Abstract
Background
Subjective memory complaints (SMC) are linked to an increased risk of neurocognitive disorders (NCD).
Objective
To estimate the prevalence of SMC and their association with sociodemographic and clinical factors in 3285 older adults (OA) from ten Latin American and Caribbean (LAC) countries.
Method
This population-based analysis used secondary data from an international multicenter study on NCD prevalence during the COVID-19 pandemic. Cognitively healthy participants were identified based on clinical criteria, cognitive assessments, and expert consensus. Participants were categorized as with (WSMC; n = 602) or without SMC (NSMC; n = 2683). Sociodemographic and clinical variables were recorded. Cognitive performance was assessed using the Montreal Cognitive Assessment–Short Version (MoCA-T), depressive symptoms with the 15-item Geriatric Depression Scale (GDS-15), and functional decline with the Eight-Item Informant Interview (AD8). Mean difference analyses and logistic regressions were performed.
Results
The regional prevalence of SMC was 18.33%, ranging from 11.59% in Guatemala to 26.30% in Peru. OA with SMC showed lower education, poorer cognitive performance, and higher rates of anxiety, falls, and fractures. Regression models revealed significant associations between SMC and lower education (p < 0.001), emotional distress (p < 0.001), age (p = 0.024), anxiety (p = 0.017), infrequent and occasional falls (p = 0.017; p = 0.002), and fractures (p = 0.028).
Conclusions
SMC are prevalent among LAC older adults and are associated with multiple risk factors, highlighting their public health relevance and potential as early indicators of NCD risk.
Keywords
Introduction
Aging involves physiological and cognitive changes, including subjective memory complaints (SMC). These are defined as the individual perception of difficulties in remembering information or everyday events, in the absence of a clinically proven neurocognitive disorder.1,2 This phenomenon is widely documented in medical literature,3–5 due to its high prevalence, its association with neurocognitive disorders (NCD), and the challenge it poses for healthcare professionals. 5
Unfortunately, knowledge about the prevalence of SMC in Latin American and Caribbean (LAC) countries is limited, with few studies reporting variable local estimates, ranging from 17.6% 6 to 70%, 7 with intermediate ranges between 25% and 50%.8,9 In addition to being a global trend, this variability reflects methodological and contextual differences that make it difficult to accurately characterize the phenomenon in the region.
On the other hand, various factors have been linked to the manifestation of SMC. At the biological level, it has been suggested that these may reflect changes in key brain structures, such as the hippocampus and the prefrontal cortex, as well as alterations in synaptic plasticity and neuronal circuits responsible for memory consolidation.4,10,11 Although not all individuals with SMC develop clinically significant cognitive impairment, 12 some studies suggest that they could represent a preclinical marker of neurodegenerative diseases, such as Alzheimer's disease, due to their association with objective deficits in specific cognitive domains.13,14 Additionally, the presence of chronic diseases, such as diabetes, hypertension, and other metabolic conditions, has been linked to a higher risk of experiencing SMC, suggesting a relevant role of systemic health in the perception of cognitive performance.15,16
Along with biological factors, various clinical and sociodemographic elements have been identified as modulators of the prevalence of SMC. Older age, lower educational attainment, and physical inactivity have been associated with a higher frequency of these complaints.9,17,18 Likewise, the coexistence of neuropsychiatric disorders, such as depression and anxiety, can exacerbate the perception of cognitive failures, even in the absence of objective neurocognitive deficits.19,20 Certain personality traits have been linked to a negative self-assessment of memory performance, increasing the perception of cognitive decline compared to earlier life stages.21–23
Moreover, sociodemographic characteristics such as a lower educational level may reduce cognitive reserve, increasing vulnerability to the onset of SMC and subtle cognitive deficits.24–26 In turn, physical inactivity decreases neuroplastic stimulation and the release of neurotrophic factors such as BDNF and IGF-1, which are essential for synaptic integrity and working memory.27,28 Regular exercise and cognitively stimulating activities not only improve executive function but have also been associated with a lower risk of cognitive decline and SMC, even in populations with a high burden of comorbidities. 29
In this regard, these preexisting conditions, which include sociodemographic, clinical, and personality factors, may interact and reinforce each other, creating a context of high vulnerability that, in the face of a disruptive event such as the COVID-19 pandemic, could intensify the risk of cognitive and emotional impairments.30–32
In this context, the COVID-19 pandemic has represented a critical event with substantial repercussions on the cognitive and emotional health of older adults. 30 During the lockdown, multiple studies reported an increase in the frequency of memory-related symptoms, probably attributable to the reduction of cognitive and social stimulation, disruption of circadian rhythms, and unhealthy lifestyle habits such as physical inactivity and changes in sleep patterns.33–35 Likewise, preventive isolation, implemented to reduce the risk of infection in this age group, exacerbated symptoms of anxiety, depression, and feelings of loneliness. 26 which may have contributed to the increased prevalence of SMC.19,20 Therefore, it has been suggested that this impact may extend over time,36,37 with a possible increase in the incidence of cognitive impairment and dementia in the coming years, especially in low-and middle-income countries,26,38,39 where access to mental health services and psychosocial support is limited.
