Abstract
Aim:
One-fifth of the Danish population smoke and exposure to second-hand smoke has well-documented adverse health effects. The smoking policy at hospital level prohibits hospital staff from smoking on the hospital grounds while patients and visitors may smoke in outdoor smoking cabins. This study aimed to quantify smoking at a Danish hospital and document any policy breaches.
Methods:
In April 2020, we collected cigarette butts and observed smokers at the outdoor grounds to document smoking behaviour.
Results:
In total, 7152 cigarette butts were collected during one week and 368 people were observed smoking at the outdoor grounds during four observation days. Of all collected cigarette butts, 55% were collected outside the smoking cabins and 62% of all smokers were observed smoking outside the smoking cabins. In addition, 31 staff were observed smoking.
Conclusions:
Background
One-fifth of the Danish population smokes daily or occasionally and one-fourth of all deaths are smoking related [1–3]. Three per cent of the Danish population uses e-cigarettes and about 1% smokes heated tobacco products [3]. The disease burden of smoking is higher in Denmark than in other Nordic countries [4]. This is likely to be because of the lack of an efficient tobacco control policy and a shorter history of such policies [5, 6]. Inhalation of second-hand smoke, defined by the World Health Organization (WHO) as smoke emitted from the burning end of a tobacco product or smoke exhaled by a smoker, is associated with an increased risk of lung cancer and cardiovascular diseases [7–11]. Globally, second-hand smoke exposure is estimated to cause 600,000 deaths per year, and in Denmark 2000 deaths per year [8, 9]. According to WHO, there is no safe level of second-hand smoke [10]. The second-hand smoke exposure level outside can be high close to active smokers depending on wind and distance to the smoker [12, 13].
The Danish national law on smoke-free environments prohibits indoor smoking at workplaces, but hospitals may allow patients and relatives to smoke outdoors [5, 14, 15]. Still, an increasing frequency of hospitals has introduced a smoke-free policy in which smoking is completely prohibited indoors and outdoors [16, 17]. International studies at hospitals with a smoke-free policy show that visitors, hospital staff and patients still smoke on hospital outdoor grounds but regulations can contribute to reduced smoking [18–24]. Also, international studies indicate that healthcare professionals, as well as hospitals, have a prominent role to play in tobacco control [25–27].
Aim
This study aimed to quantify smoking and policy breaches at a Danish hospital with a smoke-free policy that allowed patients and relatives to smoke in designated outdoor smoking cabins.
Methods
The smoking policy at the studied hospital prohibits hospital staff from smoking, whereas patients and relatives can smoke in outdoor smoking cabins on the hospital’s grounds. In April 2019, the daily average number of hospital admissions and outpatient visits was 2771, and the corresponding number in April 2020 was 1787.
Each day from 20 to 26 April 2020, eight locations around the main entrances were systematically cleared for all cigarette butts. At each location, cigarette butts were collected in separate bags (inside smoking cabins and associated ashtrays, and cigarette butts found outside on the ground) and were counted manually. The day before data collection started, all cigarette butts were removed from the smoking cabins and the surrounding areas. Time of collection and weather conditions were noted for each location. A Moldex 7000 Half Mask with AX filters (EN 14387), nitrile gloves, and a disposable protective suit with a hood covering the head were worn while collecting the cigarette butts (Figure 1).

Cigarette butt collector wearing a Moldex 7000 Half Mask with AX filters (EN 14387), nitrile gloves, and a disposable protective suit with a hood covering the head.
Each day from 4 to 7 May 2020, six locations near main entrances were visited twice a day between 6:45 a.m. and 9:00 p.m. for a 20-minute observation period. All smokers were counted and classified into four categories as either professional drivers (wearing a uniform or staff card), hospital staff (wearing a uniform or staff card), patients (wearing patient clothes or medical utensils), or unspecified smoker. We were not aware of objective criteria to subclassify the latter category further, for example, into visitors to patients of the hospital. For each observed smoker, location, time, weather conditions and whether a smoker was inside or outside the smoking cabins were noted. During the study period, the Danish Health Authority recommended keeping a 1 m distance when outdoor because of COVID-19. During each 20-minute observation period, we therefore registered if the smoking cabins were available without breaking the distance recommendation.
All statistical analysis was performed using Microsoft Excel 2016.
