Abstract
Background
Healthy lifestyles may reduce dementia risk by helping build cognitive reserve across the life course and promoting resilience and better cognitive outcomes in late-life. Whether self-reported lifestyle changes are informative for assessing brain health remains unclear.
Objective
To determine whether self-reported lifestyle changes (determinants) are associated with cognition, resilience, and Alzheimer's disease and related dementias (ADRD) biomarkers (outcomes), and whether these associations vary by sociodemographic characteristics and cognitive impairment status.
Methods
Data was obtained from 260 adults (age-range: 50–92). Self-reported change (increase/no change, decrease) in diet and physical, cognitive, and social activity from age 25 to present was evaluated in relation to cognition, resilience, and biomarkers within a cross-sectional design. ANCOVA models adjusted for age, sex, race, ethnicity, and education were used to examine associations between lifestyle change and outcomes. Effect modification by sex, race, ethnicity, and cognitive impairment status was also tested.
Results
Self-reported increases in physical activity and diet were associated with better cognition and higher resilience, while increases in social activity with higher resilience and larger amygdala volume. Associations were stronger when increases occurred in multiple lifestyle domains. Associations differed by cognitive impairment status; no variation by sex and race was observed.
Conclusions
Increases in lifestyle behaviors relative to age 25 were associated with better cognitive and brain health outcomes, especially when increases occurred across multiple domains. These findings align with longitudinal evidence linking lifestyle engagement to cognitive aging and suggest that cross-sectional self-report of change may provide a useful proxy for estimating long-term lifestyle patterns.
Keywords
Introduction
Nearly 7 million Americans are currently diagnosed with Alzheimer's disease and related dementias (ADRD), as well as its prodromal condition, mild cognitive impairment (MCI). 1 As the number of older adults continues to increase due to demographic shifts in the population, MCI and ADRD incidence is expected to rise, posing physical, emotional, and financial challenges to those affected.
Significant progress has been made in the understanding of neuropathological processes involved in the development of ADRD and the various biological factors such as aging and genetics that contribute to dementia risk. In addition to these non-modifiable factors, the 2025 Lancet Commission report identified 14 modifiable lifestyle and health-related risk factors for ADRD. 2 These factors are estimated to account for up to 45% of global dementia cases and represent key targets for intervention. The report emphasized the importance of remaining cognitively, physically, and socially active throughout life to reduce dementia risk in later years. Furthermore, maintaining a healthy diet can reduce the risk of chronic conditions such as high cardiovascular and metabolic conditions in midlife, which have deleterious effects on the brain and increase dementia risk later in life. 3
Longitudinal studies have found that lifelong physical activity is associated with better cognitive function and lower dementia risk in later life. In the British 1946 Birth Cohort Study, which collected repeated self-reported physical activity level over a 30-year period, being physically active at all ages was linked to better cognition at age 69 as compared to being physically inactive, with the strongest relationship found for lifelong maintenance of physical activity. 4 In another study, using performance-based fitness measures that track physical activity based on heart rate during activity, individuals who increased or maintained a high level of physical activity over 24 years had lower risk of dementia incidence and dementia-related mortality than inactive individuals. 5 The mechanisms through which physical activity benefits brain health include improved cerebral blood flow, myokine secretion with neuroprotective effects, and reduced neuroinflammation. 2
Late-life social activity may also reduce dementia risk in cognitively healthy older adults. Among 1900 older adults followed for an average of 6.6 years in the Rush Memory and Aging Project, higher social engagement was associated with a 5-year older age at dementia/MCI onset. 6 In the Whitehall II cohort study, which followed more than 6000 adults aged 35–55 years at baseline for 21 years, having more frequent social contacts was associated with better cognitive performance trajectories. 7 Participation in social activities may support brain health by increasing cognitive reserve, promoting healthy behaviors, and reducing stress and inflammation. 2
Maintaining high levels of cognitive activity throughout life and particularly during midlife is also important for brain health and dementia prevention. 2 High childhood cognitive stimulation (i.e., years of formal education) and occupational complexity in adulthood have been linked to reduced risk of dementia 30 years later 8 and increased dementia-free survival time. 9 Possible explanatory mechanisms include lower production of circulatory proteins that inhibit axono- (new axonal generation and extension) and synapto-genesis (synaptic growth and connection), 8 and greater efficiency of functional brain networks, both of which may help build greater cognitive reserve in individuals who maintain high levels of cognitive stimulation throughout life as compared to those who do not. 2
Finally, healthy eating habits may provide cognitive benefits such as better performance on cognitive testing, less cognitive decline, and reduced dementia risk, 10 which may be attributed to lower overall disease burden and improved cardiometabolic health, leading to improved cerebral perfusion, brain connectivity, insulin sensitivity, and reduced chronic inflammation and oxidative stress.11,12 Large cohort studies have found that compared to non-adherent participants, those who adhere to dietary guidelines are less likely to develop dementia of vascular causes possibly due to lower LDL cholesterol levels. 13 Greater adherence to the Mediterranean 14 or the MIND diets, was associated with decreased risk of dementia in middle age and older adults. 15 However, there is inconsistency across studies on whether healthy diets provide significant cognitive benefits, with some failing to find significant benefits for midlife healthy diets 16 and others finding weak supporting evidence of benefits. 17
While these lifestyle behaviors likely confer cognitive benefits to all older adults, differences by race and ethnicity in their impact have been noted. For example, in racially and ethnically diverse cohorts of older adults, the positive effects of leisure cognitive activity 18 and diet 19 on cognitive function were only found in White individuals. Moreover, a buffering effect of high social engagement on cognitive decline was found to be stronger in White individuals than Black individuals 20 while a protective effect of diet on cognitive decline was reported in Blacks but not Whites 21 and no variation across different ethnic groups in the positive effect of physical activity was reported in large multicultural studies. 22 In addition, sex differences in the effect of lifestyle on brain health have also been identified, with women receiving greater cognitive gains and brain health benefits than men in response to exercise training 23 and dietary interventions. 24 Middle-aged and older women were found to also derive more cognitive benefits from engagement in social activities than men. 25 Furthermore, evidence from observational and interventional studies suggests that not only cognitively normal, but also cognitively impaired older adults could reap cognitive benefits from maintaining a healthy lifestyle,26–28 although whether stronger benefits are derived for the latter compared to the former is still unclear. A better understanding of the impact of maintaining healthy lifestyles on brain outcomes in later life and its potential variation by cognitive status, sex, and race and ethnicity has important implications for the design of lifestyle interventions focused on improving brain health and slowing cognitive decline in at risk groups.
Finally, lifestyles combining healthy behaviors (e.g., healthy diet, physical, social, and cognitive activity) have been associated with slower rates of memory decline and lower risk of progression to MCI or dementia compared to unhealthy lifestyles. 29 Tracking lifestyle behaviors over the life course to quantify their impact on late-life cognition may be challenging but can provide useful insight into how engagement in various lifestyle behaviors may work together to promote brain health in late life. In a recently published work, Turpin and colleagues showed that while no association was found between cognitive activity in young adulthood and late-life neuroimaging, engagement in complex cognitive activities related to occupation in midlife was linked to better brain neuroimaging outcomes including perfusion and glucose metabolism in later life. 30 Moreover, multidomain lifestyle interventions such as the Finnish FINGER and the US POINTER studies have shown that lifestyles that combine healthy diets, engagement in physical, social, and cognitive activity and vascular risk monitoring help improve or maintain overall cognition and reduce risk of cerebrovascular events and cognitive impairment after 2 years.31–33
Although lifestyle behaviors are linked to cognitive aging, it remains unclear whether self-reported change in distinct lifestyle domains provides clinically meaningful information about cognitive and brain health. Determining whether self-reported change in lifestyle behaviors offers clinically relevant insight into cognitive and brain health is an important next step, as such measures may provide a scalable means of supporting risk assessment and intervention planning. Thus, the goal of the current study was to examine whether self-reported change in multiple lifestyle domains is associated with cognition, resilience, and ADRD biomarkers, and whether these associations vary by sociodemographic characteristics and cognitive impairment status. Our analytic approach allows evaluation of individual and specific combinations of lifestyle behaviors in relation to brain health outcomes, which in multidomain lifestyle interventions tend to be clumped together.31–33
Methods
Study sample
The sample is comprised of older adults participating in the Healthy Brain Initiative (HBI), an ongoing longitudinal study of brain health and risk of MCI and ADRD at the University of Miami that commenced in October 2021 with the first participant enrolled in March 2022. Participants complete identical assessments at baseline and then annually based on the anniversary of their baseline. The HBI, which is described in detail elsewhere, was designed to examine the impact of biological, psychosocial, functional, exposomal, and behavioral factors on brain health, resilience, ADRD risk, presentation, and disease progression. 34 Participants, who are aged ≥50 years and have no cognitive impairment, subjective cognitive impairment, MCI, or mild dementia, undergo a comprehensive annual battery of neuropsychological, psychosocial, neurological, and physical functional evaluations, bi-annual MRI scans, and annual blood-based biomarkers. This study was approved by the University of Miami's Institutional Review Board. All participants provided written informed consent. All study procedures were done in accordance with the Helsinki Declaration of 1975. Analyses for the current cross-sectional study used data from participants’ baseline visit. A total of 260 older adults were included, with an age range of 50 to 92 year and a ratio of 2.7 women to each man. The cohort is diverse consisting of 57% Non-Hispanic White, 17% Non-Hispanic Black, and 26% Hispanic participants.
