Abstract
Aims:
To identify associations between chronic conditions and eight key health risks (stress, loneliness, sleep, obesity/body mass index, smoking, exercise, alcohol consumption, and fruit intake) and provide a practical descriptive profile of the distribution of health risks within chronic conditions.
Methods:
The sample involved 56,988 Danish residents aged over 16 years from three national health surveys (2010/2013), one sociodemographic register, and seven national health registers. Linear and logistic regression models adjusting for socioeconomic variables were used to analyse associations with 14 disease groups and 30 common conditions.
Results:
The regression analyses revealed that stress, obesity, and physical inactivity were the most consistently associated health risk factors across disease groups. We identified three groups of health risks with similar strengths of associations. Firstly, one group comprising obesity, stress, and sleep troubles, was significantly linked to 27, 23, and 22 chronic conditions, respectively. Secondly, a group of physical inactivity/loneliness showed moderate associations, linked to 19 and five chronic conditions, particularly mental health conditions; and thirdly, a group of smoking, drinking, and low fruit intake showed the weakest and fewest associations. A descriptive profile showed that anxiety, schizophrenia, attention deficit hyperactivity disorder, headaches and chronic obstructive pulmonary disease were conditions with high proportions of patients experiencing more than four health risks.
Conclusions:
Keywords
Introduction
Multiple health risk factors (MHRFs), defined as clusters of health risk factors, have not only been associated with higher mortality and morbidity rates in various preventable chronic conditions but are also linked to a decline in health-related quality of life [1–10]. Behavioural modifiable MHRFs, such as smoking, obesity, alcohol use, physical inactivity, and unhealthy dietary choices [3,11,12], have been widely recognised as significant contributors to the burden of chronic diseases. Research also reveals similar associations between psychosocial-related health risks [13] and adverse outcomes related to perceived stress [14,15], loneliness [16–18] and sleep quality [19,20].
Specifically, behavioural modifiable MHRFs increase the risk of developing various conditions, including diabetes mellitus, cardiovascular diseases, chronic obstructive pulmonary disease (COPD), arthritis, and certain types of cancers with unfavourable outcomes [1–3,21]. The manifestation and causal pathways of these chronic conditions are primarily linked to four measurable biological parameters: blood pressure, glucose and cholesterol levels in the blood, and body mass index (BMI) [22]. It is widely acknowledged that the simultaneous presence or combined impact of multiple influencing factors on health can harm life expectancy [23,24]. The World Health Organization’s (WHO) latest estimations attribute 41 million deaths, or three-quarters of global mortality, to chronic or non-communicable diseases [25]. Importantly, WHO emphasises that risk factors such as tobacco use, excess alcohol consumption, an unhealthy diet, and physical inactivity are key contributors to this burden (the outcome, e.g. diabetes, COPD, depression) and multiple health risks factors (MHRFs, the exposure, e.g. smoking, alcohol, diet, inactivity) [1,25].
Due to the burden of chronic diseases, these modifiable risk factors increase morbidity and mortality rates and incur substantial economic costs for individuals and society [3,26,27]. Therefore, it is imperative to prioritise efforts to promote and implement interventions that support healthier lifestyles as an efficient strategy for preventing or reducing the prevalence of both the rising rates of chronic diseases and these risk factors [24]. Assessing the extent and characteristics of these risk factors within the target population is crucial to developing effective intervention programmes.
While there has been extensive research on the association between modifiable health risk factors and chronic diseases, a notable limitation in many studies is the lack of comprehensive reporting on the frequency and characteristics of these risk factors for chronic conditions [28]. This detailed understanding is crucial for effectively tailoring specific populations’ prevention strategies and treatment approaches. Additionally, current population-based studies primarily focus on behavioural risk factors, often overlooking psychosocial risk factors such as stress, loneliness, and sleep despite their well-documented impact on health outcomes. For example, social isolation has long been recognised as a significant contributor to morbidity and mortality, with its effect comparable to that of obesity, physical inactivity, and potentially even smoking [17]. Evidence from recent studies has additionally revealed that stress and loneliness have a more significant effect on health-related quality of life (HRQoL) than commonly described behavioural risk factors [9,10].
Moreover, due to variations in methodological frameworks across studies, making accurate comparisons is challenging [29]. Thus, there is a requirement for standardised estimates of different chronic conditions across numerous health risks using a uniform methodology. To address these shortcomings, a sister study has provided a descriptive catalogue of prevalence rates and means of eight behavioural and psychosocial health risks (obesity/BMI groups, smoking, physical exercise, alcohol consumption, fruit intake, loneliness, self-perceived stress, and sleep quality) for 199 chronic conditions using a uniform methodology [28]. However, descriptive statistics did not enable an analysis of the associations and significance of the health risks on diseases or identify discrepancies in effect across chronic conditions. Moreover, a simplified profile on the number of MHRFs would aid healthcare professionals in using the estimates.
Thus, the current study aims to assess the associations (hereafter primarily mentioned effect sizes) and significance of the eight health risk factors to answer which health risks have an actual associational relation with chronic conditions, what health risks have the largest effect sizes, and are related to which conditions, based on linear and logistic regression models in a Danish sample. Such adjusted analysis will enable us to identify the most critical health risk associations with the development of chronic diseases and answer what health risks should be prioritised in future interventions and policies to reduce the burden of chronic diseases. Secondly, supplementing previous work [28], we provide a simplified, descriptive population health profile with many risk factors for clinicians for easier prevention and treatment targeting.
This study is part of a series that has produced comprehensive catalogues of disease prevalence, including sociodemographic characteristics [30,31], rates of multimorbidity [32,33], disparities in socioeconomic health [34,35], HRQoL [9,10,29] and health risks [28] on 199 and more chronic conditions in the Danish population. The goal has been to provide healthcare professionals and policymakers with reliable estimates to guide prevention efforts, treatment strategies, planning initiatives, and policy decisions. The current study will inform professionals concerned with targeting and preventing health risks in clinical practice and policymakers interested in identifying the health risks and conditions with the largest disparities and potentials.