Results
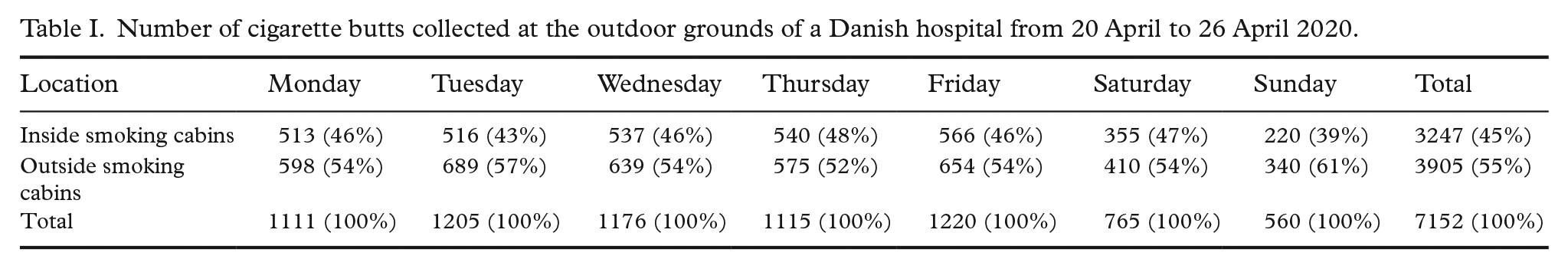
In total, 7152 cigarette butts were collected at the outdoor grounds. The majority of cigarette butts (55%) were collected outside smoking cabins (Table I). The frequency distribution (outside vs. inside smoking cabin) differed by weekday from 61% (Sunday) to 52% (Thursday). Most cigarette butts were collected on Friday (1220 cigarette butts) and the least were collected on Sunday (560 cigarette butts). In general, more cigarette butts were collected during the weekdays compared to the weekend. The weather was rather consistent throughout the week and showed no relation with the smoking pattern. On a daily average, we collected 1022 cigarette butts, which corresponds to 57% of the daily average number of 1787 hospital admissions and outpatient visits in April 2020. Most (
Number of cigarette butts collected at the outdoor grounds of a Danish hospital from 20 April to 26 April 2020.
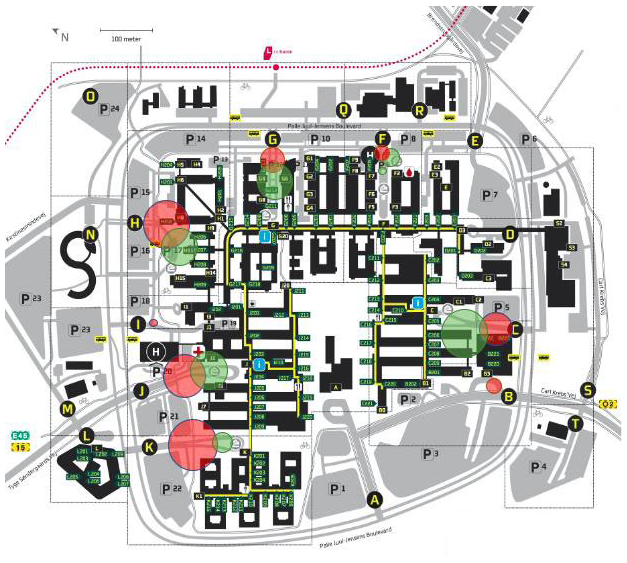
Map of the hospital showing the amount of cigarette butts collected at the different entrances.* The red circles are cigarette butts collected outside the smoking cabins, whereas the green circles are cigarette butts collected inside the smoking cabins. The size of the circle illustrates the amount of cigarette butts.
In total, 368 people were observed smoking, and the majority (62%) smoked outside smoking cabins (Table II). Out of the smokers, 47 were patients (13%), 31 were hospital staff (8%) and 290 (79%) could not be classified, while fewer than 10 were professional drivers. Most staff were observed smoking inside smoking cabins (58%) while most patients and unspecified persons smoked outside the smoking cabins (55% and 65%, respectively). In 85% of the observation periods, we registered smokers outside the cabins despite available room for smokers in the cabins without breaking the COVID-19 distance recommendation.
Number of observed smokers at the outdoor grounds of a Danish hospital from 4 May to 7 May 2020.
