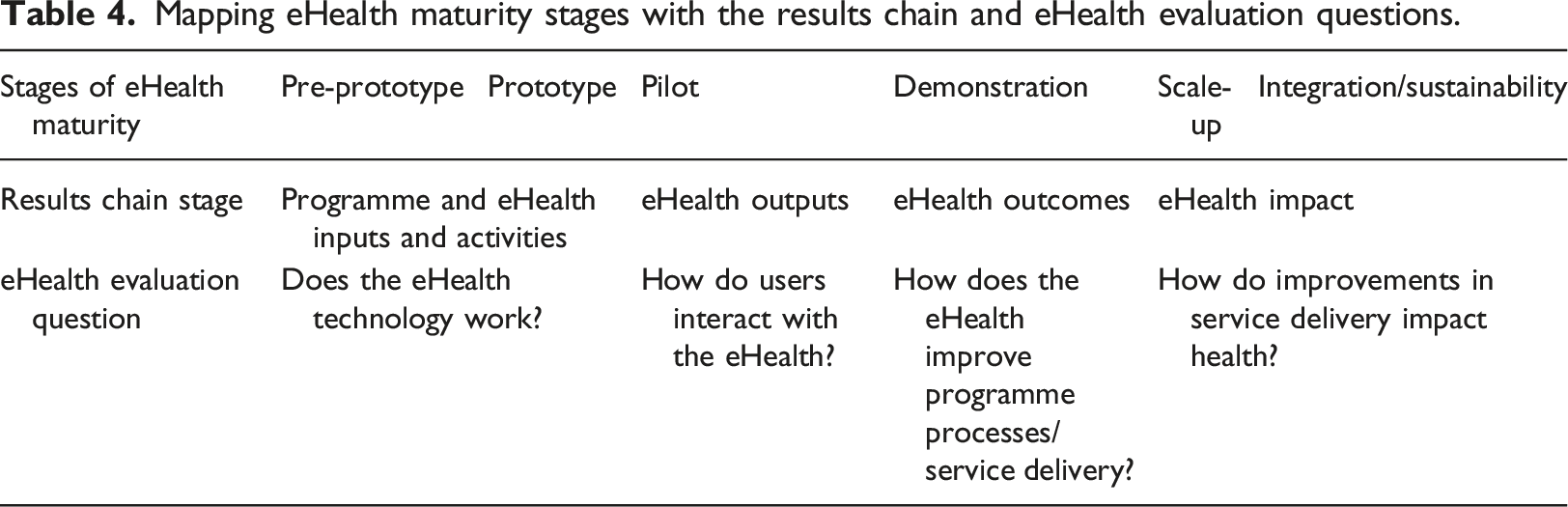
The mapping shown in Table 4 can be used to match the six stages of maturity of an eHealth intervention with the results chain and eHealth evaluation questions; 5. Define stakeholder priorities and their projected impact of the eHealth intervention and outcomes required to cause the defined impact, and the respective impact and outcome measurable indicators while ensuring that interests of all identified stakeholders are addressed. It should be noted that evaluation of an eHealth intervention can be limited to its process and early outcomes without the need to evaluate its long-term outcomes and impact if the eHealth is supporting a health intervention with known efficacy based on prior research. For example, an evaluation of an eHealth intervention for vaccination reminders should focus on measuring the percentage of children who received timely vaccination as a result of the eHealth prompt (e.g. text message) and need not seek to measure the direct impact of vaccination on the rate of child mortality from the disease they are vaccinated against, since the effectiveness of timely vaccination will have been established through prior research;
13
6. Define eHealth outputs required to lead to each defined eHealth outcome and the respective eHealth output indicators.
20
The outputs should include immediate results of the eHealth intervention and should also capture usability measures that help to quantify how users interact with the eHealth intervention; 7. Define eHealth inputs and activities and their respective measurable indicators while taking consideration of all the technical, organizational, policy and behavioral factors that influence delivery of a working eHealth application. Indicators for availability of resources required to support monitoring and evaluation functions should also be considered while defining indicators for the eHealth inputs and activities; 8. Define the baseline and target measures for the defined indicators to clearly label the situation before the eHealth implementation (baseline measures) and expected achievements (target measures) after the eHealth implementation.
