Abstract
Background & objective:
While splenectomy is performed for various trauma and non-trauma indications, there is little information about the impact of cirrhosis on the post-splenectomy outcomes, despite the intricate physiological and vascular connection between the liver and the spleen.
Methods:
2011–2017 National Inpatient Sample was used to select patient cases who underwent the splenectomy procedure, who were further stratified using cirrhosis. The cirrhosis-absent controls were matched to the study cohort using propensity score matching with nearest neighbor matching method. Endpoints included mortality, length of stay, hospitalization costs, and postoperative complications.
Results:
There were 675 patients with cirrhosis and 675 matched controls identified from the database. Cirrhosis cohort had higher mortality (20.0 vs 7.26%, p < 0.001, OR = 3.19, 95% CI = 2.26–4.52) and hospitalization costs ($210,716 vs $186,673, p = 0.003), but shorter length of stay (11.8 vs 12.5d, p = 0.04). In terms of complications, cirrhosis cohorts had higher postoperative bleeding (7.26 vs 4.3%, p = 0.027, OR = 1.74, 95% CI = 1.09–2.80) and shock (3.7 vs 1.04%, p = 0.002, OR = 3.67, 95% CI = 1.58–8.54), and were more likely to be discharged to short-term hospitals and home with home health care. On multivariate analysis, presence of cirrhosis resulted in higher mortality (p < 0.001, aOR = 3.30, 95% CI = 2.33–4.69).
Conclusions:
Cirrhosis is an independent risk factor of postoperative mortality in patients undergoing splenectomy; given this finding, further precautious and multidisciplinary care should be rendered in these at-risk patients with cirrhosis in the setting of splenectomy.
Keywords
Introduction
Patients with cirrhosis have increased risks of postoperative complications and mortality following intra-abdominal operations due to various cirrhosis-related physiologic disturbances that affect circulatory hemodynamics during surgical procedures.1–6 The surgical manipulation of the peritoneal space and the abdominal organs may sensitively affect the hemodynamics of the portal and splanchnic systems. For example, disruptions in cytoarchitecture and tissue vasculature may lead to high-grade inflammation, more significant portal-systemic shunting due to the local inflammatory response, greater bacterial translocation and endotoxemia, arterial hyperdilation, and the establishment of a hyperdynamic state.2–4 In this state, circulatory hemodynamics are more likely to change rapidly with the shifts in blood volume during surgery, which may result in organ hypoperfusion and multiorgan failure.
The increased postoperative risks and increased mortality in patients with cirrhosis undergoing intra-abdominal procedures have been validated in prior studies that evaluated the outcomes of cirrhosis patients following various abdominal surgical procedures (including cholecystectomy, appendectomy, and colonic resections).7–10 However, no similar studies have evaluated the effects of cirrhosis on the postoperative outcomes of patients undergoing splenectomy. This information is important to investigate as splenectomy is indicated in various elective and non-elective clinical situations, such as in drug-refractory immune thrombocytopenic purpura 11 or emergency situations such as traumatic splenic lacerations and ruptures. 12 Despite the broad clinical usage of splenectomy, the postoperative prognosis and complications following splenectomy in cirrhotic patients are not well-known. Therefore, the analysis of risks and benefits in this patient population becomes difficult.
In this study, we use a national database to investigate the effects of cirrhosis on the postoperative outcomes of patients undergoing splenectomy. By doing so, we aim to better characterize the risks of adverse postoperative outcomes in this vulnerable patient population.
Methods
NIS database and variable selection
As similar to prior studies conducted by the current set of authors,13,14 this research utilized the National Inpatient Sample, which is a national registry based off of US hospitals data that is collected via the Agency for Healthcare Research and Quality (AHRQ); as a whole, the database collects patient hospitalization information from non-federal and community hospitals, and contains patient demographics, discharge disposition, hospital admission characteristics, and discharge diagnoses that are encoded using the standard ICD codes. As an example, the updated 2017 database contained 7.2 million visits to 4584 hospitals, sampled from 97% of US hospitals across 48 states. 15 In 2015, the ICD coding system transitioned from ICD-9 to ICD-10. The coding software and statistical platforms adapted to these changes using official General Equivalence Mappings (GEMS) cross-referencing guidelines,16,17 which was incorporated into the search program used in this analysis. This search program was able to identify principal terms relevant to the diagnosis of interest, which was cross-linked with the other ICD set using the GEMS data. This allowed for formal transition between ICD-9 and ICD-10 codes, thus minimizing potential heterogeneity that may exist in this coding process.
This study included patients who underwent in-hospital cases of splenectomy (which included total/partial splenectomy and splenic excision). Those under 18 years of age were excluded. The exposure variable for the primary analysis was cirrhosis; endpoints included in-hospital mortality, length of stay, hospitalization costs, discharge disposition, and postoperative complications (bleeding, infection, wound complication, respiratory failure, and shock). Additional sub-analyses were performed using decompensated cirrhosis (defined as presence of ascites, varices, and portal hypertension) as the primary exposure in patients with cirrhosis; furthermore, the study population was stratified using chronic liver disease (this included nonspecific liver disease, hepatitis B/C, non-alcoholic and alcoholic liver disease; either with and without cirrhosis) and the elective (vs non-elective) nature of the procedure to compare clinical endpoints.
All study variables and corresponding ICD-9/10 codes are recorded in Supplementary Table 1.
