Abstract
Intellectual Disability (ID) is a serious life-long disability and significant public health issue that arises pre-birth or during the developmental stage. It impairs intellectual, social functioning and adaptive abilities, and is one of the most common impairments among children. Under-resourced areas such as Khayelitsha in Western Cape, South Africa, have a high prevalence of ID and face immense structural, practical, and belief-related barriers to accessing ID biopsychosocial support. In collaboration with Western-trained healthcare practitioners, traditional healers within the community can contribute towards alleviating these barriers. This qualitative study utilised a phenomenological methodological approach and Bronfenbrenner's Ecological Systems theory to explore traditional healers’ perspectives on collaborating with Western-trained healthcare practitioners to provide synergised ID support. We conducted 25 semi-structured interviews and one focus group discussion with traditional healers. We analysed 11 individual interviews and the focus group using Braun and Clarke's six-step method for thematic analysis. Seven key themes were identified and divided into barriers and facilitators of collaboration. Barriers were divergent healing practices, systemic disparities, and biases against traditional healers. Facilitators were building rapport, establishing systems for collaboration, and increasing access to resources and ID support. Traditional healers viewed collaboration as sensible in supporting children with ID; however, efforts must be made to address the presenting challenges for synergised ID support within communities. Future research should involve conducting community ID collaboration studies, garnering insight into collaboration efforts, documenting traditional healing practices, and conducting advocacy research to rectify systemic disparities.
Keywords
Introduction
There is a stark lack of access to resources and services for the care of children with Intellectual Disabilities (IDs) in low- and middle-income countries (LMICs), particularly for those living in poverty-stricken conditions who are unable to afford private healthcare services (Adnams, 2010; Kett et al., 2020; Kromberg et al., 2008; Maulik et al., 2011; Mkabile & Swartz, 2022b). ID is serious life-long disability that arises pre-birth or during the developmental stage; it impairs intellectual, social functioning and adaptive abilities, with a global prevalence rate of approximately 10 per 1,000 individuals (Hudson & Chan, 2002; Kromberg et al., 2008; Maulik et al., 2011; Mkabile & Swartz, 2020). ID is a significant public health issue and one of the most common impairments among children, being comorbid with various mental health conditions (Hinde et al., 2022; Matson & Cervantes, 2013; Maulik et al., 2011; McConkey et al., 2019; White et al., 2005; World Health Organization [WHO], 2019). Caregivers of children with ID, in rural areas or informal urban settlements, often seek treatment, care, and support from traditional healers due to their cultural beliefs and the lack of access to ID biomedical healthcare services (Adnams, 2010; Ajuwon & Brown, 2012; Aldersey et al., 2016; Anjorin & Wada, 2022; Kett et al., 2020; Kromberg et al., 2008; Masulani-Mwale et al., 2016; Mkabile & Swartz, 2022a). Approximately 80% of South Africans access traditional healers before biomedical healthcare (Adnams, 2010; Campbell-Hall et al., 2010; Solera-Deuchar et al., 2020; Van Rooyen et al., 2015).
While many South Africans engage in medical pluralism by utilising both conventional and alternative medical systems, the relationship between traditional healers and Western-trained biomedical practitioners remains tenuous and divided (Academy of Science of South Africa, 2022; Galvin et al., 2023; Hopa et al., 1998; Shih et al., 2010). This separation risks patient harm due to toxic interactions between traditional medicine and biomedical medication (Hopa et al., 1998; Kokota et al., 2022). It may also result in delayed, ineffective, or an absence of necessary care (Hopa et al., 1998; Van Rooyen et al., 2015). Collaboration between the two systems can enhance ID treatment, accessibility, and acceptability, particularly in underserved areas (Mkabile & Swartz, 2022b). There is a pressing need to bridge the gap between these systems in the interests of adequate and synergised ID support provision (Mkabile & Swartz, 2022b).
Traditional Healers’ Role in ID Support Provision
Traditional healers are rooted in their cultural heritage and spirituality and use indigenous practices to treat physical and spiritual illnesses and promote well-being (Adu-Gyamfi & Anderson, 2019; Galvin et al., 2023; Haque et al., 2018). These practices include herbal remedies, incantations, religious verses, communicating with ancestral spirits, and rituals (Adu-Gyamfi & Anderson, 2019; Galvin et al., 2023; Haque et al., 2018). They are sought for their compatibility with caregivers’ cultural beliefs about the causes of mental health difficulties and ID (Anjorin & Wada, 2022). Extant literature has indicated that traditional healers hold various beliefs regarding ID (Kpobi & Swartz, 2019; Mkabile et al., 2021; Nortje et al., 2016). While some traditional healers attribute the cause of ID to physiological problems, others attribute it to spiritual or religious reasoning (Kpobi & Swartz, 2019; Mkabile et al., 2021; Nortje et al., 2016). Studies suggest that these beliefs are informed and influenced by various ecological factors such as religion, culture, tradition, media, and societal norms (Algood et al., 2013; Kpobi & Swartz, 2019; Mkabile & Swartz, 2022b). Given the respected positions traditional healers hold in communities, they have the potential to address stigma around ID and the practical barriers to accessing biomedical services (Algood et al., 2013; Kpobi & Swartz, 2019). Traditional healers are often located in close proximity to families, sharing similar lingual, cultural, and communal backgrounds, making them vital role players in initiatives to support caregivers (Audet et al., 2022; Green & Colucci, 2020; Kong et al., 2021; Schausberger et al., 2021; Sorsdahl et al., 2009). Equipping traditional healers with biomedical skills through training and education enables accurate diagnoses, treatment plans, and care for patients with ID (Audet et al., 2022; Cordeiro-Rodrigues & Metz, 2021; Green & Colucci, 2020; Kong et al., 2021; Kpobi & Swartz, 2019). Studies acknowledge the usefulness of traditional healers’ methods and advocate for collaboration between allopathic treatment and alternative medicine (Audet et al., 2022; Gessler et al., 1995; Nortje et al., 2016). However, traditional healers express concerns about the treatment and respect they receive from Western doctors, as well as cultural incompatibilities inherent in such collaborative efforts (Green & Colucci, 2020; Kong et al., 2021).