20
A measure of the baseline situation facilitates the ability to compare situation statuses before and after the eHealth implementation. It necessitates research and analysis to determine baseline measures for each indicator, while internal analysis and input from the subject-matter experts and other health experts are necessary to determine the target measures;
32
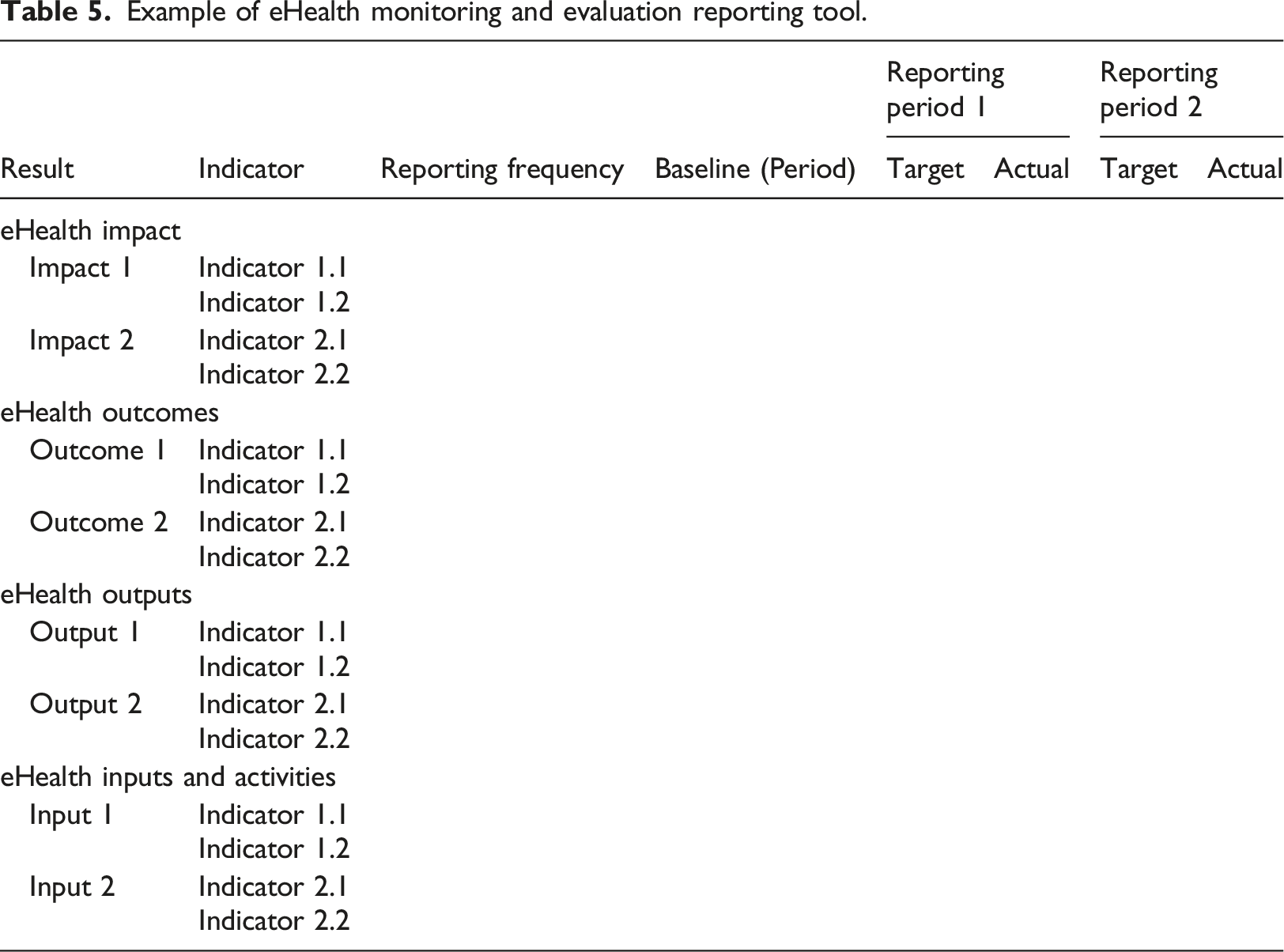
9. Define the necessary monitoring and evaluation governance and processes/activities.20,32 Considering that monitoring and evaluation tasks are conducted at different and various times and by various parties, it is imperative that their governance model is defined to guide on the available functions, roles, responsibilities, and required mechanisms to deliver them; 10. Prepare for and initiate the monitoring and evaluation process that should continue ongoing in parallel with the eHealth implementation,20,32 with monitoring or evaluation undertaken at the defined timeframes for each of the indicators. The preparation involves defining detailed monitoring and evaluation timelines and milestones and ensuring the availability of all the resources required to support the monitoring and evaluation activities including the monitoring and evaluation teams and data collection tools; 11. Execute the monitoring and evaluation data collection activities and track indicator measures according to the eHealth maturity stage, timing for delivery of the defined results, defined indicators, frequency of measuring the results, and defined monitoring and evaluation timelines; 12. Analyze collected data and report on actual situation versus target eHealth adoption and results as per defined indicators (see example reporting tool in Table 5). The analysis may also include identification of causes of divergences in actual and target performance at each stage in the results chain for each timeframe of measuring results; 13. Engage stakeholders to agree on the corrective actions to address divergence between target and actual results, and provide for management of changes in the eHealth implementation scope, if required, to implement the agreed corrective actions;20,32 14. For indicators that may be unrealistic or unachievable within the required timeframes, engage stakeholders to review and agree on refined indicators, targets and timeframes for consideration in the next round of results measurement. Mapping eHealth maturity stages with the results chain and eHealth evaluation questions. Example of eHealth monitoring and evaluation reporting tool.
