Abstract
‘Social investment’ as an idea to justify social policy reforms has become more and more accepted in recent years and has decisively shaped agenda setting and policy formulation in European welfare states. The effectiveness of this new welfare state model, however, depends highly on the capacity to provide social services. Social services – job training, counselling and support for care work – are a key component of the social investment model. Drawing on the policy capacity approach, the article provides an analytical framework to study the ‘operational core’ of the social investment state. This implementation perspective allows us to assess whether governance actors actually have the resources to fulfil the social investment idea of enhancing citizens’ freedom to act. Empirically, the article concentrates on two selected European welfare states, Germany and France, countries with similar welfare systems but very different politico-administrative systems, and on two fields of social service provision that are addressed differently in the social investment debate: early childhood education and care (ECEC) and elderly care. Empirically, we use systematic content analysis to intensively study policy documents and secondary analyses. We show that both countries (still) lack policy capacities in these two sectors as a basis for resilient implementation of the social investment paradigm.
Introduction
Social services – job training, activation, counselling and care work – have been an important component of public social policy ever since the emergence of the welfare state. Social service provision, however, has always received much less attention than social transfers, both in the scholarly literature and in political debates (Bahle, 2008). The situation, however, has changed since the beginning of the 2000s. The EU and its Member States have reconsidered the role of social services in the welfare state, especially those services expected to ‘pay off’ as a social investment in the current and future workforce. Today, against the backdrop of diverse crises, most recently the Covid-19 pandemic, well-functioning social services are considered an essential part of the envisaged new social investment state (Esping-Andersen, 2002).
The proponents of the social investment state refuse purely functional interpretations that justify the need for social services by pointing to the increased need for labour supply to ensure international competitiveness (Hemerijck, 2018: 812). On the contrary, following their critics (cf. Bothfeld and Rouault, 2015; Jenson, 2009; Saraceno, 2015), they point out that the provision of social services such as child or elderly care also serves a goal of gender and social equality. The overcoming of social problems such as unequal division of labour, the poverty risk of single mothers, or uneven access to education has developed into a major objective of the social investment state (Plavgo and Hemerijck, 2021).
However, many preconditions must be met for successful implementation of a social investment strategy which takes these perspectives into account: such a strategy requires substantial investment in what we call the ‘operational core’ of the social investment state, that is, in the state's capacities to ensure the provision of social services in a comprehensive and resilient manner. To perform this policy function, a range of different capacities are necessary: as well as resources, competences, skills and capabilities to actually provide services, governance capacities to plan, organise and evaluate service provision are essential. The literature clearly states that high levels of capacities are linked to better policy outputs and outcomes, while capacity deficits, on the other hand, are considered as a major cause of policy failure (Howlett and Ramesh, 2015). The effectiveness of the social investment model, and in the long run also its legitimacy, thus depends on what happens in the implementation phase of the policy cycle. Against this backdrop, we ask: How has the operational core of the social investment state developed in the last two decades? And what impact does this have on social and gender equality as the main legitimising principles of the social investment state?
To answer these questions, we study social service provision in the elderly and early childhood and education care sectors in Germany and France. The operational core of the social investment state is conceptualised by drawing on the policy capacity approach (Wu et al., 2018). This approach enables us to assess the ability of providers to deliver services, as well as the ability of governance actors to plan, organise and evaluate social service provision. The following initial assumptions guide our work: first, while social services are a key component of the social investment state, they can be linked to different interpretations of this model (Bothfeld and Rouault, 2015); second, to identify the different interpretations of the social investment state, an implementation perspective focusing on capacity is required; third, to increase social and gender equality, the capacity to deliver social services and to govern delivery is necessary.
The article is divided into six parts. In the next section, we introduce the implementation perspective as the missing link in the debate about the social investment state. Section three explains how the policy capacity approach (Wu et al., 2018) is used as an analytical framework to study the operational core of the social investment state and describes the research design. In a double comparative design, we study two important fields of social service provision – early childhood education and care (ECEC) and long-term care (LTC) – in two different countries (France and Germany), to assess (changes regarding) the capacity of social service systems. It is shown (sections 4‒6) that both countries (still) lack policy capacities in both sectors. While in the childcare sector, capacity development has been on the agenda for quite some time, in the elderly care sector short-term perspectives continue to prevail. We thus conclude that the idea of a social investment state is still to be fully developed.
Theoretical framework: social services as the operational core of the social investment model
Social investment policies serve different functions (Garritzmann et al., 2022: 61; Hemerijck, 2018). First, they provide income protection and safety nets to ‘buffer’ periods of unemployment or illness. In addition to these classic (re-)distributive policies, active labour market policies, including policies of continuing education, are of vital importance to enable individuals to cope with processes of labour market transition (the ‘flow’ function). Finally, policies investing in ‘capabilities’ – to create, mobilise or preserve human skills and capabilities (improving the ‘stock’) – also play a crucial role.
The different functions of the social investment state all serve one overarching objective: to enhance citizens’ freedom to act (Hemerijck, 2018: 823). While employment participation plays a major role as a necessary precondition for this freedom, the normative groundings of the social investment model depart from both the traditional model of the Bismarckian welfare state and ideas of workfare in (neo-)liberal welfare states. Unlike the Bismarckian welfare state, the social investment state is not characterised by status preservation as a main legitimising principle, but rather by ideas of increasing social and gender equality. Unlike (neo-)liberal welfare states, access to services depends less on performance and individual achievements. Instead, proponents of the social investment model stress that investing in ‘capabilities’ not only helps to maintain the competitiveness of a national economy, but also contributes to the objective of increased female work participation, better support for other disadvantaged groups, and opportunities for an improved work–life balance (Plavgo and Hemerijck, 2021: 2).
This positive framing, however, obscures the tensions inherent in the social investment model: increasing the share of the female workforce, changing work‒life balances and securing equal social participation requires, on the one hand, the de-familialisation of care work and reproductive activities, and requires, on the other hand, the personalisation of social support to be sensitive to special needs (Hemerijck, 2018: 822). Proponents of the social investment state therefore promote a shift from financial transfers to social service provision as a main instrument of social policy. Indeed, social services are ‘critical infrastructure’ for the social investment state: they build the operational core of this welfare state paradigm.