Annual clinical-cognitive assessments
Participants underwent comprehensive clinical, cognitive, functional and behavioral evaluations modelled on the Uniform Data Set (UDS v3.0) from the NIA Alzheimer's Disease Research Center program.35,36 A list of all clinical and cognitive assessments completed at baseline and each subsequent annual visit is published elsewhere. 34 Briefly, HBI participants undergo physical functional (e.g., mini Physical Performance Test) 37 and neurological examinations, body composition analysis (e.g., weight, % body fat), blood collection for biomarkers, MRI studies, and cognitive assessments. Clinical and cognitive data are consolidated using a clinical consensus conference to assign diagnosis of no cognitive impairment, MCI, or mild dementia. MCI and ADRD etiologies were assigned using their phenotypic presentation, history, and current published clinical criteria.38–43
In this study, the Montreal Cognitive Assessment (MoCA, a paper and pencil assessment tool that is part of UDS v3.0, score range: 0–30 with higher scores indicating better cognitive function) 44 and Cognivue Clarity (a computer-based cognitive assessment tool; score range: 0–100; higher scores indicate better cognitive function) were used as global measures of cognitive function.45–46 Total scores from the Number Symbol Coding Test were used as a measure of executive function (scores range: 7.0 to 64.0), with higher scores indicative of better executive function. 47 Time taken to complete the Trail Making Test Part A was used as a measure of psychomotor processing speed (score range: 0–98 s, with lower scores indicative of better attention). 48 Number of immediate recalled words across three trials on the Hopkins Verbal Learning Test—Revised and recalled after a short delay was used as measures of verbal learning and episodic memory, respectively. 49 Scores ranged from 0 to 12.0, with higher scores indicative of better episodic memory. Global cognitive measures were evaluated as primary outcomes and domain-specific cognitive measures as secondary outcomes.
Resilience Index
Resilience, which refers to the ability of the brain to resist the effects of pathology and maintain function, 50 was measured with the Resilience Index (RI), a brief assessment of brain health which incorporates several modifiable brain protective factors including current level of physical activity, cognitive activity, social engagement and dietary patterns. 51 Physical activity was measured with the Quick Physical Activity Rating Scale (QPAR), which assesses the intensity, frequency, and duration of 10 categories of physical activity with possible scores ranging from 0–153, with higher scores indicating greater levels of Physical activity. 52 Cognitive activity was measured with the Cognitive & Leisure Activity Scale (CLAS), which assesses the frequency of participation in 15 categories of cognitively stimulating activities, with scores ranging from 0–80, with higher scores being indicative of greater cognitive activity. 53 Social engagement is measured as participation in social activities, socialization, and engagement on a 4-point Likert scale (1 = poor, 2 = fair, 3 = good, and 4 = excellent), with higher scores indicating greater social engagement. Dietary patterns were assessed with the MIND Diet Score Sheet, which measures the frequency of intake of 15 categories of food, with possible scores ranging from 0–15 (higher scores represent greater adherence to the MIND diet). 54 The RI also includes measures of mindfulness and cognitive reserve. Mindfulness, which refers to the practice of awareness and living in the moment without judgement, was measured with the Applied Mindfulness Process Scale (AMPS), which measures three aspects of mindfulness practice, with scores ranging from 0–60 (higher scores used to indicate greater mindfulness).55–57 Cognitive reserve is measured with the Cognitive Reserve Unit Scale (CRUS), a standardized measure of highest educational and occupational attainment, scored on a 0–66 scale with higher scores representing greater cognitive reserve. The RI score is calculated by summing up individual subscale scores with possible scores ranging from 1–378. Higher scores on the RI indicate greater resilience and better brain health.
Lifestyle behaviors
As part of the baseline data collection, participants were asked to retrospectively self-report information about their lifestyle behaviors and health behaviors over their life-course. This included asking participants to rate their overall level of physical activity, cognitive activity, social activity, and diet at age 25 compared to their current activity level. Participants were asked to evaluate change in lifestyle behaviors from age 25 at every annual follow-up but only baseline ratings were used in this study. Examples were provided for each type of activity such as exercising, yoga, and gardening for physical activity; reading, learning new hobbies, and doing crossword puzzles for cognitive activity; and seeing friends and family, belonging to clubs or organizations, and participating in religious service for social activity. Physical, social, and cognitive activities were categorized as 0 = activity level unchanged, 1 = less activity, and 2 = higher activity (at age 25 than now). Diet/nutritional choices at age 25 were also compared against current diet and categorized as 0 = unchanged, 1 = less healthy, and 2 = healthier. Responses were considered to indicate 0 = no change if activity level/diet were rated as unchanged, 1 = improved if rated lesser/less healthy, and 2 = declined if activity level/diet were rated a higher/healthier at age 25 than now. Due to small numbers of participants reporting no change, we combined categories 0 and 1 to capture 0 = improvement/no change versus 1 = decline from age 25 in each of the 4 lifestyle and health behaviors. Combinations of behavioral change (e.g., physical activity and diet) were created and categorized as 0 = improved/no change in both behaviors; 1 = improved/no change in either behavior; or 2 = declined in both.
Blood-based biomarkers
PrecivityAD2 (C2N, St Louis, MO) 58 was used to determine the Amyloid Probability Score 2 (APS2), a measure of AD pathology (phosphorylated tau %ratio and amyloid β42/40 ratio). A higher APS2 score indicates greater likelihood of brain amyloid pathology. Simoa™SR-X (Quanterix Corporation, Billerica, MA) 59 was used as an immunohistochemical approach to provide measures of general neurodegeneration including indicators of axonal damage (neurofilament light chain NfL), and astrocyte damage (glial fibrillary acidic protein; GFAP). Higher NfL and GFAP values are indicative of greater neurodegeneration and neuroinflammation.
Magnetic resonance imaging biomarkers
HBI participants underwent MRI scans using a GE 3T 750W scanner and included high-resolution 3D sagittal MPRAGE, axial FLAIR, and T2* sequences. Quantitative morphometry was assessed with CombinosticsTM cMRI (Finland, www.combinostics.com), an FDA-cleared AI pipeline, to provide fully automated quantification of cortical, ventricular, and subcortical volumes and white matter hyperintensity (WMH) burden. 60 The cMRI suite contains important dementia biomarkers including hippocampal, amygdala, and WMH volumes, included in this analysis. Reduced hippocampus and WMH volume is indicative of neurodegeneration and associated cognitive changes in early stages of cognitive decline,61,62 while shrinkage of amygdala has been recently proposed as an early sign of AD. 63
Covariates and other factors
Demographics included age and education, measured in years, sex dichotomized as 1 = Men and 2 = Women, and self-reported race and ethnicity categorized as 0 = Non-Hispanic White; 1 = Non-Hispanic Black; 2 = Hispanic. Cognitive status was categorized as 1 = Cognitively healthy and 2 = Cognitively impaired using global disease status (1 = Cognitively healthy; 2 = Impaired but no Mild Cognitive Impairment (MCI); 3 = MCI; 4 = Dementia). Physical performance was measured with the Mini Physical Performance Test (mini PPT), 37 Timed Up and Go Test (TUG), 64 and the Fried Frailty Scale. 65 Body measurements including weight, waist girth, and percent body fat were measured with wall-mounted or handheld tape measures and bioimpedance body composition analysis (In Body USA; 770 series), respectively.
