Abstract
Background
Alzheimer's disease (AD) and mild cognitive impairment (MCI) cause progressive cognitive decline, with Western medicine only alleviating symptoms at present. Acupuncture shows potential for these disorders, but existing studies have inconsistent results.
Objective
To examine the effect of acupuncture on overall cognitive function in patients with AD and MCI via meta-analysis.
Method
Literature from six databases on acupuncture, AD, and MCI was searched. Meta-analyses and moderator analyses were performed using Comprehensive Meta Analysis V3.0.
Results
52 randomized controlled trials (RCTs) involving 3362 AD/MCI patients were included. Results showed that acupuncture alone outperformed blank or placebos (SMD=1.09, 95% CI = [0.60, 1.58], p < 0.001, I2 = 91.39%). In addition, acupuncture alone (SMD = 0.45, 95% CI = [0.22, 0.67], p < 0.001, I2 = 69.38%) and combined with Western medicine (SMD = 1.18, 95% CI = [0.92, 1.44], p < 0.001, I2 = 90.73%) were superior to Western medicine alone. Moderator analysis revealed significant effect of type of patients, showing larger effect in AD than MCI in acupuncture combined with Western medicine (Q = 10.20, p = 0.001). Regarding types of acupuncture, manual acupuncture (MA) and electroacupuncture (EA) showed no significant difference between them (alone: Q = 0.38, p = 0.536; combined with Western medicine: Q = 0.57, p = 0.449) and both outperformed Western medicine alone.
Conclusions
Acupuncture could improve overall cognitive function in AD and MCI, with similar effects between MA and EA. Due to the heterogeneity and variable methodological quality of the studies included, our results must be interpreted with caution. Still, these results suggest acupuncture may be an adjuvant to Western medicine for eligible patients and a potential alternative for short-term cognitive improvement when Western medicine is contraindicated.
Keywords
Introduction
Alzheimer's disease (AD) is a neurodegenerative disorder characterized by gradual cognitive decline and the most common cause of dementia. 1 Mild cognitive impairment (MCI) refers to cognitive function below normal aging levels (not meeting dementia diagnostic criteria) and an intermediate state between normal aging and dementia. 1 A Chinese national cross-sectional study reported a 6.04% dementia incidence and 15.54% MCI prevalence in adults over 60 years 2 ; a Mayo Clinic aging study found 10.0% dementia and 16.0% MCI prevalence in those aged 70–89 years. 3 AD imposes a heavy burden on patients, caregivers, and healthcare systems, with economic costs rising markedly as the disease progresses. 4 While early diagnosis is critical for AD management, no effective drugs to halt or reverse AD progression have been developed to date, even for early-stage cases. 5 Consequently, non-pharmacological interventions for preventing cognitive decline and dementia have become a key clinical research hotspot.6–9
Among these non-pharmacological interventions, acupuncture is a core traditional Chinese medicine therapy with a millennia-long history, well established for its role in disease treatment and health promotion.10–14 It aids post-stroke hemiplegia rehabilitation, 11 improves post-stroke depression, 12 alleviates rheumatic diseases symptoms 13 and mitigates chronic fatigue syndrome fatigue. 14 Gaining global attention in recent decades,15–18 acupuncture has emerged as an effective adjuvant therapy for MCI and AD, with clinical evidence confirming improved cognitive function and quality of life in patients.19–21 A review of animal studies has further delineated multi-faceted neuroprotective mechanisms of acupuncture in AD. These include acupuncture-induced regulation of abnormal brain protein expression, acupuncture-mediated modulation of microglial physiology and pathology, acupuncture-based regulation of mitophagy and epigenetic modifications, acupuncture-enhanced synaptic plasticity, and acupuncture-driven mitigation of oxidative stress coupled with energy metabolism. Together, these mechanisms underpin acupuncture's beneficial effects in ameliorating cognitive symptoms in affected individuals. 22
Unlike pharmacological therapies, acupuncture is a complex intervention influenced by multiple factors. Rooted in traditional Chinese medicine's “syndrome differentiation and treatment” principle, core variables influencing acupuncture efficacy include treatment type (e.g., acupuncture alone or combination with drugs), techniques (e.g., electroacupuncture (EA), manual acupuncture (MA), and manipulations like lifting-thrusting, twisting, rotating), acupoint selection (e.g., Baihui, Fengchi, Sishencong, Taixi, Dazhui, Zusanli, Yongquan, etc.), and their combinations. 23 These factors potential challenges for formulating standardized acupuncture protocols and evaluating therapeutic effects.
This study aimed to perform a meta-analysis of randomized controlled trials (RCTs) on acupuncture for AD and MCI, evaluating its effect on the cognitive function of patients with AD spectrum disorders. Building on preliminary evidence confirming acupuncture's efficacy for cognitive impairment, while the influence of specific intervention parameters remains unclear, this meta-analysis further investigates how stimulation types (MA, EA) and different stages (MCI, AD) affect outcomes. The goal is to inform the development of auxiliary acupuncture protocols for AD spectrum disorders and provide a theoretical foundation for the clinical application of traditional Chinese medicine-based acupuncture.
Methods
This study was conducted in accordance with the PRISMA guidelines (https://www.prisma-statement.org). Literature searches were performed across multiple databases: Web of Science, PubMed, Cochrane Library, Embase, Wanfang Medical Network, and China National Knowledge Infrastructure (CNKI) from their inception to May 01, 2025. Combined MeSH Terms (e.g., “Alzheimer Disease”, “Cognition”, “Cognitive Dysfunction”, “Acupuncture”, “Acupuncture Therapy”, and “Electroacupuncture”) and Free Terms (e.g., “Alzheimer's Diseases”, “Cognitions”, “Cognitive Function”, “Mild Cognitive Impairment”, “Acupuncture Treatment”, and other relevant free terms) were used. The Chinese versions of the above keywords were used for Wanfang Medical Network and CNKI. The detailed search strategies in English and Chinese databases were illustrated in Supplemental Material S1. Two authors conducted the searches independently, cross-verified results, and resolved discrepancies through a third author before initiating literature screening. The study was registered on PROSPERO (CRD420251045566).
Inclusion and exclusion criteria
Literature screening followed the PICOS framework, with specific inclusion criteria and exclusion as below:
Inclusion criteria
Study Population: Patients (either with AD or MCI) were diagnosed by clinical physicians and met the following criteria:
For AD: general classification standards (the Chinese Classification and Diagnostic Criteria for Mental Disorders (CCMD-3), 24 International Classification of Diseases (ICD-10), 25 Diagnostic and Statistical Manual of Mental Disorders (DSM-IV/5) 26 ), or AD-specific international criteria (National Institute on Aging-Alzheimer's Association (NIA-AA), 27 National Institute of Neurological and Communicative Disorders and Stroke-Alzheimer Disease and Related Disorders Association (NINCDS-ADRDA), 28 International Working Group (IWG-2), 29 relevant AD sections of the 2018 Chinese Guidelines for the Diagnosis and Treatment of Dementia and Cognitive Impairment30,31), or traditional Chinese medicine diagnostic standards for AD32–40;
For MCI: MCI-specific criteria (Petersen's criteria,
41
the Jak/Bondi 2014 criteria,
42
guidelines for MCI clinical research,
43
relevant MCI sections of the 2018 Chinese Guidelines
44
), or some traditional Chinese medicine diagnostic standards for MCI32,33,35,45;
2. Intervention: Experimental group: acupuncture alone or in combination with one of the following Western medicines (donepezil, rivastigmine, galantamine, memantine, or huperzine A). Control group: placebos (placebos needles, stimulation at non-acupoints, oral placebos), blank control (no treatment), or one of the aforementioned Western medicine alone; 3. Outcome measures: At least one scale assessing overall cognitive function: Mini-Mental State Examination (MMSE), Montreal Cognitive Assessment (MoCA), Alzheimer's Disease Assessment Scale-Cognitive Subscale (ADAS-cog), and Hasegawa Dementia Scale (HDS); 4. Study Design: RCTs.
Exclusion criteria
Animal experiments; Ineligible participants: patients with cognitive impairments caused by non-AD/MCI diseases (e.g., traumatic brain injury, Parkinson's disease, vascular dementia, frontotemporal dementia), or unrelated diseases (e.g., fibromyalgia, autism, cancer); Methodologically/typologically invalid studies: non-RCTs, reviews, retracted articles, literature lacking results (e.g., editorials, conference abstracts, trial protocols), or non-full-text articles, or non-Chinese/English literature; Non-compliant interventions (e.g., point injection, laser acupuncture, or tap-pricking); Outcome measures do not include any of the four scales (MMSE, MoCA, ADAS-cog, HDS).
Study selection
The literature screening process is illustrated in Figure 1. Retrieved studies were imported into the NoteExpress V4.1, where duplicates were removed using the software's built-in duplicate-checking function. Subsequently, YFC and SGZ independently screened titles/ abstracts against the inclusion/ exclusion criteria to excluded irrelevant studies, followed by full-texts review of the retained articles. After independent screening, the two authors cross-validated their results; any discrepancies were resolved through discussion with the corresponding author (PPL) to reach consensus.
