Abstract
Background
Dementia is a leading cause of mortality worldwide, with its prevalence projected to rise sharply in the coming decades. Established risk factors include advanced age, hypertension, diabetes, obesity, smoking, excessive alcohol consumption, physical inactivity, social isolation, and depression. Increasing evidence suggests that vaccination—by preventing infections that may trigger or accelerate neurodegeneration—could play a protective role against dementia, though findings remain inconsistent.
Objective
To systematically review observational evidence on the association between influenza vaccination and the risk of developing dementia, with attention to demographic, social, and health-related moderating factors.
Methods
This systematic review, conducted in accordance with PRISMA 2020 guidelines, synthesized evidence from Scopus and Web of Science. Eligible studies were observational in design, employed validated dementia diagnoses, and reported demographic, social, or health covariates. Study quality was assessed using the Newcastle–Ottawa Scale.
Results
Seven studies, encompassing 9,866,019 participants, met the inclusion criteria. Six of these studies reported a significant association between influenza vaccination and a reduced risk of dementia. Protective effects were particularly evident with repeated vaccinations and among individuals with chronic comorbidities. Key moderating factors included age, sex, vaccination frequency, and specific health conditions.
Conclusions
Current evidence suggest that influenza vaccination may confer a protective effect against dementia, especially in populations with chronic diseases who receive regular vaccinations. These results highlight the potential of influenza vaccination as a scalable, cost-effective public health measure to mitigate dementia risk and underscore the need for further high-quality longitudinal research.
Introduction
According to statistics of the World Health Organization (WHO), dementia is currently the seventh leading cause of death worldwide.1,2 A further increase in this disease is expected due to population aging, from the current 55 million cases to 135 million by 2050. 3 Dementia is a syndrome that can be caused by several diseases which, over time, destroy nerve cells and damage the brain. This damage usually leads to a deterioration of cognitive functions beyond what is expected from the usual consequences of natural aging.
The decline of cognitive functions is commonly accompanied, and sometimes even preceded, by changes in mood, emotional control, behavior, or motivation. 1 Dementia has physical, psychological, social, and economic impacts not only on people living with dementia, but also on their caregivers, families, and society. Informal caregivers alone account for approximately 50% of the total costs of this disease, which amount to 1.3 trillion USD worldwide. Among the factors influencing the onset of dementia are age, high blood pressure, diabetes, overweight, smoking, excessive alcohol consumption, low physical activity, social isolation, and depression. 1 For treatment, medication is used to slow down the progression of the disease and limit the symptoms of dementia; however, these drugs cannot cure the disease or stop the degeneration of brain cells. 4 For that reason, preventive strategies aimed at suppressing the above-mentioned risk factors and searching for other preventive possibilities are of crucial importance. For example, vaccines can reduce the risk of developing infections or limit their severity, reduce the neuroinflammatory burden of the individual, and modulate immune mechanisms. These processes can prevent viral, bacterial, and fungal infections which may increase neuroinflammation and thereby cause or exacerbate neurodegeneration and, consequently, dementia.5,6
According to the meta-analysis of Sun et al., which was composed of six cohort studies including 2,087,195 older adults, at least one vaccination against influenza reduced the relative risk of dementia by 31%. 7 The meta-analysis by Veronese et al. similarly reported a 29% reduction of relative dementia risk after influenza vaccination. 8 Research with animal models likewise reports improvements in the cognitive abilities of mice following vaccination. 9 In contrast to these positive results in favor of vaccination, the cohort study of Douros et al. reported that common vaccines, including influenza vaccination, were not associated with a reduced risk of dementia, and that vaccinated individuals even had an increased occurrence of dementia. 10 Similarly, the study of Appel et al. reported an increased incidence of dementia in participants vaccinated against influenza. 11
Research aim
There exist several meta-analyses and systematic reviews devoted to the relationship between influenza vaccination and dementia; however, these studies do not examine in detail the factors that could act as mediators or moderators of this relationship. Understanding the factors that play a role in the association between influenza vaccination, and the risk of dementia can help us to better explain why inconsistencies occur across studies. The inclusion of these factors into a systematic review can therefore provide a more comprehensive understanding of the complex relationship between influenza vaccination and dementia risk.