Investment in social services, however, is a highly contested issue in most European welfare states, for several reasons (Busemeyer and Garritzmann, 2017). First, it questions the cultural underpinnings of society, i.e. the norms of the ‘ideal’ family and gender relations (Bothfeld and Rouault, 2015; Saraceno, 2015; Janson, 2009). Second, provision of social services requires – in particular in times of austerity and tight public budgets – a reallocation of resources; this differs from the traditional welfare state allocative and redistributive practices, and creates new lines of conflict within the welfare state (such as the new political divide between the older and younger generations as regards the spending of financial resources either on security in old age or on early childhood care and education). Proponents of the social investment state highlight that this and other divisions will fade in the future as the social investment state – via the provision of social services – makes it possible to prevent, or at least reduce, many social risks, or opens up ways of dealing with them in a responsible, socially just manner (Hemerijck, 2018: 824). To reach this stage, however, social services and their provision need to be resilient, i.e. social services need to be stable as well as flexibly available (Trondal et al., 2022: 24) in adequate quantity and of constantly high quality. Conflicting ideas about how to define ‘resilience’, ‘sufficient’ or ‘adequate’ quantity and quality of social services constitute a third issue in the public debate concerning investments in social services. Against this background, we study the social investment state through its operational core and analyse the capacity of social services and of the relevant governance structures. We propose that a fully developed social investment state is characterised by comprehensive and resilient social service provision. This means, in quantitative terms, that access to services is organised inclusively (rather than being stratified or targeted) in order to attain, in the longer run, a more balanced relationship between demand and supply. In qualitative terms, social services in a developed social investment state are designed to realise the potential of this model for personal capability development. For this to happen, providers of social services must have adequate resources, in particular specialised staff. The main idea of the social investment state ‒ to develop (or at least maintain) human capabilities ‒ refers not only to service users such as children and the elderly. In a similar vein, ideas of creating, mobilising or preserving human skills and capabilities are relevant for employees. We can thus assess the comprehensiveness of social investment models also by checking for the existence of appropriate human resource management and job training systems. In addition, governance in a comprehensive and resilient social investment state has good information/knowledge about client needs, service utilisation and satisfaction, continuous performance and quality control discretion to provide tailor-made services and to realise the promise of personal capability development. The adoption of a life course perspective requires well-established inter-agency cooperation (Andersson, 2018). Lastly, comprehensive and resilient social service provision requires, at the system level, governance actors with sufficient competences and resources to hold service deliverers accountable, to assess their output and outcome, and to provide the appropriate institutional framework to make inter-agency cooperation work.
Analytical framework: measuring the policy capacity of social service systems
To describe the operational core of the social investment state, we draw on the work of Wu et al. (2018) and their policy capacity approach. Policy capacity refers to the systemic and structural preconditions for implementing public policies and is defined as ‘a set of skills and resources ‒ or competences and capabilities ‒ necessary to perform policy functions’ (Wu et al., 2018: 3). While in the literature, policy capacity is often understood as the capacity of the government to make collectively binding decisions, this article – following Wu et al. – adopts a wider understanding of policy capacity, which includes the resources and governance capabilities available to implement policies within the public sector.
Wu et al.'s (2018) taxonomy differentiates between three dimensions of policy capacity – analytical, operational and political skills and resources – at three different levels: the system, the organisational and the individual level (Wu et al., 2018: 3ff.). Their aim is to provide a full picture of public policy activities. While all capacities are interconnected, they are of varying relevance for the different stages of the policy process. In this article – for the sake of comparability and to make the encompassing framework manageable – we focus on the analytical and operational dimensions at the organisational and the system level to measure the operational core of the social investment state. Political capacities are relevant to maintain trust in government and political accountability for policies; they are thus of particular importance in the agenda setting and policy formulation process. Analytical and operational capacities, in contrast, are essential for sound implementation.
Capacity at the organisational level is, in our case, the capacity of social service providers, which can be either public, non-profit or private for-profit organisations. Capacity at the system level is the capacity of governance actors, i.e. political or administrative actors at the local, state or central level.
When talking about analytical capacity, we refer particularly to processes for collecting and analysing data on client needs, service utilisation and satisfaction etc., at both the organisational and the system level. Analytical capacity also includes political activities to establish data collecting systems and evidence-based policy-making at the system level. Without analytical capacities, governance actors have difficulties observing and understanding the driving forces of instabilities, holding organisational actors accountable for their results, or adapting to fluid developments.
Operational capacities align resources with policy actions so that the policy measures agreed upon can actually be implemented in practice (Heitzmann and Matzinger, 2021). They can be measured through rules of access (inclusive, stratified, targeted?) and (im-)balances between demand and supply of social services. Next to this quantitative measure, a qualitative evaluation of operational capacities is useful to assess whether organisational and governance arrangements contribute to the overall aims of the social investment state: are the social service providers able to provide tailor-made social services? Do they have sufficient discretion and appropriate performance and accountability schemes (Andersson, 2018; Brodkin, 2011)? Is governance of the system sensitive to a life course perspective? Do institutions pay heed to transition periods in the life course of welfare state recipients and do governance actors engage in meta-governance to enable inter-agency cooperation? Table 1 shows how we operationalise analytical and operational skills and resources at the organisational and the system level.
Dimensions and levels of policy capacity
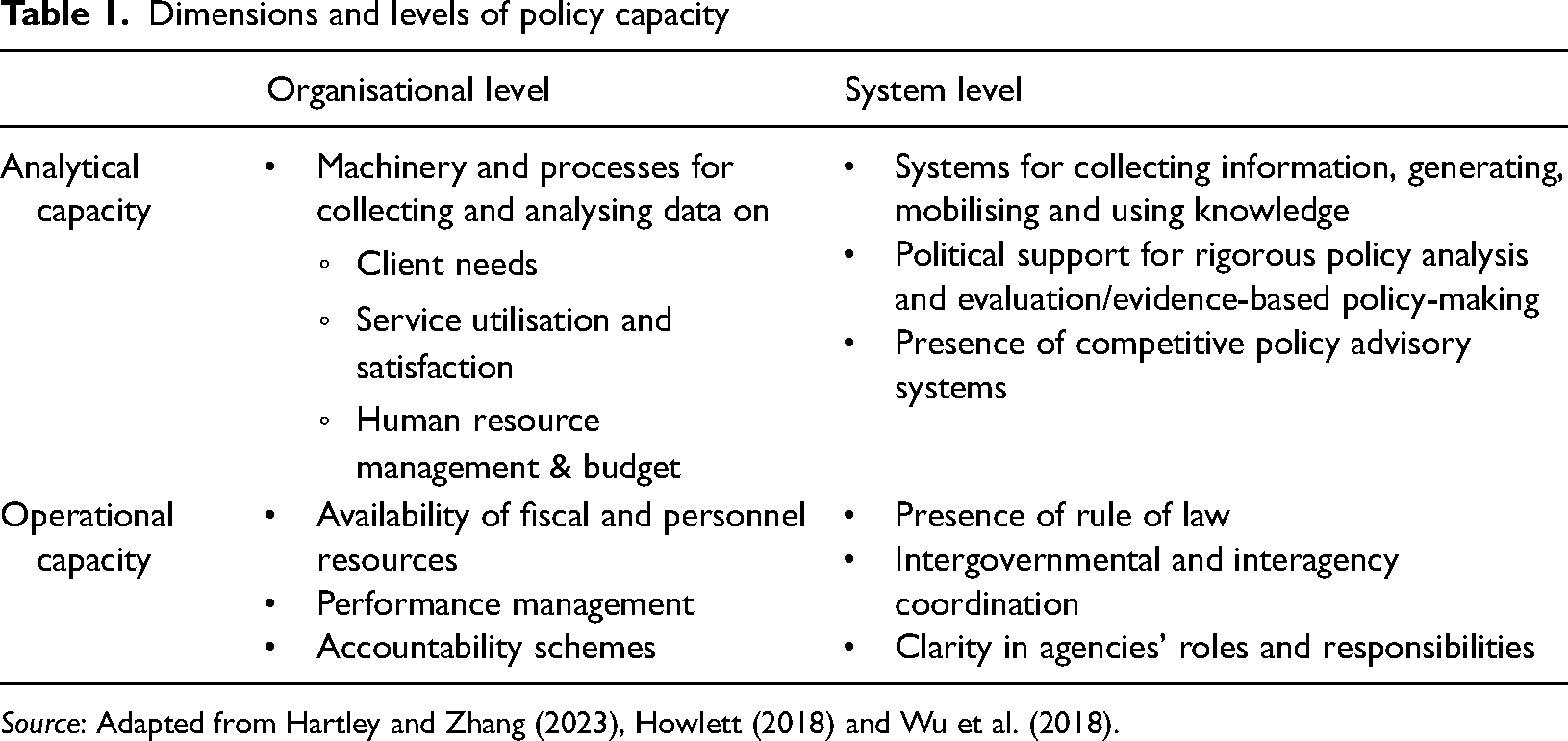
Source: Adapted from Hartley and Zhang (2023), Howlett (2018) and Wu et al. (2018).