Study design and statistical analysis
In this study, propensity score matching was used to match the cirrhosis-absent controls to those with cirrhosis, with 1:1 nearest neighbor match; the propensity score-generating multivariate model included the following variables as covariates: age, race, gender, diabetes, hyperlipidemia, hypertension, chronic obstructive pulmonary disease, coronary artery disease, chronic kidney disease, congestive heart failure, coagulopathy, alcohol use disorder, cigarette use, obesity, hypersplenism, splenomegaly, portal vein thrombosis, and elective (vs non-elective) nature of the procedure. The purpose of the propensity score match was to no-parsimoniously fit the controls to the study population, thereby reducing the inherent biases in the patient selection process. Following the match, univariate and multivariate analyses were performed using either Welch’s t-test/Student’s t-test for non-nominal variables and chi-square/Fisher’s exact tests for nominal variables. Logistic and Poisson Regression analysis was performed for endpoints; model fit and multicollinearity was evaluated using variance inflation factor analysis (VIF), Akaike information criterion (AIC), and Bayesian information criterion (BIC) model parameters.18–20 A p-value of less than 0.05 denoted statistical significance.
Results
Patient selection
The NIS database identified all patients with procedural diagnoses of partial/complete splenectomy or spleen excision. After excluding patients under age 18, there were a total of 30,732 patients. From this, there were 675 patients identified with cirrhosis and 30,057 without cirrhosis. Using the propensity score matching algorithm noted above, the post-matching comparison included 675 patients with cirrhosis and 675 without cirrhosis. Additional subgroup analyses were performed that stratified patients based on the presence of decompensated cirrhosis, chronic liver disease (with and without cirrhosis), and elective (vs non-elective) nature of the procedure, as demonstrated in Fig. 1.
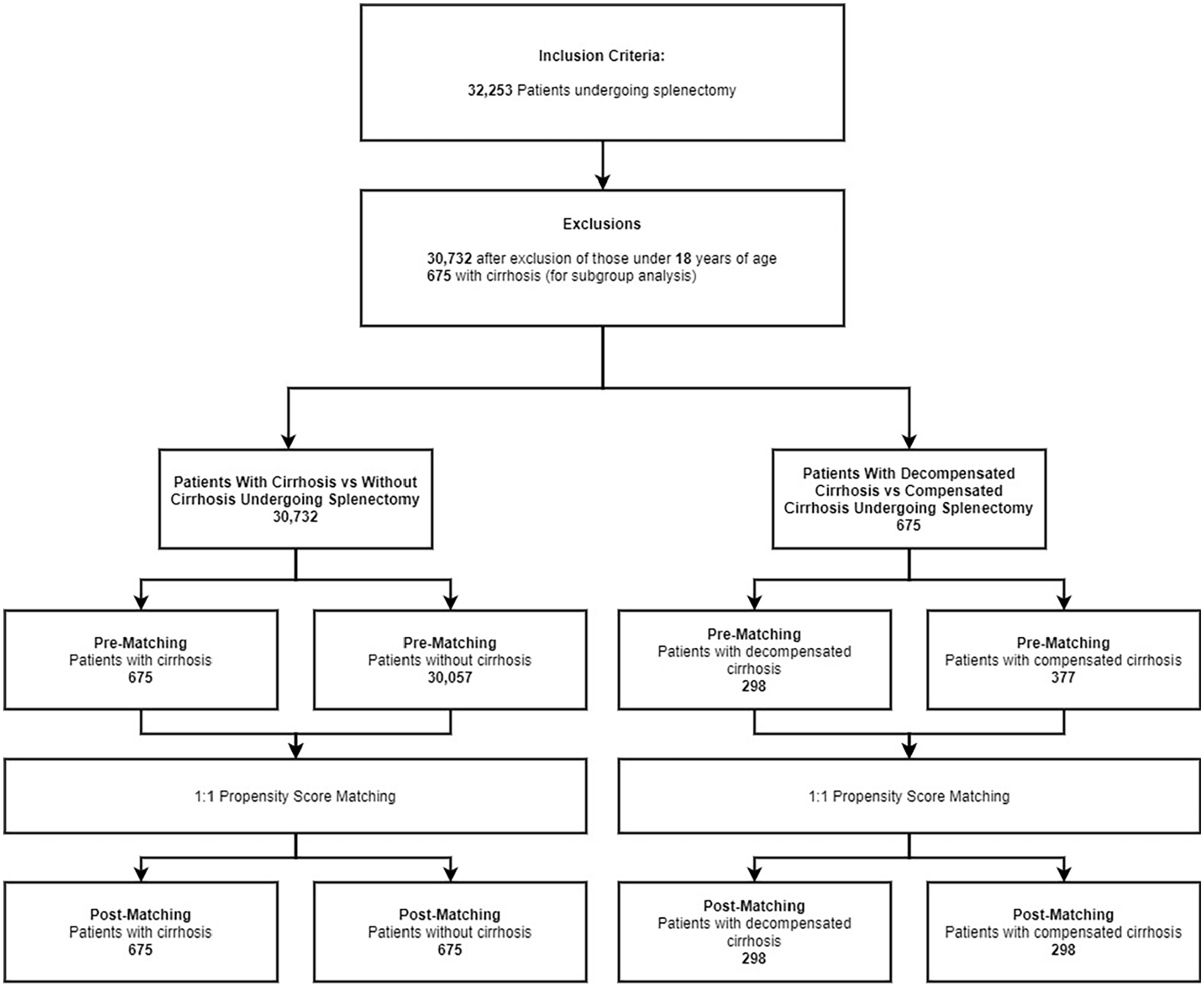
Patient selection process of the study.
Univariate comparison of patient demographics and medical covariates
The baseline demographics and medical comorbidities for the cirrhosis-present cohort and cirrhosis-absent controls are summarized in Table 1. After matching, there was no difference in age, gender, and race between the cohorts. Cirrhotic patients were more likely to be coagulopathic; however, there were no other differences noted for the remaining medical comorbidities. With respect to liver disease etiologies, cirrhotic patients had a higher incidence of alcoholic liver disease, hepatitis c, and non-alcoholic fatty liver disease.