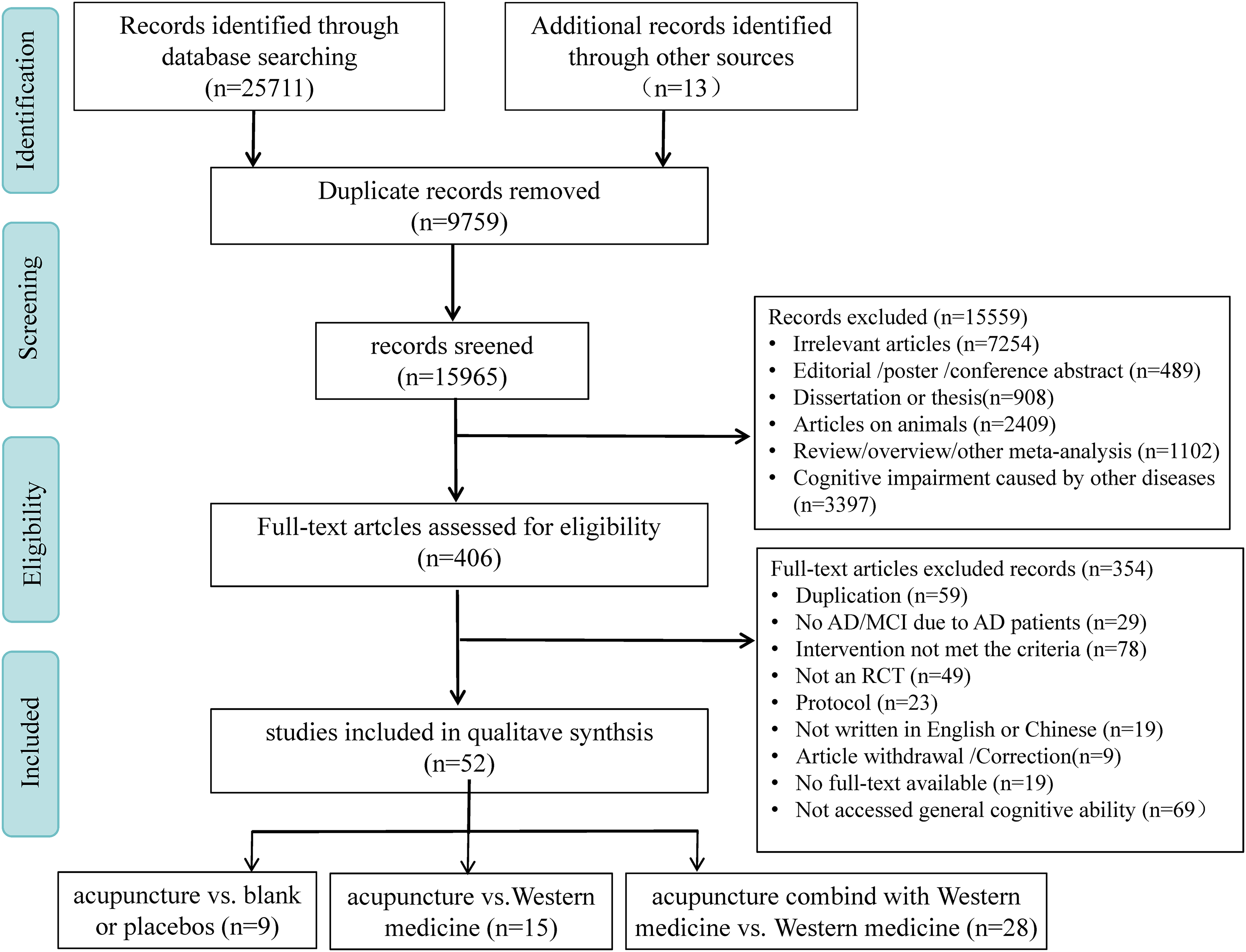
Literature screening process.
Data extraction
Data extraction covered first author, language, study characteristics (publication year, patient type, diagnostic criteria), participant characteristics (sample size, mean age, disease duration), intervention details for both the experimental and control groups, and the outcomes measures. If data were incomplete, we attempted to contact the original study's corresponding author to obtain complete information. Two authors independently extracted data using a predefined form, with any discrepancies resolved through discussion with the corresponding author.
Study risk of bias assessment
Study quality assessment followed the Cochrane Handbook for Systematic Reviews of Interventions (http://handbook.cochrane.org/), covering seven domains including random sequences generation, allocation concealment, blinding of participants and personnel, outcome assessment blinding, completeness of outcome data, selective reporting, and other biases. Risk of bias was categorized as “low risk of bias”, “unclear risk of bias”, or “high risk of bias”. Two authors independently evaluated study quality to ensure the rigor and accuracy of bias assessment; discrepancies were resolved via discussion between the two authors or by a third author. Bias analysis results were visualized using the Cochrane Risk of Bias Tool in Review Manager 5.3 (https://training.cochrane.org/online-learning/core-software/revman).
Statistical analysis
For continuous variables, effect size were calculated using the means and standard deviation, quantified as standard mean difference (SMD) with a 95% confidence interval (CI). Meta-analysis was performed in Comprehensive Meta-Analysis version 3.0 (https://zh.meta-analysis.com) with a significance level of p < 0.05.
Heterogeneity was assessed via the Cochran Q test and I2 statistic, with a random-effects model was used in cases of high heterogeneity (I2 ≥ 50%, p value of Q test < 0.05), and a fixed-effects model used when heterogeneity was low (I2 < 50%, p value of Q test ≥ 0.05). Publication bias was evaluated using Begg's test, Egger's test, and funnel plots, with the trim-and-fill procedure for correction. The fail-safe N (additional zero-effect studies needed to negate significant result) was calculated to assess publication bias. With k as the number of included studies, a fail-safe N > 5k + 10 (a threshold requiring far more additional zero-effect studies to nullify significance than k) indicated the pooled effect size was robust to publication bias.
Sensitivity analysis was performed in Stata 15 by sequentially excluding individual studies to detect sources of heterogeneity. Studies were identified as a potential source requiring further analysis if, upon their exclusion, the 95%CI significantly deviated from the original range or if the I2 statistic showed a significant decrease. To further explore heterogeneity, predefined moderator (subgroup) analysis was conducted, with classification criteria including patient type (AD vs. MCI) and acupuncture method (MA vs. EA).
Results
Study screening
A total of 25,711 articles were identified from database searches. Following literature screening (Figure 1), 52 articles46–97 were included, categorized into three comparisons including acupuncture vs. blank or placebos (n = 9), acupuncture vs. Western medicine (n = 15), and acupuncture combined with Western medicine vs. Western medicine (n = 28). The characteristics of the included studies are presented in Table 1, encompassing 3362 participants (2498 with AD; 864 with MCI).
Basic characteristics of the included studies.
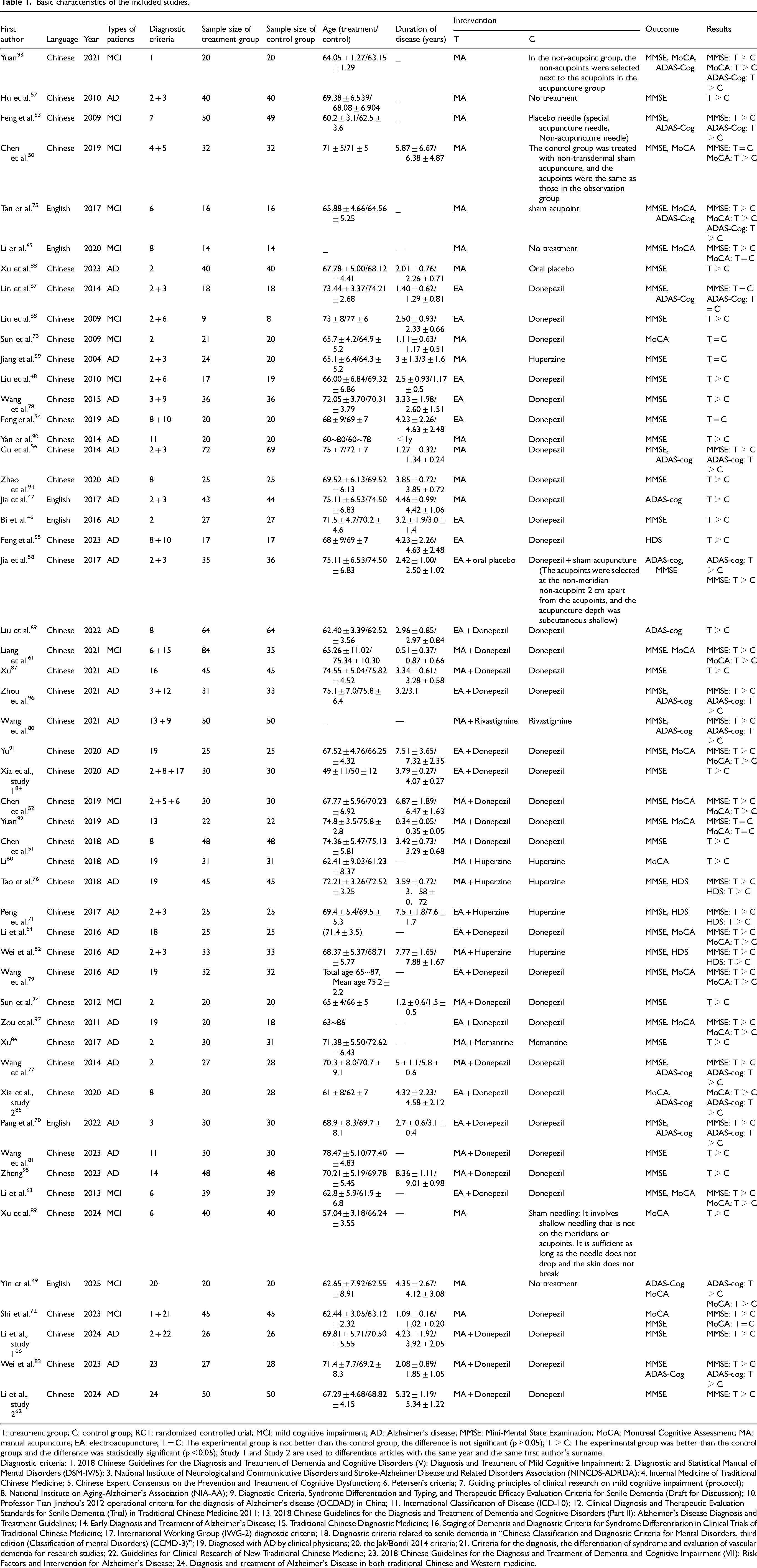
T: treatment group; C: control group; RCT: randomized controlled trial; MCI: mild cognitive impairment; AD: Alzheimer's disease; MMSE: Mini-Mental State Examination; MoCA: Montreal Cognitive Assessment; MA: manual acupuncture; EA: electroacupuncture; T = C: The experimental group is not better than the control group, the difference is not significant (p > 0.05); T > C: The experimental group was better than the control group, and the difference was statistically significant (p ≤ 0.05); Study 1 and Study 2 are used to differentiate articles with the same year and the same first author's surname.