Considering that socioeconomic, cultural, and ethnic conditions in Latin America and the Caribbean are highly heterogeneous, these factors may differentially modulate cognitive health in the region. 6 In this regard, it is essential to further analyze SMCs and their determinants in aging populations exposed to structural inequalities.
Therefore, this study aims to update the prevalence of SMC in older adults in LAC and analyze its relationship with clinical and sociodemographic factors, with an emphasis on the effects of the COVID-19 lockdown. The findings are expected to provide key evidence on the heterogeneity in the manifestation of SMC, contributing to the development of prevention and intervention strategies aimed at aging populations in vulnerable situations.
Methods
Participants
The data for this study were taken from the project “Prevalence of Cognitive Impairment in Latin America During the COVID-19 Pandemic”.
40
This cross-sectional study was conducted between June 29, 2020, and October 17, 2020
Out of a total of 11,267 evaluations conducted in the multicenter study, rigorous inclusion criteria were applied. First, all subjects had to be assessed using the same cognitive, functional, and affective instruments. Additionally, it was verified that they met the following conditions: age (≥ 60 years), fluency in Spanish, absence of a prior diagnosis or findings during the evaluation compatible with dementia, psychiatric disorders, or other medical conditions that could affect cognition; as well as the absence of severe sensory or perceptual deficits and preserved communication ability.
Subsequently, participants who, at the time of the evaluation, self-reported SMC and those who did not were identified. Finally, clinical meetings were held with work teams from each country and experts in neurocognitive disorders, in which medical history, interviews, and test results were comprehensively reviewed, applying international diagnostic criteria. 41 From this process, the final sample was formed (n = 3285), classified into two groups: with SMC (n = 602) and without SMC (n = 2683).
Instruments
Sociodemographic, clinical, and functional information was collected using a standardized protocol from the original multicenter study, 42 Regarding sociodemographic data, the following were recorded: age (in completed years), sex (male/female), years of formal education, marital status (single, married, cohabiting, separated, widowed), and racial/ethnic self-identification (White, Afro-descendant, Latin American Mestizo, Latin American Indigenous, other).
For cognitive assessment, the abbreviated version of the Montreal Cognitive Assessment (Mini-MoCA or MoCA-T) was used. 43 This test consists of five items that allow for the evaluation of memory, verbal fluency, and orientation via telephone, and has been widely used in the Latin American population.44,45 In Latin America, the MoCA test is the most commonly used brief cognitive assessment tool in clinical settings. 46 We used a cutoff point of 11 points, in accordance with the original proposal by Horton et al. 43 and Liew 47 who demonstrated that this value optimizes the detection of cognitive impairment. Furthermore, this same score has been employed in recent Latin American studies conducted by our research group.40,42
Additionally, the Alzheimer Disease 8-item (AD8) scale was used. 48 It is a brief scale (<3 min) with excellent psychometric properties (α = 0.95), widely used to detect dementia syndrome.49–52 It consists of 8 items administered to a companion, family member, or caregiver of the older adult, assessing changes in memory, judgment, daily functioning, and other cognitive areas. A cutoff score of >2 points was used. 53
Finally, we used the abbreviated version of the Geriatric Depression Scale by Yesavage (GDS-5). 54 This scale consists of five yes/no questions aimed at detecting depressive symptoms. This version has shown acceptable validity indicators for identifying mood disturbances.55,56 A cutoff score of 2 points was used to indicate signs of emotional disturbance.
Regarding clinical conditions, a list of common medical diagnoses was included by asking: “Has a doctor ever diagnosed you with…?” (dichotomous response: yes/no). For those who answered affirmatively, it was recorded whether they were receiving ongoing treatment (OT). The conditions included were: diabetes, hypertension, thyroid disorders, osteoarticular diseases, cerebrovascular diseases, anxiety, and depression.
Participants were also asked: “In the past year, how often have you experienced falls?” and “How often have you had fractures?” with the following response options: never, rarely (1–2 times), occasionally (3–4 times), and frequently (≥5 times). These categories were included as ordinal variables in the analysis, with “never” as the reference.
Finally, SMC were assessed with the question: “Do you believe your memory is worse than it was a few years ago?” The response was dichotomous: YES/NO, following the criteria of the Subjective Cognitive Decline Initiative working group. 57
Data analysis
To describe the characteristics of the sample, relative frequency measures (percentages) were used for categorical variables, and measures of central tendency and dispersion were used for quantitative variables. The comparison between participants with and without SMC was performed using the Mann-Whitney U test for quantitative variables that did not meet the normality assumption of the residuals (Kolmogorov-Smirnov and Shapiro-Wilk), and the Chi-square test for categorical variables.