The aim of our systematic review is to describe these individual factors. To achieve this research aim, we formulate the following research question:
What are the potential factors (demographic, social, and health) that can influence the relationship between influenza vaccination and the risk of developing dementia?
Methods
This systematic review was conducted in accordance with the PRISMA 2020 guidelines. The literature search was carried out in December 2024 in the databases Scopus and Web of Science. Both authors (VR and DV) participated equally in the search process.
Search strategy
The following query was used for the Scopus database: TITLE-ABS-KEY (influenza OR flu) AND TITLE-ABS-KEY (vaccin*) AND TITLE-ABS-KEY (dement* OR alzheimer* OR lewy OR “Posterior cortical atrophy” OR “Binswanger” OR “Progressive supranuclear palsy” OR “Frontotemporal disorder*” OR “Frontotemporal degeneration” OR “Corticobasal degeneration” OR “Corticobasal syndrome”) AND NOT TITLE-ABS-KEY (cross-sectional AND stud*) AND (LIMIT-TO (DOCTYPE, “ar”)) AND (LIMIT-TO (LANGUAGE, “English”)).
For the Web of Science database, the following query was applied: (((ALL = (influenza OR flu)) AND ALL = (vaccin*)) AND ALL = (dement* OR Alzheimer* OR Lewy OR “Posterior cortical atrophy” OR “Binswanger” OR “Progressive supranuclear palsy” OR Frontotemporal disorder* OR Frontotemporal degeneration OR Corticobasal degeneration OR Corticobasal syndrome) NOT TS = cross-sectional stud*) x language: English x document type: Article or Early Access
Inclusion criteria
Studies were included if they met the following criteria:
Observational study design. Examined the relationship between influenza vaccination and dementia. Contained a validated diagnosis of dementia (e.g., based on the International Classification of Diseases or the Diagnostic and Statistical Manual of Mental Disorders). Reported demographic, social, or health-related factors.
Exclusion criteria
Studies were excluded if:
They were systematic reviews or meta-analyses. They did not include human participants. They did not include adults. They employed a cross-sectional design. They were not published in English. The full text was not available.
Selection process
The selection was carried out in two phases. In the first phase, screening was performed based on title and abstract. Each researcher (VR and DV) independently searched the databases and identified studies eligible for the next stage. Data extraction was performed using a standardized Excel sheet, including study characteristics (region, sample size, population), dementia classification, and examined factors (age, gender, comorbidities, number of doses).
In the second phase, full-text articles of potentially eligible studies were reviewed in detail, and final inclusion was determined according to the predefined criteria. Any discrepancies in data extraction or study inclusion were resolved through discussion between the two researchers. The workload was evenly divided between both authors. No automation tools were used, and study authors were not contacted for additional information. The original data from the studies were not transformed in any way.
Study selection
The initial search yielded 393 records from Web of Science and Scopus. After removing 57 duplicates, 336 studies remained. Based on title and abstract screening, 323 studies were excluded. Thirteen articles proceeded to the full-text review, of which six were excluded because they did not measure factors influencing the relationship between influenza vaccination and dementia. Ultimately, seven studies met the inclusion criteria and were incorporated into the final analysis.
Quality assessment of studies
The quality of the included studies was assessed using the Newcastle–Ottawa Scale (NOS), developed jointly by the universities of Newcastle and Ottawa for evaluating non-randomized studies. 12 The NOS applies a “star system,” assessing studies across three domains: (a) selection of study groups, (b) comparability of groups, and (c) ascertainment of exposure or outcome. A maximum of 9 stars can be awarded: 4 for selection, 2 for comparability, and 3 for outcomes. 13 All included studies scored between 7 and 9 stars, which according to the NOS coding manual indicates good quality. Both researchers participated equally in quality assessment of the studies, the inconsistencies were resolved through the discussion.
Results
As shown in Diagram 1, seven studies were included in this systematic review.11,14–19 Altogether, these studies encompassed a total of 1,848,372 vaccinated individuals and 8,017,647 unvaccinated individuals.