Methods
Survey data
The study is based on data from the National Health Profile Survey (NHPS) [13]. The NHPS is a comprehensive and representative study conducted every fourth year in Denmark. It provides healthcare professionals and decision makers with detailed information about the health of Danish citizens through more than 90 different health indicators. The survey collects data from individuals identified using their unique civil registration number based on informed consent. Data collection methods include electronic distribution to a private electronic mailbox or sending letters via the postal service to a randomly selected sample of the Danish population. The NHPS encompassed various indicators of the prevalence and impact of 18 self-reported chronic diseases, measures of health-related quality of life, behavioural risk factors (such as smoking, alcohol consumption, fruit intake, and physical activity), BMI, social networks, stress using Cohen’s Perceived Stress Scale inventory score range 18–40 equivalent to the 20% most stressed participants (identical to the cutoff used and clarified in earlier published studies and reports [9,10,36–41]). Additionally, the gathered information included sleep patterns and other complementary variables.
The NHPS is coordinated by the National Institute of Public Health (NIPH) and the five regional healthcare service providers (regions). Data are collected every 4 years, comprising five regional samples, one for each of the five regions, and one national sample conducted by the NIPH. These samples were randomly selected and did not overlap within each sampling year. This study used three subsamples from two consecutive waves in early 2010 and early 2013 – one national subsample provided by NIPH [9,10,29] and two regional subsamples from the North Denmark Region [13,38,42,43]. These subsamples were chosen based on their inclusion of specific optional questions required for analysis. There was a response rate of approximately 60.2%, with 56,988 respondents across the three survey samples used here. Further details on the NHPS can be found elsewhere [13].
Sampling weighting
To address the stratified design and non-response in the sampling, Statistics Denmark provided weighting adjustments. The non-response weights included standardising the skewed and regional samples to ensure overall national representativeness based on age, sex, and educational achievements [13,44].
Register data
To gather sociodemographic data, including sex, age, place of residence, ethnicity, education, and income for the survey participants, and to obtain information on chronic conditions beyond the 18 self-reported conditions, we linked various national registers to each participant using their unique 10-digit civil registration number. These registers included the Danish Civil Registration System [45], Danish Registers on Personal Income and Transfer Payments [46], Danish Population’s Education Register [47], Somatic Hospital Contacts Register [48], Psychiatric Hospital Contacts Register [49], Primary Healthcare Visits Register [50], and Prescribed Medicines Register [51]. This allowed us to link each individual via their unique civil registration number. A more detailed methodology regarding the linkage between samples and these registers is present within Hvidberg and colleagues [10,29].
Identifying chronic conditions
The algorithms utilised to classify chronic conditions in the health registers were derived from previous research that categorised 199 chronic conditions based on data collected from several national public health registers [29–31,52,53]. Following earlier studies, a ‘chronic condition’ was defined as a ‘condition had lasted or was expected to last 12 or more months and resulted in functional limitations and/or the need for functional limitations and/or the need for ongoing medical care’ [54–56]. Based on this definition, medical experts categorised International Classification of Disease, version 10 (ICD-10) codes into 199 distinct chronic conditions [52,53]. However, within this main paper, merely 14 disease groups and 30 common, individual conditions of the 199 conditions were explored. Please refer elsewhere for more detailed explanations regarding the methods employed and register content descriptions [29,52,53].
Outcome variables
For the two linear regressions, we coded a continuous variable of MHRFs and the number of chronic conditions. In contrast, we used dichotomous variables indicating the presence of a disease or not for the 14 disease groups and each of the 30 common chronic conditions for the logistic regression models.
The 30 common chronic conditions were chosen based on typical prevalent conditions reported in national health profiles and others [13,57,58]. The 14 disease groups – B, C, D, E, G, H, I, J, K, L, M, N, Q and F – correspond to the WHOs ICD-10 classification of disease groups [59] as follows:
B: Viral hepatitis and HIV disease;
C: Malignant neoplasms;
D: In situ, benign and neoplasms of uncertain or unknown behaviour and diseases of the blood and blood-forming organs, etc.;
E: Endocrine, nutritional and metabolic diseases;
G: Diseases of the nervous system;
H: Diseases of the eye and adnexa and diseases of the ear and mastoid process;
I: Diseases of the circulatory system;
J: Diseases of the respiratory system;
K: Diseases of the digestive system;
L: Diseases of the skin and subcutaneous tissue;
M: Diseases of the musculoskeletal system and connective tissue;
N: Diseases of the genitourinary system;
Q: Congenital malformations, deformations and chromosomal abnormalities;
F: Mental and behavioural disorders.
Please also see Table II for named details of all 14 disease groups or earlier literature defining the conditions, naming and diagnosis codes [30,53].
Controlling regression variables
The eight health risk factors were assessed using a dichotomous scale, with a value of one assigned to individuals who had a BMI greater than 30, engaged in daily smoking, exceeded drinking recommendations, had low physical activity levels, experienced frequent feelings of loneliness, belonged to the most stressed quartile on the Cohen’s Perceived Stress Scale (CPSS; scoring between 18 and 40 out of 1 to 40), and reported being significantly bothered by sleep-related issues. A zero value was given if these health risks were not present or below the threshold mentioned for BMI and CPSS. Controlling socioeconomic variables were measured and ranked as described in earlier related studies [10,28,29] and include sex, age, and educational achievement.
Descriptive and socioeconomic variables
Finally, besides the above variables, the descriptive analyses (Table III) also comprise different socioeconomic variables including gender, age, education (no education/training except primary school, students or in training, short education such as high school or equivalent, middle education such as bachelor degree or equivalent, higher education at postgraduate level or above), ethnicity (Danish, other western, non-western) defined based on the individuals’ and parents’ country of birth and citizenship in accordance with common practice and earlier research [13,60,61]; family equalized income quartiles; labour market status (retired due to age, free early retirement, early retirement for health reasons, sick leave and other leave, unemployed social benefits longer term, unemployed minimum 6 months, ordinary, in training or education, employed, others not in the workforce); partnership (having a partner; not married /not in a relationship); and children living at home (yes/no).