Two logistic regression models were constructed to identify factors associated with SMC. Model 1 (Table 2) included sociodemographic variables (age, years of education, sex, race/ethnicity, and marital status) and emotional status measured by the GDS-5 Depression Scale, considering the total score as a continuous variable. Model 2 (Table 3) incorporated, in addition to age and years of schooling, clinical and functional variables. Each medical condition (thyroid disorder, arterial hypertension, diabetes mellitus, depression, and anxiety) was coded as a three-level categorical variable: no diagnosis (reference category), diagnosis without treatment, and diagnosis with continuous treatment. The history of falls and fractures was modeled as ordinal variables (never, infrequent, occasional, frequent).
The inclusion of depression as an explanatory variable was ensured through the GDS-5 score in Model 1 and as a clinical history in Model 2, in order to assess its impact from both a symptomatic and diagnostic perspective. This two-stage modeling strategy allowed for first estimating the effect of sociodemographic and emotional factors on SMC, and subsequently examining the additional influence of clinical and functional factors, thereby reducing collinearity issues and optimizing the interpretation of the results.
No sociodemographic comparisons between countries were performed, since this analysis was not part of the study objectives and such characteristics have already been described in previous publications from the same multicenter consortium. Moreover, the main objective was to estimate the prevalence and analyze the factors associated with QSM at the regional level, prioritizing a homogeneous statistical approach that avoided biases arising from differences in sample size and variable distribution across countries.
The models were adjusted for age and years of schooling, and odds ratios (OR) were reported along with their 95% confidence intervals (95% CI) and p-values. For statistically significant results, the corresponding effect sizes were calculated.
Ethical considerations
This secondary data analysis study followed the guidelines of the Declaration of Helsinki. All participants were informed of the study's objective and provided their written informed consent. Additionally, the research was reviewed and approved by the ethics committee of the Universidad de La Costa (Act No. 080), the institution that led the study (INV.140-02-003-15).
Results
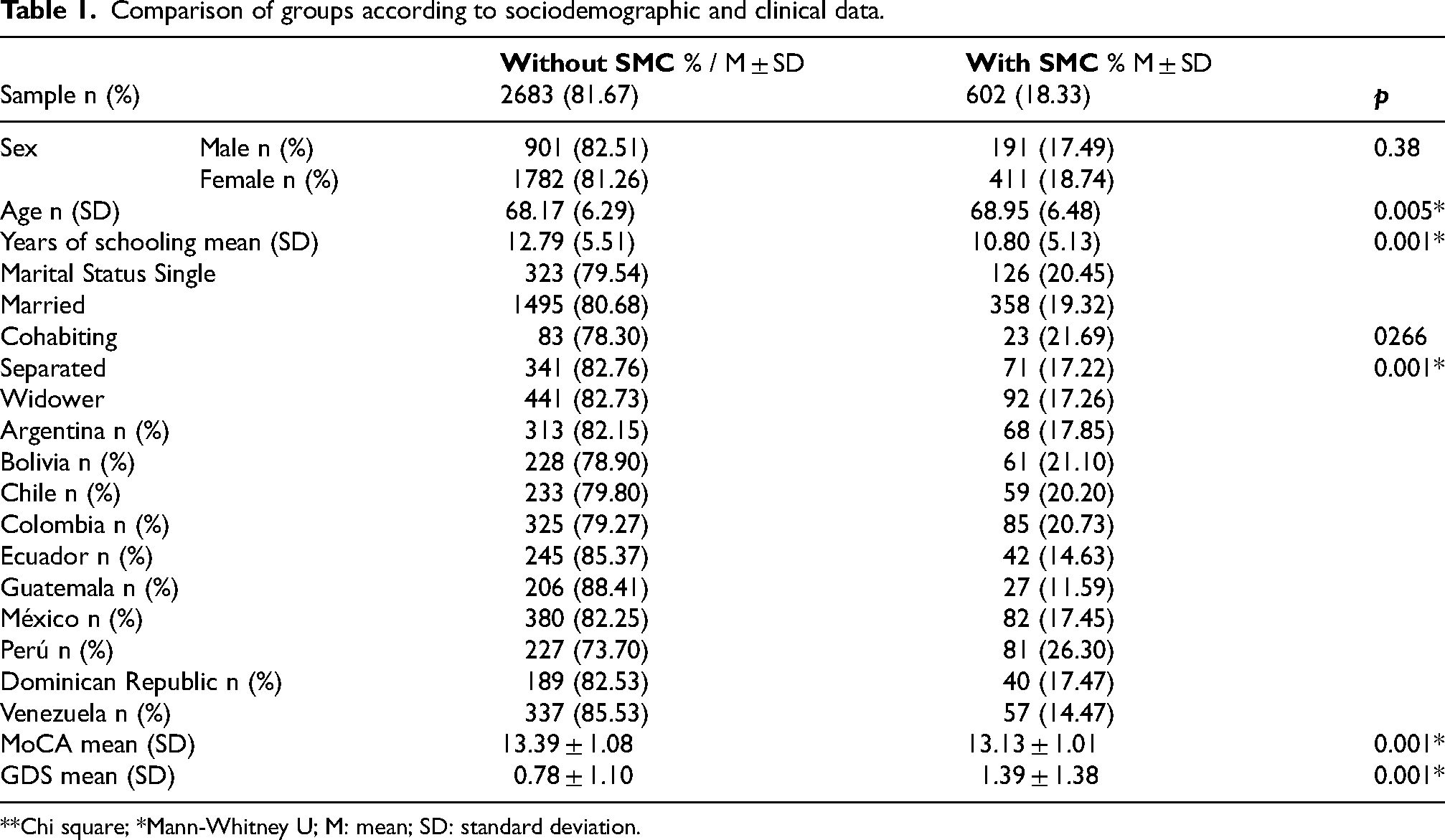
The overall prevalence of SMC was 18.33% (n = 602). No differences were found in the presence of SMC by sex (p = 0.38). However, significant differences were observed in age, with a higher average in the SMC group but a marginal effect size (d = -0.073). Similarly, significant differences were found in years of schooling, with the SMC group having a lower average level of education (see Table 1).
