Abstract
Background and Aims:
Bariatric surgery is the most effective treatment for obesity. However, not all patients have similar weight loss following surgery and many researchers have attributed this to different pre-operative psychological, eating behavior, or quality-of-life factors. The aim of this study was to determine whether there are any differences in these factors between patients electing to have bariatric surgery compared to less invasive non-surgical weight loss treatments, between patients choosing a particular bariatric surgery procedure, and to identify whether these factors predict weight loss after bariatric surgery.
Material and Methods:
This was a prospective study of 90 patients undergoing gastric bypass, vertical sleeve gastrectomy, or adjustable gastric banding and 36 patients undergoing pharmacotherapy or lifestyle interventions. All patients completed seven multi-factorial psychological, eating behavior, and quality-of-life questionnaires prior to choosing their weight loss treatment. Questionnaire scores, baseline body mass index, and percent weight loss at 1 year after surgical interventions were recorded.
Results and Conclusions:
Surgical patients were younger, had a higher body mass index, and obesity had a higher impact on their quality of life than on non-surgical patients, but they did not differ in the majority of eating behavior and psychological parameters studied. Patients opting for adjustable gastric banding surgery were more anxious, depressed, and had more problems with energy levels than those choosing vertical sleeve gastrectomy, and more work problems compared to those undergoing gastric bypass. Weight loss after bariatric surgery was predicted by pre-operative scores of dietary restraint, disinhibition, and pre-surgery energy levels. The results of this study generate a number of hypotheses that can be explored in future studies and accelerate the development of personalized weight loss treatments.
Keywords
Introduction
Over the past two decades, the obese population has increased from 13% of men and 16% of women in 1993 to 24% of men and 26% of women by 2011 (1). Psychological disorders such as depression and anxiety are very often prevalent among the obese population (2) and such disorders can potentially complicate the treatment of obesity (3).
Bariatric surgery has become an increasingly popular treatment option for individuals with obesity, as sustained postoperative weight loss and improvements in obesity-related comorbidities make it the most effective treatment for this population (4). The prevalence of psychological disorders is high in obese individuals opting for bariatric surgery (5), and in most centres, patients undergo psychological evaluation before a decision is made as to whether or not they are suitable for surgery (2). However, although most researchers agree that psychosocial and behavioral factors such as depression, anxiety, and binge eating can contribute to poor postoperative outcomes, studies are conflicting regarding their prevalence (6, 7) and how they may affect bariatric surgery outcomes (8).
It is generally assumed that psychological morbidity may make it more difficult to maintain good eating habits and therefore sustained weight loss (9). Although bariatric surgery has many health benefits and is considered very effective treatment for the management of severe obesity, there are still a significant proportion of patients (~20–30%) that fail to lose a significant amount of weight (3). This is thought to be due to a number of different factors including type of surgery, eating habits, and psychological morbidity.
To date, it has been a challenge to determine which psychological factors might influence bariatric surgery outcomes. Many studies looking at possible predictors for weight loss outcomes after bariatric surgery already exclude those with severe psychopathology; therefore, no clear psychological predictors have emerged (10). In addition, methodological weakness, different definitions of successful outcome, failure to differentiate between types of bariatric surgery, small patient groups, and different follow-up periods have complicated the interpretation of data (11). The assumption that those patients opting for surgery suffer from greater psychological comorbidity leading to their choice of more invasive treatment has little supporting evidence and it is also not known whether there are differences in baseline psychological health between patients who choose different operations, for example, adjustable gastric banding (BAND) versus Roux-en-Y gastric bypass (RYGB).
The aims of our study were to determine whether there are any differences in the pre-operative, psychological, quality of life, and eating behavior characteristics between (1) patients electing to have bariatric surgery compared to less invasive non-surgical weight loss treatments, (2) patients choosing a particular bariatric surgery procedure, and (3) identify whether these characteristics predict weight loss after bariatric surgery. By identifying specific factors that predict weight loss, we wish to add to the growing body of literature aimed at improving patient choice and personalization of obesity treatment programs.
Materials and Methods
Design
In this study, data were collected prospectively and analyzed retrospectively. The study was conducted by the Charing Cross NHS hospital obesity clinic and Imperial College London. Three types of treatments are available in our clinics: lifestyle, pharmacotherapy, and bariatric surgery. All patients attended a group session in which the available treatments were presented by all members of the multidisciplinary team including dieticians, physicians, and surgeons. Final management decisions were taken collectively by the patient and clinical team during one-to-one clinical assessments. Patients were excluded from surgical treatments only if they were at unacceptably high risk of a general anesthetic or if they had active and severe mental health disease. A total of 141 consecutive patients were asked to complete a set of questionnaires regarding their psychological characteristics, eating behavior, and quality of life on the day of their group session. In all, 15 patients were excluded from analysis as they did not understand the questionnaire instructions.