Methods: case selection, design and data collection
For our case study, we have chosen Germany and France. These two countries – as welfare states – traditionally share some common features, while differing in terms of state organisation, which is important for the governance of social policy. Both Germany and France have in the past been classified as being Bismarckian, conservative welfare states: financial social security is organised through social insurance; social services are organised at the local level, with non-governmental welfare or charitable organisations playing a central role in the provision of services alongside the municipalities. Traditionally, a large part of social services, especially care work, have been delivered unpaid within the family, usually by women. As concerns the organisation of the state and the public administration, France has traditionally been a highly centralised state. The governance of social policy, among other sectors, has been characterised by strong public control, underpinned by extensive social consultation, with central state actors playing a prominent role at all levels. Germany, on the other hand, is a decentralised federal state. The governance of social policy (partly against the background of traditionally neo-corporatist state‒society relations) has involved cross-level and cross-sectoral co-operative coordination.
A Franco-German comparison of policy capacities and capacity development in elderly care and ECEC appears particularly interesting because it is precisely in these sectors that the traditional structures described above have (in the recent past) been broken. In France, the central state, as the core advocate of the republican ideal of education, has traditionally strongly influenced the governance of child welfare, which has for a long time contributed to the de-familialisation in this sector. In Germany, it is precisely in this sector that decentralised influences of the Länder have been decisive in the shaping of policy and the structuring of governance. In the field of elderly care, on the other hand, traditional structures still prevail in France (Van Hooren and Ledoux, 2023), whereas in Germany there has been a push towards centralisation and marketisation since 1995, against the background of the introduction of long-term care insurance.
Data to assess the (change in the) analytical and operational capacity of the social services systems in these two sectors and countries stem from secondary sources (expert organisations, scientific analyses). They have been collected via intensive desk research (Van Thiel, 2014) and have been studied with the methodological help of intensive document and secondary analysis. The period of study ranges from about 2010 – the time when the model of the social investment state was defined, especially at the European level – until today. The analysis is designed as a cross-country, cross-sector comparison. The article first analyses changes in operational and analytical capacities in the ECEC sector in both countries, before, in a second step, considering developments in the elderly care sector. Both comparisons are preceded by a brief description of the institutional conditions of social service provision in the two sectors and countries.
Social service systems in Germany and France
Early childhood education and care (ECEC)
Comparing the foundations of service provision and governance in Germany and France
Governance of ECEC in Germany follows the ideas of subsidiarity and executive federalism. In addition, the governance system reflects the major social divisions in the country. The first of these, the former border between the GDR, where childcare was considered a state responsibility, and the FRG, which left the responsibility for (early) childcare in the hands of families, especially of mothers, is still clearly visible when it comes to policy capacity. Second, considerable differences exist between the economically weaker rural areas and the prosperous metropolitan areas. Both cleavages impact the policy capacity of the field decisively.
As a result of the predominance of traditional gender roles and family models, West Germany has lagged behind in developing analytical and operational capacity in the ECEC sector. After German reunification, a transformative change could, however, be observed, and Germany has started to catch up with France and the Nordic countries. Mobilising female labour market participation (and only to a lesser extent developing children's human capital) has become a top goal for the federal government, and improving the childcare infrastructure has become the preferred solution. While capacity expansion has continued since then, it was not until the early 2000s that a profound change took place towards the social investment model, triggered by external events such as the ‘PISA Shock’ and EU policies (Employment strategy, Barcelona targets). Since then, both the idea of encouraging labour market participation (of mothers) and the aim of developing human capital (by educating children) have increasingly shaped ECEC policy-making.
Political responsibility for ECEC is divided between the national, the state and the local levels. General social rights regarding access to ECEC are defined at the national level (§ 24 SGB XIII). The responsibility for organising operational capacity (e.g. the number of places available), however, is left to the 16 states. Local communities, finally, organise the practicalities of service provision (e.g. negotiating service contracts with providers). Services are provided by public and private organisations. Unlike the long-term care sector, private for-profit organisations play only a negligible role (Statistisches Bundesamt, 2021: 12).
Unlike Germany – and most other European countries – France has long been regarded as having an outstanding example of a progressive ECEC policy (West et al., 2020), characterised by the idea of reconciling family and work (Martin, 2010), a forward-looking fertility policy (Baizan, 2021: 2, 7), and a strong focus on early education of children, which even implies compulsory schooling at the age of three. 1
The French ECEC policy has traditionally been divided into a childcare part and an early education part. For both parts, responsibilities are shared between the central state and the local level (municipalities and Départements), with the governance of early education being even more centralised than the governance of childcare policy. Concerning childcare, the municipalities, who can also provide services themselves, are responsible for organising the services in cooperation with the Départements. The Départements are responsible for the overall planning and implementation of local child and family policy, for monitoring and accrediting facilities and services, and for supporting the municipalities, for example through coordination. The central state, as the upper authority, defines the institutional rules for local governance as well as the type and amount of financial support for families and children. Support for families who use childcare is paid out upon application by the CAF (Caisses d’allocations familiales), acting as the decentralised arms of the French social security branch for families (CNAF, Caisse nationale d’allocations familiales). Concerning early education in (state or privately provided) preschools, service provision is organised by the local state school authorities in cooperation with the Départements and municipalities. Similarly to Germany, facilities in both childcare and early education are predominantly publicly funded, yet the role of private providers is more important than in Germany (DEPP, 2022: 13; DREES, 2019: Table 1).