Pre- and post-match comparison of demographics and medical comorbidities in patients with and without cirrhosis undergoing splenectomy.
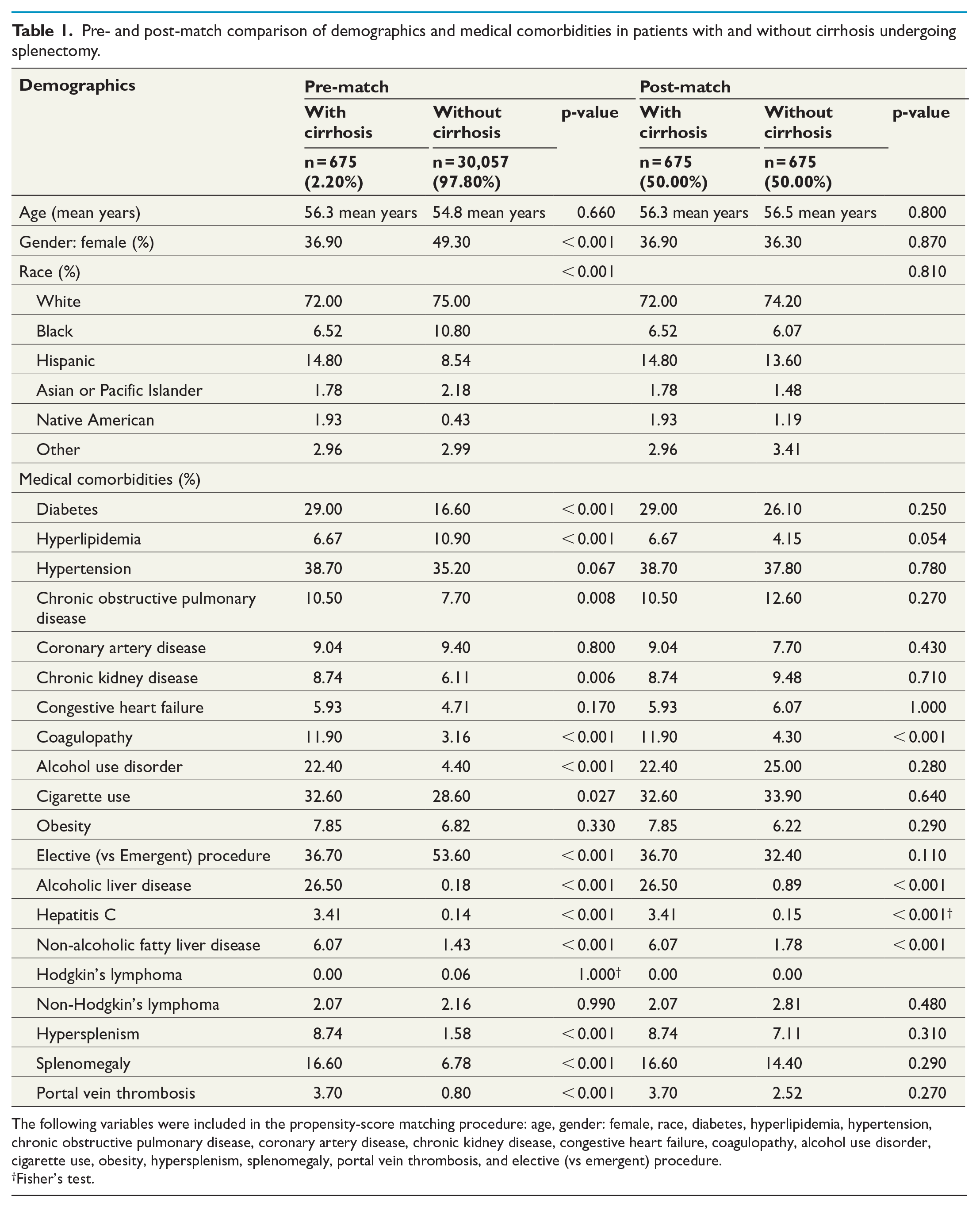
The following variables were included in the propensity-score matching procedure: age, gender: female, race, diabetes, hyperlipidemia, hypertension, chronic obstructive pulmonary disease, coronary artery disease, chronic kidney disease, congestive heart failure, coagulopathy, alcohol use disorder, cigarette use, obesity, hypersplenism, splenomegaly, portal vein thrombosis, and elective (vs emergent) procedure.
Fisher’s test.
Univariate comparison of patient socioeconomic status and hospital characteristics
Table 2 represents the univariate comparison between pre and post-match patient socioeconomic status and hospital characteristics. Following the match, cirrhotic patients were more likely to be under lower income quartiles and cover medical expenses through out-of-pocket or Medicaid/Medicare methods of payment than the non-cirrhotic controls; no difference was found in the hospital region, hospital bed size, and the hospital teaching-status between the two groups.
Pre- and post-match comparison of socioeconomic status and hospital characteristics in patients with and without cirrhosis undergoing splenectomy.