Comparison of groups according to sociodemographic and clinical data.
**Chi square; *Mann-Whitney U; M: mean; SD: standard deviation.
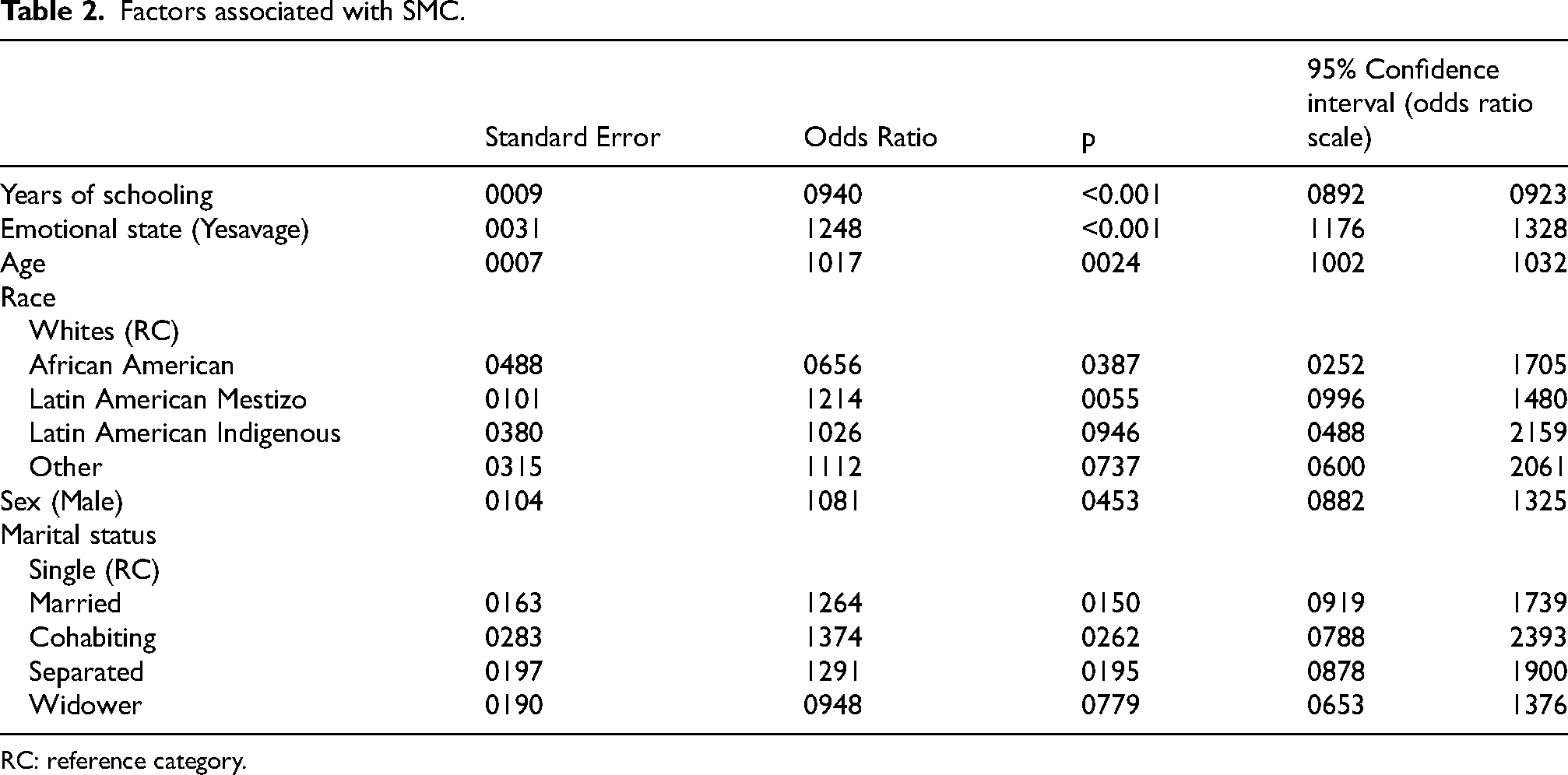
Factors associated with SMC.