Barriers to Collaboration
Of the various forms of collaboration, literature indicates that a collaborative model is the most favoured form as it allows both systems to remain autonomous, with mutual recognition and respect (Hopa et al., 1998; Shields et al., 2016). Persistent power imbalances, mistrust, and claims of superiority fuel tensions between the two systems, creating challenges to collaboration (Academy of Science of South Africa, 2022; Hopa et al., 1998; Kokota et al., 2022; Moshabela et al., 2016; van der Watt et al., 2017). Additionally, insufficient recognition from the government and institutionalised inequality contributes to the lack of effective collaboration, as traditional healers receive significantly less structural support (Academy of Science of South Africa, 2022; Hopa et al., 1998; Keikelame & Swartz, 2015; Van Rooyen et al., 2015). Studies show that traditional healers are open to collaboration, but express apprehension due to fear of exploitation, unidirectional referral practices, and perceived inadequacy and inferiority (Campbell-Hall et al., 2010; Keikelame & Swartz, 2015; Kokota et al., 2022; Solera-Deuchar et al., 2020; van der Watt et al., 2017). Conversely, biomedical practitioners’ resistance and ambivalence towards collaboration, rooted in their perceived supremacy and their belief that traditional healing lacks scientific validation, forms a barrier to collaboration (Academy of Science of South Africa, 2022; Campbell-Hall et al., 2010; Chitindingu et al., 2014; Kokota et al., 2022; Moshabela et al., 2016; Shields et al., 2016; van der Watt et al., 2017; Van Rooyen et al., 2015). When considered, collaboration is often conditional, requiring traditional healers to refer patients and conform to the biomedical paradigm, reinforcing the perceived supremacy of biomedicine (Campbell-Hall et al., 2010; Kokota et al., 2022; Moshabela et al., 2016; van der Watt et al., 2017; Van Rooyen et al., 2015).
Facilitating Effective Collaboration
Numerous studies emphasise the need for mutual respect and understanding of each other's competencies and differences (Hopa et al., 1998; Kokota et al., 2022; Moshabela et al., 2016; Shields et al., 2016; Van Rooyen et al., 2015). This principle lays the groundwork for harmonious integration of both systems, which is essential for fostering trust, humility, confidence, cooperation, and open communication, enabling a culturally sensitive healthcare system (Academy of Science of South Africa, 2022; Hopa et al., 1998; Kokota et al., 2022; Shields et al., 2016; Van Rooyen et al., 2015). Successful collaboration requires an open mind and a willingness to learn and adapt, allowing both sectors to enrich their practices (Awodele et al., 2011; Brolan et al., 2014; Keikelame & Swartz, 2015; Kokota et al., 2022; Shields et al., 2016). Formalised and coordinated approaches should be established to recognise and validate both sectors’ expertise (Academy of Science of South Africa, 2022; Brolan et al., 2014; Keikelame & Swartz, 2015; Kokota et al., 2022; Shields et al., 2016; van der Watt et al., 2017). Studies propose the need to equip traditional healers with information on identifying and treating mental health issues and referring clients to biomedical healthcare workers for cases beyond their scope (Academy of Science of South Africa, 2022; Kokota et al., 2022). Similarly, Western-trained workers should learn about traditional healing to identify spiritual ailments and refer clients accordingly (Academy of Science of South Africa, 2022; Kokota et al., 2022). Safeguarding intellectual property and integrating traditional healing into medical curricula are proposed to facilitate collaboration (Chitindingu et al., 2014; Kokota et al., 2022; Van Rooyen et al., 2015). Successful collaboration in tuberculosis, HIV/AIDS, and safe motherhood treatment has led to improved patient outcomes through training and referral (Audet et al., 2022; Keikelame & Swartz, 2015; Kokota et al., 2022; Schausberger et al., 2021; Sorsdahl et al., 2009). An ID psychoeducation intervention for traditional healers may foster similar responses, but there is a lack of literature on traditional healers’ experiences with interventions to improve their knowledge of ID (Sorsdahl et al., 2009). Masulani-Mwale Kauye et al. (2019) developed a culturally congruent psychosocial intervention in Malawi based on the lived experiences of caregivers of children with ID, which was highly acceptable in the community (Masulani-Mwale et al., 2019). The success of this approach highlights the importance of using lived experiences to develop impactful interventions (Machalicek et al., 2015; Masulani-Mwale et al., 2019).