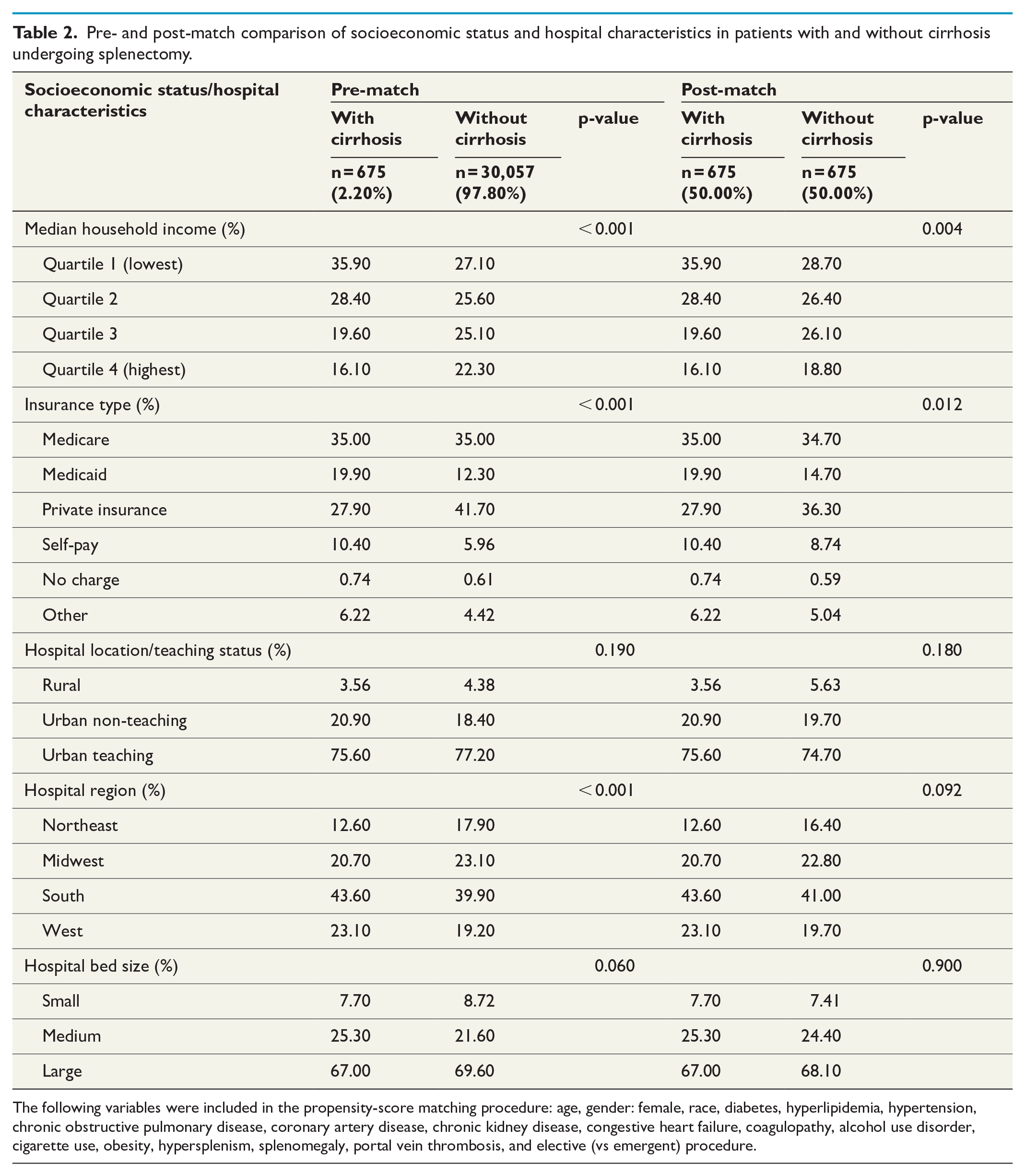
The following variables were included in the propensity-score matching procedure: age, gender: female, race, diabetes, hyperlipidemia, hypertension, chronic obstructive pulmonary disease, coronary artery disease, chronic kidney disease, congestive heart failure, coagulopathy, alcohol use disorder, cigarette use, obesity, hypersplenism, splenomegaly, portal vein thrombosis, and elective (vs emergent) procedure.
Univariate and multivariate comparison of the postoperative outcomes and clinical endpoints
Table 3 summarizes the pre and post-match postoperative outcomes following splenectomy in patients with and without cirrhosis. In terms of post-match hospital outcomes, patients in the cirrhosis cohort, compared to the controls, had an increased incidence of mortality (20.0 vs 7.26%, p < 0.001, OR = 3.19, 95% CI = 2.26–4.52), higher hospitalization costs ($210,716 vs $186,673 p = 0.003); and shorter length of hospital stay (11.8 vs 12.5d, p = 0.04). With regards to discharge disposition, the cirrhosis cohort was more likely to be discharged to short-term hospitals, home health care, and against medical advice. Postoperatively, cirrhotic patients had an increased incidence of bleeding (7.26 vs 4.3%, p = 0.027, OR = 1.74, 95% CI = 1.09–2.80) and shock (3.7 vs 1.04%, p = 0.002, OR = 3.67, 95% CI = 1.58–8.54). There was no difference in the incidence of wound complications (2.81 vs 2.07%, p = 0.48, OR = 1.37, 95% CI = 0.68–2.75), infection (2.07 vs 3.11%, p = 0.3, OR = 0.66, 95% CI = 0.33–1.31), and respiratory failure (9.19 vs 7.85%, p = 0.44, OR = 1.19, 95% CI = 0.81–1.74).
Pre- and post-match comparison of hospital outcomes in patients with and without cirrhosis undergoing splenectomy.