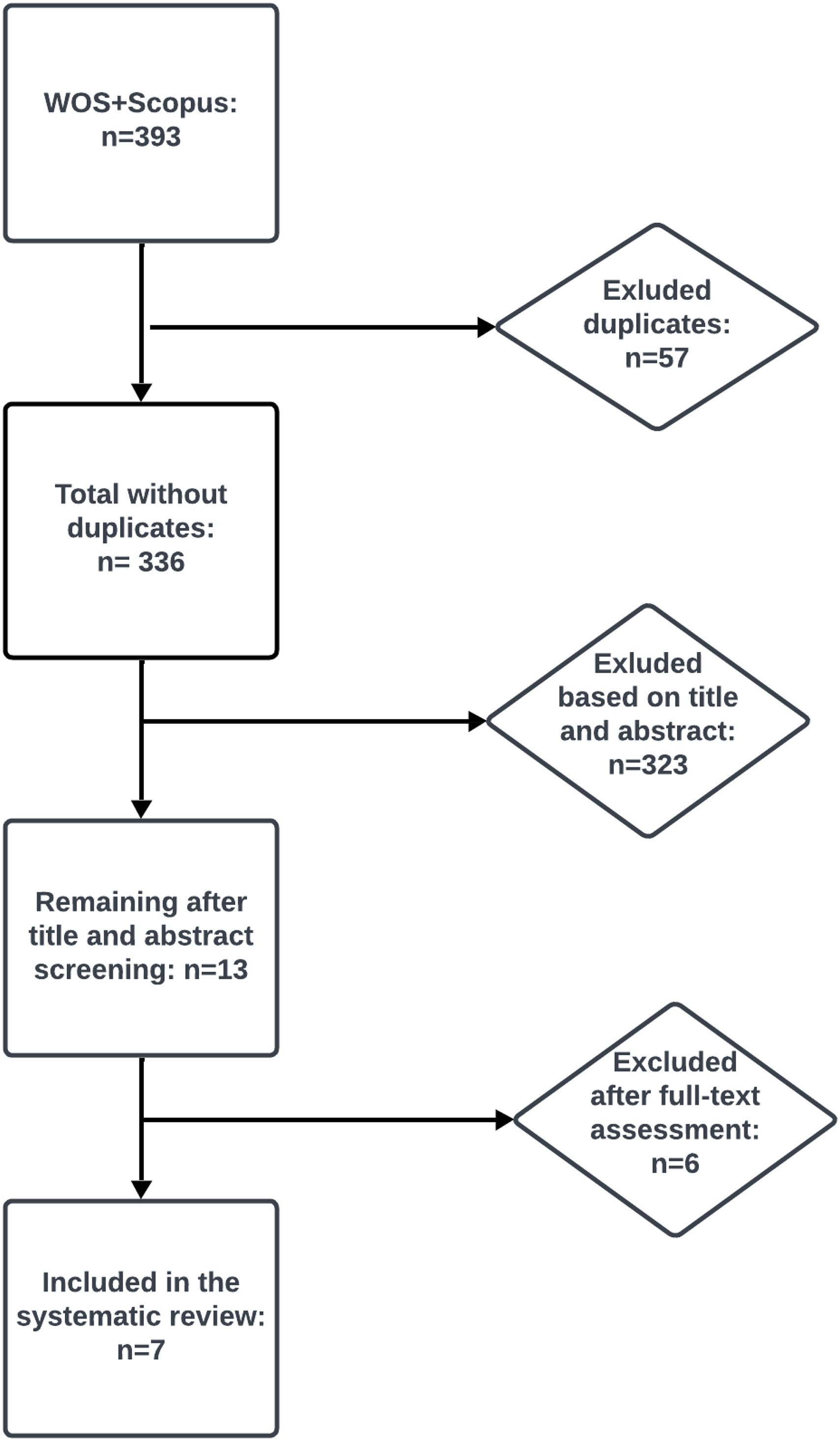
- PRISMA Flow.
As summarized in Table 1, two studies were conducted in North America, three in Europe, and two in Taiwan. Except for study by Wiemken et al., 18 where 96% of the sample were men, the remaining studies reported an approximately equal representation of men and women. The studies by Liu et al. 14 and Luo et al. 16 exclusively included patients with chronic kidney disease (CKD) and chronic obstructive pulmonary disease (COPD), respectively.
Characteristics of included studies.