There is limited literature on collaboration between Western-trained biomedical healthcare practitioners and traditional healers for providing synergised ID support to families of children with ID (Mkabile & Swartz, 2022b). To effectively enhance traditional healers’ understanding and treatment of ID, intervention programmes must be synergised with their cultural views and practices (Algood et al., 2013). Therefore, initiating pilot programmes in under-resourced communities with high ID prevalence is crucial (Brolan et al., 2014; Keikelame & Swartz, 2015; Mkabile & Swartz, 2022b; Shields et al., 2016). Subsequently, conducting emic research is essential to gauge the acceptability of such collaborative efforts, determine successful implementation strategies, and identify potential barriers (Brolan et al., 2014; Hopa et al., 1998; Keikelame & Swartz, 2015; Mkabile & Swartz, 2022b; Shields et al., 2016).
The Main Study
In Khayelitsha, a culturally congruent, collaborative psychoeducation intervention on ID equipped traditional healers, spiritual leaders, NGOs, and caregivers with a biopsychosocial understanding of ID forming part of a participatory action research study. This study is a substudy thereof and thereby uses participants from the main study (Multi-Regional Clinical Trials Center of Brigham and Women's Hospital and Harvard, 2024). The intervention with traditional healers involved a series of sessions between Western-trained workers and healers on ID service provision, representing the interaction between biomedical and traditional healing.
Aim of the Study
This study aimed to gain insight into traditional healers’ views on collaboration with Western-trained healthcare practitioners in the interests of providing synergised ID support to families of persons with ID. The obtained insights can inform collaborations between Western-trained healthcare workers and traditional healers, guiding optimal service provision for families caring for children with ID. It can also highlight positive and conflicting aspects of partnerships across ecological systems, offering direction for improvement.
Research Questions
What are traditional healers’ views on collaboration with Western-trained healthcare practitioners for the provision of ID support to families of persons with ID?
Sub-Questions
What challenges or barriers do traditional healers perceive in collaborating with Western-trained healthcare practitioners? What do traditional healers deem conducive for successful collaboration with Western-trained healthcare practitioners? How do traditional healers perceive a collaboration with Western-trained healthcare practitioners benefitting families of persons with ID?
Theoretical Framework
This study employs Bronfenbrenner's Ecological Systems theory, recognising individuals, such as children with ID or traditional healers, as embedded in interconnected systems that mutually influence each other (Bronfenbrenner, 1986, 1994). These systems, including the microsystem, mesosystem, exosystem, macrosystem, and chronosystem, shape individuals’ development, functioning, experiences, and perceptions, while individuals, in turn, impact these systems (Bronfenbrenner, 1994). The compromised functioning of these systems in this study includes the lack of accessibility to culturally congruent biopsychosocial care for children with ID and the subsequent negative impact this has on their health (Bronfenbrenner, 1994; Kromberg et al., 2008; Mkabile & Swartz, 2022b). It also involves the tenuous relations between Western-trained healthcare workers and traditional healers within the different systems (Mkabile & Swartz, 2020, 2022b). The culturally congruent ID intervention serves as a microcosm for collaboration, capturing traditional healers’ views on ID support, including their experiences beyond the intervention (Bronfenbrenner, 1994; Mkabile & Swartz, 2022b). The theory helps us understand how interrelated systems influence traditional healers’ views of collaboration, providing insights into what is needed for synergised ID support (Bronfenbrenner, 1994).
Method
Research Design
This study employed a qualitative research design to identify themes and patterns and gain insights into people's experiences, behaviours, and perceptions (Creswell, 2007; Terre Blanche et al., 2006). Following a transcendental phenomenological approach, the study aimed to understand traditional healers’ shared experiences of collaborating with Western-trained biomedical healthcare practitioners (Creswell, 2007). This approach explores how experiences are impacted by conditions and contexts, focusing on traditional healers’ perceptions within the culturally congruent ID intervention and beyond. Phenomenology asserts that human consciousness shapes the nature of a phenomenon through perception (Bliss, 2016). Rooting the collaboration perspective in the experiences of traditional healers is crucial to addressing the silencing and underrepresentation of culturally diverse groups in the literature. This challenges the reliance on Western understandings, enabling a more nuanced understanding of barriers, opportunities, and perspectives (Patton, 2002).
Setting and Participants
The study was conducted in Khayelitsha, a predominantly Black township in Cape Town, South Africa (Mkabile & Swartz, 2022a). Khayelitsha is a historically disadvantaged community and is home to many traditional healers (Mkabile & Swartz, 2022a). Purposive sampling was used to ensure that the selected participants aligned with the research question, particularly traditional healers who underwent the culturally congruent psychoeducation intervention on ID (Creswell & Poth, 2017; Mkabile et al., 2021). Twenty-five participants were recruited from the main study and interviewed with the intention that the data collected would be used for both the main study and the substudy. By the eighth interview, no new codes were being generated, the rest of the transcripts were read, and three additional interviews were analysed from these as they had novel ideas. Data saturation was reached by the analysis of these 11 individual interview transcripts and thus only 11 of the 25 interviews were analysed (see Table 1) (Saunders et al., 2017). Of the 25 participants, 16 voluntarily participated in the focus group discussion (see Table 2). Our participants included amagqirha or izangoma (diviners), amaxhwele (herbalists), a prophet, and a community healer.
Sample Demographics for Individual Interviews.