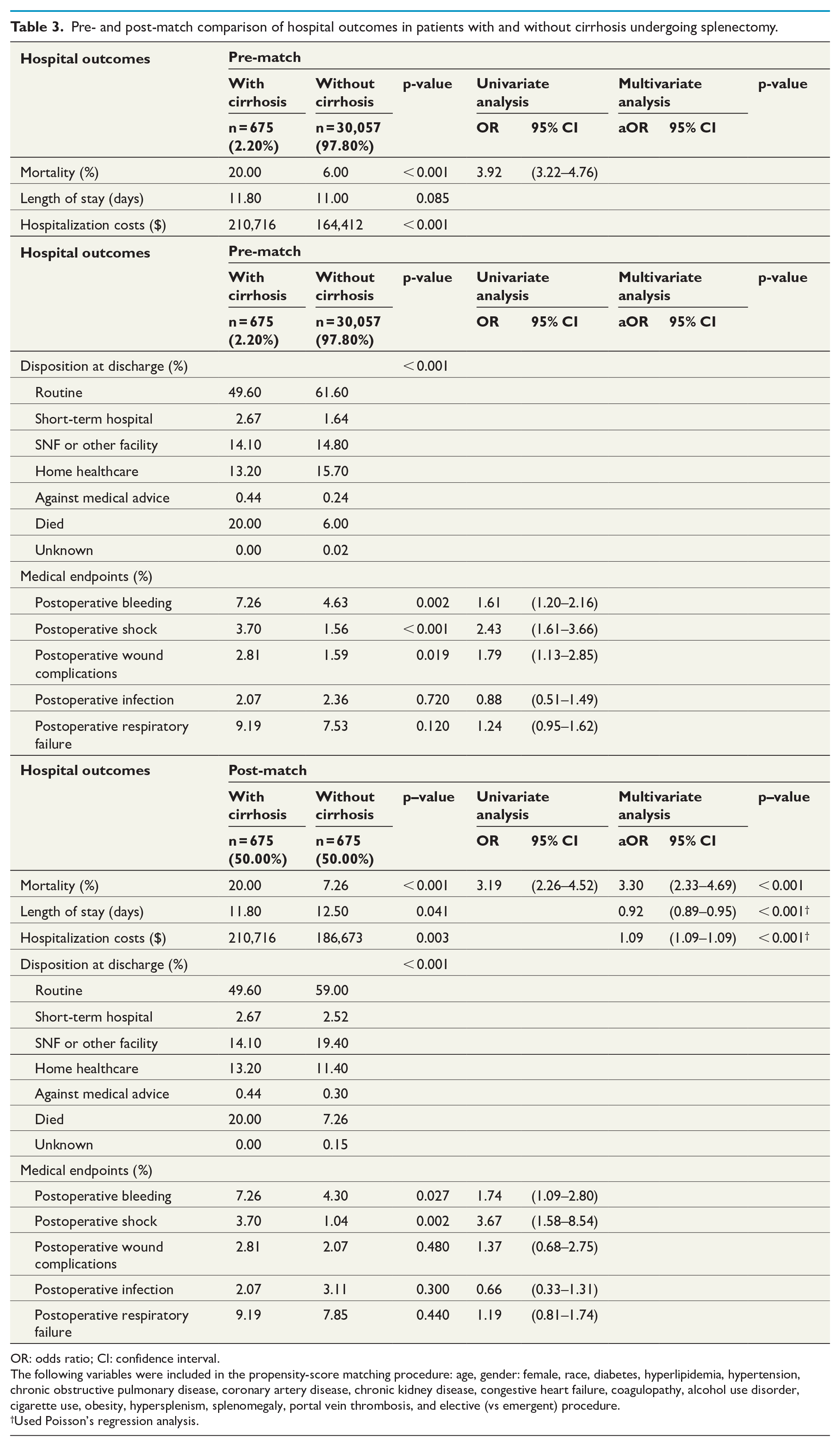
OR: odds ratio; CI: confidence interval.
The following variables were included in the propensity-score matching procedure: age, gender: female, race, diabetes, hyperlipidemia, hypertension, chronic obstructive pulmonary disease, coronary artery disease, chronic kidney disease, congestive heart failure, coagulopathy, alcohol use disorder, cigarette use, obesity, hypersplenism, splenomegaly, portal vein thrombosis, and elective (vs emergent) procedure.
Used Poisson’s regression analysis.
In the multivariate analysis, cirrhotic patients had a higher incidence of mortality (p < 0.001, aOR = 3.30, 95% CI = 2.33–4.69), shorter length of stay (p < 0.001, aOR = 0.92, 95% CI = 0.89–0.95), and increased hospitalization costs (p < 0.001, aOR = 1.09, 95% CI = 1.09–1.09), despite controlling for the non-matched socioeconomic and hospital variables. The forest plot corresponding to the post-match multivariate analysis is shown in Fig. 2.
