Abstract
Background
Nutritional problems are common among individuals living with dementia and may adversely affect quality of life. While the Mediterranean diet has been widely studied in dementia prevention, evidence regarding its role after dementia diagnosis remains limited.
Objective
This study aimed to evaluate the relationship between nutritional status, adherence to the Mediterranean diet, and quality of life among older adults with dementia.
Methods
This cross-sectional study was conducted with 150 older adults diagnosed with dementia. Data were collected using the Mini Nutritional Assessment (MNA), the Mediterranean Diet Adherence Screener (MEDAS), and the WHOQOL-OLD Quality of Life Questionnaire.
Results
Participants generally demonstrated moderate adherence to the Mediterranean diet (mean MEDAS 9.4 ± 2.4). Mediterranean diet adherence was not significantly associated with nutritional status or quality of life. In contrast, nutritional status showed a significant and independent positive association with quality of life after adjustment for potential confounders. In multiple linear regression analysis, MNA score remained a significant predictor of quality of life (β = 0.28, p = 0.002).
Conclusions
In older adults with dementia, nutritional status is independently associated with quality of life, whereas adherence to the Mediterranean diet shows no significant relationship with nutritional status or quality of life in this cross-sectional sample. These findings highlight the importance of routine nutritional assessment and individualized nutritional support in dementia care.
Introduction
Dementia refers to a decline in cognitive functions that interferes with daily life and represents one of the most common neurodegenerative conditions in older adults. Its prevalence is increasing worldwide with population aging. Dementia is not a single disease but an umbrella term encompassing various neurodegenerative and vascular conditions characterized by cognitive impairment, with Alzheimer's disease accounting for approximately 60–80% of all cases, followed by vascular dementia.1–3
Beyond genetic and neurological mechanisms, lifestyle-related factors, particularly diet, play an important role in cognitive health and dementia risk. Because dementia develops over a long prodromal period, improvements in dietary habits among cognitively healthy adults or individuals at increased risk may exert protective effects. In this context, dietary patterns such as the Dietary Approaches to Stop Hypertension (DASH), the Mediterranean-DASH Intervention for Neurodegenerative Delay (MIND), and especially the Mediterranean diet have been widely investigated. The Mediterranean diet, characterized by high consumption of plant-based foods, olive oil, and fish, with moderate intake of dairy products, also aligns closely with traditional dietary habits in Turkey. 4 Although adherence to the Mediterranean diet has been associated with a reduced risk of Alzheimer's disease and dementia,5,6 findings from systematic reviews and meta-analyses remain inconsistent, largely due to methodological heterogeneity.7,8
Importantly, most evidence supporting the neuroprotective effects of the Mediterranean diet derives from cognitively healthy populations or individuals at increased risk of dementia.9–11 In contrast, data on Mediterranean diet adherence among individuals already living with dementia are limited and inconsistent. Epidemiological and interventional studies have predominantly focused on prevention or early cognitive impairment rather than post-diagnosis disease management.12–14 A recent systematic review by Christodoulou et al. highlighted this evidence gap and emphasized that the role of Mediterranean diet adherence in nutritional status and quality of life among individuals with established dementia remains inconclusive. 15 Consequently, the relevance of Mediterranean diet adherence for nutritional status and quality of life after dementia diagnosis warrants careful interpretation.
Given the limited effectiveness and high cost of pharmacological treatments, there is growing interest in feasible and cost-effective non-pharmacological strategies for dementia management. Adequate and balanced nutrition may help preserve physical function and quality of life, whereas inadequate energy intake, micronutrient deficiencies, and irregular eating patterns may accelerate functional decline.4,16
In summary, while healthy dietary patterns, particularly the Mediterranean diet, have been extensively studied in the context of dementia prevention, their role in nutritional status and quality of life after dementia diagnosis remains unclear. Moreover, data on malnutrition prevalence, Mediterranean diet adherence, and their associations with quality of life among individuals with dementia are scarce. Therefore, the present study aims to evaluate nutritional status and malnutrition prevalence, assess adherence to the Mediterranean diet, and examine their relationships with quality of life among older adults living with dementia.
