Abstract
Background
Deaf individuals face barriers in accessing healthcare for dementia and Alzheimer's disease and are often overlooked in research. Deaf-friendly scales in German Sign Language (DGS) are urgently needed to ensure inclusive and equitable dementia care for Deaf individuals.
Objective
The aim of the study is the linguistic and cultural adaptation/validation of the Dementia Knowledge Assessment Scale (DKAS-D), the Dementia Attitude Scale (DAS-D), and the Confidence in Dementia Care Scale (CODE-D) into DGS.
Method
The three scales were adapted into DGS using a collaborative translation process involving Deaf and hearing bilingual signers. A convenience sample of 205 Deaf participants answered the DKAS-DGS and DAS-DGS; a subsample answered the CODE-DGS (n = 160) online via Google Forms or as a pencil-and-paper version in person. Psychometric validation included internal consistency, structural and construct validity. For the DKAS-DGS an item analysis was conducted.
Results
Internal consistency was acceptable to good for all scales. The removal of five items from the DKAS-DGS and four from the DAS-DGS led to improvements in structural validity for both. The CODE-DGS one-factor structure showed good model fit. Construct validity was confirmed, with participants with practical or professional experience with people living with dementia scoring higher on all scales. Item analysis of the DKAS-DGS revealed challenges in translation, as well as the need for accessible, tailored dementia education for the Deaf community.
Conclusions
The three scales are valuable tools for measuring dementia knowledge, attitudes, and confidence in care among DGS-signers and may be used in future research settings.
Introduction
Dementia is a public health challenge with major political and social implications. 1 In 2023, around 1.8 million people were living with dementia in Germany. Alzheimer's disease is the most common cause. Over the same year, approximately 445,000 people aged 65 years and older newly developed dementia. It is estimated that by 2060, up to 1.6–3.3 million people in Germany could be affected by dementia.2,3 Since there is no cure yet, key areas of the German National Dementia Strategy focus on prevention, early detection, and supporting people with dementia (PwD) and their family caregivers.2,4 Raising awareness about dementia promotes early diagnosis and prevention, while it helps family carers and the general public become more empathetic toward PwD. This is crucial, especially because 69.3% of PwD in Germany still live at home and are often supported by family members. 5 The National Dementia Strategy, therefore, emphasizes education, training, and awareness programs to improve attitudes toward dementia and enhance healthcare strategies.4,6 Moreover, Article 35 of the Charter of Fundamental Rights of the European Union postulates that “Everyone has the right of access to preventive health care and the right to benefit from medical treatment under the conditions established by national laws and practices”. 7 Thus, ignoring the special needs of underrepresented groups to promote equal access to preventive healthcare constitutes a violation of fundamental rights.
Deaf people who use sign language as their first language are a minority group who are often underrepresented. Conservative estimates suggest that there are approximately 80,000 Deaf people in Germany,8–10 following the general rule of thumb that one in a thousand people is born congenitally deaf. 11 However, other statistics show that this prevalence increases with age: While 1.33 per thousand people are born deaf or hard of hearing, the number rises to 3.5 per thousand in adolescence, suggesting that the number of Deaf individuals is higher than assumed. 12 Their preferred means of communication is German Sign Language (DGS), a fully developed visual language with its own grammar, syntax, and linguistic structure. It is recognized as an official language in Germany since 2002. 9 Deaf individuals do not define themselves by their hearing loss, but rather as members of a linguistic and cultural minority within their countries, with their own set of identity, norms, and values. In Germany, this minority is known as the German Deaf community. Individuals who primarily use DGS and identify as part of the Deaf community are considered to be culturally Deaf. This is internationally represented by writing “Deaf” with a capital D.10,13,14
To this date, dementia research in the context of Deaf individuals remains incredibly scarce. There are no statistics on how many Deaf people live with dementia worldwide or, specifically, in Germany, due to a lack of diagnostic options.15,16 However, it is assumed that dementia affects deaf individuals similarly to how it affects hearing individuals. 17 The impact of dementia on Deaf individuals may be either direct—if they themselves develop dementia—or indirect, for example, when a close friend or relative lives with dementia. Numerous German and international studies have highlighted inequalities in health, healthcare access, and health literacy among Deaf people who use sign language.10,18–22 An Australian study found that only nine out of 72 Deaf participants felt confident in their ability to understand preventive and ongoing health care information in the national language. This was largely due to their limited oral and reading language skills. 23 These challenges in access to health information have been linked to lower levels of health literacy among Deaf individuals. 24 Additionally, these disparities are mirrored by the higher rates of comorbidities among Deaf individuals, such as hypertension, diabetes, obesity, and depression—all of them known risk factors for dementia. 25 These risk factors may contribute to a higher prevalence of dementia among Deaf people than currently recognized. 26
Access to dementia-related healthcare is limited by cultural and communication barriers, including the lack of sign language skills and cultural awareness among healthcare professionals as well as the limited number of facilities tailored to the specific needs of Deaf individuals. Diagnostic challenges lead to further barriers, as standard dementia screening tools are unsuitable for Deaf individuals, which increases the likelihood of misdiagnosis and inadequate care.10,15,18 Moreover, information about dementia is difficult to access, since Deaf individuals rely on vision and sign language as a linguistic and cultural appropriate way to acquire knowledge, while most of the available health information, like print media, is largely inaccessible to them.10,27,28 One reason for this is the generally lower literacy levels among Deaf individuals, but another is that the respective national spoken and written language functions as a second language for them, which is suboptimal, as the acquisition of health-related knowledge requires culturally adapted dissemination in the mother tongue of each minority group. 29 As a result, recent studies from the UK have reported a general lack of dementia awareness among members of the Deaf community.30,31 Similarly, researchers suggest that the members of the German Deaf community also have limited awareness of dementia.15,32,33 Limited dementia awareness can delay the recognition of early symptoms, potentially leading to undetected and untreated cases among Deaf people. It may also give rise to stigma surrounding dementia, hindering the treatment of PwD in a sensitive and empathetic way. Furthermore, many Deaf PwD and their family members remain unaware of the few available diagnostic options and support services that are specialized for Deaf individuals.15,17,30 Studies suggest that there is a significant number of undetected cases of dementia among Deaf people in Germany who, therefore, remain untreated.15,27 These systemic shortcomings and communication barriers contribute to a deep-rooted mistrust and disappointment among Deaf individuals toward the healthcare system, therefore avoiding help-seeking. 30 Raising awareness about dementia within the Deaf community is a crucial first step toward improving access to timely diagnosis, appropriate care, and, ultimately, health equity. 34 Only then can Deaf individuals attain their full potential for health and access to preventive healthcare, as Article 35 of the Charter of Fundamental Rights of the European Union is postulating. 7
Measuring knowledge and attitudes toward dementia with psychometric instruments, such as questionnaires, aids in evaluating the needs of PwD and their caregivers in order to build evidence-based interventions and shape healthcare structures to better meet their actual needs.4,35 In order to ensure that all population groups, including marginalized cultural minorities such as the Deaf community, are represented in this process, culturally appropriate instruments are necessary. Unfortunately, there is still a lack of data on dementia-related knowledge and attitudes within the Deaf community. Standardized auditory-written questionnaires are unsuitable for Deaf signers, whose primary language is the national sign language of their country, as they fail to account for their linguistic and cultural needs. These instruments are developed, validated, and normed for hearing individuals, often assuming a literacy level and cultural background that excludes Deaf individuals.36,37 The absence of validated instruments in sign language compromises not only the appropriateness and reliability of assessments, but also limits Deaf people's participation in health research.37–39 In light of the Convention on the Rights of Persons with Disabilities and the principle of “Nothing about us without us”, 40 the ongoing exclusion of Deaf individuals from accessible and inclusive research represents a violation of human rights. Without linguistically and culturally adapted tools in sign language, Deaf individuals remain underrepresented in dementia research and are bereft of equal access to care. 41
In recent years, a number of health-related scales have been translated, adapted, and validated for Deaf sign language users in various national sign languages, including American Sign Language (e.g., the Multidimensional Health Locus of Control Scales 39 ), British Sign Language (e.g., the Short Warwick-Edinburgh Mental Well-Being Scale 42 ) and Brazilian Sign Language (e.g., the World Health Organization Quality of Life scale (WHOQOL) 43 ). Such adaptations have also been made in countries such as Austria, Norway, Turkey, India, and Australia, among others (e.g.,36,44–49). These involve instruments used in the fields of mental health and health literacy. Two systematic reviews examined publications that translated, adapted, and validated scales, tools, and questionnaires, identifying key challenges and effective strategies.41,50 Additionally, a theory/review manuscript has been published, which discusses the evolution of research methods related to sign language questionnaire design. 37 Furthermore, several key publications on sign language research compile ethical considerations and provide guidelines for the appropriate adaptation of research tools, aiming to ensure Deaf-friendly and inclusive methodological approaches.37,51–55 Key principles in such publications involve the Deaf communities as co-creators in the research process by building inclusive research teams and attention to linguistic and cultural adaptation. This involves tailoring and formatting the tools in ways that align with the cultural and linguistic preferences of Deaf individuals, such as using visual, sign-based materials, video technology, and online survey platforms to enhance accessibility.
Despite these advances, no dementia-related questionnaire has yet been adapted or validated in any sign language. In Germany, a program to raise awareness about dementia among Deaf people is currently being developed as part of the Erasmus+ project “DeSign”. 56 In order to evaluate this program, validated psychometric instruments in DGS are essential to ensure accurate and valid data collection from the German signing population and to reliably measure whether the program is achieving its intended outcomes or to identify areas for improvement. Furthermore, the use of standardized and validated tools ensures that findings are robust, comparable, and suitable for informing future interventions within the Deaf community.
To date, several scales have been developed to measure knowledge, attitudes, and confidence in dementia care, including the Dementia Attitude Scale (DAS; O’Connor & McFadden, 2010 57 ), the Confidence in Dementia Scale (CODE; Elvish et al., 2014 58 ), the Dementia Knowledge Assessment Tool 2 (DKAT2; Toye et al., 2014 59 ), the Knowledge in Dementia Scale (KIDE; Elvish et al., 2014 58 ), and the Dementia Knowledge Assessment Scale (DKAS; Annear et al., 2017 60 ). In the past three years, these tools have all been translated and validated for the German general population in auditory-spoken German.35,61 While the KIDE, the DKAS, and the DKAT2 measure knowledge about dementia, the German version of the DKAS (DKAS-D) demonstrated the best psychometric properties and was therefore selected for this study. The purpose of this study is to translate and validate the questionnaires about dementia knowledge (DKAS-D), confidence in dementia care (CODE-D), and attitudes toward dementia (DAS-D) into DGS, taking into account linguistic and cultural adaptation.
Methods
Design
A cross-sectional study was conducted to translate and culturally adapt three dementia-related scales into German Sign Language (DGS): the DKAS-DGS, DAS-DGS, and CODE-DGS. The present study follows the EQUATOR guidelines for the presentation of scientific papers using the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) checklist (Supplemental Material 1).
Participants
Participants were recruited from January 2024 to April 2025. Inclusion criteria required participants to have reached the age of consent (18+ years) and to be self-reported culturally Deaf and DGS users. To reach a broad spectrum of participants, several recruitment methods were employed. Initially, the research team reached out to key individuals in the Deaf community as well as strategically relevant Deaf organizations, such as the “Landesverbände der Gehörlosen” (state associations of the Deaf), who distributed the study flyer containing a QR code and survey link via their mailing lists. Additionally, community members shared the survey link informally through their personal and social networks. Participants attending the dementia awareness courses of the “DeSign” project were also invited to complete the survey prior to the start of the course. This resulted in a convenience sample complemented by purposive and snowball sampling strategies to enhance representativeness within the community.