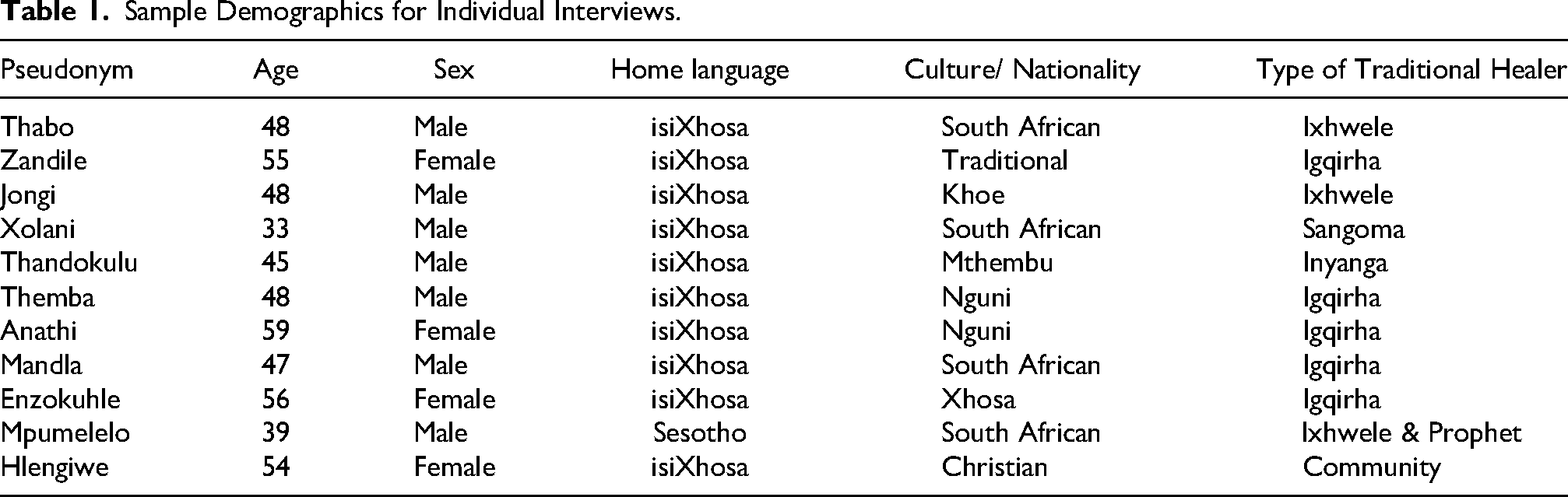
Sample Demographics for Focus Group.
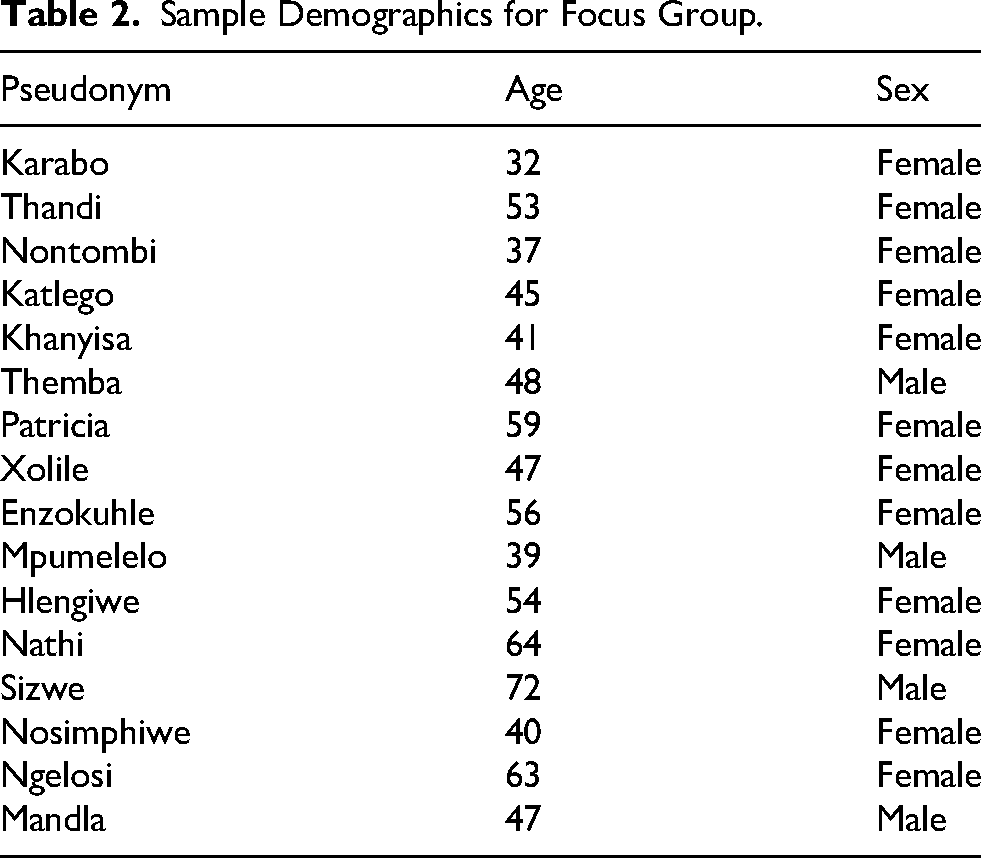
Data Collection
Data collection took place at the Church of Christ in Mandela Park, Khayelitsha, involving individual interviews and a focus group discussion. A semi-structured interview guide was created in English and translated into isiXhosa. Twenty-five individual interviews (20–60 min) were conducted to gather in-depth accounts of traditional healers’ experiences, focusing on their views of collaboration with biomedical doctors, the government's role, and ID treatment (Baumbusch, 2010). Following these, a 90-min focus group with 16 participants explored the similarities and differences within the group, uncovering aspects that did not emerge during individual interviews (Baumbusch, 2010; Creswell & Poth, 2017; Gill et al., 2008; Mkabile et al., 2021). The sessions were conducted in English or isiXhosa based on participant preference, and were transcribed and translated for analysis.