Comparing the policy capacity of the childcare sector in Germany and France
Operational capacity
In Germany, in the last two decades, there has been a steep rise in the share of children under the age of three receiving care in childcare facilities, from 13% (in 2006) to 35% in 2020 (BMFSFJ, 2021a: 13). Two major laws – the 2005 Day Care Development Act 2 and the 2008 Childcare Funding Act 3 – have pushed the states and local communities to expand the operational capacity of early childcare services at the organisational level, in particular with respect to childcare services for very young children up to the age of three. In addition, the time children spend in ECEC facilities has increased, and opening hours have become far more flexible. However, operational capacity at the organisational level continues to show vast regional variations: in terms of availability and opening hours, for instance, childcare resources continue to be more limited in West than in East Germany (Scholz et al., 2019: 44). Furthermore, the increased operational capacity is still not sufficient to fully cover parents’ demand for early childcare services. Empirical studies estimate that there is a gap of approx. 13% between demand and actual supply (BMFSFJ, 2021a: 17), which is also a result of the lack of a skilled labour force. In parallel to the quantitative development of childcare services, a debate about ensuring high quality started in the early 2000s. Performance management (monitoring quality) takes place at the organisational level, while the guidelines for monitoring are set at the system (i.e. state) level (§ 79a SGB VIII). All 16 states have adopted standards regarding staff-to-child ratios, inspection procedures and principles for staff training; yet again, we can observe huge regional variations (Bock-Famulla et al., 2021). Moreover, while the rule of law is respected, guidelines often have the character of mere policy recommendations and are non-binding.
In France, according to the OECD, 60.4% of all children under three received childcare services in 2019 (OECD Family Database, 2022: PF3.2; West et al., 2020: 688): this is high, compared to Germany and to the rest of the EU Member States (France Stratégie, 2023). What is more, the number of childcare facilities (Établissements d’accueil du jeune enfant, EAJE), of places in childcare facilities and of childminders ‒ all indicators of operational capacity at the organisational level ‒ has grown steadily in recent years (cf. DREES, 2019: Tables 5 and 6). Within the system as a whole, the operational capacity is also high, particularly due to centralised regulation. However, coordination between the national Ministry of Social Affairs and the Ministry of Education, in charge of childcare and early education respectively, is considered to be in need of improvement (Avenel et al., 2017: 41). Lacking or weak coordination between the two ministries is considered to be one reason for the persistence of regional differences in service provision (DREES, 2019: Table 26; HCFEA, 2018: 55–58; Boyer and Martin, 2020).
As a result of the divided ministerial responsibilities for ECEC, assumptions about the quality of childcare facilities are blurred. For a long time, the quality of out-of-home and out-of-school childcare facilities for under-threes, for which the Ministry of Social Affairs is responsible, has been considered mainly from a health and safety point of view (Avenel et al., 2017: 39). In the meantime, however, the focus of the quality debate has changed to give more emphasis to the educational aspect, also promoted by quality debates at the European level (HCFEA, 2018: 28–29). Central motives behind national policy, described in the 2016 Plan d’action pour la petite enfance, reflect this change. The plan highlights the objective of creating a care environment that provides comprehensive education, including in terms of social and personal development, for all children in all facilities. It is the responsibility of the Départements to monitor the implementation of these national guidelines (Article L312-5 and R.214-2 Code de l’action sociale et des familles).
Analytical capacity
When it comes to analytical capacity, in Germany private think tanks like the Bertelsmann Foundation play a crucial role. However, there are also strong public players, such as the DJI, which is tasked with conducting systematic research in the field and advising policy actors at different levels. While, at the system level, there is political consensus that quality measures and evidence-based policy-making are absolutely essential, capacity is lacking to implement such measures. Early initiatives to introduce national quality criteria (Nationale Qualitätsinitiative im System der Tageseinrichtungen für Kinder (NQI) 1999) failed, and the minimum quality standards introduced later fell short of evidence-based recommendations (Schober, 2020: 490). For a long time, there was a considerable gap between system knowledge and turning this knowledge into activities. The most recent ‘Act on good early childhood education and care’ (‘Gute-Kita-Gesetz’), which became effective in 2019, is considered an important step forward in establishing national quality objectives. Quality goals, which aim at improving capacity at the organisational level, such as improvements in access, child-to-staff ratios, the qualifications of staff or strengthening leadership in ECEC, are at the core of the law and have for the first time been jointly approved by the federal and the 16 state governments. The duration of the law, however, is limited, and quality goals are only recommended and financially incentivised, but are not binding. It thus remains to be seen whether the law will achieve the expected outcome. The policy actors have agreed on mandatory monitoring and evaluation of the law; first results signal the persistence of regional and provider-specific quality differences, as well as limited effectiveness due to the limited duration of the law (BMFSFJ, 2021b).
In France, on both the organisational and the system levels, the analytical capacity of ECEC policy is comparatively strong. As part of their child and family policy planning and implementation tasks, the Départements regularly report on childcare provision and analyse local needs. Moreover, the Observatoire nationale de la petite enfance (ONPE), a national child and family policy analysis structure attached to and supported by the CNAF, regularly provides information on the local service provision. There are also specialised statistical and analytical agencies at the national or system level, such as the DREES (Direction de la recherche, des études, de l’évaluation et des statistiques), which is part of the Ministry of Social Affairs, and the DEPP (Direction de l’évaluation, de la prospective et de la performance), which is part of the Ministry of Education. Finally, there are the regular analyses, reports and opinions of the Haut Conseil de la famille, de l’enfance et de l’âge (HCFEA), established by the President of the Republic in 2016 and assigned to the prime minister, as well as the thematic reports from parliament and the Sénat.
Overall, the comparison shows that Germany is still lagging behind in operational capacity in the ECEC sector, despite a strong expansion of care provision since around 2008 and the introduction of quality standards. In France, on the other hand, a comparatively high level of childcare provision has been in place for a long time, also for under-threes, but the insufficient application of quality standards is a challenge here as well. In both countries, there are sufficient analytical capacities to enable the identification and targeted reaction to deficits, especially at the system level (see Table 2 on the ‘Dimensions and levels of policy capacity in the field of ECEC policy in German and France’ for an overview).
Dimensions and levels of policy capacity in the field of ECEC policy in German and France.