Basic clinical characteristics including body mass index (BMI) were recorded during the first outpatient visit and 1 year after surgical intervention. The study took place in 2010–2011 and was approved by the Clinical Governance and Patient Safety Committee at Imperial College London, ref: 09/808.
Assessments
Questionnaires used to assess psychological characteristics, eating behavior, and quality of life are described in the following.
Psychological characteristics
Barratt Impulsivity Scale-11 (BIS-11) is a self-report measure of impulsivity (a personality trait) (12). A higher score represent higher impulsivity rate.
The Hospital Anxiety and Depression Scale (HADS) assesses depression and anxiety. The cut-off values for anxiety and depression levels are 0–7 “normal,” 8–10 “borderline abnormal,” and 11–21 “abnormal” (13).
Behavioral Activation Scale (BAS) measures appetitive motives, that is, to move toward something desired. It consists of three subscales: Reward Responsivity (RR) measures positive responses to the anticipation of reward; Drive (DR) measures the persistent pursuit of desired goals; and Fun-Seeking (FS) measures a willingness to approach a new event on the spur of the moment. In contrast, the BIS measures aversive motivation, that is, to move away from something unpleasant, such as punishment or negative events (14). Higher scores in both scales mean higher tendency toward the measured factor.
Eating behavior
The Three Factor Eating Questionnaire (TFEQ) is a self-report psychometric instrument that assesses eating behavior from three dimensions: cognitive restraint (consciously trying to resist eating in order to control body weight), disinhibition (loss of control over eating), and the susceptibility to hunger (15). Maximum scores for the subscales are as follows: 21, 16, and 14, respectively, with higher scores indicating greater cognitive restraint, uncontrolled eating, and food intake, in response to feelings of hunger.
The Eating Disorders Examination Questionnaire (EDE-Q) is a self-report instrument used to assess eating behaviors over a period of 28 days. The EDE-Q is adapted from the original Investigator Based Interview but retains the format of including four subscales: restraint, shape, weight, and eating concern, and a global score (16). The scores range from 0 to 6 with the global scale measuring the severity of the eating disorder psychopathology.
Quality of life
The Short Form 36 (SF-36) health survey is a self-administered questionnaire containing 36 items. It measures functional status, well-being, and the overall evaluation of health. Scores range from 0 to 100, and higher scores indicate better health status (17).
Impact of Weight on Quality of Life (IWQOL) assesses the impact of an individual’s weight on their physical function, self-esteem, sexual life, public distress and work problems, and the total quality of life of all aspects combined together to give an overall evaluation. Higher scores indicate poorer quality of life as a result of an individuals’ weight (18).
Statistical Methods
Descriptive data are shown as mean ± SD. Groups were compared either with unpaired t-tests/Mann–Whitney U or one-way ANOVA/one-way ANOVA on ranks depending on normality distribution. Pair-wise post-ANOVA comparisons were performed using the Tukey multiple comparison correction testing. Psychological predictors of percentage weight loss were determined using Pearson’s correlation test. The statistical software used was Graph Pad Prism 5 and statistical significance was accepted at the p < 0.05 level.
Results
Out of the 126 patients analyzed, 90 chose and actually underwent bariatric surgery and 36 chose to undergo either lifestyle or pharmacotherapy treatments. Out of the 90 surgical patients, 72 underwent RYGB, 12 BAND, and 6 vertical sleeve gastrectomy (VSG). The basic clinical characteristics of both surgical and non-surgical groups, as well as of the patients in each surgical sub-group are shown in Table 1.
Basic characteristics of patients undergoing surgical and non-surgical treatments (lifestyle and pharmacotherapy) for weight loss. Data are also provided for each of the three surgical subgroups.