Data Analysis
This study employed thematic analysis in preference to interpretative phenomenological analysis, as thematic analysis accommodates larger samples and encapsulates extensive qualitative data, which enabled us to treat the dataset holistically to accommodate the time constraints of the research (Braun & Clarke, 2006, 2021; Love et al., 2020). Thematic analysis allowed a reliance on traditional healers’ perceptions and maintained a close fidelity to the in-depth transcripts (Clarke & Braun, 2017; Guest et al., 2012). Eleven interviews and one focus group discussion were transcribed and translated from isiXhosa to English (Braun & Clarke, 2006). We employed Braun and Clarke's systematic thematic analysis approach, involving coding, theme development, and interpretation. To ensure rigor, transcripts were independently coded, codes were discussed and refined, and key themes were identified. Finally, we wrote up the findings, incorporating illustrative quotes from the transcripts to support our interpretations. Quality control and consistency were ensured through continuous researcher discussion (Braun & Clarke, 2006). The results, supported by transcript extracts, were written up to highlight theme salience and convey understanding and interpretations (Braun & Clarke, 2006).
Ethical Considerations
Ethical approval was obtained from the University of Cape Town's Psychology Department's Research Ethics Committee before data collection commenced. The reference number is PSY2023-015. Courtesy and respect were maintained throughout the data collection process by ensuring informed consent, explaining the purpose of the study, and emphasizing the voluntary nature of participation. Participants were assured that their information would be used solely for research purposes and that their information would be treated with the utmost confidentiality, through the use of pseudonyms and of password-protected files accessible by the researchers and supervisor. Additionally, we observed cultural norms to foster a respectful and inclusive research environment, such as greeting participants in a culturally appropriate manner (Byrne, 2001; Klopper, 2008; Mertens, 2012). Participants received a comprehensive briefing on the nature of the focus group discussion, allowing them to establish ground rules and confidentiality guidelines (Sim & Waterfield, 2019).
Reflexivity
Reflexivity involves recognizing the influence between researchers and participants on the research process (Spencer et al., 2003). Transcendental phenomenology urges researchers to bracket personal experiences (Creswell, 2007). We thus journaled and discussed our beliefs to suspend them and focus on participants’ experiences (Bliss, 2016). Given our outsider positionality as UCT Psychology Honours students living outside Khayelitsha and not being traditional healers, there may have been social desirability bias or participant hesitation. One researcher, a Coloured woman with no experience with traditional healers, approached the study openly and respectfully. The other, a Xhosa woman with experience in this area, shared cultural ties with participants, aiding rapport and communication. Despite similarities, both researchers remained open to learning from participants, and their differences helped address potential biases.
Results
Barriers to Collaboration
Divergent Approaches and Practices
The traditional healers identified that the differences in how traditional healing and biomedicine are practised, conceptualised, and approached create significant challenges for mutual understanding, and thereby collaboration: Biomedical section or sector understands only on physical symptoms, physical causes of everything. While in the traditional health practitioner we understand holistically, meaning before we talk about physical we will first look at the signs of spiritual. (Thabo) There still needs to be matter of understanding between the two. Of course they went to school, they’ve got papers, they have ways of doing things. And then we didn’t go to school for this, we sleep, we dream and then … (Focus group discussion [FGD]) The Western … they don’t believe in traditional healers. Eeh, because we have a lot of things that are different, that are, some other people will never understand … So doctors or the West, they don’t believe that someone with a disease could be helped by traditional healing. (Hlengiwe) It can be difficult because of there will be always, eh, what is so called … opposition of knowledge. (Xolani) Oh, Western medicine is complicated. In this way, they don’t see eye to eye with us. (Zandile) You don’t do medicine, you have to prescribe what has been bought by the hospital for the hospital. You don’t say as a doctor, no no, I think I can use this particular one for me, I think this works … The doctors has been taught how to prescribe what we use. So you know those limits, so you got certain limits as Western doctors. Even though you went to school extensively to be able to apply your mind, but you are not allowed to apply your mind, that is the first difference. With us we apply our minds. (Thandokulu) But we cannot disclosed. Our, you know, when you’re a sangoma your ancestors, they’ll give you the special muthi … So the minute you share, you disclose information to the Western, the minute ancestors now fold their arms, they will stop giving you another gift … So it's good. It's good, but we’ll not disclose these medications for what. We won’t disclose. Because they’re sacred, it is a secret. (Mpumelelo)
Systemic Disparities: Exploitation and Resource Allocation
Systemic disparities, exploitation, and resource allocation within the healthcare system came up frequently, with traditional healers expressing concern about the uneven playing field they perceive when comparing their practice to the biomedical sector. Participants’ perceptions of their exploitation, their lack of governmental support, and the effectiveness of Western medical approaches reveal the profound barriers that exist to collaboration. Apprehensions about the exploitation they have experienced in working with the biomedical sector were often raised: We’ve been involved with many institutions but we have never, you know, been into a level where we give out information. Because research has been … you know, has been based on milking information from us. (Thandokulu) Very much important is we need them to first give the recognition to traditional health practitioners, because most of the biomeds they want to suck information but they don’t want to bring you there. They want to get credit on behalf of all traditional healers. (Jongi) [The] problem is that our government is not recognising our herbs and they prefer the Western ones. (Mpumelelo) We are not recognised by the constitution, neh! So the constitution is only against us, that you can’t go to a specific reservoir, let's say so, nature reserve, because we don’t have licence, you can’t dig out this muthi [traditional medicine] right. Whereas, as a traditional healer, you know, what is this muthi is for, right, so that is against us. (Xolani) Our government is not really committed … government is not giving money for traditional health practitioners. Because if government can