Missing values
Self-reported survey data and register variables were utilised to address missing values. While most register-based variables (such as age, sex, and all 199 chronic conditions) were complete, some register-based variables had a few missing values. We relied on self-reported auxiliary information from the NHPS survey data to fill these gaps. For example, if a respondent’s educational achievement was missing in the register data but available in their self-report from the NHPS survey, we used this reported value instead to ensure accurate imputation. To account for missing values in survey variables that could not be replaced from the register, a separate category named ‘missing’ was created. This ensured that respondents were not excluded from the regression analysis. The total sample size consisted of 56,988 respondents. More information about the specific variables, numbers and handling of missing values can be found in previous literature [10,29].
Statistical analysis
Two overall analyses were performed. One descriptive analysis presents prevalence and profile characteristics, and one analytical analysis uses regression modelling to analyse associations between variables, health risks and chronic conditions. The associations, significance and strength of associations of each health risk were assessed using a log-transformed linear regression on the number of health risks and diseases controlling for sex, age, and educational achievement. The variables were log-transformed due to the skewed distributions of MHRFs and illnesses and anti-logged in the results section. Logistic regression was performed, and odds ratios were presented on the 14 dichotomies of disease groups and 30 common chronic conditions to assess the comparative effect sizes and significance of all health risk associations on overall disease groups (meta view) and 30 specific conditions (disease view) while controlling for sex, age, and educational achievement. The number of conditions was reduced to 14 disease groups and 30 common conditions from 199 conditions to ensure overview, model fit and presentation of reliable estimates. Further, detailed statistical estimates of all models are presented in the online Supplemental Table I.
The descriptive profile on numbers of MHRFs across 30 common chronic conditions was done for each number of health risks (0–4+) and presented with 95% confidence intervals (CIs). Profiling of all 199 chronic conditions is shown in the online Supplemental Table II.
All estimates, including regression models, used weighted data with non-response weights, and adjusted prevalence estimates were calculated from national percentages of sex and age as referenced [62,63]. Statistical analysis and data management were conducted using SAS 9.4 and Stata version 16 on Statistics Denmark’s secure research-based servers.
Results
The pooled samples closely mirrored the entire population regarding sex, age, and educational achievements despite slight proportional differences in educational attainment due to higher rates of missing observations in the whole population (Table I). Furthermore, the pooled samples exhibited alignment with the national sample concerning the mean number of MHRFs and BMI, consistent with earlier findings related to HRQoL for these samples [9,10]. However, the pooled sample showed a slightly higher mean BMI difference of 0.4 compared with the national sample, suggesting a minor difference in obesity prevalence between samples (see Toft et al. [64]). Nevertheless, the differences were minor, and the pooled samples were consistent with the national population averages.
Respondent characteristics of the three samples compared to the entire population register data (where applicable).
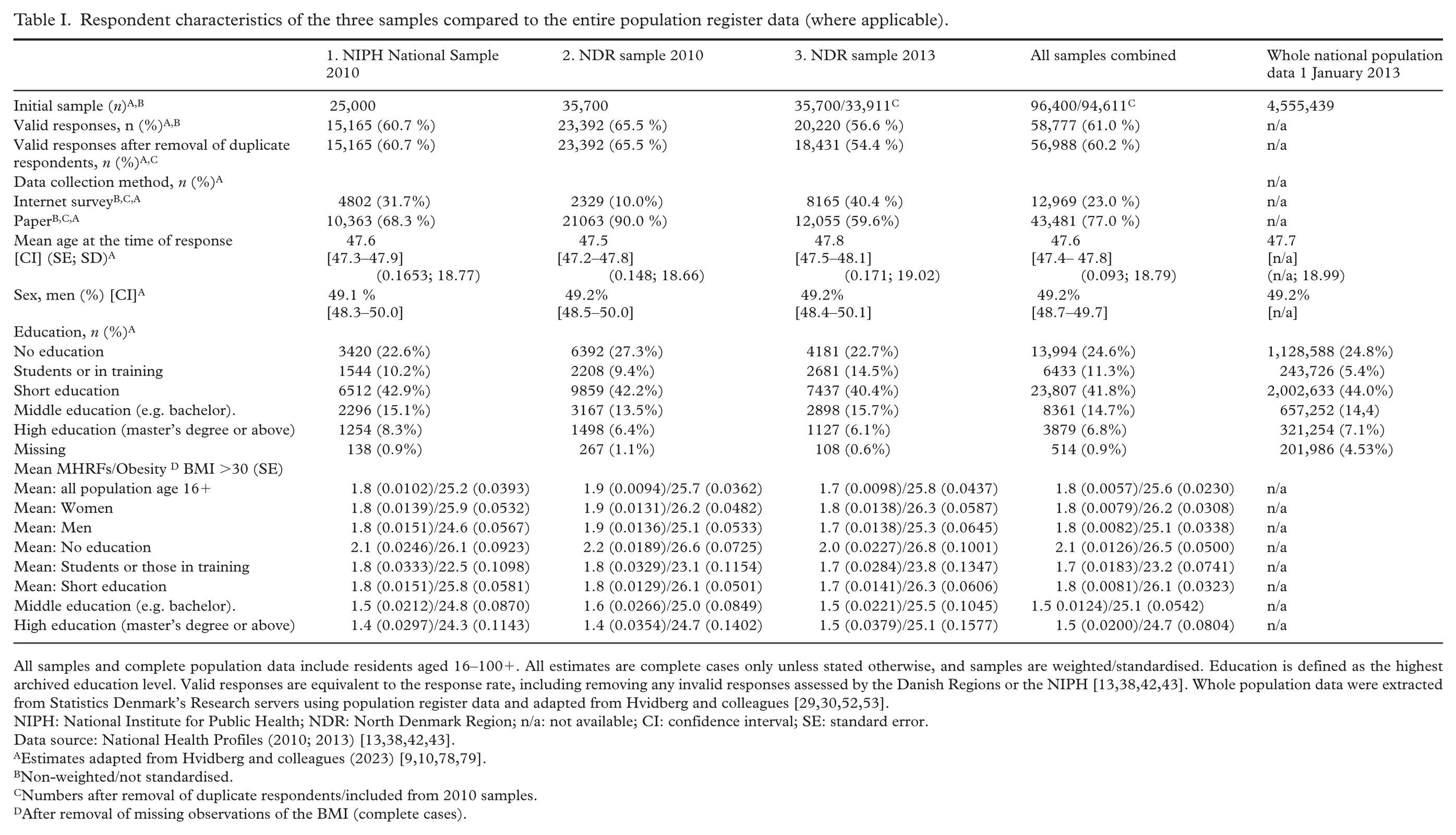
All samples and complete population data include residents aged 16–100+. All estimates are complete cases only unless stated otherwise, and samples are weighted/standardised. Education is defined as the highest archived education level. Valid responses are equivalent to the response rate, including removing any invalid responses assessed by the Danish Regions or the NIPH [13,38,42,43]. Whole population data were extracted from Statistics Denmark’s Research servers using population register data and adapted from Hvidberg and colleagues [29,30,52,53].