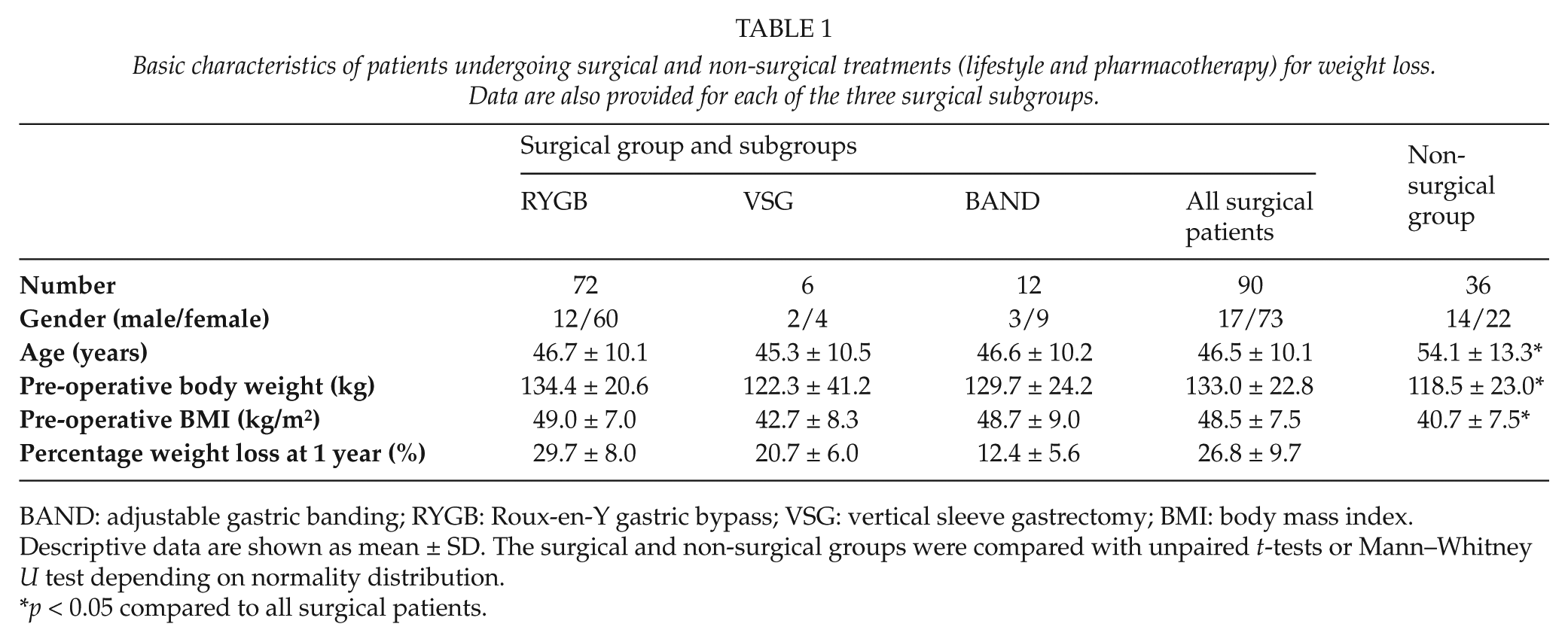
BAND: adjustable gastric banding; RYGB: Roux-en-Y gastric bypass; VSG: vertical sleeve gastrectomy; BMI: body mass index.
Descriptive data are shown as mean ± SD. The surgical and non-surgical groups were compared with unpaired t-tests or Mann–Whitney U test depending on normality distribution.
p < 0.05 compared to all surgical patients.
Comparisons Between Surgical and Non-Surgical Patients
The surgical patients were significantly younger and heavier than the non-surgical group (Table 1). There were significant differences in reward responsiveness and behavioral inhibition scores in the BIS/BAS questionnaire, with the surgical group scoring significantly higher than the non-surgical group (Table 2). Public distress and total IWQOL scores were also significantly higher in the surgical group than the non-surgical group (Table 4). There were no significant differences between the surgical and non-surgical groups in terms of eating behavior (Table 3) or quality of life as measured by the SF-36 (Table 4).
Pre-operative psychological characteristics of patients undergoing surgical and non-surgical treatments (lifestyle and pharmacotherapy) for weight loss. Data are also provided for each of the three surgical subgroups.