fund institutions … We put request of money from government, government will reject those requests. (Thandokulu) Those are the things that we don’t have. And again we don’t work with medical aids. Most of the time now they find out that it is easy for them to go to Western because they just pay with medical aid. (FGD) We are not here to suppress the problem, we are here absolutely. Then the Western are here to sustain the problem with pills. That makes our community to depend on pills and that shortens their lifespan … From all what they are saying they are healing, but those are the side effects, each and everything that come from West, that's chemicals. But they know and they are aware of the real medication that they can use to irradicate the actual problem. But they are sustaining their economy using African lives, to sustain their economy by bringing the drugs that will sustain and suppress the real problem instead of healing it out. (Jongi) If ever government would ever stop putting in politics … there are these drugs that help people in the hospitals … you find that sometimes the business women that is known is distributing these drugs in through her firm, and through her factory is making these drugs which means that she has a contract with the government for five years or three years that is worth billions … I think maybe the government doesn’t want us to maybe get into it because we will get there and it will not be of much cost. We get there, we put together our medicines, our traditional medicines, and the person is healed. (Mandla)
Biomedical Bias: Attitudes Towards Traditional Healers
Participants were asked about the attitudes, views, and beliefs that Western trained doctors hold towards traditional healers and their practices. Traditional healers shared that they have felt undermined, disrespected, and devalued by the Western biomedical sector: Western doctors, because they take us for nothing, because they have that thing that our traditional medicine like, firstly, they have that thing where they say we work from dirty places, they say so. Two, they have that thing that says, like they undermine us, let me put it that way. (Anathi) The only thing we need is when the person, maybe I see this person is not right for me and then I send to the traditional, to the Western doctors. But the Western doctors, they also need, when they know that this person, they can’t heal this person, they must send back to the traditional healers, but they don’t do that. (Themba) Now, we will be able to trust you, because you don’t trust us. And I alone I don’t blame you because we as traditional healers look down and don’t accept each other. (FGD) So it seems to me if also we can look in the mirror or ourselves to check maybe if we can accept each other first, it can be easy to fight this disease of us to be undermined with the Western. (FGD)
Facilitators of Collaboration
Building Rapport
Rapport is understood as a sense of understanding of each other's ideas and feelings which enables effective communication and harmonious relating (Travelbee, 1963). Numerous traditional healers spoke to the ways in which facilitating rapport was essential for a successful collaborative relationship to exist within ID intervention, and the ways in which this was cultivated through the presence of values, practices, and attitudes. These included trust, dignity, respect, listening, open-mindedness, humility, freedom of expression, genuineness, openness, and a recognition of traditional healing. Sincerity and a genuine intention to work with traditional healers based on an acknowledgement of their value and expertise is vital for collaboration to occur: If I am treated with dignity that, like this person knows what they are doing, they would be of assistance to us and not because they feel under pressure. (Mandla) What is important is to respect each other to each other's point of view and culture, and the way of doing things. (Mpumelelo) It's for the professors to come to us, neh, and then they engage with us and then they share what they learn from the scientific side, neh. And then learnt from our traditional healing perspective. (Xolani) It was difficult in the beginning because we did not know each other, do you understand? So you find that if you are being asked a question, you do not feel free and you are afraid … but as the time went by we became free amongst the people in front of us … We trusted them and thought, no man! They have never taken information from us, instead they bring their own, so where we meet each other halfway, we share views around how to tackle this thing. (Anathi)
Establishing Systems for Collaboration
Traditional healers emphasised the importance of government recognition, collaboration with medical and educational structures, and formalised traditional healing systems. They believed that a macrosystem change through government recognition would lead to greater collaboration between traditional healers and doctors: “The doctors come in and now that they see that, okay, the government have welcomed us, then we can collaborate and then, now it is where the doctors can be flexible for us” (Mandla). Traditional healers expressed the need for an accredited constitution and governing body to authenticate their practice and foster understanding and trust between traditional healing and the Western biomedical healthcare system. Additionally, they highlighted the need for traditional healing organisations to advocate for healers and be represented in government bodies involved in systemic changes. In addition, they emphasised the importance of unity among traditional healers to establish a formal, organised structure to facilitate their integration into the system: There are people who are traditional healers at the head who should put pressure on these people so that our request can be accepted. (FGD) If you break the law there will be something that happens to you, a constitution that bind us as sangomas in the same way that Western doctors have theirs. I think then that things would be right. (Mandla) She represents something known and it is in our constitution as traditional healers and chiefs. Then now we will be able to trust you, because you don’t trust us. (FGD) Everything is accounted for because all these particular pockets, they’ve got their own leadership hierarchy. And even all of these when you bind them together there is that particular synchronisation interaction and interrelation. Because African spiritual is African spirituality … say I’m Molozwi or I’m Ndawo, I’m Camagu, I’m Nguni. (Thandokulu) If they can’t help a person and I can they must refer them to me, and if I can’t help them I take them to them. And then they must refer them back to me. (Zandile) When the Western doctors there by the hospital find out they can’t heal this … send the person to the traditional healers … And then also then the traditional healers, when they see that this thing … need to be healed by the Western doctors as they always do, they must send straight to the doctors, to the hospital. (Themba)
Increasing Access to Resources