Method
Study design and participants
This study was conducted as a descriptive and cross-sectional study between April 15 and September 30, 2024, at the Neurology Outpatient Clinic of Dicle University Hospital. A total of 150 individuals aged 65 and over who had been diagnosed with dementia were included in the study. The sample size for this study was calculated using the G*Power V3.1.9.6 program, with a 95% confidence level and 90% test power, and was determined to be 150 geriatric individuals diagnosed with dementia. The study included individuals aged 65 and older who had been diagnosed with dementia through a standardized clinical assessment by a trained neuropsychologist that included Folstein's Mini-Mental State Evaluation (MMSE) 16 and neuroimaging. In neuroimaging, magnetic resonance imaging (MRI) was used as a fundamental method, particularly to demonstrate hippocampal and medial temporal lobe atrophy. The MMSE is a brief test scored out of 30 points that measures orientation, memory, attention, calculation, language, and visual-constructive abilities. MMSE scores are generally classified as follows: 24–30 points is considered normal or very mild cognitive impairment, 18–23 points is mild dementia, 10–17 points is moderate dementia, and ≤9 points is considered severe dementia. 17 Participants with MMSE scores below 24, MRI findings consistent with dementia, the ability to eat orally, and written informed consent provided either by themselves or their first-degree relatives were included. However, individuals younger than 65 years, those with acute infections, terminal illnesses, or advanced organ failure, those receiving enteral or parenteral nutritional support, individuals unable to respond to data collection tools due to severe hearing, speech, or communication impairments, and those receiving inpatient care, as well as individuals who refused to participate in the study or whose relatives did not give consent, were excluded from the study. A flow diagram of participant recruitment, exclusion, and inclusion is presented in Figure 1.
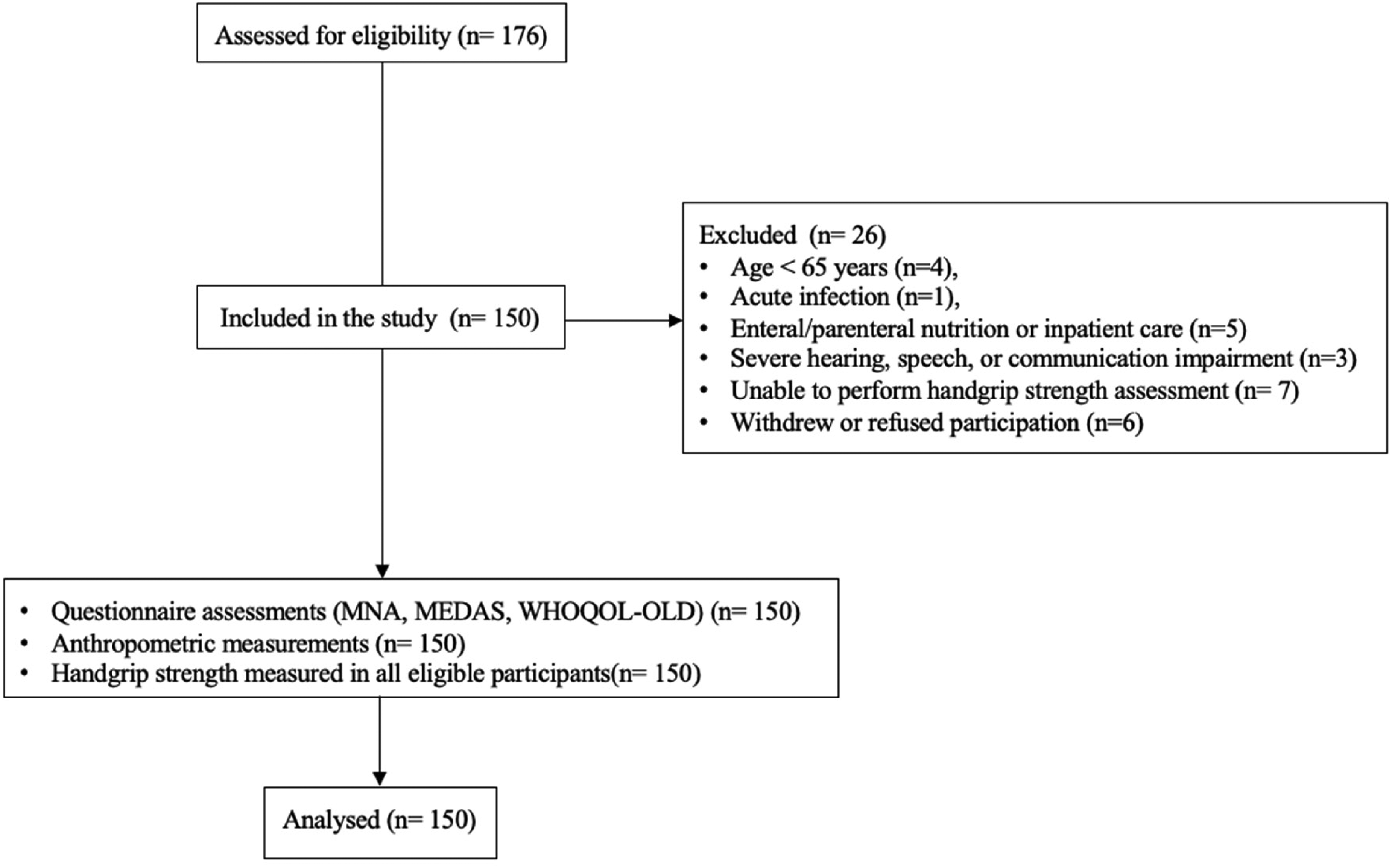
Flow diagram of participant recruitment, exclusion, and analysis.