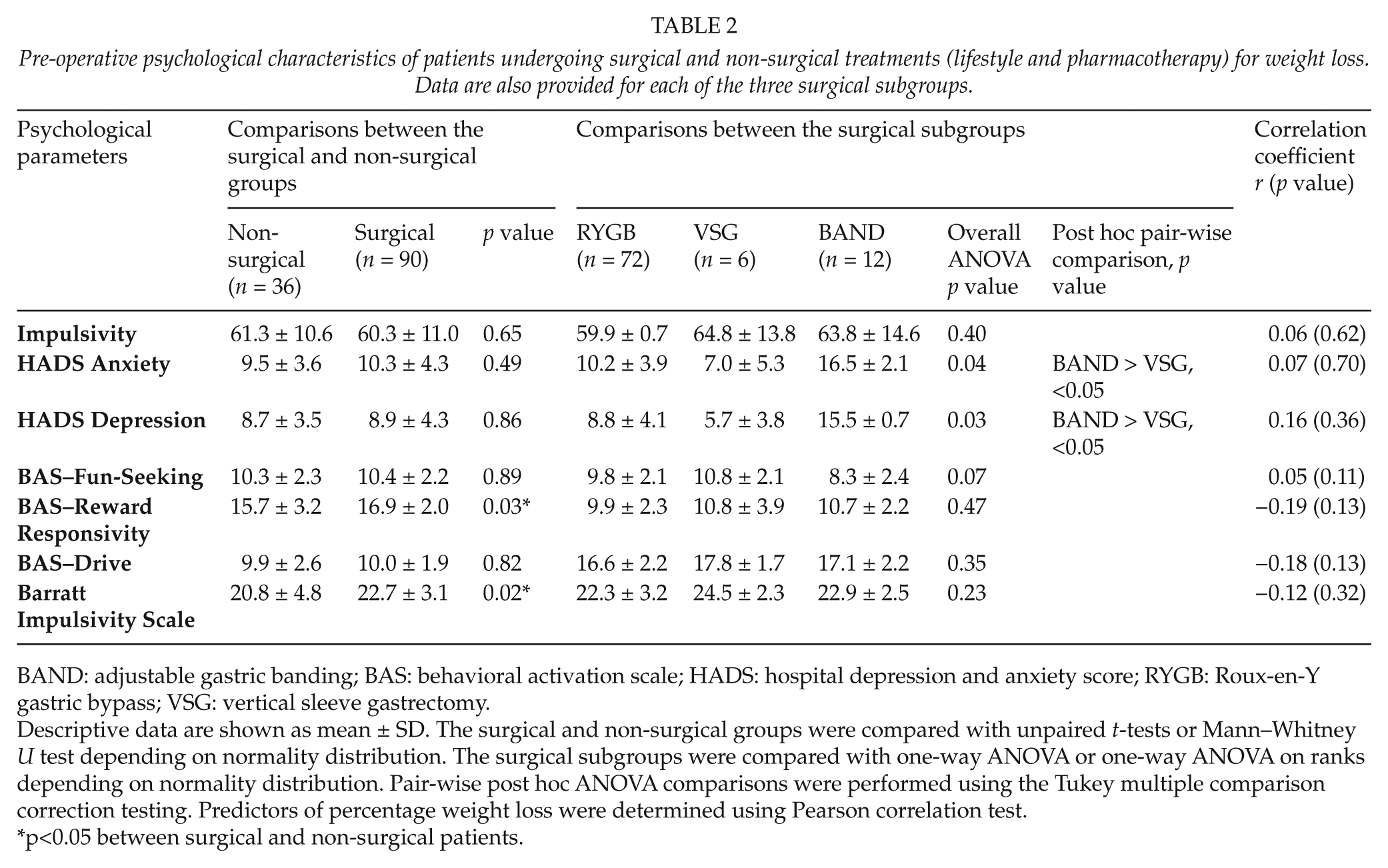
BAND: adjustable gastric banding; BAS: behavioral activation scale; HADS: hospital depression and anxiety score; RYGB: Roux-en-Y gastric bypass; VSG: vertical sleeve gastrectomy.
Descriptive data are shown as mean ± SD. The surgical and non-surgical groups were compared with unpaired t-tests or Mann–Whitney U test depending on normality distribution. The surgical subgroups were compared with one-way ANOVA or one-way ANOVA on ranks depending on normality distribution. Pair-wise post hoc ANOVA comparisons were performed using the Tukey multiple comparison correction testing. Predictors of percentage weight loss were determined using Pearson correlation test.
p<0.05 between surgical and non-surgical patients.
Pre-operative eating behavior of patients undergoing surgical and non-surgical treatments (lifestyle and pharmacotherapy) for weight loss. Data are also provided for each of the three surgical subgroups.