Diagnostic criteria: 1. 2018 Chinese Guidelines for the Diagnosis and Treatment of Dementia and Cognitive Disorders (V): Diagnosis and Treatment of Mild Cognitive Impairment; 2. Diagnostic and Statistical Manual of Mental Disorders (DSM-IV/5); 3. National Institute of Neurological and Communicative Disorders and Stroke-Alzheimer Disease and Related Disorders Association (NINCDS-ADRDA); 4. Internal Medicine of Traditional Chinese Medicine; 5. Chinese Expert Consensus on the Prevention and Treatment of Cognitive Dysfunction
Quality assessment of included studies
The bias analysis results are shown in Figures 2 and 3. Of the included studies, 4 articles46–49 had low risk of bias across all domains, while the remaining 48 articles50–97 had unclear risk of bias in at least one domain. Of these 48, 8 articles58,62,64,65,77,81,94,95 were rated high risk of bias in one of the seven domains: 3 articles62,64,95 were rated high risk in random sequence generation due to non-random group allocation (grouping by treatment method), and 5 articles58,65,77,81,94 were judged to have high risk in other biases.
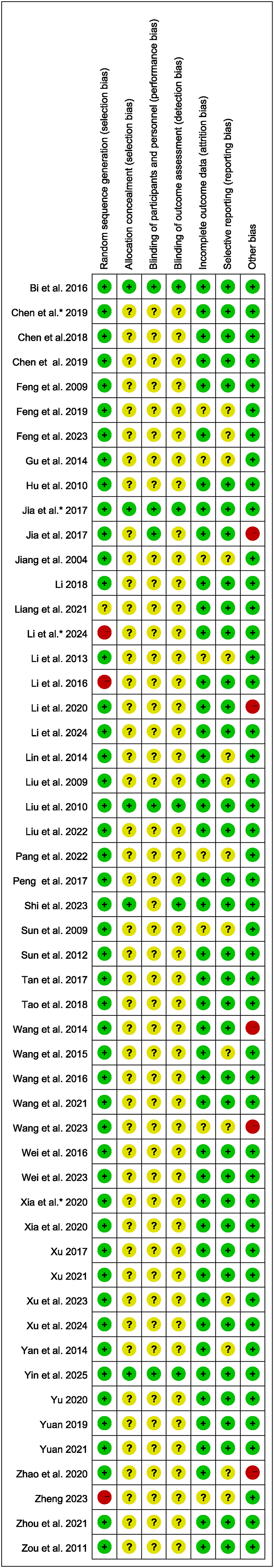
Risk of bias summary of included studies. – indicates high risk of bias, + indicates low risk of bias, and ? indicates unclear risk of bias. * was used to distinguish articles with the same year and the same first author's surname.
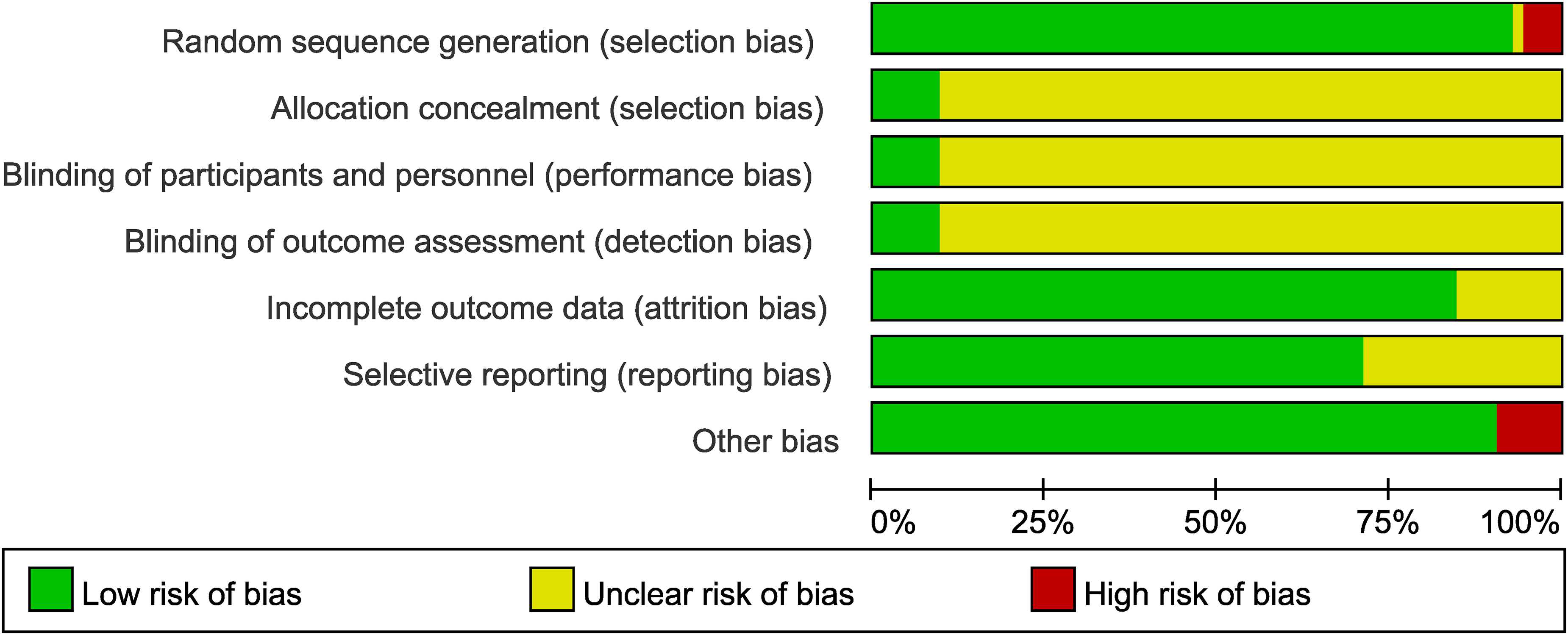
Risk of bias graph of included studies.
Specifically, Li et al. 65 did not report participants’ demographic data (e.g., gender, age, disease duration), with unknown between-group differences; Zhao et al. 94 had inconsistent total numbers of the intervention group when calculating the effective rate compared to the stated figure in the article, without providing explanations; Wang et al. 81 miscalculated the effective rate of the experimental group; Wang et al., 77 reported discrepancies between the sum of effective case count of the control group; Jia et al. 58 had inconsistencies between the combined sum of case counts for each treatment outcome and cases counts by gender in the control group and the total sample size of the control group stated in the article.
Results of meta-analyses
Acupuncture vs. Blank or Placebos
Five control conditions were used in the included studies including non-acupoints adjacent to the points chosen in the experimental group, no treatment, non-acupuncture placebo needles, non-penetrating sham acupuncture, and oral placebos. Nine articles49,50,53,57,65,75,88,89,93 (n = 543; 160 AD patients, 383 MCI patients) were included in this comparison, with manual acupuncture (MA) as the sole acupuncture intervention across all studies. Statistical analysis was performed using a random-effects model, and results are illustrated in Figure 4. Compared with blank or placebos groups, acupuncture significantly improved patients’ overall cognitive function (SMD = 1.09, 95% CI = [0.60, 1.58], p < 0.001, I2 = 91.39%) with high heterogeneity among studies.