Data analysis
Sample characteristics including covariates, change in health and lifestyle behaviors from age 25, current levels of social, cognitive, and physical activity and dietary patterns, and cognitive impairment status, were evaluated with descriptive statistics.
Given the self-reported nature of the lifestyle change measures and the likelihood of recall bias, we compared groups reporting increases (versus decline) on current self-reported lifestyle measures and objective health outcomes (mini PPT, TUG, frailty, and body composition) with t tests or chi square, depending on each variable's measurement level. Alignment with these outcomes would support these measures as brief cross-sectional measures of lifetime change. To further evaluate the validity of our lifestyle change measures, we reassessed these associations while stratifying by cognitive impairment status, which can influence how participants report current and past levels of lifestyle behaviors.
Associations between lifestyle behavior change (determinants) and cognition, resilience, and ADRD biomarkers (outcomes) were examined using a two-tier analytic approach. First, ANCOVA models (Tier 1) assessed relationships between each lifestyle change domain and each outcome (resilience, global and domain-specific cognitive performance, blood-based biomarkers, and imaging biomarkers), adjusted for age, sex, race, ethnicity, and education. Models evaluating resilience excluded education because it is a component of the RI calculation. Significant associations (p < .05; n = 30) were then evaluated using the Benjamini–Hochberg false discovery rate (FDR) correction in Tier 2 analyses. Combined effects that exceeded added individual effects were interpreted as indicating synergistic effects of joint behaviors. Given that analyses involving paired behaviors and multiple outcomes were exploratory, an FDR rate of 10% was applied to reduce the likelihood of Type II error.
Sensitivity analyses
Moderation of the relationships between measures of lifestyle change and outcomes assessed in Tier 2 analyses by sex, race, ethnicity, and cognitive impairment status was evaluated using interaction terms (e.g., physical activity × cognitive impairment). Where interaction terms were significant, follow-up stratified analyses were conducted to clarify group-specific association. Combined effects of behavior pairs were interpreted as evidence of joint associations with outcomes, including ADRD biomarkers.
Results
Characteristics of the 260 HBI participants who provided information on change in health behavior from age 25 and were included in the analysis are presented in Table 1. Participants were mostly women (73%), had an average age of 69 years, and completed 15 years of formal education, The sample was racially and ethnically heterogeneous. Most participants were cognitively healthy with 26% diagnosed with MCI and 2% with mild dementia. As expected, most participants reported a decline in physical, cognitive, and social activity but improvement/no change in dietary patterns.
Sample characteristics (N = 260).
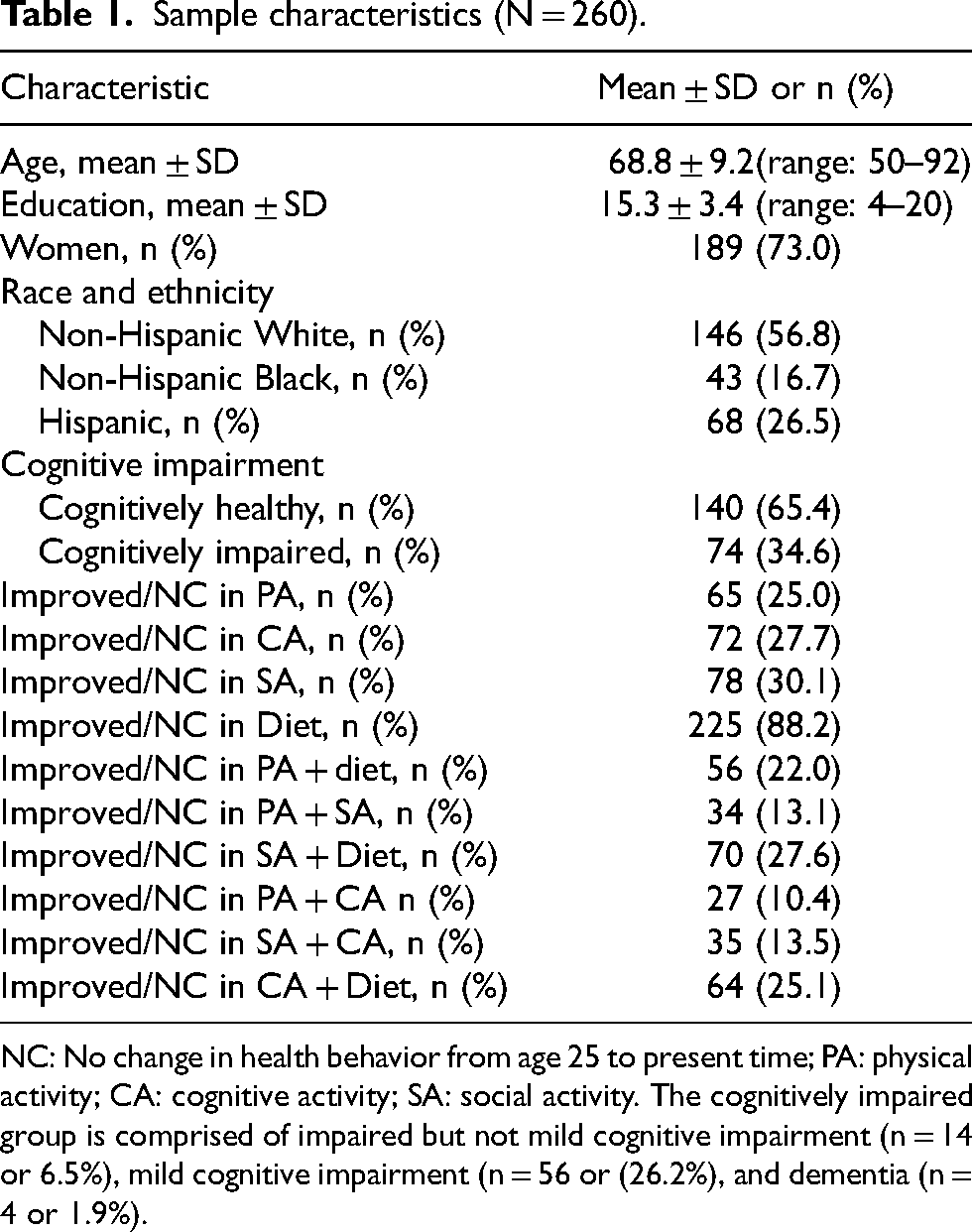
NC: No change in health behavior from age 25 to present time; PA: physical activity; CA: cognitive activity; SA: social activity. The cognitively impaired group is comprised of impaired but not mild cognitive impairment (n = 14 or 6.5%), mild cognitive impairment (n = 56 or (26.2%), and dementia (n = 4 or 1.9%).
Self-reported increases in physical activity were associated with higher current activity levels, better Mini-PPT and TUG performance, lower frailty, and greater MoCA score (Table 2). Similarly, self-reported increases in social activity were associated with higher social engagement, physical and cognitive activity, higher mini PPT, and lower frailty. Moreover, self-reported increases in dietary patterns were associated with higher MIND diet scores, greater cognitive activity, higher educational attainment, more favorable body composition profiles (lower weight, waist circumference, and percent body fat) and higher MoCA scores. However, self-reported increases in cognitive activity were not associated with current cognitive activity levels; although, those reporting increases were more socially engaged and showed better TUG and Cognivue performance than those reporting decreases. Ethnoracial differences in self-reported lifestyle change were observed for social activity (p = 0.043) and diet (p = 0.001), with increases more commonly reported by individuals identifying as White and decreases more commonly reported by those identifying as Hispanic.
Current levels of lifestyle behaviors, sociodemographics, and health behaviors by self-reported change in health behaviors from age 25.