The study was approved by the Istanbul Bilgi University Ethics Committee with 2024-20160-078 number on 03.04.2024. An informed consent form was signed by each volunteered participant. The study was conducted in accordance with the Declaration of Helsinki.
Data collection and measurements
Questionnaire assessments
Participants’ sociodemographic characteristics, lifestyle habits, and dietary habits were collected using questionnaire forms. Malnutrition risk was assessed using the Mini Nutritional Assessment (MNA) questionnaire. 18 The Mediterranean diet adherence scale (MEDAS) 19 was used to determine patients’ adherence to the Mediterranean diet, and the World Health Organization quality of life scale elderly module scale (WHOQOL-OLD) 20 was used to determine patients’ quality of life. All data were collected by the researcher through face-to-face interviews. Because the sample included individuals with mild, moderate, and severe dementia, questionnaires were administered through researcher-led interviews. For participants with moderate or severe dementia who were unable to provide reliable self-reports, responses were obtained with the assistance of a family member or the primary caregiver, in accordance with the 2024 ESPEN Dementia Guidelines. 21
The Mini Nutritional Assessment consists of 18 items, with <17 points indicating malnutrition, 17–23.5 points indicating risk of malnutrition, and ≥24 points indicating normal nutritional status. MEDAS is a 14-item scale, with ≤5 points indicating low adherence, 6-9 points indicating moderate adherence, and ≥10 points indicating high adherence to the Mediterranean diet. The WHOQOL-OLD scale comprises six subscales and 24 items, with higher scores indicating a better quality of life. In addition, the participants’ anthropometric measurements (body weight, height, and handgrip strength) were taken by the researcher.
Body weight was measured using a MESILIFE digital scale (MESILIFE Medical Technologies, Turkey; sensitivity ±0.1 kg) in participants able to stand. For those unable to stand safely, weight was measured using a hospital bed scale (TEB-LED ETT1-PSL01/02; MESPA Medical Equipment, Turkey; sensitivity ±0.2 kg). Shoes and heavy clothing were removed prior to measurement.
Height measurement procedures were adapted to participants’ functional status. In individuals who could stand safely, height was measured using a MESILIFE stadiometer (MESILIFE Medical Technologies, Turkey) with the head positioned in the Frankfurt plane whenever feasible. For participants with mobility limitations, recumbent length was measured using a non-stretch tape measure in the supine position, ensuring alignment of the head, trunk, and heels, and recording the vertex-to-heel distance to the nearest 0.5 cm.
Mid-upper arm circumference (MUAC) and calf circumference measurements were measured on the non-dominant side in accordance with ESPEN-recommended anthropometric procedures. 21 MUAC was measured at the midpoint between the acromion and olecranon with the arm relaxed, and calf circumference was measured at the point of maximal girth while seated with the knee flexed at approximately 90°. The measurements were performed twice using a non-stretch measuring tape, and the average of the two values was used to minimize measurement error.
Handgrip strength was measured using a CAMRY digital hand dynamometer (sensitivity ± 0.1 kg). Measurements were performed with participants seated, the elbow flexed at 90°, the forearm parallel to the floor, and the wrist in a neutral position. Three measurements were taken for each hand at one-minute intervals, and participants’ hand dominance was recorded. For the analysis, the mean of the three measurements of dominant hand was used as the handgrip strength value.