NIPH: National Institute for Public Health; NDR: North Denmark Region; n/a: not available; CI: confidence interval; SE: standard error.
Non-weighted/not standardised.
Numbers after removal of duplicate respondents/included from 2010 samples.
After removal of missing observations of the BMI (complete cases).
Table II provides a meta-view of associations with (a) MHRFs (linear), (b) number of chronic conditions (linear), and (c) all 14 disease groups and one model for having a chronic condition or not (logistic). Table II summarises the 17 regression models assessing the significance and effect sizes of the eight health risks adjusted for sex, age, and educational achievements. In the linear regression on MHRFs, all eight health risks had significant effect sizes when adjusted for sex, age, and educational achievement. Except for ‘recommended fruit intake’, all adjusted effect sizes ranged from 1.3 to 1.4. In ranked order, (lack of) recommended fruit intake, obesity, drinking, smoking, stress, physical inactivity, troubled sleep, and loneliness were most strongly associated with increasing health risks when adjusted. In contrast, health risks associations with multimorbidity (linear regression on the number of diseases) were only significant for stress, troubled sleep, obesity, physical inactivity and loneliness, in ranked order of highest effect sizes ranging from 1.1 to 1.2.
Meta view: linear and logistic regression models on the number of MHRFs, chronicity and 14 disease groups; adjusted of socioeconomic variables and health risks.
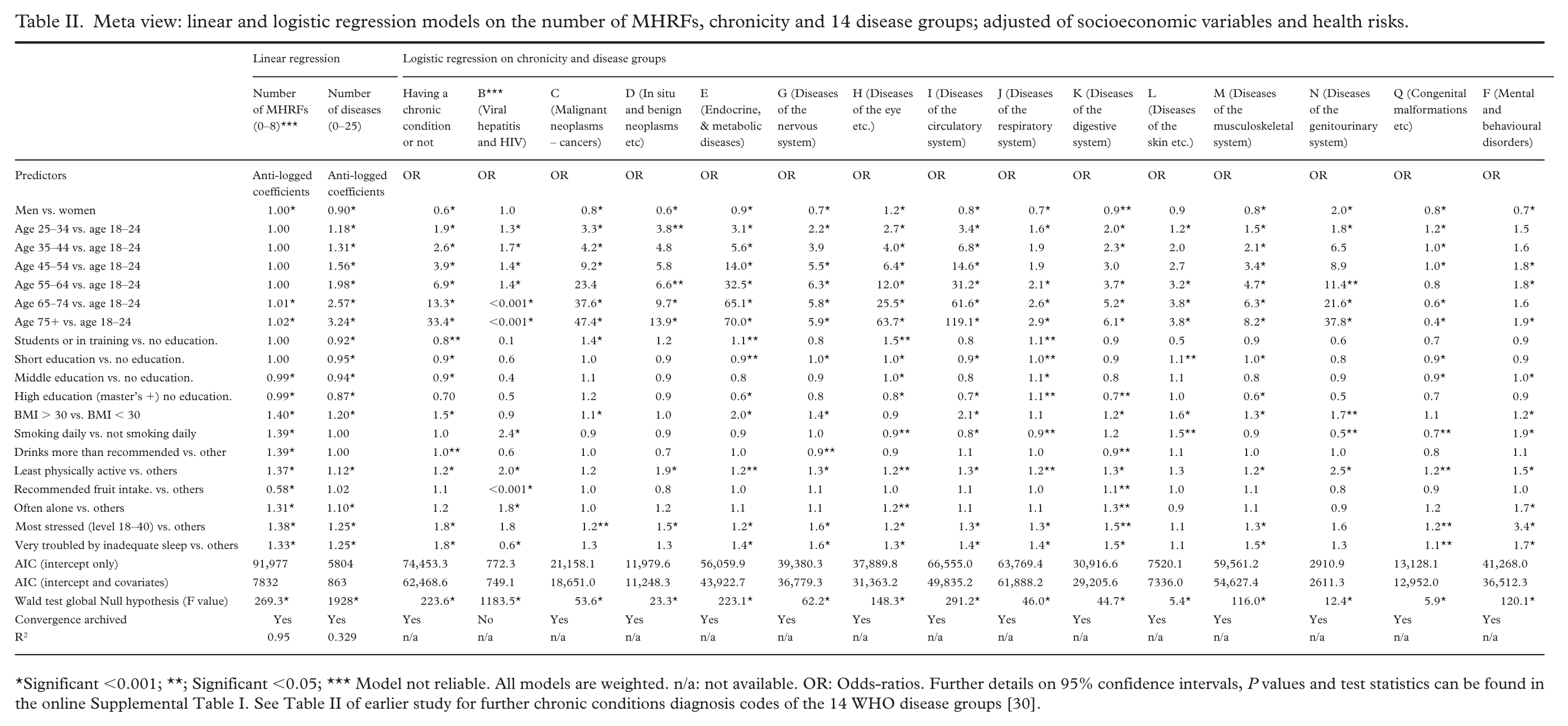
Significant <0.001; ★★; Significant <0.05; ★★★ Model not reliable. All models are weighted. n/a: not available. OR: Odds-ratios. Further details on 95% confidence intervals, P values and test statistics can be found in the online Supplemental Table I. See Table II of earlier study for further chronic conditions diagnosis codes of the 14 WHO disease groups [30].