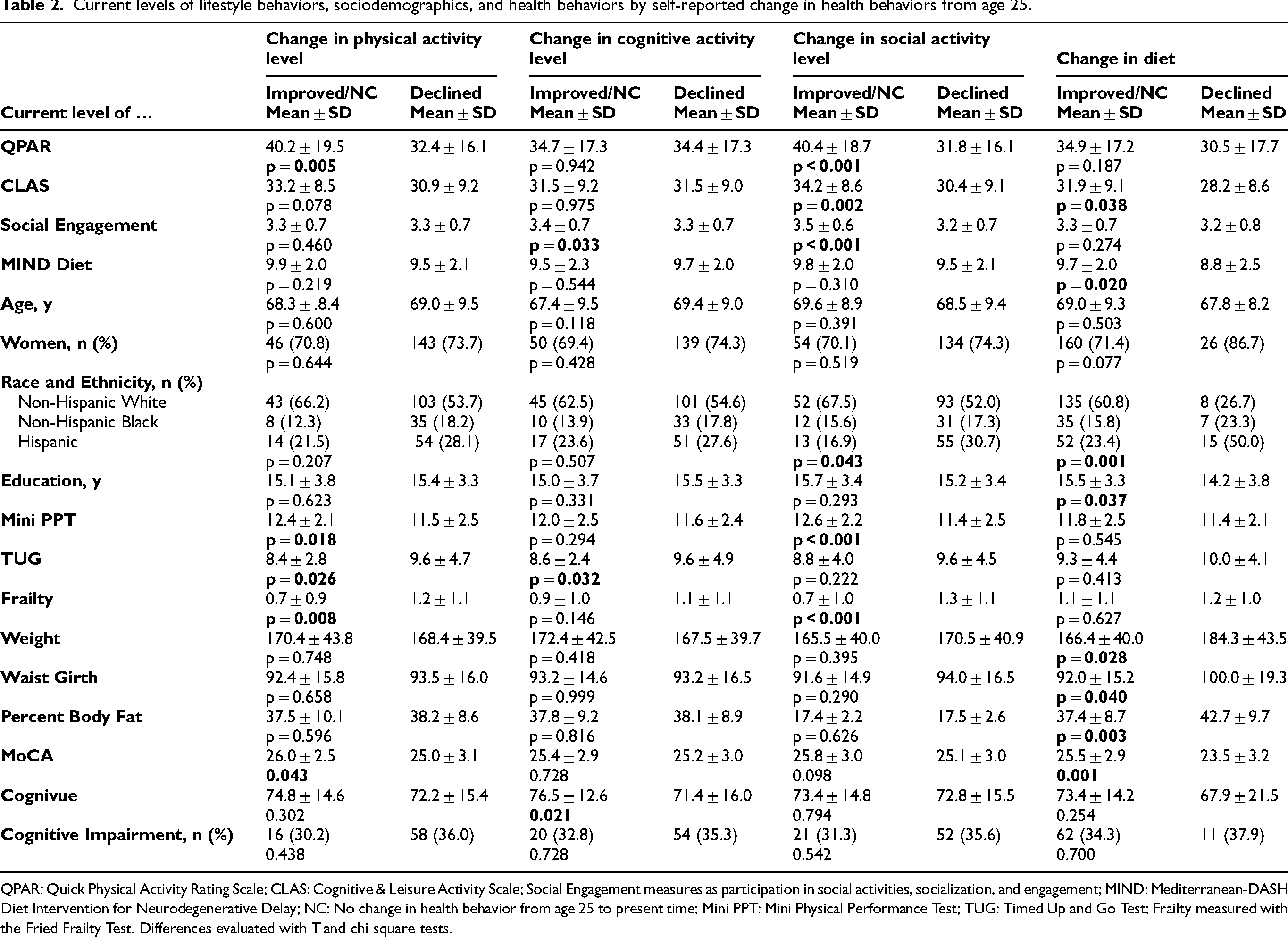
QPAR: Quick Physical Activity Rating Scale; CLAS: Cognitive & Leisure Activity Scale; Social Engagement measures as participation in social activities, socialization, and engagement; MIND: Mediterranean-DASH Diet Intervention for Neurodegenerative Delay; NC: No change in health behavior from age 25 to present time; Mini PPT: Mini Physical Performance Test; TUG: Timed Up and Go Test; Frailty measured with the Fried Frailty Test. Differences evaluated with T and chi square tests.
When we stratified relationships between self-reported lifestyle change, current lifestyle behavior, and objective health measures by cognitive impairment status, we found that those reporting improvement in lifestyle also reported higher current lifestyle behavior levels and had better health outcomes compared to those who reported decline, regardless of whether they were cognitively normal or cognitively impaired Table 3.
Associations between lifestyle change, current lifestyle behavior, and objective health outcomes by cognitive impairment status.
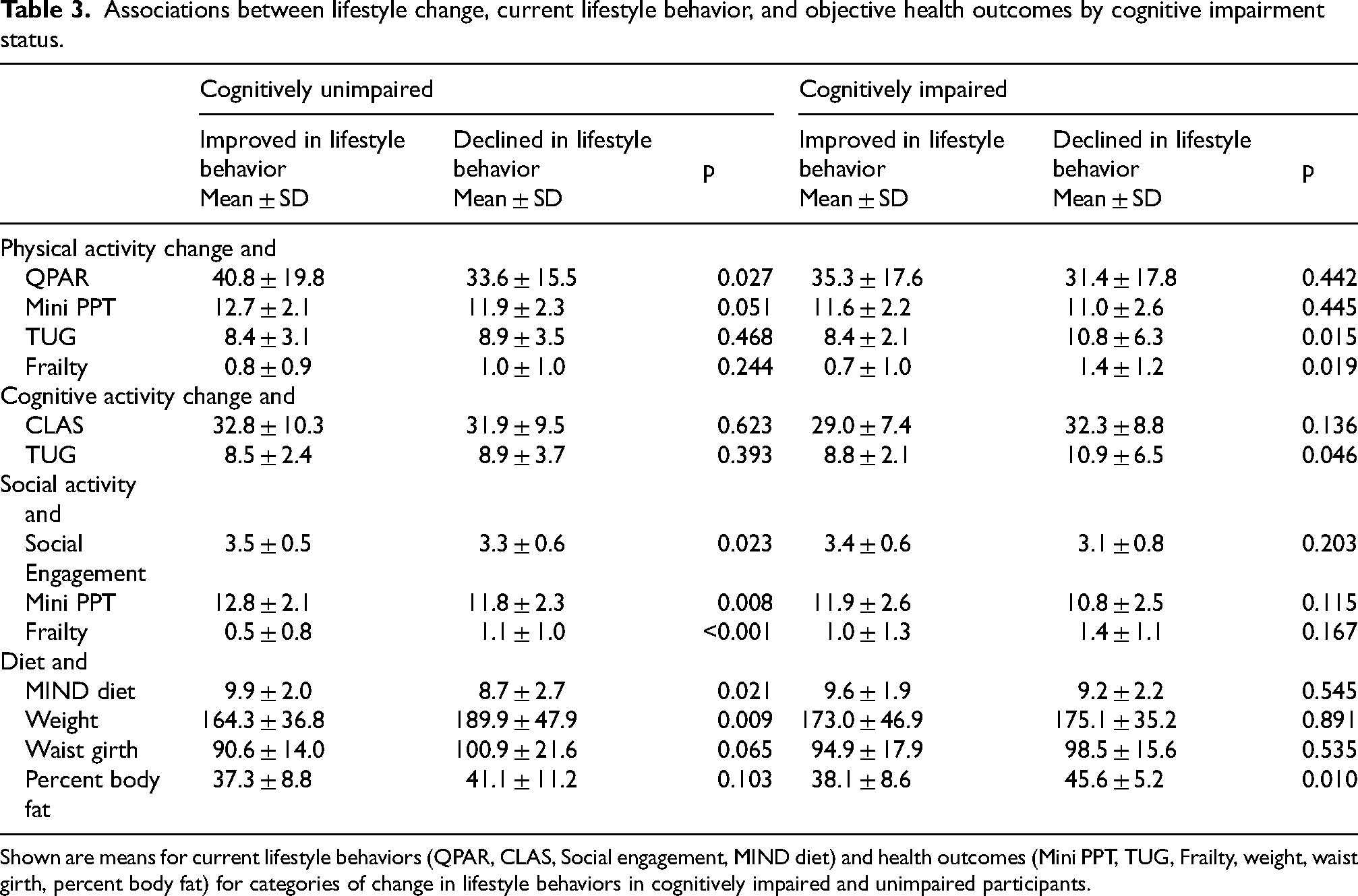
Shown are means for current lifestyle behaviors (QPAR, CLAS, Social engagement, MIND diet) and health outcomes (Mini PPT, TUG, Frailty, weight, waist girth, percent body fat) for categories of change in lifestyle behaviors in cognitively impaired and unimpaired participants.