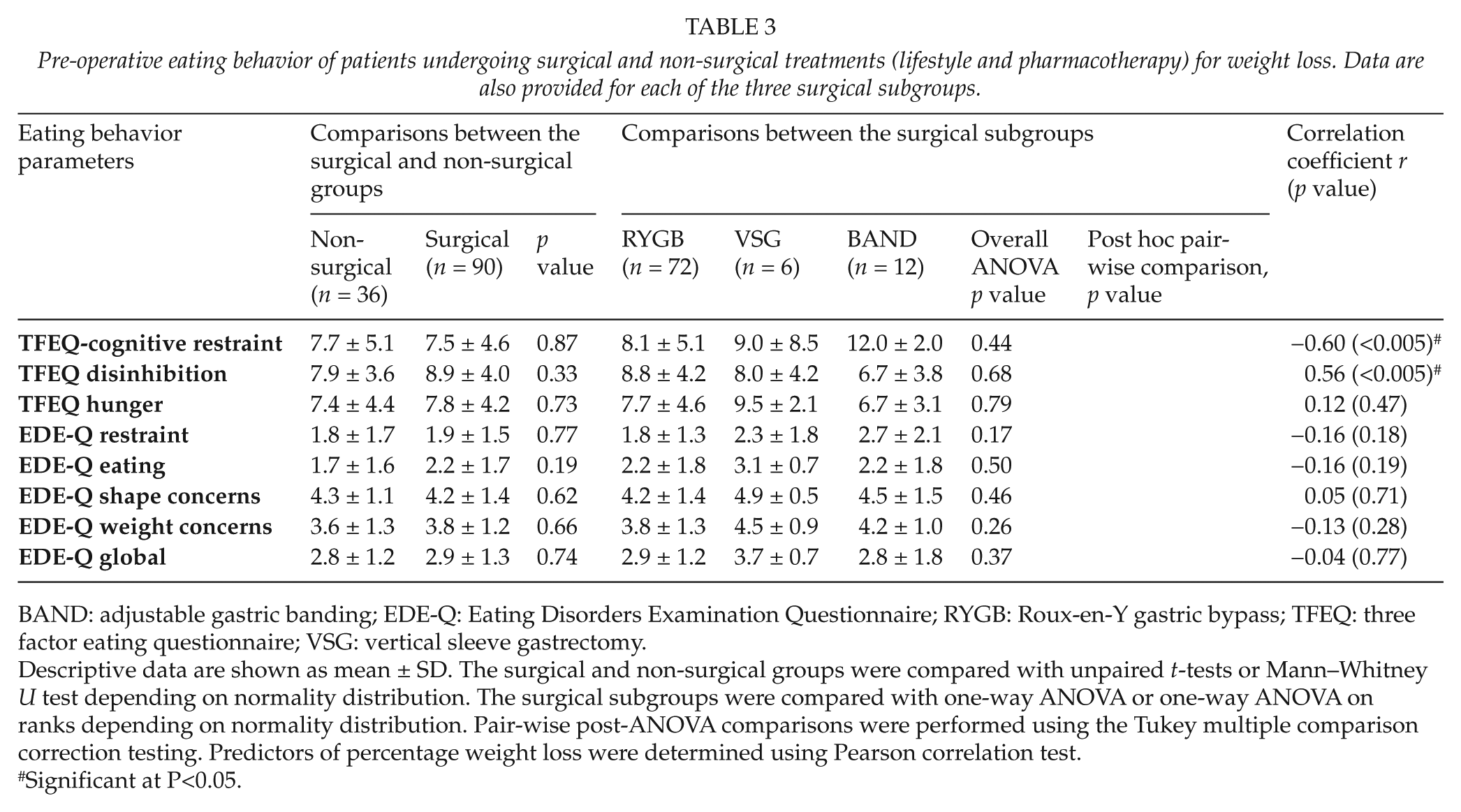
BAND: adjustable gastric banding; EDE-Q: Eating Disorders Examination Questionnaire; RYGB: Roux-en-Y gastric bypass; TFEQ: three factor eating questionnaire; VSG: vertical sleeve gastrectomy.
Descriptive data are shown as mean ± SD. The surgical and non-surgical groups were compared with unpaired t-tests or Mann–Whitney U test depending on normality distribution. The surgical subgroups were compared with one-way ANOVA or one-way ANOVA on ranks depending on normality distribution. Pair-wise post-ANOVA comparisons were performed using the Tukey multiple comparison correction testing. Predictors of percentage weight loss were determined using Pearson correlation test.
Significant at P<0.05.
Pre-operative quality of life of patients undergoing surgical and non-surgical treatments (lifestyle and pharmacotherapy) for weight loss. Data are also provided for each of the three surgical subgroups.