Similarly, the overall logistic model on chronicity (chronic, i.e. having one or more chronic conditions) showed the highest associations for stress (odds ratio (OR) 1.8), sleep troubles (OR 1.8), obesity (OR 1.5) and physical inactivity (OR 1.2). On the other hand, smoking (OR 1.0), drinking (OR 1.0), fruit intake (OR 1.1) and loneliness (OR 1.2) were either not or barely significant, all with small effect sizes.
However, differences emerge when chronicity is further differentiated into the disease groups (and even more so for specific chronic conditions). For instance, the overall less powerful predictors such as loneliness became significantly associated with psychiatric diseases (F; OR 1.7), diseases of the digestive system (K; OR 1.3) and eye or ear diseases (H; OR 1.2). Fruit intake was significantly associated with digestive system diseases (K; OR 1.1). Finally, some differences were also found for daily smoking, in which diseases F (OR 1.9) and K (OR 1.2) were the only groups with a significant OR above 1 for smoking.
Additionally, some of the largest, significant effect sizes were found for stress about disease groups F (OR 3.4), G/N (OR 1.6), and I/J/M (OR 1.4). All 14 disease groups, except disease group L (OR 1.1), were significant for stress. Large effect sizes were also found for obesity and associations with disease groups I (OR 2.1), E (OR 2.0), N (OR 1.7), and G (OR 1.4) with more variation as disease groups D, H, J, and Q had weaker and close to 1 or non-significant ORs. Finally, physical inactivity was significantly associated with most disease groups with middle to high (relatively) ORs except for disease groups C and L.
Online Supplemental Table I provides complete details on statistics, including 95% confidence intervals, P values and test statistics for all regression models on all disease groups and conditions.
Table III provides a descriptive profile of participants with 0, 1, 2, 3 or 4+ MHRFs, cross-tabulated with 30 common chronic conditions, socioeconomic variables and eight health risks. Overall, people living with any of the 30 common chronic conditions had more multiple health risk factors than individuals in the general population. In particular, people with anxiety disorders, schizophrenia, ADHD, depression, headache syndromes, overweight, COPD, and back conditions had the highest proportions of four or more health risk factors, ranging from 17.9% to 39.2%, compared with a population average of 8.6%. The correlation and trend are also apparent for comorbidity ranging from 6.5% to 22.0% for 1 to 7+ comorbidities having 4+ MHRFs.
Profiling: Health risk profile on numbers of MHRFs across 30 common chronic conditions, sociodemographic variables and the eight health risks. Percent [95% CI].
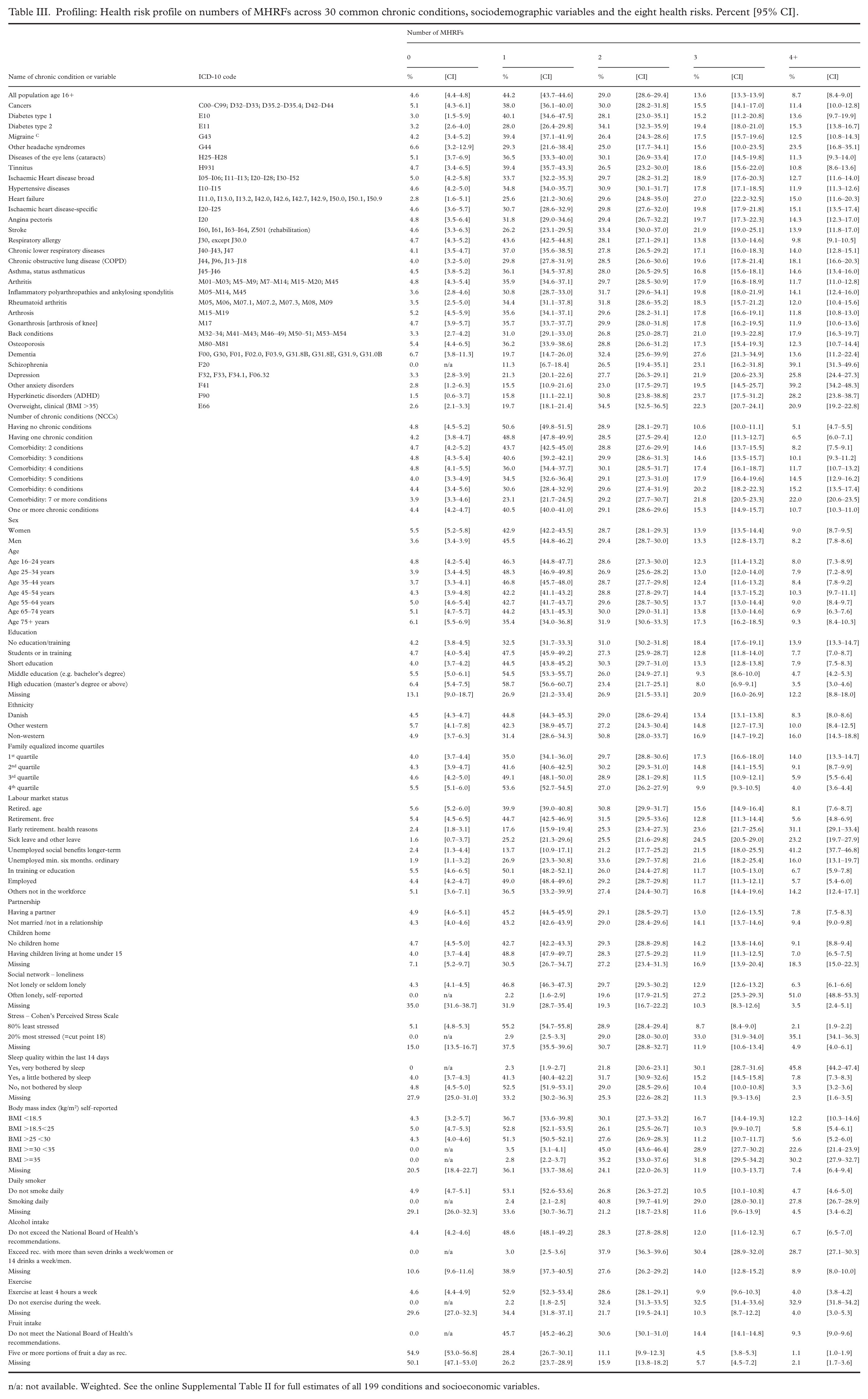
n/a: not available. Weighted. See the online Supplemental Table II for full estimates of all 199 conditions and socioeconomic variables.