Most of the evaluated domain-specific cognitive outcomes and biomarkers were not significant in Tier 1 analyses and were dropped from further investigation. Table 4 presents main effects of associations assessed in Tier 2 analyses with their Tier 1 p-values and FDR adjusted p-values. When assessed individually, positive changes from age 25 in physical activity and diet were associated with greater MoCA score and higher resilience while positive changes in social activity were associated with higher resilience and amygdala volume. When combined, positive changes in physical activity and diet were associated with greater resilience and higher MoCA score, with effects suggestive of synergistic interaction. Change in social activity, which was not individually related to MoCA, improved the relationships of physical activity and diet with MoCA by 33% (β=1.2 versus 0.9) and 54% (β=2.0 versus 1.3), respectively, while addition of positive change in cognitive activity to either physical activity or diet did not improve their effect on MoCA performance. In addition, several other behavior combinations such as social activity paired with physical activity or diet were associated with greater resilience, while addition of cognitive activity, not an individual correlate, improved the effects of physical activity and diet on resilience by 34% (β=17.4 versus 13.0) and 84% (β=23.9 versus 13.0), respectively. Moreover, pairing physical activity and cognitive activity with social activity improved the latter's effect on amygdala volume
Associations between change in lifestyle behaviors, resilience, MoCA, and amygdala volume.
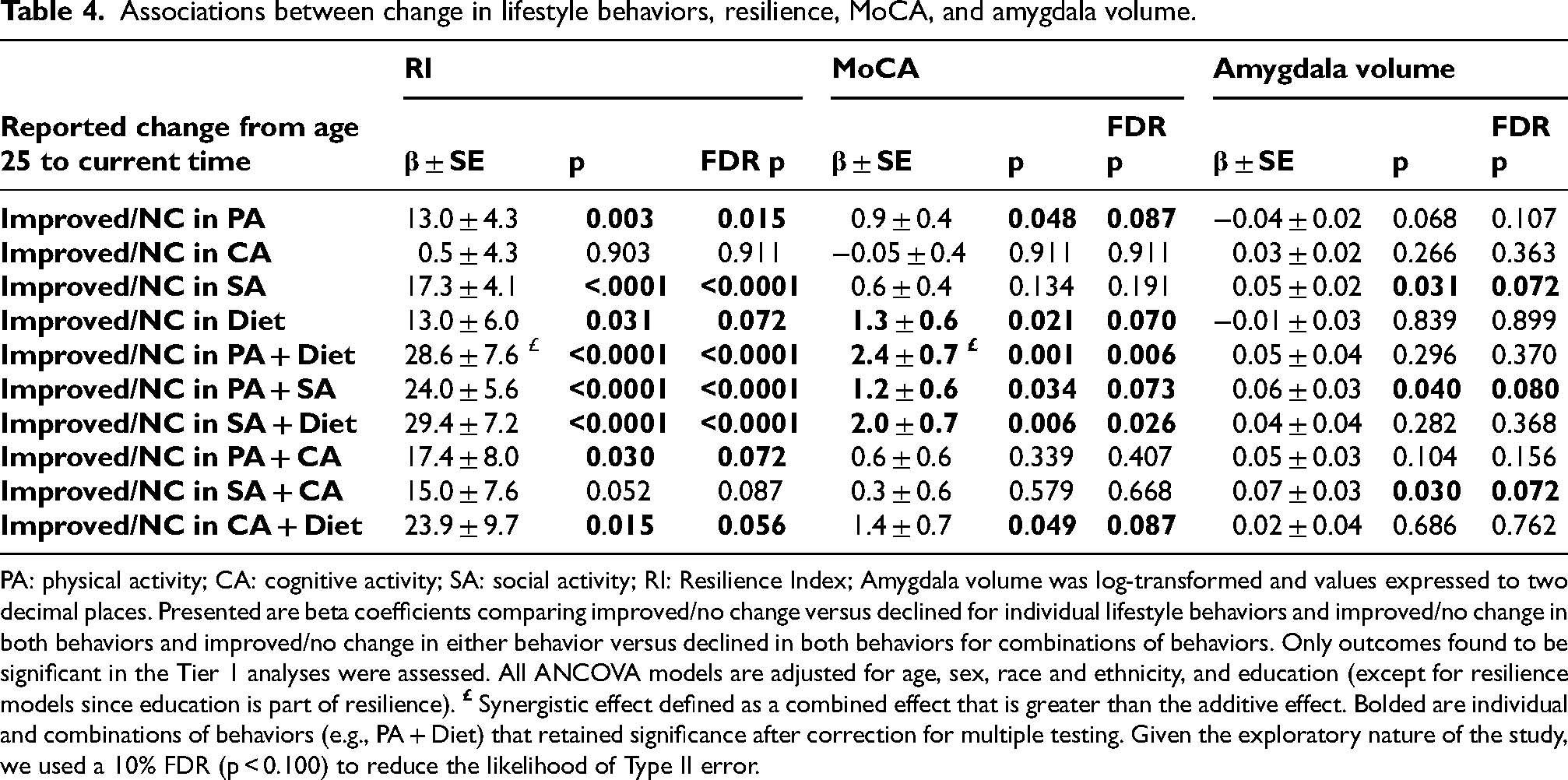
PA: physical activity; CA: cognitive activity; SA: social activity; RI: Resilience Index; Amygdala volume was log-transformed and values expressed to two decimal places. Presented are beta coefficients comparing improved/no change versus declined for individual lifestyle behaviors and improved/no change in both behaviors and improved/no change in either behavior versus declined in both behaviors for combinations of behaviors. Only outcomes found to be significant in the Tier 1 analyses were assessed. All ANCOVA models are adjusted for age, sex, race and ethnicity, and education (except for resilience models since education is part of resilience).
Relationships assessed in Tier 2 analyses (Table 4) were further evaluated for moderation by sex, race, ethnicity, and cognitive impairment status. We found no evidence of sex or racial (Non-Hispanic Black versus Non-Hispanic White) differences in the relationships between change in lifestyle behaviors and resilience, MoCA, and amygdala volume (data not shown). Moderation by ethnicity (Hispanic versus Non-Hispanic White) and cognitive impairment status are presented in Tables 5 and 6, respectively. We found significant interaction terms suggesting that social activity was associated with higher RI score (β=23.5 ± 10.5, p = 0.025) and cognitive activity + diet with lower MoCA (β=-3.6 ± 1.7, p = 0.032) in Hispanic versus Non-Hispanic White participants. In addition, several significant interaction terms with CI suggest physical activity + diet was associated with lower RI (β=-34.1 ± 15.4, p = 0.028) but greater MoCA score (β=2.8 ± 1.3, p = 0.027) in CI versus CU participants. Moreover, social activity alone (β=0.12 ± 0.04, p = 0.008) or combined with physical activity (β=0.17 ± 0.06, p = 0.005) and cognitive activity (β=0.14 ± 0.06, p = 0.021) was associated with greater amygdala volume only among CI participants. These relationships stratified by cognitive impairment status are presented visually in Figure 1 and support the significant interaction terms and their interpretation.