Participants’ BMI values were calculated using the formula [kg/m2] and evaluated according to the WHO classification. 22
Statistical analysis
Statistical analyses of the obtained data were performed using the SPSS 27 program. The normality of continuous variables was tested using the Kolmogorov-Smirnov and Shapiro-Wilk tests. Categorical variables were reported as frequencies and percentages. Descriptive statistics are presented as mean ± standard deviation for normally distributed variables and as median (minimum–maximum) for non-normally distributed variables. Categorical variables are summarized as frequencies and percentages.
For group comparisons, the Student's t-test and Mann–Whitney U test were used for two-group analyses, whereas one-way ANOVA and the Kruskal–Wallis test were applied for comparisons involving more than two groups. Associations between categorical variables were examined using the Chi-square test. Relationships between continuous variables were assessed using Pearson or Spearman correlation coefficients based on distributional assumptions. Partial correlation analyses were used to assess the independent associations between key study variables after controlling for potential confounders, including age, sex, BMI, handgrip strength, and dementia stage. In addition, a multiple linear regression analysis was used to predict QoLS by nutritional parameters and descriptive characteristics. A significance level of p < 0.05 was accepted for all analyses.
Results
Participants’ socio-demographic characteristics
The study included 150 individuals diagnosed with dementia (52% women, 48% men). The mean age of participants was 76 ± 7 years, with no significant difference between women and men. The majority of women (78%) were illiterate, while this rate was 40% among men (p = 0.001). The proportion of individuals living alone was 16%, with a significant proportion living with relatives or caregivers (48%). In terms of dementia level, 58% of individuals were in the mild dementia group, 32% in the moderate dementia group, and 10% in the severe dementia group (Table 1).
Participants’ socio-demographic characteristics.
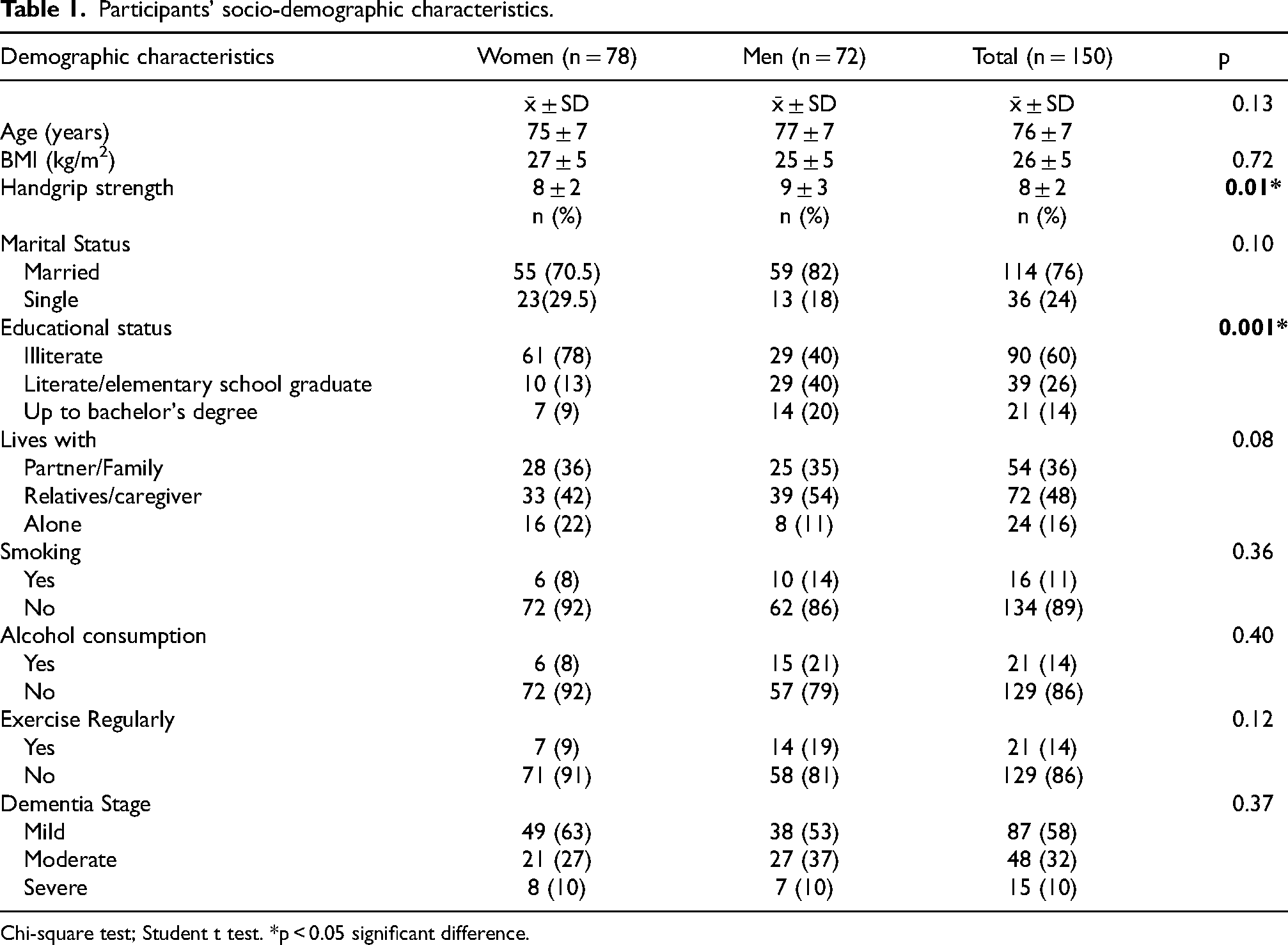
Chi-square test; Student t test. *p < 0.05 significant difference.
When individuals were compared according to MNA classification, the mean age of the malnutrition risk group was significantly higher than that of the other groups (p = 0.046). In terms of anthropometric measurements, the BMI (p < 0.001) and handgrip strength (p = 0.048) values of the normal nutritional status group were higher than those in the malnutrition and malnutrition risk groups. The mean QoLS scores were higher among individuals with normal nutritional status (p = 0.01), whereas MEDAS scores did not differ between groups (Table 2).
Participants’ socio-demographic characteristics according to MNA status.
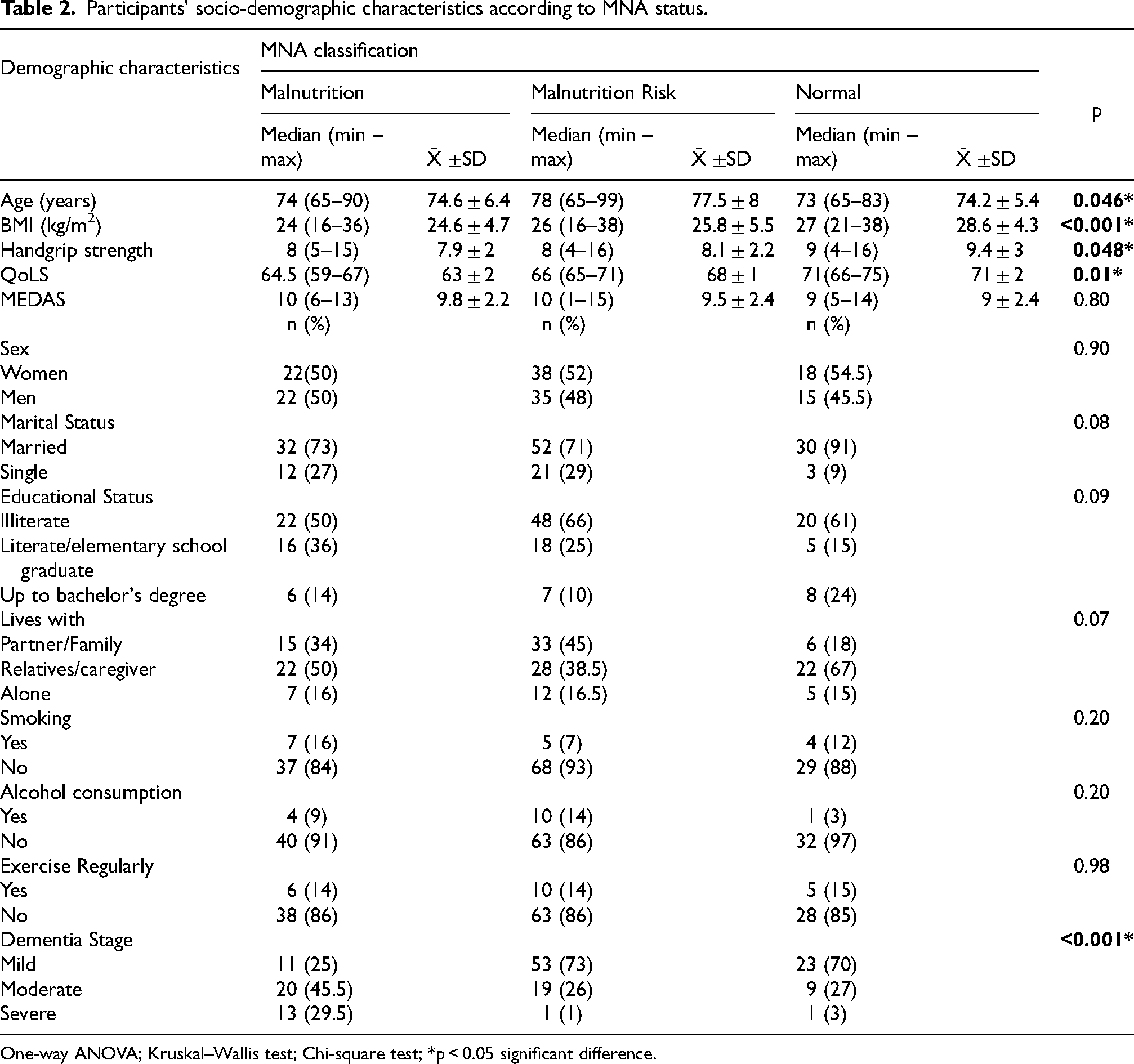