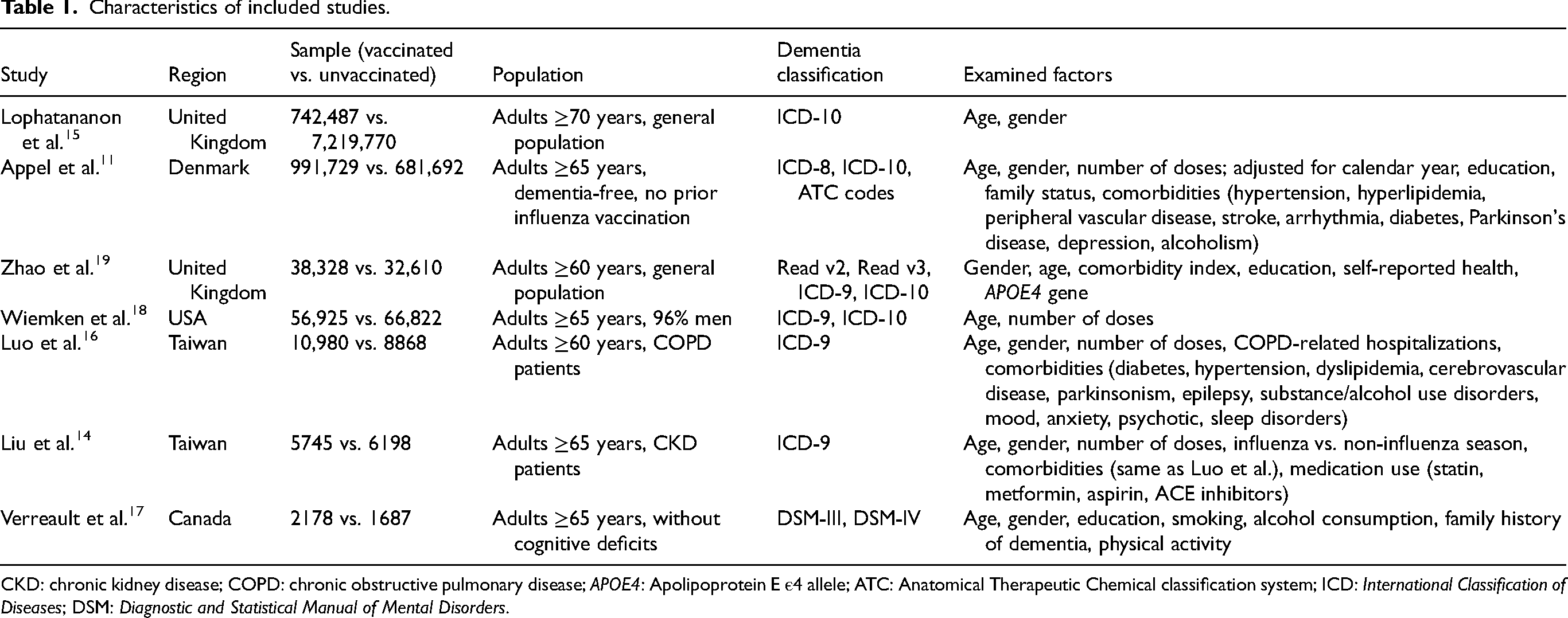
CKD: chronic kidney disease; COPD: chronic obstructive pulmonary disease; APOE4: Apolipoprotein E ε4 allele; ATC: Anatomical Therapeutic Chemical classification system; ICD: International Classification of Diseases; DSM: Diagnostic and Statistical Manual of Mental Disorders.
For dementia diagnosis, all studies relied on versions of the International Classification of Diseases (ICD), except for Verreault et al., 17 which used the Diagnostic and Statistical Manual of Mental Disorders (DSM).
