Abstract
Background and Aim:
Fistula-in-ano is a common problem among patients with Crohn’s disease and carries significant morbidity. We aimed to study the outcomes of surgical treatment of fistula-in-ano after fistulotomy or seton placement in patients with perianal fistulizing Crohn’s disease.
Material and Methods:
A retrospective observational study of 59 patients diagnosed with Crohn’s disease, who were treated surgically for fistula-in-ano between 2010 and 2014 in our department. The assessment of disease complexity included a detailed physical examination, magnetic resonance imaging of the rectum, and examination under anesthesia. Outcomes for analysis included wound healing rate and postoperative incontinence.
Results:
High transsphincteric fistula was found in 44% of the patients, while mid or low transsphincteric fistulas were found in 51%. Three women (5%) had a rectovaginal fistula. All patients with high transsphincteric fistulas were treated with loose seton placement. Patients with mid- or low-level transsphincteric fistula were offered either fistulotomy or seton placement based on the clinical evaluation. The mean follow-up duration was 1.6 ± 1.1 years. In terms of recurrence, one patient treated with seton placement presented with recurrence 6 months after seton removal and one patient with fistulotomy failed to achieve wound healing. Minor incontinence was found in six patients treated with fistulotomy and in three patients treated with seton placement; however, this difference was not significant (chi-square = 1.723, df = 1, Monte–Carlo: p = 0.273).
Conclusion:
Fistulotomy could achieve good results in terms of wound healing and incontinence in strictly selected patients with Crohn’s disease suffering from low-lying transsphincteric fistulae. For more high-lying or complicated fistulae, seton placement is more appropriate. For high transsphincteric fistulae, the only option is placement of loose seton.
Introduction
Anal fistula is a significant surgical problem due to the associated morbidity and high recurrence rates (1). The natural history of this disease comprises a periodic cycle of “crescento” with pain and discharge due to abscess formation, followed by periods of “dormancy” after drainage (surgical or spontaneous), causing patient frustration (2). Sepsis drainage is the cornerstone of surgical management, which could be consolidated by excision of the fistulous tract if that is appropriate. However, preservation of sphincter integrity and minimizing recurrence rate are the secondary main concerns (3).
Surgical options include fistulotomy, ligation of the transsphincteric fistula tract, advancement flap, or infill materials such as fibrin glue or collagen plug (1, 4–6). The decision making of the appropriate surgical approach depends on (a) the anatomy of the fistulous tract in relation to the anal sphincter (7) and (b) the presence of inflammatory bowel disease (IBD). The anatomy of the fistulous tract and the presence of IBD are the main risk factors associated with fecal incontinence and recurrence, respectively (8, 9).
Fistulotomy or “laying open” is the most definite treatment as it offers the best option for cure for a simple or a low-lying fistula (1, 2, 7). However, the majority of surgeons are cautious in implementing this technique in complex perianal fistula or in the presence of Crohn’s disease, due to previous adverse reports (9, 10), although there is a lack of high-quality evidence for this setting. To this end, we present an analysis of outcomes with fistulotomy and seton placement for the treatment of perianal fistula in patients with Crohn’s disease in our department.
Material and Methods
All patients, between 2010 and 2014, with Crohn’s disease and perianal fistulae treated by a single surgeon (I.P.) in our department were reviewed. The senior author (I.P.) assessed the complexity of disease; the assessment process included a detailed physical examination, magnetic resonance imaging (MRI) of the rectum (Fig. 1), and examination under anesthesia (EUA). All patients included in this study had a previously established diagnosis of Crohn’s disease and were under regular follow-up by a gastroenterologist. Patients presenting with sporadic fistula or ulcerative colitis, as well as children and adolescent, were excluded from the study.