RC: reference category.
Clinical history factors associated with SMC.
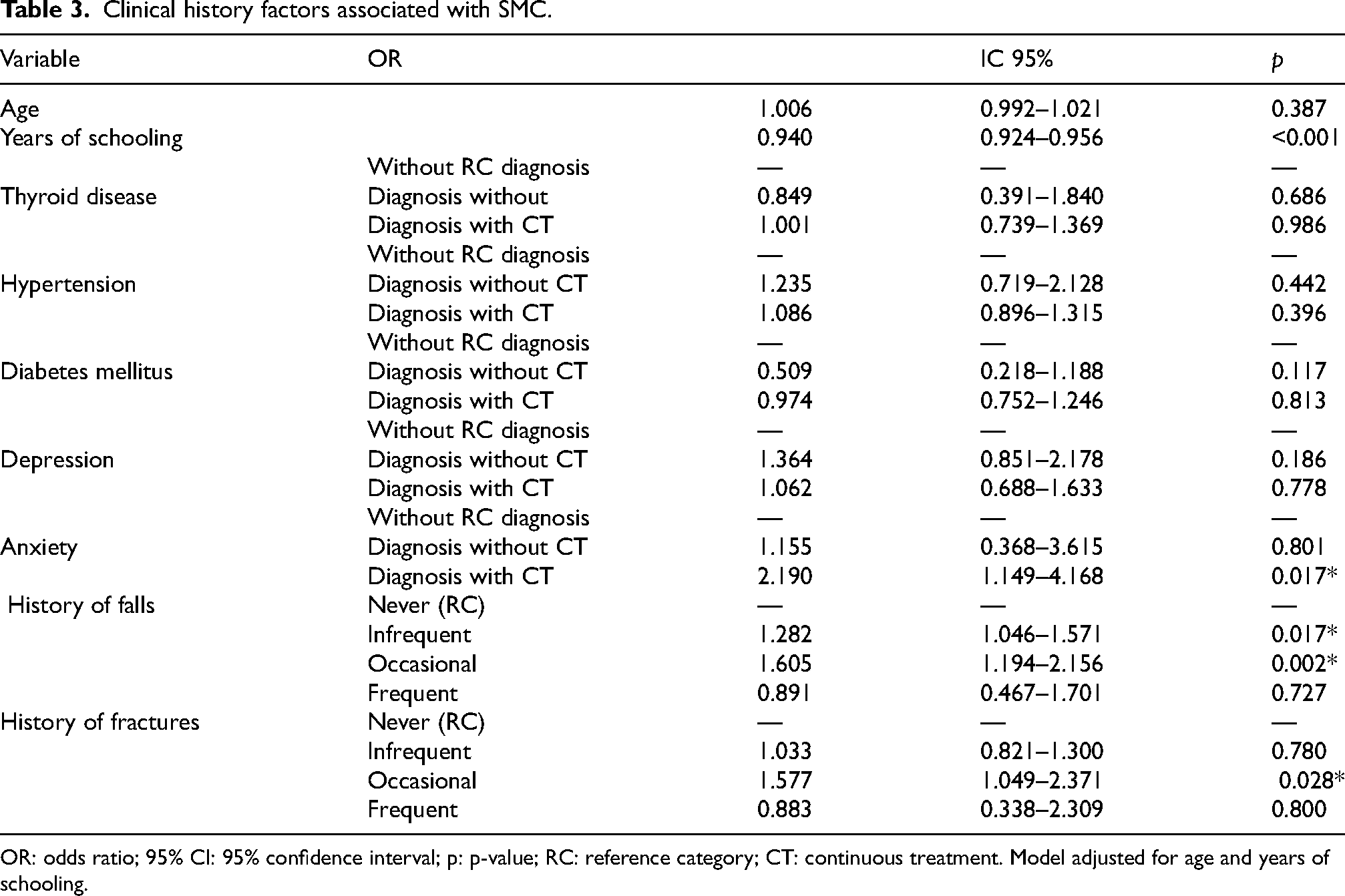
OR: odds ratio; 95% CI: 95% confidence interval; p: p-value; RC: reference category; CT: continuous treatment. Model adjusted for age and years of schooling.
Regarding marital status, no significant associations were identified with the presence of SMC. The prevalence of SMC in the different groups was similar, with a frequency of 20.45% in single individuals, 19.32% in married individuals, 21.69% in cohabiting individuals, 17.22% in separated individuals, and 17.26% in widowed individuals.
Differences were identified by country of residence (χ² = 27.6, p = 0.001), with higher prevalence rates in Peru (26.3%), Bolivia (21.1%), Colombia (20.7%), and Chile (20.2%), and the lowest in Guatemala (11.6%).
Regarding cognitive performance, significant differences were found in the MoCA test scores between the groups with and without SMC (p = 0.001), although with a marginal effect size (d = 0.24). On the other hand, participants with SMC scored significantly higher on the GDS-5 compared to the group without SMC (p < 0.001).