Data collection and procedure
The data were collected using Google Forms, where participants were required to complete all three scales consecutively. A one-clip video sign language questionnaire format was employed, featuring signed video clips displayed above the questions, with the answer options provided underneath in written language, thus allowing the participants to interact with both modalities. 37 Upon accessing the survey link, respondents were first presented with a series of sign language videos, in which a Deaf member of the research team provided detailed information about the study's purpose, data protection, the confidentiality of responses, and participants’ rights. Each video was accompanied by a written summary in easy-to-understand German. Participants viewed each item in DGS and then indicated their response by selecting one of the brief written multiple-choice options (e.g., “probably true,” “I don’t know,” etc.); they were not required to answer in writing or in sign language. To make response selection more accessible, the DAS-DGS also included visual cues (emojis) alongside the response options. Contact details for both Deaf and hearing researchers were provided for any questions or concerns. After giving informed consent, participants answered questions about sociodemographic characteristics, preferred language, and when they first learned DGS. They were also asked about their previous experience with dementia, whether they knew someone with dementia, cared for, or worked with a person with dementia, and whether they had received any dementia-related training. A subset of 54 participants completed the survey before attending two dementia awareness courses in Rastatt and Schwäbisch Gmünd either online or using a paper-and-pencil version, while the signed videos were shown on a projector before the awareness program began.
Instruments
DKAS-DGS
The 25-item scale DKAS60,62 measures a person's knowledge about dementia in four subscales: “Causes and Characteristics” (items 1–7), “Communication and Behaviours” (items 8–13), “Care Considerations” (items 14–19), and “Risks and Health Promotion” (items 20–25). Subjects respond with the following possible responses: “true”, “probably true”, “probably false” and “false”, while a fifth option “I don't know” can be selected in case of uncertainty. Two points are assigned when a statement is factually correct and the response “true” is selected. If the response is “probably true”, one point is assigned. All other response options result in zero points for the respective item. Conversely, for false statements, the response “false” achieves two points, “probably false” results in one point, while any other response leads to zero points (items 1–6, 8–10, 13, 14, 21, 23, 25). The total score, therefore, ranges from 0 to 50 points. The DKAS has been shown to be a reliable and valid way to measure knowledge about dementia, with a Cronbach's alpha (α) of 0.85. 60 The German version DKAS-D had very good internal consistency (α = 0.873) and great test-retest reliability. 61 A confirmatory factor analysis (CFA) approved the initial factor structure 60 with the removal of 5 items (4, 6, 18, 19, and 25).
DAS-DGS
The DAS 57 is a psychometric instrument developed to measure attitudes toward dementia. The DAS consists of 20 items that capture cognitive (e.g., “I am not very familiar with dementias”), behavioral (e.g., “I would avoid interacting with a person who is agitated due to dementia”), and affective (e.g., “I feel relaxed around people with dementia”) dimensions of attitudes toward dementia as outlined by the tripartite model of attitude. Respondents indicate their agreement with each item using a 7-point Likert scale ranging from 1 (strongly disagree) to 7 (strongly agree), resulting in a total score ranging from 20 to 140. Higher scores reflect more positive attitudes toward people with dementia. Negatively worded items are reverse-coded (items 2, 6, 8, 9, 16, and 17). The DAS has a two-factor structure reflecting “Social Comfort” (items 1, 2, 4–6, 8, 9, 13, 16, 17) and “Dementia Knowledge” (items 3, 7, 10–12, 14, 15, 18–20). Additionally, the DAS demonstrated strong internal consistency, with Cronbach's alpha of 0.85. The DAS has proven effective in differentiating between individuals based on their level of experience with PwD. 57 The German adaptation DAS-D is considered a reliable and valid tool for measuring attitudes toward dementia in the German-speaking general population. 35 It had a very high internal consistency (α = 0.90), an excellent test-retest reliability of 0.940 (confidence interval of 0.910–0.960), while a Principal Component Analysis (PCA) confirmed the two-factor structure proposed in the original publication. The analyses to determine construct validity showed that the German version could distinguish between individuals with or without experience with people with dementia and between those who had participated in a dementia course versus those who had not.
CODE-DGS
The CODE is a nine-item questionnaire to measure confidence in caring for people with dementia. 58 Responses are scored on a five-point Likert scale, ranging from “not confident” to “very confident”. The total score can range from 9 to 45. Higher scores indicate greater confidence in caring for PwD with the cut-offs being 0–18 points “not confident”, 19–35 “somewhat confident”, 36–45 “very confident”. The CODE is linked to the program “Getting to Know Me”, which is designed to increase staff skills, knowledge, and confidence in caring for PwD, and was validated with 115 healthcare professionals during the validation process, resulting in a Cronbach's alpha of 0.91. The German version of the CODE-D was validated with 263 participants from the general population, demonstrating high internal consistency (α = 0.93) and a strong test-retest reliability (ICC = 0.897). 35
Translation/adaptation process
Although the original versions of the three scales were developed in English, we used their already translated and validated written German versions as the basis for our study.35,61 These include the DAS-D, 57 the CODE-D, 58 and the DKAS-D. 60 The translation and adaptation process was carried out by a three-person team, consisting of two Deaf native DGS signers and one hearing bilingual DGS signer who is also a certified sign language interpreter. Forward translation was performed independently by one Deaf native signer and a hearing interpreter, who both had professional experience in sign language translation. In the second phase, these two interpreters met to compare their versions and collaboratively addressed any discrepancies, as well as linguistic, cultural, and procedural challenges encountered during the process. 41 This discussion led to a consensus on an initial synthesis of the translations. In the peer review phase, the third party, the Deaf research team member who had been specifically trained, up-skilled and informed about the three dementia tools, carefully reviewed the first draft of the linguistic and cultural adaptation. The Deaf consultant provided critical feedback, which was communicated back to the forward translators. The three members engaged in an iterative revision process, discussing and connecting via multiple video calls to navigate linguistic difficulties and cultural discrepancies and continually refined the translation, ultimately reaching an agreed-upon final version. The final signed versions of the questionnaire items were video-recorded. The Deaf signer enrolled in the forward translation served as the signing model for the questionnaire items. At the same time, the Deaf research team member appeared in explanatory videos providing information on study procedures, informed consent, and participant anonymity. In the final phase, the adapted scales were pilot-tested with five Deaf individuals, including dementia professionals and family caregivers. Participants completed the questionnaires and provided feedback on the clarity, cultural fit, and usability of the signed versions. The full signed survey, with original scale formats and DGS videos, is available in Supplemental Material 2 or at: https://forms.gle/syPALb3ykCxJ1XX69.
Statistical analysis
We examined the following psychometric properties for the DKAS-DGS, the DAS-DGS, and the CODE-DGS: reliability (internal consistency), structural validity through CFA, and construct validity (known-groups method). The scales were examined for floor and ceiling effects. An item analysis was conducted for the DKAS-DGS.
Data preparation and preliminary data checks
We conducted the descriptive and inferential statistical analysis utilizing IBM Statistical Package for Social Sciences (SPSS) Version 29.0.1.1. CFA analyses were carried out via AMOS version 29. During data preparation, the dataset was reviewed for completeness and duplicate entries. There was no missing data. Two participants who self-identified as hearing and indicated spoken German as their preferred language were excluded based on the study's inclusion criteria. Descriptive statistics were used to summarize the sociodemographic, cultural, and linguistic characteristics of the sample. Spearman's rank correlation was used for exploratory analysis to identify potential confounding variables in the context of the known-groups method for construct validity (Spearman's Rho (ρ)). Variables significantly associated with the questionnaire's scores, but not central to the hypotheses, were included as covariates in the main analyses. All scales were scored in line with their original versions and prior validation studies.57,58,60 Given the sensitivity of formal normality tests such as Shapiro–Wilk to larger sample sizes, we complemented these tests with skewness and kurtosis values (±2 threshold) and visual inspection of histograms and Q-Q plots to assess data normality.63–65
Floor and ceiling effects
Floor and ceiling effects were inspected additionally, which are defined as present when more than 10% of participants achieve the lowest or highest possible score of the scales. An existing floor or ceiling effect could be an indicator of limited content validity of the scale or a signal that the scale may not be suitable for detecting change over time. 66 This is particularly important, given that the DKAS-DGS and DAS-DGS are intended to be used for evaluating a specialized dementia awareness course for Deaf individuals in DGS.
Internal consistency
We assessed the internal consistency of the scales utilizing Cronbach's alpha, with α ranging from 0 to 1. McDonald's omega was calculated additionally, as it accounts for varying unstandardized factor loadings and error variances, which can provide a potentially more robust measure of internal consistency.67,68 Values between 0.70 and 0.95 indicate good internal consistency, while values exceeding 0.95 may suggest item redundancy due to overlapping content. 66
Structural validity
CFAs with maximum likelihood estimation (ML) were performed for all three scales to inspect structural validity. It was hypothesized that the factor structures initially proposed in the original publication studies were retained in the DGS versions. The model fit was examined using the comparative fit index (CFI), the Tucker-Levis index (TLI), the root mean square error of approximation (RMSEA), and the standardized root mean square residual (SRMR). A model fit is deemed acceptable at CFI and TLI ≥ 0.90, RMSEA < 0.08 and SRMR < 0.11 and good at CFI and TLI ≥ 0.95, RMSEA < 0.05, and SRMR < 0.08.69–71
Construct validity
Construct validity was assessed by the known-groups method testing the following predefined hypotheses: The aim was to test whether the DKAS-DGS, DAS-DGS, and CODE-DGS could discriminate between participants with and without practical or professional experience of PwD. More explicitly, we hypothesized that participants with dementia experience would score significantly higher on all scales. These hypotheses were tested using independent sample T-tests; if potential confounding variables were identified, they were controlled for by including them as covariates in the model. In that case, analysis of covariance (ANCOVA) was conducted to test hypotheses. Participants were classified as having practical experience with dementia if they indicated in the questionnaire that they either care for or work with a PwD.