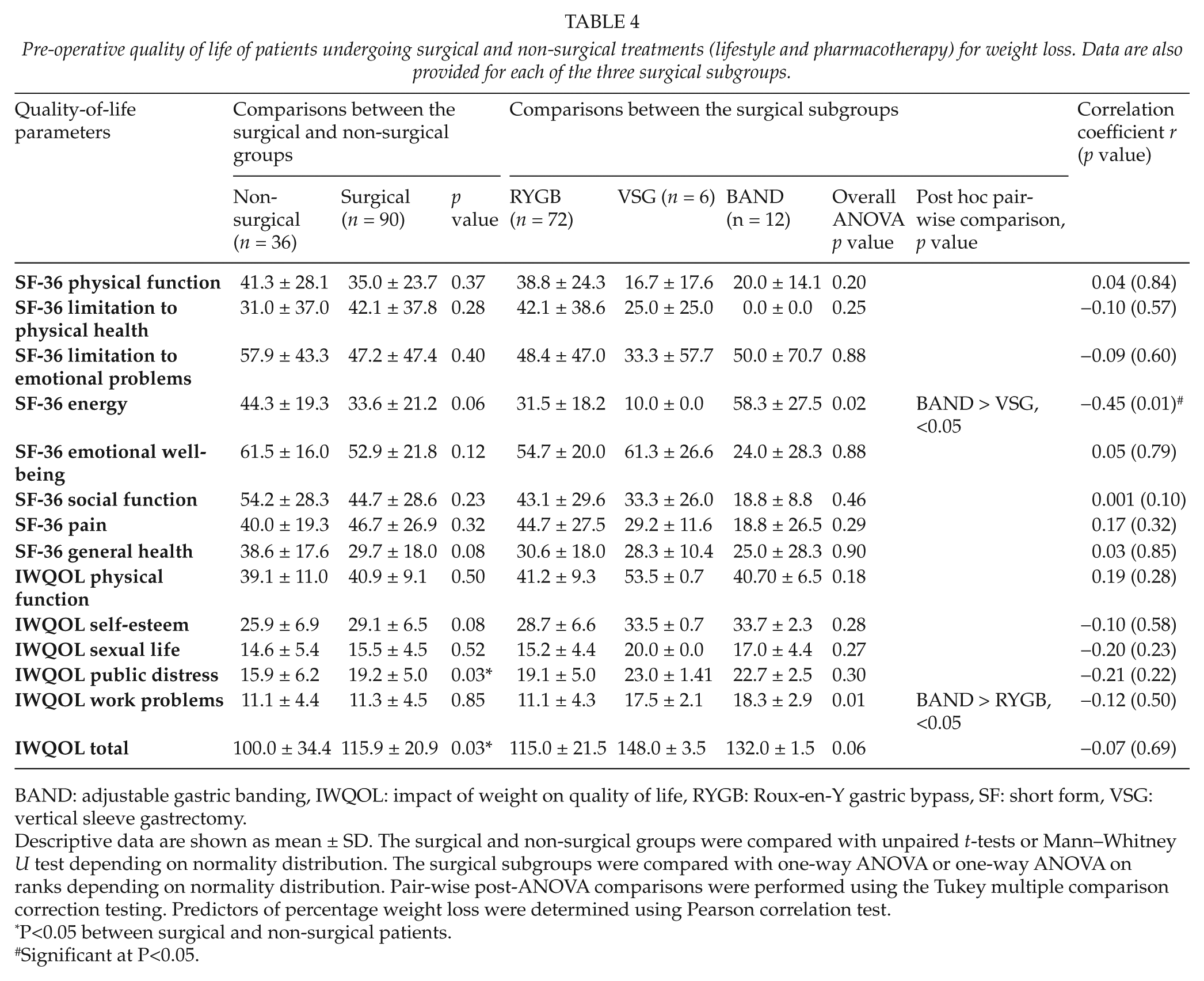
BAND: adjustable gastric banding, IWQOL: impact of weight on quality of life, RYGB: Roux-en-Y gastric bypass, SF: short form, VSG: vertical sleeve gastrectomy.
Descriptive data are shown as mean ± SD. The surgical and non-surgical groups were compared with unpaired t-tests or Mann–Whitney U test depending on normality distribution. The surgical subgroups were compared with one-way ANOVA or one-way ANOVA on ranks depending on normality distribution. Pair-wise post-ANOVA comparisons were performed using the Tukey multiple comparison correction testing. Predictors of percentage weight loss were determined using Pearson correlation test.
P<0.05 between surgical and non-surgical patients.
Significant at P<0.05.
Comparisons Between Surgical Subgroups
Anxiety and depression were significantly higher in the BAND group compared to the VSG group, but not compared to RYGB (Table 2). There were no differences between the three subgroups in any of the eating behavior factors as measured by TFEQ and EDE-Q (Table 3). In quality-of-life parameters measured by the SF-36, problems with energy levels were significantly higher in the BAND group compared to the VSG group but not compared to RYGB. However, impact of weight on work as measured by IWQOL was significantly higher in the BAND compared to RYGB but not compared to VSG (Table 4).
Pre-Operative Predictors of Weight Loss Following Bariatric Surgery
SF-36 energy and TFEQ-cognitive restraint were both negatively correlated with the percentage weight lost at 1-year post-surgery, while TFEQ disinhibition was positively correlated (Tables 3 and 4). No significant correlation was found between the other parameters and percentage weight loss (Table 2).
Discussion
In this study, we found that patients did not differ significantly in the vast majority of psychological, eating behavior, or quality-of-life characteristics compared to those choosing to undergo non-surgical treatments. The younger age, higher BMI, and impact of obesity on the quality of life of the bariatric surgery group suggest that these patients were driven to the surgical approach by the severity of their condition and in an attempt to improve their long-term health.