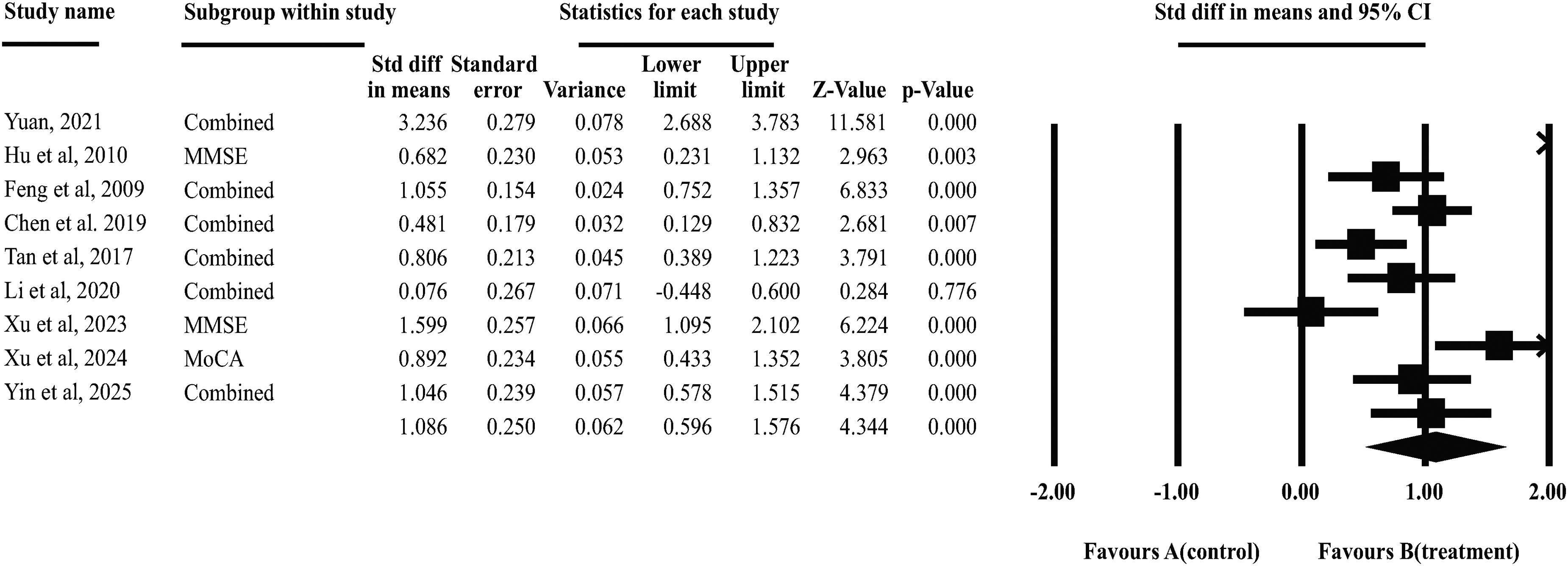
Forest plot of acupuncture vs. blank or placebos.
Begg's test, Egger's test, and funnel plot (Figure 5) showed no significant publication bias (Begg's test: p = 0.348; Egger's test: p = 0.374). As shown in Figure 5, the points were roughly symmetrically distributed. The pooled effect size remained unchanged after the trim-and-fill method was applied. The fail-safe N was 463, much larger than the threshold of “5k + 10” (k = 9, number of included studies; 5 × 9 + 10 = 55). This indicates that the significant results were unlikely to be attributed to publication bias.
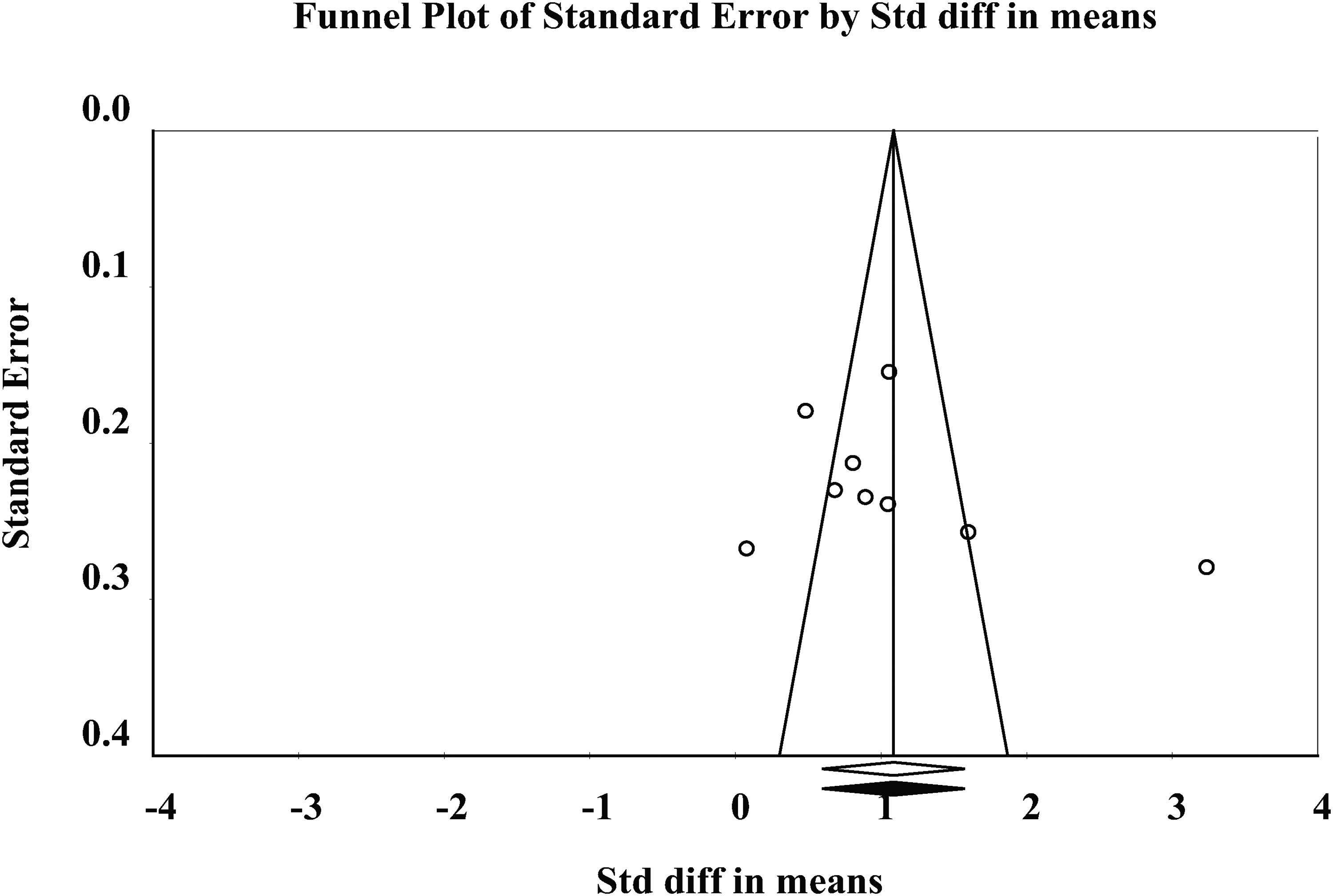
Funnel plot (trim and fill) of acupuncture vs. blank or placebos.
The sensitivity analysis (Supplemental Material S2, Figure S2-1) was conducted by sequentially excluding each included study. The 95%CI did not change significantly, indicating that the effect size estimates were stable.
Acupuncture vs. Western medicine
A total of 15 articles46–48,54–56,58,59,67,68,72,73,78,90,94 (n = 873; 689 AD patients, 184 MCI patients) were included. Statistical analysis was performed using a random-effects model, with results illustrated in Figure 6. Compared with the Western medicine group, acupuncture significantly improved patients’ overall cognitive function (SMD=0.45, 95% CI = [0.22, 0.67], p < 0.001, I2 = 69.38%) with moderate-to-high heterogeneity among studies.