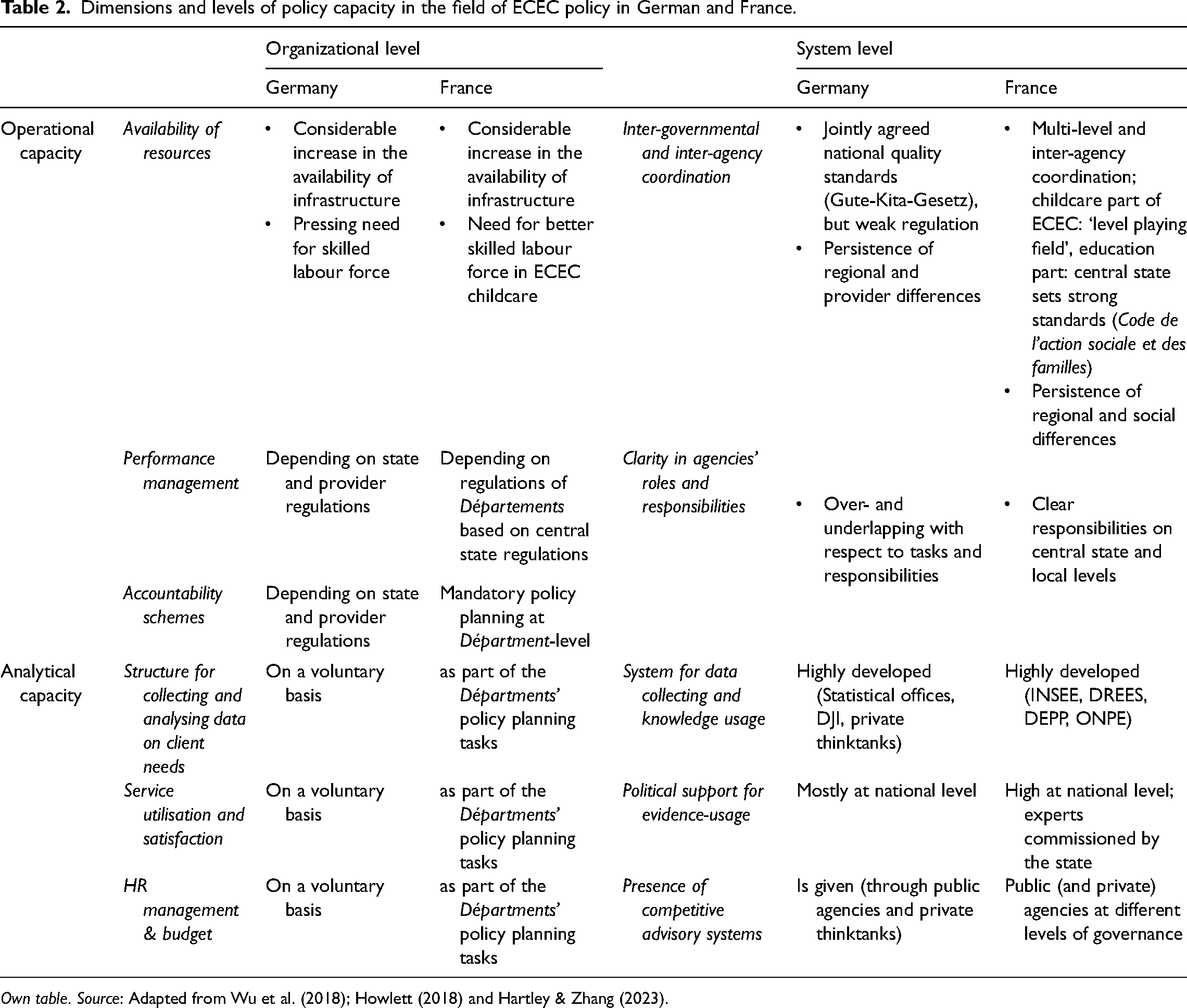
Own table. Source: Adapted from Wu et al. (2018); Howlett (2018) and Hartley & Zhang (2023).
Long-term care services
Comparing the foundations of service provision and governance in Germany and France
The German social long-term care insurance (social LTCI), established in 1995, follows the institutional design of the Bismarckian model: insurance is compulsory for wage earners and funded through social contributions on a pay-as-you-go basis. The introduction of a compulsory LTCI replaced a system in which only residual care was publicly supported (Theobald and Hampel, 2013: 119). In light of rising costs, a major goal of LTCI was to promote home care by subsidising care provision through family members and formal care provision through professionals. Accordingly, social, but also the private LTCI, provide benefits for home care (cash benefits and benefits in kind) and for care in residential facilities (benefits in kind) (European Commission, 2018: 8).
Overall, the governance of the long-term care sector can be described as rather fragmented. The fragmentation results firstly from the federalised government structure: competences for planning, decision-making, monitoring and holding implementation actors accountable are split across the different levels of the political system. Secondly, it is the result of a marketised governance structure, which encourages competition among funding agencies as well as among providers. Service provision is dominated by private organisations. While private service provision as such is nothing new in the German welfare state, the relationship between for-profit and non-profit providers has changed considerably over time: today, more than 50% of long-term care recipients in the ambulatory sector receive services from private for-profit providers. Their share is also decisive in the institutional sector, where approximately 40% of people in need of care live in private for-profit institutions (Rothgang et al., 2015: 70).
In France, the central (financing) pillar of long-term care has been, since 2002, the personal autonomy allowance (APA – Allocation personnalisée d’autonomie). The APA is a cash-for-care instrument universally accessible to all frail elderly people aged 60 or over. Approximately 70% of the financing of the APA comes from tax receipts from the Départements (counties) acting as local service and financing providers. Another approximately 30% comes from social security contributions, which are collected by the National Social Autonomy Insurance CNSA 4 and passed on to the local funding bodies. Whereas the APA finances everyday relief and support, medical care is financed from the care budget of the social health insurance. Ultimately, there are three basic financing components: ‘dépendance’ (APA), medical care and board and lodging, which flow from different sources (Libault, 2019: 11). Overall, the cost coverage is classified as insufficient by experts (Boneschi and de L’Espinay, 2022; Le Bihan and Martin, 2020). Given the constantly rising costs of elderly care, recent reforms, for example, the 2015 Act to adapt to the ageing society, 5 have been aimed at strengthening home care, especially by relatives and/or friends. While all these people are formally recognised (as ‘nearby carers’) and may – as ‘nearby carers’ – be granted additional rights to relief (e.g. ‘care holidays’), only nearby carers who are not close family relations can additionally receive a payment from the APA, whereas care work performed by close relatives (partner in a couple; daughter/son) remains unpaid.