Item analysis
We examined item difficulty (percentages of correct answers) and ignorance (proportion of “I don’t know” responses) across the entire DKAS-DGS scale. Afterward, we compared these indicators between individuals with and without prior practical or professional experience with PwD. Like in Melchior and Teichmann, 61 the difficulty index was further classified into six levels: very “difficult” (<10%), “difficult” (10.1%–25%), “somewhat difficult” (25.1–50%), “somewhat easy” (50.1%–75%), “easy” (75.1%–90%), and “very easy” (> 90%). Item-total and inter-item correlations were utilized to assess internal consistency, with values between 0.2 and 0.4 considered indicators of good internal consistency. 72
Sample size and power analysis
Sample size was determined a priori based on the statistical procedures required for the validation study. For the known-groups method, the required sample sizes were estimated with G*Power 3.1. 73 The required sample size for independent samples T-tests was 198 participants for a medium effect size (d = 0.5), power 1–β = 0.95, and α = 0.05. An allocation ratio of 2:1 was selected due to an expected imbalance in group sizes. In case covariates were controlled, ANCOVA indicated a required sample size of 100 (f = 0.40, α = 0.05, numerator df = 2, two groups, two covariates). For the CFA, recommendations from psychometric literature suggest that samples over 200 are generally considered adequate for models of moderate complexity.74,75 Additionally, Kyriazos 76 emphasizes that samples between 150 and 300 are considered acceptable when models have reliable indicators, strong factor loadings, and low to moderate complexity. The final sample size of N = 205 for the DKAS-DGS and DAS-DGS therefore exceeds these thresholds. The CODE-DGS was completed by a subsample of n = 160. This smaller number reflects the study design: whereas all participants completed the DKAS-DGS and DAS-DGS (used to evaluate dementia awareness courses), the CODE-DGS, which measures confidence in dementia care, was not administered in the course settings due to time constraints and limited relevance for course evaluation. Participants who accessed the survey link through recruitment, however, completed all three scales. Still, the CODE-DGS subsample (n = 160) falls within the required sample size range for conducting the T-test and is considered adequate for CFA given the lower complexity of the model with only nine items. 76
Ethics
Ethical approval for the study was granted by the Ethics Committee of the Faculty of Behavioral and Empirical Cultural Sciences at Heidelberg University, Germany (AZ Teich 2023 2/1). This study was conducted in accordance with the ethical principles outlined in the Declaration of Helsinki. All participants were fully informed about the purpose and procedures of the study and gave their written consent prior to participation. Data confidentiality and participant anonymity were ensured in compliance with the General Data Protection Regulation (GDPR) applicable to research contexts. 77
Results
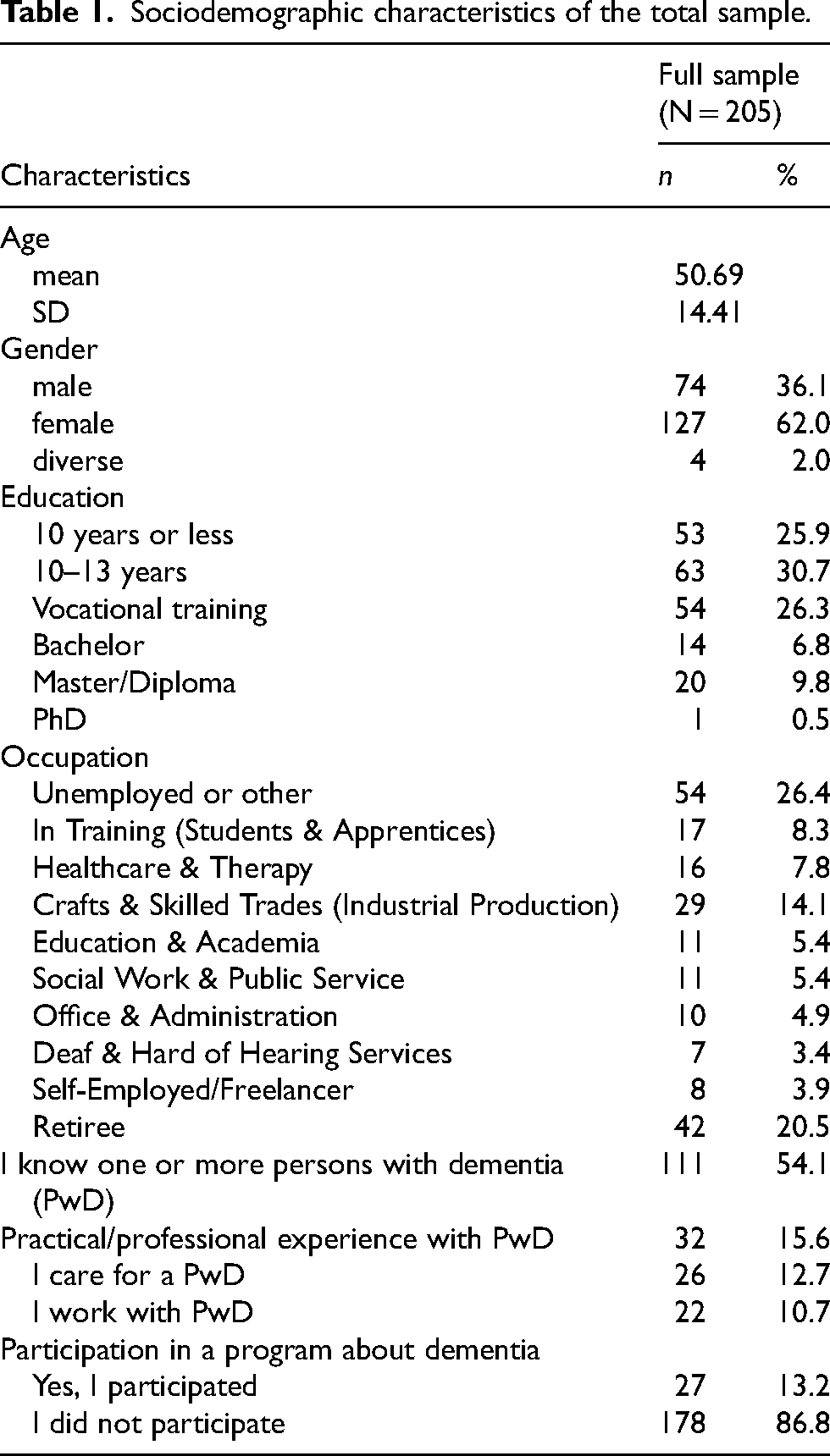
The basic sociodemographic data of the sample are depicted in Table 1. The final sample included 205 Deaf individuals, aged from 18 to 92 years, with a mean age of 50.69, out of whom 127 (62%) were female. Nearly one-third of the respondents had completed 10 to 13 years of schooling (30.7%), equivalent to a secondary school or advanced secondary qualification, while only 17.1% held higher education degrees, including a bachelor's degree or a master's diploma. More than half of the sample knew one or more PwD (54.1%), while 15.6% had practical or professional experience by either caring for or working with PwD. Only 13.2% had participated in a course or training about dementia.
Sociodemographic characteristics of the total sample.
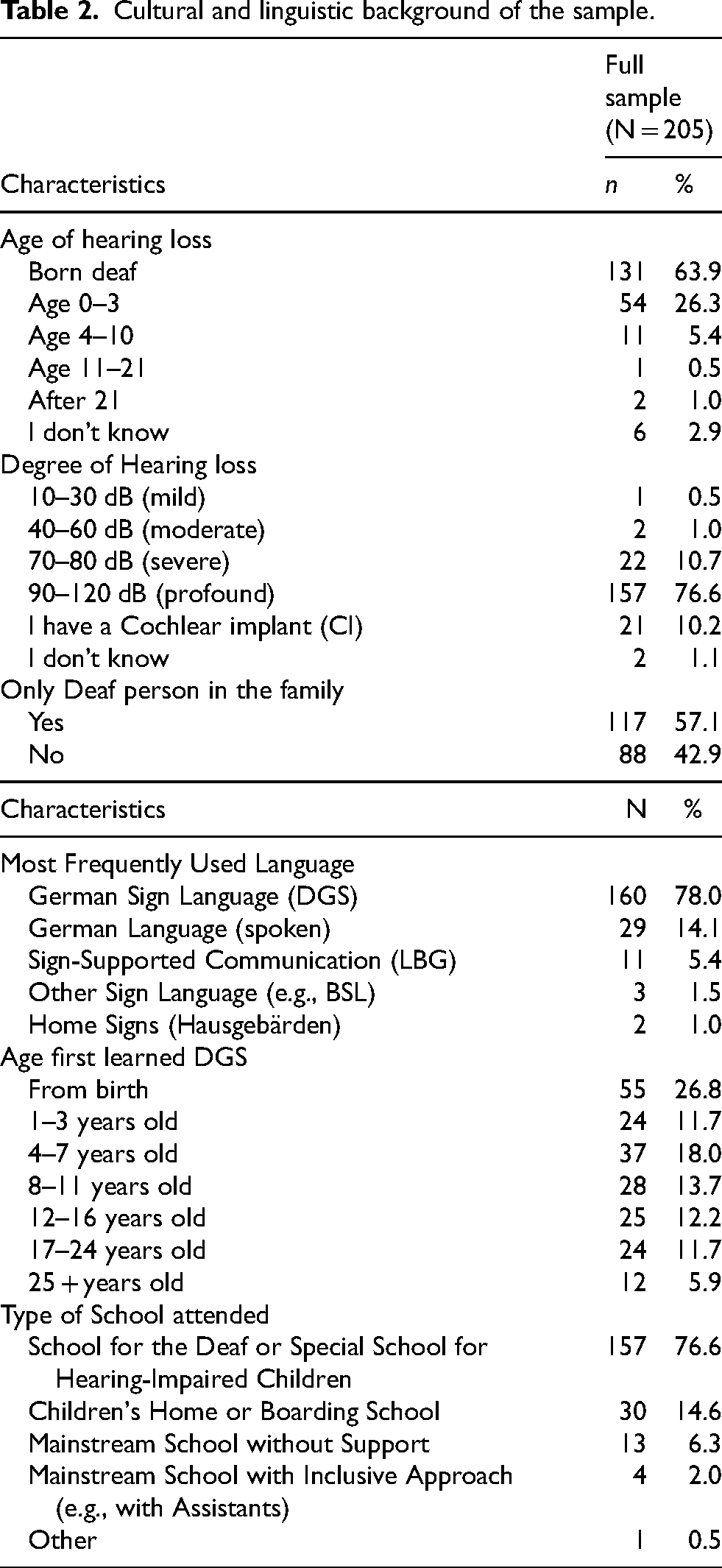
Population-specific and linguistic characteristics (e.g., preferred language use) are represented in Table 2. Most of the participants reported being congenitally Deaf (63.9%), followed by early childhood (21.3%), and 57.1% reported being the only Deaf person in their family. More than three-quarters of the participants described their degree of hearing loss as profound (90–120 dB), followed by severe (70–80 dB), while 10.2% reported having a cochlear implant. The most frequently used language was DGS (78.0%). Most participants attended a school for the Deaf or a special school for hearing-impaired children (76.6%), while 14.6% went to a children's home or boarding school. Spearman correlation analyses were conducted to explore associations between demographic variables and outcome measures. Higher age was significantly associated with later acquisition of DGS (ρ = 0.228, p < 0.001), a lower likelihood of using DGS as the main language of communication (ρ = −0.178, p = 0.010), and an overall lower education level (ρ = 0.311, p < 0.001). Higher age was also associated with less frequent attendance of school types providing signing environments (F(2053) = 16.398, p < 0.001, η2 = 0.206). Respondents from children's homes or boarding schools were the oldest (M = 65.17), followed by those from Deaf-specific schools (M = 48.58), and those from inclusive mainstream schools were the youngest (M = 30.00).
Cultural and linguistic background of the sample.
DKAS-DGS
The DKAS-DGS had a mean score of 19.26 (SD = 8.93) on a scale from 0 to 50 points. Participants scored on a range of 0 to 45 points, with a large portion scoring in the lower middle, between 18 and 24 points (37.6%). The distribution of the scoring was symmetric with a small left tail in the histogram. Visual and statistical inspection of descriptive statistics revealed the mean score to be approximately normally distributed (skewness 0.01 and kurtosis 0.04), which was supported by the Shapiro–Wilk test (W(205) = 0.989, p = 0.102).