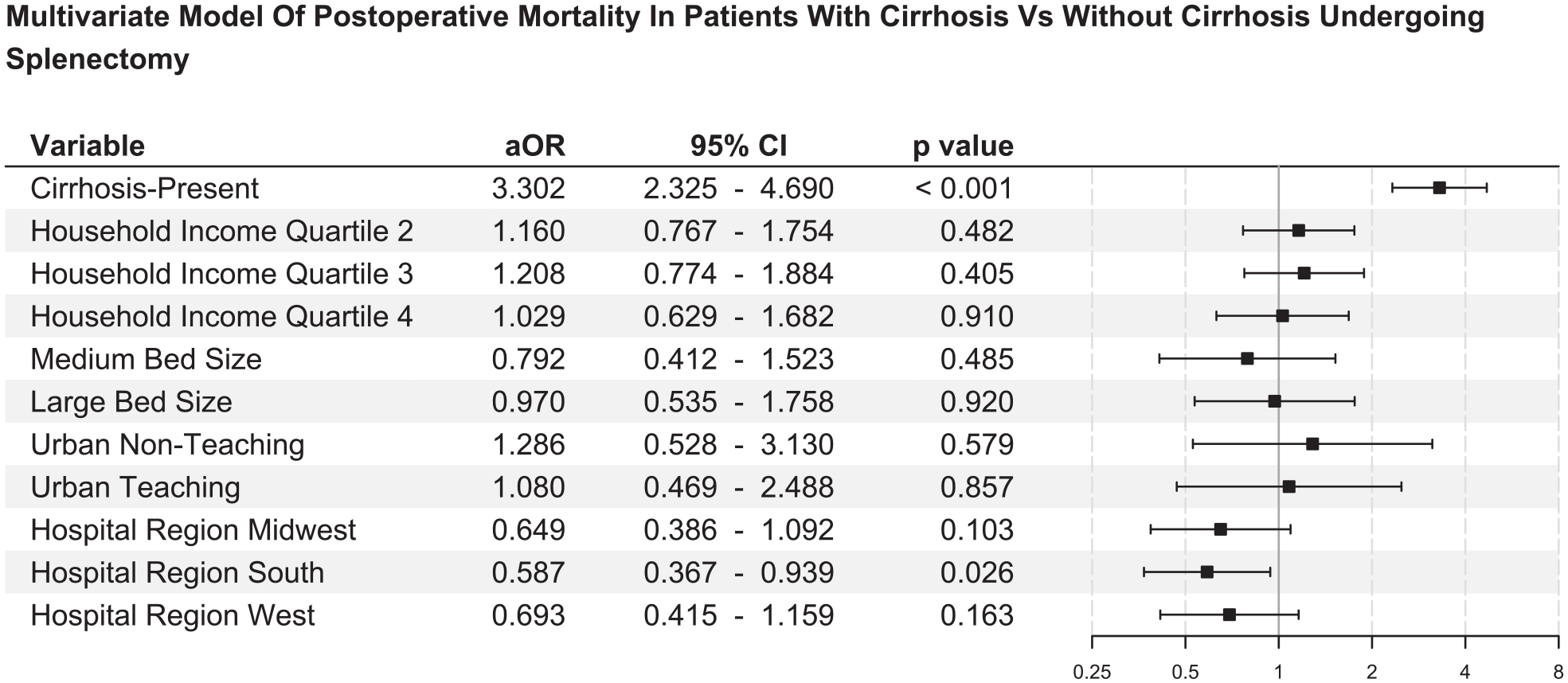
Forest plot that corresponds to the post-match multivariate model comparing the presence of cirrhosis on postoperative mortality following splenectomy.
Comparison of hospital outcomes in patients with decompensated and compensated cirrhosis
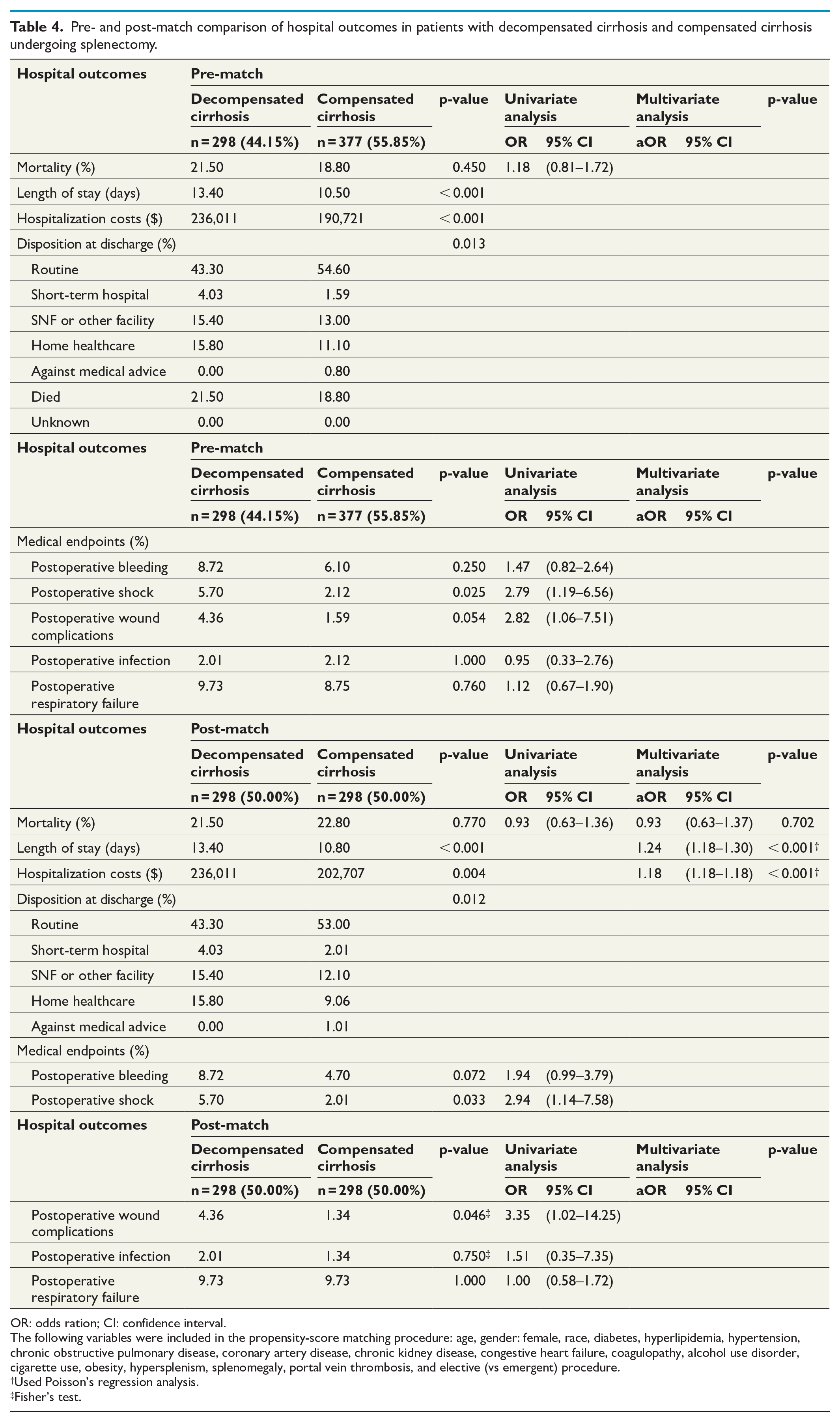
Table 4 summarizes the outcomes of a subgroup analysis of the cirrhosis cohort that was stratified using liver decompensation as the exposure variable. Patients with decompensated cirrhosis had similar mortality (21.5 vs 22.8%, p = 0.77, OR = 0.93, 95% CI = 0.63–1.36), a longer length of stay (13.4 vs 10.8d, p < 0.001), higher hospitalization costs ($236,011 vs $202,707, p < 0.001), and were more likely to be discharged to short-term hospitals, skilled nursing facilities, and home health care (Routine: 43.3 vs 53.0%; Short-term Hospital: 4.03 vs 2.01%; Skilled Nursing or other Facility: 15.4 vs 12.1%; Home Health Care: 15.8 vs 9.06%; Against Medical Advice: 0 vs 1.01%; Died: 21.5 vs 22.8%; p = 0.012). In the multivariate analysis, the presence of decompensated cirrhosis resulted in similar mortality (p = 0.702, aOR = 0.93, 95% CI = 0.63–1.37), longer length of stay (p < 0.001, aOR = 1.24, 95% CI = 1.18–1.30), hospitalization costs (p < 0.001, aOR = 1.18, 95% CI = 1.18–1.18) despite controlling for socioeconomic status and hospital characteristics. In terms of postoperative complications, patients with decompensated cirrhosis had an increased incidence of shock (5.7 vs 2.01%, p = 0.033, OR = 2.94, 95% CI = 1.14–7.58), wound complications (4.36 vs 1.34%, p = 0.046, OR = 3.35, 95% CI = 1.02–14.25), however, there was no difference in the incidence of bleeding (8.72 vs 4.7%, p = 0.072, OR = 1.94, 95% CI = 0.99–3.79), infections (2.01 vs 1.34%, p = 0.75, OR = 1.51, 95% CI = 0.35–7.35), and respiratory failure (9.73 vs 9.73%, p = 1, OR = 1, 95% CI = 0.58–1.72).
Pre- and post-match comparison of hospital outcomes in patients with decompensated cirrhosis and compensated cirrhosis undergoing splenectomy.
OR: odds ration; CI: confidence interval.
The following variables were included in the propensity-score matching procedure: age, gender: female, race, diabetes, hyperlipidemia, hypertension, chronic obstructive pulmonary disease, coronary artery disease, chronic kidney disease, congestive heart failure, coagulopathy, alcohol use disorder, cigarette use, obesity, hypersplenism, splenomegaly, portal vein thrombosis, and elective (vs emergent) procedure.
Used Poisson’s regression analysis.
Fisher’s test.
Supplementary analyses