Given the fragmented funding basis, the governance of long-term care – similarly to Germany – is also highly fragmented. While regulation takes place at the central government level, various actors at different levels are involved in the planning, organisation and implementation of elderly care policy and in the financing of care. The Départements, as the main actors at the subnational level, share their tasks, for example, the assessment and classification of degrees of care, with the regional health agencies (ARS), as devolved health policy state actors, or with the CNSA. The ARS and the Départements also share with the CNSA the task of coordinating the different service providers. As to the number of public or private (for-profit or non-profit) care services, valid data are difficult to obtain with regard to outpatient care services. 6 Overall, however, it is clear that private non-profit service providers, often independent, self-employed nurses, dominate in the outpatient sector, and that state provision only makes up a very small part (DREES, 2023).
Comparing the policy capacity of the long-term care sector in Germany and France
Operational capacity
When it comes to policy capacity in Germany, the long-term care sector has experienced impressive progress in the past two decades due to the increasing political salience of the field. The most obvious changes can be observed in terms of operational capacity on the organisational level: the number of persons in need of care and eligible for long-term care services has nearly doubled from 2,128,550 in 2005 to 4,127,605 in 2019, and a further rise is expected in light of the continuing trend of an ageing society (Flake et al., 2018). Against this background, infrastructure has been expanded, both in the inpatient sector (from 726,448 beds in stationary long-term care facilities in 2005 to 877,162 beds in 2019) and in the outpatient sector (from 10,977 ambulatory care service providers in 2005 to 14,688 service providers in 2019). More than 75% of benefit recipients (3,309,288 in 2019) are still living at home using ambulatory services. The increased availability of resources has led to increased costs. There has been a steep rise in expenses for long-term care benefits, from €4.42 bn in 1995 to €45.60 bn in 2020, not only as a result of the increasing number of people eligible for care but also due to improved service offerings (with the first and second Long-term care strengthening Acts [PSG I & II] coming into force in 2015 and 2017). The increase in fiscal resources has mainly been funded through rising contributions. While operational capacity has been increased substantially, it is still far from making the field resilient. Demand for care strongly exceeds supply. A shortage of skilled labour of about 150,000 additional employees needed by 2035 (Flake et al., 2018: 34) is a severe obstacle to improving operational capacity.
In order to cope with limited operational capacities at the organisational level, a ‘concerted action on nursing’ scheme was set up at the system level in 2019. It brings together all relevant actors in the care sector, including several ministries at the central level, professional associations and training bodies, federal states and local authorities, representatives of care recipients and their families, as well as employers, and aims at the concerted development of measures to improve operational capacity, for example regulations concerning training, remuneration, etc. (KAP, 2021).
In France, too, we can see a major growth in care supply. The number of places or beds available in inpatient facilities increased between 2007 and 2019 from 684,160 to 762,185 (DREES, 2020: Table 1; Volant, 2014: 3). In addition, the number of service providers and places offered in the outpatient sector grew between 2008 and 2018 from 2095 providers and 101,293 places offered (Bertrand and Falinower, 2011: 11) to 2125 providers and 126,600 places offered (Cour des Comptes, 2021: 17). However, the number of persons in need of long-term care with recognised entitlement to benefits rose much faster between 2005 and 2019, from 939,204 persons to 1,337,821 persons, with only 55% (805,840 in 2019) of APA beneficiaries living at home (DREES, 2022: Table A). According to the general overview ‘Le compte de la dépendance’, published by DREES, costs (including ‘dépendance’, medical care and board and lodging) rose, for the short reference period 2011 to 2014 alone, from €28.2 bn to €29.4 bn (Renoux et al., 2014: 11). That is equivalent to 0.29% of GDP private plus 1.11% of GDP public expenditure in 2014. An increase in public expenditure alone is expected in the coming decades to 1.4% of GDP in 2030 and 2.07% of GDP in 2060 (Roussel, 2017: 4). Notwithstanding the expansion of the care sector in recent years, the operational capacity of elderly care policy in France – similarly to Germany – remains insufficient. In particular, there is a glaring shortage of qualified nursing staff. Experts assess that there is an immediate need for 17,000 full-time positions in total, and estimate that the nursing sector will need 150,000 to 200,000 additional full-time positions by 2030 (Libault, 2019: 40). Against this backdrop, the resilience of the system is (still) poor, notwithstanding the increase in available resources and capacities.
Turning to the system level, the already mentioned fragmentation and overcomplexity of governance and a simultaneous lack of coordination among the relevant actors are central obstacles to building operational capacity and to being on the way to a resilient ‘future-proof’ elderly care system (cf. Le Bihan and Martin, 2020: 14; Libault, 2019). Although the Départements are equipped with far-reaching competences for capacity planning and policy implementation, 7 the governance of elderly care policy is nevertheless comparatively hierarchically structured, and the central state intervenes in local planning and implementation through various devolved agencies.
Analytical capacity
In Germany, developments in analytical capacity over the last two decades have been less pronounced, and the overall capacity is rather limited. On the organisational level, service providers are not obliged by law to collect and analyse data on client needs and satisfaction, service utilisation or human resource management and budgets. The machinery of data collection is further hampered by the structure of the long-term care industry. The ambulatory sector in particular is dominated by small and very small businesses with only semi-professionalised customer satisfaction or performance management systems.
On the system level, analytical capacity has been strengthened through two recent reforms to improve the quality evaluation and publication system. First, a new board (Qualitätsausschuss Pflege), representing all relevant stakeholders in the quality of care, has been set up to continually assess quality standards. Second, a reform in 2020 8 was aimed at bringing more clarity into the roles and responsibilities of the quality assessment agency (MDK - Medical Review Board of the Statutory Health Insurance Funds) by increasing its organisational autonomy and separating more clearly the role of funding agencies from that of quality assessment agencies. Overall, abundant data are collected by the statistical offices (Statistisches Bundesamt, 2021), by local communities and ministries at the state level (local or state long-term care reports), insurance agencies and scientific institutions.
In France, analytical capacity at the organisational level is rather complex. Three actors – the Départements, 9 the CNSA and the ARS – share the task of collecting and documenting information on the locally available supply of care services. Obviously, a lack of data and documentation is not the problem, but it is problematic to turn the large amount of available knowledge into practical measures. Against this backdrop, a lack of ‘readability’ (‘lisibilité’; Libault, 2019) of care policy activities on the ground has been identified, leading to permanent coordination deficits (Libault, 2019).
With regard to the system level, a similar picture emerges. There are numerous structures that regularly collect, analyse and publish information, for example, the CNSA, DREES and the National Court of Auditors (Cour des Comptes). These structures are an expression of the system's analytical capacity, which has been strong for years. However, only recently, with the preparation and publication of two national policy reports (Libault Report, 2019; El Komrhi Report, 2019; Borgetto, 2021), commissioned by the prime minister, has it been possible to bundle the widely available information into a consistent analysis and to use it as a basis for the formulation of a national policy strategy (‘Ageing well at home’ or ‘Bien vieillir chez soi’).