Among patients choosing surgical options, those who opted for the BAND had significantly higher anxiety and depression, and more problems with energy levels than those who opted for VSG, and more work problems than those choosing RYGB. Cognitive restraint and disinhibition as measured by the TFEQ, and low energy levels as measured by SF-36, emerged as the only baseline predictors of percentage weight loss at 1 year in patients who underwent bariatric surgery of any type.
Comparisons Between Surgical and Non-Surgical Patients
Our comparison of surgical and non-surgical patients suggests that patients who have a higher BMI, especially at a relatively young age, may be more inclined to choose an invasive treatment option. Despite their higher BMI, patients opting for surgery did not have significantly higher impulsivity, anxiety, and depression, or worse eating behavior as measured by the BIS-11, HADS, TFEQ, EDE-Q, respectively, compared to patients opting for non-surgical treatments.
Patients opting for surgery had significantly higher scores in behavioral inhibition and reward responsiveness. Individuals with high behavioral inhibition tend to have higher levels of anxiety and are more cautious with regard to risk taking behavior (14, 19, 20). In this context, in our sample group, the decision to undergo a surgical treatment may represent an exchange of perceived higher short-term risk (e.g. risk of anesthetic complications) in favor of lower long-term risk (e.g. reduction in obesity-related morbidity and current health complications). Alternatively, observed differences in behavioral inhibition and reward responsiveness may be related to the lower age or higher BMI in the surgical group. Both behavioral inhibition and behavioral activation, of which reward responsiveness is included, decrease with increasing age (20) due to changes in personality characteristics including being less fearful, less anxious, and less depressed with age (14). RR has been linked to food craving, overeating, and preference for sweet and fatty food which, in turn, lead to weight gain over the long term and increased BMI (21, 22).
Obesity had a higher impact on the overall quality of life of surgical patients as measured by the IWQOL and even more particularly by public distress. Impairment of quality of life has been linked by many studies to the severity of obesity and thus to the approached method of treatment, with heavier patients opting for more invasive treatments (e.g. Kolotkin et al. (23)).
In summary, while the psychological and eating behavior of obese patients seeking a surgical compared to a non-surgical treatment did not differ significantly, bariatric surgery may appeal more to those who are younger or who have a higher BMI and therefore have increased impact of weight on quality of life and are at a higher long-term risk of obesity-related comorbidity.
Comparisons Between Surgical Subgroups
Only two studies to date have compared pre-surgical psychological profiles of bariatric patients undergoing RYGB compared to BAND. Walfish (24) found no difference in baseline scores of depression, anxiety, anger, and “self-assessed reasons for weight gain” between female BAND and RYGB patients but found that BAND patients had higher rates of “eating when anxious” than RYGB. On the other hand, Hood et al. (25) found that RYGB patients had higher baseline depression, binge eating symptoms, somatic complaints, and antisocial features than BAND patients.
In our study, we found that BAND patients had higher levels of depression and anxiety than the VSG but not RYGB group. Importantly this was not explained by differences in their age and BMI, suggesting a role for other factors. At the time of the study, VSG was a relatively new treatment option, compared to BAND and RYGB. It may be that patients at that time viewed VSG as irreversible and potentially more risky than the other surgeries, and particularly the BAND. Those with higher depression and anxiety, and therefore more cautious and less risk taking, may therefore have perceived BAND as a safer and more acceptable intervention.
The weight-related quality of life among the surgical subgroups did not differ significantly in the SF-36, but in the IWQOL, BAND patients scored significantly higher for work problems than the RYGB but not the VSG group, indicating greater difficulties in carrying out work effectively or from progressing at work as a result of their weight. In his study in 1999, Anderson (26) found that BAND patients were of a higher socioeconomic status than the RYGB. This may explain our findings to some degree, since BAND surgery is technically less demanding and requires less hospitalization than RYGB surgery (27), and may therefore appeal more to those in employment, especially if their work is suffering. In keeping with higher anxiety and depression, BAND patients also reported more problems with energy levels than VSG (and a non-significant trend for more problems compared to RYGB). It should, however, be noted that the comparisons involving the VSG group should be interpreted with some caution, as the number of patients in the group was small.
Pre-Operative Predictors of Weight Loss Following Bariatric Surgery
A number of attempts have been made to investigate whether weight outcomes could be predicted from participants’ psychological and behavioral characteristics prior to bariatric surgery. Previous studies examined a limited number of variables at a time such as cognitive function, or psychological characteristics (e.g. Belanger et al. (28)). For the majority of variables examined, studies have shown no correlations with weight loss or inconsistent findings. We add to this work, by finding that dietary dishinhibiton according to the TFEQ scores and worse energy scores on SF-36 positively predicted weight loss following surgery, and that TFEQ dietary restraint scores negatively predicted weight loss following surgery.