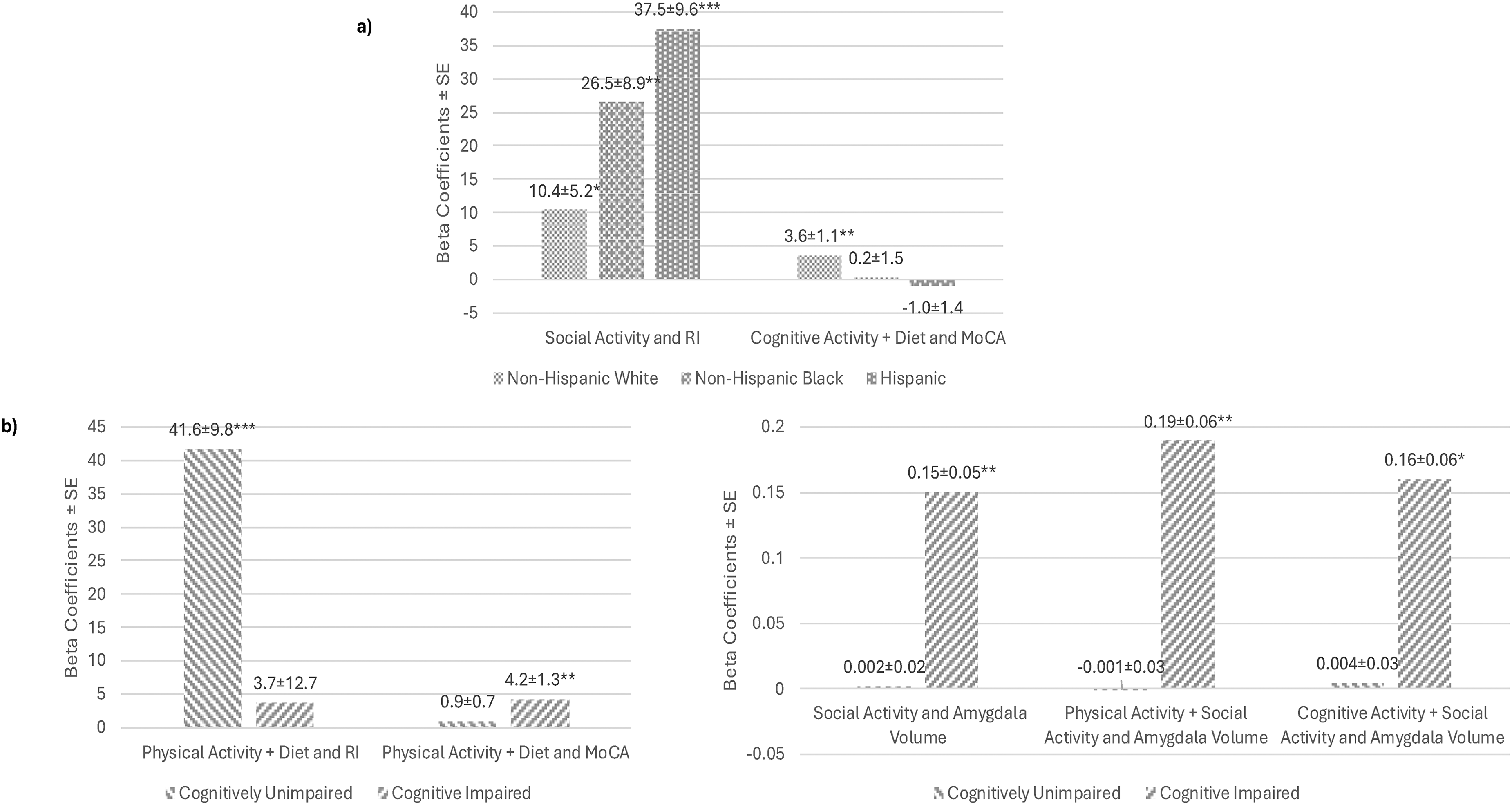
Relationships between individual and combined behavioral factors and outcomes stratified by race and ethnicity and cognitive impairment status. RI: Resilience Index; MoCA: Montreal Cognitive Assessment. Beta coefficients for relationships between change in individual (improvement/no change versus decline) and combined behaviors (improved in both versus declined in both) are shown to help visualize the interaction terms presented in Tables 5 and 6. Panel a) presents relationships stratified by race and ethnicity and panel b) presents relationships stratified by cognitive impairment status.
Moderation by ethnicity (hispanic versus non-hispanic white).
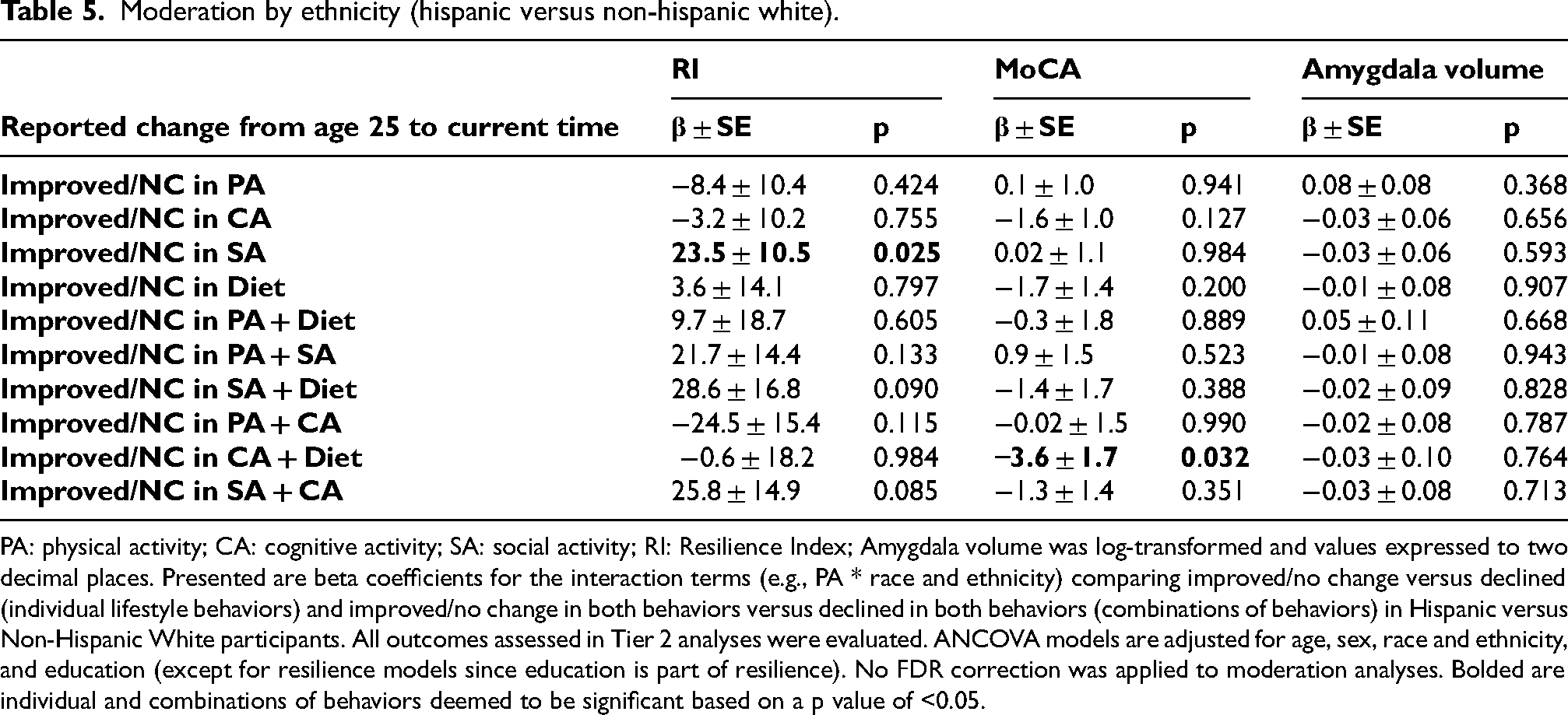
PA: physical activity; CA: cognitive activity; SA: social activity; RI: Resilience Index; Amygdala volume was log-transformed and values expressed to two decimal places. Presented are beta coefficients for the interaction terms (e.g., PA * race and ethnicity) comparing improved/no change versus declined (individual lifestyle behaviors) and improved/no change in both behaviors versus declined in both behaviors (combinations of behaviors) in Hispanic versus Non-Hispanic White participants. All outcomes assessed in Tier 2 analyses were evaluated. ANCOVA models are adjusted for age, sex, race and ethnicity, and education (except for resilience models since education is part of resilience). No FDR correction was applied to moderation analyses. Bolded are individual and combinations of behaviors deemed to be significant based on a p value of <0.05.
Moderation by cognitive impairment status (ci versus cu).