One-way ANOVA; Kruskal–Wallis test; Chi-square test; *p < 0.05 significant difference.
Correlation analyses between the study variables showed that QoLS scores were positively correlated with BMI (r = 0.19, p = 0.02). MNA scores demonstrated positive correlations with BMI (r = 0.29, p = 0.001), handgrip strength (r = 0.20, p = 0.01), and QoLS (r = 0.34, p = 0.001). In addition, MNA scores were negatively correlated with dementia stage (r = -0.44, p < 0.001). On the other hand, no statistically significant relationship was observed between age, MEDAS, and other variables (Table 3).
Correlation between scale points.

Pearson and Spearman correlation test. *p < 0.05 significant difference.
A multiple linear regression analysis was conducted to identify determinants of QoLS, with MNA, handgrip strength, age, gender, and dementia stage included as explanatory variables. These variables explained 12.1% of the variation in QoLS. Higher MNA scores (B = 0.65, 95% CI: 0.24–1.05, p = 0.002) were associated with higher QoLS scores, whereas handgrip strength, age, gender, and dementia stage were not significantly associated with QoLS (p > 0.05) (Table 4).
Multiple linear regression analysis of the variables that can affect the QoLS.
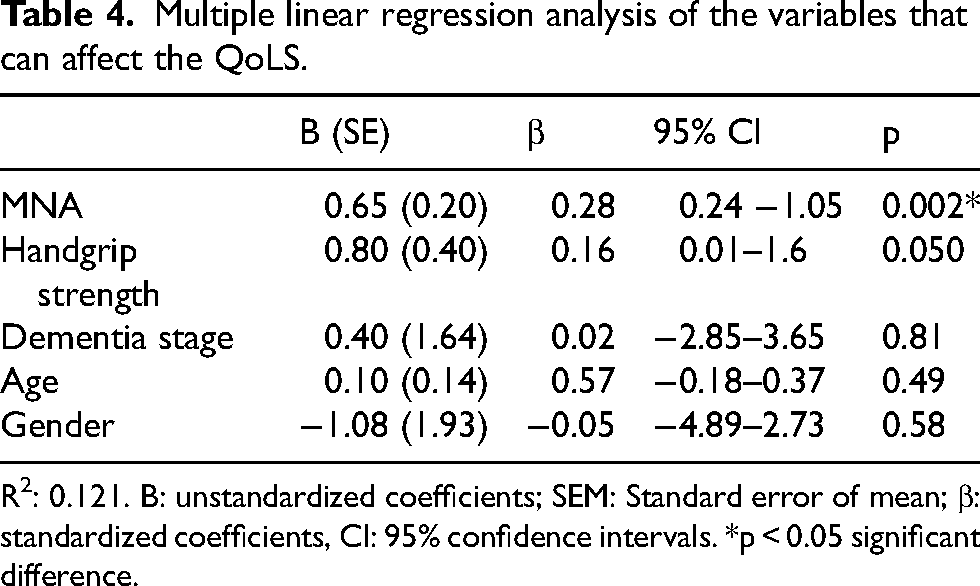

R2: 0.121. B: unstandardized coefficients; SEM: Standard error of mean; β: standardized coefficients, CI: 95% confidence intervals. *p < 0.05 significant difference.