Supplementary Tables 2 and 3 respectively show the elective and non-elective stratum-specific results for cirrhosis and post-splenectomy outcomes. Supplementary Tables 4 and 5 show the effects of chronic liver disease on post-splenectomy outcomes. When stratifying by elective procedures, the post-match results show that the presence of cirrhosis does not result in higher mortality (univariate: 4.44 vs 2.42%, p = 0.320, OR = 1.87, 95% CI = 0.68–5.14; multivariate: p = 0.372, aOR = 1.60, 95% CI = 0.57–4.52); however, presence of cirrhosis was associated with higher hospital stay and hospitalization costs. When stratifying by urgent procedures, the post-match results show that the presence of cirrhosis is associated with higher mortality (univariate: 29 vs 8.43%, p < 0.001, OR = 4.44, 95% CI = 2.98–6.63; multivariate: p < 0.001, aOR = 4.65, 95% CI = 3.09–6.99). Furthermore, hospital stay and costs were also higher in the multivariate. When using chronic liver disease with inclusion of cirrhosis as the primary exposure variable (Supplementary Table 4), those with chronic liver disease had higher mortality (12.6 vs 6.13%, p < 0.001, OR = 2.21, 95% CI = 1.69–2.89; multivariate: p < 0.001, aOR = 2.23, 95% CI = 1.70–2.93). Likewise, hospital stay and costs were higher in the multivariate. On the other hand, when using chronic liver disease without cirrhosis, there was no difference in mortality (univariate: 5.77 vs 4.40%, p = 0.280, OR = 1.33, 95% CI = 0.83–2.13; multivariate: p = 0.199, aOR = 1.37, 95% CI = 0.85–2.20); however, hospital stay and costs remained higher in the chronic liver disease cohort.
Discussion
As demonstrated by the results, cirrhosis is an independent risk factor for in-hospital mortality and higher cost of care in patients undergoing splenectomy; this was despite controlling for major covariates that are commonly present in surgical populations, including cardiac and pulmonary risk factors, as well as the elective (vs non-elective) nature of the procedure and etiologic indicators (portal vein thrombosis, hypersplenism, and splenomegaly) in the propensity score matching process. The length of hospital stay was noted to be shorter among those with cirrhosis (compared to non-cirrhotic controls), which is presumably due to shorter survival in these patients. Furthermore, cirrhosis was associated with higher risk of bleeding and shock, which can be attributed to cirrhosis-associated coagulopathy, 21 which originates from liver synthetic dysfunction that reduces the hepatic production of proteins and clotting factors which comprise the coagulation cascade. These nutritional and protein deficiencies invariably produce exacerbated cases of bleeding, with delayed or complicated hemostasis, which can culminate to hemorrhagic shock or hypotension during or following the operation. Interestingly, the sub-analyses show that the mortality risks are exclusively associated with cirrhosis; the presence of either decompensated cirrhosis or chronic liver disease (without cirrhosis) did not demonstrate similar associations with mortality. In addition, the stratum-specific analyses using the elective (vs non-elective) nature of the procedure demonstrate that cirrhosis differentially affects the hospital outcomes; emergent, non-elective cases are where cirrhosis significantly increases risk of postoperative mortality and complications.