Altogether (Table 2), the comparison shows that in the field of care, both in Germany and ‒ in this sector ‒ also in France, an increase in supply has taken place in the past two decades, which, however, does not even come close to covering the demand in either of the two countries. Both countries face the challenge of recruiting skilled workers. In addition, the installation and systematic use of quality management mechanisms is in its infancy in both countries, even if – in France more strongly than in Germany – analytical capacities have been expanded in the (recent) past, both at the operational and at the system level (see Table 3 on the ‘Dimensions and levels of policy capacity in the field of long-term care in Germany and France’ for an overview).
Dimensions and levels of policy capacity in the field of long-term care in Germany and France.
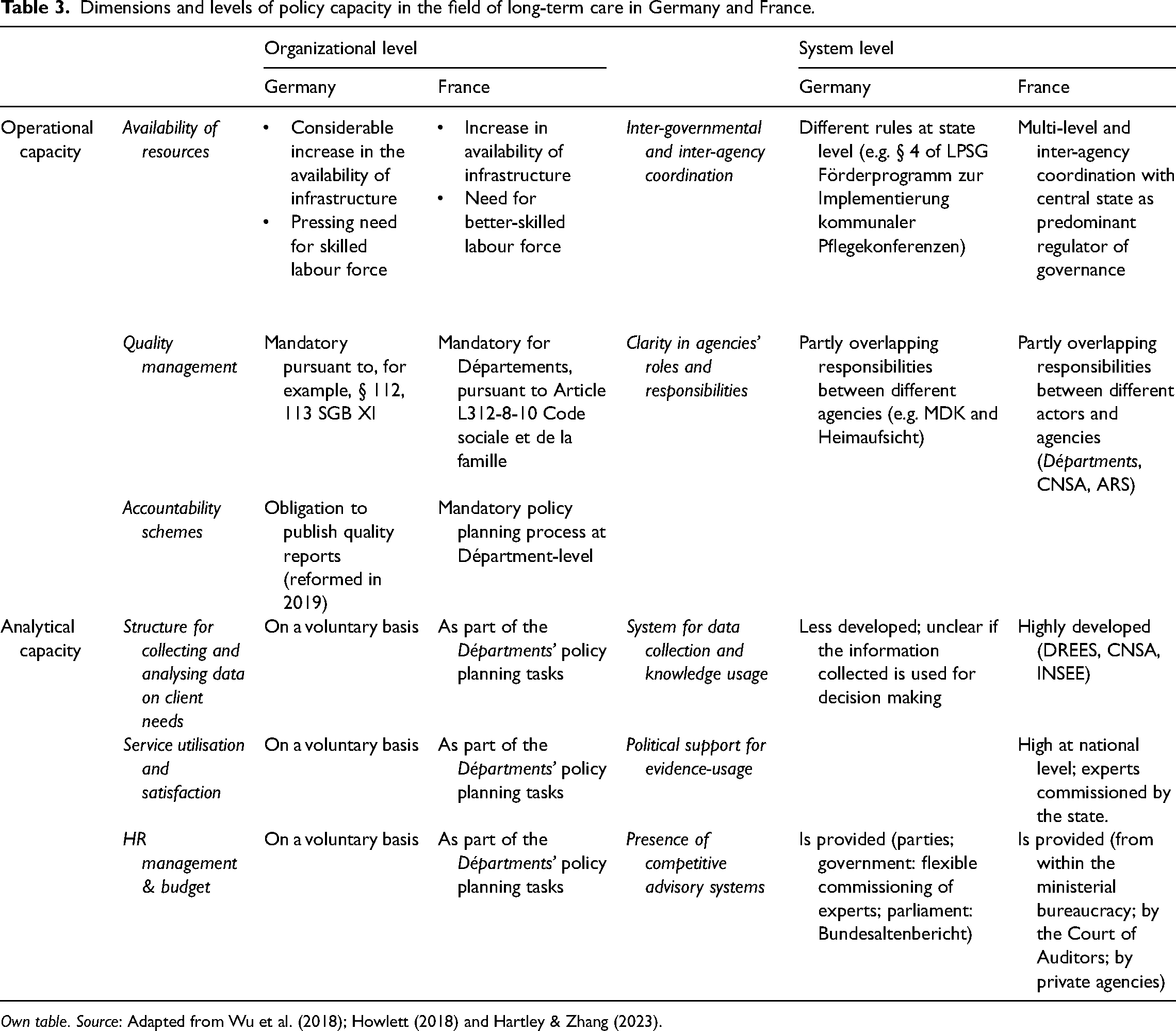
Own table. Source: Adapted from Wu et al. (2018); Howlett (2018) and Hartley & Zhang (2023).
Discussing the status of policy capacity of the social service systems in Germany and France
When comparing the developments in the two sectors and in the two countries, we can observe similarities and differences in terms of the evolution and status of policy, notably operational and analytical capacity. From a cross-sectorial perspective, the analysis has shown that the development of operational and analytical capacities in the childcare sector is more advanced than in the long-term care sector. Both countries, France and with some reservations Germany, where this is a rather new development, have comparatively advanced analytical capacities in the childcare sector and the long-term care sector. In both countries, this is particularly true at the system level, at which policy measures are decided. At the organisational level, where these measures are implemented, there is a formal system of information collection and processing, especially in France. What appears to be problematic is turning the vast amount of data into meaningful information and processing it into sound policy solutions. The expansion of analytical capacities at the system level could become an important impetus for further reforms that place more emphasis on the quality of care than on mere quantitative capacity expansion, and on the implementation of the social investment goals of social and gender equality. A first approach in this direction may be seen in France in the recently envisaged care reform. However, it is too early to assess whether a comprehensive increase in capacity will really happen. In addition, recent privatisation and re-familialisation trends, especially in the elderly care sector, have perpetuated quality concerns and reinforced gender inequalities in both countries. Recent legal approaches to counteract this, for example by recognising family care-work and relieving the burden on mostly female family carers, do little to counter this development.
The lack of ability (and/or of political willingness) to use evidence for public policy-making became obvious during the Covid-19 crisis. In the early months of the pandemic, Germany in particular had difficulties developing solutions that went beyond strict closure strategies, which are undesirable from a social investment perspective due to their detrimental effects on both gender equality and the well-being of children and the elderly (Blum and Dobrotić, 2021). The pandemic experience has clearly brought to light that social services are not yet considered as critical social infrastructure. In both countries, the impact of crisis management measures on the child- and long-term care sectors was only taken into consideration in a second stage. In line with various contributions to the current academic and public debate, we interpret the preferred treatment of the interests of economic actors compared to the interests of recipients of social services as a sign that in both countries a rather narrow understanding of the social investment state still prevails (cf. Palier, 2020).