Internal consistency
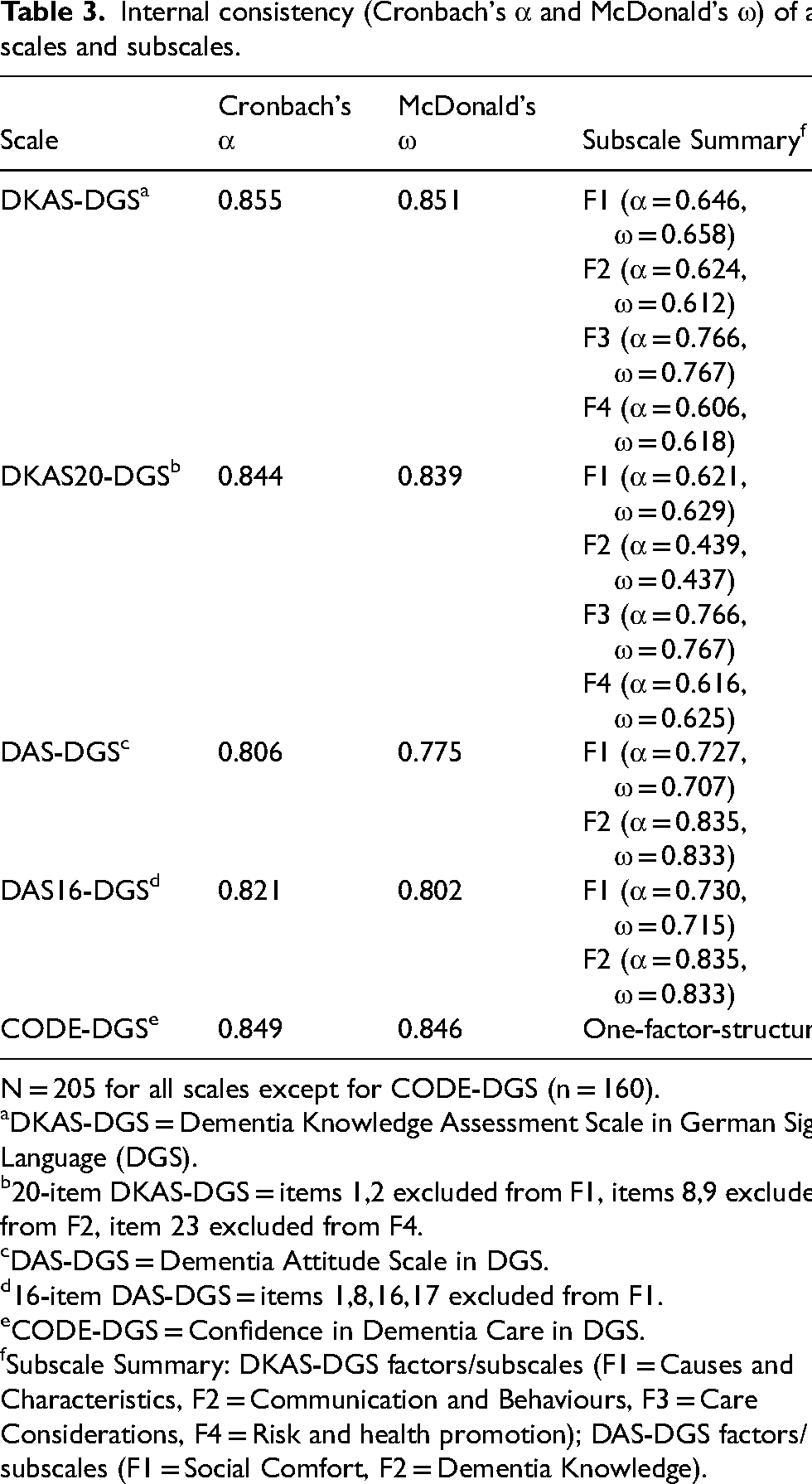
The internal consistency of all scales and subscales is presented in Table 3. For the 25-item DKAS-DGS, internal consistency was good, with a Cronbach's alpha of 0.86 and a McDonald's omega of 0.85, both well within the recommended threshold of (0.70–0.95).63,66 No items would improve these indicators if deleted.
Internal consistency (Cronbach's α and McDonald's ω) of all scales and subscales.

N = 205 for all scales except for CODE-DGS (n = 160).
DKAS-DGS = Dementia Knowledge Assessment Scale in German Sign Language (DGS).
20-item DKAS-DGS = items 1,2 excluded from F1, items 8,9 excluded from F2, item 23 excluded from F4.
DAS-DGS = Dementia Attitude Scale in DGS.
16-item DAS-DGS = items 1,8,16,17 excluded from F1.
CODE-DGS = Confidence in Dementia Care in DGS.
Subscale Summary: DKAS-DGS factors/subscales (F1 = Causes and Characteristics, F2 = Communication and Behaviours, F3 = Care Considerations, F4 = Risk and health promotion); DAS-DGS factors/subscales (F1 = Social Comfort, F2 = Dementia Knowledge).
Structural validity
CFA results of the DKAS-DGS are presented in Figure 1. We included all 25 items in the initial CFA to test the appropriateness of the original four-factor structure. The first results of the CFA provided an overall insufficient model fit with some acceptable properties (χ²(269, N = 205) = 460.15, p < 0.001, CFI = 0.799, TLI = 0.776, RMSEA = 0.059 (90% CI [0.050, 0.068]), SRMR = 0.0748). To improve model fit, items with low factor loadings (< 0.4), low standardized regression weights (< 0.4), low squared multiple correlations (< 0.2), and overall high standardized residual covariances (> 2 with many items) were deleted. 78 Items 8 and 9 of the factor “Communication and Behaviours” had substantially low and insignificant factor loadings and were excluded from the model immediately (λ = -0.02 and 0.06; p = 0.736 and 0.396, respectively). In the next step, items 23, 2, and 1 were excluded because they showed the lowest standardized regression weights (< 0.2) and squared multiple correlations (< 0.1). Modification indices >15 were added to the model as correlated error terms on items 15 and 16 of the third factor. The final model fit was: χ²(163, N = 205) = 278.93, p < 0.001, CFI = 0.86, TLI = 0.841, RMSEA = 0.059 with 90% CI [0.047, 0.071] and SRMR = 0.0682. Four additional items had loadings below 0.40 and could be considered for removal (items 4, 11, 13, 21). However, they were kept due to theoretical considerations and their conceptual relevance for future research.
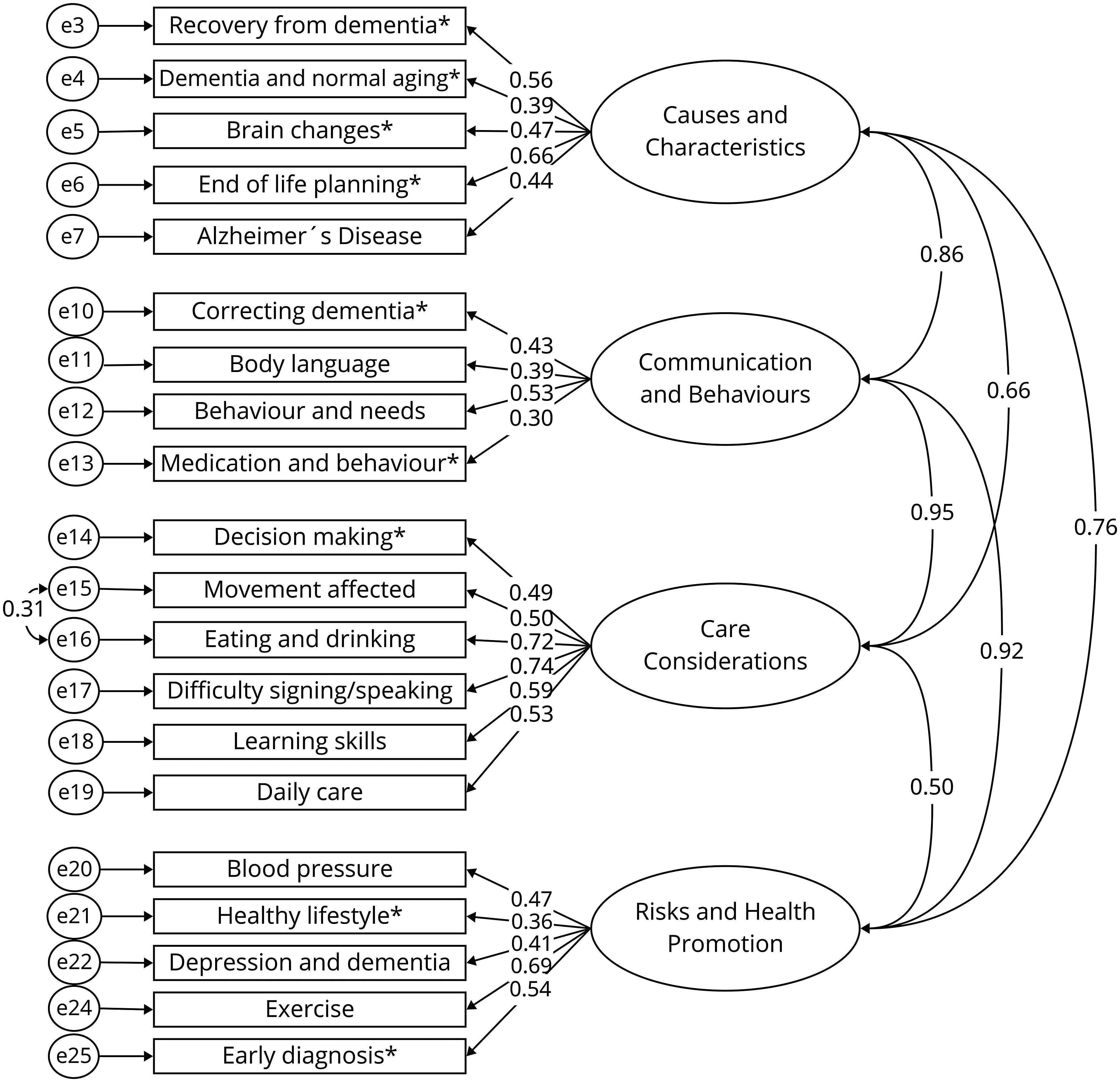
Confirmatory factor analysis of the DKAS-DGS without items 1, 2, 8, 9 and 23. Standardized factor loadings are presented for each item. Items marked with an asterisk (*) are reverse-coded. All path coefficients are statistically significant (p < 0.05).
Internal consistency of the four DKAS-DGS subscales ranged from acceptable to good, with Cronbach's alpha and McDonald's omega ranging from 0.61 to 0.77. After excluding the five problematic items, the modified version was called DKAS20-DGS and showed good internal consistency overall (α = 0.84; ω = 0.84). Subscale values ranged from 0.43 to 0.77 (see Table 3 for details).
Item analysis
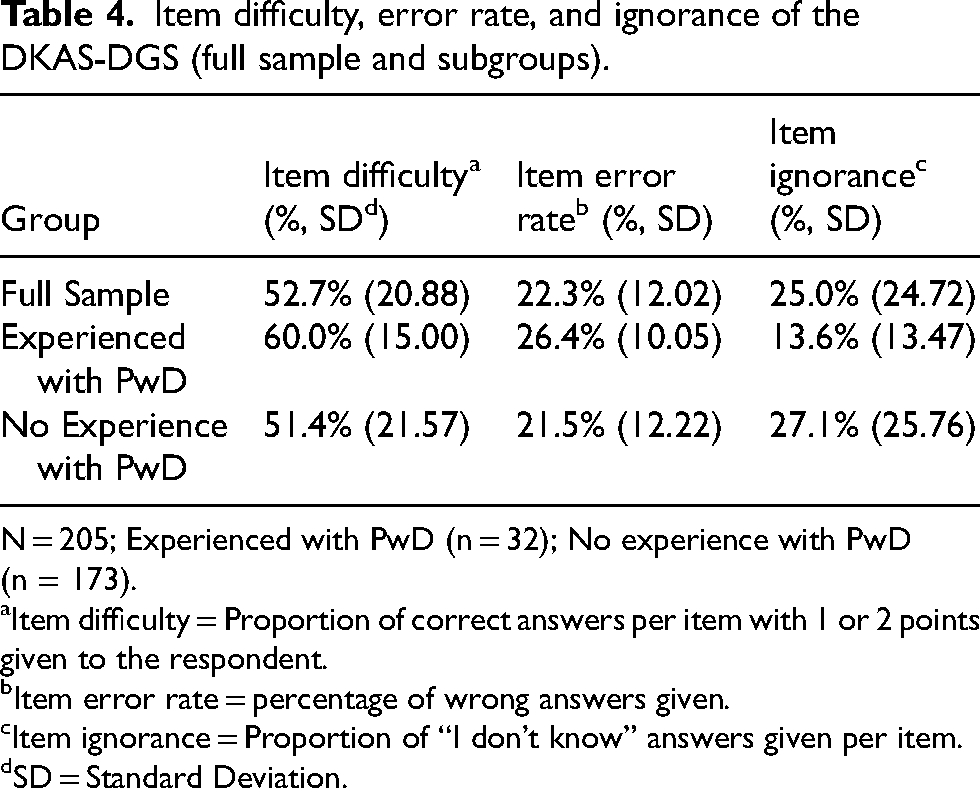
We estimated item difficulty and ignorance for each item for the total sample and separately for participants with practical and/or professional experience with PwD and without (Table 4). On average, 52.7% of the items were answered correctly, meaning respondents received either one or two points per answer. When examining individual items, the most common classification among the items was “somewhat difficult” with eleven items (25.1%–50% correct answers) (see Supplemental Table 1 for item wording and response patterns). Items 23 and 2 were classified as “difficult” (10.1%–25%). Three items were answered correctly in over 78% of the cases and classified as “easy”, while the ten remaining items were “somewhat easy” (50.1%–75%). The subgroup with practical or professional experience had more correct answers (60.0%), compared to the inexperienced participants (51.4%), with great differences in items 6, 8, 10, and 11. They also showed more incorrect responses (23.04%), especially in items 2 and 23. The proportion of “I don’t know” answer was much lower than for inexperienced participants (13.6% versus 27.1%).