There were no noteworthy sex differences, and only minor age differences were observed, showing a U shape, with the highest proportion of 4+ MHRFs occurring in the 45–54 year age group. Trends in educational achievement and income indicated that non-educated and those in lower income quartiles had a higher risk of having 4+ MHRFs. Non-western backgrounds almost doubled the risk of having 4+ MHRFs compared with Danish ethnicity (8.3% vs. 16.0%). Being longer-term unemployed, on early retirement, or sick leave was associated with some of the highest proportions: 41.2%, 31.1 and 23.2% having 4+ MHRFs, respectively.
Among the health risks, loneliness had the highest proportion associated with 4+ MHRFs, with 51.0%, followed by sleep troubles (45.8%), perceived stress (35.1%), lack of physical exercise (32.9%), obesity of BMI 35+ (30.2%), smoking daily (27.8%), and lack of recommended fruit intake (9.3%).
Supplemental Table II provides the same numbers as above but for 199 chronic conditions in line with earlier research [28].
Table IV presents a regression-based disease view of the 30 common conditions, the eight health risks, and their adjusted associations. The following merely comment on general tendencies related to the health risks, using the ‘All common conditions’ condition as an overall, combined estimate of all 30 conditions.
Disease view: logistic regression models (OR) on 30 common conditions, socioeconomic variables and health risks.
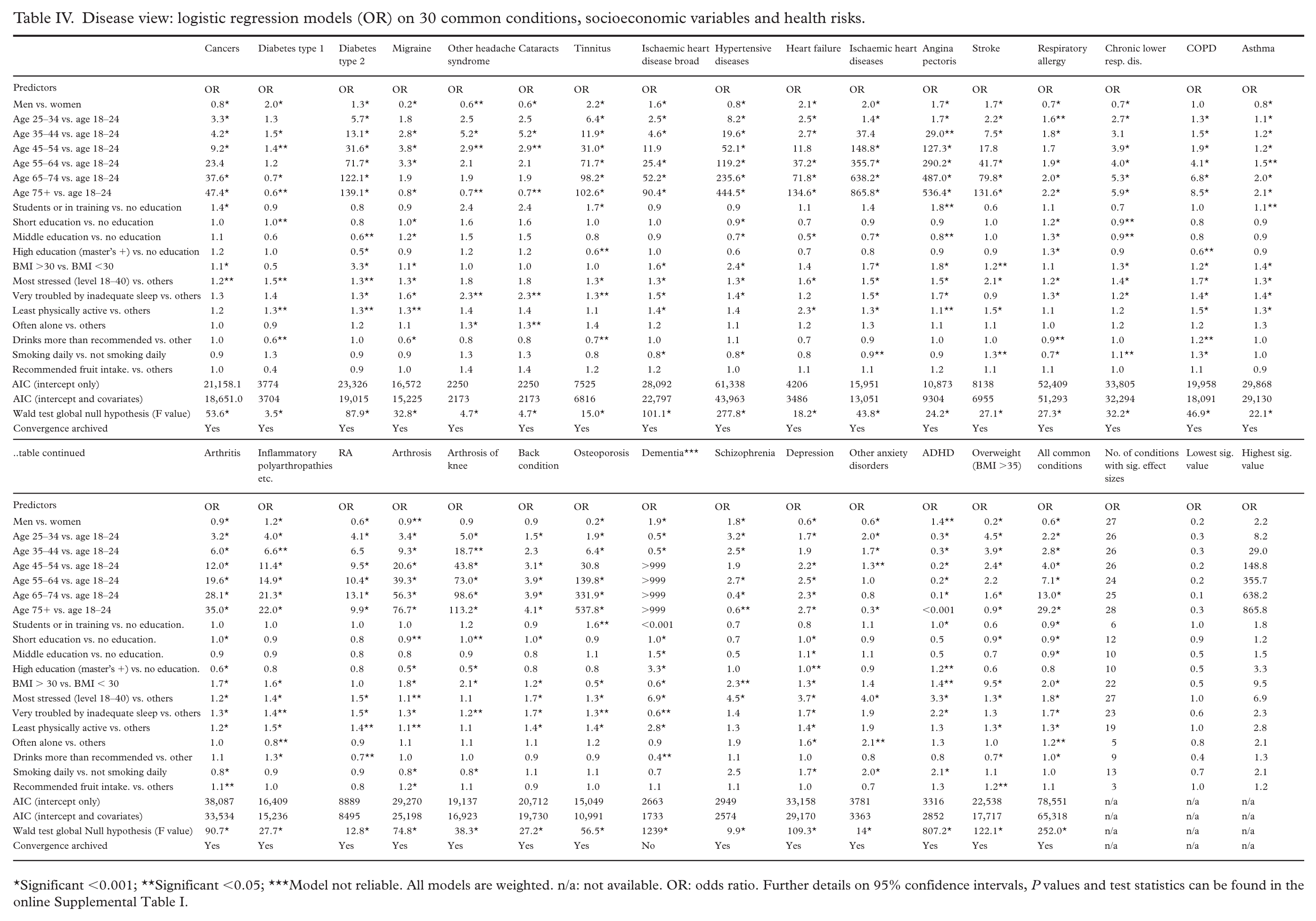
Significant <0.001; ★★Significant <0.05; ★★★Model not reliable. All models are weighted. n/a: not available. OR: odds ratio. Further details on 95% confidence intervals, P values and test statistics can be found in the online Supplemental Table I.