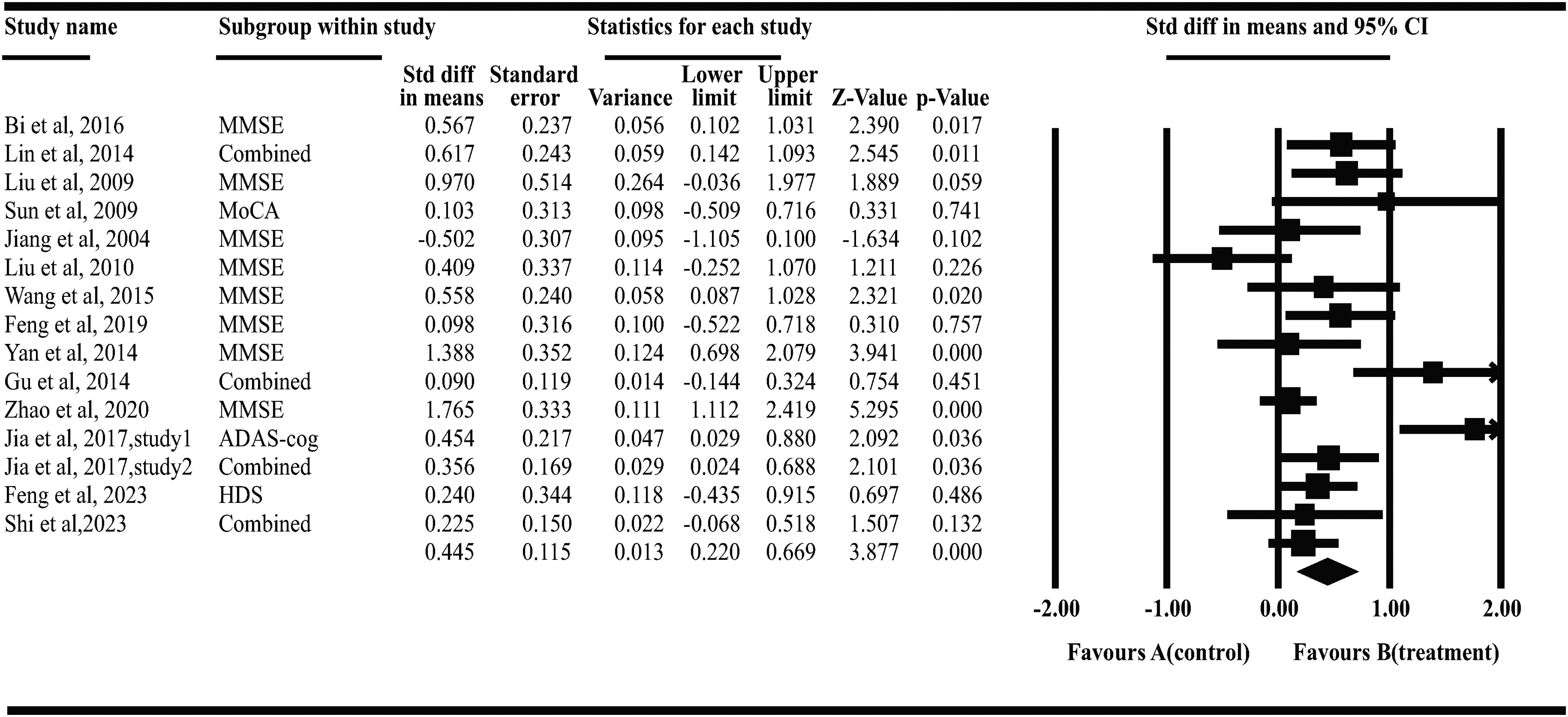
Forest plot of acupuncture vs. Western medicine. Study 1 and Study 2 are used to differentiate articles with the same year and the same first author's surname.
Begg's test, Egger's test, and funnel plot (Figure 7) suggested a potential publication bias trend (Begg's test: p = 0.075; Egger's test: p = 0.096). After applying the trim-and-fill method, the small effect size indicates no significant difference in the impact of acupuncture and Western medicine on overall cognitive function (SMD=0.242, 95%CI = [-0.010, 0.494]). However, the fail-safe N was 158, much larger than the “5k + 10” threshold (k = 15, number of included studies; 5 × 15 + 10 = 85). This indicates that the findings, though statistically no-significant and suggesting a trend of better overall cognitive function in the acupuncture group than the control group, were unlikely due to publication bias. Inconsistent findings across methods highlight the need for caution in interpreting these results.
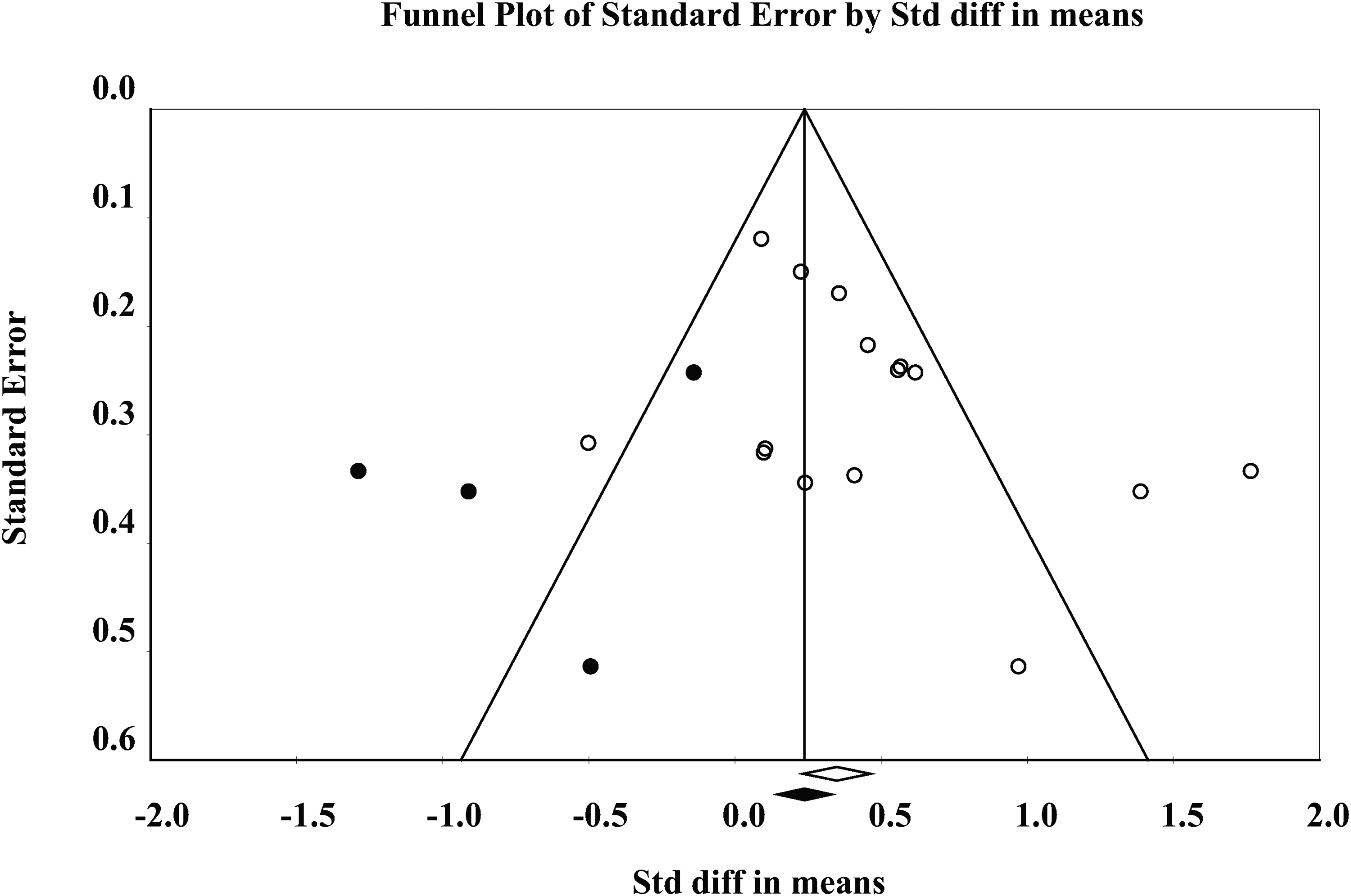
Funnel plot (trim and fill) of acupuncture vs. Western medicine.
Sensitivity analysis (Supplemental Material S2, Figure S2-2) was conducted by sequentially excluding each included study. The 95%CI did not change significantly, indicating that the effect size estimates were stable.
Acupuncture combined with western medicine vs. Western medicine
A total of 28 articles51,52,60–64,66,69–71,74,76,77,79–87,91,92,95–97 (n = 1946; 1649 AD patients, 297 MCI patients) were included. Statistical analysis was performed using a random-effects model, with results illustrated in Figure 8. Compared with Western medicine alone, acupuncture combined with Western medicine significantly improved patients’ overall cognitive function (SMD = 1.18, 95% CI = [0.92, 1.44], p < 0.001, I2 = 90.73%) with high heterogeneity among studies.