Validation of the eHealth evaluation framework
Figure 4 provides the criteria score analysis of the feedback regarding the framework validation. We observed that 80% and above of the participants agreed that the model met all the criteria, apart from efficiency (76%) and ease of use (71%). The results indicated that the framework is able to fulfill its purpose (average score of 85.5% on effectiveness and efficiency), its components and their relationship are adequately defined (score of 81% on each of completeness, and depth and breadth), and also fits and aligns well with other knowledge in the field of eHealth (score of 81% on fidelity). The validation results demonstrated acceptance that the framework is suitable for adaptation to eHealth interventions of different purposes and scope (score of 95% on each of generality and robustness), and further indicate the framework is simple to use (average score of 78.5% on ease of use and understandability). eHealth evaluation framework validation results.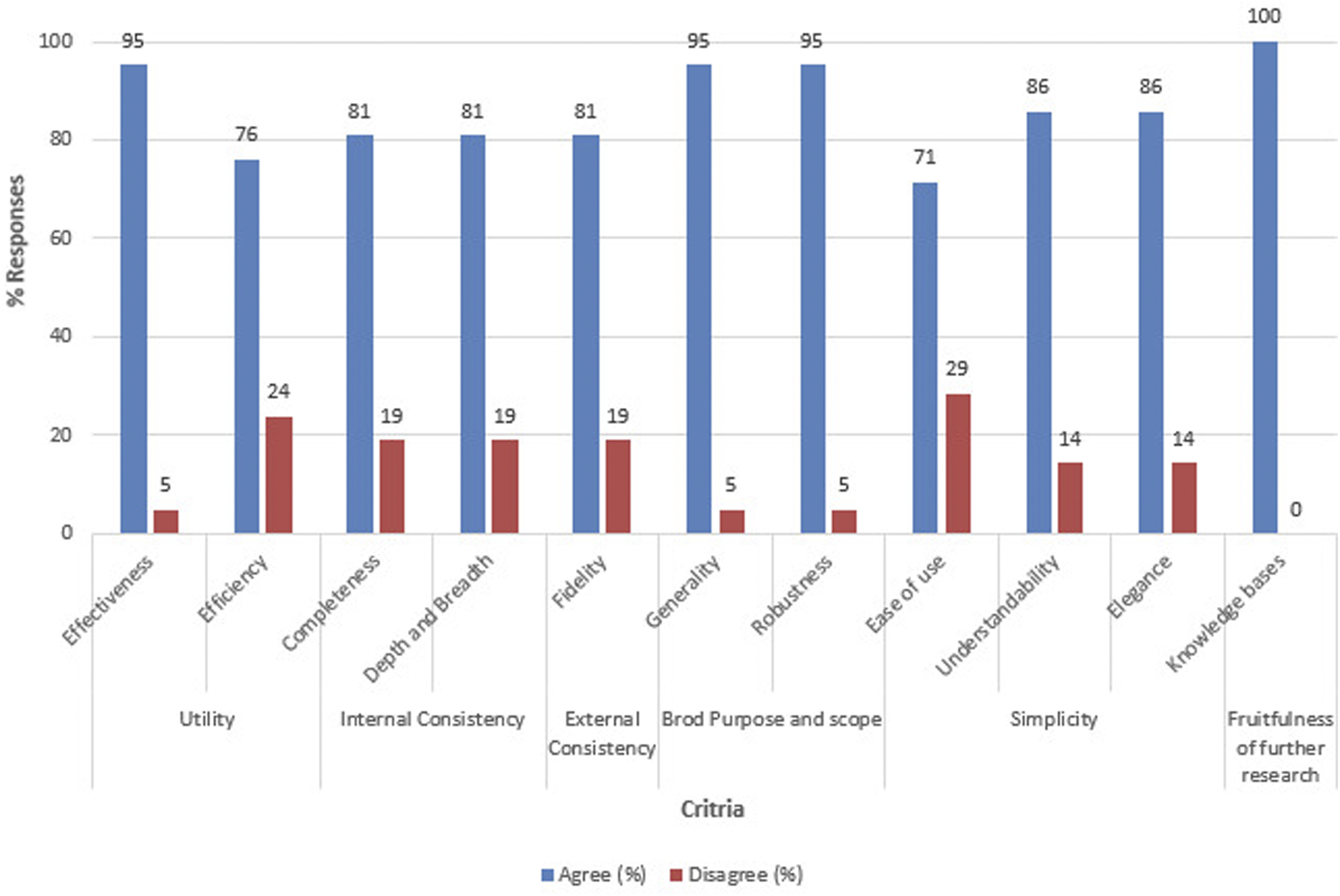
Discussion
The developed framework consists of a generic reference model that demonstrates key aspects (dimensions) of eHealth monitoring and evaluation, performance indicators used to measure eHealth performance and their operationalization tools, as well as a set of guidelines on how to conduct monitoring and evaluation of eHealth interventions. The framework was developed with consideration of guidance and recommendations from varied literature and it facilitates the understanding of the distinction between the notions of “monitoring” and “evaluation” of eHealth interventions. While the monitoring notion focuses on routine collection, review, and analysis of data intended to measure implementation progress for an eHealth intervention and results into adjustments in intervention activities necessary to maintain or improve the quality and consistency of the eHealth deployment; the evaluation notion deals with measuring the changes in outcome and impact that are attributed to the eHealth intervention. This distinction is worth a significant asset in the research disciplines and practice of eHealth, medical/health informatics and information systems (with attention to healthcare).
From the framework validation results (Figure 4), such a high score of 80% and above on each criterion apart from efficiency (76%) and ease of use (71%) suggested that participants appreciated the framework’s fitness for purpose. The remaining 24% and 29% of the participants, who did not agree on the framework’s efficiency and ease of use respectively, may gain confidence in the framework and appreciate its ease of use and application with minimal resources after having more time of training and application of the framework in eHealth evaluations as suggested by other studies.23,34,35 The high acceptance of the framework confirmed the same experience as that from an artifact validation study by Al Nadabi where acceptance was as high as 80% and above. 