Traditional healers stressed the need for access to resources, including education, training, funding, facilities, and protected areas for traditional healing practices. They believed these resources would empower them, promote collaboration with the biomedical sector, and improve support for various health conditions within the community. Traditional healers also wanted to have access to hospitals and patient records to understand patient history and ensure suitable treatments. Medical equipment and training in its use were particularly highlighted to enhance patient safety and complement their work: They should give us a stethoscope, things to look at blood sugar, but they should train us. (Anathi) So what we really need are medical measuring devices, like the oxygen, thermometer so that we can check the body temperature. So that we don’t just give someone medication and their condition becomes worse. (Zandile) I think that we gonna help if we can just work together in facilities like this. You bring these people here and you pay us like you are getting paid because it's a hard job, it's not an easy job. (Xolani) Government must protect these sacred places … And also protect our rivers and uh, because we use to also to practise by using those rivers … definitely we protect the medicine, the herbs, because there are herbs on those mountains that we are using. (Mpumelelo) So we want government to come back to work with the ground roots projects. Then by doing that will … by doing that will doing much more important things. (Jongi) You mustn’t just say, no, we have released funding for this and that, but we don’t see it. (FGD) I think the way in which we can collaborate, eeh! there would be a need for like that thing we were saying, ahh structures in our communities. If we used these structures … we know that through them, things can reach the people. (Hlengiwe)
ID Support
Traditional healers highlighted that collaboration would enhance ID support within communities, perceiving that collaboration would provide access to both traditional and Western perspectives on understanding and healing ID. Numerous healers spoke about the benefits of acquiring ID biomedical knowledge, particularly that it expanded their understanding of ID—providing them with additional ways to examine and understand individuals with ID and its underlying causes. Traditional healers were open to collaboration and there was a shared recognition of a need for the two systems to meet each other halfway in light of the high prevalence of ID in underprivileged communities: We need to have, ehhh more collaborations with the Western doctors to help our community in those disabilities … Now and then we meet each other and then we can get an answer, how to deal with, solve the problem. (Themba) We learned that not all the people, neh, that are intellectual disable are like, you can just recognise witchcraft from that situation … there are intellectual challenges in life … besides examining them using traditional healing, also examine them with another eye, which is use both eyes, not one eye to see things. (Xolani) This is something that can take us to another level and we can also make us find ourselves working with the communities, because this is not known in our community, it is known by us who already have this privilege to be here in this class. (FGD) Western doctors, they know nothing about our communities. We are living here. We know everything that's going on here … So it will be really, really it’ll it’ll do big good for the community to work together. Only if they recognise us … we need each other. So, when you have the knowledge of something, then you need to share so that you save that life, even without you knowing that you have saved the life, you understand. (Enzokuhle)
Discussion
Traditional healers shared that they gained knowledge and skills from the Western biomedical perspective, which equipped them not only to identify signs of ID within the community but also to impart critical knowledge on its treatment and management, thus combating the inaccessibility of biomedical services support (Mkabile & Swartz, 2020). They raised concerns about the treatment of children with ID, expressing the need for ongoing ID awareness and education interventions for themselves and their communities, supporting findings that traditional healers find collaboration in the interests of ID support provision a feasible and desirable endeavour in Khayelitsha, Western Cape (Mkabile & Swartz, 2022b). Given the healing positions and social connections that traditional healers hold within their communities, they can play a pivotal role in recognising and addressing ID among community members (Aldersey et al., 2016; Kpobi & Swartz, 2019; Masulani-Mwale et al., 2016; Mkabile & Swartz, 2022b). They are uniquely positioned to lead transformative conversations about the social exclusion and discrimination faced by persons with ID, which can lead to dismantling the stigma and prejudice associated with ID, thus fostering a more inclusive environment (Kpobi & Swartz, 2019). These findings align with previous studies emphasising the advantages of collaborative efforts between traditional healers and Western-trained healthcare professionals in mitigating healthcare disparities, combatting stigma, and uplifting the community (Mkabile & Swartz, 2020, 2022b).
Additionally, traditional healers raised their concern about the government's perceived preference for the approaches employed by the biomedical sector. This preference translated into substantial support for Western medicine, leaving traditional healers with inadequate funding, facilities, equipment, and training opportunities (Devenish, 2005; Mokgobi, 2013; Sorsdahl & Stein, 2010). Hence, traditional healers emphasised the need for access to resources to empower them, alleviate their challenges, and protect and recognise indigenous knowledge. The current lack of recognition and support from the government further isolates traditional healers from the formal healthcare system. Recognition goes beyond mere acknowledgement; it encompasses legal status, inclusion in the Council of Medical Scheme, and access to resources that could enhance traditional healing practices (Devenish, 2005; Nxumalo et al., 2011; Vawda, 2019). They believed that government recognition at a broader level could enhance the partnership between traditional healers and medical professionals. Hence, traditional healers further stressed the significance of government recognition, formalised structures, unity, and co-referral with biomedical professionals to promote collaboration in healthcare. Significant literature has supported the requirement of a co-referral system (Campbell-Hall et al., 2010; Green & Colucci, 2020; Kokota et al., 2022; Musyimi et al., 2016; Shields et al., 2016). Co-referral practices already exist in some other countries. Tan and colleagues (2021) found that in Rwanda, hospitals referred patients to traditional healers when they recognised that they were suffering from culture-specific illnesses to ensure that they were treated adequately, thereby acknowledging their expertise. However, in the extant literature, biomedical practitioners are unwilling to refer patients back to traditional healers due to their perceptions of them posing a challenge to effective collaboration (Mokgobi, 2013; Sorsdahl & Stein, 2010).