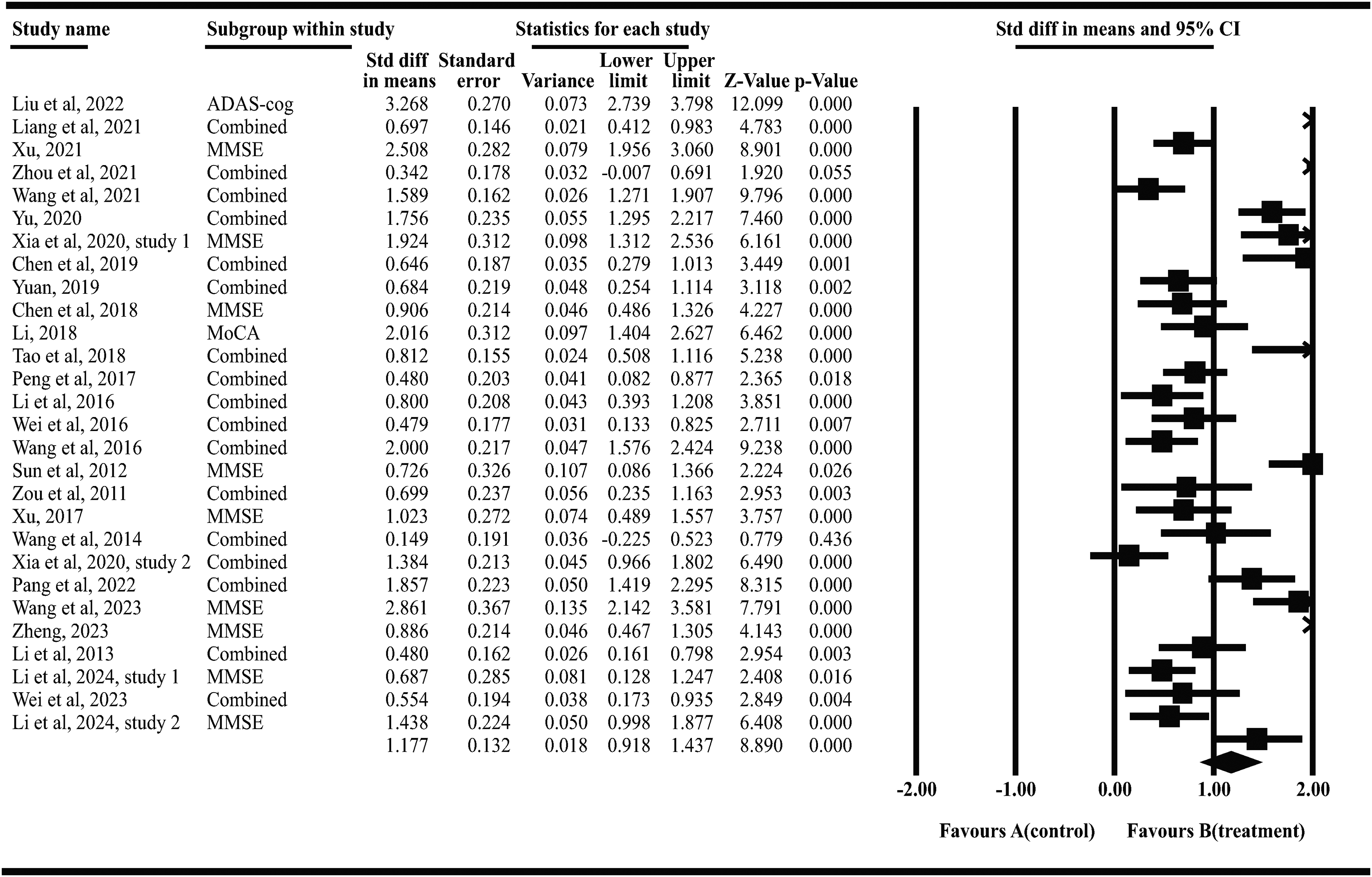
Forest plot of acupuncture combined with western medicine vs. Western medicine. Study 1 and Study 2 are used to differentiate articles with the same year and the same first author's surname.
Begg's test, Egger's test, and funnel plot (Figure 9) indicated significant publication bias (Begg's test: p = 0.001; Egger's test: p = 0.003). After applying the trim-and-fill procedure, the pooled effect size remained significant (SMD=0.94, 95%CI = [0.65, 1.23]). The fail-safe N was 5285, for exceeding the “5k + 10” threshold (k = 28, number of included studies; 5k + 10 = 150). This indicates that that though publication bias may exist, it could not account for the significant results.
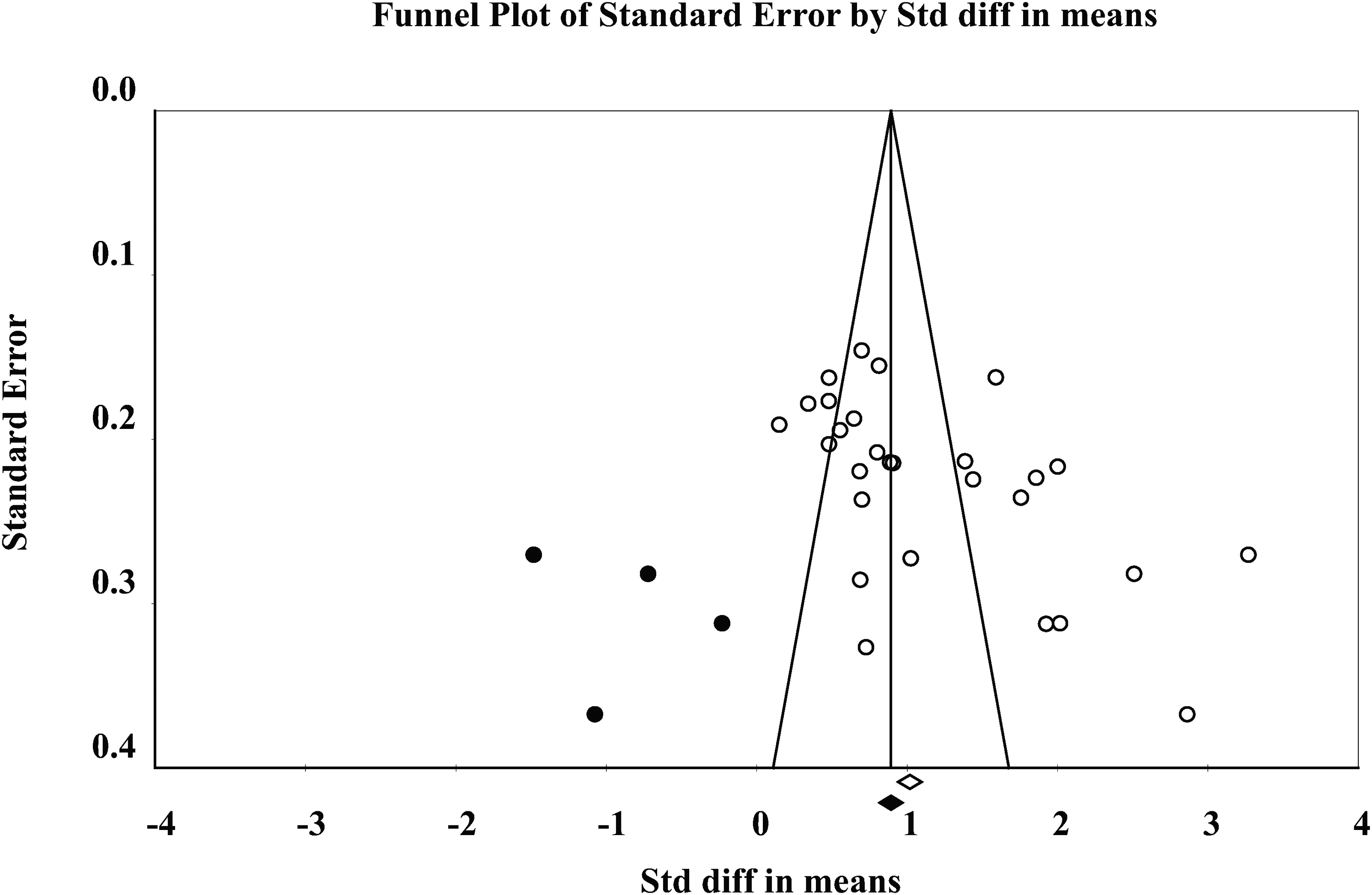
Funnel plot (trim and fill) of acupuncture combined with western medicine vs. Western medicine.
Sensitivity analysis (Supplemental Material S2, Figure S2-3) was conducted by sequentially excluding each included study. The 95%CI did not change significantly, indicating that the effect size estimates were stable.
Subgroup analyses
Type of participants
Subgroup analyses by patient type were performed for the three aforementioned contrasts, with results presented in Table 2 and Supplemental Material S2, Figure S2-4.
Subgroup analysis results for patient type and acupuncture stimulation methods.