Item difficulty, error rate, and ignorance of the DKAS-DGS (full sample and subgroups).

N = 205; Experienced with PwD (n = 32); No experience with PwD (n = 173).
Item difficulty = Proportion of correct answers per item with 1 or 2 points given to the respondent.
Item error rate = percentage of wrong answers given.
Item ignorance = Proportion of “I don’t know” answers given per item.
SD = Standard Deviation.
The mean inter-item correlation was 0.19 (r ranging from −0.06 to 0.62). While several item pairs exceeded the recommended range of 0.2 to 0.4, 72 several fell below this threshold, which indicates inconsistent relationships among some items. The mean item-total correlation of the DKAS-DGS was 0.40, which lies within the optimal range, suggesting that most items contributed meaningfully to the overall scale score. Only item 23 fell slightly below the commonly used threshold (r = 0.196), and it was among the five items excluded in the CFA.
Construct validity
Prior to the known-groups analyses, chi-squared test and Spearman correlations were employed to identify possible confounding variables and inspect whether the scale's outcomes are affected by general (age, gender, education) and/or Deaf-specific sociodemographic characteristics (e.g., language use, schooling type). Age and education were both significantly associated with DAS-DGS and DKAS-DGS scores (p < 0.001). Age showed weak negative correlations with both scales (ρ = 0.254 for DAS-DGS; −0.290 for DKAS-DGS), while education showed weak to moderate positive associations (ρ = 0.286 to 0.337). Although age descriptively differed between participants with and without practical experience (M = 46.38 and 51.49), this difference was not statistically significant (t(203) = 1.854, p = 0.065). Education level was also similarly distributed between the two groups (p = 0.471, φ = 0.086). Nevertheless, both variables were significantly associated with the outcome measures (DKAS-DGS and DAS-DGS scores) and were therefore included as covariates in the known-groups analyses to improve model precision.
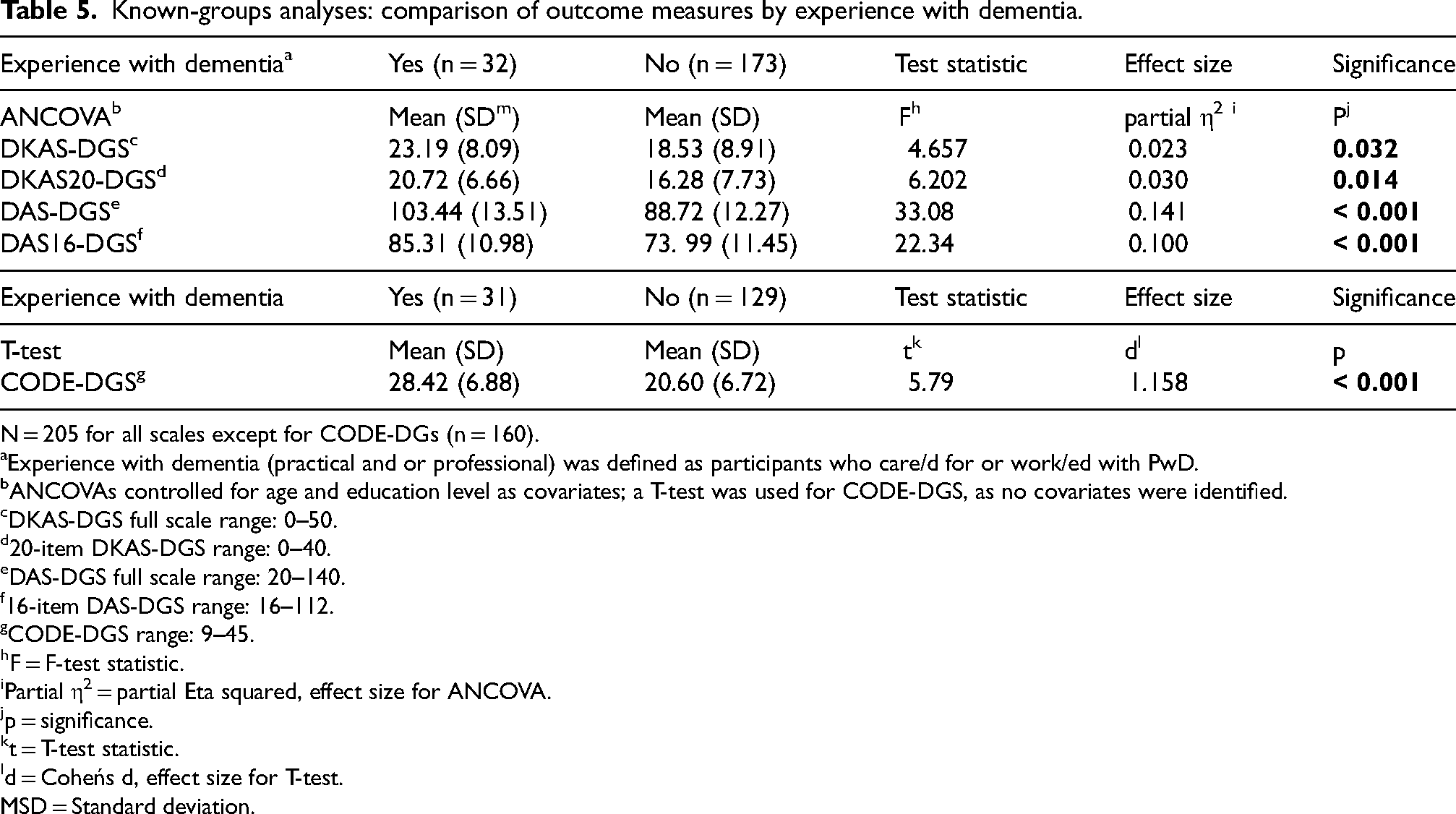
The results of the known-groups analyses are depicted in Table 5. In addition to the full scale, the DKAS20-DGS was also examined for construct validity. Results revealed that the difference in dementia knowledge scores between the experienced and inexperienced groups is statistically significant for both the full scale and the 20-item scale, with small to medium effect sizes. 79
Known-groups analyses: comparison of outcome measures by experience with dementia.
N = 205 for all scales except for CODE-DGs (n = 160).
Experience with dementia (practical and or professional) was defined as participants who care/d for or work/ed with PwD.
ANCOVAs controlled for age and education level as covariates; a T-test was used for CODE-DGS, as no covariates were identified.
DKAS-DGS full scale range: 0–50.
20-item DKAS-DGS range: 0–40.
DAS-DGS full scale range: 20–140.
16-item DAS-DGS range: 16–112.
CODE-DGS range: 9–45.
F = F-test statistic.
Partial η2 = partial Eta squared, effect size for ANCOVA.
p = significance.
t = T-test statistic.
d = Coheńs d, effect size for T-test.
MSD = Standard deviation.
Floor and ceiling effects
No floor or ceiling effect was present in the DKAS-DGS (more than 10% of the sample scored the minimum or maximum scores. 66 Seven individuals scored the minimum score with zero points (3.4%), while the highest score achieved was 45 out of 50 points.
DAS-DGS
The mean score for the DAS-DGS was 90.02 (SD = 13.54) from a possible range of 20 to 140 points. The score ranged between 56 and 138 points, with the majority of the respondents scoring between 80 and 100, and a peak centered around the mean score of 90 points. Visual inspection and descriptive statistics indicated approximate normality (skewness = –0.37, kurtosis = 0.09). This was supported by a non-significant Shapiro–Wilk test (W(205) = 0.989, p = 0.127).
Internal consistency
The DAS-DGS demonstrated acceptable to good internal consistency, with a Cronbach's alpha of 0.81 and McDonald's omega of 0.77 for the overall scale. No item would improve Cronbach's alpha if removed.
Structural validity
A CFA has been performed on the DAS-DGS (Figure 2) with the original two-factor structure of “Social Comfort” and “Dementia Knowledge”. The initial results of the CFA demonstrated an overall poor model fit, with χ²(169, N = 205) = 459.12, p < 0.001, CFI = 0.721, TLI = 0.686, RMSEA = 0.092 (90% CI [0.082; 0.102]), and SRMR = 0.107. Based on high modification indices, several correlated error terms were added between items within the same factor. The four items 1, 8, 16, 17 were excluded due to low factor loadings, standardized regression weights, and squared multiple correlations, while they also had standardized residual covariances over 2 in one or more occasions. The final model gave an improved fit to the data, but comparative indices still remained below common thresholds: χ²(169) = 459.12, p < 0.001, CFI = 0.881, TLI = 0.854, RMSEA = 0.072 (90% CI [0.058, 0.086]), and SRMR = 0.087. No further items were excluded, as the remaining items demonstrated adequate factor loadings. Τhe DAS16-DGS showed an improved internal consistency after deleting items 1, 8, 16, and 17 (α = 0.82; ω = 0.80) (see Table 3 for details).