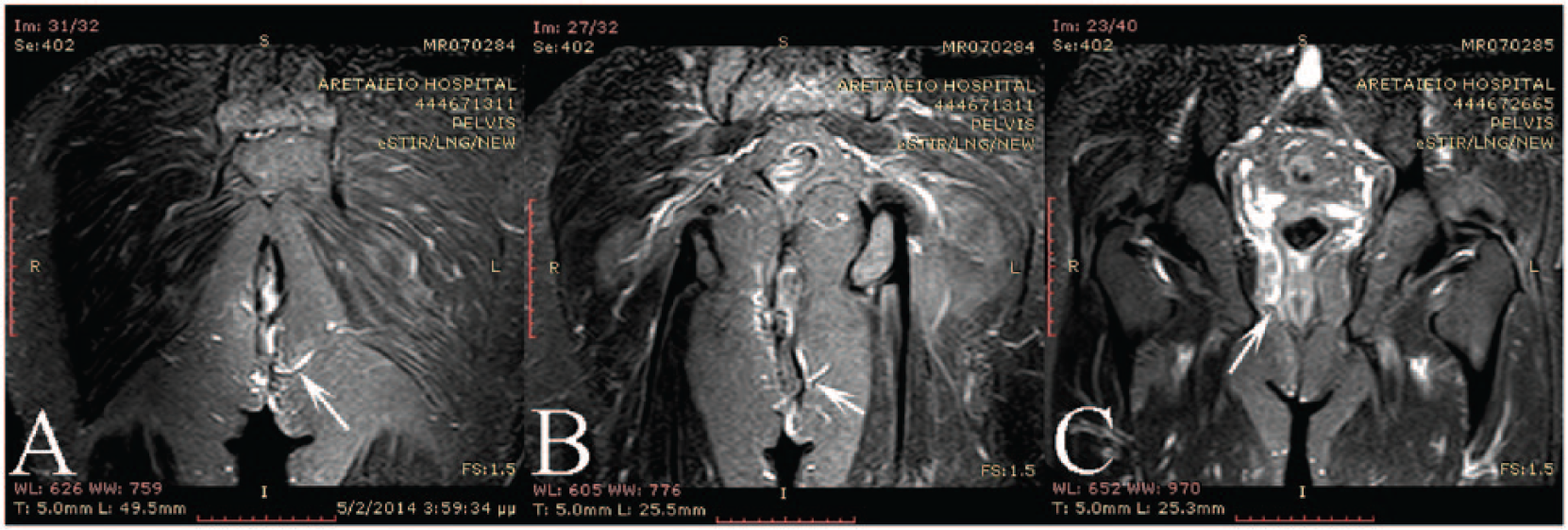
Rectal MRI from a male patient presenting with a complex anal fistula. As shown in A) (white arrow) a single superficial fistulous tract, which in a deeper plane and a higher level, B) bifurcates (white arrow), C) giving rise to inner abscess on the contralateral side (white arrow).
Data obtained for analysis included patients’ demographic data, anatomy of the fistulous tract with special regard to the internal opening, and presence of other co-morbidities affecting the outcome such as diabetes mellitus, surgical technique implemented, and follow-up data for wound healing or incontinence. Fistulae were grossly divided into three groups: high-level transsphincteric, mid-level transsphincteric, and low-level transsphincteric. This classification was based on the length of the anal sphincter below the internal opening of the fistula as follows: the length of the anal sphincter was divided in thirds; when the internal opening of the fistula was located within the upper third, it was considered high fistula. Accordingly, when the internal opening of the fistula was located at lower third, it was considered a low fistula. The remaining fistulas were considered mid-level transsphincteric fistulas. The follow-up consisted of physical examination at 3 monthly intervals by I.P. In suspicion of recurrence, further examinations (i.e. EUA and/or rectal MRI), if clinically mandated, were obtained. Recurrence after fistulotomy or seton placement was defined as re-occurrence of a perianal external fistula orifice with or without the presence of abscess during follow-up. However, in regard to seton placement, recurrence was considered only if seton was removed prior to recurrence. Fecal incontinence was assessed in every regular outpatient follow-up appointment, through a structured interview; the assessment of severity of incontinence was evaluated by means of the Wexner Fecal Incontinence Score (11). Informed consent for all patients included, as well as ethical approval for the study from the hospital scientific committee, was obtained.
The decision making of the proposed treatment was based on the clinical and MRI findings. Special consideration was given to the following factors: severe uncontrolled proctitis at the time of presentation, high suprasphincteric fistula affecting most of or the entire anal sphincter, multiple previous fistulotomies for complex perianal fistula, established severe fecal incontinence, anterior fistula in female patients, and newly diagnosed Crohn’s disease on exacerbation which has not yet been adequately addressed.