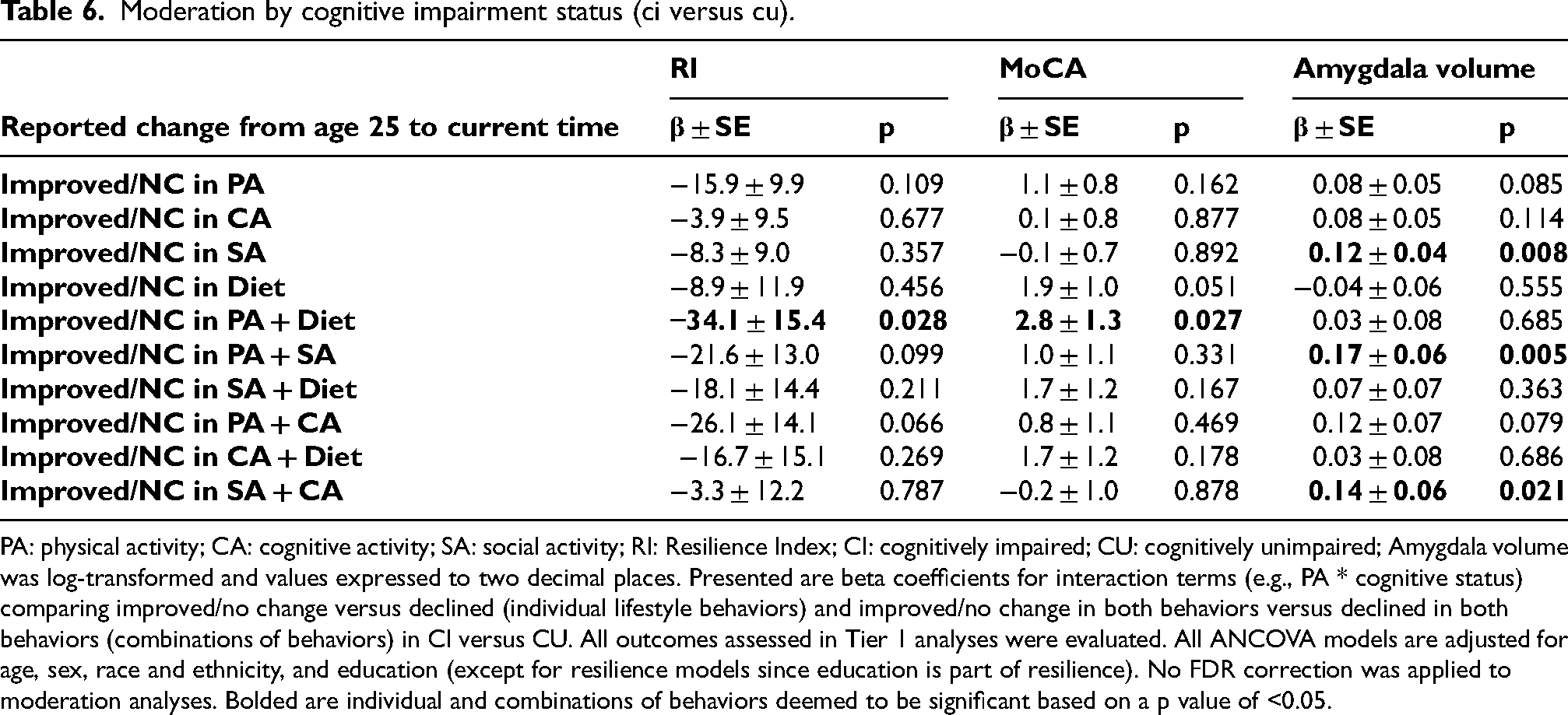
PA: physical activity; CA: cognitive activity; SA: social activity; RI: Resilience Index; CI: cognitively impaired; CU: cognitively unimpaired; Amygdala volume was log-transformed and values expressed to two decimal places. Presented are beta coefficients for interaction terms (e.g., PA * cognitive status) comparing improved/no change versus declined (individual lifestyle behaviors) and improved/no change in both behaviors versus declined in both behaviors (combinations of behaviors) in CI versus CU. All outcomes assessed in Tier 1 analyses were evaluated. All ANCOVA models are adjusted for age, sex, race and ethnicity, and education (except for resilience models since education is part of resilience). No FDR correction was applied to moderation analyses. Bolded are individual and combinations of behaviors deemed to be significant based on a p value of <0.05.
Discussion
Consistent with prior reports, we found that retrospective self-reported healthy changes in lifestyle appear to promote brain health in later life. By asking participants to compare their lifestyle behaviors at age 25 against current behaviors, we were able to provide plausible evidence linking healthy lifestyle behaviors throughout much of adulthood with better late-life brain health outcomes across global cognition, resilience, and biomarkers. Moreover, we showed that, while individual lifestyles may offer brain health benefits, the greatest benefits come from combining lifestyle behaviors (e.g., physical activity + diet). Furthermore, we showed that these benefits vary based on ethnic background and cognitive status. These findings have important public health implications.
Physical activity and brain health
The cognitive benefits of physical activity are well recognized. Longitudinal prospective studies such as the British 1946 Birth Cohort Study 4 and the Trondelag Health Study (HUNT, previously Nord-Trondelag Health Study) 5 have indicated that while being physically active at any time in adulthood is linked to better cognition in late-life, maintaining or improving physical activity level provides the most benefits. Using a simple question asking participants to compare their level of physical activity behaviors at age 25 to their current level, we found support for the idea that maintaining a physically active lifestyle provides late-life cognitive benefits as measured by better performance on the MoCA, a global measure of cognition. This question allowed us to track patterns of change in physical activity since early life. While asking individuals to recall their activity level so far back in time may raise questions of recall bias, the significant positive correlations of this measure with current reported levels of physical activity as well as with objective measures of global physical performance (i.e., better performance on mini PPT and TUG) and frailty (i.e., lower frailty in individuals who report improvement/maintenance of physical activity level since age 25) support its use as a proxy measure of change in “lifelong” patterns of physical activity. Other lifestyle measures including change in social activity and diet were similarly correlated with current levels and with objective health outcomes. These relationships were observed in both CU and CI participants, providing further support for these novel cross-sectional measures of change in lifetime lifestyle behavior.
In addition, we found greater levels of resilience in individuals reporting increases in physical activity level than in those reporting decline. Our findings are aligned with longitudinal reports that staying physically active throughout life helps sustain cognitive function and support the idea that lifelong engagement in physical activity contributes to building cognitive reserve and resilience in later life, 66 findings supported by reports from large prospective studies and systematic reviews.67,68 Positive change in physical activity was however not related in our study to blood-based or imaging biomarkers of neurodegeneration or AD pathology, which is partially in line with findings from a recent longitudinal study of no link between lifetime walking and neurodegeneration or WMH volume. 69 The lack of a relationship between change in physical activity from age 25 and AD pathology in our study may be explained by the makeup of our sample, which consisted of older adults who were either cognitively normal or in very early stages of disease. Taken together, these findings suggest that lifelong physical activity, late-life resilience, and current physical activity may be engaged in a dynamic way to explain the cognitive benefits of lifelong physical activity.
Diet and brain health
Healthy diets such as the MIND diet have been previously linked to better global cognitive functioning in older adults. 70 Our finding that maintaining a healthy diet throughout life is associated with better global cognitive performance is in line with prior reports of a decreased risk of dementia among individuals who adhere to healthy diets such as the MIND diet, 15 with the added benefit of a longer “follow-up period” as recalled by study participants. Maintaining a healthy diet was additionally associated with higher levels of resilience, finding that is supported by prior reports linking the MIND diet to better cognitive functioning, independently of brain pathology, which is suggestive of possible contributions of a healthy diet to cognitive resilience in older adults. 70 In terms of impact on biomarkers, we found no associations between changes in diet and disease biomarkers investigated in our study, which is in line with recent reports from large longitudinal studies with extended follow-up times 16 reporting no relationship between long-term adherence to dietary recommendations including Mediterranean diet and late-life AD pathology. Larger studies may be needed to detect more robust responses in disease biomarkers. These findings highlight how importance maintaining a healthy diet is to brain health in later life and suggest greater resilience as a potential mechanism through which it may exert its cognitive benefits.
Cognitive activity and brain health
Sustained engagement in cognitive activity in early and midlife has been linked to better cognitive outcomes in later life including reduced risk of dementia and increased dementia-free survival 2 although clear evidence of a relationship with global cognitive function is lacking. Most of the evidence for midlife cognitive activity comes from studies of workplace occupational complexity, often measured with indicators of cognitive stimulation (job demands and controls) and occupational skill level.8,9 In our study, increases in cognitive activity however were not linked to cognitive function, resilience, or ADRD biomarkers. These null associations differ from other reports supporting significant relationships between lifelong cognitive activity and brain health outcomes.71,72 These differences may be due to how change in cognitive activity was measured (self-report; work versus nonwork related cognitive activities were not differentiated), 73 or to differences in the study populations in terms of ethnoracial and cognitive status makeup.71,74 Incorporating measures that combine workplace and leisure cognitive stimulation levels may better capture the positive impact of lifelong cognitive engagement on global cognition, resilience, and disease biomarkers in later life.
Social activity and brain health
Late-life social isolation is a well-known risk factor for dementia. 2 Higher frequency in midlife social contacts has also been linked to more favorable global cognitive function trajectories in later life 7 suggesting a lifelong impact of social engagement on late-life cognitive function. In support of this notion, we found evidence of a positive impact of remaining socially engaged in late-life brain health. Compared to participants reporting decline, those who maintained or improved level of social activity from age 25 had higher resilience levels. Moreover, although we did not find a relationship with cognitive performance in our study, increases in social engagement were correlated with greater amygdala volumes. This finding is supported by evidence that social capital characteristics such as more extensive social networks 75 and social bridging are linked to preserved gray matter density in limbic system structures including amygdala, 76 while loneliness with smaller amygdala volumes in older adults. 77 Prior reports from the AD Neuroimaging Initiative 3 study of reduced amygdala volume in the absence of atrophy in other brain areas including the hippocampus among cognitively healthy individuals who converted to MCI 78 and in MCI groups who converted to AD compared to those who remained stable over 2 years, 79 further support our findings by suggesting that amygdala atrophy may be an early biomarker of disease progression in AD. The significant relationships with amygdala but the lack of a link with other ADRD imaging biomarkers suggest that our MCI participants may be in the process of transitioning to AD but have not yet reached the stage where there is significant atrophy in the hippocampus, temporal lobe, and cortical thickness.