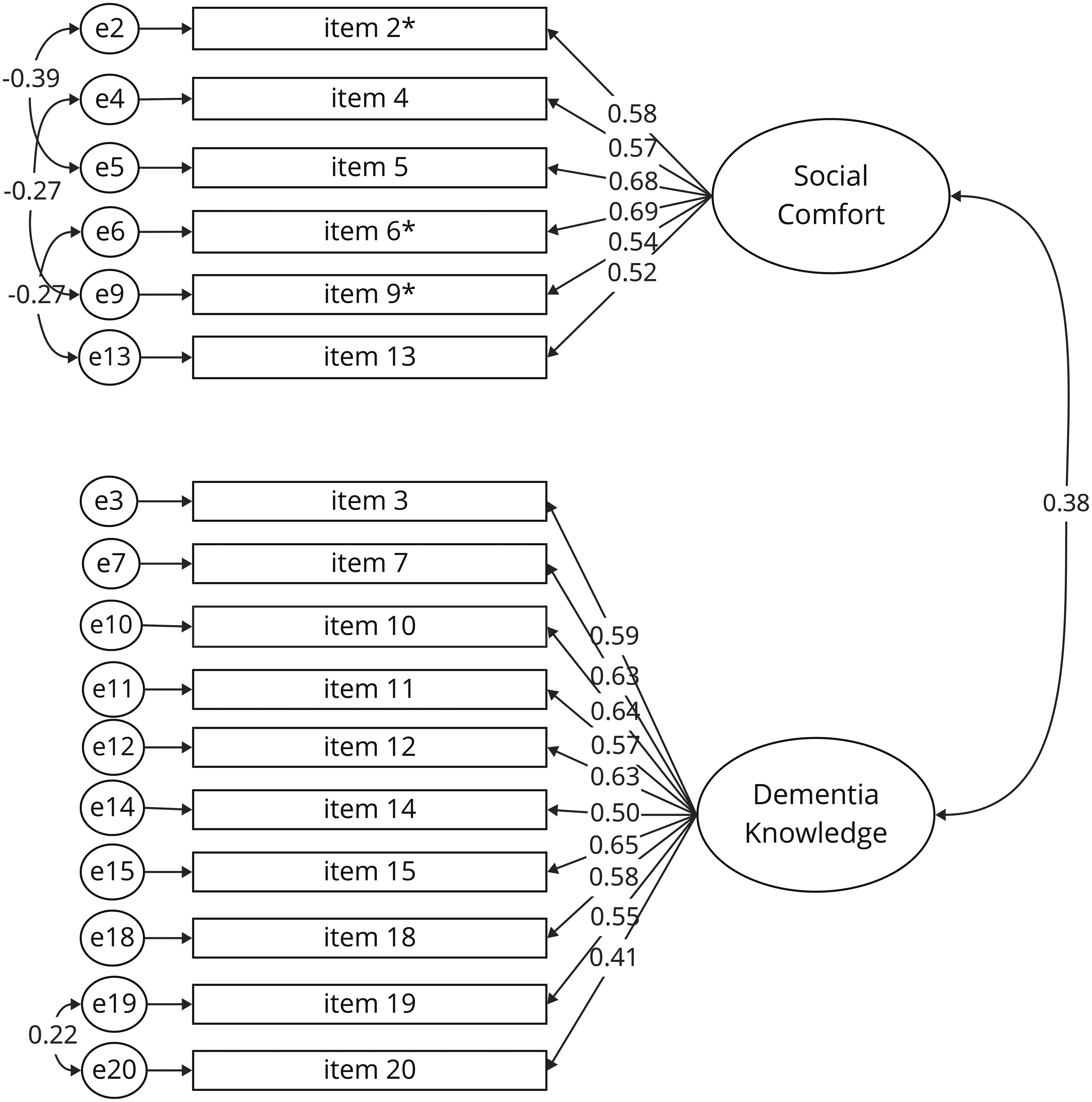
Confirmatory factor analysis of the DAS-DGS without items 1, 8, 16 and 17. Standardized factor loadings are presented for each item. Items marked with an asterisk (*) are reverse-coded. All path coefficients are statistically significant (p < 0.05).
Construct validity
As shown in Table 5, participants with practical or professional dementia experience also scored significantly higher on the DAS-DGS (M = 103.44) than those without (M = 85.31), with a large effect size (partial η2 = 0.141), even after controlling for age and education level. The shortened 16-item version of the DAS-DGS also distinguished between both groups with a large effect (partial η² = 0.100).
Floor and ceiling effects
No participants scored the minimum and maximum possible score, denying the presence of floor or ceiling effects.
CODE-DGS
The mean CODE-DGS score was 22.12 (SD = 7.41; range 9–45, n = 160). The distribution showed slight positive skew (skewness = 0.24; kurtosis = –0.50). Although the Shapiro–Wilk test indicated a minor deviation from normality (W(160) = 0.982, p = 0.034), the distribution was considered approximately normal for the purposes of analysis.
Internal consistency
The indicators of internal consistency were within the acceptable thresholds of good internal consistency (α = 0.85; ω = 0.85). 66
Structural validity
To confirm the one-factor-structure proposed by the original study, a CFA was conducted (Figure 3). Results showed that the CODE-DGS initially did not fit the one-factor structure: χ²(27) = 111.91, p < 0.001, CFI = 0.833, TLI = 0.777, RMSEA = 0.141 (90% CI [0.114, 0.168]), SRMR = 0.075. When correlated error terms were added between items 8 and 9, and items 3 and 9, due to high modification indices (MI = 49.03; MI = 17.02) and overlapping item content, the revised CFA showed good model fit: χ²(25, N = 205) = 41.17, p = 0.022; CFI = 0.968; TLI = 0.954; GFI = 0.943; RMSEA = 0.064 (90% CI [0.024, 0.098]), and SRMR = 0.047.
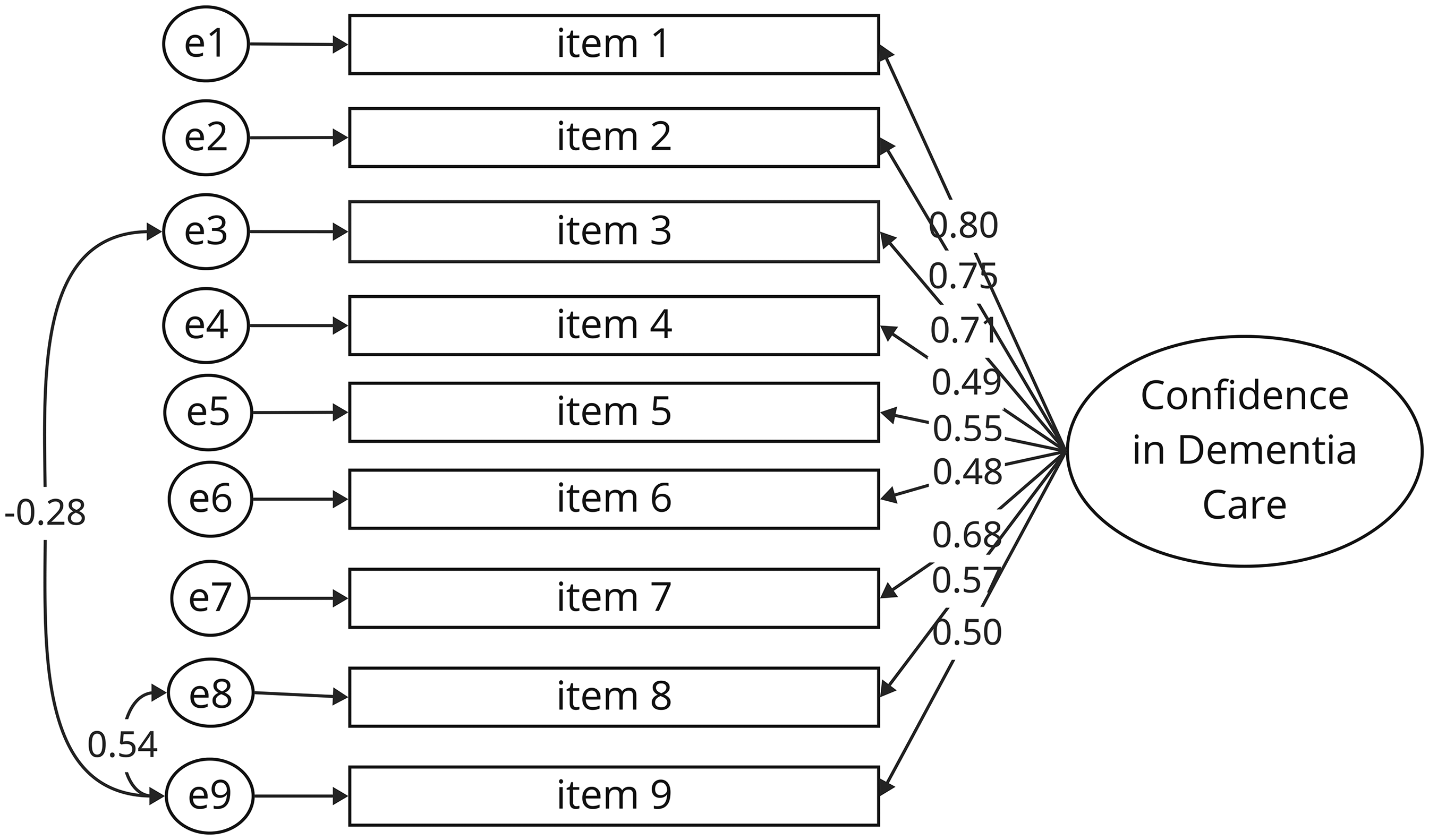
Confirmatory factor analysis of the CODE-DGS. Standardized factor loadings are presented for each item. All path coefficients are statistically significant (p < 0.05).
Construct validity
As depicted in Table 5, an independent samples T-test revealed that the CODE-DGS effectively distinguished between participants with practical and/or professional experience with dementia and those without, with a substantial effect size (Cohen's d = 1.158). CODE-DGS scores were significantly higher for participants with experience with PwD (M = 28.42, SD = 6.88) than without (M = 20.69, SD = 6.72).
Floor and ceiling effects
The range in which participants scored was 9 tο 43 points. Eight participants (5%) scored the minimum score, indicating their uncertainty in caring for a PwD. By our definition, no floor or ceiling effect was present.
Discussion
The aim of this study was to adapt the DKAS-D, DAS-D, and CODE-D into DGS, and to assess their psychometric properties within the German general Deaf population in order to provide, for the first time, linguistically and culturally appropriate tools for assessing dementia knowledge, attitudes, and confidence in dementia care within this community. All three scales and the shortened versions of the DKAS20-DGS and the DAS16-DGS showed good internal consistency. Construct validity was approved for all three scales and their shortened versions, as all could differentiate between participants with and without practical and/or professional experience with PwD. The one-factor structure was confirmed for the CODE-DGS demonstrating a good model fit. For the DKAS-DGS and the DAS-DGS, the CFA revealed that while absolute fit indices of the proposed models were acceptable, comparative fit indices did not reach the recommended thresholds. No floor or ceiling effects were present in any of the scales. An item analysis of the DKAS-DGS revealed which items had high item ignorance and item error rates, therefore giving us the opportunity to inspect content and cultural adaptation of these items.
The DKAS-DGS showed good internal consistency with a Cronbach's alpha of 0.85 and McDonald's omega of 0.85. These results fall well within the internal consistency values reported in previous DKAS adaptations across different languages, e.g., the German version DKAS-D, 61 the original scale, 60 the Greek adaptation DKAS-G, 80 or the Spanish version DKAS-S. 81 Subscale-level internal consistency was not reported in the German validation study, limiting direct comparison. However, our results are similar to the original version, 60 which reported Cronbach's alpha scores ranging from 0.65 to 0.85, while Carnes and colleagues showed slightly lower scores in the Spanish adaptation (α = 0.56–0.72). 81 The shortened version of the DKAS20-DGS still showed good internal consistency. However, a noticeable reduction in subscale-level reliability was observed in the DKAS20-DGS, particularly in Factor 2 “Communication and Behaviours”. This decline may be due to the reduction in items from six to four in this factor/subscale. While the DKAS20-DGS as a whole remains psychometrically reliable, the separate use of the subscales in future research contexts should therefore be approached with caution. McDonald's omega was additionally calculated in our study as a more robust estimate of the internal consistency. Future research validation studies of the DKAS should also include this estimate to offer a more comprehensive evaluation of internal consistency. Although there are currently no other sign language-based adaptations of the DKAS available for direct comparison, the present findings are very promising and support the reliability of the full and short versions of the DKAS-DGS.