For the factors associated with SMC (see Table 2), binary logistic regression was used. The results indicate that years of schooling (p < 0.001), emotional state (p < 0.001), assessed using the GDS-5 (p < 0.001) and age (p = 0.024) are significantly associated with a higher probability of presenting SMC. In this model, depression was considered as a symptomatic variable through the GDS-5 score, in order to control for the influence of depressive state on the presence of SMC.
Regarding race, a trend was observed toward a higher prevalence of SMC in mestizo participants compared to the reference group, although it did not reach statistical significance (p = 0.055). Likewise, no significant associations were identified for Afro-descendant participants (p = 0.387) or Latin American Indigenous participants (p = 0.0946); however, in the latter group, a high OR was observed, suggesting that contextual factors may modulate this relationship.
On the other hand, marital status did not show a significant relationship with the presence of SMC, as the categories of married, cohabiting, separated, and widowed did not present significant differences compared to the reference group (single) in the adjusted model (p > 0.05). Likewise, male sex was not associated with a higher risk of presenting SMC.
In the second model (see Table 3), when considering clinical conditions as three-level variables (no diagnosis, diagnosis without treatment, and diagnosis with treatment), only anxiety with ongoing treatment was significantly associated with the presence of QSM (OR = 2.19; 95% CI = 1.15–4.17; p = 0.017). In contrast, the other evaluated conditions (thyroid disease, hypertension, diabetes mellitus, and depression), whether in participants with an untreated diagnosis or those receiving treatment, showed no statistically significant associations.
Regarding functional factors, participants with a history of infrequent falls (OR = 1.28; 95% CI = 1.05–1.57; p = 0.017) and occasional falls (OR = 1.61; 95% CI = 1.19–2.16; p = 0.002) had a higher risk of QSM compared to those who never reported falls. Conversely, frequent falls showed no significant association. Similarly, a history of occasional fractures was associated with a higher likelihood of QSM (OR = 1.58; 95% CI = 1.05–2.37; p = 0.028), while infrequent or frequent fractures did not reach statistical significance.
These results remained robust after adjusting for age and years of education, confirming that the main correlates of QSM in this model were anxiety with ongoing treatment and a history of occasional falls and fractures.
Discussion
In this study, the prevalence of SMC among older adults in Latin America and the Caribbean was 18.3%, confirming that this is a highly prevalent phenomenon in the region. When comparing these findings with international evidence, there is notable heterogeneity in the estimates. In Asia, studies report prevalence rates ranging from 7.1% to 64%.25,58–63 In Europe, values vary between 16.4% and 81.3%,31,64–66 while in the United States, figures between 10.8% and 84.2% have been described,67–72 In Latin America, available studies report prevalence rates fluctuating between 17.6% and 70%.6,7 In this regard, the most recent global meta-analysis, 73 which included 39,387 cognitively healthy older adults from 16 countries in Europe, Asia, North America, and Africa, estimated a global prevalence of SMC between 23.8% (95% CI: 23.3–24.4%) and 25.6% (95% CI: 25.1–26.1%). This range places the values observed in our regional cohort below the international average but within the spectrum of global variability.
These discrepancies could be explained by methodological variations, differences in the diagnostic criteria used, and the influence of sociocultural factors on the perception and reporting of cognitive difficulties. In contexts with greater access to information on cognitive health and public awareness programs, older adults tend to show greater awareness of their cognitive performance, increasing the likelihood of self-reporting SMC.74,75 In contrast, in low-income countries with fragile healthcare systems, limited access to care and low health literacy contribute to the perception of cognitive changes as a normal part of aging, leading to an underestimation of SMC prevalence in population-based studies.76,77
In the case of LAC, the limited availability of population-based research restricts a comprehensive characterization of SMC. The available estimates come from heterogeneous sociocultural contexts, making direct comparisons between countries difficult and reducing the external validity of the findings. The most recent and largest study in the region, conducted in Chile, reported a prevalence of 17.6%, 6 a figure that aligns with the one found in our multinational cohort (18.3%). This parallel suggests a certain epidemiological consistency in the region, although significant evidence gaps remain. In this regard, multicenter studies that reflect the socioeconomic and cultural diversity of the region are needed in order to more accurately characterize SMC and its impact on neurocognitive burden and public health in LAC.