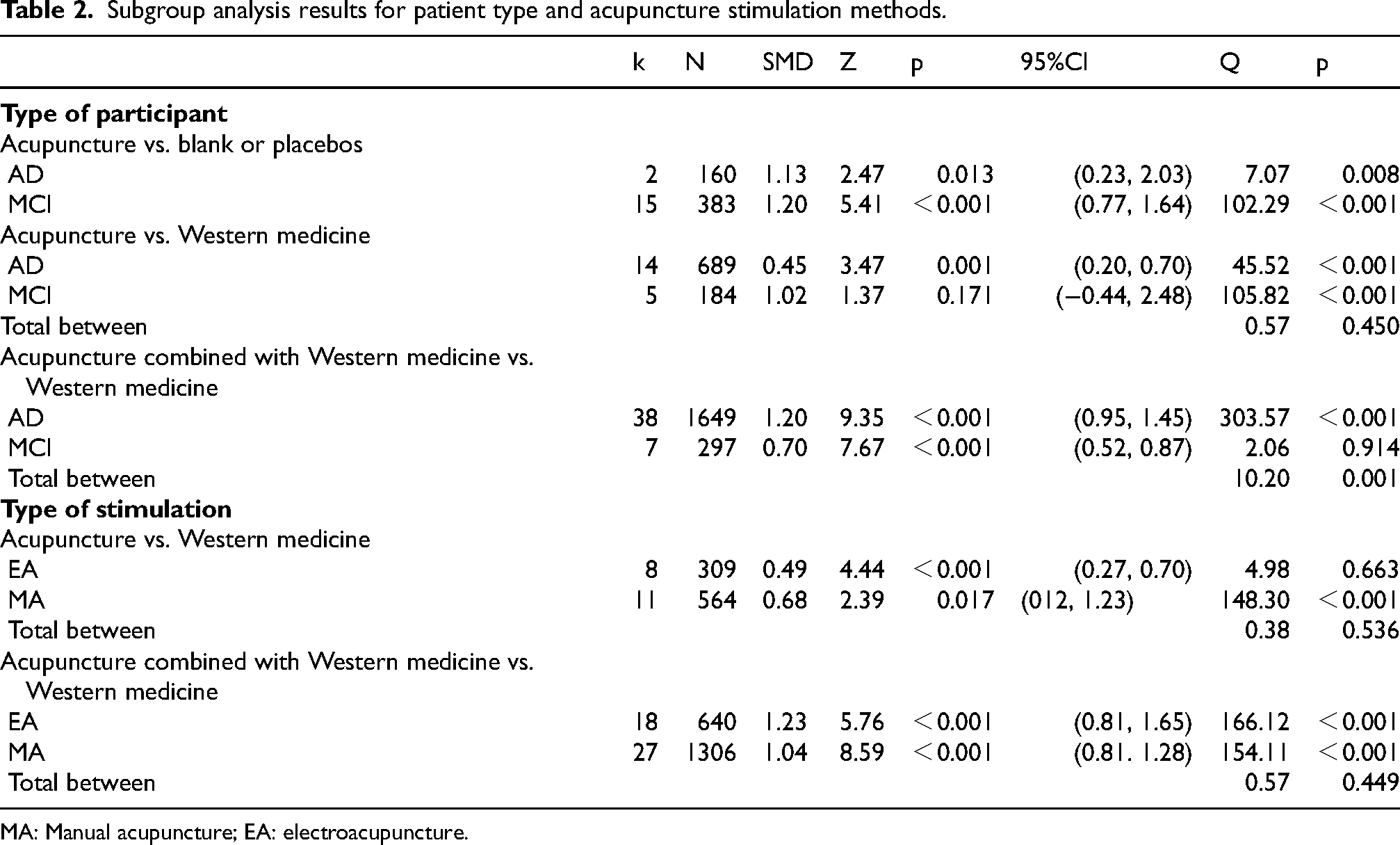
MA: Manual acupuncture; EA: electroacupuncture.
In the acupuncture vs. blank or placebos contrast, acupuncture significantly improved overall cognitive function in MCI patients (SMD = 1.20, 95% CI = [0.77, 1.64], p < 0.001, I2 = 86.31%) and AD patients (SMD=1.13, 95% CI = [0.23, 2.03], p < 0.05, I2 = 85.86%) compared to controls. However, only 2 articles57,88 were included in the AD subgroup; therefore, moderator effect analysis was not conducted for this contrast.
In the acupuncture vs. Western medicine contrast, acupuncture significantly improved overall cognitive function in AD patients compared to the Western medicine (SMD = 0.45, 95% CI = [0.20, 0.70], p = 0.001, I2 = 71.44%). However, acupuncture did not significantly improve overall cognitive function in MCI patients (SMD = 1.02, 95% CI = [−0.44, 2.48], p > 0.05, I2 = 96.22%), exhibiting extremely high heterogeneity in the MCI subgroup. Moderator effect analysis showed no significant difference in the therapeutic effect on overall cognitive function between AD and MCI patients in this contrast (Q = 0.57, p = 0.450). All results are presented in Table 2 and Supplemental Material S2, Figure S2-5.
In the acupuncture combined with medication vs. medication control contrast, acupuncture combined with medication significantly improved overall cognitive function in both AD and MCI patients compared to medication alone (AD: SMD = 1.20, 95% CI = [0.95, 1.45], p < 0.001, I2 = 87.81%; MCI: SMD = 0.70, 95% CI = [0.52, 0.88], p < 0.001, I2 = 0%). Moderator effect analysis showed that the therapeutic effect on overall cognitive function was superior in AD patients than in MCI patients in this contrast (Q = 10.20, p = 0.001). All results are presented in Table 2 and Supplemental Material S2, Figure S2-6.
Type of stimulation
MA method was used in all the 9 articles49,50,53,57,65,75,88,89,93 included in the acupuncture vs. blank or placebos contrast, so subgroup analysis by stimulation type was not feasible. Subgroup analyses by stimulation type (MA/EA) were conducted for the latter two contrasts (acupuncture vs. Western medicine, and acupuncture combined with Western medicine vs. Western medicine alone), with results presented in Table 2.
In the acupuncture vs. Western medicine contrast, both EA and MA exerted a moderate effect in improving overall cognitive function compared to Western medicine (EA: SMD = 0.49, 95% CI = [0.27, 0.70], p < 0.001, I2 = 0%; MA: SMD=0.68, 95% CI = [0.12, 1.23], p < 0.05, I2 = 93.26%), with extremely high heterogeneity in the MA subgroup (Table 2, Supplemental Material S2, Figure S2-7). However, moderator effect analysis showed no significant difference in therapeutic effect between EA and MA (Q = 0.38, p = 0.536) (Table 2).
In the acupuncture combined with Western medicine vs. Western medicine alone contrast, both EA and MA combined with Western medicine significantly improved overall cognitive function compared to Western medicine alone (EA: SMD = 1.23, 95% CI = [0.81, 1.65], p < 0.001, I2 = 89.77%; MA: SMD = 1.04, 95% CI = [0.81, 1.28], p < 0.001, I2 = 83.13%), with extremely high heterogeneity in the EA combined with Western medicine subgroup (Table 2, Supplemental Material S2, Figure S2-8). Moderator effect analysis showed no significant difference in therapeutic effect between the two acupuncture types (Q = 0.57, p = 0.449) (Table 2).
Discussion
This meta-analysis evaluated the effects of acupuncture on overall cognitive function in patients with AD and MCI. The pooled results demonstrated that acupuncture was effective in improving overall cognitive function across these AD spectrum disorders. Specifically, for AD patients, acupuncture, whether as a standalone therapy or combined with Western medicine, resulted in greater cognitive improvement than control interventions, a benefit observed for both EA and MA. In contrast, for MCI patients, acupuncture alone was superior to control interventions but did not differ significantly from Western medicine in efficacy. Furthermore, when combined with Western medicine, the intervention effect was more pronounced in AD patients than in MCI patients.
Effects of acupuncture on different stages of dementia
Effects of acupuncture for AD
Previous studies20,98–101 have shown that acupuncture could improve cognitive function in AD. In the International Clinical Practice Guidelines for Traditional Chinese Medicine - Alzheimer's Disease (2019), the World Federation of Chinese Medicine and the China Association of Chinese Medicine included acupuncture as level III evidence (Grade D recommendation) for non-pharmacological interventions in AD. 98 A Delphi expert consensus, 20 based on low/very low GRADE evidence, recommends acupuncture as an adjuvant therapy for mild-to-moderate cognitive impairment due to AD to improve cognitive domains (e.g., memory, attention, comprehension, linguistic ability, etc.). Additionally, the latest Chinese expert consensus on multimodal rehabilitation intervention for AD 99 strongly recommends tailored traditional Chinese medicine and acupuncture based on AD stages to enhance cognitive function, improve quality of life, and delay disease progression (moderate evidence quality).
Consistent with these recommendations, the present study confirms that acupuncture effectively improves overall cognitive function in AD patients. Specifically, acupuncture alone has a better effect in improving the overall cognitive function of patients with AD compared to Western medicine monotherapy, and acupuncture combined with Western medicine significantly outperformed Western medicine alone, findings that aligned with previous research.100,101 To a certain extent, these results further strengthen the evidence base for the aforementioned guidelines and consensus recommendations.
However, some prior meta-analyses100–104 have reported inconsistent conclusions regarding the efficacy of acupuncture relative to Western medicine, a discrepancy that may stem from heterogeneity in control group medication selection. Specifically, previous meta-analyses101,103,104 included a variety of drugs in the control group, both Chinese and Western drugs (e.g., donepezil, piracetam, Yizhi Jiannao Tablets, nimodipine, hydergine, duxil, Huperzine A, Naofukang Tablets, Danggui Shaoyao powder, Jian nao San). In contrast, the control group in this study was restricted to five first-line symptomatic agents including four FDA-approved drugs (donepezil, rivastigmine, galantamine, memantine) and huperzine A, all of which are recommended as first-line treatments in the Chinese Guidelines for the Diagnosis and Treatment of AD. 30 This targeted selection of control medications enhances the comparability and clinical relevance of our findings, addressing a key limitation of prior studies.
Effects of acupuncture for MCI
Lai et al. 105 suggested that acupuncture may serve as an effective non-pharmacological intervention for MCI of AD origin. Using a network meta-analysis approach with the MMSE and ADAS-Cog as outcome measures, they evaluated nine interventions, including medications (acetylcholinesterase inhibitors, ginkgo biloba, nimodipine, Chinese herbal medicine), non-pharmacological treatments (acupuncture, music therapy, exercise therapy, nutritional therapy), and placebo, for improving overall cognitive function in MCI patients. Acupuncture ranked second among all interventions for MMSE outcomes and first for ADAS-Cog outcomes. Additionally, a Delphi expert consensus 20 (based on low/very low GRADE evidence) recommends acupuncture for the management of subjective cognitive decline (SCD) or MCI.