Six out of the seven included studies suggest that influenza vaccination is associated with a reduced risk of developing dementia. Lophatananon et al. 15 reported that influenza vaccination was associated with a slightly reduced risk of dementia (aHR = 0.96, 95% CI [0.94, 0.97]). Zhao et al. 20 found a stronger effect, showing that influenza vaccination was negatively related to the risk of dementia (HR = 0.74, 95% CI [0.65, 0.84]). Wiemken et al. 18 likewise reported that the probability of developing dementia was significantly lower in vaccinated individuals compared to those without vaccination (HR = 0.86, 95% CI [0.83, 0.88]). Luo et al. 16 observed an adjusted hazard ratio of 0.68 (95% CI [0.62, 0.74], p < 0.001), indicating greater protection against dementia in vaccinated patients. Similarly, Liu et al. 14 reported that the risk of dementia was lower in vaccinated patients than in those unvaccinated across influenza season, non-influenza season, and all seasons combined (aHR = 0.68, 0.58, and 0.64; all p < 0.0001). Verreault et al. 17 also found a lower risk of dementia in vaccinated individuals (OR = 0.81, 95% CI [0.55, 1.19]), though the association did not reach statistical significance. In contrast to these findings, the study by Appel et al. 11 indicated that individuals who had ever been vaccinated against influenza experienced a 4% higher rate of dementia occurrence compared to those who had not been vaccinated (IRR = 1.04, 95% CI [1.02, 1.05]).
The analysis of included studies further considered several key factors, the detailed overview of which is presented in Table 2. With respect to gender, four of the seven studies reported no statistically significant difference in dementia risk between men and women following influenza vaccination. Lophatananon et al. 15 observed a slightly lower risk in women (HR = 0.95, 95% CI [0.93, 0.97]) compared to men (HR = 0.97, 95% CI [0.94, 0.99]). Luo et al. 16 found that vaccination provided a somewhat greater protective effect in men receiving four or more doses (HR = 0.77, 95% CI [0.67, 0.89], p < 0.001) compared with women at the same dose level (HR = 0.85, 95% CI [0.72, 0.99], p < 0.05). Wiemken et al. 18 did not report gender-specific results.
Main statistical results of included studies.
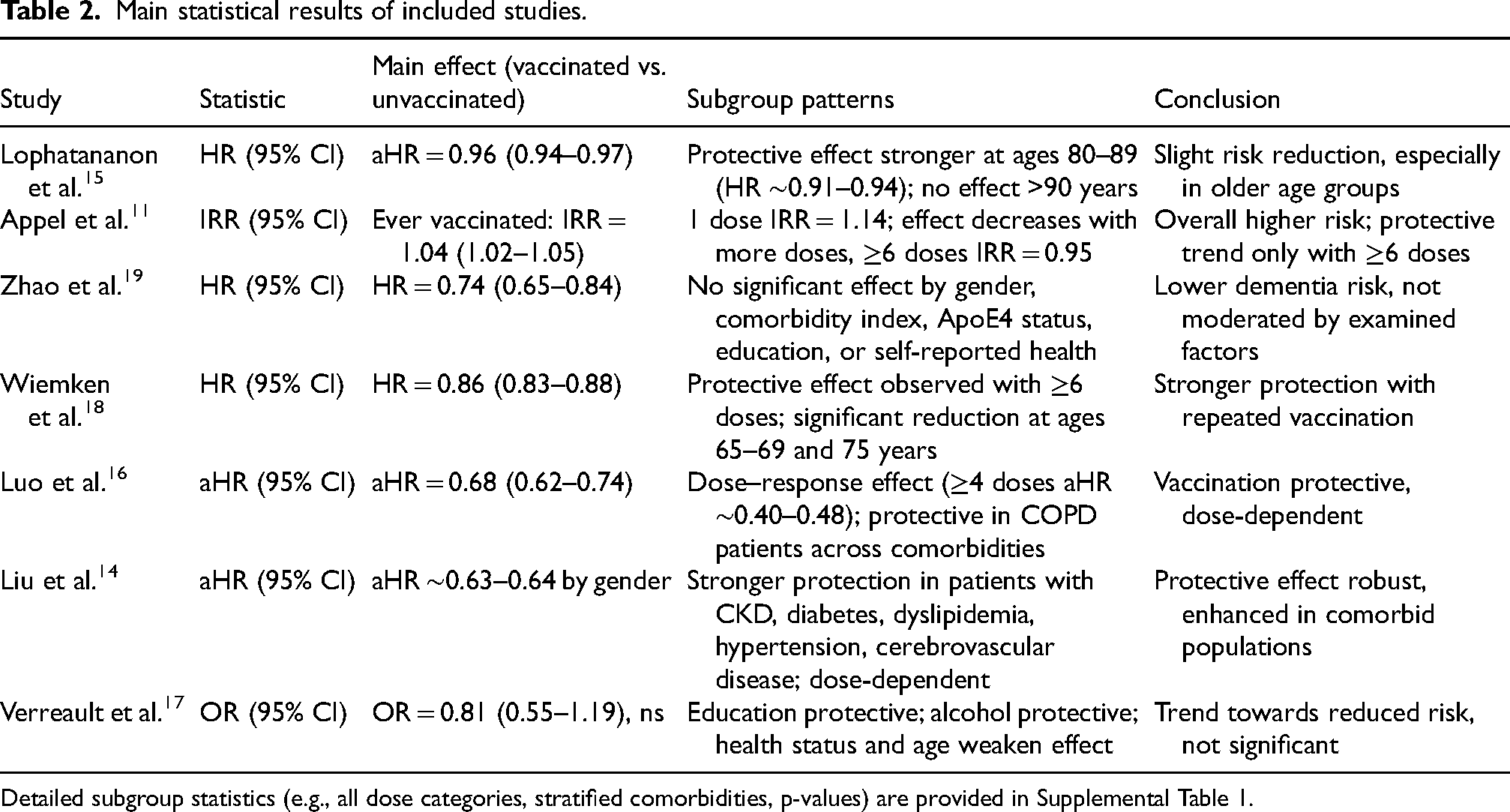
Detailed subgroup statistics (e.g., all dose categories, stratified comorbidities, p-values) are provided in Supplemental Table 1.
Age effects were inconsistent across studies. Liu et al. 14 and Luo et al. 16 both reported that higher age at vaccination was associated with stronger protective effects against dementia, whereas Verreault et al. 17 found the opposite, namely that older age at vaccination was associated with weaker protection. The remaining four studies reported heterogeneous and inconclusive findings.