When analyzing regional differences, our results revealed statistically significant variations in the prevalence of SMC across countries. Peru reported the highest rate (26.3%), while Guatemala (11.6%) and Venezuela (14.5%) had the lowest. In Peru, the elevated prevalence of SMC (26.3%) may be related to the sustained impact of the COVID-19 pandemic on the mental health of older adults. The strict lockdown measures implemented in the country may have exacerbated social isolation and contributed to the emergence of depressive symptoms-factors closely linked to the presence of SMC.40,78–80 Additionally, Peru shows a high Gini index-a standard measure of income inequality that ranges from 0 (perfect equality) to 1 (maximum inequality)-with a value around 0.44, reflecting deep economic disparities and limited access to healthcare services.71,81 Likewise, insufficient geriatric care coverage and low digital literacy may have hindered early detection of cognitive changes in this population. 61
In contrast, the low SMC rates observed in Guatemala (11.6%) and Venezuela (14.5%) are striking. This phenomenon may be explained by the precarious healthcare systems and the political and economic instability that characterize these countries. 82 In such contexts, the identification of cognitive symptoms is often deprioritized in favor of more immediate needs. In fact, the National Institute on Aging, 83 emphasizes that dementia is not an inevitable consequence of aging; however, this distinction is not always recognized in low-resource communities, which contributes to the underestimation of cognitive decline. Furthermore, chronic economic insecurity may lead older adults to prioritize financial survival over cognitive health care. Along these lines, the Economic Commission for Latin America and the Caribbean 84 warns that recurring economic crises compromise the overall well-being of the older population, with direct repercussions on their brain health and functional capacity.
Beyond these epidemiological variations, it is essential to explore the clinical implications of SMC. In particular, their impact on cognitive performance and emotional state. In our study, participants with SMC showed significantly lower performance on the MoCA test compared to those without SMC (p = 0.001), which is consistent with previous studies. A recent systematic review of 167 studies confirmed that SMC is consistently associated with alterations in episodic memory and executive functions, constituting a risk factor for clinical progression toward neurodegenerative. 85 In fact, longitudinal evidence indicates that older adults with SMC have approximately twice the risk of developing mild cognitive impairment or dementia in the future, compared to their peers without memory complaints. 86 Moreover, a recent analysis reported that SMC precede the conversion to mild cognitive impairment or dementia by 4 to 7 years, doubling the risk of dementia even after adjusting for the APOE ε4 allele and other genetic factors. 87 From an applied perspective, a primary care review highlighted that both SMC and mild cognitive impairment are frequent reasons for consultation and require early interventions with strategies aimed at controlling vascular risk factors to delay progression. Taken together, these findings reinforce a consistent pattern in the literature, in which the presence of SMC is recognized as an early indicator of cognitive vulnerability and a potential preclinical stage of transition toward mild cognitive impairment and dementia.
Complementarily, our results showed that older adults with SMC had significantly higher scores on the Geriatric Depression Scale compared to those without SMC (p < 0.001), indicating that the perception of recurrent forgetfulness is associated with greater emotional distress. Available evidence has shown that symptoms such as anxiety and depression not only increase the perception of cognitive failures but may also amplify somatic symptoms. 88 In this regard, 89 reported that SMC are often accompanied by negative emotions such as anxiety, depression, and frustration, intensifying concern about possible cognitive decline. Consistently, a recent population-based study including more than 270,000 older adults demonstrated that comorbid symptoms such as anxiety and depression increase the risk of presenting SMC by nearly twentyfold, 90 underscoring the critical role of emotional symptoms in this population. Thus, the evidence confirms that SMC encompass both cognitive and emotional dimensions, where memory-related concerns heighten psychological distress and represent a relevant risk factor for future decline.
Finally, in the multivariate analysis (Model 2), after recoding clinical conditions into three levels, only anxiety with continuous treatment was significantly associated with the presence of SMC. In contrast, the other conditions (thyroid disorders, hypertension, diabetes, and depression), both in participants with a diagnosis without treatment and in those under treatment, did not show statistically significant associations. This finding highlights the clinical relevance of anxiety as an independent risk factor, in line with research emphasizing its role in the subjective perception of memory failures.
Regarding the analysis of individual risk and protective factors for SMC, advanced age emerged as a significant predictor, although with a marginal effect size. This finding is consistent with the literature, which recognizes age as a key determinant in the onset of memory complaints; however, its influence may be modulated by other factors such as lifestyle, emotional changes, and the presence of medical comorbidities.91–93
Another relevant finding was the protective role of educational level, supporting the cognitive reserve hypothesis as a compensatory mechanism against cognitive decline.24,94,95 Available evidence indicates that higher educational attainment and quality are associated with better cognitive performance in old age.40,96–99 Moreover, stronger education promotes neural network efficiency and helps compensate for the effects of neurodegenerative events on the brain.100–102 However, recent literature is not conclusive regarding the role of education. Although longitudinal studies have supported its protective effect in delaying the onset of decline and supporting the cognitive reserve hypothesis,103,104 recent large-scale research has questioned its direct influence on the rate of decline. Fjell et al. 105 analyzed more than 170,000 older adults and found no evidence that education modifies the pace of cognitive or brain aging. This suggests that schooling may provide an initial compensatory advantage, higher baseline performance, and a delay in clinical manifestation, but not necessarily sustained protection against cognitive decline.