Discussion
This study examined the relationships between nutritional status, adherence to the Mediterranean diet, and quality of life in older adults with dementia. The principal finding was that nutritional status, assessed by the MNA, was independently associated with QoLS, whereas adherence to the Mediterranean diet was not associated with either nutritional status or quality of life in this population.
After adjustment for age, sex, handgrip strength, and dementia stage, nutritional status as assessed by the total MNA score remained a significant independent predictor of quality of life, underscoring the independent contribution of nutritional status to quality-of-life outcomes in older adults with dementia. These findings are consistent with previous studies conducted in both community-dwelling and institutionalized older adults, which have consistently demonstrated that malnutrition is associated with poorer quality of life.23–25 Similarly, Rasheed and Woods reported that nutritional status scores are significant predictors of quality of life, reinforcing the clinical relevance of nutritional adequacy in dementia care. 26 These findings suggest that overall nutritional adequacy may be an important contributor to quality-of-life outcomes in individuals living with dementia.
In contrast, our study found no statistically significant association between adherence to the Mediterranean diet and either quality of life or nutritional status. Notably, all participants demonstrated a moderate level of adherence to the Mediterranean diet (mean MEDAS score: 9 ± 2.4), which may have limited the variability required to detect meaningful associations. Comparable findings have been reported in studies focusing on individuals already living with dementia. Martín et al. observed moderate Mediterranean diet adherence among individuals with Alzheimer's disease, with no significant difference compared with cognitively healthy controls. 13 Dominguez et al. reported that although most individuals with mild to moderate Alzheimer's disease showed moderate adherence to the Mediterranean diet, adherence was significantly lower than that observed in cognitively healthy controls, and the presence of Alzheimer's disease itself was the only factor independently associated with reduced adherence. 14
Intervention studies provide further insight into this issue. In a multidomain intervention study by Hassan et al., baseline Mediterranean diet adherence among individuals with mild cognitive impairment and mild dementia was also moderate; however, following the intervention, adherence increased to levels indicative of high adherence and was accompanied by improvements in physical activity and health-related quality of life. 12 These findings raise the possibility that moderate adherence alone may be insufficient to influence quality-of-life outcomes, and that higher levels of adherence might be associated with measurable benefits, particularly in the context of multidomain interventions.
While numerous observational studies and meta-analyses have demonstrated protective effects of Mediterranean and MIND dietary patterns on incident cognitive decline and dementia risk, relatively few studies have examined their role in individuals with established dementia.6,9,11 In line with our findings, Calil et al. suggested that nutrition exerts a greater influence on cognitive health prior to the onset of neurodegenerative disease, whereas dietary patterns appear to have a limited impact once cognitive and functional impairments are present. 27 Emerging evidence therefore suggests that the benefits of the Mediterranean diet may be largely confined to the pre-diagnostic or prodromal phases of dementia rather than to post-diagnostic disease management.
After a dementia diagnosis, eating behaviors are increasingly influenced by disease-related factors, care dependency, and environmental conditions, which may attenuate the potential impact of dietary patterns on nutritional status and quality of life. Moreover, evidence regarding the effects of the Mediterranean diet on disease progression, functional outcomes, or quality of life in Alzheimer's disease remains limited and inconsistent. This inconsistency may be partly explained by methodological heterogeneity across studies, differences in dietary assessment tools and cultural dietary patterns, as well as the influential role of caregivers in shaping food choices.15,21,28–30
Taken together, these findings suggest that in established dementia, overall nutritional adequacy—particularly sufficient energy, protein, and micronutrient intake—may be more relevant to quality of life than adherence to an idealized dietary pattern such as the Mediterranean diet. Accordingly, individualized and pragmatic nutritional strategies may be more feasible and clinically meaningful than strict dietary models in this population.