Obesity, stress and sleep troubles have the overall highest OR (average 1.7–2.0; see model ‘All common conditions’). However, the three health risks vary significantly across the 30 conditions. For instance, obesity ranges from OR 0.5–9.5; stress has an OR ranging from 1.0 to 6.9, and sleep troubles have an OR ranging from 0.6 to 2.3. Moreover, those three health risks also have significant associations with the highest number of conditions, with 27, 23 and 22 conditions showing significant effect sizes, respectively.
A second group of two health risks, physical inactivity and loneliness, has slightly smaller effect sizes with an overall OR of 1.3 and 1.2, respectively. While physical inactivity significantly affects sizes in 19 conditions, loneliness is only associated with five conditions, of which nearly half are mental conditions. Both physical inactivity and loneliness also vary in effect sizes across significant estimates.
Finally, a third group of health risks, including smoking, drinking, and recommended fruit intake, have the fewest significant effect sizes across the 30 conditions – 13, 9 and 3, respectively – and the smallest effect sizes. Overall effect sizes are only significant for drinking and range from 1.0 to 1.1 for the three health risks. However, smoking varies widely across the associated 13 significant conditions, ranging from OR 0.7 to 2.1. Drinking also shows varying effect sizes but for a lower and narrower range (OR 0.4–1.3), while fruit intake has a smaller range (OR 1.0–1.2).
Discussion
This study aims to analyse the associations and impact of modifiable health risk factors on the 14 aggregated disease groups and 30 common, specific chronic conditions. We aim to answer which health risks have an actual associational effect, what correlates the most, and for which conditions. By doing so, we aim to provide healthcare professionals with practical off-the-shelf resources on health risk factors across common chronic conditions and disease groups. These resources are intended to support the development of effective prevention strategies, tailored treatment approaches, and informed healthcare planning.
In summary, the findings show that multiple health risks are more common among people with chronic conditions; for instance, two or more risks are the norm for 55.1% of those with one or more chronic conditions compared with 44.5% of individuals without. This clustering of health risks may serve as a useful marker for identifying individuals at higher risk and can be applied in both clinical practice and public health to support targeted prevention and more tailored treatment strategies. These results align with previous international studies that have demonstrated strong associations between behavioural risk factors such as obesity, smoking, alcohol use, and physical inactivity and the risk of chronic disease and multimorbidity [3,6,7,11]. Our findings also extend this evidence by including psychosocial risks, confirming earlier work suggesting that stress, loneliness, and sleep problems can have health impacts comparable to, or greater than, traditional behavioural risks [9,14,17]. Similar to Fortin et al. [6] and Dhalwani et al. [7], we found that multimorbidity is particularly associated with the accumulation of several risk factors rather than single risks alone.
Finally, the findings are consistent with the most recent Danish disease burden report [65], which identified smoking, alcohol, physical inactivity, and unhealthy diet as major risk factors to disease burden. Our study adds to this evidence by showing that psychosocial risks such as stress, sleep problems, and loneliness are also strongly associated with chronic conditions. In line with the national report’s emphasis on the impact of multiple simultaneous risk factors (p. 292), we likewise found that patients with chronic conditions frequently accumulate four or more co-occurring risks.
The meta-view analysis illuminated that the health risk factors most highly and significantly associated with most disease groups were stress, obesity, physical inactivity and partly loneliness when adjusted for socioeconomic factors, although variation was observed between disease groups. The health risks least and almost not significantly associated with disease groups were drinking beyond recommendations and fruit intake. However, the disease view analysis revealed that the variation and order of significant health risks increased when analysing the individual 30 chronic conditions, multimorbidity, number of MHRFs, and the overall disease burden of having one or more chronic conditions. For example, we identified three levels or clusters of health risks based on effect sizes: The first health risk cluster – obesity, stress and sleep troubles – had the highest overall effect sizes with the highest number of distinct conditions, although varying wildly across the 30 chronic conditions.
A second cluster of two health risks with similar effect sizes – physical inactivity and loneliness – had slightly smaller and more significant effect sizes in fewer conditions, in which loneliness was explicitly associated with mental conditions.
Finally, a third group of health risks, including smoking, drinking, and recommended fruit intake, had the fewest significant and lowest effect sizes across the 30 chronic conditions. In particular, smoking varied across the associated 13 significant conditions. Drinking also showed varying effect sizes, while fruit intake had the smallest range.
Finally, the descriptive health risk profile showed that not only did all 30 common chronic conditions have more MHRFs than the average population, but the high-risk populations with 4+ health risks were proportionally more common for people with multimorbidity. Anxiety disorders, schizophrenia, ADHD, depression, headache syndromes, overweight, COPD, and back conditions showed a high proportion of 4+ MHRFs. Within the 4+ MHRFs, the most prevalent health risk ranked was loneliness, followed by sleep troubles, stress, physical inactivity, obesity, smoking, and lack of recommended fruit intake. Additionally, while other studies have found an increasing multimorbidity with age [66,67], the present study indicated minor, U-shaped age differences; and no fundamental sex differences for people with 4+ MHRFs. Finally, an educational achievement trend suggested that uneducated people had a higher risk of having 4+ health risk factors, whereas being longer-term unemployed, in early retirement and sick leave were associated with some of the highest proportions of having 4+ health risk factors.
Strengths and limitations
The study exhibits several strengths, enhancing the reliability and applicability of its findings. It leverages a high-quality dataset from diverse registers and surveys, employing a uniform methodology endorsed by WHO and scholars [2,68–71]. This ensures robust comparisons across a broad spectrum of chronic diseases, catering to the needs of healthcare planners and clinicians.
Including social aspects in the definition of health risks goes beyond traditional behavioural factors, adding depth to the analysis. Additionally, the study’s regression models offer valuable insights into the relative effect sizes of each health risk factor, disentangled from confounding associations related to sex, age, and educational achievement. These models reveal differentiated associations, shedding light on the varying strengths of connections between health risks and chronic diseases.
However, acknowledging several limitations is imperative. Challenges arise in defining ‘chronic’ due to variable interpretations [52,72,73]. Relying on register data introduces the possibility of unregistered cases, impacting the accuracy of chronic disease burden identification [29,30,52].