In non-crisis situations too, however, the limits of policy capacity have become obvious in the two sectors in the two countries. This is true in particular for operational capacity. Regarding the childcare sector, France seems at first sight to be particularly well positioned. There has been an expansion of childcare facilities for years, and France has long occupied a top position in this area compared to other European countries. In Germany, the expansion of capacity, especially for the care of children under the age of three, has picked up speed only in the recent past. It is interesting to note that, until only recently, the social investment idea was interpreted from a rather short-term perspective in Germany: the expansion of childcare facilities was considered to be an instrument to make more effective use of the female labour force to spur on economic development. In France, however, other motives as well, i.e. population and fertility development and – more recently – the motive of investing in children's futures, have long been in the foreground. Interestingly, the (rather old) idea of investment in children – in contrast to the interpretation of this idea prevalent in the social investment state – does not first and foremost have the future labour force in mind. Rather, state investment in children's education as a primary instrument to realise the republican ideal of equality has long been a core motive of French education policy (cf. Mattei and Aguilar, 2016). The fact that the French welfare state has, to date, only been partially successful in achieving this goal is shown by persistent social inequalities in the use and usability of child education services for all members of society.
In the elderly care sector, too, strong expansion of operational capacities (in both the inpatient and outpatient care infrastructure) can be observed in both countries in the recent past. This expansion is even more striking in Germany than in France, where there are shortages in the supply of services, especially in outpatient care for the elderly. In both countries, the recognition of care work within the family, i.e. predominantly female care work, not only ideally but also materially and through targeted relief and support (e.g. training opportunities), is a recent development. All in all, however, such developments have not contributed to building up a sufficient, let alone resilient, supply of social infrastructure in the elderly care sector. In fact, there is a strong imbalance between demand and supply. A central problem in this context is the glaring lack of qualified personnel, which affects the care sector in both countries.
From the very beginning, the evolution of the social investment model has been accompanied by a critical debate (e.g. Garritzmann et al., 2022). Scholars are concerned about the strong orientation towards the norms and values of the (neo-)liberal model of the welfare state and the lack of a critical stance regarding the exploitative mechanisms of capitalist societies (de la Porte and Natali, 2018; Umbach and Tkalec, 2021). Our analysis shows that these concerns are justified – not necessarily with respect to the overarching idea of the social investment state, but with respect to its realisation in two countries in two fields. Particularly from a gender and social equality perspective, the social investment state is ambiguous and leaves ample room for interpretation. Our analysis of the analytical and operational capacities of the social investment state shows that there are unresolved issues with regard to ensuring a consistently adequate quality of social service provision as an important basis for a resilient, crisis-proof system. The lack of resilience in the elderly care sector was most recently evident during the Covid-19 pandemic, both in Germany and in France. Indeed, the pandemic has shown that social service provision is a critical infrastructure at least in two respects: social services are necessary to keep things ticking over even in major crises, but also because their lack of analytical and operational capabilities results in a lack of resilience. Poor resilience, again, makes them a vulnerable field of public policy, where service provision can easily collapse in situations of external turbulence.
This experience of poor resilience has helped to bring the question of social service governance onto the policy agenda as a pressing issue. Our analysis thus confirms earlier research that has shown that governments largely maintain their commitment to expanding the quantity and quality of social services, even in situations of crisis (Bothfeld and Rouault, 2015, 80). Overall, the pandemic has functioned in both countries as a (co-)trigger for reforms, in the sense of public investment in the care sector. In the context of this article, however, it is also important to state that the idea of ‘social investment’ has played no explicit role in these reforms, in either Germany or France.
With respect to the financial crisis in 2011, Bothfeld and Rouault (2015, 81) have convincingly revealed that ‒ irrespective of formal commitments ‒ disinvestment in social services served as a mechanism to cope with post-crisis budget constraints. Since the financial crisis of 2011, disinvestment has been practised in a hidden way by ignoring former principles of equality or solidarity and taking a more selective approach. A decade later, after the Covid-19 pandemic experience, we cannot yet confirm whether the same has happened. Instead, a positive observation from our analysis is that in both countries, increased attention is being paid to social inequalities in access. Specific qualifications of staff and awareness training, and improved analytical capacities at the organisational level, are considered an effective remedy. However, against the backdrop of severe staff shortages, these strategies show only limited effects. As a result, territorial inequalities in the distribution of operational capacities, notably in the childcare sector, are exacerbated and are proving to be a serious obstacle to the achievement of a resilient social investment state in both countries. Obstacles to (full) realisation of the underlying ideas of the social investment model – providing tailor-made social services to enable citizens to cope with periods of unemployment and with turbulent transitions throughout their life course – are also the result of a lack of collaboration within and across policy sectors.
Conclusion
The core concern of this article has been to study how social service systems in two selected European welfare states, Germany and France, have developed since 2010. The analysis was driven by a wish to assess the extent to which the two countries under consideration were able to build or to expand the necessary capacities for a social investment state. To answer this question, we used the policy capacity concept of Wu et al. (2018), with a special focus on the analytical and operational capacities at the organisational and the system levels of policy capacity, and thus on the dimensions that are most decisive for sound and coherent implementation arrangements.
The study makes both an analytical and an empirical contribution to the literature. It advances our understanding of the operational core of the social investment state, by developing an analytical framework to explore a set of resources, competences and capabilities necessary to perform social investment policy functions. We started from the initial assumption that, while social services are a key component of the social investment state, they can be linked to different interpretations of the social investment model ‒ which again have an impact on social and gender equality. Our analytical grid allows us to detect the variance in the analytical and operational capacities of social service systems in different countries in different sectors. These differences regarding, for example, systems for data collection and evidence-based decision-making (analytical capabilities) or interagency coordination (operational capacity), enable us to draw conclusions as to what extent ‘social investment’ is really connected to the idea of ‘enhancing citizens’ freedom to act’.
Our empirical analysis of the capacities of social service systems in two sectors in two countries shows that the idea of a social and gender equality-enhancing social investment state has indeed shaped agenda setting and decision-making in both countries. Yet, its influence on the implementation phase is still limited. Even though policy capacity has been expanded considerably in both countries in both sectors, the set of skills, resources, competences and capabilities are still insufficient to bring about the evolution of a social investment state which enhances ‘citizens’ freedom to act’. On the contrary, limited capacities – for example, staff shortages at the organisational level or limited capacities at the system level to plan and manage implementation – are creating new or reinforcing existing inequalities in access to or the quality of social services, and may threaten the legitimacy of the social investment model in the longer run.
All in all, the role of social services in the overall resilience of Western societies is still underestimated, even their role in serving labour supply and human resource development. Judging from the current policy capacity of the social service systems in Germany and France, we thus conclude that the idea of a social investment state is yet to be fully developed.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