All high transsphincteric fistulas were treated by means of seton placement. I.P. made the decision for offering fistulotomy or seton placement for mid- or low-level transsphincteric fistula based on the presence or absence of proctitis and the pattern of bowel habits of the patient, namely, the number of daily bowel motions and the estimation of length of good-quality contracting muscle cephalad to the internal opening of the fistula, as described previously by Tozer et al. (2). Prerequisites for offering fistulotomy were a mid- or low-level transsphincteric fistula, absence of proctitis, normal bowel habits, and presence of at least 1.5–2 cm of good-quality contracting muscle above the internal opening of the fistula.
Comparisons between non-parametric variables were performed with chi-square test. When the observed count within cells was less than five, the Monte–Carlo method for calculating the p value was used (12). Statistical analysis was performed with the aid of SPSS 21 for Macintosh.
Results
During the study period, 59 patients with Crohn’s disease were referred for treatment of perianal fistulae in our department. The mean age was 34.8 ± 14.2 years (95% confidence intervals (CIs) lower–upper: 31.1–38.5), including 38 male and 21 female patients. Table 1 presents the anatomy of the fistulous tract in the patients included in our study. In 14.2% (3/21) of female patients, there was a rectovaginal fistula. Also two patients (one male and one female) had hidradenitis suppurativa. Six patients had a previous fistula surgery, namely, a drainage procedure. In this study, five of them were treated by means of seton placement and one by fistulotomy.
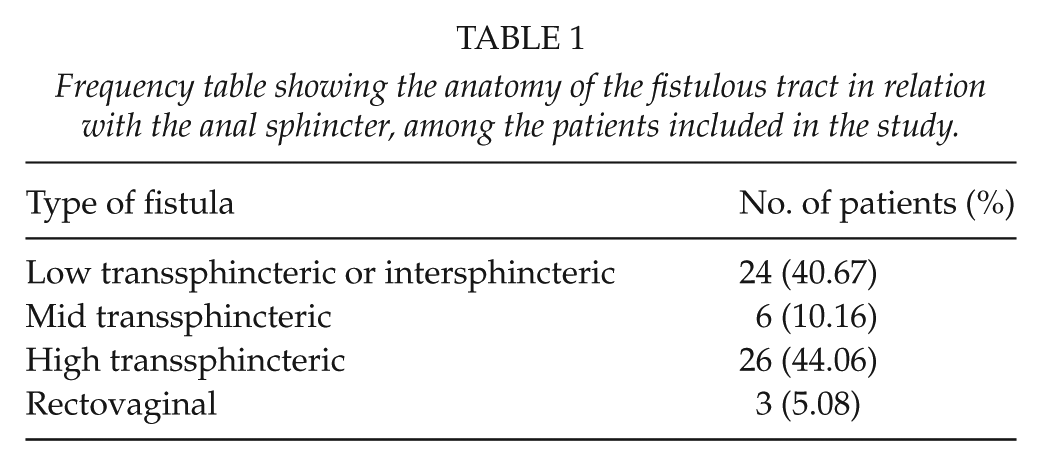
Frequency table showing the anatomy of the fistulous tract in relation with the anal sphincter, among the patients included in the study.

In all patients, during the initial treatment of the fistula (i.e. fistulotomy or seton placement), any septic collection was drained at the same time. All patients included in this study were administered ciprofloxacin 400 mg BD and metronidazole 500 mg TDS, with the first dose being given preoperatively and continued postoperatively for at least 7 days. A soft elastic vessel loop was used as the seton material. The procedures performed were as follows: (a) fistulotomy in 29 patients, (b) a fistulotomy and a proximal diverting colostomy in 1 patient, (c) seton placement in 25 patients, and (d) seton placement and a proximal diverting colostomy. In the three patients with rectovaginal fistulae, the treatment implemented was as follows: total proctocolectomy due to severe perianal and colonic disease refractory to medical treatment in one patient (Fig. 2), loose seton placement in one patient, and levator ani muscle interposition and diverting colostomy in one patient.