For structural validity, the original four-factor structure 60 could be largely confirmed after excluding items 1, 2, 8, 9, and 23 due to low factor loadings, standardized regression weights, and squared multiple correlations. Removing these five items led to the shortened DKAS20-DGS, which demonstrated a model fit with satisfying RMSEA and SRMR values, while comparative fit indices like CFI and TLI remained slightly below the traditional cut-off of 0.90. Nevertheless, this fit pattern and the need for model revision are consistent with findings in previous DKAS adaptations into auditory-spoken languages. For instance, the German DKAS-D 61 and the Greek DKAS-G 80 also reached an acceptable model fit only after excluding problematic items, showing similarly good RMSEA and SRMR values and CFI and TLI values just above 0.90—a little higher than in our study. The Spanish DKAS-S was eventually confirmed for structural validity, although greater difficulties at the item level were noted. 81 Other studies, such as the Chinese 82 and Turkish adaptations 83 were not conducted with the general population but with specific professional or caregiver populations, which may partially explain their superior model fits. In contrast, the present study sampled a general Deaf population utilizing the DKAS in a visual-gestural modality for the first time, making the achieved model fit particularly encouraging. Taking all of this into account, the structural validity of the DKAS-DGS aligns well with previous adaptations, encouraging further use with Deaf DGS-signers.
There is a methodological consideration addressing the CFA conducted on the DKAS-DGS, where the scoring (0 = incorrect or “I don’t know, 1 = probably correct, 2 = correct) results in ordinal data, which partially does not meet the assumptions of continuity required for ML estimation. Nonetheless, given the approximately normal distribution of our data and a sample size above 200, ML estimation was considered appropriate, as methodical literature supports its robustness under these conditions.84,85 Moreover, this scoring has been consistently applied in the original DKAS and all published adaptations, enabling direct comparison across adaptations. Alternative approaches, such as changing the scoring and assigning “I don’t know” responses a midpoint value on a 1–5 scale, raise conceptual concerns, as they imply equal intervals between response categories. Rather than altering the scoring system, future research should consider estimation methods specifically developed for ordinal data, such as weighted least squares with mean and variance adjustment (WLSMV). 84
Examining which items specifically were perceived as difficult valuable insight into the dementia health literacy of the Deaf population sample or flags items with cultural and linguistic adaptation challenges (see Supplemental Table 1 for item wording). During item analysis, thirteen items of the DKAS-DGS were classified as “difficult” or “somewhat difficult”, showing less than 50% correct responses. Among them were items 1, 2, 8, 9, and 23, which were excluded from the DKAS-DGS during the CFA. Item 23 (due to different item ordering in the Spanish and Greek versions, the item referred to here as item 23 corresponds to the same content as item 13 in the DKAS-S and the DKAS-G: “The sudden onset of cognitive problems is characteristic of common forms of dementia”) was also excluded in the Greek DKAS-G, where it demonstrated very high item ignorance rates, while it also showed significant misalignment issues in the Spanish DKAS-S.80,81 Interestingly enough, the German DKAS-D for the hearing population found entirely different items to be psychometrically problematic during CFA (items 4, 6, 18, 19, and 25). 61 However, items 2 and 23 were the most difficult and showed very few correct answers for both the hearing and the Deaf German sample (see Supplemental Table 2). These partial overlaps and differences between samples could indicate that some items are consistently problematic in general or reflect differences in dementia knowledge among the tested populations. However, in our case, they could also indicate linguistic, procedural, and cultural challenges during translation/adaptation in DGS. 41 These include overly complex item phrasing or cultural mismatch between hearing-centric concepts and Deaf lived experience. Similar observations were reported by Fellinger and colleagues, 36 who attributed poorly performing items of the WHOQOL in Austrian Sign Language not only to their complexity but also to a “different way of thinking” shaped by the visual modality of sign language and the Deaf cultural experience.
Item analysis provided valuable insights into the performance of problematic items (see Supplemental Table 1). Some of them were affected by linguistic and conceptual challenges during translation. For item 1, the phrase “forms of dementia” was flagged in hindsight by the translation team, as the initial translation as separate signs “dementia” and “forms” lacked clarity. Signing “dementia” as a visual umbrella term and spatially mapping its subtypes would have achieved better semantic equivalence, rather than a literal translation in DGS.41,86 Other flagged terms included “physical changes” (item 5), “most effective way” (item 13), and “physical environment” (item 9), adding complexity and requiring more elaboration than a single sentence allows. Item 2 contained the term “vascular dementia”, which has no established sign in DGS and had to be fingerspelled by the signer. The absence of standardized signs for key health-related terms has been noted in other sign language validations as well, such as in Chaveiro and colleagues, 87 who criticized the lack of a sign for “Quality of Life” during their validation of the WHOQOL in Brazilian Sign Language. Culture, language, and knowledge go hand in hand. The absence of terminology, such as signs for different dementia types, therefore, not only complicates adaptation but also limits opportunities for health education and awareness. This is crucial, given that different dementia types have distinct symptoms and rehabilitation needs, while some forms, secondary dementias, are even treatable. 3 Signs within a Deaf community are usually naturally and spontaneously developed. However, it could be very helpful to explicitly develop dementia-specific signs through collaboration between native Deaf signers, preferably Deaf linguists and Deaf dementia experts. This method has already proven effective in other contexts, such as the development of technical vocabulary in BSL for science education by the Scottish Sensory Centre at the University of Edinburgh (www.ssc.education.ed.ac.uk/BSL/) or existing initiatives in Germany, such as the Sign2MINT project (www.sign2mint.de).88,89 Applying a similar strategy and establishing standardized DGS signs for dementia types is essential to enable such critical distinctions, support awareness, and, therefore, ensure equal access to dementia knowledge and health opportunities for Deaf individuals.
Nearly all of the problematic items, 11 out of 13, were false statements, which the participants may have agreed with due to a genuine lack of relevant knowledge. However, cultural factors may also have played a role, such as Deaf individuals’ limited exposure to false or trick-formulated statements that are common in written formats or transference effects described by Roberts and colleagues 55 : Unlike written questionnaires, signed versions require a signing individual, which introduces potential transference effects and non-manual features or the perceived features of the signer can unintentionally shape how questions are interpreted. While our signer attempted to remain neutral, this objectivity may possibly have made these theoretical, unfamiliar false statements to seem more plausible. Item 23, for example, may appear true due to the abstract medical terms “cognitive problems” and “sudden onset”. Among these 11 false statements, five additionally included grammatical negations (items 1, 5, 9, 21, 25), a structure previously identified as challenging to adapt in BSL, 90 but also seen as problematic in auditory-spoken contexts.91,92 In our case, the negations of these items lead to double negations on a cognitive level, meaning that respondents have to disagree with a negation (e.g., item 1 “Most forms of dementia do not generally shorten a person's life”). This might add extra cognitive load to already unfamiliar or complex questions. However, it is notable that not all items containing double negations performed poorly: Items 6 and 14 were answered correctly by the majority, with item 6 even having the highest mean score in the sample. Conversely, items 20 and 22 are neither false nor contain negation, nor were flagged during translation and performed poorly, suggesting a genuine lack of knowledge in the Deaf sample.
Participants who work/ed or care/d for PwD outperformed inexperienced participants on practical care-related items, including item 6 (end-of-life planning), item 10 (correcting a person with dementia), item 19 (comfort-focused care), item 8 (communication with persons with dementia), and item 11 (use of body language). This result underlines that practical experience improves applied dementia knowledge, which was also approved in our known-groups analysis: Participants with practical experience scored higher than inexperienced respondents, confirming the construct validity of the scale, as in other DKAS validation studies.60,61,80
Overall, participants struggled with certain items of the DKAS-DGS due to a combination of factors: genuine knowledge gap, theoretical complexity, abstract terminology, false statements, or negation. However, the fact that the experienced subgroup outperformed others even on such items, indicates that limited dementia knowledge, rather than translation alone, was the main issue. In short, while a clear linguistic and cultural adaptation is imperative, so is addressing the underlying knowledge gaps through tailored education interventions in DGS for the Deaf community.
The DKAS-DGS showed a mean score of 19.26 (SD = 8.93) out of 50 points. In comparison, the mean performance of the German hearing general population was considerably higher at 28.80 (SD = 9.46). 61 This difference may mirror disparities in dementia-related knowledge between hearing and Deaf populations of Germany, which has been assumed by several researchers due to the limited availability of tailored health information, fewer opportunities for dementia education, and language barriers experienced by Deaf individuals.9,17,18,30 The low performances on items regarding risk factors and the possibility of prevention (e.g., items 4, 20, 21) or communication with PwD (items 8, 9) highlights the need for dementia awareness courses.
The DAS-DGS had a mean score of 90.02 (SD = 13.54) among our sample and was also lower than the mean score of the German hearing population (M = 103.69, SD = 105.28). 35 This difference could reflect findings from other authors who refer to a lack of dementia awareness in the Deaf community, often leading to negative attitudes, stigma, misconceptions, and avoidance of PwD.30,93 Nevertheless, the present mean score still reflects a generally positive attitude toward dementia. Since this is the first time, attitudes have been measured using a DGS version of the scale, the results should be interpreted with caution.
The DAS-DGS further showed good values of internal consistency, comparable to the original English 57 and German version DAS-D. 35 Other cultural adaptations in auditory-spoken languages had even lower values of internal consistency compared to the DAS-DGS, e.g., the Greek version. 94 Internal consistency of the two factors “Social Comfort” and “Dementia Knowledge” were also similar to the original version and the German DAS-D. Again, this is the first version of the DAS in sign language, and the internal consistency cannot be compared to that of another signed version, but the results are very promising.
Structural validity examined whether the two-factor model proposed by the creators 57 could be confirmed through CFA. This model had previously been confirmed through PCA in the DAS-D for the German hearing general population. 35 During model revision, several error covariances were added between item pairs with overlapping content. 95 In the factor “Social Comfort”, negatively correlated error terms were observed between item pairs containing opposite affective content, such as item 2 and item 4, which address emotional comfort/discomfort (Supplemental Material 2). The model fit indicated an acceptable model fit in some indices, but did not meet the recommended thresholds across all criteria. However, due to the DAS-DGS being in an entirely different modality, we consider the results to be reasonable. The shortened DAS16 scale indicated improved levels of internal consistency than the full scale, meaning that it is a robust instrument to measure dementia attitudes among the DGS-signing population.
Among the excluded items, item 1 also performed poorly in the German DAS-D, possibly due to the replacement of the verb “work” with “interact”, when adapting it for the general population instead of care professionals. 35 Items 8, 16, and 17 were previously flagged by our Deaf translation team as difficult to naturally translate into DGS within a single sentence. Furthermore, all require reflecting on someone's own emotions and ability to care for PwD in negatively phrased statements. Negatively worded items in self-report measures are widely recognized as problematic, as they often lead to factor structure distortion (cross-loadings) and increase the risk of misinterpretation due to added complexity and cognitive load.91,92 Similar challenges have been noted in sign language adaptations, where the translation of negatively framed and emotionally complex items introduced unwanted barriers.54,55,96 Additionally, the response format of the DAS was also flagged during translation and pilot testing because of its repetitive and text-heavy nature. The research team, in collaboration with the translation team and Deaf experts, recommended adding visual cues (emojis) to reduce cognitive load and response fatigue.37,97 The greater agreement was represented by increasingly happier facial expressions. While this procedural adaptation aligns with recommendations of using modality-appropriate facilitators during adaptation, 41 its effectivity remains exploratory.