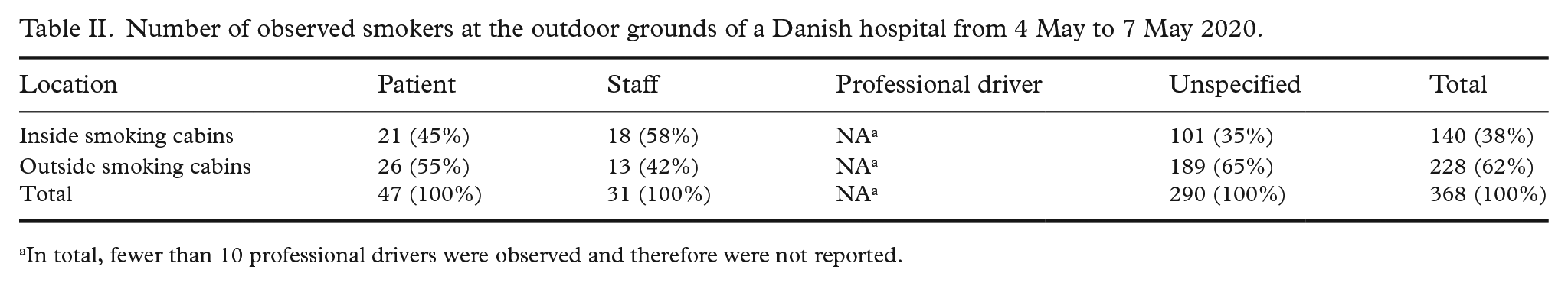
In total, fewer than 10 professional drivers were observed and therefore were not reported.
Discussion
This study shows a high number of smokers at a smoke-free hospital. More than half of all cigarette butts collected in this study were collected outside smoking cabins, and more than half of the observed smokers smoked outside smoking cabins. This is consistent with what has been seen in other hospital settings with a smoke-free policy [18–21].
This study has several strengths. The butts of each smoked cigarette are expected to have been left where smoking took place and we were, therefore, able to quantify smoking by counting the cigarette butts. The thorough clean-up of all butts before data collection started prevented any overestimation for the first study day. Our registrations of smokers were solely based on observations and classification into person categories based on predefined and objective criteria, and reporting bias cannot have affected the validity of our results as it may have in other studies [18, 21]. During the observations, we stayed at a distance and did not wear personal protective equipment (contrary to during the collection of cigarette butts) and our mere presence can hardly have influenced smoking activity. The one-week follow-up made us able to observe any tendencies across weekdays. The weather did not have an effect on the differences between the number of collected cigarette butts during the weekdays.
This study also has limitations. Other kinds of tobacco products than cigarettes were not investigated, therefore the exposure to second-hand smoke can be underestimated. However, the proportion of Danes who smoke other tobacco products than cigarettes is minor [3]. Wind may have blown cigarette butts away from where they were tossed, or cigarette butts might have been hidden. We did not investigate cigarette butts thrown into, for example, trash cans or pocket ashtrays, which would lead to an underestimation. We expected that each smoked cigarette butt was left where smoking took place, but this might not have been the case. The appropriate personal protective equipment that we used when collecting cigarette butts could have affected people’s smoking behaviour to be more conscientious, which would lead to an underestimation. Most of the observed smokers were categorised as unspecified smokers, and this group can include patients, visitors, drivers and staff. This may also lead to misclassification.
Because of the COVID-19 pandemic, the number of hospital admissions and outpatient visits during the study period was about 64% of the numbers prior to the pandemic in 2019 (1787/2771). The numbers of visitors, staff and smokers during the study period are expected to have been correspondingly lower. Our findings indicate that recommendations to keep a distance from others may in some instances have influenced people not to smoke inside the cabins. Also, people may have been afraid to gather with others in the smoking cabins during the pandemic, despite available room. Otherwise, we have no reason to believe that the distributions of cigarettes smoked and smokers across days and smoker categories were affected by the pandemic.
Conclusions
This study shows a high number of smokers at a smoke-free hospital. More than half of the smokers smoked outside the designated smoking cabins and violated the hospital’s smoking policy. The frequency of smoking outside the cabins may at least partly be influenced by the COVID-19 pandemic. Several hospital staff were also seen smoking, which is also against the policy. Healthcare professionals, as well as hospitals, should be exemplary tobacco-free role models in making smoke-free environments the norm and not the exception. Future studies should investigate why Danish hospitals still accept smoking.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