As a secondary finding, nutritional status declined with increasing dementia severity, with a substantial proportion of individuals with moderate to severe dementia classified as malnourished or at risk of malnutrition. The findings presented in Table 2 complement the main analyses by demonstrating consistency between categorical and continuous approaches to nutritional assessment. Individuals classified as malnourished or at risk of malnutrition exhibited significantly poorer clinical profiles, including lower handgrip strength and lower quality of life scores, compared with those with normal nutritional status. Furthermore, a notable decline in nutritional status was observed as dementia severity progressed. These categorical comparisons align with the correlation and regression analyses, supporting the conclusion that nutritional status is independently associated with quality of life in older adults with dementia. This internal consistency across different statistical methods reinforces the robustness of our data and underscores the clinical importance of routine nutritional screening in this population. Evidence from cohort studies and meta-analyses suggests that progressive cognitive impairment increases nutritional vulnerability through mechanisms such as reduced appetite, swallowing difficulties, motor impairment, and behavioral symptoms.31–33 In line with the ESPEN Dementia Guidelines, these findings reinforce the importance of routine nutritional screening and individualized nutritional care as essential components of dementia management.21,34 In contrast, quality of life did not show a clear association with dementia stage, indicating that disease severity alone does not determine quality of life. Psychosocial factors, caregiver support, and the care environment appear to play a central role in maintaining quality of life across dementia stages.35–40 The high proportion of participants living with family members or caregivers in our sample may have contributed to the preservation of quality of life despite cognitive decline.
Strengths and limitations
A major strength of this study is that it is among the few investigations evaluating the interplay between nutritional status, Mediterranean diet adherence, and quality of life in older adults with a clinical diagnosis of dementia. The inclusion of validated and widely used assessment tools, such as MNA, MEDAS, and the WHOQOL-OLD, enhances the reliability and comparability of the findings. Furthermore, the relatively good sample size and the evaluation of anthropometric indicators, such as body mass index and handgrip strength, provide a multidimensional understanding of the nutritional and functional status of this population.
Despite these strengths, some limitations should be acknowledged. First due to the cross-sectional design of the study, no conclusion of causality could be made, and therefore it was not possible to identify which condition was the cause and which was consequence. In addition, although MEDAS provides a useful screening tool, it may not fully capture the complexity of dietary intake and cultural variations in non-Western populations. Future longitudinal and multicenter studies with more detailed dietary assessments are warranted to clarify causal relationships and strengthen the evidence base for nutritional interventions in dementia care.
Conclusion
This study demonstrated that nutritional status is a key determinant of quality of life among older adults with dementia. Although adherence to the Mediterranean diet, as assessed by MEDAS, was not associated with nutritional status or quality of life, malnutrition risk increased with advancing dementia severity. Higher MNA scores were consistently associated with better quality of life, underscoring the clinical relevance of maintaining adequate nutritional status in this vulnerable population. These findings highlight the importance of early nutritional assessment, multidisciplinary care, and personalized nutritional support in accordance with evidence-based ESPEN recommendations. Strengthening nutritional interventions may contribute to improved functional outcomes and help preserve quality of life throughout the course of dementia.
Supplemental Material
sj-docx-1-alz-10.1177_13872877261434990 - Supplemental material for Nutritional status, Mediterranean diet adherence, and quality of life in older adults with dementia: A cross-sectional study
Supplemental material, sj-docx-1-alz-10.1177_13872877261434990 for Nutritional status, Mediterranean diet adherence, and quality of life in older adults with dementia: A cross-sectional study by Ezgi Barin Sessiz Menekşe, Damla Zeynep Bayraktar, Mehmet Uğur Çevik, Velat Menekşe and Negin Elmas in Journal of Alzheimer's Disease
Footnotes
Acknowledgements
The authors would like to thank all participants and their caregivers for their valuable contribution to this study.
Ethical considerations
The study was approved by the Istanbul Bilgi University Ethics Committee with 2024-20160-078 number on 03.04.2024. An informed consent form was signed by each volunteered participant. This research was conducted ethically in accordance with the World Medical Association Declaration of Helsinki.
Consent to participate
All participants provided written informed consent prior to participating.
Consent for publication
Not applicable
Author contribution(s)
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
The data supporting the findings of this study are available on request from the corresponding author.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