A significant association was also found between SMC and emotional factors, particularly anxiety and depressive symptoms. The literature indicates that depression impairs executive functioning,106,107 amplifies the perception of cognitive deficits, and increases the risk of progression to dementia.47,108 Additionally, anxiety has been linked to hyperactivation of the salience network, which heightens vigilance over subjective memory changes and exacerbates the perception of cognitive decline.109,110 These findings highlight the need to systematically integrate mental health assessment into SMC screening protocols, considering that early intervention for affective symptoms could improve both cognitive performance and quality of life in older adults.111,112
An additional aspect identified was the relationship between a history of falls and fractures and the presence of SMC. These traumatic events compromise the functional independence of older adults and reduce their participation in cognitive and social activities, thereby initiating a cycle of decline that intensifies the subjective perception of memory failures.113,114 Indeed, recurrent falls have been associated with executive dysfunction and altered brain network connectivity.115–117 This reinforces the close interaction between physical and cognitive factors during aging, with direct implications for daily functioning and future risk of cognitive decline. 118
Conversely, evidence shows that regular physical activity acts as a protective factor. Physical exercise promotes synaptic plasticity and supports neurogenesis, ultimately reducing the risk of age-related cognitive decline.119–121 This beneficial effect of physical activity on brain health is consistent with numerous studies in geriatric populations, which report improvements in cognitive function and lower incidence of cognitive decline among physically active older adults.121–124
In this regard, it is essential to acknowledge the heterogeneity of the social determinants of cognitive health in LAC compared to higher-income regions. In the region, structural inequalities in access to healthcare and education services hinder the timely detection of symptoms and contribute to the normalization of SMC as a natural part of aging.125,126 This phenomenon is reinforced by the urban-rural divide, where the identification of cognitive deficits is often deprioritized in favor of more immediate needs and due to the lack of specialized services. 127 Additionally, low educational attainment and variability in educational quality are associated with higher prevalence of SMC and poorer cognitive performance, modulating older adults’ ability to recognize forgetfulness as pathological.40,42
In this context, several regional studies have shown that structural inequalities and lower educational levels are associated with poorer cognitive performance and neuroanatomical markers of decline in Latino participants 128 ; Functional difficulties and days of poor mental health mediate the association with SMC, with a more pronounced effect among women, low-income individuals, and Latino racial minorities. 129 Consistently, a study in the Chilean population has reported that sex, comorbidities, and self-reported health status increase the risk of SMC. 6 Finally, at a cultural level, stigma and local beliefs reinforce the perception of memory loss as a “normal part of aging,” which contributes to underreporting of symptoms and delays in help-seeking. 130
Despite the relevance of these findings, our study has limitations that should be considered. First, its cross-sectional design prevents the establishment of causal relationships between SMC and associated factors, highlighting the need for longitudinal studies to assess the progression of SMC and its potential development into mild cognitive impairment or dementia. Second, the assessment of SMC through a dichotomous question may have oversimplified a phenomenon with a multidimensional nature. Future research should incorporate standardized instruments that allow for the evaluation of various cognitive and emotional domains, in order to more accurately characterize the clinical profile of older adults. 71 Nevertheless, this study employed a rigorous approach, integrating clinical criteria and expert consensus on neurocognitive disorders, which strengthened the validity of case identification and the composition of the analyzed groups.
Finally, a detailed comparison of sociodemographic characteristics between countries was not conducted. Although these differences could influence the prevalence of SMC, such an analysis was beyond the scope of the present study and has already been addressed in previous publications from the same multicenter consortium.
Considering these limitations, the findings of this study show that 18.33% of older adults in Latin America and the Caribbean report SMC, with significant variations across countries-Peru showing the highest prevalence (26.3%), and Guatemala (11.6%) and Venezuela (14.5%) the lowest. Identified risk factors included advanced age, lower educational level, anxiety and depressive symptoms, as well as a history of falls and fractures. Conversely, higher educational attainment and healthy lifestyle habits such as physical activity emerge in the literature as protective factors against cognitive decline.
Overall, these findings underscore the need for a comprehensive and context-sensitive approach to the assessment of SMC in LAC, one that takes into account structural, emotional, and sociocultural factors. The observed variability in prevalence reflects deep inequalities in access to healthcare, education, and perceptions of aging, highlighting the urgency of implementing tailored strategies for prevention, early detection, and clinical management in vulnerable older populations across the region.
Footnotes
Acknowledgements
The authors have no acknowledgments to report.
ORCID iDs
Ethical considerations
Ethical approval was obtained from the Ethics Committee of la Universidad de La Costa, with approval reference Act No. 080 and research project code: INV.140-02-003-15.
Consent to participate
Informed consent to participate was obtained from all participants included in the study. Consent was provided in written form, following the approval and guidelines established by the Ethics Committee of la Universidad de la Costa.
Consent for publication
Not applicable
Author contribution(s)
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was funded by la Universidad de la Costa under the research project code INV.140-02-003-15.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
The data supporting the findings of this study are not publicly available due to ethical and legal considerations. However, they can be made available by the corresponding author upon reasonable request. Requests for data access will be considered in accordance with the guidelines established by the Ethics Committee of la Universidad de La Costa and applicable regulations on data confidentiality and participant privacy.