The temporal aspect poses a limitation as the data extend beyond a decade, and newer estimates may reflect evolving health behaviours. For instance, obesity rates have steadily increased while smoking rates have decreased [12,74]. While studies indicate such trends, it is not within the current study’s reach to assess their impact on chronic conditions.
The data analysed in this study were collected from 2010–2013. While the findings are consistent with the current general landscape, the age of the data represents a limitation. Changes in clinical practices, healthcare policies, and patient demographics since the time of data collection may influence the applicability of these results to the present day. However, as the data are identical to earlier studies in the same series [9,10,28,30,32,34], using the same data despite age also possesses a strength regarding high validity, useability and comparability when used in combination with the above-referenced studies of different aspects of disease burden.
Moreover, the study’s findings may be context-specific to the Danish population, cautioning against generalising to settings with differing cultural, healthcare, and lifestyle contexts.
Finally, as this study purely explores associations, we cannot draw conclusions about causal relationships between health risks and specific diseases. The findings should therefore be interpreted as statistical associations that may vary in strength across conditions, rather than as causal effects.
Implications for use and research
Based on a robust sample of 56,988 Danish residents, this study explores intricate associations between health risk factors and 30 diverse chronic conditions. It provides insight into health risks primarily associated with disease groups and specific chronic conditions. By revealing clear connections, including a hierarchy of clusters of health risks, healthcare planners and clinicians gain valuable insights to optimise treatments tailored to individual patient profiles or diseases.
For combatting chronic diseases, focus on health risks is crucial [75]. Based on the findings, we suggest that specific, prioritised attention is given to the identified first high-effect size clusters of health risk, including obesity, stress and sleep troubles, followed by the second cluster, including physical inactivity and loneliness. Combined with a specified focus on chronic conditions with a high number of health risks identified here, including anxiety disorders, schizophrenia, ADHD, depression, headache syndromes, COPD, and back conditions, healthcare professionals have information to guide future individual treatments and overall treatment programmes of diseases.
Furthermore, specialised healthcare professionals of individual disease areas can use the findings as an off-the-shelf catalogue for a specific disease(s) of interest. For this purpose, the present findings, the online Supplemental Table II and a related study [28] can also be utilised to acquire descriptive information on over 200 chronic conditions and their health risks.
Future research should focus on clusters of chronic conditions and identify related health risks to address multimorbidity challenges. This includes identifying specific and prevalent clusters of multimorbidity and their corresponding health risks, using appropriate statistical methods specific for this purpose not explored here [76,77]. Relatedly, future research should explore the present results by visualising the chronic conditions associated with the three clusters of health risks identified here. Finally, future research should refine treatment planning based on current and future findings.
Conclusions
The findings reveal varying and distinct associations between health risks and chronic conditions, underscoring the importance of tailored interventions considering MHRFs and chronic conditions based on a Danish sample. The findings also underpin that having high numbers of multiple health risks is more common for people with chronic conditions compared with individuals with no chronic conditions. Moreover, it identifies a hierarchy of health risks with varying significance depending on chronic conditions. The findings indicate this hierarchy of health risks impacting disease burden that may differ from common perceptions and political focus, such as less emphasis on smoking and a higher focus on psychological factors such as stress, sleep troubles and partly loneliness. However, the hierarchy also confirms the widespread focus on obesity and physical inactivity. The findings are crucial for health administrators, health professionals, decision makers, and future treatments. Future studies should aim to identify clusters of multiple high-risk factors and co-occurring chronic health conditions. To our knowledge, this study represents the most comprehensive analysis of numerous high-risk factors across a wide range of disease groups and common chronic conditions within a single framework.
Supplemental Material
sj-xlsx-1-sjp-10.1177_14034948251404093 – Supplemental material for How eight health risks and chronic conditions relate: identifying associations and profiling characteristics of multiple health risk factors among 14 disease groups and 30 common chronic conditions in Denmark
Supplemental material, sj-xlsx-1-sjp-10.1177_14034948251404093 for How eight health risks and chronic conditions relate: identifying associations and profiling characteristics of multiple health risk factors among 14 disease groups and 30 common chronic conditions in Denmark by Michael Falk Hvidberg, Anne Frølich, Pia Ryom and Sanne Lykke Lundstrøm in Scandinavian Journal of Public Health
Supplemental Material
sj-xlsx-2-sjp-10.1177_14034948251404093 – Supplemental material for How eight health risks and chronic conditions relate: identifying associations and profiling characteristics of multiple health risk factors among 14 disease groups and 30 common chronic conditions in Denmark
Supplemental material, sj-xlsx-2-sjp-10.1177_14034948251404093 for How eight health risks and chronic conditions relate: identifying associations and profiling characteristics of multiple health risk factors among 14 disease groups and 30 common chronic conditions in Denmark by Michael Falk Hvidberg, Anne Frølich, Pia Ryom and Sanne Lykke Lundstrøm in Scandinavian Journal of Public Health
Footnotes
Data availability
Data sharing is protected by the European General Data Protection Regulation (GDPR). Due to the protection of patient privacy and Danish data protection law restrictions, the combined dataset used in the current study can only be made available via a trusted third party, Statistics Denmark. This state organisation holds and controls the data used for this study. Danish scientific organisations can be authorised to work with data provided by Statistics Denmark. Such organisations can provide data access to individual researchers inside and outside Denmark. Requests for data can be sent to Statistics Denmark: ![]() .
.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The Danish National Health Survey was funded by the Capital Region, Region Zealand, the South Denmark Region, the Central Denmark Region, the North Denmark Region, Ministry of Health and the National Institute of Public Health, University of Southern Denmark.
Ethical Approval
The Danish Data Protection Agency and the Secretariat for Research Processing Records, Data and Development Support, Region Zealand, Denmark (REG-142-2021) granted permission to conduct the study. Participants provided informed consent through survey responses, as outlined in Christensen et al. [13] and Pedersen et al. [![]() ]. Statistics Denmark anonymised the data before making them accessible on their secure server.
]. Statistics Denmark anonymised the data before making them accessible on their secure server.
Supplemental material
Supplemental material for this article is available online.