Clinical considerations
The higher risk of postoperative mortality and complications in cirrhotic patients undergoing splenectomy is concerning, especially for patients who undergo an emergent procedure. In light of these findings, a multidisciplinary approach is needed for the care of these vulnerable patients. While full preoperative consideration of cirrhosis may be difficult and too time consuming in the setting of emergency surgery, efforts should be made to provide the ancillary support needed during these high-risk cases. Such support measures include preparing additional blood products and hemostatic devices 22 as well as consulting interventional radiology for splenic artery embolization in the setting of severe hemorrhage.23–26 Though cirrhosis was not associated with elevated mortality in non-emergent cases, these patients still had increased risk for bleeding and shock. Therefore, similar ancillary support should be provided peri and postoperatively for these patients.22–26 Given that elective cases may allow for additional preoperative time to optimize risks, vitamin K and other anti-coagulopathic derivatives may be considered in these patients (especially if INR is elevated), although it is not fully clear whether this is safe and effective.21,27
Limitation
The primary limitation of this study is the type of data contained in the NIS database; it does not contain the laboratory data needed to stratify patients based on the liver prognostic scores such as MELD or Child-Pugh.28,29 Nevertheless, this deficiency is amended by the use of ICD diagnosis codes specific for the features of portal hypertension in order to stratify patients based on the severity of their cirrhosis. Likewise, due to the observational nature of this study, further prospective studies are needed to clearly define the effects of cirrhosis on post-splenectomy outcomes, in order to identify the causal agents of mortality in this vulnerable population. In light of this, prospective studies should evaluate the long-term effects of cirrhosis on post-splenectomy results, including the postsurgical course following hospital discharge.
Conclusion
This study demonstrates that cirrhosis is associated with increased postoperative mortality, bleeding, and shock in patients undergoing splenectomy. Furthermore, hepatic decompensation in cirrhotic patients resulted in increased post-surgical death following splenectomy. Given these findings, cirrhotic patients must be identified early during the preoperative evaluation, provided an in-depth risk-benefit assessment around the post-surgical risks, and provided appropriate multidisciplinary care that optimizes risks.
Supplemental Material
sj-pdf-1-sjs-10.1177_14574969211042457 – Supplemental material for The impact of cirrhosis on the postoperative outcomes of patients undergoing splenectomy: Propensity score matched analysis of the 2011–2017 US hospital database
Supplemental material, sj-pdf-1-sjs-10.1177_14574969211042457 for The impact of cirrhosis on the postoperative outcomes of patients undergoing splenectomy: Propensity score matched analysis of the 2011–2017 US hospital database by David U. Lee, Gregory H. Fan, David J. Hastie, Elyse A. Addonizio and Raffi Karagozian in Scandinavian Journal of Surgery
Supplemental Material
sj-pdf-2-sjs-10.1177_14574969211042457 – Supplemental material for The impact of cirrhosis on the postoperative outcomes of patients undergoing splenectomy: Propensity score matched analysis of the 2011–2017 US hospital database
Supplemental material, sj-pdf-2-sjs-10.1177_14574969211042457 for The impact of cirrhosis on the postoperative outcomes of patients undergoing splenectomy: Propensity score matched analysis of the 2011–2017 US hospital database by David U. Lee, Gregory H. Fan, David J. Hastie, Elyse A. Addonizio and Raffi Karagozian in Scandinavian Journal of Surgery
Supplemental Material
sj-pdf-3-sjs-10.1177_14574969211042457 – Supplemental material for The impact of cirrhosis on the postoperative outcomes of patients undergoing splenectomy: Propensity score matched analysis of the 2011–2017 US hospital database
Supplemental material, sj-pdf-3-sjs-10.1177_14574969211042457 for The impact of cirrhosis on the postoperative outcomes of patients undergoing splenectomy: Propensity score matched analysis of the 2011–2017 US hospital database by David U. Lee, Gregory H. Fan, David J. Hastie, Elyse A. Addonizio and Raffi Karagozian in Scandinavian Journal of Surgery
Supplemental Material
sj-pdf-4-sjs-10.1177_14574969211042457 – Supplemental material for The impact of cirrhosis on the postoperative outcomes of patients undergoing splenectomy: Propensity score matched analysis of the 2011–2017 US hospital database
Supplemental material, sj-pdf-4-sjs-10.1177_14574969211042457 for The impact of cirrhosis on the postoperative outcomes of patients undergoing splenectomy: Propensity score matched analysis of the 2011–2017 US hospital database by David U. Lee, Gregory H. Fan, David J. Hastie, Elyse A. Addonizio and Raffi Karagozian in Scandinavian Journal of Surgery
Supplemental Material
sj-pdf-5-sjs-10.1177_14574969211042457 – Supplemental material for The impact of cirrhosis on the postoperative outcomes of patients undergoing splenectomy: Propensity score matched analysis of the 2011–2017 US hospital database
Supplemental material, sj-pdf-5-sjs-10.1177_14574969211042457 for The impact of cirrhosis on the postoperative outcomes of patients undergoing splenectomy: Propensity score matched analysis of the 2011–2017 US hospital database by David U. Lee, Gregory H. Fan, David J. Hastie, Elyse A. Addonizio and Raffi Karagozian in Scandinavian Journal of Surgery
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical statement
This study was exempt from undergoing the standard ethics requirements as the primary database used in the study was the National Inpatient Sample sponsored by the Agency for Healthcare Research and Quality (AHRQ); this database contains stratified samples of US hospital data with de identified cases that is compiled for research use following the data user standards and agreements.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