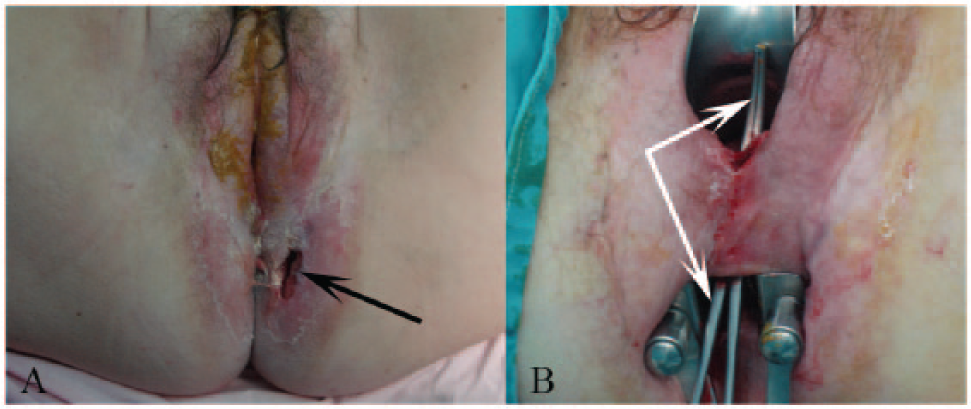
Female patient with severe uncontrollable perianal Crohn’s disease refractory to all medical treatments was referred due to complex perianal fistula A) with spontaneous drained abscess (black arrow) B) associated with a wide rectovaginal fistula (white arrows showing a large forceps placed within the fistula). This patient was treated with proctocolectomy.
None of the patients was lost to follow-up, and the average follow-up duration was 1.6 ± 1.1 years (95% CI: 1.3–1.9). None of the patients who underwent diverting colostomy, indifferently of the treatment of the fistula, had recurrence of the fistula-in-ano. In the fistulotomy group, no true recurrence was observed. In one patient treated with fistulotomy, the wound of the fistulotomy failed to heal. Respectively, in the seton group, only one patient presented with recurrence of the fistula-in-ano after seton removal. Thus, the overall recurrence rate in our study was 3.6% (2/56), which could be clustered further in 3.4% (1/29 patients) within the fistulotomy only group and 4% (1/25 patients) within the seton placement only group, with no significant difference between the two groups (chi-square = 0.011, df = 1, Monte–Carlo method: p = 0.718).
Among the 55 patients treated in this study (excluding all patients treated with a diverting stoma), only 9 patients (16.3%) have presented minor incontinence (flatus ± <1 teaspoon of mucus leakage in a 24-h period) during follow-up. Six patients were treated with fistulotomy, while three patients were treated with seton placement. All patients treated with seton placement, who presented incontinence, had a high transsphincteric fistula. In contrast, among the patients treated with fistulotomy, three patients had a low-level transsphincteric fistula and three patients had a mid-level transsphincteric fistula.
Discussion
Fistulotomy has been historically considered the mainstay of treatment for fistula-in-ano (1, 2, 7). The arguments in favor of fistulotomy for the treatment of fistula-in-ano are mainly two; fistulotomy has been proven that could cure the fistula-in-ano with a low associated morbidity (13). This has been attributed to the technique of fistulotomy, that is, when the appropriate plane of dissection between the internal and external anal sphincter is followed, the drainage of the intersphincteric space is achieved, thus addressing the cryptoglandular hypothesis which historically has been considered to be the pathogenetic mechanism in sporadic anal fistulae (14, 15). However, the cryptoglandular hypothesis is not the explanatory mechanism in perianal fistulizing Crohn’s disease, even when isolated perianal Crohn’s disease is present (9). Hence, it has been considered with caution in this setting (9, 10). However, nowadays, studies advocate in favor of its safety (13), hence fistulotomy is the treatment of option for symptomatic superficial, low intersphincteric, and low transsphincteric fistulae in perianal Crohn’s disease (Grade of recommendation 2C) (16). In contrast, young woman with an anterior low- or mid-level transsphincteric fistula should not be offered with fistulotomy because the anterior portion of the anal sphincter in woman is extremely thin, consequently they may be at increased risk of developing incontinence (16).