Combined lifestyle behaviors and brain health
Most importantly, we identified pairs of healthy behaviors that work together to promote brain health. Maintained/improved engagement in physical activity and diet showed the most consistent relationships with brain health outcomes. Positive changes in these two health behaviors synergistically interacted to enhance their impact on MoCA performance and resilience level. Interestingly, while not correlated with cognitive performance, increases in social activity level improved the positive effects of physical activity and diet on MoCA, suggesting a more “supportive” role for lifelong social engagement on late-life cognition. In a similar manner, positive changes in cognitive activity improved the observed effects of physical activity and diet on resilience and that of diet on MoCA score. Moreover, the positive effect of lifelong social activity on amygdala volume, was further improved when combined with positive change in physical activity or cognitive activity, supporting their joint effect on preservation of brain structures, which may be affected early in the disease process. Given that prior reports on lifelong patterns of health behaviors and brain aging 30 including multi-domain intervention studies32–33 tended to pool together various health behaviors when measuring healthy lifestyles, precluding direct comparison, our findings provide valuable insights into the brain health benefits conferred by specific combinations of health behaviors, therefore aiding in the development of more effective multidomain lifestyle interventions to improve brain health and reduce risk of cognitive decline and dementia in late-life.
Noteworthily, we found these relationships to vary by ethnic background and cognitive status. More specifically, self-reported increases in cognitive activity + diet were associated with lower global cognition in Hispanic participants. This finding aligns well with prior reports of differential associations between lifestyle behaviors and later life cognitive function, favoring White individuals,80,81 possibly stemming from differences in SES, education, early life adversities, and other psychosocial factors affecting lifestyle habits and risk factors for dementia. 19 Interestingly, we found ethnic differences in the impact of social activity on resilience, where Hispanic older adults reaped greater benefits on resilience by maintaining social engagement compared to White older adults.
While social engagement has been previously linked to better health and cognitive outcomes in most older adults including those of Hispanic, 82 whether its impact on cognition varies by race and ethnicity remains unclear. Some studies report positive associations in White individuals but not Black individuals, 83 while others report negative relationships in Hispanic individuals. 84 Though not investigated in our study, the observed greater benefits on resilience in Hispanic participants may be the result of larger and more integrated social networks, 85 which are highly valued in the Hispanic culture. Little differences by race were found. Further studies are needed to understand the extent and potential mechanisms for the ethnic differences observed in our study, which will help guide the design of effective interventions to address these disparities.
We also found that the positive effect of increased physical activity + diet on MoCA was greater in CI than CU participants. Support for these findings comes from the recently published POINTER study, a 2-year multi-domain lifestyle intervention in a large cohort of older adults at risk for cognitive decline and dementia, which found greater benefits on global cognitive function in participants with lower baseline cognitive function. 33 Moreover, CI individuals benefited more than CU from maintaining social activity, alone or in combination with physical activity or cognitive activity, on gray matter volume in the amygdala, a brain structure implicated in emotional memory formation/processing and cognitive functions. Interestingly, we also found that the positive effect of physical activity + diet on resilience was lower in the CI group. Together, these findings suggest that maintaining a healthy lifestyle that combines physical activity, diet, cognitive activity, and social activity can impact brain health in ways that could be more salient in the presence of CI, although this and the lower impact on resilience should be the focus of future investigation.
The null relationships of lifestyle change with most disease biomarkers and individual cognitive measures assessed in this study may be specific to our study population, which consists of individuals with early-stage disease, who have not yet reached significant levels of neuropathology. The possibility that other biomarkers, not assessed in our study, may be more sensitive to lifestyle changes should also be evaluated in future studies. Moreover, the impact of lifestyle change on global but not domain-specific cognition suggests that the effects of lifestyle change in early ADRD are subtle and may be easier detected by global measures than specific cognitive tests. In addition, the lack of moderation of these relationships by sex, which is in line with prior reports 86 supports the idea that lifelong increases in lifestyle behaviors may have similar impact on late-life brain health in women and men, although validation in future studies is warranted given the lack of consensus among studies.
Limitations
Our study has several limitations that need to be considered when interpreting the results. First, our measures of life-course health behavioral change required participants to recall activity levels going decades back in time. This could lead to recall bias. While we were unable to directly measure recall bias in our study, our “informal” validation approach of comparing patterns of lifestyle change on current levels of engagement and with objective health measures provides support against the idea of recall bias significantly impacting the results. As these measures did not require participants to recall specific levels of participation in activities (e.g., number of hours of physical activity per week) but rather asked for a gross recall of overall engagement at age 25, this may capture past activity better 87 and make the comparison against current levels easier. Additional validation comes from evidence that the associations between lifestyle change, current lifestyle behaviors, and health outcomes were similar regardless of cognitive status. While recall is more accurate in the short term, reports that distant recall of lifestyle behaviors as far as 30–35 years in the past is fairly accurate88,89 further support the validity of our self-reported measures of lifelong lifestyle change. Second, while the measure of change in cognitive activity was not correlated with CLAS, this may have less to do with recall bias than to CLAS‘ focus on cognitive leisure activities, rather than work-related cognitive activities, which the extant literature suggests may provide the strongest benefits. Third, patterns of change in lifestyle behaviors were based on perceived changes from age 25 to current time and are therefore a proxy measure of lifelong behaviors. Future studies evaluating the impact of individual or combined lifelong health behaviors on brain health in later life need to consider multiple points of measurement throughout life. Fourth, the high preponderance of women in our sample limits the generalizability of findings. While overrepresentation of women in dementia research is a common occurrence, possibly due to women's greater longevity and higher prevalence of AD, future studies should seek a more balanced sex distribution to enhance the generalizability of research findings. Finally, while a prospective study design would be a better choice to measure change over time, our innovative way of measuring change in lifestyle behaviors within a cross-sectional design allowed for an effective “proxy” evaluation of lifelong change.
Conclusions
We found “lifelong” engagement in healthy lifestyle behaviors including physical activity, diet, cognitive activity, and social activity to promote brain health in later life across measures of cognitive function, resilience, and amygdala volume. We identified combinations of lifestyle behaviors that offer stronger benefits than individual lifestyle factors as well as specific lifestyle behaviors that maximize the impact of other behaviors by increasing resilience, improving cognitive performance, and promoting brain health. Potential variations in these relationships by ethnic background and cognitive impairment status may exist but need to be further investigated. Findings provide insights into the late-life brain benefits of maintaining a healthy lifestyle and aid in the design of effective targeted multidomain lifestyle interventions to improve brain health and prevent cognitive decline.
Footnotes
Acknowledgements
HBI would not be possible without the support of the Comprehensive Center for Brain Health's staff, postdoctoral fellows, and study participants.
ORCID iDs
Ethical considerations
The Institutional Review Board at University of Miami approved the Health Brain Initiative study (approval: 20200208) on April 28, 2020.
Consent to participate
HBI participants provide written informed consent at baseline and are re-consented as needed with protocol changes. Study partners provide verbal consent (waiver of written consent approved by IRB).
Consent for publication
Not applicable
Author contribution(s)
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The Healthy Brain Initiative is supported by NIH R01AG071514, R01AG071514S1, R01NS101483, R01NS101483S1, and R56AG074889.
Declaration of conflicting interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Dr. Galvin is the creator of the NSCT, QPAR, CLAS, and RI used in this study. Dr. Galvin is the Chief Scientific Officer for Cognivue, a device used in this study. Dr. Tolea, Dr. Besser, Dr. O'Shea, and Dr. Galvin are Associate Editors of this journal but were not involved in the peer-review process of this article nor had access to any information regarding its peer-review. Dr. Sol, Dr. Chrisphonte, Dr. Kleiman, Dr. Baig, and Dr. Joshi declare no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
The data supporting the findings of this study are available on request from the corresponding author. The data are not publicly available due to privacy or ethical restrictions.