With regard to eating behavior, disinhibition results in erratic eating and unplanned meals, and is associated with binge eating, a higher BMI, and obesity (29). Bariatric surgery, and in particular RYGB, results in decreased disinhibition and improved eating behavior, which may contribute to weight loss (30, 31). In contrast to our findings, previous studies have not found disinhibition to be a predictor of weight loss outcomes (32, 33). Bariatric surgery may modify erratic eating behavior by various mechanisms, including reducing the hedonic value of food (31, 34). Therefore, those with higher disinhibition and erratic and emotional eating behavior pre-operatively may experience a greater benefit from these modifications than those where obesity has been influenced by other factors.
We also found a negative correlation between TFEQ-cognitive restraint and percentage weight loss. Dietary restraint is defined as a conscious effort to resist eating with the aim of controlling body weight (35). In their study, Sarwer et al. (36) found that higher baseline dietary restraint results in more weight loss following RYGB as a result of better adherence to the postoperative diet. However, based on the restraint theory, Polivy and Herman (37) argued that high dietary restraint can lead to increased periods of overeating, resulting in higher consumption of calories following dieting. Our results are consistent with this finding and suggest that high baseline dietary restraint can negatively influence long-term weight loss results.
SF-36 poor energy levels in this study were associated with poorer weight loss following surgery. In bariatric patients, Dixon et al. (7) found that energy was not correlated to weight loss following surgery. However, lower energy levels caused by the health complications of obesity pre-bariatric surgery can be strong motivators for weight loss (9). As bariatric surgery improves the quality of health of obese patients, most are likely to engage more in physical exercise, but those with poorer energy levels to start with may not see as much improvement and may struggle more to engage in physical activity resulting in less weight loss and poorer weight maintenance at 1 year follow-up.
While providing important new findings, the present study has a number of limitations. In our study, very few patients underwent VSG and therefore further studies are necessary to confirm findings involving this subgroup. In order to determine predictors for weight loss, we collapsed all the sub-surgical patients in one group. Therefore, most of the findings may have been driven by the large RYGB group potentially reducing the generalizability of the conclusions that can be drawn. However, RYGB is the most commonly performed bariatric surgery worldwide (38) and our findings are therefore representative of most bariatric surgery centres.
Psychological, eating behavior, and quality-of-life parameters tend to be altered following bariatric surgeries. Therefore, it would have been valuable to collect data post-surgery and determine the association of those factors with weight loss at 1 year post-surgery. In addition, no information was available on other important factors, that is, education, socioeconomic status, medical comorbidities, and functional impairment all of which may also contribute to patient choice of treatment and to their psychological characteristics, eating behavior, and quality of life.
We compared a number of parameters between the groups and performed multiple comparisons. In order to reduce the impact of multiple testing, we corrected for multiple comparison testing in the ANOVAS using the Tukey post hoc method. Even though our patients underwent an extensive assessment of their eating behavior, psychological traits, and quality of life, we limited the number of variables studied to those that were more relevant to clinical bariatric practice.
Finally, even though it is possible that the eating behavior, personality, and quality of life characteristics of our patient population may differ from those of obese patients not attending a specialist bariatric centre, this was beyond the scope of our study.
In summary, this study has explored some of the patient characteristics which may influence weight loss treatment choice and success. The results of this study suggest that psychological and eating behavior factors may not play a major role in the choice of weight loss treatments, but this may be influenced more by age and the severity of obesity. Among bariatric surgery patients, patients opting for adjustable gastric banding surgery were more anxious, depressed, and had more problems with energy levels than those choosing VSG, and more work problems compared to those undergoing gastric bypass. Weight loss after bariatric surgery was predicted by lower pre-operative scores of dietary restraint, higher disinhibition, and lower pre-surgery energy levels. The results of this study generate a number of hypotheses that can be explored in future studies and accelerate the development of personalized weight loss treatments.
Footnotes
Acknowledgements
The authors would like to thank Ronette L. Kolotkin for allowing Dr Scholtz to use and report the results of the Impact of Weight on Quality of Life (IWQOL) assessment questionnaire. Alexander D. Miras and Werd Al-Najim contributed equally to the manuscript.
Declaration of Conflicting Interests
There are no conflicts of interest for any of the authors.
Funding
Work supported by grants from UK Medical Research Council (MRC), Wellcome Trust, and National Institute for Health Research (NIHR). Alexander D. Miras has received funding from an MRC Clinical Training Fellowship, MRC Centenary Award, and an NIHR Clinical Lectureship. Christina G. Prechtl was funded by the British Research Council (BRC). Carel W. le Roux has received funding from the Science Foundation Ireland and the Moulton Foundation UK. Samantha Scholtz was funded by a Wellcome Trust Research Training Fellowship. The views expressed are those of the authors and not necessarily those of the funders, NHS, the NIHR, or the Department of Health.