Traditional healers approach healing from a deeply spiritual and holistic perspective, guided by ancestral spirits and spiritual elements (Adu-Gyamfi & Anderson, 2019; Galvin et al., 2023; Haque et al., 2018). In contrast, Western doctors undergo extensive formal medical education and training and approach healing from a scientific and evidence-based perspective (Finkler, 1994). Traditional healers begin by consulting their ancestors, whereas Western doctors rely on patient consultations and scientific methods (Adu-Gyamfi & Anderson, 2019; Finkler, 1994; Galvin et al., 2023; Haque et al., 2018). The divergence in approaches and foundational beliefs about healing results in a profound gap in understanding between the two systems (Sorsdahl & Stein, 2010). Traditional healers feel that their knowledge and expertise are undervalued due to Western-trained doctors’ inability to accept their practices (Keikelame & Swartz, 2015; Mokgobi, 2013). This scepticism about traditional healers’ ability to treat patients erodes trust between the two, thus creating a barrier to effective collaboration (Lampiao et al., 2019; Mokgobi, 2013). Traditional healers also expressed reservations about the motivations of Western doctors and the pharmaceutical industry, suggesting that profit making takes precedence over genuine healing. This finding was consistent with a study carried out by Sorsdahl and Stein (2010) on traditional healers’ perceptions of referral. This perception adds to the mistrust between the two sectors, particularly regarding pharmaceutical interventions. However, traditional healers experienced a willingness to collaborate when rapport was built, and they experienced reciprocity and respect when they had the opportunity to engage and develop the relationship, and were treated as equals (Kokota et al., 2022; Peu et al., 2020). Many traditional healers suggested that learning about each other's perspectives was vital in mitigating this as it could bridge the understanding between the systems. Despite differences within the interventions, rapport building was a vital key to supporting collaboration and circumventing the challenges of divergent healing practices and approaches. Rapport is also a powerful antidote to traditional healers’ perceptions of biomedical healthcare workers’ poor attitudes towards them. Cultural competence and sensitivity regarding values and norms, and speaking the local languages, have been cited as helpful in rapport building with traditional healers (Peu et al., 2020). Successful rapport building in the intervention could thus be understood as partly facilitated by the nature of the mother study, being participatory action research, the Xhosa Western-trained workers, and a fieldworker who is a community leader and traditional healer (Peu et al., 2020).
Interestingly, our study found that internal challenges, specifically disunity and distrust among traditional healers, act as barriers to effective collaboration with Western-trained practitioners. This may make Western-trained practitioners hesitant to trust and cooperate with traditional healers (Lampiao et al., 2019). The inherent heterogeneity among traditional healers presents a substantial challenge in terms of organisation and regulation, which are essential prerequisites for accessing state resources, conducting research, and receiving training, as stipulated by the government (Devenish, 2005). Literature has cited concerns regarding traditional healers’ lack of regulation and accountability (Campbell-Hall et al., 2010; Green & Colucci, 2020; Keikelame & Swartz, 2015). While willing to consider regulation, traditional healers recognise its limitations of their autonomy and how government-imposed rules and regulations may not align with their spiritual practices and traditions. Therefore, they remain apprehensive about fully disclosing their healing methods, as it may violate their spiritual laws (Muller & Steyn, 1999; Pouchly, 2012). In line with recommendations in the literature, the traditional healers, however, showed a desire to establish a suitable, bottom-up regulatory framework to authenticate traditional healers, ensure accountability, and aid in being formally incorporated into the healthcare system (Campbell-Hall et al., 2010; Hopa et al., 1998; Tan et al., 2021).
Limitations
Firstly, a small sample restricted to Khayelitsha in Cape Town, South Africa, was utilised, therefore the results cannot be generalised to the entire population of traditional healers. Secondly, sampling bias could have occurred due to the use of a fieldworker who helped with the recruitment of participants—he may have recruited members known to him. Some participants opted to speak in English to accommodate one of the principal researchers, which may have hindered their ability to fully articulate and express themselves. Lastly, participants being compensated for their time and them perceiving researchers as representatives of the Western biomedical sector may have induced social desirability bias.
Conclusion
Traditional healers were willing to collaborate for ID support provision in Khayelitsha, viewing it as beneficial and essential. While perceived negative attitudes from Western-trained practitioners and differences in practices and approaches pose challenges to collaboration, establishing rapport at multiple levels of the ecology can counteract these. Furthermore, increasing access to resources for traditional healers, and formally including traditional healing in governmental, educational, and medical institutions, would address the significant barriers that systematic disparities pose to collaboration. Additionally, bottom-up regulations, guidelines, and working practices for collaboration should be established and implemented, and community structures and projects should be invested in to support the community directly. Future research can conduct more synergised pilot studies within communities for ID support provision, ascertaining the views and experiences of collaboration from both systems, and generating emic studies and documentation of African spirituality and traditional healing practice. Advocacy research to correct systemic disparities and promote a practical recognition of traditional healing is also imperative.
Footnotes
Acknowledgements
We would like to sincerely thank the traditional healers from Khayelitsha, Western Cape, South Africa, whose valuable insights are integral to this study.
Funding
The research project whose data this manuscript reports was funded by the South African National Research Foundation (NRF).
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