However, some previous studies10,19,106,107 reported that acupuncture is more effective than medication for MCI, a finding slightly inconsistent with ours. This discrepancy arises because previous studies19,106 classified acupuncture alone and acupuncture combined with other interventions (e.g., Chinese herbal medicine, Western medicine, cognitive training) under “acupuncture”, leading to overly general conclusions. In contrast, the present study separately analyzed acupuncture monotherapy and acupuncture combined with medication, and further performed subgroup stratification by patient type (AD vs. MCI), and the conclusions were more detailed and targeted.
Notably, despite a certain degree of publication bias in this study, Orwin's fail-safe N analysis indicates that the results were not attributed to publication bias. Furthermore, excluding 8 articles58,62,64,65,77,81,94,95 identified as high-risk factors in quality assessment had no impact on the meta-analysis results (Supplemental Material S3), confirming the robustness of our conclusions.
Effects of the types of acupuncture stimulation
Two acupuncture modalities were included in this study including EA and MA. EA involves inserting acupuncture needles into acupoints to deliver weak electrical stimulation, and the synergy between acupuncture and electrical stimulation enhances the overall therapeutic response. 108 The present study demonstrated that MA alone, EA alone, and both combined with Western medicine significantly improved overall cognitive function compared to Western medicine monotherapy; however, no significant difference in cognitive improvement was observed between MA and EA. Notably, after excluding 8 articles58,62,64,65,77,81,94,95 identified as having high-risk factors in quality assessment, subgroup analysis of the acupuncture alone versus Western medicine group showed that MA trended to be superior to Western medicine (p = 0.082), while EA was significantly superior to Western medicine (p < 0.001) (Supplemental Material S3).
These findings are subject to certain confounding factors. For instance, EA employs continuous 20-min stimulation, whereas MA involves multiple techniques each lasting only a few seconds. Such differences in stimulation duration and periodicity (including intermittent versus continuous) may modulate biological progress such as cellular signal transduction, gene expression, and tissue plasticity, thereby potentially influencing the comparative efficacy of MA and EA. 109
Despite these limitations, the significant efficacy of EA endows it with substantial value for promoting acupuncture intervention schemes. This is because EA is easy to operate, features accurately adjustable and quantifiable treatment intensity, and does not require dedicated acupuncturists, in contrast to MA interventions. Additionally, EA parameters can be better quantified, and different stimulation parameters (including electrical pulse type, applied voltage and current magnitude, stimulation frequency, and continuous versus intermittent mode) may yield distinct effects. 110 This parameter-dependence highlights the need for in-depth exploration of optimal EA parameter combinations in future research to enhance the stability and individualization of acupuncture efficacy.
Potential mechanisms of acupuncture on AD/MCI
Beyond clinical efficacy, acupuncture exerts its effects in AD/MCI through several potential mechanisms. Anatomically, over 80% of authentic acupoints correspond to intermuscular or intramuscular connective tissue planes. 16 Acupuncture manipulations (e.g, rotation and lifting-thrusting) induce “de qi” (needle sensation) via connective tissue entanglement, converting mechanical stimulation into biochemical signals to regulate central nervous system function. 16 In core pathological regulation, EA exerts effects via specific pathways that include activating transcription factor EB (TFEB) through the Akt-MAPK1-MTORC1 pathway to promote Aβ degradation111–113; reducing phosphorylated tau levels via the PI3K/Akt/GSK-3β pathway111,114,115; inhibiting microglial activation and inflammatory factors release through the HMGB1/TLR4 and RAGE/NADPH oxidase pathways to alleviate neuroinflammation111,116–118; and simultaneously enhancing synaptic plasticity,12,22 increasing hippocampal synapses density, and promoting neurogenesis to improve cognitive function.111,119
In addition, acupuncture can regulate the blood-brain barrier (BBB), a newly identified therapeutic target for apolipoprotein E (APOE4)-associated cognitive decline (independent of Aβ or tau pathology). 120 EA can enhance BBB permeability, which not only facilitates the entry of Aβ/tau-targeting macromolecules drugs into the brain 121 and assists in endogenous Aβ clearance,121–123 but also lays a foundation for acupuncture as an adjuvant to pharmacotherapy. Studies have confirmed that EA can improve cognitive impairment and reduce BBB permeability in AD model mice 118 ; specific EA modalities can also mediate the delivery of nerve growth factor across the hippocampal BBB via the p65-VEGFA-TJs pathway, 124 among which sparse-dense wave is the potential frequency for BBB regulation.110,122,123
It should be noted that current mechanisms studies on acupuncture for AD/MCI are mostly based on mouse models. While multi-directional mechanisms remain preliminary, and the synergy or interaction between them is not fully understood.
Limitations and future directions
This study has several limitations. First, the nature of acupuncture (e.g., manual operation, physical stimulation) complicates participant blinding, limiting the number of low-bias studies. Second, included RCTs inadequately complied with the Revised Standards for Reporting Interventions in Clinical Trials of Acupuncture (STRICTA), 23 omitting key details such as needle type, acupoint selection rationale and acupuncturist qualifications. Third, studies were geographically concentrated (mostly in China), and used heterogeneous controls between acupuncture and blank or placebos (e.g., non-acupoints, no intervention, placebo needles, or oral placebos), potentially affecting placebo comparisons. 18 Fourth, significant heterogeneity and varying methodological quality warrant cautious interpretation. Finally, long-term efficacy data are lacking.
High-quality, multicenter, large-sample RCTs across diverse countries, strictly adhering to STRICTA, are urgently needed. These would improve enhance credibility, generalizability and reduce heterogeneity. Advancing technology could also integrate artificial intelligence into this research, 17 facilitating the modernization of traditional Chinese medicine for clinical application.
Conclusions
This meta-analysis, based on evidence-based medicine principles, examined acupuncture's effects on cognitive function in AD spectrum disorders. Current evidence indicates acupuncture effectively improves overall cognitive function in MCI and AD; acupuncture combined with Western medicine is significantly more effective than Western medicine alone for advanced dementia. Acupuncture can serve as an effective adjuvant intervention for AD, and a short-term cognitive improvement alternative for some patients with Western medicine contraindications. Both MA and EA improve cognitive function. Future RCTs on acupuncture for MCI and AD need refined design to enhance evidence quality and guide clinical practice more effectively.
Supplemental Material
sj-docx-1-alz-10.1177_13872877261438495 - Supplemental material for The interventional effect of acupuncture on overall cognitive function in Alzheimer's disease spectrum disorders: A meta-analysis
Supplemental material, sj-docx-1-alz-10.1177_13872877261438495 for The interventional effect of acupuncture on overall cognitive function in Alzheimer's disease spectrum disorders: A meta-analysis by Yifan Chen, Shenggang Zhao, Fenglei Yang, Ya Wang, Zhenxiang Han, Fang Han, Zhiqun Wang, Zhenbo Chen, Kai Sun, Peipeng Liang and Kuncheng Li in Journal of Alzheimer's Disease
Supplemental Material
sj-docx-2-alz-10.1177_13872877261438495 - Supplemental material for The interventional effect of acupuncture on overall cognitive function in Alzheimer's disease spectrum disorders: A meta-analysis
Supplemental material, sj-docx-2-alz-10.1177_13872877261438495 for The interventional effect of acupuncture on overall cognitive function in Alzheimer's disease spectrum disorders: A meta-analysis by Yifan Chen, Shenggang Zhao, Fenglei Yang, Ya Wang, Zhenxiang Han, Fang Han, Zhiqun Wang, Zhenbo Chen, Kai Sun, Peipeng Liang and Kuncheng Li in Journal of Alzheimer's Disease
Supplemental Material
sj-docx-3-alz-10.1177_13872877261438495 - Supplemental material for The interventional effect of acupuncture on overall cognitive function in Alzheimer's disease spectrum disorders: A meta-analysis
Supplemental material, sj-docx-3-alz-10.1177_13872877261438495 for The interventional effect of acupuncture on overall cognitive function in Alzheimer's disease spectrum disorders: A meta-analysis by Yifan Chen, Shenggang Zhao, Fenglei Yang, Ya Wang, Zhenxiang Han, Fang Han, Zhiqun Wang, Zhenbo Chen, Kai Sun, Peipeng Liang and Kuncheng Li in Journal of Alzheimer's Disease
Footnotes
Acknowledgements
We would like to thank Dong Ding and Xinrui Cui for their assistance in compiling the data.
ORCID iDs
Ethical considerations
Not applicable.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Author contribution(s)
Funding
This study was supported by the National Key Research and Development Project of China (2023YFC3605005, 2020YFC2007302), the Beijing Outstanding Young Scientists Program (JWZQ20240201004), Natural Science Foundation of China (grant numbers 81873892), and the Key Project of Medical and Health Technology of Longgang District, Shenzhen (grant number LGKCYLWS2022034).
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
All data generated or analyzed during this study are included in this published article and its Supplemental Material.
Supplemental material
Supplemental material for this article is available online.