Several studies also examined the effect of the number of vaccination doses. Three studies suggested a dose–response relationship, whereby greater numbers of influenza vaccinations conferred stronger protection. Wiemken et al. 18 reported that patients with one to five doses had a similar risk of dementia as those unvaccinated, whereas those with six doses exhibited a significantly lower risk (HR = 0.88, 95% CI [0.83, 0.94]). Liu et al. 14 and Luo et al. 16 similarly showed that protection increased with the number of doses (1, 2–3, ≥4). By contrast, Appel et al. 11 reported that a single dose was associated with a 14% increased dementia risk, which gradually decreased with additional doses, reaching a 5% risk reduction at the sixth dose in the fully adjusted model including comorbidities. The other three studies did not report dose-specific outcomes.
The role of comorbidities was also investigated, but results were mixed. Zhao et al. 19 concluded that comorbidities did not significantly influence the relationship between influenza vaccination and dementia risk. Appel et al. 11 reported that vaccinated individuals had a higher dementia risk than unvaccinated individuals regardless of comorbidity status, although adjustment for comorbidities slightly attenuated this effect (IRR = 1.04, 95% CI [1.03, 1.05]) compared to models without comorbidities (IRR = 1.07, 95% CI [1.05, 1.08]). Liu et al. 14 found that patients with diabetes experienced greater protection from influenza vaccination than those without diabetes, while Luo et al. 16 reported no such difference. Similarly, the two studies diverged with respect to dyslipidemia, hypertension, and cerebrovascular disease, with Liu et al. 14 identifying stronger protective effects in affected patients, whereas Luo et al. 16 did not. Both studies agreed that vaccination offered no differential effect for patients with anxiety disorders.
Liu et al. 14 further noted that influenza vaccination remained an independent protective factor against dementia regardless of the use of medications such as statins, metformin, aspirin, or angiotensin-converting enzyme inhibitors, and that protection increased dose-dependently in patients with CKD. Luo et al. 16 reached similar conclusions in patients with COPD, reporting that influenza vaccination remained an independent protective factor even after adjusting for medications including statins, metformin, renin–angiotensin–aldosterone system inhibitors, and aspirin, with protection again depending on dose.
Discussion
This systematic review examined factors that may influence the relationship between influenza vaccination and the risk of developing dementia, specifically gender, age, number of doses, and comorbidities. It is important to note that some factors were reported only in demographic tables of the primary studies and were not included in analytical models, which limited their interpretability and therefore their inclusion in the present synthesis.