The DAS-DGS and DAS16-DGS could differentiate between participants with practical/professional dementia experience, confirming construct validity and indicating that experienced participants have more positive attitudes toward PwD. Similar results were found in previous validation studies of the DAS.35,57,94
The CODE-DGS's internal consistency was slightly lower than in spoken-auditory versions like the original version 58 or the German CODE-D, 61 but still good. The CODE-DGS continued to reveal good psychometric properties like structural validity, confirming the originally proposed factor structure without excluding any items, surpassing even stricter thresholds of TLI, CFI > 0.95, especially after including error variances between items with conceptual overlap, such as items 8 and 9. The original version of these items did not directly apply to the Deaf population, as they specifically ask about verbal communication. Therefore, “communicate (well) verbally” was not translated literally but adapted to “communicate (well)”, which is a broader and more inclusive phrasing, while still preserving the intended meaning of the items. This strategy aligns with what Chatzidamianos and colleagues 41 and other authors in sign-language-based validation studies describe. 98 Another linguistic challenge of the CODE-DGS is the question format in first-person (e.g., “I feel able to identify when a person may have a dementia”), which can pose problems in sign language because the signer and the respondent are not the same person. 55 The statements should, therefore, be reframed, e.g., by shifting perspective and changing the pronoun to “You”. However, even without this alteration, the CODE-DGS revealed stronger psychometric properties compared to the DKAS-DGS and the DAS-DGS. This could be attributed to the simpler structure of the questions, which is in line with the results of Fellinger and colleagues. 36 Finally, the CODE-DGS also proved capable of discriminating between participants with prior experience with dementia, either by working with or caring for PwD. As also found in the German version for the German hearing general population, experienced respondents had a much higher mean score in the CODE-DGS than inexperienced persons.35,58
The fact that participants with practical/ professional experience with PwD have greater confidence in care is reflected when looking at the performance of more practical and care-related items of the DKAS-DGS, e.g., for item 8, where experienced participants achieved more points, but also in the higher mean scores of the DAS-DGS because attitudes toward people with dementia are likely shaped through direct contact and practical experience may provide more empathy and reduced stigma toward PwD. All in all, the known-groups analyses found clear associations between practical/professional experience and dementia knowledge (DKAS-DGS; DKAS20-DGS), attitudes toward dementia (DAS-DGS; DAS16-DGS), and greater confidence in dementia care (CODE-DGS).
Besides, this study offered the rare opportunity to work with a larger sample of the German Deaf community. Exploring participants’ sociodemographic, cultural, and linguistic background not only reflects the community's diversity 14 but also aligns with generational differences previously described in German literature linked to language exposure, education, and lived experience.9,18 In our data, older participants were significantly more likely to have attended boarding schools or children's homes, reported later acquisition and less frequent use of DGS, and showed lower formal education levels overall. In contrast, younger respondents were more often educated in inclusive or signing-rich environments, acquired DGS earlier, and overall had higher levels of education. These findings reflect the lasting impact of historical educational settings, where older generations were often subjected to oralist educational models that stigmatized the use of sign language, limiting their access to formal education and professional opportunities.18,99 This also underscores the importance of considering generational shifts when interpreting results and designing future interventions.
The present study shows that the adaptation process presented unique linguistic and cultural challenges given the lack of prior validation studies translating German-written questionnaires into DGS, particularly in the context of dementia. However, a promising DGS adaptation of the British Sign Language Cognitive Screening Test 100 has recently completed norming, which is a promising screening tool for the DGS-signing population. 101 We followed established guidelines in cultural linguistic adaptation within the limits of organizational and budgetary resources to create valid DGS scales. Translation into DGS was carried out by one bilingual Deaf and one bilingual hearing sign language interpreter and, finally, overviewed by a Deaf researcher with content-specific training. This process reflects recommendations by previous authors to involve bilingual and bicultural professionals with diverse cultural and linguistic backgrounds in the translation.50,55 The DKAS specifically posed several adaptational challenges due to the complex structure and vocabulary of certain items. Complex items in the written version usually lead to equally complex adaptations in sign language. 98 During translation, the research team therefore discussed strategies such as explaining the statements more with examples, role play, or explanatory second sentences to improve understanding. It was also considered to include an extra layer during the translation process, where the German-written versions of the scales would first be altered into easy German (leichte Sprache) 101 and then adapted to DGS as a final step. This, however, raised a central dilemma: How far can cultural adaptation go before it alters the construct being measured? Would clarifications make the DGS version easier than the auditory-written one? This dilemma between conceptual equivalence and cultural equivalence in adapting questionnaires to sign language is discussed by various authors.36,55,98 While some eventually decided to retranslate and simplify several of their BSL items for their cohort, acknowledging the limits of the standard forward-back translation for sign language adaptation, 55 others recommend creating original measures in sign languages that emerge conceptually from the Deaf lived experience and culture from the very beginning. 41 In the context of our study, we chose to adapt DKAS because of its psychometric robustness in prior validations. However, we acknowledge that linguistically simpler questionnaires, such as the KIDE 58 might have been better suited for adaptation into DGS. Ultimately, choosing the KIDE could not be justified because of its insufficient psychometric properties within the German hearing population. 61 Even though the DKAS-DGS has difficult knowledge items, it has still demonstrated good psychometric properties, supporting its use in future settings. Future research should include a section with new deaf-specific items such as “A signing PwD has fewer communication problems in later stages” or items that emerge from specific questions which Deaf participants ask during dementia awareness courses. This section can serve as a separate subscale of the DKAS20-DGS that specifically explores the Deaf experience of dementia.
Limitations
When interpreting our findings, it is important to consider several possible sources of sample bias. First, although various recruitment strategies were used to reach a broad sample, including collaboration with different regional Deaf associations and online data collection to enhance accessibility, the target population is very specific and geographically dispersed across Germany. 9 It cannot be ruled out that the sample represents a more connected and engaged subgroup of the Deaf community and that a grey area of Deaf individuals who are less accessible may have been excluded. Second, a subset of 54 participants was recruited during senior meet-ups before attending two dementia awareness courses in Rastatt and Schwäbisch Gmünd (both located in the state of Baden-Würtemberg). While this likely introduced an age bias, it also allowed for the inclusion of individuals who might have been unlikely to participate digitally. Third, language bias cannot be ruled out since the questionnaires were adapted into DGS. While most of the participants reported DGS as their primary language, language proficiency and dialect use among Deaf individuals are heterogeneous. 9 Participants also had to handle a bimodal format of processing sign language clips while choosing written answers. This could favor those with stronger bilingual skills in DGS and written German, which was the case in our data: Younger and higher-educated participants scored higher on the DKAS and DAS versions of the study, which is why age and education were statistically controlled for known-groups analyses. It would be ideal to develop a format that could adjust to different linguistic needs and language registers of Deaf individuals, but that was beyond the scope of this study. While the sample was heterogeneous in most respects, the proportion of individuals with at least a university degree was disproportionately small, indicating a potential educational bias. Finally, only 32 participants reported caring for or working with PwD prior to answering our questionnaire, which limits the generalizability of our findings in the known-groups analyses.
Regarding the translation/adaptation process, this study presents two methodological limitations. First, a formal back-translation was not conducted, although traditionally considered the best practice in instrument adaptation, particularly for written language, and authors like Andrade and colleagues 50 include it in their recommendations of adaptation in sign language. However, some studies have noted that there is no gold standard method, and that forward-back translation may have limited effectiveness in cross-modal translations.50,55,103 Second, a full-scale pilot test or cognitive interview with a larger sample of Deaf individuals could not be conducted due to organizational and budgetary constraints. In future studies, we will integrate methods such as group translations, back translation, along with broader pilot testing and cognitive interviews. This should help improve the quality of adaptations and add to the evidence base for sign-language adaptations in dementia research.41,50,55
Conclusion
For the first time, three dementia-related scales were adapted in DGS, the DKAS-DGS, the DAS-DGS, and the CODE-DGS. Findings revealed satisfying psychometric properties for all scales, including good internal consistency, approved construct validity, no floor or ceiling effects, and acceptable structural validity. All scales can, therefore, be seen as valid tools to measure dementia knowledge, attitudes, and confidence in dementia care in the German Deaf community and among DGS-signers. They may also be used in future research settings. At the same time, the study highlighted important methodological and linguistic challenges that emerged during cross-modal translation/adaptation, especially for the DKAS-DGS. However, to our knowledge, this is the first quantitative study conducted by Deaf and hearing researchers in an inclusive process that successfully recruited a sample of 205 Deaf individuals from Germany and validated dementia-related scales in DGS. Ultimately, making validated tools available in DGS is a necessary step toward equal access to dementia research, education, and care for the Deaf community. Future studies should build on these findings by recruiting larger and more diverse samples and by further refining and culturally adapting the survey instruments, e.g., through combining methods such as pilot-testing and cognitive interviews in their translation strategies to ensure linguistic and cultural equivalence.
Our findings lead to a broad spectrum of discussion points with both theoretical and practical implications, including the absence of dementia-specific terminology as standardized signs in DGS, e.g., of the different dementia types, which limits awareness and may delay appropriate treatment. Addressing this would be very helpful, ideally in a collaborative effort of Deaf communities together with Deaf dementia professionals, DGS linguists, and healthcare providers, as discussed in relation to existing projects that create terminology, such as the Sign2MINT project for DGS and the BSL Science Glossary.
To this date, there is a crucial need for further inclusive research settings that include Deaf, bilingual, and hearing researchers to improve the quality of scale adaptations and development but also to embrace the topic of dementia awareness and mental health awareness among the signing population. Moreover, a growing interest in research and intervention will hopefully foster attention to Deaf signers and their preferences and needs in the context of dementia and mental health among society and associations responsible for shaping the health care structure, like the German Alzheimer Society and the Federal Ministry for Education, Family Affairs, Senior Citizens, Women and Youth.
Supplemental Material
sj-docx-1-alz-10.1177_13872877251390842 - Supplemental material for Measuring dementia knowledge and attitudes among the German Deaf community: Adaptation and validation of the Knowledge Assessment Scale, the Dementia Attitude Scale, and the Confidence in Dementia Scale in German Sign Language
Supplemental material, sj-docx-1-alz-10.1177_13872877251390842 for Measuring dementia knowledge and attitudes among the German Deaf community: Adaptation and validation of the Knowledge Assessment Scale, the Dementia Attitude Scale, and the Confidence in Dementia Scale in German Sign Language by Ioanna Antigoni Angelidou, Tarsitsa Ntova, Ege Karar, Marianna Tsatali and Birgit Teichmann in Journal of Alzheimer's Disease
Footnotes
Acknowledgements
We sincerely thank all participants of the German Deaf community who participated in this study, including the five Deaf dementia experts who were enrolled in pilot testing. We would like to thank Taisiya Baysalova for proofreading the manuscript in English and Anna Tzanetoulakou for her support with the signed video recordings in DGS. This research study is independent, and the views expressed in this publication are those of the authors.
Ethical considerations
Ethical approval for the study was granted by the Ethics Committee of the Faculty of Behavioral and Empirical Cultural Sciences at Heidelberg University, Germany (AZ Teich 2023 2/1). This study was conducted in accordance with the ethical principles outlined in the Helsinki Declaration of 1975. All participants were fully informed about the purpose and procedures of the study and gave their written consent prior to participation. Data confidentiality and participant anonymity were ensured in compliance with the General Data Protection Regulation (GDPR) applicable to research contexts [76].
Consent to participate
All participants were required to give written informed consent upon accessing the survey link where they were presented with a series of sign language videos in which the Deaf research team member signed detailed information about the study's purpose, data protection, the confidentiality of responses, and participants’ rights. The consent videos were accompanied by written subtitles in easy-to-understand German. Contact details for both Deaf and hearing researchers were provided for any questions or concerns.
Consent for publication
Consent for publication was obtained from all participants and all data were anonymized prior to analysis. No identifiable information is included in this manuscript.
Author contribution(s)
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research paper was supported by the Erasmus + project “DeSign—Raising Awareness for Dementia in Deaf Older Adults in Europe” (Grant/Award No. KA220-ADU-5821C986), funded by the European Commission (![]() ) and by a doctoral scholarship of the German Hans Böckler Foundation awarded to the first author.
) and by a doctoral scholarship of the German Hans Böckler Foundation awarded to the first author.
Declaration of conflicting interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: B.T. and M.T. are Editorial Board Members of this journal but were not involved or had access to any information regarding the peer review of this paper. The remaining authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