A loose or noncutting seton has been advocated by authors as a better option in the presence of IBD as it facilitates drain of any septic collection and healing of the fistulous tract when combined with medical therapy (17). Nevertheless, seton placement has some disadvantages when compared to fistulotomy, namely, seton placement prolongs morbidity as it needs to stay in place for a prolong period of time. Therefore, it needs frequent follow-up and has been associated with patient discomfort. Furthermore, removal of the seton may be associated with recurrence of the fistula (18); this is in accordance with the results of our study, where the one patient who presented with recurrence in the seton group, the recurrence occurred after seton removal. Hence, temporary seton placement should be considered as a bridging therapy toward a more definitive surgical treatment (i.e. fistulotomy or advancement flap) when feasible; otherwise, a permanent lose seton should be considered. The management strategy of our center consists of long-term preservation of the seton (no less than 6 months). When complete control of symptoms and improvement of the MRI findings has been achieved, we may consider a closure procedure, namely, advancement flap. However, before considering an advancement flap, an absolute prerequisite is the complete remission of the accompanying proctitis.
Our results have shown that fistulotomy may be safely and effectively applied in the treatment of simple fistulizing perianal Crohn’s disease. Both techniques (i.e. fistulotomy or seton placement) in expert hands could achieve good outcomes in patients with perianal Crohn’s disease. Nevertheless, there is a fraction of patients which will eventually require a diverting colostomy or more complex surgery such as interposition of a muscle for treatment of their fistula-in-ano. This is especially true for patients with complex fistula incorporating the entire anal sphincter and/or extending to neighboring organs, that is, rectovaginal fistula.
Clearly though, fistulotomy is not the best option for all fistulae in ano in the presence of IBD. Fistulotomy incorporates a large laceration of the rectum as well as partial division of the muscle fibers of the anal sphincter. It follows that in patients with extensive rectal inflammation and/or inflammation of the perineal skin (e.g. proctitis or hidradenitis suppurativa), the results of fistulotomy will be suboptimal. Furthermore, a significant factor, which should be considered in the decision making of the offered treatment, is previous fistulotomies. Surely, a typical fistulotomy for a low- or mid-level anal fistula may not jeopardize the entire anal sphincter when performed properly. However, repeated fistulotomies due to recurrence of the fistula-in-ano, as it is especially true in patients with IBD, will eventually compromise the anal sphincter, thus rendering the patients incontinent. Therefore, the patients who will be offered with fistulotomy should be strictly selected, with previous fistulotomies being a significant deterring factor toward another fistulotomy.
Patients with Crohn’s disease represent a rather challenging group of patients, where fistula-in-ano is one of many manifestations of their disease. Therefore, these patients need to have a combination therapy (medical and surgical). It has been proven that medical therapy only, namely, anti-TNF-α antibodies, will achieve cure of fistulizing disease in only 36% of the patients and of fraction of these patients may achieve long-term closure (10, 19). Furthermore, medical therapy with anti-TNF-α and/or immunosuppressant in the presence of fistulizing perianal disease is contraindicated, since the fistula-in-ano represents a potential septic process, often associated with septic collections or abscess which should be excluded or drained prior commencement of immunosuppressive therapy. Also the presence of perianal abscess may be a reason of failure of completing medical therapy. Immunosuppressive therapy may be associated with wound healing failure in patients undergoing fistulotomy and the timing of the anti-TNF-α and fistulotomy remain subject under study, with few available studies (9). None of the patients included in this study were operated, while being administered anti-TNF treatment. Anti-TNF was initiated postoperatively, if appropriate, at the discretion of the referring gastroenterologist. This major issue is yet to be answered and remains beyond the scope of this study.
In conclusion, in patients with a low-lying fistula without significant or controllable rectal inflammation, fistulotomy should be offered as a definitive surgical treatment (2, 20). On the contrary, patients with high-level transsphincteric fistulas should not be offered with fistulotomy, as by definition a fistulotomy in this case will incorporate severing of the entire anal sphincter, thus rendering the patient incontinent. However, this study has some limitations; the average follow-up period in this study was 1.6 years, which could be considered relatively short, given that Crohn’s disease represents a chronic illness. However, all these patients still remain under regular follow-up to assess the long-term results of the implemented treatment. In all cases, the goal of treatment in patients with fistulizing perianal Crohn’s disease is to control the perianal sepsis, secondary to a fistula and an associated abscess, which cannot be treated medically, in order for these patients to recommence their medical treatment for the background disease, that is, Crohn’s disease. To this end, both fistulotomy and loose seton placement could benefit the appropriately selected patients.
Footnotes
Declaration of Conflicting Interests
This study has been, in part, presented at the 29th Annual Greek Congress of Surgery-International Forum of Surgery, Athens, Greece, 12–15 November 2014.