36 The high acceptance of the framework by the eHealth experts in Uganda further suggest its applicability to other low- and middle-income countries with similar eHealth settings, which may require none to less customization of the framework to fit/align with their respective eHealth evaluation goals. 37
It should be noted, however, that the framework demonstration and validation activities were undertaken amid the COVID-19 pandemic which resulted in conducting the activities while strictly adhering to the Uganda Ministry of Health COVID-19 infection prevention and control guidelines. This limited the extent of stakeholder engagement and the field activities that could be conducted. Demonstration and validation of the framework’s utility was done through walk-throughs in a workshop setting where COVID-19 related guidelines could easily be enforced. This approach could not provide feedback about the framework’s application in real-life eHealth implementation settings. To counteract this limitation, the researchers are currently conducting empirical validation of the framework to further understand its applicability and benefits in the field.
Conclusion
In this research, we present both the relationship and difference between monitoring of eHealth interventions implementation and evaluation of outcomes and impact realized from the interventions. We developed and validated an eHealth evaluation framework to guide the process of monitoring and evaluating eHealth interventions performance in healthcare. The high acceptance (>80%) that the framework met its validation criteria suggested its fitness for purpose during its validation. To get started with using the eHealth evaluation framework, eHealth implementers will need to first read and understand its three components in order to appreciate how to apply it depending on the nature and purpose of the eHealth intervention in consideration. The framework is applicable to the evaluation of individual eHealth interventions and it yields substantial results if its guidelines’ prescription is followed in a timely manner (that is, starting with the initial planning phases of the eHealth interventions). We recommend the application of the framework to evaluations in real-life settings and/or scenarios of eHealth interventions in Uganda and other low- and middle-income countries to further evidence its applicability and benefits. Further research could assess the suitability of the framework for monitoring and evaluation of eHealth in the context of developed countries.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