One of the key differences across the included studies was sample size. Two studies11,15 analyzed exceptionally large cohorts (n = 7,962,257 and n = 1,673,421, respectively), whereas Verreault et al. 17 relied on a much smaller sample (n = 3865) and used an earlier diagnostic system (DSM-III), raising concerns about comparability. Moreover, vaccination status in Verreault et al. 17 was based on self-report, which may introduce recall bias. Wiemken et al. 18 included a sample composed predominantly of men (96%), limiting generalizability to both sexes. Such methodological heterogeneity likely contributes to the inconsistent findings across gender and age, as well as to differences in effect size estimates.
The two studies focusing on patient groups with chronic diseases, Liu et al. 14 and Luo et al. 16 provide particularly important insights. CKD and COPD are conditions associated with increased dementia risk, in part due to vascular and metabolic comorbidities such as hypertension, diabetes, and hyperlipidemia.21,22 Preventive strategies for these high-risk groups are therefore essential. Evidence from these studies suggests that influenza vaccination may reduce dementia risk among patients with CKD or COPD, highlighting vaccination as a potentially cost-effective and scalable preventive intervention for populations at elevated risk.
The results also support the “infectious hypothesis” of dementia, which posits that infectious diseases may contribute to the pathogenesis of dementia, whereas vaccination reduces neuroinflammatory burden by preventing infections. 23 Three studies in this review found dose–response relationships, with more frequent influenza vaccinations associated with progressively lower dementia risk.14,16,18 This pattern suggests that vaccination may not only prevent infections but could also provide immune training that enhances resilience against neurodegeneration.
Nevertheless, vaccination may also act as a proxy marker of other factors. Prior literature suggests that vaccination is more common among individuals with healthier lifestyles and greater healthcare engagement.17,24,25 Consequently, lower dementia risk observed in vaccinated groups may partly reflect confounding by health behaviors. While several studies adjusted for comorbidities and socioeconomic indicators, residual confounding cannot be excluded. More research integrating detailed lifestyle and behavioral data is needed to clarify whether vaccination itself exerts direct neuroprotective effects or serves as an indicator of broader preventive health engagement.
Overall, this systematic review indicates that number of doses and comorbidity status are the most consistent moderators of the relationship between influenza vaccination and dementia risk. Gender and age effects were inconsistent, and methodological variability across studies limits firm conclusions.
Conclusion and clinical implications
This review suggests that influenza vaccination may contribute to reducing dementia risk, particularly among individuals with chronic diseases and in those who receive multiple vaccinations over time. The findings support the integration of influenza vaccination into preventive strategies for populations at elevated dementia risk. From a clinical perspective, encouraging annual influenza vaccination in older adults, especially those with comorbidities such as diabetes, hypertension, COPD, or CKD, may represent a pragmatic and cost-effective component of dementia prevention programs.
For healthcare providers, these results underline the importance of viewing vaccination not only as infection prevention but also as part of a broader strategy to reduce long-term neurocognitive decline. Public health programs should consider emphasizing repeated vaccination schedules for high-risk populations. At the same time, further high-quality, large-scale prospective studies are needed to disentangle direct biological effects of vaccination from confounding by lifestyle and healthcare access.
By linking preventive neurology with routine vaccination policy, these findings point to a potentially scalable strategy that may mitigate the future burden of dementia, which is projected to rise dramatically in aging populations worldwide.
Supplemental Material
sj-docx-1-alz-10.1177_13872877261420240 - Supplemental material for Factors influencing the relationship between influenza vaccination and the risk of developing dementia: A systematic review
Supplemental material, sj-docx-1-alz-10.1177_13872877261420240 for Factors influencing the relationship between influenza vaccination and the risk of developing dementia: A systematic review by Veronika Ročinová, David Vácha, Martin Anders and Martina Sebalo Vňuková in Journal of Alzheimer's Disease
Footnotes
Acknowledgements
The first two authors gratefully acknowledge the constructive feedback and methodological guidance received from colleagues during the development of this review.
Ethical considerations
Not applicable.
Consent to participate
Not applicable.
Consent for publication
Not applicable
Author contribution(s)
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Cooperatio Program, research area Neuroscience and by the project MH CZ – DRO VFN64165.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
The data that support the findings of this study are available from the corresponding author upon reasonable request.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
